Ophthalmology
ataGlance
J. OLVER & L. CASSIDY
Ophthalmology at a Glance
Ophthalmology
at a Glance
JANE OLVER
DO, FRCS, FRCOphth
Consultant Ophthalmic, Oculoplastic and Orbital Surgeon
Honorary Senior Lecturer in Ophthalmology
Charing Cross Hospital and Imperial College, London
and the Western Eye Hospital, London
LORRAINE CASSIDY
DO, FRCSI, FRCOphth
Consultant Ophthalmologist, Neuro-ophthalmologist and Oculoplastic Surgeon
Professor of Ophthalmology, Trinity College, Dublin
The Royal Victoria Eye and Ear Hospital, Dublin
The Adelaide and Meath Hospital, incorporating the National Childrens’ Hospital, Dublin
Blackwell
Science
© 2005 by Blackwell Science Ltd
a Blackwell Publishing company
Blackwell Science, Inc., 350 Main Street, Malden, Massachusetts 02148-5020, USA
Blackwell Publishing Ltd, 9600 Garsington Road, Oxford OX4 2DQ, UK
Blackwell Science Asia Pty Ltd, 550 Swanston Street, Carlton, Victoria 3053, Australia
The right of the Author to be identified as the Author of this Work has been asserted in
accordance with the Copyright, Designs and Patents Act 1988.
All rights reserved. No part of this publication may be reproduced, stored in a retrieval system,
or transmitted, in any form or by any means, electronic, mechanical, photocopying, recording
or otherwise, except as permitted by the UK Copyright, Designs and Patents Act 1988, without
the prior permission of the publisher.
First published 2005
Library of Congress Cataloging-in-Publication Data
Olver, Jane.
Ophthalmology at a glance / Jane Olver.
p. ; cm.
ISBN-13: 978-0-632-06473-1
ISBN-10: 0-632-06473-0
1. Ophthalmology —Outlines, syllabi, etc.
2. Ophthalmology —Examinations,
questions, etc. [DNLM:
1. Eye Diseases —Examination Questions.
2. Ophthalmology —methods —Examination Questions. WW 18.2 O52o 2005]
I. Cassidy, Lorraine. II. Title.
RE50.O45 2005
617.7 —dc22
2004011464
ISBN-13: 978-0-632-06473-1
ISBN-10: 0-632-06473-0
A catalogue record for this title is available from the British Library
Set in 9/11.5 Times by SNP Best-set Typesetter Ltd., Hong Kong
Printed and bound in India by Replika Press PVT. Ltd
Commissioning Editor: Fiona Goodgame, Vicki Noyes
Development Editor: Geraldine Jeffers
Production Controller: Kate Charman
For further information on Blackwell Publishing, visit our website:
The publisher’s policy is to use permanent paper from mills that operate a sustainable forestry
policy, and which has been manufactured from pulp processed using acid-free and elementary
chlorine-free practices. Furthermore, the publisher ensures that the text paper and cover board
used have met acceptable environmental accreditation standards.
Contents
Preface 6
25.
Common eyelid malpositions 56
Acknowledgements 7
26.
Lacrimal (tearing) 58
27.
Basic orbital assessment 60
Section 1: Principles of ophthalmology
28.
Orbital and thyroid eye disease 62
1.
Introduction: what is ophthalmology? 8
2.
Medical student aims 10
Section 9: Sub-specialty —External eye disease
3.
Social and occupational aspects of vision 12
29.
Common conditions affecting the external eye 64
30.
Common conditions affecting the cornea 66
Section 2: Ophthalmic history and examination
31.
Therapeutic contact lenses 68
4.
Taking the history and recording the findings 14
32.
Corneal and laser photorefractive surgery 70
5.
Visual acuity in adults 16
6.
Examination of visual fields 18
Section 10: Sub-specialty —Corneal, refractive and
7.
Other visual functions 20
cataract surgery
33.
Cataract assessment 72
Section 3: Correction of refractive errors
34.
Cataract surgery 74
8.
Basic optics and refraction 22
35.
Cataract surgery postoperative care 76
9.
Glasses, contact lenses and low-vision aids 24
Section 11: Sub-specialty —Glaucoma
Section 4: Basic eye examination
36.
Glaucoma—the basics 78
10.
External eye and anterior segment 26
37.
Detecting glaucoma 80
11.
Posterior segment and retina 28
38.
Medical and surgical treatment of glaucoma 82
12.
Use of eye drops 30
Section 12: Sub-specialty —Vitreoretinal and medical retina
Section 5: Acute ophthalmology
39.
Retinal detachment 84
13.
The red eye 32
40.
Retinal and choroidal anatomy and imaging 86
14.
More on the red eye 34
41.
Inherited retinal dystrophies and age-related macular
15.
Ophthalmic trauma principles and management of chemical
degeneration 88
injuries 36
42.
Diabetic retinopathy classification and typical lesions 90
16.
Specific features of blunt and sharp injuries 38
43.
Diabetic retinopathy treatment 92
17.
Sudden painful loss of vision in a non-inflammed eye 40
44.
Retinal vein occlusion 94
18.
Sudden painless loss of vision 42
45.
Retinal artery obstruction 96
46.
HIV infection and AIDS 98
Section 6: Gradual loss of vision
19.
Gradual loss of vision 44
Section 13: Sub-specialty—Neuro-ophthalmology
47.
Pupil abnormalities 100
Section 7: Sub-specialty —Paediatric ophthalmology
48.
Optic nerve disease 102
20.
Visual acuity in children 46
49.
Cranial nerve palsies and eye movement disorders 104
21.
Strabismus (squints) 48
50.
Visual fields defects 106
22.
Neonates 50
23.
Infants and older children 52
Appendix: Red eye 108
Section 8: Sub-specialty —Eyelid, lacrimal and orbit
Index 109
24.
Common eyelid lumps 54
5
Preface
This book is intended primarily for medical students and junior
time that Lorraine Cassidy was about to go to Dublin to become
doctors preparing for examinations (regardless of whether they
Professor of Ophthalmology. Slowly we gathered together a team
are medical or surgical). In addition we hope that general practi-
of colleagues and friends who over 2-3 years all pulled together —
tioners and non-ophthalmic consultants who care for patients with
were cajoled? —into writing this book. As editors we have knitted
eye diseases will find this book invaluable in its simplicity and clar-
together our own and their contributing work. We are incredibly
ity. We have tried to create a balanced, up to date, practical book.
grateful to everyone who made this book a reality.
Blackwell’s have supported our need for extensive colour pictures
and diagrams which characterize this ‘visual’ subject.
Jane Olver and Lorraine Cassidy
Ophthalmology at a Glance took form in London around the
London and Dublin, 2004
6
Acknowledgements
In particular we want to thank Susie Downes and her team, es-
tact lenses), Suzanne Mitchell (HIV), Jonathan Barnes (arterial
pecially Raman Malhotra and also Damien Louis and Anne
and venous occlusion) and Mandeep Sagoo (ocular oncology).
Boulton, for several of the medical retinal chapters —retinal imag-
Others helped at the beginning including Jane Leitch, and towards
ing, age-related macular degeneration, retinal dystrophies, diabet-
the end, Roger Armour, Kuki Hundal, Jod Mehta,Arosha Fernan-
ic retinopathy —all vital subjects. We thank Anthony Kwan for his
dez, Mona Loufti, Nicholas Lee, Karl Southerton, Vickie Lee,
chapters with wonderful photos on the red eye, eye drops and ad-
Bijan Beigi, Graham Duguid, Eamon Sharkawi, Hugh Nolan and
ditional photos of cataract surgery, Siedel positive, etc. We also
Donal Brosnahan who baled us out with last-minute pictures we
want to thank Dilani Siriwardena for her enormous contribution
couldn’t find anywhere. The Medical Illustration Departments at
to the Glaucoma chapters, similarly Jugnoo Rahi (social and occu-
the Charing Cross Hospital and the Royal Victoria Eye and Ear
patinal aspects), Bernadette MacCarry (orthoptics), Veronica
Hospital in Dublin were very supportive. Lastly, Lorraine’s nieces
Ferguson (cataract), Raj Maini and Ursula Vogt (corneal and con-
had a star role as actresses in the orthoptic department.
7
1 Introduction: what is ophthalmology?
The medicine and surgery of the eye and its surrounding structures and connections to the brain,
in order to maintain clear, pain-free and useful vision with an aesthetic attractive appearance
Normal female appearance with arched high eyebrow
Normal male eye with straighter lower eyebrow
Supracilia
Pupil
Lid fold
Cornea
Caruncle
Limbus
Medial canthus
Upper punctum
Plica
Lower punctum
Cilia
Lash line
Lateral canthus
Lid margin
Sub-specialties
Paediatric ophthalmology and strabismus
Oculoplastic, lacrimal and orbital surgery
External eye disease
Lower lid entropion
Conjunctivitis
Paediatric ptosis
Vitreo-retinal surgery
Corneal, refractive and cataract surgery;
Glaucoma
contact lenses
Dendritic ulcer
Goldmann tonometry
Retinal detachment
Medical retina
Neuro-ophthalmology
Vision is central to the way we live; our social world,
education, mobility and ability to communicate all
depend on clear vision. The eyes and the face are
important for interpersonal communication -
‘the eyes are the window of the soul’.
Economically, many occupations are dependent on
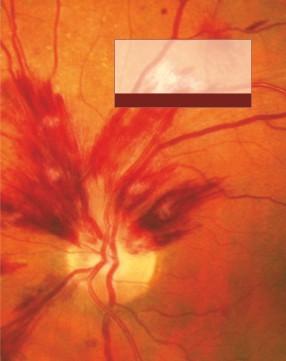
Occluded retinal arteriole
precise visual requirements
Pituitary tumour
8 Principles of ophthalmology
What is ophthalmology?
before you are allowed to do intraocular surgery. A certificate of
Ophthalmology is a large subject for a very small area: it is the
eligibility is required from one of the Royal Colleges before
medical and surgical care of the eye, the adjacent adnexal and
entering Higher Surgical Training (HST) (4.5 years duration),
periocular area and the visual system. It encompasses the upper
which provides experience in all the sub-specialties. There is exit
and mid face, eyebrows and eyelids, lacrimal system and orbit,
assessment before being awarded the Fellowship in Ophthalmol-
as well as the globe and eye muscles, optic nerve and nervous
ogy (FRCOphth, FRCSEd(Ophth)) and Certificate of Com-
connections all the way back to the visual cortex. Many medical
pletion of Specialist Training (CCST) necessary to be placed on
conditions have ocular features as their first presentation, e.g.
the Specialist Register. Advanced Subspecialist Training (ASTO)
in diabetes, cardiovascular disease, rheumatology, neurology,
towards the end of HST offers further sub-specialty training.
endocrinology and oncology. There is overlap with maxillofacial,
Training will be shortened with the introduction of Foundation
plastic, otolaryngology and neurosurgery and strong links with
Training and a subsequent unified training grade.
dermatology with Mohs’ micrographic surgery for excision of
periocular skin tumours. There are links with neuroradiology and
Membership examination: MRCOphth, MRCSEd
pathology. It combines medical and surgical skills and uses mini-
Part
1 Basic sciences. General physiology and pharmacology. Ocular
mally invasive microsurgery and lasers as well as delicate plastic
anatomy, physiology, embryology, pharmacology. No clinical experience in
surgical techniques.
ophthalmology needed to sit.
Part 2 (i) Optics and refraction. (ii) Assessment of clinical methods. One year’s
Type of patients
experience as SHO required. The practical refraction is the hardest part.
Predominantly the very young and the elderly. Also, middle-aged
Part 3 Clinical ophthalmology including microbiology, histopathology, medi-
patients with thyroid eye disease, diabetes or inherited disorders.
cal and neurology clinical examination. Eighteen months’ experience as SHO
Ophthalmic trauma affects particularly the young adult. Very few
required. The medical and neurology parts are the most difficult.
eye patients become ill and die. Most remain ambulatory and are
seen as out patients or have day-case surgery.
Team
Colleges
General practitioners, eye casualty officers, hospital ophthalmolo-
gists, medical physicists, optometrists, orthoptists and ophthalmic
nurse practitioners, all collaborate in the investigation and man-
agement of ophthalmic patients.
Education website
Sub-specialties
The eye can be subdivided into several sub-specialty areas. Some
eyeanat.html
ophthalmologists practice general ophthalmology alone; although
most have a significant sub-specialty interest. Sub-specialties
Eye associations
include:
• Paediatric ophthalmology and strabismus
• American Associated Ophthalmic Plastic and Reconstructive Surgery:
• Oculoplastic, lacrimal and orbital (including oncology).
• External eye disease including contact lenses.
• American Association Paediatric Ophthalmology and Strabismus:
• Cornea and refractive surgery, cataract.
• Glaucoma.
• Association for Research Vision and Ophthalmology: www.arvo.org
• Vitreoretinal surgery.
• Medical retina.
• Neuro-ophthalmology.
• Intraocular microsurgery.
Further reading
1 The Wills Eye Manual. Office and Emergency Room Diagnosis and Treat-
How to get into ophthalmology
ment of Eye Disease. Douglas J. Rhee and Mark F. Pyfer.
Good eye-hand coordination helps if you want to do micro-
2 Clinical Anatomy of the Eye. Richard S. Snell and Micheal A. Lemp.
surgery and there are ample opportunities for people with good
3 Ophthalmology. An Illustrated Text. M. Batterbury and B. Bowling.
medical skills to practice medical ophthalmology, including neuro-
4 ABC of Eyes. P.T. Khaw and A.R. Elkington.
ophthalmology, medical retina and glaucoma, or to conduct oph-
5 Pocket Book of Ophthalmology. Philip I. Murray and Alistair Fielder.
thalmic research. Examination hurdles are hard. Details of Basic
Specialist Training and Higher Specialist Training curricula are ob-
tainable from the Royal Colleges. Getting Part 1 MRCOphth
KEY POINTS
helps you obtain your first Senior House Officer (SHO) post. Do
• Ophthalmology is multidisciplinary.
Part 2 and 3 whilst an SHO in Basic Surgical Training (BST) (2
• Interfaces with medicine.
years minimum in recognized posts).You have to attend the Royal
• Involves microsurgery.
College of Ophthalmologists’ Basic Microsurgical Skills course
Introduction: what is ophthalmology? 9
2 Medical student aims
Systematic approach
topics are covered. Try and cover the items identified in this chap-
The time spent in ophthalmology is very short so a systematic ap-
ter and refer back to it as a check list.
proach is needed in order to ensure that the necessary skills and
Aim: The aim of this book is to provide a balanced understanding of clinical ophthalmology and equip
Essential ophthalmic skills
the medical student with the knowledge and skills to identify, treat or refer common eye disorders
You MUST be able to:
1 Take an ophthalmic
2 Measure visual acuity
3 Detect an abnormal pupil
history
6/60
E
6/36
N
D
6/24
H C U S
6/18
A
O HTGL
6/12
B D R L G P N
6/6
W R H M S Q X
4 Examine eye movements
and detect a squint
Look straight
5 Examine the red reflex
6 Perform a confrontational
visual field test
Look right
Dx= R incomitant
Ophthalmoscope
squint
Look straight
Look right
Dx= R comitant
squint
7 Examine the fundus
7ii Detect diabetic retinopathy and hypertensive retinopathy
8 Recognize common
ophthalmic conditions
e.g. Meibomian cyst (chalazion)
7i Identify a normal disc
7iii Identify glaucomatous cupping and papilloedema
9 Recognize ophthalmic
emergencies
e.g. acute angle-closure glaucoma
Glaucomatous cupping
Papilloedema
10 Principles of ophthalmology
Aims
Things to do when you visit the eye department
The aim of this book is to provide a balanced understanding of
1 Attend: (i) a general eye or primary eye clinic, and (ii) a special-
clinical ophthalmology and equip the medical student/physician
ist eye clinic.
with the knowledge and skills to identify, treat or refer common
2 Attend an eye casualty clinic.
eye disorders.
3 Observe an orthoptist assessing ocular motility in a child or
adult.
Core knowledge
4 Observe an automated visual field test being done.
A basic understanding of:
5 Watch a phaco-cataract extraction operation.
• ocular physiology and pharmacology;
6 Watch an eyelid lump being incised or excised, e.g. incision and
• neuroanatomy;
curettage (I&C) of a chalazion or biopsy of a basal cell carcinoma.
• optics.
7 See retinal lasering for diabetic retinopathy or maculopathy.
Medical student objectives
There are essential ophthalmic skills such as taking a history, use-
Essential clinical topics
ful practical skills such as putting in eye drops, things to do when
You must know about the following topics.
you visit the eye department such as watch a visual field being
1 Differential diagnosis of a red eye (Chapters 13 and 14).
done and, lastly, essential clinical topics such as the red eye.
2 Management of an eye injury (Chapters 15, 16 and 28).
3 Differential diagnosis of visual loss (Chapters 17-19).
Essential ophthalmic skills —see figure
4 Orbital cellulitis (Chapter 23).
1 Take an ophthalmic history.
5 Differential diagnosis of a leucocoria (Chapter 22).
2 Measure visual acuity using Snellen and Logmar charts, with
6 Differential diagnosis of a watery eye in childhood (Chapters 22 and 23).
and without a pinhole.
7 Recognition of thyroid eye disease (Chapter 27).
3 Detect an abnormal pupil, e.g. fixed dilated pupil, Horner’s
8 Management of diabetic retinopathy (Chapter 43).
pupil or afferent pupillary defect.
4 Examine the eye movements and extraocular muscle function.
Detect a squint using the cover test. Differentiate between a para-
lytic and non-paralytic squint.
KEY POINTS
5 Examine the red reflex and recognize leucocoria.
• Visit the eye department and theatre.
6 Perform a confrontation visual field test, and detect a bitempo-
• Know essential clinical topics.
ral hemianopia and homonymous hemianopia.
• Gain essential practical skills.
7 Use a direct ophthalmoscope to: (i) examine the fundus and
identify a normal disc; (ii) detect diabetic retinopathy and hyper-
tensive retinopathy; and (iii) detect papilloedema, glaucomatous
cupping of the optic nerve head and a pale disc with optic atrophy.
8 Recognize common ophthalmic conditions, e.g. benign eyelid
chalazion and malignant eyelid basal cell carcinoma.
9 Recognize ophthalmic emergencies, e.g. acute closed-angle
glaucoma, and central retinal artery occlusion.
Additional useful practical skills
You may only do a few of these during your training. Try and do at least points
1-5.
1 Instil eye drops.
2 Evert an eyelid.
3 Examine the eyelids, conjunctiva and cornea with a torch, magnifying aid
and slit lamp.
4 Examine cranial nerves including the corneal reflex.
5 Put in or take out a contact lens or eye prosthesis.
6 Detect a lacrimal sac mucocoele.
7 Detect a dendritic ulcer.
8 Remove a foreign body from the conjunctiva and cornea.
9 Irrigate an eye contaminated with a chemical.
10 Assess colour vision.
Medical student aims 11
3 Social and occupational aspects of vision
Blindness is a severe form of visual impairment and must be defined. The WHO classification helps:
World Health Organisation (WHO) Classification of Visual Impairment and Blindness
Category of vision
Level of visual impairment
Visual acuity in better eye with optical correction
Normal vision
Slight if visual actuity <6/7.5 (20/30)
6/18 (20/40) or better
Low vision
Visual impairment (VI)
Vision between 6/18 and 6/60 (20/40-20/100)
Definitions:
Low vision
Severe visual impairment (SVI)
Vision between 6/60 and 3/60 (20/100-20/300)
BL = Blind
Blindness
Blind (BL)
Less than 3/60 to no light perception or
SVI = Severely visually impaired
visual field ≤ 10° around central fixation
VI = Visually impaired
Economic impact of reduced vision
A visual acuity of 6/12 (20/30) or worse in the better eye excludes entry into the following occupations:
Driving including
Entry to armed forces
taxi drivers
Fire brigade
Entry to the police force
DVLA Visual Standards for Driving for ordinary driving licence
N.B. Professional and Vocational licence eyesight regulations are stricter for
Large Goods Vehicle (LGV) and Passenger Carrying Vehicle (PCV) licences
Visual acuity: ‘read in good light (with the aid of glasses or contact lenses
if worn) a registration mark fixed to a motor vehicle and containing letters
and figures 79.4 mm high at a distance of 20.5 m’. This is equivalent to
between 6/9 (20/25) and 6/12 (20/30)
Visual fields: ‘a field of vision of at least 120° on the horizontal measured
by a Goldman perimeter using a III4e target setting (or automated
Bus driver
perimetry equivalent), with no defect in binocular field within 20° of
fixation above or below fixation, i.e. total 40°’
A patient can have diplopia in extremes of vision and still be allowed to drive.
If in doubt, the patient should contact the DVLA
For LGV and PCV a minimum vision of 3/60 unaided, in each eye, is required,
as long as it corrects to 6/9 in the better eye and 6/12 in the worst eye -
monocular driving or any field defect is a contraindication
Pilot
12 Principles of ophthalmology
Aims
A visual acuity of worse than 6/12 in the better eye in adults can be
1 Different needs of developing and industrialized countries.
considered ‘economic blindness’ as it:
2 Main causes of blindness in children and adults in industrialized
• precludes driving;
countries.
• prevents entry into certain occupations;
3 Visual requirements for driving.
• decreases ability to function in the workplace;
• increases risk of serious morbidity;
Size of the problem
• increases social isolation and the risk of psychological problems,
Worldwide
including depression;
• One adult becomes blind every 5 seconds and one child every
• decreases overall quality of life and is associated with increased
minute.
(doubling) overall risk of death.
• Approximately 45 million adults and 1.5 million children are
currently blind.
Services and support in the UK and Ireland (children and
• Visual impairment and blindness is very costly from loss of work
adults)
and managing and supporting them. The global cost of blindness
1 National registers of partial sight and blindness. Certification as
exceeds US$ 167 000 million.
partially sighted or blind (approximately equivalent to SVI/BL) is
• The WHO ‘Vision 2020 —the right to sight’ is a global initiative
voluntary. It is the main mechanism for ensuring access to statu-
for the elimination of avoidable (preventable or treatable) visual
tory economic benefits and relevant social services. It provides
impairment throughout the world, by the year 2020.
national data about levels of visual impairment.
Developing countries
• Most BL and SVI/VI people live in developing countries.
• Most affected individuals have preventable or treatable
conditions, due to infection or malnutrition.
TIPS: Certification of partially sighted or blind
• There is often poor access to treatment, e.g. cataract.
1 Both visual acuity and visual field are considered.
2 A patient can be SVI or BL in one eye and even have a prosthetic eye, but if
Industrial countries
the other eye sees 6/12 with a good visual field, they cannot be registered par-
Most preventable blinding diseases have been eliminated.
tially sighted or blind.
United Kingdom / industrialized countries
Children
• Approximately 1 per 1000 children is VI or BL —equivalent to
35-45 children in an average-sized urban health district.
2 Statement of Educational Needs (SEN). It is a UK legal re-
• There may be learning, hearing, speech/language or mobility
quirement to assess and regularly review the educational needs of
impairment.
children with SVI in a ‘Statement of Educational Needs’. Children
• Major causes of childhood visual disorders include:
registered blind in Ireland are assessed by the visually impaired
—visual pathway or cerebral visual impairment;
assessment team (VICAT).The SEN or VICAT report determines
—inherited retinal dystrophies;
the educational placement, support and facilities provided by the
—congenital cataract and other ocular anomalies such as
government.VI children are educated in mainstream schools with
microphthalmos, and optic nerve hypoplasia and atrophy;
support from an advisory teacher; special visual impairment units
—retinopathy of prematurity.
integrated within mainstream schools; schools and colleges for the
• Profound impact on all aspects of the child’s development, their
visually impaired; or residential schools for children with special
family and management by professionals.
needs.
• Affects educational, employment and social prospects.
• Although many of the disorders are untreatable, affected
children may benefit from visual rehabilitation with low-vision
aids and specific educational or developmental interventions.
Useful websites
Adults
The incidence and major causes of partial sight or blindness certi-
fication in the UK at various ages are given in the table below.
• National Council for the Blind of Ireland: www.ncbi.ie
Age in
Incidence per 100 000
years
per year
Major causes of VI and BL
16-64
13
Diabetic retinopathy
Macular degeneration
KEY POINTS
Hereditary retinal disorders
• Diabetic retinopathy is the commonest cause of blindness in the working
Optic atrophy
age group.
65-74
122
Age-related macular
• Age-related macular degeneration accounts for over 50% of blind or par-
degeneration (AMD)
tially sighted registrations in Western Europe and the USA.
75-84
471
Glaucoma
85 and over
1038
Cataract
• Both good visual acuity and field of vision are necessary for driving.
Social and occupational aspects of vision 13
4 Taking the history and recording the findings
Record history and examination: Ophthalmologists use a standard format with accepted abbreviations and notation. The findings
for the patient’s right eye are recorded on the left hand side of the page and for the left eye on the right side (vice versa for fields)
Name: John Smith
Hospital No. 12345
DOB: 23/01/32
Age: 70 y/o
Date: 04/05/02
PC
Slow progressive loss of RVA
Not improved with new spectacles
HPC
Started 3 years ago with glare caused by oncoming car lights when driving at night
Vision then gradually deteriorated and now can hardly see with R eye
POH
Nil
FH
Brother with DM
PMH
NIDDM x 20 years No hypertension
Meds
Daonil 2.5 mg mane
Eye drops - nil
Allergies - NKA
SH
Cigs + 10 per day
O/E
VR
6/36 UA
VL
6/12 UA
6/24 PH
6/9 PH
N48 c + 2.00
Near
N8 c + 2.00
RAPD
RAPD
17/17
Ishihara
17/17
(see section on pupils)
Lids
Conj
white
white
Cornea
clear
clear
A/C
D&Q
D&Q
Lens
dense NS++
mild NS+
IOP
16
17
Fields
Full to confrontation
EOM
CT - Orthophoric
ROM - Full
Dilate - G Tropicamide 1% & Cyclopentolate 1%
Fundi
R
L
(see section on glaucoma)
(Hazy view)
CDR 0.3
Disc
CDR 0.3
no DR
Macula
no DR
BV's
Periph
Impression:
Right cataract
Surgery risks and benefits explained - pt would like op
Plan: W/L for Rt Phaco + IOL LA
(see section on cataract surgery)
14 Ophthalmic history and examination
Aims
Other medical conditions including multiple sclerosis, sarcoid, col-
1 Take a good ophthalmic history.
lagen disorders and inflammatory bowel disease may present with
2 Take a thorough medical history.
ophthalmic problems. Enquire about nasal disease such as sinusi-
3 Examine the eye in a systematic way.
tis and hayfever, trauma or surgery.
4 Record the eye examination in a standard fashion.
Medications
Firstly, always introduce yourself to the patient and explain who
• Ask ‘Are you taking any tablets/medication?’ (you may pick up
you are. It may be useful to record the patients’ vision before talk-
on diabetes or hypertension which wasn’t mentioned in the PMH,
ing to them, as getting an idea of their visual acuity and which eye
especially warfarin or blood-thinning medication).
is involved, helps you relate to their history better.
• Ask ‘Have you ever been on eye drops before?’ as they may
have had previous relevant conjunctivitis.
Structure of ophthalmic history
• Ask in particular about hormone replacement therapy and the
Presenting complaint (PC)
contraceptive pill, as both may play a role in the aetiology of ret-
The patient may not always volunteer information, and you
inal vascular occlusive disease. Ask about non-prescription drugs,
should ask ‘What is the problem with your eyes?’ or ‘What did
e.g. aspirin, which can be contraindicated during ophthalmic
you notice wrong with your vision?’ or ‘Do you know why the
surgery.
optometrist referred you?’ Sometimes the patient hasn’t no-
ticed anything wrong with their eyes and was referred by the
Social history
optometrist who noticed an abnormality during a routine eye
Does the patient smoke? How many? Smoking may be a causative
examination, e.g. early cataract or a pigmented area on the retina.
factor in retinal or optic nerve vascular occlusive disease and is a
Establish whether the PC is acute, e.g. sudden loss of vision.Ask
recognised risk factor in Graves’ ophthalmopathy and Leber’s
the patient to be specific about which eye is involved or whether it
optic neuropathy.
is both eyes —they may not be sure. Enquire about associated
symptoms such as headache, jaw claudication or temporal tender-
Review of systems (ROS)
ness which would point to a specific diagnosis such as temporal
As relevant.
arteritis.
If the problem is chronic, e.g. slowly developing bulgy eye
Systematic ophthalmic examination
(proptosis), ask the patient when they or their relatives first no-
Wash your hands first, especially if working in an ophthalmic
ticed it —ask them to bring photographs taken a few years earlier
emergency clinic where patients may have conjunctivitis.
for comparison and to help establish how long the problem has
• Visual acuity (see Chapter 5). When testing the distance vision,
been there.
ensure that if the patient has glasses, that they are wearing them!
And their reading glasses for near vision tests. Measure each eye
History of the presenting complaint (HPC)
separately! Use the pinhole if vision measures 6/9 or less.
• ‘When did the symptom first start?’
• Visual fields (see Chapter 6).
• ‘Constant or intermittent?’
• Colour vision, Amsler chart and pupils (see Chapter 7).
• ‘How many attacks/episodes?’
• Systematic examination. Observe the patient’s whole person,
• ‘Any associated features?’
speech and face as many tips can be picked up —myotonic dystro-
• ‘Getting worse, staying the same or improving?’
phy, facial palsy, Graves’ ophthalmopathy —as the patient walks
in.
Family history (FH)
Ask about eye conditions such as squint, glasses and glaucoma,
TIPS
childhood cataract, ocular tumours, any ‘eye disease’ and medical
• Do visual acuity and other function tests such as Ishihara colour, Amsler
conditions such as diabetes or hypertension.
chart, pupil reactions, visual fields, and eye movements first.
• Examine the eye from the front to the back. Start with the periocular area,
Past ocular history (POH)
lids, external eye, cornea, anterior segment, lens, vitreous, macula, retina and
Ask about previous eye problems, eye surgery or ‘lazy eye’
optic nerve head and measure the intraocular pressure.
(amblyopia).
• Start with the right then the left eye, even if the problem is on the left!
• Only dilate the pupils once you are sure you have established all the above.
Allergies
Enquire about drug allergies.
KEY POINTS
Past medical history (PMH)
• Establish if eye problem is acute or chronic.
Ask about diabetes, hypertension, irregular heart rate, asthma and
• Medical history is very important.
chronic obstructive airway disease (COAD) as beta-blockers used
• Always measure the visual acuity before dilating the pupils.
in drop form for glaucoma should be avoided in these patients.
Taking the history and recording the findings 15
5 Visual acuity in adults
Snellen charts
VA conversion chart
Europe
UK
USA
H
6/60
E
(LogMar)
6/6
20/20
0
P N
6/36
6/12
20/40
X U T
6/24
E
6/36
20/120
A H D F
6/18
E
6/60
20/200
1.0
E
Z A P F X
6/12
E
CF
20/400
U Z N X T A
6/9
E
E
D H T N F P Z
6/6
T Z D F X A H V
6/5
E
E
Principles of LogMar acuity
Standard Snellen
‘Illiterate E’
The LogMar chart has 10 lines, each with the same number of letters
Snellen
(5 per line). Each letter has an equal value of 0.02 LogMar units. If
the patient can read 3 of 5 letters on the line, take the score for the
line and add 0.02 per letter not seen (a higher score is worse)
Distance
acuity
LogMar chart
Near
We've spokenabout evidence-
N5
based design fromtime to time, how
N10
acuity
we use research to
We've spoken about evidence-baseddesign from time to time, how we use
We've spoken
research to shape our designdecisions, but I'm just wondering
about evidence-
N6
about the other side of the coin - howdo we *generate* evidence?
based design from
N12
time to time, how
We've spoken about
We've spoken
evidence-based designfrom time to time, how
about evidence-
TIP
N8
we use research to shape
based design from
N14
our design decisions, but
time to time, how
If the patient has an artificial eye (AE) /
ocular prosthesis record the vision as AE
Pinhole
Pinhole test:
If the subject's vision is improved with a pinhole
he/she may have a refactive error, early lens or
corneal opacities. If there is a retinal, optic nerve
or brain lesion, vision will NOT improve with a pinhole
Artifical eye
Aims
ence of small to moderate refractive errors. (See Chapter 8 for pin-
1 Measure distance and near visual acuity.
hole optics.)
2 Know why and how to use the pinhole test.
Distance and near vision
Definitions
VA must be measured, one eye at a time, for both distance and
• Visual acuity (VA): An objective measure of what the person
near type, with the patient wearing their best spectacle correction.
can see.
• Test the distance VA first.
• Pinhole test (PH): Simple optical test used to detect the pres-
• Always start with the right eye.
16 Ophthalmic history and examination
• If the eyelid is droopy (ptosis), use a finger to lift it gently above
• Ask the patient to read down the chart as far as possible.
the visual axis.
• Repeat for the other eye.
• Insert topical anaesthesia if needed, e.g. if with a painful corneal
• Use the pinhole (see Chapter 8) if the VA is less than 6/9. If a
abrasion and blepharospasm.
refractive error is revealed, this patient needs to be assessed for
The methods of vision testing described here can be used in
glasses.
children 6 years and older, but if an adult or an older child has a
• If the VA is worse than 6/60, even when using the pinhole, move
severe learning disability, then a method of vision testing appro-
the patient 3 m closer to the chart —if the top line is now read
priate to that individual should be used (see Chapter 20).
record the VA as 3/60.
• If the patient cannot see 3/60, sit them 1 m from the chart. If the
chart still cannot be seen, proceed to measure ‘counting fingers’
TIP
vision. Ask how many fingers are held up, and if an accurate re-
It is important to test both distance and near visual acuity; conditions such as
sponse, record as CF (counts fingers) and the distance measured.
age-related macular degeneration are often disproportionately worse for
• If CF cannot be seen, move your hand in front of the patient’s
distance.
eye and if movement is accurately seen, record a VA of HM (hand
movements), specifying the distance at which movement was seen.
• If hand movements are not perceived, shine a torch light into
the eye from various angles and record whether or not the patient
Distance vision
has PL (perception of light), from which direction it is perceived,
• Snellen acuity: this is the traditional chart. Snellen vision is
and the distance at which the torch was held.
measured at 6 m (Europe) or 20 feet (USA).
• If still no PL, record the vision in that eye as NPL (no perception
• LogMar acuity: this is increasingly being used for children and
of light).
patients with poor vision or contrast problems and is useful for re-
• NB, if a patient cannot read use the illiterate E test (see figure).
search and statistical analysis. The test is done with the patient 4 m
The patient is asked to indicate with his hand which way the E’s
from the chart.A LogMar score of 0 is normal, equivalent to 6/6 or
point.
20/20; a score of 1.0 is equivalent to 6/60.
Near vision
Principles of Snellen acuity
How to test near vision
The Snellen chart has letters but there are also versions with the
• Ask patient to wear reading glasses if owned.
‘illiterate E’ and numbers.
• Test each eye separately.
• The 6/6 (20/20) line is ‘normal’ vision —patients can often read
• Patient holds the near test chart at about 0.3 m to read the small-
the lower lines, 6/5 or 6/4, which is better than normal.
est print that they can comfortably see.
• The number above the line describes the distance the patient
• The smallest print is recorded as N4 or N5 and the print in-
is from the Snellen chart; 6/6 (20/20) means the patient is at 6 m
creases in increments to the largest, which is N48.
(20 feet).
• Some near reading test types use Jaeger type, which is similar
• The number below the line denotes which line is seen, e.g. 6/12
but is recorded as J and the number of the line read.
(20/40). At 6 m, the patient reads the fifth line down (the ‘12’ line).
• On the 6/6 (20/20) line each letter is constructed to subtend an
angle of 1 minute of arc at a testing distance of 6 m.
• On the 6/18 or 20/60 line each letter subtends an angle of 3
TIP
minutes of arc; the 6/60 (20/200) line 10 minutes of arc.
N8 is the most common size print in most books.
• Each line is constructed in a similar way, so that letters on the
6/18 line subtend an angle of 1 minute of arc if tested at 18 m from
the chart, and the 6/60 line at 60 m from the chart.
KEY POINTS
How to test distance Snellen VA
• Test each eye separately.
• Patient sits 6 m from the chart.
• Assess VA before dilating the pupil and before shining a bright light into
• Distance glasses are worn.
the eye.
• Occlude one eye completely using the palm of their hand or an
• Test with a pinhole to detect a refractive error.
eye occluder.
Visual acuity in adults 17
6 Examination of visual fields
The visual fields are always mapped denoting the left field on the L side of the page and
the right field on the R side - in other words the fields are represented as the patient’s
field actually is as they look at the page. (Have your own fields plotted by the
orthoptist in the eye department if she has time and this way you won’t forget!)
Normal visual field
Left
Right
60° Superior
60°
60°
Nasal
Temporal
Temporal
Nasal
100°
10
20 30 40 50 60
70
80
60°
60°
80
70
60 50 40 30 20
10
100°
75°
100°
60°
75°
75°
Test right eye
NB Head heights are LEVEL for test
Red hat pin
Patient
Examiner
(a)
(b)
(c)
(d)
Now test left eye
TIP
Some elderly patients, and patients on
antiepileptic drugs may have a slightly
delayed reaction with confrontation field
testing - don’t be fooled into thinking
they have constricted fields, move the
target slowly to allow for this
(e)
Humphrey
automated
For abnormal field findings see Chapters 36 and 50
field analyser
Aim
• Test visual fields by confrontation for detecting gross abnormal-
Examine a visual field by confrontation.
ities and neurological problems.
• Automated static perimetry is very sensitive and therefore bet-
Visual field
ter for detecting more subtle defects such as those seen in early
The visual field is a map representing the patient’s retina, optic
glaucoma (see Chapters 36 and 37).
nerve and central visual system.
In your final exam you may be asked to examine the patient’s
18 Ophthalmic history and examination
visual fields by confrontation. You should also be aware of
the patient if he can see your face clearly, or if any bits appear to be
other methods of plotting visual fields, in particular the
missing.This will pick up any gross field defects (e.g. if there is a left
Goldmann, Humphrey and Esterman automated field analysers.
homonymous hemianopia, the right side of your face will be miss-
The Esterman binocular visual field is useful for driving licence
ing or blurred).
purposes (see Chapter 3).
• Now present your target equidistant between yourself and the
patient, starting outside the field of vision in the superotemporal
Normal field of vision
quadrant of the visual field (a), and bring it slowly in towards the
In individuals with normal, healthy visual pathways, a typical map
centre, keeping the target equidistant between yourself and the
of the visual field is represented pictorially. There is a blind spot
patient at all times.
temporally in each field —this represents the optic nerve.
• Maintain fixation on the patient’s right eye and make a mental
note of when you first see the target in your peripheral field; com-
pare this with when the patient can first see the target. You should
WARNING
both become aware of the target at the same time if there is no
A person with poor visual acuity (e.g. as a result of cataract) will have a normal
field defect.
visual field if the visual pathways are intact, but will require a large target in
• Now repeat in the inferotemporal (b), inferonasal (c) and
order for their fields to be plotted. Don’t be fooled into believing that a patient
superonasal quadrants (d).
with poor acuity has field loss because you have used a target which is too
small —assess visual acuity for near and distance with glasses first.
TIP
An alternative method that can be used if the patient’s acuity is too poor to vi-
Examination technique
sualize the target is to present 1, 3 or 4 fingers in each quadrant of the visual
Necessary equipment for confrontational field examination: a red
field while the patient looks straight ahead (avoid 2 fingers so as not to offend).
hat pin is best, but a biro with a red cap will do. Red desaturation is
an early sign of visual pathway compression.
Ask the patient how many digits he can see out of the corner of his eye (vary
the number of fingers in each quadrant).
• Introduce yourself to the patient and ask him if he would mind
you performing an examination of his ‘side’ or peripheral vision.
• Show the patient the target you will be using and ask if he can
see it at a distance of 0.5 m.
• Check the blind spot (if the patient has an obvious homony-
• If the patient cannot see the target at that distance, ask if he can
mous hemianopia, altitudinal field defect, bitemporal hemianopia
see where your fingers are, and if so use them as your target as
or grossly constricted fields, there is no need to assess the blind
described below.
spot). Examine one eye at a time. Ensure stable eye fixation at all
• If your fingers are not visible, use a pen torch.
times. Slowly bringing a small target (hat pin is best here) from the
• Sit 1 m in front of the patient with your eyes and the patient’s
centre, on a straight line towards the temporal periphery (e). Ask
eyes at the same level.
the patient to indicate when the top of the hat pin disappears, and
• Always examine the right eye first to avoid any confusion.
when it reappears. Compare with your own blind spot.
• Ask the patient to cover his left eye (make sure it is comple-
• Now examine the left field.
tely occluded), and if this is not possible, cover the eye with an
occluder.
• Ask the patient to look at your left eye and not to look for the
KEY POINTS
target. Explain that you are examining ‘side’ or peripheral vision
• Confrontation visual field tests are good for marked field defects, but are
and instruct the patient to say ‘yes’ whenever he becomes aware of
unlikely to detect subtle field changes.
the target in his peripheral vision (or ‘out of the corner of his eye’),
• Goldmann fields are best for neurological defects.
making sure that their eye gaze is maintained on your left eye at all
• Automated perimetry is best to detect and monitor glaucomatous field
times.
defects.
• Before you start testing peripheral vision with a small target, ask
Examination of visual fields 19
7 Other visual functions
Left posterior pole - optic nerve transmits all retinal
nerve fibres centrally. Macula has dense cones
Colour vision testing is a NEAR VISION TEST - patient must have their
reading spectacles on
Copyright S Downes
Do colour vision tests before shining a bright light in the patient’s eyes
and before dilating their pupils
Right posterior pole. There are 6 million cones at the posterior pole.
Macula has almost 200000 cones responsible for colour vision
Copyright S Downes
area centralis
Posterior pole
d = 5-6 mm
fovea
Macula
Optic disc
d = 1.5 mm
d = 1.5mm
The Amsler chart tests the central 20°
foveola
Fovea
d = 0.35 mm
10
degrees
180
Cone peak
Optic disc
180
160
Rod peak
160
140
140
10
120
120
degrees
100
Rods
100
80
80
Copyright S Downes
60
60
10
10
40
40
degrees
degrees
20
Cones
20
0
0
70
50
30
10 0 10
30
50
70
90
Temporal
Fovea
Nasal
Eccentricity (degrees)
The Amsler chart is a grid given to patients with
dry age-related macular degeneration (AMD) to
Pupil testing in left optic neuropathy by swinging flashlight test
take home and look at regularly. If the lines on the
(a)
grid become wavy or distorted in a new place this
Both pupils constricted
may indicate that the patient has developed a
as a result of direct and
leaky or bleeding subretinal neovascular
consentual light reflex
membrane. This needs urgent assessment to
decide suitability for laser treatment
Chart given
(b)
to patient
Pen moved towards left
affected eye
(c)
Both pupils appear to dilate
relative to (a) as less light
Relative afferent
being interpreted by left
pupillary defect
affected eye
Central distorted lines
noted with maculopathy
20 Ophthalmic history and examination
Aims
Amsler chart
1 Assess optic nerve function by testing: (i) colour vision, and (ii)
This chart (see figure) is a test of macular function and is useful for
pupil reactions.
picking up subtle paracentral scotomas seen in macular disease,
2 Assess macular function using Amsler chart.
e.g. AMD.
• Ask the patient to hold the grid at arm’s length and to fixate on
Colour vision
the central black dot.
Colour vision is detected by cones at the macula and is transmitted
• Test each eye separately.
centrally via the optic nerve. It is a sensitive indicator of optic
• They must note whether or not the black lines look distorted
nerve function and it is vital to assess when there is anterior visual
(metamorphopsia) or absent (scotoma).
pathway disease. It is also an indicator of central retinal (cone)
• Ask them to draw in the area of distortion or missing area.
function.
Pupil reactions
Optic nerve
The pupil reactions to a direct torch light (light response) and to
• Colour vision is a test of anterior visual pathway function —
accommodation (near response) are important to exclude optic
mainly of the optic nerve.
nerve and neurological disease. (See also Chapter 47 for pupil
• In optic neuritis (e.g. may be associated with multiple sclerosis),
abnormalities.)
papilloedema, optic nerve compression from tumour or Graves’
ophthalmopathy or any optic neuropathy, visual acuity may be
normal and only colour vision is affected.
WARNING
• Acquired colour vision defects will be noticed by the patient,
If there is gross retinal disease, the direct pupil reactions will also be abnormal
and may be asymmetric. NB, a lesion compressing the optic chiasm
due to retinal nerve fibre damage.
may cause bilateral colour vision defects, is usually associated with
a visual field defect, and may progress.
1 Direct light response: tests gross retinal and optic nerve function.
Macula
• Sit opposite patient at arm’s length.
• Macular disease due to involvement of the cones, either con-
• Ask the patient to look past you into the distance (avoids
genital or acquired, causes a disturbance of colour vision.
accommodative reaction).
• An X-linked anomaly of the retinal cones in males will lead to
• Shine a pen torch light into one eye and assess pupil constric-
red-green ‘colour anomaly’ or confusion.This is the common form
tion —the direct pupil light response. The consensual reflex is
of ‘colour blindness’.
the simultaneous constriction of the other pupil.
• Repeat in other eye.
Clinical assessment
2 Swinging flashlight test: to detect a relative afferent pupil defect
Ishihara
(RAPD), which would be a sign of optic nerve damage.
• Assess colour vision using pseudo-isochromatic
‘Ishihara
• Swing the light quickly back to the first eye, the patient still
plates’ —a booklet of plates held at the normal reading distance.
looking into the distance —the first pupil should constrict and
Each plate has a series of various sized, colour dots arranged in
the second equally constrict.
patterns of hues to represent numbers. Red and green cone func-
• Repeat swinging the torch quickly from eye to eye to double
tion is predominantly tested by this test.
check.
• The numbers are large to aid people with poor vision see them.
• If one pupil dilates instead of constricts, this is an afferent
• The first plate is a ‘test plate’, which identifies subjects whose
pupil defect indicating a serious retinal or optic nerve problem.
reading skills or acuity levels exclude them from doing the test.
• Always ensure you use the brightest light source available
• Ask the patient to read each plate, testing each eye separately to
when looking for a RAPD because abnormalities can be subtle.
exclude a uniocular problem.
3 Accommodation (near response): to test for neurological
• There are up to 17 plates of numbers; record colour vision as
diseases.
‘17/17’ if the patient reads all 17 plates, or ‘5/17’ if he could only
• Ask the patient to look from the distance fixation to a small
read five, or ‘test plate only’ if he could only read the test plate.
accommodative target brought towards them slowly, up to a
• If the patient cannot read ask him to trace the coloured pattern
distance of about 20 cm.
on the illiterate plates with his finger.
• Both pupils should constrict equally.
Red desaturation
Colour vision can be estimated by the patient looking at a red ob-
KEY POINTS
ject (e.g. a red pen) with each eye. If there is an optic nerve or tract
• Ishihara plates measure colour vision.
lesion on one side the colour looks pink, dull or washed out with
• Amsler grid tests central macular function.
that eye. This is ‘red desaturation’.
• Swinging flashlight test detects afferent pupil defect.
Farnsworth Munswell 100-hue test
This is a sensitive and specific test for congenital colour defects. It
covers all cone function, not just red and green.
Other visual functions 21
8 Basic optics and refraction
Emmetropia = Normal eye with no refractive error
The pinhole test (PH)
Light from sources beyond 5 m is focused by the non-
In emmetropia (more detail in Chapter 9) every point
accommodating eye as a sharp but inverted image on the
in an object of regard is brought to point focus on the
fovea. The brain interprets this as a clear upright image
retina and the sum of all the points yields a clear
image, i.e. point-to-point correspondence
If there is a refractive error present, a blur circle is
formed on the retina, which is dependent on the size
of their pupil (smaller pupil = smaller blur circle)
Emmetropia
Object
When a pinhole aperture is placed in front of the eye,
it acts as an artificial small pupil and the size of the
at
infinity
blur circle is abolished/reduced, producing a clearer
image
Shortsighted
Hypermetropic eye
Large blur circle
Myopia (long eye)
Blurred image
Object
without pinhole
at
E
infinity
Pinhole only lets
in smallest blur
circle and letter
Pinhole
is seen more
Longsighted
clearly
Hypermetropia (short eye)
Object
at
infinity
Accommodation
The ciliary body relaxes and the lens becomes fatter
Retinoscopy
Near object
Ciliary Fat lens
Inverted
body
erect image
Aims
Refraction by the eye
1 Refractive errors:
• The ability of the eye to bend light rays.
• What is longsighted?
• Determined by the refractive media (cornea and lens) plus the
• What is shortsighted?
axial length of the eye.
• What is astigmatism?
• It is calculated in dioptres (D) (1D is the power of a conver-
2 Accommodative changes with age.
gent lens to focus parallel light at its focal point (f) 1 m behind the
This chapter summarizes the basic optics of the eye and defines
lens.)
refraction.
• The total refractive power of an emmetropic eye (normal
22 Correction of refractive errors
length) is approximately 58D, of which 43D is contributed by the
Emmetropia = normal eye with no refractive error
cornea and 15D by the lens, the aqueous and the vitreous.
Light from sources beyond 5 m is focused by the non-accommodating eye as
a sharp but inverted image on the fovea. The brain interprets this as a clear up-
Refraction techniques
right image.
These are techniques for testing the refraction of the eye.
Subjective refraction
The patient distinguishes between the effect of various lenses on
Refractive errors
the visibility of letters on the Snellen and LogMar charts.
Correction of refractive errors, see Chapters 8 and 9.
• Hypermetropia: longsightedness. Patient can see clearly in the
Objective refraction
distance but not near.
This includes examination with the ophthalmoscope, the
Optics: The focal point is behind the retina. The converging rays
retinoscope or various types of autorefractors.
that fall on the retina produce a blurred image.
Cause: The axial length is too short.
Retinoscopy
Correction: Convex (plus) glasses.
• This technique is particularly useful in testing children under 7
• Myopia: shortsightedness. Patient can see clearly close up but
years for glasses.
their distance vision is blurred.
• In children under 7 years old retinoscopy must be done with cy-
Optics: The focal point is in front of the retina. Divergent light rays
cloplegia (drops inserted to temporarily paralyse the ciliary body
falling on the retina produce a blurred image.
and inhibit accommodation; see Chapter 12) in order to obtain an
Cause: Most commonly excessive axial length (axial myopia) and
accurate refraction.
rarely due to too great refractive power (e.g. cataract refractive
• A retinoscope is an instrument used to assess the objective
myopia).
refraction of the eye. A bright streak of light is shone
Correction: Concave (minus) glasses.
through the pupil and is seen as a red reflex reflected from the
• Astigmatism: part of the image in one plane is out of focus due
retina.
to unequal refraction.
• The retinoscope streak is moved gently and the direction of the
Optics: The parallel incoming rays deform and do not focus at a
light reflex from the retina is observed.
single point, causing a blurred retinal image.
• By placing a series of plus or minus lens in front of the patient’s
Cause: Corneal curvature.
eye, the observer can calculate whether the patient is short (my-
Correction: Cylinders (toric lenses), corneal surgery or laser.
opic) or longsighted (hypermetropic) and measure the amount of
• Presbyopia: gradual loss of focusing power.The subject is usual-
astigmatism that needs correcting.
ly over 45 years old and cannot see clearly to read near type. They
progressively hold the type further and further away until their
Accommodation
arms no longer long enough.
The ability of the eye to focus clearly on an object at any distance,
Optics: There is a normal loss of accommodative range with in-
is due to the elasticity of the lens. The far point is the furthest
creasing age, due to decline of lens elasticity.
distance away at which an object can be seen clearly. In order
Correction: The reading correction (plus sphere) is added to the
to see a near object clearly, the ciliary muscle must relax (parasym-
distance correction.
pathetic) enabling the lens to become fatter, and bend (refract)
the light rays more, so that they are in focus on the retina. The
KEY POINTS
nearest point, which the eye can see clearly with maximum ac-
• The refractive power of the eye is largely due to the cornea and lens.
commodation in force, is called the near point. The distance
• Myopic eyes have a long axial length; hypermetropic eyes a short axial
between these two points is the range of accommodation. See
length.
presbyopia!
• Presbyopia is reading text blurring due to changes in accommodation at
around age 45 years.
Basic optics and refraction 23
9 Glasses, contact lenses and low-vision aids
Correction of refractive errors
Contact lenses
Each point of the E
Light rays converge
Emmetropia
is focused on the
on an imaginary
retina as a
E line
E
'point focus'
E
Myopia
After light converges
(large eye)
Point focus
it diverges
Blur circle
?
E
Biconcave
For myopia
E
Concave lenses
Myopic concave lens
make eyes look
diverges light
smaller
Hypermetropia
(small eye)
Biconvex
?
E
For presbyopia
and hypermetropia
E
Convex lenses
Hypermetropic
make eyes look
convex lens
bigger
converges light
Hypermetropia
Emmetropia
Prism
Myopia
For diplopia
Fresnel prisms
Low-vision aids
Transparent spectacle stick-on thin lens
Hand held magnification devices
CCTV
Copyright S Downes
to correct double vision
Copyright S Downes
a. Without Fresnel - normal volunteer
Simple magnifying glass
Spectacles with magnifying aids
b. Fresnel stuck on right lens appears to
Copyright S Downes
move position of eye
Homework
FOR
Hand-held pocket
telescope
CCTV - scrolling
24 Correction of refractive errors
Aims
Disposable soft CLs
1 Correction of refractive errors with glasses and contact lenses.
• Disposable lens are replaced daily, weekly or monthly.
2 Types of contact lenses.
• Disadvantage: higher infection rate, e.g. acanthamoeba.
3 Use of low-vision aids.
For laser refractive surgery, see Chapter 32.
Extended wear soft CLs
• Risk of overwear syndrome.
Optical lenses
• Complications more common see Chapter 31.
Spherical lens
This lens has an equal curvature in all meridians.
Coloured/tinted CLs (soft or hard/rigid)
1 Concave (minus) lens:
Used for prosthetic purpose as hand-painted iris-coloured lenses:
• Used to correct myopia.
• cover corneal opacities, iris defects or cataracts in blind eyes;
• Refracts light rays making them more divergent.
• prevent photophobia and improve vision in aniridia and
• Objects seen through a minus lens look smaller.
albinism.
2 Convex (plus) lens:
• Used to correct hypermetropia, presbyopia and aphakia.
Rigid gas permeable CLs
• Refracts light rays to make them more convergent.
• Made from a mixture of hard and soft CL materials.
• Objects seen through a plus lens look larger.
• Transmit oxygen much better than PMMA.
• Good for patients allergic to soft CLs.
Toric (cylinder) lens
• Used to correct astigmatism.
Scleral lenses
• Shaped like a section through a rugby ball with one meridian
• A type of hard CL approximately 23 mm diameter that bridge
more curved than the other (at right angles to each other).
the corneoscleral junction.
• Used for prosthesis purposes and keratoconus.
Prisms
• A prism deviates light rays.
Low-vision aids
• Used to relieve diplopia by redirecting light on to the fovea.
Important in the visual rehabilitation of patients with central
• Fresnel prisms are temporary plastic prisms that are stuck on to
visual field loss, especially macular degeneration.
the patient’s glasses to join diplopia, e.g. sixth cranial nerve palsy.
Text magnification
Contact lenses (CLs)
Optical magnification with magnifiers and telescopic glasses:
• CLs are superior in severe refractive errors and give a better
• Magnifiers increase the image at least ¥4 times normal size.
quality vision (e.g. correction of aphakia where an intraocular lens
• Telescopic glasses increase the image size at least ¥8 times, but
has not been placed is best corrected with a convex CL).
cause constriction of the visual field.
• Also used therapeutically in corneal disease as bandage CLs or
• Closed circuit television (CCTV) systems allowing a magnifica-
as cosmetic lenses for the scarred cornea. See Chapter 31.
tion of 25 times and are beneficial for patients with high degree of
vision loss. Expensive!
Indications for CLs
• Cosmetic, e.g. avoid glasses in low myopia.
Page navigation
• For sport, e.g. tennis and skiing for wider field.
In patients with macular degeneration, fixation stability is often
• Severe refractive errors:
very poor and they have chaotic reading eye movements using a
—high myopia, e.g.
6D myopia; a patient with high myopia de-
lot of searching with small saccades. This can be improved by en-
pends on contact lenses for visual acuity and a wider visual field;
couraging non-foveal reading.
—aphakic children without an intraocular lens post congenital
• Eccentric vision training.
cataract surgery;
• New methods of presenting text, e.g. electronic scrolled text (i.e.
—irregular astigmatism, e.g. rigid contact lenses for corneal
move text to them or serial presentation on a TV screen).
scarring and keratoconus. In the later stages, surgery (penetrat-
• High tech magnification and image enhancement using a head-
ing keratoplasty) may be required (see Chapter 32).
mounted CCTV with image processing of contrast enhancement
(virtual reality).
Types of CLs
Hard/rigid CLs
• Polymethylmethacrylate (PMMA).
• Poor oxygen transmission.
Soft CLs
KEY POINTS
• Hydroxymethylmethacrylate (HMMA).
• Glasses’ correction of myopia reduces the size of the image.
• Better oxygen permeability but fragile.
• Contact lenses’ correction of myopia gives a larger visual field than glasses.
• Most common type of contact lens worn for simple refractive
• Fresnel prisms are stuck on to glasses to correct diplopia.
errors and as bandage contact lenses.
Glasses, contact lenses and low-vision aids 25
10 External eye and anterior segment
Diagram of external eye
Diagram of
Diagram of
Frontal bone
anterior segment
eyelids
Pre-aponeurosis fat
Supracilia
Supracilia
Iris
Levator aponeurosis
Upper lid
Canal of Schlemm
Corneal limbus
Müller's muscle
Posterior chamber
skin fold
Upper punctum
Orbicularis muscle
Cilia
Anterior chamber
Lens
Plica
Grey line
Cornea
Lateral
Medial canthus
Posterior
Meibomian orifice
Anterior chamber
canthus
Caruncle
capsule
Tarsal plate
angle and
of lens
Lower lid
Lower punctum
Capsulopalpebral fascia
trabecular meshwork
margin
Orbital septum
Lower lid skin crease
Orbicularis muscle
Maxilla bone
Direct visual assessment with adequate magnification
and illumination is required, using a loup and pen torch,
direct ophthalmoscope or slit lamp
Dislocated lens
How to evert the upper eyelid
Gross conjunctival chemosis and haemorrhage
Place a cotton bud or Minims gently on the upper lid skin
crease, hold the central eyelashes and draw them
upwards, at the same time pressing gently downwards
with the cotton bud/Minims as counter pressure. Ask the
patient to look downwards as this makes it more
comfortable. Topical anaesthetic drops are recommended
to anaesthetize the ocular surface as everting the eyelid
can be uncomfortable. See Chapters 12 and 24
Mini-Armour Ophthalmoscope—a simple pen torch with attached basic
Everted upper eyelid
optical system. (Courtesy of Roger Armour)
Slit lamp
This provides the best magnification and illumination with a stereoscopic view.
The Goldmann tonometer can be attached to it to measure intraocular
pressure and a variety of hand-held lenses used with it to view the fundus
Goldmann tonometry to measure
Corneal abrasion staining
intraocular pressure
Using the slit lamp
with fluorescein
See Chapter 37
See also Chapter 11
See Chapter 16
26 Basic eye examination
Aims
Intraocular pressure (IOP)
1 Anatomy of the external eye and anterior segment.
For eye pressure measurement, see Chapter 37.
2 Examination.
Anterior chamber (AC)
Anatomy
Information about the AC is best obtained with the slit lamp. The
The external eye includes the eyelids, lashes, lacrimal puncta,
direct ophthalmoscope (set at +10D) or a pen torch and loup will
caruncle, plica semilunaris, corneal epithelium and conjunctiva.
provide useful but limited information.
The anterior segment includes the cornea, iris, anterior chamber
• Is the AC quiet, i.e. is the aqueous clear? A slit lamp will show
angle and lens.
the presence of cells and keratoprecipitates (KPs) (condensation
of cells on the inner surface of the cornea).
Systematic examination
• Is there a hyphaema (accumulation of blood in the AC)? This
This should be undertaken in the following order.
may result from trauma, spontaneously ruptured iris new vessels
(rubeosis iridis) with a central retinal vein occlusion, longstanding
Lids
glaucoma, diabetic retinopathy, or in patients with intraocular
• Observe the upper eyelids for symmetry. If asymmetrical, decide
tumours.
which lid is ptotic (drooping) or whether the other lid is retracted.
• Observe lid position relative to the pupil and cornea.
• A ptotic lid will cover more cornea and may partially or totally
WARNING
obscure the pupil.
Beware the child with a hyphaema and no history of trauma —think of
• A retracted lid will cover little or no cornea, with the sclera vis-
retinoblastoma or non-accidental injury.
ible above the cornea (upper scleral show).
• Observe the lower eyelid position for entropion (lid turning in-
wards) or ectropion (lid everted outwards).
• Is there a hypopyon (accumulation of white blood cells in the
• Look for evidence of inflammation, e.g. erythema, oedema.
AC)? This may be seen in uveitis, infective endophthalmitis, with
• Note any lid lesions present.
a corneal abscess, and as a manifestation of leukaemia or
• Observe the eyelashes —any missing? Are they growing in the
lymphoma.
correct direction or in-growing (trichiasis)?
• When appropriate, evert the eyelid.
Iris
Use the slit lamp, ophthalmoscope at +8D or the pen torch and
Conjunctiva
loup.
• Use the slit lamp at low (¥10) magnification, a pen torch or oph-
• Notice the colour of each iris. Different colour irides (‘iris
thalmoscope set at +12D held close to the eye or set to zero and
heterochromia’) may be associated with iritis or congenital
held further away.
Horner’s syndrome.
• Colour:
• Identify iris lesions: iris melanoma, Lisch nodules in neurofibro-
—Red. Is there injection (i.e. redness?). Does it involve the en-
matosis or abnormal iris vessels (rubeosis irides), which may
tire conjunctival surface, a segment of conjunctiva or just the
signify an underlying ocular tumour, central retinal vein occlusion
area where the conjunctiva meets the cornea (circumcilliary)?
or diabetes.
—Bluish/purple circumcilliary injection suggests anterior
• Notice iatrogenic iris changes, e.g. peripheral iridectomy.
uveitis.
—In chemical burns, patches of ischaemia appear white, sur-
Lens
rounded by severe congestion (see Chapter 15).
The slit lamp or direct ophthalmoscope is best to examine the lens.
—Yellow. Patients with jaundice may have a yellow tinge to
• Use the direct ophthalmoscope set at 0, and stand at arm’s
their conjunctiva (icterus).
length from the patient directing the beam of light to the pupil, to
• Appearance/texture of the conjunctiva:
assess the red reflex. Lens opacities are seen as discrepancies in the
—Are there tarsal conjunctival follicles or papillae? These are
red reflex.
pinkish or fine red velvety lumps.
• Next, move closer the patient at the same time increasing the
—Does the patient have chemosis (conjunctiva has an oedema-
magnification (usually to +6) until the lens is in focus.
tous jelly-like appearance)?
• Detect a dislocated lens with the pupil dilated. It may be caused
by trauma, or may indicate an underlying hereditary systemic dis-
Cornea
order such as Marfan’s syndrome or homocystinuria.
Use the same equipment as when examining the conjunctiva.
• Is the cornea clear, or are there opacities present?
• If there is a corneal irregularity or opacity, instil a drop of fluor-
KEY POINTS
escein into the conjunctival sac and note any fluorescein uptake
• Examine the eye systematically, starting with the eyelids, the external eye
(i.e. staining), which indicates a break in the epithelium. A blue
and anterior segment.
torch light is best.
• The cornea is usually avascular with a shiny smooth surface.
• Are there abnormal vessels (neovascularization) growing into
• Cataract is the most common lens disorder.
the cornea? It should be avascular.
External eye and anterior segment 27
11 Posterior segment and retina
Tight junction
Posterior pole anatomy
Ten retinal layers
Choriocapillaris
Bruch's membrane
Retinal pigment epithelium (1)
Sclera
Rod
Photoreceptors
Choroid
(outer segment)
Outer segments (2)
Retina
Cone
External limiting membrane (3)
(outer segment)
Fovea
Cup
Outer nuclear layer (4)
Optic
disc
Outer plexiform layer (5)
Horizontal cell
Lamina
cribrosa
Inner nuclear layer (6)
Human methylmethacrylate vascular
cast of blood vessels at optic disc
Inner plexiform layer (7)
Copyright J Olver
Ganglion cell layer (8)
The optic nerve head consists of
Nerve fibre layer (9)
approximately 1.3 million axons exiting
Internal limiting membrane (10)
the globe via the lamina cribrosa at the
posterior scleral foramen (small hole in
the back of the sclera). The neural rim
Indirect ophthalmoscope
Best through dilated pupils
(pink) contains axons and the central
cup (yellow), glial tissue
The head-mounted
indirect
ophthalmoscope is
Direct ophthalmoscope
Normal optic disc
Glaucomatous disc
used to view the
posterior pole and
The hand-held
peripheral retina -
ophthalmoscope is
binocular view
commonly used in clinical
Useful for detecting retinal
medicine to view the pupil
tears
reactions, red reflex, lens,
retina and optic nerve
head, even through an
Slit lamp
78D lens used
undilated pupil. It has a
In glaucoma, the raised
at slit lamp to
monocular view
intraocular pressure
see retina-
causes progressive
binocular view
Optic disc drusen
Central retinal vein
damage and death of
occlusion
axons, hence they reduce
in number, the central glial
or empty space enlarges,
resulting in an increased
cup:disc ratio
Special lenses are held in front
of the patient's eye to view the
disc and macula at high
magnification - image seen is
Often an incidental finding
inverted and horizontally
but may cause field defects
There is a swollen disc with
transposed
marked venous engorgement
Central retinal artery
and haemorrhages
occlusion
Laser at macula
Drusen (age-related changes)
What you see with each technique
at macula in AMD
Indirect
ophthalmoscope
25∞ - wide field of vision
Direct
ophthalmoscope
6∞
There is a pale retina,
Yellow drusen in
Small regular pale
Slit lamp, 78D lens
occluded arterioles and
Bruch's membrane
laser burns in retina
Amount of retina seen with each examining technique
a cherry red spot
28
Basic eye examination
Aims
• Stand or sit at arm’s length, looking through the ophthalmoscope aperture,
1 Define the fundus.
directing the light beam towards the patient’s right pupil to view their red
2 Understand how to use an ophthalmoscope to examine the
reflex.
fundus.
• Move closer to the patient looking at the red reflex until the retinal details be-
3 Have observed: (i) the use of an indirect ophthalmoscope; and
come clear, with the patient continually looking over your right shoulder into
(ii) slit lamp plus special lenses.
the distance.
• Examine the optic nerve head/disc.
Direct ophthalmoscopy is an essential skill since retinal examina-
• Follow the blood vessels out from the disc in their four directions.
tion is widely used in general practice and hospital medicine.
• Ask the patient to look up, down, right and left, to examine as much of the
equatorial retina as possible.
Definitions
• Lastly, ask the patient to look straight at the ophthalmoscope light beam to
• Fundus: Retina including the macula, blood vessels and optic
examine the vessel-free macula and fovea.
nerve head.
Assess the optic nerve head/disc.
• Posterior segment: Area behind the lens, includes posterior
• Disc margins —should be clearly defined/distinct from the surrounding
chamber, vitreous, retina, choroid and optic disc.
tissue.
• Fundoscopy: Examination of the fundus.
• Disc colour —central cup yellow and pink surrounding rim. If the disc is
• Posterior pole: Posterior retina including the optic nerve head,
completely yellow or white, suspect optic atrophy.
macula and retinal blood vessels.
• Cup : disc ratio (CDR) —this is the ratio of the size of the central yellow cup
• Periphery or peripheral fundus:The retina from the equator out
to the size of the entire disc. Normally 0.1-0.3 and symmetrical.
towards the pars plana.
Assess the blood vessels.
• Calibre:
Examination technique
—Are the arteries excessively narrow as in arteriosclerosis?
Equipment needed to examine posterior segment:
—Are the veins tortuous and dilated as in venous occlusion or ocular
• Direct ophthalmoscope: monocular.
ischaemia?
• Indirect ophthalmoscope: binocular with 20D lens.
• Arteriovenous
(AV) nipping, which occurs in hypertension and
• Slit lamp biomicroscope +/- +90D or +78D lens; binocular.
arteriosclerosis.
• Abnormality, e.g. arteriovenous malformation (AVM), new vessel formation,
Dilate the pupils
sheathing.
The fundus can be examined with the pupil undilated (best in
Assess the retina.
darkness to ensure maximum pupil size).A better view is achieved
• Colour —retinal colour can vary between races.
if the pupils are dilated.
• Contour —are there any elevated lesions such as metastases, malignant
In adults, Guttae cyclopentolate 1% or tropicamide 0.5% are
melanoma or retinoblastoma?
used, ±guttae phenylephrine 2.5% for greater dilation, especially
Assess the macula.
with brown irides (see Chapter 12).
• When the patient looks directly onto the light, you should be
focused on the macula.
Do not dilate the pupils
—Fovea is avascular and there is a sheen from a healthy young fovea.
• When pupillary responses are being monitored for neuro-
—Look for changes in colour and contour in the para-fovea and macula.
observation.
• when there is a risk of precipitating angle-closure glaucoma (i.e.
individuals with shallow anterior angles) (see Chapter 36).
Direct ophthalmoscopy
Indirect ophthalmoscopy
The light source is focused by a series of minilenses and directed
This binocular head-mounted device with hand-held condensing
via a mirror into the patient’s eye. The observer views the illumin-
lenses is used to examine the retina binocularly. It gives a wide
ated retina through a sight hole in the mirror. The disc of rotating
field of view at low magnification.
lenses can be rotated to compensate for both the observer and pa-
tient’s refractive errors —if both the observer and patient are em-
Slit lamp biomicroscope
metropic then no lens (zero) is incorporated. The image produced
Is widely used by ophthalmologists for macular and disc
is erect and magnified (¥15) with a field of view of 6°.
examination.
How to use the direct ophthalmoscope
If you wear glasses or contact lenses for distance keep them on. NB, start with
KEY POINTS
the ophthalmoscope magnification set at 0.
• Examine the right eye first.
• Ask the patient to look straight ahead.
• Optic nerve cup : disc ratio is normally 0.1-0.3.
• Examine the right eye first.
• The fovea normally does not have any blood vessels.
Posterior segment and retina 29
12 Use of eye drops
1
2
Fluorescein preparations
1 Fluorescein paper strips (Fluorets)
2 Single-dose Fluorescein Minims
3 Combined single-dose fluorescein with local anaesthetic,
such as proxymetacaine Minims are useful for measuring
intraocular pressure by Goldmann tonometry
TIP
Fluorescein stains soft contact lenses yellow/green
therefore these should be removed prior to examination
Eye drops should be applied in the followng way:
3
4
FIRST WASH YOUR HANDS
i) Advise the patient to look up to the ceiling and away
from the eye drop bottle
ii) Gently pull the lower eyelid down or ask the patient to
do so; this will expose the lower fornix
iii) The bottle or Minims is placed directly above the
exposed lower fornix, without touching it
iv) Apply the drop.
v) Have a tissue ready to dab the cheek in case of over-
spill but not touch the ocular surface
NB After some eyelid operations eye drops are applied
without pulling the lid down. Instead the patient looks up
and the drop is applied to the ocular surface medially
1 Instilling eye drops
2 Fluorescein staining cornea - dendritic ulcer
3 Using a Fluoret to apply fluorescein.
With the lower lid pulled slightly downwards and away from the globe,
Iris and ciliary body innervation
the strip is gently placed in the conjunctival sac and the fluorescein released
4 Inferior corneal abrasion staining with fluorescein
Constrictor (sphincter) pupillae
- Parasympathetic
via oculomotor nerve (IIIrd cranial nerve)
Ciliary muscle
- Parasympathetic
Pupil size is controlled by the iris and its
DILATING DROPS WARNING !
autonomic nervous innervation. The action of
dilating drops is to modulate the effect of the
Warn patients of the after effects for the next
autonomic control of the iris and ciliary body
few hours: i) blurred vision - especially for near
and hence pupil size
vision and ii) glare in bright light
Avoid driving until the effect has worn off
Dilator (sphincter) pupillae
Accommodation of the lens (focusing ability)
Risk of precipitating an attack of acute angle
- Sympathetic
is controlled by the ciliary body which is also
closure glaucoma in patients with a narrow
via superior cervical ganglion
innervated by the parasympathetic nervous
iridocorneal angle: the patient must see an
system and loss of this results in loss of
ophthalmologist urgently if symptoms of blurred
accommodation (cycloplegia) with blurred near
vision persist and a halo effect around a light
vision
source occurs
Aims
Definitions
1 Understand the indications for fluorescein, and the use of
Mydriatic: Drop that causes mydriasis (pupil dilation).
common dilating and anaesthetic drops.
Miotic: Drop that causes miosis (pupil contriction).
2 Know how to instill eye drops correctly.
Cycloplegia: Loss of accommodation caused by blocking the
3 Be aware of the risks of dilating drops.
parasympathetic innervation to the ciliary body.
30 Basic eye examination
Drops for ocular surface examination
advantage of being short acting and having a greater cycloplegic
Fluorescein
effect than tropicamide. It is commonly used in refraction in
Fluorescein is an orange-brown crystalline substance and belongs
children to abolish accommodation.
to the triphenylmethane dyes. It is available as Minims drops or
• Mydriasis and cycloplegia within 20-30 min.
dried onto paper (Fluoret). It adopts its characteristic yellow-
• Maximum cycloplegic effect lasts 45-60 min.
green colour after dilution. Use a cobalt blue light from a slit
• Effect wears off after 24 h.
lamp or direct ophthalmoscope to see the typical green-yellow
Side effects: risk of allergic reaction and raised intraocular pres-
fluorescence.
sure. In a baby <3 months old, cyclopentolate 0.5% should be used.
• Absorbtion spectrum: 465 and 490 nm (blue end).
Hypersensitivity is less common than with atropine. Rare side ef-
• Emission spectrum: 520 and 530 nm (green-yellow region).
fects: visual hallucinations, disorientation and ataxia.
Fluorescein is water-soluble and does not stain corneal epithelium
In patients with darkly pigmented irides, the cyclopentolate ef-
(hydrophobic). It does stain Bowman’s membrane and stroma in
fect may be insufficient for full cycloplegia, therefore use atropine
an epithelial defect, e.g. dendritic ulcer.
1% drops. NB, atropine has a longer acting period and higher risk
of side effects.
Rose Bengal
Rose Bengal is a red soluble dye and belongs to the group of fluo-
Topical anaesthetic drops
rine dyes. It is available as a 1% Minims preparation. It stains
Topical anaesthesia is used for:
wherever there is insufficient protection of the preocular tear film:
• ocular examination (tonometry and gonioscopy);
• Decreased tear components, e.g. keratoconjunctivitis sicca.
• contact lens fitting;
• Abnormal surface epithelial cells, e.g. degenerating or dead
• to alleviate pain due to injury and to facilitate thorough exam-
cells.
ination, e.g. for a foreign body, abrasion or ulcer;
• Mucous strands.
• in children prior to instillation of often stingy eye drops.
After staining, cells loose their vitality. Rose Bengal should be
They must be used sparingly and in short courses as they poten-
used very sparingly, as it causes stinging due to its acid properties.
tially mask the severity of pain if the injury worsens. Prolonged use
It is advisable to instil topical anaesthetic prior to its use and warn
is epithelial toxic.
the patient about discomfort.
Mode of action: prevent generation and conduction of nerve
impulses —mostly belong to amine group of compounds.
Common dilating drops for fundal examination
Anaesthetic drops are obtainable in Minims without preserva-
In order to examine the fundus adequately, the pupil needs to be
tives or in bottles with preservatives.
dilated.
Oxybuprocaine 0.4% (Benoxinate)
Tropicamide 1%
Well absorbed with onset of action within 60 s. One drop lasts
This is a synthetic analogue of atropine. It reduces the parasympa-
approximately 15 min.
thetic innervation to both the sphincter pupillae and the ciliary
body, resulting in a marked mydriatic action and weak cycloplegic
Tetracaine 0.5% and 1.0% (Amethocaine)
action. It is used alone or in combination with phenylephrine for
Onset within 60 s and effect lasts 20 min. Contact dermatitis has
better dilation.
been reported.
• Maximum effect after 20-30 min.
• Effect wears off after at least 6 h.
Proxymetacaine 0.5% (Ophthaine)
Onset 30 s, lasts 15 min. It is less stingy than the above anaesthetic
Phenylephrine 2.5%
drops, therefore useful in children. Also available as a combina-
This is a synthetic compound and is biochemically closely related
tion with fluorescein in Minims, and useful for Goldmann contact
to adrenaline; it acts as a potent sympathomimetic. It stimulates
tonometry.
dilator pupillae and causes mydriasis. However, the dilator pupil-
lae is a weaker muscle than the sphincter pupillae, hence the my-
driatic effect of phenylephrine is less than tropicamide. It is used in
combination with tropicamide or cyclopentolate. Useful to help
KEY POINTS
maximize dilation in dark brown irides.
• Fluorescein needs a blue light to visualize its yellow colour.
• Maximum effect after 30 min.
• Rose Bengal stains devitalized cells but should be used sparingly as it
• Effect wears off after 5 h.
stings.
• Phenylephrine 10% is rarely used due to systemic side effects.
• Tropicamide and cyclopentolate dilating drops also cause cycloplegia (blur-
ring of near vision).
Cyclopentolate 0.5% and 1%
• Proxymetacaine is the only topical anaesthetic that does not sting.
This is a synthetic substance similar to atropine and has the
Use of eye drops 31
13 The red eye
There are many causes of a red eye, some are sight-
IMPORTANT
threatening and some are not. See Chapter 14 and also
The sight-threatening causes of a red eye include
related Chapter 29, on external eye disease
acute angle closure glaucoma
corneal ulcer/abscess
penetrating eye injury
These require immediate ophthalmologist attention
Circumciliary
injection
Localized dense red
haemorrhage
Pupil dilated by
cycloplegic drops
b) Subconjunctival haemorrhage - can be
caused by trauma, hypertension or blood
dyscrasia, but is most commonly
(a) Acute anterior uveitis
(b)
idiopathic, see Chapter 14
Periocular skin
is red, dry and
Generalized conjunctival redness
flaky
Tarsal conjunctival redness
Follicles
(c) Contact dermatitis - from topical
(d) Viral conjunctivitis
eye drops
Hazy corneal oedema
Fixed vertically oval pupil
Shallow anterior chamber
Whorled iris appearance
Lens pushed forward
due to ischaemia
Iridocorneal touch
Brick red
Acute angle closure glaucoma
Cornea
Limbus
Schlemm's canal
Conjunctiva
Episclera
Sclera
Uvea
Iris root
Episcleritis
Pterygium
Benign localized inflammation of the episclera - the layer lying beneath the conjunctiva and superficial to the
sclera. Usually idiopathic but may be associated with a rheumatological disorder. No symptoms or mild dull
pain. No treatment required. If severe pain suspect scleritis which is more serious and needs investigating
32
Acute ophthalmology
Aims of Chapters 13 and 14
• Antiviral ointment (e.g. Aciclovir five times per day) is used for
1 Identify the four most common causes of a red eye.
herpes simplex virus (HSV) dendritic ulcer.
2 Understand how the distribution of redness helps make the
diagnosis.
WARNING
3 Recognize sight-threatening red eye.
Never give steroids for HSV dendritic ulcer —they exacerbate the condition
(steroids can only be used by an ophthalmologist in combination with Aci-
clovir once the epithelium has healed to prevent scarring)
Red eye is the presenting symptom of a variety of ocular problems. The most
important symptoms are visual loss and pain, which suggest serious
• Intensive antibiotic drops are required for bacterial ulcer (e.g.
conditions.
ofloxacin hourly).
• Acanthoamoeba corneal ulcer can be seen in soft contact lens
Infective conjunctivitis
wearers —beware as pain is disproportionately greater than ap-
pearance of the eye.
Symptoms
• Red eye.
Uveitis
• Discomfort or itch.
Inflammation of the uveal tract: iris, ciliary body and choroid.
• Discharge (watery or purulent).
• Crusting of lid margins
Symptoms
• General flu-like symptoms in viral cases.
• Painful and red.
• History of contact with people with red eyes.
• Photophobic eye with or without a history of autoimmune
disease (e.g. ankylosing spondylitis, inflammatory bowel disease,
Signs
sarcoidosis) or infection (e.g. toxoplasmosis).
• Generalized redness of conjunctiva and especially the tarsal
• Blurred vision or floaters.
conjunctiva (posterior surface of the lids).
• Cervical lymphadenopathy in viral cases.
Signs
• Ciliary/circumcorneal injection
(engorgement of episcleral
Management
vessels around the iris root).
• Hygiene advice, e.g. avoid sharing towels.
• Reduced visual acuity.
• In purulent cases, swab for C&S (culture and sensitivity).
• ±Sluggish or irregular pupil due to reflex sphinter spasm or
• Prescribe topical antibiotics, e.g. chloramphenicol hourly for 1
inflammatory adhesions of iris to the anterior lens surface
day then qds for 1 week or fusidic acid bd for 1 week.
(posterior synechiae).
Special consideration
• Iris details may be hazy due to inflammatory cells in the aqueous.
• Tiny round opacities may be visible on the inferior posterior
• Chlamydial conjunctivitis should be suspected in adults with bi-
lateral chronic conjunctivitis with or without a history of venereal
corneal surface keratitic precipitates (inflammatory cells on the
corneal endothelium).
disease. Corneal scarring is a risk, and referral to ophthalmologist
is recommended.
• Raised intraocular pressure because of inflammation or adhe-
sion of iris and cornea (anterior synechia), which hinders drainage
• Ophthalmia neonatorum is conjunctivitis in newborns less than
1 month old. It is a reportable disease and immediate ophthalmic
of the aqueous.
• Cataract is seen in recurrent or chronic uveitis.
referral is recommended. In cases of gonococcal infection there is
a danger of visual loss due to corneal involvement.
Management
Corneal ulcer/keratitis/abscess
• Refer the patient to an ophthalmologist for further investigation
and management. For uveitis the treatment is a reducing regimen
Symptoms
• Painful red eye in a patient who may give a history of wearing
of topical steroid (e.g. dexamethasone 0.1%) to reduce the inflam-
mation and a cycloplegic and dilating drop (e.g. cyclopentolate 1%)
contact lens, foreign material injuring the eye, facial cold sores or
similar previous episodes.
for pain relief and prevention of synechiae formation.
• Photophobia.
Acute angle-closure glaucoma
• Purulent discharge is seen in bacterial cases.
A sudden rise in intraocular pressure due to closed iridocorneal
Signs
drainage angle. (See Chapters 36 and 38.)
• May have decreased visual acuity depending on the location of
the ulcer (keratitis).
WARNING
• Pus in fornices in bacterial cases.
If diagnosis is delayed, vision can be lost. Urgent treatment is required.
• Decreased corneal sensation with dendritic corneal ulcer.
• Fluorescein staining reveals area of epithelial defect under
KEY POINTS
cobalt blue light.
• A subconjunctival haemorrhage is usually idiopathic.
• Common causes of red eye are conjunctivitis, keratitis, uveitis and acute
Management
angle-closure glaucoma.
• Immediate ophthalmological opinion plus corneal scrape as
• Untreated angle-closure glaucoma blinds.
risk of perforation and permanent central corneal scar.
The red eye 33
14 More on the red eye
Cellulitis
Subconjunctival haemorrhage
Signs and symptoms
- Swollen erythematous lids
i
Pre septal
- normal VA
- no diplopia
ii
Post septal - diplopia
- % VA
Episcleritis
- v. unwell
- painless or mild pain
Meibomian cyst/chalazion
- pyrexia
- normal vision
or stye/hordeolum
- emergency
- no discharge
Blepharo conjunctivitis
Scleritis
± meibomianitis
- very painful
- gritty sensation
- may have VA
- itch
- very tender globe
- ± sticky/crusty in a.m.
Outer
Conjunctivitis
Herpes simplex
Associated
covering
- itch
- infective
Vesicles
'red lid'
of globe
- allergic
- FB sensation
- VKC
- normal VA
- green/yellow
discharge if
bacterial
Red eye
Subtarsal FB (STFB)
Acute glaucoma
- pain++
- corneal oedema
- VA
- fixed semi-dilated pupil
Everted
Keratitis
- severe pain ± vomiting
upper
- blurred VA++± preceeded
Corneal FB
eyelid
by halos and lights
Dendritic ulcer
Corneal abrasions
Redness
- pain++
2° STFB
Uveitis
mainly
- VA
circum-
Photophobia+
ciliary
± floaters+
Corneal
pain+
Circumcilliary
abscess
VA+
injections
± sterile hypopyon
Marginal ulcer
Pterygium
± hypopyon
Nasal
Temporal
Excess CL wear
corneal hypoxia
Pterygial head
encroaching
on visual axis
Causes of a red eye
Red eye
Infection
Allergy
Trauma
Inflammation
Acute angle
Other
• Abrasion
closure glaucoma
• Pterygium
• Foreign body
• Blepharitis
• Subconjunctival
haemorrhage
Keratitis/ulcer
Conjunctivitis
Endophthalmitis
Uveitis
Episcleritis
Marginal
Scleritis
• Bacterial
• Bacterial
• Endogenous
keratitis
• Viral
• Viral
• Exogenous
• Acanthoamoebic
• Chlamydial
• Post-operative
34
Acute ophthalmology
Allergic conjunctivitis (see Chapter 29)
• Non-necrotizing: Treat with systemic indomethacin 100 mg od
Symptoms
for 4 days, then reduce to 75 mg po od until inflammation is
• Itchy red eye in patient who may have a history of atopy (e.g.
resolved.
asthma, eczema, hay fever).
• Necrotizing: high dose immunosupression.
Blepharitis/meibomianitis
Signs
• Diffuse or localized conjunctival injection.
Signs and symptoms
See Chapter 29.
• Chemosis, normal vision.
Treatment
Treatment
• Topical mast cell stabilizer and antihistamine bd (such as
• Lid hygiene bd.
• G fucithalmic bd for up to 3 months.
Opatanol or Zaditen).
• Topical steroids initially if severe.
• Topical lubricant six times per day.
• Review after 3 months, if no improvement add minocycline
• Vernal keratoconjunctivitis sicca (VKC): treat as for allergic
and refer to an ophthalmic unit.
100 mg bd for 3 months.
Meibomian cyst or chalazion/stye or hordeolum (see
Subconjunctival haemorrhage (SCH)
Chapters 23 and 24)
Symptoms
Treatment
• Sudden onset of painless red eye.
• G chloromycetin hourly for 3 days, qds for 10 days.
• Occasionally patient says he ‘felt something give’ or ‘pop’.
• Hot compresses and remove lash if there is a stye.
• If early pre-septal cellulitis, add systemic antibiotics for 10 days.
Signs
• Localized dense red haemmorhage on an otherwise normal eye.
Orbital cellulitis
Signs, symptoms and management. See Chapter 23.
Treatment
• Reassure it will resolve spontaneously.
Primary herpes simplex infection of eyelids
• Ask patient about excessive straining such as severe coughing
Symptoms
or vomiting which can cause SCH —usually bilateral.
Sore red eye and eyelid usually in a child.
• Check blood pressure, full blood count (FBC) and
blood
glucose.
Signs
Vesicles on lids in early stages —eschar in later stages.
Episcleritis
Symptoms
Treatment
• Red eye.
• Occ aciclovir five times per day for 1 week, then tds for 1 week,
• Usually painless, or can have mild dull pain.
bd for 1 week, od for 1 week and then stop.
• Exclude corneal involvement with fluorescein.
Signs
• Localized or diffuse episcleral injection.
Pterygium (see Chapter 32)
• Non-tender.
• Normal vision.
Symptoms
• No discharge.
Localized redness medially, irritation +/- blurred vision.
Treatment
Signs
• G Voltarol qds.
Wing-shaped abnormal growths of conjunctival-derived fibrovas-
• Rarely systemic indomethacin.
cular tissue. Inflammation and blurred vision due to visual axis ob-
struction or astigmatism.
Scleritis
Symptoms
Aetiology
• Extremely painful red eye.
Subconjunctival elastotic degeneration from UV damage and dry-
• May have blurred vision.
ness, e.g. Australia and other dry desert equatorial countries.
Signs
Treatment
• Intense injection of the scleral and episcleral vessels.
• Medical—topical lubricants +/- G Volterol.
• Globe extremely tender.
• Surgical—excision and conjunctival autografts.
—b-irradiation or antimetabolites applied periopera-
Treatment
tively in recurrence.
• Rule out systemic disease, e.g. rheumatoid arthritis.
More on the red eye 35
15 Ophthalmic trauma principles and management of
chemical injuries
Medicolegal considerations
Meticulous history recording, clinical examination, visual
The principles of trauma apply:
Ophthalmic trauma is:
acuity recording, note taking and photographs of the
Airway
Chemical-Emergency
injuries are required. All trauma cases should be
Breathing
Blunt
regarded as potential medicolegal cases especially when
Cardiovascular
Sharp and perforating
an alleged assault has taken place or it has been an
Once these are stabilized the
occupational injury. Always sign your name clearly and
ophthalmologist is asked to examine
date and time the clinical notes accurately
the orbital / eye injury
Retinal tear and detachment
Vitreous haemorrhage
Subtarsal
Scleral rupture
foreign body
Choroidal rupture
Orbital haemorrhage
Traumatic optic
neuropathy
How to wash out a chemical injury
This is the only occasion when you wash out the
eye first then measure the visual acuity second.
It is an emergency!
Perforating
metal hook
IRRIGATE!!!
Water or saline
Corneal
foreign body
Penetrating
corneal injury
Lid laceration
Lens cataract
Iris dialysis
Orbital floor
Intraocular
fracture -
foreign body
fat ± muscle
Commotio
prolapse and
retinae
entrapment
Examination
Take a thorough history and record exactly what happened
Measure the visual acuity (in chemical injury can do after
washout)
Examine the eye systematically from the outside lids to
the retina, incuding pupil reactions
Dilate pupils for fundal examination
± Radiological investigation
Photograph for medicolegal purposes
36 Acute ophthalmology
Aims
WARNING
1 List the main causes of loss of vision due to trauma.
Sympathetic ophthalmia is a rare condition following perforating eye injury
2 How to wash out a chemical injury.
that results in chronic ocular inflammation and possibly loss of vision.
Principles of ophthalmic trauma
Basic ophthalmic trauma knowledge is required in the accident
The five main causes of loss of vision with trauma are:
and emergency setting, in intensive care and in the primary eye
1 Corneal scarring and anterior segment damage from severe alkali burn.
care clinic. The trauma patient may be managed by plastics and
2 Severe disrupted globe from penetrating injury, e.g. road traffic accident.
maxillofacial surgeons if there are facial or orbital fractures, or
3 Unrecognized intraocular metallic foreign body causing siderosis bulbi.
neurosurgeons if there is a head injury.
4 Compressive optic neuropathy from retrobulbar haemorrhage.
5 Traumatic optic neuropathy from optic canal bony or shearing injury.
Trauma can affect the periocular region, bony orbit, orbital contents, globe or optic nerve.
1 Eyelid and periocular and orbital haematoma —fully assess to rule out orbital floor fracture and fracture of base of skull
2 Orbital bony wall fracture —floor > medial wall with diplopia, needs repair
3 Eyelid subtarsal foreign body —evert lid and remove with cotton bud
4 Eyelids —partial or full thickness laceration: explore wound, exclude penetrating eye injury and repair within 48 h
5 Lacrimal drainage system —most commonly lower canaliculus; needs oculoplastics repair and stent, e.g. MiniMonaka tube
6 Conjunctival laceration —may need suturing; exclude more extensive deeper injury
7 Corneal abrasion —treat with topical antibiotics ± cycloplegia and a pad
8 Corneal foreign body —needs removal and dilated fundoscopy
9 Corneal penetrating injury ± sclera, iris, lens or retinal injury —all require urgent surgical repair
10 Hypahaema (blood in the anterior chamber) —can cause secondary glaucoma; needs urgent ophthalmic assessment
11 Dislocated lens —may need surgery to remove lens
12 Traumatic cataract —most need surgical removal
13 Glaucoma secondary to angle recession (i.e. damage to trabecular meshwork) —needs specialist treatment
14 Blunt vitreous haemorrhage and retinal commotio —needs vitreoretinal assessment to exclude retinal tear
15 Retinal tear/dialysis —needs urgent retinal surgery
16 Choroidal rupture —may lose vision if underlies macula; untreatable
17 Scleral perforation —needs surgical exploration and repair; if extensive may loose eye (enucleation)
18 Massive retrobulbar haemorrhage —needs urgent lateral canthotomy/cantholysis to decompress orbit
19 Traumatic optic neuropathy —needs to be treated with high dose steroids within hours
20 Traumatic cranial nerve injury —IVth, IIIrd and VIth cranial nerves need MRI scan
21 Complete globe disruption —needs enucleation within 14 days to prevent sympathetic ophthalmia
If any of the above are suspected refer immediately to eye casualty
Chemical injuries
check for fragments of cement, etc. and remove them. Swipe the
Which chemical? Substances include alkalis (lime, cement, plaster
cotton bud along the lower fornix to remove particulate debris.
or ammonia), acids, solvents, detergents, irritants (e.g. mace and
5 Now measure the visual acuity and check the eye, including
pepper) and super-glue. Alkalis (e.g. ammonia or wet cement) are
intra-ocular pressure.
the most destructive, penetrating the deep layers of the eye with
6 Admit.
time. In high concentrations they cause severe ischaemia of the
7 Topical treatment: intensive topical antibiotics, vitamin C and
conjunctiva, corneal limbus, cornea and sclera, and cause subse-
cycloplegia (to prevent pain) ± steroids. Treat raised intra-ocular
quent scarring and blindness. There may be associated severe
pressure as necessary.
uveitis and cataract formation. Wash out the eye immediately!
8 Oral high dose vitamin C.
1 Measure the pH of the tear meniscus if litmus paper is handy.
9 Later surgery if need —limbal cell transplant and penetrating
2 Otherwise, apply immediately topical anaesthetic drops if
keratoplasty (corneal graft).
handy.
3 Copious irrigation with normal saline or Ringer’s solution. If
neither are available, put the patient’s head under a cold water tap
KEY POINTS
or into a bowl of cold water —with eyes open! Irrigate/splash the
• All trauma cases are medicolegal cases until proved otherwise.
eyes for 5-10 min, then repeat the pH measurement.
• Ocular trauma is chemical, blunt or sharp (perforating).
4 Ensure that the surface of the eye and the upper and lower
• Alkali burns can cause blindness and must be irrigated immediately.
fornices are included. Using a cotton bud, evert the upper lid and
Ophthalmic trauma principles and management of chemical injuries 37
16 Specific features of blunt and sharp injuries
Blunt injuries
Small hyphaema
Blackball
Acute massive orbital haemorrhage with proptosis
Sphincter
3 mm
Subconjunctival haemorrhage
NB May need urgent lateral cantholysis and canthotomy
pupil
and chemosis
to drain a traumatic retrobulbar haemorrhage
ruptures
Retinal and choroidal blunt injury
Choroidal rupture
(yellow-white streak)
Commotio retinae
(white)
Commotio retinae is likely
to recover but the rarer choroidal rupture
can persist and, if on the macula, cause
severe decreased vision
Dislocated lens
WARNING
CT scan of left orbital medial wall and floor fracture -
Exclude small entry wound of an intraocular foreign body (IOFB). Dilate the pupil and
patient has severe enophthalmos and diplopia from
examine the fundus to exclude IOFB. If there is a history of hammering, use orbital X-ray to
restricted eye movement
exclude IOFB
Sharp injuries
Anterior segment sharp injury
Lens perforation
Corneal foreign bodies
Axial corneal
full thickness
laceration
Iris pulled up
to wound
Corneoscleral
laceration
Corneal perforation with
Medial eyelid and lacrimal canaliculus
fishing hook - may have
avulsion. Needs primary repair and
perforated lens
canalicular intubation
Subtarsal
Scratch marks on
foreign body
cornea lightly staining
Remove with a cotton bud or sharp
needle with good illumination and
magnification. May leave a rust ring
which needs later further removal
with a needle
Double eversion of upper eyelid
Severe ocular trauma with a
corneo-scleral rupture, lens
Exploratory microsurgery is indicated
disclocation, retinal detachment
Intraocular foreign body
to determine the extent of the globe
and vitreous haemorrhage
Needs vitrectomy and removal
rupture and to carry out a primary repair
38 Acute ophthalmology
Aims
eyelid, corneoscleral, iris, lens and retinal lacerations. Often,
1 How to manage a retrobulbar haemorrhage.
though, the entry wound is small and a high index of suspicion
2 How to remove a corneal foreign body.
should therefore exist for hammering and other high velocity in-
3 How to manage a corneal abrasion.
juries. Perforating injuries require urgent exploration and repair
by the on-duty ophthalmologist. The vitreo-retinal and oculoplas-
Blunt injuries
tics surgeons work closely together with these patients. Sometimes
From a fist/cricket/squash/tennis ball/champagne cork, etc.
the eye must be enucleated when the injury is very severe.
• Causes lid echymosis, orbital and subconjunctival haematoma,
hyphaema, ± lens iris injury, vitreous haemorrhage and commotio
TIPS
retinae.
• Do not put pressure on an eye that may be perforated or contents may
• Look for associated conjunctival and corneal foreign bodies,
extrude!
abrasions and lacerations and a red reflex.
• X-ray for suspected intraocular foreign body.
• Exclude traumatic emphysema from bony fracture —rare.
• Exclude a perforating ocular injury, traumatic retinal detach-
Superficial corneal injuries
ment or optic neuropathy (vision will be markedly reduced with
Corneal foreign bodies
(FBs) and subtarsal foreign bodies
an afferent pupil defect and normal optic disc).
(STFBs). History of a particle entering the eye, either dust or
• Exclude orbital floor fracture by examining eye movements and
metal flying in whilst walking past a building site, grinding
for infraorbital numbness. If a fracture is suspected arrange an
metal/hammering/doing DIY.
orbital CT scan.
The following are the main blunt injuries seen.
Symptoms
• Painful photophobic red watering eye —worse for corneal FBs
Traumatic hyphaema
than STFBs.
This is blood in the anterior chamber. It can be microscopic (seen
only on slit lamp), or it can form a level, the height of which is
Signs
measured in millimetres, or it can be a complete blackball. Causes
• Corneal FB sits embedded superficially on corneal epithelium.
pain and blurred vision.
• STFB lies embedded on the upper tarsal conjunctiva and
causes typical superior corneal superficial epithelial abrasions.
Traumatic iritis
White cells and flare in the anterior chamber (seen only on slit
Management
lamp), causing dull pain and photophobia.
• Use topical anaesthesia to examine. Instil fluorescein drops to
help see the FB and epithelial scratches from the STFB.
Orbital haematoma
• Try and flick the corneal FB off with a cotton bud. If it is too em-
• Eyelid echymosis. There are usually superficial lacerations caus-
bedded, the ophthalmologist can use a sharp needle end to remove
ing the bleeding. Insert a topical anaesthetic drop to help open the
it at the slit lamp.
eye gently and measure the visual acuity, examine the eye move-
• Evert the upper eyelid to see and remove the STFB with a cot-
ments, exclude a perforating eye injury and look at the fundus.
ton bud wiped across it. Immediate symptomatic relief.
• Retrobulbar haemorrhage. This is potentially sight-threatening.
• Instil topical antibiotics, cycloplegic drops and pad for 24 h, then
There is pain, decreased vision, proptosis and diffuse subconjunc-
a short course of topical antibiotics.
tival haemorrhage extending posteriorly. It can follow periocular
infiltrative anaesthesia or blunt trauma (with orbital wall fracture)
Corneal abrasion
and be associated with a ruptured globe and carotid-cavernous
History of scratch from a sharp plant, paper, child’s finger nail, etc.
sinus fistula. Emergency lateral canthotomy and cantholysis is
necessary to relieve high orbital pressure and to reduce the risk of
Symptoms
Severe pain and FB sensation, photophobia and watering.
compressive optic neuropathy.
Signs
Retinal bruising (commotio retinae)
Blurred vision can occur due to retinal bruising and loss of central
Red eye with fluorescein staining epithelial abrasion.
vision from a choroidal rupture across the macula.
Management
• Use topical anaesthesia to examine.
Traumatic optic neuropathy
This may respond to high dose steroids or optic canal decompression.
• Instil fluorescein to show abrasion clearly with blue light.
• Pad with a cycloplegic drop and topical antibiotic.
Orbital floor fracture
Sharp objects heal initially but later can cause symptoms of noc-
Blow-out fracture of the floor or medial wall into the sinus. Orbital
turnal and early morning FB sensation —called recurrent erosion
soft tissue entrapment may cause diplopia and limited eye move-
syndrome (RES).
ments. Enophthalmos may not be immediately apparent until
KEY POINTS
swelling/haemorrhage has settled.
• Retrobulbar haemorrhage — canthotomy + cantholysis saves vision.
• Evert the upper eyelid to remove a subtarsal foreign body with a cotton bud.
Sharp, penetrating and perforating injuries
• Corneal abrasion from a sharp object can cause RES.
Sharp objects, e.g. glass, spiky plant, hammer and chisal, cause
Specific features of blunt and sharp injuries 39
17 Sudden painful loss of vision in a non-inflamed eye
Sudden painful loss of vision
Sudden loss of vision associated with eye pain or headache in the
1 mm
white non-inflamed eye needs urgent attention as it may be due to
30 mm
sight or even life-threatening illness. The frequency of each disease
varies between age groups
Left altitudinal field defect
typical of anterior ischaemic
optic neuropathy
Giant cell arteritis (GCA)
1 mm
GCA - inflammation of the lining of large and medium sized
arteries. Immediate treatment with corticosteroids usually
relieves symptoms and prevents loss of vision
Optic neuritis/retrobulbar neuritis
Swollen disc of arteritic anterior
Elderly patient
ischaemic optic neuropathy - colour
Non pulsatile tender
and fluorescein angiogram appearance
temporal artery
May have swollen optic nerve or
± Headache (may be painless)
look normal if retrobulbar neuritis
± Jaw claudication
(i.e. inflammation behind globe)
± Weight loss
High ESR and CRP
Young woman
Pain on eye movement
Haemorrhage from pituitary tumour
May involve one
Benign intracranial hypertension (BIH)
optic nerve or
Pituitary
tract causing
tumour
sudden vision
Usually overweight females
loss
(though can occur in slim adults
and children of either sex)
Causes progressive field loss
Migraine
but also sudden visual loss
in the form of transient visual
Fortification spectra
obscurations (TVOs)
Scintillating
May see zigzag lines
scotoma
Can lose vision temporarily
Fields showing constriction.
Shaded area is where target is
Cast of blood supply of human eye
Copyright J Olver
not visualized
Vortex vein
Optic nerve
Aetiology of optic neuritis
Central retinal
artery/vein
Typical: Idiopathic
Short posterior
Multiple sclerosis is the most common
ciliary artery
cause of retrobulbar neuritis
Atypical: Infectious (viral)
PONAA/circle of
Post infectious
Haller and Zinn
Granulomatous
Outer choroidal
Autoimmune
vessels
Contiguous inflammation of orbit,
Long posterior
sinuses or meninges
ciliary artery
40 Acute ophthalmology
Aim
—there is often associated eye pain, particularly induced by eye
1 Identify the main causes of sudden painful loss of vision in a
movement.
white eye.
• Typically, the vision improves over a period of 4-6 weeks,
2 Note that the pain may be ocular or cranial or both.
though this is not always the case.
• There may be other symptoms attributable to demyelination,such
Giant cell arteritis (GCA)/Temporal arteritis
as paraesthesia, bladder or bowel dysfuntion, and limb weakness.
This is visual disturbance with headache in elderly patients. This
• There may have been a recent viral illness.
inflammatory condition can result in occlusion of the larger blood
• The diagnosis of optic or retrobulbar neuritis can be aided by
vessels supplying the anterior optic nerve leading to anterior
performing visual evoked potential (VEP), which will demon-
ischaemic optic neuropathy (AION); this is referred to as arteritic
strate increased latency, i.e. a ‘delayed response’.
AION when the aetiology is GCA. There is also a non-arteritic
• MRI also helps to confirm the diagnosis, as the affected nerve
AION which is painless and is caused by occlusion or hypoperfu-
lights up, and it will show up demyelinating plaques in the brain.
sion within the smaller blood vessels supplying the optic nerve, the
• In most centres systemic steroid therapy for optic neuritis is re-
circle of Haller and Zinn (see figure of cast, opposite).
served for bilateral cases; as although it has been shown to speed
• In arteritic AION the patient is usually elderly and complains
up visual recovery, it has not been demonstrated to improve final
of:
visual outcome.
—sudden loss of vision, which may only affect the upper or
lower half of the visual field (altitudinal visual field defect);
Migraine
—headache (not always present).
This is visual disturbance with headache.
—sometimes a recent history of pain in the cheeks when
These visual disturbances most commonly present as fortification
chewing —jaw claudication;
spectra or scintillating scotoma, but occasionally as field loss or
—often a recent history of weight loss, myalgia and arthralgia.
even total loss of vision, which recovers. There is often a family
• On examination there may be temporal artery tenderness.
history of migraine.
• If there is associated chest pain suspect coronary artery involve-
ment, which may lead to cardiac infarction and death if not
Idiopathic intracranial hypertension (IIH) or benign
treated.
intracranial hypertension (BIH)
• Inflammation of the cerebral vessels can lead to a cerebrovas-
Presents with headache and transient visual obscurations (TVOs).
cular accident (CVA).
TVOs last for a few seconds, are unilateral or bilateral, and are
• Patients with GCA often have a high ESR, and invariably an
usually precipitated by movement or postural changes. They are
elevated CRP (though both may be normal initially).
pathognomonic of papilloedema.
• Definitive diagnosis is by temporal artery biopsy. This is best
• Occurs typically in obese females, but can affect slim individuals
done within a few days of commencing steroids.
of either sex, and children.
• Treatment, which must be swift in order to prevent blindness, is
• The optic discs are swollen and there is field loss.
with high dose steroids and requires hospital admission. Treat-
• An MRI should be performed to exclude a space-occupying
ment must not be delayed whilst waiting for a biopsy; once a clini-
lesion and an MRA to exclude venous sinus thrombosis, or an
cal diagnosis is made, instigate treatment immediately.
arteriovenous malformation affecting the venous sinuses.
• Patients with this condition may be on steroids for several years
• Thyroid dysfunction is a cause and must be excluded.
and must be put on calcium and a biphosphonate (to reduce
• Patients should be referred for urgent treatment, as this disease
osteoporosis), and a proton pump inhibitor. They must have
often results in permanent loss of the visual field.
their weight, blood pressure and blood glucose monitored.
• Treatment includes:
—conservative: weight loss; stop any medications that may
Optic neuritis/retrobulbar neuritis
cause BIH (e.g. NSAIDs, tetracyclines);
This is visual disturbance with eye pain.
—medical: acetazolamide;
• Inflammation of the optic nerve. If the entire anterior part of the
—surgical: lumbo- or ventriculo-peritoneal shunt, or optic nerve
nerve is inflammed, the optic disc will appear swollen (papillitis).
sheath fenestration.
• Retrobulbar neuritis (RBN): If the part of the nerve behind
the globe (i.e. the retrobulbar part of the nerve) is affected, with
Haemorrhage associated with pituitary tumour
sparing of the nerve head, the patient will have the same symp-
Rarely, a small haemorrhage into an undiagnosed pituitary
toms with reduced visual acuity, red desaturation and a relative af-
tumour can cause sudden loss of vision associated with headache.
ferent papillary defect, but the disc will appear normal in the acute
Such patients require urgent referral to a neurosurgical unit, as this
phase.
is a precursor of pituitary apoplexy.
Typical optic neuritis/retrobulbar neuritis:
• Most commonly affects young adults.
• Females affected more than males.
KEY POINTS
• Patient presents with:
• Painful loss of vision in a quiet eye may have a systemic cause, e.g. giant cell
—sudden loss of vision —this may vary from complete loss of
arteritis.
vision to alteration in colour perception (e.g. the patient may
• Retrobulbar neuritis —the disc looks normal in the acute phase.
complain of colours looking ‘washed out’ with the affected
• Idiopathic intracranial hypertension —the discs are swollen.
eye);
Sudden painful loss of vision in a non-inflammed eye 41
18 Sudden painless loss of vision
Retinal detachment
Symptoms
Vitreous haemorrhage
Sudden visual loss preceded by
floaters and flashes (photopsia)
Retinal tear
Retinal tear
i.e. from
Pale detached
Subretinal fluid
neovascularization
retina
Retina detached
in diabetes
Vitreous
Retinal
Detached vitreous
haemorrhage
arteriole
Optic disc
in distance
Central retinal vein occlusion
Central retinal artery occlusion
NB Check
NB Check
Intraocular pressure
BP
BP
Pulse ?Afibrillation
Viscosity
Carotids ?Bruit
Heart ?Murmur
Refer to cardiologist
Cherry red
Central or branch retinal
spot
vein occlusion - this is
Flame-shaped
a sub-total CRVO
haemorrhage
May see
or 3 quadrant BRVO
emboli
Tortuous
vessels
Vascular anatomy
Anterior optic nerve supply
Optic nerve layers:
Circle of Haller
Nerve fibre layer of retina
and Zinn or
Choroid (prelaminar)
PONAA
Sclera (lamina cribosa)
Paraoptic short
Retrolaminar optic nerve
posterior
ciliary artery
Vascular cast: Circle of Haller and Zinn
or perioptic nerve arteriolar
Pial arterioles
Central retinal artery (CRA)
anastomosis (PONAA)
Copyright J Olver
Age-related macular degeneration
Cerebrovascular
accident
A sudden haemorrhage may
This affects
cause sudden loss of vision
visual pathways
Age-related macular degeneration—disciform scar
42 Acute ophthalmology
Aim
WARNING
Identify the main causes of painless loss of vision, in particular:
• All patients with vein occlusion must have their blood pressure checked,
• retinal detachment;
should be examined for arteriosclerosis, have their intraocular pressure
• vitreous haemorrhage;
checked and be checked for diabetes and systemic inflammation.
• types of vascular occlusion.
• Young patients presenting with CRVO or BRVO, or older patients in whom
there is no obvious cause, should be fully checked out for hyperviscosity
Retinal detachment (see Chapter 39)
syndromes.
• Sudden (sometimes gradual) painless loss of vision.
• Usually preceded by symptoms of flashing lights (photopsia)
Central retinal artery occlusion (CRAO) or a branch retinal
and/or floaters and/or visual field defects.
artery occlusion also presents as acute painless loss of vision.
• When the macula is not involved the visual loss involves the pe-
Aetiology:
ripheral field and visual acuity may be normal.
• Very high intraocular pressure, as seen in acute angle-closure
• Once the macula is involved the central vision is lost.
glaucoma.
• Arterial embolus from diseased carotid, valvular heart disease,
Management
atrial fibrillation.
Laser to retinal hole or retinal surgery ± vitrectomy.
• Arterial occlusion from atheroma or inflammation (e.g. giant
cell arteritis).
Vitreous haemorrhage
Haemorrhage into the vitreous cavity can result in sudden pain-
less loss of vision. The extent of visual loss will depend on the de-
WARNING
gree of haemorrhage.
All patients with CRAO need full cardiovascular work-up.
• A large haemorrhage will cause total visual loss
• A small haemorrhage will present as floaters and normal or only
Non-arteritic anterior (AION) or posterior ischaemic optic
slightly reduced visual acuity.
neuropathy (PION):
Aetiology:
• Results from occlusion or hypoperfusion of the small blood ves-
• Proliferative retinopathy —spontaneous rupture of abnormal
sels supplying the optic nerve head (AION) or posterior optic
fragile new vessels that grow on the retinal surface cause bleeding
nerve (PION).
into the vitreous cavity. Most common is proliferative diabetic
• In AION the optic disc is swollen; this swelling may be segmen-
retinopathy.
tal or involve the entire nerve head. There are usually associated
• Retinal detachment —a small retinal blood vessel may rupture
splinter haemorrhages at the disc.
when the retinal break occurs, bleeding into the vitreous cavity.
• In PION the optic disc looks normal.
• Trauma.
• There may be arteriosclerosis and arteriovenous nipping, de-
• Posterior vitreous detachment (see Chapter 39 for details) can
pending on the cause.
result in vitreous haemorrhage if, as the vitreous separates from
• Risk factors: arteriosclerosis, hypertension, hypotensive
the retina, it pulls and ruptures a small blood vessel.
episode, smoking, ‘disc at risk’ (e.g. small optic nerve head with no
• Age-related macula degeneration (AMD) —haemorrhage may
central cup).
occur into the vitreous from the abnormally weak vessels forming
a subretinal neovascular membrane (see Chapter 41).
Cerebrovascular accident (CVA)
A haemorrhagic or embolic CVA affecting the visual pathways
Management
will present as acute painless visual loss. Depending on the site of
Referral to an ophthalmologist to determine cause and manage
the lesion, the patient will have a corresponding field defect on
any complications (e.g. glaucoma due to red blood cells clogging
fields to confrontation. (See Chapter 50.)
up trabecular meshwork) that may occur.
Acephalgic migraine
Vascular occlusion (see Chapters 44 and 45)
This rare form of migraine presents with transient visual
Central retinal vein occlusion (CRVO) or a branch retinal vein oc-
disturbances involving one or both eyes in the absence of
clusion (BRVO) often presents with sudden painless loss of vision.
headaches.
Aetiology:
• Systemic hypertension.
KEY POINTS
• Raised intraocular pressure.
1 Retinal detachment is an ocular cause of sudden painless loss of vision.
• Hyperviscosity syndromes.
2 Central retinal vein occlusion is commonly caused by systemic
• Vessel wall disease
(e.g. diabetes, inflammation such as
hypertension.
sarcoidosis).
3 Central retinal artery occlusion may be caused by giant cell arteritis.
Sudden painless loss of vision 43
19 Gradual loss of vision
Be suspicious of the presence
When a patient presents with a gradual
of these common conditions
painless loss of vision, the cause will
Cataract
often vary with age, as certain
1 Uncorrected refractive error
conditions can be more common in
2 Cataract
certain age groups, e.g. cataract and
3 Chronic simple glaucoma
E
?
ageing maculoplathy in the elderly
4 Ageing maculopathy
Patient may complain of
glare initially or short-
sightedness
Refractive error
E
E
E
Correct with cataract
i.e. myopia in a teenager
surgery and intraocular
lens implant
Correct with spectacles
Age-related macular degeneration
Primary open angle glaucoma
Causes progressive visual field loss
Causes loss of
Treat with laser
Intraocular pressure (IOP) elevated
central vision
if amenable
+ 21 mmHg
Treat with ocular
antihypertensives
30 mmHg
Cupped disc
Age-related macular degeneration - geographic
macula atrophy
Tumours
Low tension glaucoma with cupped optic disc - need to
reduce IOP further (within normal range 10-20 mmHg)
Causes optic pathway compression
Diabetic retinopathy
Pituitary tumour
Optic nerve tumour,
e.g. glioma or meningioma
Occipital lobe tumour
Treat with laser
TIP
Elderly patients with cataract may also have ageing macular degeneration and the
contribution of each to their gradual painless loss of vision must be established
Diabetic maculopathy
prior to offering cataract surgery, or they may not get an optimum result
White circles are laser burns
44 Gradual loss of vision
Aim
toms, the optic disc will show evidence of damage and be very
Easily identify the common causes of gradual painless loss of vi-
cupped (end-stage disease).
sion in a white eye.
Glaucoma screening will often pick up POAG before any
severe damage has occurred and many patients are maintained on
Refractive error
topical medication without significant progression or the need for
Undetected and uncorrected refractive error is a common cause
drainage surgery (see Chapters 36-38).
of gradual visual loss in all age groups. Hypermetropia occurs in
young children, axial myopia in teenagers and young adults, and
Retinal disease
lenticular myopia in older patients.
Should be considered in the patient with none of the above causes
• Early cataract formation (nuclear sclerosis) may induce a re-
of reduced vision. It occurs particularly in patients at risk:
fractive error (most commonly myopia) in the elderly —they are
• Patients with diabetes (diabetic retinopathy).
briefly happy because they discard their glasses for reading! How-
• Patients with hypertension (hypertensive retinopathy).
ever, their distance visual acuity gradually deteriorates and they
• The elderly (age-related macular degeneration,ARMD).This is
require surgery.
the commonest cause of blindness in the elderly, in which their
• Children with refractive errors don’t complain until they attend
central vision for reading, colour and fine detail is affected. They
school and have difficulty seeing the blackboard (myopia) or
cannot see people’s faces or expressions clearly or read the labels
the print in their text books (hypermetropia or astigmatism),
on food in the supermarket or read the newspaper.
or complain of headaches at the end of the day due to eye
• Children or young adults with neurometabolic diseases or a
strain
(asthenopia). The child often doesn’t complain at all,
family history of retinal disease (e.g. retinitis pigmentosa).
and it is the teacher who notices a problem. Unfortunately,
• An individual with a history of an intraocular foreign body
for some children with hypermetropia, amblyopia has already
(IOFB) may develop siderosis bulbi; this is a condition where iron
occurred in one eye by the time the diagnosis is made and
from an IOFB that has not been removed can cause retinal toxi-
despite full refractive error correction with glasses and
city. The patient presents years after the initial injury with gradual
patching, vision in one eye does not improve. (See Chapters 9 and
loss of vision. The iris in the affected eye of a blue-eyed individual
21).
may have a greenish hue.
• Individuals taking medications known to cause drug-induced
Cataract
macular disease (e.g. chloroquine, hydroxychloroquine, tamox-
• A common cause of gradual loss of vision in the elderly. They
ifen, chlorpromazine, thioridazine, vigabatrin).
may notice nothing at all and the presence of an early cataract is
detected by their optician or they will have a gradual blurring of
Tumours and inflammation
distant, then near, vision. If the cataract is placed posterior in the
Any tumour that affects the visual pathway may cause symptoms
lens as a plaque (posterior sub-capsular lens opacity) they will
of gradual, painless loss of vision by pressure on the optic nerve or
notice glare and reduced vision in bright sunlight with improved
eye. Examples include:
vision indoors.
• Intraocular tumour (e.g. choroidal malignant melanoma or
• It may also occur in younger age groups who are at risk (e.g.
choroidal metastases from the breast or prostate in adults,
patient with diabetes, patients on steroids, patients with chronic
retinoblastoma in children)
uveitis and those with a family history of cataract).
• Intraocular lymphoma, which may masquerade as bilateral
• Cataract may also occur in young children (congenital cataract).
uveitis.
It is very important to check the red reflex of any child who pres-
• Tumour of the optic nerve (e.g. meningioma or glioma).
ents with reduced vision, and any baby who does not fix and follow,
• Tumour of the orbit or optic nerve (e.g. orbital lymphoma, sphe-
as they require urgent treatment with patching and glasses to pre-
noidal wing meningioma, dysthyroid eye disease).
vent amblyopia. (See Chapter 21).
• Any brain tumour involving the visual pathways (e.g. pituitary
tumour, occipital lobe tumour).
Primary open-angle glaucoma (POAG) (chronic simple)
These are not common and should always be considered when no
Causes slowly progressive painless visual field loss.
other cause can be found.
• It is most commonly seen in adults over 40 years of age, though
it can occur in younger adults.
• Risk factors include Afro-Caribbean origin, family history of
KEY POINTS
primary open angle glaucoma and hypertension.
• Myopia is common in young teenagers.
• The patient is usually completely unaware that they have open
• Patients with POAG are usually unaware of their disease.
angle glaucoma and it is detected by their optician finding raised
• Cataract and ageing maculopathy cause decreased vision in the elderly.
intraocular pressure or noticing a cupped disc.
• Tumours are a rare cause.
• By the time a patient with glaucoma presents with visual symp-
Gradual loss of vision 45
20 Visual acuity in children
Newborn up to 2 months old
1. Fix and follow. In the newborn see if they will fix
2. Spinning. Another way of
and follow a shiny colourful target
getting a crude idea of vision
is to pick the child up, and hold
him at arm's length and spin
him around in a circle
3. More advanced ways of checking a newborn’s vision include
4. Electrophysiological testing with visual evoked
forced choice preferential looking (FPL or PL), a clinical test
potentials (VEPs) /visual evoked responses (VERs)
Infant and toddler up to 3 years old
4 to 5 year olds
In the pre-verbal infant, vision can be
Depending on social background and learning
assessed as for the newborn.
ability most 4 and 5 year olds will be able to
Older infants can see pictures of
match letters, and some children at this age
familiar objects (fish, apple, boat)
can even read letters. For children who cannot
read letters the “Sheridan-Gardner singles”
test is used
Cardiff Acuity Cards
- best for infants
Cup
Kay Pictures
Sheridan-Gardner singles
– best for toddlers
46 Sub-specialty —Paediatric ophthalmology
Aim
• VEP: the child has electrodes on its head which record brain
How to assess visual acuity in different aged children.
signals if they see the pattern on the screen.
Visual development
Infant (up to 2 years)
A child’s vision continues to develop after birth and maturation
Cardiff cards
does not fully occur until after age 2 years. Normal visual develop-
• A more accurate way of recording vision in these infants is to
ment in both eyes is important for the child to perceive the world,
use Cardiff cards (CC).
their education and social interactions.An infant who appears not
• Each card has a line drawing of a familiar object on either the
to see well may have delayed visual maturation or a more serious
upper or lower half of the card, and the thickness of the lines vary.
cause. Measuring visual acuity in children requires skill and pa-
According to the thickness of the line, the card will have a letter
tience, but even simple techniques can be used to elicit vision and
(e.g. CC H) and a Snellen equivalent (Sn Eq) on the back (e.g. 6/6
reassure the parent.
for the finest line).
• From a distance of 50 cm or 1 m, the cards are rapidly shown to
Newborn child up to 2 months
the child and the examiner observes the child making vertical eye
Assessment of vision in the neonate is dependant on the age and
movements up and down to the corresponding picture, and
behavioural state of the child. Because the child is pre-verbal you
records the acuity as, for example, ‘CC H at 50 cm-Sn Eq 6/9’. If
depend on their eye movements for information about visual
possible the acuity of each eye should be recorded separately.
function. If the child is smiling (usually at 6 weeks), then you smile
at the child without making any noise, and if they smile back, you
Toddler (2-3 years)
know they can see!
Once the child can speak you can ask them to identify verbally
There are a number of techniques used to test vision.
some simple and familiar pictures.
Fix and follow
Kay’s pictures
• Use a large brightly coloured shiny toy to see if the child fixes
• The most common method of assessing vision in this group is
and follows.
with Kay’s pictures.This test consists of a booklet of cards, on each
• With the child sitting on their mother’s knee, move the toy
of which there is a line drawing.
slowly from left to right about 50 cm in front of the child’s face. If
• Each line drawing has a Snellen equivalent depending on the
the child can see he will only follow the toy if he is awake and if the
size of the drawing (i.e. the largest drawing is equivalent to the 6/60
toy is moved extremely slowly as eye movements are immature at
letter on the Snellen chart).
this age.
• The examiner stands 6 m from the child and asks him to identify
• If possible, test each eye separately, by occluding one eye with
each picture.
an occlusive patch.
• If the child is too shy to tell you what each picture is he will usu-
• If the child fixes and follows the target, record the vision as ‘fixes
ally whisper it to his parent who in turn will indicate to you if he
and follows’.
was correct.
• If the child doesn’t follow the toy this may be because
he can’t see or is drowsy, or he is just not interested —try again
Young children (4-5 years)
later.
Sheridan-Gardner test
• The child is given a card with several letters randomly arranged
Spinning
on it.
Whilst spinning the child, observe his eye movements. He will have
• The examiner stands 6 m away and presents single letters on a
nystagmus during spinning if he can see. This is the vestibulo-
card of varying Snellen equivalence.
ocular reflex or VOR. When you stop, the nystagmus will change
• The child is asked to match each letter with the letter on his
direction for 1 or 2 beats in a seeing child. This is post-rotational
card. Each eye is examined separately and the acuity recorded.
nystagmus. If it persists the child is either severely visually im-
paired or has a cortical lesion.
KEY POINTS
• In newborn children use ‘fix and follow’ or spinning to elicit presence of
Other clinical tests
vision.
Preferential looking (PL) and visual evoked potentials (VEP).
• In infant less than 2 years old use Cardiff cards.
• PL: a card with different sized grating patterns on one side and
• In infants aged 2-3 years use Kay’s pictures.
plain on the other is shown to the infant who will look towards the
• In children aged 4-5 years use Sheridan-Gardner letters.
grating side if they can see it.
Visual acuity in children 47
21 Strabismus (squints)
Examination
Long-sight (hypermetropia) and convergent squint (esotropia)
Corneal Hirschberg reflection test - to detect a squint
Left accommodative esotropia
Fully corrected by wearing hypermetropic glasses
The corneal reflex position is observed - each mm of
displacement is equal to about 15 prism dioptres (7 degrees)
Example: Right 45 prism
dioptre convergent squint
(esotropia)
Assessment of ocular movements in 9 positions of gaze (primary gaze and
The cover tests
8 directions)
1. The cover-uncover test - to detect the presence of a squint:
Note the defective movement
Upgaze
Observe if one eye is preferred for fixation
of the left eye in left gaze
Ask the patient to look at the fixation target - if in a child
in left lateral
this can be a light or toy
rectus palsy
Dextroversion
Latroversion
Occlude (for a few seconds) the eye that appears to be fixing.
As you cover the eye, watch the other uncovered eye to see if it
Esotropia in
moves to take up fixation
primary gaze
Remove the occluder and see if the original eye retakes up
Limited left
fixation. If it does, it is the preferred fixating eye and the other
Downgaze
abduction
eye has a squint (non-alternating heterotropia)
Do this for near and then distance vision
Amblyopia therapy - Patching
Left good eye is patched
in order to encourage use
of right amblyopic eye
2. The alternate cover test - to detect a latent squint or
phoria in a patient with straight eyes on cover test:
Orthoptic definitions
Ask the patient to fixate on an object
Cover one eye then rapidly move cover to the other eye
i) Strabismus / squint
Repeat rapidly several times
Malalignment of the two eyes. If it is constantly present, it is manifest, but if it
Observe the movement of the covered eye as it becomes
is only detected on dissociation with an alternate cover-uncover test, it is latent
uncovered
ii) Binocular single vision (BSV)
If it moves inwards to take up fixation the patient has an
The use of both eyes together to achieve binocular depth perception - stereopsis
‘exophoria’
iii) Amblyopia - ‘lazy eye’ in 2% of the population
Do test for near and then distance
Amblyopia occurs from insufficient use of the eye(s) during visual development
Also can be used with a prism bar to measure the maximum
(birth - 7 years) commonly due to the presence of a manifest squint
size of a squint
and/or refractive error. The brain suppresses the image from a deviating or
defocused eye, particularly under 2 years of age - the sensitive period - when
Example cover test:
visual development is especially vulnerable to disruption. Other causes include
When the left fixing eye is covered with an opaque occluder,
congenital cataract or ptosis
the right eye moves inwards to take up fixation of the target.
iv) Amblyopia therapy
The squint is divergent (exotropia)
The treatment of squints in childhood with glasses and patching
v) Heterophoria = latent strabismus
Both eyes look straight but deviate on dissociation. It is common and usually
does not need treatment. Types: esophoria - convergent (inwards), exophoria -
divergent (outwards), hyperphoria - upward, hypophoria - downward
vi) Heterotropia = manifest strabismus in 5 - 8% of the population
One or other eye is not directed towards the fixation point. Types: esotropia -
convergent, exotropia - divergent, hypertropia - upward, hypotropia - downward
Squint
vii) Concomitant strabismus
The size of the squint is measured with a prism bar
The deviation remains the same in all directions of gaze
viii) Incomitant strabismus
The angle of deviation changes with the direction of gaze
ix) Patching
Prism alternate cover test
The patch completely covers the good eye to encourage the bad eye (amblyopic
one) to be used and develop vision. Generally unsuccessful after age 7 years
x) Diplopia
Double vision
48
Sub-specialty —Paediatric ophthalmology
Aims
Childhood concomitant and congenital incomitant squint
1 Understand squint terminology.
Orthoptist
2 Do a cover test to detect a squint.
• Measures visual acuity (VA).
3 Know the basic principles of amblyopia therapy.
• Detects and measures squint using cover tests.
• Assesses eye movements.
Children with a squint will not ‘grow out’ of it. There may be a sin-
• Assesses binocular vision (including tests for stereopsis).
ister cause such as cataract or retinoblastoma, so do a red reflex.
• Monitors amblyopia therapy with patching ± atropine occlusion.
Any child suspected of having a squint should be referred to an or-
thoptist and ophthalmologist for assessment.
Refraction
Orthoptists are allied health professionals who assess patients
The optometrist or ophthalmologist performs refraction
with diplopia, strabismus and eye movement defects. They work
(cycloplegic if child aged <7 years). In fully or partial accommoda-
closely with ophthalmologists in the management of children’s
tive esotropia with high hypermetropia, wearing glasses will fully
visual development, testing paediatric visual acuity (see Chapter
or partially correct the squint as well as improve visual acuity, and
20) and treating amblyopia.
surgery may not be required.
Aetiology and pathophysiology
Amblyopia therapy
Concomitant strabismus
Spectacles (if applicable) and a patch worn on the better eye for a
• Binocular single vision (BSV) usually develops by 3-5 months
specified number of hours per day, depending on the child’s age
old. If BSV does not ‘lock in’, esotropia (convergent squint) can
and VA.
develop at this time, although most concomitant squints develop
later at around 2-4 years, particularly with hypermetropia.
Surgery
• Any cause of reduced vision in one eye interrupts BSV and re-
Strabismus surgery is performed if the squint is socially unaccept-
sults in a squint, e.g. cataract, retinoblastoma or anisometropia.
able and to restore/improve binocular vision. In esotropia, the
• Children with a family history of strabismus or refractive error
horizontal rectus muscles are operated; recessing the medial
and those with developmental abnormalities have a higher inci-
rectus and resecting the lateral rectus or bimedial rectus recessions.
dence of concomitant squint.
Acquired incomitant squint (children and adults)
Incomitant strabismus
• The underlying cause must be established and treated (e.g.
• Congenital causes are rare, e.g. third, fourth or sixth nerve palsy.
intracranial tumour, diabetes, hypertension).
• Acquired incomitant squint presents with diplopia in adults.
• Orthoptic management is by joining diplopia with Fresnel
A child may adopt a compensatory head posture to minimize
prisms or prisms incorporated into the spectacle prescription.
diplopia and therefore may not complain of diplopia. A very
• Surgery is performed if BSV is not comfortably restored once
young child will suppress the second image and develop ambly-
the extraocular muscle(s) recover or have been stable for at least
opia if untreated.
6 months.
• Acquired causes include cranial nerve palsy (paralytic) second-
ary to intracranial pathology, thyroid eye disease and postorbital
floor fracture (restrictive).
KEY POINTS
• Esotropia is a convergent squint.
Management
• Amblyopia must be treated early —ideally before age 5 years.
Orthoptists, optometrists and ophthalmologists collaborate in the
• Beware: squint may be a presentation of an intracranial tumour or
management of squint using a combination of glasses, surgery and
retinoblastoma.
orthoptic treatment.
Strabismus (squints) 49
22 Neonates
Leukokoria
Retinopathy of prematurity
Dragged disc
Proliferating retinal vessels on ridge
There is an International classification of retinopathy of prematurity (ROP) where
worsening stages are recognized. The retina is divided into zones for its development
Temporal
12
12
Temporal
equator
equator
Leukokoria - a white coloured pupil
Zone III
Zone III
- exclude congenital cataract or
Zone II
Zone II
retinoblastoma
Zone I
Zone I
9
3 9
3
Retinoblastoma
Hereditary (usually bilateral) or sporadic (usually
unilateral)
Ora
Treatment: Radioactive plaque or enucleation and
serrata
adjuvant chemotherapy
6
6
Survival: Untreated only 2-4 years (brain metastases).
OD
OS
Treated 90-95% 5 year survival
Screening for ROP
Congenital glaucoma with buphthalmos
• Infants <1500 g
• 31 weeks or less gestational age
• Begin at 6 weeks post-natally, not immediately
• Two-weekly intervals
• Weekly if ROP develops until it regresses or is treated
• Indirect ophthalmoscopy and indenter to see the
peripheral retina (pupils dilated)
CNLDO
Buphthalmos—child with big watering
Buphthalmos examination under anaesthesia—
photophobic eyes and corneal oedema
intra-ocular pressure monitoring with hand-held
tonometer
Microphthalmia
Right eyelid coloboma and microphthalmos.
Right microphthalmia with soft tissue
Congenital nasolacrimal
Partial cryptophthalmus (hidden eye)
expander. Left iris coloboma
duct obstruction
50 Sub-specialty —Paediatric ophthalmology
Aims
• Suspect Neisseria gonorrhoeae or Chlamydia trachomatis until
1 Differential diagnosis of leukokoria.
proved otherwise as both can cause blindness.
2 Main sight-threatening eye problems in neonates.
• Systemic and topical treatment is essential.
3 Management of a watering eye.
• Refer both parents to STD clinic.
In a neonate the three most important topics are leukokoria,
Buphthalmos (see Chapter 36)
retinoblastoma and ophthalmia neonatorum.
• A large eye in an infant associated with congenital glaucoma
and a cause of blindness/defective vision.
Leukokoria
• The infant has photosensitivity and watering with elevated in-
A white-coloured pupillary reflex seen when an ophthalmoscope
traocular pressure.
is shone at the pupil. Causes include:
• Needs specialized paediatric ophthalmology management.
• Congenital cataract.
• Hyperplastic primary persistant vitreous (HPPV).
Anophthalmos and microphthalmos
• Retinoblastoma.
• Rare total absence of an eye (anophthalmos) or a very small oc-
• Infections: toxoplasmosis and toxocariasis.
ular remnant (microphthalmos).
• Retinopathy of prematurity (ROP).
• The aim of management is to promote orbital bony develop-
• Coats’ disease.
ment by keeping the ocular remnant (microphthalmos or cyst)
and expanding the soft tissue of the orbit and eyelids sequentially,
Congenital cataract
prior to placing an ocular prosthesis (artificial eye).
• Presents as leukokoria, a dull red reflex, squint or nystagmus.
• If bilateral, the child may be visually inattentive.
Watering eyes/epiphora due to congenital nasolacrimal
• The eye may be smaller but there is usually no relative afferent
duct obstruction (NLDO)
papillary defect unless there is other retinal or optic nerve pathology.
• Causes watery sticky eyes.
• Causes include: idiopathic (most common), familial autosomal
• Aetiology: opening of the lower end of the nasolacrimal duct
dominant, galactosaemia and rubella (also causes microcephaly,
(where it enters the nose in the inferior meatus at the valve of Has-
congenital heart defects, corneal clouding and retinopathy).
ner) is often delayed for several months. Rare causes include ab-
• Needs urgent (within days) assessment with a view to cataract
sent canaliculus and absent or imperforate punctum.
surgery and subsequent amblyopia therapy. Some cataracts are
• Treatment of congenital NLDO:
small and need monitoring and amblyopia therapy.
—Advise the parent that the watering is likely to resolve by age
1 year in 90%.
Retinoblastoma
—Daily small finger massage over the lacrimal sac at the medial
• This malignant tumour of the retina is the most common in-
canthus to open the valve.
traocular tumour of childhood.
—Clean the eyelids with sterile saline.
• It often appears as a white mass growing into the vitreous and
—Antibiotic drops are only rarely required.
causing leukokoria when it is advanced/big.
—If there is an amniocoele (bluish lump) it will usually resolve
• Urgent assessment and treatment is required by a joint paediatric
with systemic antibiotic course. If this doesn’t work do an early
oncology and paediatric ophthalmology team in a specialist centre.
probing at <2 month’s age.
—An expressible mucocoele suggests nasolacrimal duct block
Non-accidental injury (NAI)
requiring dacryocystorhinostomy surgery.
A neonate with leukokoria or ocular trauma may have NAI.
—For persistant watering aged over 1 year, do a syringe and
probing (S&P) ± nasal endoscopic monitering.
Retinopathy of prematurity (ROP)
—If recurrent epiphora, repeat S&P with endoscopic moni-
• This important cause of childhood blindness occurs in pre-term
toring and consider intubation or dacryocystorhinostomy
babies and is screened for by ophthalmologists.
(DCR).
• Treatment with cryotherapy or laser has limited success in
threshold disease.
Ptosis (see Chapter 23)
• Prevention remains the key.
A neonate with an upper eyelid drooping across the visual
• Advanced/untreated ROP may have leukokoria.
axis should be referred urgently to an ophthalmologist with a
• Complications of treatment include cataract and myopia.
view to urgent frontalis suspension surgery and amblyopia
• In severe ROP with retinal detachment, vitreoretinal surgery is
therapy. Otherwise usually wait until age 4 years if visual develop-
often only palliative.
ment is not threatened.
Ophthalmia neonatorum
• Notifiable disease.
• The neonate usually has a unilateral or bilateral purulent con-
KEY POINTS
junctivitis within a few days of birth.
• Leukokoria —retinoblastoma and congenital cataract.
• The ophthalmologist must examine the child and take swabs/
• A watering eye from congenital NLDO usually resolves by 1 year.
scrapes for bacteria (including Gram and Giemsa stains), Chlamy-
• Beware: congenital glaucoma may present with large or watery eyes.
dia immunofluorescent antibody test and viral culture.
Neonates 51
23 Infants and older children
Differential diagnosis in orbital cellulitis
Infants and older children
The most common visual problems (apart
• Rare malignant orbital tumour
from myopia) have usually been detected
of childhood that can
by age 2-4 years. The problems of a child
metastasize. It may present
over 2 and under 12 years relate commonly
as orbital cellulitis
to the eyelids, lacrimal system and orbits.
• Average age of onset: 7 years
Teenagers have their own visual problems
• Grows fast and progresses
with the onset of myopia, presentation of
• If suspected, urgent referral
Leber's optic neuropathy (usually in mid
and biopsy required
to late teens), “hysterical” loss of vision,
headaches and convergence insufficiency.
Post-septal orbital cellulitis
Rhabdomyosarcoma
Reduced vision from albinism has usually
– pre-drainage
been detected by this age
Ptosis
Allergy
Vernal keratoconjunctivitis causing
Vernal giant papillae
Congenital left ptosis
bilateral acquired ptosis
Lumps on and around eyelid
• Benign congenital conjunctival and
subconjunctival yellow fatty lesion.
Lies very close to the lacrimal
ductules, therefore excision is not
advised as it risks a severe dry eye
from lacrimal ductile damage
Orbital, peri-orbital and
Dermolipoma
eyelid haemangioma
Dermoid cyst
• Smooth round non-tender relatively
• Benign congenital tumour often
immobile lump in the superolateral
associated with eyelid coloboma in
> superomedial orbit that gradually
Goldenhar's syndrome. Only very
grows in size. Risk of rupture if in a
limited excision is recommended
prominent position. CT scan is
required to assess extent and plan
surgery. Removal of an intact cyst is
necessary as its yellow cheesy
Limbal dermoid
contents are very irritant
Infections
• Endemic in schools
• Causes chronic follicular
• Typically from pubic lice -
conjunctivitis. Small dome-shaped
unilateral or bilateral causing
itchy lesions around the eyelids and
itchy eyes with crusty lashes
on the hands or arms
from the nits and blood-tinged
debris. Pilocarpine gel to
remove
Molluscum contagiosum
Headlice = pediculosis
52 Sub-specialty —Paediatric ophthalmology
Aims
aberrant eyelid movements with chewing and talking to detect
1 Identify common paediatric eyelid and orbital problems.
Marcus Gunn jaw-winking ptosis. Check under the eyelid.
2 Know why and when to operate on ptosis.
3 Management of orbital cellulitis.
Type of surgery
This depends largely on the level of the levator function. If the
The infant has different problems from the neonate. The most im-
levator function is very poor (<5 mm) the eyelid is internally sus-
portant condition is orbital cellulitis, which must be diagnosed and
pended to the frontalis muscle (frontalis suspension). If there is
treated promptly. Other common paediatric problems encoun-
good levator function, the levator muscle is shortened (anterior
tered include persistent mild drooping eyelid (ptosis), a sticky wa-
levator resection, ALR). When there is a risk of amblyopia in
tering eye and eyelid lumps.
neonate because the lid covers the pupil most of the time, then ur-
Squints are covered in Chapter 21.
gent frontalis suspension with a prolene suture is required.
The child may later need autogenous fascia lata frontalis sus-
Orbital cellulitis
pension (where fascial strips are taken from their upper leg).
Distinguish between pre-septal and post-septal orbital cellulitis.
If the eyelid is only slightly drooping and the child can easily ‘see
The child can be quite ill and febrile, and requires admission.
out from beneath it’ by adopting a small chin-up head position,
there is less risk of amblyopia and the child can wait until aged 4
Pre-septal
years before having ptosis surgery.
• Pre-septal involves only the eyelids but can spread posterior to
the orbital septum to become post-septal.
• One or both eyelids are swollen and tender.
Persistant sticky watering eyes
• White eye, which moves fully with no impairment of vision or
• Blocked nasolacrimal duct requires dacryocystorhinostomy (DCR).
proptosis.
• Vernal/atopic conjunctivitis. Photophobic with swollen eyelids and itchy,
• Treat with i.v. antibiotics.
stringy discharge that is worse in summer —can give an acquired ptosis. His-
tory of atopy. Large giant papillae on tarsal conjunctiva and possibly small lim-
Post-septal
bal lumps (limbal vernal). Treat with topical anti-inflammatory drops.
• Potentially severe life-threatening condition (cavernous sinus
• Blepharitis. Red rimmed sticky eyes with a tendency to recurrent blepharo-
thrombosis), unless treated.
conjunctivitis and watering. Treat with lid toilet and topical antibiotic ointment.
• Painful orbital/eyelid red swelling and proptosis; child is fever-
ish and unwell.
• Associated with an upper respiratory tract infection and un-
Lumps on and around the eye
diagnosed sinusitis.
There are many different lumps —identify capillary haeman-
• May not be able to open eye to see limited eye movements.
gioma, dermolipoma, limbal dermoid and dermoid cyst.
• Conjunctiva red and swollen.
• Vision may be affected: reduced visual acuity and red desatura-
Capillary haemangioma
tion with a relative afferent papillary defect due to optic nerve
Swelling appears at birth or shortly afterwards, then increases in
compression.
size for about 6 months. Most common in the superonasal orbit
• Do a CT scan to exclude sinus disease and subperiosteal ab-
and eyelid. Grows slowly, during which it can cause mechanical
scess, which need surgical draining and bacteriology.
ptosis and risk of amblyopia if the lid covers the visual axis or its
• Infection from: Haemophilus infuenzae, Streptococcus,
weight causes astigmatism. Treated with local infiltration of
Staphylococcus negative rods or Gram.
steroids to speed up resolution and reduce the bulk of the
• Urgent admission, blood cultures and treatment with i.v.
haemangioma. Spontaneously regresses usually after age 1 year.
antibiotics.
Stye (external hordeolum)
• Lash follicle infection —hot red lump that resolves rapily.
WARNING
Rhabdomyosarcoma and leukaemia are important differential diagnoses of
Chalazion
bacterial orbital cellulitis.
• Lump due to an inflamed blocked meibomian gland duct, which
will usually gradually resolve over a few weeks without treatment.
• Topical antibiotic ointment for 7-10 days.
Ptosis (drooping eyelid)
• Incise and curette under short general anaesthetic if not im-
• Congenital dystrophic.
proving with treatment (see Chapter 24).
• Acquired third cranial nerve palsy (rare).
• Inflammation, e.g. vernal keratoconjunctivitis.
KEY POINTS
Ptosis assessment
• Ptosis —risk of amblyopia when eyelid covers the visual axis.
Measure the visual acuity, strength of the levator muscle in mil-
• Ptosis —usually wait until age 4 years before surgery is done.
limetres (levator function), vertical palpebral aperture distance
• Drain subperiosteal abscess in orbital cellulitis.
and skin crease height. Observe Bell’s phenomenon. Look for
Infants and older children 53
24 Common eyelid lumps
Eyelid and periocular anatomy
Orbital
Septum orbitale
Eyelid posterior
margin
Conjunctival fornix
lamella
Superior tarsal
Meibomian
Skin crease
plate
Tarsal plate
glands
Lash line
Conjunctiva
Meibomian orifice
Lateral
Medial palpebral
Eyelid anterior
Grey line
canthal
ligament
lamella
Mucocutaneous
tendon
Lacrimal sac
junction
Skin
Septum
Inferior tarsal
Orbicularis
orbitale
plate
muscle
Cross-section lids
Front view tarsal plates
How to do an I & C
Layers of the skin
Local anaesthetic (topical plus infiltrative)
Tumours may arise from any component of the skin
Chalazion or
Place a small eyelid clamp and evert the eyelid
meibomian cyst
Use an 11 blade to incise vertically into the cyst on
Keratin layer
Melanocytes
Epidermis
arises in tarsal
the tarsal surface (in a direction away from the eye
Basal layer
plate meibomian
and avoiding the eyelid margin)
Basal cell carcinoma
arises from here
gland
Curette spoon to curette out the jelly
Dermis
Place a firm pad plus chloromycetin ointment for up
Basement
membrane
to 24 h
Sebaceous
Continue the ointment three times a day for 4 days
gland
Subcutaneous
Follicle
layer
I & C chalazion
Sweat gland
Artery Vein Nerve
How to evert an upper eyelid
Cysts of Moll - simple fluid
(chalazion)
retention cysts from sweat glands
(a)
(b)
(c)
(d)
Patient looks down
Basal cell carcinoma (BCC)
Squamous cell carcinoma
Pull on eyelashes and place a
cotton bud above the skin crease
Right lower eyelid nodular BCC Right medial canthal nodular BCC
Mohs' micrographic excision
periocular tumour
Evert!
54 Sub-specialty —Eyelid, lacrimal and orbit
Aims
tissue locally. It can invade the orbit if neglected or inadequately
1 Recognize a chalazion and understand its treatment.
treated. Early treatment is recommended —incisional biopsy to
2 Recognize a basal cell carcinoma.
make the diagnosis and excisional biopsy with a 2-4 mm margin of
3 Treatment of periocular basal cell carcinoma.
clear tissue, to completely remove the tumour.
Nodular BCC is the commonest form and its edges are easy to
Differential diagnosis of periocular tumours
define. There is a rarer morphoeic type with ill-defined edges and
Many different lumps are found on the eyelids, both benign and
extent, which is more difficult to manage and has a higher recur-
malignant.
rence rate. BCC does not metastasize. Surgical excision and re-
• Benign: chalazion, papilloma, retention cyst and sebaceous cyst.
construction is the mainstay of treatment of BCC although
• Malignant:
cryotherapy and radiotherapy are occasional options.
—basal cell carcinoma (BCC);
—squamous cell carcinoma (SCC);
Mohs’ micrographic surgery
—sebaceous gland carcinoma (SGC);
Mohs’ micrographic excision of BCC is a special technique to re-
—malignant melanoma;
move the tumour with frozen sections of the deep bed of the
—Merkel cell tumour;
tumour to ensure complete excision, done by dermatological
—other rare, e.g. sweat gland tumours.
surgeons especially trained in the technique. It provides good
clearance of tumour with maximum normal tissue preservation
Benign lumps
and low recurrence. An oculoplastics-trained ophthalmologist
Chalazion/meibomian cyst
then does the periocular reconstruction.
Inflamed painful lid swelling due to a blocked meibomian duct —
there are at least 27 ducts in each eyelid and each one has the po-
Squamous cell carcinoma
tential to block! Initial treatment in an adult is by hot compresses
SCC is rarer than BCC but more rapidly growing with a greater
and topical antibiotic ointment four times a day for 2 weeks. If the
potential for spread, especially perineural. It is a red lump with
lump persists, do an incision and curettage (I&C).
a variable appearance. It is much more common in immuno-
If an assumed chalazion recurs, particularly in an older person,
suppressed patients, for instance post renal or liver transplant pa-
do an incisional biopsy urgently for histopathological analysis as
tients on long-term immunosuppression drugs.
this may be a sebaceous gland carcinoma (meibomian gland
carcinoma). This is highly malignant.
Sebaceous gland carcinoma
SGC may masquerade as a recurrent chalazion or unilateral ble-
Solar keratoses (actinic keratoses)
pharitis in an elderly female patient.A large incisional biopsy is re-
These are dry scaly patches due to dysplastic intraepidermal pro-
quired for histopathologic analysis. This tumour can spread by
liferation of atypical keratinocytes and occur on the face in older,
lymphatics and the patient requires radical neck excision. There is
fair-skinned persons who have lived in sunny climates. There is a
a significant 5-year mortality.
low risk of malignant transformation into squamous cell carcino-
ma. Fortunately many solar keratoses regress spontaneously over
Malignant melanoma
1-2 years, but 15% recur. Treatment is with cryotherapy or 5-
Very rare but potentially very serious. Most pigmented lesions
fluorouracil.
around the eye are benign but the usual caveats apply —if there is
an increase in size or bleeds, urgent referral is needed.
Malignant lumps
Basal cell carcinoma (‘Rodent ulcer’)
KEY POINTS
This is the commonest periocular malignant tumour. It occurs
• A recurrent chalazion may be a malignant tumour —sebaceous gland
most commonly on the lower eyelid, then medial canthus, upper
carcinoma.
lid and lateral canthus. It is typically a nodular pearly lump with no
• Basal cell carcinoma is the commonest eyelid malignancy.
hair or lashes on it, but with telangiectatic blood vessels. The cen-
• Mohs’ micrographic surgery is the gold standard for excising periocular
tral zone may bleed and ulcerate. It can be morphoeic and have in-
basal cell carcinoma.
distinct margins. It grows slowly by direct extension and destroys
Common eyelid lumps 55
25 Common eyelid malpositions
Supracilia
Nerve supply to eyelids
Limbus
Upper eyelid
Upper lid
Upper punctum
Levator palpebrae superioris (cranial nerve III) and Müller's superior tarsal
skin fold
muscle (sympathetic) open the upper eyelid
Plica
Cilia
Orbicularis oculi (cranial nerve VII) closes the eyelid
Lateral
Medial canthus
Lower eyelid
canthus
Caruncle
The capsulopalpebral fascia (linked to the inferior rectus muscle - cranial
Lower lid margin
Lower punctum
nerve III) and Müller’s lower tarsal muscle (sympathetic) help the lower lid
Lower lid skin crease
Pretarsal orbicularis
move 2-4 mm downwards on downgaze and help open the lids
Preseptal orbicularis
Orbicularis oculi (cranial nerve VII) closes the eyelid
Whitnall's
Pre-aponeurosis fat
ligament
Entropion
Distichiasis
Levator aponeurosis
Müller's muscle
Levator muscle
Orbicularis muscle
Superior rectus
muscle
Tarsal plate
Intracanal fat
Pretarsal orbicularis
Preseptal orbicularis
Inferior rectus
muscle
Congenital lower lid entropion
Müller's inferior
Inferior oblique
- epiblepharon
tarsal muscle
muscle
Ectropion
Involutional lower lid entropion
ii) Botulinum toxin A temporary
i) Causing red sore eye
oricularis chemodenervation (surgery
Involutional ectropion
Cicatricial ectropion
is the definitive treatment)
Contact dermatitis from glaucoma
drops (reversible on stopping drops)
Facial palsy with anaesthtic cornea
Graves’ orbitopathy (thyroid eye disease)
(VIIth and Vth CN palsies) causing
- mild proptosis, right upper and bilateral
neurotrophic keratitis and scarring
lower lid retraction
Eyelid and brow measurements
Lateral tarsal strip
ULB
LidF
Facial palsy (lower motor neurone) and lagophthalmos
UMRD
LMRD
PA
The lateral tarsal strip is tucked into the lateral orbit at the lateral
LSS
canthus and sutured to the periosteum at the lateral orbital rim.
This is a widely used useful technique
ULB
= Upper lid brow
PA
= Palpebral aperture
Definitions
LidF
= Lid fold
Trichiasis
=
rubbing of abnormal inturned eyelashes
UMRD
= Upper margin reflex distance
against the eye causing discomfort
Used to shorten eyelid in entropion
LMRD
= Lower margin reflex distance
Distichiasis
= additional row of aberrant lashes arising
and ectropion surgery
LSS
= Lower scleral show
from the meibomian orifices
56 Sub-specialty —Eyelid, lacrimal and orbit
Aims
Aetiology
1 Examine an eyelid.
• Involutional —older persons.
2 Identify entropion (lid in) and ectropion (lid out).
• Cicatricial causes, e.g. post blepharoplasty, actinic, following
3 Identify ptosis (lid down) and eyelid retraction (lid up).
skin tumour excision, etc., and contact dermatitis.
• Mechanical —the weight of an eyelid tumour pulling the eyelid
Lid function
outwards.
• Ocular protection.
• Facial palsy (VIIth nerve palsy).
• Tear film distribution.
Symptoms
Examine an eyelid
Watering, irritation, grittiness and redness.
• Measure visual acuity!
• Look at the whole face, eyebrow height and symmetry
Treatment
• Measure the vertical palpebral aperture (PA) and margin reflex distances
• Involutional ectropion —shorten the eyelid horizontally and
(MRDs) and amount of scleral show (SS) above or below the limbus in mm
turn the medial part inwards using a lateral tarsal strip and exci-
• Measure the levator function (LF) in mm—upperlid excursion from full
sion of a diamond shape of medial tarsal conjunctiva or medial
downgaze to full upgaze
spindle (LTS + MS).
• Assess orbicularis strength and Bell’s phenomenon (do the eyes roll up-
• Cicatricial ectropion —skin graft or flap to lengthen the anterior
wards under lid on closure?)
lamella; horizontal shortening may also be required.
• Exclude aberrant movements
• Contact dermatitis —stop the causative eye drops or change to
• Lag on downgaze —eyelid hangs up a bit on downgaze
preservative-free drops. No surgery needed.
• Detect lagophthalmos —eye remains partially open on attempted closure
• For facial palsy, see below.
• Exclude distichiasis, trichiasis, entropion and ectropion
• Examine tarsal conjunctiva and conjunctival fornices to exclude scar or
Ptosis
tumour
Definition of eyelid ptosis: Abnormally low position of the upper
eyelid margin caused by poor function of the levator palpebrae
Entropion
superioris or Müller’s muscle.
Entropion: Eyelid turns in towards cornea and lashes touch the
Paediatric ptosis see Chapter 23.
surface of the eye.
Actiology:
• Involutional or aponeurotic (thinning or dehiscence of the an-
Aetiology
terior part of the levator, the aponeurosis). There is good levator
• Involutional —older persons.
function (LF). Occurs commonly in the elderly.
• Spastic (causes by severe squeezing of the eyelids in response to
• Myogenic. LF is very poor. Includes the congenital dystrophic
ocular discomfort).
(fatty) levator muscles in children and myopathies in adults, e.g.
• Cicatricial entropion secondary to conjunctival scarring, e.g.
chronic progressive external ophthalmoplegia.
staphylococcal lid margin disease (mild entropion) or ocular
• Neurogenic. The LF is usually poor, e.g. IIIrd nerve palsy.
cicatricial pemphigoid (severe entropion) or trachoma.
• Mechanical. Usually good LF. A tumour weighs the eyelid
down, e.g. neurofibromatosis.
Pathogenesis
• Traumatic ptosis may be aponeurotic, myogenic or neurogenic.
Thinning of the lamellae and disinsertion of the lower lid retrac-
tors. The pre-septal overrides the pretarsal orbicularis causing in-
Symptoms
turning of the lower lid.
• Cosmetically poor appearance.
• Functional —reduces the visual field.
Symptoms
Ocular irritation, discomfort, reflex watering (hypersecretion),
Management
redness and occasionally keratitis if left untreated. It is worse lying
Depends on the type of ptosis and LF. Normal or good LF is
down, e.g. reading in bed.
>10 mm. Moderate LF is 5-10 mm. Poor LF is <5 mm.
• Good and moderate LF: anterior levator resection —tuck / ad-
Treatment
vance the levator aponeurosis or muscle.
1 Temporary treatment:
• Poor LF: frontalis suspension with autogenous fascia lata.
• Lid taping and topical lubricants.
• Botulinum toxin A injected into the pre-septal orbicularis alle-
Eyelid retraction
viates symptoms for up to 4 months but has to be repeated.
Lower motor neurone facial palsy (7th CN palsy) and thyroid eye
2 Surgery is the mainstay of treatment.
disease can both cause exposure keratitis. See Chapters 28 and 49.
• Lateral tarsal strip with everting sutures (LTS + ES).This short-
ens the lower eyelid horizontally and everts the eyelid.
KEY POINTS
• Simple everting sutures (ES) alone.
• Measurement is important in eyelids.
• Involutional entropion is treated temporarily with botulinum toxin A.
Ectropion
• Facial palsy causes lagophthalmos and a risk of exposure keratltis.
Ectropion: Lower eyelid turns outwards away from the eye.
Common eyelid malpositions 57
26 Lacrimal (tearing)
Lacrimal anatomy
Lacrimal syringing
The lacrimal drainage system consists of the punta,
canaliculi, lacrimal sac and nasolacrimal duct (NLD)
Lacrimal
Canaliculi
gland
Lacrimal
Lacrimal physiology
Tear
sac
The tears are produced by the lacrimal gland and the
accessory lacrimal tissue (glands of Krause and
meniscus
Lacrimal pump
Middle
Wolfring) and are swept over the eye surface with
turbinate
Nasolacrimal
each blink. Tear evaporation occurs (approximately
Inside of
duct (NLD)
25%). The marginal tear strip drains via the lower
nose
Inferior meatus
canaliculus predominantly (70%) and 30% via the
Inferior
upper canaliculus. The lacrimal pump mechanism
turbinate
refers to the action of the eyelids contracting and
pumping the tears into the lacrimal sac
Nasal endoscopy
This is a very useful technique that provides direct
observation of the nasal space both in out-patients
and during lacrimal surgery. A rigid Hopkins 4 mm 0∞
rigid nasal endoscope is used to look at the opening
Right mucocoele-chronic dacryocystitis
of the NLD into the nose and at the DCR surgery
site
Normal dacryocystography (DCG) - left side
DCG shows right anatomically blocked
shows free drainage contrast media into nose
NLD. Note that no contrast material
Left external skin approach
is seen entering the NLD
dacryocystorhinostomy (DCR) -
per-operative view
Lacrimal sac
Canula in inferior
canaliculus
Lacrimal sac
NLD
Canula in inferior
canaliculus
Dotted line shows
Contrast in lateral
where NLD should
wall of nose
normally fill
A mucosal-lined opening is made from
the lacrimal sac to the nose after the
Nuclear lacrimal scintigraphy - showing
intervening bone has been removed
left functional NLD block
R
L
Pooling of tears containing technetium 99
New opening
in the conjunctival fornix
from sac into
Blocked
nose for tears
Functioning DCR rhinostomy
NLD
Fluorescein passing freely down
lateral wall of nose
NLD
Lacrimal sacs
Canaliculi
Conjunctival fornix
Lacrimal
sac
Keratome
Middle
Endonasal endoscopic
turbinate
surgical DCR
Endoscope
- the lacrimal sac is
Inferior
Jones Pyrex bypass tube
approached from inside the
Floor
turbinate
- per-operative insertion
nose instead of via the skin
of nose
58 Sub-specialty —Eyelid, lacrimal and orbit
Aims
•
Slit lamp examination:
1 Understand the difference between hypersecretion and
—exclude blepharitis;
epiphora.
—exclude punctual stenosis;
2 Use of syringing in assessment of epiphora.
—tear meniscus.
3 Dacryocystorhinostomy.
•
Probe and syringe/irrigate lacrimal system
(use topical
Nasolacrimal duct obstruction is a common cause of epiphora
anaesthesia) After the punctum has been dilated, a curved
(watering eye). Surgery to correct this is called dacryocystorhinos-
lacrimal canula is gently introduced into the canaliculus and
tomy (DCR) and can be done via the nose (endonasal) or via the
advanced into the lacrimal sac and saline is irrigated. If there is
skin (external). However, there are many causes of a watering eye
passage of saline into the throat this indicates a patent system,
and careful assessment is required.
whereas no passage indicates a blocked system. Sometimes only
some saline goes down, indicating a partial NLD block.
Definitions
•
Special clinical tests: Jones’ tests used to confirm and localize
Epiphora: Reduced tear outflow from lacrimal system obstruction
functional epiphora (not used much).
at any point from the punctum, canaliculus, sac and nasolacrimal
•
Nasal endoscopy:
duct. Nasolacrimal duct obstruction is the commonest.
—The nasal endoscope is used to look inside the nasal space
Hypersecretion: Excess production of tears in response to stimu-
preoperatively to exclude nasal pathology such as tumours, in-
lation of the trigeminal nerve from corneal irritation (e.g. corneal
flammation and polyps as well as anatomical variations.
foreign body), dry eye or conjunctival irritation (e.g. blepharitis,
—It is also used to inspect the internal opening (rhinostomy)
conjunctivitis).
made by the DCR surgery and to check its function.
Functional epiphora: Epiphora in the presence of patent syringing
—A successful DCR has a positive functional endoscopic dye
without hypersecretion due to:
test (FEDT), i.e. a drop of fluorescein 2% placed in the conjunc-
• eyelid malposition, e.g. lower lid ectropion;
tival fornix is seen emerging from the rhinostomy a few seconds
• lacrimal pump failure, e.g. facial palsy;
later.
• punctual, canalicular and nasolacrimal duct stenosis (without a
•
Radiology imaging studies
complete obstruction).
—Dacryocystography (DCG) with radio-opaque material for
Mucocoele: A dilated lacrimal sac containing mucous. often seen
anatomical detail. Used to determine the site of the obstruction.
as a lump at the medial canthus. The nasolacrimal duct distal to it
—Lacrimal scintigraphy is a nuclear scanning technique using a
is blocked.
drop of technetium 99 placed in the conjunctival fornix and a
gamma camera to observe its passive drainage. It is used to de-
Pathogenesis
tect physiological tear drainage in the assessment of functional
• The commonest cause of epiphora is a blocked nasolacrimal
NLD obstruction.
duct (NLD). This can be primary from chronic inflammation with
subsequent fibrosis and stenosis, or less commonly, secondary
Surgery
from sarcoidosis, Wegner’s, tumour or trauma. DCR is the treat-
DCR can be external (via the skin) or endonasal (via the nose).
ment of choice.
• Aim of DCR. To relieve watering and/or sticky eye from NLD
stenosis/obstruction by creating a functioning rhinostomy be-
tween the lacrimal sac and the nasal space.
• External (skin incision) approach DCR has the best track
WARNING
record and is the gold standard —success rates 95-98%.
Canalicular disease. If there is severe canalicular obstruction (e.g. following
• Endonasal DCR (via the nose) approach DCR is less invasive
radiotherapy, some chemotherapy drugs, herpes simplex infection) a DCR is
but also has lower results, 70-86%. The rigid nasal endoscope
done with a Jones Pyrex glass tube inserted.
provides good illumination and magnification transnasally, with
either: (i) laser, (ii) surgical, or (iii) powered instruments to make
the rhinostomy. The xomed diamond burr has the best results.
Investigate the watering eye
Many patients prefer endonasal DCR because it avoids skin in-
History
cision. However, the advantage of external DCR is that its surgical
Stickiness/watering worse is outside or constant. There is an
outcome is still better than endonasal techniques.
inflamed or quiet lump at the medial canthus. History of nasal
disease, sinusitis, polyps or nasal trauma. Previous conjunctivitis,
eye drops and drugs.
KEY POINTS
• Ectropion is a cause of epiphora.
Assessment of the watering eye
• Endoscopic endonasal DCR avoids a skin incision.
• External examination of the forehead, periocular and medial
• External approach DCR still has the best results —95-98% success.
canthus to exclude eyelid malposition and mucocoele.
• Fluorescein dye retention test: watch a drop of fluorescein 2%
rapidly disappear from the conjunctiva if the system is patent or
dye retention if blocked.
Lacrimal (tearing) 59
27 Basic orbital assessment
Levator palpebral
Eye and orbit
superioris
Superior rectus
Lacrimal
Superior oblique
gland
Ethmoid sinus
Lateral
Medial rectus
rectus
Lacrimal sac
Zygoma
Inferior rectus
bone
Inferior oblique
Fat
Infraorbital nerve
Nasolacrimal
duct (NLD)
Maxillary sinus
Nose
Maxilla bone
Orbital bones
Medial orbital wall
Superior orbital
fissure
Sac/NLD
Ethmoid lamina
Eye
papyracea
Ethmoid
air cells
Optic foramen
Lacrimal bone
Medial
Zygoma
rectus
Inferior orbital
Lateral
fissure
rectus
Maxilla bone
Optic nerve
Zygomatico
Infraorbital
Optic
facial foramen
foramen
foramen
Zygoma bone
Proptosis / enophthalmos
Orbital cellulitis
Hertel exophthalmometry to measure proptosis / enophthalmos
Left orbital
subperiosteal
abscess and
sinus disease
Blue triangle lined up with marker line
before drainage
This patient measures 21 mm at
100 mm
Aims
Pseudophthalmia: Socket contains an orbital implant.
Assessment of a patient with proptosis. This chapter covers the
Microphthalmia: Socket contains a very small eye/ocular remnant.
anatomy of the orbit and the systematic approach to examining
Phthisical eye: A blind shrunken eye.
a patient with proptosis. The most common cause of proptosis
Enucleation: Removal of an eye in its entirety —detaching it from
in adult patients is thyroid eye disease, also known as Graves’
the optic nerve and the extraocular muscles.
orbitopathy.
Evisceration: Removal of the contents of the eye leaving
the outer sclera, attached optic nerve and extraocular muscles.
Definitions
Post-enucleation socket syndrome: Deep sunken ‘eye’ when the
Proptosis: Eye protruding.
volume of the removed eye has not been adequately replaced.
Enophthalmos: Eye sunken in.
Decompression orbit: Removing usually the medial and lateral
Anophthalmia: Socket contains no eye.
orbital walls to expand the orbit in thyroid eye disease.
60 Sub-specialty —Eyelid, lacrimal and orbit
Orbital anatomy
Enophthalmos. Is there a history of trauma and possible orbital
The bony orbit has four margins and walls and is adjacent to the
floor fracture? Is there a phthisical eye? Is there an ocular pros-
ethmoid sinus (medial) and maxillary sinus (inferior). It contains
thesis? Has the patient had an eye enucleated? Was there an or-
the optic foramen for the optic nerve and ophthalmic artery, the
bital implant placed after enucleation/evisceration? Is there a
superior orbital fissure (cranial nerves and blood vessels) and in-
secondary post-enucleation socket syndrome? Are the eye move-
ferior orbital fissure. The infraorbital nerve lies in the floor, partly
ments restricted? Is the socket lining contracted?
in a bony canal.The orbit contains a lot of fat and connective tissue
septae that support and cushion the eye and its muscles, optic
Check cranial nerve (CN) function
nerve, nerves and blood vessels.
• IIIrd, IVth and VIth CN: extraocular muscle movement.
• VIIth CN: upper facial musculature.
Orbital assessment
• Vth CN: corneal, periorbital and forehead sensation.
History
• Gradual or sudden onset. If slow/non-inflamed it is more likely
Feel the orbit
to be benign.
Palpate the orbital rim. If a mass is detected, is it separate from the
• Unilateral or bilateral.
rim? Describe its feel and shape and draw a picture of its shape
• Orbital swelling/sunken.
and location.
• Orbital pain.
• Periorbital redness (e.g. orbital cellulitis).
Complete the examination
• Periorbital numbness.
Palpate the temporal fossa for extension of swelling. Exclude
• Visual disturbance.
pre-auricular, submandibular and cervical lymphadenopathy.
• Double vision.
Examine the neck for thyroid enlargement or thyroid scar. Check
• Drooping eyelid.
sensation in skin around orbit.
• Systemic: malignancy or thyroid problem.
• Previous trauma.
• Ascultation for a bruit —caroticocavernous fistula.
WARNING
Orbital tumour spread. The orbit does not have lymphatics, but extensive tu-
Clinical examination
mour that involves the lids and periorbital area can metastasize to local lymph
Visual function (if eye present) and eye examination
nodes.
• Visual acuity and pupil reactions.
• Colour vision ± visual fields.
• Retina and optic disc.
Investigations
• CT scanning. Axial and coronal views show the position of the
Globe position
optic nerve well and also the sinuses and orbital walls (request
Measure proptosis with Hertel exophthalmometry —is it axial or
bone window settings too). Suspected vascular lesions need
non-axial?
contrast.
• MRI. Good for soft tissue but does not show bone so well.
• Orbital ultrasound. Colour Doppler ultrasound to measure size
Proptosis
and show bloodflow/velocity within lesion.
• Axial
(anteroposterior protruding globe) without horizontal or vertical
displacement. This suggests a generalized orbitopathy such as thyroid eye
disease or an intraconal mass.
• Non-axial. Horizontal or vertical displacement of globe caused by a
KEY POINTS
mass pushing it sideways. For instance, a lacrimal gland tumour in the
• Proptosis is axial or non-axial.
superolateral quadrant pushes the globe inferomedially.
• Palpate the orbit to help detect a mass.
Basic orbital assessment 61
28 Orbital and thyroid eye disease
Graves’ orbitopathy (thyroid eye disease)
Bilateral proptosis, periorbital swelling and left esotropia
Marked proptosis and redness - active phase
- quiet phase
CT scan - enlarged medial
and inferior rectus muscles
in Graves’ orbitopathy
Tumour behind eye
CT scan showing tumour
(benign)
Right proptosis from
large cavernous
haemangioma
Enucleation
Indications for enucleation include a painful blind eye, choroidal malignant melanoma
and a severely disrupted eye following trauma.
The eye is eviscerated if there is an intractable endophthalmitis
Post-enucleation socket syndrome - no orbital implant
placed at time of enucleation
Wearing a thick artificial eye
Thick artificial eye
Porous polyethylene sphere implant inserted into socket.
but still very enophthalmic
Orbital sphere implant is needed to replace lost volume
Aims
Graves’ orbitopathy
1 Management of Graves’ orbitopathy.
Most patients present within the first 6-12 months of hyperthy-
2 Recognize an artificial eye.
roidism. Male patients and smokers have a more aggressive dis-
This chapter cover proptosis, orbital masses and enucleation.
ease. There is an active phase with inflammation which lasts up to
1 year, and a subsequent inactive stable phase.The former is treat-
Common orbital problems
ed medically with immunosuppression (e.g. steroids and azathio-
• Adult:
prine) and once the disease is inactive surgery to the orbit, muscles
—Graves’ orbitopathy (thyroid eye disease) (most common);
and eyelids can be considered.
—idiopathic orbital inflammation;
—cavernous haemangioma;
WARNING
—lacrimal gland tumour;
Early orbital decompression surgery is only done if there is marked compres-
—secondary tumours;
sive optic neuropathy.
—nerve cell or sheath tumours.
• Child:
There is a varied presentation:
—dermoid cyst;
• Proptosis.
—haemangioma;
• Reduced colour vision from optic nerve compression.
—rhabdomyosarcoma;
• Restrictive strabismus with mainly inferior and/or medial rectus
—Craniofacial abnormality.
muscle enlargement causing diplopia.
62 Sub-specialty —Eyelid, lacrimal and orbit
• Eyelid retraction.
Orbital and lacrimal gland tumours
• Lagophthalmos.
Orbital and lacrimal gland tumours cause proptosis and require
• Exposure keratitis.
incisional or excisional biopsy by a trained oculoplastics orbital
• Conjunctival redness and cheimosis.
surgeon. Lymphoma and metastases are the commonest malig-
• Periorbital swelling.
nant tumours.
The aim of treatment is to preserve vision, with eyes comfort-
Many anterior and mid orbital tumours can be biopsied via a
able and looking normal, with full lid closure.
skin approach. More posterior intraconal and lacrimal gland
tumours (pleomorphic adenoma) require excision via a lateral
Graves’ orbitopathy management
orbitotomy.
Indication
Phase
Medical treatment
Surgery
Enucleation
Compressive Active
• Pulsed steroid
Orbital
When an eye is removed its volume must be replaced by a buried
optic
therapy
decompression
spherical orbital implant to which the rectus muscles are attached.
neuropathy
• Systemic
An ocular prosthesis (artificial eye) is made to match the normal
steroids,
eye; usually it is acrylic and hand painted. If the volume of the enu-
azathioprine
cleated eye is not replaced the patient has a sunken socket ap-
and orbital
pearance called post-enucleation socket syndrome and may need
radiotherapy
a secondary buried orbital implant.
Proptosis
Inactive
Orbital
decompression
Strabismus
Inactive
Adjustable suture
KEY POINTS
rectus recession
• Graves’ orbitopathy —do decompression before eyelid surgery.
• Important to replace eye volume lost at enucleation/evisceration with an or-
Eyelid
Inactive
• Graduated
bital implant and artificial eye.
retraction
retractor recession
(upper eyelids)
• Hard palate
mucosal graft,
alloderm or
auricular cartilage
(lower eyelids)
Periorbital
Inactive
Blepharoplasty
swelling
Skin changes Inactive
Laser resurfacing skin
Orbital and thyroid eye disease 63
29 Common conditions affecting the external eye
External eye and lid margin zone
Tear film
Lipid layer
Aqueous layer
Posterior margin
Meibomian orifice
Posterior margin
Meibomian orifice
Grey line
Mucin
Grey line
Lash line
Mucocutaneous
Corneal epithelial
Lash line
junction
cells (microvilli)
Tarsal
plate
Rhinophyma with lower eyelid ectropion, blepharitis and meibomianitis
Upper eyelid entropion - mild cicatricial from chronic
staphylococcal lid margin disease
Pit
Thick meibomian
secretion
Crusts
Red rimmed
margin
Collarettes
Upper eyelid cicatricial entropion
Upper eyelid held up
Everted upper eyelid
Conjunctival
Linear
scarring and
scarring
Punctate fluorescein
symblepharon
Tarsal
or rose bengal stain
(adhesion)
conjunctiva
Superior limbic keratitis
Ocular cicatricial pemphigoid
Conjunctiva
Scarring
Cornea
Posterior
marginization of
meibomian orifice
Lashes
and blunting of
touch
posterior margin
Pterygium
Ocular cicatricial pemphigoid
cornea
Aims
Diseases primarily affecting the tear
Detection and medical management of:
film/epithelium/conjunctiva
• blepharitis
• Idiopathic dry eye.
• dry eyes
• Severe dry eye associated with Sjögren’s syndrome and other
• allergic eye disease.
autoimmune conditions.
• Graft versus host disease.
Diseases of the external eye
• Stevens-Johnson syndrome.
• Blepharitis.
• Ocular cicatricial pemphigoid.
• Trachoma causing cicatricial entropion.
• Pterygium.
Treatment
• Allergic eye disease.
Treatment depends on the underlying cause in conjunction with
topical lubricating drops. If severe, corneal scarring with super-
ficial vascularization leads to reduced vision and even corneal
perforation.
64 Sub-specialty —External eye disease
Common conditions
idiopathic (approximately 50%) and secondary causes include
Blepharitis and meibomionitis
rheumatoid athritis, lupus or scleroderma.
Blepharitis
Other causes of dry eye
Low-grade chronic staphylococcal lid margin disease with ‘red-
• Stevens-Johnson syndrome.
rimmed’ eyelids in young adults and middle-aged persons.
• Ocular cicatricial pemphigoid.
Symptoms
• Lacrimal gland trauma (surgical excision or ductile destruction)
Itchy, sore, watery eyes.
and chemical, radiotherapy and thermal injury.
• Fibromyalgia.
Signs
• Chronic fatigue syndrome.
Red-rimmed lid margins, eyelash crusts and collarettes, and
distorted lid margin microanatomy: irregularities, pits and
Allergic eye disease
telangiectasia.
• Hayfever: seasonal allergic conjunctivitis. Bilateral, itchy, wa-
tery eyes with lid swelling and sometimes mucous discharge. It is
Management
a type 1 immediate immune response with histamine release to
• Daily lid hygiene using sodium bicarbonate or dilute baby
allergens such as pollen. It is worse in the young with a history
shampoo and cotton bud lash scrubbing.
of atopy. May also have rhinorrhoea and sneezing. Management
• Chloramphenicol ointment, or G fusithalmic
is with topical mast cell stabilizer (e.g. sodium chromoglycate or
• ±Doxycycline or Minocycline.
lodoxamide).
Meibomianitis
• Perennial allergic conjunctivitis. Bilateral, episodic symptoms.
Thick oily meibomian secretion causing stingy sore eyes and red
Triggered by allergens such as house-dust mites, moulds, pollens,
thickened eyelids. Often associated with rosacea. Management is
food preservatives and animal danders. Management is as for
as for blepharitis, adding tetracycline antibiotic for rosacea.
hayfever, plus oral and topical antihistamine when severe.
• Vernal keratoconjunctivitis sicca (VKC). This is a young per-
Upper eyelid entropion
son’s disease (7-11 years) with characteristic upper tarsal con-
Mild upper eyelid entropion from chronic staphylococcal lid mar-
junctival cobblestones (see Chapter 23). Also includes bilateral,
gin disease.
seasonal, red, puffy, itchy eyes with photophobia, watering and
mucous. It may induce ptosis. There are often perilimbal giant
Symptoms
papillae, known as limbal vernal. Management is as for hayfever,
Foreign body lash sensation and dry, gritty eyes.
plus topical steroids when severe.
Signs
• Acute allergic conjunctivitis. Sudden, unilateral, itchy lid
Trichiasis and punctate epithelial corneal stain.
swelling and marked conjunctival chemosis. Signs are worse than
symptoms. Triggered by plant allergens. Resolves spontaneously
Management
without treatment within 24-36 h.
• Epilate, electrolysis and cryotherapy trichiasis.
• Topical lubricants.
Superior limbic keratitis (SLK)
• Surgery: anterior lamella reposition.
Symptoms
Redness, burning, grittiness, photophobia and frequent blinking.
Pterygium (see Chapter 14).
Signs
Dry eyes
Bilateral superior conjunctival punctate stain with fluorescein and
Idiopathic dry eyes
rose bengal. The superior limbal conjunctiva is swollen and there
Symptoms
may be fine tarsal conjunctival papillae.
Gritty, sandy, burning dry eyes with reflex tear flooding
(hypersecretion).
Treatment
Treatment is with intense topical lubricant drops.
Signs
Poor tear film, interpalpebral punctuate epithelial staining, and
Ocular cicatricial pemphigoid (OCP)
poor wetting on litmus paper (Schirmer’s test).
This severe and fortunately rare conjunctival disease has an insidi-
ous onset with redness, grittiness and photophobia (early stages).
Management
Later there is cicatricial entropion, severe dry eye, corneal scarring
• Vigorously treat any meibomianitis and blepharitis.
and opacification. There is conjunctival fornix loss with sym-
• Artificial tears without preservatives and carbomeric gels.
blepharon and reduction of eye movements. Other mucous mem-
• Punctal occlusion can be done.
branes may be involved (e.g. mouth, nasal mucosa). Treatment is
with systemic immunosuppression, e.g. dapsone.
Sjögren’s syndrome
Hypofunction of the exocrine glands affecting the lacrimal and
salivary glands and the gastrointestinal tract. It affects women in
KEY POINTS
90% cases, with onset between 35 and 55 years. There is severe fa-
• Blepharitis is a common cause of red-rimmed, itchy eyes.
tigue, dry eyes, nose, throat, dental caries and digestive problems.
• Use topical lubricant drops (hypromellose) for dry eyes.
Vision can be impaired from epithelial damage and subsequent
• Excise pterygium only if encroaching onto the cornea and visual axis.
conjunctival and corneal scarring. Primary Sjögren’s syndrome is
Common conditions affecting the external eye 65
30 Common conditions affecting the cornea
Corneal structure
Aim
Air
5 corneal layers
Corneal disease
Tear film
Epithelium
Corneal opacity ± vascularization
Bowman's layer
Reduced vision
Stroma
Aqueous
Descemet's membrane
Grafting
Endothelium - contains
‘pump’ which dehydrates
The aim is to treat corneal disease
the corneal stroma
medically and to avoid progression
Bacterial keratitis with
Wessely's ring
hypopyon
Bacterial keratitis
(acanthamoeba)
Immune ring in
corneal stroma
Abscess
Acanthamoeba
nidus of infection
Hypopyon
(inflammatory
cell layer)
Dendritic keratitis
Herpes simplex dendritic ulcer
Herpes simplex disciform keratitis
Dendritic
ulcer
Herpes zoster ophthalmicus
Note that
vesicles
and
Vi
Normal cornea
redness
does NOT
Vii
Conical corneal
cross the
ectasia
midline
Viii
Affects the area
Keratoconic cornea
supplied by the first
division (Vi) of the
trigeminal nerve
Early vesicular phase
Hydrops in keratocous
- acute central corneal
CCIN
swelling and reduced
vision
Pearly elevated
intraepithelial
neoplasia
66 Sub-specialty —External eye disease
Aims
Treatment of epithelial disease is with antiviral medication (e.g.
1 Outline the basic anatomy of the cornea.
aciclovir topically and/or systemically). Judicious use of topical
2 Signs and symptoms of corneal disease.
corticosteroids for disciform keratitis.
3 Describe common disease processes involving the cornea.
WARNING
Corneal clarity
Steroid drops. Do not give steroid drops in the presence of active epithelial
The cornea is a clear because it has a highly organized structure of
disease as may cause ulceration and blindness.
collagen fibrils, it is free of blood vessels and allows the passage of
light in an organized way so a clear image may be focused on the
2 Herpes zoster ophthalmicus
retina. The corneal layers all contribute to its function. The en-
This affects the Vth cranial nerve with segmental skin vesicles and
dothelial cells actively pump out fluid from the stroma. A healthy
erythema which includes the upper eyelid.The rash does not cross
tear film (with all its constituent layers) and eyelids are vital to
the forehead midline. There is associated headache, malaise and
maintain corneal integrity and clarity.
fever. There is follicular conjunctivitis with variable involvement
Disturbance of the eyelids, conjunctiva or tear film may lead to
of the cornea —multiple epithelial pseudodendrites and anterior
corneal problems including ulceration. If the disease is severe,
stromal infiltration —responsive to topical corticosteroids. In-
corneal scarring with vascularization may lead to reduced vision
creased risk in immunocompromised patients, e.g. HIV.Treatment
and in rare cases to corneal perforation requiring surgical
is with systemic antivirals.
management. Corneal anaesthesia (Vth nerve palsy) predisposes
Inflammation
to severe keratitis.
Peripheral necrotizing keratitis
Corneal disease
This is related to an underlying systemic vasculitis, e.g. rheumatoid
Keratitis
arthritis, systemic lupus erythematosis or Wegener’s granulomato-
General term used to denote inflammation of the cornea from in-
sis. Peripheral destruction of corneal tissue is secondary to an is-
fection and inflammation.
chaemic microvasculitis in the adjacent scleral and conjunctival
Symptoms
vessels or it is mediated immunologically by blood-borne factors
or matrix metalloproteinases secreted into the tears. This patho-
Pain and photosensitivity (maybe absent in herpetic disease due
to corneal hypaesthesia), reduced visual acuity and/or discharge.
logical process is exacerbated by secondary Sjögren’s syndrome.
Treat the underlying disease process with systemic immunosup-
Signs
pression.Treat corneal perforation conservatively with tissue glue,
Reduced Snellen visual acuity and circumcorneal injection —a
bandage contact lenses or corneal grafting.
red, inflamed eye, presence of staining on fluorescein drop instilla-
tion, visible corneal infiltrate with or without anterior chamber
Corneal dystrophies
These are hereditary and occur at any level in the cornea —epithe-
hypopyon and blepharospasm.
lial, stromal and endothelial. With severe corneal dystrophies,
Infections
corneal grafting may be required to restore vision, although dys-
Bacterial keratitis
trophic changes often recur in the grafts.
Secondary to minor trauma (corneal abrasion or contact lens
Fingerprint and map-dot corneal epithelial dystrophies cause
wear). Treat as an emergency.
acute painful recurrent corneal erosions, particularly on waking.
A variety of bacteria may be responsible. Pseudomonas is com-
The most common corneal dystrophy, which is potentially sight
mon in contact lens-related keratitis and is rapidly destructive.
threatening, is keratoconus —associated with Down’s syndrome,
There is rapid corneal opacification and melt over less than 24 h.
disorders of collagen metabolism, atopic eye disease or idiopathic.
Rapidly identify the infective agent by C&S intensive topical
Keratoconic patients require special fit contact lenses and, if
antibiotics. Severe infections can lead to corneal perforation, en-
needed, corneal grafting. (See Chapters 31 and 32)
dophthalmitis and loss of vision.
Other dystrophies include lattice dystrophy, with deposition of
Acanthamoeba keratitis
amyloid in the corneal stroma, and inherited disorders of corneal
Acanthamoeba causes prolonged corneal infection. It is associated
metabolism (e.g. granular and macular dystrophy).
with poor contact lens hygiene —especially tap water in lens clean-
Fuchs’ endothelial dystrophy results in corneal clouding be-
ing —and with daily wear soft contact lenses. Characterized by se-
cause of endothelial pump failure. It causes a painful bullous
vere pain.
keratopathy, which is treated with a bandage contact lens and
Diagnosis may require corneal biopsy and histological assess-
eventual penetrating keratoplasty.
ment. Look for a corneal Wessely ring using the slit lamp.
Corneal neoplasia
Chronic infection with acanthamoeba cysts deep in the corneal
Although rare, conjunctival-corneal intraepithelial neoplasia
stroma may cause scarring requiring corneal graft.
(CCIN) and squamous carcinoma are important conditions. They
Viral keratitis
are more common in fairer-skinned individuals in hotter climes
1 Herpes simplex types 1 and 2
and immunocompromised patients with HIV. Needs to be treated
Epithelial disease — dendritic ulceration.
with excision or local destructive procedures.
Stromal disease — disciform keratitis
KEY POINTS
• immune mediated, presenting as a disc-shaped area of
corneal oedema, hence the term disciform;
• The healthy cornea is avascular and transparent due to endothelial pump.
• Topical steroids may worsen dendritic keratitis and should never be used.
• stromal necrosis may result in scarring with vascularization
reducing corneal sensation, clarity and vision.
• Bacterial keratitis in a contact lens wearer is an emergency.
Common conditions affecting the cornea 67
31 Therapeutic contact lenses
Soft contact lenses are very fragile. Bandage soft contact lenses are used in small perforation and bullous keratopathy
Epithelial
Endothelial cell
Bullous
bullae are
'pump' failure
keratopathy
painful
Thickened
oedematous
stroma
Tight lens syndrome
Contact lens too
tight at limbus
Epithelial oedema
- lack of oxygen
Oedematous
red limbus
Cosmetic contact lens
Hand-painted contact lens
- may have painted black pupil
Hypopyon ulcer
if corneal scar or a clear
window left if iris
abnormality
Unsightly
corneal
scar or iris
abnormality
Aims
Therapeutic bandage contact lenses
1 Medical indications for contact lenses (CL).
These are soft contact lenses with several functions.
2 Complications of contact lens wear.
Protection of normal epithelium
Contact lenses are an excellent alternative to glasses.They are also
• Trichiasis —to prevent lashes from rubbing the cornea.
widely used therapeutically in corneal disease. They are fitted for
• Lid margin deformation, e.g. lower lid entropion with lashes
each patient based on the steepness and diameter of the cornea.
touching the cornea, as temporary relief until surgery can be
The types of lenses (hard, gas permeable hard, etc.) and materials
performed.
used are summarized in Chapter 9.
• Protection of corneal graft epithelium.
• Dry eye, e.g. pemphigoid and Stevens-Johnson syndrome.
Keratoconus
• Exposure keratitis —following seventh nerve palsy.
In keratoconus, (GPH) CL are used. Some soft CL are suitable too
• To protect the cornea if there are sutures on the lid margin or
in the early stages. Once the corneal curvature is very ‘steep’ either
under the eyelid, abrading the cornea. Use until sutures dissolve or
GPH lenses are used or eventual corneal graft (see Chapter 32).
can be removed.
68 Sub-specialty —External eye disease
Healing abnormal epithelium
• Three and 9 o’clock staining (drying of corneal surface, abnor-
• Corneal epithelial dystrophy, e.g. Cogan’s microcystic epithelial
mal blink).
dystrophy, Meesman’s dystrophy, Reis-Buckler’s dystrophy and
• Inferior corneal stain (incomplete blinking).
map-dot or fingerpoint dystrophy.
• Dimple veil (static air bubble under lens).
• Chronic corneal ulcers —due to herpes simplex or vernal
• Overwearing syndrome (mechanical and metabolic factors).
keratoconjunctivitis.
• Abrasions and erosions.
Biological activity
• Filamentary keratitis —also rapid relief of the discomfort
The presence of a CL acting as a biological active surface can
caused by the corneal filaments.
cause several syndromes:
• Chemical, thermal and irradiation burns —high water content
• Toxic keratopathy (proteolytic enzyme —the chemical preser-
lenses may be useful to restore normal epithelialization.
vative in the cleaning solutions).
• Thiomersal keratopathy (the preservative in CL solutions
Moulding and splinting
or instilled eye drops acts as a hapten causing a delayed
• Post keratoplasty (corneal grafting) —to flatten and reposition
hypersensitivity response).
the graft when lifting or displacement of graft occurs.
• Giant papillary conjunctivitis
(multifactorial aetiology —
• Wound leaks —small corneal perforations need tight fitting;
immune response to antigenic proteins on lenses and mechanical
post-trabeculectomy bleb leaks need large lenses to cover the
effects of lens edge) causes red sticky eye.
leak.
• Sterile corneal infiltrate —inflammatory response in absence of
infecting organism, hypersensitivity to disinfectants and bacterial
Pain relief
products as well as lens fit are aetiological factors.
• Bullous keratopathy —CL help to alleviate pain by covering ex-
posed nerve endings.
Microbial keratitis
• Postrefractive surgery —PRK and LASEK for pain relief and
This is caused by a complex interaction of various factors and in-
wound healing. See Chapter 32.
creased ocular susceptibility and exposure to pathogens, associ-
ated with Pseudomonas, Staphylococcus and Acanthamoeba
Complications of contact lenses
(ubiquitous free-living protozon).
Corneal physiology
The constant metabolic activity in the cornea maintains trans-
Guidelines for managing microbial conjunctivitis
parency, temperature, cell reproduction and the transport of tissue
Emergencies are a routine occurrence in CL practice.
materials. The main nutrients are glucose, amino acids (from the
aqueous humour) and oxygen (from the tear film by diffusion
WARNING
when the eye is open and from the tarsal conjunctiva when the
In a contact lens wearer corneal and conjunctival complications are due to
eyelids are closed). Without oxygen there is hypoxia or anoxia.
contact lens wear until proved otherwise.
Hypoxia and anoxia
There are virtually no lenses available that fully meet the oxygen
requirements of the cornea, and there is no CL as physiological or
• Leave the lens out —Inflammatory symptoms of lens-related dis-
oxygen permeable as having no CL on the eye!
ease respond within a few days of ceasing lens wear.
One of the first important effects of hypoxia (which the patient
• Exclude microbial keratitis.
is unaware of) is a drop in corneal sensitivity. Anoxia causes
• Do not treat a red eye with steroids when there is a corneal ulcer.
corneal swelling, especially of the epithelium. If there is not
enough oxygen available to convert glucose, by the means of gly-
Advice for patients
colysis, into energy, the waste product (lactic acid) is allowed to
Maintain a high standard of CL hygiene. Lenses should be cleaned
diffuse and build up in the stroma. Sufficient osmotic pressure is
and disinfected each time they are removed. Avoid overnight
created to allow water to be drawn into the stroma faster than the
wear! Have back up spectacles! Leave lenses out when adverse
endothelial pump can remove it, so eventually corneal epithelial
symptoms or a red eye develops.
and stromal swelling occurs.
Lack of oxygen results in:
Feel good —look good —see good, if these critieria are not met the patient
• Acute epithelial necrosis.
should seek help.
• Microcystic epitheliopathy.
• Epithelial and stromal oedema.
• Corneal neovascularization.
KEY POINTS
• Use bandage CL for corneal protection, to aid healing, splinting and pain
Anatomical effects
relief.
Anatomical effects result in:
• Anoxia causes corneal swelling, cloudiness and pain.
• Tight lens syndrome.
• Beware bacterial contact lens complications!
• Corneal abrasions (foreign bodies).
Therapeutic contact lenses 69
32 Corneal and laser photorefractive surgery
Normal anatomy corneal limbus
Pterygium
Keratoconus
Cornea
Keratoconic
Iris
cornea
Invasive
Corneoscleral
pterygium
junction
Central core
Thinned
Conjunctiva
Fibro-
corneal
vascular
Stromal
Lens
apex
growth
Kaiser-Fleischer
(K-F) ring seen on
slit lamp
Pterygium surgery
Graft
site
Keratoglobus
Wide ectasia
- entire
ectasia
Kaiser-Fleischer
very thin
ring
Pterygium
Conjunctival
dissected off cornea
autograft
and sclera
Corneal topography scan showing shape of a keratoconic cornea
Corneal surgery - penetrating keratoplasty (CPK)
Approximately 7mm diameter
diseased cornea trephined out
Discard
Full-thickness corneal graft
sutured in
Diseased host
cornea
Clear donor cornea
Refractive laser surgery techniques: excimer laser uses
LASIK = LASer in situ keratomileusis
1 Cut a superficial flap with the microkeratome
Myopia
Effect of refractive surgery
2 Laser treatment to remodel the cornea
3 Replace the hinged flap
4 Place a postoperative contact lens on cornea
Photorefractive
LASIK
keratectomy (PRK)
Light focused
Flattens central cornea - light
anterior to retina
is focused further posteriorly
Hypermetropia
Laser applied
Laser applied
after epithelial
after partial
debridement
thickness flap
elevated
Flattens peripheral
Flattened anterior corneal
cornea - light is
DANGER
curvature in myopia
focused further
Laser
hazard
anteriorly
70 Sub-specialty —External eye disease
Aims
Wavefront technology enables precision planning for each individual.
1 Management of keratoconus.
2 Principles of corneal surgery.
Photorefractive keratectomy (PRK)
3 Know about current laser techniques.
Excimer laser ablation reshapes the anterior corneal surface after
manual debridement of the epithelium. >10 years’ track record.
Cornea
• Suitable for low refractive errors (-1 to -6D).
The healthy cornea is clear, tough and free of blood vessels or
• Disappointing for hypermetropia.
opacification and acts as an important refractive surface. Corneal
• Bandage contact lenses as eye painful for 48 h.
clarity is dependent on the integrity and normal functioning of all
• Variable slow healing and remodelling over months .
of its 5 cellular layers (see Chapter 30). Of particular importance is
• Quality of vision —temporary haze common after treatment.
the corneal endothelium, a single cell layer of non-mitotic cells
• Regression can occur in higher degrees of myopia (>-10D).
that maintains the cornea in a state of partial ‘dehydration’ and
• Recurrent erosions are a complication.
hence transparency through the use of cellular metabolic ‘pumps’.
When that pump fails, the stroma swells and becomes hazy, e.g.
Laser-assisted in intrastromal in situ keratomileusis (LASIK)
bullous keratopathy (see Chapter 31) requiring bandage CL or
A partial thickness corneal hinged epithelial ‘cap’ is raised and the
full thickness corneal graft (penetrating keratoplasty, PK).
excimer laser ablation is applied to stromal tissue below this, after
Keratitis causing corneal scarring can require PK. In order for
which the ‘cap’ is replaced. <10 years’ track record.
the graft to take, the host cornea should not have many blood ves-
• Suitable for higher degrees of myopia with less risk of regres-
sels, which could contribute to corneal graft rejection, and should
sion (up to -10D).
have near or near normal sensation. A partial thickness corneal
• Disappointing for hypermetropia.
graft is a lamellar keratoplasty.
• No haze.
• Best visual acuity achieved more rapidly than PRK.
Corneal diseases
• Dry eye for a few months.
Keratoconus
This common corneal dystrophy is a chronic progressive disease
Laser epithelium keratomileusis (LASEK)
characterized by thinning, cone formation and irregular myopic
This is large optical zone corneal surface excimer laser ablation.
astigmatism (see Chapter 30). The criteria for diagnosis are steep
The epithelium is treated with 15% alcohol for 20 s and is pre-
keratometric readings with irregular light reflexes on the corneal
served or delaminated with a microkeratome and is later replaced.
surface seen with the keratoscope and corneal topography.
This is the newest technique with a short track record, 5 yrs.
Early management is with SPH CL, and late management with
• A bandage contact lens is worn for 3-4 days whilst the epitheli-
PK.
um heals.
• There is speedy healing because the epithelium is retained.
Pterygium
• Mild pain only.
Microscopic lamella excision is needed if it encroaches on the vi-
• Good for astigmatism.
sual axis (See Chapter 14.)
• Excellent for myopia
6D, good for myopia -6 to
10D, all-
right for myopia -10 to -12D and for hypermetropia up to +4D.
Corneal neoplasia (See Chapter 30)
• Studies have limited follow-up data, often <2 years.
Corneal surgery
• Less haze risk than in PRK.
Corneal grafting
Who can have laser refractive surgery?
From human donor material. Donor eyes are stored in eye banks
• Patients should be >21 years, have a stable refraction, not
e.g. in London, Bristol, Manchester and Dublin. Donors are
pregnant and have no keratoconus, cataract or glaucoma.
screened for many contagious diseases including HIV.
• They should not be on systemic steroids.
Indications
• Patients should have realistic expectations and have been
• Visual rehabilitation following scarring, dystrophic changes or
warned of potential side effects of haze, night time glare, ghost-
endothelial dysfunction resulting in loss of corneal clarity.
ing images, starburst around lights, dry eye and risk of macular
• Restoration of structural integrity following perforation.
haemorrhage.
• Alleviation of pain in intractable corneal disease without visual
• It is also essential that patients are warned that intraocular pres-
potential, e.g. bullous keratopathy.
sure and A-scan/biometry measurements cannot be made accu-
rately after refractive surgery.
Refractive surgery
Surgery and/or laser is used to reshape the main refractive surface
WARNING
of the eye, (anterior corneal surface), and to bring light rays in
1 Corneal refractive surgery can have serious, potentially sight-threatening
focus on the retina without the need for glasses or contact lenses.
complications as with any ocular surgery.
The main indication is myopia.
2 Lasered donor eyes are not accepted for corneal grafting.
There are three methods of laser, in all of which the excimer
3 Refractive surgery effects may regress with time.
laser is used to correct myopia, hypermetropia and astigmatism
under local anaesthesia.
KEY POINTS
In myopia the corneal surface is flattened so that the image fo-
• A healthy corneal endothelium is essential for corneal clarity.
cuses onto the retina. The effect in hypermetropia is not always
• Corneal grafting is successful particularly in keratoconus patients.
stable.
• The main indication for laser refractive surgery is myopia.
Corneal and laser photorefractive surgery 71
33 Cataract assessment
Anatomy
Definition
The lens is crystalline with an inner nucleus of older inactive cells and an outer cortex, the whole
Cataract: Opacity of the lens of the eye,
being encapsulated. The epithelium is active metabolically, it synthesizes protein for lens fibres,
which occurs when fluid gathers between the
transports amino acids and maintains a cation pump to keep the lens clear. At the equator of
lens fibres. The refractive index alters and
the lens, epithelial cells differentiate into lens fibres, which lose their organelles and ability for
causes light scatter with resultant blurred
aerobic metabolism
vision. Acquired lens changes occur in 95%
Zonule filaments suspend the lens ciliary processes to the ciliary muscle. When the muscle
of people over 65, however, not all these
contracts the filaments relax allowing the lens to become more convex with a shorter focal length
people will require cataract surgery
for reading
Diagram of normal anterior segment
Close up of normal lens cross-section
Lens with cataract
Anterior
Posterior
Anterior
Posterior
Equator
Capsule
Cortical
Cortex
Anterior
Anterior
Anterior
epithelium
subcapsular
Embryonic
segment
Vitreous
Nuclear
nucleus
Lens fibres
(nucleosclerosis)
humour
Lens
New lens fibre
Cornea
Zonule
production
Posterior
Ciliary
subcapsular
Corneo-
Equator
process
Posterior
scleral limbus
Zonules
capsule
Sclera
Causes of cataract
• Old age (commonest)
Slit lamp view of nucleosclerosis
• Associated with other ocular and systemic diseases (diabetes,
uveitis, previous ocular surgery)
• Associated with systemic medication (steroids, phenothiazines)
• Trauma and intraocular foreign bodies
• Ionizing radiation (X-ray, UV)
• Congenital (dominant, sporadic or part of a syndrome, abnormal
galactose metabolism, hypoglycaemia)
• Associated with inherited abnormality (myotonic dystrophy,
Marfan's syndrome, Lowe's syndrome, rubella, high myopia)
Biometry: intraocular lens power calculation
The desired implant should produce a sharp image
on the retina. Since each eye has a different corneal
Natural lens
curvature and axial length, the implant size has to
15D
be measured preoperatively in each patient. The
Cornea
optics of the eye are such that light is refracted by
43D
the cornea (effective power of 43D) and by the
natural lens (effective power 15D), both of these
together give the total power of the focusing
components of the eye. A special equation is used
to calculate the intraocular lens power, which is
usually in the range of 19-22D, with some very
Optics of cornea
short-sighted eyes needing lower powers and long-
and lens refract light
sighted eyes needing higher powers for clear
focused distance vision
72 Sub-specialty —Corneal, refractive and cataract surgery
Aims
TIP
1 Anatomy of the lens.
Pupils are normal if there is no other ocular or optic nerve disease.
2 Causes of cataract.
3 Symptoms and signs.
4 Treatment of cataract.
Treatment
• Cataract alters the refractive power of the natural lens so a
change in glasses prescription may allow good vision to be main-
tained. The eye may become more myopic (lenticular-induced
myopia) or hyperopic. The legal requirement for driving a car in
Cataract is the most common cause of blindness in adults worldwide.
the UK is 6/10 in one eye. NB, the Snellen chart only has lines
corresponding to 6/9 and 6/12.
• If further changes occur in the lens, with increased disturbance
of the lens fibres, the visual acuity cannot be improved with
Symptoms
glasses and surgical removal of the cataractous lens is required.
• Reduced visual acuity (near and distant objects).
• Modern surgery involves removal of the lens fibres, which form
• Glare in sunshine or with street or car lights.
the nucleus and cortex of the cataract, leaving the posterior
• Distortion of lines.
epithelial capsule to hold the new artificial lens and keep the
• Monocular diplopia.
vitreous humour away from the anterior chamber.
• Altered colours (white objects appear yellowish).
• Not associated with pain, discharge or redness of the eye.
Preparation for cataract surgery
• Biometry: ultrasound measurement of the length of the eye and
Signs
keratometry to measure the curvature of the cornea and hence
• Reduced acuity measured on a Snellen chart or LogMar and
calculate the power of the implant to be inserted in the eye during
near vision chart.
surgery.
• An abnormally dim red reflex is seen when the retina is viewed
• Confirm that general health problems are stable, particularly
with an ophthalmoscope at arms length. Nuclear cataract causes a
hypertension, respiratory disease and diabetes.
central black shadow across the red reflex and cortical cataracts
• Some medication increases the incidence of haemorrhage.War-
cause black spoke-like shadows coming from the edge of the red
farin does not need to be stopped but the INR should be less than
reflex.
3. Aspirin may be stopped 1 week before surgery.
• Reduced contrast sensitivity can be measured by the
• Inform patients of expected outcome and the complications of
ophthalmologist.
surgery (informed consent).
• Only very dense cataracts causing severely impaired vision
cause a white pupil.
KEY POINTS
• After pupils have been dilated, slit lamp examination shows
• Cataract is common, it is one of the three main causes of blindness world-
whether the cataract is cortical, nuclear or posterior subcapsular
wide.
and allows fundus examination.
• Can occur at any age and in all races.
• Cataract in children is unusual but may be associated with a
• Effectively treated by glasses in the early stages and by surgery when more
white pupil, inability to fix on a target (e.g. a light) and the devel-
advanced.
opment of a squint.
Cataract assessment 73
34 Cataract surgery
An operating microscope is needed. In order to reach the lens, a small corneal
Model of eye showing anterior chamber depth
incision is made close to the limbus for the phaco-probe. It is important to
Epithelium
appreciate ANTERIOR CHAMBER DEPTH and to keep all instruments away
from the corneal endothelium, in the plane of the iris
Endothelium
Anterior
chamber
depth
Corneoscleral
limbus
Phacoemulsification surgery
Phaco-probe
3. Foldable intraocular lens (IOL)
2.75 mm incision in cornea
Corneal incision
1. Keratome corneal incision
being inserted
Limbus
profile - self-sealing
sutureless wound
Paracentesis incision
Phaco-probe in lens
Capsulorhexis
Dilated pupil
Intraocular lens
Capsulorhexis edge
Intraocular lens
placed in bag
Anterior capsule
Iris
Ciliary body
Zonule
Posterior capsule
Anterior capsule
Capsulorhexis
edge
Intraocular in capsular
2. Phaco-probe sculpting lens
4. IOL unfolded in capsular bag
bag
nucleus
Steps:
New techniques
• Corneal incision 2.75-3.2 mm
Clear lens surgery - a novel lens refractive technique
• Viscoelastic to anterior chamber
• Capsulorhexis
Phacoemulsification is used for cataract surgery and also for CLEAR
• Hydrodissection
LENS surgery. Clear lens surgery is called lens refractive surgery and is
• Phaco removal of nucleus
increasingly being offered for presbyopia and high myopia. Technology for
• Aspiration of cortex
lens surgery is accelerating at a phenomenal speed
• More viscoelastic:
• A folded IOL is inserted under a cushion of viscoelastic fluid,
1. Clear lens IOL - the patient's lens is removed and an IOL of a different
which protects the corneal endothelium; the lens unfolds
power inserted. E.g. Prelex lens exchange - this is a special IOL which
spontaneously within the capsular bag
tilts with accommodation maintaining clear 'unaided' distance and near
• Viscoelastic removed and replaced with balanced salt solution
vision! Myopic patients having LASER corneal refractive surgery now
• Self-sealing wound
may opt for this when prebyopic!
• Subconjunctival injection of steroid and antibiotic
• Eyepad and protective eye shield
2. Phakic IOL - the patient’s clear lens is left in situ and a second lens
placed in front of it - used for myopia correction
Both these techniques have potential complications and the patient
needs to be fully informed before going ahead
74 Sub-specialty —Corneal, refractive and cataract surgery
Aims
the lashes. The drape is light and also covers the face —lifted up
1 Understand methods of anaesthesia and cataract removal.
from it as a small tent —to protect the face from irrigation fluids
2 Be able to explain cataract surgery to a patient.
used in the surgery, which are collected into a small bag at the side
of the head.
Microsurgical cataract surgery in developed countries has reached
a very high level due to the developments in microsurgical instru-
Small speculum
ments and intraocular lens design. There is controlled and precise
The eyelids are kept open by a combination of the drape and a
removal of part of the lens with the assistance of an operating
small wire speculum which does not cause the patient discomfort.
microscope. Part of the lens capsule is retained to hold the implant
within it.
TIP
Phacoemulsification lens surgery with small, foldable intraocular lens im-
Definitions
plants is the gold standard. It gives rapid visual rehabilitation with a low com-
Pseudophakia: An eye that has had a cataract removed and artifi-
plication rate.
cial intraocular lens implanted.
Aphakia: An eye that has had a cataract removed without an arti-
ficial lens inserted.
Surgery
Extracapsular cataract surgery is a technique in which the posteri-
Anaesthesia for cataract surgery
or capsule of the lens is retained, keeping the vitreous separate
from the anterior chamber of the eye. It may be small or large in-
cision surgery.
TIP
• Small incision surgery is by using phacoemulsification (phaco)
Most adult cataract surgery is done under topical or local anaesthesia. The pa-
to crumble the lens in the eye. Fragments are irrigated out auto-
tient may see bright lights and different colours, shadows of the surgeon’s
matically. A soft, foldable intraocular lens implant (IOL) can be
hands moving or complete darkness during surgery.
inserted through the small incision into the lens capsule (posterior
chamber IOL).This incision is usually sutureless, or a single suture
Local anaesthesia
is placed, which can be removed as early as 2 weeks after surgery.
• Topical (drops of proxymethocaine or amethocaine).
Phaco is the most commonly used technique.
• Subtenons using a blunt canula to administer 2 ml of lidocaine.
• Large incision surgery involves removal of the entire nucleus as
• Peribulbar injection to distribute 5-10 ml lidocaine within the
one piece; the soft cortex is aspirated and a rigid or soft implant is
orbit.
inserted. The corneal wound requires microsutures, which are
• Retrobulbar injection to direct 1-2 ml lidocaine within the mus-
removed as late as 8 weeks after surgery.
cle cone —now becoming less commonly used.
Implant power
Sedation
The IOL power is carefully calculated to take into account the pa-
Intravenous drugs may be given with local anaesthetics but are not
tients postoperative visual requirements. For instance, a myopic
preferred as the patient could drift off to sleep and then suddenly
person may prefer to remain slightly myopic after surgery so that
wake up with a jolt and move their head —undesirable in cataract
they can still read without glasses. Multifocal IOLs and accom-
surgery.
modative IOLs are increasingly being used.
General anaesthesia
Clear lens surgery for presbyopia
This is used for young and uncooperative patients.
Over the next few years an increasing number of people in their
fifties will have their lenses removed for presbyopia, in order to
Surgical technique for cataract removal
avoid having to wear reading glasses, and special accommodative
Patients have to lie supine so a microscope with a bright light and
IOLs will be inserted. Hence the number of people developing
good magnification can be positioned above them. The surgeon
cataract will be reduced.
works from the side or above the head, looking down the micro-
scope, using the red reflex from the retina to aid cataract removal.
KEY POINTS
• Microsurgery involving the replacment of the natural lens with an artificial
Draping
one.
Before surgery can start, the eyelids and lashes are covered with a
• Day-case procedure under local anaesthesia.
thin transparent plastic drape in order to keep contaminated
• Patient needs to be able to lie still and flat for 30 min.
lashes out of the surgical field. Staphylococci live in abundance on
Cataract surgery 75
35 Cataract surgery postoperative care
Early postoperative
Symptom
Sign
Treatment
problems
Raised intraocular
Pain, deep ache,
Hazy cornea
Ophthalmologist needs to measure pressure and
pressure
blurred vision
treat with systemic acetazolamide 250 mg
2-4 times daily (1-2 days) and glaucoma drops
Leaking incision
Poor vision
Siedel positive
Ophthalmologist may need to suture the wound in
with fluorescein
the operating theatre. If the anterior chamber is
deep and the ocular pressure is normal, a soft
contact lens may be placed on the eye. Daily review
is required
Subconjunctival
Red eye. No pain
Diffuse redness on
Continue drops. Reinforce good technique for
Leaking wound - a positive
haemorrhage
the globe
instilling drops
Siedel test (trabeculectomy
bleb leak)
Corneal oedema
Poor vision
Hazy cornea
Ophthalmologist needs to exclude raised pressure
and increase topical steroid drops
Epithelial erosion
Gritty, watering
Fluorescein staining,
Continue drops, reassure. Monitor carefully to
(conjunctiva or
may have injected
exclude early infection
cornea)
bulbar conjunctiva
Conjunctivitis
Pain, redness with
Swollen, red tarsal
Prescribe different antibiotic, (e.g. ofloxacin) to be
mucopurulent
conjunctiva while
used 2 hourly. Frequent review to confirm no
discharge
maintaining good
progression to endophthalmitis
vision
Sight-threatening
Symptom
Signs
Slit lamp signs
Treatment (by ophthalmologist)
postop problems
observed
observed by
requiring urgent
with pen
ophthalmologist
Hypopyon indicates
treatment by
torch
endophthalmitis
ophthalmologist
Endophthalmitis
Painful, red eye
Red eye with hazy
Flare, cells and
URGENT in-patient management.
usually with a
cornea. A relative
and hypopyon in
Intensive topical broad spectrum
mucopurulent
afferent pupillary
anterior
antibiotics (drops). Requires
discharge and
defect indicates
chamber
aqueous and vitreous sample for
poor vision at
serious visual
microscopy, culture and
day 3-5
damage
sensitivity
Fibrin plaque - intense
Macular oedema
Poor vision
Normal anterior
Slit lamp fundus
Treated with anti-inflammatory drops
(retina)
during first
segment of the
examination and
(steroid and non-steroidal), steroid
postoperative inflammation
in endophthalitis
60 days after
eye
fluorescein angio-
injection around the eye, systemic non-
surgery
graphy show
steroidal anti-inflammatory, e.g.
increased fluid in
neurofen
the retina around
the fovea
Opacity of posterior
Gradual
White eye with no
Posterior capsule
Make a hole in the capsule using a YAG
part of the original
deterioration
external
hazy or white.
laser (clinic procedure requiring
epithelial capsule of
of vision, as
abnormality. Red
Implant is
anaesthetic drops). Cornea, anterior
the natural lens
though
reflex from fundus
unaffected
chamber and implant are not affected
(can occur between
cataract is
may be obscured
by the laser
1 month and 2 years
reforming
after surgery)
Definitions:
Endophthalmitis = infection and inflammation involving the whole of the
Cystoid macular oedema (CMO)
contents of the eyeball
- typical colour fundus and
IOP = Intraocular pressure
fluorescein angiographic
YAG laser capsulotomy = laser treatment for posterior capsular opacity
appearance
Siedel test = fluorescein test to look for wound leakage of aqueous humour
YAG capsulotomy hole made
in thickened posterior capsule
from the eye
76 Sub-specialty —Corneal, refractive and cataract surgery
Aims
Undesirable postoperative events (complications)
1 Awareness of normal and undesirable early and late postopera-
Watering and a foreign body sensation are common after surgery.
tive events.
Usually the patient can be reassured, but the possibility of infec-
2 Recognize postop complications from history.
tion —endophthalmitis —the most important sight-threatening
3 Use of pen torch and fluorescein drops to detect a leaking
complication, must be considered. This is an acute sight-threaten-
wound and see hypopyon.
ing postoperative event that requires urgent admission and treat-
ment. Its onset is usually 4-5 days after surgery. Symptoms include
Routine postoperative management
worsening vision and pain.
Patients use steroid and antibiotic drops four times daily for 2-4
See Tables for early and late complications.
weeks after surgery. During that time they can read, take gentle
exercise, shop, shower or bath and wash their hair carefully. The
implant inserted at surgery normally gives them clear vision for
KEY POINTS
distance (e.g. TV, buses) but they will need to wear reading glasses
• Over 97% of cataract surgery is successful.
(approximate prescription +2.5D); these can be prescribed from
• Endophthalmitis is the most serious postoperative complication.
2-4 weeks after phacocataract surgery. Some patients have a
• Sympathetic ophthalmia affects the other eye —rare <0.01%.
multifocal implant inserted so they are less dependent on glasses
for reading.
Reading glasses
Patients who have had phacocataract surgery usually have good vision from
the first postoperative day and can be tested for spectacles (refraction) for
reading 2 weeks after surgery.
In contrast, patients who have had large excision extracapsular cataract
surgery have corneal sutures, which are not removed for 2-3 months. Only
after these have been removed are reading spectacles prescribed, i.e. there is
a longer rehabilitation period.
Cataract surgery postoperative care 77
36 Glaucoma—the basics
Anatomy: aqueous production, drainage and resistance to flow
Intraocular pressure (IOP) is due to the production of aqueous humour
by the ciliary body. Aqueous flows forward over the anterior surface of
Cornea
the lens, through the pupil and drains through the trabecular
meshwork into Schlemm’s canal. The alternative uveoscleral pathway
drains 10% of aqueous
Iris
4
3
5
Ciliary
Sites of blockage:
2
1 Ciliary block
body
2 Pupil block
Lens
1
3 Pre-trabecular - neovascular membrane or cellular debris
4 Trabecular
5 Post-trabecular - elevated episcleral venous pressure
Anatomy: Normal and cupped optic nerve heads in chronic primary open angle glaucoma
Disc
Cup
(a) Normal disc
(b) Glaucoma:
(c) Glaucoma:
focal notch
diffuse cup
Cup disc ratio
enlargement
approx 0.3
Cup disc ratio
approx 0.8
IOP and glaucoma risk
Normal population
Acute angle-closure glaucoma
distribution of IOP
Glaucoma risk
Glaucoma
risk
NTG
NTG = Normal tension
15.5
21.0
30.0
glaucoma
IOP (mmHg)
Aims
Classification
1 Understand the group of conditions classed as glaucoma.
The glaucomas are a diverse group of eye conditions (at least 60
2 Know the symptoms and signs of acute angle-closure glaucoma
types), which can be divided into diagnostic groups in the follow-
to enable urgent referral for treatment of this ophthalmic
ing way:
emergency.
1 Defined by absence or presence of causative factors: primary or
secondary.
Definitions
2 Defined by the anatomy of the drainage angle: open angle or
Glaucoma: A multifactorial optic neuropathy with characteristic
angle closure.
acquired loss of optic nerve fibres. Commonest cause of irre-
3 Defined by speed of onset: acute or chronic.
versible blindness in the world, affecting 2% of people over 40
4 Defined by age of onset: congenital, juvenile or adult.
years of age, and 4% of people over 70 years.
5 Defined by level of IOP: normal tension glaucoma (characteris-
Intraocular pressure (IOP): The ‘normal’ range of IOP varies be-
tic glaucomatous optic neuropathy with IOP in the normal range)
tween 10 and 21 mmHg but there is no absolute limit. Elevated
or ocular hypertension (IOP above the normal range but no glau-
IOP is a major risk factor for the development of glaucoma.
comatous optic neuropathy).
Skills to obtain
Chronic primary open-angle glaucoma (POAG)
Use of direct ophthalmoscope to evaluate optic disc colour and
This is by far the commonest form of glaucoma in Caucasian and
cup : disc ratio.
Afro-Caribbean populations.The exact mechanism of pathogene-
78 Sub-specialty —Glaucoma
sis is unknown, but various factors are implicated including
Treatment
elevated IOP and altered vascular supply to the optic nerve.
Urgent treatment needed to prevent permanent loss of vision.
Genetics also plays a role, with nine loci in the human genome
• Treat medically (topical and systemic) to bring down IOP and
known to be associated with glaucoma. Risk factors include ele-
break attack.
vated IOP, family history and Afro-Caribbean descent.
• Prevent further attacks with YAG laser iridotomy or surgical
peripheral iridectomy (in both eyes).
Symptoms
• The second eye is treated prophylactically to prevent later
Usually asymptomatic until disease is advanced with advanced
AACG (see Chapter 38).
optic disc cupping, when peripheral field defect may be noticed
and central vision lost. ‘Tunnel’ vision is not noticed early on.
Secondary glaucoma
Multiple causes including uveitis, rubeofis and trauma.
Signs
• Usually raised IOP >21 and <40 mmHg.
Treatment
• Normal open angle on gonioscopy.
Treat the cause and control IOP.
• Characteristic optic disc changes with gradual thinning of the
neurosensory rim superiorly and inferiorly with time, nerve fibre
Chronic angle-closure glaucoma
layer defect, optic disc rim notching and cupping, cup : disc ratio
Younger age group with intermittent angle-closure symptoms.
enlarged and/or asymmetrical.
• Visual field changes on automated fields analysis with charac-
Treatment
teristic arcuate scotoma.
Laser peripheral iridotomy.
Treatment
Congenital glaucoma / infantile glaucoma / buphthalmos
• Medical with daily or twice daily topical drops, laser and surgi-
Occurs in infancy, and can be unilateral or bilateral. Primary or
cal options (see Chapter 38 for details).
associated with ocular malformation or systemic syndrome, e.g.
• Most patients are maintained on regular topical medication
Sturge-Weber. Can go blind if not detected and treated.
with monitoring of disc appearance and visual field analysis.
Symptoms
Acute angle-closure glaucoma (AACG)
Watering photophobic eyes.
Commoner in older, hypermetropic people. Commonest glau-
coma in Chinese people.
Signs
• Large eyes (myopic) —buphthalmos.
Symptoms
• Diameter of corneas wider than normal.
• Sudden onset of severly painful red eye.
• Reduced vision.
• Blurred vision.
• Clouding of corneas.
• Halos around lights.
• Linear tears in Descemet’s membrane.
• Headache.
• Raised IOP.
• ±Nausea and vomiting.
• ± Red eyes.
Treatment
WARNING
• Specialist medical management by paediatric ophthalmologist.
Patients with AACG can go blind if the glaucoma is unrecognized and
• Then various surgeries, goniotomy, trabeculotomy or tra-
untreated.
beculectomy.
• Goniotomy is the first choice and may have to be repeated.
Signs
• Reduced visual acuity.
KEY POINTS
• Brick red eye.
• Normal range of intraocular pressure is 10-21 mmHg.
• Hazy cornea (corneal oedema).
• Primary open-angle glaucoma is the commonest form.
• Vertically mid-dilated fixed pupil.
• Acute angle-closure glaucoma occurs in older persons and is usually
• Very high IOP, that can be felt digitally.
painful.
• Closed iridocorneal angle on gonioscopy.
Glaucoma—the basics 79
37 Detecting glaucoma
Scanning laser ophthalmoscopy (SLO) picture to monitor
Goldmann tonometry at slit lamp
disc changes: show progressive disc cupping with thinning
neural rim especially inferiorly
Two half rings are seen and approximated
to read pressure in mmHg
Too small/
low reading error
Tonometer touches anaesthezied cornea
Correct endpoint
Too large/
high reading error
Automated visual field testing
Humphrey analyser - progressing field defect: superior arcuate
Blind
spot
Early
Peripheral
Arcuate
arcuate
defect
defect
Gonioscope
Observation
Gonio lens to allow view
of drainage angle
Gonioscopic view of anterior chamber angle
Structures seen in angle
Pupil
Cornea
Cornea
Schwalbe's white line
Anterior chamber
Trabecular meshwork
Schwalbe's white line
Scleral spur
Pigment line
Trabecular meshwork
Iris root (ciliary body)
Schlemm's canal
Scleral spur
Iris
Iris
Ciliary body
Lens
80 Sub-specialty —Glaucoma
Aim
Monitoring
Understand how glaucoma is diagnosed.
Once a patient has been diagnosed and started on treatment, the
same techniques are used at regular intervals to assess for pro-
History taking
gression. Finding the correct treatment to prevent progression is
Apart from acute angle-closure glaucoma, most forms of glau-
dependent on these same examination techniques.
coma are asymptomatic until very advanced optic nerve damage
has occurred. A positive family history of glaucoma and myopia
Screening
are important risk factors in the history.
Most forms of glaucoma are asymptomatic until very advanced
optic nerve damage has occurred. Treatment at this stage is often
Clinical examination
too late, so glaucoma patients may be actively sought out from the
1 Visual acuity. Reduced by advanced chronic glaucoma damage
community, i.e. screened. This is usually done by opticians, who
or acute angle-closure glaucoma.
assess IOP, visual fields and optic disc appearance. Two main
2 Ocular examination.
groups of people are screened:
• Slit lamp examination for anterior segment abnormalities
1 People with a family history of glaucoma, especially primary
associated with glaucoma.
open-angle glaucoma.
• Detailed assessment of optic disc. Ideally the optic disc is
2 All people over 40 will have IOP measured at a sight test.
photographed (conventional or with 3D scanning laser ophthal-
If an abnormality suggestive of glaucoma is detected in this
moscope) to enable detection of progression.
screening process, the person is referred to the hospital ophthal-
3 IOP measurement. Using Goldmann applanation tonometer.
mology department.
Measures force needed to flatten a defined area of cornea. This
force corresponds to intraocular pressure (IOP, measured in mm
Problems of glaucoma screening
of mercury). NB, low tension glaucoma has normal range IOP.
• People are missed if they do not attend opticians.
4 Visual field testing. Usually assessed with automated perimetry
• False positives are common because the initial assessment of
to allow efficient repeat testing to detect progression. Classic
field and disc is difficult.
defect is arcuate scotoma.
5 Gonioscopy. Used to assess the anterior chamber angle. Can not
be viewed directly so gonioprism lens is used —the optics of which
WARNING
allow visualization of the angle between the cornea and iris.
Some patients have low-tension glaucoma in which they have field loss and
Glaucoma is diagnosed if a glaucomatous optic neuropathy
cupped discs with normal IOP.
(typical optic disc and field changes) is found to be present. Other
parts of the examination help classify the glaucoma so appropriate
treatment can be given.
KEY POINTS
• Glaucoma screening by opticians helps detect primary open-angle
TIP
glaucoma.
Do not rely on IOP measurement alone for the diagnosis and monitoring of
• A family history of primary open-angle glaucoma is a risk factor for devel-
glaucoma as the IOP may be in the normal range, yet disc and field changes
oping glaucoma.
may be present.
• Automated visual field analysis is used to monitor visual field progression.
Detecting glaucoma 81
38 Medical and surgical treatment of glaucoma
Medical treatment
Glaucoma surgery
This is the first line of treatment for glaucoma
Laser or drainage surgery is indicated when there is
progression of glaucoma not controlled by medication.
Laser iridotomy prevents acute angle-closure attacks
Laser treatments
Peripheral iridotomy
PI
Cyclodiode
Argon laser trabeculoplasty
Argon laser burns
Schwalbe's line
Trabecular meshwork
Ciliary body
Iris
Pupil
Surgical treatments
Trabeculectomy
Drainage devices/tubes
Bleb
Cornea
Iris
Diffuse bleb
PI
Scleral flap
Scleral flap
Sclerostomy
Bleb
PI
Sclera
Pupil
Lens Zonules
Tube in anterior chamber
Aims
Medical therapy
1 Understand the aims of medical, laser and surgical treatment
Treatment is tailored to each patient’s findings —intraocular pres-
2 Be familiar with the different classes of drugs used to treat
sure (IOP), visual field and optic disc appearance —and their type
chronic open-angle glaucoma.
of glaucoma. Most patients with chronic open-angle glaucoma are
3 Manage a case of acute angle-closure glaucoma (AACG).
treated medically and do not require surgery to drain the aqueous.
The aim of medical treatment is to prevent progression of disc
cupping or visual field defect.
Treatment goal
To preserve patient’s sight throughout their lifetime with minimum side
effects.
• Treat to lower IOP. This is the main aim of current glaucoma therapy.
• Treat to increase ocular perfusion. Prevent low blood pressure (nocturnal
dips), treat vasospasm (calcium antagonists) and prevent arteriosclerosis.
Treatment options
1 Medical therapy.
2 Laser.
3 Surgery.
82 Sub-specialty —Glaucoma
Table of topical medical treatments
Class of agent
Method of action
Side effects
Examples (trade name)
Beta-blocker
Decreases aqueous humour
Bradycardia/heart block
Timolol (Timoptol)
production
Bronchoconstriction
Betaxolol (Betoptic)
Depression
Carteolol (Teoptic)
Impotence
Levobunolol (Betagan)
Miotic (parasympathomimetic)
Increases outflow through
Blurred vision
Pilocarpine
trabecular meshwork
Headache
Eye ache
Carbonic anhydrase inhibitor
Decreases aqueous humour
Malaise
Dorzolamide (Trusopt)
production
Depression
Brinzolamide (Azopt)
Metallic taste
Acetazolamide (Diamox), oral and i.v.
Alpha-1 agonist
Decreases aqueous
Allergy
Brimonidine (Alphagan)
production and increases
Dry mouth
Apraclonidine (Iopidine)
uveoscleral outflow
Fatigue
Prostaglandin agonist
Increases uveoscleral outflow
Increased iris pigment
Latanoprost (Xalatan)
Eyelash growth
Travoprost (Travatan)
Macular oedema
Docosanoid
Increases uveoscleral outflow
Allergy
Unoprostone (Rescula)
Nausea
Nasal congestion
Prostamide
Increases uveoscleral outflow
Allergy
Bimatoprost (Lumigan)
Adrenergic agonist
Increases uveoscleral outflow
Rarely used now
Epinephrine (Eppy)
Dipivinyl epinephrine (Propine)
Laser treatment
Treatment of AACG
• Peripheral iridotomy. Procedure of choice to prevent angle-
AACG requires medical, laser and surgical treatment. Immediate
closure glaucoma or after an acute attack has been broken with
treatment is medical to reduce the IOP and to break the attack of
medical treatment. A YAG laser hole in the iris allows aqueous
angle closure.
flow from posterior to anterior chamber.
• Intravenous carbonic anhydrase inhibitor
(acetazolamide
• Cyclodestruction. Diode laser (usually) to ciliary body to re-
500 mg) is used to halt the production of aqueous fluid.
duce aqueous production.
• Oral acetazolamide may also be needed for up to 24 h.
• Argon laser trabeculoplasty. Laser to trabecular meshwork to
• Pilocarpine may be needed to break the attack, but is not used
increase aqueous outflow.
intensively.
• Other topical agents will also help reduce the IOP (timolol or
Surgical treatment
iopidine).
• Peripheral iridectomy. Used in AACG when laser is not possible.
• To prevent further attacks: pilocarpine drops (2-4%) are used
• Trabeculectomy. Standard glaucoma surgery to filter aqueous
(not intensively) in both eyes to constrict the pupil as a temporary
from anterior chamber to subconjunctival space, used most com-
measure. Bilateral laser iridotomies (and occasionally surgical
monly for open-angle glaucoma. Antimetabolites such as 5-
irridectomy) must then be performed as a permanent prevention.
fluorouracil and mitomycin C are used to modulate conjunctival
• Rarely, trabeculectomy is required.
healing and improve success rates. Risks include cataract, hy-
potony, infection and bleb leakage.
KEY POINTS
Other surgical techniques
• Most primary open-angle glaucoma patients are treated medically, e.g. with
• Drainage devices/tubes. Silicone tube inserted into anterior
topical beta-blockers.
chamber and connected to subconjunctival silicone chamber to
• Trabeculectomy lowers the IOP by draining aqueous into a small sub-
drain aqueous. Used when trabeculectomy may fail, for instance in
conjunctival bleb from where the fluid is reabsorbed.
congenital glaucoma and some of the secondary glaucomas.
• Surgery is indicated for disease progression in primary open-angle
• Deep sclerectomy. Section of sclera and roof of Schlemm’s
glaucoma.
canal are excised. No penetration into anterior chamber so less
complications than trabeculectomy, but less IOP control.
• Viscocanalostomy. Deep sclerectomy with additional mechani-
cal opening of Schlemm’s canal by injecting high viscosity fluid.
WARNING
Acute angle-closure glaucoma (AACG) is an ophthalmic emergency.
Medical and surgical treatment of glaucoma 83
39 Retinal detachment
Ora serrata
Anatomy of retina
Sclera
Choroid (supplies
outer 2/3 of retina)
Macula
Retina
Ciliary body
Foveola
Fovea
Vitreous
humour
Retinal
/body
vessels
(supply inner
Optic nerve (composed
1/3 of retina)
of ~ 1.3 million axons
coming from 1.3 million
rods and cones)
Floaters
Posterior vitreous detachment (PVD)
More noticeable on a sunny clear day against a blue sky,
or white snow, or a white wall/ceiling. They can be
Patient may see
On ophthalmoscopy:
particularly annoying when patients find that they get in
'dirt' or 'a cobweb'
the way of reading. They are common at any age.
or 'a fly'!
NB many people have floaters
Posterior vitreous detachment (PVD)
The vitreous gel 'jelly' separates from the posterior retina.
This also causes 'floaters' such as a Weiss ring and is
more common in older patients and myopics
WARNING
May see Weiss' ring
Vitreous body pulls away
Patients with PVD should be warned of the risk of retinal
floating in front of disc
from retina (to which it
tear and detachment - should they notice a sudden
is normally attached)
shower of floaters or new flashing lights or a shadow at
the edge of their vision, they should seek an urgent
ophthalmological opinion
Retinal detachment (RD)
On ophthalmoscopy:
May get small haemorrhage
Attached flat retina
Retinal tear
Tractional
Subretinal fluid
RD
Macula
Bullous RD
overhanging
Pale detached retina
disc and macula
Vitreous
Tobacco dust
Tractional band from
Retinal hole
old perforation site
Detached retina
WARNING
Blood vessel on detached retina
If the macula is detached there is a risk
Attached flat retina
of permanent visual impairment
Optic disc
84 Sub-specialty —Vitreoretinal and medical retina
Aims
reous to enter the space between the retina and the RPE.This type
1 Understand significance of eye floaters.
of RD is known as a rhegmatogenous retinal detachment. Individ-
2 Types of retinal detachment.
uals with high myopia are at increased risk of this type of RD.
3 Principles of managing a retinal tear.
• Some inflammatory and neoplastic conditions can lead to
serous exudation from leaky blood vessels beneath the retina in
Posterior vitreous detachment (PVD)
the absence of a retinal break or hole, this is referred to as an
A PVD is when the posterior aspect of the vitreous body pulls
exudative retinal detachment.
away or separates from the retina and collapses towards the vitre-
• Fibrous or vascular membranes growing abnormally in the vit-
ous base. Noticed as a floating cobweb, ring or tadpole, which
reous (e.g. in patients with diabetes or who have had a penetrating
moves with eye movement.
eye injury) can contract and pull the retina away from the RPE.
This is known as a tractional retinal detachment.
Aetiology
• A tumour such as a malignant melanoma originating in the
• Trauma to the eye or head.
choroid behind the retina can elevate the retina, causing a solid
• Spontaneous —especially in myopic eyes. Onset can be gradual
retinal detachment. This can metastasize and needs urgent
or more acute, and is due to degeneration of the vitreous gel.
treatment.
Symptoms
Symptoms
• Photopsia (i.e. flashing lights) results from physical traction of
Rhegmatogenous RD presents with:
the retina —not necessarily indicating a retinal tear. The flashing
• Photopsia ± floaters.
lights are more noticeable in dim lighting.
• Followed by gradual blurring or loss of vision, which may start
• Floaters result from a small amount of haemorrhage which may
off as a shadow in the peripheral visual field. As the SRF spreads
occur, or the collapsed vitreous which casts a shadow on the
to involve the macula, the vision becomes very blurred.
retina.A ring shape (Weiss’ ring) may be seen or cobwebs or a tad-
• Other types of RD present with reduced vision.
pole shape.
Natural history of floaters
Signs
The majority of floaters from PVD are self-limiting, setting as
• Visual acuity may appear normal when macula on.
occasional floaters and becoming less noticeable. Only a small
• Reduced visual acuity may be due to macular SRF or may result
proportion of patients develop a retinal tear.
from a bullous RD falling in front of the macula.
• On slit lamp examination, ‘tobacco dust’ may be visible in the
Complications
anterior vitreous (these are red blood cells and/or RPE cells that
In up to 15% of patients who present with an acute symptomatic
have migrated into the vitreous from the tear).
PVD the detaching vitreous pulls a hole in the retina, which can
• Intraocular pressure may be reduced.
lead to a rhegmatogenous retinal detachment.
• Detached retina on fundoscopy —indirect ophthalmoscopy
with scleral indentation is the preferred method of viewing this. A
Management
three-mirror contact lens at the slit lamp can be used if a retinal
• Full retinal assessment is needed to rule out a retinal tear —
tear is likely to require laser treatment and not full surgery.
examine through dilated pupils. The periphery of the retina can
be seen on the slit lamp using a three-mirror contact lens. Indirect
Complications
ophthalmoscopy with scleral indentation is the best method of
• If the RD involves the macular area, the chance of regaining
mapping the retinal detachment and location of the retinal tear.
vision is very much reduced.
• If a simple retinal tear is present with minimal or no subretinal
• Recurrent RD carries the risk of subretinal membrane and sec-
fluid—use laser treatment to seal the tear and to prevent retinal
ondary tractional detachment.
detachment.
• No tear —reassurance only, no treatment is required.
Management
• Rhegmatogenous RD —use reattachment surgery: laser, cryo-
Retinal detachment (RD)
therapy plus explant or internal surgery with vitrectomy.
• An RD occurs when the retina is separated from the retinal pig-
• Exudative and solid RD —establish and treat the cause.
ment epithelium (RPE) by fluid (this fluid is known as subretinal
• Tractional RD —relieve traction by vitreoretinal surgery.
fluid or SRF).
• Once the retina has been separated from its main blood supply,
the photoreceptors slowly begin to degenerate, becoming non-
functional by 6 weeks.
• It is therefore essential that once an RD has been diagnosed,
that it is surgically reattached as soon as possible in order to regain
KEY POINTS
vision.
• PVD results in floaters and there may be a retinal tear.
• If the macula is detached (off) surgery is urgent.
• Subretinal fluid gets under the retina through a tear and lifts the sensory
retina off the retinal pigment epithelium, causing a detachment.
Aetiology
• Some RDs do not have tears but are exudative, tractional or solid in origin.
• A full thickness tear in the retina, which may result from a spon-
taneous PVD or may occur as a result of trauma, allows liquid vit-
Retinal detachment 85
40 Retinal and choroidal anatomy and imaging
Knowledge of retinal anatomy and physiology is vital to interpret retinal images
Anatomy
Choroid: fenestrated capillary-rich layer which supplies oxygen and micronutrients
to the retinal pigment epithelium and the outer third of the neurosensory retina.
The capillary layer is the choriocapillaris
Retinal pigment epithelium (RPE): monolayer of pigmented cells between the
Fovea
neurosensory retina and Bruch’s membrane. Tight junctions exclude large
Foveola
molecules and form the outer part of the blood retinal barrier
Inner limiting
Bruch’s membrane: an acellular layer between the choroid and RPE, which does
membrane
not form a significant part of the blood retinal barrier
Retinal vessels
Ganglion cell layer
Neurosensory retina: includes photoreceptors, ganglion cells and their axons
Retina
Layer of intermediary
(nerve fibre layer), other neurons (e.g. bipolar cells) and glial cells (e.g. Müller cells)
neurons
Retinal arteries, capillaries and veins: non-fenestrated vessels forming the inner
Photoreceptor layer
blood retinal barrier
Foveal avascular zone: approximately 0.045 mm zone in which retinal capillaries
Cones only
Cones, some rods
are absent
Rods and cones
Retinal pigment
epithelium
Human methylmethacrylate vascular cast
Choroid
Bruch's membrane
Inner choriocapillaris surface -
Cross section of choroid showing
Sclera
Choriocapillaris
large surface area for nutrient
flattened choriocapillary sheet and
exchange to the outer retina
outer larger choroidal blood vessels
Fluorescein photography filters
Exciter filter
Barrier filter
Retinal pigment
490 mm
515 mm
epithelium cells
Bruch's membrane
Flat
Choriocapillaris
sheet
Intermediate-sized
chorio-
choroidal vessels
Outer larger
capillaris
choroidal vessels
Absorption
Emission
Copyright J Olver
Copyright J Olver
spectrum
spectrum
Topography of the posterior pole and retina
area centralis
Posterior pole
d = 5-6 mm
400
500
600
Wavelength (nm)
fovea
Indiocyanine green photography filters
Optic disc
Macula
Exciter filter
Barrier filter
d = 1.5mm
d = 1.5 mm
795 mm
830 mm
foveola
• Posterior pole area centralis (5-6 mm)
Fovea
• Macula fovea (1.5 mm)
d = 0.35 mm
• Fovea foveola (350 µm)
Fluorescein
Retinopathy pre-laser treatment
angiogram in a
Normal left macula in same eye
Disc
diabetic
new
Absorption
Emission
seen with i) fluorescein and
showing leaking
vessels
spectrum
spectrum
ii) indocyanine green
'new vessels
elsewhere'
FAZ
700
800
900
i) Retinal vessels imaged with
Wavelength (nm)
fluorescein angiogram showing
Fundus fluorescein angiogram of a
loss of capillary network at
left eye with gross myopia and
foveal avascular zone (FAZ)
consequent
chorioretinal
degeneration
ii) Choroidal vessels imaged.
and atrophy
Indocyanine green angiogram
(ICGA) showing rich choroidal
blood supply at macula
86 Sub-specialty —Vitreoretinal and medical retina
Aims
red or brown pigments (e.g. melanin in RPE cells or subretinal
1 Know the anatomy of the choroid and retina.
blood). ICGA is useful in investigating choroidal disease, e.g.
2 Identify the main priorities of medical retinal disease.
choroidal neovascularization and choroidal tumours.
3 Methods of retinal imaging and appropriate use of a particular
imaging system.
Confocal scanning laser ophthalmoscope (SLO)
4 Understand the need for more than one modality of imaging.
A fundus camera using a low-power scanning laser for illumination
at different focal planes in the retina to produce tomographic images.
Medical retinal disease priorities
Diabetic retinopathy and age-related macular degeneration are
Optical coherence tomography (OCT)
the main priorities in medical retina in terms of socioeconomic
Non-invasive diagnostic imaging analogous to an ultrasound B
health care burden (see Chapter 3) but vascular occlusions occur
scan except that light and not sound is used; a higher resolution is
commonly with age particularly in association with systemic
therefore obtainable.A highly coherent light source is used to scan
disease. The inherited retinal dystrophies affect 1 in 4000 of the
the retina and produces high-resolution, cross-sectional and 3D
population —young and old. The management of medical retinal
images. Used for assessing retinal thickness, retinal oedema and
disease has been revolutionized as a result of developments in
optic nerve head imaging in glaucoma.
retinal imaging, the advent of molecular genetics and new treat-
ment modalities.
Terms used when describing fluorescein angiograms
Retinal imaging modalities, together with psychophysical and
Hyperfluorescence: Increased fluorescence relative to other struc-
electrophysiological evaluation, are very valuable in diagnosing
tures seen as black on white if negative film is used and white on
disorders of the retina, retinal pigment epithelium (RPE) and
black with digital photography.
choroid.
Hypofluorescence:Reduced fluorescence relative to other structures,
e.g. due to blocked fluorescence or decreased vascular perfusion.
Imaging
Window defect: Increased choroidal fluorescence seen through a
A fundus camera can be used to document baseline retinal find-
window of attenuated RPE, e.g. geographic atrophy or laser scars.
ings, track disease progression, screening
(e.g. for diabetic
Blocked fluorescence: Masking of fluorescence by opacity anter-
retinopathy) and clinical studies.
ior to it, e.g. subretinal haemorrhage.
• A fundus camera ensures high resolution, high quality images.
Fluorescein leakage: Characteristic of conditions in which the
• Colour fundus photography, fluorescein and indocyanine
outer (RPE) or inner (retinal vasculature) blood-retinal barrier is
green angiography are used to image the retina and surrounding
disrupted.
structures.
Autofluorescence: Fluorescence occurring without the injection
• Digital images allow rapid diagnosis and review, and are elec-
of fluorescein dye.
tronically transferred; they are useful for telemedicine.
Side effects of fluorescein and indocyanine green
Dyes used in imaging
Fluorescein
Indocyanine green (ICG)
Fluorescein. Sodium fluorescein is an orange dye that is excited by a blue
light to emit a yellow-green light. It is a small molecule, only 80% bound to
Contraindications
blood proteins, which diffuses freely through the choriocapillaris, Bruch’s
Absolute
Fluorescein allergy ICG, iodine or shellfish
History of severe
allergy
membrane, optic nerve and sclera.
allergies
History of severe
Indocyanine green (ICG). This is a green dye, which when excited by a near
Relative
Asthma
allergies
infrared light emits a near infrared light. It is almost 100% protein bound so it
Ischaemic heart
Asthma
only leaks slowly through the fenestrated capillaries of the choriocapillaris.
disease
Ischaemic heart disease
Previous allergic
Previous allergic reaction
reaction
Liver failure
Renal failure (use
Fundus fluorescein angiogram (FFA)
lower dose)
This is a sequence of fundus images taken immediately after so-
Adverse effects
Skin discolouration Mild to moderate 0.35%
dium fluorescein dye is injected into a peripheral vein. The fundus
Nausea 3-5%
(e.g. hypotension)
is illuminated by a blue light causing the fluorescein molecules to
Allergy 0.5-1%
Severe 0.05% (e.g.
fluoresce in the yellow-green spectrum. Barrier filters block re-
anaphylaxis)
flected blue light so that only yellow-green (i.e. fluorescent) light is
Excretion
Liver and kidneys
Liver
transmitted to the film or digital camera.A detailed 3D view of the
retina and of the level of fluorescence can be achieved by using a
stereoscopic viewing device or computer software. Good for view-
ing retinal detail.
KEY POINTS
• Fluorescein angiography provides fine detail of the retinal structures and
Indocyanine green angiography (ICGA)
vessels.
Near infrared fluorescence is recorded with infrared film or more
• Indocyanine green provides information about the choroidal vessels.
commonly with a digital camera, after the injection of ICG into a
• There are potential side effects or complications of these dyes.
peripheral vein. Light of this wavelength has better penetration of
Retinal and choroidal anatomy and imaging 87
41 Inherited retinal dystrophies and age-related macular degeneration
Microanatomy
Classification of age related macular degeneration (AMD)
ARM
Photoreceptors: Rods: for vision in dim light (shades of black
and white) and motion vision. Cones: for vision in bright light
Histopathology and colour fundus picture of soft confluent Drusen at macula
(high resolution and colour). Rods predominate outside the
Courtesy of Victor Chong
fovea, cones are most dense at the fovea. Retinal Pigment
Epithelium (RPE): Single layer of cells with an important role
in the turnover and support of photoreceptor outer-segments
and formation of photosensitive pigments. Forms the blood-
retinal barrier. Bruch’s Membrane: Separates the RPE from
choriocapillaris. See Chapter 40
Definitions
Soft Drusen
Dystrophy: Inherited disorder
AMD
Photophobia: Painful sensation in bright light
Nyctalopia: Poor or lack of vision in the dark
Choroidal neovascularization (CNV)
Geographic atrophy (GA)
Neurosensory
Phenotype: Clinical characterization including symptoms
retina
(e.g. photophobia, nyctalopia), fundus appearance and
Exudate
functional assessment
Oedema
Inherited retinal dystrophies
Haemorrhage
A. Peripheral dystrophies - affect peripheral vision and vision
CNV
in low light levels, e.g. retinitis pigmentosa, choroideraemia
RPE
= 80% AMD
and Leber's congenital amaurosis
Bruch's
See Chapter 19
membrane
Retinitis pigmentosa (RP) varies in severity, mode of
Choroid
inheritance, age at onset, progression and phenotype.
Inheritance patterns include: autosomal dominant (AD),
autosomal recessive (AR), X-linked (Xl). Mitochondrial and
Classic CNV
Occult CNV
Pigment epithelium
syndromic retinopathy are also described
detachment (PED)
B. Central dystrophies - affect the macular region. Early
onset central visual difficulties with photophobia, loss of
detailed vision and colour vision defects, e.g. cone
dystrophies, macular dystrophies including Best disease,
Stargardt/fundus flavimaculatus, Sorsby, Bull’s eye,
Dominant drusen (Doyne honeycombe) dystrophy
PED
C. Mixed dystropies - Cone-rods affected with loss of
central and peripheral vision
Urgent referral for consideration: laser or surgery
D. Syndromal - e.g. AR Usher syndrome with hearing loss
and RP
Laser depends on position,
Photodynamic therapy depends
Peripheral dystrophy: Retinitis
character and size
on level of vision, position,
pigmentosa with intra retinal
character and size
mid peripheral bone spicule
pigmentation
Treatments under evaluation
• TTT: Trans-pupillary thermotherapy
• Surgery:
• Submacular surgery
• Macular translocation, RPE transplantation
Disciform scar
• Anti-angiogenesis: steroids, modulation
See Chapter 19
of vascular endothelial growth factor
Rehabilitation: Registration, low visual aids, advice re second eye - to report
distortion/decrease in vision
Educate AMD patient to report if decrease or distortion in vision. Consider
Central dystrophy:
Mixed dystrophy:
vitamin supplementation: Age Related Eye Disease Study recommendations.
Best dystrophy
cone rod
See Amsler chart, Chapter 7
88 Sub-specialty —Vitreoretinal and medical retina
Aims
• Pigment epithelial detachment
(PED): Accumulation of
1 Types of inherited retinal degeneration.
oedema ± blood beneath the RPE. An underlying CNV is com-
2 Know the significance of early central visual symptoms and
monly present in older patients.
prompt referral for possible early treatment of neovascular age-
• Retinal oedema and exudate: Leakage of serum into and behind
related macular degeneration (AMD).
the retina from CNV. Lipid components not easily removed by
3 Treatment options and importance of low-vision aids and social
macrophages accumulate, often at the edge of the oedema, as
support in both inherited retinal degeneration and AMD.
characteristic yellowish lesions.
Skills to obtain
Pathology
Use the ophthalmoscope to learn to recognize retinitis pigmen-
• RPE. Accumulation of photoreceptor, outer-segment waste
tosa and AMD.
products and vesicular granular material. GA may be due to re-
duced metabolic exchange between the choroid and RPE.
Inherited retinal dystrophies
• Bruch’s membrane. Focal and diffuse thickening with age.
A large number of disorders with progressive retinal degeneration
Accumulation of Drusen and presumed degrade collagen ma-
which are variable in severity, age of onset and may have distin-
terial from the RPE.
guishing phenotypic and functional features.The term retinitis pig-
• Choroid. Neovascularization arises from the capillary layer of
mentosa is used to describe peripheral dystrophies, but the latter
choroid. Photoreceptor atrophy and scarring begins early in neo-
term covers a spectrum of inherited progressive retinal degenera-
vascularization, even without haemorrhage.
tions. Features include night blindness, progressive visual field loss,
reduced or non-recordable electroretinograms and characteristic
Risk factors for AMD
pigmentary retinal degenerative changes in 1 in 4000.
• Genetic and environmental are implicated.
Classification of these disorders is enhanced by knowledge
• Cigarette smoking is a known risk factor.
of the inheritance pattern, causative gene(s) and mutation(s) if
• Vascular disease, hypertension and light exposure are asso-
known, and more sophisticated phenotypic characterization in-
ciated with AMD but are not risk factors.
cluding psychophysics and electrophysiology.
• Supplementation with extra carotenoids, certain vitamins and
antioxidants may be associated with a decreased risk of develop-
Age-related macular degeneration
ing AMD in certain types of ARM/AMD.
• Commonest cause of blindness in the elderly population.
• Approximately 2% of over 65 year olds are registered blind in
Diagnosis and assessment
one or both eyes from AMD in the UK.
• Recent symptoms of central distortion/blurring raise the pos-
• Geographic atrophy accounts for approximately 80%.
sibility of neovascular AMD.
• Treatment options are limited and are mainly targeted at neo-
• An Amsler chart (p. 20) is useful in evaluating central vision.
vascular AMD using laser photocoagulation or photodynamic
• Gradual decline, however, suggests GA.
therapy. Anti-angiogenesis therapies are being evaluated.
• Dilated fundus examination and FFA is essential in order to iden-
• Early symptoms require prompt referral for evaluation and
tify treatable CNV.
possible treatment of choroidal neovascularization (CNV). See
Treatment
Chapter 7, Amsler chart.
• Various types of laser, including photodynamic therapy for neo-
Definitions
vascular AMD.
• Age-related maculopathy (ARM): Disorder of the macular
• 90% of AMD is untreatable. GA or neovascular AMD with
area most often occurring after 50 years of age, characterized by
occult subfoveal CNV often results in significant scarring and/or
Drusen ± changes in the retinal pigment epithelium (RPE).
haemorrhage. New therapies are undergoing evaluation.
• Age-related macular degeneration (AMD): Late stages of
Rehabilitation
ARM that lead to progressive central vision loss. Includes: geo-
Blind/partially sighted registration
graphic atrophy of the RPE and subsequently photoreceptor cell
• Financial allowance.
loss, CNV, pigment epithelial detachment, haemorrhages, exu-
• Talking books/clocks.
dates and scar tissue.
• Home visit by low-vision therapist to assess disability.
• Drusen: Yellowish deposits external to the neuroretina and
• Initiate community care, Social and/or voluntary services.
RPE. May be well defined and small (hard) or ill defined (soft).
• Contact with self-help groups.
Drusen may be discrete or confluent and are hallmarks of age-
related change found at the level of Bruch’s membrane.
Low-vision aids (see Chapter 9)
• Geographic atrophy (GA): Demarcated zones of apparent
• Optical aids: magnifiers, telescopes.
RPE atrophy.Associated with Drusen. Gradual central vision loss.
• Non-optical aids: lighting, large print books/bank statements.
• Choroidal neovascularization (CNV): Abnormal new blood
• Electronic aids: closed circuit television (CCTV).
vessels that arise from the choroid and proliferate with subse-
quent fibrous tissue. Often not identifiable on ophthalmoscopy
but may be visualized using FFA.
KEY POINTS
• Disciform scar: Subretinal fibrovascular scar. Usually part of the
• Inherited retinal degenerations common, but no therapy available.
healing response following CNV. Permanent vision loss occurs as
• AMD is the leading cause of blindness in industrialized countries.
the outer retina (including photoreceptors) becomes atrophic or
• Sudden-onset central distortion/blurring may represent treatable CNV.
replaced by fibrous scar tissue.
Inherited retinal dystrophies and age-related macular degeneration 89
42 Diabetic retinopathy classification and typical lesions
Cotton wool spot (CWS)
Non-proliferative diabetic retinopathy (DR)
Severe non-proliferative DR
Intraretinal
Microaneurysms
microvascular
abnormalities
Looping
White vessel
Needs referral to ophthalmologist to decide treatment
Does not need treatment
Proliferative DR
Mixed diabetic maculopathy (DM)
Clinically significant macular
oedema (CSMO)
and ischaemic maculopathy
Hard exudate
New vessels on disc
(NVD)
Haemorrhages
Cotton wool spot
Advanced diabetic eye disease
Needs laser
Traction band
Beading
Tractional and fibrotic
changes with laser scars.
New vessels elsewhere
This is end-stage disease.
(NVE) with fibrovascular
Vitreo-retinal surgery
changes
may help
Needs laser
All figures copyright S Downes
Classification
Non-proliferative
Severe non-proliferative
Proliferative DR
Advanced proliferative
Maculopathy (especially
(background) DR
(preproliferative) DR
DR
late-onset diabetes)
Microaneurysms
Multiple haemorrhages
NV at disc (NVD) or
Vitreous haemorrhage
Focal or diffuse retinal oedema
Retinal haemorrhages
in all four quadrants
elsewhere (NVE)
Tractional retinal
near fovea
Cotton wool spots
Venous beading
Traction on NV causes
detachment
Focal oedema with ring of
Exudates outside
Intraretinal new vessels
vitreous haemorrhage
Neovascular glaucoma
exudates ('circinate') near fovea
temporal arcades
(NV)
or retinal detachment
Exudates near fovea
Haemorrhages near fovea
Loss of capillaries at macula
Sight-threatening — REFER TO OPHTHALMOLOGIST
(macula ischaemia)
Pathology
Basement membrane thickening
Acellular capillaries
'Angiogenesis' with
(Early) non-proliferative DR
Loss of endothelial cells and
'Capillary closure'
formation of NV
(Later) proliferative DR
pericytes
Local areas of retinal
Alteration of vascular
(Early, especially in late-onset DM)
Loss of vascular tone regulation
ischaemia and hypoxia
permeability
Maculopathy
Altered cellular adhesion
'VEGF response' and
Macular oedema
molecules
intracellular activation
Macular ischaemia
(including protein kinase C)
90
Sub-specialty —Vitreoretinal and medical retina
Aims
neovascularization (whose growth is induced by the release of
1 Learn the classification of diabetic retinopathy (DR) and its
angiogenic cytokines from the ischaemic retina).
pathogenesis.
• If new vessels grow at the optic disc they are referred to as
2 Be aware of contributory risk factors to severity of retinopathy
NVD.
(e.g. duration of diabetes, pregnancy, blood pressure).
• If new vessels grow at any other location they are described as
3 Understand the importance of DR screening.
new vessels elsewhere (NVE).
The new vessels are a response to hypoxia and ischaemia in an
• DR is the major cause of poor vision in the working population
attempt to increase the oxygen supply to the retina. However,
in the UK, Ireland, USA, Australia and the Indian subcontinent.
these vessels are weak and friable and bleed easily casing vitreous
The annual incidence of blindness from DR varies between 0.02%
haemorrhage.They may also cause traction on the retina resulting
and 1%.
in tractional retinal detachment.
• Alterations in different biochemical pathways as a result of
diabetes have been implicated in the development of the micro-
Microvascular changes resulting in leaking vessels
vasculature abnormalities that are seen in DR.
• Endothelial cell loss, pericyte loss of vascular tone result in in-
• An international standard classification of DR is essential for
creased permeability of the retinal vessels and hence exudation of
guidelines in screening, treatment protocols and research.
blood and blood products into the retina.
• Blot and dot haemorrhages, hard exudates and diffuse oedema
Definitions
are seen.
Microaneurysms: Outpouching of retinal capillaries. May bleed,
• These changes can also lead to localized vessel wall weakness
leak or become occluded.
and microaneurysm formation. These microaneurysms leak and
Cotton wool spot: Microinfarct of the retinal nerve fibre layer
exudates form in a circle around the aneurysm —‘circinate
(NFL) causing a localized swelling of the NFL axon (non-specific
exudates’.
indicator of retinal ischaemia).
Retinal oedema and exudate: Leakage of serum into the neural
Screening
retina due to vessel wall damage. Lipid components that are not
• DR is the leading cause of blindness in the working population
easily removed by macrophages accumulate, often at the edge of
in the UK.
the oedema, as characteristic yellowish lesions.
• Twenty-five per cent of diabetics develop DR; 10-13% of dia-
Venous beading: Venous irregularities, ‘sausaging’ and engorge-
betics have sight-threatening DR.
ment. Sign of retinal ischaemia and powerful predictor of conver-
• Prevalence of DR increases with duration of diabetes.
sion to proliferative retinopathy.
• Natural history of DR is known.
Retinal neovascularization/new vessels: Fragile new vessels grow
• Early treatment is effective in preventing visual impairment.
outside the retina along the posterior surface of the vitreous.
• An effective screening service requires effective recall of eligi-
Changes in bloodflow or traction on the new vessels, including
ble patients, 80% sensitivity, 95% specificity and quality assurance.
posterior vitreous detachment, may cause them to haemorrhage
• Digital photographic screening is the preferred method.
into the vitreous cavity (vitreous haemorrhage).
• Detection of any DR should direct attention towards improving
blood pressure and glycaemic control.
Pathology
Microvasculature changes causing ischaemia
KEY POINTS
• Basement membrane thickening, endothelial cell damage and
• DR is the leading cause of blindness in the working population of the devel-
loss, and increased platelet adhesiveness lead to narrowing of the
oped world.
retinal vessels and hence ischaemia.
• Screening and early treatment can prevent vision loss.
Ischaemia is manifest as: cotton wool spots, deep retinal
• Uncontrolled hypertension makes DR worse.
haemorrhages, venous beading and new vessel formation/
Diabetic retinopathy classification and typical lesions 91
43 Diabetic retinopathy treatment
Treatment options
Blood pressure, lipid and
Panretinal photocoagulation
Macular laser
Vitrectomy
glycaemic control
(PRP) laser
Reduce progression and severity
Laser (usually argon)
Focal or grid pattern
Aims: to
of diabetic retinopathy (DR)
Indicated for proliferative DR to
Encourages absorption of
Clear vitreous haemorrhage
Reduce need for laser
reduce risk of vision loss due to
oedema
Allow further PRP laser
vitreous haemorrhage or
Relieve retinal traction and repair
tractional retinal detachment
retinal detachment
Treat diffuse macula oedema due
to vitreous traction
In the UK and Ireland, the National Framework for Diabetes aims to raise
the standards for diabetic care including DR, and reduce blindness from DR
Proliferative diabetic retinopathy (DR)
Clinically significant macular oedema (CSMO)
Panretinal
Laser scar
photocoagulation
Parafovea with exudate
New vessels
Microaneurysms
on disc (NVD)
Needs more laser
Treated CSMO
Multiple episodes
Macula now dry
Microaneurysms
Panretinal
photocoagulation
Exudate
New vessels
elsewhere (NVE) -
Coalescing laser scars
still proliferative
and undergoing
more laser
Needs more laser
Needs gentle laser burns
DR treatment options
Good diabetic, blood pressure and lipid control.
Antiangiogenesis agents under evaluation.
Current therapies include (a) laser and
(b) vitrectomy surgery
(a)
(b)
All figures copyright S Downes
92 Sub-specialty —Vitreoretinal and medical retina
Aims
• Once adequate laser has been applied, the abnormal vessels will
1 Be aware of the treatment options in diabetic retinopathy
regress in about 8 weeks.
(DR).
2 Be able to explain about laser treatment to the patient.
Macular laser
• Focal laser is used to destroy microaneurysms that are leaking
• Blood pressure, lipid and glycaemic control:
exudate into the macular area. After the aneurysm has been
—reduces the progression and severity of DR;
treated the exudates will resorb.
—reduces the need for laser treatment.
• Grid laser is used to treat non-ischaemic diffuse macular
• Patients should also be advised not to smoke as this contributes
oedema. The entire macula, excluding the fovea, is treated with
to vascular damage.
very tiny low-powered laser in order to encourage absorption of
• Any underlying anaemia should be treated.
oedema.
• Patients must be warned that macular laser treatment is used to
prevent vision getting worse, and does not always improve visual
TIP
acuity. Some patients notice a scotoma after macular laser
Early treatment = better vision.
treatment.
Vitrectomy
This is a specialized procedure whereby the vitreous is removed
Treatment options
via a trans-pars plana incision, hence the term trans-pars plana vit-
The commonest treatment for DR is laser photocoagulation —
rectomy (TPPV). TPPV is carried out by a vitreoretinal surgeon,
either panretinal, or focal laser or grid laser to the macula. DR
usually under general anaesthesia.
often requires multiple treatments.
Indications
Panretinal photocoagulation (PRP)
• To clear vitreous haemorrhage —this allows the surgeon to visu-
• Indicated for proliferative DR to reduce the risk of vision loss
alize the retina and apply further PRP laser.
due to vitreous haemorrhage or tractional retinal detachment.
• To relieve retinal traction and repair retinal detachment.
• An argon laser is used to produce 1500-3000 tiny burns in the
• To treat diffuse macula oedema due to vitreous traction.
peripheral retina, sparing the macula, papillomacular bundle and
optic nerve head.This causes regression of new vessels at the optic
disc (NVD) and new vessels elsewhere (NVE).
• The patient will have reduced peripheral and night vision post
PRP.
KEY POINTS
• PRP is performed in the out-patient clinic using a laser attached
• Tight blood pressure, lipid and glycaemic control reduces the progression
to a slit lamp. The treatment requires topical anaesthesia as a spe-
and severity of DR and the need for laser treatment.
cial contact lens is used to apply the laser burns.
• PRP is the treatment for proliferative DR.
• Depending on the patient’s ability to tolerate the treatment and
• Focal laser is used to treat leaking microaneurysms at the macula, that are
the amount of burns required, the laser is applied over a number
threatening vision.
of sessions.
Diabetic retinopathy treatment 93
44 Retinal vein occlusion
The central retinal vein drains all the layers of the retina
Anatomy
Central retinal vein (CRV) course at optic nerve head
and the optic nerve head anterior to the lamina cribosa.
When it is occluded, there is marked venous engorgement
Layers
and leakage with retinal oedema, ischaemia and haemorrhage
Retina
Nerve fibre layer
Choroid
Prelaminar
Sclera
Laminar
Central
Human methylmethacrylate vascular cast
retinal
vein
Retrolaminar
All tissue has been dissolved away from the intralumen vascular casts
The optic disc: retinal venule
Isolated retinal cast
tributaries forming the central
with central retinal
retinal vein deep in the optic cup
artery and vein
Central
Retinal vasculature
retinal artery
Optic
cup
Retinal vein
tributaries
Neural
Central retinal vein
rim
Central retinal artery
Copyright J Olver
Copyright J Olver
Central retinal vein occlusion (CRVO) (left eye)
Neovascular glaucoma - iris new vessels and pathology
Histopathology of iris
surface with arrows
showing iris
neovascularization
Acknowledgements to Dr Brendon McDonald,
Neuropathologist, Oxford Radcliffe Infirmary,
Oxford for the histopathology slide
Rubeosis iridis: (iris neovascularization)
- end-stage disease
Hypertensive retinopathy
Branch retinal vein occlusion (BRVO)
• Usually asymptomatic and bilateral
• Can have BRVO or CRVO
• Range of features from generalized retinal
arteriolar narrowing, cotton wool spots, exudates,
arteriovenous crossing changes, flame-shaped
haemorrhages, to optic nerve head swelling
Fluorescein angiogram
Affecting three quadrants
Affecting one quadrant
of branch vein occlusion
(left eye)
(right eye)
Medical associations with retinal vein occlusion
Systemic
Retinal flame
BRVO and silver wiring
• ↑ Blood pressure
• Hyperviscosity syndromes
haemorrhages
• Diabetes mellitus
• Hypercoaguable disorders
• Hyperlipidaemia
94 Sub-specialty —Vitreoretinal and medical retina
Aims
Non-ischaemic CRVO
1 Identify the clinical features of central and branch retinal vein
• Mild fundus changes.
occlusion (CRVO and BRVO).
• No afferent papillary defect.
2 Management of CRVO.
• Visual loss not as profound as in ischaemic CRVO.
3 Management of BRVO.
• May not require laser treatment.
Skills to obtain
Branch retinal vein occlusion
Identify retinal vein occlusion with an ophthalmoscope.
Occur at arterovenous crossings and are 3 times more common
than CRVOs.
Retinal vein occlusion
Presents as with CRVO if extensive, or incidental finding. Reti-
Common cause of painless loss of vision—the condition can occur
nal haemorrhages and cotton wool spots are confined to one area.
at any age, with 85% of patients aged >50 years. Classified into
Chronic retinal changes: exudate, macular oedema and collateral
central (CRVO) and branch (BRVO), depending on the site of the
vessels. New vessels arise from the retina rather than the iris,
obstruction.The vein is occluded with thrombus, which represents
therefore these patients may get a vitreous haemorrhage but not
a secondary event following:
neovascular glaucoma.
• changes to the vascular endothelium;
• external pressure from an overlying arteriole that shares a
Management
common adventitial sheath (BRVO);
In both CRVO and BRVO it is important to detect and treat any
• increased thrombotic tendency.
underlying systemic disease in order to prevent the recurrence of
the venous occlusion.
Pathology
• Ophthalmic management:
Exact aetiology is unknown.The resulting venous occlusion causes:
—Check intraocular pressure (IOP) as may cause CRVO.
• Increased intravascular pressure:
—Screen for presence of new vessels (over 2 years).
—intraretinal haemorrhage;
• Medical management:
—retinal oedema;
—Check FBC, ESR, U&E, lipid profile, blood sugar, plasma
—altered vascular permeability.
proteins and blood pressure.
• Stagnation of flow:
—Medical treatment of cardiovascular risk factors.
—capillary non-perfusion;
—Aspirin.
—retinal ischaemia leading to the growth to new vessels at the
optic disc, retina or iris.
Treatment
Visual prognosis depends on the type of occlusion, the severity
CRVO
of the initial insult and the ocular sequelae. Visual loss is worse in
• Look for iris neovascularization in ischaemic CRVO—typically
CRVO than BRVO. Some small BRVO are asymptomatic, espe-
occurs at 3 months (‘100 day glaucoma’).
cially if it affects only one quadrant nasal to the disc (i.e. away from
• Reduce IOP if over 22 mmHg.
the macula) —only a slightly enlarged blind spot is found.
• Laser PRP is applied in the presence of new vessels.
Visual loss may follow:
• Cyclodiode if advanced and glaucoma.
• Ischaemic—vein occlusion affecting the fovea. New vessels give
BRVO
rise to vitreous haemorrhage or neovascular glaucoma.
• Follow up BRVO every 4-6 weeks for 6 months. If it worsens
• Exudation—blood-retinal barrier breakdown causes macular
and looks ischaemic, use PRP.
oedema and retinal exudate.
Central retinal vein occlusion
Hypertension and the eye
The CRV deep in the optic cup is occluded, affecting drainage
Looking at the retina you are looking at blood vessels in the body,
from all four retinal quadrants, resulting in usually unilateral pain-
which gives some idea of vascular damage. Severe vascular
less visual loss.
damage in the general population is uncommon and is seen in
special groups, for instance patients with renal failure.
Signs
• Afferent pupillary defect common.
• Dilated retinal examination demonstrates:
Systemic hypertension
Accelerated hypertension (rare!)
—retinal haemorrhages in all four quadrants;
Early changes:
Marked systemic changes plus lots
—optic disc swelling;
silver wiring
of retinal flame haemorrhages,
—venous dilation and tortuosity ±cotton wool spots.
AV nipping
star exudates at macula,
Later changes:
papilloedama, BRVO or CRVO
Ischaemic CRVO
flame haemorrhages
Up to 33% of cases are ischaemic, associated with new vessel
papilloedema
formation on the iris (rubeosis iridis) or disc, a risk of neovascular
glaucoma, and vitreous haemorrhage, and blindness. Requires
laser treatment.
KEY POINTS
Signs:
• The CRV drains the entire retina and prelaminar optic nerve head.
• Deep retinal haemorrhages.
• Ischaemic-type CRVO may develop neovascular glaucoma.
• More than 10 cotton wool spots.
• Some BRVOs are asymptomatic, but indicate systemic disease.
• Large areas of capillary non-perfusion (detected with FFA).
Retinal vein occlusion 95
45 Retinal artery obstruction
Central retinal artery course at optic nerve head
Anatomy
Retinal
arteriole
Layers
Retina
Nerve fibre layer
Choroid
Prelaminar
Sclera
Laminar
Central
retinal
Retrolaminar
artery
(CRA)
Human methylmethacrylate vascular cast
All tissue has been dissolved away from the intralumen vascular casts
Whole eye
View of PCA supply to choroids
and retrolaminar optic nerve
Vortex vein
Outer choroid
CRA
Optic nerve
Circle of Haller
and Zinn
Temporal bundle
Copyright J Olver
short posterior
ciliary arteries
Copyright J Olver
Central retinal artery
Optic disc
Choroid with
vasculature -
retinal arteriole
CRA divides
and residual
into four
capillaries
Choriocapillaris
arterioles at
the optic disc
Fine retinal capillaries
CRA
Retinal arteriole
Copyright J Olver
Copyright J Olver
Central retinal artery occlusion (CRAO)
CRAO with cilioretinal
Branch retinal artery
sparing
occlusion
Very ischaemic retina
Central patch of vision
Occluded branch (arrow)
is maintained
Cherry red spot
96 Sub-specialty —Vitreoretinal and medical retina
Aims
Diagnosis and management
1 Understand the vascular anatomy of the retina and optic nerve
Symptoms
head.
• Painless loss of vision (NB, non-ocular pain may occur such as
2 Identify the clinical features of a central retinal artery occlusion
temporal or scalp tenderness in giant cell arteritis (GCA)).
(CRAO).
• Profound drop in visual acuity
(unless cilioretinal artery
3 Be able to manage a patient with CRAO.
sparing).
• Afferent papillary defect.
Anatomy
The eye has a rich blood supply from the ophthalmic artery via the
Signs
central retinal artery (CRA) and the posterior ciliary arteries
Perform a dilated fundal examination to detect:
(PCAs). The CRA supplies the superficial nerve fibre layer and
• Cherry red spot at macula.
inner two-thirds of the retina. The PCAs supply the rest of the
• Embolus occasionally visible at optic disc.
anterior optic nerve and uvea (iris, ciliary body and choroid), and
• Attenuation of arterioles.
hence the deep retinal layers.The anatomy is known from vascular
• Retinal pallor.
casts (in vitro) and fluorescein angiography.
• Mild disc swelling.
In vascular casts of the eye the cadaver ophthalmic artery has
been injected with a plastic and the tissue has been dissolved away
Treatment
leaving only the vessel lumen —the cast.
The aim is to re-establish circulation within the CRA. This is at-
The CRA is an end artery of the ophthalmic artery, which sup-
tempted by:
plies the inner two-thirds of the retina. The choriocapillaris sup-
• Lowering the intraocular pressure (IOP) using:
plies the outer retina.
—acetazolamide 500 mg i.v.;
—ocular massage;
—anterior chamber paracentesis (1 ml aqueous withdrawn).
WARNING
• Vasodilation: rebreathe into a paper bag
(carbon dioxide
CRA obstruction causes ischaemia of the inner retinal layers resulting in
increases).
oedema of the nerve fibre layer (NFL).
• Start cholesterol lowering statins, e.g. Simvastatin,Atorvastatin.
Urgent: If bloodflow is not restored within 100 min, irreversible damage oc-
• Start antiplatelets, e.g. aspirin 300 mg stat then 75 mg daily or
curs at its narrowest point, which is the lamina cribrosa. A blockage more dis-
clopidogrel 75 mg daily, within 48 hrs.
tally gives rise to a branch artery occlusion.
WARNING
It is essential to check the erythrocyte sedimentation rate (ESR) and CRP to
Pathology
investigate for an inflammatory cause for CRAO, since GCA is often a bilateral
condition with catastrophic visual loss if not treated appropriately.
Retinal
Arterial occlusion
Inner retinal ischaemia
infarction gives
results from
causes
rise to
Outcome
Visual recovery is dependent on the interval between onset and
• Circulating
• Intracellular oedema —
• Loss of NFL
presentation. There has not been a clinical trial comparing treat-
embolus (e.g.
the retina appears white
• Pale optic disc
ment versus no treatment —but it is believed that 66% of patients
heart, carotids)
which masks the
have vision <6/60 following CRAO.
• Local atheroma
choroidal circulation,
• Arteritis (e.g.
except at the macula
giant cell arteritis)
‘cherry red spot’
Other investigations
• Miscellaneous
Examine for carotid bruits, heart murmurs and irregular pulse
(e.g. migraine,
(atrial fibrillation is a cause —needs anticoagulation). Arrange
syphilis, herpes
carotid Doppler studies, 24 h Holter monitor and echocardiogram.
zoster)
Follow-up by a physician.
Cilioretinal artery
KEY POINTS
NB, 15-20% of individuals have a supplementary arterial supply
• The CRA supplies the inner two-thirds of the retina.
to the macula via a cilioretinal artery derived from the posterior
• Do an ESR in all cases of CRAO to exclude GCA.
ciliary circulation at the disc. In the event of a CRAO, the macula
• A cilioretinal artery is present in 15-20% of individuals, which affords some
would remain perfused in these patients with some preservation
protection from severe visual loss.
of vision.
Retinal artery obstruction 97
46 HIV infection and AIDS
• AIDS (acquired immune deficiency syndrome) is caused by
Eyelids
infection with HIV (human immunodeficiency virus). It was
first described in 1981 in the USA and is now a global pandemic
• The number of reported cases underestimates the true extent
of this infection with over 75% of cases occurring in
sub-Saharan Africa, where the major mode of transmission
is heterosexual sex
• The incidence of heterosexual transmission is increasing in the
USA, Europe and Australia whereas intravenous drug users
(IVDU) and homosexual transmission is plateauing
• HIV infects cells by attachment to the CD4 antigen complex
found on many cells (CD4 cells, B-lymphocytes, macrophages,
Molluscum contagiosum on
Kaposi sarcoma lower eyelid
cells in CNS)
eyelid (usually multiple in HIV)
Intraocular inflammation
Retinal ischaemia
Herpes zoster ophthalmicus (5i) plus
maxillary branch involvement (5ii)
Anterior uveitis with
Cotton wool spots
granulomatous keratoprecipitates
Retinal/choroidal infections
Cytomegalovirus (CMV) papillitis and chorioretinitis
Varicella zoster virus retinitis (VZVR)
Toxoplasmosis retinochoroiditis
HIV modes of transmission
Sexual transmission (homosexual and heterosexual)
Parenteral transmission with blood and blood products:
semen from artificial insemination and organ transplantation
Occupational risk: small risk for healthcare workers of 0.3%
WARNING
after a single percutaneous exposure to HIV-infected blood.
Varicella zoster virus retinitis (VZVR) - may
Infection risk also from blood contamination of mucous
blind patients
membranes, non-intact skin and conjunctiva
Pneumocystis carinii pneumonia
• Acute retinal necrosis (ARN) and
Perinatal transmission: accounts for 80-90% of all
(PCP) choroiditis
progressive outer retinal necrosis (PORN)
paediatric HIV infections. Congenital HIV infection may occur
when immunocompetent and
transplacentally or intrapartum. The majority of infection
Visual prognosis:
immunosuppressed
occurs during birth or from breastfeeding
VZVR, CMV, toxoplasmosis
• PORN: bilateral multifocal retinitis with
retinochoroiditis and candida
Other routes: no evidence of HIV transmission from tears,
opacification in the outer retina and rapid
endophthalmitis may cause
sweat, urine or other body fluids
progression. Minimal or no vitritis. Very poor
severe visual loss.
NB. 30-50% of the non-HIV population will have serological
prognosis with standard therapies, leading
PCP and cryptococcal retinitis
evidence of previous toxoplasmosis
to blindness in most cases
is treatable
98 Sub-specialty —Vitreoretinal and medical retina
Aims
Toxoplasmosis retinochoroiditis (Toxoplasma gondii)
1 Modes of transmission of HIV (no evidence via tears).
• White or yellow patch of focal retinal necrosis. In HIV lesions
2 Lid, anterior segment, orbit, retinal and neuro-ophthalmic
tend to be larger; bilateral disease in 18-38%; unusual forms occur
manifestations.
(solitary, multifocal or miliary), often there is no pre-existing scar;
3 Causes of permanent visual loss in HIV.
minimal vitritis; prolonged therapy is required.
Ophthalmologic disorders in HIV
Syphilitic retinitis
Ophthalmic problems in AIDS are common and range from mild
Myriad presentations —vitritis, multifocal choroiditis, retinal vas-
conjunctivitis to sight-threatening retinitis. Any ocular or orbital
culitis, neuroretinitis, optic atrophy or oedema, exudative retinal
tissue may be involved. The commonest and most important op-
detachment, choroidal effusion, pigmentary retinopathy, and ve-
portunistic infection is cytomegalovirus retinitis (CMVR).
nous and arterial occlusions.
Lids/conjunctiva
Cryptococcal choroiditis (Cryptococcus neoformans)
• Trichomegaly —long eyelashes.
Variably-sized deep choroidal infiltrates; may be asymptomatic.
• Molluscum contagiosum on eyelids.
Pneumocystis carinii choroiditis
• HIV-related conjunctivitis.
Superficial yellow-white choroidal lesions.
• HIV conjunctival microvasculopathy —dilated, corkscrew-like,
tortuous vessels seen on slit lamp examination.
Mycobacterium tuberculosis choroiditis
• Kaposi’s sarcoma —flat or raised (if present >4/12) violaceous
Single large granuloma or multifocal; ±retinal vasculitis; frequent-
vascular lesion, surrounded by tortuous and dilated vessels. Com-
ly bilateral; choroidal neovascularization may develop at sites of
mon in conjunctival fornix. Treated by excision, chemotherapy or
healed spots.
radiotherapy.
Mycobacterium avium-intracellulare choroiditis
• Conjunctival granulomas due to cryptococcal infection, tuber-
Similar to multifocal choroiditis seen in cryptococcal and Pneu-
culosis and other mycotic infections.
mocystis carinii pneumonia (PCP) infection.
• Squamous cell carcinoma (see Chapter 24). Associated with
human papillomavirus infection. Aggressive tumour found on the
Candida endophthalmitis (Candida albicans)
lid or conjunctiva.
Small, whitish, multifocal, circumscribed chorioretinal infiltrates;
• Herpes zoster opthalmicus (HZO) often affects the VIIth nerve
retinal haems; dense vitritis and ‘fluff balls’ (vitreous abscesses)
too.
progress to endophthalmitis; often IVDU.
Cornea/anterior uveitis
Aspergillus endophthalmitis
• Anterior uveitis from drug toxicity (rifabutin, cidofovir).
Dense vitritis and vitreoretinal abscesses (similar to Candida
• Herpes simplex keratitis.
infection).
• HZO keratitis.
Ocular histoplasmosis infection (Histoplasma capsulatum)
• Microsporidia: a protozoal infection causing coarse, superficial,
punctate keratitis with minimal conjunctival reaction.
Endophthalmitis (iritis, vitritis, yellow iris infiltrates, multiple
creamy foci of retinochoroiditis + pulmonary or disseminated
Orbital disease
infection) or solitary chorioretinal granuloma (±vitritis).
• Periorbital B cell lymphoma.
• Aspergillus mass.
Primary intraocular B cell lymphoma
• Burkitt’s lymphoma.
Typically high grade; significant vitritis
± iritis; peripapillary
• Kaposi’s sarcoma.
infiltrates; disc swelling; yellow-white sub-RPE lesions; vascular
sheathing; and vein or artery occlusion.
Retinal disease
HIV retinopathy
Neuro-ophthalmic disorders in HIV
• Cotton wool spots.
• Optic disc swelling secondary to cryptococcal meningitis.
• Retinal haemorrhages.
• Papilloedema secondary to progressive multifocal leucoen-
• Microaneurysms.
cephalopathy (PML), cerebral infarction, intracranial toxoplas-
• Ischaemic maculopathy.
mosis or lymphoma.
• Immune recovery uveitis (IRU). Occurs in eye with quiescent
• Optic atrophy secondary to retinal disease.
CMVR in patients responding to HAART, defined as vitritis of
• Visual field defects secondary to space-occupying lesions.
≥1+ or trace of cells + epiretinal membrane or cystoid macular
• Cranial nerve palsies secondary to intracranial SOL or
oedema.
infection.
• Unilateral facial palsy may be secondary to aseptic meningitis.
Retinal infections
Cytomegalovirus retinitis (CMVR)
Haemorrhagic or non-haemorrhagic, frosted-branch angiitis or
mimic central retinal vein occlusion.
KEY POINTS
Epstein-Barr virus (EBV) retinitis
• No evidence that HIV is transmitted from tears.
Multifocal choroidal inflammation; typically prodromal malaise.
• HZO or multiple molluscum contagiosum in a young adult may indicate HIV.
EBV DNA is present in normal ocular tissue hence its presence in
• Increased orbital B cell lymphoma in HIV.
vitreous biopsy is not conclusive evidence of EBV uveitis.
HIV infection and AIDS 99
47 Pupil abnormalities
Pupil abnormalities
Sympathetic innervation of pupil
Midbrain
Edinger-Westphal
nucleus
Hypothalamus
Dilator
Periaqueductal
pupillae
gray
Aqueduct
Sphincter
Pons
NA
pupillae
Pretectal
Long ciliary nerve
nuclei
Postganglionic neurone
Cervical
in carotid plexus
Posterior
Ach
cord
commissure
Superior cervical ganglion
Lateral
Preganglionic neurone
Ach
Ciliospinal
geniculate
centre of bulge
body
C8-T1
NA = Noradrenaline
Ach= Acetylcholine
Ciliary ganglion
Occulomotor
(3rd) nerve
Small
Horner's syndrome
pupil(s)
Uveitis
Drugs, i.e. pilocarpine
Neurosyphilis, i.e. Argyl Robertson
Long-standing Holmes-Adie pupil(s)
Sphincter pupillae
Congenital miosis or microcoria
Both pupils
Light to
constrict
Asymmetric
Physiological anisocoria
right pupil
pupils
(20% of population)
Physiological anisocoria (i.e. unequal pupil size)
Large
3rd nerve palsy
This can be distinguished from pathological anisocoria by observing
pupil(s)
Sphincter damage
the pupil size in the dark and then in the light — physiological
Drugs
anisocoria which is usually subtle should not change dramatically in
Dorsal midbrain syndrome
different levels of illumination (as opposed to Horner's syndrome which
Holmes-Adie pupil(s)
looks worse in the dark)
Posterior communicating
A relative afferent pupillary defect (RAPD) indicates serious ophthalmic
artery aneurysm
pathology (most commonly retinal or optic nerve disease) which
warrants immediate referral to an ophthalmologist
Holmes-Adie pupil
Congenital Horner's syndrome
3rd cranial
Pupillomotor
nerve
fibres are
superficial
Aims
• Size.
1 Understand how to assess a patient with abnormal pupils.
• Shape.
2 Understand the causes of pupil abnormalities.
• Light response.
3 Understand the neuroanatomy of pupillary light reflexes.
• Near response.
Pupil examination
Afferent pupil defect (APD) / relative afferent pupillary
When examining pupils you need to check for:
defect (RAPD)
• Symmetry.
• An APD results from damage to the visual pathway anywhere
100 Sub-specialty —Neuro-ophthalmology
from the retinal ganglion cell layer to the lateral geniculate body,
• Horner’s syndrome can be confirmed by putting 4% cocaine
thus causing a reduction in the input (afferent) signal reaching the
drops into each eye and observing the pupils 40 min later.The nor-
brainstem when a light is directed at the affected eye. Hence there
mal pupil will dilate, the Horner’s pupil will not.
is a similarly reduced output (efferent) signal reaching the pupil,
• Causes of Horner’s syndrome include Pancoast’s tumour of the
which consequently constricts to a lesser extent than if it had
lung, thoracic aortic aneurysm, trauma, carotid artery dissection
received a full signal.
(usually accompanied by neck pain) and CNS disease.All patients
• Because of the consensual light reflex, the unaffected pupil will
should be investigated appropriately.
also constrict to an equally lesser extent when the light is directed
• In congenital Horner’s syndrome the iris on the affected side is
towards the damaged side.
a different colour —iris heterochromia.
• Hence, if a light is directed at the better eye both pupils will con-
• Contamination of the eye with pilocarpine causes miosis.
strict fully and equally. If it is the immediately swung over (‘swing-
• Uveitis that has resulted in posterior synechiae can result in a
ing flash light test’) and directed at the affected eye (e.g. an eye
small pupil.
with an optic nerve lesion) both pupils will appear to dilate —
• Rarely, congenital microcoria can occur.
RAPD. In fact what has happened here is that both pupils are con-
stricting but to a lesser degree than when the light was directed at
Light-near dissociation
the normal eye, hence they only appear to dilate. When the light is
In some cases the pupil(s) will accommodate but not react to light.
swung back to the better eye the pupils will constrict.
This dissociation of the light and near reflex can occur in various
syndromes.
Fixed dilated pupil
• Dorsal midbrain or Parinaud’s syndrome. This may be due to a
• If a pupil is dilated and doesn’t react to light or accommodation,
lesion (e.g. pinealoma, cranipharyngioma) compressing the pupil-
it is important to examine eye movements and levator function in
lary light reflex fibres. The pupils may be large and eccentric.
order to exclude a third nerve palsy. NB, a unilateral enlarged
Associated features include absence of upgaze, upper lid retrac-
pupil caused by uncal herniation is a neurosurgical emergency.
tion and convergence retraction nystagmus, characterized by
• Because of the superficial location of the pupillomotor fibres
rapid convergence movements and retraction of both eyes on
(see figure), a partial third nerve palsy can occur where only the
attempted upgaze.
pupil is involved. In such cases a tumour or posterior communicat-
• Neurosyphilis or Argyll Robertson pupils. These pupils are
ing artery aneurysm must be excluded.
small and irregular, do not react to light but react briskly to near
• A fixed dilated pupil can result from inadvertent or accidental
stimuli.
contamination of the eye with cycloplegic agents such as atropine
• Holmes-Adie pupil. This is thought to result from a viral infec-
or cyclopentolate, hence the importance of a detailed history.
tion; the affected pupil is initially large and eventually may become
• Previous trauma or surgery where there has been extensive
miosed.There is no reaction to light, the near reflex is intact but de-
damage to the sphincter pupillae can result in a fixed dilated pupil.
layed and tonic (the patient should be asked to focus on a near tar-
• A fixed semidilated pupil in the presence of a hazy cornea, red
get for at least 1 min before the pupils begin to constrict, and when
eye and pain is seen in acute angle-closure glaucoma.
the patient is then asked to relax his accommodation the pupils are
slow to dilate again). These patients may also have absent tendon
Small pupil (miosis)
reflexes. Both pupils may eventually become involved.
• A small pupil in association with a very small amount of ptosis
• Patients with Myotonic dystrophy may have light-near
(no more than 2 mm —due to paralysis of Müller’s muscle) is
dissociation.
known as Horner’s syndrome. This results from a lesion of the
• Patients with diabetes may develop a pupil neuropathy result-
sympathetic chain anywhere from the hypothalmus to the eye.
ing in light-near dissociation.
• On dimming the lights the anisocoria will become more obvious
as the affected pupil doesn’t dilate in the dark as well as its
counterpart.
KEY POINTS
• There may be other associated features such as elevation of the
• Fixed dilated pupil —‘surgical third’ must be outruled.
lower lid, which together with the ptosis gives the appearance of
• Unilateral miosis —Horner’s syndrome must be outruled.
enophthalmos, reduced sweating on the ipsilateral side of the face
• RAPD —indicates optic nerve or retinal disease.
and occasionally conjunctival hyperaemia.
Pupil abnormalities 101
48 Optic nerve disease
Features of optic atrophy and papilloedema
Visual field loss
Reduced visual acuity
Reduced colour vision
Relative afferent
pupillary defect
Enlarged blind spot in papilloedema
12
N D
Centrocaecal scotoma in Lebers optic
Reduced
atrophy or vitamin B12 deficiency
visual
acuity
or
Red desaturation
Bitemporal hemianopia in optic
atrophy 2∞E pituitary tumour
Swollen discs
Multiple sclerosis (MS)
Pale
Left nerve is normal
Acute right papillitis
(swollen disc) in MS
Right unilateral optic
Left disc normal
optic neuritis
atrophy in MS
Demyelinating
plaque
Dawson's fingers
Benign intracranial hypertension (BIH)
Right optic
nerve higher
signal than
left
Coronal MRI scan showing
demyelination and high
Sagittal MRI scan showing
signal in right optic nerve
demyelination involving the
corpus callosum
Bilateral chronic papilloedema secondary to BIH
Leber’s Hereditary Optic Neuropathy (LHON)
A hereditary optic neuropathy affecting young males 20-30 years
Leber’s Hereditary Optic Neuropathy - bilateral involvement
Mitochondrial inheritance (i.e. passed via mitochondrial DNA) passed
through female side of the family in most cases
Often smokers
Presents with
Subacute painless loss of central vision in one or both eyes
Second eye involved within weeks-months
Centrocaecal scotoma
Typical circumpapillary telangiectatic microangiopathy
The primary mutation has prognostic implications:
11778 -
2-17% recovery
Blurred nasal disc margins and pre-capillary telangiectasis
3460 - 15-30% recovery
Typically discs swollen in the acute phase
14484 - 37-50% recovery
Treatment : none, advise to stop smoking
102 Sub-specialty —Neuro-ophthalmology
Aims
• Visual field defect: enlarged blind spot if there is significant
Know the causes of optic atrophy (pale disc) and swollen discs.
swelling; altitudinal defect if disc swelling is secondary to is-
chaemic optic neuropathy.
Optic atrophy/neuropathy
• Blurred disc margin ± splinter haemorrhages (see figure).
Clinical features
• VA is reduced, but can be normal, depending on the degree of
Aetiology
optic atrophy.
• Vascular: e.g. AION, CRV or diabetic papillopathy.
• In those patients with subtle optic atrophy and apparently nor-
• Inflammatory: ‘papillitis’, e.g. uveitis, sarcoidosis, viral, systemic
mal visual acuity, colour vision may be reduced and a visual field
lupus erythematosus or paranasal sinus disease.
defect present. Formal perimetry is essential, but confronta-
• Demyelination: multiple sclerosis —disc swelling may become
tional fields using a red target can be most informative.
bilateral. Disc(s) swollen or normal in acute phase, and eventually
• Relative afferent pupillary defect.
become pale after recurrent attacks.
• Disc pallor. In severe optic atrophy the entire disc may be pale,
• Hereditary: LHON—may become bilateral.
in many cases only part of the disc (e.g. the temporal part) will be
• Infiltrative: e.g. lymphoma.
affected and subtle disc pallor will be missed if both discs are not
• Infective: e.g. toxoplasmosis, herpes or Lyme’s disease.
compared.
Investigations
Aetiology
• Visual field analysis.
• Hereditary:
• Full blood count (FBC), blood glucose, ESR, CRP, coagulation
—Autosomal dominant optic atrophy: visual acuity may be
screen, infective screen (e.g. toxoplasmosis and Borelia titres),
minimally reduced. Affected family members may vary con-
autoantibody screen.
siderably in abnormalities.
• Blood sent for analysis for Leber’s mutation if suspected.
—Autosomal recessive optic atrophy: poor visual acuity.
• Neuroimaging if demyelination or a compressive lesion is sus-
—Leber’s hereditary optic atrophy (LHON), (see figure).
pected. MRI of the brain and optic nerves should be requested.
• Retinal dystrophy:
• Lumbar puncture if demyelination, neurosarcoidosis or lym-
—Cone dystrophy: very poor acuity, markedly reduced colour
phoma are suspected.
vision, photophobia, central scotoma, nystagmus, typical ERG.
—Retinitis pigmentosa: typical retinal appearance, constricted
Bilateral disc swelling/papilloedema
visual fields and characteristic electroretinogram (ERG).
Clinical features
• Vascular: central retinal artery occlusion (history of angina or
• Visual acuity may be normal or severely reduced.
peripheral vascular disease and sudden profound loss of vision,
• Patients with papilloedema may complain of episodes of unilat-
typical fundal appearance in acute phase —cherry red spot, arteri-
eral or bilateral transient visual loss lasting for a few seconds.
olar attenuation).
These are transient visual obscurations (TVOs) and can be pre-
• Nutritional/toxic: vitamin B12
deficiency
(gradual bilateral
cipitated by changes in posture.
visual loss associated with pins and needles in hands and feet,
• Colour vision is often reduced.
poor diet, reduced colour vision, centrocaecal scotoma), tobacco-
• Enlarged blind spot if the swelling is significant; it will be normal
alcohol amblyopia or drugs (e.g. ethambutol, chloramphenicol).
in mild cases.
• Inflammatory: sarcoidosis, polyarteritis nodosa, contiguous
sinus disease —more commonly present with disc swelling.
Aetiology
• Demyelination (may have past history of typical attacks of optic
• Raised intracranial pressure: SOL, hydrocephalus, benign/
neuritis, and may have other neurological symptoms). It is a
idiopathic intracranial hypertension (BIH/IIH).
common cause.
• Malignant hypertension.
• Compressive: optic nerve glioma or meningioma, orbital tu-
• Diabetic papillopathy.
mour or intracranial tumour.
• Infiltrative papilloedema, e.g. lymphoma.
• Toxic, e.g. ethambutol or chloramphenicol uraemia.
Investigations
• Formal visual field testing.
Investigations
• Visual evoked response/potential (VER/VEP).
• Blood pressure.
• ERG.
• Glucose, FBC and differential WCC, U&E, creatinine and ESR.
• Relevant blood tests depending on clinical history (e.g. vitamin
• Neuroimaging.
B12 and folate levels in a patient who is a vegan and has bilateral
• Lumbar puncture if the MRI is normal and BIH is suspected.
optic atrophy with glove and stocking paraesthesia).
• Visual fields (to monitor blind spot).
• Neuroimaging: MRI optic nerves and brain
Disc swelling
KEY POINTS
Unilateral disc swelling
• Rule out malignant hypertension in papilloedema.
Clinical features
• Urgent CT brain if headache, nausea, papilloedema, normal BP.
• Visual acuity may be normal or reduced.
• MRI if demyelination suspected.
• Reduced colour vision.
Optic nerve disease 103
49 Cranial nerve palsies and eye movement disorders
Neuroanatomy of the 3rd, 4th, 6th and 7th cranial nerves
Nystagmus, e.g. Albinism
Albino - this child's parents
are coloured. Notice the pale
skin and white eye lashes
Levator palpebre
Superior oblique
Albinism
Signs: • infantile nystagmus
Superior rectus
• decreased VA and photophobia
Medial rectus
• iris transillumination
2 types i) oculocutaneous: hair, skin, eyes
Lateral rectus
Pons
Tyrosinase +ve - some pigment as adult
Tyrosinase -ve - never pigment, typical 'albino'
Inferior oblique
ii) ocular: eye pigment affected, hair, skin are normal
Inferior rectus
Needs visual aids, tinted spectacles for glare, sun/skin advice,
3rd nerve
genetic counselling
4th ventricle
4th nerve
6th nerve
Right 4th cranial nerve palsy
Right 3rd cranial nerve palsy
Ptosis globe
'down and out'
Right hypertropia
PCA aneurysm
Bielchowsky +ve
Compensatory head tilt
Posterior
i.e. hypertropia worse
i.e. hypertropia less on tilting
communicating
on tilting to same side
to opposite side
artery (PCA)
Most patients will
adopt a head tilt
Occulomotor/
Pupillomotor
to minimise diplopia
3rd cranial
fibre superficial
nerve
Right 6th cranial nerve palsy
Right 7th cranial nerve palsy
Right internuclear ophthalmoplegia (INO)
Failure of right
Failure of right
abduction
adduction +
left abducting
nystagmus
Patient is attempting to close both eyes
but cannot close right eye
WARNING
Risk of blindness - needs urgent lid lowering
(botulinum toxin) if exposive keratitis and
Aetiology
subsequent eyelid surgery
WARNING
• Vascular (elderly)
• Demyelination of medial longitudinal fasciculus (MLF)
Acquired 6th nerve palsy in patient with
WARNING
shunted hydrocephalus = blocked shunt
in young people
= emergency
Management, investigate, surgery
• Needs MRI brainstem
104 Sub-specialty —Neuro-ophthalmology
Aim
• Watery eye (due to weakness of orbicularis oculi).
• Describe clinical features of IIIrd, IVth, VIth and VIIth cranial
• Sore red eye (due to corneal exposure).
nerve palsies, internuclear ophthalmoplegia (INO), gaze palsies
• Blurred vision secondary to exposure keratitis.
and nystagmus.
• Drooling.
Third nerve palsy
Signs
Symptoms
• Ipsilateral facial muscle weakness, involving the frontalis in
• Double vision —horizontal and/or vertical.
lower motor neurone lesions. The frontalis is spared in upper
• Droopy lid.
motor neurone lesions.
• Enlarged pupil.
• Lower lid ectropion secondary to orbicularis oculi weakness.
• Headache. NB, painful third with pupil involvement —exclude
• Corneal exposure may vary from superficial punctate erosions
posterior communicating artery aneurysm as soon as possible.
to corneal abrasion, and must be treated urgently to prevent ab-
scess formation and endophthalmitis.
Signs
• Ptosis.
WARNING
• Exotropia and hypotropia (globe appears down and out).
May have Vth nerve palsy and corneal anaesthesia.
• Fixed dilated pupil.
• Limitation of elevation, depression, and adduction.
Aetiology
May present with any of these or combination.
• Viral/idiopahtic, e.g. Bell’s palsy
(usually improves sponta-
Aetiology
neously) or Ramsay-Hunt syndrome (herpes simplex infection).
• Ischaemic/vascular (usually pupil sparing due to anatomy of the
• Compressive lesion:intracranial tumour,e.g.acoustic neuroma (may
pupillomotor fibres, and referred to as a ‘medical third’): diabetes
have associated Vth,VIth and VIIIth nerve palsy ) or parotid tumour.
mellitus (DM), hypertension, vasculitis or migraine.
• Vascular/ischaemic: DM, hypertension or vasculitis.
• Compressive lesion (pupil nearly always involved, and referred
• Inflammation, e.g. sarcoidosis.
to as a ‘surgical third’): posterior communicating artery aneurysm,
Internuclear ophthalmoplegia
tumour.
Symptoms
• Trauma.
• Horizontal diplopia.
• Congenital third.
• Inability to coordinate eye movements.
Fourth nerve palsy
Signs
Symptoms
• Failure to adduct the ipsilateral eye.
Double vision —vertical.
• Abducting nystagmus of the contralateral eye.
Signs
Gaze palsies
• Head tilt opposite to the side of the lesion.
Symptoms
• Hypertropia on the affected side.
• Usually asymptomatic.
• Limitation of eye movement down and to the right if left fourth
• May be unable to move eyes together to one side.
nerve palsy, and visa versa.
Signs
• Positive Bielchowsky’s sign, i.e. the hypertropia on the affected
• Failure to move both eyes to one side.
side gets worse on tilting the head to the same side.
• Both eyes may be deviated to one side.
Aetiology
Aetiology
• Trauma is the most common cause of IVth nerve palsy as has
Lesion affecting the supranuclear
(i.e. the neural pathways
the longest intracranial course, is very slender and runs under the
superior to the IIIrd, IVth and VIth nerve nuclei) pathways in the
tentorial edge. Trauma may result in bilateral fourths.
cerebral cortex or brainstem, e.g. stroke, demyelination or SOL.
• Ischaemic/vascular: DM, hypertension or vasculitis.
• Compressive lesion, e.g. intracranial tumour.
Nystagmus
• Congenital.
This is involuntary rhythmic to-and-fro oscillation of the eyes.
Fifth nerve palsy
Symptoms
Corneal anaesthesia.
• Congenital nystagmus is asymptomatic.
• Acquired nystagmus may cause oscillopsia, a sensation of rapid
Sixth nerve palsy
movement or oscillation of the visual environment.Patients describe
Symptoms
it as though looking at an old black and white film where everything
Double vision —horizontal.
flickers or wobbles; others notice only blurred vision, especially if
Signs
gaze-evoked nystagmus.
• Esotropia, worse for distance.
• Limitation of abduction of the affected eye.
WARNING
Refer any patient with nystagmus for prompt assessment by a neuro-
Aetiology
ophthalmologist to exclude intracranial SOL.
• Vascular/ischaemic: DM, hypertension, or vasculitis.
• Invading intracranial or nasopharyngeal tumour.
• Trauma, e.g. fractured skull base.
KEY POINTS
• Painful third —posterior communicating artery aneurysm.
Seventh nerve palsy
• Traumatic sixth —basal skull fracture.
Symptoms
• Internuclear ophthalmoplegia —demyelination.
• Inability to close eyelid (lagophthalmos) and facial weakness.
50 Visual field defects
A detailed knowledge of the neuroanatomy
of the visual pathway can help the clinician
to localize lesions from the field defect found
Left
Right
Left
Left
Right
Right
1
Optic nerve
temporal
nasal
nasal
temporal
1a
Superior arcuate scotoma
field
field
field
field
e.g. glaucoma
1b
Inferior arcuate scotoma
Nasal
e.g. glaucoma
retina
1c
Temporal
Centrocaecal scotoma
10
e.g. B12 deficiency optic neuropathy
retina
Leber's optic neuropathy
1
Optic nerve
Chiasm
1d
Superior altitudinal defect
Von Willbrand's
e.g. aion or pion
2
knee
3
1e
Inferior altitudinal defect
Optic tract
e.g. aion or pion
4
2
Junction optic nerve with chiasm
Lateral
Junctional scotoma
geniculate body
e.g. pit tumour, suprasellar meningioma,
Meyer's loop
craniopharyngioma, supraclinoid aneurysm
5
3
Chiasm
6
Bitemporal hemianopia
Inferior
i.e. pit tumour, chiasmal glioma,
horn of
meningioma, sarcoidosis, MS, abscess
lateral
4
Optic tract
ventricle
Incongruous left homonymous hemianopia
8
7
optic tract lesion, i.e. glioma, MS,
Optic
metastasis
radiation
5
Meyer's loop
Left superior quadrantinopia
i.e. temporal lobe lesion ('pie in the sky')
9
6
Parietal lobe fibres
Occipital
visual cortex
Left homonymous hemianopia
denser below, i.e. parietal lobe lesion
(mnemiopic LP = lower parietal)
7
Posterior optic radiation
Congruous left hemianopia
8
Deep occipital cortex
Left homonymous hemianopia with macular
sparing, e.g. SOL, MS, trauma, vasculitis
9
Macular fibres at occipital cortex
Central scotomatous left hemianopia,
e.g. SOL, MS, trauma, vascular constriction
10
Retina
Grossly constricted fields - retinal
dystrophy, e.g. RP or severe BIH
106 Sub-specialty —Neuro-ophthalmology
Aims
4 Optic tract
1 Understand the neuroanatomy of the various visual field
A lesion of the optic tract involves the temporal fibres (nasal field)
defects.
from the ipsilateral eye and the crossed nasal fibres (temporal
2 Recognize the causes of different field defects.
field) from the contralateral eye. A lesion completely destroying,
for example the right optic tract, will result in a complete left
Visual field defects
homonymous hemianopia. However, most optic tract lesions are
The most common visual field defects encountered in clinical
partial, and because corresponding fibres from the nasal and
practice include homonymous hemianopia, altitudinal field
retinal fields are not so close together in the tract, the homo-
defect, bitemporal hemianopia, grossly constricted fields, and
nymous hemianopia produced is incongruous (i.e. the hemi-field
enlarged blind spots.
defect from the right eye is not an identical shape to that of the
Note obvious clues that will help you, e.g. a hemiparesis —this
left) (4 on figure).
patient is most likely to have an ipsilateral hemianopia as the
result of a lesion in the contralateral cortex (see figure).
5 Meyer’s loop
A lesion of the optic radiation in the temporal lobe will affect
1 Optic nerve
Meyer’s loop, which contains fibres representing the inferior
A unilateral optic nerve lesion can result in various unilateral field
quadrant of the ipsilateral temporal retina, and the contralateral
defects depending on the nature of the lesion. The shape of field
nasal retina. This results in a superior homonymous quadran-
defect can give a clue to the diagnosis. For example:
tanopia, sometimes referred to as a ‘pie in the sky’ defect (5 on
• Glaucomatous cupping can result in an arcuate scotoma of the
figure).
superior (1a on figure) or inferior field (1b).
• Vitamin B12 deficiency can result in a centrocaecal scotoma (1c
6 Parietal lobe
on figure).
A lesion in the parietal lobe may affect the fibres from the superi-
• Anterior ischaemic optic neuropathy (a swollen disc can be
or quadrants of the ipsilateral temporal and contralateral nasal
seen in the acute phase) and posterior ischaemic optic neuropathy
retina, giving rise to an inferior homonymous quadrantanopia or a
(the disc will look normal in the acute phase) can result in an alti-
homonymous hemianopia denser below than above (6 on figure).
tudinal field defect. This can be superior (1d on figure) or inferior
(1e), depending on which vessels are involved.
7,8 Optic radiation to occipital cortex
• Complete severing of the optic nerve (e.g. as a result of trauma)
Any unilateral lesion affecting the more anterior portion of the
will cause complete ipsilateral visual field loss.
occipital cortex will give rise to a homonymous hemianopia. Be-
cause of the close proximity of the cells representing the corre-
2 Junction optic nerve with chiasm
sponding retinal points, the hemianopia will be congruous (7 on
Because of the arrangement of nerve fibres in the optic nerve and
figure), unlike the incongruous hemianopia seen with an optic
chiasm, a lesion pressing on the visual pathway at the junction of
tract lesion (the more posterior the lesion, the more congruous the
the intracranial optic nerve and the chiasm can produce a charac-
field defect). Because the macula has a large representation in the
teristic field defect (2 on figure), known as a junctional scotoma.
occipital cortex, and a dual blood supply, the central 5° of vision is
Such a field defect results because the lesion compresses both
maintained in an anterior cortical lesion —macular sparing (8 on
fibres from the nasal fibres (serving the temporal visual field) of
figure).
the ipsilateral optic nerve and the inferonasal fibres (superotem-
poral field) from the contralateral eye in Willbrand’s knee.
9 Macular fibres at occipital cortex
A posterior lesion affecting one side of the occipital cortex will re-
3 Chiasm
sult in a homonymous hemianopic scotomatous field defect (9 on
A lesion pressing on the optic chiasm, such as a pituitary tumour,
figure).
will result in damage to the nasal fibres from both eyes as they
cross the midline, and therefore results in a bitemporal hemi-
KEY POINTS
anopia (3 on figure). Early on, if the lesion is only minimally com-
• Bitemporal hemianopia indicates a chiasmal lesion —most commonly a
pressing the chiasm, the field defect will be very subtle, and may
pituitary tumour.
only be picked up by using a red target (the individual will have
• Left homonymous hemianopia indicates a right cortical brain lesion.
red desaturation in the affected field —this is true for all subtle
• Altitudinal field defect is typical of anterior ischaemic optic neuropathy.
lesions).
Visual fields defects 107
Appendix: Red eye
Signs and symptoms of different causes of a red eye
Signs and
Subconjunctival Corneal
Acute
Corneal
Symptoms
Conjunctivitis
haemorrhage
abrasion
Allergy
Iritis
glaucoma
ulcer
History
Family/
Trauma,
Injury
Hay fever,
Nil or other
Change of
Contact lens,
friend
hypertension
asthma,
inflammatory
lighting
injury
eczema
disease
Sensation
Grittiness
None, mild
Pain,
Itching
Pain,
Pain,
Pain,
irritation
photophobia
photophobia
photophobia,
photophobia
nausea
Vision
Normal
Normal
Decreased
Normal
Decreased
Decreased
Decreased
(if central)
Discharge
Purulent/clear
None
Tearing
Mucus
Tearing
Tearing
Tearing and
mucopurulent
Pupillary light
Brisk
Brisk
Brisk
Brisk
Sluggish
Mid-dilated
May be
reflex
and fixed
sluggish
Conjunctival
Diffuse, tarsal
Localized,
Diffuse
Diffuse, tarsal
Circumcorneal Diffuse
Circumcorneal
injection
area
bright red
area
Corneal
Clear
Clear
Stains with
Clear
Keratic
Cloudy
Stains with
appearance
fluorescein
precipitates
cornea
fluorescein
Intraocular
Normal
Normal
Normal
Normal
Normal or
Markedly
Normal or
pressure
elevated
elevated
elevated
Basic
Hygiene, may
Reassurance,
Padding,
Topical
Ophthalmic
Ophthalmic
Ophthalmic
management
require topical
check blood
topical
antihistamine
referral
referral
referral
antibiotics
pressure
antibiotics
108 Appendix: Red eye
Index
Note: page numbers in italics refer to figures, those in bold refer to tables.
Acanthamoeba
capillary haemangioma 52, 53
conjunctival-corneal intraepithelial neoplasia
corneal ulcer 33
capsulotomy, YAG laser 76
(CCIN) 66, 67
keratitis
66, 67, 69
Cardiff cards 46, 47
conjunctivitis 8
accommodation 20, 21, 22, 23
cataract 27, 33, 44, 45
allergic
34, 35, 65
age 22
assessment 72, 73
vernal/atopic 52, 53
loss with cycloplegia 30, 30
causes 72
children 52
range 23
congenital 45, 51
giant papillary 69
acetazolamide 83
surgery 8, 9, 74, 75, 76, 77
HIV infection 98, 99
aesthenopia 45
cavernous haemangioma 62, 62
infective 32, 33
age
central areolar choroidal dystrophy
88
perennial allergic 65
accommodation 22
central visual field loss 25
post-cataract surgery 76
see also macular degeneration, age-
cerebrovascular accident 42, 43
red eye 108
related
chalazion 10, 11, 34, 35, 53, 54, 55
vernal/atopic 52, 53
AIDS 98, 99
chemical injuries 36, 37
viral
32, 33
alkali burn 37
chiasm 106, 107
contact dermatitis 32
allergies 15, 64, 65
children
contact lenses 8, 9, 24, 25
conjunctivitis 34, 35, 65
blindness 13
acanthamoeba corneal ulcer
33
vernal/atopic 52, 53
cataract 45
bacterial keratitis 67
red eye 108
hyphaema 27
bandage 68, 68-9
vernal keratoconjunctivitis 52, 53
infants 46, 47, 52, 53
complications 68, 69
amaurosis, Leber’s congenital 88
newborn up to 2 months 46, 47
cosmetic 68
amblyopia 45
non-accidental injury 27, 51
therapeutic 68, 68-9
capillary haemangioma 53
ophthalmia neonatorum 33
cornea 66, 67, 70, 71
treatment 48, 49
orbital conditions 62
abrasion 26, 30, 39
amethocaine 31
red reflex 45
bacterial keratitis 67
Amsler chart 20, 21
refractive errors 45
contact lens 69
anaesthesia, topical drops 31
retinal disease 45
red eye 108
anisocoria, physiological 100
retinoblastoma 27
abscess 27, 32, 33
anophthalmia 51, 60
toddlers 46, 47
clarity
67
anterior chamber 27
visual development 47, 49
disease 66, 67
depth 74
visual impairment 13
dystrophy 67, 69
anterior segment 26, 27
young 46, 47
epithelial erosion 76
normal 72
see also neonates
examination 26, 27
trauma 37
chlamydial conjunctivitis 33
foreign body 38, 39
aphakia 75
chorioretinal degeneration/atrophy
86
grafting 70, 71
argon laser trabeculoplasty 82, 83
chorioretinitis, CMV 98
HIV infection 99
Aspergillus endophthalmitis 99
choroid 86
inflammation 67
astigmatism 23, 45, 53
central areolar dystrophy 88
neoplasia 66, 67
atropine 31
inflammation 33
oedema 76
autofluorescence 87
pathology 89
perforation 38
choroidal neovascularization 89
physiology 69
bacterial keratitis 66, 67
choroideraemia 88
sterile infiltrate
69
basal cell carcinoma of eyelid 11, 54, 55
choroiditis, HIV-associated 99
superficial injuries 38, 39
Bell’s phenomenon 53, 57
cicatricial pemphigoid 64, 64, 65
surgery 8, 9, 70, 71
benign intracranial hypertension 102, 103
ciliary arteries, posterior 96, 97
topography scan 70
benoxinate 31
ciliary body 30, 30
traumatic scarring 36, 37
Best dystrophy 88
inflammation 33
ulcer 32, 33
Bielchowsky’s sign 104, 105
cilioretinal artery 97
herpes simplex dendritic 66, 67
binocular single vision (BSV) 48, 49
circumciliary injection 32, 33
red eye 108
biometry 72, 73
clear lens surgery 74, 75
corneo-scleral rupture 38
blepharitis 34, 35, 53, 64, 64, 65
closed circuit television 24, 25, 87
cotton wool spots 90, 91, 98, 99
blind spot 19
colleges 9
cover tests 48
blindness 13
coloboma, eyelid 52
cranial nerve functions 61
diabetic retinopathy 91
colour blindness 21
cranial nerve palsy 99, 104, 105
economic 13
colour vision 20, 21
third 53, 100, 101, 104, 105
national registers 13
acquired defects 21
fourth-seventh 104, 105
night 89
commotio retinae 38, 39
cryptococcal choroiditis 99
registration 87
communicating artery, posterior, aneurysm
100,
cyclodestruction 82, 83
WHO classification 12
101, 104, 105
cyclopentolate 31
blocked fluorescence 87
cones
cycloplegia 30, 30
blood pressure control 92, 92
dystrophies 88
cytomegalovirus retinitis (CMVR) 98, 99
blowout fracture 38, 39
macula 20, 21
blunt injuries 38, 39
confocal scanning laser ophthalmoscope 87
dacryocystitis 58
brain tumours 44, 45
confrontation field testing 18, 18, 19
dacryocystography 58, 59
breast carcinoma 45
conjunctiva
dacryocystorhinostomy 53, 58, 59
Bruch’s membrane 86, 88
diseases 64, 64, 65
demyelination 104, 105
pathology 89
epithelial erosion 76
optic nerve 102, 103
bull’s eye dystrophy 88
examination 26, 27
dendritic ulcer 8, 30
buphthalmos 50, 51, 79
granuloma 99
HSV 33, 66, 67
HIV infection 98, 99
dermatitis, contact 32
canalicular disease 58, 59
microvasculopathy 99
dermoid cyst 52
Candida endophthalmitis 99
squamous cell carcinoma 99
dermolipoma 52
109
developing countries 13
Farnsworth Munswell 100-hue test 21
hordeolum 34, 35
diabetic neuropathy 101
fibrin plaque 76
external 53
diabetic retinopathy 10, 11, 90, 91
fix and follow 46, 47
Horner’s syndrome 100, 101
blindness 13
floaters 33, 42, 43, 84, 85
congenital 27
classification
90, 91
fluorescein angiogram 86, 87, 94
hyperfluorescence 87
definitions 91
fluorescein leakage 87
hypermetropia 22, 23, 45
health care burden 87
fluorescein photography filters 86, 87
correction 48, 49
treatment 92, 92-3
fluorescein preparations 30, 30-1
lenses 24
vision gradual loss 44, 45
fluorescence 87
refractive surgery 70, 71
diplopia 12, 48
foreign body
hypertension 45
Fresnel prisms 24, 25
corneal 38, 39
intracranial 40, 41
lenses 24
corneal abrasion 69
benign 40, 41, 102, 103
disciform scar 89
intraocular 45
ocular 78, 78
distance vision 16, 16-17
metallic 36, 37
retinopathy 94, 95
distichiasis
56
sensation 39
systemic 43
dorsal midbrain syndrome 100, 101
subtarsal 38, 39
hypertropia 104, 105
Doyne honeycomb macular dystrophy
88
fovea 29
hyperviscosity syndromes 43
driving 12, 13
avascular zone 86
hyphaema 27
cataract 73
Fresnel prisms 24, 25
child 27
driving licence 12
Fuchs’ endothelial dystrophy 67
traumatic 38, 39
drusen 28, 89
fundoscopy 28, 29
hypofluorescence 87
dominant 88
fundus 28, 29
hypopyon 27, 76
dry eyes 64, 64, 65
examination 10, 11, 31
ulcer 68
DVLA Visual Standards 12
flavimaculatus 88
fluorescein angiogram 86, 87
indocyanine green angiography 86, 87
ectropion 56, 57, 64, 65
photography 87
industrialized countries 13
epiphora 59
fundus camera 87
infants 46, 47, 52, 53
electronic scrolled text 24, 25
glaucoma 79
emmetropia 22, 22-3, 24
gaze palsies 105
infections
endophthalmitis
geographic atrophy 89
children 52, 53
HIV-associated 99
giant cell arteritis
40, 41, 43
eyelid 64
infective 27
glasses 24, 25
keratitis
66, 67
post-cataract surgery 76, 77
glaucoma 8, 9, 28, 78, 78-9
orbital cellulitis
52, 53
enophthalmos 38, 39, 60, 60
acute closed-angle 11, 32, 33, 78, 78-9
injury, penetrating 36, 37
entropion 56, 57, 64, 65
fixed dilated pupil 101
internuclear ophthalmoplegia 104, 105
enucleation 60, 61, 62, 63
treatment 83
intracranial hypertension
epiphora
chronic angle-closure 79
benign 40, 41, 102, 103
congenital nasolacrimal duct obstruction
50,
chronic simple 44, 45
idiopathic 40, 41
51
congenital 51, 79
intraocular lens 74, 75
see also eye, watering
detection 80, 81
intraocular pressure 26, 27
episcleritis
32, 34, 35
drainage 82, 83
glaucoma 78, 78-9
Epstein-Barr virus (EBV) retinitis
99
infantile 79
measurement 80, 81
esotropia 48, 49
medical treatment 82, 82-3
raised 76
evisceration 60, 61
neovascular 94
intraocular tumours 44, 45
exophthalmometry 60, 61
normal tension 78, 78
iodipine 83
exotropia 48
primary open-angle 44, 45, 78-9
iridectomy, peripheral 27, 83
eye
medical therapy 82
iridotomy, peripheral 82, 83
blood supply 40
red eye 108
iris
27
external 26, 27, 64, 64-5
secondary 78, 78, 79
heterochromia 27
disease 8, 9
surgery 82, 82-3
inflammation 33
penetrating injury 32, 33
topical treatments 83
injury 38, 39
phthisical 60, 61
glaucomatous cupping 10, 11
innervation 30
watering 50, 51, 53, 58, 59
globe position 61
neovascularization 94
eye department 11
glycaemic control 92, 92
iritis
27
eye drops 30, 30-1
Goldenhar’s syndrome 52
red eye 108
eye movements 10, 11
Goldmann fields 19
traumatic 39
disorders 104, 105
Goldmann tonometry 8, 26, 80, 81
Ishihara plates 21
eyelashes 26, 27
gonioscopy 80, 81
eyelid 26, 27
Graves’ orbitopathy 15, 56, 57, 62, 62-3
Jones Pyrex bypass tube 58, 59
basal cell carcinoma 11, 54, 55
coloboma 52
hand movements 17
Kaposi’s sarcoma 98, 99
ecchymosis 38, 39
hayfever 65
Kay’s pictures 46, 47
eversion 26, 27
headache 45
keratectomy, photorefractive 70, 71
examination 56, 57
visual disturbance 40, 41
keratitis
33, 66, 67
herpes simplex virus 34, 35
see also migraine
exposure 57
HIV infection 98, 99
hemianopia, bitemporal/homonymous 106, 107
herpes simplex disciform 66, 67
infections 64
herpes simplex virus (HSV)
microbial 69
lumps 54, 55
dendritic ulcer 33, 66, 67
peripheral necrotizing 67
malignant melanoma 54, 55
disciform keratitis 66, 67
superior limbic 65
malposition 56, 57
eyelid 34, 35
keratoconjunctivitis, vernal 52, 53, 65
measurements 56, 57
herpes zoster ophthalmicus 66, 67, 98, 99
keratoconus 66, 67, 68, 70, 71
nerve supply 56
Hertel exophthalmometry 60, 61
keratomileusis 70, 71
retraction 57
heterophoria 48
keratopathy, contact lens 69
squamous cell carcinoma 54, 55
heterotropia 48
keratoplasty, penetrating 70
tumours 54, 55
histoplasmosis 99
see also ectropion; entropion; ptosis
HIV infection 98, 99
lacrimal drainage anatomy/physiology
58
Holmes-Adie pupil 100, 101
lacrimal glands 58, 59
facial palsy 15, 56, 57
homocystinuria 27
tumours 62, 63
HIV-associated 99
homonymous hemianopia 106, 107
lacrimal scintigraphy 58, 59
family history 14, 15
homonymous quadrantanopia 106, 107
lacrimal surgery 8, 9, 58, 59
110 Index
lacrimal syringing 58, 59
Minims 26, 30, 31
optical coherence tomography 87
lagophthalmos 56, 57
miosis 100, 101
optical lenses 24, 25
laser, macular 92, 93
miotic eye drops 30
optics 22, 22-3
laser epithelium keratomileusis (LASEK) 71
Mohs’ migrographic surgery 54, 55
orbicularis muscle strength 57
laser ophthalmoscope, confocal scanning 87
molluscum contagiosum 98, 99
orbit
laser photocoagulation 92, 93
mucocele 58, 59
anatomy 60, 61
laser photoreactive surgery 70, 71
multiple sclerosis 102, 103
assessment 60, 60-1
laser therapy, glaucoma 82, 82, 83
Mycobacterium tuberculosis choroiditis 99
cellulitis
34, 35, 52, 53, 60
laser-assisted intrastromal in situ keratomileusis
mydriatic eye drops 30
child 62
(LASIK) 70, 71
myopia 22, 23, 44, 45
decompression 60
Leber’s congenital amaurosis 88
lenses 24
disease 62, 62-3
Leber’s hereditary optic neuropathy 102, 103
lenticular-induced 73
haematoma 38, 39
lens 27
refractive surgery 70, 71
HIV infection 99
cataract assessment 72, 73
myotonic dystrophy 15, 101
imaging 61
dislocated 26, 27, 38
implants 62, 63
nasal endoscopy 58, 59
injury 38, 39
surgery 8, 9
nasolacrimal duct obstruction 53, 58, 59
intraocular 74, 75
tumours 45, 62, 62, 63
congenital 50, 51
opacity 76
spread 61
near response 21
perforation 38
orbital floor fracture 38, 39, 61
near vision 16, 16-17
see also accommodation
orthoptists 49
blurred 30
leukaemia 27
oscillopia 105
neonates 46, 47, 50, 51
orbital cellulitis differential diagnosis 53
oxybuprocaine 31
neovascularization 27
leukokoria 50, 51
neuro-ophthalmic HIV-associated disorders
99
levator function 57
paediatric ophthalmology 8
neuro-ophthalmology 8, 9
light
page navigation 24, 25
neurosyphilis 100, 101
perception 17
palpebral aperture 56, 57
night blindness 89
response 20, 21
panretinal photocoagulation 92, 93
nits
52
light-near dissociation 101
papilloedema 10, 11, 99, 102, 103
non-accidental injury 27
lipids, control 92, 92
parietal lobe lesions 106, 107
neonates 51
LogMar acuity 16, 17
Parinaud’s syndrome 101
nucleosclerosis 72, 73
longitudinal fasciculus, medial, demyelination
partial sight 13
nyctalopia 89
104, 105
registration 87
nystagmus 104, 105
low-vision aids 24, 25, 87
patching 48
lumps
occupations 12, 13
patient types 9
around eye 52, 53
exclusions 12
pemphigoid, cicatricial 64, 64, 65
eyelid 54, 55
ocular history, past 14, 15
penetrating injury 36, 37
lymphoma 27, 45, 63
ocular hypertension 78, 78
perimetry, automated 19
primary intraocular B cell 99
ocular prosthesis 60, 61
periphery 29
oculoplastic surgery 8, 9
phacoemulsification surgery 74, 75
macula
ophthalmia
phenylephrine 31
clinically significant oedema 92
neonatorum 33, 51
photography, fundus 87
cones 20, 21
sympathetic 37
photophobia 89
dystrophy 88
ophthalmic emergencies 11
photopsia 42, 43, 85
examination 28, 29
ophthalmic examination, systematic 14, 15
photoreceptors, retinal 88
oedema 76
ophthalmic history 10, 11, 14, 15
photorefractive keratectomy 70, 71
sparing lesion 106, 107
ophthalmic skills, essential 10, 11
phthisical eye 60, 61
macular degeneration 13
ophthalmologists 49
pigment epithelial detachment 89
age-related 42, 43, 45, 87, 88, 89
ophthalmology
pilocarpine 100, 101
management 87
sub-specialties 8, 9
pinhole test 16, 16, 17, 22
visual rehabilitation 25
team 9
pituitary apoplexy 41
macular disease 21
training 9
pituitary tumour 8, 44, 45
drug-induced 45
ophthalmoplegia, internuclear 104, 105
haemorrhage 40, 41
macular fibres at occipital cortex 106, 107
ophthalmoscope 27
Pneumocystis carinii pneumonia (PCP)
macular laser 92, 93
confocal scanning laser 87
choroiditis 98, 99
maculopathy, age-related 89
direct/indirect 28, 29
post-enucleation socket syndrome 60, 61, 62, 63
magnifiers 24, 25
optic atrophy 11, 99, 102, 103
posterior pole 28, 29
malignant melanoma, eyelid 54, 55
optic canal trauma 36, 37
posterior segment 28, 29
Marfan’s syndrome 27
optic disc swelling 99, 102, 103
preferential looking 46, 47
margin reflex distance 56, 57
optic nerve 21
presbyopia 23
medical history, past 14, 15
cup : disc ratio 29
clear lens surgery 75
medical students, aims 10, 11
cupping of head 11, 78
lenses 24
medications 14, 15
damage 21
presenting complaint 15
medicolegal cases 36, 37
demyelination 102, 103
prisms 24, 25
meibomian cyst 10, 11, 34, 35, 55
disc 28, 29
proptosis 60, 60, 61
meibomian gland
disease 102, 103
orbital tumour 62, 63
blocked duct 53
head 29, 78
proxymetacaine 31
carcinoma 55
junction with chiasm 106, 107
Pseudomonas keratitis 67, 69
meibomianitis 34, 35, 64, 65
tumours 44, 45
pseudophakia 75
melanoma
visual field defects 106, 107
pseudophthalmia 60
iris
27
optic neuritis 20, 40, 41
pterygium 32, 34, 35, 64, 64, 65
malignant of eyelid 54, 55
optic neuropathy 102, 103
surgery 70, 71
membership examination 9
anterior ischaemic 40, 41
ptosis 57
metastases 63
compressive 37
neonatal 51
Meyer’s loop 106, 107
Leber’s hereditary 102, 103
paediatric 8, 52, 53
microaneurysms 91
non-arteritic anterior 43
third nerve palsy 104, 105
microphthalmia 60
posterior ischaemic 43
pubic lice 52
microphthalmos 50, 51
traumatic 36, 37, 39
pupils
micro-surgery 9
optic radiation to occipital cortex 106, 107
abnormal 10, 11, 100, 100-1
migraine 41
optic tract lesions 106, 107
afferent defect 100, 100-1
acephalgic 43
optical aids 87
dilatation 29
Index 111
examination 100, 100
scleritis
32, 34, 35
conjunctiva 99
fixed dilated 100, 101
scotoma 106, 107
eyelid 54, 55
leukokoria 50, 51
sharp injuries 38, 39
intraocular 44, 45
reactions 20, 21
Sheridan-Gardner test 46, 47
lacrimal gland 62, 63
relative afferent defect 100, 100-1
siderosis bulbi 37, 45
malignant 55
size control 30
Siedel test 76
orbital 62, 62, 63
small 100, 101
Sjögren’s syndrome 64, 65, 67
periocular 55
white 73
skull base fracture 105
slit lamp 26, 27
uveitis 27, 33
quadrantanopia, homonymous 106, 107
biomicroscope 29
anterior 98, 99
Snellen acuity 16, 17
immune recovery 99
reading glasses 77
social factors 12, 13
posterior synechiae 101
recurrent erosion syndrome 39
social history 14, 15
red desaturation 21
solar keratosis 55
varicella zoster virus retinitis 98
red eye 32, 33, 34, 35
Sorsby dystrophy 88
vascular occlusion 42, 43
signs/symptoms 108
spinning 46, 47
venous beading 90, 91
red reflex 10, 11
squamous cell carcinoma
vernal keratoconjunctivitis 52, 53
cataract 73
conjunctiva 99
sicca 65
children 45
eyelid 54, 55
viral keratitis
66, 67
red-green colour anomaly 21
squint see strabismus
viscocanalostomy 83
reflex, consensual 20, 21
staphylococcal keratitis 69
vision 8
refraction 22, 22-3
staphylococcal lid margin disease 64, 65
binocular single 48, 49
refractive errors 22, 22, 23, 44, 45
Stargardt dystrophy 88
blurred 33
family history 49
Statement of Educational Needs 13
delayed maturation 47
refractive surgery 8, 9, 70, 71
steroid eye drops 67
development 47, 49
relative afferent pupil defect (RAPD)
21
Stevens-Johnson disease 64, 65
distance 16, 16-17
retina 28, 29
strabismus 8, 48, 49
near 16, 16-17, 30
anatomy 28, 84, 86
detection 10, 11
occupational aspects 12, 13
bruising 39
stye 34, 35, 53
rehabilitation 24, 25
detachment 8, 9, 38, 42, 43, 84, 85
subconjunctival haemorrhage 32, 33, 34, 35, 38, 39
social aspects 12, 13
disease 44, 45
post-cataract surgery 76
Vision 2020 —the right to sight (WHO)
13
dystrophy 103
red eye 108
visual acuity 13
HIV infection 99
surgery
adults 16, 16-17
imaging 86, 87
cataract 74, 75, 76, 77
cataract 73
inherited dystrophies 87, 88, 89
clear lens 74, 75
children 46, 47
laser burns 28
cornea 8, 9, 70, 71
testing 49
medical 8, 9, 87
glaucoma 82, 82-3
definition 16
microanatomy 88
lacrimal 8, 9, 58, 59
driving licence 12
neovascularization 90, 91
laser photoreactive 70, 71
measurement 10, 11, 14, 15
neurosensory 86
Mohs’ migrographic 54, 55
retinal artery obstruction 96
occluded arteriole 8
orbit 8, 9
retinal detachment 85
oedema and exudate 89
ptosis 53
testing 49
photoreceptors 88
refractive 70, 71
visual disturbance 40, 41
retinal arterioles 96
strabismus 49
visual evoked potentials 41
retinal artery, central
training 9
children 46, 47
anatomy 96, 97
swinging flashlight test 20, 21
visual field
occlusion 11, 28, 42, 43, 96, 97
sympathetic ophthalmia 37
altitudinal defect 106, 107
retinal pigment epithelium 86, 88
syphilis 100, 101
central loss 25
pathology 89
syphilitic retinitis
99
defects 106, 107
retinal vein anatomy 94
examination 18, 18-19
retinal vein occlusion
tarsal strip
56
HIV-associated defects 99
branch 43, 94, 95
tear film 64, 64, 65
mapping 18, 18-19
central 42, 43, 94, 95
tearing 58, 59
normal 18, 19
retinal vessels 86
tears, hypersecretion 59
testing 80, 81
retinitis
telescopic glasses 24, 25
visual field test
10, 11
cytomegalovirus 98, 99
temporal arteritis 41
driving licence 12
HIV-associated 98, 99
tetracaine 31
visual function 61
pigmentosa 88, 89
text magnification 24, 25
visual impairment
retinoblastoma
thyroid eye disease 56, 57, 62, 62-3
trauma 37
child 27
decompression orbit 60
WHO classification 12
neonatal 51
proptosis 61
visual loss
retinochoroiditis, toxoplasmosis 98, 99
tight lens syndrome 68, 69
gradual 44, 45
retinopathy
timolol 83
retinal artery obstruction 97
HIV 99
torch, pen 26, 27
sudden
hypertensive 10, 11, 44, 45, 94, 95
toric lens 25
painful 40, 41
pre-laser treatment 86
toxoplasmosis retinochoroiditis 98, 99
painless 42, 43
of prematurity 50, 51
trabeculectomy 82, 83
visual pathway anatomy 106
proliferative 43
trabeculoplasty, argon laser 82, 83
vitrectomy 92, 93
see also diabetic retinopathy
trachoma 64
vitreoretinal surgery 8, 9
retinoschisis, X-linked 88
transient visual obscurations (TVOs) 40, 41
vitreous, posterior detachment 43, 84, 85
retinoscopy 22, 23
trauma 36, 37
vitreous haemorrhage 38, 39, 42, 43
retrobulbar haemorrhage 36, 37, 39
blunt injuries 38, 39
diabetic retinopathy 90, 91
retrobulbar neuritis 40, 41
penetrating injury 36, 37
trauma 38, 39, 42, 43
rhabdomyosarcoma 52, 53
sharp injuries 38, 39
rhinophyma 64
vitreous haemorrhage 38, 39, 43
wave front technology 70, 71
rodent ulcer see basal cell carcinoma
trichiasis
27, 56, 57, 65
Weiss’ ring 84, 85
Rose Bengal 31
tropicamide 31
Wessely’s ring 66, 67
rubeosis iridis 27, 94
tumours
window defect 87
scleral show 56, 57
benign 55
sclerectomy, deep 83
congenital 52
YAG laser capsulotomy 76
112 Index