CLINICAL
ANATOMY
BY SYSTEMS
Richard S. Snell, MD, PhD
CD-ROM
Preface
Welcome to Clinical Anatomy by Systems by Richard S.
logic investigations. The anatomy of Common Medical
Snell, MD, PhD. This CD-ROM is designed for medical
Procedures has also been included, and the complications
students doing their clinical rotations, allied health stu-
caused by an ignorance of normal anatomy have been
dents, dental students, nurses, and residents.
emphasized.
The information provided is in the form of Clinical
Examples of clinical cases are given at the end of each
Notes, which are linked to the appropriate chapters of the
group of Clinical Notes. Each clinical vignette is followed
main text. This gives students ready access to the basic
by multiple choice questions. Answers and explanations for
anatomic and clinical material. Sections on Congenital
the problems are given at the end of the section in the CD-
Anomalies are also included.
ROM.
The clinical material provides the medical professional
*No part of this CD-ROM may be reproduced in any
with the practical application of anatomic facts that he or
form or by any means without written permission from the
she will require when examining patients. It will also be of
copyright owner.
great assistance when interpreting the findings of techno-
iii
Introduction to Clinical
Anatomy
1
Chapter Outline
Skin
2
Blood Vessels
4
Lines of Cleavage
2
Diseases of Blood Vessels
4
Skin Infections
3
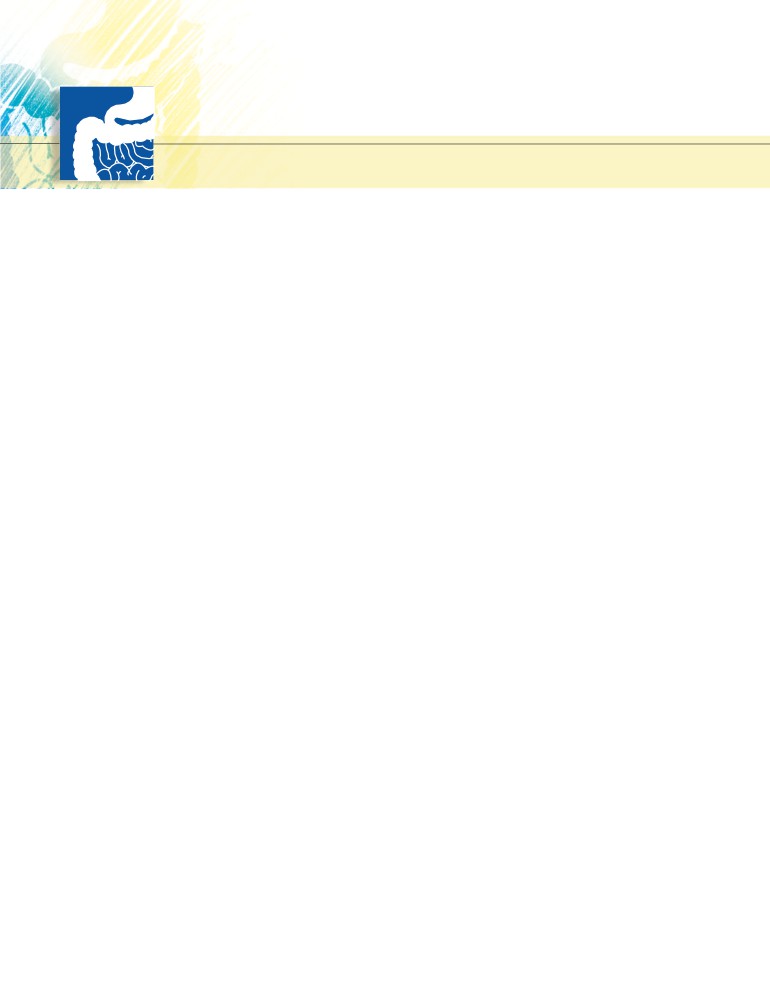
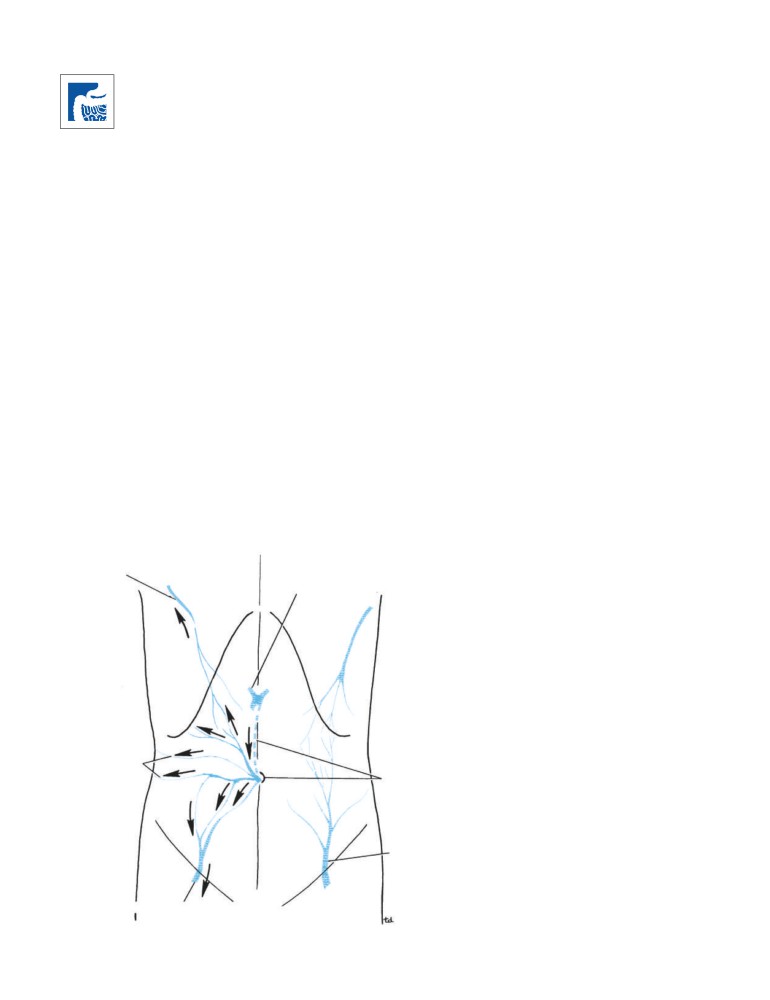
Lymphatic System
5
Sebaceous Cyst
3
Diseases of the Lymphatic System
5
Shock
3
Nervous System
5
Skin Burns
3
Segmental Innervation of Skin
5
Skin Grafting
3
Segmental Innervation of Muscle
5
Fasciae
3
Clinical Modification of the Activities of the
Fasciae and Infection
3
Autonomic Nervous Systems
5
Skeletal Muscle
3
Mucous and Serous Membranes
5
Muscle Attachments
3
Mucous and Serous Membranes and Inflammatory
Disease
5
Muscle Shape and Form
3
Bones
6
Cardiac Muscle
3
Bone Fractures
6
Necrosis of Cardiac Muscle
3
Rickets
7
Joints
4
Epiphyseal Plate Disorders
7
Examination of Joints
4
Clinical Significance of Sex, Race, and
Ligaments
4
Age on Structure
9
Damage to Ligaments
4
Clinical Problem Solving Questions
9
Bursae and Synovial Sheaths
4
Trauma and Infection of Bursae and Synovial Sheaths
4
Answers and Explanations
11
SKIN
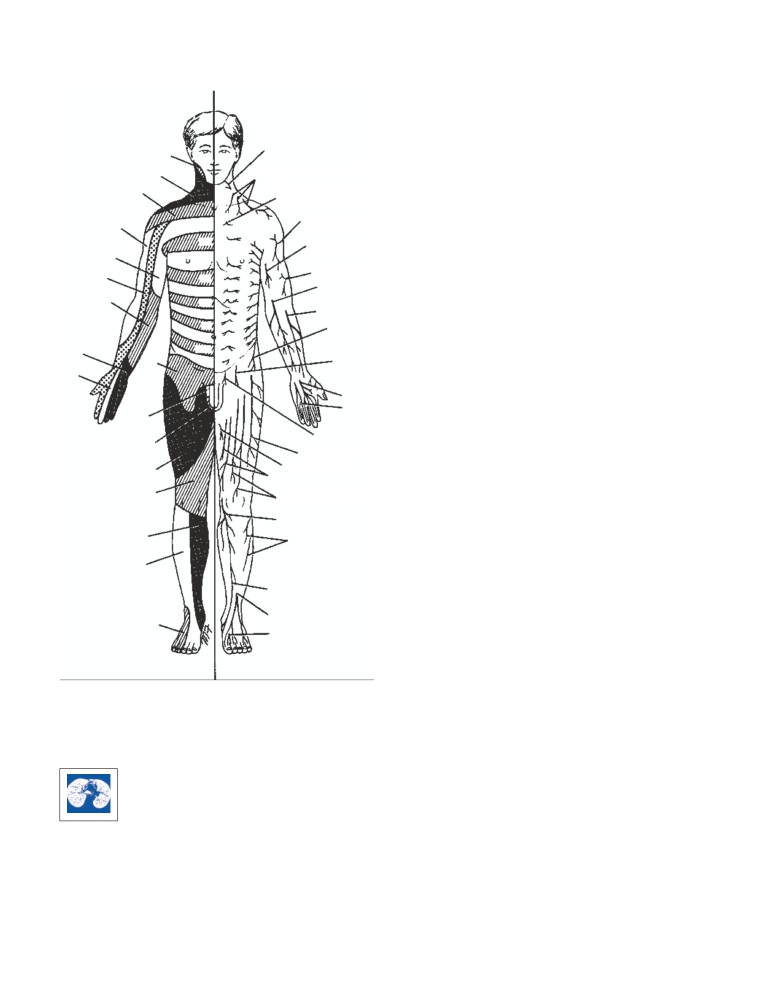
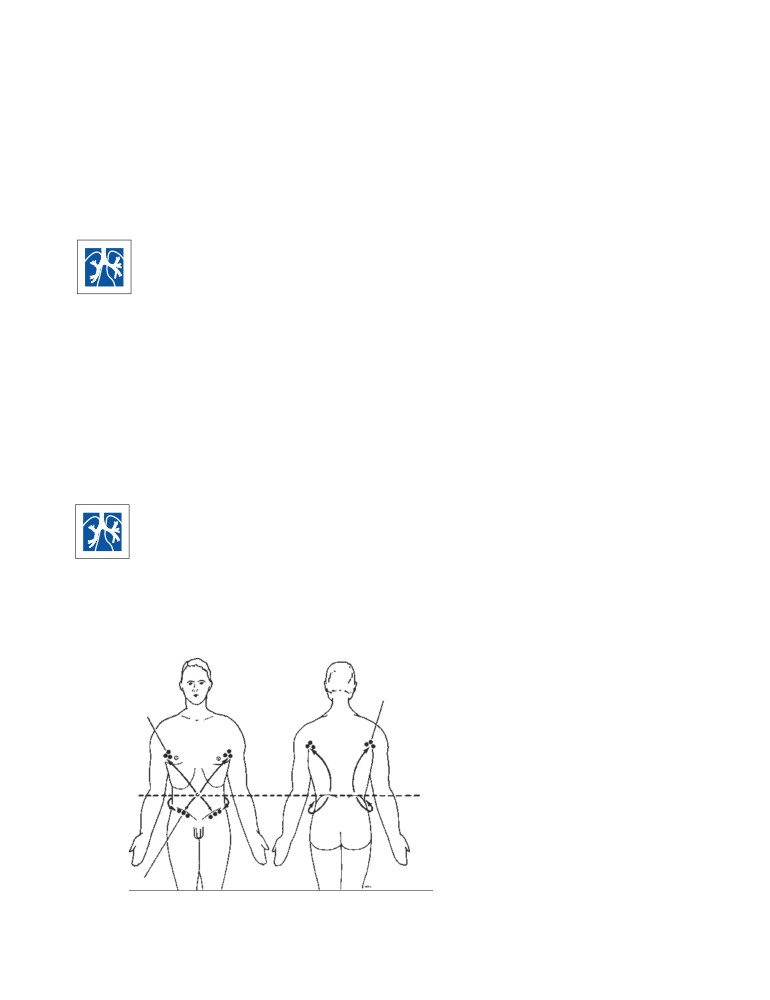
Lines of Cleavage
In the dermis, the bundles of collagen fibers are mostly
arranged in parallel rows. A surgical incision through the
skin made along or between these rows causes the mini-
mum of disruption of collagen, and the wound heals with
minimal scar tissue. Conversely, an incision made across
the rows of collagen disrupts and disturbs it, resulting in the
massive production of fresh collagen and the formation of a
broad, ugly scar. The direction of the rows of collagen is
known as the lines of cleavage (Langer’s lines), and they
tend to run longitudinally in the limbs and circumferen-
tially in the neck and trunk (CD Fig. 1-1).
CD Figure 1-1
Cleavage lines of the skin.
Introduction to Clinical Anatomy
3
A general knowledge of the direction of the lines of
new circulation within it at the recipient site. The donor site
cleavage greatly assists the surgeon in making incisions that
is usually covered with a split-thickness graft. In certain cir-
result in cosmetically acceptable scars. This is particularly
cumstances the full-thickness graft is made in the form of a
important in those areas of the body not normally covered
pedicle graft, in which a flap of full-thickness skin is turned
by clothing. A salesperson, for example, may lose his or her
and stitched in position at the recipient site, leaving the base
job if an operation leaves a hideous facial scar.
of the flap with its blood supply intact at the donor site.
Later, when the new blood supply to the graft has been
established, the base of the graft is cut across.
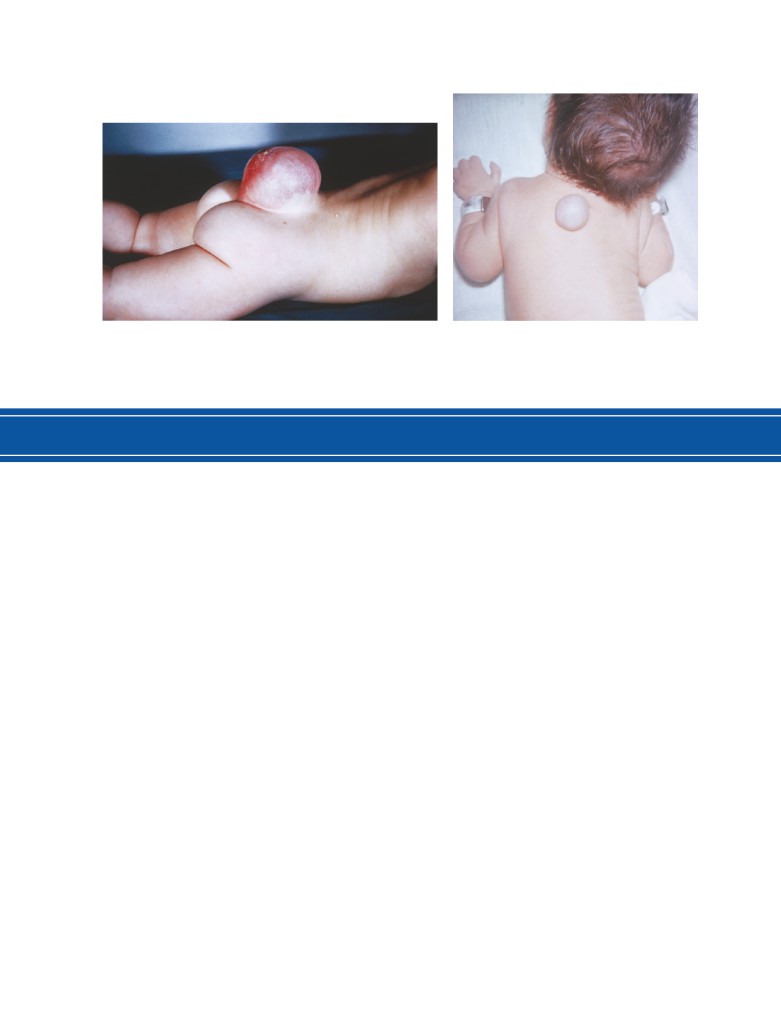
Skin Infections
The nail folds, hair follicles, and sebaceous glands are
common sites for entrance into the underlying tissues of
FASCIAE
pathogenic organisms such as Staphylococcus aureus.
Infection occurring between the nail and the nail fold is
called a paronychia. Infection of the hair follicle and seba-
Fasciae and Infection
ceous gland is responsible for the common boil. A carbuncle
Knowledge of the arrangement of the deep fasciae often
is a staphylococcal infection of the superficial fascia. It fre-
helps explain the path taken by an infection when it spreads
quently occurs in the nape of the neck and usually starts as an
from its primary site. In the neck, for example, the various
infection of a hair follicle or a group of hair follicles.
fascial planes explain how infection can extend from the
region of the floor of the mouth to the larynx.
Sebaceous Cyst
A sebaceous cyst is caused by obstruction of the mouth of a
SKELETAL MUSCLE
sebaceous duct and may be caused by damage from a comb
or by infection. It occurs most frequently on the scalp.
Muscle Attachments
Shock
The importance of knowing the main attachments of all
A patient who is in a state of shock is pale and exhibits goose-
the major muscles of the body need not be emphasized.
flesh as a result of overactivity of the sympathetic system,
Only with such knowledge is it possible to understand the
which causes vasoconstriction of the dermal arterioles and
normal and abnormal actions of individual muscles or
contraction of the arrector pili muscles.
muscle groups. How can one even attempt to analyze,
for example, the abnormal gait of a patient without this
information?
Skin Burns
The depth of a burn determines the method and rate of
Muscle Shape and Form
healing. A partial-skin-thickness burn heals from the cells of
the hair follicles, sebaceous glands, and sweat glands as well
The general shape and form of muscles should also be
as from the cells at the edge of the burn. A burn that extends
noted, since a paralyzed muscle or one that is not used (such
deeper than the sweat glands heals slowly and from the
as occurs when a limb is immobilized in a splint) quickly
edges only, and considerable contracture will be caused by
atrophies and changes shape. In the case of the limbs, it is
fibrous tissue. To speed up healing and reduce the inci-
always worth remembering that a muscle on the opposite
dence of contracture, a deep burn should be grafted.
side of the body can be used for comparison.
Skin Grafting
CARDIAC MUSCLE
Skin grafting is of two main types: split-thickness grafting
and full-thickness grafting. In a split-thickness graft the
greater part of the epidermis, including the tips of the der-
Necrosis of Cardiac Muscle
mal papillae, are removed from the donor site and placed on
the recipient site. This leaves at the donor site for repair pur-
The cardiac muscle receives its blood supply from
poses the epidermal cells on the sides of the dermal papillae
the coronary arteries. A sudden block of one of the large
and the cells of the hair follicles and sweat glands.
branches of a coronary artery will inevitably lead to necro-
A full-thickness skin graft includes both the epidermis
sis of the cardiac muscle and often to the death of the
and dermis and, to survive, requires rapid establishment of a
patient.
4
Chapter 1
clot at the damaged site is invaded by blood vessels and
fibroblasts. The fibroblasts lay down new collagen and elas-
JOINTS
tic fibers, which become oriented along the lines of me-
chanical stress.
Examination of Joints
When examining a patient, the clinician should assess
the normal range of movement of all joints. When
BURSAE AND
the bones of a joint are no longer in their normal
anatomic relationship with one another, then the joint is
SYNOVIAL
said to be dislocated. Some joints are particularly suscep-
tible to dislocation because of lack of support by ligaments,
the poor shape of the articular surfaces, or the absence
SHEATHS
of adequate muscular support. The shoulder joint, tem-
poromandibular joint, and acromioclavicular joints are
Trauma and Infection of Bursae
good examples. Dislocation of the hip is usually congeni-
tal, being caused by inadequate development of the
and Synovial Sheaths
socket that normally holds the head of the femur firmly
in position.
Bursae and synovial sheaths are commonly the site of
The presence of cartilaginous discs within joints, espe-
traumatic or infectious disease. For example, the extensor
cially weightbearing joints, as in the case of the knee, makes
tendon sheaths of the hand may become inflamed after ex-
them particularly susceptible to injury in sports. During
cessive or unaccustomed use; an inflammation of the
a rapid movement the disc loses its normal relationship
prepatellar bursa may occur as the result of trauma from re-
to the bones and becomes crushed between the weight-
peated kneeling on a hard surface.
bearing surfaces.
In certain diseases of the nervous system (e.g., sy-
ringomyelia), the sensation of pain in a joint is lost. This
means that the warning sensations of pain felt when a joint
moves beyond the normal range of movement are not
BLOOD VESSELS
experienced. This phenomenon results in the destruction of
the joint.
Diseases of Blood Vessels
Knowledge of the classification of joints is of great value
because, for example, certain diseases affect only certain
Diseases of blood vessels are common. The surface anatomy
types of joints. Gonococcal arthritis affects large synovial
of the main arteries, especially those of the limbs, is dis-
joints such as the ankle, elbow, or wrist, whereas tubercu-
cussed in the appropriate sections of this book. The collat-
lous arthritis also affects synovial joints and may start in the
eral circulation of most large arteries should be understood,
synovial membrane or in the bone.
and a distinction should be made between anatomic end
Remember that more than one joint may receive the
arteries and functional end arteries.
same nerve supply. For example, the hip and knee joints
All large arteries that cross over a joint are liable to be
are both supplied by the obturator nerve. Thus, a patient
kinked during movements of the joint. However, the distal
with disease limited to one of these joints may experience
flow of blood is not interrupted because an adequate anas-
pain in both.
tomosis is usually between branches of the artery that arise
both proximal and distal to the joint. The alternative blood
channels, which dilate under these circumstances, form the
collateral circulation. Knowledge of the existence and posi-
LIGAMENTS
tion of such a circulation may be of vital importance should
it be necessary to tie off a large artery that has been damaged
by trauma or disease.
Damage to Ligaments
Coronary arteries are functional end arteries, and if
Joint ligaments are very prone to excessive stretching and
they become blocked by disease (coronary arterial occlusion
even tearing and rupture. If possible, the apposing damaged
is common), the cardiac muscle normally supplied by that
surfaces of the ligament are brought together by positioning
artery will receive insufficient blood and undergo necrosis.
and immobilizing the joint. In severe injuries, surgical
Blockage of a large coronary artery results in the death of the
approximation of the cut ends may be required. The blood
patient.
Introduction to Clinical Anatomy
5
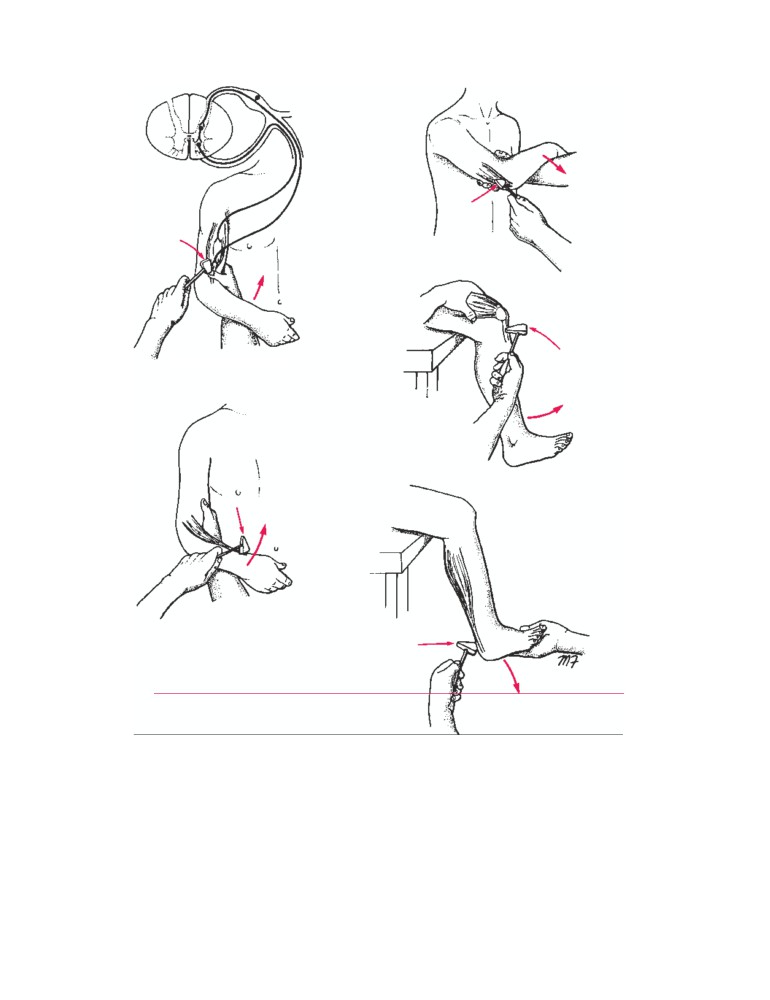
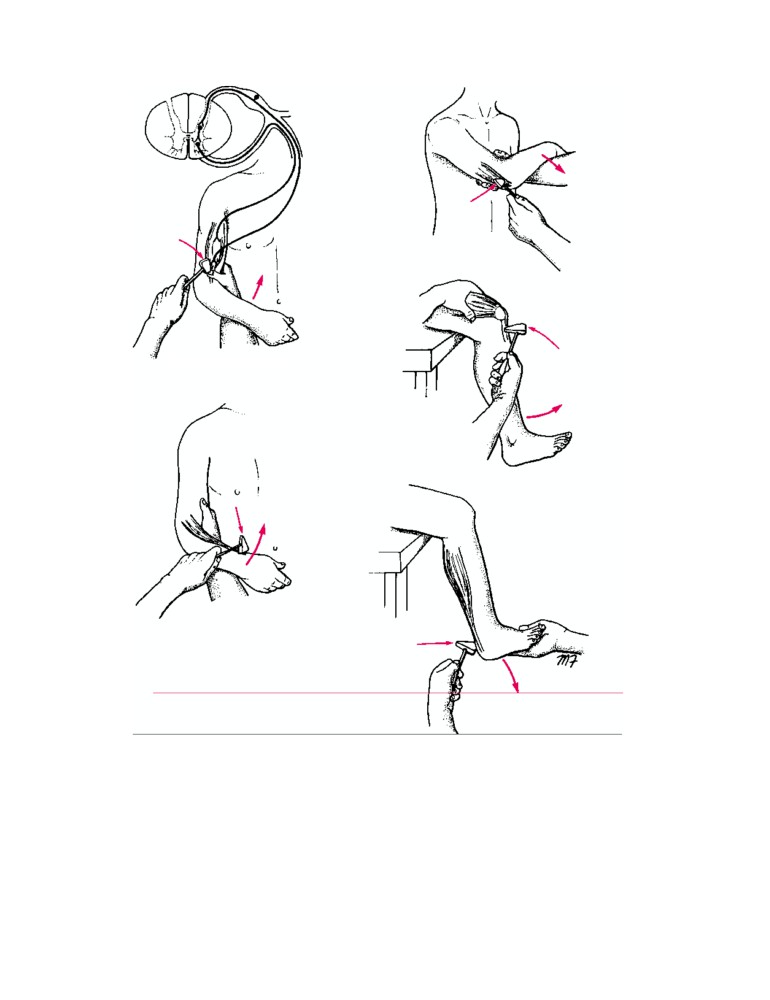
Learning the segmental innervation of all the muscles
LYMPHATIC
of the body is an impossible task. Nevertheless, the segmen-
tal innervation of the following muscles should be known
because they can be tested by eliciting simple muscle
SYSTEM
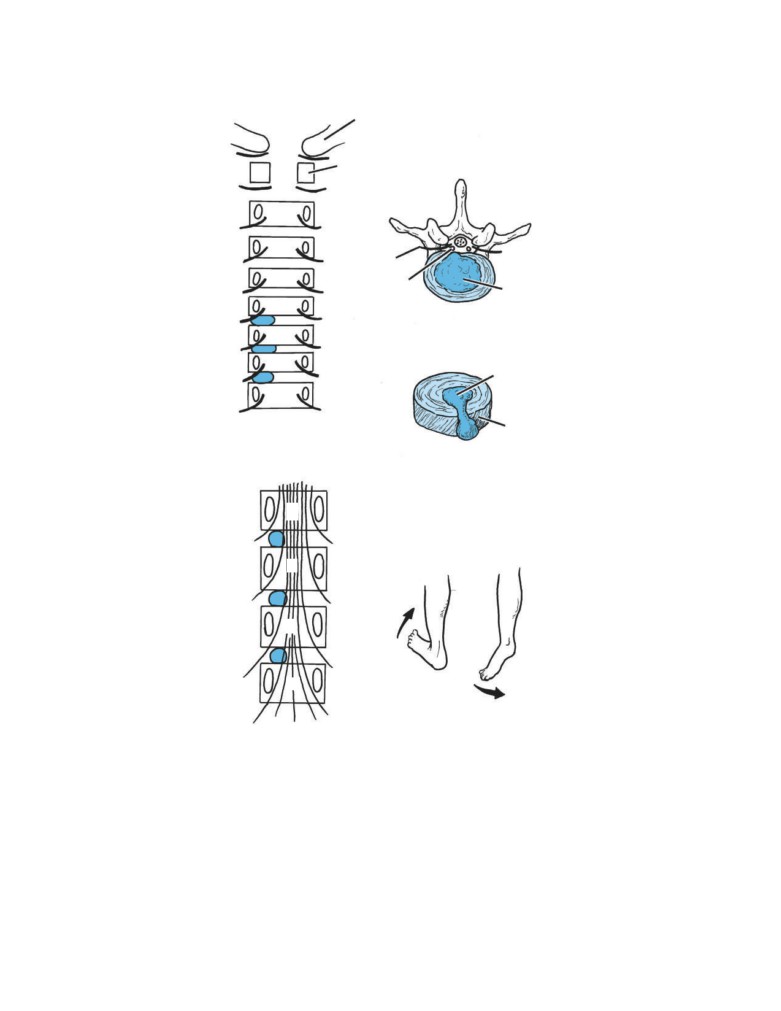
reflexes in the patient (CD Fig. 1-4):
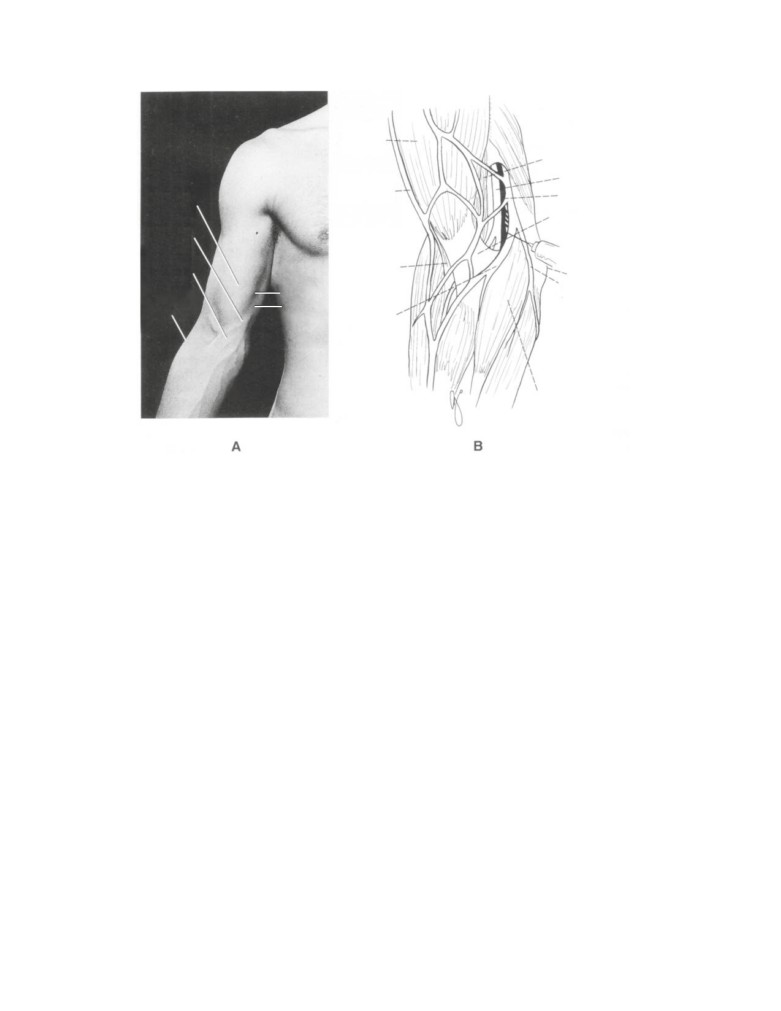
■ Biceps brachii tendon reflex: C5 and 6 (flexion of the
Diseases of the Lymphatic System
elbow joint by tapping the biceps tendon)
The lymphatic system is often de-emphasized by anatomists
■ Triceps tendon reflex: C6, 7, and 8 (extension of the
on the grounds that it is difficult to see on a cadaver. However,
elbow joint by tapping the triceps tendon)
it is of vital importance to medical personnel, since lymph
■ Brachioradialis tendon reflex: C5, 6, and 7 (supination
nodes may swell as the result of infection, metastases, or pri-
of the radioulnar joints by tapping the insertion of the
mary tumor. For this reason, the lymphatic drainage of all ma-
brachioradialis tendon)
jor organs of the body, including the skin, should be known.
■ Abdominal superficial reflexes (contraction of underly-
A patient may complain of a swelling produced by the
ing abdominal muscles by stroking the skin): Upper
enlargement of a lymph node. A physician must know the
abdominal skin T6-7, middle abdominal skin T8-9, and
areas of the body that drain lymph to a particular node if he
lower abdominal skin T10-12
or she is to be able to find the primary site of the disease. Of-
■ Patellar tendon reflex (knee jerk): L2, 3, and 4 (exten-
ten the patient ignores the primary disease, which may be a
sion of the knee joint on tapping the patellar tendon)
small, painless cancer of the skin.
■ Achilles tendon reflex (ankle jerk): S1 and S2 (plantar
Conversely, the patient may complain of a painful ulcer
flexion of the ankle joint on tapping the Achilles
of the tongue, for example, and the physician must know the
tendon)
lymph drainage of the tongue to be able to determine whether
the disease has spread beyond the limits of the tongue.
Clinical Modification of the
Activities of the Autonomic
NERVOUS SYSTEM
Nervous System
Many drugs and surgical procedures that can modify the
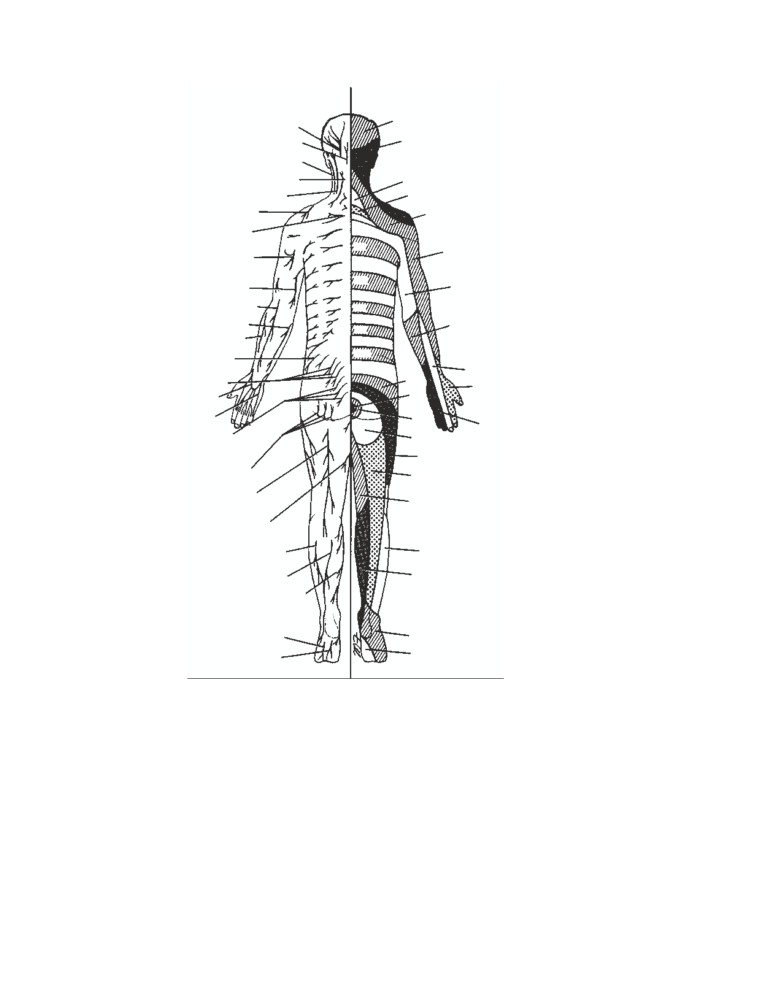
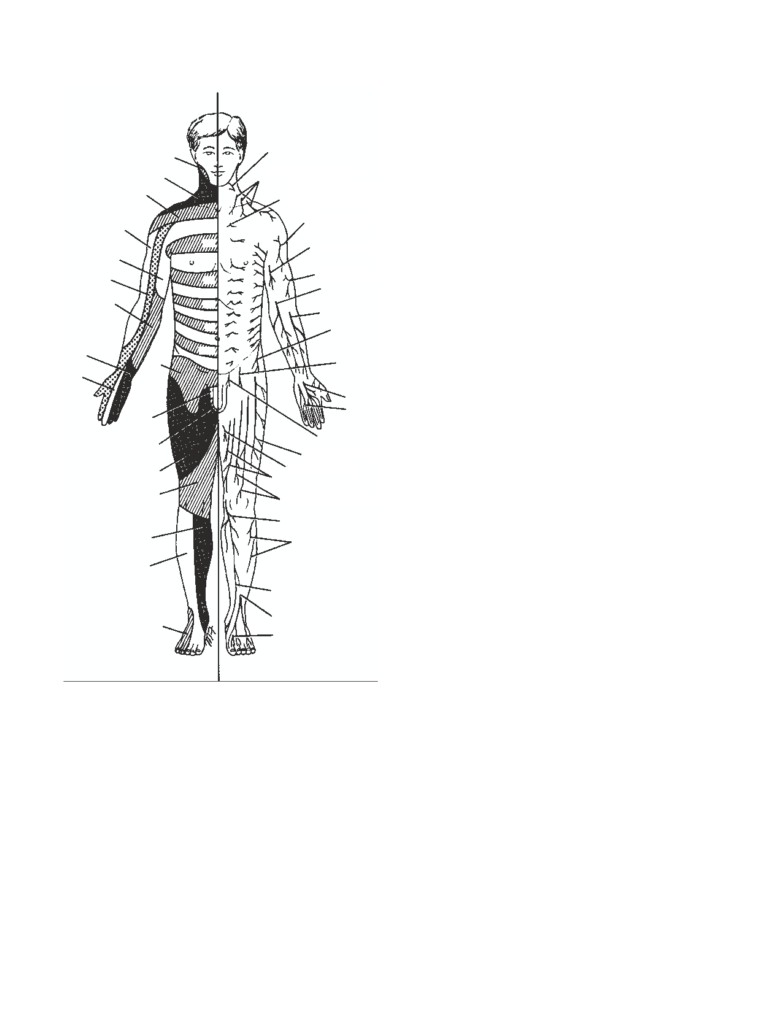
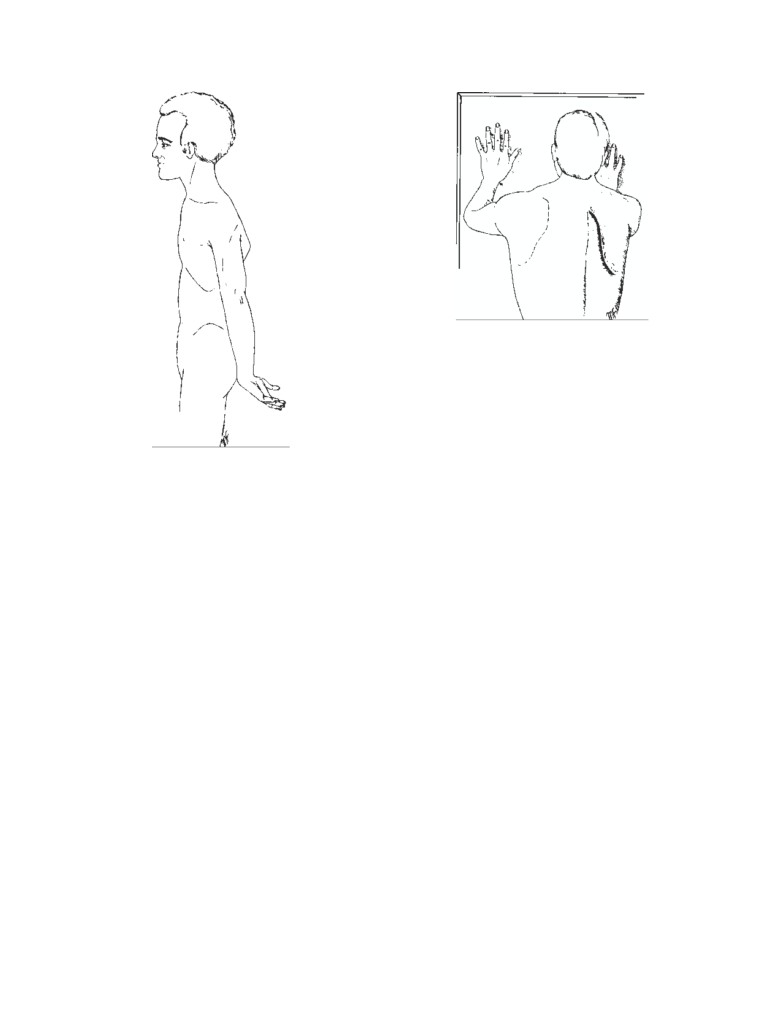
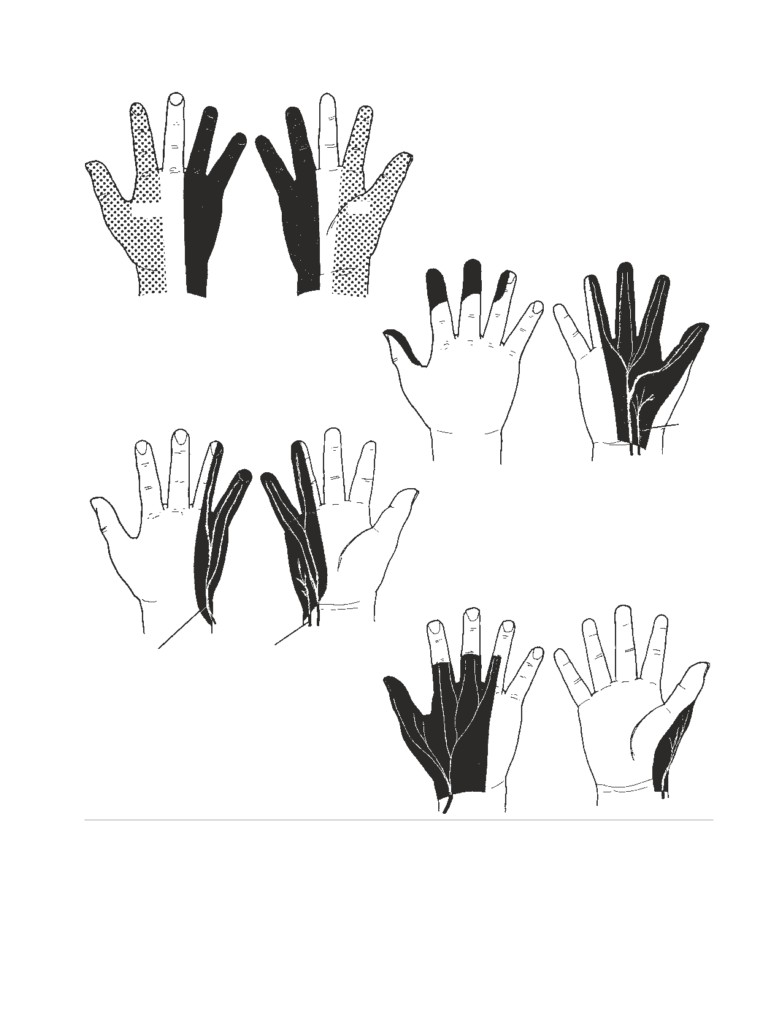
Segmental Innervation of the Skin
activity of the autonomic nervous system are available. For
example, drugs can be administered to lower the blood
The area of skin supplied by a single spinal nerve, and
pressure by blocking sympathetic nerve endings and causing
therefore a single segment of the spinal cord, is called a
vasodilatation of peripheral blood vessels. In patients with
dermatome. On the trunk, adjacent dermatomes overlap
severe arterial disease affecting the main arteries of the lower
considerably; to produce a region of complete anesthesia, at
limb, the limb can sometimes be saved by sectioning the
least three contiguous spinal nerves must be sectioned. Der-
sympathetic innervation to the blood vessels. This produces
matomal charts for the anterior and posterior surfaces of the
a vasodilatation and enables an adequate amount of blood to
body are shown in CD Figs. 1-2 and 1-3.
flow through the collateral circulation, thus bypassing the
In the limbs, arrangement of the dermatomes is more
obstruction.
complicated because of the embryologic changes that take
place as the limbs grow out from the body wall.
A physician should have a working knowledge of the
segmental (dermatomal) innervation of skin, because with
MUCOUS AND
the help of a pin or a piece of cotton he or she can determine
whether the sensory function of a particular spinal nerve or
SEROUS
segment of the spinal cord is functioning normally.
MEMBRANES
Segmental Innervation of Muscle
Skeletal muscle also receives a segmental innervation. Most
Mucous and Serous Membranes
of these muscles are innervated by two, three, or four spinal
nerves and therefore by the same number of segments of the
and Inflammatory Disease
spinal cord. To paralyze a muscle completely, it is thus nec-
essary to section several spinal nerves or to destroy several
Mucous and serous membranes are common sites for in-
segments of the spinal cord.
flammatory disease. For example, rhinitis, or the common
6
Chapter 1
transverse cutaneous nerve of neck
C2
supraclavicular nerves
C3
anterior cutaneous branch of second
C4
intercostal nerve
upper lateral cutaneous nerve of arm
C5
T3
medial cutaneous nerve of arm
T2
T4
lower lateral cutaneous nerve of arm
C6
T5
medial cutaneous nerve of forearm
T6
T1
T7
T8
lateral cutaneous nerve of forearm
T9
lateral cutaneous branch of
T10
subcostal nerve
C8
T11
T12
femoral branch of genitofemoral
L1
C7
nerve
median nerve
ulnar nerve
S3
ilioinguinal nerve
S4
lateral cutaneous nerve of thigh
obturator nerve
L2
medial cutaneous nerve of thigh
L3
intermediate cutaneous nerve of thigh
infrapatellar branch of saphenous nerve
L4
lateral sural cutaneous nerve
L5
saphenous nerve
superficial peroneal nerve
S1
deep peroneal nerve
CD Figure 1-2
Dermatomes and dis-
tribution of cutaneous nerves on the
anterior aspect of the body.
cold, is an inflammation of the nasal mucous membrane,
rections taken by the bony fragments depend not only on
and pleurisy is an inflammation of the visceral and parietal
the mechanism of injury, but also on the pull of the mus-
layers of the pleura.
cles attached to the fragments. Ligamentous attachments
also influence the deformity. In certain situations—for
example, the ileum—fractures result in no deformity be-
cause the inner and outer surfaces of the bone are splinted
BONES
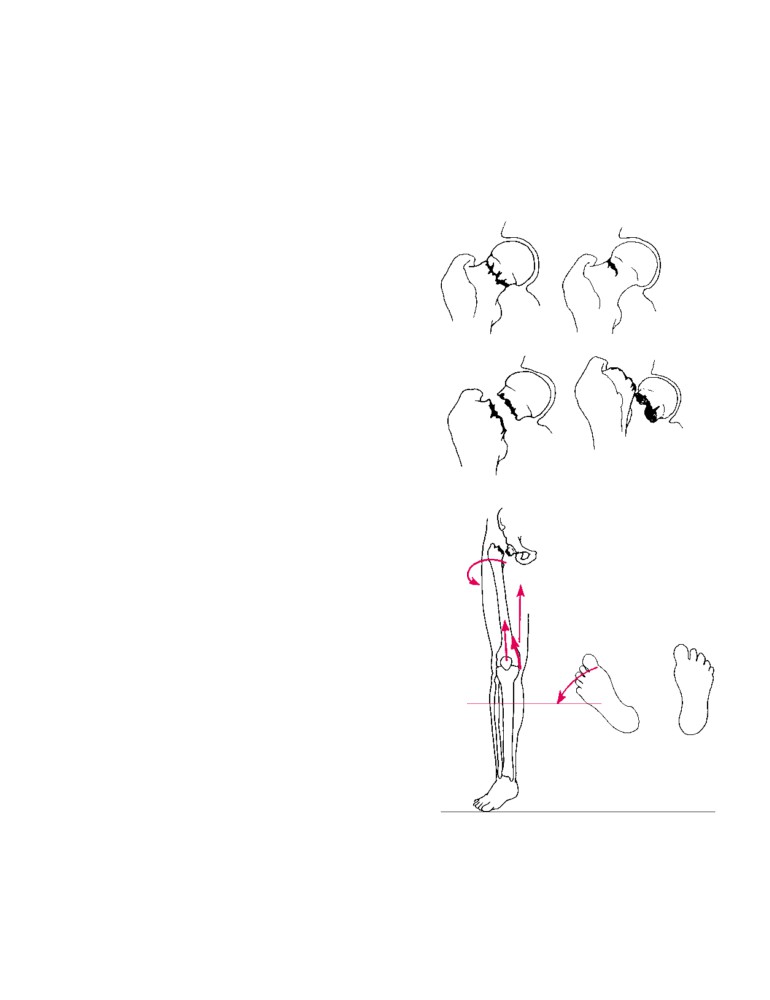
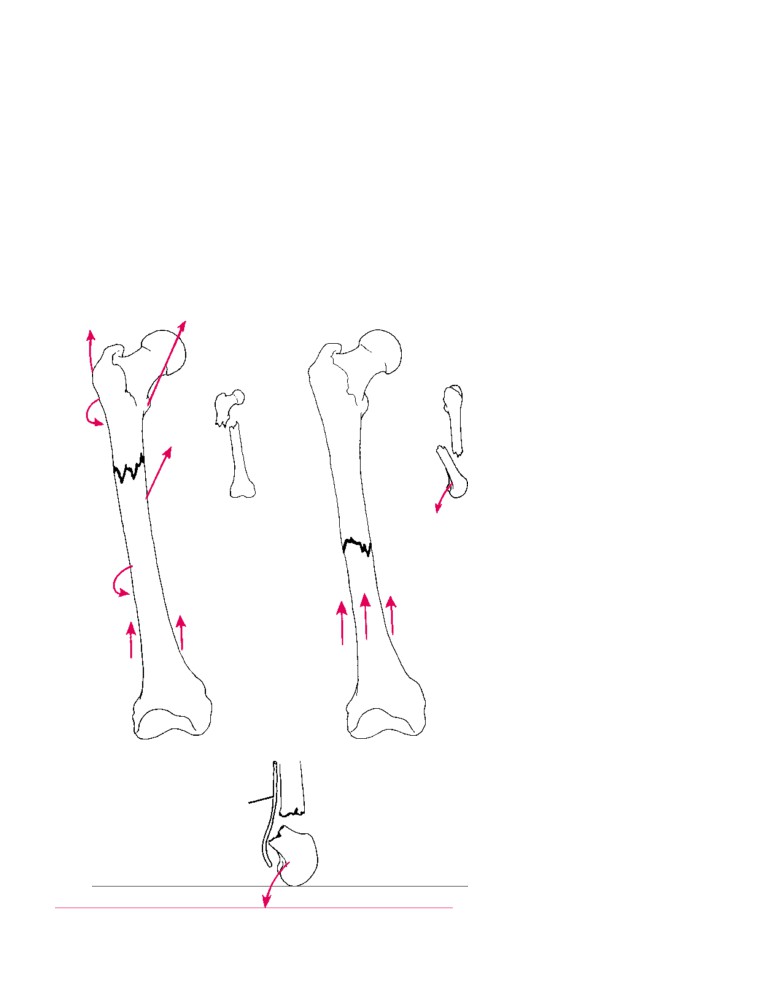
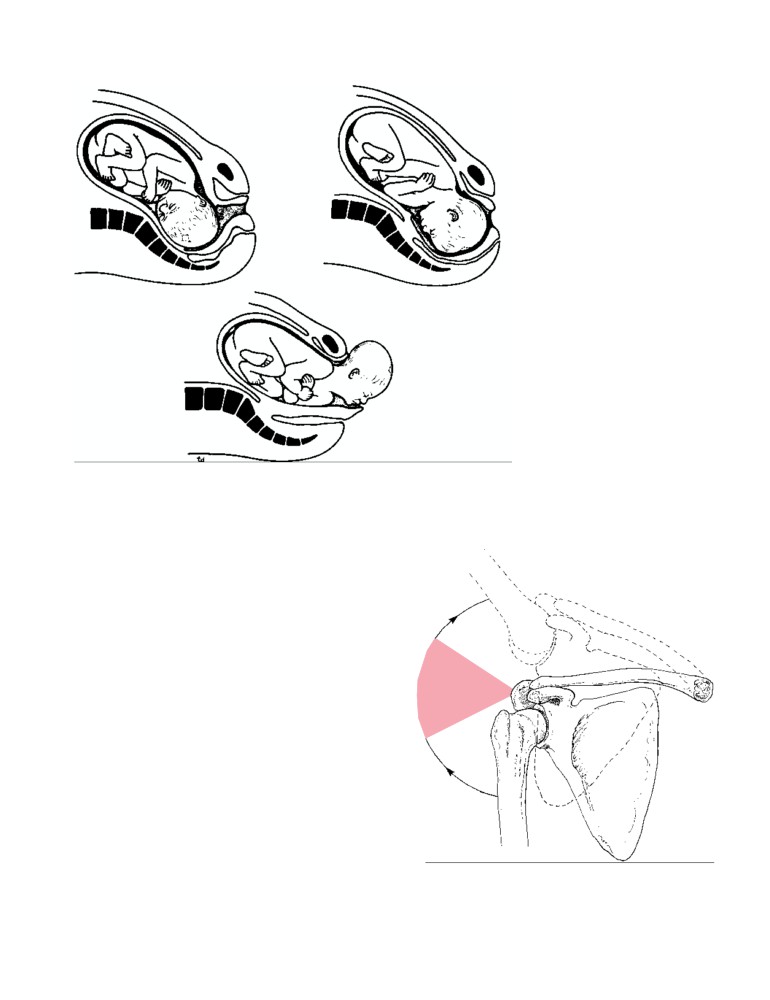
by the extensive origins of muscles. In contrast, a fracture
of the neck of the femur produces considerable displace-
ment. The strong muscles of the thigh pull the distal frag-
Bone Fractures
ment upward so that the leg is shortened. The very strong
Immediately after a fracture, the patient suffers severe lo-
lateral rotators rotate the distal fragment laterally so that
cal pain and is not able to use the injured part. Deformity
the foot points laterally.
may be visible if the bone fragments have been displaced
Fracture of a bone is accompanied by a considerable
relative to each other. The degree of deformity and the di-
hemorrhage of blood between the bone ends and into the
Introduction to Clinical Anatomy
7
C2
greater occipital nerve
third cervical nerve
C3
great auricular nerve
fourth cervical nerve
C5
lesser occipital nerve
C6
supraclavicular nerve
C4
first thoracic nerve
T2
T3
C5
posterior cutaneous nerve of arm
T4
T5
medial cutaneous nerve of arm
T2
T6
posterior cutaneous nerve of forearm
T7
T8
medial cutaneous nerve of forearm
T9
T1
lateral cutaneous nerve of forearm
T10
T11
lateral cutaneous branch of T12
T12
C7
posterior cutaneous branches of
L1
C6
L1, 2, and 3
S5
radial nerve
ulnar nerve
S4
C8
posterior cutaneous branches of
S3
S1, 2, and 3
L2
branches of posterior cutaneous
S2
nerve of thigh
posterior cutaneous nerve of thigh
L3
obturator nerve
lateral cutaneous nerve
L5
of calf
sural nerve
L4
saphenous nerve
lateral plantar nerve
S1
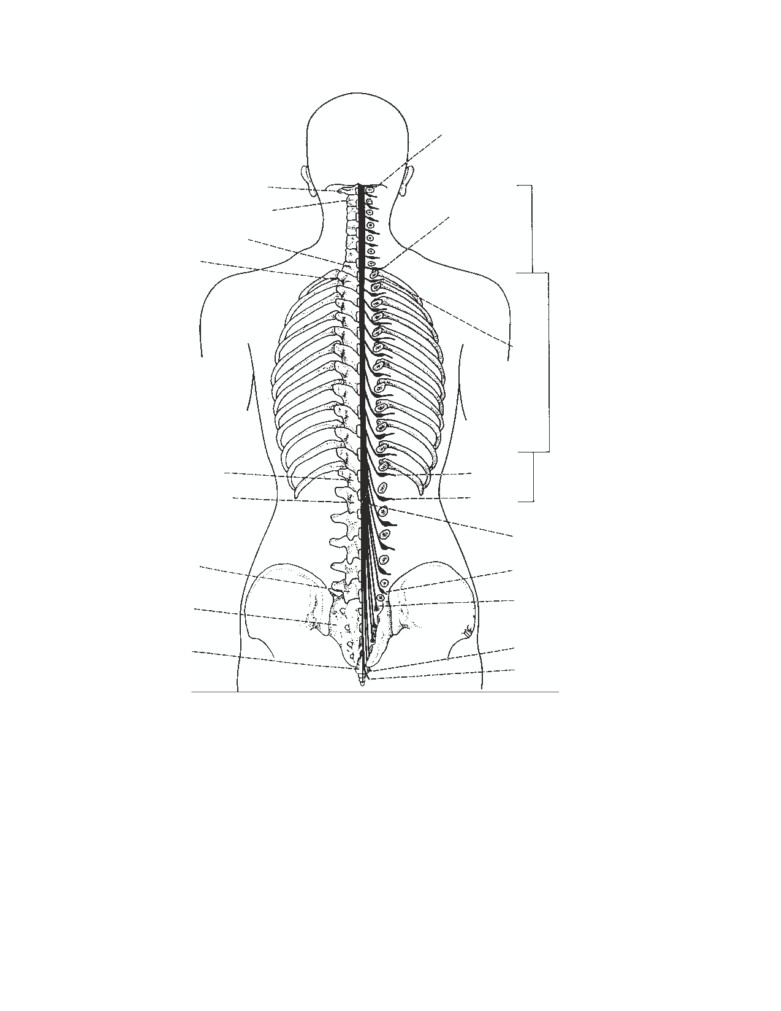
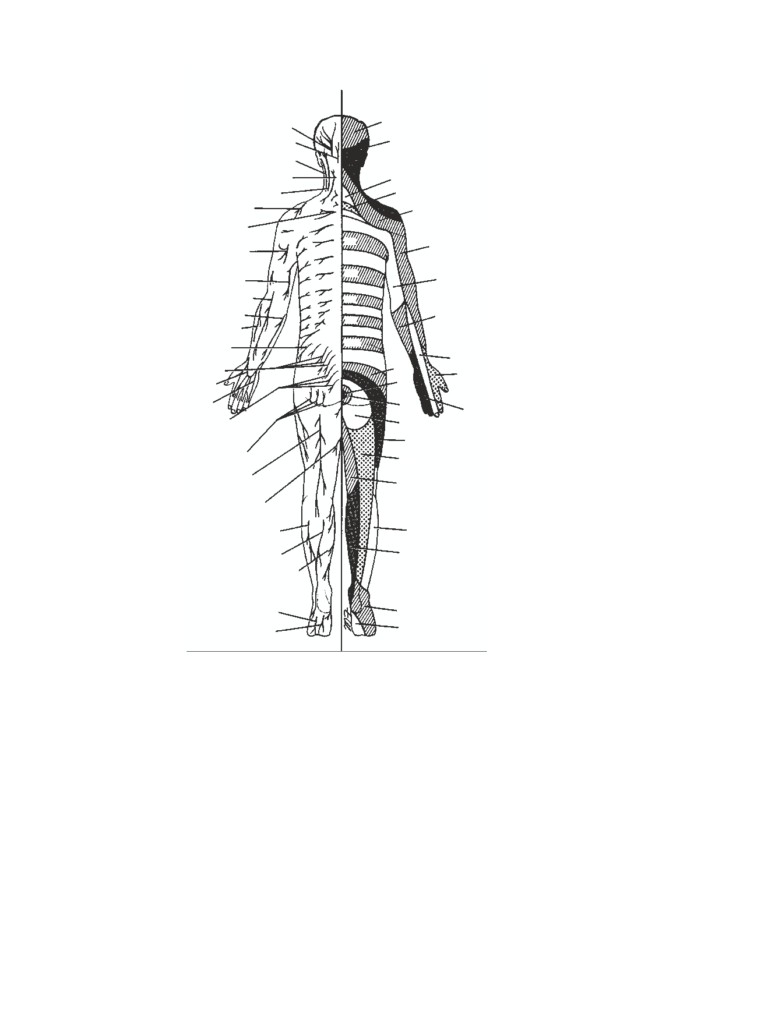
CD Figure 1-3
Dermatomes and distri-
L5
medial plantar nerve
bution of cutaneous nerves on the pos-
terior aspect of the body.
surrounding soft tissue. The blood vessels and the fibroblasts
bossing of the frontal bones of the skull. Deformities of the
and osteoblasts from the periosteum and endosteum take
pelvis may also occur.
part in the repair process.
Epiphyseal Plate Disorders
Rickets
Epiphyseal plate disorders affect only children and adoles-
Rickets is a defective mineralization of the cartilage matrix
cents. The epiphyseal plate is the part of a growing bone con-
in growing bones. This produces a condition in which the
cerned primarily with growth in length. Trauma, infection,
cartilage cells continue to grow, resulting in excess cartilage
diet, exercise, and endocrine disorders can disturb the growth
and a widening of the epiphyseal plates. The poorly miner-
of the hyaline cartilaginous plate, leading to deformity and loss
alized cartilaginous matrix and the osteoid matrix are soft,
of function. In the femur, for example, the proximal epiphysis
and they bend under the stress of bearing weight. The
can slip because of mechanical stress or excessive loads. The
resulting deformities include enlarged costochondral junc-
length of the limbs can increase excessively because of in-
tions, bowing of the long bones of the lower limbs, and
creased vascularity in the region of the epiphyseal plate sec-
8
Chapter 1
C6, 7, and 8
C5 and 6
triceps tendon reflex
biceps brachii tendon reflex
L2, 3, and 4
patellar tendon reflex
C5, 6, and 7
brachioradialis
S1 and 2
tendon
reflex
Achilles tendon reflex
CD Figure 1-4
Some important tendon reflexes used in medical practice.
Introduction to Clinical Anatomy
9
ondary to infection or in the presence of tumors. Shortening
2. The liver is relatively much larger in the child than in
of a limb can follow trauma to the epiphyseal plate resulting
the adult. In the infant, the lower margin of the liver ex-
from a diminished blood supply to the cartilage.
tends inferiorly to a lower level than in the adult. This
is an important consideration when making a diagnosis
of hepatic enlargement.
CLINICAL
3. The urinary bladder in the child cannot be accommo-
dated entirely in the pelvis because of the small size of
SIGNIFICANCE OF
the pelvic cavity and thus is found in the lower part of
the abdominal cavity. As the child grows, the pelvis en-
SEX, RACE, AND
larges and the bladder sinks down to become a true
pelvic organ.
AGE ON STRUCTURE
4. At birth, all bone marrow is of the red variety. With
advancing age, the red marrow recedes up the
The fact that the structure and function of the human body
bones of the limbs so that in the adult it is largely
change with age may seem obvious, but it is often over-
confined to the bones of the head, thorax, and
looked; a child is just not a small adult. A few examples of
abdomen.
such changes are given here:
1. In the infant, the bones of the skull are more resilient
5. Lymphatic tissues reach their maximum degree of de-
than in the adult, and for this reason fractures of the
velopment at puberty and thereafter atrophy, so the vol-
skull are much more common in the adult than in the
ume of lymphatic tissue in older persons is considerably
young child.
reduced.
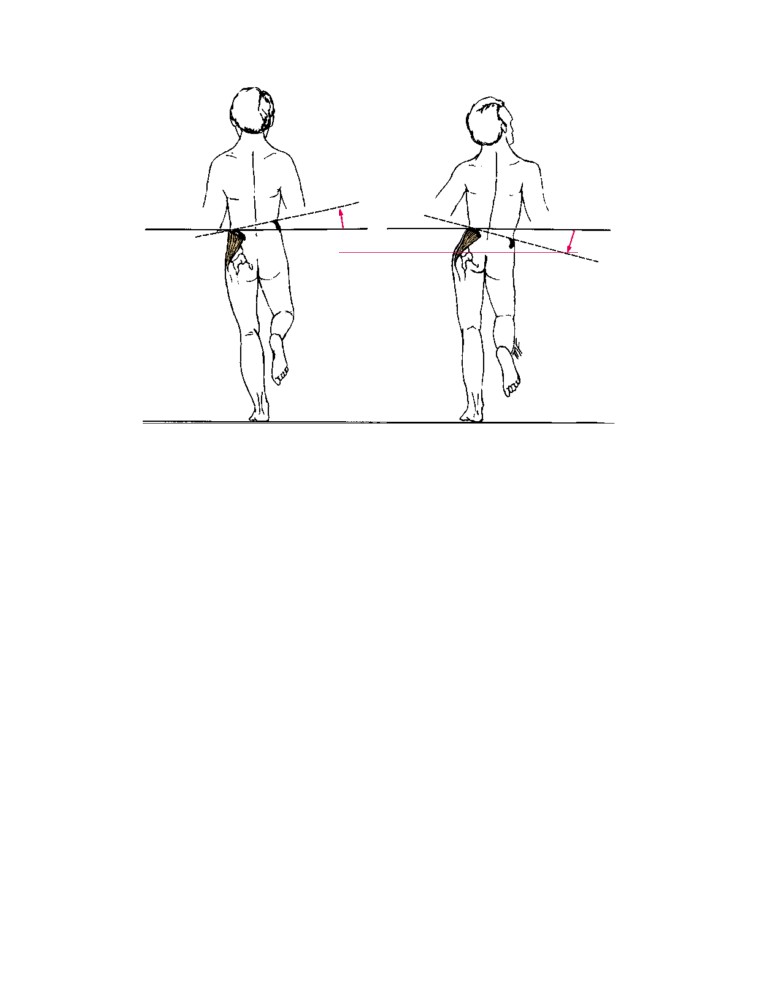
Clinical Problem Solving Questions
Read the following case histories/questions and give
examination, she has severe right lateral flexion defor-
the best answer for each.
mity of the vertebral column.
2. The following statement is correct about this case:
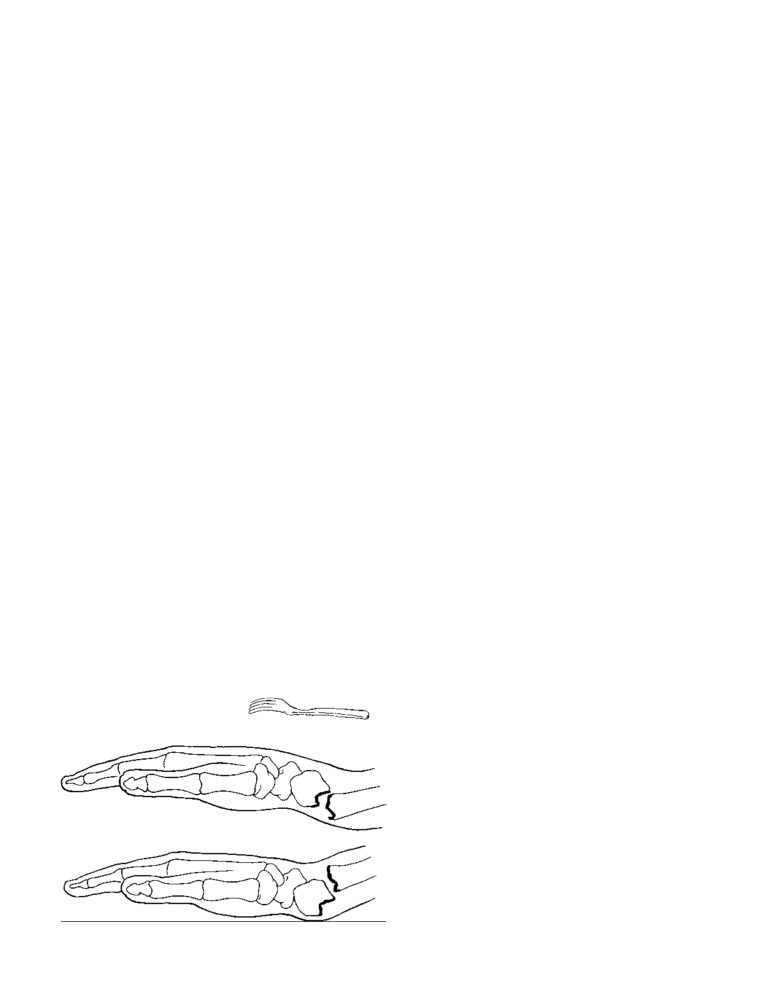
A 45-year-old patient has a small, firm, mobile tumor
A. The virus of poliomyelitis attacks and always destroys
on the dorsum of the right foot just proximal to
the motor anterior horn cells of the spinal cord.
the base of the big toe and superficial to the bones and
B. The disease resulted in the paralysis of the muscles
the long extensor tendon but deep to the superficial
that normally laterally flex the vertebral column on
fascia. The patient has a neurofibroma of a digital
the left side.
nerve.
C. The muscles on the right side of the vertebral col-
1. The following information concerning the tumor is
umn are hyperactive.
correct:
D. The right lateral flexion deformity is caused by the
A. It is situated on the lower surface of the foot close to
slow degeneration of the sensory nerve fibers origi-
the root of the big toe.
nating from the vertebral muscles on the right side.
B. It is attached to the first metatarsal bone.
C. On palpation, it moves more freely from medial to
A 20-year-old woman severely sprains her left ankle while
lateral than from proximal to distal.
playing tennis. When she tries to move the foot so that
D. It lies deep to the tendon of the extensor hallucis
the sole faces medially, she experiences severe pain.
longus muscle.
3. What is the correct anatomic term for the movement of
E. It is attached to the capsule of the metatarsopha-
the foot that produces the pain?
langeal joint of the big toe.
A. Pronation
A 31-year-old woman has a history of poliomyelitis af-
B. Inversion
fecting the anterior horn cells of the lower thoracic and
C. Supination
lumbar segments of the spinal cord on the left side. On
D. Eversion
10
Chapter 1
A 25-year-old man has a deep-seated abscess in the pos-
A woman recently took up employment in a factory.
terior part of the neck.
She is a machinist, and for 6 hours a day she has to
move a lever repeatedly, which requires that she extend
4.
The following statement is correct concerning the
and flex her right wrist joint. At the end of the second
abscess:
week of her employment, she began to experience pain
A. The abscess probably lies superficial to the deep
over the posterior surface of her wrist and noticed a
fascia.
swelling in the area.
B. The deep fascia does not determine the direction of
spread of the abscess.
8.
The following statements concerning this patient are
C. The abscess would be incised through a vertical skin
correct except which?
incision.
A. Extension of the wrist joint is brought about by
D. The lines of cleavage are not important when
several muscles that include the extensor digitorum
considering the direction of skin incisions.
muscle.
E. The abscess would be incised, if possible, through a
B. The wrist joint is diseased.
horizontal skin incision.
C. Repeated unaccustomed movements of tendons
through their synovial sheaths can produce trau-
A 40-year-old workman received a severe burn on
matic inflammation of the sheaths.
the anterior aspect of his right forearm. The area of the
D. The diagnosis is traumatic tenosynovitis of the long
burn exceeded 4 in.2 (10 cm2). The greater part of
tendons of the extensor digitorum muscle.
the burn was superficial and extended only into the
superficial part of the dermis.
A 19-year-old boy was suspected of having leukemia. It
was decided to confirm the diagnosis by performing a
5.
In the superficially burned area, the epidermis cells
bone marrow biopsy.
would regenerate from the following sites except which?
A. The hair follicles
9.
The following statements concerning this procedure
B. The sebaceous glands
are correct except which?
C. The margins of the burn
A. The biopsy was taken from the lower end of the
D. The deepest ends of the sweat glands
tibia.
6.
In a small area the burn penetrated as far as the superfi-
B. Red bone marrow specimens can be obtained from
cial fascia; in this region, the epidermal cells would
the sternum or the iliac crests.
regenerate from the following sites except which?
C. At birth, the marrow of all bones of the body is red
A. The ends of the sweat glands that lie in the superfi-
and hematopoietic.
cial fascia
D. The blood-forming activity of bone marrow in
B. The margins of the burn
many long bones gradually lessens with age, and
C. The sebaceous glands
the red marrow is gradually replaced by yellow
marrow.
In a 63-year-old man, a magnetic resonance imaging
scan of the lower thoracic region of the vertebral col-
A 22-year-old woman had a severe infection under the
umn reveals the presence of a tumor pressing on the
lateral edge of the nail of her right index finger. On ex-
lumbar segments of the spinal cord. He has a loss of
amination, a series of red lines were seen to extend up
sensation in the skin over the anterior surface of the left
the back of the hand and around to the front of the fore-
thigh and is unable to extend his left knee joint. Exam-
arm and arm, up to the armpit.
ination reveals that the muscles of the front of the left
10.
The following statements concerning this patient are
thigh have atrophied and have no tone and that the
probably correct except which?
left knee jerk is absent.
A. Palpation of the right armpit revealed the presence
7.
The following statements concerning this patient are
of several tender enlarged lymph nodes
(lym-
correct except which?
phadenitis).
A. The tumor is interrupting the normal function of the
B. The red lines were caused by the superficial lym-
efferent motor fibers of the spinal cord on the left side.
phatic vessels in the arm, which were red and in-
B. The quadriceps femoris muscles on the front of the
flamed (lymphangitis) and could be seen through
left thigh are atrophied.
the skin.
C. The loss of skin sensation is confined to the der-
C. Lymph from the right arm entered the bloodstream
matomes L1, 2, 3, and 4.
through the thoracic duct.
D. The absence of the left knee jerk is because of
D. Infected lymph entered the lymphatic capillaries
involvement of the first lumbar spinal segment.
from the tissue spaces.
Introduction to Clinical Anatomy
11
Answers and Explanations
1.
C is the correct answer. The tumor is a neurofibroma of
neck plays an important role in the direction of spread
a small digital nerve. This fact explains why the tumor
of a deep-seated abscess. C. The abscess would only be
is relatively superficial and moves with the digital nerve
incised through a vertical incision if a horizontal inci-
more freely from medial to lateral than from proximal
sion along a line of cleavage was not possible. A vertical
to distal. A. The tumor is situated on the dorsum or up-
incision in the neck would result in an unsightly scar.
per surface of the foot. B. The tumor is mobile and not
D. The lines of cleavage (see CD Fig. 1-1) are very im-
attached to the first metatarsal bone. D. The tumor lies
portant when considering the direction of skin inci-
superficial to the tendon of the extensor hallucis longus
sions. However, cosmetic concerns have to take second
muscle. E. The tumor is mobile and is not attached to
place in life-threatening situations.
the capsule of the metatarsophalangeal joint.
5.
D is the correct answer. In a superficial burn, the epi-
2.
B is the correct answer. The disease infected the ante-
dermal cells would regenerate from the hair follicles,
rior horn cells, whose axons supply the muscles that
the sebaceous glands, and the margins of the burn.
normally laterally flex the vertebral column on the left
6.
C is the correct answer. The sebaceous glands are lo-
side. A. The virus of poliomyelitis attacks anterior horn
cated superficially (see text Fig. 1-4) and are destroyed
cells in the spinal cord. The result may be death of the
in deep burns.
cells and muscle paralysis or, depending on the severity
of the attack, the nerve cells may recover and the mus-
7.
D is the correct answer. The patellar tendon reflex (knee
cle paralysis may also recover. C. The muscles on the
jerk) involves L2, 3, and 4 segments of the spinal cord.
right side of the vertebral column are contracting nor-
mally against the paralyzed left-sided vertebral muscles.
8.
B is the correct answer. The wrist joint is not diseased
D. The sensory nerves of muscles are unaffected by the
in this patient. The swelling on the posterior surface of
polio virus.
the wrist region was caused by the excessive production
of fluid in the synovial sheaths of the extensor tendons
3.
B is the correct answer. The movement of the foot so
secondary to repeated and excessive extensor move-
that the sole comes to face medially is called inversion
ments, a condition called traumatic tenosynovitis.
(see text Fig. 1-3). For a full discussion of the move-
ments of inversion and eversion of the foot at the subta-
9.
A is the correct answer. In a 19-year-old boy, the bone
lar and transverse joints of the foot, see text.
marrow at the lower end of the tibia is yellow. A biopsy
specimen of red marrow in an adult, who is suspected
4.
E is the correct answer. The abscess would be incised,
of suffering from leukemia, is easily obtained from the
if possible, through a horizontal skin incision along a
iliac crests or the sternum.
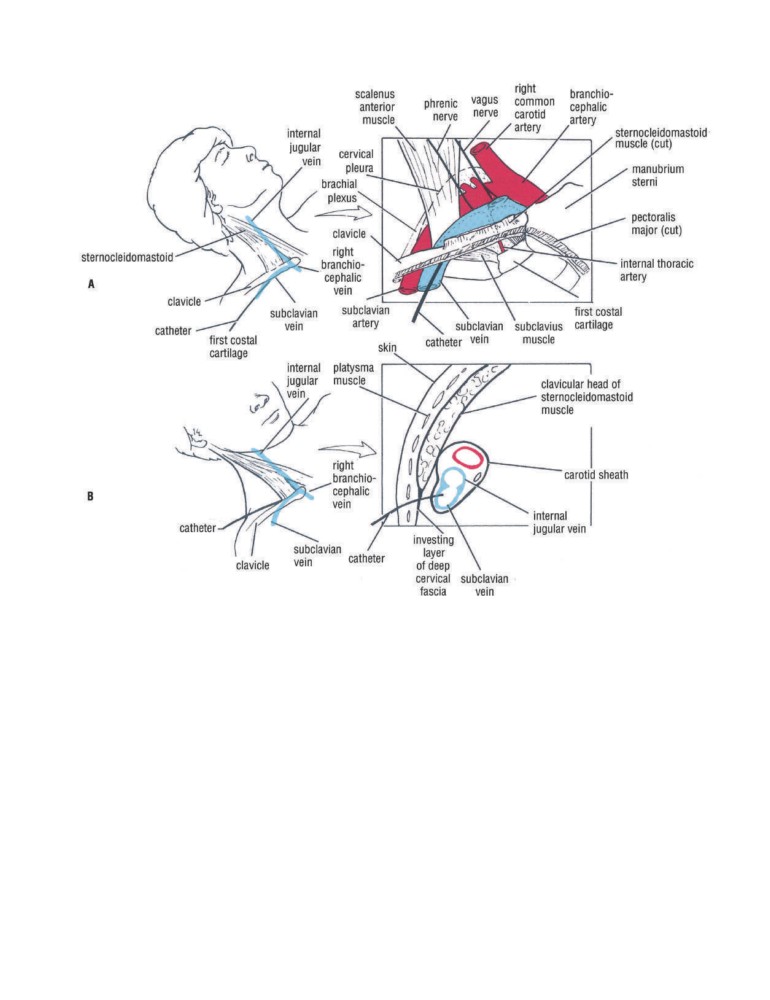
line of cleavage (see CD Fig. 1-1). A. A deep-seated
abscess in the neck usually lies deep to the superficial
10.
C is the correct answer. Lymph from the right upper
fascia and beneath the investing layer of deep cervical
limb enters the bloodstream through the right lym-
fascia. B. The arrangement of the deep fascia in the
phatic duct.
The Upper and Lower
Airway and Associated
Structures
2
Chapter Outline
The Nose
17
Parotid Duct and Facial Injuries
22
Pupillodilatation
17
Submandibular Gland: Calculus Formation
22
Examination of the Nasal Cavity
17
Sublingual Gland and Cyst Formation
22
Infection of the Nasal Cavity
17
The Pharynx
22
Nasal Obstruction
18
Killian’s Dehiscence and Foreign Bodies
22
Trauma to the Nose
18
The Piriform Fossa and Foreign Bodies
22
Nasal Fractures
18
The Process of Swallowing (Deglutition)
22
Skin Lacerations
18
Swallowing in Unconscious Individuals
22
Congenital Anomalies of the Nose
18
Pharyngeal Obstruction of the Upper Airway
22
Median Nasal Furrow
18
Loss of the Gag Reflex
22
Lateral Proboscis
18
Palatine Tonsils
23
The Paranasal Sinuses
18
Examination of the Tonsils
23
Sinusitis and the Examination of the
Tonsillitis
23
Paranasal Sinuses
18
Quinsy
23
The Mouth
19
Adenoids
23
Examination of the Mouth
19
The Larynx
23
Lips and Vestibule and Facial Paralysis
20
The Cricoid Cartilage and the Sellick Maneuver
23
Ranula
20
Relationship between Vocal Folds and
The Tongue
20
Cricothyroid Ligament
23
Laceration of the Tongue
20
Larynx in Children
23
Tongue and Airway Obstruction
20
Epiglottitis
23
Anatomy of Procedures
20
Pulling the Tongue Forward in Airway
Foreign Bodies in the Airway
23
Obstruction
20
Anatomic Rationale for Differences in Procedures for
Oral Endotracheal Intubation
20
Removing Foreign Bodies in Adults and Children
23
Oral Endotracheal Intubation and the
Lesions of the Laryngeal Nerves
24
Incisor Teeth
20
Oral Endotracheal Intubation and the
Inspection of the Vocal Cords (Folds) with the
Small Mandible
20
Laryngeal Mirror and Laryngoscope
25
The Palate
20
Important Anatomic Axes for Endotracheal
Intubation
26
Angioedema of the Uvula (Quincke’s Uvula)
20
Anatomy of the Visualization of the Vocal Cords
Congenital Anomalies of the Palate
21
with the Laryngoscope
27
Cleft Palate
21
Reflex Activity Secondary to Endotracheal
The Salivary Glands
21
Intubation
28
Parotid Salivary Gland and Lesions of the
The Trachea
28
Facial Nerve
21
Palpation of the Trachea
28
Parotid Gland Infections
21
The Upper and Lower Airway and Associated Structures
17
Compromised Airway
28
The Bronchi
32
Anatomy of Cricothyroidotomy
28
Aspiration of Foreign Bodies and Stomach Contents
32
Complications
29
Anatomy of Tracheostomy
29
Suction Catheters, Endotracheal Tubes, and the
Complications
31
Bronchi
32
Some Important Airway Distances
31
Bronchopulmonary Segments
32
Changes in the Tracheal Length with
Clinical Problem Solving Questions
32
Respiration and Position of the Head
and Neck
31
Answers and Explanations
33
Infection of the Nasal Cavity
THE NOSE
Infection of the nasal cavity can spread in a variety of
directions. The paranasal sinuses are especially prone to
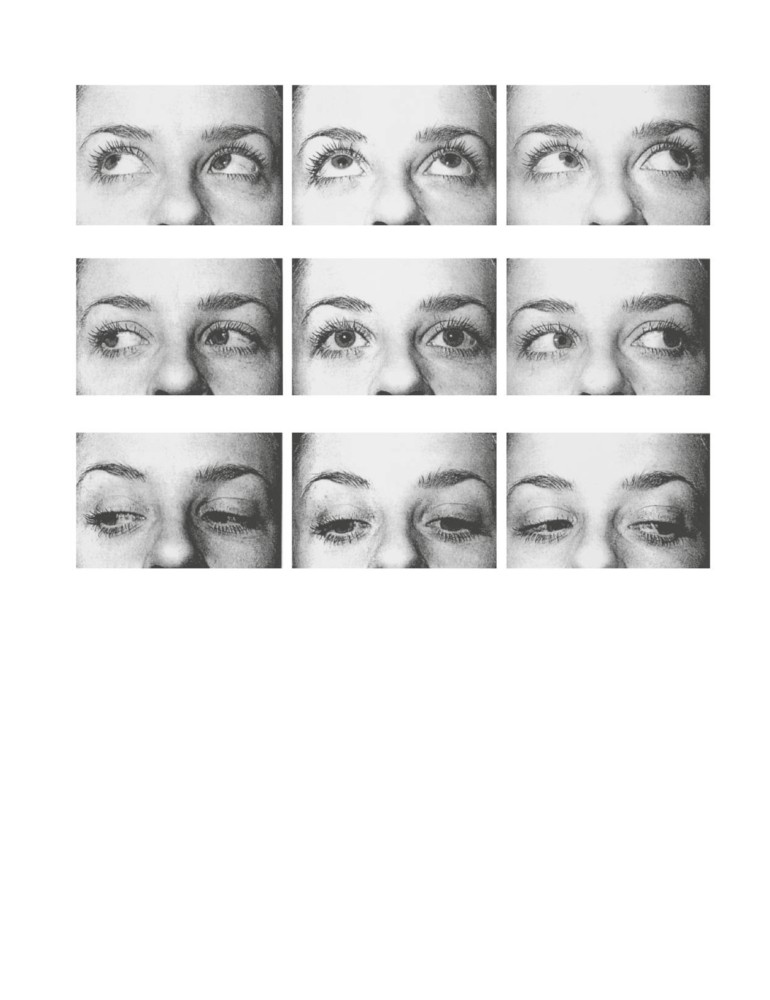
Pupillodilatation
infection. Organisms may spread via the nasal part of the
pharynx and the auditory tube to the middle ear. It is pos-
A vasoconstrictor sprayed into the nasal vestibule can ascend
sible for organisms to ascend to the meninges of the ante-
in the nasolacrimal duct to the conjunctival sac, where it is
rior cranial fossa, along the sheaths of the olfactory nerves
absorbed, and may produce pupillodilatation.
through the cribriform plate, and produce meningitis.
Epistaxis, or bleeding from the nose, is a frequent con-
dition. The most common cause is nose picking. The
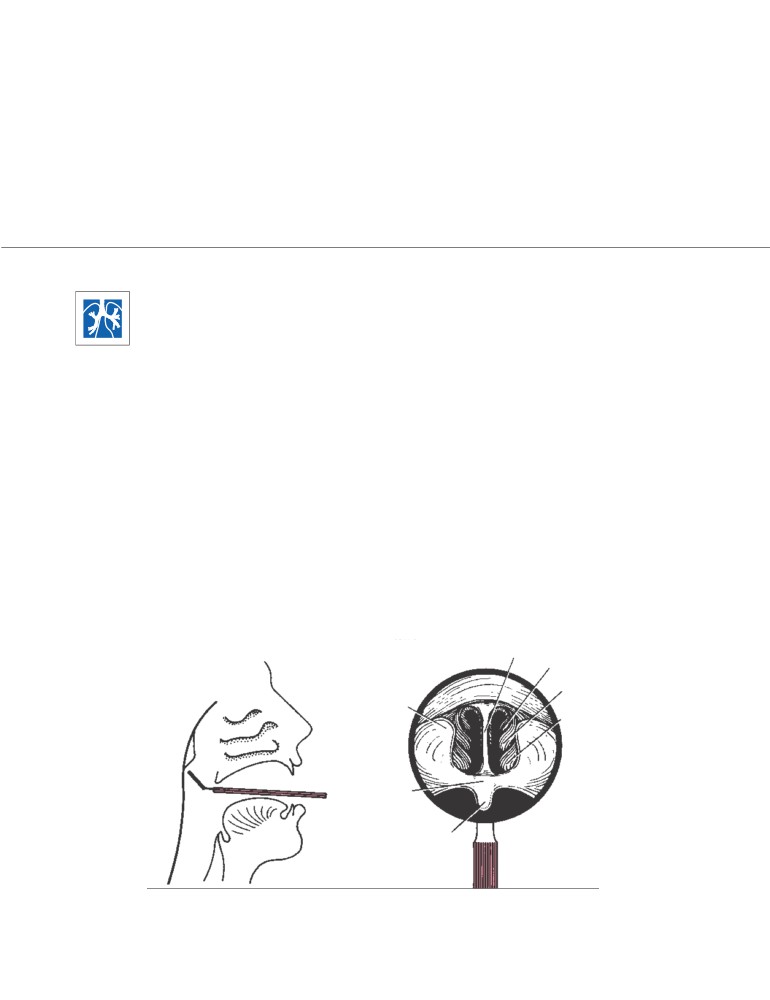
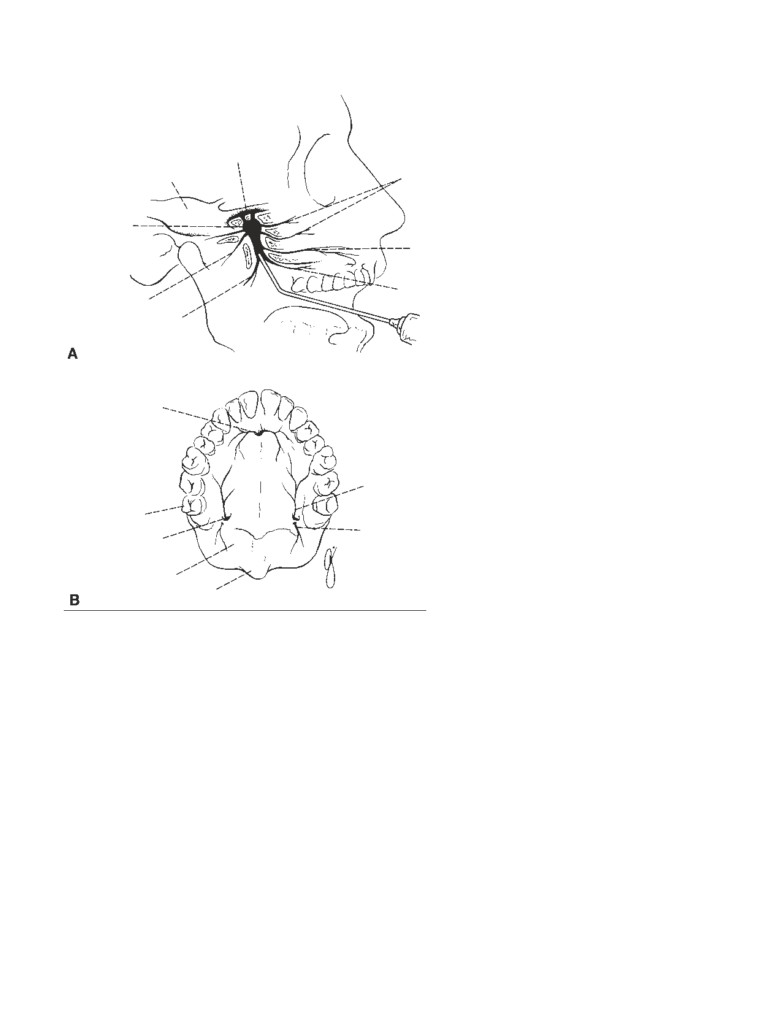
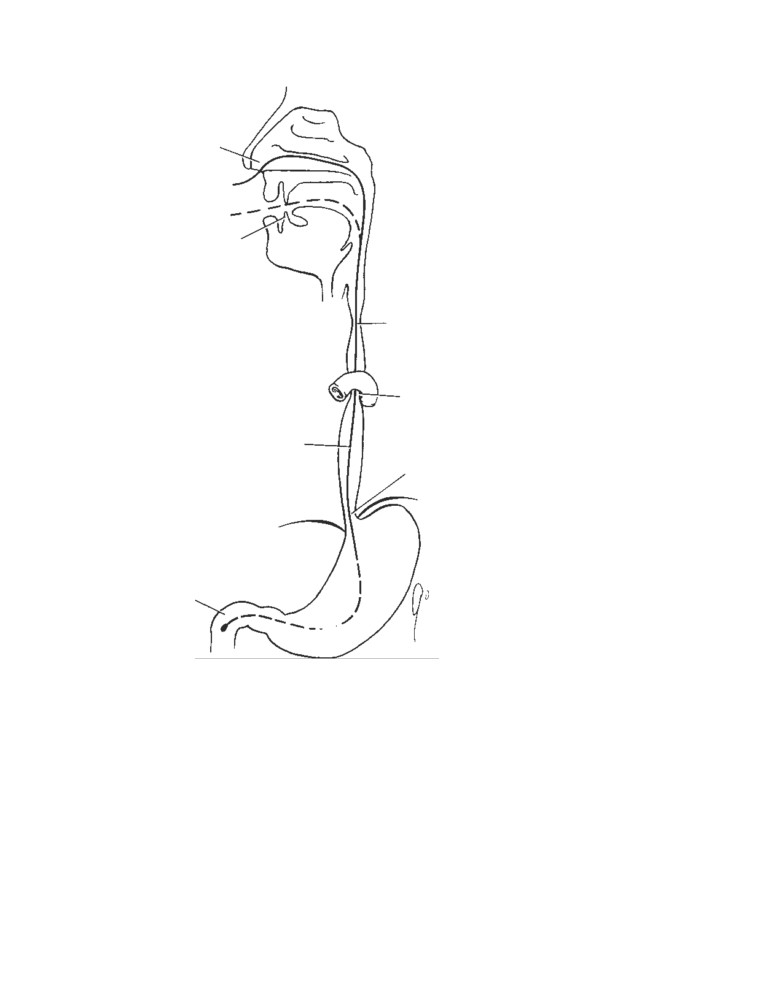
Examination of the Nasal Cavity
bleeding may be arterial or venous, and most episodes oc-
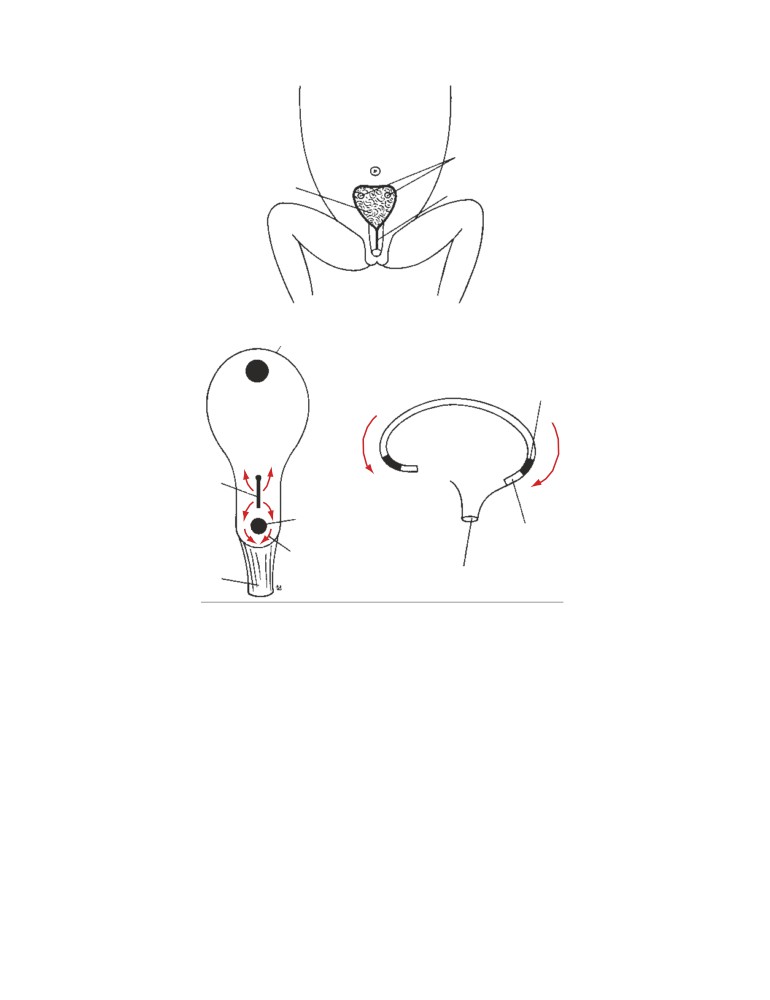
Examination of the nasal cavity may be carried out by insert-
cur on the anteroinferior portion of the septum and in-
ing a speculum through the external nares or by means of a
volve the septal branches of the sphenopalatine and facial
mirror in the pharynx. In the latter case, the choanae and the
vessels.
posterior border of the septum can be visualized (CD Fig. 2-
Beware of bilateral cauterization of the septal mucous
1). It should be remembered that the nasal septum is rarely
membrane. It could compromise the blood supply to the
situated in the midline. A severely deviated septum may
perichondrium and cause necrosis of the cartilaginous part
interfere with drainage of the nose and the paranasal sinuses.
of the septum.
nasal septum
superior concha
middle concha
tubal elevation
inferior concha
soft palate
uvula
A
B
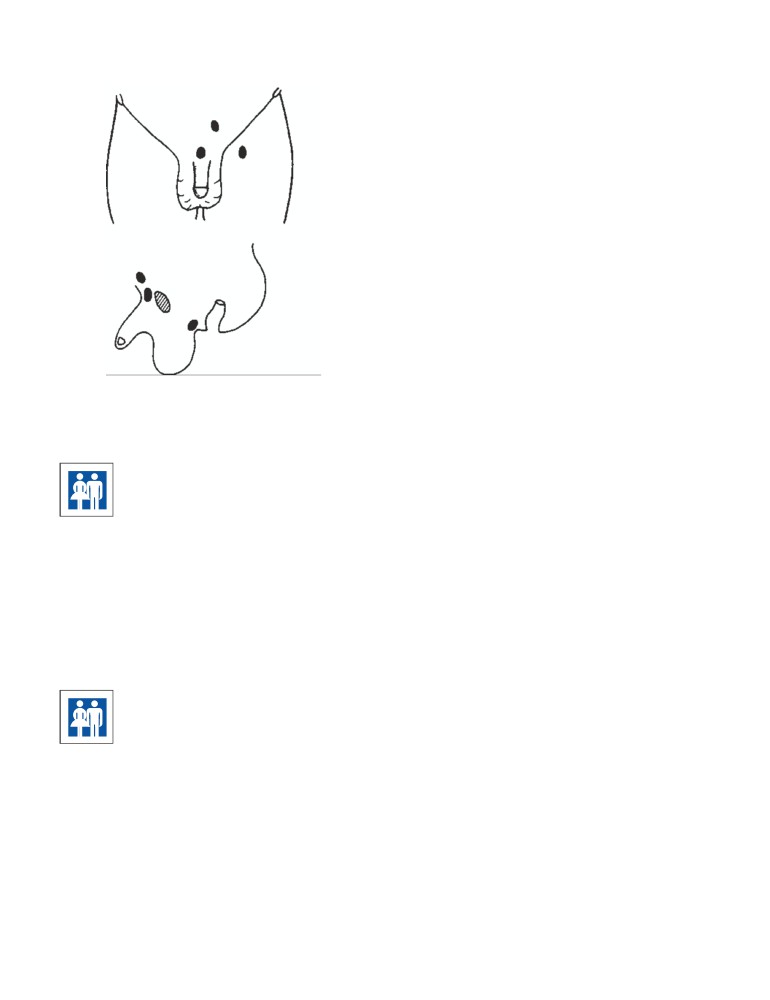
CD Figure 2-1
A. Position of the mirror in posterior rhinoscopy. B. Structures seen in
posterior rhinoscopy.
18
Chapter 2
lip, or across the lower eyelid, since future scars tend to con-
Nasal Obstruction
tract and distort the depression.
Nasal obstruction can be caused by edema of the mucous
membrane secondary to infection, or by foreign bodies
lodged between the conchae. The shelf-like conchae make
CONGENITAL
impaction and retention of balloons, peas, and small toys
relatively easy in children. Other causes include tumors,
ANOMALIES OF
polyps, and septal abscesses.
Deflection of the nasal septum is common. It is be-
THE NOSE
lieved to occur most commonly in males because of trauma
in childhood.
The most voluminous part of the nasal cavity is close to
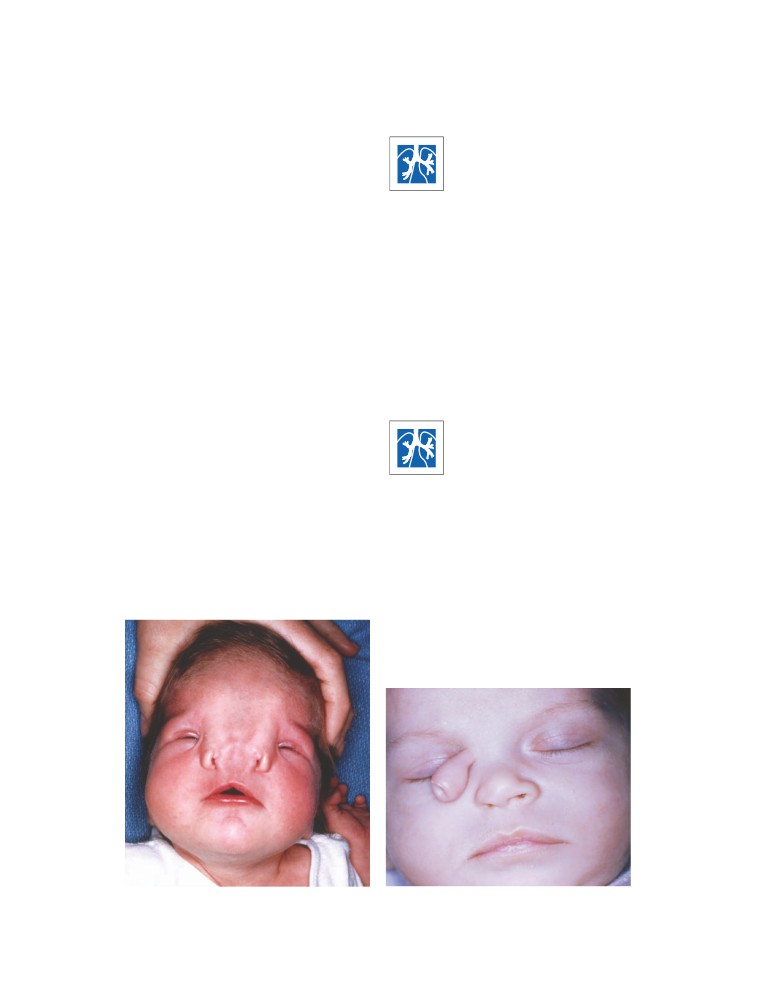
Median Nasal Furrow
the floor, and it is usually possible to pass a well-lubricated
tube through the nostril along the inferior meatus into the
In median nasal furrow, the nasal septum is split, separating
nasopharynx.
the two halves of the nose (CD Fig. 2-2A).
Trauma to the Nose
Lateral Proboscis
In lateral proboscis, a skin-covered process develops, usually
Nasal Fractures
with a dimple at its lower end (CD Fig. 2-2B).
Fractures involving the nasal bones are common. Blows di-
rected from the front may cause one or both nasal bones to
be displaced downward and inward.
THE PARANASAL
Lateral fractures also occur in which one nasal bone is
driven inward and the other outward; the nasal septum is
usually involved.
SINUSES
Skin Lacerations
Sinusitis and the Examination of
Lacerations are sutured in the usual way. Remember, how-
ever, that there is very little excess of skin so that the vascu-
the Paranasal Sinuses
larity may be compromised if too much tension is placed on
the sutures. Avoid making incisions across depressed areas
Infection of the paranasal sinuses is a common complication
on the side of the nose or at the junction of the nose and the
of nasal infections. Rarely, the cause of maxillary sinusitis is
A
B
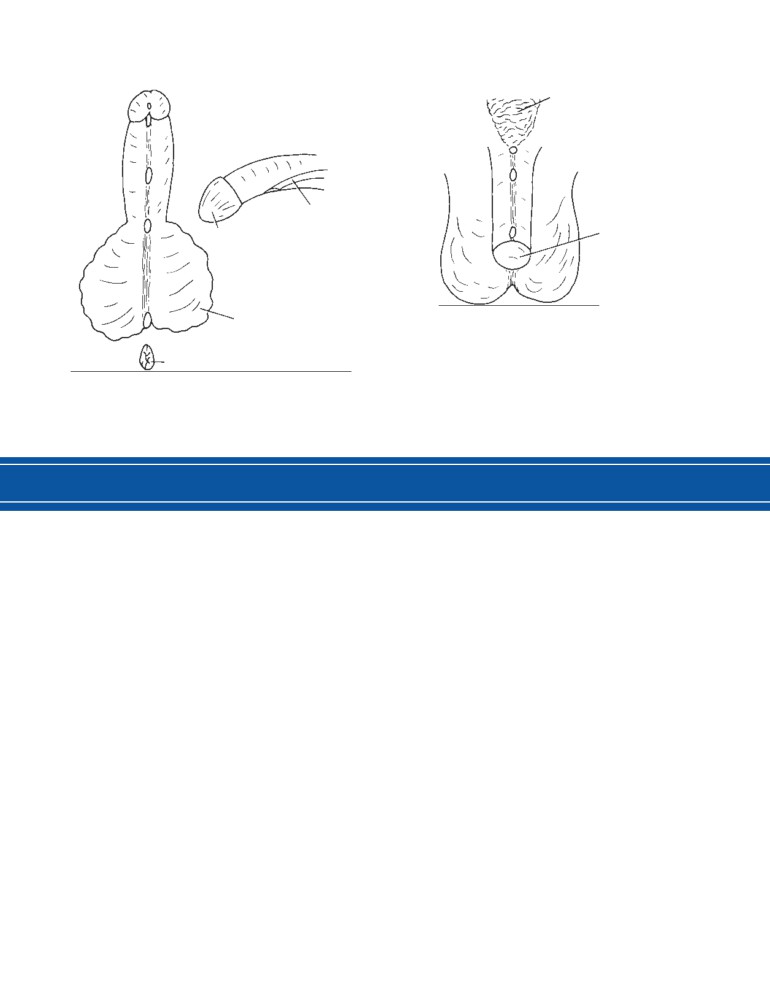
CD Figure 2-2
A. Median nasal furrow in which the nasal septum has completely split,
separating the two halves of the nose. Note that the external nares are separated by a wide
furrow. (Courtesy of L Thompson.) B. Lateral proboscis.
The Upper and Lower Airway and Associated Structures
19
frontal sinus
maxillary sinus
A
B
sphenoethmoidal recess
superior concha
frontal sinus
superior meatus
ethmoidal sinuses
middle meatus
middle concha
bulla ethmoidalis
hiatus semilunaris
maxillary sinus
inferior meatus
inferior concha
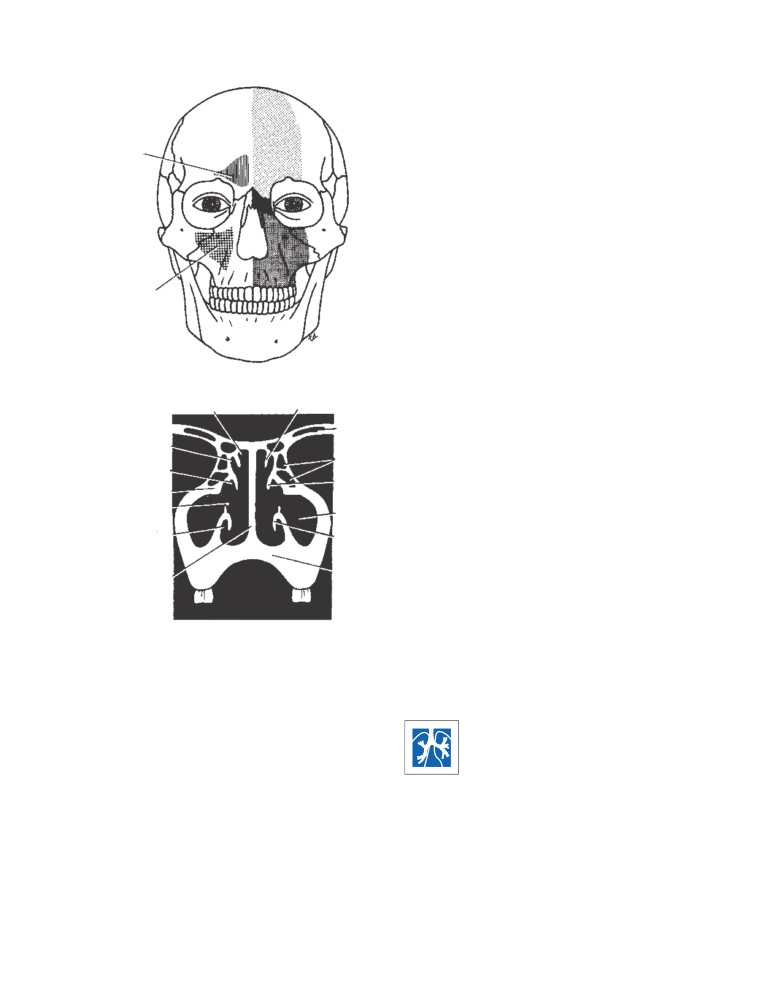
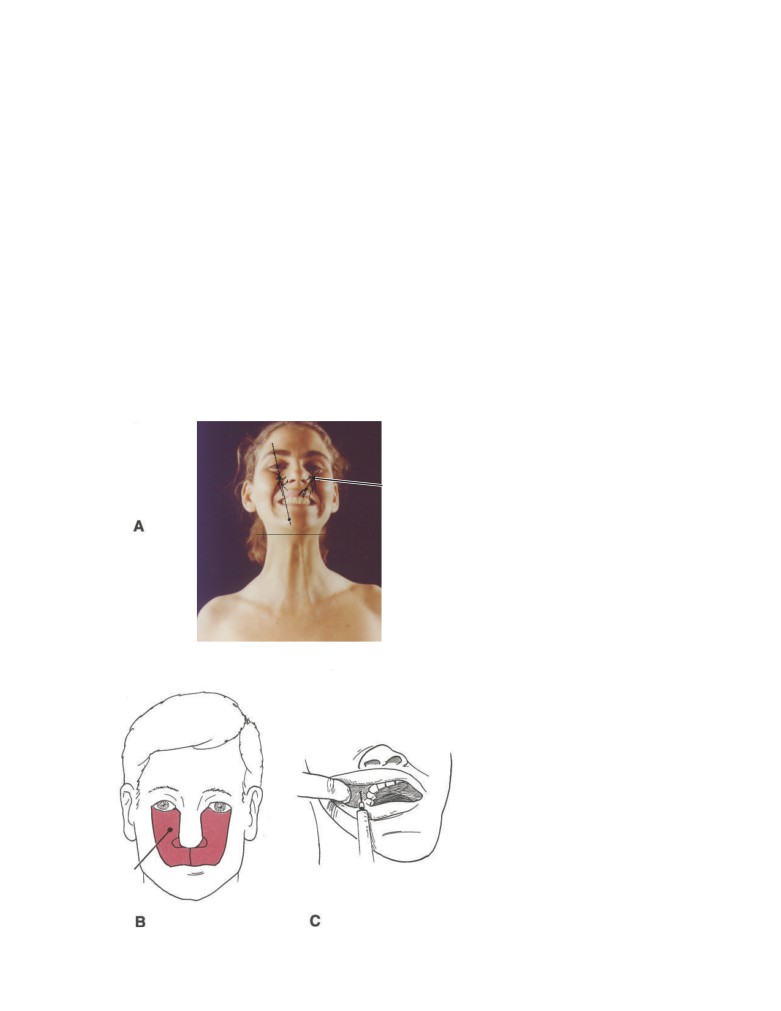
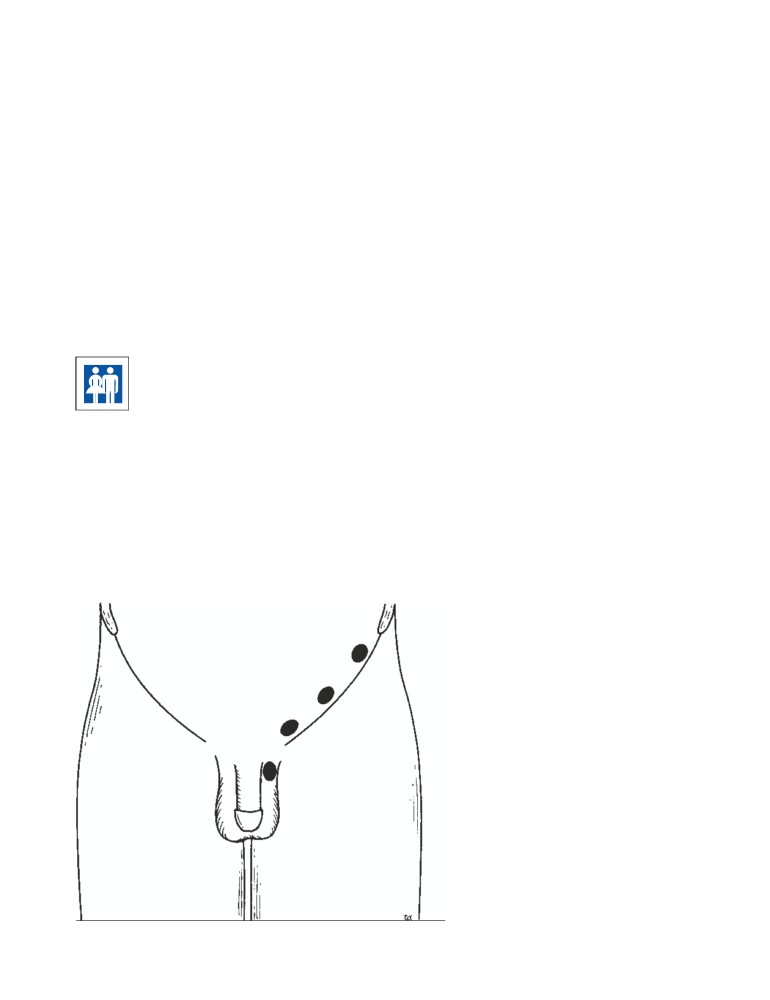
CD Figure 2-3
A. Bones of the face showing the po-
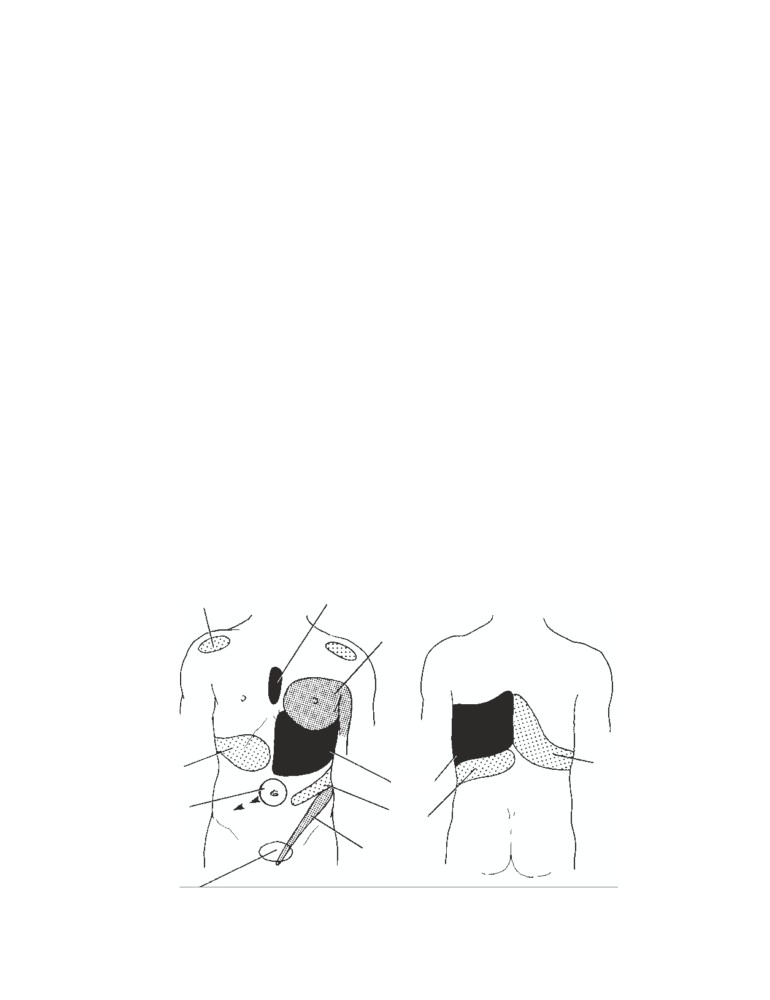
sitions of the frontal and maxillary sinuses. B. Regions
where pain is experienced in sinusitis (lightly dotted
palate
nasal septum
area in frontal sinusitis; solid area in sphenoethmoidal
sinusitis; and heavily dotted area in maxillary sinusi-
tis). C. Coronal section through the nasal cavity show-
C
ing the frontal, ethmoidal, and maxillary sinuses.
extension from an apical dental abscess. The extreme thin-
have pain referred over this area (see CD Fig. 2-3). The
ness of the medial wall of the orbit relative to the ethmoidal
maxillary sinus is innervated by the infraorbital nerve and,
air cells must be emphasized. Ethmoidal sinusitis is the most
in this case, pain is referred to the upper jaw, including the
common cause of orbital cellulitis. The infection can easily
teeth (see CD Fig. 2-3).
spread through the paper-thin bone.
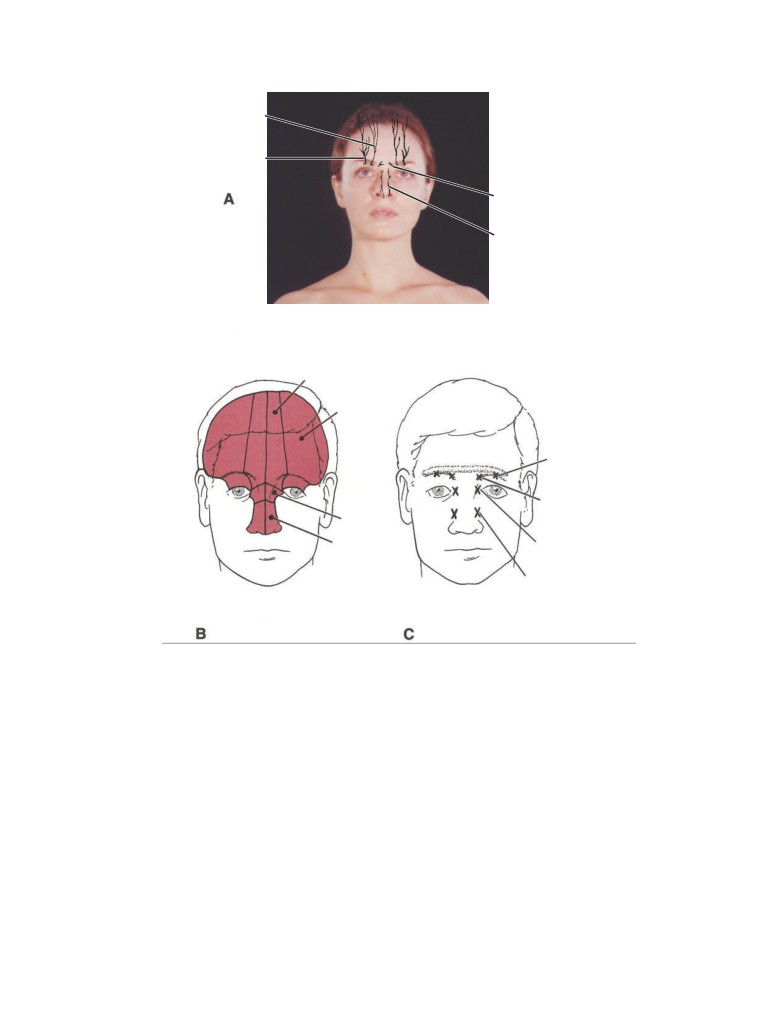
The frontal, ethmoidal, and maxillary sinuses can be
palpated clinically for areas of tenderness (CD Fig. 2-3).
THE MOUTH
The frontal sinus can be examined by pressing the finger up-
ward beneath the medial end of the superior orbital margin.
Here the floor of the frontal sinus is closest to the surface.
Examination of the Mouth
The ethmoidal sinuses can be palpated by pressing the
finger medially against the medial wall of the orbit. The
The mouth is one of the most important areas of the body
maxillary sinus can be examined for tenderness by pressing
that the medical professional is called on to examine. Need-
the finger against the anterior wall of the maxilla below the
less to say, the health professional must be able to recognize
inferior orbital margin; pressure over the infraorbital nerve
all the structures visible in the mouth and be familiar with
may reveal increased sensitivity.
the normal variations in the color of the mucous membrane
The frontal sinus is supplied by the supraorbital nerve,
covering the underlying structures. The sensory nerve sup-
which also supplies the skin of the forehead and scalp. It is
ply and lymph drainage of the mouth cavity should be
not surprising, therefore, that patients with frontal sinusitis
known. The close relation of the lingual nerve to the lower
20
Chapter 2
third molar tooth should be remembered. The close rela-
Sometimes this is inadequate to relieve the obstruction and
tion of the submandibular duct to the floor of the mouth
should be supplemented by placing the fingers behind the
may enable one to palpate a calculus in cases of periodic
angles of the mandible and exerting forward pressure. This
swelling of the submandibular salivary gland.
moves the mandible forward, causing displacement of the
tongue away from the laryngeal opening, since the mandible
is attached to the tongue by the genioglossus muscles.
Lips and Vestibule and Facial
Oral Endotracheal Intubation
Paralysis
Total visualization of the glottis with a laryngoscope is not
Asymmetry of the lips and paralysis of the buccinator with a
necessary for endotracheal intubation. If the epiglottis is vis-
tendency to accumulate saliva and food in the vestibule in-
ible, the tube is laid on the laryngeal side of the epiglottis
dicate a lesion of the facial nerve on that side.
and advanced along its surface. Often this procedure alone
will allow the tube to go into the trachea. If only the esoph-
Ranula
agus is visible and not the vocal cords, the endotracheal tube
can be placed “blindly” just anterior to the esophageal open-
Ranula is a cystic swelling arising in a distended mucous
ing. Occasionally when the tube is caught at the anterior
gland of the mucous membrane. It commonly occurs in the
glottic constriction, the head should be flexed slightly, al-
floor of the mouth, and because of its transparent covering,
lowing the pressure of the tongue to displace the endotra-
it resembles frog skin.
cheal tube posteriorly and hence move it into the opening
of the glottis. Frequently this maneuver has to be supple-
mented by turning the head slightly to one side or another.
THE TONGUE
The use of styleted endotracheal tubes also may help in this
situation. “Trigger tubes” may be used, which allow the tip
to be manipulated from above.
Laceration of the Tongue
When oral endotracheal intubation is impossible in the
above situations, nasotracheal intubation may be successful,
A wound of the tongue is often caused by the patient’s teeth
since the tube approaches the glottis slightly more posteri-
following a blow on the chin when the tongue is partly pro-
orly and is directed more toward it.
truded from the mouth. It can also occur when a patient ac-
cidentally bites the tongue while eating, during recovery
Oral Endotracheal Intubation and the Incisor Teeth
from an anesthetic, or during an epileptic attack. Bleeding
Interference with endotracheal intubation may be caused
is halted by grasping the tongue between the finger and
by the presence of protruding incisor teeth, often making it
thumb posterior to the laceration, thus occluding the
necessary to put the endotracheal tube in an extreme lateral
branches of the lingual artery.
position to approach the glottis.
Oral Endotracheal Intubation and the Small Mandible
Tongue and Airway Obstruction
Patients with receding jaws, secondary to a small mandible,
In an unconscious patient, there is a tendency for the
often make intubation difficult, and in some cases the nasal
tongue to fall backward and obstruct the laryngeal opening.
route or a lighted stylet or digital intubation must be used.
This is caused by the loss of tone of the extrinsic muscles
However, since this anatomic configuration approaches the
and, unless quickly corrected “with a jaw thrust or chin lift
picture seen in younger children, many times a small
maneuver,” will lead to all of the signs and symptoms of air-
straight blade such as a Miller no. 2 or Miller no. 3 can over-
way obstruction.
come the visual difficulties noted when a curved blade of
the Macintosh type is used.
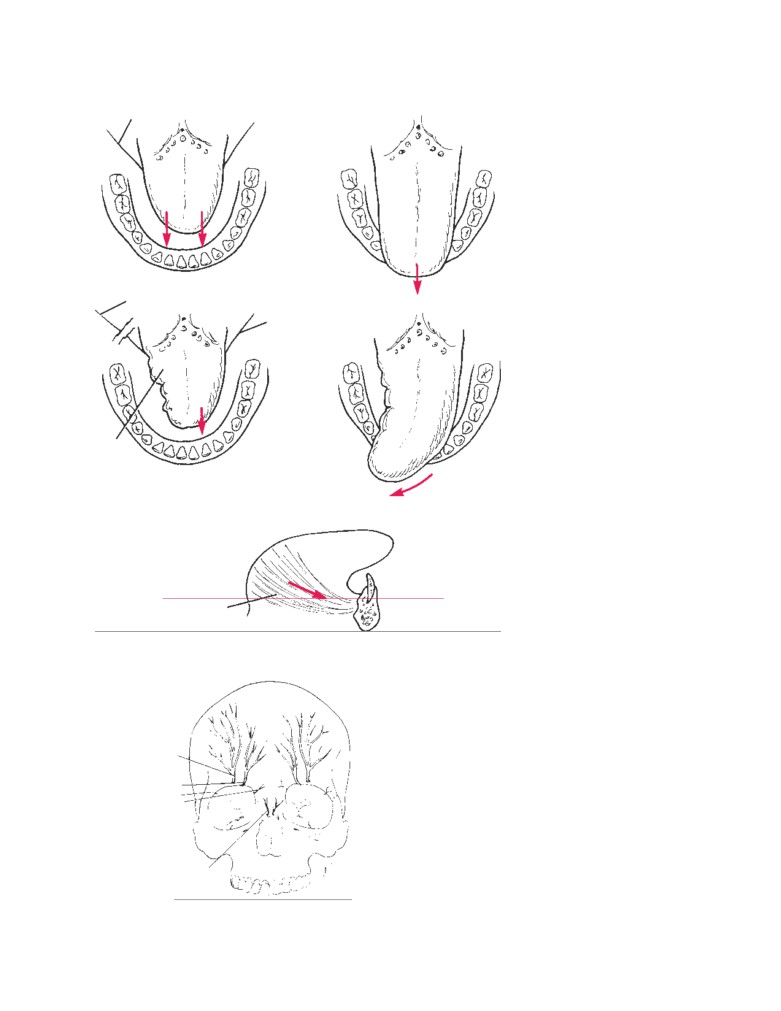
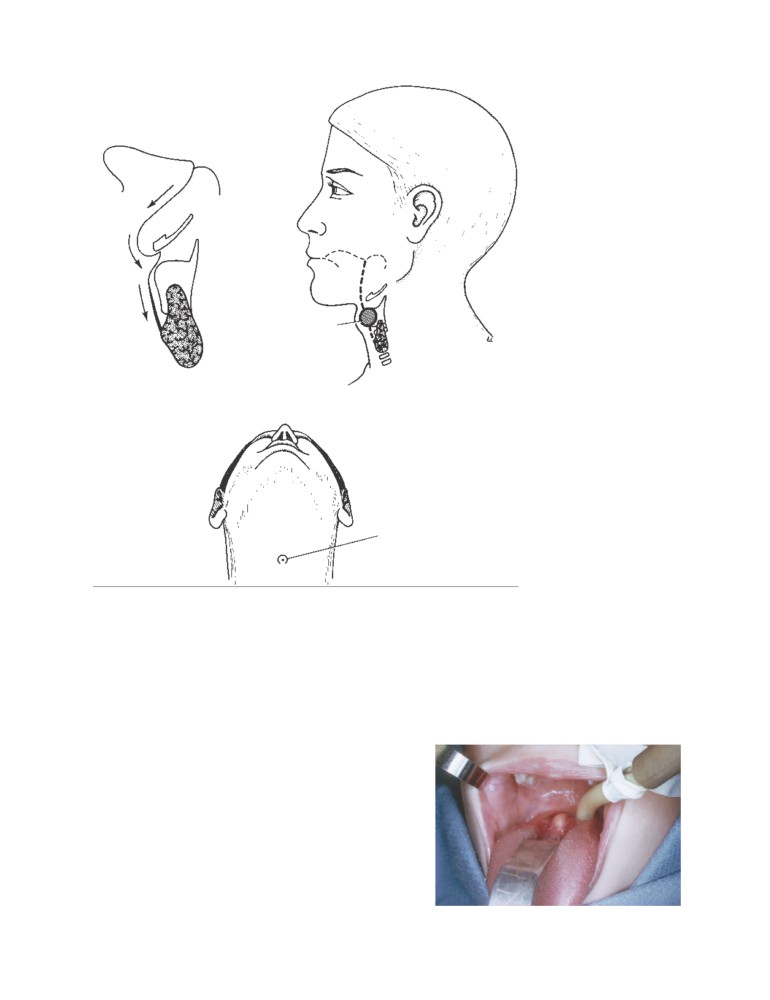
Anatomy of Procedures
Pulling the Tongue Forward in Airway
THE PALATE
Obstruction
The head should be extended at the atlantooccipital joint
Angioedema of the Uvula (Quincke’s
and the neck flexed at the C4 to C7 joints. The extended
head stretches the fascia and muscles of the front of the neck
Uvula)
and causes a forward and downward movement of the
mandible that is correctable by placing a finger below the
The uvula has a core of voluntary muscle, the musculus
symphysis menti and pulling the mandible forward and up.
uvulae, that is attached to the posterior border of the hard
The Upper and Lower Airway and Associated Structures
21
palate. Surrounding the muscle is the loose connective tis-
sue of the submucosa that is responsible for the great
swelling of this structure secondary to angioedema.
CONGENITAL
A
B
ANOMALIES OF
THE PALATE
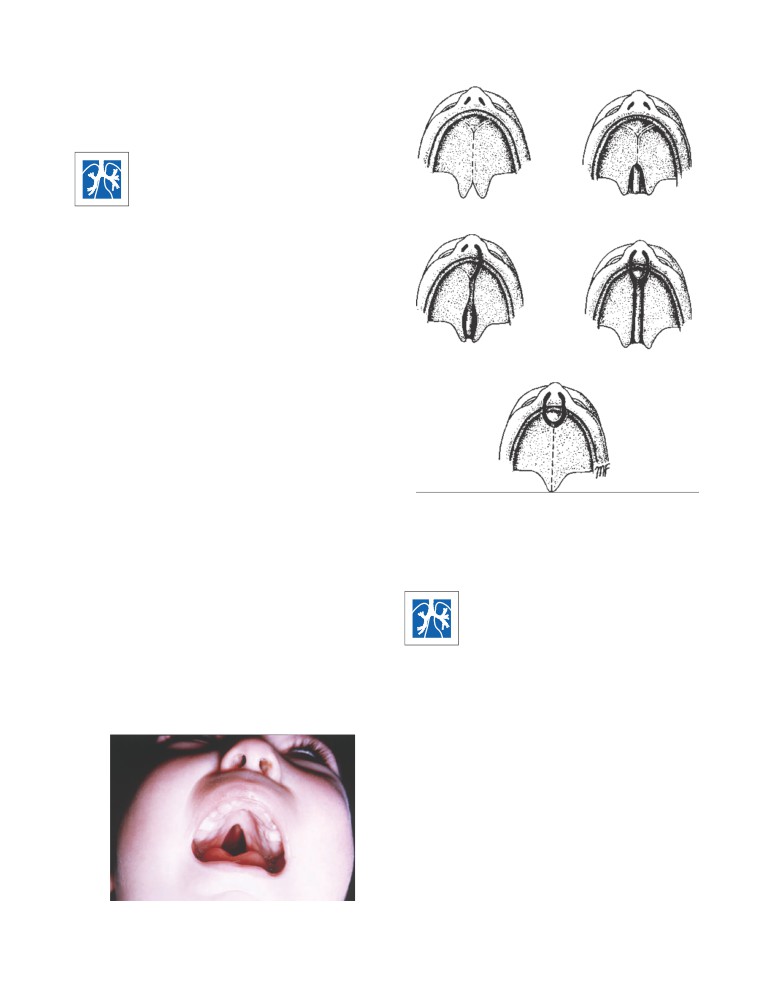
Cleft Palate
Cleft palate is commonly associated with cleft upper lip.
All degrees of cleft palate occur and are caused by failure
of the palatal processes of the maxilla to fuse with each
C
D
other in the midline; in severe cases, these processes also
fail to fuse with the primary palate (premaxilla) (CD Figs.
2-4 and 2-5). The first degree of severity is cleft uvula, and
the second degree is ununited palatal processes. The third
degree is ununited palatal processes and a cleft on one side
of the primary palate. This type is usually associated with
unilateral cleft lip. The fourth degree of severity, which is
rare, consists of ununited palatal processes and a cleft on
both sides of the primary palate. This type is usually asso-
E
ciated with bilateral cleft lip. A rare form may occur in
which a bilateral cleft lip and failure of the primary palate
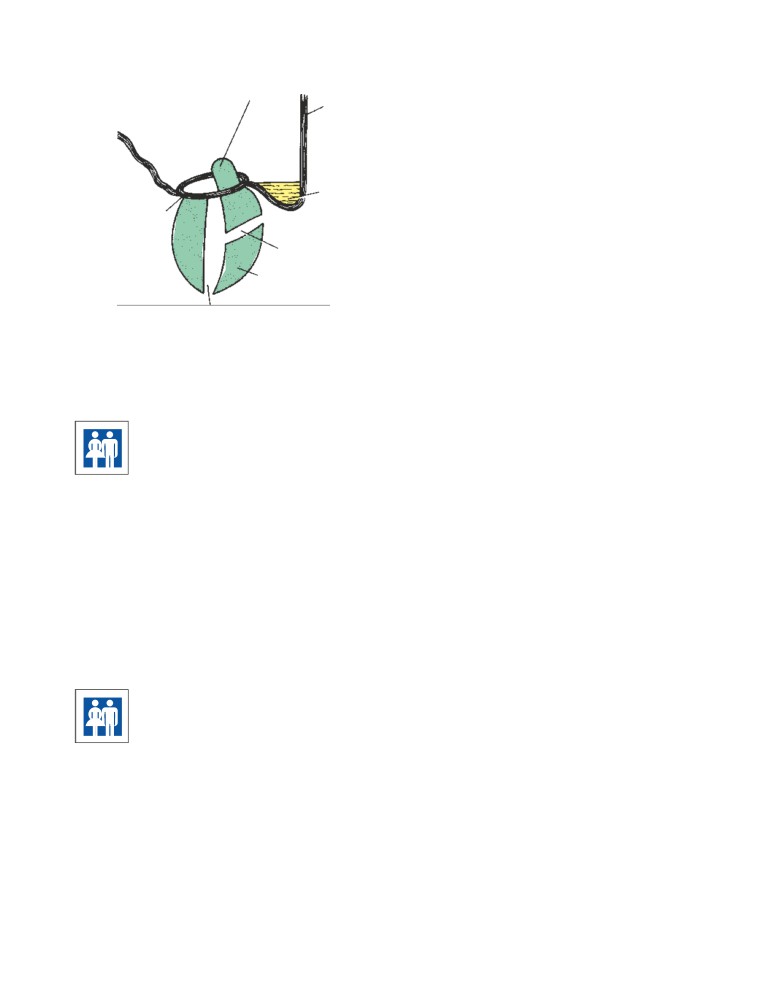
CD Figure 2-5
Different forms of cleft palate: cleft uvula (A),
cleft soft and hard palate (B), total unilateral cleft palate and
to fuse with the palatal processes of the maxilla on each
cleft lip (C), total bilateral cleft palate and cleft lip (D), and
side are present.
bilateral cleft lip and jaw (E).
A baby born with a severe cleft palate presents a difficult
feeding problem, since he or she is unable to suck effi-
ciently. Such a baby often receives in the mouth some milk,
which then is regurgitated through the nose or aspirated into
THE SALIVARY
the lungs, leading to respiratory infection. For this reason,
careful artificial feeding is required until the baby is strong
enough to undergo surgery. Plastic surgery is recommended
GLANDS
usually between 1 and 2 years of age, before improper
speech habits have been acquired.
Parotid Salivary Gland and Lesions
of the Facial Nerve
The facial nerve lies in the interval between the superficial
and deep parts of the gland. A benign parotid tumor rarely,
if ever, causes facial palsy. A malignant tumor of the parotid
is usually highly invasive and quickly involves the facial
nerve, causing unilateral facial paralysis.
Parotid Gland Infections
The parotid gland may become acutely inflamed as a result
of retrograde bacterial infection from the mouth via the
parotid duct. The gland may also become infected via the
CD Figure 2-4
Cleft hard and soft palate.
bloodstream, as in mumps.
22
Chapter 2
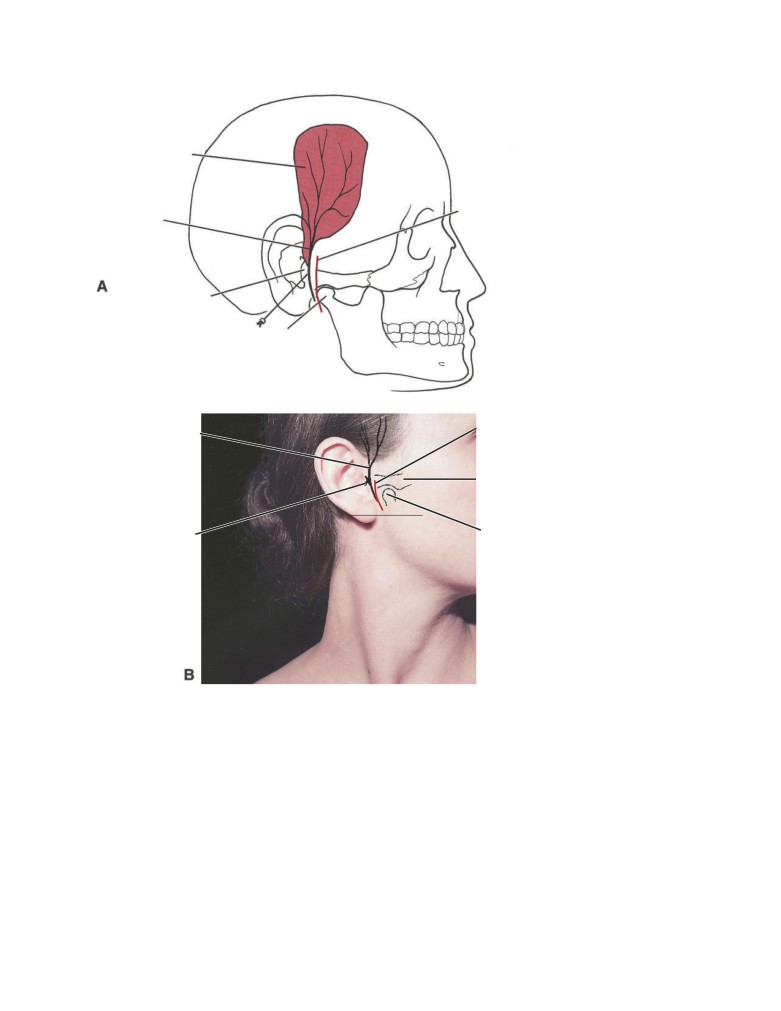
Parotid Duct and Facial Injuries
THE PROCESS OF
The parotid duct, which is a comparatively superficial struc-
ture on the face, runs forward from the parotid gland one
SWALLOWING
fingerbreadth below the zygomatic arch (see text Fig. 2-18).
It is about 2 in. (5 cm) long and can be rolled beneath the
(DEGLUTITION)
examining finger at the anterior border of the masseter as it
turns medially and pierces the buccinator muscle; it then
opens into the mouth opposite the upper second molar
Swallowing in Unconscious
tooth (see text Fig. 2-8).
The parotid duct may be damaged in injuries to the
Individuals
face or may be inadvertently cut during surgical operations
on the face. The integrity of the parotid duct can be estab-
During swallowing in conscious individuals, food and
lished by wiping the inside of the cheek dry and then press-
fluid cross naturally from the mouth to the esophagus,
ing on the parotid gland. Look for a drop of viscid saliva to
and movements of air from the nose to the larynx is
appear on the tip of the papilla in the mouth.
momentarily stopped. In unconscious individuals, when
the reflex mechanisms are not functioning, it is possible
for food and fluid to enter the bronchial tree or air to enter
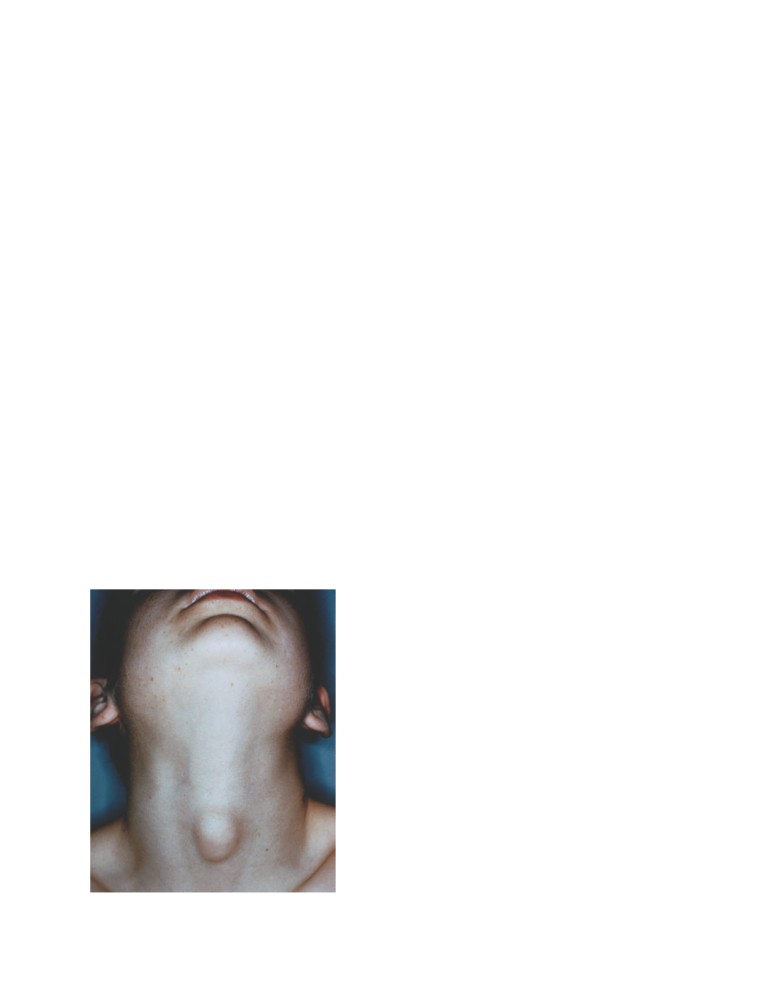
Submandibular Gland: Calculus
the stomach. Moreover, should vomiting occur, the regur-
gitated gastric contents may be inhaled into the lungs
Formation
(see below).
The submandibular salivary gland is a common site of cal-
culus formation. The presence of a tense swelling below the
body of the mandible, which is greatest before or during a
Pharyngeal Obstruction of the
meal and is reduced in size or absent between meals, is di-
agnostic of the condition. Examination of the floor of the
Upper Airway
mouth will reveal absence of ejection of saliva from the ori-
fice of the duct of the affected gland. Frequently, the stone
This condition frequently occurs in patients during
can be palpated in the duct, which lies below the mucous
cardiopulmonary arrest or in the decreased level of con-
membrane of the floor of the mouth.
sciousness that accompanies a major cerebrovascular acci-
dent or drug overdose. The obstruction is caused when the
Sublingual Gland and Cyst
atonic tongue falls back and the pharyngeal wall caves in
due to loss of tone of the pharyngeal muscles. The obstruc-
Formation
tion may clear if the patient is placed in the lateral decubi-
tus position, with the neck extended and the jaw pulled
Blockage of one of the ducts of the sublingual gland may
forward (which pulls the tongue forward). If the patient
cause cysts under the tongue.
must lie in a supine position, an oropharyngeal or nasopha-
ryngeal airway may have to be inserted to counteract the
flaccid pharyngeal walls.
THE PHARYNX
The Killian’s Dehiscence and
Loss of the Gag Reflex
In conscious patients the airway is protected by a number of
Foreign Bodies
important reflexes, including the gag reflex, the laryngeal
Inverted foreign bodies tend to get snared in the region of
reflex, and the cough reflex. The gag or swallowing reflex
Killian’s dehiscence.
occurs in response to stimulation of the pharyngeal mucous
membrane, which is innervated by the glossopharyngeal
nerve. The laryngeal and cough reflexes (trachea and
The Piriform Fossa and Foreign
bronchi) are mediated by the vagus nerve. These protective
reflexes are lost in descending order as the patient becomes
Bodies
less and less responsive. In these circumstances the airway
The piriform fossa is a common site for fish bones or other
may be blocked by aspiration of vomit and gastric and pha-
foreign bodies to become lodged.
ryngeal secretions.
The Upper and Lower Airway and Associated Structures
23
Relationship between Vocal Folds
PALATINE TONSILS
and Cricothyroid Ligament
Text Fig. 2-27 shows the relationship between the vocal folds
Examination of the Tonsils
and the cricothyroid ligament. It is clear that the folds may
With the mouth wide open and with a good light shining into
be damaged in puncture wounds in the front of the larynx.
the mouth, the tongue is depressed with a spatula. The ton-
sils can be clearly seen on each side of the oral pharynx in the
Larynx in Children
depression between the palatoglossal and palatopharyngeal
folds. Note the size and color of the tonsil; a reddened tonsil
In children the neck is shorter and the larynx is more cepha-
covered with mucus or pus is a clear indication of tonsillitis.
lad than in adults (CD Fig. 2-6). At birth the cricoid cartilage
lies at the level of the fourth cervical vertebra, and only at the
age of 6 years does it lie opposite the sixth cervical vertebra.
Tonsillitis
The glottis at birth lies opposite the second cervical vertebra.
The palatine tonsils reach their maximum normal size in
The epiglottis is U-shaped and less flexible in children,
early childhood. After puberty, together with other lym-
which sometimes makes it difficult to line up the oral, pha-
phoid tissues in the body, they gradually atrophy. The pala-
ryngeal, and tracheal axes when passing a laryngoscope.
tine tonsils are a common site of infection, producing the
The rima glottidis tends to be more anterior in children
characteristic sore throat and pyrexia. The deep cervical
than in adults. The vocal folds in children have thicker sub-
lymph node situated below and behind the angle of the
mucosa, so that edema of the folds is more likely to occlude
mandible, which drains lymph from this organ, is usually
the glottis.
enlarged and tender.
As mentioned previously, the cavity of the larynx is nar-
Tonsillectomy, which is often the treatment for recur-
rowest within the cricoid ring in children, whereas the glot-
rent episodes of tonsillitis, is sometimes accompanied by
tis is the narrowest part of the cavity in adults.
troublesome postoperative bleeding from the external pala-
tine vein.
Epiglottitis
An acute inflammatory swelling of the mucous membrane of
Quinsy
the epiglottis can compromise the upper airway. The inflam-
A peritonsillar abscess, or quinsy, is caused by spread of in-
mation may spread rapidly in the loosely arranged submucosa
fection from the palatine tonsil to the loose connective tis-
down to the vocal cords. Here the spreading stops because the
sue outside the capsule (see text Fig. 2-24).
mucosa is tightly adherent to the underlying vocal ligaments.
The condition is most often seen in children where the nar-
row passageway quickly leads to upper airway obstruction.
Adenoids
Adenoids are enlarged nasopharyngeal tonsils usually associ-
Foreign Bodies in the Airway
ated with infection. Excessive enlargement blocks the poste-
The laryngeal and cough reflexes mediated through the va-
rior nasal openings and causes the patient to snore loudly at
gus nerves are the natural defense mechanisms for expelling
night and to breathe through the open mouth. The close re-
foreign bodies from the airway at all ages. If coughing is suc-
lationship of the infected lymphoid tissue to the auditory
cessfully freeing the obstruction, it should be encouraged to
tube may be the cause of deafness and recurrent otitis media.
continue. If intervention is necessary, anatomic and physio-
logic age differences dictate treatment.
THE LARYNX
Anatomic Rationale for
The Cricoid Cartilage and the
Differences in Procedures for
Sellick Maneuver
Removing Foreign Bodies in
The continuous ring structure of the cricoid cartilage is uti-
Adults and Children
lized when applying pressure on the cricoid to control re-
gurgitation of stomach contents during the induction of
It is generally agreed that all maneuvers are directed toward
anesthesia.
the increase in intrathoracic pressure by compressing the
24
Chapter 2
mandible
hyoid cartilage
mandible
thyroid cartilage
body of
cricoid cartilage
hyoid bone
manubrium sterni
thyroid cartilage
cricoid cartilage
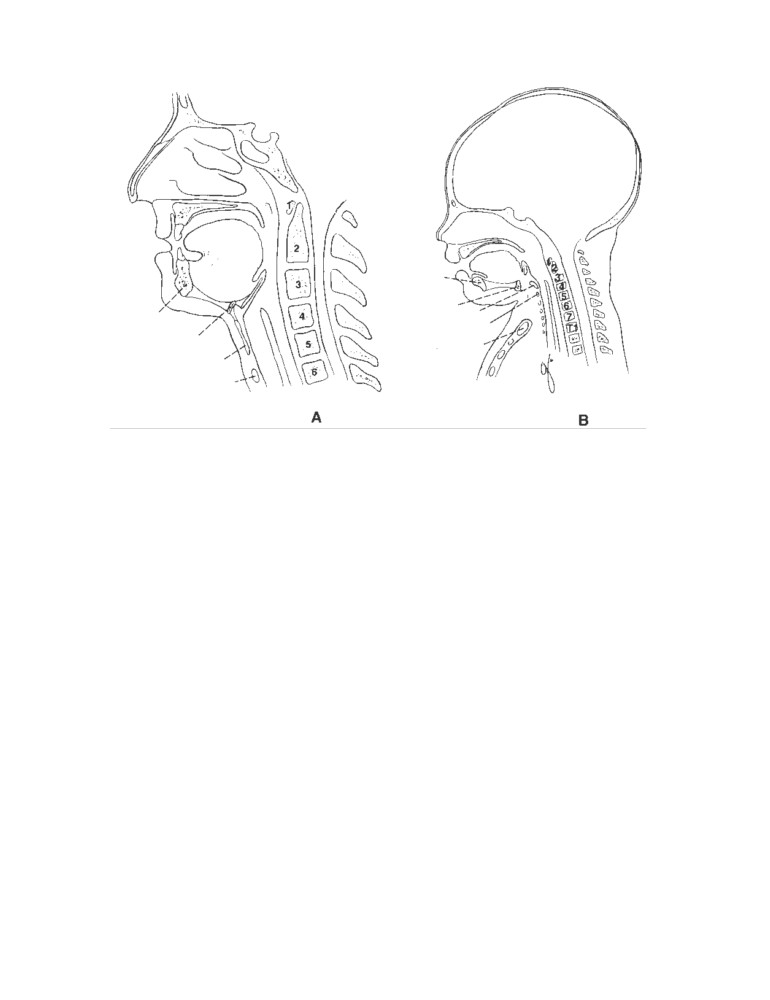
CD Figure 2-6
Sagittal sections of the neck of an adult (A) and an infant (B) shortly after
birth. Different vertebral levels in these age groups are shown.
intrathoracic gas volume to expel the foreign body from
may be involved in a bronchial or esophageal carcinoma or
the airway. For children older than 1 year and for adults,
in secondary metastatic deposits in the mediastinal lymph
the abdominal thrust (Heimlich maneuver) should be used.
nodes. The right and left recurrent laryngeal nerves may be
The rapid compression of the abdominal viscera suddenly
damaged by malignant involvement of the deep cervical
forces the diaphragm into the thoracic cavity. In infants, the
lymph nodes.
relatively large size of the liver and the delicate structure of
Section of the external laryngeal nerve produces weak-
the abdominal viscera generally preclude its use. Children
ness of the voice because the vocal fold cannot be tensed.
younger than 1 year should be placed face down over the
The cricothyroid muscle is paralyzed (CD Fig. 2-7).
rescuer’s arm, with the head lower than the trunk, and mea-
Unilateral complete section of the recurrent laryn-
sured back blows should be delivered between the scapulae.
geal nerve results in the vocal fold on the affected side
If this fails to open the airway, they should be rolled over,
assuming the position midway between abduction and
and four rapid sternal compressions should be administered.
adduction. It lies just lateral to the midline. Speech is not
It is now accepted that sudden blows to the back in the
greatly affected because the other vocal fold compensates to
older age groups, especially in the standing or sitting
some extent and moves toward the affected vocal fold (CD
position, extends the thoracic part of the vertebral column
Fig. 2-7).
and may displace the foreign body further down the airway,
Bilateral complete section of the recurrent laryngeal
leading to impaction or complete obstruction.
nerve results in both vocal folds assuming the position
midway between abduction and adduction. Breathing is
impaired because the rima glottidis is partially closed, and
Lesions of the Laryngeal Nerves
speech is lost (CD Fig. 2-7).
The muscles of the larynx are innervated by the recurrent la-
Unilateral partial section of the recurrent laryngeal
ryngeal nerves, with the exception of the cricothyroid mus-
nerve results in a greater degree of paralysis of the abductor
cle, which is supplied by the external laryngeal nerve. Both
muscles than of the adductor muscles. The affected vocal
these nerves are vulnerable during operations on the thyroid
fold assumes the adducted midline position (CD Fig. 2-7).
gland because of the close relationship between them and
This phenomenon has not been explained satisfactorily.
the arteries of the gland. The left recurrent laryngeal nerve
It must be assumed that the abductor muscles receive a
The Upper and Lower Airway and Associated Structures
25
epiglottis
rima
right vocal fold (cord)
glottidis
A. Bilateral
external laryngeal
nerve palsy
aryepiglottic fold
corniculate cartilage
inspiration
B. Unilateral
complete section
of right recurrent
laryngeal nerve
inspiration
phonation
C. Bilateral
complete section
of recurrent laryngeal
nerves
inspiration
D. Unilateral partial section
of right recurrent
laryngeal nerve
inspiration
E. Bilateral partial section
of recurrent laryngeal
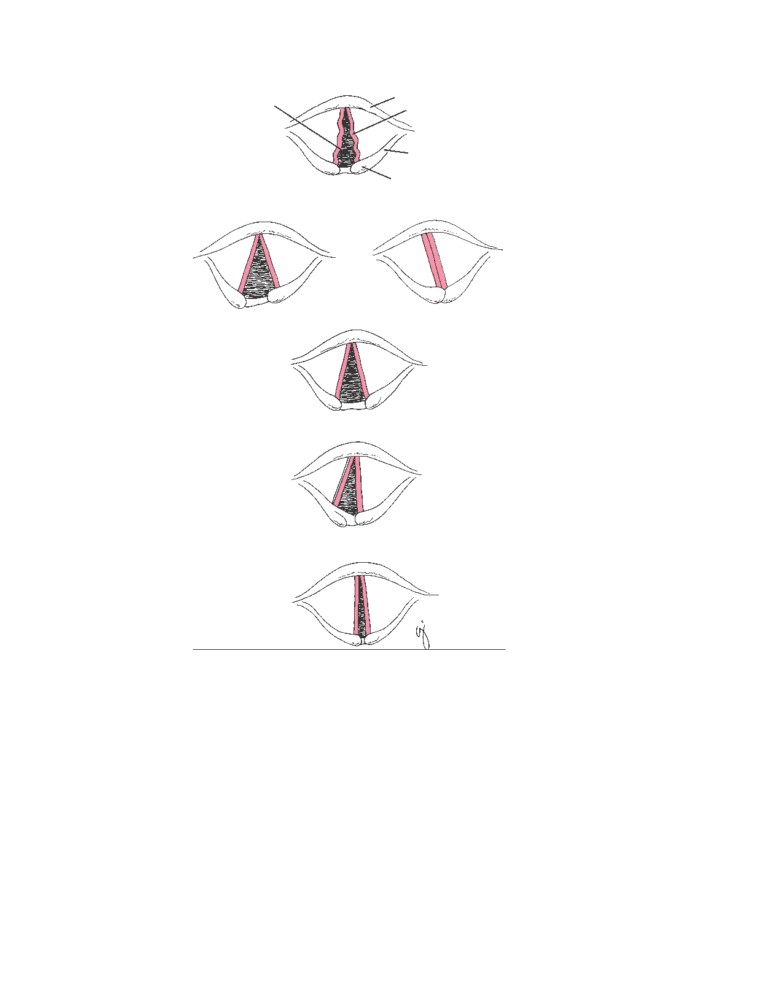
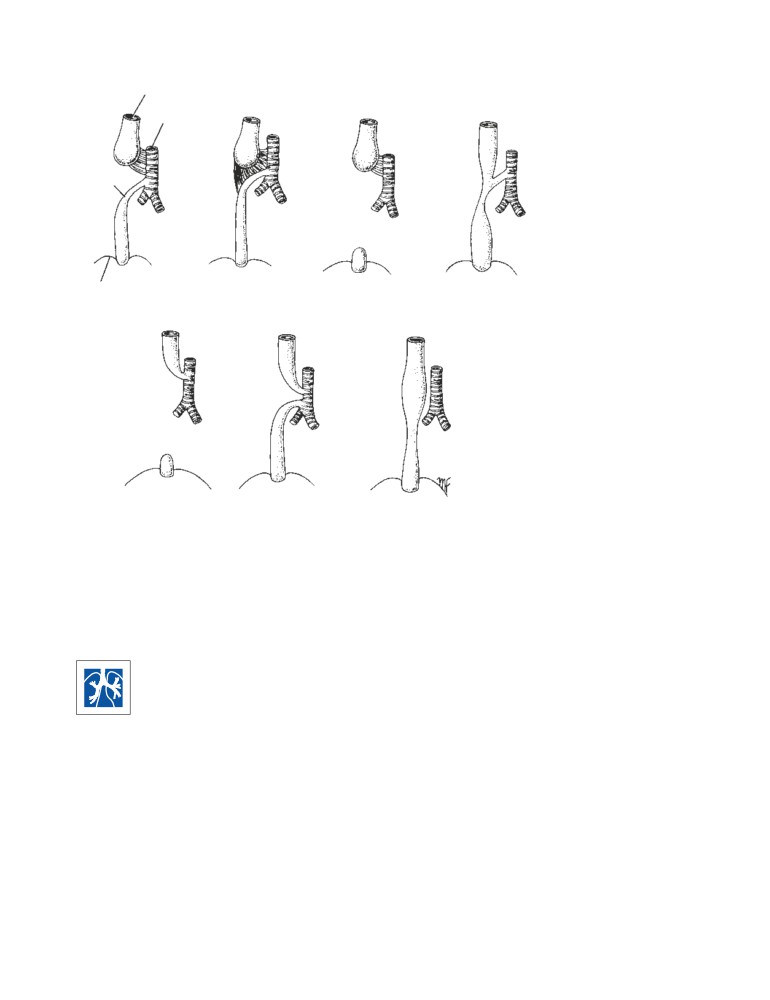
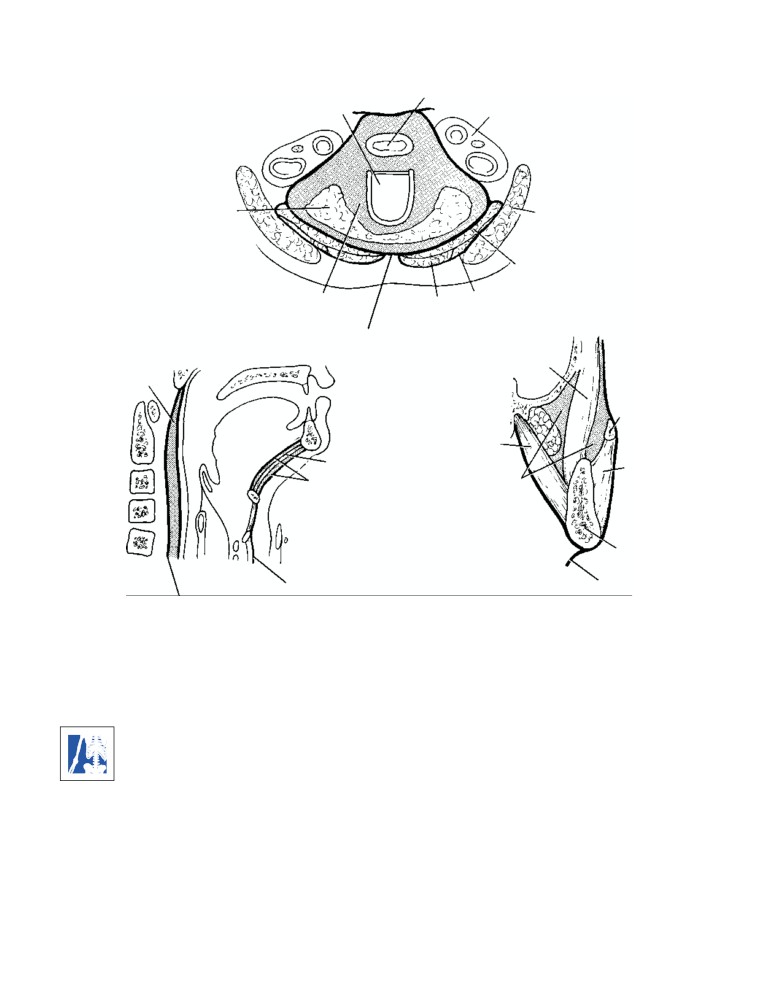
CD Figure 2-7
The position of the
nerves
vocal folds (cords) after damage to
the external and recurrent laryngeal
inspiration
nerves.
greater number of nerves than the adductor muscles, and
thus partial damage of the recurrent laryngeal nerve results
Inspection of the Vocal Cords
in damage to relatively more nerve fibers to the abductor
muscles. Another possibility is that the nerve fibers to the ab-
(Folds) with the Laryngeal Mirror
ductor muscles are traveling in a more exposed position in
the recurrent laryngeal nerve and are therefore more prone
and Laryngoscope
to be damaged.
The interior of the larynx can be inspected indirectly
Bilateral partial section of the recurrent laryngeal
through a laryngeal mirror passed through the open mouth
nerve results in bilateral paralysis of the abductor muscles
into the oral pharynx (CD Fig. 2-8). A more satisfactory
and the drawing together of the vocal folds (CD Fig. 2-7).
method is the direct method using the laryngoscope. The
Acute breathlessness (dyspnea) and stridor follow, and
neck is brought forward on a pillow and the head is fully
cricothyroidotomy or tracheostomy is necessary.
extended at the atlantooccipital joints. The illuminated
26
Chapter 2
orientation of
laryngeal inlet
vocal fold
epiglottis
hard palate
(cord)
vestibular fold
rima glottidis
examiner's
eye
cuneiform
cartilage
tongue
corniculate
cartilage
A
entrance into larynx
laryngoscope
examiner's
eye
tongue
entrance
into larynx
B
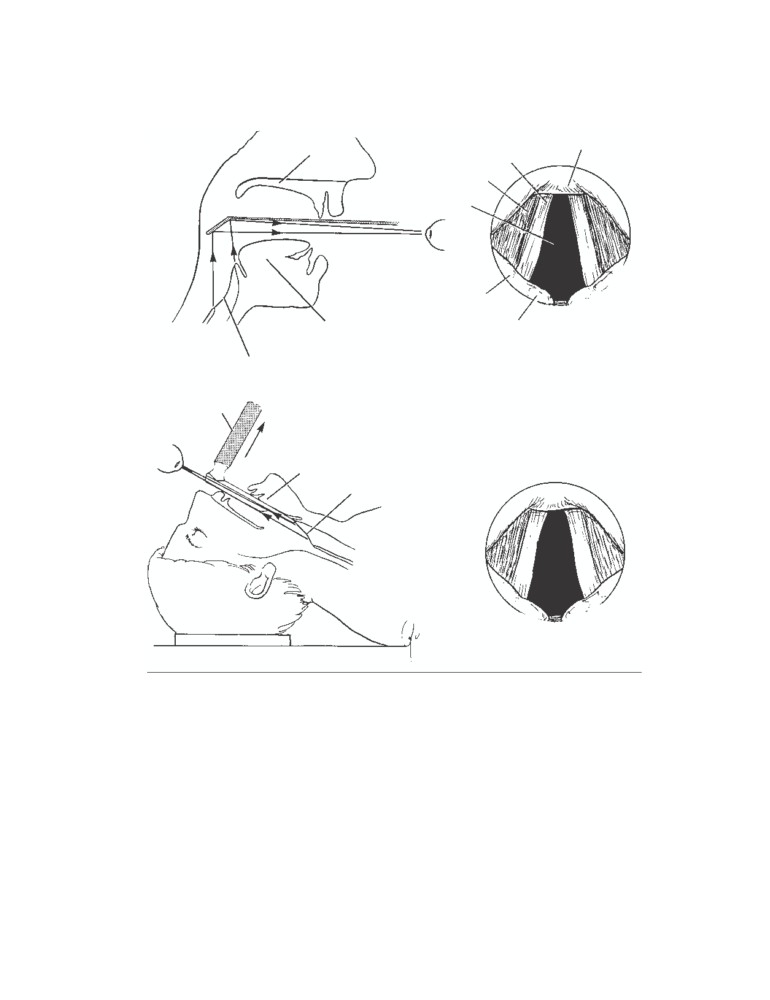
CD Figure 2-8
Inspection of the vocal folds (cords) indirectly through a laryngeal mirror
(A) and through a laryngoscope (B). Note the orientation of the structures forming the
laryngeal inlet.
instrument can then be introduced into the larynx over the
If the patient is asked to breathe deeply, the vocal folds
back of the tongue (CD Fig. 2-8). The valleculae, the piri-
become widely abducted, and the inside of the trachea can
form fossae, the epiglottis, and the aryepiglottic folds are
be seen.
clearly seen. The two elevations produced by the corniculate
and cuneiform cartilages can be recognized. Within the lar-
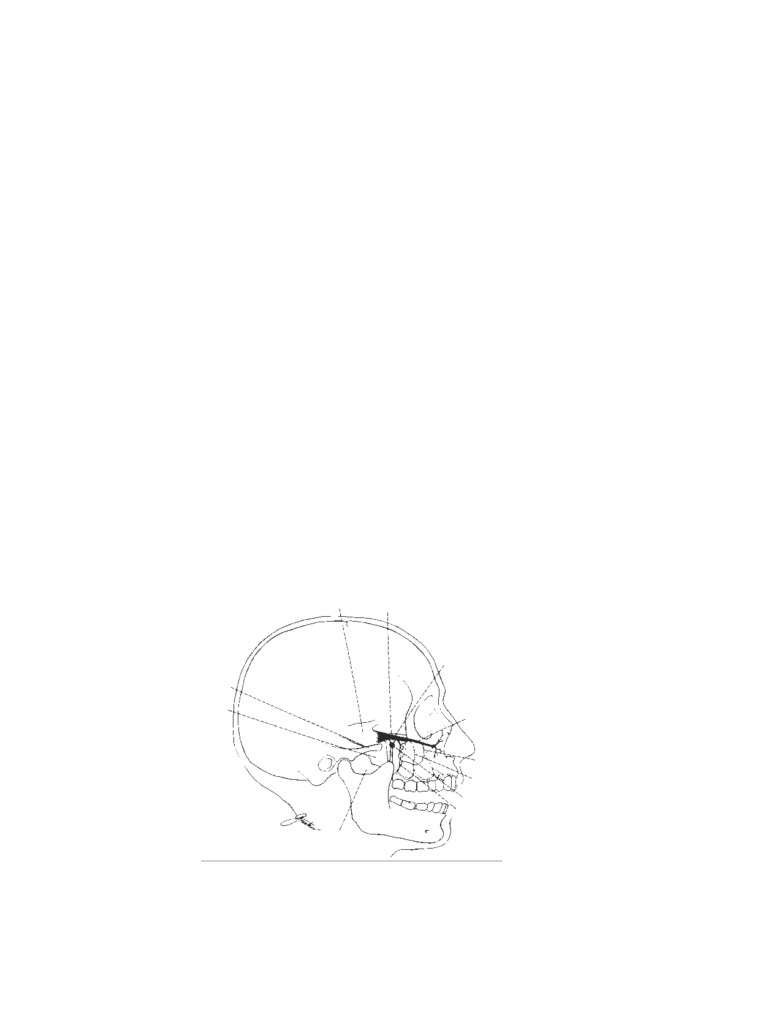
Important Anatomic Axes for
ynx, the vestibular folds and the vocal folds can be seen. The
former are fixed, widely separated, and reddish in color; the
Endotracheal Intubation
latter move with respiration and are white in color. With
quiet breathing, the rima glottidis is triangular, with the apex
The upper airway has three axes that have to be brought into
in front. With deep inspiration, the rima glottidis assumes a
alignment if the glottis is to be viewed adequately through a
diamond shape because of the lateral rotation of the ary-
laryngoscope—the axis of the mouth, the axis of the phar-
tenoid cartilages.
ynx, and the axis of the trachea (CD Fig. 2-9).
The Upper and Lower Airway and Associated Structures
27
M
A
T
P
B
M
T
P
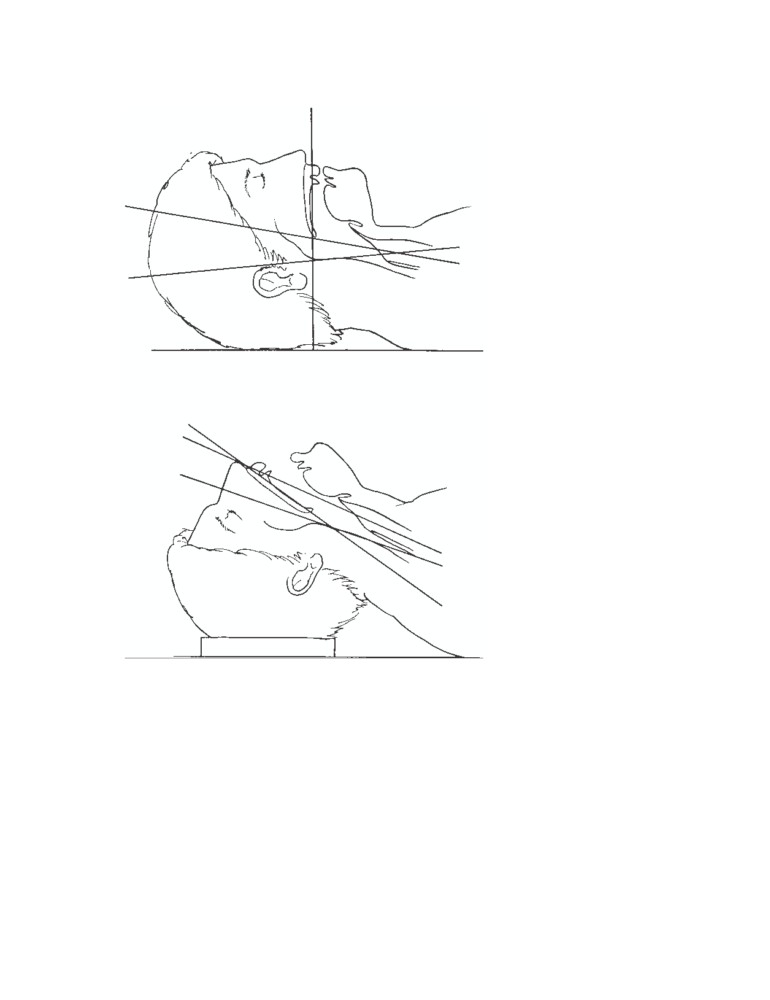
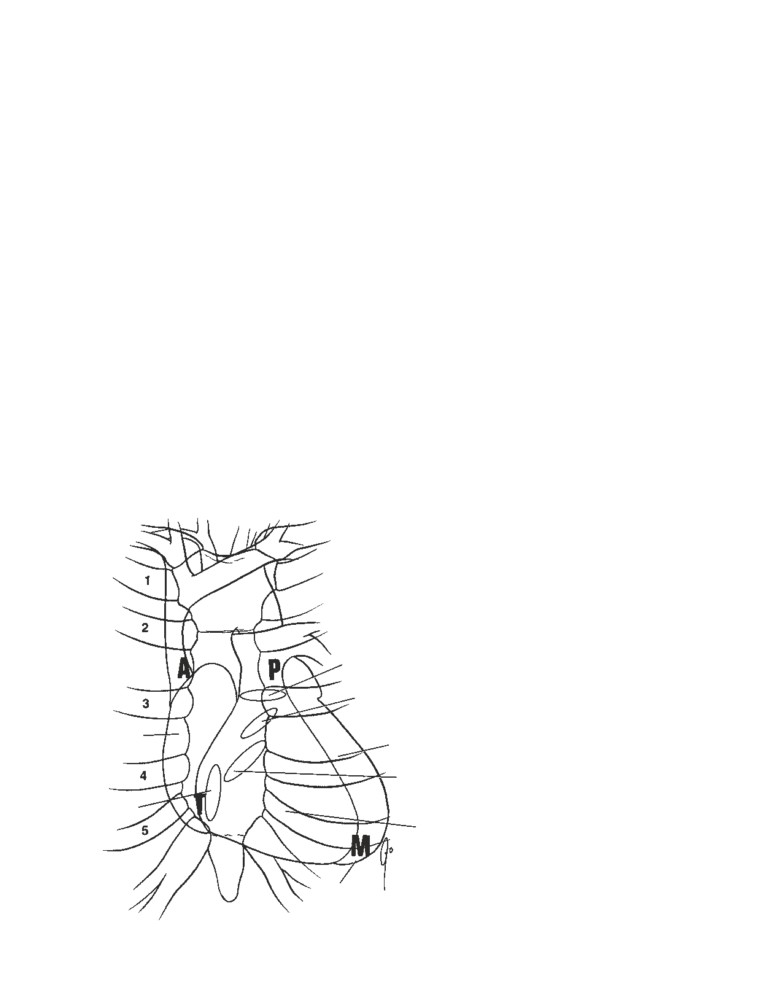
CD Figure 2-9
Anatomic axes for endo-
tracheal intubation. A. With the head in
the neutral position, the axis of the mouth
(M), the axis of the trachea (T), and the
axis of the pharynx (P) are not aligned
with one another. B. If the head is ex-
tended at the atlantooccipital joints, the
axis of the mouth is correctly placed. If
the back of the head is raised off the table
with a pillow, thus flexing the cervical
vertebral column, the axes of the trachea
and pharynx are brought in line with the
axis of the mouth.
The following procedures are necessary: First the head
2. The vocal cords (ligaments) are attached at their ante-
is extended at the atlantooccipital joints. This brings the axis
rior ends to the thyroid cartilage just below the attach-
of the mouth into the correct position. Then the neck is
ment of the epiglottis (see text Fig. 2-26).
flexed at cervical vertebrae C4 to C7 by elevating the back
3. Because of the above two facts, it follows that manipu-
of the head off the table, often with the help of a pillow. This
lation of the epiglottis and possibly the thyroid cartilage
brings the axes of the pharynx and the trachea in line with
will greatly assist the operator in visualizing the cords
the axis of the mouth.
and the glottis.
Anatomy of the Visualization of the
The patient’s head and neck are correctly positioned so
that the three axes of the airway (noted above) have been es-
Vocal Cords with the Laryngoscope
tablished and the patient has assumed the “sniffing” posi-
tion. The laryngoscope is inserted into the patient’s mouth,
1. The pear-shaped epiglottis is attached by its stalk at its
and the blade is correctly placed alongside the right
lower end to the interior of the thyroid cartilage (see text
mandibular molar teeth. The blade can then be passed over
Fig. 2-26).
the tongue and down into the esophagus. The tip of the
28
Chapter 2
median
tongue
glossoepi-
glottic fold
epiglottis
vallecula
tubercle of
epiglottis
vestibular fold
lateral
glossoepi-
glottic fold
vocal fold
aryepiglottic fold
piriform fossa
cuneiform cartilage
rima glottidis
CD Figure 2-10
The laryngeal inlet as seen
corniculate cartilage
from above.
blade must be fully inserted into the esophagus (so that you
changes are largely mediated through the branches of the
know where it is anatomically). The blade should by now
vagus nerves.
have moved toward the midline and followed the anatomic
curvature on the posterior surface of the tongue.
The laryngoscopic blade is then gently and slowly with-
THE TRACHEA
drawn. The tip of the blade is kept under direct vision at all
times and is permitted to rise up out of the esophagus. Re-
member that the tip of the blade is at first in the esophagus
Palpation of the Trachea
and therefore distal to the level of the vocal cords. Once the
blade tip has left the esophagus, it is in the laryngeal part of
The trachea can be readily felt below the larynx. As it
the pharynx, and a view of the glottis should immediately be
descends, it becomes deeply placed and may lie as much as
apparent (CD Fig. 2-10). This is the critical stage. If the glot-
1.5 in. (4 cm) from the surface at the suprasternal notch.
tis is not visualized, then the operator is viewing the poste-
Remember that in the adult it may measure as much as 1 in.
rior surface of the epiglottis. Now use your anatomic
(2.5 cm) in diameter, but in a 3-year-old child it may
knowledge.
measure only 0.5 in. in diameter. The trachea is a mobile
With the tip of the blade of the laryngoscope applied to
elastic tube and is easily displaced by the enlargement of
the posterior surface of the epiglottis, gently lift up and
adjacent organs or the presence of tumors. Remember also
elevate the epiglottis to expose the glottis. If the glottis is still
that lateral displacement of the cervical part of the trachea
not in view, do not panic! Again use your knowledge of
may be caused by a pathologic lesion in the thorax.
anatomy. With the right free hand grasp the thyroid carti-
lage (to which the cords and the epiglottis are attached) be-
Compromised Airway
tween your finger and thumb and apply firm backward,
upward, rightward pressure (BURP). This maneuver re-
In a medical emergency immediate treatment is necessary.
aligns the box of the larynx relative to the laryngoscopic
Anatomy of Cricothyroidotomy
blade, and the visual axis of the operator and the glottis
should immediately be seen.
In cricothyroidotomy, a tube is inserted in the interval be-
tween the cricoid cartilage and the thyroid cartilage. The
trachea and larynx are steadied by extending the neck over a
Reflex Activity Secondary to
sandbag.
A vertical or transverse incision is made in the skin in
Endotracheal Intubation
the interval between the cartilages (CD Fig. 2-11). The
Stimulation of the mucous membrane of the upper airway
incision is made through the following structures: the skin,
during the process of intubation may produce cardiovascu-
the superficial fascia (beware of the anterior jugular veins,
lar changes such as bradycardia and hypertension. These
which lie close together on either side of the midline), the
The Upper and Lower Airway and Associated Structures
29
A
body of hyoid
thyrohyoid
bone
membrane
(ligament)
sternohyoid
muscle
superior belly of
thyroid cartilage
omohyoid muscle
site of skin
cricothyroid membrane
incision
(ligament)
cricothyroid
cricoid
muscle
cartilage
anterior jugular
vein
isthmus
first tracheal ring
of thyroid
gland
fascia
thyroid
thyroid cartilage
skin
cartilage
edge
cricothyroid
membrane
small
(ligament)
cricothyroid
artery
cricothyroid
membrane
cricoid
(ligament)
cartilage
C
B
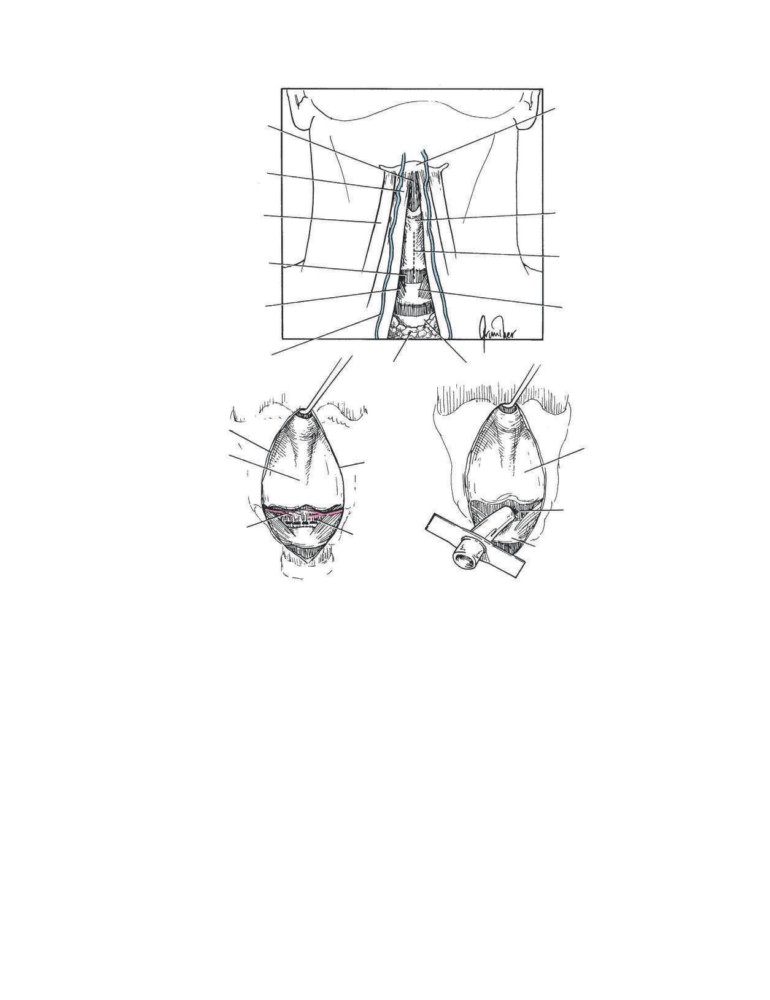
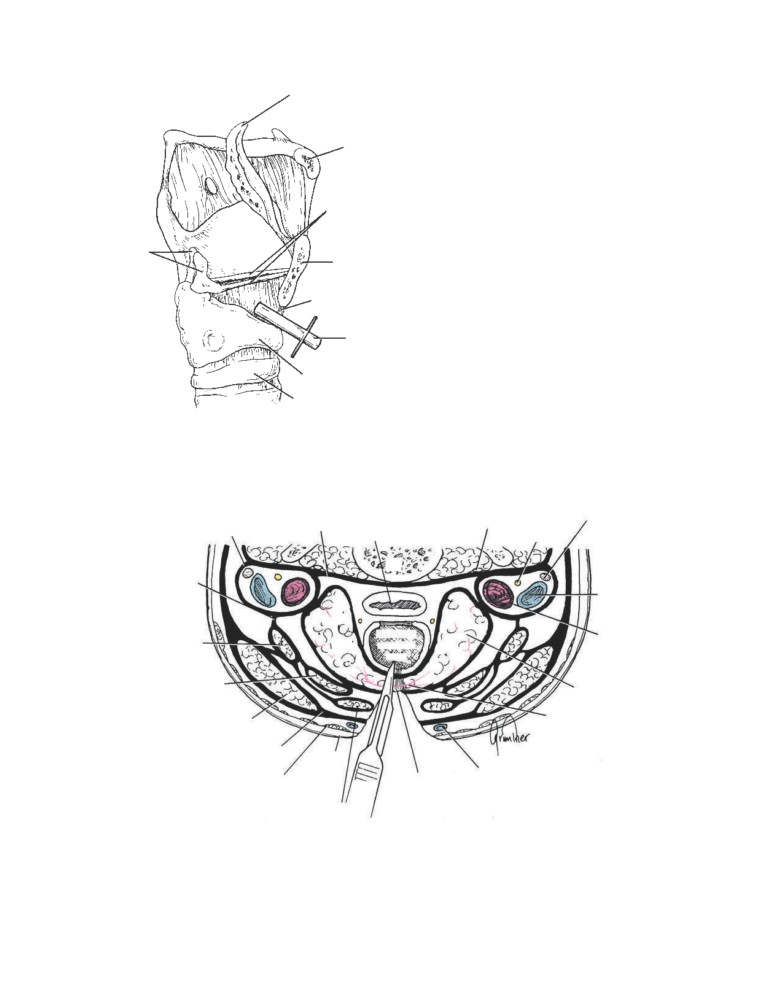
CD Figure 2-11
The anatomy of cricothyroidotomy. A. A vertical incision is made through
the skin and superficial and deep cervical fasciae. B. The cricothyroid membrane (ligament)
is incised through a horizontal incision close to the upper border of the cricoid cartilage.
C. Insertion of the tube.
investing layer of deep cervical fascia, the pretracheal fascia
2. Hemorrhage: The small branches of the superior
(separate the sternohyoid muscles and incise the fascia), and
thyroid artery that occasionally cross the front of the
the larynx. The larynx is incised through a horizontal inci-
cricothyroid membrane to anastomose with one an-
sion through the cricothyroid ligament and the tube in-
other should be avoided.
serted (CD Fig. 2-12).
Anatomy of Tracheostomy
Complications
Tracheostomy is rarely performed and is limited to patients
1. Esophageal perforation: Because the lower end of the
with extensive laryngeal damage and infants with severe air-
pharynx and the beginning of the esophagus lie directly
way obstruction. Because of the presence of major vascular
behind the cricoid cartilage, it is imperative that the
structures (carotid arteries and internal jugular vein), the
scalpel incision through the cricothyroid membrane
thyroid gland, nerves (recurrent laryngeal branch of vagus
not be carried too far posteriorly. This is particularly im-
and vagus nerve), the pleural cavities, and esophagus, metic-
portant in young children, in whom the cross diameter
ulous attention to anatomic detail has to be observed (CD
of the larynx is so small.
Fig. 2-13).
30
Chapter 2
epiglottis
body of hyoid bone
right and left vocal
ligaments (cords)
right and left
arytenoid
thyroid cartilage
cartilages
cricothyroid membrane
or ligament
CD Figure 2-12
View of the interior of
tube
the larynx as seen from the right side (the
right lamina of the thyroid cartilage has
been removed). Note the closeness of the
cricoid cartilage
deep end of the cricothyroidotomy tube to
the vocal cords, especially if the tube is
first tracheal ring
directed upward.
prevertebral
deep cervical
layer of
lymph node
deep cervical
sympathetic
carotid sheath
fascia
trunk
esophagus
vagus nerve
C7
pretracheal
layer of deep
internal
cervical fascia
jugular
vein
common
omohyoid muscle
carotid
artery
sternothyroid muscle
thyroid gland
sternocleidomastoid muscle
branch of superior
thyroid artery
investing layer of
deep cervical fascia
skin
anterior jugular vein
isthmus
platysma muscle
of thyroid
gland
sternohyoid
muscle
CD Figure 2-13
Cross section of the neck at the level of the second tracheal ring. A vertical
incision is made through the ring, and the tracheostomy tube is inserted.
The Upper and Lower Airway and Associated Structures
31
The procedure is as follows:
3. Pneumothorax: The cervical dome of the pleura may
be pierced. This is especially common in children be-
1. The thyroid and cricoid cartilages are identified and the
cause of the high level of the pleura in the neck.
neck is extended to bring the tracheal forward.
4. Esophageal injury: Damage to the esophagus, which is
2. A vertical midline skin incision is made from the region
located immediately posterior to the trachea, occurs
of the cricothyroid membrane inferiorly toward the
most commonly in infants; it follows penetration of the
suprasternal notch.
small-diameter trachea by the point of the scalpel blade.
3. The incision is carried through the superficial fascia
and the fibers of the platysma muscle. The anterior
jugular veins in the superficial fascia are avoided by
SOME IMPORTANT
maintaining a midline position.
AIRWAY DISTANCES
4. The investing layer of deep cervical fascia is incised.
CD Table 2-1 shows some important distances between
5. The pretracheal muscles embedded in the pretracheal
the incisor teeth or nostrils to anatomic landmarks in
fascia are split in the midline two fingerbreadths supe-
the airway in the adult. These approximate figures are
rior to the sternal notch.
helpful in determining the correct placement of an endo-
6. The tracheal rings are then palpable in the midline, or
tracheal tube.
the isthmus of the thyroid gland is visible. If a hook is
placed under the lower border of the cricoid cartilage
and traction is applied upward, the slack is taken out of
CHANGES IN THE
the elastic trachea; this stops it from slipping from side
to side.
TRACHEAL LENGTH
7. A decision is then made as to whether to enter the tra-
chea through the second ring above the isthmus of the
WITH RESPIRATION
thyroid gland; through the third, fourth, or fifth ring by
first dividing the vascular isthmus of the thyroid gland;
AND POSITION OF
or through the lower tracheal rings below the thyroid
isthmus. At the latter site, the trachea is receding from
the surface of the neck, and the pretracheal fascia
THE HEAD AND
contains the inferior thyroid veins and possibly the
thryoidea ima artery.
NECK
8. The preferred site is through the second ring of the tra-
On deep inspiration the carina may descend by as much as
chea in the midline, with the thyroid isthmus retracted
3 cm. Extension of the head and neck, as when maintaining
inferiorly. A vertical tracheal incision is made, and the
an airway in an anesthetized patient, may stretch the trachea
tracheostomy tube is inserted.
and increase its length by 25%.
Complications
Most complications result from not adequately palpating
and recognizing the thyroid, cricoid, and tracheal cartilages
Important Airway
CD Table 2-1
and not confining the incision strictly to the midline.
Distances (Adult)a
1. Hemorrhage: The anterior jugular veins located in the
Distances
superficial fascia close to the midline should be
Airway
(approximate)
avoided. If the isthmus of the thyroid gland is tran-
sected, secure the anastomosing branches of the supe-
Incisor teeth to the vocal cords
5.9 in. (15 cm)
rior and inferior thyroid arteries that cross the midline
Incisor teeth to the carina
7.9 in. (20 cm)
on the isthmus.
External nares to the carina
11.8 in. (30 cm)
2. Nerve paralysis: The recurrent laryngeal nerves may be
aAverage figures given
1-2 cm.
damaged as they ascend the neck in the groove between
the trachea and the esophagus.
32
Chapter 2
Suction Catheters, Endotracheal
THE BRONCHI
Tubes, and the Bronchi
Suction catheters and endotracheal tubes are more likely to
Aspiration of Foreign Bodies and
enter the right more vertical principal bronchus than the
obliquely positioned left principal bronchus in adults and
Stomach Contents
older children.
In adults, foreign bodies and stomach contents tend to be
aspirated into the right principal bronchus, since this is
more in line with the trachea than the left bronchus.
BRONCHOPULMO-
In young babies, since both bronchi arise from the trachea
at equal angles, no predilection for the right bronchus
NARY SEGMENTS
exists.
See CD-ROM Chapter 3.
Clinical Problem Solving Questions
Read the following case histories/questions and give
a hoarse cry. The cough then became croupy, and
the best answer for each.
aphonia occurred. The mother, hearing the commo-
tion, rushed into the room and quickly realized what
1.
A 36-year-old man was taken to the emergency depart-
had happened. She turned the child upside down and
ment after having been found lying unresponsive in a
hit his back several times, but with no effect. The child,
local park with an empty whisky bottle nearby. He was
now in obvious respiratory distress, was rushed to the
given oxygen by an open face mask during the 15-
local emergency department. On examination, he was
minute ride in the ambulance. The paramedic decided
tachypneic, with suprasternal retractions. He was not
to improve the airway by passing a soft nasal tube. On
coughing, and although he attempted to cry, there was
attempting to pass the well-lubricated tube into the
no sound. He would not tolerate being laid down. On
patient’s nose, the paramedic found it impossible to
the basis of your knowledge of the anatomy of the air-
push it much beyond the nasal vestibule on either side.
way, where do you think the foreign body was lodged?
What are the common anatomic causes of obstruction
Describe the normal protective reflexes that exist in the
of the nasal airway?
airway to prevent the inhalation of a foreign body. What
is the anatomic and physiologic rationale behind the
2.
A 12-year-old girl was brought to the hospital with a his-
use of back blows, chest thrusts, and abdominal thrusts
tory of fever, malaise, anorexia, and a sore throat. She
(Heimlich procedure) in the management of upper
also had hoarseness, a cough, and rhinitis. On exami-
airway obstruction? Which of these procedures is most
nation there was erythema of the posterior pharyngeal
appropriate for a 3-year-old child?
wall, with small ulcers on the palatoglossal folds and
soft palate. The tonsils were seen to be red and en-
4.
A 17-year-old boy was driving his minibike at high
larged, and an obvious white-yellow exudate was seen
speed along a country lane, when he suddenly saw what
on the surface of the left tonsil. Examination of the
he thought was a shortcut through a gap in a hedge. He
deep cervical lymph nodes showed enlargement and
did not see that the gap was closed by a strand of barbed
tenderness of the node below and behind the angle of
wire. He struck the wire with his neck and was thrown
the mandible; the enlargement was greatest on the left
from the bicycle. On arrival at the emergency depart-
side. A diagnosis of viral pharyngitis was made. List the
ment, he had all the signs and symptoms of upper air-
various lymphoid organs found in the nasal and oral
way obstruction. Using your knowledge of the anatomy
parts of the pharynx. Explain Waldeyer’s ring.
of the neck, explain the type of injury that could have
3.
A 3-year-old boy was playing with his toys on the floor
occurred in this case. Does the position of the vocal
when his sister decided to share some peanuts with
cords at the time of impact influence the type of injury
him. A few minutes later he started to cough and gave
that occurs? What anatomic factors normally protect
The Upper and Lower Airway and Associated Structures
33
the upper airway from serious blunt injuries? Does age
rior pharyngeal wall. At times, why is it not possible to
play a role in the severity of the injury?
pull the tongue forward in the presence of a fractured
mandible?
5. A 39-year-old man with extensive maxillofacial injuries
following an automobile accident was brought to the
6. When a laryngoscope is passed it is important to align
hospital. Evaluation of the airway revealed partial
the mouth, the oropharynx, and the larynx into one
obstruction. Despite an obvious fractured mandible, an
plane. How do you bring the axes of the oropharynx
attempt was made to move the tongue forward from the
and the larynx in line? How do you bring the axis of
posterior pharyngeal wall by pushing the angles of
the mouth in line with the other axes? Describe the
the mandible forward. This maneuver failed to move
structures in the order that you can view them through
the tongue, and it became necessary to hold the tongue
a laryngoscope from the base of the tongue down to
forward directly in order to pull it away from the poste-
the trachea.
Answers and Explanations
1.
The most common cause for difficulty in passing a
4.
The impact of the wire to the front of the neck caused
nasal tube is a deflected nasal septum. This occurs
hyperextension of the cervical part of the vertebral col-
more commonly in the male, and is thought to be due
umn with stretching of the larynx and trachea. This ef-
to previous trauma to the septum during the period of
fectively fixed the airway structures in the midline so
active growth. Nasal spurs and polyps may cause diffi-
that they were not deflected laterally at the moment of
culty and swelling of the mucous membrane secondary
impact. Under these circumstances the cartilages of the
to infection or chemical irritation, and can also cause
larynx are fractured or crushed. Depending on the
blockage. The widest part of the nasal cavity is near
speed of the impact, the larynx could be completely
the floor.
avulsed from the trachea. In this situation the tone of
the suprahyoid muscles would cause the larynx to be re-
2.
The lymphoid tissue around the openings of the mouth
tracted superiorly and the elasticity of the trachea
and nasal cavities into the pharynx include (1) the pala-
would cause it to retract inferiorly to the root of the neck
tine tonsil, (2) the lingual tonsil, (3) the tubal tonsils,
or behind the sternum.
and (4) the pharyngeal tonsil. For details of Waldeyer’s
ring, see text Chapter 2.
If the glottis were closed at the time of impact,
the raised intraluminal pressure within the upper
3.
The presence of severe respiratory distress with supraster-
airway may contribute to the severity of the injury.
nal retractions and aphonia indicates the presence of up-
The upper airway receives a considerable amount of
per airway obstruction, probably located within the
protection from blows to the front of the neck and
larynx. The airway is protected by a number of important
chest because of the presence of the mandible and
reflexes, including the gag reflex, the laryngeal reflex,
manubrium sterni. With the head and neck in the
and the cough reflex. The gag reflex occurs in response
flexed position, the larynx and trachea are remarkably
to stimulation of the pharyngeal mucous membrane in-
mobile and often deflected laterally by an anterior
nervated by the glossopharyngeal nerve. The laryngeal
blow to the neck.
and the cough reflexes are mediated via the vagus nerve.
These protective reflexes are lost in descending order as
In children, the very flexible nature of the laryngeal and
a patient loses consciousness.
tracheal cartilages and looseness of the supporting con-
nective tissue reduce the likelihood of severe damage to
All maneuvers that are directed toward freeing an ob-
these structures.
struction of the airway by an inhaled foreign body are
based on an attempt to increase the intrathoracic pres-
5.
The root of the tongue is attached anteriorly to the
sure by compressing the intrathoracic gas volume, so
mental spines on the posterior surface of the symph-
that the foreign body is expressed from the mouth. The
ysis menti of the mandible by the right and left
underlying mechanisms involved in the use of back
genioglossus muscles. If this bony origin were floating
blows, chest thrusts, and abdominal thrusts are dis-
because of fractures on both sides of the body of
cussed in this CD chapter. It is now generally agreed
the mandible, pulling the angles of the mandible for-
that the best and safest method to use on a 3-year-old
ward would have no effect on the position of the
child is the abdominal thrust.
tongue.
34
Chapter 2
6. The axis of the oropharynx and the larynx are brought
side of the median fold; (3) the upper edge of the
into direct line by flexing the cervical part of the verte-
epiglottis and the opening into the larynx, bounded in
bral column. The axis of the mouth is brought in line
front by the epiglottis with its tubercle and laterally by
with the oropharynx by extending the atlantooccipital
the aryepiglottic folds—the rounded elevations of
joints.
the cuneiform and corniculate cartilages in the folds
can be recognized; (4) the reddish fixed vestibular folds;
The following structures may be viewed: (1) the base of
(5) the whitish mobile vocal cords; and (6) below the
the tongue; (2) the median glossoepiglottic fold, the two
glottis the interior of the trachea with the upper two or
lateral glossoepiglottic folds, and the valleculae on each
three rings.
The Chest Wall, Chest
Cavity, Lungs, and
Pleural Cavities
3
Chapter Outline
The Chest Wall
37
Lymph Drainage of the Thoracic Wall
43
Sternum and Marrow Biopsy
37
The Breasts
43
The Ribs
37
Witch’s Milk in the Newborn
43
Cervical Rib
37
Breast Examination
43
Rib Excision
37
Mammography
43
The Intercostal Nerves
37
Supernumerary and Retracted Nipples
44
Skin Innervation of the Chest Wall and
The Importance of Fibrous Septa
44
Referred Pain
37
Lymph Drainage and Carcinoma of the Breast
45
Herpes Zoster
38
Congenital Anomalies of the Breast
45
Anatomy of Intercostal Nerve Block
38
Polythelia
45
Area of Anesthesia
38
Retracted Nipple or Inverted Nipple
45
Indications
38
Procedure
38
Micromastia
45
Anatomy of Complications
39
Macromastia
45
The Sternum, Ribs, and Costal Cartilages
39
Gynecomastia
46
Chest Cage Distortion
39
The Mediastinum
46
Chest Trauma
39
Deflection of Mediastinum
46
Mechanics of Chest Trauma
39
Mediastinitis
46
Rib Contusion
39
Rib Fractures
39
Mediastinal Tumors or Cysts
46
Flail Chest
39
Mediastinoscopy
46
Fractured Sternum
39
Traumatic Injury to the Back of the Chest
40
The Pleura
46
Traumatic Injury to the Chest and Abdominal
Pleural Fluid
46
Viscera
40
Pleurisy
46
The Diaphragm
40
Pneumothorax
46
Hiccup
40
Spontaneous Pneumothorax
46
Paralysis of the Diaphragm
40
Open Pneumothorax
47
Tension Pneumothorax
47
Penetrating Injuries of the Diaphragm
40
Fluid in the Pleural Cavity
47
Rupture of the Diaphragm
41
Pleural Effusion
47
Congenital Anomalies of the Diaphragm
41
Hydropneumothorax
47
Pyopneumothorax
47
Congenital Herniae
41
Hemopneumothorax
48
Acquired Herniae
41
Empyema
48
Internal Thoracic Artery in the Treatment
Position of Thoracic and Upper
of Coronary Artery Disease
41
Abdominal Viscera during Different
Phases of Respiration
49
The Clavicle and Its Relationship with the
Thoracic Outlet
41
Root of the Neck Injuries
49
The Thoracic Outlet Syndromes
41
Traumatic Asphyxia
49
The Adson Maneuver
42
Cardiopulmonary Resuscitation
49
The Chest Wall, Chest Cavity, Lungs, and Pleural Cavities
37
The Chest Wall
49
Segmental Resection of the Lung
54
Thoracocentesis
49
Pulmonary Contusion
54
Needle Thoracostomy
49
Tracheobronchial Injury
54
Anterior Approach
49
Bronchogenic Carcinoma
54
Lateral Approach
49
Conditions That Decrease Respiratory Efficiency
54
Tube Thoracostomy
50
Constriction of the Bronchi (Bronchial Asthma)
54
Thoracotomy
50
Loss of Lung Elasticity
54
Loss of Lung Distensibility
54
The Trachea and Principal Bronchi
51
Postural Drainage
54
Compression of the Trachea
51
Tracheitis or Bronchitis
51
Congenital Anomalies of the Trachea
and Lungs
55
Inhaled Foreign Bodies
51
Esophageal Atresia and Tracheoesophageal Fistula
55
Bronchoscopy
51
Neonatal Lobar Emphysema
55
The Lungs
51
Congenital Cysts of the Lung
55
Clinical Examination of the Chest
51
Trauma to the Lungs
53
Clinical Problem Solving Questions
56
Fractured Ribs and the Lungs
53
Answers and Explanations
58
Pain and Lung Disease
53
Surgical Access to the Lungs
54
also exert pressure on the overlying subclavian artery and
THE CHEST WALL
interfere with the circulation of the upper limb.
Rib Excision
Sternum and Marrow Biopsy
Rib excision is commonly performed by thoracic surgeons
Since the sternum possesses red hematopoietic marrow
wishing to gain entrance to the thoracic cavity. A longitudi-
throughout life, it is a common site for marrow biopsy.
nal incision is made through the periosteum on the outer
Under a local anesthetic, a wide-bore needle is introduced
surface of the rib and a segment of the rib is removed. A sec-
into the marrow cavity through the anterior surface of the
ond longitudinal incision is then made through the bed of
bone. The sternum may also be split at operation to allow
the rib, which is the inner covering of periosteum. After the
the surgeon to gain easy access to the heart, great vessels,
operation, the rib regenerates from the osteogenetic layer of
and thymus.
the periosteum.
THE RIBS
THE INTERCOSTAL
Cervical Rib
NERVES
A cervical rib (i.e., a rib arising from the anterior tubercle of
the transverse process of the seventh cervical vertebra)
Skin Innervation of the Chest
occurs in about 0.5% of humans (CD Fig. 3-1). It may have
a free anterior end, may be connected to the first rib by a
Wall and Referred Pain
fibrous band, or may articulate with the first rib. The
importance of a cervical rib is that it can cause pressure on
Above the level of the sternal angle, the cutaneous innerva-
the lower trunk of the brachial plexus in some patients,
tion of the anterior chest wall is derived from the supraclav-
producing pain down the medial side of the forearm and
icular nerves (C3 and 4). Below this level, the anterior and
hand and wasting of the small muscles of the hand. It can
lateral cutaneous branches of the intercostal nerves supply
38
Chapter 3
scalenus medius
brachial plexus
cervical rib
CD Figure 3-1
Thoracic outlet as
seen from above. Note the pres-
ence of the cervical ribs (black) on
scalenus anterior
lower trunk of plexus
both sides. On the right side of the
thorax, the rib is almost complete
and articulates anteriorly with the
first rib. On the left side of the tho-
rax, the rib is rudimentary but is
subclavian artery
continued forward as a fibrous
band that is attached to the first
cervical rib
costal cartilage. Note that the cervi-
fibrous band
cal rib may exert pressure on the
lower trunk of the brachial plexus
and may kink the subclavian artery.
oblique bands of skin in regular sequence. The skin on the
the distribution of the sensory neuron in a thoracic spinal
posterior surface of the chest wall is supplied by the posterior
nerve, followed in a few days by a skin eruption. The
rami of the spinal nerves. The arrangement of the der-
condition occurs most frequently in patients older than
matomes is shown in CD Figures 1-2 and 1-3.
50 years.
An intercostal nerve supplies not only areas of skin but
also the ribs, costal cartilages, intercostal muscles, and the
Anatomy of Intercostal Nerve Block
parietal pleura lining the intercostal space. Furthermore,
the seventh to eleventh intercostal nerves leave the thoracic
Area of Anesthesia
wall and enter the anterior abdominal wall so that they, in
addition, supply dermatomes on the anterior abdominal
The skin and the parietal pleura cover the outer and inner
wall, muscles of the anterior abdominal wall, and parietal
surfaces of each intercostal space, respectively; the seventh
peritoneum. This latter fact is of great clinical importance
to eleventh intercostal nerves supply the skin and the pari-
because it means that disease in the thoracic wall may be re-
etal peritoneum covering the outer and inner surfaces of the
vealed as pain in a dermatome that extends across the costal
abdominal wall, respectively. Therefore, an intercostal
margin into the anterior abdominal wall. For example, a
nerve block will also anesthetize these areas. In addition, the
pulmonary thromboembolism or pneumonia with pleurisy
periosteum of the adjacent ribs is anesthetized.
involving the costal parietal pleura could give rise to ab-
Indications
dominal pain and tenderness and rigidity of the abdominal
musculature. The abdominal pain in these instances is
Intercostal nerve block is indicated for repair of lacerations
called referred pain.
of the thoracic and abdominal walls, for relief of pain in rib
fractures, and to allow pain-free respiratory movements.
Herpes Zoster
Procedure
Herpes zoster, or shingles, is a relatively common condi-
tion caused by the reactivation of the latent varicella-zoster
To produce analgesia of the anterior and lateral thoracic
virus in a patient who has previously had chickenpox. The
and abdominal walls, the intercostal nerve should be
lesion is seen as an inflammation and degeneration of
blocked before the lateral cutaneous branch arises at the
the sensory neuron in a cranial or spinal nerve with the for-
midaxillary line. The ribs may be identified by counting
mation of vesicles and inflammation of the skin. In the
down from the second (opposite sternal angle) or up
thorax, the first symptom is a band of dermatomal pain in
from the twelfth. The needle is directed toward the rib
The Chest Wall, Chest Cavity, Lungs, and Pleural Cavities
39
near the lower border (Text Fig. 3-4) and the tip comes to
Rib Contusion
rest near the subcostal groove, where the local anesthetic is
Bruising of a rib, secondary to trauma, is the most common
infiltrated around the nerve. Remember that the order of
rib injury. In this painful condition, a small hemorrhage
structures lying in the neurovascular bundle from above
occurs beneath the periosteum.
downward is intercostal vein, artery, and nerve and that
these structures are situated between the posterior inter-
costal membrane of the internal intercostal muscle and
Rib Fractures
the parietal pleura. Furthermore, laterally the nerve lies
Fractures of the ribs are common chest injuries. In chil-
between the internal intercostal muscle and the innermost
dren, the ribs are highly elastic, and fractures in this age
intercostal muscle.
group are therefore rare. Unfortunately, the pliable chest
wall in the young can be easily compressed so that the un-
Anatomy of Complications
derlying lungs and heart may be injured. With increasing
Complications include pneumothorax and hemorrhage.
age, the rib cage becomes more rigid, owing to the deposit
Pneumothorax can occur if the needle point misses
of calcium in the costal cartilages, and the ribs become
the subcostal groove and penetrates too deeply through the
brittle. The ribs then tend to break at their weakest part,
parietal pleura.
their angles.
Hemorrhage is caused by the puncture of the intercostal
The ribs prone to fracture are those that are exposed or
blood vessels. This is a common complication, so aspiration
relatively fixed. Ribs five through 10 are the most commonly
should always be performed before injecting the anesthetic.
fractured ribs. The first four ribs are protected by the clavi-
A small hematoma may result.
cle and pectoral muscles anteriorly and by the scapula and
its associated muscles posteriorly. The eleventh and twelfth
ribs float and move with the force of impact.
Because the rib is sandwiched between the skin exter-
THE STERNUM,
nally and the delicate pleura internally, it is not surprising
that the jagged ends of a fractured rib may penetrate the
lungs and present as a pneumothorax.
RIBS, AND COSTAL
Severe localized pain is usually the most important
symptom of a fractured rib. The periosteum of each rib is in-
CARTILAGES
nervated by the intercostal nerves above and below the rib.
To encourage the patient to breathe adequately, it may be
necessary to relieve the pain by performing an intercostal
Chest Cage Distortion
nerve block.
The shape of the thorax can be distorted by congenital
anomalies of the vertebral column or by the ribs. Destruc-
Flail Chest
tive disease of the vertebral column that produces lateral
In severe crush injuries, a number of ribs may break. If lim-
flexion or scoliosis results in marked distortion of the tho-
ited to one side, the fractures may occur near the rib angles
racic cage.
and anteriorly near the costochondral junctions. This
causes flail chest, in which a section of the chest wall is
Chest Trauma
disconnected to the rest of the thoracic wall. If the fractures
occur on either side of the sternum, the sternum may be
Traumatic injury to the thorax is common, especially as a re-
flail. In either case, the stability of the chest wall is lost, and
sult of automobile accidents.
the flail segment is sucked in during inspiration and driven
out during expiration, producing paradoxic and ineffective
Mechanics of Chest Trauma
respiratory movements (CD Fig. 3-2).
Chest organ injuries from blunt trauma occur as the result
of rapid acceleration or deceleration, by compression, or
Fractured Sternum
by a sudden increase in intrathoracic or intraabdominal
pressure. A knife wound piercing the chest wall injures the
The sternum is a resilient structure that is held in position
organs along its path. A bullet wound does not follow a
by relatively pliable costal cartilages and bendable ribs. For
straight path but yaws, tumbles, and may fragment, causing
these reasons, fracture of the sternum is not common; how-
widespread tissue damage. In addition, the kinetic energy
ever, it does occur in high-speed motor vehicle accidents.
generated by a speeding bullet may damage tissue that is
Remember that the heart lies posterior to the sternum and
distant from the actual path of the bullet.
may be severely contused by the sternum on impact.
40
Chapter 3
spinal cord should be considered. Remember also the pres-
ence of the scapula, which overlies the upper seven ribs.
This bone is covered with muscles and is fractured only in
cases of severe trauma.
Traumatic Injury to the Chest and
Abdominal Viscera
When the anatomy of the thorax is reviewed, it is important
to remember that the upper abdominal organs—namely,
the liver, stomach, and spleen—may be injured by trauma
to the rib cage. In fact, any injury to the chest below the level
of the nipple line may involve abdominal organs as well as
chest organs.
inspiration
THE DIAPHRAGM
Hiccup
Hiccup is the involuntary spasmodic contraction of the di-
aphragm accompanied by the approximation of the vocal
folds and closure of the glottis of the larynx. It is a common
condition in normal individuals and occurs after eating or
drinking as a result of gastric irritation of the vagus nerve
endings. It may, however, be a symptom of disease such as
pleurisy, peritonitis, pericarditis, or uremia.
Paralysis of the Diaphragm
A single dome of the diaphragm may be paralyzed by
crushing or sectioning of the phrenic nerve in the neck.
This may be necessary in the treatment of certain forms of
expiration
lung tuberculosis, when the physician wishes to rest the
lower lobe of the lung on one side. Occasionally, the con-
tribution from the fifth cervical spinal nerve joins the
phrenic nerve late as a branch from the nerve to the sub-
CD Figure 3-2
Flail chest is a condition in which a portion of
clavius muscle. This is known as the accessory phrenic
the chest wall is drawn inward during inspiration and bulges
outward during expiration; it occurs when several ribs are
nerve. To obtain complete paralysis under these circum-
fractured in two or more places. A. On inspiration the frac-
stances, the nerve to the subclavius muscle must also be
tured ribs are pulled inward as the pressure within the chest
sectioned.
decreases. The inspired air passing down the trachea tends
to be drawn into the lung on the unaffected side. B. On expi-
ration the fractured ribs are pushed outward as the pressure
Penetrating Injuries of
within the chest rises. Note that some of the air in the bronchi
tends to enter the lung on the affected side as well as passing
up the trachea.
the Diaphragm
Penetrating injuries can result from stab or bullet wounds
to the chest or abdomen. Any penetrating wound to the
Traumatic Injury to the Back of the
chest below the level of the nipples should be suspected
Chest
of causing damage to the diaphragm until proved other-
The posterior wall of the chest in the midline is formed by
wise. The arching domes of the diaphragm can reach
the vertebral column. In severe posterior chest injuries, the
the level of the fifth rib (the right dome can reach a
possibility of a vertebral fracture with associated injury to the
higher level).
The Chest Wall, Chest Cavity, Lungs, and Pleural Cavities
41
Rupture of the Diaphragm
INTERNAL THOR-
In severe crushing injuries to the chest or abdomen, the di-
aphragm may rupture, usually through the central tendon.
ACIC ARTERY IN
Herniation of abdominal viscera into the thorax may occur,
especially if the left dome of the diaphragm is the site of the
THE TREATMENT
rupture. The rupture of the right dome or the central tendon
is usually plugged by the large right lobe of the liver, unless
OF CORONARY
the opening is very great. A ruptured diaphragm, if not re-
paired, may result in a delayed herniation of abdominal
contents.
ARTERY DISEASE
In patients with occlusive coronary disease caused by ather-
osclerosis, the diseased arterial segment can be bypassed by
CONGENITAL
inserting a graft. The graft most commonly used is the great
saphenous vein of the leg. In some patients, the my-
ANOMALIES OF
ocardium can be revascularized by surgically mobilizing
one of the internal thoracic arteries and joining its distal cut
end to a coronary artery.
THE DIAPHRAGM
THE CLAVICLE
Congenital Herniae
Congenital herniae may occur as the result of incomplete
AND ITS
fusion of the septum transversum, the dorsal mesentery, and
the pleuroperitoneal membranes from the body wall. The
herniae occur at the following sites: (1) the pleuroperitoneal
RELATIONSHIP
canal (more common on the left side; caused by failure of
fusion of the septum transversum with the pleuroperitoneal
WITH THE
membrane), (2) the opening between the xiphoid and costal
origins of the diaphragm, and (3) the esophageal hiatus.
THORACIC OUTLET
Acquired Herniae
The Thoracic Outlet Syndromes
Acquired herniae may occur in middle-aged people with
The brachial plexus of nerves (C5, 6, 7, and 8 and T1) and
weak musculature around the esophageal opening in the
the subclavian artery and vein are closely related to the
diaphragm. These herniae may be either sliding or parae-
upper surface of the first rib and the clavicle as they enter
sophageal (CD Fig. 3-3).
the upper limb see (see CD Fig. 3-4). It is here that the
esophagus
diaphragm
stomach
stomach
peritoneum
CD Figure 3-3
A. Sliding esophageal hernia. B. Parae-
A
B
sophageal hernia.
42
Chapter 3
brachial plexus
subclavian artery
first rib
clavicle
axillary artery
first rib
part of
brachial plexus
subclavian artery
axillary artery
axillary
artery
pectoralis
minor
CD Figure 3-4
Examples of thoracic outlet syndrome. A. The relationship between the
brachial plexus, the subclavian and axillary arteries, the clavicle, the first rib, and the pec-
toralis minor tendon. B. How the cords of the brachial plexus and the subclavian artery can
be squeezed between the clavicle and the first rib in some individuals. C. How the axillary
artery and the branches of the brachial plexus might be pressed upon by the pectoralis
minor tendon when the arm is abducted at the shoulder joint.
nerves or blood vessels may be compressed between
The Adson Maneuver
the bones. Most of the symptoms are caused by pressure on
the lower trunk of the plexus producing pain down the me-
This maneuver was commonly used in making the diagno-
dial side of the forearm and hand and wasting of the small
sis of thoracic outlet syndrome; recently the reliability of the
muscles of the hand. Pressure on the blood vessels may
test has been questioned. The patient takes a deep breath
compromise the circulation of the upper limb. Examples of
(raises the first rib), extends the neck (takes up the slack of
the thoracic outlet syndromes are shown in CD Fig. 3-4.
the brachial nerve plexus and subclavian vessels), and turns
The Chest Wall, Chest Cavity, Lungs, and Pleural Cavities
43
his or her chin to the side being examined (narrows the in-
of the duct epithelium and the surrounding connective tis-
terval between the scalene muscles); at the same time the
sue. This proliferation may cause swelling of the mammary
pulse of the radial artery is palpated. Disappearance or re-
glands in both sexes during the first week of life; in some
duction of the pulse, and possibly coldness and paleness of
cases a milky fluid, called witch’s milk, may be expressed
the hand, would indicate that the subclavian artery is being
from the nipples. The condition is resolved spontaneously as
compressed by the scalene muscles and/or the first (or cer-
the maternal hormone levels in the child fall.
vical) rib. In addition to looking for vascular compromise,
the physician should also look for replication of the nerve
Breast Examination
symptoms down the arm.
The breast is one of the common sites of cancer in women.
It is also the site of different types of benign tumors and may
LYMPH DRAINAGE
be subject to acute inflammation and abscess formation.
For these reasons, clinical personnel must be familiar
with the development, structure, and lymph drainage of
OF THE THORACIC
this organ.
With the patient undressed to the waist and sitting up-
WALL
right, the breasts are first inspected for symmetry. Some de-
gree of asymmetry is common and is the result of unequal
The lymph drainage of the skin of the anterior chest wall
breast development. Any swelling should be noted. A
passes to the anterior axillary lymph nodes; that from the
swelling can be caused by an underlying tumor, cyst, or ab-
posterior chest wall passes to the posterior axillary nodes
scess formation. The nipples should be carefully examined
(CD Fig. 3-5). The lymph drainage of the intercostal spaces
for evidence of retraction. A carcinoma within the breast
passes forward to the internal thoracic nodes, situated along
substance can cause retraction of the nipple by pulling on
the internal thoracic artery, and posteriorly to the posterior
the lactiferous ducts. The patient is then asked to lie down
intercostal nodes and the paraaortic nodes in the posterior
so that the breasts can be palpated against the underlying
mediastinum. The lymphatic drainage of the breast is
thoracic wall. Finally, the patient is asked to sit up again and
described in the next section.
raise both arms above her head. With this maneuver, a car-
cinoma tethered to the skin, the suspensory ligaments, or
the lactiferous ducts produces dimpling of the skin or re-
traction of the nipple.
THE BREASTS
Mammography
Witch’s Milk in the Newborn
Mammography is a radiographic examination of the breast
While the fetus is in the uterus, the maternal and placental
(CD Fig. 3-6). This technique is extensively used for screen-
hormones cross the placental barrier and cause proliferation
ing the breasts for benign and malignant tumors and cysts.
posterior
anterior axillary
axillary
nodes
lymph
nodes
watershed
superficial
CD Figure 3-5
Lymph drainage of the skin of the
inguinal
thorax and abdomen. Note that levels of the umbili-
lymph
cus anteriorly and iliac crests posteriorly may be
nodes
regarded as watersheds for lymph flow.
44
Chapter 3
skin
dense
fibrous
septa
nipple
CD Figure 3-6
Mediolateral
mammogram showing the glan-
glandular tissue supported
dular tissue supported by the
by connective tissue
connective tissue septa.
Extremely low doses of x-rays are used so that the dangers are
may result in a mistaken diagnosis of warts or moles. A long-
minimal and the examination can be repeated often. Its suc-
standing retracted nipple is a congenital deformity caused by
cess is based on the fact that a lesion measuring only a few
a failure in the complete development of the nipple. A re-
millimeters in diameter can be detected long before it is felt
tracted nipple of recent occurrence is usually caused by an
by clinical examination.
underlying carcinoma pulling on the lactiferous ducts.
Supernumerary and
The Importance of Fibrous Septa
The interior of the breast is divided into 15 to 20 compart-
Retracted Nipples
ments that radiate from the nipple by fibrous septa that ex-
Supernumerary nipples occasionally occur along a line ex-
tend from the deep surface of the skin. Each compartment
tending from the axilla to the groin; they may or may not be
contains a lobe of the gland. Normally, the skin feels
associated with breast tissue. This minor congenital anomaly
completely mobile over the breast substance. However,
The Chest Wall, Chest Cavity, Lungs, and Pleural Cavities
45
should the fibrous septa become involved in a scirrhous car-
This means that the breast and the associated structures con-
cinoma or in a disease such as a breast abscess, which results
taining the lymph vessels and nodes must be removed en
in the production of contracting fibrous tissue, the septa will
bloc. The excised mass is therefore made up of the follow-
be pulled on, causing dimpling of the skin. The fibrous
ing: a large area of skin overlying the tumor and including
septa are sometimes referred to as the suspensory ligaments
the nipple; all the breast tissue; the pectoralis major and
of the mammary gland.
associated fascia through which the lymph vessels pass to the
An acute infection of the mammary gland may occur
internal thoracic nodes; the pectoralis minor and associated
during lactation. Pathogenic bacteria gain entrance to the
fascia related to the lymph vessels passing to the axilla; all
breast tissue through a crack in the nipple. Because of
the fat, fascia, and lymph nodes in the axilla; and the fascia
the presence of the fibrous septa, the infection remains
covering the upper part of the rectus sheath, the serratus
localized to one compartment or lobe in the beginning.
anterior, the subscapularis, and the latissimus dorsi muscles.
Abscesses should be drained through a radial incision to
The axillary blood vessels, the brachial plexus, and the
avoid spreading of the infection into neighboring compart-
nerves to the serratus anterior and the latissimus dorsi are
ments; a radial incision also minimizes the damage to the
preserved. Some degree of postoperative edema of the arm
radially arranged ducts.
is likely to follow such a radical removal of the lymph vessels
draining the upper limb.
A modified form of radical mastectomy for patients with
Lymph Drainage and Carcinoma
clinically localized cancer is also a common procedure and
consists of a simple mastectomy in which the pectoral mus-
of the Breast
cles are left intact. The axillary lymph nodes, fat, and fascia
The importance of knowing the lymph drainage of the
are removed. This procedure removes the primary tumor
breast in relation to the spread of cancer from that organ
and permits pathologic examination of the lymph nodes for
cannot be overemphasized. The lymph vessels from the
possible metastases.
medial quadrants of the breast pierce the second, third,
and fourth intercostal spaces and enter the thorax to drain
into the lymph nodes alongside the internal thoracic
CONGENITAL
artery. The lymph vessels from the lateral quadrants of the
breast drain into the anterior or pectoral group of axillary
nodes. It follows, therefore, that a cancer occurring in the
ANOMALIES OF
lateral quadrants of the breast tends to spread to the axillary
nodes. Thoracic metastases are difficult or impossible to
THE BREAST
treat, but the lymph nodes of the axilla can be removed
surgically.
Approximately 60% of carcinomas of the breast occur
Polythelia
in the upper lateral quadrant. The lymphatic spread of
Supernumerary nipples occasionally occur along a line cor-
cancer to the opposite breast, to the abdominal cavity, or
responding to the position of the milk ridge. They are liable
into lymph nodes in the root of the neck is caused by
to be mistaken for moles.
obstruction of the normal lymphatic pathways by malig-
nant cells or destruction of lymph vessels by surgery or
radiotherapy. The cancer cells are swept along the lymph
Retracted Nipple or Inverted Nipple
vessels and follow the lymph stream. The entrance of can-
cer cells into the blood vessels accounts for the metastases
Retracted nipple is a failure in the development of the nip-
in distant bones.
ple during its later stages. It is important clinically, because
In patients with localized cancer of the breast, most sur-
normal suckling of an infant cannot take place, and the nip-
geons do a simple mastectomy or a lumpectomy, followed
ple is prone to infection.
by radiotherapy to the axillary lymph nodes and/or hormone
therapy. In patients with localized cancer of the breast with
Micromastia
early metastases in the axillary lymph nodes, most authori-
ties agree that radical mastectomy offers the best chance of
An excessively small breast on one side occasionally occurs,
cure. In patients in whom the disease has already spread be-
resulting from lack of development.
yond these areas (e.g., into the thorax), simple mastectomy,
followed by radiotherapy or hormone therapy, is the treat-
Macromastia
ment of choice.
Radical mastectomy is designed to remove the primary
Diffuse hypertrophy of one or both breasts occasionally oc-
tumor and the lymph vessels and nodes that drain the area.
curs at puberty in otherwise normal girls.
46
Chapter 3
opening the pleural cavities. A small incision is made in the
Gynecomastia
midline in the neck just above the suprasternal notch, and
the superior mediastinum is explored down to the region of
Unilateral or bilateral enlargement of the male breast occa-
the bifurcation of the trachea. The procedure can be used to
sionally occurs, usually at puberty. The cause is unknown,
determine the diagnosis and degree of spread of carcinoma
but the condition is probably related to some form of hor-
of the bronchus.
monal imbalance.
THE PLEURA
THE MEDIASTINUM
Pleural Fluid
Deflection of Mediastinum
The pleural space normally contains 5 to 10 mL of clear
In the cadaver, the mediastinum, as the result of the hard-
fluid, which lubricates the apposing surfaces of the visceral
ening effect of the preserving fluids, is an inflexible, fixed
and parietal pleurae during respiratory movements. The
structure. In the living, it is very mobile; the lungs, heart,
formation of the fluid results from hydrostatic and osmotic
and large arteries are in rhythmic pulsation, and the esoph-
pressures. Since the hydrostatic pressures are greater in the
agus distends as each bolus of food passes through it.
capillaries of the parietal pleura than in the capillaries of
If air enters the pleural cavity (a condition called pneu-
the visceral pleura (pulmonary circulation), the pleural
mothorax), the lung on that side immediately collapses and
fluid is normally absorbed into the capillaries of the vis-
the mediastinum is displaced to the opposite side. This con-
ceral pleura. Any condition that increases the production
dition reveals itself by the patient’s being breathless and in a
of the fluid
(e.g., inflammation, malignancy, congestive
state of shock; on examination, the trachea and the heart are
heart disease) or impairs the drainage of the fluid (e.g., col-
found to be displaced to the opposite side.
lapsed lung) results in the abnormal accumulation of fluid,
called a pleural effusion. The presence of 300 mL of fluid
Mediastinitis
in the costodiaphragmatic recess in an adult is sufficient to
enable its clinical detection. The clinical signs include de-
The structures that make up the mediastinum are embed-
creased lung expansion on the side of the effusion, with
ded in loose connective tissue that is continuous with that of
decreased breath sounds and dullness on percussion over
the root of the neck. Thus, it is possible for a deep infection
the effusion.
of the neck to spread readily into the thorax, producing a
mediastinitis. Penetrating wounds of the chest involving the
Pleurisy
esophagus may produce a mediastinitis. In esophageal per-
forations, air escapes into the connective tissue spaces and
Inflammation of the pleura (pleuritis or pleurisy), sec-
ascends beneath the fascia to the root of the neck, produc-
ondary to inflammation of the lung (e.g., pneumonia),
ing subcutaneous emphysema.
results in the pleural surfaces becoming coated with inflam-
matory exudate, causing the surfaces to be roughened. This
Mediastinal Tumors or Cysts
roughening produces friction, and a pleural rub can be
heard with the stethoscope on inspiration and expiration.
Because many vital structures are crowded together within
Often the exudate becomes invaded by fibroblasts, which
the mediastinum, their functions can be interfered with by
lay down collagen and bind the visceral pleura to the pari-
an enlarging tumor or organ. A tumor of the left lung can
etal pleura, forming pleural adhesions.
rapidly spread to involve the mediastinal lymph nodes,
which on enlargement may compress the left recurrent la-
Pneumothorax
ryngeal nerve, producing paralysis of the left vocal fold. An
expanding cyst or tumor can partially occlude the superior
As a result of disease or injury (stab or gunshot wounds), air
vena cava, causing severe congestion of the veins of the up-
can enter the pleural cavity from the lungs or through the
per part of the body. Other pressure effects can be seen on
chest wall (pneumothorax).
the sympathetic trunks, phrenic nerves, and sometimes the
trachea, main bronchi, and esophagus.
Spontaneous Pneumothorax
A spontaneous pneumothorax is a condition in which air
Mediastinoscopy
enters the pleural cavity suddenly without its cause being
Mediastinoscopy is a diagnostic procedure whereby speci-
immediately apparent. After investigation, it is usually found
mens of tracheobronchial lymph nodes are obtained without
that air has entered from a diseased lung and a bulla (bleb)
The Chest Wall, Chest Cavity, Lungs, and Pleural Cavities
47
has ruptured. The resulting signs of pneumothorax are ab-
sent or diminished breath sounds over the affected lung and
deflection of the trachea to the opposite side.
Open Pneumothorax
Open pneumothorax occurs when the air enters the pleural
cavity through an opening in the chest wall and may result
from stab or bullet wounds (CD Fig. 3-7). Sucking pneu-
mothorax occurs when the hole in the chest wall is larger
than the glottis. With each inspiration the negative pressure
created is more effective at sucking air in through the chest
wound than air entering through the glottis; this produces a
sucking sound. The lung cannot be expanded, and respira-
tion is compromised.
Tension Pneumothorax
inspiration
Tension pneumothorax occurs when air is sucked into the
pleural cavity through a chest wound with each inspiration
but does not escape (CD Fig. 3-8). This can occur as the
result of clothing and/or the layers of the chest wall com-
bining to form a valve so that air enters on inspiration but
cannot exit through the wound. In these circumstances,
the air pressure builds up on the wounded side and pushes
the mediastinum progressively over to the opposite side.
Because of the anatomic thin walls of the great veins (vena
cavae) and the atria of the heart, the increase in air pres-
sure within the chest cavity interferes with blood return
to the heart; the patient may die because of lack of venous
return. The clinical signs are hypertension, hyperreso-
nance to percussion on the affected side, the engorgement
of the neck veins, and the evidence of mediastinal deflec-
tion. Eventually, hypotension (secondary to lack of venous
return) results. The treatment is immediate decompres-
expiration
sion of the affected side by the insertion of a needle thora-
costomy.
Fluid in the Pleural Cavity
CD Figure 3-7
Open pneumothorax without tension. A. On
inspiration air is drawn in through the wound in the chest
wall at atmospheric pressure, and the lung partially or com-
Pleural Effusion
pletely collapses (depending on the size of the hole in the
chest wall) from its own inherent elasticity; the mediastinum
The presence of fluid in the cavity is referred to as a pleural
is deflected to the opposite side. B. On expiration air passes
effusion. Fluid (serous, blood, or pus) can be drained from
out of the chest wound as the diaphragm rises and the
the pleural cavity through a wide-bore needle, as described
mediastinum is deflected to the same side. With large chest
later in this section.
openings (larger than the cross-sectional area of trachea), air
will preferentially use the hole in the chest wall rather than
passing up and down the trachea, and respiratory ventilation
Hydropneumothorax
will cease.
Air in the pleural cavity associated with serous fluid is
known as hydropneumothorax.
Pyopneumothorax
Air in the pleural cavity associated with pus is known as
pyopneumothorax.
48
Chapter 3
CD Figure 3-8
Tension pneumothorax. A. Following penetration of the chest wall, cloth-
ing and/or tissue create a valve-like mechanism that permits air entry into the pleural space
during inspiration but prevents exit during expiration. B. The lung collapses on the
wounded side and the buildup of air pressure with each respiration causes severe deflec-
tion of the mediastinum to the opposite side. C. Spontaneous pneumothorax with air
entering the pleural space through a ruptured bulla; the lung collapses and the mediastinum
is deflected to the opposite side.
Hemopneumothorax
Empyema
Air in the pleural cavity associated with blood is known as
A collection of pus (without air) within the pleural cavity is
hemopneumothorax.
called an empyema.
The Chest Wall, Chest Cavity, Lungs, and Pleural Cavities
49
POSITION OF
CARDIOPULMONARY
THORACIC AND
RESUSCITATION
Cardiopulmonary resuscitation (CPR), achieved by compres-
UPPER ABDOMINAL
sion of the chest, was originally believed to succeed because
of the compression of the heart between the sternum and the
VISCERA DURING
vertebral column. Now it is recognized that the blood flows in
CPR because the whole thoracic cage is the pump; the heart
DIFFERENT PHASES
functions merely as a conduit for blood. An extrathoracic
pressure gradient is created by external chest compressions.
The pressure in all chambers and locations within the chest
OF RESPIRATION
cavity is the same. With compression, blood is forced out of
the thoracic cage. The blood preferentially flows out the arte-
It is important to remember that the pleura, lungs, and heart
rial side of the circulation and back down the venous side be-
in the chest cavity, and the upper abdominal viscera in the
cause the venous valves in the internal jugular system prevent
abdominal cavity, move extensively during the different
a useless oscillatory movement. With the release of compres-
phases of respiration. This movement largely results from
sion, blood enters the thoracic cage, preferentially down the
the rising and falling of the diaphragm. It is particularly
venous side of the systemic circulation.
important when trying to work out the path taken by a sharp
instrument or bullet following penetrating wounds to the
lower chest.
THE CHEST WALL
ROOT OF THE NECK
Thoracocentesis
INJURIES
Needle Thoracostomy
A needle thoracostomy is necessary in patients with tension
The cervical dome of the parietal pleura and the apex of the
pneumothorax (air in the pleural cavity under pressure) or to
lungs extend into the neck so that at their highest point
drain fluid (blood or pus) away from the pleural cavity to al-
they lie about 1 in. (2.5 cm) above the clavicles (see text
low the lung to reexpand. It may also be necessary to withdraw
Fig.
3-51). Consequently, they are vulnerable to stab
a sample of pleural fluid for microbiologic examination.
wounds in the root of the neck.
Anterior Approach
For the anterior approach, the patient is in the supine posi-
TRAUMATIC
tion. The sternal angle is identified, and then the second
costal cartilage, the second rib, and the second intercostal
space are found in the midclavicular line.
ASPHYXIA
Lateral Approach
The sudden caving in of the anterior chest wall associated
with fractures of the sternum and ribs causes a dramatic rise
For the lateral approach, the patient is lying on the lateral
in intrathoracic pressure. Apart from the immediate evi-
side. The second intercostal space is identified as above, but
dence of respiratory distress, the anatomy of the venous
the anterior axillary line is used.
system plays a significant role in the production of the char-
The skin is prepared in the usual way, and a local anes-
acteristic vascular signs of traumatic asphyxia. The thinness
thetic is introduced along the course of the needle above the
of the walls of the thoracic veins and the right atrium of the
upper border of the third rib. The thoracostomy needle will
heart causes their collapse under the raised intrathoracic
pierce the following structures as it passes through the chest
pressure, and venous blood is dammed back in the veins of
wall (see text Fig. 3-4): (a) skin, (b) superficial fascia (in the
the neck and head. This produces venous congestion;
anterior approach the pectoral muscles are then penetrated),
bulging of the eyes, which become injected; and swelling of
(c) serratus anterior muscle, (d) external intercostal muscle,
the lips and tongue, which become cyanotic. The skin of the
(e) internal intercostal muscle, (f) innermost intercostal mus-
face, neck, and shoulders becomes purple.
cle, (g) endothoracic fascia, and (h) parietal pleura.
50
Chapter 3
The needle should be kept close to the upper border of
of the rib above and maintains that position as it courses
the third rib to avoid injuring the intercostal vessels and
forward.
nerve in the subcostal groove.
The introduction of a thoracostomy tube or needle
through the lower intercostal spaces is possible provided that
the presence of the domes of the diaphragm is remembered
Tube Thoracostomy
as they curve upward into the rib cage as far as the fifth rib
The preferred insertion site for a tube thoracostomy is the
(higher on the right). Avoid damaging the diaphragm and
fourth or fifth intercostal space at the anterior axillary line
entering the peritoneal cavity and injuring the liver, spleen,
(CD Fig. 3-9). The tube is introduced through a small inci-
or stomach.
sion. The neurovascular bundle changes its relationship to
the ribs as it passes forward in the intercostal space. In the
Thoracotomy
most posterior part of the space, the bundle lies in the mid-
dle of the intercostal space. As the bundle passes forward to
In patients with penetrating chest wounds with uncon-
the rib angle, it becomes closely related to the lower border
trolled intrathoracic hemorrhage, thoracotomy may be a
4
5
A
4
intercostal vein
intercostal artery
5
4
intercostal nerve
tube
C
lung
5
visceral pleura
pleural cavity (space)
B
parietal pleura
innermost intercostal
skin
internal intercostal
superficial fascia
external
serratus anterior
intercostal
CD Figure 3-9
Tube thoracostomy. A. The site for insertion of the tube at the anterior ax-
illary line. The skin incision is usually made over the intercostal space one below the space
to be pierced. B. The various layers of tissue penetrated by the scalpel and later the tube as
they pass through the chest wall to enter the pleural cavity (space). The incision through the
intercostal space is kept close to the upper border of the rib to avoid injuring the intercostal
vessels and nerve. C. The tube advancing superiorly and posteriorly in the pleural space.
The Chest Wall, Chest Cavity, Lungs, and Pleural Cavities
51
life-saving procedure. After preparing the skin in the usual
peanuts, and parts of chicken bones and toys have all found
way, the physician makes an incision over the fourth or fifth
their way into the bronchi. Parts of teeth may be inhaled
intercostal space, extending from the lateral margin of the
while a patient is under anesthesia during a difficult dental
sternum to the anterior axillary line
(CD Fig. 3-10).
extraction. Because the right bronchus is the wider and
Whether to make a right or left incision depends on the site
more direct continuation of the trachea (see text Fig. 3-22),
of the injury. For access to the heart and aorta, the chest
foreign bodies tend to enter the right instead of the left
should be entered from the left side. The following tissues
bronchus. From there, they usually pass into the middle or
will be incised (see CD Fig. 3-9): (a) skin, (b) subcutaneous
lower lobe bronchi.
tissue, (c) serratus anterior and pectoral muscles, (d) exter-
nal intercostal muscle and anterior intercostal membrane,
Bronchoscopy
(e) internal intercostal muscle, (f) innermost intercostal
muscle, (g) endothoracic fascia, and (h) parietal pleura.
Bronchoscopy enables a physician to examine the interior of
Avoid the internal thoracic artery, which runs vertically
the trachea; its bifurcation, called the carina; and the main
downward behind the costal cartilages about a fingerbreadth
bronchi (CD Figs. 3-11 and 3-12). With experience, it is
lateral to the margin of the sternum, and the intercostal ves-
possible to examine the interior of the lobar bronchi and the
sels and nerve, which extend forward in the subcostal groove
beginning of the first segmental bronchi. By means of this
in the upper part of the intercostal space (see CD Fig. 3-9).
procedure, it is also possible to obtain biopsy specimens of
mucous membranes and to remove inhaled foreign bodies
(even an open safety pin).
THE TRACHEA AND
PRINCIPAL
THE LUNGS
BRONCHI
Clinical Examination of the Chest
As medical personnel, you will be examining the chest to
Compression of the Trachea
detect evidence of disease. Your examination consists of in-
The trachea is a membranous tube kept patent under normal
spection, palpation, percussion, and auscultation.
conditions by U-shaped bars of cartilage. In the neck, a uni-
Inspection shows the configuration of the chest,
lateral or bilateral enlargement of the thyroid gland can cause
the range of respiratory movement, and any inequalities on
gross displacement or compression of the trachea. A dilatation
the two sides. The type and rate of respiration are also
of the aortic arch (aneurysm) can compress the trachea. With
noted.
each cardiac systole the pulsating aneurysm may tug at the
Palpation enables the physician to confirm the impres-
trachea and left bronchus, a clinical sign that can be felt by
sions gained by inspection, especially of the respiratory
palpating the trachea in the suprasternal notch.
movements of the chest wall. Abnormal protuberances or re-
cession of part of the chest wall is noted. Abnormal pulsa-
tions are felt and tender areas detected.
Tracheitis or Bronchitis
Percussion is a sharp tapping of the chest wall with
The mucosa lining the trachea is innervated by the recur-
the fingers. This produces vibrations that extend through
rent laryngeal nerve and, in the region of its bifurcation, by
the tissues of the thorax. Air-containing organs such as the
the pulmonary plexus. A tracheitis or bronchitis gives rise to
lungs produce a resonant note; conversely, a more solid
a raw, burning sensation felt deep to the sternum instead of
viscus such as the heart produces a dull note. With prac-
actual pain. Many thoracic and abdominal viscera, when
tice, it is possible to distinguish the lungs from the heart or
diseased, give rise to discomfort that is felt in the midline. It
liver by percussion.
seems that organs possessing a sensory innervation that is not
Auscultation enables the physician to listen to the
under normal conditions directly relayed to consciousness
breath sounds as the air enters and leaves the respiratory
display this phenomenon. The afferent fibers from these or-
passages. Should the alveoli or bronchi be diseased and
gans traveling to the central nervous system accompany au-
filled with fluid, the nature of the breath sounds will be al-
tonomic nerves.
tered. The rate and rhythm of the heart can be confirmed
by auscultation, and the various sounds produced by the
heart and its valves during the different phases of the car-
Inhaled Foreign Bodies
diac cycle can be heard. It may be possible to detect fric-
Inhalation of foreign bodies into the lower respiratory tract
tion sounds produced by the rubbing together of diseased
is common, especially in children. Pins, screws, nuts, bolts,
layers of pleura or pericardium.
neck
line of incision
pectoralis
major
pectoralis
minor
A
B
4
5
3
pericardium
C
diaphragm
latissimus
serratus
dorsi
anterior
long thoracic
nerve
left phrenic ner ve
left lung
CD Figure 3-10
Left thoracotomy. A. Site of skin incision over fourth or fifth intercostal
space. B. The exposed ribs and associated muscles. The line of incision through the inter-
costal space should be placed close to the upper border of the rib to avoid injuring the inter-
costal vessels and nerve. C. The pleural space opened and the left side of the mediastinum
exposed. The left phrenic nerve descends over the pericardium beneath the mediastinal
pleura. The collapsed left lung must be pushed out of the way to visualize the mediastinum.
The Chest Wall, Chest Cavity, Lungs, and Pleural Cavities
53
To make these examinations, the physician must be
familiar with the normal structure of the thorax and must
have a mental image of the normal position of the lungs and
heart in relation to identifiable surface landmarks. Further-
more, it is essential that the physician be able to relate any
abnormal findings to easily identifiable bony landmarks so
that he or she can accurately record and communicate them
to colleagues.
Since the thoracic wall actively participates in the
movements of respiration, many bony landmarks change
their levels with each phase of respiration. In practice, to sim-
plify matters, the levels given are those usually found at about
midway between full inspiration and full expiration.
For physical examination of the patient, it is good to
remember that the upper lobe of the lungs is most easily
examined from the front of the chest and the lower lobe
from the back. In the axilla, areas of all three lobes can be
examined (see text Fig. 3-53).
Trauma to the Lungs
A physician must always remember that the apex of the lung
projects up into the neck (1 in. [2.5 cm] above the clavicle)
and can be damaged by stab or bullet wounds in this area.
CD Figure 3-11
The bifurcation of the trachea as seen
through an operating bronchoscope. Note the ridge of the ca-
rina seen in the center and the opening into the right main
Fractured Ribs and the Lungs
bronchus on the right, which is a more direct continuation of
the trachea. (Courtesy of E.D. Andersen.)
Although the lungs are well protected by the bony thoracic
cage, a splinter from a fractured rib can nevertheless pene-
trate the lung, and air can escape into the pleural cavity,
causing a pneumothorax and collapse of the lung. It can also
find its way into the lung connective tissue. From there, the
air moves under the visceral pleura until it reaches the lung
root. It then passes into the mediastinum and up to the neck.
Here, it may distend the subcutaneous tissue, a condition
known as subcutaneous emphysema.
The changes in the position of the thoracic and upper
abdominal viscera and the level of the diaphragm during
different phases of respiration relative to the chest wall are of
considerable clinical importance. A penetrating wound in
the lower part of the chest may or may not damage abdomi-
nal viscera, depending on the phase of respiration at the
time of injury.
Pain and Lung Disease
Lung tissue and the visceral pleura are devoid of pain-
sensitive nerve endings, so that pain in the chest is always
the result of conditions affecting the surrounding struc-
tures. In tuberculosis or pneumonia, for example, pain
may never be experienced.
Once lung disease crosses the visceral pleura and the
pleural cavity to involve the parietal pleura, pain becomes a
CD Figure 3-12
The interior of the left main bronchus as
prominent feature. Lobar pneumonia with pleurisy, for
seen through an operating bronchoscope. The openings into
the left upper lobe bronchus and its division and the left lower
example, produces a severe tearing pain, accentuated by
lobe bronchus are indicated. (Courtesy of E. D. Andersen.)
inspiring deeply or coughing. Because the lower part of the
54
Chapter 3
costal parietal pleura receives its sensory innervation from
Bronchogenic Carcinoma
the lower five intercostal nerves, which also innervate the
skin of the anterior abdominal wall, pleurisy in this area
Bronchogenic carcinoma accounts for about one third of all
commonly produces pain that is referred to the abdomen.
cancer deaths in men and is becoming increasingly common
This has sometimes resulted in a mistaken diagnosis of an
in women. It commences in most patients in the mucous
acute abdominal lesion.
membrane lining the larger bronchi and is therefore situated
In a similar manner, pleurisy of the central part of the
close to the hilum of the lung. The neoplasm rapidly spreads
diaphragmatic pleura, which receives sensory innervation
to the tracheobronchial and bronchomediastinal nodes and
from the phrenic nerve (C3, 4, and 5), can lead to referred
may involve the recurrent laryngeal nerves, leading to hoarse-
pain over the shoulder because the skin of this region is sup-
ness of the voice. Lymphatic spread via the bronchomediasti-
plied by the supraclavicular nerves (C3 and 4).
nal trunks may result in early involvement in the lower deep
cervical nodes just above the level of the clavicle. Hematoge-
Surgical Access to the Lungs
nous spread to bones and the brain commonly occurs.
Surgical access to the lungs or mediastinum is commonly
Conditions That Decrease
undertaken through an intercostal space. Special rib retrac-
tors that allow the ribs to be widely separated are used. The
Respiratory Efficiency
costal cartilages are sufficiently elastic to permit consider-
able bending. Good exposure of the lungs is obtained by this
method.
Constriction of the Bronchi (Bronchial
Asthma)
Segmental Resection of the Lung
One of the problems associated with bronchial asthma is the
A localized chronic lesion such as that of tuberculosis or a
spasm of the smooth muscle in the wall of the bronchioles.
benign neoplasm may require surgical removal. If it is re-
This particularly reduces the diameter of the bronchioles
stricted to a bronchopulmonary segment, it is possible to
during expiration, usually causing the asthmatic patient to
carefully dissect out a particular segment and remove it,
experience great difficulty in expiring, although inspiration is
leaving the surrounding lung intact. Segmental resection re-
accomplished normally. The lungs consequently become
quires that the radiologist and thoracic surgeon have a
greatly distended and the thoracic cage becomes perma-
sound knowledge of the bronchopulmonary segments and
nently enlarged, forming the so-called barrel chest. In addi-
that they cooperate fully to localize the lesion accurately be-
tion, the air flow through the bronchioles is further impeded
fore operation.
by the presence of excess mucus, which the patient is unable
to clear because an effective cough cannot be produced.
Pulmonary Contusion
Loss of Lung Elasticity
This condition is caused by a sudden rapid compression of
the chest wall and underlying lung. It may be produced by
Many diseases of the lungs, such as emphysema and pul-
blunt trauma or gunshot wounds. Because of the pliability
monary fibrosis, destroy the elasticity of the lungs, and thus
of the chest wall in children, lung contusion is often
the lungs are unable to recoil adequately, causing incom-
present in the absence of rib fractures. The localized
plete expiration. The respiratory muscles in these patients
endothelial damage to the capillaries results in the transu-
have to assist in expiration, which no longer is a passive
dation of fluid into the lung parenchyma, thus compro-
phenomenon.
mising lung function. In cases of blunt trauma, the area of
Loss of Lung Distensibility
damage to the lung will depend on the site of impact
and will not be determined by anatomic subdivisions of
Diseases such as silicosis, asbestosis, cancer, and pneumo-
the lung.
nia interfere with the process of expanding the lung in
inspiration. A decrease in the compliance of the lungs
Tracheobronchial Injury
and the chest wall then occurs, and a greater effort has to
be undertaken by the inspiratory muscles to inflate the lungs.
The lung root is the site where the mobile lung is connected
by the main bronchi to the relatively fixed lower end of the
trachea. It is not surprising, therefore, to find that when a
Postural Drainage
rapid deceleration or shearing force is applied to the lungs,
injuries occur to the bronchi. In the majority of patients, the
Excessive accumulation of bronchial secretions in a lobe or
tear occurs within 1 in. of the carina.
segment of a lung can seriously interfere with the normal
The Chest Wall, Chest Cavity, Lungs, and Pleural Cavities
55
esophagus
trachea
fistula
CD Figure 3-13
Different types
of esophageal atresia and tra-
cheoesophageal fistula. A. Com-
plete blockage of the esophagus
with a tracheoesophageal fistula.
B. Similar to type A, but the two
A
B
C
D
parts of the esophagus are joined
diaphragm
together by fibrous tissue.
C. Complete blockage of the
esophagus; the distal end is
rudimentary. D. A tracheoe-
sophageal fistula with narrowing
of the esophagus. E. An
esophagotracheal fistula; the
esophagus is not connected with
the distal end, which is rudimen-
tary. F. Separate esophagotra-
cheal and tracheoesophageal
fistulas. G. Narrowing of the
esophagus without a fistula.
In most cases, the lower
esophageal segment communi-
cates with the trachea, and types
E
F
G
A and B occur more commonly.
flow of air into the alveoli. Furthermore, the stagnation of
septum formed by the fusion of the margins of the laryngotra-
such secretions is often quickly followed by infection. To aid
cheal groove should be deviated posteriorly, the lumen of the
in the normal drainage of a bronchial segment, a physio-
esophagus would be much reduced in diameter. The differ-
therapist often alters the position of the patient so that grav-
ent types of atresia, with and without fistula, are shown in CD
ity assists in the process of drainage. Sound knowledge of the
Fig. 3-13). Obstruction of the esophagus prevents the child
bronchial tree is necessary to determine the optimum posi-
from swallowing saliva and milk, and this leads to aspiration
tion of the patient for good postural drainage.
into the larynx and trachea, which usually results in pneu-
monia. With early diagnosis, it is often possible to correct this
serious anomaly surgically.
CONGENITAL
Neonatal Lobar Emphysema
ANOMALIES OF
This condition occurs shortly after birth and is an overdisten-
tion of one or more lobes of the lung. It is a result, in many
THE TRACHEA AND
cases, of a failure of development of bronchial cartilage,
which causes the bronchi to collapse. Air is inspired through
the collapsed bronchi, but it is trapped during expiration.
LUNGS
Congenital Cysts of the Lung
Esophageal Atresia and Tracheo-
Lung cysts may be solitary or may form multiple honey-
comb-like masses. They are believed to be caused by sepa-
esophageal Fistula
ration of lung tissue occurring during development. Prompt
If the margins of the laryngotracheal groove fail to fuse ade-
surgical removal of the cysts is necessary to prevent com-
quately, an abnormal opening may be left between the laryn-
pression and collapse of surrounding lung and infectious
gotracheal tube and the esophagus. If the tracheoesophageal
complications.
56
Chapter 3
Clinical Problem Solving Questions
Read the following case histories/questions and give
A 65-year-old man and a 10-year-old boy were involved
the best answer for each.
in a severe automobile accident. In both patients the
thorax had been badly crushed. Radiographic examina-
A 31-year-old soldier received a shrapnel wound in the
tion revealed that the man had five fractured ribs but
neck during the Persian Gulf War. Recently, during a
the boy had no fractures.
physical examination, it was noticed that when he blew
4.
What is the most likely explanation for this difference in
his nose or sneezed, the skin above the right clavicle
medical findings?
bulged upward.
A. The patients were in different seats in the vehicle.
1.
The upward bulging of the skin could be explained by
B. The boy was wearing his seat belt and the man was
A. injury to the cervical pleura.
not.
B. damage to the suprapleural membrane.
C. The chest wall of a child is very elastic, and fractures
C. damage to the deep fascia in the root of the neck.
of ribs in children are rare.
D. ununited fracture of the first rib.
D. The man anticipated the impact and tensed his
muscles, including those of the shoulder girdle and
A 52-year-old woman was admitted to the hospital with
abdomen.
a diagnosis of right-sided pleurisy with pneumonia. It
was decided to remove a sample of pleural fluid from
On examination of a posteroanterior chest radiograph
her pleural cavity. The resident inserted the needle
of an 18-year-old woman, it was seen that the left dome
close to the lower border of the eighth rib in the ante-
of the diaphragm was higher than the right dome and
rior axillary line. The next morning he was surprised to
reached to the upper border of the fourth rib.
hear that the patient had complained of altered skin
5.
The position of the left dome of the diaphragm could
sensation extending from the point where the needle
be explained by the following conditions except which?
was inserted downward and forward to the midline of
A. The left lung could be collapsed.
the abdominal wall above the umbilicus.
B. There is a collection of blood under the diaphragm
2.
The altered skin sensation in this patient after the nee-
on the left side.
dle thoracostomy could be explained by which of the
C. There is an amoebic abscess in the left lobe of the
following?
liver.
A. The needle was inserted too low down in the inter-
D. The left dome of the diaphragm is normally higher
costal space.
than the right dome.
B. The needle was inserted too close to the lower bor-
E. There is a peritoneal abscess beneath the diaphragm
der of the eighth rib and damaged the eighth inter-
on the left side.
costal nerve.
A 43-year-old man was involved in a violent quarrel
C. The needle had impaled the eighth rib.
with his wife over another woman. In a fit of rage, the
D. The needle had penetrated too deeply and pierced
wife picked up a carving knife and lunged forward at
the lung.
her husband, striking his anterior neck over the left
A 68-year-old man complained of a swelling in the skin
clavicle. The husband collapsed on the kitchen floor,
on the back of the chest. He had noticed it for the last 3
bleeding profusely from the wound. The distraught
years and was concerned because it was rapidly enlarg-
wife called for an ambulance.
ing. On examination, a hard lump was found in the skin
6.
On examination in the emergency department of the
in the right scapula line opposite the seventh thoracic
hospital the following conditions were found except
vertebra. A biopsy revealed that the lump was malignant.
which?
3.
Because of the rapid increase in the size of the tumor,
A. A wound was seen about 1 in. (2.5 cm) wide over the
the following lymph nodes were examined for metas-
left clavicle.
tases:
B. Auscultation revealed diminished breath sounds
A. Superficial inguinal nodes
over the left hemithorax.
B. Anterior axillary nodes
C. The trachea was deflected to the left.
C. Posterior axillary nodes
D. The left upper limb was lying stationary on the table,
D. External iliac nodes
and active movement of the small muscles of the left
E. Deep cervical nodes
hand was absent.
The Chest Wall, Chest Cavity, Lungs, and Pleural Cavities
57
E. The patient was insensitive to pin prick along the lat-
B. The carcinoma had metastasized to the broncho-
eral side of the left arm, forearm, and hand.
mediastinal lymph nodes, causing their enlarge-
ment and producing a widening of the mediastinal
A 72-year-old man complaining of burning pain on the
shadow seen on the chest radiograph.
right side of his chest was seen by his physician. On ex-
C. The enlarged lymph nodes had pressed on the left
amination the patient indicated that the pain passed
recurrent laryngeal nerve.
forward over the right sixth intercostal space from the
D. Partial injury to the recurrent laryngeal nerve re-
posterior axillary line forward as far as the midline over
sulted in paralysis of the abductor muscles of the vo-
the sternum. The physician noted that there were sev-
cal cords, leaving the adductor muscles unopposed.
eral watery blebs on the skin in the painful area.
E. The enlarged lymph nodes pressed on the left re-
7.
The following statements are correct except which?
current nerve as it ascended to the neck anterior to
A. This patient has herpes zoster.
the arch of the aorta.
B. A virus descends along the cutaneous nerves, caus-
A 35-year-old woman had difficulty breathing and
ing dermatomal pain and the eruption of vesicles.
sleeping at night. She says she falls asleep only to wake
C. The sixth right intercostal nerve was involved.
up with a choking sensation. She finds that she has to
D. The condition was confined to the anterior cuta-
sleep propped up in bed on pillows with her neck flexed
neous branch of the sixth intercostal nerve.
to the right.
An 18-year-old woman was thrown from a horse while
10.
The following statements concerning this case are
attempting to jump a fence. She landed heavily on the
correct except which?
ground, striking the lower part of her chest on the left
A. Veins in the skin at the root of the neck are
side. On examination in the emergency department she
congested.
was conscious but breathless. The lower left side of her
B. The U-shaped cartilaginous rings in the wall of the
chest was badly bruised, and the ninth and tenth ribs
trachea prevent it from being kinked or compressed.
were extremely tender to touch. She had severe tachy-
C. The left lobe of the thyroid gland is larger than the
cardia, and her systolic blood pressure was low.
right lobe.
8.
The following statements are possibly correct except
D. On falling asleep, the patient tends to flex her neck
which?
laterally over the enlarged left thyroid lobe.
A. There was evidence of tenderness and muscle spasm
E. The enlarged thyroid gland extends down the neck
in the left upper quadrant of the anterior abdominal
into the superior mediastinum.
wall.
F. The brachiocephalic veins in the superior medi-
B. A posteroanterior radiograph of the chest revealed
astinum were partially obstructed by the enlarged
fractures of the left ninth and tenth ribs near their
thyroid gland.
angles.
A 15-year-old boy was rescued from a lake after falling
C. The blunt trauma to the ribs had resulted in a tear of
through thin ice. The next day, he developed a severe
the underlying spleen.
cold, and 3 days later his general condition deterio-
D. The presence of blood in the peritoneal cavity had
rated. He became febrile and started to cough up blood-
irritated the parietal peritoneum, producing reflex
stained sputum. At first, he had no chest pain, but later,
spasm of the upper abdominal muscles.
when he coughed, he experienced severe pain over the
E. The muscles of the anterior abdominal wall are not
right fifth intercostal space in the midclavicular line.
supplied by thoracic spinal nerves.
11.
The following statements would explain the patient’s
A 55-year-old man states that he has noticed an alter-
signs and symptoms except which?
ation in his voice. He has lost 40 lb (18 kg) and has a
A. The patient had developed lobar pneumonia and
persistent cough with blood-stained sputum. He
pleurisy in the right lung.
smokes 50 cigarettes a day. On examination, the left vo-
B. Disease of the lung does not cause pain until the
cal fold is immobile and lies in the adducted position.
parietal pleura is involved.
A posteroanterior chest radiograph reveals a large mass
C. The pneumonia was located in the right middle
in the upper lobe of the left lung with an increase in
lobe.
width of the mediastinal shadow on the left side.
D. The visceral pleura is innervated by autonomic
9.
The symptoms and signs displayed by this patient can
nerves that contain pain fibers.
be explained by the following statements except which?
E. Pain associated with the pleurisy was accentuated
A. This patient has advanced carcinoma of the
when movement of the visceral and parietal pleurae
bronchus in the upper lobe of the left lung, which
occurred, for example, on deep inspiration or
was seen as a mass on the chest radiograph.
coughing.
58
Chapter 3
A 2-year-old boy was playing with his toy car when his
C. The costodiaphragmatic recess is situated between
baby-sitter noticed that a small metal nut was missing
the lower border of the lung and the parietal
from the car. Two days later the child developed a
pleura.
cough and became febrile.
D. The lung on extreme inspiration could descend in
the costodiaphragmatic recess only as far as the
12.
This child’s illness could be explained by the following
eighth rib.
statements except which?
E. No breath sounds were heard because the stetho-
A. The child had inhaled the nut.
scope was located over the liver.
B. The metal nut could easily be seen on posteroante-
rior and right oblique radiographs.
A 36-year-old woman with a known history of emphy-
C. The left principal bronchus is the more vertical and
sema (dilatation of alveoli and destruction of alveolar
wider of the two principal bronchi, and inhaled for-
walls with a tendency to form cystic spaces) suddenly
eign bodies tend to become lodged in it.
experiences a severe pain in the left side of her
D. The nut was successfully removed through a bron-
chest, is breathless, and is obviously in a state of
choscope.
shock.
E. Children who are teething tend to suck on hard toys.
14.
Examination of this patient reveals the following
A 23-year-old woman was examined in the emergency
findings except which?
department because of the sudden onset of respiratory
A. The trachea is displaced to the right in the supraster-
distress. The physician was listening to breath sounds
nal notch.
over the right hemithorax and was concerned when no
B. The apex beat of the heart can be felt in the fifth left
sounds were heard on the front of the chest at the level
intercostal space just lateral to the sternum.
of the tenth rib in the midclavicular line.
C. The right lung is collapsed.
13.
The following comments concerning this patient are
D. The air pressure in the left pleural cavity is at
correct except which?
atmospheric pressure.
A. In a healthy individual, the lower border of the right
E. The air has entered the left pleural cavity as the
lung in the midclavicular line in the midrespiratory
result of rupture of one of the emphysematous cysts
position is at the level of the sixth rib.
of the left lung (left-sided pneumothorax).
B. The parietal pleura in the midclavicular line crosses
F. The elastic recoil of the lung tissue caused the lung
the tenth rib.
to collapse.
Answers and Explanations
1. B is the correct answer. The shrapnel had torn the
6. E is the correct answer. The lower trunk of the brachial
suprapleural membrane, which normally prevents
plexus was cut by the knife. This would explain the loss
the cervical dome of the pleura from bulging up into
of movement of the small muscles of the left hand. It
the neck.
would also explain the loss of skin sensation that oc-
curred in the C8 and T1 dermatomes on the medial,
2. B is the correct answer. The intercostal nerve is located
not on the lateral, side of the left forearm and hand. The
in the subcostal groove on the lower border of the rib
knife had also pierced the left dome of the cervical
(see text Fig. 3-4).
pleura, causing a left pneumothorax with left-sided
3. C is the correct answer. The lymphatic drainage of the
diminished breath sounds and a deflection of the tra-
skin of the back above the level of the iliac crests is
chea to the left.
upward and forward into the posterior axillary lymph
7. D is the correct answer. The skin over the sixth inter-
nodes.
costal space is innervated by the lateral cutaneous
4. C is the correct answer. The chest wall of a child is very
branch as well as the anterior cutaneous branch of the
elastic, and fractures of ribs in children are rare.
sixth intercostal nerve.
5. D is the correct answer. The right dome of the di-
8. E is the correct answer. The seventh to the eleventh in-
aphragm is normally higher than the left dome due to
tercostal nerves supply the muscles of the anterior ab-
the large size of the right lobe of the underlying liver.
dominal wall.
The Chest Wall, Chest Cavity, Lungs, and Pleural Cavities
59
9. E is the correct answer. The left recurrent laryngeal
12. C is the correct answer. The right principal (main)
nerve ascends to the neck by passing under the arch of
bronchus is the more vertical and wider of the two prin-
the aorta; it ascends in the groove between the trachea
cipal bronchi, and for this reason an inhaled foreign
and the esophagus.
body passes down the trachea and tends to enter the right
main bronchus, where it was lodged in this patient.
10. B is the correct answer. The trachea is a mobile, fibro-
13. B is the correct answer. The parietal pleura in the mid-
elastic tube that can be kinked or compressed despite
clavicular line only extends down as far as the eighth rib
the presence of the cartilaginous rings.
(see text Fig. 3-51).
11. D is the correct answer. Lung tissue and the visceral
14. C is the correct answer. The left lung collapsed imme-
pleura are not innervated with pain fibers. The costal
diately when air entered the left pleural cavity because
parietal pleura is innervated by the intercostal nerves,
the air pressures within the bronchial tree and in the
which have pain endings in the pleura.
pleural cavity were then equal.
The Cardiovascular
System
The Heart, Coronary
Vessels, and Pericardium
4
Chapter Outline
The Heart
64
Cardiac Injuries
68
Cardiac Contusion
68
Chordae Tendineae and Papillary Muscle Rupture
64
Valve and Septal Injuries
69
Mitral Valve Prolapse
64
Penetrating Injuries to the Heart
69
Accessory Atrioventricular Bundles
64
Congenital Anomalies
69
Atrial Septal Defects
69
Circus Movement
64
Ventricular Septal Defects
69
Failure of Conduction System
65
Tetralogy of Fallot
69
Coronary Angiography
65
Mitral Valve Prolapse
69
Bicuspid Aortic Valve
70
Coronary Artery Disease
65
Persistent Truncus Arteriosus
70
Myocardial Infarction and Papillary Muscle Rupture
66
Patent Ductus Arteriosus
71
Chest Pain
66
The Pericardium
71
Somatic Pain
66
Visceral Pain
67
Traumatic Injury to the Pericardium
71
Referred Pain
67
Pericardial Disruption
71
Hemopericardium
71
Clinical Significance of Thoracic Dermatomes
Pericardiocentesis
71
Relative to Chest Pain
67
Anatomy of Complications
72
Cardiac Pain
67
Auscultation of Heart Valves
68
Clinical Problem Solving Questions
72
Valvular Disease of the Heart
68
Answers and Explanations
74
Valvular Heart Murmurs
68
Accessory Atrioventricular Bundles
THE HEART
Accessory atrioventricular bundles are thought to exist. They
are believed to be slender and normally have no functional
Chordae Tendineae and Papillary
significance. However, in the condition of accelerated atri-
oventricular conduction, the aberrant connection (bundle of
Muscle Rupture
Kent) permits one ventricle to be excited early. In this condi-
tion the PR interval is shortened and a delta wave appears on
Rupture of the chordae tendineae by disease, such as acute
the initial part of the QRS complex. Another aberrant con-
bacterial endocarditis, may cause sudden valvular insuffi-
nection (bundle of Mahaim) bypasses the atrioventricular
ciency and cardiac decompensation. Rupture of a papillary
node and inserts just distal to the node. In this condition,
muscle, since each has many chordae attached to its apex, is
known as the Lown-Ganong-Levine syndrome, the PR inter-
much more serious. Rupture of a papillary muscle may oc-
val is short but the QRS complex is normal.
cur in penetrating wounds of the heart.
Mitral Valve Prolapse
Circus Movement
In this condition, one or both mitral valve cusps balloon up
This abnormal form of conduction allows a wave of excita-
into the left atrium during ventricular systole. The valve
tion to travel continuously in a circle. This ring may occur
cusps are larger than normal and the chordae tendineae
in the atrioventricular node, causing abnormal atrial con-
may be excessively long. The posterior cusp is always in-
tractions and paroxysmal nodal tachycardia. If the individ-
volved; the anterior cusp is involved less frequently.
ual has an accessory atrioventricular bundle, the circus
The Heart, Coronary Vessels, and Pericardium
65
movement may pass in one direction through the atrioven-
scopic control, a long narrow catheter is passed into the as-
tricular node and in the opposite direction through the
cending aorta via the femoral artery in the leg. The tip of the
bundle of Kent.
catheter is carefully guided into the orifice of a coronary
artery and a small amount of radiopaque material is injected
to reveal the lumen of the artery and its branches. The in-
Failure of Conduction System
formation can be recorded on radiographs (CD Fig. 4-1) or
The sinuatrial node is the spontaneous source of the cardiac
by cineradiography. Using this technique, pathologic nar-
impulse. The atrioventricular node is responsible for picking
rowing or blockage of a coronary artery can be identified.
up the cardiac impulse from the atria. The atrioventricular
bundle is the only route by which the cardiac impulse can
Coronary Artery Disease
spread from the atria to the ventricles. Failure of the bundle
to conduct the normal impulses results in alteration in the
The myocardium receives its blood supply through the right
rhythmic contraction of the ventricles (arrhythmias) or, if
and left coronary arteries. Although the coronary arteries
complete bundle block occurs, complete dissociation be-
have numerous anastomoses at the arteriolar level, they are
tween the atria and ventricular rates of contraction. The com-
essentially functional end arteries. A sudden block of one of
mon cause of defective conduction through the bundle or its
the large branches of either coronary artery will usually lead
branches is atherosclerosis of the coronary arteries, which re-
to necrosis of the cardiac muscle (myocardial infarction) in
sults in a diminished blood supply to the conducting system.
that vascular area, and often the patient dies. Most cases of
coronary artery blockage are caused by an acute thrombosis
on top of a chronic atherosclerotic narrowing of the lumen.
Coronary Angiography
Arteriosclerotic disease of the coronary arteries may pre-
The coronary arteries can be visualized by the introduction
sent in three ways, depending on the rate of narrowing of the
of radiopaque material into their lumen. Under fluoro-
lumina of the arteries: (1) General degeneration and fibrosis
A
B
CD Figure 4-1
Coronary angiograms. A. An area of extreme narrowing of the circumflex
branch of the left coronary artery (white arrow). B. The same artery after percutaneous
transluminal coronary angioplasty. Inflation of the luminal balloon has dramatically im-
proved the area of stenosis (white arrow).
66
Chapter 4
CD Table 4-1
Coronary Artery Lesions, Infarct Location, and ECG Signature
Coronary Artery
Infarct Location
ECG Signature
Proximal LAD
Large anterior wall
ST elevation: I, L, V1-V6
More distal LAD
Anteroapical
ST elevation: V2-V4
Inferior wall if
ST elevation: II, III, F
wraparound LAD
Distal LAD
Anteroseptal
ST elevation: V1-V3
Early obtuse, marginal
High lateral wall
ST elevation: I, L, V4-V6
More distal marginal
Small lateral wall
ST elevation: I, L, or V4-V6, or no abnormality
branch, circumflex
Circumflex
Posterolateral
ST elevation: V4-V6; ST depression: V1-V2
Distal RCA
Small inferior wall
ST elevation: II, III, F; ST depression: I, L
Proximal RCA
Large inferior wall and
ST elevation: II, III, F;
posterior wall
ST depression: I, L, V1-V3
Some lateral wall
ST elevation: V5-V6
RCA
Right ventricular
ST elevation: V2R-V4R; some
ST elevation: V1, or ST depression: V2-V3
Usually inferior
ST elevation: II, III, F
ECG, electrocardiographic; LAD, left anterior descending (interventricular); RCA, right coronary artery.
of the myocardium occur over many years and are caused by
supplied by a single artery, the right coronary artery. The an-
a gradual narrowing of the coronary arteries. (2) Angina pec-
terolateral papillary muscle is less likely to rupture since it
toris is cardiac pain that occurs on exertion and is relieved
has a dual blood supply from the anterior interventricular
by rest. In this condition, the coronary arteries are so nar-
and circumflex branches of the left coronary artery.
rowed that myocardial ischemia occurs on exertion but not
at rest. (3) Myocardial infarction occurs when coronary flow
Chest Pain
is suddenly reduced or stopped and the cardiac muscle un-
dergoes necrosis. Myocardial infarction is the major cause
The presenting symptom of chest pain is a common and
of death in industrialized nations.
classic problem in medicine. Unfortunately, chest pain is a
CD Table 4-1 shows the different coronary arteries that
symptom common to a large number of conditions and may
supply the different areas of the myocardium. This informa-
be caused by disease in the thoracic and abdominal walls or
tion can be helpful when attempting to correlate the site of
in many different chest or abdominal viscera. The severity of
myocardial infarction, the artery involved, and the electro-
the pain is often unrelated to the seriousness of the cause.
cardiographic signature.
Myocardial pain may mimic esophagitis, musculoskeletal
Because coronary bypass surgery, coronary angioplasty,
chest wall pain, and other non-life-threatening causes. Un-
and coronary artery stenting are now commonly accepted
less medical personnel are astute, a patient may be dis-
methods of treating coronary artery disease, it is incumbent on
charged from the hospital with a more serious condition
the student to be prepared to interpret still- and motion-picture
than the symptoms indicate. It is not good enough to have a
angiograms that have been carried out before treatment. For
correct diagnosis only 99% of the time with chest pain. An
this reason, a working knowledge of the origin, course, and dis-
understanding of the anatomy of chest pain will help the
tribution of the coronary arteries should be memorized.
physician in the systematic consideration of the differential
diagnosis.
Myocardial Infarction and
Somatic Pain
Papillary Muscle Rupture
Pain arising from the chest or abdominal walls is intense and
Rarely, in acute myocardial infarction involving the left ven-
discretely localized. Somatic pain arises in sensory nerve
tricle, a papillary muscle may rupture. Rupture of the pos-
endings in these structures and is conducted to the central
teromedial papillary muscle is more common since it is
nervous system by somatic segmental spinal nerves.
The Heart, Coronary Vessels, and Pericardium
67
Visceral Pain
disease of neighboring viscera, such as the gallbladder, liver,
or stomach, could send afferent impulses up to the central
Visceral pain is diffuse and poorly localized. It is conducted
nervous system. Because of the phenomenon of referred
to the central nervous system along afferent autonomic
pain, the patient would presume that the cause of the pain
nerves. Most visceral pain fibers ascend to the spinal cord
was located over the upper part of the chest wall or shoulder.
along sympathetic nerves and enter the cord through the
Below the level of the sternal angle and the spine of the
posterior nerve roots of segmental spinal nerves. Some pain
scapula, the chest skin is innervated by the thoracic segments
fibers from the pharynx and upper part of the esophagus and
of the spinal cord. The anterior chest wall is supplied by the
the trachea enter the central nervous system through the
intercostal nerves T2 through T6; the seventh intercostal
parasympathetic nerves via the glossopharyngeal and vagus
nerve enters the anterior abdominal wall to supply the skin
nerves. The descending colon, the pelvic colon and rectum,
in the xiphoid area. The posterior chest wall is supplied by
and the bladder reach the sacral spinal cord through the
the posterior primary rami of the thoracic spinal nerves T2
parasympathetic nerves.
through T11. Remember that the seventh to the eleventh in-
tercostal nerves cross the costal margin and innervate the full
Referred Pain
thickness of the anterior abdominal wall including the pari-
Visceral pain frequently is referred to skin areas that are in-
etal peritoneum. This would explain how irritation of the
nervated by the same segment of the spinal cord as is the
parietal peritoneum caused by disease of abdominal viscera
painful viscus. The explanation for referred pain is not
could give rise to pain referred to the chest wall.
known. One theory is that the nerve fibers from the viscus
Note also the distribution of the T1 and T2 der-
and the dermatome ascend in the central nervous system
matomes; they extend down the medial side of the upper
along a common pathway and the cerebral cortex is inca-
limbs. The second thoracic nerve reaches the skin of the ax-
pable of distinguishing between the sites of origin. Another
illa and the medial (ulnar) side of the arm via the intercos-
theory is that under normal conditions the viscus does not
tobrachial nerve (a branch of the second intercostal nerves).
give rise to painful stimuli, whereas the skin area repeatedly
T1 reaches the ulnar side of the forearm via the medial cu-
receives noxious stimuli. Because both afferent fibers enter
taneous nerve of the forearm from the brachial plexus.
the spinal cord at the same segment, the brain interprets the
information as coming from the skin rather than the viscus.
Cardiac Pain
Pain arising from the gastrointestinal tract is referred to the
midline. This can probably be explained since the tract
Pain originating in the heart as the result of acute myocardial
arises embryologically as a midline structure and receives a
ischemia is assumed to be caused by oxygen deficiency and
bilateral nerve supply.
the accumulation of metabolites, which stimulate the sen-
sory nerve endings in the myocardium. The afferent nerve
fibers ascend to the central nervous system through the car-
Clinical Significance of Thoracic
diac branches of the sympathetic trunk and enter the spinal
cord through the posterior roots of the upper four thoracic
Dermatomes Relative to Chest Pain
nerves. The nature of the pain varies considerably, from a se-
The dermatomes on the anterior and posterior chest walls
vere crushing pain to nothing more than mild discomfort.
are shown in CD Figs. 1-2 and 1-3. A dermatome is an area
The pain is not felt in the heart, but is referred to the
of skin supplied by a single spinal nerve and, therefore, a
skin areas supplied by the corresponding spinal nerves. The
single segment of the spinal cord. On the trunk, adjacent
skin areas supplied by the upper four intercostal nerves and
dermatomes overlap considerably and a given area of skin is
by the intercostobrachial nerve (T2) are therefore affected.
innervated by three adjacent spinal nerves.
The intercostobrachial nerve communicates with the me-
Each thoracic spinal nerve innervates a large number of
dial cutaneous nerve of the arm and is distributed to skin on
structures, including the vertebrae; the ribs and costal carti-
the medial side of the upper part of the arm. A certain
lages and their joints; the postvertebral, intercostal, and ab-
amount of spread of nervous information must occur within
dominal muscles; and the costal parietal pleura and parietal
the central nervous system, for the pain is sometimes felt in
peritoneum. Any one of these structures could be the source
the neck and the jaw.
of chest pain.
Myocardial infarction involving the inferior wall or di-
The skin of the anterior and posterior chest walls, down
aphragmatic surface of the heart often gives rise to discom-
as far as the sternal angle in front and the spine of the
fort in the epigastrium. One must assume that the afferent
scapula behind, is supplied by the supraclavicular nerves
pain fibers from the heart ascend in the sympathetic nerves
(C3 and C4). The phrenic nerves (C3, C4, and C5) supply
and enter the spinal cord in the posterior roots of the sev-
the parietal pleura over the central part of the diaphragm
enth, eighth, and ninth thoracic spinal nerves and give rise
and a corresponding area of parietal peritoneum over the
to referred pain in the T7, T8, and T9 thoracic dermatomes
lower surface of the diaphragm. Irritation of these areas by
in the epigastrium.
68
Chapter 4
Because the heart and the thoracic part of the esopha-
Valvular Disease of the Heart
gus probably have similar afferent pain pathways, it is not
surprising that painful acute esophagitis can mimic the pain
Inflammation of a valve can cause the edges of the valve cusps
of myocardial infarction.
to stick together. Later, fibrous thickening occurs, followed by
loss of flexibility and shrinkage. Narrowing (stenosis) and
Auscultation of Heart Valves
valvular incompetence (regurgitation) result, and the heart
ceases to function as an efficient pump. In rheumatic disease
On listening to the heart with a stethoscope, one can hear
of the mitral valve, for example, not only do the cusps undergo
two sounds: l
¯ b-du˘ p. The first sound is produced by the con-
fibrosis and shrink, but also the chordae tendineae shorten,
traction of the ventricles and the closure of the tricuspid and
preventing closure of the cusps during ventricular systole.
mitral valves. The second sound is produced by the sharp
closure of the aortic and pulmonary valves. It is important
Valvular Heart Murmurs
for a physician to know where to place the stethoscope on
the chest wall so that he or she will be able to hear sounds
Apart from the sounds of the valves closing, l
¯b-du˘p, the
produced at each valve with the minimal distraction or in-
blood passes through the normal heart silently. Should the
terference (CD Fig. 4-2).
valve orifices become narrowed or the valve cusps distorted
■ The tricuspid valve is best heard over the right half of the
and shrunken by disease, however, a rippling effect would
lower end of the body of the sternum.
be set up, leading to turbulence and vibrations that are
■ The mitral valve is best heard over the apex beat, that is,
heard as heart murmurs.
at the level of the fifth left intercostal space, 3.5 in. (9 cm)
from the midline.
Cardiac Injuries
■ The pulmonary valve is heard with least interference
over the medial end of the second left intercostal
Cardiac Contusion
space.
■ The aortic valve is best heard over the medial end of the
The heart, although protected by the thoracic cage, can be
second right intercostal space.
squeezed between the sternum and the vertebral column
pulmonary valve
aortic valve
right atrium
left ventricle
mitral valve
tricuspid
CD Figure 4-2
Surface
valve
anatomy of the heart and great
right ventricle
blood vessels. Note the position
of the heart valves relative to
the chest wall. The bold letters
indicate positions where valves
may be heard with least interfer-
apex
ence. A aortic valve, M mi-
tral valve, P pulmonary valve,
T tricuspid valve.
The Heart, Coronary Vessels, and Pericardium
69
(see text Fig. 4-8) when the thorax is subjected to a severe
and results in oxygenated blood from the left atrium passing
frontal impact. Moreover, if the force is also applied to the
over into the right atrium (CD Fig. 4-3).
anterior abdominal wall, the diaphragm is thrust upward,
impinging on the heart from below. The highly flexible rib
Ventricular Septal Defects
cage present in children makes myocardial contusion a
The ventricular septum is formed in a complicated manner
common occurrence in this age group. The result of heart
and is complete only when the membranous part fuses with
muscle damage is precordial pain, similar in nature to a my-
the muscular part. Ventricular septal defects are less fre-
ocardial infarction. Tachycardia often occurs and, if enough
quent than atrial septal defects. They are found in the
cardiac muscle is contused, cardiac output may decrease.
membranous part of the septum and can measure 1 to 2 cm
Depending on the severity of the injury, there may be ar-
in diameter. Blood under high pressure passes through the
rhythmias and evidence of heart block.
defect from left to right, causing enlargement of the right
ventricle. Large defects are serious and can shorten life if
Valve and Septal Injuries
surgery is not performed.
In both blunt and penetrating injuries to the heart, the valve
cusps, the papillary muscles, and the chordae tendineae can
Tetralogy of Fallot
be damaged. The incidence of valve involvement is in the
Normally, the bulbus cordis becomes divided into the aorta
following order: aortic, mitral, and pulmonary. Acute valvu-
and pulmonary trunk by the formation of the spiral aorti-
lar insufficiency can be diagnosed clinically, but it should
copulmonary septum. This septum is formed by the fusion
be confirmed by cardiac catheterization. In severe cases
of the bulbar ridges. If the bulbar ridges fail to fuse correctly,
prompt surgical repair may be necessary.
unequal division of the bulbus cordis may occur, with con-
sequent narrowing of the pulmonary trunk and resulting in
Penetrating Injuries to the Heart
interference with the right ventricular outflow.
The anatomy of the heart relative to the front of the thoracic
This congenital anomaly is responsible for about 9% of
cage determines the common sites of injury. The anterior sur-
all congenital heart disease (see CD Fig. 4-3). The anatomic
face of the heart is formed largely by the right ventricle; the
abnormalities include large ventricular septal defect; steno-
left border is formed by the left ventricle and the right border
sis of the pulmonary trunk, which can occur at the in-
is formed by the right atrium. The right ventricle is most com-
fundibulum of the right ventricle or at the pulmonary valve;
monly injured, followed by the left ventricle and the right
exit of the aorta immediately above the ventricular septal de-
atrium. The anterior interventricular branch of the left coro-
fect (instead of from the left ventricular cavity only); and se-
nary artery is the most common artery to be damaged.
vere hypertrophy of the right ventricle, because of the high
Since the pericardium has to be penetrated for the
blood pressure in the right ventricle. The defects cause con-
heart to be injured, cardiac tamponade is often present. The
genital cyanosis and considerably limit activity; patients
hemopericardium quickly presses on the thin-walled atria
with severe untreated abnormalities die. Once the diagnosis
and large veins and compromises the venous return. The
has been made, most children can be successfully treated
classic triad of (1) distension of the jugular veins of the neck,
surgically.
(2) faint heart sounds (damped down by blood in the peri-
Most children find that assuming the squatting position
cardial sac), and (3) hypotension may all be present. If there
after physical activity relieves their breathlessness. This
is substantial concomitant blood loss or volume depletion,
happens because squatting reduces the venous return by
the jugular veins may not be enlarged. Do not expect to see
compressing the abdominal veins and increasing the sys-
a greatly enlarged heart shadow on a chest radiograph. Even
temic arterial resistance by kinking the femoral and
though the blood in the pericardial sac may be under high
popliteal arteries in the legs; both these mechanisms tend to
pressure caused by a ventricular leak, the tough fibrous tis-
decrease the right-to-left shunt through the ventricular sep-
sue in the wall of the fibrous pericardium prevents its undue
tal defect and improve the pulmonary circulation.
distension. Hemopericardium must be relieved surgically.
Mitral Valve Prolapse
Congenital Anomalies
In this condition, one or both mitral valve cusps balloon up
into the left atrium during ventricular systole. The valve
Atrial Septal Defects
cusps are larger than normal and the chordae tendineae
After birth, the foramen ovale becomes completely closed as
may be excessively long. The posterior cusp is always in-
the result of the fusion of the septum primum with the sep-
volved; the anterior cusp is involved less frequently. The ma-
tum secundum. In 25% of hearts, a small opening persists,
jority of the patients are female, and there may be a familial
but this is usually of such a minor nature that it has no clin-
incidence of the syndrome. The typical symptoms are chest
ical significance. Occasionally, the opening is much larger
pain and palpitations, and dysrhythmias may occur.
70
Chapter 4
septum secundum
septum primum
foramen ovale
A
B
pulmonary stenosis
left recurrent laryngeal
nerve
displaced aortic opening
hypertrophy of
right ventricle
septal defect
D
C
E
CD Figure 4-3
A. Normal fetal heart. B. Atrial septal defect. C. Tetralogy of Fallot.
D. Patent ductus arteriosus (note the close relationship to the left recurrent laryngeal
nerve). E. Coarctation of the aorta.
Bicuspid Aortic Valve
Persistent Truncus Arteriosus
This is a congenital anomaly occurring in 1% to 2% of the
This condition represents about 1% of all congenital
population. At first it causes no functional problems. How-
heart defects. Only one artery arises from the heart, the
ever, with advancing years and continued wear and tear, the
pulmonary artery and aorta sharing a common trunk. A
valve cusps become damaged and undergo fibrosing steno-
large ventricular septal defect is usually present. The
sis and calcification. The valve is also prone to the develop-
child exhibits mild cyanosis and heart failure. Surgical
ment of infective endocarditis.
correction of the ventricular septal defect and the
The Heart, Coronary Vessels, and Pericardium
71
establishment of a separate pulmonary and aortic outflow
Hemopericardium
are necessary.
With blunt or penetrating injuries to the heart, blood can es-
Patent Ductus Arteriosus
cape into the pericardial cavity. The normal volume of peri-
cardial fluid, about 50 mL, is used to lubricate the apposing
The ductus arteriosus represents the distal portion of the
surfaces of the serous pericardium during heart movements.
sixth left aortic arch and connects the left pulmonary artery
Once the fluid in the cavity exceeds about 250 mL, the dias-
to the beginning of the descending aorta (see CD Fig. 4-3).
tolic filling is compromised, a condition known as cardiac
During fetal life, blood passes through it from the pul-
tamponade.
monary artery to the aorta, thus bypassing the lungs. After
birth, it normally constricts, later closes, and becomes the
ligamentum arteriosum.
Pericardiocentesis
Failure of the ductus arteriosus to close may occur as an
This procedure is used in the treatment of cardiac
isolated congenital abnormality or may be associated with
tamponade.
congenital heart disease. A persistent patent ductus arterio-
The patient is placed in a supine position with the
sus results in high-pressure aortic blood passing into the pul-
shoulders raised 60° from the horizontal position. The
monary artery, which raises the pressure in the pulmonary
usual skin preparation is now completed. The needle is in-
circulation. A patent ductus arteriosus is life threatening and
serted in the angle between the xiphoid process and the
should be ligated and divided surgically.
left costal margin. With the positions of the cardiac
notches of the lungs and pleura in mind (CD Fig. 4-5), the
tip of the needle is directed upward, backward, and to the
left in the left xiphocostal angle, that is, toward the left
THE PERICARDIUM
shoulder. The following structures will be penetrated by
the needle:
Traumatic Injury to the Pericardium
1. Skin
Pericardial Disruption
2. Subcutaneous tissue
This may occur from blunt trauma from a puncture following
3. Aponeurosis of the external oblique muscle of the
penetration by a fractured rib and rupture from a sudden in-
abdomen
crease in pressure. The most common location of rupture is
4. Anterior lamina of the aponeurosis of the internal
along the lateral margins, especially on the left side. The
oblique muscle of the abdomen
phrenic nerve may be involved, as it is situated between the
mediastinal parietal pleura and the pericardium (CD Fig. 4-4)
5. Rectus abdominis muscle
left phrenic
right phrenic
nerve
nerve
rupture of
rupture of
left ventricle
right atrium
CD Figure 4-4
Anterior view of
the heart showing common sites
for rupture of the pericardium on
the anterior surface. Note the po-
sition of the right and left phrenic
nerves.
72
Chapter 4
pleural reflection
internal thoracic
artery
pericardium
cardiac notch
xiphoid
pericardial cavity
process
heart
lower border
of lung
liver
diaphragm
liver
xiphoid
pleural
process
reflection
CD Figure 4-5
A and B. The xiphisternal approach for pericardiocentesis. Note that the
needle is aimed upward and backward in the direction of the left shoulder.
Anatomy of Complications
6. Posterior lamina of the aponeurosis of the internal
oblique and the transversus abdominis muscles
1. The needle is advanced too far and enters the my-
7. Extraperitoneal fat; avoid entering the peritoneal cavity
ocardium of the right ventricle.
8. Diaphragm
2. The needle pierces the anterior descending branch of
9. Pericardium (fibrous pericardium and parietal serous
the left coronary artery.
pericardium)
3. The needle enters the pleural cavity, producing a pneu-
The long large-bore needle is advanced through
mothorax or a hydropneumothorax.
the above structures and when pericardial penetration is
4. The needle pierces the liver.
achieved there is a sudden “give.” The needle is connected
to a 20-mL syringe with a three-way stopcock to permit
aspiration of the fluid.
Clinical Problem Solving Questions
Read the following case histories/questions and give
the discomfort disappeared with rest after about 5 min-
the best answer for each.
utes. The reason he came to the emergency department
was that the chest discomfort had occurred with much
A 61-year-old man was seen in the emergency depart-
less exertion.
ment complaining of a feeling of pressure within his
chest. On questioning, he said that he had several attacks
1. The following comments concerning this case are cor-
before and that they had always occurred when he was
rect except which?
climbing stairs or digging in the garden. He found that
A. The diagnosis is a classic case of angina pectoris.
The Heart, Coronary Vessels, and Pericardium
73
B. The sudden change in history, that is, pain caused
A 38-year-old woman was taken from the scene of an au-
by less exertion, should cause the physician concern
tomobile accident to the local hospital. She had been
that the patient now has unstable angina or an actual
driving her car without a seat belt on and had hit a util-
myocardial infarction.
ity pole head on. On examination she was conscious and
C. The afferent pain fibers from the heart ascend to the
alert but had sustained severe facial and chest injuries.
central nervous system through the cardiac branches
A careful examination of the chest cage revealed the
of the sympathetic trunk to enter the spinal cord.
presence of a sternal fracture (middle of the body) and
D. The afferent pain fibers enter the spinal cord via the
fractures of the third and fourth left ribs near their cos-
posterior roots of the tenth to the twelfth thoracic
tochondral junctions. After an extensive workup it was
nerves.
decided that the patient had a ruptured pericardium.
E. Pain is referred to dermatomes supplied by the up-
4.
The following observations are in agreement with the
per four intercostal nerves and the intercostal
diagnosis except which?
brachial nerve.
A. Blunt trauma had been applied to the anterior chest
A 55-year-old woman has severe aortic incompetence,
wall.
with the blood returning to the cavity of the left ventri-
B. The fractures of the third and fourth left ribs were
cle during ventricular diastole.
situated over the anterior surface of the heart.
C. The left dome of the diaphragm was paralyzed.
2.
To hear the aortic valve with the least interference from
D. The patient had tachycardia.
the other heart sounds, the best place to place your
E. The right lateral margin of the pericardium was the
stethoscope on the chest wall is
site of the rupture.
A. the right half of the lower end of the body of the
F. There were diminished breath sounds over the
sternum.
lower lobe of the left lung.
B. the medial end of the second right intercostal space.
C. the medial end of the second left intercostal space.
A 21-year-old man was walking along a city street when
D. the apex of the heart.
suddenly a burst of automatic gunfire came from a pass-
E. the fifth left intercostal space 3.5 in. (9 cm) from the
ing car. The man, who was an innocent bystander, was
midline.
struck in the front of the chest by a stray bullet. He was
rushed to the emergency department by an ambulance.
A 33-year-old woman was jogging across the park at 11
The position of the entry wound was the fourth left
PM when she was attacked by a gang of youths. After she
intercostal space about 3 in. from the midline.
was brutally mugged and raped, one of the youths de-
cided to stab her in the heart to keep her silent. Later in
5.
The following observations are in agreement with the
the emergency department she was unconscious and in
findings in this patient except which?
extremely poor shape. A small wound about 0.5 in. in di-
A. The right ventricle is the most likely chamber of the
ameter was present in the left fifth intercostal space
heart to be injured should a bullet enter the frontal
about 0.5 in. from the lateral sternal margin. Her carotid
surface of the chest.
pulse was rapid and weak, and her neck veins were dis-
B. If the bullet continues on its path, the left ventricle
tended. No evidence of a left-sided pneumothorax ex-
is also damaged, since the left ventricle lies posterior
isted. A diagnosis of cardiac tamponade was made.
to the right ventricle.
C. The circumflex branch of the left coronary artery
3.
The following observations are in agreement with the
may be damaged by the bullet as it runs down the
diagnosis except which?
anterior surface of the heart.
A. The tip of the knife had pierced the pericardium.
D. The chordae tendineae of the anterior cusp of the
B. The knife had pierced the anterior wall of the left
tricuspid valve could be injured.
ventricle.
C. The blood in the pericardial cavity was under right
A 5-year-old boy was seen in the emergency room fol-
ventricular pressure.
lowing an attack of breathlessness during which he had
D. The blood in the pericardial cavity pressed on the
lost consciousness. The mother, on questioning, said
thin-walled atria and large veins as they traversed the
that her child had had several such attacks before and
pericardium to enter the heart.
sometimes his skin had become bluish. Recently she
E. The backed-up venous blood caused congestion of
had noticed that he breathed more easily when he was
the veins seen in the neck.
playing in a squatting position; he also seemed to sleep
F. The poor venous return severely compromised the
more easily with his knees drawn up. On physical ex-
cardiac output.
amination, the child was found to be thinner and
G. A left-sided pneumothorax did not occur because
shorter than normal. His lips were cyanotic, and his fin-
the knife passed through the cardiac notch.
gers and toes were clubbed. A systolic murmur was
74
Chapter 4
present along the left border of the sternum, and the
husband the previous day and that they had been
heart was considerably enlarged to the right. An exten-
caught in a storm. She described the pain as a continu-
sive workup, including angiography, demonstrated
ous dull ache that was made worse by taking deep
tetralogy of Fallot.
breaths and using the left arm. She indicated that the
pain was localized over the sixth left costal cartilage
6.
Using your knowledge of cardiac development, criti-
about 2 in. to the left of the sternum, which corre-
cally read the following observations made in this case
sponded to an area of tenderness over the sixth left cos-
and determine the one that is incorrect.
tochondral junction.
A. The systolic murmur heard along the left border of
the sternum was caused by the pulmonary stenosis.
7.
The following possible conditions could explain the se-
B. A right-to-left shunt of blood occurs through the
vere chest pain. Choose the most likely diagnosis based
large ventricular septal defect.
on your knowledge of anatomy.
C. The aortic blood is poorly oxygenated resulting in
A. Myocardial infarction
the impaired growth of the child, the cyanosis of the
B. Lobar pneumonia of the left lung
lips, and the clubbing of the fingers and toes
C. Tearing of muscle fibers in the chest wall, possibly
D. Maintaining the squatting position during play and
the serratus anterior muscle
sleeping with the knees drawn up increases the pe-
D. Separation of the sixth left costochondral joint or an
ripheral resistance in the systemic circulation and
acute costochondritis
decreases the right-to-left shunt through the ventric-
E. Left-sided pleurisy
ular septum.
8.
The following anatomic structures are penetrated by a
E. If the patient had a large ductus arteriosus as well as the
needle when performing a pericardiocentesis except
tetralogy of Fallot, the cyanosis would be much worse.
which?
A 43-year-old woman was seen in the emergency de-
A. Skin and subcutaneous tissue
partment complaining of a severe localized pain over
B. The aponeuroses of the external and internal
the left side of the chest. She stated that the pain started
oblique muscles
quite suddenly, about 1 hour previously, when she was
C. The left parietal and visceral layers of pleura
reaching for a book on a high shelf. On further ques-
D. The rectus abdominis muscle
tioning she disclosed that she had been sailing with her
E. The diaphragm and fibrous pericardium
Answers and Explanations
1. D is the correct answer. The afferent pain fibers from
6. E is the correct answer. The tetralogy of Fallot consists
the heart enter the spinal cord via the posterior nerve
of the following: (1) a large ventricular septal defect, (2)
roots of the upper four thoracic spinal nerves.
a stenosis of the pulmonary trunk or the pulmonary
valve, (3) an exit of the aorta that lies immediately above
2. B is the correct answer. The best location to place your
the ventricular septal defect and thus communicates
stethoscope on the chest wall to hear the aortic valve is
with both ventricles, and (4) a right ventricular hyper-
the medial end of the second right intercostal space (see
trophy secondary to the ventricular septal defect and
CD Fig. 4-2).
pulmonary stenosis. Should the child have a large
3. B is the correct answer. The knife had pierced the an-
patent ductus arteriosus, cyanosis is reduced to a mini-
terior wall of the right ventricle.
mum. This is because a large patent ductus allows aor-
4. E is the correct answer. The left lateral margin of the
tic blood to enter the pulmonary trunk distal to the
pericardium had ruptured, injuring the left phrenic
stenosis of the pulmonary artery or valve and, in this
nerve; this resulted in the paralysis of the left dome of
way, enables the blood to enter the pulmonary circula-
the diaphragm and the diminished breathing heard
tion for oxygenation.
over the lower lobe of the left lung.
7. D is the correct answer. Separation of the sixth left
5. C is the correct answer. The anterior interventricular
costochondral joint or an acute costochondritis can be
(descending) branch of the left coronary artery is the
extremely painful conditions. The injury must have oc-
most likely artery to be damaged in such a wound
curred when the patient was pulling on the ropes of the
through the frontal surface of the chest.
sailing boat during the storm on the previous day. The
The Heart, Coronary Vessels, and Pericardium
75
joint is innervated by the sixth intercostal nerve and the
costal margin and directing the tip of the needle up-
pain is localized over the affected joint. This case is a
ward, backward, and to the left toward the left shoulder,
good example of somatic pain that may be intense and
the left pleura is not pierced. By passing the needle
localized, in contradistinction to visceral pain, which is
through the cardiac notches of the left lungs and pleura
diffuse and poorly localized.
both these structures are avoided (see CD Fig. 4-5).
Entry of the needle into the pleural cavity produces a
8. C is the correct answer. By placing the needle correctly
pneumothorax or hydropneumothorax.
in the angle between the xiphoid process and the left
The Blood Vessels of the
Thorax
5
Chapter Outline
Large Arteries of the Thorax
78
Coarctation of the Aorta
82
Double Aorta and Right Aortic Arch
82
The Aorta
78
Ascending Aorta and the Pericardium
78
Large Veins of the Thorax
83
Aneurysm of the Arch of the Aorta
78
Penetrating Injuries
83
Coarctation of the Aorta
78
Migrating Bullets
83
Trauma to the Aorta in the Thorax
78
Deceleration Injuries
78
Superior Vena Cava or Brachiocephalic Vein
Penetrating Injuries of the Aorta
79
Thrombosis
83
The Descending Thoracic Aorta and the
Important Connections between the Superior and
Esophagus in Posterior Thoracotomy
79
Inferior Venae Cavae
83
The Descending Thoracic Aorta and Left
79
Embryologic Note: Fetal Circulation and
Hemothorax
Aortic Dissection
79
Changes in Fetal Circulation at Birth
83
Fetal Circulation
83
The Pulmonary Trunk
80
Penetrating Injuries of the Pulmonary Trunk
80
Changes in the Fetal Circulation at Birth
84
Pulmonary Artery (Swan-Ganz) Catheterization
80
Physiologic Note: Blood Flow in the
Pulmonary Embolism
80
Umbilical Cord after Delivery
84
Embryologic Note: Detailed Development
Physiologic Note: The Heart in
of the Large Arteries of the Thorax and
the Newborn
87
the Ductus Arteriosus
81
Clinical Problem Solving Questions
87
Congenital Anomalies
82
Patent Ductus Arteriosus
82
Answers and Explanations
87
Coarctation of the Aorta
LARGE ARTERIES
Coarctation of the aorta is a congenital narrowing of the aorta
just proximal, opposite, or distal to the site of attachment of
OF THE THORAX
the ligamentum arteriosum (CD Fig. 5-1). Clinically, the
cardinal sign of aortic coarctation is absent or diminished
pulses in the femoral arteries of both lower limbs. To com-
The Aorta
pensate for the diminished volume of blood reaching the
lower part of the body, an enormous collateral circulation
Ascending Aorta and the Pericardium
develops, with dilatation of the internal thoracic, subclavian,
and posterior intercostal arteries. The dilated intercostal
The entire ascending aorta lies within the pericardial sac.
arteries erode the lower borders of the ribs, producing char-
Consequently, tear or rupture of this part of the aorta results
acteristic notching, which is seen on radiographic examina-
in a massive outpouring of blood into the pericardial cavity,
tion. The condition should be treated surgically.
producing cardiac tamponade.
Trauma to the Aorta in the Thorax
Aneurysm of the Arch of the Aorta
Deceleration Injuries
The arch of the aorta lies behind the manubrium sterni. A
gross dilatation of the aorta (aneurysm) may show itself as a
The heart is suspended from the aorta much like a weight
pulsatile swelling in the suprasternal notch.
attached to the end of a curved piece of flexible tubing.
The Blood Vessels of the Thorax
79
left subclavian
The Descending Thoracic Aorta and the
artery
Esophagus in Posterior Thoracotomy
arch of aorta
The relationship of the aorta and the esophagus in the pos-
terior mediastinum is important when distinguishing
descending aorta
between these structures when performing an emergency
thoracotomy.
coarctation of
aorta
The Descending Thoracic Aorta and
ligamentum
arteriosum
Left Hemothorax
The close relationship of the descending thoracic aorta to
the left pleura and lung means that rupture of the aorta may
occur into the left pleural cavity, producing a massive
hemothorax.
Aortic Dissection
CD Figure 5-1
Coarctation of the aorta.
This is the most serious and difficult form of aortic disease
to treat (CD Fig. 5-2). Degeneration of the tunica media
of the aortic wall is believed to be the basic cause, and the
In horizontal deceleration injuries the movement of
condition is associated with a history of hypertension in the
the body is suddenly stopped and the heart continues to
majority of patients. Marfan’s disease can also be responsi-
move forward within the pericardial sac. The descending
ble for the degeneration. Hemorrhage occurs through the
thoracic aorta from the point of origin of the left subclavian
tunical intima and extends as an expanding hematoma
artery onward is firmly attached to the vertebral column by
between the middle and outer thirds of the tunica media.
connective tissue and pleura. As the heart continues to
The initial tear may occur anywhere along the thoracic
move forward on body impact, the curve of the arch of the
aorta. Type A (proximal dissection) involves the ascend-
aorta is slightly straightened and the vessel shears just distal
ing aorta or ascending and descending aorta (see CD Fig.
to the origin of the left subclavian artery. The aorta may be
5-2). Type B (distal dissection) does not involve the
completely transected and be accompanied by a massive
ascending aorta and usually begins distal to the left subcla-
hemorrhage. If the trauma to the aorta is less, a tear may
vian artery. The clinical signs and symptoms will depend
occur in the aortic wall, leaving the more resilient outer
on the type of aneurysm present and the extent of distal
connective tissue coat intact. Blood then dissects between
propagation.
the layers of the aortic wall, producing a false aneurysm.
The sudden onset of excruciating, sharp, tearing pain
In vertical deceleration injuries, as in falls from a
localized to the front or the back of the chest and back is a
height, the violent pull of the heart on the end of the aortic
typical presenting symptom. It must be assumed that the
arch causes a tear in the inner coat of the aortic wall at the
pain impulses originate in the aortic wall, ascend to the
root of the ascending aorta. If rupture of the ascending aorta
central nervous system along with the sympathetic nerves,
should ensue, the aortic blood would burst into the pericar-
and enter the spinal cord through the posterior roots of the
dial sac, causing immediate cardiac tamponade. The
segmental spinal nerves. The pain is then referred along
ascending aorta together with the pulmonary trunk is sur-
the somatic spinal nerves of the same segments. The num-
rounded only by a thin sleeve of serous pericardium and by
ber of dermatomes involved will depend on the extent of
the fibrous pericardium. Once the sleeve of serous peri-
the dissection. If the dissection continues to spread distally,
cardium gives way, the blood enters the pericardial cavity,
the pain may be felt segmentally in the abdomen, lower
causing cardiac tamponade. Most of these injuries are fatal.
back, and legs.
An aneurysm of the ascending aorta has the highest
Penetrating Injuries of the Aorta
mortality since it may rupture into the pericardial cavity, pro-
Penetrating vascular injuries are likely to occur when the
ducing immediate cardiac tamponade; it may rupture into
entrance and exit wounds are on opposite sides of the chest,
the mediastinum or pleural cavities; it may extend into the
indicating that the bullet has crossed the midline of the
coronary arteries, causing occlusion; or it may extend to
chest. Penetrating injuries involving blood vessels and not
the aortic valve, producing acute aortic incompetence.
the heart have the highest mortality when they occur in the
Involvement of the brachiocephalic, left common carotid, or
superior mediastinum; here the aortic arch gives rise to its
left subclavian arteries at their origin from the aortic arch may
major branches, and the superior vena cava and brachio-
give rise to symptoms of cerebral ischemia or upper limb
cephalic veins are present.
ischemia.
80
Chapter 5
CD Figure 5-2
Aortic dissec-
tion. Type A (proximal dissec-
tion) involves the ascending
aorta or ascending and descend-
ing aorta. Type B (distal dissec-
tion) does not involve the
ascending aorta.
An aneurysm of the descending thoracic aorta can rup-
into the pericardial cavity from either of these vessels could
ture into the pleural cavity on the left side. If the dissection
result in cardiac tamponade.
progresses distally to involve the abdominal aorta, occlusion
Pulmonary Artery (Swan-Ganz)
of the mesenteric arteries could result in bowel infarction,
and occlusion of the renal arteries could result in renal
Catheterization
failure. Ischemic necrosis of the spinal cord resulting in para-
The pulmonary artery catheter is used to assess left and right
plegia could follow blockage of the posterior intercostal
ventricular function, measure pulmonary artery and right and
arteries arising from the thoracic aorta or the lumbar arteries
left atrial pressures, measure cardiac output, and take samples
arising form the abdominal aorta.
of right atrial and pulmonary arterial blood.
Rupture of the aneurysm below the diaphragm may
The catheter is introduced through the right internal
produce catastrophic retroperitoneal hemorrhage.
jugular vein, right subclavian vein, right basilic vein, or the
femoral vein. The catheter is advanced into the right atrium
The Pulmonary Trunk
through the tricuspid valve into the right ventricle (CD Fig.
5-3). The balloon is advanced into the pulmonary trunk and
Penetrating Injuries of the Pulmonary
then into the left pulmonary artery.
Trunk
Pulmonary Embolism
Any missile injury with entry or exit wounds close to the
manubrium sterni may damage the pulmonary trunk or any
In the great majority of patients, the pulmonary emboli arise
other vessel in the superior mediastinum, Remember that
from a thrombosis in the large deep veins of the lower
the pulmonary trunk and the ascending aorta together are
extremity, especially from the femoral veins, and from the
surrounded by a sheath of serous pericardium within the
internal iliac veins in the pelvis. Thromboses in the veins of
fibrous pericardium (see text Fig. 4-21), so that hemorrhage
the calf muscles following prolonged immobility, such as
The Blood Vessels of the Thorax
81
carotid sheath
platysma
skin
thyroid gland
sternocleido-
mastoid
muscle
investing layer of
deep fascia
common carotid
artery
catheter
sternocleidomastoid
muscle
catheter
scalenus anterior
internal
vagus nerve
subclavian
muscle
jugular
vein
vein
arch of aorta
left pulmonary
superior
artery
vena cava
pulmonary valve
right atrium
tricuspid valve
right ventricle
catheter
CD Figure 5-3
Pulmonary artery (Swan-Ganz) catheterization. A. The catheter has been
introduced through the right internal jugular vein (posterior approach). B. Diagram show-
ing the course taken by the catheter through the right side of the heart into the pulmonary
trunk and the left pulmonary artery.
commonly occurs in long-distance plane flights, may be the
The ascending aorta below the right pulmonary
origin of pulmonary emboli.
artery and the main pulmonary trunk are derived from the
truncus arteriosus (see CD Fig. 5-4). The aorta, from the
level of the right pulmonary artery up to the level of the left
E M B R Y O L O G I C N O T E
common carotid artery, is derived from the aortic sac.
The brachiocephalic artery also is formed from
Detailed Development of the Large Arteries
the aortic sac. The remainder of the arch of the aorta is
of the Thorax and the Ductus Arteriosus
formed from the left fourth aortic arch artery and the left
The truncus arteriosus, which is the distal part of the
dorsal aorta (see CD Fig. 5-4).
bulbus cordis (CD Fig. 5-4) is continuous beyond the peri-
The fourth right aortic arch artery becomes the root
cardium with a large vessel called the aortic sac. This sac
of the right subclavian artery, which also is derived in
gives off two branches, each of which runs dorsally in the
sequence from a small part of the right dorsal aorta and
first pharyngeal arch on each side in the developing em-
the right seventh segmental artery.
bryo. The branches then pass caudally in the posterior
The third aortic arch artery on both sides becomes
wall of the embryo as the two dorsal aortae. Five addi-
the common carotid artery; this sends off a bud of
tional arteries now join the aortic sac to the dorsal aortae
mesenchyme that becomes the external carotid
(see CD Fig. 5-4). Meanwhile, the two dorsal aortae fuse
artery. The remainder of the third aortic arch artery and
throughout much of their lengths to form the descend-
part of the dorsal aorta form the internal carotid artery
ing thoracic aorta and the abdominal aorta.
on each side.
82
Chapter 5
CD Figure 5-4 The formation and fate of the aortic arch arteries.
The first, second, and fifth aortic arch arteries
with congenital heart disease. A persistent patent ductus
disappear completely. The right and left pulmonary
arteriosus results in high-pressure aortic blood passing
arteries are formed from the sixth aortic arch arteries.
into the pulmonary artery, which raises the pressure
The distal part of the right sixth aortic arch artery
in the pulmonary circulation. A patent ductus arteriosus
disappears, while the remainder of the left sixth aortic
is life threatening and should be ligated and divided
arch artery becomes the important ductus arteriosus,
surgically.
which after birth becomes the ligamentum arte-
Coarctation of the Aorta
riosum.
Coarctation of the aorta is a congenital narrowing of the
The descending thoracic aorta below the level of
aorta just proximal, opposite, or distal to the site of attach-
the fourth thoracic vertebra is formed from the fusion of
ment of the ligamentum arteriosum (see CD Fig. 5-1). This
the dorsal aortae (see CD Fig. 5-4).
condition is believed to result from an unusual quantity of
ductus arteriosus muscle tissue in the wall of the aorta.
Congenital Anomalies
When the ductus arteriosus contracts, the ductal muscle in
Patent Ductus Arteriosus
the aortic wall also contracts, and the aortic lumen be-
The ductus arteriosus represents the distal portion of the
comes narrowed. Later, when fibrosis takes place, the aor-
sixth left aortic arch and connects the left pulmonary
tic wall also is involved, and permanent narrowing occurs.
artery to the beginning of the descending aorta (see CD
Fig. 5-4). During fetal life, blood passes through it from
Double Aorta and Right Aortic Arch
the pulmonary artery to the aorta, thus bypassing the
Anomalies involving double parts of the arterial system
lungs. After birth, it normally constricts, later closes, and
are rare conditions that result from the persistence of
becomes the ligamentum arteriosum.
aortic arch arteries, which normally disappear. In the
Failure of the ductus arteriosus to close may occur as
case of the right aortic arch, the development of the left
an isolated congenital abnormality or may be associated
arch does not take place.
The Blood Vessels of the Thorax
83
E M B R Y O L O G I C N O T E
LARGE VEINS OF
Fetal Circulation and Changes in Fetal
THE THORAX
Circulation at Birth
Fetal Circulation
Penetrating Injuries
Starting at the placenta, the fetal blood may be traced in
the circulation as follows:
As has been emphasized before with arterial injuries, the
Having circulated through the capillaries of the pla-
highest mortality can occur in penetrating injuries in the re-
cental villi, the fetal blood returns through the umbilical
gion of the superior mediastinum. Behind the manubrium
vein to the fetus about 80% saturated with oxygen and
sterni lie not only the aortic arch and its large branches but
containing many important nutrients, antibodies, and
also the right and left brachiocephalic veins and the superior
hormones (CD Fig. 5-6). The oxygenated blood then
vena cava. Moreover, the thoracic cage may hide the extent
passes toward the liver. However, the greater volume of
of the bleeding, which may take place entirely within the
it bypasses the liver, since this organ is not fully func-
thoracic cavity. The cage also renders the veins relatively
tioning, and travels to the inferior vena cava by way of
inaccessible to the operating physician.
the ductus venosus. The remainder is distributed to the
liver sinusoids by offshoots of the umbilical vein, and this
Migrating Bullets
in turn passes to the inferior vena cava by the hepatic
veins. At the same time, the ductus venosus receives
Bullets entering a large artery or vein may migrate with the
poorly oxygenated blood from the gut by way of the left
blood from their site of entrance. Bullets in the aorta can
branch of the portal vein. In addition, the inferior vena
migrate to the distal branches until they become wedged,
cava already contains venous blood from the lower part
causing blockage and ischemia. In the same manner, a
of the trunk and the lower limbs of the fetus. As a conse-
bullet entering a pulmonary vein can migrate to the left
quence of this admixture of blood from these various
atrium and left ventricle and enter the systemic circulation.
sources, the inferior vena cava contains blood about 67%
A bullet entering the superior vena cava can migrate into the
saturated with oxygen.
right atrium and right ventricle and enter the pulmonary
Before considering the further passage of the fetal
circulation. Paradoxic movement of bullets through a
blood, it is necessary to examine the anatomic arrange-
patent atrial septum has been reported.
ment of the inferior vena cava and its relationship with
the right and left atria in the fetal heart (CD Fig. 5-7). In the
Superior Vena Cava or
fetus, the opening of the inferior vena cava into the right
atrium lies directly opposite the foramen ovale. Thus,
Brachiocephalic Vein
blood entering the heart through the inferior vena cava is
directed through the foramen ovale and enters the left
Thrombosis
atrium. This process is assisted by the presence of the
This condition usually results from compression of the veins
valve of the inferior vena cava.
by tumors in the superior mediastinum; enlarging lymph
The nutritious oxygenated fetal blood, on reaching
node metastases secondary to a bronchial carcinoma is a
the foramen ovale, is divided into two streams by the
common cause. Venous blockage results in engorgement of
crista dividens, which is the lower margin of the sep-
the veins of the head and neck.
tum secundum. The greater volume of blood enters the
left atrium, and the remainder, joined by venous blood
from the superior vena cava and coronary sinus, passes
Important Connections between
from the right atrium into the right ventricle.
The oxygenated blood in the left atrium is joined by
the Superior and Inferior Venae
a relatively small volume of blood from the nonaerated
fetal lungs. The left atrial blood then passes into the left
Cavae
ventricle and out into the aorta. The oxygen saturation of
In obstruction of the superior or inferior venae cavae, the
this blood is about 62%. This is distributed chiefly to the
azygos veins provide an alternative pathway for the return of
arteries of the head, neck, and upper extremities. Thus, it
venous blood to the right atrium of the heart. This is possi-
is apparent that blood that is richer in oxygen and nutri-
ble since these veins and their tributaries connect the supe-
ents is transported to the cephalic region rather than the
rior and inferior venae cavae (CD Fig. 5-5).
caudal regions of the fetus.
84
Chapter 5
brachiocephalic
vein
superior vena cava
subclavian vein
first rib
axillary vein
hemiazygos veins
azygos vein
internal thoracic vein
lateral thoracic vein
diaphragm
inferior vena cava
ascending lumbar
vein
lumbar veins
inferior mesenteric
inferior epigastric vein
vein ascending to
portal vein
CD Figure 5-5
The possible col-
lateral circulations of the superior
and inferior venae cavae. Note the
superficial epigastric
alternative pathways that exist for
vein
superior rectal vein
blood to return to the right atrium
internal iliac vein
of the heart if the superior vena
external iliac vein
cava becomes blocked below the
entrance of the azygos vein (upper
inguinal ligament
black bar). Similar pathways exist
if the inferior vena cava becomes
middle rectal vein
blocked below the renal veins
femoral vein
(lower black bar). Note also the
connections that exist between the
portal circulation and systemic
great saphenous
inferior rectal vein
vein
veins in the anal canal.
Changes in Fetal Circulation at Birth
Meanwhile, the right ventricular blood passes into
the pulmonary trunk. Only a small portion of this passes
Immediately after birth the umbilical cord is tied,
into the unexpanded lungs, since the vascular resistance
thus severing the placental extension of the fetal
is high. Most of the blood bypasses the lungs by being
circulation.
directed through the wide channel, the ductus arterio-
sus, into the descending thoracic aorta (see CD Fig. 5-6).
The now relatively poor oxygenated blood passes
P H Y S I O L O G I C N O T E
down the descending thoracic and abdominal aortae and
supplies the thoracic and abdominal viscera and lower
Blood Flow in the Umbilical Cord after
limbs. The fetal blood, which by this time is loaded with
Delivery
waste products of metabolism and carbon dioxide, then
returns to the placenta through the right and left umbili-
In cases in which the umbilical cord is not tied, the blood
cal arteries, where the waste products and carbon
flow may continue for several minutes after delivery,
dioxide are eliminated and oxygen is picked up. The cir-
although at a rapidly decreasing rate. A number of fac-
culatory cycle then is repeated.
tors may contribute to this diminishing flow, including (1)
The Blood Vessels of the Thorax
85
CD Figure 5-6
Fetal circulation. R.A. right atrium, R.V. right ventricle, L.A. left
atrium, L.V. left ventricle.
the contraction of the uterus and the effect of this on the
The interruption of umbilical flow when the cord is tied
placental attachment and (2) constriction of the umbilical
results in an immediate fall in blood pressure in the inferior
vessels as the result of mechanical stimulation or the
vena cava. This fact, coupled with the increased left atrial
presence in the fetal circulation of catecholamines. The
pressure from the increased pulmonary blood flow, causes
fetal blood volume may be increased by as much as 100
the foramen ovale to close (CD Fig. 5-8). From that moment
mL if the tying of the cord is delayed. However, it gener-
onward the valve of the foramen ovale is kept closed by the
ally is agreed that there is no advantage in delaying the
hemodynamic changes, and within a few days of birth the
tying beyond a minute after delivery.
valve becomes attached to the edge of the foramen ovale.
86
Chapter 5
CD Figure 5-7
Relationship between
the opening of the inferior vena cava
and the foramen ovale.
CD Figure 5-8
The circulatory
system after birth. Compare
this with the circulation in the
fetus (CD Fig. 5-6). R.A. right
atrium, R.V. right ventricle,
L.A. left atrium, L.V. left
ventricle.
The Blood Vessels of the Thorax
87
The diminished pulmonary vascular resistance asso-
P H Y S I O L O G I C N O T E
ciated with inflation of the lungs cause the direction of
flow (from right to left) through the ductus arteriosus
The Heart in the Newborn
to be changed to the neonatal route of left to right. The
ductus arteriosus constricts as a reaction of its muscle
The heart in the newborn is relatively large and is higher
to the raised oxygen tension. It later closes and becomes
in the thorax and in a more horizontal position than it is
the ligamentum arteriosum. One week after birth its
in later life. The pulse rate is rapid, with an average of 130
lumen is 2 mm or less in diameter, and by the end of the
beats per minute. The rate may rise considerably with
first month it usually has closed (see CD Fig. 5-8). In ad-
crying and fall to around 80 during sleep. The peripheral
dition, the wall of the ductus venosus contracts and the
circulation initially is slow in the newborn. The hands and
lumen is closed. Later the ductus becomes fibrosed to
feet may be cold and slightly cyanotic for the first few
form the ligamentum venosum.
hours after birth.
Clinical Problem Solving Questions
Read the following case histories/questions and give
were swollen 3 weeks earlier. He admitted being a heavy
the best answer for each.
smoker and had on several occasions coughed up blood-
stained sputum. On examination, his face looked puffy,
1. A 16-year-old girl, on examination in the doctor’s of-
especially around the eyes. Pitting edema was present in
fice, was found to have absent pulses in both femoral
both the upper limbs, the face, and the neck. With the
arteries. In addition, her blood pressure was higher
patient in the recumbent position, numerous dilated su-
in both upper limbs than in both lower limbs.
perficial veins were seen over the chest wall and ab-
An anteroposterior radiograph of the chest showed
domen. Later a chest radiograph revealed a large opac-
notching of the necks of the upper ribs on both sides.
ity in the upper lobe of the right lung. A diagnosis of ad-
What is your diagnosis? Why is there notching of the
vanced bronchogenic carcinoma of the right upper lobe
ribs?
was made. Can you explain the presence of edema in
2. Name the common sites on the thoracic aorta where
both the upper limbs, the face, and the neck? What is the
damage occurs in blunt trauma. Between 80% and 90%
cause of the dilated superficial veins of the chest and ab-
of such injuries result in immediate death. Explain in
dominal walls? Is there normally communication be-
anatomic terms the path commonly taken by the escap-
tween the main veins draining the upper part of the body
ing blood in cases of traumatic rupture of the thoracic
and those draining the lower half of the body?
aorta. Name the tissues that can sometimes temporarily
4. A fourth-year medical student was asked by a pediatri-
control the leak, thus permitting the patients to be taken
cian what factors are responsible for the closure of the
to the emergency department alive.
foramen ovale in the atrial septum at birth. The student
3. A 56-year-old man was seen in the emergency depart-
also was asked if oxygenated or deoxygenated blood nor-
ment complaining of swelling of both arms. On
mally passes through the foramen ovale during fetal
questioning, he said that he first noticed that his hands
life. How would you answer these questions?
Answers and Explanations
1. Coarctation of the aorta is a narrowing of the aorta just
ductus muscle in the aortic wall also contracts and the
proximal, opposite, or distal to the site of attachment of
aortic lumen becomes narrowed. Later, fibrosis occurs
the ligamentum arteriosum. It is believed to result from
and permanent narrowing takes place. The notching of
the presence of an unusual quantity of ductus arteriosus
the lower borders of the ribs is caused by the opening up
muscle tissue incorporated in the wall of the aorta.
of the collateral circulation through the subclavian, in-
When the ductus arteriosus contracts after birth, the
ternal thoracic, and posterior intercostal arteries to carry
88
Chapter 5
blood from above the coarctation to the distal part of
clearly indicate the presence of a superior vena caval
the aorta ; it is the dilated posterior intercostal arteries
obstruction. This obstruction was caused by the ex-
that notch the ribs.
panding metastases in the mediastinal lymph nodes
secondary to the bronchogenic carcinoma. The dilated
2.
Blunt traumatic injury to the thoracic aorta involving
superficial veins included the lateral thoracic vein, a
horizontal deceleration occurs most commonly just dis-
tributary of the axillary vein; lumbar veins, tributaries
tal to the origin of the left subclavian artery. This site is
of the inferior vena cava; and the superficial epigastric
vulnerable since the heart and the aortic arch are mobile
vein, a tributary of the great saphenous vein of the leg
and the descending aorta is fixed. Sudden vertical de-
that drains into the femoral vein. These venous chan-
celeration, as in a fall, may result in an intimal tear at the
nels provide an alternative pathway in superior vena
root of the ascending aorta; the momentum of the heart
caval obstruction, permitting superior vena caval blood
filled with blood is sufficient to produce the tear.
to return to the heart via the inferior vena cava. The
Rupture of the ascending aorta occurs into the pericar-
superior vena cava normally communicates with the
dial cavity, producing immediate cardiac tamponade
inferior vena cava through the azygos veins. However,
and death. Rupture of the descending thoracic aorta
in this case the tumor was pressing on the superior vena
frequently occurs into the left pleural cavity. The tear
cava proximal to the entrance of the azygos vein.
initially occurs in the tunica intima; the tunica media
4.
The foramen ovale is closed after birth by the valve-like
and adventitia and the surrounding connective tissue
flap formed by the lower part of the septum primum
and the pleura may delay the complete rupture or tem-
pressing against the septum secundum and fusing with it.
porarily control the leak. If untreated, delayed rupture
This takes place as a result of a rise in blood pressure in
and death usually occur in these cases within 2 weeks.
the left atrium, which occurs once the child takes a deep
3.
The swelling of both upper extremities and the head
breath and the pulmonary circulation is established.
and neck, caused by edema, and the engorgement of
During fetal life, oxygenated blood passes through the
the superficial veins of the chest and abdominal walls
foramen ovale from the right atrium to the left atrium..
The Blood Vessels of the
Head and Neck
6
Chapter Outline
Large Arteries of the Head and Neck
90
Cavernous Sinus Thrombosis and Facial Infection
93
Taking the Carotid Pulse
90
Spread of Infection and the Emissary Veins
93
Carotid Sinus Sensitivity
90
Visibility of the External Jugular Vein
94
Facial Artery Pulse
90
The External Jugular Vein as Venous Manometer
94
Temporal Artery Pulse
91
External Jugular Vein Catheterization
94
Middle Meningeal Artery and
Penetrating Wounds of the Internal Jugular Vein
94
Extradural Hemorrhage
91
Internal Jugular Vein Catheterization
94
Atherosclerosis of the Carotid Arteries and
Subclavian Vein Thrombosis
94
Neurologic Injury
91
Subclavian Vein Catheterization
94
Penetrating Neck Injuries to the Carotid Arteries
92
Infraclavicular Approach
95
Anatomy of the Procedure
95
Aneurysms of the Carotid Arteries
92
Anatomy of Problems
96
Cerebral Circulation and the Circle of Willis
93
Anatomy of Complications
96
Compression of the Subclavian Artery and the
The Procedure in Children
97
Brachial Plexus at the Root of the Neck
93
Supraclavicular Approach
97
Anatomy of the Procedure
98
Cerebrovascular Disease
93
Anatomy of Complications
98
Cerebral Ischemia
93
Internal Thoracic Artery and Coronary Bypass
Clinical Problem Solving Questions
98
Operations
93
Palpation and Compression of the Subclavian Artery
Answers and Explanations
100
in Patients with Upper Limb Hemorrhage
93
Veins of the Head and Neck
93
The Sigmoid Sinus and Infection from the
Mastoid Antrum
93
rior border of the thyroid cartilage. This is a convenient site
LARGE ARTERIES
to take the carotid pulse.
OF THE HEAD ANDCarotid Sinus Sensitivity
In cases of carotid sinus hypersensitivity, pressure on one or
NECK
both carotid sinuses can cause excessive slowing of the heart
rate, a fall in blood pressure, and cerebral ischemia with
fainting.
Taking the Carotid Pulse
The bifurcation of the common carotid artery into the in-
Facial Artery Pulse
ternal and external carotid arteries (see text Figs. 6-1 and
6-3) can be easily palpated just beneath the anterior border
The facial artery (see text Fig. 6-1), as it winds around the
of the sternocleidomastoid muscle at the level of the supe-
lower margin of the mandible level with the anterior border
The Blood Vessels of the Head and Neck
91
of the masseter, is commonly used by the anesthetist to take
pressure on the underlying motor area in the precentral
the patient’s pulse.
gyrus. Blood may also pass outward through the fracture line
to form a soft swelling under the temporalis muscle.
To stop the hemorrhage, the torn artery or vein must be
Temporal Artery Pulse
ligated or plugged. The burr hole through the skull wall
The superficial temporal artery, as it crosses the zygomatic
should be placed about 1 to 1.5 in. (2.5 to 4 cm) above the
arch in front of the ear (see text Fig. 6-1), can also be used
midpoint of the zygomatic arch (CD Fig. 6-2).
by the anesthetist to take the patient’s pulse.
Atherosclerosis of the Carotid
Middle Meningeal Artery and
Arteries and Neurologic Injury
Extradural Hemorrhage
Approximately 70% of strokes are caused by extracranial ar-
Extradural hemorrhage results from injuries to the
teriosclerosis of the carotid and/or vertebral arteries. In the
meningeal arteries or veins. The most common artery to be
carotid arteries the atherosclerotic thromboses usually form
damaged is the anterior division of the middle meningeal
slowly in the distal part of the common carotid and the first
artery (CD Fig. 6-1). A comparatively minor blow to the side
parts of the external and internal carotid arteries. The result
of the head, resulting in fracture of the skull in the region of
is a diminished blood flow to the central nervous system. Less
the anteroinferior portion of the parietal bone, may sever the
commonly, emboli, formed of fragments of plaques or blood
artery. The arterial or venous injury is especially liable to
clots, are carried distally to lodge in the ipsilateral central
occur if the artery and vein enter a bony canal in this region.
artery of the retina or in the smaller branches of the middle
Bleeding occurs and strips up the meningeal layer of dura
cerebral artery. Such a situation could produce the classic
from the internal surface of the skull. The intracranial
syndrome of ipsilateral blindness and contralateral hemiple-
pressure rises, and the enlarging blood clot exerts local
gia, although it is unusual to have both at the same time.
central sulcus
motor area of cerebral cortex
trunk
parietal
eminence
head
pterion
anterior branch of
middle meningeal artery
nasion
baseline
external occipital
protuberance
cerebellum
mastoid
process
zygomatic
arch
CD Figure 6-1
Surface landmarks on the right side of the head. The relations of the mid-
dle meningeal artery and the brain to the surface of the skull are shown.
92
Chapter 6
site of
of burr hole
A
tragus
of ear
anterior branch of
middle meningeal
artery
blood clot
lying between
endosteal layer
and meningeal
layer of dura
CD Figure 6-2
A. Surface
landmarks for a temporal burr
hole. B. The vertical incision
zygomatic
passes through the temporalis
arch
muscle down to bone. The
B
middle meningeal artery lies
between the endosteal and
meningeal layers of dura and is
embedded in the endosteal
layer of dura or lies in a bony
tunnel.
likely to cause neurologic problems, provided there is ade-
Penetrating Neck Injuries to the
quate collateral circulation through the external carotid
arteries and their branches.
Carotid Arteries
Hemorrhage may be severe, with consequent hypotension
Aneurysms of the Carotid Arteries
or shock. An enlarging hematoma may press on the larynx
or trachea, compromising the airway. Injuries to the internal
Aneurysms of the carotid arteries in the neck are rare and are
carotid artery are usually associated with a central neuro-
usually caused by arteriosclerosis. They are commonly located
logic deficit. Injuries to the common carotid arteries are less
at the bifurcation of the common carotid artery. Expansion of
The Blood Vessels of the Head and Neck
93
the aneurysm may create pressure on the vagus nerve (causing
inserting a graft. The graft most commonly used is the great
hoarseness), glossopharyngeal nerve (causing dysphagia), or
saphenous vein of the leg. In some patients, the my-
hypoglossal nerve (causing weakness of the tongue); pressure
ocardium can be revascularized by surgically mobilizing
on the sympathetic trunk as it lies behind the carotid sheath
one of the internal thoracic arteries (see text Fig. 6-2) and
may cause Horner’s syndrome. Rupture of the aneurysm re-
joining its distal cut end to a coronary artery.
sulting in hemorrhage may exert pressure on surrounding
structures and compromise the airway (see text Fig. 6-5).
Palpation and Compression of the
Cerebral Circulation and the Circle
Subclavian Artery in Patients
of Willis
with Upper Limb Hemorrhage
The circle of Willis allows blood that enters by either internal
In severe traumatic accidents to the upper limb involving
carotid or vertebral arteries to be distributed to any part of
laceration of the brachial or axillary arteries, it is important
both cerebral hemispheres. The arterial circle permits the
to remember that the hemorrhage can be stopped by ex-
blood to flow across the midline, as shown when the internal
erting strong pressure downward and backward on the
carotid or vertebral artery on one side is blocked by disease.
third part of the subclavian artery (see text Fig. 6-2). The
use of a blunt object to exert the pressure is of great help,
and the artery is compressed against the upper surface of
Compression of the Subclavian
the first rib.
Artery and the Brachial Plexus at
the Root of the Neck
VEINS OF THE
At the root of the neck, the brachial plexus and the subcla-
vian artery enter the posterior triangle through a narrow
HEAD AND NECK
muscular-bony triangle (see text Fig. 6-2). The boundaries
of the narrow triangle are formed in front by the scalenus
The Sigmoid Sinus and Infection
anterior, behind by the scalenus medius, and below by the
first rib. In the presence of a cervical rib, the first thoracic
from the Mastoid Antrum
nerve and the subclavian artery are raised and angulated as
they pass over the rib. Partial or complete occlusion of the
Infection of the mastoid antrum of the ear may spread
artery causes ischemic muscle pain in the arm, which is
to the sigmoid venous sinus, causing thrombosis and
worsened by exercise. Rarely, pressure on the first thoracic
septicemia.
nerve causes symptoms of pain in the forearm and hand and
wasting of the small muscles of the hand.
Cavernous Sinus Thrombosis and
Cerebrovascular Disease
Facial Infection
The area of facial skin bounded by the nose, the eye,
Cerebral Ischemia
and the upper lip is a potentially dangerous zone to
Unconsciousness occurs in 5 to 10 seconds if the blood flow
have an infection. For example, a boil in this region can
to the brain is completely cut off. Irreversible brain damage
cause thrombosis of the facial vein, with spread of
with death of nervous tissue rapidly follows complete arrest
organisms through the inferior ophthalmic veins to
of cerebral blood flow. It has been estimated that neuronal
the cavernous sinus. The resulting cavernous sinus
function ceases after about 1 minute and that irreversible
thrombosis may be fatal unless adequately treated with
changes start to occur after about 4 minutes, although this
antibiotics.
time may be longer if the patient’s body has been cooled.
Spread of Scalp Infections and
Internal Thoracic Artery and
the Emissary Veins
Coronary Bypass Operations
Infections of the scalp tend to remain localized and are
In patients with occlusive coronary disease caused by ather-
usually painful because of the fibrous tissue in the subcu-
osclerosis, the diseased arterial segment can be bypassed by
taneous layer. Occasionally, an infection of the scalp
94
Chapter 6
spreads by the emissary veins (see text Fig. 6-8), which are
lacerated wall of the internal jugular vein. Because the wall
valveless, to the skull bones, causing osteomyelitis. Infected
of this large vein contains little smooth muscle, its injury is
blood in the diploic veins may travel by the emissary veins
not followed by contraction and retraction (as occurs with
farther into the venous sinuses and produce venous sinus
arterial injuries). Moreover, the adventitia of the vein wall is
thrombosis.
attached to the deep fascia of the carotid sheath, which hin-
ders the collapse of the vein. Blind clamping of the vein is
prohibited because the vagus and hypoglossal nerves are in
Visibility of the External
the vicinity.
Jugular Vein
Internal Jugular Vein
The external jugular vein is less obvious in children and
Catheterization
women because their subcutaneous tissue tends to be
thicker than the tissue of men. In obese individuals, the vein
The internal jugular vein is remarkably constant in position.
may be difficult to identify even when they are asked to hold
It descends through the neck from a point halfway between
their breath, which impedes the venous return to the right
the tip of the mastoid process and the angle of the jaw to the
side of the heart and distends the vein.
sternoclavicular joint. Above, it is overlapped by the anterior
The superficial veins of the neck tend to be enlarged
border of the sternocleidomastoid muscle, and below, it is
and often tortuous in professional singers because of pro-
covered laterally by this muscle. Just above the sternoclavic-
longed periods of raised intrathoracic pressure.
ular joint the vein lies beneath a skin depression between
the sternal and clavicular heads of the sternocleidomastoid
muscle. In the posterior approach, the tip of the needle and
The External Jugular Vein as a
the catheter are introduced into the vein about two finger-
Venous Manometer
breadths above the clavicle at the posterior border of the
sternocleidomastoid muscle (CD Fig. 6-4). In the anterior
The external jugular vein serves as a useful venous manome-
approach, with the patient’s head turned to the opposite
ter. Normally, when the patient is lying at a horizontal angle
side, the triangle formed by the sternal and clavicular heads
of 30°, the level of the blood in the external jugular veins
of the sternocleidomastoid muscle and the medial end of
reaches about one third of the way up the neck. As the pa-
the clavicle are identified. A shallow skin depression usually
tient sits up, the blood level falls until it is no longer visible
overlies the triangle. The needle and catheter are inserted
behind the clavicle.
into the vein at the apex of the triangle in a caudal direction
(see CD Fig. 6-4).
External Jugular Vein
Subclavian Vein Thrombosis
Catheterization
Spontaneous thrombosis of the subclavian and/or axillary
The external jugular vein can be used for catheterization,
veins occasionally occurs after excessive and unaccustomed
but the presence of valves or tortuosity may make the
use of the arm at the shoulder joint. The close relationship
passage of the catheter difficult. Because the right exter-
of these veins to the first rib and the clavicle and the possi-
nal jugular vein is in the most direct line with the supe-
bility of repeated minor trauma from these structures is
rior vena cava, it is the one most commonly used (CD
probably a factor in its development.
Fig. 6-3).
Secondary thrombosis of subclavian and/or axillary
The vein is catheterized about halfway between the
veins is a common complication of an indwelling venous
level of the cricoid cartilage and the clavicle. The passage of
catheter. Rarely, the condition may follow a radical mas-
the catheter should be performed during inspiration when
tectomy with a block dissection of the lymph nodes of the
the valves are open.
axilla. Persistent pain, heaviness, or edema of the upper
limb, especially after exercise, is a complication of this
condition.
Penetrating Wounds of the
Internal Jugular Vein
Subclavian Vein Catheterization
The hemorrhage of low-pressure venous blood into the
The subclavian vein is located in the lower anterior cor-
loose connective tissue beneath the investing layer of deep
ner of the posterior triangle of the neck (CD Fig. 6-5),
cervical fascia may present as a large, slowly expanding
where it lies immediately posterior to the medial third of
hematoma. Air embolism is a serious complication of a
the clavicle.
The Blood Vessels of the Head and Neck
95
angle of mandible
A
superior
external
vena
jugular
cava
vein
right
brachiocephalic
vein
midpoint
of clavicle
skin
external
jugular vein
B
platysma
right
catheter
subclavian
sternocleidomastoid
vein
muscle
external
jugular vein
investing
layer of
deep cervical
fascia
catheter
C
trapezius
CD Figure 6-3
Catheterization of the right external jugular vein. A.
Surface marking of
the vein. B. Site of catheterization. Note how the external jugular vein joins the subclavian
vein at a right angle. C. Cross section of the neck showing the relationships of the
external jugular vein as it crosses the posterior triangle of the neck.
Infraclavicular Approach
border of the origin of the clavicular head of the sternoclei-
domastoid muscle on the upper border of the clavicle (see
Since the subclavian vein lies close to the undersurface of
CD Fig. 6-5). The needle pierces the following structures:
the medial third of the clavicle (see CD Fig. 6-5), this is a
relatively safe site for catheterization. The vein is slightly
■ Skin
more medially placed on the left side than on the right side.
■ Superficial fascia
■ Pectoralis major muscle (clavicular head)
Anatomy of the Procedure
■ Clavipectoral fascia and subclavius muscle
■ Wall of subclavian vein
The needle should be inserted through the skin just below
the lower border of the clavicle at the junction of the medial
The needle is pointed upward and posteriorly toward
third and outer two thirds, coinciding with the posterior
the middle of the suprasternal notch.
96
Chapter 6
internal jugular vein
right
brachiocephalic
carotid sheath
vein
sternocleidomastoid muscle
common
skin
carotid artery
platysma
muscle
vagus
catheter
nerve
sternocleidomastoid
muscle
subclavian
deep
clavicle
vein
fascia
catheter
A
phrenic
scalenus
internal
nerve
anterior
jugular
muscle
vein
carotid sheath
sternal origin of
common
sternocleidomastoid muscle
carotid
sternal origin of
artery
sternocleidomastoid muscle
internal
subclavian
jugular
vagus
vein
vein
nerve
clavicle
internal
jugular
vein
clavicular origin of
sternocleidomastoid muscle
catheter
B
catheter
CD Figure 6-4
Catheterization of the right internal jugular vein. A. Posterior approach.
Note the position of the catheter relative to the sternocleidomastoid muscle and the com-
mon carotid artery. B. Anterior approach. Note that the catheter is inserted into the vein
close to the apex of the triangle formed by the sternal and clavicular heads of the stern-
ocleidomastoid muscle and the clavicle.
posterior to the scalenus anterior muscle and perforated
Anatomy of Problems
the subclavian artery.
■ Hitting the clavicle: The needle may be “walked” along
the lower surface of the clavicle until its posterior edge is
Anatomy of Complications
reached.
Refer to CD Fig. 6-5.
■ Hitting the first rib: The needle may hit the first rib if it
is pointed downward and not upward.
■ Pneumothorax: The needle may pierce the cervical
■
Hitting the subclavian artery: A pulsatile resistance and
dome of the pleura, permitting air to enter the
bright red blood flow indicates that the needle has passed
pleural cavity. This complication is more common in
The Blood Vessels of the Head and Neck
97
CD Figure 6-5
Subclavian vein catheterization. A. Infraclavicular approach. Note the
many important anatomic structures located in this region. B. Supraclavicular approach.
The catheter enters the subclavian vein close to its junction with the internal jugular vein
to form the brachiocephalic vein.
children, in whom the pleural reflection is higher than
beneath the skin to enter the subclavian vein at the point
in adults.
where the clavicle and the first rib cross.
■ Hemothorax: The catheter may pierce the posterior wall
The more oblique approach in children minimizes the
of the subclavian vein and the pleura.
possibility of entering the subclavian artery.
■ Subclavian artery puncture: The needle pierces the wall
Supraclavicular Approach
of the artery during its insertion.
■ Internal thoracic artery injury: Hemorrhage may occur
This approach (see CD Fig. 6-5) is preferred by many for the
into the superior mediastinum.
following anatomic reasons:
■ Diaphragmatic paralysis: This occurs when the needle
■ The site of penetration of the vein wall is larger, since it
damages the phrenic nerve.
lies at the junction of the internal jugular vein and the
subclavian vein, which makes the procedure easier.
The Procedure in Children
■ The needle is pointed downward and medially toward
The needle pierces the skin in the deltopectoral groove
the mediastinum, away from the pleura, avoiding the
about 2 cm from the clavicle. The catheter is tunneled
complication of pneumothorax.
98
Chapter 6
■ The catheter is inserted along a more direct course into
The needle is directed downward in the direction of the
the brachiocephalic vein and superior vena cava.
opposite nipple. The needle enters the junction of the in-
ternal jugular vein and the subclavian vein. It is important
Anatomy of the Procedure
that the operator understands that the pleura is not being
penetrated and that it is possible for the needle to lie in a
With the patient in the Trendelenburg position (patient
zone between the chest wall and the cervical dome of the
supine with head tilted downward) or simple supine posi-
parietal pleura but outside the pleural space (cavity).
tion and the head turned to the opposite side, the posterior
border of the clavicular origin of the sternocleidomastoid
Anatomy of Complications
muscle is palpated (see CD Fig. 6-5). The needle is inserted
through the skin at the site where the posterior border of the
The following complications may occur as the result of dam-
clavicular origin of sternocleidomastoid is attached to the
age to neighboring anatomic structures (see CD Fig. 6-5):
upper border of the clavicle. At this point, the needle lies
■ Paralysis of the diaphragm: This is caused by injury to the
lateral to the lateral border of scalenus anterior muscle
phrenic nerve as it descends posterior to the internal jugu-
and above the first rib. The needle pierces the following
lar vein on the surface of the scalenus anterior muscle.
structures (see CD Fig. 6-5):
■ Pneumothorax or hemothorax: This is caused by
■
Skin
damage to the pleura and/or internal thoracic artery by
■
Superficial fascia and platysma
the needle passing posteriorly and downward.
■ Investing layer of deep cervical fascia
■ Brachial plexus injury: This is caused by the needle
■ Wall of the subclavian vein
passing posteriorly into the roots or trunks of the plexus.
Clinical Problem Solving Questions
Read the following case histories/questions and give
against a window. The glass was shattered and a knife-
the best answer for each.
like piece became impaled in her neck. Within seconds
the wound spurted bright red blood and she ran scream-
A 40-year-old man mentioned to his physician during a
ing to her parents. In the emergency department of the
medical checkup that on four occasions during the past
local hospital it was immediately apparent that a large
5 months he had fainted at work. On each occasion the
artery in the front of the neck had been pierced by the
fainting attack occurred while he was sitting at his desk.
glass.
He said that the attack took place when he turned his
face to the left and bent down to open a bottom drawer.
2. The examining physician made the following observa-
He also complained that he first felt dizzy before he
tions and comments, all of which were correct except
fainted. The physician noted that the patient was rather
which?
formally dressed with a stiff collar and a regimental tie.
A. The entry wound was situated along the anterior
When the physician commented on his collar, the pa-
border of the sternocleidomastoid muscle at about
tient stated that he always wore this type of collar to
the level of the upper border of the thyroid carti-
work. On careful examination of the patient no abnor-
lage.
mal physical signs were found. In fact, the man looked
B. The artery involved could be either the terminal
very fit.
part of the common carotid artery or the beginning
of the external or internal carotid arteries.
1. Using your knowledge of anatomy and physiology,
C. The arteries were situated beneath the investing
make the most likely diagnosis.
layer of deep cervical fascia within the carotid fascial
A. Atrial fibrillation
sheath.
B. Cardiac ischemia
D. The internal jugular vein, which is also located
C. Carotid sinus syndrome
within the carotid sheath, is not involved because
D. Anemia
the blood was bright red in color and spurted from
E. Petit mal (a form of epilepsy)
the wound on removing the pressure gauze pad.
Two sisters were playing in their bedroom having a pil-
E. Branches of the trigeminal nerve lie in the sheath at
low fight, when one of them tripped and fell head first
this level and are likely to have been damaged.
The Blood Vessels of the Head and Neck
99
A 7-year-old boy was playing in his grandparents’ garden
cut to pieces and he fell to the ground in agony and
when he suddenly disappeared from view. His grandfa-
quickly lost consciousness. When the emergency
ther rushed over to see what had happened to his grand-
personnel arrived on the scene they found the man to
son when he heard muffled crying coming from a hole
be still alive but unconscious and lying in a pool of
in the ground. On peering into the hole, the child’s
blood. They had to stop the bleeding immediately.
head was just visible about five feet from the surface.
5.
Using your knowledge of anatomy, where would you ap-
The local rescue team determined that the child had
ply pressure at the root of the limb to stop the bleeding?
fallen down a disused well. Fortunately, the opening of
A. Just above the manubrium sterni in the midline to
the hole was large enough to allow the emergency
compress the right brachiocephalic artery
physician to be lowered to the child. Having reassured
B. Above the right sternoclavicular joint to compress
the child, it was necessary to check his vital signs. The
the right subclavian artery
only arteries that could be palpated were restricted to
C. Behind the medial part of the right clavicle, apply-
the head and neck.
ing pressure downward and backward on the right
3.
Name sites in the head and neck where the arterial
subclavian artery as it lies on the upper surface of the
pulse can be felt.
first rib
A. On the upper surface of the head in the midline
D. High up in the right armpit to compress the axillary
B. Just in front of the auricle of the ear, the lower
artery
margin of the mandible, or the anterior border of the
E. Behind the lateral part of the right clavicle, applying
sternocleidomastoid muscle at the level of the upper
pressure backward to compress the right subclavian
margin of the thyroid cartilage
artery as it becomes the axillary artery
C. Behind the ear over the mastoid process or at the
A 45-year-old man was rushed to hospital complaining
root of the nose
of cardiac pain referred to the root of his neck. After a
D. In the midline of the front of the neck in the
thorough workup, including a coronary arteriogram,
suprasternal notch or just below the mandible
which showed extensive blockage of the coronary arter-
E. At the apex of the posterior triangle of the neck or
ies, it was decided to do an immediate triple bypass op-
halfway down the posterior border of the sternoclei-
eration. At operation, because of the poor condition of
domastoid muscle
his superficial leg veins, an artery rather than a vein was
A 53-year-old man was admitted to the emergency room
selected to perform the bypass.
unconscious. Apparently he had attempted to cross the
6.
From the list of arteries given below, choose an artery
road on crutches when he was hit on the side of the
in the chest cavity that could be used to perform a
head by a car. On examination he was found to have a
coronary bypass.
large swelling over the left side of the head in the tem-
A. Right superior intercostal artery
poral region. The neurologic findings included a right-
B. Right and left anterior thoracic arteries
sided hemiplegia. A lateral radiograph of the skull
C. Phrenic arteries
showed a fracture line across the region of the lower
D. Musculophrenic artery
anterior end of the right parietal bone.
E. Superior epigastric artery
4.
Name the artery that was most likely to have been
A patient with a malignant melanoma in the left tem-
damaged in the accident.
poral region was told that because of the seriousness of
A. The left middle cerebral artery
the condition and the likelihood of metastases, an ex-
B. The right posterior cerebral artery
tensive operation was required including the removal of
C. The anterior division of the left middle meningeal
the deep cervical lymph nodes in the neck.
artery
D. The posterior division of the left middle meningeal
7.
Using your knowledge of anatomy, explain why it is
artery
necessary to remove the internal jugular vein in the
E. The left superficial temporal artery
neck as well as the deep cervical lymph nodes.
A. The deep cervical lymph nodes lie deep to the in-
A 42-year-old workman was cutting down a tree. During
ternal jugular vein, and it is necessary to remove the
the cleanup of the site, he was feeding the cut branches
vein to get at the lymph nodes.
into a large wood chipping machine and the sleeve of
B. Damage to the internal jugular vein would result in
his shirt on his right arm became caught in the ma-
serious air embolism.
chinery. Within seconds his arm was dragged into the
C. The numerous tributaries of the internal jugular
cutters. The man attempted to turn off the machine but
vein would complicate the procedure
could not reach the switch. His right upper limb was
100
Chapter 6
D. The deep cervical lymph nodes are embedded
C. The catheter tip may enter the mouth of the anterior
in the carotid sheath and the tunica adventitia of
division of the retromandibular vein.
the internal jugular vein.
D. The vein may be very small in professional singers.
E. Metastases of the melanoma commonly invade the
E. The vein is normally constricted as it passes behind
internal jugular vein.
the clavicle.
A 57-year-old woman was examined by her physician
10.
In deep penetrating injuries of the neck involving the
and found to have right-sided heart failure. As the pa-
common carotid artery, the status of the collateral cir-
tient lay propped up on pillows in bed, her physician no-
culation determines the feasibility of ligation versus a
ticed that the blood in a superficial vein on the side of
reconstructive procedure. Describe the collateral circu-
the neck (in the posterior triangle) could be easily seen.
lation of the common carotid artery. How may injury to
the artery produce loss of sight on the same side and
8.
From the list of veins in the neck given below, select the
contralateral hemiplegia? How may a carotid artery
most likely one that the physician could see.
injury produce airway obstruction?
A. Anterior jugular vein
B. Suprascapular vein
11.
Why is air embolism a complication of a lacerated wall
C. Superficial cervical vein
of the internal jugular vein?
D. Internal jugular vein
12.
In subclavian vein catheterization using the infraclavic-
E. External jugular vein
ular approach, the following problems may occur, even
9.
The jugular veins are commonly used to establish a
when great care is exercised: (a) The needle may hit the
central venous line. Why is it sometimes difficult to pass
clavicle; (b) the needle may hit the first rib; (c) the nee-
a catheter from the external jugular vein into the right
dle may hit the subclavian artery. How would you deal
atrium?
with these problems?
A. The catheter tip may catch in the valves.
B. The vein turns at a right angle before it drains into
the subclavian vein.
Answers and Explanations
1. C is the correct answer. The carotid sinus syndrome is
the body for taking the pulse, the following arteries are
a condition in which the carotid sinus reflex is hyper-
easily palpable: The pulsating facial artery can be felt as
sensitive. Pressure on one or both carotid sinuses can
it winds around the lower margin of the mandible in
cause excessive slowing of the heart, a fall in blood pres-
line with the anterior border of the masseter muscle
sure, and cerebral ischemia with fainting. In this
(see text Fig. 6-10). The superficial temporal artery may
patient the pressure of the stiff collar on the carotid
be palpated in front of the auricle of the ear as it ascends
sinuses, caused by bending over to gain access to the
over the zygomatic arch (see text Fig. 6-1). The classi-
bottom desk drawer, was sufficient to cause the episodes
cal site for feeling the pulse in the neck is along the an-
of fainting and loss of consciousness.
terior border of the sternocleidomastoid muscle at the
level of the upper border of the thyroid cartilage (see
2. E is the correct answer. The trigeminal nerve is not
text Fig. 6-3). Here, the common carotid artery divides
related to the carotid arteries in the neck. However, the
into the external carotid and internal carotid arteries,
hypoglossal nerve crosses the external carotid artery op-
and all three are quite superficial at this location.
posite the level of the tip of the greater cornu of the hyoid
bone.The glossopharyngeal nerve is related to the inter-
4. C is the correct answer. The anterior division of the
nal and external carotid arteries high up in the neck (see
middle meningeal artery is the most common artery to
text Fig. 6-4). The vagus nerve lies within the carotid
be damaged after a blow to the lateral side of the head.
sheath and accompanies the internal jugular vein and
The arterial or venous injury is especially liable to oc-
common and internal carotid arteries down the neck.
cur if the artery and vein enter a bony canal in the re-
The sympathetic trunk lies behind the common and
gion of the anterior inferior angle of the parietal bone
internal carotid arteries (see text Fig. 6-4).
(see CD Fig. 6-1).
3. B is the correct answer. In a difficult situation, when the
5. C is the correct answer. The arterial supply to the upper
patient’s head and neck are the only accessible parts of
limb can be cut off by applying deep pressure to the
The Blood Vessels of the Head and Neck
101
third part of the subclavian artery, as it lies on the upper
external carotid artery, however, gives off numerous im-
surface of the first rib. Here, the subclavian artery lies
portant branches in the neck that anastomose with the
behind the medial part of the clavicle and becomes
fellow branches from the opposite side.
continuous with the axillary artery (see text Fig. 6-10).
Since the internal carotid artery gives off the oph-
6.
B is the correct answer. The anterior thoracic artery,
thalmic artery and the middle cerebral artery, severe
which is a branch of the first part of the subclavian
damage or blockage of the common carotid artery
artery, can be used in coronary bypass operations.
could cause ipsilateral blindness and contralateral
hemiplegia.
7.
D is the correct answer. The deep cervical lymph nodes
are embedded in the carotid sheath and in the tunica
The common carotid artery is contained within the
adventitia of the internal jugular vein. The aim of the
carotid sheath beneath the investing and pretracheal
operation is to remove all the lymph nodes on the af-
layers of deep cervical fascia. Hemorrhage beneath the
fected side of the neck.
deep fascia could spread medially and compress the
larynx or the trachea, thus compromising the airway.
8.
E is the correct answer. The external jugular vein lies
superficially beneath the platysma muscle and can be
11.
Air embolism is a serious complication of a lacerated
easily seen in a good light (in an obese patient it may
wall of the internal jugular vein. Because the wall of
be difficult to see). The vein serves as a useful venous
this large vein contains very little smooth muscle, its in-
manometer. It runs from the angle of the jaw to the
jury is not followed by contraction and retraction (as
midpoint of the clavicle (see text Fig. 6-10). The level
occurs with arterial injuries). Moreover, the outer coat
of the blood in the vein normally reaches about one
of the vein is attached to the fascia of the carotid sheath,
third of the way up the neck when the patient is lying at
which hinders the collapse of the vein.
a horizontal angle of 30°. As the patient sits up, the
12.
When performing a subclavian vein catheterization
blood level falls until the vein is no longer visible
using the infraclavicular approach, the clavicle may
behind the clavicle.
be hit by the advancing needle. The needle may then
9.
A is the correct answer. The catheter tip may catch in
be “walked” along the lower surface of the clavicle un-
the valves. The external jugular vein has two sets of
til its posterior edge is reached and then inserted into
valves: One pair lies at its entrance into the subclavian
the subclavian vein. The needle may hit the first rib.
vein and the other pair lies abut 4 cm superior to the
This is due to the fact that the needle is pointing down-
clavicle. The valves are usually incompetent.
ward and not upward. The needle may hit the subcla-
vian artery. This is recognized by feeling the pulsatile
10.
The common carotid artery has no branches in the
resistance to the advancing needle and the presence of
neck except for its terminal branches, the internal and
bright red blood in the catheter. It indicates that the
external carotid arteries. The internal carotid artery has
needle has passed too deeply posterior to the scalenus
no branches in the neck, but at the base of the brain it
anterior muscle and perforated the wall of the subcla-
takes part in the arterial circle of Willis, where it anas-
vian artery (see CD Fig. 6-5). The needle should be
tomoses with the branches of the vertebral arteries and
partially withdrawn and the vein approached again.
the internal carotid artery of the opposite side. The
The Blood Vessels of the
Upper Extremity
7
Chapter Outline
Arteries of the Upper Extremity
104
Finding the Superficial Veins of the
Upper Extremity
106
The Importance of the Collateral Circulation when
Anatomy of Basilic and Cephalic
Ligating Arteries of the Upper Extremity
104
Vein Catheterization
106
Anatomy of Arterial Injuries in the Upper Extremity 104
Thrombosis of the Superficial Veins
106
Penetrating Arterial Injuries
104
Anatomy of Arteriovenous Shunts and Fistulas
Injuries to the Axillary Artery
105
Injuries to the Brachial Artery
105
in the Upper Limb for Hemodialysis
106
Allen Test
105
External Arteriovenous Shunt
106
Injuries to the Radial Artery
105
Internal Arteriovenous Fistula
108
Injuries to the Ulnar Artery
105
Deep Veins of the Upper Extremity
108
Intraarterial Injections by Drug Users
105
Axillary-Subclavian Vein Thrombosis
108
Arterial Venous Fistulas
105
Anatomy of Subclavian Vein Catheterization
108
Anatomy of the Procedure of Arterial Puncture
105
Venous Tone and Hypovolemic Shock
108
Brachial Artery
106
Radial Artery
106
Clinical Problem Solving Questions
108
Needle Approach
106
Cutdown Approach
106
Answers and Explanations
110
Superficial Veins of the Upper Extremity
106
may be sufficient to prevent the signs of ischemia; it is rare,
ARTERIES OF THE
however, for the physician to be able to palpate the distal
pulse at the initial examination.
UPPER EXTREMITY
Anatomy of Arterial Injuries in
The Importance of the Collateral
the Upper Extremity
Circulation when Ligating
Many of the injuries are directly related to the anatomy of
the upper limb. The extreme mobility of the limb at the
Arteries of the Upper Extremity
shoulder joint permits the forearm and hand to be raised as
The arteries of the upper limb may be damaged by pene-
a shield to ward off an attack. This position of the arm com-
trating wounds or may require ligation in amputation op-
monly results in laceration of the blood vessels.
erations. Because of adequate collateral circulation around
the shoulder, elbow, and wrist joints, ligation of the main
Penetrating Arterial Injuries
arteries of the upper limb is not followed by tissue necrosis
Arterial injuries of the upper limb are common and may oc-
or gangrene, provided, of course, that the arteries forming
cur from guns, knives, automobile accidents, and iatrogenic
the collateral circulation are not diseased and that the pa-
causes. Basically, three types of arterial injury are possible,
tient’s general circulation is satisfactory. Nevertheless, it
and the structure of the artery determines the signs and
may take days or weeks for the collateral vessels to open up
symptoms as well as the type of treatment instituted.
sufficiently to provide the distal part of the limb with the
same volume of blood as previously provided by the main
1. In a completely severed artery the circular smooth-mus-
artery.
cle fibers of the tunica media contract, immediately
At the time of the injury, where there is a complete in-
slowing the bleeding. In addition, the elastic fibers and
terruption of the main arterial supply, the collateral flow
longitudinal smooth-muscle fibers of the media contract,
The Blood Vessels of the Upper Extremity
105
causing the ends of the artery to retract. The contraction
the skin of the palms is at first white, and then normally the
and retraction of the arterial ends usually slow the blood
blood quickly flows into the arches through the ulnar arter-
flow to such an extent that bleeding ceases sponta-
ies, causing the palms to promptly turn pink. This estab-
neously, and a firm blood clot plugs both ends of the sev-
lishes that the ulnar arteries are patent. The patency of the
ered artery. The loss of distal pulses is immediate.
radial arteries can be established by repeating the test, only
with the ulnar arteries compressed where they lie lateral to
2. In a partially severed artery the vessel is unable to con-
the pisiform bone
tract and retract; in fact, any retraction that does occur
causes the arterial wound to gape, resulting in serious
Injuries to the Radial Artery
bleeding. Hemorrhage into the surrounding tissues
may produce an enlarging pulsatile hematoma that
These are common and occur in the lacerations of the front of
may slowly expand along fascial planes to reach the sur-
the forearm. The close relation of the artery to the radial nerve
face and cause a severe hemorrhage. Another possibil-
and the forearm tendons means that these structures are also
ity is that the damaged arterial wall gives way, leaving
commonly damaged (see text Figs. 7-12 and 7-13). Catheter
only the tunica adventitial intact. In these circum-
injuries are also common just proximal to the wrist joint.
stances, a pseudoaneurysm is formed.
Injuries to the Ulnar Artery
Since with partial arterial injury the arterial wall is still
intact, blood flow continues into the distal end, and a
These are relatively common and occur in lacerations in the
distal pulse is usually recognizable.
front of the wrist and flexor retinaculum. Here the artery is
superficial and easily cut in glass or knife wounds (see text
3. In an artery with intimal damage only secondary to ex-
Figs. 7-12 and 7-13). The closely related ulnar nerve is fre-
ternal blunt trauma, excessive stretching, or internal
quently involved also.
damage from a catheter, there is a reduction in blood
flow and an absence of external hemorrhage. Later, as a
Intraarterial Injections by Drug Users
result of progressive thrombosis or bleeding into the
wall at the site of injury, the blood flow becomes di-
In cases of intraarterial injection by drug abusers, the patient
minished and the distal pulses disappear.
presents with a swollen and extremely painful hand. The
drug is often injected into the radial or ulnar arteries. The
Injuries to the Axillary Artery
pharmacologic agent and its diluent causes damage at
the arteriole level as the result of blockage by crystal, chem-
These are often caused by penetrating wounds in the pec-
ical necrosis of the tunica intima, or vasospasm of the
toral region, fractures of the surgical neck of the humerus,
smooth muscle in the tunica media. Extensive tissue necro-
or excessive stretching following anterior dislocations of the
sis or gangrene may occur in the area of anatomic distribu-
shoulder joint (see text Fig. 7-7). Damage to the branches of
tion of the artery injected.
the brachial plexus may be an added complication.
Arterial Venous Fistulas
Injuries to the Brachial Artery
Arteriovenous fistulas are common complications of arterial
These may follow supracondylar fractures of the lower end of
injuries in the upper limbs. This results from the close rela-
the humerus (especially in children), a site where the artery
tionship that exists between the arteries and veins in the
is close to the shaft of the humerus as it lies on the brachialis
limbs. The axillary artery has the axillary vein on its medial
muscle (see text. Fig. 7-9). Damage to the adjacent median
side; the brachial, radial, and ulnar arteries have venae
nerve may also occur. Severe dislocations of the elbow joint
comitantes running alongside.
may damage the artery in the cubital fossa. Since the brachial
Arteriovenous fistulas occur when the penetrating arte-
artery is located superficially in the upper part of the arm, it
rial injury also perforates the accompanying vein. Bleeding
is a common site for arterial catheterization. Frequently the
from the artery follows the path of least resistance, and there-
tunical intima is damaged on the wall opposite the penetra-
fore an arteriovenous communication is established with re-
tion site, and arterial thrombosis may follow.
sulting venous hypertension, varicosities, and edema distal
to the communication site.
Allen Test
This test may be used to determine the patency of the ulnar
Anatomy of the Procedure of
and radial arteries. With the patient’s hands resting in his or
her lap, the radial arteries are compressed against the ante-
Arterial Puncture
rior surface of each radius. The patient then tightly clenches
his or her fists, which closes off the superficial and deep pal-
The brachial, radial, and ulnar arteries are commonly used
mar arterial arches. When he or she opens his or her hands,
for arterial puncture.
106
Chapter 7
Brachial Artery
obese persons the veins cannot always be seen. The surface
anatomy of the superficial veins is given on text page 209.
The brachial artery is usually cannulated as it descends into
the cubital fossa on the medial border of the biceps brachii
Anatomy of Basilic and Cephalic
muscle (see text Fig. 7-11). Unfortunately, the brachial
artery has been associated with a higher incidence of post-
Vein Catheterization
catheterization thrombosis than the radial artery. This is
probably because of the motility of the brachial artery asso-
The median basilic or basilic veins are the veins of choice
ciated with movements at the elbow joint.
for central venous catheterization, because from the cubital
fossa until the basilic vein reaches the axillary vein, the
Radial Artery
basilic vein increases in diameter and is in direct line with
With the radial artery it is first essential to determine the ad-
the axillary vein (see text Fig. 7-19). The valves in the axil-
equacy of the collateral circulation of the hand by perform-
lary vein may be troublesome, but abduction of the shoulder
ing the Allen test. This precaution is necessary in case
joint may permit the catheter to move past the obstruction.
thromboid occurs during or after cannulation. The forearm
The cephalic vein does not increase in size as it ascends
is then supinated and the wrist joint is extended to an ap-
the arm, and it frequently divides into small branches as it
proximately 50° angle (CD Fig. 7-1). The radial artery can
lies within the deltopectoral triangle. One or more of these
then easily be palpated as it lies anterior to the distal end of
branches may ascend over the clavicle and join the external
the radius.
jugular vein. In its usual method of termination, the
cephalic vein joins the axillary vein at a right angle. It may
Needle Approach
be difficult to maneuver the catheter around this angle.
The needle is passed through the arterial wall at an angle of
about 25° to the anterior surface of the wrist (see CD Fig. 7-
Thrombosis of the Superficial
1). The catheter can then be advanced into the arterial lu-
men and the needle withdrawn.
Veins
Prolonged intravenous infusion and, rarely, bacterial cel-
Cutdown Approach
lulitis of the superficial fascia can produce thrombosis of the
A transverse incision is made over the radial artery just above
superficial veins. In both cases injury to the tunical intima is
the proximal transverse skin crease at the wrist. The artery is
the initiating factor.
gently mobilized on the anterior surface of the radius and
the cannula is introduced.
Anatomy of Arteriovenous
Some physicians make a vertical incision for the radial
artery cutdown to lessen the risk of cutting a nerve and also
Shunts and Fistulas in the Upper
to avoid giving the patient a horizontal cut that could po-
tentially be misinterpreted (as a suicide attempt) on the an-
Limb for Hemodialysis
terior surface of the forearm.
Vascular access for hemodialysis can be provided by the
construction of an external arteriovenous shunt or an inter-
nal arteriovenous fistula. Most methods can be performed
SUPERFICIAL
under local anesthesia.
VEINS OF THE
External Arteriovenous Shunt
This is commonly used when a short period of treatment is
UPPER EXTREMITY
required. The shunt is constructed if possible in the non-
dominant limb. The radial artery or the ulnar artery, and the
cephalic vein or the basilic vein may be used. The proce-
Finding the Superficial Veins of
dure is as follows:
■ The branches of the lateral and medial cutaneous nerves
the Upper Extremity
of the forearm are blocked with a local anesthetic.
The cephalic, basilic, median cubital, median cephalic, me-
■ A midline incision is made on the anterior surface of the
dian basilic, and median veins of the forearm can all be used
distal part of the forearm.
for venipuncture and blood transfusion. These veins are fairly
■ The cephalic vein or the basilic vein is located in the su-
large and relatively constant in position. Unfortunately, in
perficial fascia as it winds around from the dorsum of the
The Blood Vessels of the Upper Extremity
107
deep palmar arch
palmar digital
arteries
thenar muscles
superficial palmer
arch
branch of radial artery
completing the superficial
palmar arch
deep palmar branch
abductor pollicis longus
pisiform bone
radial artery
flexor carpi ulnaris
flexor carpi radialis
ulnar nerve
ulnar artery
needle
radial artery
CD Figure 7-1
A. The positions of the radial and ulnar arteries in front of the wrist. Note
that the superficial palmar arch is formed mainly from the ulnar artery and the deep pal-
mar arch receives its major contribution from the radial artery. B. The wrist joint is ex-
tended during cannulation of the radial artery.
108
Chapter 7
hand to ascend the front of the forearm (see text Figs. 7-
from the dialyzer is inserted into the distended vein, and
18 and 7-19).
the cannula to the dialyzer is inserted into the fistula to
■
The deep fascia is incised and the artery is located. The
enter the radial artery.
radial artery can be palpated (see text Fig. 7-13) as it lies
A similar arrangement can be made using the ulnar
anterior to the distal third of the radius and between the
artery and the basilic vein.
tendons of flexor carpi radialis (medially) and the bra-
chioradialis (laterally). The ulnar artery can be felt just
lateral to the pisiform bone and can be traced proximally
into the forearm (see text Fig. 7-13).
DEEP VEINS OF
■ The appropriate artery and vein are then connected to
the dialyzer.
THE UPPER
In those patients in whom the distal vessels have been
previously used, the same vessels can be cannulated at a
EXTREMITY
more proximal site.
In children, if the distal arteries and veins are too small,
a shunt can be constructed between the brachial artery and
Axillary-Subclavian Vein
cephalic vein just proximal to the cubital fossa.
Thrombosis
Internal Arteriovenous Fistula
Spontaneous thrombosis of the axillary and or subclavian
This procedure is most often used when it is necessary to
veins occasionally occurs following excessive and
have a prolonged period of hemodialysis. The procedure is
unaccustomed use of the arm at the shoulder joint. The
as follows:
close relationship of these veins to the first rib and the
clavicle and the possibility of repeated minor trauma
■ The branches of the lateral and medial cutaneous nerves
from these structures is probably a factor in its devel-
of the forearm are blocked with a local anesthetic.
opment.
■ A midline incision is made on the anterior surface of the
Secondary thrombosis of axillary and/or subclavian
distal part of the forearm.
veins is a common complication of an indwelling venous
■ The cephalic vein is located in the superficial fascia.
catheter.
■ The deep fascia is incised and the radial artery is located
in front of the distal end of the radius, as described in the
previous section.
Anatomy of Subclavian Vein
■ A side-to-side anastomosis is performed between the
radial artery and the cephalic vein. Alternatively, an end-
Catheterization
to-end or end of vein-to-side of artery anastomosis can
be constructed. The peripheral circulation is maintained
Venous Tone and Hypovolemic Shock
by the extensive anastomoses from the ulnar artery
around the wrist and through the palmar arches.
In extreme hypovolemic shock, excessive venous tone may
■
The vein quickly becomes arterialized and distended and
inhibit venous blood flow and thus delay the introduction of
can be easily punctured with a cannula. The cannula
intravenous blood into the vascular system.
Clinical Problem Solving Questions
Read the following case histories/questions and give
from a superficial laceration in front of her left wrist.
the best answer for each.
She had sensory loss over the palmar aspect of the me-
dial one and a half fingers but normal sensation of the
A young secretary, running from her office, had a glass
back of these fingers over the middle and proximal pha-
door swing back in her face. To protect herself, she held
langes. She had difficulty in grasping a piece of paper
out her left hand, which smashed through the glass. On
between her left index and middle fingers. All her long
admission to the hospital, she was bleeding profusely
flexor tendons were intact.
The Blood Vessels of the Upper Extremity
109
1.
The following statements concerning this patient are
the reduction of the fracture, a suitable splint was ap-
correct except which?
plied and the child was sent home. A few hours later,
A. The radial artery was cut in front of the flexor
the child complained of pain in the forearm, which
retinaculum, and this accounted for the profuse
persisted. Four hours later, the parents decided to re-
bleeding.
turn to the hospital, since the child’s left hand looked
B. The loss of skin sensation on the palmar aspect of
dusky white and the pain in the forearm was still pre-
the medial one and a half fingers was caused by the
sent. On examination, there was found to be a com-
severance of the ulnar nerve as it crossed in front of
plete loss of skin sensation of the hand. After removal
the flexor retinaculum.
of the splint, the pulse of the radial and ulnar arteries
C. The normal sensation on the back of the medial one
could not be felt. Every possible effort was made to re-
and a half fingers over the proximal phalanges was
store the circulation of the forearm, without avail.
caused by the fact that the posterior cutaneous
What has happened to this child’s circulation in the
branch of the ulnar nerve arises about 2.5 in. (6.25
forearm? What deformity would you expect this child
cm) proximal to the flexor retinaculum and was
to have 1 year later?
spared.
5.
Why is the radial artery chosen in preference to the ul-
D. The inability to hold the piece of paper was caused
nar artery or brachial artery for direct blood pressure
by the paralysis of the second palmar interosseous
monitoring? Why are the upper limb arteries used in
muscle, which is supplied by the deep branch of the
preference to the dorsalis pedis artery of the foot? What
ulnar nerve.
are the important anatomic relations of the radial artery
E. There was no sensory loss on the palm of the hand
at the site of cannulation? Why is it necessary to extend
because the palmar cutaneous branch of the ulnar
the wrist joint when the canula is introduced?
nerve was not cut.
6.
During an emergency procedure it is sometimes neces-
2.
A middle-aged man with a history of chronic duodenal
sary to monitor central venous pressure via peripheral
ulcer was seen in the emergency department in a state
access. Why is the basilic vein more often used to es-
of severe shock. He was pale, restless, and sweating,
tablish a central venous pressure line than the cephalic
and his blood pressure was 80/60 mm Hg. The resi-
vein?
dent made a diagnosis of internal hemorrhage, proba-
bly due to the erosion of the gastroduodenal artery or
7.
A 29-year-old woman was seen in the emergency de-
one of its branches, and decided to set up a blood
partment complaining of severe pain and discoloration
transfusion immediately. Based on your knowledge of
of the fourth and fifth fingers of both hands. She said
anatomy, into which superficial vein of the upper limb
that she had had similar symptoms before and that they
would you perform the transfusion: in the elbow
always occurred in very cold weather. Initially, her fin-
region or in the forearm? If the veins were too
gers turned white on exposure to cold and then became
collapsed to be identified, where, in an emergency,
deep blue in color. The color change was confined to
could you cut down on a superficial vein in the upper
the distal half of each finger and was accompanied by
limb?
an aching pain. Placing her hands in hot water was the
only treatment that relieved the pain. As the pain disap-
3.
Palpation of the radial artery at the wrist can provide the
peared, she said, her fingers became red and swollen.
experienced medical professional with considerable in-
Using your knowledge of anatomy, make the diagnosis.
sight into the state of the patient’s circulatory system. The
8.
A 23-year-old medical student decided to assist his fa-
degree of hardness of the arterial wall can be appreciated
ther in building a garden shed. Unfortunately, much of
by the examining finger; the pulse rate and quality of the
the wood had to be cut to length by using a hand saw.
rhythm can be determined; and the amount of pressure
He noticed on the third day that his right arm felt heavy
required to occlude the vessel can be used to assess the
and that his right hand was swollen. At the emergency
blood pressure. What are the relations of the radial artery
department, a diagnosis of right subclavian vein throm-
at this site where the pulse is taken?
bosis was made. Can you explain the possible anatomic
4.
An 8-year-old boy fell off a swing and sustained a
reasons why thrombosis occurred in this vein in a
supracondylar fracture of his left humerus. Following
healthy individual?
110
Chapter 7
Answers and Explanations
1.
A is the correct answer. The radial artery does not enter
transverse crease of the wrist. Here the artery lies ante-
the palm by passing in front of the flexor retinaculum;
rior to the distal third of the shaft of the radius, medial
it does so by passing forward between the two heads of
to the tendon of the brachioradialis and lateral to the
the first dorsal interosseous muscles between the first
tendon of flexor carpi radialis. It is covered anteriorly
and second metacarpal bones (see text Fig. 7-14). It was
by skin and fascia. The forearm is supinated, and the
the ulnar artery that was cut with the ulnar nerve in
wrist is extended to an approximately 50° angle (see
front of the flexor retinaculum.
CD Fig. 7-1). Extension stretches and stabilizes the
artery during the process of introducing the needle
2.
The cephalic, basilic, and median cubital veins, and
and the catheter.
their tributaries, are located in front of the cubital fossa
and may be used for transfusion (see text Fig. 7-19). In
6.
The basilic vein is used more often than the cephalic
the forearm, the cephalic and basilic veins can be seen
vein for the following reasons: (a) The basilic vein in-
as they wind around the lateral and medial borders of
creases progressively in diameter from the cubital fossa
the forearm, respectively. The cephalic vein lies in a
to the axillary and subclavian veins, whereas the diame-
constant position behind the styloid process of the ra-
ter of the cephalic vein increases only slightly as it as-
dius (see text Fig. 7-18), and it is here that it may be ex-
cends the upper extremity; (b) the basilic vein is in line
posed through a small skin incision.
with the axillary vein (see text Figs. 7-19, 7-22, and 7-23),
whereas the cephalic vein opens into the axillary vein at
3.
The radial artery lies in front of the distal third of the
a right angle; and (c) the basilic vein is directly continu-
shaft of the radius; it is directly in contact with the front
ous with the end of the axillary vein, whereas the
of the bone (see text Fig. 7-11. On its lateral side lies the
cephalic vein may bifurcate into several small veins near
tendon of the brachioradialis, and on its medial side is
its termination or may join the external jugular vein.
the tendon of the flexor carpi radialis muscle. The
artery is covered anteriorly by skin and fascia.
7.
This patient had Raynaud’s disease. The initial pallor of
4.
At the time of sustaining the supracondylar fracture of
the fingers is due to spasm of the digital arterioles. The
the humerus or the application of the splint, the
cyanosis that follows is due to local capillary dilatation
brachial artery went into spasm in the distal third of the
caused by an accumulation of metabolites. Since there
upper arm. This effectively shut off the blood flow
is no blood flow through the capillaries, blue deoxy-
through the radial and ulnar arteries, including the col-
genated hemoglobin accumulates within them. It is
lateral circulation around the elbow joint (see text Fig.
during this period of prolonged cyanosis that the patient
7-8). During the following hours, when the child was
experiences severe aching pain. On exposing the fin-
complaining of severe pain, avascular necrosis of the tis-
gers to warmth, the vasospasm disappears, and oxy-
sues of the forearm was taking place. Later this was fol-
genated blood flows back into the very dilated capillar-
lowed by Volkmann’s contracture.
ies. Reactive hyperemia is responsible for the swelling
of the affected fingers.
5.
The radial artery has a lower incidence of arterial
thrombosis than the brachial artery, possibly because
8.
The subclavian vein is closely related to the upper sur-
the tunica intima of the brachial artery is more likely
face of the first rib and to the posterior surface of the
to be damaged by the point of the catheter, since the
medial third of the clavicle (see text Fig. 7-3). Repeated
brachial artery is more difficult to immobilize because
minor trauma to the vein wall by these bones during the
of the movements at the elbow joint. The dorsalis
movements of the right shoulder while sawing resulted
pedis artery can be easily cannulated. It has a higher
in damage to the tunica intima, followed by thrombo-
incidence of thrombosis, however, and sometimes the
sis. This problem is particularly likely to occur in an in-
circulation of the foot is compromised by the inade-
dividual who is not used to this type of excessive move-
quate collateral circulation. The radial artery is
ment of the shoulder. Usually there is some preexisting
usually cannulated 2 to 3 cm proximal to the distal
compression.
The Blood Vessels of the Upper Extremity
111
The Blood Vessels of
the Abdomen, Pelvis,
and Perineum
8
Chapter Outline
The Abdominal Aorta
112
The Portal Vein
115
Traumatic Injury to the Abdominal Aorta
112
Portal-Systemic Anastomoses
115
Aortic Aneurysm
112
Portal Hypertension
117
Gradual Occlusion of the Abdominal Aorta
113
Blood Flow in the Portal Vein and Malignant
Embolic Blockage of the Abdominal Aorta
113
Disease
117
Mesenteric Artery Occlusion
113
Penetrating Injuries to the Portal Vein
117
The Inferior Vena Cava
113
Clinical Problem Solving Questions
117
Caval-Caval Anastomosis
113
Compression of the Inferior Vena Cava
114
Answers and Explanations
119
Trauma to the Inferior Vena Cava
115
however, is relatively mobile and continues to move for-
ward after body impact, being finally restrained by the at-
THE ABDOMINAL
tachment of the renal artery to the aorta. Excessive stretch-
ing of the renal artery may cause intimal damage with clot
AORTA
formation. The renal vessels may be avulsed from the
hilum of the kidney, or the renal artery may be torn free
from the aorta. The hemorrhage may be contained in the
Traumatic Injury to the Abdominal
retroperitoneal space, and hypovolemic shock may not im-
mediately occur.
Aorta
Penetrating injuries to the abdominal aorta are
Because of the deep position of the aorta on the posterior
common and are usually associated with multiple intraab-
abdominal wall behind the peritoneum (see text Figs. 8-1
dominal injuries. The peritoneum has been violated, and
and 8-2), blunt injuries to the aorta are relatively rare.
hemorrhage occurs directly into the peritoneal cavity. The
In children the elasticity of the aortic wall and the usual
signs of a distended abdomen associated with those of hypo-
absence of atherosclerosis make the condition even
volemic shock make the diagnosis relatively simple. How-
more rare.
ever, when the arterial leak is small, peritoneal lavage may
In blunt trauma from an automobile accident, the ab-
be necessary to confirm the diagnosis. Penetrating injuries
dominal aorta can be injured by the crossing band of a seat
through the back or flank (especially when directed from
belt. The tunical intima is commonly damaged just distal to
the left) may cause a retroperitoneal injury to the aorta; the
the origin of the inferior mesenteric artery at the level of the
blood may be contained within the retroperitoneal space
third lumbar vertebra. The diagnosis is difficult since occlu-
and delay the onset of hypovolemic shock.
sion due to thrombosis may occur at the time of the trauma
or be delayed for several months. In the presence of com-
Aortic Aneurysms
plete occlusion, the femoral pulses are absent, and motor
and sensory deficits may be present in the lower limbs due
Localized or diffuse dilatations of the abdominal part of the
to ischemia of the peripheral nerves.
aorta (aneurysms) usually occur below the origin of the re-
Deceleration injuries to the renal vessels may occur as
nal arteries (CD Fig. 8-1). Most result from atherosclerosis,
the body stops its forward motion. The abdominal aorta,
which causes weakening of the arterial wall, and occur most
like the descending thoracic aorta, is tightly attached to the
commonly in elderly men. Large aneurysms should be sur-
vertebral column by connective tissue. The kidney,
gically excised and replaced with a prosthetic graft.
The Blood Vessels of the Abdomen, Pelvis, and Perineum
113
common
iliac
artery
CD Figure 8-1
Aneurysms of the abdominal
aorta. A. Above the origin of the renal arteries.
B. Below the level of the renal arteries. The latter
aneurysms, which are the most common, may
extend inferiorly to involve the common iliac
arteries.
clusive disease of the superior mesenteric artery is much
Gradual Occlusion of the
more common than that of the inferior mesenteric artery,
which may be explained by the angle of takeoff of the su-
Abdominal Aorta
perior artery from the aorta. In cases of embolus of the su-
perior mesenteric artery, the embolus usually lodges in the
Gradual occlusion of the aorta may occur due to athero-
region of the middle colic artery so that the jejunum may
sclerosis. Intermittent claudication in both legs may be pre-
be spared.
sent due to insufficient arterial blood reaching the muscles
of the lower limbs. If the progress of the atherosclerosis is
slow, an adequate collateral circulation may become estab-
lished (CD Fig. 8-2).
THE INFERIOR
Embolic Blockage of the Abdominal
VENA CAVA
Aorta
Caval-Caval Anastomosis
The bifurcation of the abdominal aorta where the lumen
suddenly narrows may be a lodging site for an embolus dis-
A caval-caval shunt is the opening up of an alternative ve-
charged from the heart. Severe ischemia of the lower limbs
nous pathway should the superior or inferior vena cava
results.
become blocked by disease. The anastomoses of the
vena cava are as follows (CD Fig. 8-3): The lumbar veins,
which are tributaries of the inferior vena cava, anastomose
Mesenteric Artery Occlusion
behind the diaphragm with the azygos and hemiazygos
Occlusion of the superior or inferior mesenteric arteries
veins, which are tributaries of the superior vena cava. The
with intestinal ischemia is discussed in CD Chapter 19.
lumbar veins also anastomose with the superficial veins
The occlusive process commonly occurs at the origin of
of the trunk, which eventually drain into the superior
the artery or in the proximal 1 to 2 cm of the artery and
vena cava via the lateral thoracic veins, tributaries of the
may be caused by an embolus, a thrombus, or trauma. Oc-
axillary veins.
114
Chapter 8
right subclavian artery
left subclavian artery
posterior intercostal
internal thoracic
arteries
artery
thoracic part of aorta
musculophrenic artery
diaphragm
superior epigastric
artery
phrenic artery
left renal artery
middle colic artery
superior mesenteric
artery
abdominal aorta
right colic artery
lumbar arteries
marginal artery
ileocolic artery
left colic artery
inferior epigastric artery
inferior mesenteric
artery
fourth lumbar
artery
sigmoid arteries
deep circumflex
superior rectal
iliac artery
artery
middle rectal artery
internal iliac artery
median
sacral
inferior rectal artery
artery
CD Figure 8-2
The possible collateral circulations of the abdominal aorta. Note the great
dilatation of the mesenteric arteries and their branches, which occurs if the aorta is slowly
blocked just below the level of the renal arteries (white bar).
moses of the tributaries (see CD Fig. 8-3). This alternative
Compression of the Inferior
pathway for the blood to return to the right atrium of the
heart is commonly referred to as the caval-caval shunt. The
Vena Cava
same pathway comes into effect in patients with a superior
The inferior vena cava is commonly compressed by the en-
mediastinal tumor compressing the superior vena cava.
larged uterus during the later stages of pregnancy. This produces
Clinically, the enlarged subcutaneous anastomosis between
edema of the ankles and feet and temporary varicose veins.
the lateral thoracic vein, a tributary of the axillary vein, and
Malignant retroperitoneal tumors can cause severe
the superficial epigastric vein, a tributary of the femoral
compression and eventual blockage of the inferior vena
vein, may be seen on the thoracoabdominal wall (see CD
cava. This results in the dilatation of the extensive anasto-
Fig. 8-3).
The Blood Vessels of the Abdomen, Pelvis, and Perineum
115
brachiocephalic
vein
superior vena cava
subclavian vein
first rib
axillary vein
hemiazygos veins
azygos vein
internal thoracic vein
lateral thoracic vein
diaphragm
inferior vena cava
ascending lumbar
vein
lumbar veins
inferior mesenteric
inferior epigastric vein
vein ascending to
portal vein
CD Figure 8-3
The possible collat-
eral circulations of the superior and
superficial epigastric
interior venae cavae. Note the alter-
vein
superior rectal vein
native pathways that exist for blood
internal iliac vein
to return to the right atrium of the
external iliac vein
heart if the superior vena cava be-
comes blocked below the entrance
inguinal ligament
of the azygos vein (upper black bar).
middle rectal vein
Similar pathways exist if the inferior
vena cava becomes blocked below
femoral vein
the renal veins (lower black bar).
Note also the connections that exist
between the portal circulation and
great saphenous
inferior rectal vein
vein
the systemic veins in the anal canal.
Trauma to the Inferior Vena Cava
THE PORTAL VEIN
Injuries to the inferior vena cava are commonly lethal, de-
spite the fact that the contained blood is under low pressure.
The anatomic inaccessibility of the vessel behind the liver,
Portal-Systemic Anastomoses
duodenum, and mesentery of the small intestine and the
blocking presence of the right costal margin make a surgical
Under normal conditions, the portal venous blood traverses
approach difficult. Moreover, the thin wall of the vena cava
the liver and drains into the inferior vena cava of the sys-
makes it prone to extensive tears.
temic venous circulation by way of the hepatic veins. This is
Because of the multiple anastomoses of the tributaries
the direct route (see text Fig. 8-19). However, other, smaller
of the inferior vena cava (see CD Fig. 8-3), it is possible in
communications exist between the portal and systemic sys-
an emergency to ligate the vessel. Most patients have venous
tems, and they become important when the direct route be-
congestion of the lower limbs.
comes blocked (CD Fig. 8-4).
116
Chapter 8
inferior vena cava
tributaries of
phrenic
1
azygos veins
veins
esophageal tributaries of
left gastric vein
5
liver
veins on posterior
abdominal wall
paraumbilical veins
4
3
umbilicus
colic veins
superficial veins
of anterior abdominal
wall
superior rectal vein
2
middle and inferior rectal
veins
CD Figure 8-4
Important portal-systemic anastomoses.
These communications are as follows:
■ At the lower third of the esophagus, the esophageal
■ The paraumbilical veins connect the left branch of the
branches of the left gastric vein (portal tributary) anasto-
portal vein with the superficial veins of the anterior
mose with the esophageal veins draining the middle third
abdominal wall (systemic tributaries). The paraumbilical
of the esophagus into the azygos veins (systemic tributary).
veins travel in the falciform ligament and accompany the
■ Halfway down the anal canal, the superior rectal veins
ligamentum teres.
(portal tributary) draining the upper half of the anal canal
■ The veins of the ascending colon, descending colon,
anastomose with the middle and inferior rectal veins (sys-
duodenum, pancreas, and liver (portal tributary) anas-
temic tributaries), which are tributaries of the internal il-
tomose with the renal, lumbar, and phrenic veins
iac and internal pudendal veins, respectively.
(systemic tributaries).
The Blood Vessels of the Abdomen, Pelvis, and Perineum
117
the liver via the hepatic artery. The wide angle of union of
Portal Hypertension
the splenic vein with the superior mesenteric vein to form
the portal vein leads to streaming of the blood flow in the
Portal hypertension is a common clinical condition; thus,
portal vein. The right lobe of the liver receives blood mainly
the list of portal-systemic anastomoses should be remem-
from the intestine, whereas the left lobe plus the quadrate
bered. Enlargement of the portal-systemic connections is
and caudate lobes receive blood from the stomach and the
frequently accompanied by congestive enlargement of the
spleen. This distribution of blood may explain the distribu-
spleen. Portacaval shunts for the treatment of portal
tion of secondary malignant deposits in the liver.
hypertension may involve the anastomosis of the portal vein,
because it lies within the lesser omentum, to the anterior
wall of the inferior vena cava behind the entrance into the
Penetrating Injuries to the
lesser sac. The splenic vein may be anastomosed to the left
renal vein after removing the spleen.
Portal Vein
Penetrating injuries to the portal vein are life threatening and
Blood Flow in the Portal Vein
are usually associated with multiple abdominal injuries. A
deep penetrating abdominal wound on the transpyloric
and Malignant Disease
plane, about two fingerbreadths to the right of the midline,
The portal vein conveys about 70% of the blood to the liver.
could easily penetrate the liver and perforate the first part
The remaining 30% is oxygenated blood, which passes to
of the duodenum, the portal vein, and the inferior vena cava.
Clinical Problem Solving Questions
Read the following case histories/questions and give
Into which hollow viscera or blood vessels may an aortic
the best answer for each.
aneurysm rarely rupture into?
1.
A 59-year-old man was involved in a head-on automobile
3.
Explain in anatomic terms why penetrating injuries to
accident. When seen in the emergency department, he
the inferior vena cava are commonly fatal. Explain how
was in hypovolemic shock and showed signs of extensive
it is possible to ligate the inferior vena cava below the
bruising on the lower part of the anterior abdominal wall.
level of the renal veins without adverse effects.
He was wearing a seat belt at the time of the accident. On
A 63-year-old man with a long history of a duodenal ul-
examination, his abdomen was distended and tense; he
cer was seen in the emergency department after vomit-
had hypotension and tachycardia. A diagnosis of ruptured
ing blood-stained fluid and exhibiting all the signs and
abdominal aorta was made during an emergency laparo-
symptoms of severe hypovolemic shock.
tomy. In cases of blunt traumatic injury to the abdominal
aorta, do all patients become hypotensive immediately?
4.
The following statements concerning duodenal ulcers
Explain the possible role that the kidneys may play in
could apply to the patient’s condition except which?
causing damage to the aorta in deceleration injuries.
A. Hemorrhage from a duodenal ulcer often reveals it-
self by the passage of black stools on defecation.
2.
A 74-year-old man was seen in the emergency depart-
B. The pyloric sphincter prevents most of the blood from
ment complaining of the sudden onset of severe lumbar
the duodenal lumen from passing up into the stomach.
back pain. Three years previously he had had a myocar-
C. The gastroduodenal artery lies behind the first part of
dial infarction. On questioning, the patient admitted
the duodenum and was probably eroded by the ulcer.
that he often experienced mild back and hip pains on
D. The gastroduodenal artery is a small branch of the
getting up in the morning, but never had he experienced
hepatic artery.
such a severe back pain. On examination, a somewhat
E. The duodenal ulcer was most likely to be situated on
tender pulsatile swelling could be felt in the abdomen at
the posterior wall of the first part of the duodenum.
the level of the umbilicus. Both femoral pulses were pre-
sent. A diagnosis of abdominal aortic aneurysm was
A 58-year-old man was in a restaurant when he suddenly
made. What is the surface marking of the abdominal
started to vomit blood. He was taken unconscious to the
aorta? Explain why the back pain had started so suddenly
emergency department of a local hospital. On examina-
and its significance. When an abdominal aneurysm rup-
tion, he had all the signs of severe hypovolemic shock.
tures, does an immediate fatal outcome always occur?
On palpation of the anterior abdominal wall, the right
118
Chapter 8
lobe of the liver was felt three fingerbreadths below the
7.
The symptoms and signs displayed by this patient
costal margin. Several enlarged superficial veins could
can be explained by the following statements except
be seen around the umbilicus. His wife said that he had
which?
vomited blood 3 months previously and had nearly died.
A. The enlarged uterus is an abdominal organ and
She admitted that he was a chronic alcoholic. The
often compresses the inferior vena cava.
diagnosis was cirrhosis of the liver secondary to chronic
B. Venous back pressure causes the tissue fluid to ac-
alcoholism.
cumulate in the subcutaneous tissues of the feet and
ankles.
5.
The symptoms and signs displayed by this patient can
C. Venous back pressure impairs the venous return in
be explained by the following statements except which?
the superficial veins in both the legs, leading to vari-
A. The normal flow of portal blood through the liver is
cose veins.
impaired by cirrhosis of the liver.
D. High levels of progesterone in the blood during preg-
B. The portal-systemic anastomoses become enlarged
nancy cause the smooth muscle in the wall of the
in this condition.
veins to relax, thus permitting the veins to dilate.
C. At the lower end of the esophagus, a branch from the
E. The pregnant uterus presses on the sympathetic
right gastric vein anastomoses with an esophageal
trunks, causing vasodilatation of the blood vessels of
tributary of the azygos vein.
the legs.
D. Rupture of a varicosed esophageal vein could pro-
duce a severe hemorrhage so that the patient would
8.
After complete occlusion of the origin of the inferior
vomit up blood.
mesenteric artery with a blood clot, the blood supply of
E. With portal hypertension the paraumbilical veins
the left portion of the colon is maintained by the
linking the superficial veins of the skin (systemic
following arteries except which?
veins) to the portal vein become congested and
A. The marginal artery
visible.
B. The middle colic artery
C. The left lumbar arteries
A 56-year-old man visited his physician complaining
D. Anastomoses between the superior, middle, and
that he experiences severe pain in both legs when taking
inferior hemorrhoidal arteries
long walks. He noticed recently that the cramp-like pain
E. Sigmoid arteries
occurs after walking only a hundred yards. On ques-
tioning, he said that the pain quickly disappears on rest
9.
In patients with an obstruction of the superior vena cava,
only to return after he walks the same distance. When
blood may return to the right atrium through the
the physician asked about his sex life the patient admit-
following anastomotic channels except which?
ted that he was experiencing difficulty with erection.
A. The lateral thoracic, lumbar, and superficial epigas-
tric veins
6.
The symptoms and signs displayed by this patient can
B. The superior and inferior epigastric veins
be explained by the following statements except which?
C. The lateral thoracic, paraumbilical, and portal veins
A. Arteriography of the abdominal aorta revealed
D. The posterior intercostal and lumbar veins
blockage in the region of the bifurcation.
E. The lateral thoracic veins alone
B. Only the right common iliac artery was involved by
disease.
10.
If the common hepatic artery is unavoidably ligated
C. The gradual blockage of the aorta was caused by
during surgery, the arterial supply to the liver is main-
advanced arteriosclerosis.
tained by the following anastomotic connections except
D. An insufficient amount of blood was reaching both
which?
legs, causing pain (claudication) on walking.
A. The superior pancreaticoduodenal artery anasto-
E. The lack of blood entering both internal iliac
mosing with the inferior pancreaticoduodenal artery
arteries was responsible for the difficulty with
B. The right gastric artery anastomosing with the left
erection.
gastric artery
C. The gastroduodenal artery anastomosing with the
A 23-year-old woman, who was 8 months pregnant, told
splenic artery
her obstetrician that she had recently noticed that her
D. The esophageal arteries anastomosing with the infe-
feet and ankles were swollen at the end of the day. She
rior phrenic arteries
said that the swelling was worse if she had been stand-
E. The right gastroepiploic artery anastomosing with
ing for long periods. She also noticed that the veins
the left gastroepiploic artery
around her ankles were becoming prominent.
The Blood Vessels of the Abdomen, Pelvis, and Perineum
119
Answers and Explanations
1.
Frequently, patients with blunt rupture to the abdomi-
site of the injury is inaccessible behind the liver, duo-
nal aorta may not immediately show signs of hypov-
denum, and the mesentery of the small intestine; (b)
olemic shock because the aorta is situated behind the
the presence of the right costal margin makes surgical
peritoneum in the retroperitoneal space and the blood
access difficult; (c) the thin walls of the vena cava are
may not escape immediately into the peritoneal cavity
likely to tear extensively and make repair difficult; and
(see text Fig. 5-62).
(d) the almost certain possibility that the liver is also
damaged.
On impact, the patient may be held stationary by the
seat belt, but the kidneys may continue forward until re-
The extensive anastomosis of the lumbar veins with
strained by the vascular pedicles. Avulsion of the renal
other retroperitoneal veins ensures that the blood is
artery from the side of the aorta may take place under
able to bypass the obstruction should the inferior vena
these circumstances.
cava be ligated below the level of the renal veins (see
CD Fig. 8-3).
2.
The abdominal aorta is a midline structure that enters
the abdomen at the level of the twelfth thoracic verte-
4.
D is the correct answer. The gastroduodenal artery is a
bra, and its entrance may be projected onto the anterior
large branch of the hepatic artery.
abdominal wall just above the transpyloric plane (see
5.
C is the correct answer. At the lower end of the
text Fig. 8-3). The vessel extends downward to its bifur-
esophagus, a branch from the left gastric vein
cation into the common iliac arteries at the level of the
anastomoses with an esophageal tributary of the azygos
summit of the iliac crests.
vein.
The sudden onset of severe back pain can be explained
6.
B is the correct answer. The blockage of the aorta in the
by the aneurysm suddenly expanding or rupturing and
region of the bifurcation had effectively blocked the en-
pressing on the vertebral column, which lies immedi-
trances into both common iliac arteries.
ately posterior to the aorta.
7.
E is the correct answer. The sympathetic trunks are not
Death does not always immediately follow an abdomi-
pressed on by the pregnant uterus.
nal aneurysm rupture. This can be explained by the fact
that the hemorrhage may be initially confined to the
8.
C is the correct answer. The left lumbar arteries do not
retroperitoneal space, and a tamponade effect may tem-
significantly contribute to the left portion of the colon.
porarily prevent further bleeding.
The middle colic artery from the superior mesenteric
artery, the sigmoid arteries, and the marginal artery, as
The abdominal aorta is crossed by the third part of the
well as the hemorrhoidal arteries, will maintain the
duodenum, and cases have been reported of an
blood supply to the left portion of the colon.
aneurysm rupturing into the duodenal lumen. The in-
ferior vena cava lies along the right side of the aorta, and
9.
E is the correct answer. The lateral thoracic and the su-
an aneurysm has been known to rupture into it, pro-
perior epigastric veins are directly or indirectly con-
ducing a massive arteriovenous fistula.
nected with the superior vena cava only.
3.
Penetrating injuries of the upper part of the
10.
C is the correct answer. The gastroduodenal artery does
inferior vena cava are commonly fatal because (a) the
not directly anastomose with the splenic artery.
The Blood Vessels of the
Lower Extremity
9
Chapter Outline
The Arteries
122
Great Saphenous Vein Cutdown
125
Anatomy of Ankle Vein Cutdown
126
Collateral Circulation
122
Anatomy of Groin Vein Cutdown
126
Femoral Artery Catheterization
122
The Great Saphenous Vein in Coronary Bypass
Anatomy of Technique
123
Surgery
126
Anatomy of Complications
123
Intraosseous Infusion in the Infant
126
Traumatic Injury to Arteries of the Lower Limb
124
Varicose Veins
126
Anatomy of Complications of Arterial Injury
124
Varicose Leg Ulcers
126
Compartmental Syndromes
124
Traumatic Bleeding from a Varicosed Vein
127
Occlusion of the Popliteal, Anterior, and Posterior
Superficial Thrombophlebitis
127
Tibial Arteries
124
Deep Thrombophlebitis
127
Intermittent Claudication and Arterial Occlusive
Deep Vein Thrombosis and Long-Distance Air
Disease of the Lower Extremity
124
Travel
127
Femoropopliteal and Femorotibial Bypass for
Femoral Vein Catheterization
127
Lower Extremity Vascular Insufficiency
124
Anatomy of the Procedure
127
Lumbar Sympathectomy and Occlusive Arterial
Doppler Ultrasound Examination of Venous Flow
Disease
124
in the Lower Extremity
127
Aneurysms of the Lower Extremity
124
Venous Tone in Hypovolemic Shock
128
The Veins
125
Arterial Palpation
128
Great Saphenous Vein Variations and Venous
Vein Cutdown
125
Clinical Problem Solving Questions
129
Answers and Explanations
130
branches of the profunda femoris artery and the articular
THE ARTERIES
and muscular branches of the femoral and popliteal
arteries.
Collateral Circulation
Femoral Artery Catheterization
If the arterial supply to the leg is occluded, necrosis or gan-
A long, fine catheter can be inserted into the femoral
grene will follow unless an adequate bypass to the obstruc-
artery as it descends through the femoral triangle. The
tion is present—that is, a collateral circulation. Sudden
catheter is guided under fluoroscopic view along the ex-
occlusion of the femoral artery by ligature or embolism, for
ternal and common iliac arteries into the aorta. The
example, is usually followed by gangrene. However, grad-
catheter can then be passed into the inferior mesenteric,
ual occlusion such as occurs in atherosclerosis is less likely
superior mesenteric, celiac, or renal arteries. Contrast
to be followed by necrosis because the collateral blood ves-
medium can then be injected into the artery under exam-
sels have time to dilate fully. The collateral circulation for
ination and a permanent record obtained by taking a
the proximal part of the femoral artery is through the cru-
radiograph. Pressure records can also be obtained by guid-
ciate and trochanteric anastomoses; for the femoral artery
ing the catheter through the aortic valve into the left
in the adductor canal, it is through the perforating
ventricle.
The Blood Vessels of the Lower Extremity
123
Anatomy of Technique
Anatomy of Complications
The femoral artery is first located just below the inguinal lig-
The femoral vein lies immediately medial to the artery and
ament midway between the symphysis pubis and the ante-
may be entered in error. The nonpulsatile nature of the vein
rior superior iliac spine (CD Fig. 9-1). The needle or
on palpation should exclude this possibility. Since the hip
catheter is then inserted into the artery. The following struc-
joint lies posterior to the femoral artery, the erroneous pas-
tures are pierced:
sage of the needle through the posterior arterial wall may
■ Skin
cause it to pierce the psoas muscle and enter the joint cav-
■ Superficial fascia
ity. Some difficulty may be experienced in passing the
■ Deep fascia
catheter up the femoral artery if the artery is tortuous or if
■ Anterior layer of the femoral sheath
there is extensive atherosclerosis of the arterial wall.
external iliac vessels
inguinal
ligament
anterior superior
iliac spine
pubic tubercle
femoral vessels
symphysis pubis
long saphenous
vein
CD Figure 9-1
Surface markings of the major blood vessels on the anterior surface of
the left thigh.
124
Chapter 9
Traumatic Injury to Arteries of the
Intermittent Claudication and
Lower Limb
Arterial Occlusive Disease of the
Injury to the large femoral artery can cause rapid exsan-
Lower Extremity
guination of the patient. Unlike in the upper extremity,
arterial injuries of the lower limb do not have a good prog-
Atherosclerosis of the lower limb arteries is common in
nosis. The collateral circulations around the hip and knee
men. Ischemia of the muscles produces a cramp-like pain
joints, although present, are not as adequate as that around
with exercise. Intermittent claudication is a condition
the shoulder and elbow. Damage to a neighboring large
characterized by calf muscle cramping pain on exertion that
vein can further complicate the situation and causes further
is relieved by rest. Thrombosis in a diseased segment of the
impairment of the circulation to the distal part of the limb.
artery may lead to a sudden worsening of the symptoms and
even cause nocturnal ischemic pain. The common sites for
occlusion are the femoral, popliteal, and tibioperoneal ar-
Anatomy of Complications of
teries. If the obstruction occurs more proximally in the aorta
or iliac arteries, impotence is common.
Arterial Injury
A single perforating injury to an artery in the lower limb may
Femoropopliteal and Femorotibial
also perforate an accompanying vein and establish an acute
arteriovenous fistula. This complication is common in re-
Bypass for Lower Extremity
gions where large vessels run close together, such as the
femoral artery and vein in the femoral triangle and the sub-
Vascular Insufficiency
sartorial canal, and the popliteal artery and vein behind the
knee. Such a shunt produces a continuous machinery-like
Bypasses have been used with success in patients with severe
murmur over the fistula with the later development of vari-
distal extremity ischemia. In the presence of gangrene or se-
cosities and edema of the distal part of the limb.
vere rest pain, the distal limb has been successfully salvaged.
Anatomically, a true aneurysm is one whose wall con-
A reversed ipsilateral autogenous saphenous vein, a con-
tains all three layers of the arterial wall, namely, the intima,
tralateral saphenous vein, or a cephalic vein graft has been
media, and adventitia. A false aneurysm, sometimes called
used to connect the proximal femoral artery or popliteal
a pulsating hematoma, is one whose wall contains only the
artery to the distal popliteal or tibial or peroneal arteries.
tunica adventitia. An arterial perforation may lead to a false
aneurysm that becomes walled off by the adventitia and sur-
Lumbar Sympathectomy and
rounding tissues. Pressure on neighboring nerves may give
rise to neurologic symptoms.
Occlusive Arterial Disease
Lumbar sympathectomy may be advocated as a form of
Compartmental Syndromes
treatment in occlusive arterial disease of the lower extremity
Delay in the diagnosis and repair of injured arteries, espe-
to increase the blood flow through the collateral circulation.
cially when accompanied by vein damage, may lead to
Preganglionic sympathectomy is performed by removing
muscle necrosis and compartmental edema. The compart-
the upper three lumbar ganglia and the intervening parts of
ment syndromes are discussed on CD Chapter 13.
the sympathetic trunk.
Occlusions of the Popliteal, Anter-
Aneurysms of the Lower Extremity
These occur much less frequently than abdominal aortic
ior, and Posterior Tibial Arteries
aneurysms and are usually caused by atherosclerosis. Most
Popliteal artery occlusion occurs just below the beginning
patients are over 50 years of age, and the common sites are
of the artery (just below the opening in the adductor mag-
the femoral and popliteal arteries. The diagnosis is usually
nus muscle). In some cases the occlusion extends distally to
made by finding an expansile swelling along the course of
involve the origins of the anterior and posterior tibial arter-
the artery. Patients may present in the emergency depart-
ies and even the peroneal artery. Symptoms include inter-
ment with complications, which include sudden embolic
mittent claudication, night cramps, and rest pain caused by
obstruction to arteries distal to the aneurysm or sudden
ischemic neuritis. Signs include impaired or absent arterial
thrombotic occlusion of the aneurysm. Pressure on neigh-
pulses, lowered skin temperature, color changes, muscle
boring nerves may give rise to symptoms; for example, an en-
weakness, and trophic changes.
larging popliteal aneurysm may press on the tibial nerve,
The Blood Vessels of the Lower Extremity
125
causing pain in the foot. Rupture of femoral or popliteal
large one. This possibility is of great clinical importance
aneurysms is rare.
when performing a venous cutdown
Great Saphenous Vein Cutdown
THE VEINS
Exposure of the great saphenous vein through a skin inci-
sion (a “cutdown”) is usually performed at the ankle (CD
Fig. 9-2). This site has the disadvantage that phlebitis (in-
flammation of the vein wall) is a potential complication.
Great Saphenous Vein Variation
The great saphenous vein also can be entered at the groin
in the femoral triangle, where phlebitis is relatively rare;
and Venous Vein Cutdown
the larger diameter of the vein at this site permits the use
Occasionally the great saphenous vein at the medial malle-
of large-diameter catheters and the rapid infusion of large
olus is replaced by several small veins instead of a single
volumes of fluids.
saphenous nerve
great saphenous vein
A
medial malleolus of tibia
saphenous nerve
great saphenous vein
B
anterior superior
iliac spine
edge of saphenous opening
in deep fascia
femoral artery
pubic
femoral vein
great saphenous
vein
C
D
CD Figure 9-2
Great saphenous vein cutdown. A and B. At the ankle. The great saphe-
nous vein is constantly found in front of the medial malleolus of the tibia. C and D. At the
groin. The great saphenous vein drains into the femoral vein two fingerbreadths below
and lateral to the pubic tubercle.
126
Chapter 9
Anatomy of Ankle Vein Cutdown
Intraosseous Infusion in the Infant
The procedure is as follows:
This technique may be used for the infusion of fluids and
1. The sensory nerve supply to the skin immediately in
blood when it has been found impossible to obtain an intra-
front of the medial malleolus of the tibia is from
venous line. The procedure is easy and rapid to perform as
branches of the saphenous nerve, a branch of the
follows:
femoral nerve. The saphenous nerve branches are
■ With the distal leg adequately supported, the anterior
blocked with local anesthetic.
subcutaneous surface of the tibia is palpated.
2. A transverse incision is made through the skin and sub-
■ The skin is anesthetized about 1 in. (2.5 cm) distal to the
cutaneous tissue across the long axis of the vein just an-
tibial tuberosity, thus blocking the infrapatellar branch of
terior and superior to the medial malleolus (see CD
the saphenous nerve.
Fig. 9-2). Although the vein may not be visible through
■ The bone marrow needle is directed at right angles
the skin, it is constantly found at this site.
through the skin, superficial fascia, deep fascia, and tib-
ial periosteum and the cortex of the tibia. Once the
3. The vein is easily identified, and the saphenous nerve
needle tip reaches the medulla and bone marrow, the
should be recognized; the nerve usually lies just ante-
operator senses a feeling of “give.” The position of the
rior to the vein (see CD Fig. 9-2).
needle in the marrow can be confirmed by aspiration.
The needle should be directed slightly caudad to avoid
Anatomy of Groin Vein Cutdown
injury to the epiphyseal plate of the proximal end of the
tibia. The transfusion may then commence.
1. The area of thigh skin below and lateral to the scrotum
or labium majus is supplied by branches of the ilioin-
Varicose Veins
guinal nerve and the intermediate cutaneous nerve of
A varicosed vein is one that has a larger diameter than nor-
the thigh. The branches of these nerves are blocked
mal and is elongated and tortuous. Varicosity of the
with local anesthetic.
esophageal and rectal veins is described elsewhere. This
2. A transverse incision is made through the skin and sub-
condition commonly occurs in the superficial veins of the
cutaneous tissue centered on a point about 1.5 in. (4
lower limb and, although not life threatening, is responsible
cm) below and lateral to the pubic tubercle (see CD
for considerable discomfort and pain.
Fig. 9-2). If the femoral pulse can be felt (may be absent
Varicose veins have many causes, including hereditary
in patients with severe shock), the incision is carried
weakness of the vein walls and incompetent valves; elevated
medially just medial to the pulse.
intraabdominal pressure as a result of multiple pregnancies
or abdominal tumors; and thrombophlebitis of the deep
3. The great saphenous vein lies in the subcutaneous fat
veins, which results in the superficial veins becoming the
and passes posteriorly through the saphenous opening in
main venous pathway for the lower limb. It is easy to under-
the deep fascia to join the femoral vein about 1.5 in. (4
stand how this condition can be produced by incompetence
cm), or two fingerbreadths, below and lateral to the pu-
of a valve in a perforating vein. Every time the patient exer-
bic tubercle. It is important to understand that the great
cises, high-pressure venous blood escapes from the deep
saphenous vein passes through the saphenous opening
veins into the superficial veins and produces a varicosity,
to gain entrance to the femoral vein. However, the size
which might be localized to begin with but becomes more
and shape of the opening are subject to variation.
extensive later.
The successful operative treatment of varicose veins de-
The Great Saphenous Vein in
pends on the ligation and division of all the main tributaries
of the great or small saphenous veins, to prevent a collateral
Coronary Bypass Surgery
venous circulation from developing, and the ligation and di-
In patients with occlusive coronary disease caused by ather-
vision of all the perforating veins responsible for the leakage
osclerosis, the diseased arterial segment can be bypassed by
of high-pressure blood from the deep to the superficial
inserting a graft consisting of a portion of the great saphe-
veins. It is now common practice to also remove or strip the
nous vein. The venous segment is reversed so that its valves
superficial veins. Needless to say, it is imperative to ascertain
do not obstruct the arterial flow. Following removal of the
that the deep veins are patent before operative measures are
great saphenous vein at the donor site, the superficial
taken.
venous blood ascends the lower limb by passing through
Varicose Leg Ulcers
perforating veins and entering the deep veins.
The great saphenous vein can also be used to bypass
These occur in the region of the medial malleolus, are
obstructions of the brachial or femoral arteries.
caused by venous skin stasis, and may be a complication of
The Blood Vessels of the Lower Extremity
127
varicose veins; many are caused by postthrombotic incom-
petent perforating veins in the region.
Deep Vein Thrombosis and
A venous ulcer must be distinguished from an arterial
ulcer caused by atherosclerosis of the skin arteries. An arterial
Long-Distance Air Travel
ulcer tends to occur on the lateral side of the distal leg, and
Passengers who sit immobile for hours on long-distance
the leg is often pulseless and cool. A venous ulcer occurs on
flights are very prone to deep vein thrombosis in the legs.
the medial side of the distal leg because skin venous stasis
Preventative measures include stretching of the legs every
tends to be more severe on the medial side in the presence of
hour to improve the venous circulation.
varicose veins. The explanation for the laterally placed arter-
ial ulcer is that the skin over the lateral malleolus receives a
Femoral Vein Catheterization
poorer arterial supply than that over the medial malleolus.
Femoral vein catheterization is used when rapid access to a
Traumatic Bleeding from a
large vein is needed. The femoral vein has a constant rela-
Varicosed Vein
tionship to the medial side of the femoral artery just below
the inguinal ligament and is easily cannulated. However,
Profuse bleeding from a pierced varicosed vein may cause a
because of the high incidence of thrombosis with the possi-
patient to seek medical treatment. Pressure over the vein,
bility of fatal pulmonary embolism, the catheter should be
proximal to the injury, should stop the blood escaping. The
removed once the patient is stabilized.
varicosed veins have incompetent valves and venous blood
is merely draining downward by gravity from the abdominal
Anatomy of the Procedure
veins. Raising the leg to a level above the heart should also
stop the bleeding.
1. The skin of the thigh below the inguinal ligament is
supplied by the genitofemoral nerve; this nerve is
blocked with a local anesthetic.
Superficial Thrombophlebitis
2. The femoral pulse is palpated midway between the an-
Thrombosis of the superficial veins of the lower limb is often
terior superior iliac spine and the symphysis pubis, and
associated with varicose veins. The condition is painful, and
the femoral vein lies immediately medial to it.
the thrombosed vein is tender to touch; the overlying skin is
reddened and edematous. The thrombus is usually strongly
3. At a site about two fingerbreadths below the inguinal
adherent to the wall of the vein so that emboli are rarely
ligament, the needle is inserted into the femoral vein.
formed. However, should the thrombosis extend to the deep
veins through a perforating vein, embolic formation in the
Doppler Ultrasound Examination
deep vein can be a serious, although rare, complication.
of Venous Flow in the Lower
Deep Thrombophlebitis
Extremity
Thrombosis of the deep veins can occur at any time, but sig-
nificant predisposition is immobility of the lower limbs in
Posterior tibial veins: The probe is applied to the skin
bed or in a splint. The common site where the process starts
just posterior to the medial malleolus of the tibia. Here
is the veins draining the soleus muscle in the calf. It must be
the posterior tibial veins accompany the posterior tibial
assumed that the pressure of the bed on the calf veins dam-
artery between the tendon of the flexor digitorum longus
ages the tunica intima, and this together with certain predis-
and the posterior tibial nerve (CD Fig. 9-3).
posing factors, such as surgical trauma, malignant disease,
Popliteal vein: The probe is applied to the skin over the
pregnancy, or estrogen therapy, initiates thrombus forma-
popliteal space with the knee partly flexed to relax the
tion. Once formed, the thrombus may extend proximally
deep fascia. The flow signal is best heard over the vein
into the popliteal and femoral veins and even higher into the
just lateral to the popliteal artery (see CD Fig. 9-3).
iliac veins. The symptoms include discomfort and tightness
Femoral vein: The probe is placed over the vein at
in the calf, especially when the patient is using the calf mus-
midthigh as it lies in the subsartorial canal with the
cles, as in standing and walking. Tenderness of the calf mus-
femoral artery (see CD Fig. 9-3). The probe can also be
cles may be apparent, and edema of the ankles, pretibial area,
applied higher up on the skin covering the femoral trian-
or thigh may be present. The superficial veins may be dilated
gle just below the inguinal ligament. Here the femoral
and more obvious than normal. The great danger of deep
vein lies medial to the femoral artery (see CD Fig. 9-3).
vein thrombosis is the high incidence of pulmonary em-
The pulse of the femoral artery can easily be felt at the
bolism. A secondary problem is residual chronic venous in-
midpoint between the anterior superior iliac spine and
sufficiency of the lower extremities.
the symphysis pubis.
128
Chapter 9
flexor digitorum
longus tendon
popliteal
medial malleolus
tendo
vein and
of tibia
calcaneus
artery
posterior
tibial veins
and artery
tibial
posterior
nerve
tibial nerve
lateral
femur
vastus medialis
sartorius
Anterior superior
femoral artery
iliac spine
femoral vein
inguinal ligament
adductor
longus
Femoral
gracilis
midline
artery
femoral
vein
CD Figure 9-3
Doppler ultrasound of venous blood flow in the lower limb. A. Posterior
tibial veins at the ankle. B. Popliteal vein behind the knee. C. Femoral vein and the subsar-
torial (adductor) canal in the midthigh. D. Femoral vein just below the inguinal ligament.
may be called on to arrest a severe hemorrhage or palpate
Venous Tone in Hypovolemic
different parts of the arterial tree in patients with arterial
occlusion.
Shock
The femoral artery enters the thigh behind the in-
In extreme hypovolemic shock, excessive venous tone
guinal ligament at a point midway between the anterosupe-
caused by the contraction of the smooth muscle in the vein
rior iliac spine and the symphysis pubis (see text Fig. 9-2 and
walls may inhibit the venous flow and thus delay the intro-
CD Fig. 9-1). The artery is easily palpated here because it
duction of intravenous blood into the vascular system.
can be pressed backward against the pectineus and the su-
perior ramus of the pubis.
The popliteal artery can be felt by gentle palpation in
Arterial Palpation
the depths of the popliteal space provided that the deep fas-
Every health professional should know the precise position
cia is fully relaxed by passively flexing the knee joint (see text
of the main arteries within the lower limb, for he or she
Fig. 9-7).
The Blood Vessels of the Lower Extremity
129
The dorsalis pedis artery lies between the tendons of
longus. The pulsations of the artery can be felt midway be-
extensor hallucis longus and extensor digitorum longus,
tween the medial malleolus and the heel (see text Fig. 9-14).
midway between the medial and lateral malleoli on the
It should be remembered that the dorsalis pedis artery
front of the ankle (see text Fig. 9-9).
is sometimes absent and is replaced by a large perforating
The posterior tibial artery passes behind the medial
branch of the peroneal artery. In the same manner, the per-
malleolus and beneath the flexor retinaculum; it lies between
oneal artery may be larger than normal and replace the pos-
the tendons of flexor digitorum longus and flexor hallucis
terior tibial artery in the lower part of the leg.
Clinical Problem Solving Questions
Read the following case histories/questions and give
branches of the femoral artery and the muscular and
the best answer for each.
genicular branches of the popliteal artery.
E. The collateral circulation in the left leg was ade-
A 47-year-old woman complaining of a dull, aching
quate to prevent gangrene but was insufficient to
pain in the lower part of both legs visited her physician.
supply oxygen to the active leg muscles.
She stated that the pain was particularly severe at the
F. The perforating branches of the profunda femoris
end of a long day of standing at her work. On examina-
artery did not participate in the collateral circulation
tion, the patient was found to have widespread varicose
around the blocked femoral artery.
veins in both legs.
A 58-year-old businessman flew to Korea from New
1.
The following symptoms and signs supported the diag-
York by plane. Except for infrequent visits to the toilet,
nosis except which?
he remained in his seat sleeping or reading. Toward
A. The patient stated that the skin down the medial
the end of the long flight, he experienced mild cramp-
side of the leg was irritated especially in dry weather.
like pain in his right calf. On feeling his leg, he found
B. If the patient coughed in the standing position, a
it to be tender but thought nothing more about it. On
fluid thrill was transmitted from the abdomen to the
reaching his destination, he was walking down the
hand palpating the veins.
ramp from the plane when he suddenly collapsed with
C. The skin showed marked discoloration over the me-
severe pain in his left chest and was experiencing ex-
dial malleoli and was dry and scaly.
treme respiratory distress. The airport physician made
D. The patient had a large family of six children and
the diagnosis of pulmonary embolism, secondary to
the varicose veins showed improvement during
deep vein thrombosis of the right calf.
each pregnancy.
3.
The blood clot (embolus) reached the left lung via the
E. The great and small saphenous veins in both legs
following blood vessels except which?
were enlarged and elongated.
A. The right popliteal vein
A 65-year-old man told his physician that he could walk
B. The right common iliac vein
only about 50 yd (46 m) before a cramp-like pain in his
C. The inferior vena cava
left leg forced him to rest. After a thorough physical
D. The pulmonary trunk
examination, a diagnosis of severe intermittent claudi-
E. The left pulmonary vein
cation of the left leg was made.
4.
A 65-year-old man was seen in the emergency depart-
2.
The following findings in this patient supported the
ment complaining of the onset of a sudden pain in his
diagnosis except which?
right foot. He said that for the past 6 months he had
A. His femoral pulses were normal in both legs.
experienced some aching pain in the lower part of the
B. The popliteal, posterior tibial, and dorsalis pedis
right leg, but the foot pain had occurred quite sud-
pulses were present in the right leg and completely
denly and was different. On examination, a tender
absent in the left leg.
pulsatile swelling could be palpated in the right
C. Arteriography revealed a blockage of the left femoral
popliteal space. In anatomic terms explain the chronic
artery at the level of the adductor tubercle.
aching pain in the right lower leg. What is your ex-
D. The lower part of the left leg was receiving its blood
planation for the sudden onset of pain in the right
supply through the muscular and genicular
foot?
130
Chapter 9
5. Explain the significance of the valved perforating veins
7. Compare in anatomic and practical terms the advan-
of the lower limbs. What is the surface marking of the
tages and disadvantages of cutting down on the great
small saphenous vein at the ankle?
saphenous vein at the groin and ankle. What is the sur-
face marking of the great saphenous vein in the groin
6. What is the surface marking of the femoral artery? Name
and at the ankle? What is the relationship of the saphe-
the structures that are pierced by the insertion of a
nous nerve to the great saphenous vein at the ankle?
catheter into the femoral artery. What is the relationship
of the femoral artery to the femoral vein and the hip
8. What are the common complications of femoral vein
joint?
catheterization? What is the surface marking of the
femoral vein?
Answers and Explanations
1.
D is the correct answer. During the later months of
fibula. Here the position is constant and it can be
pregnancy, the enlarged uterus presses on the inferior
readily seen.
vena cava and impedes the venous return from the
6.
The femoral artery enters the thigh beneath the in-
lower limbs. This condition results in a worsening of
guinal ligament at a point midway between the anterior
preexisting varicosed veins.
superior iliac spine and the symphysis pubis (see CD
2.
F is the correct answer. The profunda femoris artery
Fig. 9-1).
arises from the femoral artery about 1.5 in. (3.8 cm) be-
The following structures are pierced by a catheter en-
low the inguinal ligament. It plays a major role in the for-
tering the femoral artery in the thigh just below the in-
mation of the collateral circulation around the knee joint.
guinal ligament: (a) skin, (b) superficial fascia, (c) deep
fascia, and (d) anterior layer of femoral sheath.
3.
E is the correct answer. The embolus does not enter the
left pulmonary vein. The embolus ascends the venous
The femoral vein lies along the medial side of the
system via the popliteal, femoral, external iliac, and
femoral artery within the femoral sheath. The cavity of
common iliac veins and inferior vena cava to reach the
the hip joint lies posterior to the femoral artery, sepa-
right atrium of the heart. It then passes into the right
rated by the psoas muscle and the fibrous joint capsule.
ventricle, pulmonary trunk, and left pulmonary artery
to finally reach the small or medium-sized branches of
7.
The advantages of great saphenous vein cutdown at the
the left pulmonary artery, where it becomes lodged and
ankle are (a) the position of the vein in front of the me-
obstructs the circulation.
dial malleolus is constant, and (b) apart from the pres-
ence of the saphenous nerve, there are no other
4.
The chronic aching pain in the right lower leg could be
anatomic structures to damage—the cutdown is made
explained by the pressure of the expanding popliteal
over bone. The disadvantages are (a) phlebitis is a com-
aneurysm on the tibial nerve (see text Fig. 9-7) in the
mon complication, and (b) the small diameter pre-
popliteal space. The sudden onset of severe pain in the
cludes the rapid instillation of large volumes of fluid; in
foot could be explained by the lodging of an embolus
young children the small diameter of the vein some-
in one of the arteries in the foot. The embolus could
times make it difficult to identify.
have originated as a thrombus in the wall of the
popliteal aneurysm.
The advantages of great saphenous cutdown in the
groin are (a) the larger diameter of the vein at this site
5.
Normally, the valved perforating veins drain the super-
permits the rapid instillation of large volumes of fluid,
ficial veins through the deep fascia into the deep veins.
and (b) there is easier recognition of the vein at this site.
Incompetence of these important veins permits reflux
The disadvantages of the groin site are (a) the great
of deep venous blood into the superficial veins and
saphenous vein lies in thick subcutaneous fat about 1
commonly results in the formation of local superficial
1/2 in. below and lateral to the pubic tubercle; its iden-
varices.
tification may prove difficult in obese patients; and (b)
The small saphenous vein drains the lateral end of the
other important structures may be damaged, including
dorsal venous arch of the foot and ascends in the su-
the femoral artery and vein, if the procedure is carried
perficial fascia posterior to the lateral malleolus of the
out by an inexperienced individual.
The Blood Vessels of the Lower Extremity
131
The saphenous nerve usually lies just anterior to the
or misses the vein and traverses the psoas muscle and
great saphenous vein as it ascends anterior to the medial
the anterior part of the capsule of the hip joint; and
malleolus of the tibia (see CD Fig. 9-2).
(d) damage to the femoral nerve, which normally lies
some distance laterally to the femoral artery (midpoint
8. The common complications of femoral vein catheter-
between the anterior superior iliac spine and the pu-
ization are (a) thrombophlebitis of the femoral vein,
bic tubercle).
especially if the catheterization is prolonged (since the
catheter entering the saphenous vein at the groin also
The surface marking of the femoral vein is just medial
goes into the femoral vein, there is risk of phlebitis
to the pulsating femoral artery below the inguinal liga-
with saphenous catheterization as well); (b) hematoma
ment. If the artery is pulseless, the position of the artery
formation if the procedure is poorly carried out and
may be determined as being midway between the ante-
the vein wall is torn; (c) infection of the hip joint if an
rior superior iliac spine and the symphysis pubis; the
infected catheter pierces the femoral vein completely
vein lies just medial to it (see text Fig. 9-1).
The Lymph Vessels and
Lymph Tissue
10
Chapter Outline
The Lymph Vessels and Lymph Tissue
136
Examination of the Axillary Lymph Nodes
137
Edema and Lymphatic Obstruction
136
Carcinoma of the Breast and the Axillary Lymph
Nodes
138
Lymphangitis and Lymphadenitis
136
Mediastinoscopy and the Tracheobronchial
Lymph Flow in Clinical Medicine
136
Lymph Nodes
138
Lymph Vessels and the Spread of Malignant
Lymphatics of the Lower Limb
138
Disease
137
The Thymus
139
Enlargement of the Submandibular Lymph Nodes
and Swelling of the Submandibular Salivary
Allograft Rejection
139
Gland
137
Tumors of the Thymus
139
Clinical Significance of the Cervical Lymph Nodes
137
Clinical Problem Solving Questions
139
Examination of the Deep Cervical Lymph Nodes
137
Carcinoma Metastases in the Deep Cervical
Answers and Explanations
141
Lymph Nodes
137
may resemble that of an elephant, hence the name
THE LYMPH
elephantiasis.
■ Malignant metastases in lymph nodes and lymphatic
vessels: This condition may cause edema of the skin of
VESSELS AND
the breast or arm in advanced carcinoma of the breast.
LYMPH TISSUE
Lymphangitis and Lymphadenitis
Lymphangitis is an infection of the lymphatic vessels and is
Edema and Lymphatic Obstruction
a common occurrence. Red streaks along the course of the
lymphatic vessels are characteristic of the condition. For
An inability to absorb protein from the tissue fluid into the
example, a severe infection of the thumb may be followed
lymphatic capillary will result in an accumulation of protein
by the spread of the bacteria into the lymphatic vessels drain-
in the tissue fluid outside the capillary and cause edema.
ing the area. Red streaks may be seen on the anterior aspect
This occurs in several conditions:
of the forearm, following the course of the cephalic vein.
■ Congenital lymphatic obstruction (Milroy’s disease):
Once the infection reaches the lymph nodes, the nodes
In this condition the lymphatic vessels, especially those
become enlarged and tender, a condition known as
of the lower limbs, fail to develop.
lymphadenitis.
■ Surgical removal of lymph nodes and lymph vessels:
This occurs when an attempt is made to completely re-
Lymph Flow in Clinical Medicine
move cancer cells that may have spread from their pri-
mary locus. This form of edema commonly occurs in the
The factors responsible for normal lymph flow in lymphatic
upper limbs following a radical mastectomy for carci-
vessels include muscle activity, local arterial pulsation,
noma of the breast.
valves in lymphatic vessels, tissue fluid pressure, and gravity.
■ Filariasis: In this mosquito-spread disease, common in
There are clinical situations in which it is important to di-
the tropics, the worm larvae enter the lymphatic vessels
minish the speed of lymph flow. For example, a patient who
and progressively block the lymph nodes. After a number
has a severe bacterial infection of the hand may have the
of years, the lymphatic drainage of the leg may become
arm immobilized in a sling as an important part of the treat-
totally obstructed and the grossly edematous lower limb
ment. This procedure reduces the muscular activity of the
The Lymph Vessels and Lymph Tissue
137
limb and, consequently, the lymph flow, lessening the pos-
sibility of bacterial spread via the lymphatic vessels and di-
Examination of the Deep Cervical
minishing the rate of entry of toxins into the blood stream
via the lymph. In some conditions, it may be necessary to
Lymph Nodes
have the patient rest in bed to reduce lymph flow.
Lymph nodes in the neck should be examined from behind
Other clinical conditions may require an increase in
the patient. The examination is made easier by asking the
the flow of lymph in lymphatic vessels. In postural edema,
patient to flex the neck slightly to reduce the tension of the
an individual who has been standing in one position for
muscles. The groups of nodes should be examined in a
hours may experience swelling of the ankles and feet. In-
definite order to avoid omitting any.
creasing lymph flow also may be important in someone who
After the identification of enlarged lymph nodes, possi-
has had a limb immobilized for a long period in a splint.
ble sites of infection or neoplastic growth should be exam-
Muscular exercises, raising the limb to use the force of grav-
ined, including the face, scalp, tongue, mouth, tonsil, and
ity, or massage applied to the area will aid the flow of lymph
pharynx.
along the valved lymphatic vessels.
Carcinoma Metastases in the Deep
Lymph Vessels and the Spread of
Cervical Lymph Nodes
Malignant Disease
In the head and neck, all the lymph ultimately drains into
Lymphatic vessels provide a pathway for the spread of cer-
the deep cervical group of nodes. Secondary carcinoma-
tain types of malignant tumors from their site of origin.
tous deposits in these nodes are common. The primary
When the cancer cells reach a lymph node, they may be
growth may be easy to find. On the other hand, at certain
temporarily stopped by the network of reticular fibers.
anatomic sites the primary growth may be small and over-
However, the cancer cells may continue to multiply in
looked, for example, in the larynx, the pharynx, the cervical
situ, leading to the formation of a secondary growth or
part of the esophagus, and the external auditory meatus. The
metastasis.
bronchi, breast, and stomach are sometimes the site of the
primary tumor. In these cases, the secondary growth has
Enlargement of the Submandibu-
spread far beyond the local lymph nodes.
When cervical metastases occur, the surgeon usually
lar Lymph Nodes and Swelling of
decides to perform a block dissection of the cervical nodes.
This procedure involves the removal en bloc of the internal
the Submandibular Salivary Gland
jugular vein, the fascia, the lymph nodes, and the sub-
mandibular salivary gland. The aim of the operation is re-
The submandibular lymph nodes are commonly enlarged as
moval of all the lymph tissues on the affected side of the
a result of a pathologic condition of the scalp, face, maxillary
neck. The carotid arteries and the vagus nerve are carefully
sinus, or mouth cavity. One of the most common causes of
preserved. It is often necessary to sacrifice the hypoglossal
painful enlargement of these nodes is acute infection of the
and vagus nerves, which may be involved in the cancerous
teeth. Enlargement of these nodes should not be confused
deposits. In patients with bilateral spread, a bilateral block
with pathologic swelling of the submandibular salivary gland.
dissection may be necessary. An interval of 3 to 4 weeks is
necessary before removing the second internal jugular vein.
Clinical Significance of the
Examination of the Axillary
Cervical Lymph Nodes
Knowledge of the lymph drainage of an organ or region is of
Lymph Nodes
great clinical importance. Examination of a patient may re-
With the patient standing or sitting, he or she is asked to place
veal an enlarged lymph node. It is the physician’s responsi-
the hand of the side to be examined on the hip and push hard
bility to determine the cause and be knowledgeable about
medially. This action of adduction of the shoulder joint
the area of the body that drains its lymph into a particular
causes the pectoralis major muscle to contract maximally so
node. For example, an enlarged submandibular node can
that it becomes hard like a board. The examiner then pal-
be caused by a pathologic condition in the scalp, the face,
pates the axillary nodes (see text Fig. 10-3) as follows:
the maxillary sinus, or the tongue. An infected tooth of the
upper or lower jaw may be responsible. Often a physician
■ The anterior (pectoral) nodes may be palpated by press-
has to search systematically the various areas known to drain
ing forward against the posterior surface of the pectoralis
into a node to discover the cause.
major muscle on the anterior wall of the axilla.
138
Chapter 10
■ The posterior (subscapular) nodes may be palpated by
Radical mastectomy is designed to remove the pri-
pressing backward against the anterior surface of the sub-
mary tumor and the lymph vessels and nodes that drain
scapularis muscle on the posterior wall of the axilla.
the area. This means that the breast and the associated
■
The lateral nodes may be palpated against the medial
structures containing the lymph vessels and nodes must
side of the axillary vein. The examiner’s fingers are
be removed en bloc. The excised mass is therefore made
pressed laterally against the subclavian vein and the pul-
up of the following: a large area of skin overlying the tu-
sating axillary artery.
mor and including the nipple; all the breast tissue; the
■
The central nodes may be palpated in the center of the
pectoralis major and associated fascia through which the
axilla between the pectoralis major (anterior wall) and
lymph vessels pass to the internal thoracic nodes; the pec-
the subscapularis (posterior wall).
toralis minor and associated fascia related to the lymph
■
For the apical nodes, the patient is asked to relax the
vessels passing to the axilla; all the fat, fascia, and lymph
shoulder muscles and let the upper limb hang down at
nodes in the axilla; and the fascia covering the upper part
the side. The examiner then gently places the tips of the
of the rectus sheath, the serratus anterior, the subscapu-
fingers of the examining hand high up in the axilla to the
laris, and the latissimus dorsi muscles. The axillary blood
outer border of the first rib. If the nodes are enlarged they
vessels, the brachial plexus, and the nerves to the serratus
can be felt.
anterior and the latissimus dorsi are preserved. Some de-
gree of postoperative edema of the arm is likely to follow
The examination of the axillary lymph nodes always
such a radical removal of the lymph vessels draining the
forms part of the clinical examination of the breast.
upper limb.
A modified form of radical mastectomy for patients with
clinically localized cancer is also a common procedure and
Carcinoma of the Breast and the
consists of a simple mastectomy in which the pectoral mus-
cles are left intact. The axillary lymph nodes, fat, and fascia
Axillary Lymph Nodes
are removed. This procedure removes the primary tumor
The importance of knowing the lymph drainage of the
and permits pathologic examination of the lymph nodes for
breast in relation to the spread of cancer from that organ
possible metastases.
cannot be overemphasized. The lymph vessels from the me-
dial quadrants of the breast pierce the second, third, and
Mediastinoscopy and the Tracheo-
fourth intercostal spaces and enter the thorax to drain into
the lymph nodes alongside the internal thoracic artery. The
bronchial Lymph Nodes
lymph vessels from the lateral quadrants of the breast drain
into the anterior or pectoral group of axillary nodes. It fol-
Mediastinoscopy is a diagnostic procedure whereby speci-
lows, therefore, that a cancer occurring in the lateral quad-
mens of tracheobronchial lymph nodes are obtained with-
rants of the breast tends to spread to the axillary nodes.
out opening the pleural cavities. A small incision is made in
Thoracic metastases are difficult or impossible to treat, but
the midline in the neck just above the suprasternal notch,
the lymph nodes of the axilla can be removed surgically.
and the superior mediastinum is explored down to the re-
Approximately 60% of carcinomas of the breast occur in
gion of the bifurcation of the trachea. The procedure can be
the upper lateral quadrant. The lymphatic spread of cancer
used to determine the diagnosis and degree of spread of car-
to the opposite breast, to the abdominal cavity, or into
cinoma of the bronchus.
lymph nodes in the root of the neck is caused by obstruction
of the normal lymphatic pathways by malignant cells or de-
Lymphatics of the Lower Limb
struction of lymph vessels by surgery or radiotherapy. The
cancer cells are swept along the lymph vessels and follow
The superficial and deep inguinal lymph nodes not only
the lymph stream. The entrance of cancer cells into the
drain all the lymph from the lower limb, but also drain
blood vessels accounts for the metastases in distant bones.
lymph from the skin and superficial fascia of the anterior
In patients with localized cancer of the breast, most sur-
and posterior abdominal walls below the level of the um-
geons do a simple mastectomy or a lumpectomy, followed
bilicus; lymph from the external genitalia and the mucous
by radiotherapy to the axillary lymph nodes and/or hormone
membrane of the lower half of the anal canal also drains
therapy. In patients with localized cancer of the breast with
into these nodes. Remember the large distances the lymph
early metastases in the axillary lymph nodes, most authori-
has had to travel in some instances before it reaches the
ties agree that radical mastectomy offers the best chance of
inguinal nodes. For example, a patient may present with
cure. In patients in whom the disease has already spread be-
an enlarged, painful inguinal lymph node caused by lym-
yond these areas (e.g., into the thorax), simple mastectomy,
phatic spread of pathogenic organisms that entered the
followed by radiotherapy or hormone therapy, is the treat-
body through a small scratch on the undersurface of the
ment of choice.
big toe.
The Lymph Vessels and Lymph Tissue
139
the immunocompetent lymphocytes with drugs have been
THE THYMUS
moderately successful.
Tumors of the Thymus
Allograft Rejection
Thymomas are tumors of the thymus and are some of the
At about the time of birth, T lymphocytes leave the thymus
most common tumors found in the anterior mediastinum.
and populate the peripheral lymphatic tissue; it is these cells
Many of the tumors are associated with myasthenia gravis
that will bring about rejection of an allograft. Grafts between
and aplasia of blood cells. It is thought that these diseases are
identical twins or from an individual to himself or herself
autoimmune in origin and may develop as a result of the for-
will survive indefinitely, because there is no antigenic re-
mation of T lymphocytes that react to the individual’s own
sponse. Although the thymus in the adult continues to in-
tissues. Myasthenia gravis is a disease in which there is a
fluence the activities of the T lymphocytes, possibly by
possible reduction of acetylcholine receptors at the motor
means of thymosin, thymectomy has been unsuccessful in
end-plates of skeletal muscle. Thymomas may be benign or
preventing the rejection of allografts. Attempts to suppress
malignant.
Clinical Problem Solving Questions
Read the following case histories/questions and give
normal lymph flow. Describe the main factors respon-
the best answer for each.
sible for lymph flow.
4.
Explain the mechanism of allograft rejection. What
1.
A 23-year-old woman is treated in the emergency de-
form of immunity is lacking in a patient who has a con-
partment for an infected right index finger. Three days
genital absence of the thymus?
previously, she had got a rose thorn in her finger while
gardening. On examination, the finger is red, tender,
A 70-year-old man complaining of a small painless
and very swollen. After removing the thorn and apply-
swelling below his chin visited his physician. On ques-
ing a dressing, the physician prescribes a course of an-
tioning, he said that he had first noticed the swelling 4
tibiotics. He asks the nurse to put the patient’s right arm
months earlier and that it was gradually increasing in
in a sling, and warns the patient not to move the arm ex-
size. Because it had not caused any discomfort, he had
cessively. Explain why the patient’s arm has been
chosen to ignore it. On examination, a single, small,
placed in a sling.
hard swelling could be palpated in the submental tri-
angle. It was mobile on the deep tissues and not at-
2.
A 54-year-old man visits his doctor complaining of a
tached to the skin.
skin infection of the auricle of the right ear. The patient
had scratched his ear 4 days previously and since then
5.
The following statements suggest that the hard swelling
his ear has become greatly swollen, and his wife has
is a secondary malignant deposit in a lymph node ex-
noted that the right side of his neck is also swollen. The
cept which?
physician’s assistant made the diagnosis of impetigo and
A. The submental lymph nodes are located in the sub-
gave the patient an antibiotic to be taken orally. She ad-
mental triangle just below the chin.
vised the patient to place a warm compress over the ear
B. The submental lymph nodes drain the tip of the
twice daily to reduce the auricular swelling. Using your
tongue, the floor of the mouth in the region of the
knowledge of anatomy and physiology, explain the fol-
frenulum of the tongue, the gums and incisor teeth,
lowing: (a) Why is the ear swollen? (b) Why is the right
the middle third of the lower lip, and the skin over
side of the neck swollen? and (c) Why will the applica-
the chin.
tion of a warm compress to the ear reduce the swelling?
C. A small, hard-based carcinomatous ulcer was found
3.
A 58-year-old woman following a right radical mastec-
on the right side of the tongue near the tip.
tomy (which involves the removal of the right breast
D. The deep cervical group of lymph nodes beneath
and the right axillary lymph nodes) has lymphatic
the sternocleidomastoid muscle receive lymph from
edema of the right arm because of obstruction of the
the submental lymph nodes.
140
Chapter 10
E. The submental lymph nodes lie deep to the superfi-
carcinoma of the left breast was made, with secondary
cial part of the submandibular salivary gland.
deposits in the axilla.
An 8-year-old boy was examined by a pediatrician and
8.
The following statements concerning this patient are
found to have a painful swelling below and behind the
correct except which?
angle of the jaw on the left side. The skin over the
A. The contracting fibrous tissue of the malignant tu-
swelling was red and hot. Palpation of the neck revealed
mor had pulled on the lactiferous ducts of the nip-
a tender firm swelling beneath the anterior border of
ple, raising it above the level of the opposite nipple.
the sternocleidomastoid muscle on the left side. The
B. The dimpling of the skin was caused by the fibrous
right side of the neck was normal. Examination of the
tissue pulling on the suspensory ligaments of the
pharynx and palatine tonsils showed marked redness of
breast.
the mucous membrane and enlargement of both ton-
C. The upper lateral quadrant of the breast is drained
sils, especially the one on the left. The left tonsil also
into the pectoral or anterior axillary lymph nodes.
showed a yellow exudate draining from the tonsillar
D. The enlarged pectoral lymph nodes could be pal-
crypts.
pated against the surgical neck of the humerus.
E. The malignant tumor had spread by way of the
6.
Using your knowledge of anatomy, name the group of
lymph vessels to the pectoral lymph nodes.
lymph nodes involved in the disease.
A 45-year-old man complaining of a lump in the groin
An 18-year-old woman complaining of severe pain and
was seen by his physician. The lump, which caused
redness around the base of the nail of the right thumb
him no pain or discomfort, was first recognized 3
visited her physician. She stated that she had trimmed
months previously. On examination, a large discrete
the cuticle (eponychium) of her nail with scissors, and
hard lump was found about 2 in. (5 cm) below and lat-
the following day the pain commenced. On examina-
eral to the pubic tubercle on the front of the right thigh.
tion, the skin folds around the root of the nail were red,
swollen, and extremely tender. The thumb was swollen,
9.
The following signs indicated that this patient had a
and red streaks were seen coursing up the front of the
melanoma of the right big toe with secondaries in the
forearm.
inguinal lymph nodes except which?
A. Two smaller hard swellings were found immediately
7.
The following symptoms and signs in this patient were
below the large swelling.
consistent with a diagnosis of an acute bacterial infec-
B. On flexing the right knee joint, three small hard
tion under the nail folds (paronychia) of the right
swellings could be palpated in the popliteal fossa.
thumb except which?
C. The external genitalia were found to be normal.
A. Some tender lymph nodes could be palpated in the
D. Examination of the anal canal revealed nothing ab-
infraclavicular fossa.
normal.
B. The patient’s temperature was raised.
E. A small pigmented mole was discovered beneath the
C. The infection had spread into the lymph vessels
nail of the right big toe.
draining the finger.
10.
A senior medical student taking a surgical examination
D. The red streaks on the front of the forearm were
was asked to look at a 55-year-old man. On examination
caused by the local vasodilatation of the blood ves-
of the abdomen, he found a hard, fixed mass in the mid-
sels along the course of the lymph vessels.
line, about 4 in. (10 cm) in diameter, lying on the transpy-
E. The lymph vessels from the thumb drain into the
loric plane. On questioning, the patient said that he had
supratrochlear node, which was inflamed and en-
recently lost 20 lb and had a poor appetite. The student
larged.
told the examiner that the patient was suffering from a car-
A 45-year-old woman having her yearly physical exami-
cinoma of the stomach and should have an immediate
nation was found to have a hard, painless lump in the
gastrectomy. The examiner then asked the student if he
upper lateral quadrant of the left breast. On examina-
had examined the patient’s scrotum, and the student ad-
tion with her arms at her sides, the left nipple was seen
mitted he had not. On examination, the scrotum was
to be higher than the right, and a small dimple of skin
found to contain a large, hard mass on the right side that
was noted over the lump. On examination of the left ax-
was not tethered to the skin. The inguinal lymph nodes
illa, three small, hard discrete nodules could be pal-
on the right side were normal. Explain the connection be-
pated below the lower border of the pectoralis major
tween the abdominal swelling and the scrotal swelling.
muscle. The right breast was normal. A diagnosis of
Why were the inguinal lymph nodes normal?
The Lymph Vessels and Lymph Tissue
141
Answers and Explanations
1.
The immobilization of the patient’s arm in a sling re-
6.
This patient had a streptococcal pharyngitis with in-
duces the muscular activity and, thus, the rate of lymph
volvement of the palatine tonsils, especially the one on
flow from the limb. This serves to limit the spread of
the left. The infection had spread on the left side to in-
toxins and bacteria from the site of infection.
volve the jugulodigastric member of the deep cervical
lymph nodes (see text Fig. 10-2). This node had en-
2.
(a) The auricle of the ear is swollen by inflammatory
larged due to the inflammatory process and was re-
edema. Edema is an abnormal accumulation of tissue
sponsible for the tender swelling on the left side of the
fluid in the intercellular spaces. The fluid dynamics of
neck.
inflammatory edema includes the vasodilatation of the
arterioles and capillaries at the site of infection with an
7.
E is the correct answer. The lymph vessels from the in-
outpouring of protein-rich plasma into the tissue spaces
dex finger drain into the deltopectoral nodes (see text
along with the outpouring of neutrophils. (b) The right
Fig. 10-1).
side of the neck is swollen because the bacteria have
8.
D is the correct answer. The enlarged pectoral lymph
spread from the right auricle via the lymphatic vessels to
nodes can be palpated against the posterior surface of
the right superficial and deep cervical lymph nodes,
the contracted pectoralis major muscle (see text Fig. 10-
which are enlarged as a result of the proliferation of the
4).
contained lymphocytes. (c) In the early stages of
infection, heat causes arteriolar vasodilatation, which in
9.
B is the correct answer. Melanomas, which are highly
turn raises blood flow through the infected skin,
malignant tumors, tend to initially spread via the lymph
hastening the arrival of neutrophils, antibodies, and an-
vessels to the local lymph nodes. These become en-
tibiotics to the site of infection. Once the infection is
larged and firm on palpation. The lymphatic drainage
controlled, the increased vascular and lymphatic flow
of the big toe is into the vertical group of superficial in-
will help reduce the local accumulation of tissue fluid
guinal lymph nodes (see text Fig. 10-7).
and cause the swelling of the ear to diminish.
10.
The student failed to examine the entire patient and
3.
The factors responsible for lymph flow are summarized
made an erroneous diagnosis. He may have been
in the CD paragraph under Lymph Flow in Clinical
sidetracked in his thoughts by the patient stating that
Medicine.
he had a poor appetite. One thing is certain—the stu-
dent had forgotten his anatomy! (a) Malignant dis-
4.
The mechanism of allograft rejection is summarized in
ease of the testis metastasizes to the lateral aortic
the CD paragraph under Allograft Rejection. In con-
nodes lying on the side of the body of the first lum-
genital absence of the thymus, the patient lacks T lym-
bar vertebra in the abdomen (on the transpyloric
phocytes and, therefore, cellular immunity.
plane). This is the normal lymph drainage of the
5.
E is the correct answer. The submental lymph nodes
testis.
(b) The inguinal lymph nodes are only in-
are not covered by the superficial parts of the sub-
volved if the tumor spreads locally into the tissues of
mandibular salivary gland (see text Fig. 10-2).
the scrotum outside the testis.
The Musculoskeletal
System
Chapter Outline
Bones
147
Greater Tuberosity Fractures
152
Lesser Tuberosity Fractures
152
Bone Fractures
147
Surgical Neck Fractures
152
Rickets
147
Fractures of the Shaft of the Humerus
152
Fractures of the Distal End of the
Epiphyseal Plate Disorders
147
Humerus
152
Skull
147
Bones of the Forearm
152
Clinical Features of the Neonatal Skull
147
Fractures of the Radius and Ulna
152
Fontanelles
147
Olecranon Bursitis
154
Tympanic Membrane
147
Bones of the Hand
154
Forceps Delivery and the Facial Nerve
147
Injuries to the Bones of the Hand
154
Fractures of the Skull
147
Bones of the Lower Limb
154
Fractures of the Anterior Cranial Fossa
148
Bones of the Pelvic Girdle
154
Fractures of the Middle Cranial Fossa
148
Clinical Concept: The Pelvis is a Basin
Fractures of the Posterior Cranial Fossa
148
with Holes in its Walls
154
Bone Injuries of the Skull and Skeletal
Pelvic Measurements in Obstetrics
155
Development
148
Internal Pelvic Assessments
155
Anatomy of Common Facial Fractures
148
The Female Pelvis
155
Nasal Fractures
148
Fractures of the Pelvis
156
Maxillofacial Fractures
148
Fractures of the False Pelvis
156
Blowout Fractures of the Maxilla
148
Fractures of the True Pelvis
156
Fractures of the Zygoma or Zygomatic
Fractures of the Sacrum and Coccyx
158
Arch
149
Minor Fractures of the Pelvis
158
Mandible
149
Anatomy of Complications of Pelvic
Fractures of the Mandible
149
Fractures
158
Vertebral Column
149
Bones of the Thigh
158
Examination of the Back
149
Tenderness of the Head of the Femur and
Abnormal Curves of the Vertebral Column
150
Arthritis of the Hip Joint
158
Partial Fusion of the Sacral Vertebrae
150
Blood Supply to the Femoral Head and
Fracture of the Sacrum in Trauma of the Pelvis
150
Neck Fractures
159
Fractures of the Coccyx and Coccydynia
150
The Neck of the Femur and Coxa Valga
and Coxa Vara
159
Thoracic Bones
150
Fractures of the Femur
159
Clinical Importance of the Sternal Angle
Patellar Dislocations
161
(Angle of Louis)
150
Patellar Fractures
161
Sternum and Marrow Biopsy
150
Bones of the Leg
161
Cervical Rib
150
Fractures of the Tibia and Fibula
161
Rib Excision
151
Interosseous Infusion of the Tibia in the
Bones of the Upper Limb
151
Infant
161
Bones of the Shoulder Girdle
151
Bones of the Foot
161
Fractures of the Clavicle
151
Fractures of the Calcaneum
161
Compression of the Brachial Plexus,
Fractures of the Talus
161
Subclavian Artery, and Subclavian Vein
Fractures of the Metatarsal Bones
162
by the Clavicle
151
Fractures of the Scapula
151
Clinical Problem Solving Questions
162
Dropped Shoulder and Winged Scapula
151
Bones of the Arm
152
Answers and Explanations
165
Fractures of the Proximal End of the
Humerus
152
Humeral Head Fractures
152
Bones and Cartilage
147
Skull
BONES
Clinical Features of the Neonatal Skull
Bone
Fractures
Fontanelles
Immediately after a fracture, the patient suffers severe local
pain and is not able to use the injured part. Deformity may
Palpation of the fontanelles enables the physician to deter-
be visible if the bone fragments have been displaced relative
mine the progress of growth in the surrounding bones, the
to each other. The degree of deformity and the directions
degree of hydration of the baby (e.g., if the fontanelles are
taken by the bony fragments depend not only on the mech-
depressed below the surface, the baby is dehydrated), and
anism of injury but also on the pull of the muscles attached
the state of the intracranial pressure (a bulging fontanelle
to the fragments. Ligamentous attachments also influence
indicates raised intracranial pressure).
the deformity. In certain situations—for example, the
Samples of cerebrospinal fluid can be obtained by pass-
ileum—fractures result in no deformity because the inner
ing a long needle obliquely through the anterior fontanelle
and outer surfaces of the bone are splinted by the extensive
into the subarachnoid space or even into the lateral ventricle.
origins of muscles. In contrast, a fracture of the neck of the
Clinically, it is usually not possible to palpate the ante-
femur produces considerable displacement. The strong
rior fontanelle after 18 months, because the frontal and
muscles of the thigh pull the distal fragment upward so that
parietal bones have enlarged to close the gap.
the leg is shortened. The very strong lateral rotators rotate
Tympanic Membrane
the distal fragment laterally so that the foot points laterally.
Fracture of a bone is accompanied by a considerable
At birth, the tympanic membrane faces more downward and
hemorrhage of blood between the bone ends and into the
less laterally than in maturity; when examined with the oto-
surrounding soft tissue. The blood vessels and the fibroblasts
scope, it therefore lies more obliquely in the infant than in
and osteoblasts from the periosteum and endosteum take
the adult.
part in the repair process.
Forceps Delivery and the Facial Nerve
Rickets
In the newborn infant, the mastoid process is not developed,
and the facial nerve, as it emerges from the stylomastoid
Rickets is a defective mineralization of the cartilage matrix
foramen, is close to the surface. Thus, it can be damaged by
in growing bones. This produces a condition in which the
forceps in a difficult delivery.
cartilage cells continue to grow, resulting in excess cartilage
and a widening of the epiphyseal plates. The poorly miner-
Fractures of the Skull
alized cartilaginous matrix and the osteoid matrix are soft,
and they bend under the stress of bearing weight. The re-
Fractures of the skull are common in the adult but much
sulting deformities include enlarged costochondral junc-
less so in the young child. In the infant skull, the bones are
tions, bowing of the long bones of the lower limbs, and boss-
more resilient than in the adult skull, and they are separated
ing of the frontal bones of the skull. Deformities of the pelvis
by fibrous sutural ligaments. In the adult, the inner table of
may also occur.
the skull is particularly brittle. Moreover, the sutural liga-
ments begin to ossify during middle age.
The type of fracture that occurs in the skull depends on
Epiphyseal Plate Disorders
the age of the patient, the severity of the blow, and the area
Epiphyseal plate disorders affect only children and adoles-
of skull receiving the trauma. The adult skull may be
cents. The epiphyseal plate is the part of a growing bone
likened to an eggshell in that it possesses a certain limited re-
concerned primarily with growth in length. Trauma, infec-
silience beyond which it splinters. A severe, localized blow
tion, diet, exercise, and endocrine disorders can disturb the
produces a local indentation, often accompanied by splin-
growth of the hyaline cartilaginous plate, leading to defor-
tering of the bone. Blows to the vault often result in a series
mity and loss of function. In the femur, for example, the
of linear fractures, which radiate out through the thin areas
proximal epiphysis can slip because of mechanical stress or
of bone. The petrous parts of the temporal bones and the oc-
excessive loads. The length of the limbs can increase exces-
cipital crests strongly reinforce the base of the skull and tend
sively because of increased vascularity in the region of the
to deflect linear fractures.
epiphyseal plate secondary to infection or in the presence of
In the young child, the skull may be likened to a table-
tumors. Shortening of a limb can follow trauma to the epi-
tennis ball in that a localized blow produces a depression
physeal plate resulting from a diminished blood supply to
without splintering. This common type of circumscribed
the cartilage.
lesion is referred to as a “pond” fracture.
148
Chapter 11
skull is developed from membrane (whereas the remainder
Fractures of the Anterior Cranial Fossa
is developed from cartilage); therefore, this part of the skull
In fractures of the anterior cranial fossa, the cribriform plate
in children is relatively flexible and can absorb considerable
of the ethmoid bone may be damaged. This usually results in
force without resulting in a fracture.
tearing of the overlying meninges and underlying mucope-
Signs of fractures of the facial bones include deformity,
riosteum. The patient will have bleeding from the nose
ocular displacement, or abnormal movement accompanied
(epistaxis) and leakage of cerebrospinal fluid into the nose
by crepitation and malocclusion of the teeth. Anesthesia or
(cerebrospinal rhinorrhea). Fractures involving the orbital
paresthesia of the facial skin will follow fracture of bones
plate of the frontal bone result in hemorrhage beneath the
through which branches of the trigeminal nerve pass to
conjunctiva and into the orbital cavity, causing exophthal-
the skin.
mos. The frontal air sinus may be involved, with hemorrhage
The muscles of the face are thin and weak and cause lit-
into the nose.
tle displacement of the bone fragments. Once a fracture of
the maxilla has been reduced, for example, prolonged fixa-
Fractures of the Middle Cranial Fossa
tion is not needed. However, in the case of the mandible,
Fractures of the middle cranial fossa are common, because
the strong muscles of mastication can create considerable
this is the weakest part of the base of the skull. Anatomi-
displacement, requiring long periods of fixation.
cally, this weakness is caused by the presence of numerous
The most common facial fractures involve the nasal
foramina and canals in this region; the cavities of the mid-
bones, followed by the zygomatic bone and then the
dle ear and the sphenoidal air sinuses are particularly vul-
mandible. To fracture the maxillary bones and the supra-
nerable. The leakage of cerebrospinal fluid and blood from
orbital ridges of the frontal bones, an enormous force is
the external auditory meatus is common. The seventh and
required.
eighth cranial nerves may be involved as they pass through
Nasal Fractures
the petrous part of the temporal bone. The third, fourth,
and sixth cranial nerves may be damaged if the lateral wall
Fractures of the nasal bones, because of the prominence of
of the cavernous sinus is torn. Blood and cerebrospinal
the nose, are the most common facial fractures. Because the
fluid may leak into the sphenoidal air sinuses and then into
bones are lined with mucoperiosteum, the fracture is con-
the nose.
sidered open; the overlying skin may also be lacerated. Al-
though most are simple fractures and are reduced under
Fractures of the Posterior Cranial Fossa
local anesthesia, some are associated with severe injuries
In fractures of the posterior cranial fossa, blood may escape
to the nasal septum and require careful treatment under
into the nape of the neck deep to the postvertebral muscles.
general anesthesia.
Some days later, it tracks between the muscles and appears
Maxillofacial Fractures
in the posterior triangle, close to the mastoid process. The
mucous membrane of the roof of the nasopharynx may be
Maxillofacial fractures usually occur as the result of
torn, and blood may escape there. In fractures involving the
massive facial trauma. There is extensive facial swelling,
jugular foramen, the ninth, tenth, and eleventh cranial
midface mobility of the underlying bone on palpation,
nerves may be damaged. The strong bony walls of the hy-
malocclusion of the teeth with anterior open bite, and pos-
poglossal canal usually protect the hypoglossal nerve from
sibly leakage of cerebrospinal fluid (cerebrospinal rhinor-
injury.
rhea) secondary to fracture of the cribriform plate of the
ethmoid bone. Double vision (diplopia) may be present,
Bone Injuries of the Skull and Skeletal
owing to orbital wall damage. Involvement of the infraor-
Development
bital nerve with anesthesia or paresthesia of the skin of the
The developing bones of a child’s face are more pliable than
cheek and upper gum may occur in fractures of the body
an adult’s, and fractures may be incomplete or greenstick. In
of the maxilla. Nose bleeding may also occur in maxillary
adults, the presence of well-developed, air-filled sinuses and
fractures. Blood enters the maxillary air sinus and then
the mucoperiosteal surfaces of the alveolar parts of the up-
leaks into the nasal cavity.
per and lower jaws means that most facial fractures should
The sites of the fractures were classified by Le Fort
be considered to be open fractures, susceptible to infection
as type I, II, or III; these fractures are summarized in
and requiring antibiotic therapy.
CD Fig. 11-1.
Anatomy of Common Facial Fractures
Blowout Fractures of the Maxilla
Automobile accidents, fisticuffs, and falls are common
A severe blow to the orbit (as from a baseball) may cause the
causes of facial fractures. Fortunately, the upper part of the
contents of the orbital cavity to explode downward through
Bones and Cartilage
149
CD Figure 11-1
Le Fort classification of maxillofacial fractures. The red line denotes the
fracture line.
the floor of the orbit into the maxillary sinus. Damage to the
the ring, causing a single fracture or multiple fractures of
infraorbital nerve, resulting in altered sensation to the skin
the mandible, often far removed from the point of impact.
of the cheek, upper lip, and gum, may occur.
Fractures of the Zygoma
Vertebral Column
or Zygomatic Arch
Examination of the Back
The zygoma or zygomatic arch can be fractured by a blow
to the side of the face. Although it can occur as an isolated
It is important that the whole area of the back and legs be
fracture, as from a blow from a clenched fist, it may be asso-
examined and that the shoes be removed. Unequal length of
ciated with multiple other fractures of the face, as often seen
the legs or disease of the hip joints can lead to abnormal cur-
in automobile accidents.
vatures of the vertebral column. The patient should be
asked to walk up and down the examination room so that the
normal tilting movement of the pelvis can be observed. As
Mandible
one side of the pelvis is raised, a coronal lumbar convexity
develops on the opposite side, with a compensatory thoracic
Fractures of the Mandible
convexity on the same side. When a person assumes the
The mandible is horseshoe shaped and forms part of a
sitting position, it will be noted that the normal lumbar cur-
bony ring with the two temporomandibular joints and the
vature becomes flattened, with an increase in the interval
base of the skull. Traumatic impact is transmitted around
between the lumbar spines.
150
Chapter 11
Partial Fusion of the Sacral Vertebrae
The normal range of movement of the different parts of
the vertebral column should be tested. In the cervical re-
The first sacral vertebra can be partly or completely sepa-
gion, flexion, extension, lateral rotation, and lateral flexion
rated from the second sacral vertebra. Occasionally, on ra-
are possible. Remember that about half of the movement re-
diographs of the vertebral column, examples are seen in
ferred to as flexion is carried out at the atlantooccipital
which the fifth lumbar vertebra has fused with the first sacral
joints. In flexion, the patient should be able to touch his or
vertebra.
her chest with the chin, and in extension he or she should
be able to look directly upward. In lateral rotation the pa-
tient should be able to place the chin nearly in line with the
Fracture of the Sacrum in Trauma of
shoulder. Half of lateral rotation occurs between the atlas
the Pelvis
and the axis. In lateral flexion the head can normally be
Trauma to the true pelvis can result in fracture of the lateral
tilted 45° to each shoulder. It is important that the shoulder
mass of the sacrum.
is not raised when this movement is being tested.
In the thoracic region the movements are limited by the
Fractures of the Coccyx
presence of the ribs and sternum. When testing for rotation,
and Coccydynia
make sure that the patient does not rotate the pelvis.
In the lumbar region, flexion, extension, lateral rota-
Fractures of the coccyx are rare. However, coccydynia is
tion, and lateral flexion are possible. Flexion and extension
common and is usually caused by direct trauma to the
are fairly free. Lateral rotation, however, is limited by the
coccyx, as in falling down a flight of concrete steps. The
interlocking of the articular processes. Lateral flexion in
anterior surface of the coccyx can be palpated with a rectal
the thoracic and lumbar regions is tested by asking the pa-
examination.
tient to slide, in turn, each hand down the lateral side of
the thigh.
Thoracic Bones
Abnormal Curves of the
Clinical Importance of the Sternal
Vertebral Column
Angle (Angle of Louis)
Kyphosis is an exaggeration in the sagittal curvature present
When one is examining the chest from the front, the sternal
in the thoracic part of the vertebral column. It can be caused
angle (angle of Louis) is an important landmark. Its posi-
by muscular weakness or by structural changes in the verte-
tion can easily be felt and can often be seen by the presence
bral bodies or by intervertebral discs. In sickly adolescents,
of a transverse ridge. The finger moved to the right or to the
for example, where the muscle tone is poor, long hours of
left passes directly onto the second costal cartilage and then
study or work over a low desk can lead to a gently curved
the second rib. All other ribs can be counted from this point.
kyphosis of the upper thoracic region. The person is said to
The twelfth rib can usually be felt from behind, but in some
be “round-shouldered.” Crush fractures or tuberculous de-
obese persons this may prove difficult.
struction of the vertebral bodies leads to acute angular
kyphosis of the vertebral column. In the aged, osteoporosis
Sternum and Marrow Biopsy
(abnormal rarefaction of bone) and/or degeneration of the
intervertebral discs leads to senile kyphosis, involving the
Since the sternum possesses red hematopoietic marrow
cervical, thoracic, and lumbar regions of the column.
throughout life, it is a common site for marrow biopsy.
Lordosis is an exaggeration in the sagittal curvature pre-
Under a local anesthetic, a wide-bore needle is introduced
sent in the lumbar region. Lordosis may be caused by an
into the marrow cavity through the anterior surface of the
increase in the weight of the abdominal contents, as with
bone. The sternum may also be split at operation to allow
the gravid uterus or a large ovarian tumor, or it may be
the surgeon to gain easy access to the heart, great vessels,
caused by disease of the vertebral column such as spondy-
and thymus.
lolisthesis. The possibility that it is a postural compensation
for a kyphosis in the thoracic region or a disease of the hip
Cervical Rib
joint (congenital dislocation) must not be overlooked.
Scoliosis is a lateral deviation of the vertebral column.
A cervical rib (i.e., a rib arising from the anterior tubercle of
This is most commonly found in the thoracic region and
the transverse process of the seventh cervical vertebra) occurs
may be caused by muscular or vertebral defects. Paralysis of
in about 0.5% of humans (CD Fig. 11-2). It may have a free
muscles caused by poliomyelitis can cause severe scoliosis.
anterior end, may be connected to the first rib by a fibrous
The presence of a congenital hemivertebra can cause scol-
band, or may articulate with the first rib. The importance of
iosis. Often scoliosis is compensatory and may be caused by
a cervical rib is that it can cause pressure on the lower trunk
a short leg or hip disease.
of the brachial plexus in some patients, producing pain down
Bones and Cartilage
151
scalenus medius
brachial plexus
CD Figure 11-2
Thoracic outlet as
cervical rib
seen from above. Note the
presence of the cervical ribs (black)
on both sides. On the right side of
scalenus anterior
lower trunk of plexus
the thorax, the rib is almost
complete and articulates anteriorly
with the first rib. On the left side of
the thorax, the rib is rudimentary
but is continued forward as a
subclavian artery
fibrous band that is attached to the
first costal cartilage. Note that the
cervical rib
cervical rib may exert pressure on
fibrous band
the lower trunk of the brachial
plexus and may kink the subclavian
artery.
the medial side of the forearm and hand and wasting of the
pectoralis major. The medial end is tilted upward by the
small muscles of the hand. It can also exert pressure on the
sternocleidomastoid muscle.
overlying subclavian artery and interfere with the circulation
The close relationship of the supraclavicular nerves
of the upper limb.
to the clavicle may result in their involvement in callus for-
mation after fracture of the bone. This may be the cause of
Rib Excision
persistent pain over the side of the neck.
Rib excision is commonly performed by thoracic surgeons
Compression of the Brachial Plexus,
wishing to gain entrance to the thoracic cavity. A longitudi-
Subclavian Artery, and Subclavian Vein
nal incision is made through the periosteum on the outer
by the Clavicle
surface of the rib and a segment of the rib is removed. A sec-
ond longitudinal incision is then made through the bed of
The interval between the clavicle and the first rib in some
the rib, which is the inner covering of periosteum. After the
patients may become narrowed and thus is responsible for
operation, the rib regenerates from the osteogenetic layer of
compression of nerves and blood vessels.
the periosteum.
Fractures of the Scapula
Bones of the Upper Limb
Fractures of the scapula are usually the result of severe
trauma, such as occurs in run-over accident victims or in
Bones of the Shoulder Girdle
occupants of automobiles involved in crashes. Injuries
are usually associated with fractured ribs. Most fractures
Fractures of the Clavicle
of the scapula require little treatment because the muscles
on the anterior and posterior surfaces adequately splint the
The clavicle is a strut that holds the arm laterally so that it
fragments.
can move freely on the trunk. Unfortunately, because of its
position, it is exposed to trauma and transmits forces from
Dropped Shoulder and Winged Scapula
the upper limb to the trunk. It is the most commonly frac-
tured bone in the body. The fracture usually occurs as a re-
The position of the scapula on the posterior wall of the tho-
sult of a fall on the shoulder or outstretched hand. The force
rax is maintained by the tone and balance of the muscles at-
is transmitted along the clavicle, which breaks at its weakest
tached to it. If one of these muscles is paralyzed, the balance
point, the junction of the middle and outer thirds. After the
is upset, as in dropped shoulder, which occurs with paraly-
fracture, the lateral fragment is depressed by the weight
sis of the trapezius, or winged scapula (CD Fig. 11-3),
of the arm, and it is pulled medially and forward by the
caused by paralysis of the serratus anterior. Such imbalance
strong adductor muscles of the shoulder joint, especially the
can be detected by careful physical examination.
152
Chapter 11
Fractures of the Shaft of the Humerus
Fractures of the humeral shaft are common; displacement
of the fragments depends on the relation of the site of the
fracture to the insertion of the deltoid muscle (see CD Fig.
11-4). When the fracture line is proximal to the deltoid in-
sertion, the proximal fragment is adducted by the pectoralis
major, latissimus dorsi, and teres major muscles; the distal
fragment is pulled proximally by the deltoid, biceps, and tri-
ceps. When the fracture is distal to the deltoid insertion, the
proximal fragment is abducted by the deltoid, and the distal
fragment is pulled proximally by the biceps and triceps. The
radial nerve can be damaged where it lies in the spiral
groove on the posterior surface of the humerus under cover
of the triceps muscle.
CD Figure 11-3
Winging of the right scapula.
Fractures of the Distal End
of the Humerus
Bones of the Arm
Supracondylar fractures (see CD Fig. 11-4) are common in
children and occur when the child falls on the outstretched
Fractures of the Proximal End
hand with the elbow partially flexed. Injuries to the medial,
of the Humerus
radial, and ulnar nerves are not uncommon, although func-
tion usually quickly returns after reduction of the fracture.
Humeral Head Fractures
Damage to or pressure on the brachial artery can occur at
Fractures of the humeral head (CD Fig. 11-4) can occur
the time of the fracture or from swelling of the surrounding
during the process of anterior and posterior dislocations of
tissues; the circulation to the forearm may be interfered
the shoulder joint. The fibrocartilaginous glenoid labrum
with, leading to Volkmann’s ischemic contracture.
of the scapula produces the fracture, and the labrum can
The medial epicondyle (see CD Fig. 11-4) can be
become jammed in the defect, making reduction of the
avulsed by the medial collateral ligament of the elbow joint
shoulder joint difficult.
if the forearm is forcibly abducted. The ulnar nerve can be
injured at the time of the fracture, can become involved
Greater Tuberosity Fractures
later in the repair process of the fracture (in the callus), or
The greater tuberosity of the humerus can be fractured by di-
can undergo irritation on the irregular bony surface after the
rect trauma, displaced by the glenoid labrum during disloca-
bone fragments are reunited.
tion of the shoulder joint, or avulsed by violent contractions
of the supraspinatus muscle. The bone fragment will have the
Bones of the Forearm
attachments of the supraspinatus, teres minor, and infra-
spinatus muscles, whose tendons form part of the rotator cuff.
Fractures of the Radius and Ulna
When associated with a shoulder dislocation, severe tearing of
the cuff with the fracture can result in the greater tuberosity
Fractures of the head of the radius can occur from falls on
remaining displaced posteriorly after the shoulder joint has
the outstretched hand. As the force is transmitted along the
been reduced. In this situation, open reduction of the fracture
radius, the head of the radius is driven sharply against the ca-
is necessary to attach the rotator cuff back into place.
pitulum, splitting or splintering the head (see CD Fig. 11-4).
Fractures of the neck of the radius occur in young chil-
Lesser Tuberosity Fractures
dren from falls on the outstretched hand (see CD Fig. 11-4).
Occasionally, a lesser tuberosity fracture accompanies pos-
Fractures of the shafts of the radius and ulna may or
terior dislocation of the shoulder joint. The bone fragment
may not occur together (see CD Fig. 11-4). Displacement of
receives the insertion of the subscapularis tendon (see CD
the fragments is usually considerable and depends on the
Fig. 11-4), a part of the rotator cuff.
pull of the attached muscles. The proximal fragment of the
radius is supinated by the supinator and the biceps brachii
Surgical Neck Fractures
muscles (see CD Fig. 11-4). The distal fragment of the
The surgical neck of the humerus (see CD Fig. 11-4),
radius is pronated and pulled medially by the pronator
which lies immediately distal to the lesser tuberosity, can be
quadratus muscle. The strength of the brachioradialis and
fractured by a direct blow on the lateral aspect of the shoulder
extensor carpi radialis longus and brevis shortens and angu-
or in an indirect manner by falling on the outstretched hand.
lates the forearm. In fractures of the ulna, the ulna angulates
Bones and Cartilage
153
S
anatomical neck
head
greater tuberosity
SUB
surgical neck
D
PM
deltoid tuberosity
shaft of humerus
A
TR
olecranon process
trochlear notch
head
coronoid process
coronoid
radial fossa
fossa
bicipital tuberosity
lateral epicondyle
medial
epicondyle
capitulum
trochlea
shaft of ulna
CF
shaft
of radius
CD Figure 11-4
A. Common
fractures of the humerus.
B
B. Common fractures of the
radius and ulna. The
displacement of the bony
fragments on the site of the
head
fracture line and the pull of the
muscles. CF pull of common
flexure muscles, D deltoid,
styloid process
styloid process
PM pectoralis major,
S supraspinatus, SUB
subscapularis, and TR triceps.
posteriorly. To restore the normal movements of pronation
and an anterior dislocation of the radial head with rupture
and supination, the normal anatomic relationship of the ra-
of the anular ligament. In Galeazzi’s fracture, the proximal
dius, ulna, and interosseous membrane must be regained.
third of the radius is fractured and the distal end of the ulna
A fracture of one forearm bone may be associated with
is dislocated at the distal radioulnar joint.
a dislocation of the other bone. In Monteggia’s fracture, for
Fractures of the olecranon process can result from a
example, the shaft of the ulna is fractured by a force applied
fall on the flexed elbow or from a direct blow. Depending on
from behind. There is a bowing forward of the ulnar shaft
the location of the fracture line, the bony fragment may be
154
Chapter 11
displaced by the pull of the triceps muscle, which is inserted
The blood vessels to the scaphoid enter its proximal and
on the olecranon process (see CD Fig. 11-4). Avulsion frac-
distal ends, although the blood supply is occasionally con-
tures of part of the olecranon process can be produced by
fined to its distal end. If the latter occurs, a fracture de-
the pull of the triceps muscle. Good functional return after
prives the proximal fragment of its arterial supply, and this
any of these fractures depends on the accurate anatomic re-
fragment undergoes avascular necrosis. Deep tenderness
duction of the fragment.
in the anatomic snuffbox after a fall on the outstretched
Colles’ fracture is a fracture of the distal end of the
hand in a young adult makes one suspicious of a fractured
radius resulting from a fall on the outstretched hand. It com-
scaphoid.
monly occurs in patients older than 50 years. The force dri-
Dislocation of the lunate bone occasionally occurs in
ves the distal fragment posteriorly and superiorly, and the
young adults who fall on the outstretched hand in a way that
distal articular surface is inclined posteriorly (CD Fig. 11-5).
causes hyperextension of the wrist joint. Involvement of the
This posterior displacement produces a posterior bump,
median nerve is common.
sometimes referred to as the “dinner-fork deformity” be-
Fractures of the metacarpal bones can occur as a re-
cause the forearm and wrist resemble the shape of that eat-
sult of direct violence, such as the clenched fist striking a
ing utensil. Failure to restore the distal articular surface to its
hard object. The fracture always angulates dorsally. The
normal position will severely limit the range of flexion of the
“boxer’s fracture” commonly produces an oblique fracture
wrist joint.
of the neck of the fifth and sometimes the fourth metacarpal
Smith’s fracture is a fracture of the distal end of the
bones. The distal fragment is commonly displaced proxi-
radius and occurs from a fall on the back of the hand. It is
mally, thus shortening the finger posteriorly.
a reversed Colles’ fracture because the distal fragment is
Bennett’s fracture is a fracture of the base of the
displaced anteriorly (see CD Fig. 11-5).
metacarpal of the thumb caused when violence is applied
along the long axis of the thumb or the thumb is forcefully
Olecranon Bursitis
abducted. The fracture is oblique and enters the car-
pometacarpal joint of the thumb, causing joint instability.
A small subcutaneous bursa is present over the olecranon
Fractures of the phalanges are common and usually
process of the ulna, and repeated trauma often produces
follow direct injury.
chronic bursitis.
Bones of the Hand
Bones of the Lower Limb
Injuries to the Bones of the Hand
Bones of the Pelvic Girdle
Fracture of the scaphoid bone is common in young adults;
Clinical Concept: The Pelvis Is a
unless treated effectively, the fragments will not unite, and
Basin with Holes in Its Walls
permanent weakness and pain of the wrist will result, with
the subsequent development of osteoarthritis. The fracture
The walls of the pelvis are formed by bones and ligaments;
line usually goes through the narrowest part of the bone,
these are partly lined with muscles (obturator internus and
which because of its location is bathed in synovial fluid.
piriformis) covered with fascia and parietal peritoneum. On
A
CD Figure 11-5
Fractures of the distal end of the radius.
B
A. Colles’ fracture. B. Smith’s fracture.
Bones and Cartilage
155
the outside of the pelvis are the attachments of the gluteal
the baby’s head as it descends through the pelvis during
muscles and the obturator externus muscle. The greater part
childbirth (CD Figs. 11-6 and 11-7A).
of the bony pelvis is thus sandwiched between inner and
outer muscles.
Internal Pelvic Assessments
The basin has anterior, posterior, and lateral walls and
Internal pelvic assessments are made by vaginal examination
an inferior wall or floor formed by the important levator ani
during the later weeks of pregnancy, when the pelvic tis-
and coccygeus muscles and their covering fascia.
sues are softer and more yielding than in the newly pregnant
The basin has many holes: The posterior wall has holes
condition.
on the anterior surface of the sacrum, the anterior sacral
■ Pubic arch: Spread the fingers under the pubic arch and
foramina, for the passage of the anterior rami of the sacral
examine its shape. Is it broad or angular? The examiner’s
spinal nerves. The sacrotuberous and sacrospinous liga-
four fingers should be able to rest comfortably in the
ments convert the greater and lesser sciatic notches into the
angle below the symphysis.
greater and lesser sciatic foramina. The greater sciatic fora-
■ Lateral walls: Palpate the lateral walls and determine
men provides an exit from the true pelvis into the gluteal re-
whether they are concave, straight, or converging. The
gion for the sciatic nerve, the pudendal nerve, and the gluteal
prominence of the ischial spines and the position of the
nerves and vessels; the lesser sciatic foramen provides an en-
sacrospinous ligaments are noted.
trance into the perineum from the gluteal region for the pu-
■ Posterior wall: The sacrum is palpated to determine
dendal nerve and the internal pudendal vessels. (One can
whether it is straight or well curved. Finally, if the patient
make a further analogy here: For the wires to gain entrance
has relaxed the perineum sufficiently, an attempt is made
to the apartment below, without going through the floor,
to palpate the promontory of the sacrum. The second
they have to pierce the wall [greater sciatic foramen] to get
finger of the examining hand is placed on the promon-
outside the building and then return through a second hole
tory, and the index finger of the free hand, outside the
[lesser sciatic foramen]. In the case of the human body, the
vagina, is placed at the point on the examining hand
pudendal nerve and internal pudendal vessels are the wires
where it makes contact with the lower border of the sym-
and the levator ani and the coccygeus muscles are the floor.)
physis. The fingers are then withdrawn and the distance
The lateral pelvic wall has a large hole, the obturator
measured (CD Fig. 11-7B), providing the measurement
foramen, which is closed by the obturator membrane, ex-
of the diagonal conjugate, which is normally about 5 in.
cept for a small opening that permits the obturator nerve to
(13 cm). The anteroposterior diameter from the sacro-
leave the pelvis and enter the thigh.
coccygeal joint to the lower border of the symphysis is
then estimated.
Pelvic Measurements in Obstetrics
■ Ischial tuberosities: The distance between the ischial
The capacity and shape of the female pelvis are of funda-
tuberosities may be estimated by using the closed fist
mental importance in obstetrics. The female pelvis is well
(CD Fig. 11-7D). It measures about 4 in. (10 cm), but it
adapted for the process of childbirth. The pelvis is shallower
is difficult to measure exactly.
and the bones are smoother than in the male. The size of the
Needless to say, considerable clinical experience is re-
pelvic inlet is similar in the two sexes, but in the female, the
quired to be able to assess the shape and size of the pelvis by
cavity is larger and cylindrical and the pelvic outlet is wider
vaginal examination.
in both the anteroposterior and the transverse diameters.
Four terms relating to areas of the pelvis are commonly
used in clinical practice:
The Female Pelvis
■ The pelvic inlet or brim of the true pelvis (CD Fig. 11-
Deformities of the pelvis may be responsible for dystocia
6) is bounded anteriorly by the symphysis pubis, laterally
(difficult labor). A contracted pelvis may obstruct the nor-
by the iliopectineal lines, and posteriorly by the sacral
mal passage of the fetus. It may be indirectly responsible for
promontory.
dystocia by causing conditions such as malpresentation or
■ The pelvic outlet of the true pelvis (see CD Fig. 11-6) is
malposition of the fetus, premature rupture of the fetal
bounded in front by the pubic arch, laterally by the is-
membranes, and uterine inertia.
chial tuberosities, and posteriorly by the coccyx. The
The cause of pelvic deformities may be congenital
sacrotuberous ligaments also form part of the margin of
(rare) or acquired from disease, poor posture, or fractures
the outlet.
caused by injury. Pelvic deformities are more common in
■ The pelvic cavity is the space between the inlet and the
women who have grown up in a poor environment and are
outlet (see CD Fig. 11-6).
undernourished. It is probable that these women suffered in
■ The axis of the pelvis is an imaginary line joining
their youth from minor degrees of rickets.
the central points of the anteroposterior diameters from
In 1933, Caldwell and Moloy classified pelves into four
the inlet to the outlet and is the curved course taken by
groups: gynecoid, android, anthropoid, and platypelloid
156
Chapter 11
promontory
pelvic inlet
pelvic outlet
diagonal conjugate
axis of pelvis
Female
Male
pelvic inlet
pelvic outlet
pelvic cavity
CD Figure 11-6
Pelvic inlet, pelvic outlet, diagonal
conjugate, and axis of the pelvis. Some of the main
pubic arch
differences between the female and the male pelvis are
also shown.
(CD. Fig. 11-7C).The gynecoid type, present in about 41%
Fractures of the Pelvis
of women, is the typical female pelvis, which was previously
described.
Fractures of the False Pelvis
The android type, present in about 33% of white fe-
Fractures of the false pelvis caused by direct trauma occa-
males and 16% of black females, is the male or funnel-
sionally occur. The upper part of the ilium is seldom dis-
shaped pelvis with a contracted outlet.
placed because of the attachment of the iliacus muscle on
The anthropoid type, present in about 24% of white fe-
the inside and the gluteal muscles on the outside.
males and 41% of black females, is long, narrow, and oval
shaped.
Fractures of the True Pelvis
The platypelloid type, present in only about 2% of
The mechanism of fractures of the true pelvis can be better
women, is a wide pelvis flattened at the brim, with the
understood if the pelvis is regarded not only as a basin but
promontory of the sacrum pushed forward.
also as a rigid ring (see CD Fig. 11-8). The ring is made up
Bones and Cartilage
157
A
B
axis of birth canal
measuring the diagonal conjugate
gynecoid
android
C
anthropoid
platypelloid
D
measuring transverse diameter of pelvic outlet
CD Figure 11-7
A. Birth canal. Interrupted line indicates the axis of the canal.
B. Procedure used in measuring the diagonal conjugate. C. Different types of pelvic inlets,
according to Caldwell and Moloy. D. Estimation of the width of the pelvic outlet by means
of a closed fist.
of the pubic rami, the ischium, the acetabulum, the ilium,
unstable and displacement will occur, because the postver-
and the sacrum, joined by strong ligaments at the sacroiliac
tebral and abdominal muscles will shorten and elevate the
and symphyseal joints. If the ring breaks at any one point,
lateral part of the pelvis (see CD Fig. 11-8). The break in the
the fracture will be stable and no displacement will occur.
ring may occur not as the result of a fracture but as the result
However, if two breaks occur in the ring, the fracture will be
of disruption of the sacroiliac or symphyseal joints. Fracture
158
Chapter 11
A
B
anterior superior
iliac spine
CD Figure 11-8
A-C. Different types of
fractures of the pelvic basin. D. Avulsion
fractures of the pelvis. The sartorius
muscle is responsible for the avulsion of
anterior inferior
the anterior superior iliac spine; the
iliac spine
straight head of the rectus femoris muscle,
C
D
for the avulsion of the anterior inferior iliac
spine; and the hamstring muscles, for the
ischial tuberosity
avulsion of the ischial tuberosity.
of bone on either side of the joint is more common than dis-
fascial beneath the parietal peritoneum can be the source of
ruption of the joint.
a massive hemorrhage, which may be life threatening.
The forces responsible for the disruption of the bony
The male urethra is often damaged, especially in vertical
ring may be anteroposterior compression, lateral compres-
shear fractures that may disrupt the urogenital diaphragm.
sion, or shearing.
The bladder, which lies immediately behind the pubis in
A heavy fall on the greater trochanter of the femur
both sexes, is occasionally damaged by spicules of bone; a full
may drive the head of the femur through the floor of the
bladder is more likely to be injured than is an empty bladder.
acetabulum into the pelvic cavity.
The rectum lies within the concavity of the sacrum and
is protected and rarely damaged. Fractures of the sacrum or
Fractures of the Sacrum and Coccyx
ischial spine may be thrust into the pelvic cavity, tearing the
Fractures of the lateral mass of the sacrum may occur as part
rectum.
of a pelvic fracture. Fractures of the coccyx are rare.
Nerve injuries can follow sacral fractures; the laying
down of fibrous tissue around the anterior or posterior nerve
Minor Fractures of the Pelvis
roots or the branches of the sacral spinal nerves can result in
The anterior superior iliac spine may be pulled off by the
persistent pain.
forcible contraction of the sartorius muscle in athletes (see
Damage to the sciatic nerve may occur in fractures
CD Fig. 11-8). In a similar manner the anterior inferior il-
involving the boundaries of the greater sciatic notch. The
iac spine may be avulsed by the contraction of the rectus
peroneal part of the sciatic nerve is most often involved, re-
femoris muscle (origin of the straight head). The ischial
sulting in the inability of a conscious patient to dorsiflex the
tuberosity can be avulsed by the contraction of the ham-
ankle joint or failure of an unconscious patient to reflexly
string muscles. Healing may occur by fibrous union, possi-
plantar-flex (ankle jerk) the foot.
bly resulting in elongation of the muscle unit and some
reduction in muscular efficiency.
Bones of the Thigh
Anatomy of Complications of Pelvic Fractures
Tenderness of the Head of the Femur
Fractures of the true pelvis are commonly associated with
and Arthritis of the Hip Joint
injuries to the soft pelvic tissues.
If damaged, the thin pelvic veins—namely, the internal
The head of the femur—that is, that part that is not intraac-
iliac veins and their tributaries—that lie in the parietal pelvic
etabular—can be palpated on the anterior aspect of the thigh
Bones and Cartilage
159
just inferior to the inguinal ligament and just lateral to the
the leg is shortened (as measured from the anterior superior
pulsating femoral artery. Tenderness over the head of the fe-
iliac spine to the adductor tubercle or medial malleolus).
mur usually indicates the presence of arthritis of the hip joint.
The gluteus maximus, the piriformis, the obturator inter-
nus, the gemelli, and the quadratus femoris rotate the distal
Blood Supply to the Femoral Head
fragment laterally, as seen by the toes pointing laterally.
and Neck Fractures
Trochanteric fractures commonly occur in the young
and middle-aged as a result of direct trauma. The fracture
Anatomic knowledge of the blood supply to the femoral
head explains why avascular necrosis of the head can occur
after fractures of the neck of the femur. In the young, the
epiphysis of the head is supplied by a small branch of the ob-
turator artery, which passes to the head along the ligament
of the femoral head. The upper part of the neck of the femur
receives a profuse blood supply from the medial femoral cir-
cumflex artery (see text Fig. 12-25). These branches pierce
the capsule and ascend the neck deep to the synovial mem-
brane. As long as the epiphyseal cartilage remains, no
communication occurs between the two sources of blood.
type 1
type 2
In the adult, after the epiphyseal cartilage disappears, an
A
anastomosis between the two sources of blood supply is es-
tablished. Fractures of the femoral neck interfere with or
completely interrupt the blood supply from the root of the
femoral neck to the femoral head. The scant blood flow
along the small artery that accompanies the round ligament
may be insufficient to sustain the viability of the femoral
head, and ischemic necrosis gradually takes place.
type 3
type 4
The Neck of the Femur and Coxa Valga
and Coxa Vara
The neck of the femur is inclined at an angle with the shaft;
the angle is about 160° in the young child and about 125°
GM
in the adult. An increase in this angle is referred to as coxa
PI
RF
valga, and it occurs, for example, in cases of congenital dis-
OI
AM
location of the hip. In this condition, adduction of the hip
GE
HS
joint is limited. A decrease in this angle is referred to as coxa
QF
vara, and it occurs in fractures of the neck of the femur
and in slipping of the femoral epiphysis. In this condition,
B
abduction of the hip joint is limited. Shenton’s line is a use-
ful means of assessing the angle of the femoral neck on a
radiograph of the hip region (see text Fig. 11-66).
Fractures of the Femur
Fractures of the neck of the femur are common and are of
two types, subcapital and trochanteric. The subcapital frac-
ture occurs in the elderly and is usually produced by a mi-
nor trip or stumble. Subcapital femoral neck fractures are
particularly common in women after menopause. This gen-
der predisposition is because of a thinning of the cortical
CD Figure 11-9
A. Fractures of the neck of the femur.
and trabecular bone caused by estrogen deficiency. Avascu-
B. Displacement of the lower bone fragment caused by the
lar necrosis of the head is a common complication. If the
pull of the powerful muscles. Note in particular the outward
rotation of the leg so that the foot characteristically points
fragments are not impacted, considerable displacement oc-
laterally. GM gluteus maximus, AM adductor muscles,
curs. The strong muscles of the thigh (CD Fig. 11-9), in-
GE gemelli, HS hamstring muscles, OI obturator
cluding the rectus femoris, the adductor muscles, and the
internus, PI piriformis, QF quadratus femoris,
hamstring muscles, pull the distal fragment upward, so that
RF rectus femoris.
160
Chapter 11
line is extracapsular, and both fragments have a profuse
quadriceps, and laterally rotated by the adductors and the
blood supply. If the bone fragments are not impacted, the
weight of the foot (see CD Fig. 11-10).
pull of the strong muscles will produce shortening and
In fractures of the middle third of the shaft of the fe-
lateral rotation of the leg, as previously explained.
mur, the distal fragment is pulled upward by the hamstrings
Fractures of the shaft of the femur usually occur in
and the quadriceps (see CD Fig. 11-10), resulting in con-
young and healthy persons. In fractures of the upper third
siderable shortening. The distal fragment is also rotated
of the shaft of the femur, the proximal fragment is flexed by
backward by the pull of the two heads of the gastrocnemius
the iliopsoas; abducted by the gluteus medius and minimus;
(see CD Fig. 11-10).
and laterally rotated by the gluteus maximus, the piriformis,
In fractures of the distal third of the shaft of the femur,
the obturator internus, the gemelli, and the quadratus
the same displacement of the distal fragment occurs as seen
femoris (CD Fig. 11-10). The lower fragment is adducted by
in fractures of the middle third of the shaft. However, the
the adductor muscles, pulled upward by the hamstrings and
distal fragment is smaller and is rotated backward by the
GME
IP
GMI
GM
PI
OI
GE
AM
QF
GAST
AM
QDF
HAM
HAM
QDF
CD Figure 11-10
Fractures of the shaft
of the femur. A. Upper third of the
femoral shaft. Note the displacement
A
B
caused by the pull of the powerful
muscles. B. Middle third of the femoral
shaft. Note the posterior displacement of
the lower fragment caused by the
gastrocnemius muscle. C. Lower third of
the femoral shaft. Note the excessive
displacement of the lower fragment
popliteal
caused by the pull of the gastrocnemius
artery
muscle, threatening the integrity of the
popliteal artery. AM adductor muscles,
GAST gastrocnemius, GE gemelli,
GM gluteus maximus, GME gluteus
medius, GMI gluteus minimus,
HAM hamstrings, IP iliopsoas,
OI obturator internus, PI piriformis,
GAST
QDF quadriceps femoris,
C
QF quadratus femoris.
Bones and Cartilage
161
gastrocnemius muscle (see CD Fig. 11-10) to a greater
aged and elderly; they usually result from direct violence to
degree and may exert pressure on the popliteal artery and
the lateral side of the knee joint, as when a person is hit by
interfere with the blood flow through the leg and foot.
the bumper of an automobile. The tibial condyle may
From these accounts it is clear that knowledge of the
show a split fracture or be broken up, or the fracture line
different actions of the muscles of the leg is necessary to un-
may pass between both condyles in the region of the inter-
derstand the displacement of the fragments of a fractured
condylar eminence. As a result of forced abduction of the
femur. Considerable traction on the distal fragment is usu-
knee joint, the medial collateral ligament can also be torn
ally required to overcome the powerful muscles and restore
or ruptured.
the limb to its correct length before manipulation and oper-
Fractures of the distal end of the tibia are considered
ative therapy to bring the proximal and distal fragments into
with the ankle joint.
correct alignment.
Intraosseous Infusion of the Tibia
Patellar Dislocations
in the Infant
The patella is a sesamoid bone lying within the quadriceps
The technique may be used for the infusion of fluids and
tendon. The importance of the lower horizontal fibers of the
blood when it has been found impossible to obtain an intra-
vastus medialis and the large size of the lateral condyle of
venous line. The procedure is easy and rapid to perform, as
the femur in preventing lateral displacement of the patella
follows:
have been emphasized. Congenital recurrent dislocations
1. With the distal leg adequately supported, the anterior
of the patella are caused by underdevelopment of the lateral
subcutaneous surface of the tibia is palpated.
femoral condyle. Traumatic dislocation of the patella results
from direct trauma to the quadriceps attachments of
2. The skin is anesthetized about 1 in. (2.5 cm) distal to
the patella (especially the vastus medialis), with or without
the tibial tuberosity, thus blocking the infrapatellar
fracture of the patella.
branch of the saphenous nerve.
3. The bone marrow needle is directed at right angles
Patellar Fractures
through the skin, superficial fascia, deep fascia, and tib-
A patella fractured as a result of direct violence, as in an au-
ial periosteum and the cortex of the tibia. Once the nee-
tomobile accident, is broken into several small fragments.
dle tip reaches the medulla and bone marrow, the
Because the bone lies within the quadriceps femoris tendon,
operator senses a feeling of “give.” The position of the
little separation of the fragments takes place. The close rela-
needle in the marrow can be confirmed by aspiration.
tionship of the patella to the overlying skin may result in the
The needle should be directed slightly caudad to avoid
fracture being open. Fracture of the patella as a result of in-
injury to the epiphyseal plate of the proximal end of the
direct violence is caused by the sudden contraction of the
tibia. The transfusion may then commence.
quadriceps snapping the patella across the front of the
femoral condyles. The knee is in the semiflexed position, and
Bones of the Foot
the fracture line is transverse. Separation of the fragments
usually occurs.
Fractures of the Calcaneum
Compression fractures of the calcaneum result from falls
Bones of the Leg
from a height. The weight of the body drives the talus down-
ward into the calcaneum, crushing it in such a way that it
Fractures of the Tibia and Fibula
loses vertical height and becomes wider laterally. The pos-
Fractures of the tibia and fibula are common. If only one
terior portion of the calcaneum above the insertion of the
bone is fractured, the other acts as a splint and displacement
tendo calcaneus can be fractured by posterior displacement
is minimal. Fractures of the shaft of the tibia are often open
of the talus. The sustentaculum tali can be fractured by
because the entire length of the medial surface is covered
forced inversion of the foot.
only by skin and superficial fascia. Fractures of the distal
third of the shaft of the tibia are prone to delayed union or
Fractures of the Talus
nonunion. This can be because the nutrient artery is torn at
the fracture line, with a consequent reduction in blood flow
Fractures occur at the neck or body of the talus. Neck frac-
to the distal fragment; it is also possible that the splint-like
tures occur during violent dorsiflexion of the ankle joint
action of the intact fibula prevents the proximal and distal
when the neck is driven against the anterior edge of the dis-
fragments from coming into apposition.
tal end of the tibia. The body of the talus can be fractured by
Fractures of the proximal end of the tibia, at the tib-
jumping from a height, although the two malleoli prevent
ial condyles (tibial plateau), are common in the middle-
displacement of the fragments.
162
Chapter 11
Fractures of the Metatarsal Bones
Stress fracture of a metatarsal bone is common in jog-
gers and in soldiers after long marches; it can also occur in
The base of the fifth metatarsal can be fractured during
nurses and hikers. It occurs most frequently in the distal
forced inversion of the foot, at which time the tendon of in-
third of the second, third, or fourth metatarsal bone. Mini-
sertion of the peroneus brevis muscle pulls off the base of
mal displacement occurs because of the attachment of the
the metatarsal.
interosseous muscles.
Clinical Problem Solving Questions
Read the following case histories/questions and give
had received a blow on the head with an empty bottle.
the best answer for each.
On examination, the patient was conscious and had a
large dough-like swelling over the back of the head
A 19-year-old boy was suspected of having leukemia. It
that was restricted to the area over the occipital bone.
was decided to confirm the diagnosis by performing a
The skin was intact, and the swelling fluctuated on
bone marrow biopsy.
palpation.
1.
The following statements concerning this procedure
3.
The following statements concerning this patient are
are correct except which?
correct except which?
A. The biopsy was taken from the lower end of the
A. The hematoma, although large, did not extend for-
tibia.
ward to the orbital margins and did not extend later-
B. Red bone marrow specimens can be obtained from
ally as far as the temporal lines.
the sternum or the iliac crests.
B. The hematoma was located just beneath the scalp
C. At birth, the marrow of all bones of the body is red
and was superficial to the periosteum of the occipi-
and hematopoietic.
tal bone.
D. The blood-forming activity of bone marrow in many
C. The swelling did not occupy the subcutaneous tis-
long bones gradually lessens with age, and the red
sue of the scalp.
marrow is gradually replaced by yellow marrow.
D. The hematoma was restricted to one skull bone and
was situated beneath the periosteum.
A 45-year-old man with extensive maxillofacial injuries
after an automobile accident was brought to the emer-
A 45-year-old woman visited her physician because of a
gency department. Evaluation of the airway revealed
low back pain of 3 months’ duration. She was otherwise
partial obstruction. Despite an obvious fractured
very fit. On examination of her back, nothing abnormal
mandible, an attempt was made to move the tongue for-
was discovered. The physician then listened to her
ward from the posterior pharyngeal wall by pushing the
chest, examined her thyroid gland, and finally exam-
angles of the mandible forward. This maneuver failed to
ined both breasts. A large, hard mass was found in the
move the tongue, and it became necessary to hold the
left breast.
tongue forward directly to pull it away from the posterior
pharyngeal wall.
4.
The following facts supported the diagnosis of carci-
noma of the left breast with secondaries in the vertebral
2.
The most likely reason the physician was unable to pull
column except which?
the tongue forward in this patient is which?
A. The lump in the breast was painless and the pa-
A. The hypoglossal nerves were damaged on both sides
tient had noticed it while showering 6 months
of the neck.
previously.
B. Spasm of the styloglossus muscles
B. Several large, hard, pectoral lymph nodes were
C. The mandibular origin of the genioglossus muscles
found in the left axilla.
was floating because of bilateral fractures of the body
C. A lateral radiograph of the lumbar vertebral column
of the mandible.
showed extensive metastases in the bodies of the
D. The presence of a blood clot in the mouth
second and third lumbar vertebrae.
E. The resistance of the patient
D. The lump was situated in the upper outer quadrant
A 46-year-old man was seen in the emergency depart-
of the left breast and was fixed to surrounding
ment after being knocked down in a street brawl. He
tissues.
Bones and Cartilage
163
E. Although the cancer had spread by the lymph ves-
7.
The following statements concerning this case are
sels, no evidence of spread via the bloodstream was
correct except which?
present.
A. The clavicle is one of the most common bones in
the body to be fractured.
A 65-year-old man and a 10-year-old boy were involved
B. Anatomically, the weakest part of the clavicle is the
in a severe automobile accident. In both patients the
junction of the medial and middle thirds, and this is
thorax had been badly crushed. Radiographic examina-
where the fracture commonly occurs.
tion revealed that the man had five fractured ribs but
C. The lateral bony fragment is depressed downward by
the boy had no fractures.
the weight of the arm.
5.
What is the most likely explanation for this difference
D. The lateral fragment is pulled forward and medially
in medical findings?
by the pectoral muscles.
A. The patients were in different seats in the vehicle.
E. The medial fragment is elevated by the sternoclei-
B. The boy was wearing his seat belt and the man was
domastoid muscle.
not.
F. The supraclavicular nerves or a communicating
C. The chest wall of a child is very elastic, and fractures
vein between the cephalic and internal jugular vein
of ribs in children are rare.
may be damaged by the bone fragments.
D. The man anticipated the impact and tensed his
A 22-year-old medical student fell off her bicycle onto
muscles, including those of the shoulder girdle and
her outstretched hand. She thought she had sprained
abdomen.
her right wrist joint and treated herself by binding her
An 18-year-old woman was thrown from a horse while
wrist with an elastic bandage. Three weeks later, how-
attempting to jump a fence. She landed heavily on
ever, she was still experiencing pain on moving her
the ground, striking the lower part of her chest on
wrist and so decided to visit the emergency department.
the left side. On examination in the emergency de-
On examination of the dorsal surfaces of both hands,
partment she was conscious but breathless. The lower
with the fingers and thumbs fully extended, a localized
left side of her chest was badly bruised, and the ninth
tenderness could be felt in the anatomic snuffbox of her
and tenth ribs were extremely tender to touch. She
right hand. A diagnosis of fracture of the right scaphoid
had severe tachycardia, and her systolic blood pressure
bone was made.
was low.
8.
The following statements concerning this patient are
correct except which?
6.
The following statements are possibly correct except
A. The fracture line on the scaphoid bone may deprive
which?
the proximal fragment of its arterial supply.
A. There was evidence of tenderness and muscle spasm
B. A bony fragment deprived of its blood supply may
in the left upper quadrant of the anterior abdominal
undergo ischemic necrosis.
wall.
C. Because the scaphoid bone articulates with other
B. A posteroanterior radiograph of the chest revealed
bones, the fracture line may enter a joint cavity and
fractures of the left ninth and tenth ribs near their
become bathed in synovial fluid, which would in-
angles.
hibit repair.
C. The blunt trauma to the ribs could not result in
D. The scaphoid bone is an easy bone to immobilize
injury to the underlying spleen.
because of its small size.
D. The presence of blood in the peritoneal cavity had
E. Fractures of the scaphoid bone have a high incidence
irritated the parietal peritoneum, producing reflex
of nonunion.
spasm of the upper abdominal muscles.
E. The muscles of the anterior abdominal wall are
A heavily built, middle-aged man running down a flight
supplied by thoracic spinal nerves.
of stone steps misjudged the position of one of the steps
and fell suddenly onto his buttocks. Following the fall,
A 15-year-old girl, while demonstrating to her friends
he complained of severe bruising of the area of the cleft
her proficiency at standing on her hands, suddenly
between the buttocks and persistent pain in this area.
went off balance and put all her body weight on her left
outstretched hand. A distinctive cracking noise was
9.
The following statements concerning this patient are
heard, and she felt a sudden pain in her left shoulder re-
correct except which?
gion. On examination in the emergency department,
A. The lower end of the vertebral column was trauma-
the smooth contour of her left shoulder was absent. The
tized by the stone step.
clavicle was obviously fractured, and the edges of the
B. The coccyx can be palpated beneath the skin in the
bony fragments could be palpated.
natal cleft.
164
Chapter 11
C. The anterior surface of the coccyx cannot be felt
13.
Fracture of the neck of the femur in the adult com-
clinically.
monly results in avascular necrosis of part of the
D. The coccyx is usually severely bruised or fractured.
femoral head. Can you explain this on anatomic
E. The pain is felt in the distribution of dermatomes S4
grounds? Trochanteric fractures are never accompa-
and S5.
nied by avascular necrosis. Why?
An elderly woman was run over by an automobile as she
A 37-year-old woman was involved in a light plane
was crossing the road. Radiographic examination of the
accident. She and her husband were flying home from
pelvis in the emergency department of the local hospi-
a business trip when they had to make a forced land-
tal revealed a fracture of the ilium and iliac crest on the
ing in a field due to fog. On landing, the plane hit
left side.
a tree and came to rest on its nose. Her husband
was killed on impact and she was thrown from the
10.
The following statements about fractures of the pelvis
cockpit. She was evaluated in the emergency depart-
are correct except which?
ment with multiple injuries. Radiographic examina-
A. Fractures of the ilium have little displacement.
tion of her pelvis showed a fracture of her left ilium
B. Displacement is prevented by the presence of the il-
and iliac crest.
iacus and the gluteal muscles on the inner and outer
surfaces of this bone, respectively.
14.
From your knowledge of anatomy, would you expect
C. If two fractures occur in the ring forming the true
much displacement of the bony fragments?
pelvis, the fracture will be unstable and displace-
A 25-year-old man was running across a field when
ment will occur.
he caught his right foot in a rabbit hole. As he fell,
D. Fractures of the true pelvis do not cause injury to the
the right foot was violently rotated laterally and
pelvic viscera.
overeverted. On attempting to stand, he could place
E. The postvertebral and abdominal muscles are re-
no weight on his right foot. On examination by a
sponsible for elevating the lateral part of the pelvis
physician, the right ankle was considerably swollen,
should two fractures occur.
especially on the lateral side. After further exami-
F. A heavy fall on the greater trochanter of the femur
nation, including a radiograph of the ankle, a diag-
may drive the head of the femur through the floor of
nosis of severe fracture dislocation of the ankle joint
the acetabulum and into the pelvic cavity.
was made.
A pregnant woman visited an antenatal clinic. A vaginal
examination revealed that the sacral promontory could
15.
The following statements concerning this patient are
be easily palpated and that the diagonal conjugate
correct except which?
measured less than 4 in. (10 cm).
A. This type of fracture dislocation is caused by forced
external rotation and overeversion of the foot.
11.
The following statements concerning this examination
B. The talus is externally rotated against the lateral
are correct except which?
malleolus of the fibula, causing it to fracture.
A. Normally it is difficult or impossible to feel the
C. The torsion effect on the lateral malleolus produces
sacral promontory by means of a vaginal examina-
a spiral fracture.
tion.
D. The medial ligament of the ankle joint is strong and
B. The normal diagonal conjugate measures about 10
never ruptures.
in. (25 cm).
E. If the talus is forced to move farther laterally and
C. This patient’s pelvis was flattened anteroposteriorly,
continues to rotate, the posterior inferior margin of
and the sacral promontory projected too far forward.
the tibia will be sheared off.
D. It is likely that this patient would have an obstructed
labor.
16.
A 32-year-old woman was rock climbing when she de-
E. This patient was advised to have a cesarean section.
cided to jump from a ledge down to a flat rock some five
feet below. On landing she maintained her balance but
On a routine anteroposterior radiographic examination
experienced a severe pain in her right foot in the region
of a patient’s right hip joint, the long axis of the neck of
of the heel. On examination later in the emergency de-
the femur was found to be at an angle of 160° with the
partment of the local hospital, the physician’s assistant
long axis of the femoral shaft.
noted the extreme tenderness felt over the sides and in-
12.
Is this angle normal in a 5-year-old child? In a 35-year-
ferior surface of the right calcaneum. She also noted
old man? What is the clinical condition called in which
that the right calcaneum appeared wider than the one
the angle is smaller than normal? Which movement of
on the left. Using your knowledge of anatomy, make the
the hip joint is limited by this condition?
diagnosis.
Bones and Cartilage
165
Answers and Explanations
1.
A is the correct answer. In a 19-year-old boy, the bone
12.
This angle is within normal limits in a 5-year-old child.
marrow at the lower end of the tibia is yellow.
It is too great in a 35-year-old man; the condition is
called coxa valga, in which adduction of the hip joint is
2.
C is the correct answer. The genioglossus muscle arises
limited. When the angle of the femoral neck is smaller
from the superior mental spines behind the symphysis
than normal (coxa vara), abduction of the hip joint is
menti of the mandible (see text Fig. 11-10).
limited.
3.
B is the correct answer. The hematoma was located
13.
Fractures of the neck of the femur in the adult com-
deep to the periosteum of the occipital bone.
monly result in avascular necrosis of part of the femoral
4.
E is the correct answer. The carcinoma of the left breast
head. The femoral head receives its blood supply from
was in an advanced stage and had spread by way of the
two sources—a small artery, a branch of the obturator
lymph vessels to the axillary lymph nodes and by the
artery, that runs with the round ligament of the femoral
bloodstream to the bodies of the second and third lum-
head and a profuse blood supply from the medial
bar vertebrae. Carcinoma of the thyroid, bronchus,
femoral circumflex femoral artery, branches that as-
breast, kidney, and prostate tend to metastasize via the
cend the femoral neck beneath the synovial membrane.
bloodstream to bones.
Fracture of the femoral neck may deprive the femoral
head of part or all of the blood from the medial femoral
5.
C is the correct answer. The chest wall of a child is very
circumflex femoral artery, and avascular necrosis will
elastic, and fractures of ribs in children are rare.
occur. In trochanteric fractures, both fragments have a
6.
C is the correct answer. Trauma to the lower part of the
profuse blood supply.
woman’s left chest could easily severely damage the
14.
Most fractures of the upper part of the ilium have little
spleen in the abdomen, resulting in hemorrhage into
displacement of the bone fragments. This is because
the peritoneal cavity.
the iliacus muscle is attached to the inner surface and
7.
B is the correct answer. Anatomically, the weakest part of
the gluteal muscles are attached to the outer surface
the clavicle is the junction of the middle and lateral thirds,
(see text Fig. 11-54). Splinting the bones is unnecessary
and that is where the fracture occurred in this patient.
because of the attachment of these muscles.
8.
D is the correct answer. The scaphoid bone is a difficult
15.
D is the correct answer. Although the medial ligament
bone to immobilize because of its position and small
of the ankle joint is strong, extreme force can result in
size.
rupture of the ligament, or the ligament can be torn
from the medial malleolus, or the pull on the ligament
9.
C is the correct answer. The anterior surface of the coc-
can fracture the medial malleolus.
cyx can be palpated with a gloved finger placed in the
anal canal.
16.
This woman had suffered a compression fracture
of the right calcaneum as a result of the fall from a
10.
D is the correct answer. Fractures of the true pelvis are
height. The weight of the body drives the talus down-
commonly associated with injuries to the soft pelvic vis-
ward into the calcaneum, crushing it in such a way that
cera, especially the bladder and the urethra.
it loses vertical height and becomes wider laterally. The
11.
B is the correct answer. The normal diagonal conjugate
diagnosis was confirmed on an anteroposterior and a
measures about 5 in. (11.5 cm) (see CD Fig. 11-6).
lateral radiograph of the right ankle.
Chapter Outline
General Clinical Features Concerning
Radioulnar Joint
174
Radioulnar Joint Disease
174
Joints
169
Wrist Joint
174
Examination of Joints
169
Wrist Joint Injuries
174
Dislocation of Joints
169
Falls on the Outstretched Hand
174
Presence of Cartilaginous Discs within Joints
169
Joints of the Pelvis
174
Loss of Joint Innervation
169
Changes in the Pelvic Joints with Pregnancy
174
Value of Joint Classification
169
Changes in the Pelvic Joints with Age
174
Joint Pain and Joint Innervation
169
Sacroiliac Joint Disease
175
Temporomandibular Joint
169
Joints of the Lower Limb
175
Clinical Significance of the Temporomandibular
Hip Joint
175
Joint
169
Referred Pain from the Hip Joint
175
Dislocation of the Temporomandibular Joint
169
Congenital Dislocation of the Hip
175
Traumatic Dislocation of the Hip
175
Joints of the Vertebral Column
170
Hip Joint Stability and Trendelenburg’s Sign
175
Abnormal Curves of the Vertebral Column
170
Arthritis of the Hip Joint
175
Dislocations of the Vertebral Column
170
Knee Joint
175
Fractures of the Vertebral Column
170
Strength of the Knee Joint
175
Fractures of the Spinous Processes,
Knee Injury and the Synovial Membrane
176
Transverse Processes, or Laminae
170
Ligamentous Injury of the Knee Joint
176
Anterior and Lateral Compression Fractures
170
Medial Collateral Ligament
176
Fracture Dislocations
170
Lateral Collateral Ligament
176
Vertical Compression Fractures
170
Cruciate Ligaments
176
Fractures of the Odontoid Process of the Axis
172
Meniscal Injury of the Knee Joint
178
Fractures of the Pedicles of the Axis
Pneumoarthrography of the Knee Joint
178
(Hangman’s Fracture)
172
Arthroscopy of the Knee Joint
179
Spondylolisthesis
172
Ankle Joint
179
Ankle Joint Stability
179
Joints of the Upper Limb
172
Acute Sprains of the “Lateral Ankle”
179
Sternoclavicular Joint
172
Acute Sprains of the “Medial Ankle”
179
Sternoclavicular Joint Injuries
172
Fracture Dislocations of the Ankle Joint
179
Acromioclavicular Joint
172
Joints of the Foot
179
Acromioclavicular Joint Injuries
172
Metatarsophalangeal Joint of the Big Toe
179
Acromioclavicular Joint Dislocation
172
Clinical Examination of the Arches of the Foot
179
Shoulder Joint
173
The “Stone Bridge” Mechanisms for Arch
Stability of the Shoulder Joint
173
Support
179
Dislocations of the Shoulder Joint
173
Maintenance of the Medial Longitudinal Arch
181
Anterior-Inferior Dislocations
173
Maintenance of the Lateral Longitudinal Arch
181
Posterior Dislocations
173
Maintenance of the Transverse Arch
181
Shoulder Pain
173
Physiologic Note: Muscle Tone and the
Elbow Joint
173
Arches of the Foot
181
Stability of the Elbow Joint
173
Clinical Problems Associated with the Arches
Dislocations of the Elbow Joint
173
of the Foot
181
Arthrocentesis of the Elbow Joint
173
Damage to the Ulnar Nerve with Elbow Joint
Clinical Problem Solving Questions
182
Injuries
173
Radiology of the Elbow Region after Injury
174
Answers and Explanations
185
Joints
169
such as the ankle, elbow, or wrist, whereas tuberculous
GENERAL CLINICAL
arthritis also affects synovial joints and may start in the syn-
ovial membrane or in the bone.
FEATURES
Joint Pain and Joint Innervation
CONCERNING
Remember that more than one joint may receive the same
nerve supply. For example, the hip and knee joints are
JOINTS
both supplied by the obturator nerve. Thus, a patient with
disease limited to one of these joints may experience pain
in both.
Examination of Joints
When examining a patient, the clinician should assess the
normal range of movement of all joints. When the bones
of a joint are no longer in their normal anatomic relation-
TEMPOROMANDIB-
ship with one another, then the joint is said to be
dislocated.
ULAR JOINT
Dislocation of Joints
Clinical Significance of the
Some joints are particularly susceptible to dislocation be-
cause of lack of support by ligaments, the poor shape of the
Temporomandibular Joint
articular surfaces, or the absence of adequate muscular sup-
port. The shoulder joint, temporomandibular joint, and
The temporomandibular joint lies immediately in front of
acromioclavicular joints are good examples. Dislocation of
the external auditory meatus. The great strength of the lat-
the hip is usually congenital, being caused by inadequate
eral temporomandibular ligament prevents the head of the
development of the socket that normally holds the head of
mandible from passing backward and fracturing the tym-
the femur firmly in position.
panic plate when a severe blow falls on the chin.
The articular disc of the temporomandibular joint may
become partially detached from the capsule, and this results
Presence of Cartilaginous Discs
in its movement becoming noisy and producing an audible
click during movements at the joint.
within Joints
The presence of cartilaginous discs within joints, especially
weightbearing joints, as in the case of the knee, makes
Dislocation of the
them particularly susceptible to injury in sports. During a
rapid movement the disc loses its normal relationship to
Temporomandibular Joint
the bones and becomes crushed between the weightbear-
Dislocation sometimes occurs when the mandible is de-
ing surfaces.
pressed. In this movement, the head of the mandible and
the articular disc both move forward until they reach the
summit of the articular tubercle. In this position, the
Loss of Joint Innervation
joint is unstable, and a minor blow on the chin or a sud-
In certain diseases of the nervous system (e.g., syringomyelia),
den contraction of the lateral pterygoid muscles, as in
the sensation of pain in a joint is lost. This means that the warn-
yawning, may be sufficient to pull the disc forward be-
ing sensations of pain felt when a joint moves beyond the nor-
yond the summit. In bilateral cases the mouth is fixed in
mal range of movement are not experienced. This phenome-
an open position, and both heads of the mandible lie in
non results in the destruction of the joint.
front of the articular tubercles. Reduction of the disloca-
tion is easily achieved by pressing the gloved thumbs
downward on the lower molar teeth and pushing the jaw
Value of Joint Classification
backward. The downward pressure overcomes the tension
Knowledge of the classification of joints is of great value be-
of the temporalis and masseter muscles, and the back-
cause, for example, certain diseases affect only certain types
ward pressure overcomes the spasm of the lateral ptery-
of joints. Gonococcal arthritis affects large synovial joints
goid muscles.
170
Chapter 12
greatest. In unilateral dislocations the inferior articular process
JOINTS OF THE
of one vertebra is forced forward over the anterior margin of
the superior articular process of the vertebra below. Because
the articular processes normally overlap, they become locked
VERTEBRAL
in the dislocated position. The spinal nerve on the same side
is usually nipped in the intervertebral foramen, producing se-
COLUMN
vere pain. Fortunately, the large size of the vertebral canal al-
lows the spinal cord to escape damage in most cases.
Bilateral cervical dislocations are almost always associ-
Abnormal Curves of the Vertebral
ated with severe injury to the spinal cord. Death occurs im-
mediately if the upper cervical vertebrae are involved be-
Column
cause the respiratory muscles, including the diaphragm
(phrenic nerves C3 to C5), are paralyzed.
Kyphosis is an exaggeration in the sagittal curvature pre-
sent in the thoracic part of the vertebral column. It can be
caused by muscular weakness, by structural changes in the
Fractures of the Vertebral Column
vertebral bodies, or by intervertebral discs. In sickly adoles-
cents, for example, where the muscle tone is poor, long
Fractures of the Spinous Processes,
hours of study or work over a low desk can lead to a gently
Transverse Processes, or Laminae
curved kyphosis of the upper thoracic region. The person
Fractures of the spinous processes, transverse processes, or
is said to be “round-shouldered.” Crush fractures or tuber-
laminae are caused by direct injury or, in rare cases, by se-
culous destruction of the vertebral bodies leads to acute an-
vere muscular activity.
gular kyphosis of the vertebral column. In the aged, osteo-
porosis (abnormal rarefaction of bone) and/or degenera-
Anterior and Lateral Compression
tion of the intervertebral discs leads to senile kyphosis,
Fractures
involving the cervical, thoracic, and lumbar regions of the
column.
Anterior compression fractures of the vertebral bodies are
Lordosis is an exaggeration in the sagittal curvature pre-
usually caused by an excessive flexion compression type of
sent in the lumbar region. Lordosis may be caused by an in-
injury and take place at the sites of maximum mobility or at
crease in the weight of the abdominal contents, as with the
the junction of the mobile and fixed regions of the column.
gravid uterus or a large ovarian tumor, or it may be caused
It is interesting to note that the body of a vertebra in such a
by disease of the vertebral column such as spondylolisthesis.
fracture is crushed, whereas the strong posterior longitudi-
The possibility that it is a postural compensation for a kypho-
nal ligament remains intact. The vertebral arches remain
sis in the thoracic region or a disease of the hip joint (con-
unbroken and the intervertebral ligaments remain intact so
genital dislocation) must not be overlooked.
that vertebral displacement and spinal cord injury do not
Scoliosis is a lateral deviation of the vertebral column.
occur. When injury causes excessive lateral flexion in ad-
This is most commonly found in the thoracic region and
dition to excessive flexion, the lateral part of the body is also
may be caused by muscular or vertebral defects. Paralysis of
crushed.
muscles caused by poliomyelitis can cause severe scoliosis.
The presence of a congenital hemivertebra can cause scol-
Fracture Dislocations
iosis. Often scoliosis is compensatory and may be caused by
a short leg or hip disease.
Fracture dislocations are usually caused by a combination of
a flexion and rotation type of injury; the upper vertebra is ex-
cessively flexed and twisted on the lower vertebra. Here
Dislocations of the Vertebral
again, the site is usually where maximum mobility occurs,
as in the lumbar region, or at the junction of the mobile and
Column
fixed region of the column, as in the lower lumbar verte-
brae. Because the articular processes are fractured and the
Dislocations without fracture occur only in the cervical re-
ligaments are torn, the vertebrae involved are unstable, and
gion because the inclination of the articular processes of the
the spinal cord is usually severely damaged or severed, with
cervical vertebrae permits dislocation to take place without
accompanying paraplegia.
fracture of the processes. In the thoracic and lumbar re-
gions, dislocations can occur only if the vertically placed ar-
Vertical Compression Fractures
ticular processes are fractured.
Dislocations commonly occur between the fourth and
Vertical compression fractures occur in the cervical and
fifth or fifth and sixth cervical vertebrae, where mobility is
lumbar regions, where it is possible to fully straighten the
Joints
171
site of
site of
destruction
nipping
of spinal cord
of spinal nerve
A
B
C
waist fracture
anterior arch
of odontoid process
of atlas
transverse ligament
odontoid process
base fracture
of atlas
of atlas
of odontoid process
fracture
of pedicle
D
E
posterior arch
of atlas
CD Figure 12-1
Dislocations and fractures of the vertebral column. A. Unilateral disloca-
tion of the fifth or the sixth cervical vertebra. Note the forward displacement of the inferior
articular process over the superior articular process of the vertebra below. B. Bilateral dis-
location of the fifth on the sixth cervical vertebra. Note that 50% of the vertebral body
width has moved forward on the vertebra below. C. Flexion compression-type fracture of
the vertebral body in the lumbar region. D. Jefferson’s-type fracture of the atlas. E. Frac-
tures of the odontoid process and the pedicles (hangman’s fracture) of the axis.
172
Chapter 12
vertebral column (CD Fig. 12-1). In the cervical region,
with the neck straight, an excessive vertical force applied
JOINTS OF THE
from above will cause the ring of the atlas to be disrupted
and the lateral masses to be displaced laterally (Jefferson’s
UPPER LIMB
fracture). If the neck is slightly flexed, the lower cervical ver-
tebrae remain in a straight line and the compression load is
transmitted to the lower vertebrae, causing disruption of the
Sternoclavicular Joint
intervertebral disc and breakup of the vertebral body. Pieces
Sternoclavicular Joint Injuries
of the vertebral body are commonly forced back into the
spinal cord.
The strong costoclavicular ligament firmly holds the medial
It is possible for nontraumatic compression fractures to
end of the clavicle to the first costal cartilage. Violent forces
occur in severe cases of osteoporosis and for pathologic frac-
directed along the long axis of the clavicle usually result in
tures to take place.
fracture of that bone, but dislocation of the sternoclavicular
In the straightened lumbar region, an excessive force
joint takes place occasionally.
from below can cause the vertebral body to break up, with
Anterior dislocation results in the medial end of
protrusion of fragments posteriorly into the spinal canal.
the clavicle projecting forward beneath the skin; it
Fractures of the Odontoid Process of
may also be pulled upward by the sternocleidomastoid
muscle.
the Axis
Posterior dislocation usually follows direct trauma ap-
Fractures of the odontoid process are relatively common
plied to the front of the joint that drives the clavicle back-
and result from falls or blows on the head (see CD Fig. 12-
ward. This type is the more serious because the displaced
1). Excessive mobility of the odontoid fragment or rupture
clavicle may press on the trachea, esophagus, and major
of the transverse ligament can result in compression injury
blood vessels in the root of the neck.
to the spinal cord.
If the costoclavicular ligament ruptures completely, it is
difficult to maintain the normal position of the clavicle once
Fracture of the Pedicles of the Axis
reduction has been accomplished.
(Hangman’s Fracture)
Severe extension injury of the neck, such as might occur in
Acromioclavicular Joint
an automobile accident or a fall, is the usual cause of hang-
man’s fracture. Sudden overextension of the neck, as pro-
Acromioclavicular Joint Injuries
duced by the knot of a hangman’s rope beneath the chin, is
the reason for the common name. Because the vertebral
The plane of the articular surfaces of the acromioclavicular
canal is enlarged by the forward displacement of the verte-
joint passes downward and medially so that there is a ten-
bral body of the axis, the spinal cord is rarely compressed (see
dency for the lateral end of the clavicle to ride up over the
CD Fig. 12-1).
upper surface of the acromion. The strength of the joint de-
pends on the strong coracoclavicular ligament, which binds
the coracoid process to the undersurface of the lateral part
Spondylolisthesis
of the clavicle. The greater part of the weight of the upper
In spondylolisthesis, the body of a lower lumbar vertebra,
limb is transmitted to the clavicle through this ligament,
usually the fifth, moves forward on the body of the vertebra
and rotary movements of the scapula occur at this important
below and carries with it the whole of the upper portion of
ligament.
the vertebral column. The essential defect is in the pedicles
of the migrating vertebra. It is now generally believed that, in
Acromioclavicular Joint Dislocation
this condition, the pedicles are abnormally formed and
accessory centers of ossification are present and fail to unite.
A severe blow on the point of the shoulder, as is incurred
The spine, laminae, and inferior articular processes remain
during blocking or tackling in football or any severe fall,
in position, whereas the remainder of the vertebra, having
can result in the acromion being thrust beneath the lateral
lost the restraining influence of the inferior articular
end of the clavicle, tearing the coracoclavicular ligament.
processes, slips forward. Because the laminae are left behind,
This condition is known as shoulder separation. The dis-
the vertebral canal is not narrowed, but the nerve roots may
placed outer end of the clavicle is easily palpable. As in the
be pressed on, causing low backache and sciatica. In severe
case of the sternoclavicular joint, the dislocation is easily
cases the trunk becomes shortened, and the lower ribs con-
reduced, but withdrawal of support results in immediate re-
tact the iliac crest.
dislocation.
Joints
173
Injury to the shoulder joint is followed by pain, limita-
Shoulder Joint
tion of movement, and muscle atrophy owing to disuse. It is
important to appreciate that pain in the shoulder region can
Stability of the Shoulder Joint
be caused by disease elsewhere and that the shoulder joint
The shallowness of the glenoid fossa of the scapula and the
may be normal; for example, diseases of the spinal cord and
lack of support provided by weak ligaments make this joint
vertebral column and the pressure of a cervical rib can cause
an unstable structure. Its strength almost entirely depends
shoulder pain. Irritation of the diaphragmatic pleura or peri-
on the tone of the short muscles that bind the upper end of
toneum can produce referred pain via the phrenic and
the humerus to the scapula—namely, the subscapularis in
supraclavicular nerves.
front, the supraspinatus above, and the infraspinatus and
teres minor behind. The tendons of these muscles are fused
Elbow Joint
to the underlying capsule of the shoulder joint. Together,
these tendons form the rotator cuff.
Stability of the Elbow Joint
The least supported part of the joint lies in the inferior
The elbow joint is stable because of the wrench-shaped ar-
location, where it is unprotected by muscles.
ticular surface of the olecranon and the pulley-shaped
trochlea of the humerus; it also has strong medial and lateral
Dislocations of the Shoulder Joint
ligaments. When examining the elbow joint, the physician
The shoulder joint is the most commonly dislocated large
must remember the normal relations of the bony points. In
joint.
extension, the medial and lateral epicondyles and the top of
the olecranon process are in a straight line; in flexion, the
Anterior-Inferior Dislocations
bony points form the boundaries of an equilateral triangle.
Sudden violence applied to the humerus with the joint fully
Dislocations of the Elbow Joint
abducted tilts the humeral head downward onto the inferior
weak part of the capsule, which tears, and the humeral head
Elbow dislocations are common, and most are posterior. Pos-
comes to lie inferior to the glenoid fossa. During this move-
terior dislocation usually follows falling on the outstretched
ment, the acromion has acted as a fulcrum. The strong flex-
hand. Posterior dislocations of the joint are common in chil-
ors and adductors of the shoulder joint now usually pull the
dren because the parts of the bones that stabilize the joint are
humeral head forward and upward into the subcoracoid po-
incompletely developed. Avulsion of the epiphysis of the me-
sition.
dial epicondyle is also common in childhood because then
the medial ligament is much stronger than the bond of union
Posterior Dislocations
between the epiphysis and the diaphysis.
Posterior dislocations are rare and are usually caused by
Arthrocentesis of the Elbow Joint
direct violence to the front of the joint.
On inspection of the patient with shoulder disloca-
The anterior and posterior walls of the capsule are weak, and
tion, the rounded appearance of the shoulder is seen to be
when the joint is distended with fluid, the posterior aspect of
lost because the greater tuberosity of the humerus is no
the joint becomes swollen. Aspiration of joint fluid can eas-
longer bulging laterally beneath the deltoid muscle. A sub-
ily be performed through the back of the joint on either side
glenoid displacement of the head of the humerus into the
of the olecranon process.
quadrangular space can cause damage to the axillary
Damage to the Ulnar Nerve with
nerve, as indicated by paralysis of the deltoid muscle and
loss of skin sensation over the lower half of the deltoid.
Elbow Joint Injuries
Downward displacement of the humerus can also stretch
The close relationship of the ulnar nerve to the medial side
and damage the radial nerve.
of the joint often results in its becoming damaged in dislo-
cations of the joint or in fracture dislocations in this re-
Shoulder Pain
gion. The nerve lesion can occur at the time of injury or
The synovial membrane, capsule, and ligaments of the
weeks, months, or years later. The nerve can be involved in
shoulder joint are innervated by the axillary nerve and the
scar tissue formation or can become stretched owing to lat-
suprascapular nerve. The joint is sensitive to pain, pressure,
eral deviation of the forearm in a badly reduced supra-
excessive traction, and distension. The muscles surrounding
condylar fracture of the humerus. During movements of
the joint undergo reflex spasm in response to pain originat-
the elbow joint, the continued friction between the medial
ing in the joint, which in turn serves to immobilize the joint
epicondyle and the stretched ulnar nerve eventually results
and thus reduce the pain.
in ulnar palsy.
174
Chapter 12
Radiology of the Elbow Region after
Injury
In examining lateral radiographs of the elbow region, it is
important to remember that the lower end of the humerus
is normally angulated forward 45° on the shaft; when exam-
ining a patient, the physician should see that the medial epi-
condyle, in the anatomic position, is directed medially and
A
posteriorly and faces in the same direction as the head of the
humerus.
Radioulnar Joint
Radioulnar Joint Disease
B
The proximal radioulnar joint communicates with the el-
bow joint, whereas the distal radioulnar joint does not com-
CD Figure 12-2
Fractures of the distal end of the radius.
A. Colles’ fracture. B. Smith’s fracture.
municate with the wrist joint. In practical terms, this means
that infection of the elbow joint invariably involves the prox-
imal radioulnar joint. The strength of the proximal radioul-
nar joint depends on the integrity of the strong anular liga-
the clavicle, and finally, to the sternum. If the forces are ex-
ment. Rupture of this ligament occurs in cases of anterior
cessive, different parts of the upper limb give way under
dislocation of the head of the radius on the capitulum of the
the strain. The area affected seems to be related to age. In
humerus. In young children, in whom the head of the ra-
a young child, for example, there may be a posterior dis-
dius is still small and undeveloped, a sudden jerk on the arm
placement of the distal radial epiphysis; in the teenager the
can pull the radial head down through the anular ligament.
clavicle might fracture; in the young adult the scaphoid is
commonly fractured; and in the elderly the distal end of
the radius is fractured about 1 in. (2.5 cm) proximal to the
Wrist Joint
wrist joint (Colles’ fracture) (CD Fig. 12-2).
Wrist Joint Injuries
The wrist joint is essentially a synovial joint between the dis-
tal end of the radius and the proximal row of carpal bones.
JOINTS OF THE
The head of the ulna is separated from the carpal bones by
the strong triangular fibrocartilaginous ligament, which sep-
PELVIS
arates the wrist joint from the distal radioulnar joint. The
joint is stabilized by the strong medial and lateral ligaments.
Changes in the Pelvic Joints with
Because the styloid process of the radius is longer than
that of the ulna, abduction of the wrist joint is less extensive
Pregnancy
than adduction. In flexion-extension movements, the hand
can be flexed about 80° but extended to only about 45°. The
During pregnancy, the symphysis pubis and the ligaments
range of flexion is increased by movement at the midcarpal
of the sacroiliac and sacrococcygeal joints undergo soften-
joint.
ing in response to hormones, thus increasing the mobility
A fall on the outstretched hand can strain the anterior lig-
and increasing the potential size of the pelvis during child-
ament of the wrist joint, producing synovial effusion, joint
birth. The hormones responsible are estrogen and proges-
pain, and limitation of movement. These symptoms and signs
terone produced by the ovary and the placenta. An addi-
must not be confused with those produced by a fractured
tional hormone, called relaxin, produced by these organs
scaphoid or dislocation of the lunate bone, which are similar.
can also have a relaxing effect on the pelvic ligaments.
Falls on the Outstretched Hand
Changes in the Pelvic Joints with
In falls on the outstretched hand, forces are transmitted
from the scaphoid to the distal end of the radius, from the
Age
radius across the interosseous membrane to the ulna, and
from the ulna to the humerus; thence, through the glenoid
Obliteration of the cavity in the sacroiliac joint occurs in
fossa of the scapula to the coracoclavicular ligament and
both sexes after middle age.
Joints
175
Hip Joint Stability and Trendelen-
Sacroiliac Joint Disease
burg’s Sign
The sacroiliac joint is innervated by the lower lumbar and
The stability of the hip joint when a person stands on one leg
sacral nerves so that disease in the joint can produce low back
with the foot of the opposite leg raised above the ground de-
pain and pain referred along the sciatic nerve (sciatica).
pends on three factors:
The sacroiliac joint is inaccessible to clinical examina-
tion. However, a small area located just medial to and below
■ The gluteus medius and minimus must be functioning
the posterior superior iliac spine is where the joint comes
normally.
closest to the surface. In disease of the lumbosacral region,
■ The head of the femur must be located normally within
movements of the vertebral column in any direction cause
the acetabulum.
pain in the lumbosacral part of the column. In sacroiliac
■ The neck of the femur must be intact and must have a
disease, pain is extreme on rotation of the vertebral column
normal angle with the shaft of the femur.
and is worst at the end of forward flexion. The latter move-
If any one of these factors is defective, then the pelvis
ment causes pain because the hamstring muscles hold the
will sink downward on the opposite, unsupported side. The
hip bones in position while the sacrum is rotating forward as
patient is then said to exhibit a positive Trendelenburg’s
the vertebral column is flexed.
sign (CD Fig. 12-3).
Normally, when walking, a person alternately contracts
the gluteus medius and minimus, first on one side and then
JOINTS OF THE
on the other. By this means he or she is able to raise the
pelvis first on one side and then on the other, allowing the
leg to be flexed at the hip joint and moved forward—that is,
LOWER LIMB
the leg is raised clear of the ground before it is thrust forward
in taking the forward step. A patient with a right-sided con-
genital dislocation of the hip, when asked to stand on the
Hip Joint
right leg and raise the opposite leg clear of the ground, will
Referred Pain from the Hip Joint
exhibit a positive Trendelenburg’s sign, and the unsup-
ported side of the pelvis will sink below the horizontal. If the
The femoral nerve not only supplies the hip joint but, via
patient is asked to walk, he or she will show the characteris-
the intermediate and medial cutaneous nerves of the thigh,
tic “dipping” gait. In patients with bilateral congenital dislo-
also supplies the skin of the front and medial side of the
cation of the hip, the gait is typically “waddling” in nature.
thigh. It is not surprising, therefore, for pain originating in
the hip joint to be referred to the front and medial side of the
Arthritis of the Hip Joint
thigh. The posterior division of the obturator nerve supplies
both the hip and knee joints. This would explain why hip
A patient with an inflamed hip joint will place the femur in
joint disease sometimes gives rise to pain in the knee joint.
the position that gives minimum discomfort—that is, the po-
sition in which the joint cavity has the greatest capacity to
Congenital Dislocation of the Hip
contain the increased amount of synovial fluid secreted. The
hip joint is partially flexed, abducted, and externally rotated.
The stability of the hip joint depends on the ball-and-socket
Osteoarthritis, the most common disease of the hip
arrangement of the articular surfaces and the strong liga-
joint in the adult, causes pain, stiffness, and deformity. The
ments. In congenital dislocation of the hip, the upper lip of
pain may be in the hip joint itself or referred to the knee (the
the acetabulum fails to develop adequately, and the head of
obturator nerve supplies both joints). The stiffness is caused
the femur, having no stable platform under which it can
by the pain and reflex spasm of the surrounding muscles.
lodge, rides up out of the acetabulum onto the gluteal sur-
The deformity is flexion, adduction, and external rotation
face of the ilium.
and is produced initially by muscle spasm and later by mus-
Traumatic Dislocation of the Hip
cle contracture.
Traumatic dislocation of the hip is rare because of its
strength; it is usually caused by motor vehicle accidents.
Knee Joint
However, should it occur, it usually does so when the joint
Strength of the Knee Joint
is flexed and adducted. The head of the femur is displaced
posteriorly out of the acetabulum, and it comes to rest on the
The strength of the knee joint depends on the strength of the
gluteal surface of the ilium (posterior dislocation). The
ligaments that bind the femur to the tibia and on the tone of
close relation of the sciatic nerve to the posterior surface of
the muscles acting on the joint. The most important muscle
the joint makes it prone to injury in posterior dislocations.
group is the quadriceps femoris; provided that this is well
176
Chapter 12
normal
positive Trendelenburg's sign
CD Figure 12-3
Trendelenburg’s test.
developed, it is capable of stabilizing the knee in the pres-
occur at its femoral or tibial attachments. It is useful to re-
ence of torn ligaments.
member that tears of the menisci result in localized tender-
ness on the joint line, whereas sprains of the medial collat-
Knee Injury and the Synovial
eral ligament result in tenderness over the femoral or tibial
attachments of the ligament.
Membrane
Lateral Collateral Ligament
The synovial membrane of the knee joint is extensive, and if
the articular surfaces, menisci, or ligaments of the joint are
Forced adduction of the tibia on the femur can result in in-
damaged, the large synovial cavity becomes distended with
jury to the lateral collateral ligament (less common than
fluid. The wide communication between the suprapatellar
medial ligament injury).
bursa and the joint cavity results in this structure becoming
distended also. The swelling of the knee extends three or
Cruciate Ligaments
four fingerbreadths above the patella and laterally and me-
dially beneath the aponeuroses of insertion of the vastus lat-
Injury to the cruciate ligaments can occur when excessive
eralis and medialis, respectively.
force is applied to the knee joint. Tears of the anterior cru-
ciate ligament are common; tears of the posterior cruciate
Ligamentous Injury of the Knee Joint
ligament are rare. The injury is always accompanied by
damage to other knee structures; the collateral ligaments
Four ligaments—the medial collateral ligament, the lateral
are commonly torn or the capsule may be damaged. The
collateral ligament, the anterior cruciate ligament, and the
joint cavity quickly fills with blood (hemarthrosis) so that
posterior cruciate ligament—are commonly injured in the
the joint is swollen. Examination of patients with a rup-
knee. Sprains or tears occur depending on the degree of
tured anterior cruciate ligament shows that the tibia can be
force applied.
pulled excessively forward on the femur; with rupture of
the posterior cruciate ligament, the tibia can be made to
Medial Collateral Ligament
move excessively backward on the femur (CD Fig. 12-4).
Forced abduction of the tibia on the femur can result in par-
Because the stability of the knee joint depends largely on
tial tearing of the medial collateral ligament, which can
the tone of the quadriceps femoris muscle and the integrity
Joints
177
direction of impact
direction
of fall
medial meniscus
A
foot on ground
test for anterior
test for posterior
B
cruciate ligament
C
cruciate ligament
ruptured anterior
ruptured posterior
cruciate ligament
cruciate ligament
CD Figure 12-4
A. Mechanism involved in damage to the medial meniscus of the knee
joint from playing football. Note that the right knee joint is semiflexed and that medial ro-
tation of the femur on the tibia occurs. The impact causes forced abduction of the tibia on
the femur, and the medial meniscus is pulled into an abnormal position. The cartilaginous
meniscus is then ground between the femur and the tibia. B. Test for integrity of the ante-
rior cruciate ligament. C. Test for integrity of the posterior cruciate ligament.
178
Chapter 12
of the collateral ligaments, operative repair of isolated torn
being subjected to a severe grinding force, and it splits
cruciate ligaments is not always attempted. The knee is im-
along its length (CD Fig. 12-5). When the torn part of the
mobilized in slight flexion in a cast, and active physiother-
meniscus becomes wedged between the articular surfaces,
apy on the quadriceps femoris muscle is begun at once.
further movement is impossible, and the joint is said to
Should, however, the capsule of the joint and the collat-
“lock.”
eral ligaments be torn in addition, early operative repair is
Injury to the lateral meniscus is less common, proba-
essential.
bly because it is not attached to the lateral collateral liga-
ment of the knee joint and is consequently more mobile.
Meniscal Injury of the Knee Joint
The popliteus muscle sends a few of its fibers into the lat-
eral meniscus, and these can pull the meniscus into a
Injuries of the menisci are common. The medial meniscus
more favorable position during sudden movements of the
is damaged much more frequently than the lateral, and
knee joint.
this is probably because of its strong attachment to the me-
dial collateral ligament of the knee joint, which restricts its
Pneumoarthrography of the Knee
mobility. The injury occurs when the femur is rotated on
Joint
the tibia, or the tibia is rotated on the femur, with the knee
joint partially flexed and taking the weight of the body.
Air can be injected into the synovial cavity of the knee joint
The tibia is usually abducted on the femur, and the medial
so that soft tissues can be studied. This technique is based on
meniscus is pulled into an abnormal position between the
the fact that air is less radiopaque than structures such as the
femoral and tibial condyles (CD Fig. 12-4A). A sudden
medial and lateral menisci, so their outline can be visual-
movement between the condyles results in the meniscus
ized on a radiograph (see text Fig. 12-43).
medial meniscus
B
A
C
D
CD Figure 12-5
Tears of the medial meniscus of the knee joint. A. Complete bucket han-
dle tear. B. The meniscus is torn from its peripheral attachment. C. Tear of the posterior
portion of the meniscus. D. Tear of the anterior portion of the meniscus.
Joints
179
Arthroscopy of the Knee Joint
Joints of the Foot
Arthroscopy involves the introduction of a lighted instru-
ment into the synovial cavity of the knee joint through a
Metatarsophalangeal Joint of the Big
small incision. This technique permits the direct visualiza-
Toe
tion of structures, such as the cruciate ligaments and the
Hallux valgus, which is a lateral deviation of the great toe at
menisci, for diagnostic purposes.
the metatarsophalangeal joint, is a common condition. Its
incidence is greater in women than in men and is associated
Ankle Joint
with badly fitting shoes. It is often accompanied by the pres-
ence of a short first metatarsal bone. Once the deformity is
Ankle Joint Stability
established, it is progressively worsened by the pull of the
flexor hallucis longus and extensor hallucis longus muscles.
The ankle joint is a hinge joint possessing great stability.
Later, osteoarthritic changes occur in the metatarsopha-
The deep mortise formed by the lower end of the tibia and
langeal joint, which then becomes stiff and painful; the con-
the medial and lateral malleoli securely holds the talus in
dition is then known as hallux rigidus.
position.
Clinical Examination of the Arches of
Acute Sprains of the “Lateral Ankle”
the Foot
Acute sprains of the lateral ankle are usually caused by ex-
On examination of the imprint of a wet foot on the floor
cessive inversion of the foot with plantar flexion of the ankle.
made with the person in the standing position, one can see
The anterior talofibular ligament and the calcaneofibular
that the heel, the lateral margin of the foot, the pad under
ligament are partially torn, giving rise to great pain and local
the metatarsal heads, and the pads of the distal phalanges are
swelling.
in contact with the ground (see text Figs. 12-41 and 12-42).
The medial margin of the foot, from the heel to the first
Acute Sprains of the “Medial Ankle”
metatarsal head, is arched above the ground because of the
important medial longitudinal arch. The pressure exerted
Acute sprains of the medial ankle are similar to but less
on the ground by the lateral margin of the foot is greatest at
common than those of the lateral ankle. They may occur
the heel and the fifth metatarsal head and least between
to the medial or deltoid ligament as a result of excessive
these areas because of the presence of the low-lying lateral
eversion. The great strength of the medial ligament usually
longitudinal arch. The transverse arch involves the bases of
results in the ligament pulling off the tip of the medial
the five metatarsals and the cuboid and cuneiform bones.
malleolus.
This is, in fact, only half an arch, with its base on the lateral
border of the foot and its summit on the foot’s medial bor-
Fracture Dislocations of the Ankle
der. The foot has been likened to a half-dome, so that when
Joint
the medial borders of the two feet are placed together, a
complete dome is formed.
Fracture dislocations of the ankle are common and are
From this description, it can be understood that the
caused by forced external rotation and overeversion of the
body weight on standing is distributed through a foot via the
foot. The talus is externally rotated forcibly against the lat-
heel behind and six points of contact with the ground in
eral malleolus of the fibula. The torsion effect on the
front, namely, the two sesamoid bones under the head of the
lateral malleolus causes it to fracture spirally. If the force
first metatarsal and the heads of the remaining four
continues, the talus moves laterally, and the medial
metatarsals.
ligament of the ankle joint becomes taut and pulls off the
tip of the medial malleolus. If the talus is forced to move
The “Stone Bridge” Mechanisms for
still farther, its rotary movement results in its violent con-
tact with the posterior inferior margin of the tibia, which
Arch Support
shears off.
Examination of the design of any stone bridge reveals the
Other less common types of fracture dislocation are
following engineering methods used for its support (CD
caused by forced overeversion (without rotation), in which
Fig. 12-6).
the talus presses the lateral malleolus laterally and causes it
to fracture transversely. Overinversion (without rotation), in
■ The shape of the stones: The most effective way of sup-
which the talus presses against the medial malleolus, pro-
porting the arch is to make the stones wedge shaped,
duces a vertical fracture through the base of the medial
with the thin edge of the wedge lying inferiorly. This
malleolus.
applies particularly to the important stone that occupies
180
Chapter 12
"keystone"
keystone
shape of stones
shape of bones
short plantar
ligament
long plantar
ligament
calcaneonavicular
ligament
staples
strong plantar ligaments
tendon of flexor
hallucis longus
tie beam
peroneus longus
suspension bridge
CD Figure 12-6
Different methods by which the arches of the foot may be supported.
the center of the arch and is referred to as the “key-
beam connecting the ends effectively prevents separation
stone.”
of the pillars and consequent sagging of the arch.
■ The inferior edges of the stones are tied together: This is
■ A suspension bridge: Here, the maintenance of the arch
accomplished by interlocking the stones or binding their
depends on multiple supports suspending the arch from
lower edges together with metal staples. This method ef-
a cable above the level of the bridge.
fectively counteracts the tendency of the lower edges of the
stones to separate when the arch is weightbearing.
Using the bridge analogy, one can now examine the
■ The use of the tie beams: When the span of the bridge is
methods used to support the arches of the feet (see CD Fig.
large and the foundations at either end are insecure, a tie
12-6).
Joints
181
Maintenance of the Medial Longitudi-
■ Suspending the arch from above are the peroneus
longus tendon and the peroneus brevis.
nal Arch
■ Shape of the bones: The sustentaculum tali hold up
the talus; the concave proximal surface of the navicular
bone receives the rounded head of the talus; the slight
P H Y S I O L O G I C N O T E
concavity of the proximal surface of the medial
cuneiform bone receives the navicular. The rounded
Muscle Tone and the Arches of the Foot
head of the talus is the keystone in the center of the
The arches of the feet are maintained by the shape of the
arch (see CD Fig. 12-6).
bones, strong ligaments, and muscle tone. Which of
■ The inferior edges of the bones are tied together by
these factors is the most important? Basmajian and
the plantar ligaments, which are larger and stronger
Stecko demonstrated electromyographically that the tib-
than the dorsal ligaments. The most important ligament
ialis anterior, the peroneus longus, and the small mus-
is the plantar calcaneonavicular ligament (see CD Fig.
cles of the foot play no important role in the normal static
12-6). The tendinous extensions of the insertion of the
support of the arches. They are commonly totally inac-
tibialis posterior muscle play an important role in this
tive. However, during walking and running, all these
respect.
muscles become active. Standing immobile for long pe-
■ Tying the ends of the arch together are the plantar
riods, especially if the person is overweight, places
aponeurosis, the medial part of the flexor digitorum bre-
excessive strain on the bones and ligaments of the feet
vis, the abductor hallucis, the flexor hallucis longus, the
and results in fallen arches or flat feet. Athletes, route-
medial part of the flexor digitorum longus, and the flexor
marching soldiers, and nurses are able to sustain their
hallucis brevis (see CD Fig. 12-6).
arches provided that they receive adequate training to
■ Suspending the arch from above are the tibialis ante-
develop their muscle tone.
rior and posterior and the medial ligament of the ankle
joint.
Clinical Problems Associated with the
Arches of the Foot
Maintenance of the Lateral Longitudi-
nal Arch
Of the three arches, the medial longitudinal is the largest
and clinically the most important. The shape of the
■ Shape of the bones: Minimal shaping of the distal end of
bones, the strong ligaments, especially those on the plan-
the calcaneum and the proximal end of the cuboid. The
tar surface of the foot, and the tone of muscles all play an
cuboid is the keystone.
important role in supporting the arches. It has been
■ The inferior edges of the bones are tied together by the
shown that in the active foot the tone of muscles is an im-
long and short plantar ligaments and the origins of the
portant factor in arch support. When the muscles are fa-
short muscles from the forepart of the foot (see CD Fig.
tigued by excessive exercise (a long-route march by an
12-6).
army recruit), by standing for long periods (waitress or
■ Tying the ends of the arch together are the plantar
nurse), by being overweight, or by illness, the muscular
aponeurosis, the abductor digiti minimi, and the lateral
support gives way, the ligaments are stretched, and pain is
part of the flexor digitorum longus and brevis.
produced.
■ Suspending the arch from above are the peroneus
Pes planus (flat foot) is a condition in which the medial
longus and the brevis (see CD Fig. 12-6).
longitudinal arch is depressed or collapsed. As a result, the
forefoot is displaced laterally and everted. The head of the
Maintenance of the Transverse Arch
talus is no longer supported, and the body weight forces it
■ Shape of the bones: The marked wedge shaping of the
downward and medially between the calcaneum and the
cuneiform bones and the bases of the metatarsal bones
navicular bone. When the deformity has existed for some
(see text Fig. 12-42)
time, the plantar, calcaneonavicular, and medial ligaments
■ The inferior edges of the bones are tied together by the
of the ankle joint become permanently stretched, and the
deep transverse ligaments, the strong plantar ligaments,
bones change shape. The muscles and tendons are also per-
and the origins of the plantar muscles from the forepart
manently stretched. The causes of flat foot are both congen-
of the foot; the dorsal interossei and the transverse head
ital and acquired.
of the adductor hallucis are particularly important in this
Pes cavus (clawfoot) is a condition in which the medial
respect.
longitudinal arch is unduly high. Most cases are caused by
■ Tying the ends of the arch together is the peroneus
muscle imbalance, in many instances resulting from po-
longus tendon.
liomyelitis.
182
Chapter 12
Clinical Problem Solving Questions
Read the following case histories/questions and give
particularly daring dive, he surfaced quickly and climbed
the best answer for each.
out of the pool, holding his head between his hands. He
said that he had hit the bottom of the pool with his head
and now had severe pain in the root of the neck, which
General Joint Questions
was made worse when he tried to move his neck. A lateral
A 31-year-old woman has a history of poliomyelitis af-
radiograph revealed that the right inferior articular
fecting the anterior horn cells of the lower thoracic and
process of the fifth cervical vertebra was forced over the
lumbar segments of the spinal cord on the left side. On
anterior margin of the right superior articular process of
examination, she has severe right lateral flexion defor-
the sixth cervical vertebra, producing a unilateral disloca-
mity of the vertebral column.
tion with nipping of the right sixth cervical nerve.
1.
The following statements are true about this case ex-
4.
The following symptoms and signs confirmed the diag-
cept which?
nosis except which?
A. The virus of poliomyelitis attacks and destroys the
A. The head was rotated to the right.
motor anterior horn cells of the spinal cord.
B. There was spasm of the deep neck muscles on the
B. The disease resulted in the paralysis of the muscles
right side of the neck, which were tender to touch.
that normally laterally flex the vertebral column on
C. The patient complained of severe pain in the region
the left side.
of the back of the neck and right shoulder.
C. The muscles on the right side of the vertebral col-
D. The slightest movement produced severe pain in the
umn are unapposed.
right sixth cervical dermatome.
D. The right lateral flexion deformity is caused by the
E. The large size of the vertebral canal in the cervical
slow degeneration of the sensory nerve fibers origi-
region permitted the spinal cord to escape injury.
nating from the vertebral muscles on the right side.
A 50-year-old coal miner was crouching at the mine
A 20-year-old woman severely sprains her left ankle
face when a large rock suddenly became dislodged
while playing tennis. When she tries to move the foot so
from the roof of the mine shaft and struck him on the
that the sole faces medially, she experiences severe pain.
upper part of his back. The emergency department
physician suspected a displacement of the upper tho-
2.
What is the correct anatomic term for the movement of
racic spines on the sixth thoracic spine.
the foot that produces the pain?
A. Pronation
5.
The following physical signs confirmed a diagnosis of
B. Inversion
fracture dislocation between the fifth and sixth thoracic
C. Supination
vertebrae except which?
D. Eversion
A. A lateral radiograph revealed fractures involving the
superior articular processes of the sixth thoracic ver-
Joints of the Skull
tebra and the inferior articular processes of the fifth
3. An exhausted medical student decided to brush up on
thoracic vertebra.
gross anatomy by attending a lecture given by an old and
B. Considerable forward displacement of the body of
revered visiting professor. After 45 minutes the lecture be-
the fifth thoracic vertebra on the sixth thoracic ver-
gan to bore him, and his mind began to wander. He could
tebra occurred.
not forget the attractive brunette nurse in the surgical
C. The patient had signs and symptoms of spinal shock.
clinic whom he had dated the previous evening. After 5
D. The large size of the vertebral canal in the thoracic
more minutes he found he just could not keep his eyes
region leaves plenty of space around the spinal cord
open. When would this lecture end? Just then, he invol-
for bony displacement.
untarily opened his mouth wide and yawned. To his great
E. The patient later showed signs and symptoms of
consternation he could not close his mouth. His jaw was
paraplegia.
stuck in the open position. What is your diagnosis?
A 66-year-old woman was seen in the emergency de-
partment complaining of a burning pain over the upper
Joints of the Vertebral Column
part of her right arm. The pain had started 2 days previ-
An 11-year-old boy was showing off in front of friends by
ously and had progressively worsened. Physical exami-
diving into the shallow end of a swimming pool. After one
nation revealed weakness and wasting of the right
Joints
183
deltoid and biceps brachii muscles. The patient also
A 22-year-old student was driving home from a party
had hyperesthesia in the skin over the lower part of the
and crashed his car head on into a brick wall. On
right deltoid and down the lateral side of the arm. Ra-
examination in the emergency department, he was
diologic examination showed extensive spur formation
found to have a fracture dislocation of the seventh tho-
on the bodies of the fourth, fifth, and sixth cervical ver-
racic vertebra, with signs and symptoms of severe dam-
tebrae. These signs and symptoms suggested severe os-
age to the spinal cord.
teoarthritis of the cervical vertebral column.
8. On recovery from spinal shock, he was found to have
6.
This disease produced the following changes in the ver-
the following signs and symptoms except which?
tebrae and related structures except which?
A. Fracture dislocation of the seventh thoracic verte-
A. Repeated trauma and aging had resulted in degen-
bra, which would result in severe damage to the sev-
erative changes at the articulating surfaces of the
enth thoracic segment of the spinal cord
fourth, fifth, and sixth cervical vertebrae.
B. A band of cutaneous hyperesthesia extending around
B. Extensive spur formation resulted in narrowing of
the abdominal wall on the left side at the level of the
the intervertebral foramina with pressure on the
umbilicus that was caused by the irritation of the cord
nerve roots.
immediately above the site of the lesion
C. The burning pain and hyperesthesia were caused by
C. On the right side, total analgesia, thermoanesthesia,
pressure on the third and fourth cervical posterior
and partial loss of tactile sense of the skin of the ab-
roots.
dominal wall below the level of the umbilicus in-
D. The weakness and wasting of the deltoid and biceps
volving the whole of the right leg
brachii muscles were caused by pressure on the fifth
D. Upper motor neuron paralysis of his left leg
and sixth cervical anterior roots.
E. Unequal sensory and motor losses on the two sides,
E. Movements of the neck intensified the symptoms by
which indicate a left hemisection of the spinal cord
exerting further pressure on the nerve roots.
F. Coughing or sneezing raised the pressure within the
Joints of the Ribs
vertebral canal and resulted in further pressure on
9. A 36-year-old woman went sailing with her husband
the roots.
and they were caught in a severe gale. While the hus-
A medical student offered to move a grand piano for his
band at the helm desperately managed to keep the boat
landlady. He had just finished his final examinations in
under control, the wife tried to get the sails down. Even-
anatomy and was in poor physical shape. He struggled
tually the squall died down and they were able to return
with the antique monstrosity and suddenly experienced
safely to port. The next morning, the woman woke up
an acute pain in the back, which extended down the
with severe pain over the left side of her chest. On be-
back and outer side of his left leg. On examination in
ing examined in the emergency department of the local
the emergency department, he was found to have a
hospital for a suspected myocardial infarction, the
slight scoliosis with the convexity on the right side. The
physician found that the patient was acutely tender over
deep muscles of the back in the left lumbar region felt
her left costal margin, which was made worse on taking
firmer than normal. No evidence of muscle weakness
a deep breath. What is the possible diagnosis?
was present, but the left ankle jerk was diminished.
Joints of the Upper Extremity
7.
The symptoms and signs of this patient strongly suggest a
diagnosis of prolapsed intervertebral disc except which?
10. Separation of the acromioclavicular joint is common in
A. The pain was the worst over the left lumbar region
football and soccer players. Explain why such separa-
opposite the fifth lumbar spine.
tions are unstable after reduction.
B. The pain was accentuated by coughing.
A father, seeing his 3-year-old son playing in the garden,
C. With the patient supine, flexing the left hip joint
ran up and picked him up by both hands and swung
with the knee extended caused a marked increase in
him around in a circle. The child’s enjoyment sud-
the pain.
denly turned to tears, and he said his left elbow hurt.
D. A lateral radiograph of the lumbar vertebral column
On examination, the child held his left elbow joint
revealed nothing abnormal.
semiflexed and his forearm pronated.
E. A magnetic resonance imaging study revealed the
presence of small fragments of the nucleus pulposus
11. The following statements concerning this case are con-
that had herniated outside the anulus in the disc be-
sistent with the diagnosis of dislocation of the superior
tween the fifth lumbar vertebra and the sacrum.
radioulnar joint except which?
F. The pain occurred in the dermatomes of the third
A. The head of the radius was pulled out of the anular
and fourth lumbar segments on the left side.
ligament.
184
Chapter 12
B. At age 3 years, the child’s anular ligament has a large
E. On reduction of the fracture the distal end of the ra-
diameter and the head of the radius can easily be
dius should lie at an angle of 15° anteriorly.
pulled out of the ligament by traction.
F. The hand should always be splinted in the position
C. The incidence of this condition is equal in both sexes.
of function.
D. The pain from the joint caused reflex contraction of
A 22-year-old medical student fell off her bicycle onto
the surrounding muscles to protect the joint from
her outstretched hand. She thought she had sprained her
further movement.
right wrist joint and treated herself by binding her wrist
E. The subluxation of the joint can be treated by
with an elastic bandage. Three weeks later, however, she
pulling downward on the forearm and at the same
was still experiencing pain on moving her wrist and so de-
time performing the movement of pronation and
cided to visit the emergency department. On examina-
supination. Finally, the elbow joint is flexed and
tion of the dorsal surfaces of both hands, with the fingers
held in that position.
and thumbs fully extended, a localized tenderness could
A 60-year-old woman fell down the stairs and was admit-
be felt in the anatomic snuffbox of her right hand. A di-
ted to the emergency department with severe right shoul-
agnosis of fracture of the right scaphoid bone was made.
der pain. On examination, the patient was sitting up with
14.
The following statements concerning this patient are
her right arm by her side and her right elbow joint sup-
correct except which?
ported by the left hand. Inspection of the right shoulder
A. The scaphoid bone is an easy bone to immobilize
showed loss of the normal rounded curvature and evi-
because of its small size.
dence of a slight swelling below the right clavicle. Any at-
B. A bony fragment deprived of its blood supply may
tempt at active or passive movement of the shoulder joint
undergo ischemic necrosis.
was stopped by severe pain in the shoulder. A diagnosis
C. Because the scaphoid bone articulates with other
of dislocation of the right shoulder joint was made.
bones, the fracture line may enter a joint cavity and
become bathed in synovial fluid, which would in-
12.
The following statements concerning this patient are
hibit repair.
consistent with the diagnosis except which?
D. The fracture line on the scaphoid bone may deprive
A. This patient had a subcoracoid dislocation of the
the proximal fragment of its arterial supply.
right shoulder joint.
E. Fractures of the scaphoid bone have a high inci-
B. The head of the humerus was dislocated downward
dence of nonunion.
through the weakest part of the capsule of the joint.
C. The pull of the pectoralis major and subscapularis
15.
A 46-year-old woman slipped on a shiny floor and sus-
muscles had displaced the upper end of the
tained a fracture of the fifth metacarpal bone on her left
humerus medially.
hand. What type of angulation of the fragments is com-
D. The greater tuberosity of the humerus no longer dis-
monly found in fractures at this site? When a splint is
placed the deltoid muscle laterally, and the curve of
applied with the little finger flexed, in which direction
the shoulder was lost.
should the little finger be pointing?
E. The integrity of the axillary nerve should always be
tested by touching the skin over the upper half of the
Joints of the Lower Extremity
deltoid muscle.
A medical student, while playing football, collided with
A 63-year-old man fell down a flight of stairs and sus-
another player and fell to the ground. As he fell, the
tained a fracture of the lower end of the left radius. On
right knee, which was taking the weight of his body, was
examination the distal end of the radius was displaced
partially flexed; the femur was rotated medially; and the
posteriorly. This patient had sustained a Colles’ fracture.
leg was abducted on the thigh. A sudden pain was felt
in the right knee joint, and he was unable to extend it.
13.
The following statements concerning this case are cor-
The student was diagnosed as having a torn medial
rect except which?
meniscus of the knee joint.
A. Occasionally the styloid process of the ulna is also
fractured.
16. The following statements concerning this case con-
B. The median nerve may be injured at the time of the
firmed the diagnosis except which?
fall.
A. The right knee joint quickly became swollen.
C. When the fracture is reduced, the styloid process of
B. Severe local tenderness was felt along the medial
the radius should come to lie about 0.75 in. (1.9 cm)
side of the joint line.
proximal to that of the ulna.
C. The medial meniscus split along part of its length,
D. The fracture produces posterior angulation of the
and the detached portion became jammed between
distal fragment of the radius.
the articular surfaces, limiting further extension.
Joints
185
D. The trauma stimulated the production of synovial
E. Because the cruciate ligaments are located outside
fluid, which filled the joint cavity.
the synovial membrane, bleeding from a torn liga-
E. The distension of the suprapatellar bursa was re-
ment does not enter the joint cavity.
sponsible for the large amount of swelling above the
A 25-year-old man was running across a field when he
injured knee.
caught his right foot in a rabbit hole. As he fell, the right
F. The pain sensation from the injured knee was con-
foot was violently rotated laterally and overeverted. On
fined to the femoral nerve as it ascended to the cen-
attempting to stand, he could place no weight on his
tral nervous system.
right foot. On examination by a physician, the right an-
A 27-year-old woman was found to have an unstable
kle was considerably swollen, especially on the lateral
right knee joint following a severe automobile accident.
side. After further examination, including a radiograph
On examination it was possible to pull the tibia exces-
of the ankle, a diagnosis of severe fracture dislocation of
sively forward on the femur. A diagnosis of ruptured an-
the ankle joint was made.
terior cruciate ligament was made.
18.
The following statements concerning this patient are
17.
The following statements concerning this patient are
correct except which?
correct except which?
A. This type of fracture dislocation is caused by forced
A. The anterior cruciate ligament is attached to
external rotation and overeversion of the foot.
the tibia in the anterior part of the intercondylar
B. The talus is externally rotated against the lateral
area.
malleolus of the fibula, causing it to fracture.
B. The anterior cruciate ligament passes upward, back-
C. The medial ligament of the ankle joint is strong and
ward, and laterally from its tibial attachment.
never ruptures.
C. The anterior cruciate ligament is attached above to
D. The torsion effect on the lateral malleolus produces
the posterior part of the medial surface of the lateral
a spiral fracture.
femoral condyle.
E. If the talus is forced to move farther laterally and
D. The anterior cruciate ligament is more commonly
continues to rotate, the posterior inferior margin of
torn than is the posterior cruciate ligament.
the tibia will be sheared off.
Answers and Explanations
1. D is the correct answer. The right lateral flexion defor-
4. A is the correct answer. The right inferior articular
mity is not caused by the slow degeneration of the sen-
process of the fifth cervical vertebra was forced over the
sory nerve fibers originating from the vertebral muscle
anterior margin of the right superior articular process of
on the right side. It is the motor nerves supplying the
the sixth cervical vertebra, causing the head of the pa-
vertebral muscles on the left side that are affected in
tient to be rotated to the left.
this patient.
5. D is the correct answer. The vertebral canal in the tho-
2. B is the correct answer. Moving the foot at the subtalar
racic region is small and round and little space is
and midtarsal joints so that the sole faces medially is
around the spinal cord for bony displacement to occur
called inversion.
without causing severe damage to the cord.
3. The student had dislocated his temporomandibular
6. C is the correct answer. The burning pain and hyperes-
joints on both sides. When he yawned, his lateral
thesia were caused by pressure on the fifth and sixth cer-
pterygoid muscles reflexly contracted forcibly and
vical posterior roots.
pulled the head of the mandible and the articular disc
7. F is the correct answer. The pain occurred in the der-
forward over the summit of the articular tubercle in
matomes of the fifth lumbar and first sacral segments on
each joint. Reduction is easily performed by pressing
the left side.
gloved thumbs downward and backward on the last
molar teeth. The lateral pterygoid, the temporalis, and
8. A is the correct answer. Fracture dislocation of the
the masseter muscle tension is overcome and the head
seventh thoracic vertebra would result in severe
of the mandible snaps back over the articular tubercle
damage to the tenth thoracic segment of the spinal
to assume its normal anatomical position.
cord.
186
Chapter 12
9.
The localized tenderness over the left costal margin is
of the deltoid muscle. The skin of the curve of the
strongly suggestive of subluxation of one of the inter-
shoulder, including the skin covering the upper half of
chondral joints on the costal margin. Subluxation of a
the deltoid muscle, is supplied by the supraclavicular
joint implies that the ligaments and capsule are
nerves.
stretched or torn but the damage is not so severe that the
13.
C is the correct answer. The normal position of the tip
articulating surfaces lose contact with one another.
of the styloid process of the radius is about 0.75 in. (1.9
This condition can be extremely painful and in this pa-
cm) distal to that of the ulna.
tient was secondary to trauma caused by excessive
pulling of the muscles connecting the thoracic cage to
14.
A is the correct answer. The scaphoid bone is a difficult
the upper limb. The sixth, seventh, eighth, ninth, and
bone to immobilize because of its position and small
tenth costal cartilages articulate with each other along
size.
their borders by small synovial joints.
15.
Fractured metacarpal bones show dorsal angulation
10.
In subluxation of the acromioclavicular joint, the lat-
caused by the forward pull of the long flexor tendons
eral end of the clavicle elevates and becomes more
and the lumbricals and interossei on the distal frag-
prominent than normal; there is a definite step down
ment. When flexed individually, all fingers (excluding
onto the acromion. A dislocation occurs when the dam-
the thumb) point toward the tubercle of the scaphoid.
age to the restraining structures is more severe and the
When a finger is unstable following a fracture, it
articulating surfaces lose contact with one another. In
should be aligned so that its tip points to the scaphoid
the case of the acromioclavicular joint, the clavicle rises
tubercle; failure to achieve this will result in malfunc-
above the acromion and the joint is very unstable.
tion.
The main strength of the acromioclavicular joint de-
16.
F is the correct answer. The sensation of pain from the
pends on the integrity of the strong coracoclavicular lig-
knee joint ascends to the central nervous system via the
ament (see text Fig. 12-14). Should this ligament be dis-
femoral, obturator, common peroneal, and tibial nerves.
rupted, the acromioclavicular joint dislocates; the lat-
17.
E is the correct answer. The synovial membrane cover-
eral end of the clavicle rides over the acromion and the
ing the cruciate ligaments (see text Fig. 12-31) is torn
upper limb is depressed.
along with the ligaments, and the joint cavity quickly
11.
B is the correct answer. Under age 6 years, the child’s
fills with blood.
head of the radius is of a relatively small size and may
18.
C is the correct answer. Although the medial ligament
easily be pulled out of the anular ligament by traction
of the ankle joint is strong, extreme force can result in
on the forearm.
rupture of the ligament, the ligament can be torn from
12.
E is the correct answer. The integrity of the axillary
the medial malleolus, or the pull on the ligament can
nerve is tested by touching the skin over the lower half
fracture the medial malleolus.
Chapter Outline
General Clinical Features Concerning
Rupture of the Supraspinatus Tendon
195
Muscles
189
Axillary Nerve and the Quadrangular Space
196
Muscle Tone
189
Carpal Tunnel Syndrome
196
Muscle Attachments
189
Tenosynovitis of the Synovial Sheaths of the
Muscle Shape and Form
189
Flexor Tendons
196
Segmental Innervation of Muscle
189
Trigger Finger
198
Mallet Finger
198
Muscles of the Head
189
Boutonniere Deformity
198
Lacerations of the Scalp
189
Dupuytren’s Contracture
198
Facial Muscle Paralysis
189
Muscles of the Lower Limb
199
Muscles of the Neck
191
Gluteus Maximus and Intramuscular Injections
199
Sternocleidomastoid Muscle and Protection
from Trauma
191
Gluteus Maximus and Bursitis
199
Congenital Torticollis
191
Gluteus Medius and Minimus and Poliomyelitis
199
Spasmodic Torticollis
191
Quadriceps Femoris as a Knee-Joint Stabilizer
200
Clinical Significance of the Deep Fascia of the
Rupture of the Rectus Femoris
200
Neck
191
Rupture of the Ligamentum Patellae
200
Fascial Spaces
191
Femoral Sheath and Femoral Hernia
200
Acute Infections of the Fascial Spaces
of the Neck
191
Adductor Muscles and Cerebral Palsy
201
Chronic Infection of the Fascial Spaces
The Adductor Magnus and Popliteal Aneurysms
202
of the Neck
191
Semimembranosus Bursa Swelling
202
Clinical Significance of the Triangles of the Neck
191
Anterior Compartment of the Leg Syndrome
202
Muscles of the Abdominal Wall
192
Tenosynovitis and Dislocation of the Peroneus
Hematoma of the Rectus Sheath
192
Longus and Brevis Tendons
202
Abdominal Muscles, Abdominothoracic Rhythm,
Gastrocnemius and Soleus Muscle Tears
202
and Visceroptosis
192
Ruptured Tendo Calcaneus
202
Muscle Rigidity and Referred Pain
193
Rupture of the Plantaris Tendon
202
Surgery and the Tendinous Intersections of the
Plantaris Tendon and Autografts
202
Rectus Abdominis Muscle
193
Plantar Fasciitis
202
Psoas Abscess
193
Clinical Problems Associated with the Arches
Muscles of the Pelvis
193
of the Foot
203
Pelvic Floor
193
Bursae and Bursitis in the Lower Limb
203
Functional Significance of the Pelvic Floor
in the Female
193
Clinical Problem Solving Questions
203
Injury to the Pelvic Floor
194
Muscles of the Upper Limb
194
Answers and Explanations
206
Rotator Cuff Tendinitis
194
Skeletal Muscles
189
tal innervation of the following muscles should be known
GENERAL CLINICAL
because they can be tested by eliciting simple muscle re-
flexes in the patient (CD Fig. 13-1).
FEATURES
■ Biceps brachii tendon reflex: C5 and 6 (flexion of the el-
bow joint by tapping the biceps tendon)
■ Triceps tendon reflex: C6, 7, and 8 (extension of the el-
CONCERNING
bow joint by tapping the triceps tendon)
■ Brachioradialis tendon reflex: C5, 6, and 7 (supination
MUSCLES
of the radioulnar joints by tapping the insertion of the
brachioradialis tendon)
■ Abdominal superficial reflexes (contraction of underly-
Muscle Tone
ing abdominal muscles by stroking the skin): Upper ab-
dominal skin T6-7, middle abdominal skin T8-9, and
Determination of the tone of a muscle is an important clin-
lower abdominal skin T10-12
ical examination. If a muscle is flaccid, then either the af-
■ Patellar tendon reflex (knee jerk): L2, 3, and 4 (exten-
ferent, the efferent, or both neurons involved in the reflex
sion of the knee joint on tapping the patellar tendon)
arc necessary for the production of muscle tone have been
■ Achilles tendon reflex (ankle jerk): S1 and S2 (plantar
interrupted. For example, if the nerve trunk to a muscle is
flexion of the ankle joint on tapping the Achilles tendon)
severed, both neurons will have been interrupted. If po-
liomyelitis has involved the motor anterior horn cells at a
level in the spinal cord that innervates the muscle, the ef-
MUSCLES OF THE
ferent motor neurons will not function. If, conversely, the
muscle is found to be hypertonic, the possibility exists of a
lesion involving higher motor neurons in the spinal cord or
HEAD
brain.
Lacerations of the Scalp
Muscle Attachments
The tension of the epicranial aponeurosis (see text Fig. 13-
The importance of knowing the main attachments of all the
6), produced by the tone of the occipitofrontalis muscles, is
major muscles of the body need not be emphasized. Only
important in all deep wounds of the scalp. If the aponeuro-
with such knowledge is it possible to understand the normal
sis has been divided, the wound will gape open. For
and abnormal actions of individual muscles or muscle
satisfactory healing to take place, the opening in the
groups. How can one even attempt to analyze, for example,
aponeurosis must be closed with sutures.
the abnormal gait of a patient without this information?
Often a wound caused by a blunt object such as a
baseball bat closely resembles an incised wound. This is
Muscle Shape and Form
because the scalp is split against the unyielding skull, and
the pull of the occipitofrontalis muscles causes a gaping
The general shape and form of muscles should also be
wound. This anatomic fact may be of considerable foren-
noted, since a paralyzed muscle or one that is not used (such
sic importance.
as occurs when a limb is immobilized in a cast) quickly at-
rophies and changes shape. In the case of the limbs, it is al-
ways worth remembering that a muscle on the opposite side
Facial Muscle Paralysis
of the body can be used for comparison.
The facial muscles are innervated by the facial nerve. Dam-
age to the facial nerve in the internal acoustic meatus (by a
tumor), in the middle ear (by infection or operation), in the
Segmental Innervation of Muscle
facial nerve canal (perineuritis, Bell’s palsy), or in the
Skeletal muscle receives a segmental innervation. Most of
parotid gland (by a tumor) or caused by lacerations of the
these muscles are innervated by two, three, or four spinal
face will cause distortion of the face, with drooping of
nerves and therefore by the same number of segments of the
the lower eyelid, and the angle of the mouth will sag on the
spinal cord. To paralyze a muscle completely, it is thus nec-
affected side. This is essentially a lower motor neuron le-
essary to section several spinal nerves or to destroy several
sion. An upper motor neuron lesion (involvement of the
segments of the spinal cord.
pyramidal tracts) will leave the upper part of the face normal
Learning the segmental innervation of all the muscles
because the neurons supplying this part of the face receive
of the body is an impossible task. Nevertheless, the segmen-
corticobulbar fibers from both cerebral cortices.
190
Chapter 13
C6, 7, and 8
C5 and 6
triceps tendon reflex
biceps brachii tendon reflex
L2, 3, and 4
patellar tendon reflex
C5, 6, and 7
brachioradialis
S1 and 2
tendon
reflex
Achilles tendon reflex
CD Figure 13-1
Some important tendon reflexes used in medical practice.
Skeletal Muscles
191
layers (see text Fig. 13-11). These fascial layers are easily rec-
MUSCLES OF THE
ognizable to the surgeon at operation.
NECK
Fascial Spaces
Between the more dense layers of deep fascia in the neck is
Sternocleidomastoid Muscle and
loose connective tissue that forms potential spaces that are
clinically important. Among the more important spaces are
Protection from Trauma
the visceral, retropharyngeal, submandibular, and mastica-
tory spaces (CD Fig. 13-2).
The sternocleidomastoid, a strong, thick muscle crossing
The deep fascia and the fascial spaces are important
the side of the neck (see text Fig. 13-9), protects the
because organisms originating in the mouth, teeth, phar-
underlying soft structures from blunt trauma. Suicide
ynx, and esophagus can spread among the fascial planes
attempts by cutting one’s throat often fail because the
and spaces, and the tough fascia can determine the direc-
individual first extends the neck before making several
tion of spread of infection and the path taken by pus. It is
horizontal cuts with a knife. Extension of the cervical part
possible for blood, pus, or air in the retropharyngeal space
of the vertebral column and extension of the head at the
to spread downward into the superior mediastinum of the
atlantooccipital joint cause the carotid sheath with its
thorax.
contained large blood vessels to slide posteriorly beneath
the sternocleidomastoid muscle. To achieve the desired
Acute Infections of the Fascial Spaces of
result with the head and neck fully extended, some indi-
viduals have to make several attempts and only succeed
the Neck
when the larynx and the greater part of the sternocleido-
Dental infections most commonly involve the lower
mastoid muscles have been severed. The common sites for
molar teeth. The infection spreads medially from
the wounds are immediately above and below the hyoid
the mandible into the submandibular and masticatory
bone.
spaces and pushes the tongue forward and upward.
Further spread downward may involve the visceral space
and lead to edema of the vocal cords and airway ob-
Congenital Torticollis
struction.
Most cases of congenital torticollis are a result of excessive
Ludwig’s angina is an acute infection of the sub-
stretching of the sternocleidomastoid muscle during a diffi-
mandibular fascial space and is commonly secondary to
cult labor. Hemorrhage occurs into the muscle and may be
dental infection.
detected as a small, rounded “tumor” during the early weeks
after birth. Later, this becomes invaded by fibrous tissue,
Chronic Infection of the Fascial Spaces of
which contracts and shortens the muscle. The mastoid
the Neck
process is thus pulled down toward the sternoclavicular joint
of the same side, the cervical spine is flexed, and the face
Tuberculous infection of the deep cervical lymph
looks upward to the opposite side. If left untreated, asym-
nodes can result in liquefaction and destruction of one or
metrical growth changes occur in the face, and the cervical
more of the nodes. The pus is at first limited by the in-
vertebrae may become wedge shaped.
vesting layer of the deep fascia. Later, this becomes
eroded at one point, and the pus passes into the less re-
stricted superficial fascia. A dumbbell-shaped abscess is
Spasmodic Torticollis
now present. The clinician is aware of the superficial ab-
Spasmodic torticollis, which results from repeated chronic
scess but must not forget the existence of the deeply
contractions of the sternocleidomastoid and trapezius mus-
placed abscess.
cles, is usually psychogenic in origin. Section of the spinal
part of the accessory nerve may be necessary in severe
Clinical Significance of the
cases.
Triangles of the Neck
Clinical Significance of the Deep
The triangles of the neck (see text Fig. 13-12) assist
the medical examiner in accurately localizing a wound,
Fascia of the Neck
tumor, or swelling. Commit to memory the boundaries
The deep fascia in certain areas of the neck forms distinct
and make a list of the important contents of each
sheets called the investing, pretracheal, and prevertebral
triangle.
192
Chapter 13
esophagus
trachea
carotid sheath
thyroid gland
sternocleidomastoid
muscle
sternothyroid
A
superior belly of
visceral space
sternohyoid muscle
omohyoid muscle
pretracheal
layer of deep
cervical fascia
temporalis
retropharyngeal
space
zygomatic
arch
medial pterygoid
muscle
mylohyoid muscle
masseter
submandibular
muscle
masticatory
space
space
mandible
investing
pretracheal layer
C
layer of deep
B
prevertebral
of deep cervical fascia
cervical fascia
layer of deep
cervical fascia
CD Figure 13-2
A. Cross section of the neck showing the visceral space. B. Sagittal
section of the neck showing the positions of the retropharyngeal and submandibular
spaces. C. Vertical section of the body of the mandible close to the angle showing the
masticatory space.
vessels may be stretched during a severe bout of coughing or
in the later months of pregnancy, which may predispose to
MUSCLES OF THE
the condition. The cause is usually blunt trauma to the ab-
dominal wall, such as a fall or a kick. The symptoms that fol-
ABDOMINAL WALL
low the trauma include midline abdominal pain. An acutely
tender mass confined to one rectus sheath is diagnostic.
Hematoma of the Rectus Sheath
Abdominal Muscles, Abdominotho-
Hematoma of the rectus sheath is uncommon but impor-
racic Rhythm, and Visceroptosis
tant, since it is often overlooked. It occurs most often on the
right side below the level of the umbilicus. The source of
The abdominal muscles contract and relax with respiration,
the bleeding is the inferior epigastric vein or, more rarely,
and the abdominal wall conforms to the volume of the ab-
the inferior epigastric artery (see text Fig. 19-7). These
dominal viscera. There is an abdominothoracic rhythm.
Skeletal Muscles
193
Normally, during inspiration, when the sternum moves for-
culous abscess. Tuberculous disease of the thoracolumbar
ward and the chest expands, the anterior abdominal wall
region of the vertebral column results in the destruction of
also moves forward. If, when the chest expands the anterior
the vertebral bodies, with possible extension of pus laterally
abdominal wall remains stationary or contracts inward, it is
under the psoas fascia (CD Fig. 13-3). From there, the pus
highly probable that the parietal peritoneum is inflamed
tracks downward, following the course of the psoas muscle,
and has caused a reflex contraction of the abdominal
and appears as a swelling in the upper part of the thigh be-
muscles.
low the inguinal ligament. It may be mistaken for a
The shape of the anterior abdominal wall depends on
femoral hernia.
the tone of its muscles. A middle-aged woman with poor ab-
dominal muscles who has had multiple pregnancies is often
incapable of supporting her abdominal viscera. The lower
MUSCLES OF THE
part of the anterior abdominal wall protrudes forward, a con-
dition known as visceroptosis. This should not be confused
with an abdominal tumor such as an ovarian cyst or with the
PELVIS
excessive accumulation of fat in the fatty layer of the super-
ficial fascia.
Pelvic Floor
Muscle Rigidity and Referred Pain
The pelvic diaphragm is a gutter-shaped sheet of muscle
Sometimes it is difficult for a physician to decide whether
formed by the levatores ani and coccygeus muscles and their
the muscles of the anterior abdominal wall of a patient are
covering fasciae (see text Figs. 13-19 and 13-20). From their
rigid because of underlying inflammation of the parietal
origin, the muscle fibers on the two sides slope downward and
peritoneum or whether the patient is voluntarily contracting
backward to the midline, producing a gutter that slopes
the muscles because he or she resents being examined or be-
downward and forward.
cause the physician’s hand is cold. This problem is usually
A rise in the intraabdominal pressure, caused by the
easily solved by asking the patient, who is lying supine on
contraction of the diaphragm and the muscles of the ante-
the examination table, to rest the arms by the sides and draw
rior and lateral abdominal walls, is counteracted by the
up the knees to flex the hip joints. It is practically impossible
contraction of the muscles forming the pelvic floor. By this
for a patient to keep the abdominal musculature tensed
means, the pelvic viscera are supported and do not “drop
when the thighs are flexed. Needless to say, the examiner’s
out” through the pelvic outlet. Contraction of the puborec-
hand should be warm.
talis fibers greatly assists the anal sphincters in maintaining
A pleurisy involving the lower costal parietal pleura
continence under these conditions by pulling the anorectal
causes pain in the overlying skin that may radiate down into
junction upward and forward. During the act of defecation,
the abdomen. Although it is unlikely to cause rigidity of the
however, the levator ani continues to support the pelvic
abdominal muscles, it may cause confusion in making a di-
viscera but the puborectalis fibers relax with the anal
agnosis unless these anatomic facts are remembered:
sphincters.
■ The xiphoid process-T7
Functional Significance of the Pelvic
■ The umbilicus-T10
Floor in the Female
■ The pubis-L1
The female pelvic floor serves an important function dur-
ing the second stage of labor (CD Fig. 13-4). At the pelvic
Surgery and the Tendinous
inlet, the widest diameter is transverse so that the longest
axis of the baby’s head (anteroposterior) takes up the trans-
Intersections of the Rectus
verse position. When the head reaches the pelvic floor, the
gutter shape of the floor tends to cause the baby’s head to
Abdominis Muscle
rotate so that its long axis comes to lie in the anteroposte-
Note that the anterior wall of the rectus sheath is firmly at-
rior position. The occipital part of the head now moves
tached to the tendinous intersections of the rectus abdo-
downward and forward along the gutter until it lies under
minis muscle. The posterior wall of the sheath, however, has
the pubic arch. As the baby’s head passes through the
no attachment to the muscle.
lower part of the birth canal, the small gap that exists in the
anterior part of the pelvic diaphragm becomes enormously
enlarged so that the head may slip through into the per-
Psoas Abscess
ineum. Once the baby has passed through the perineum,
The psoas fascia covers the anterior surface of the psoas
the levatores ani muscles recoil and take up their previous
muscle and can influence the direction taken by a tuber-
position.
194
Chapter 13
A
inguinal ligament
CD Figure 13-3
A. Muscles and
bones forming the posterior abdominal
wall. B. Case of advanced tuberculous
disease of the thoracolumbar region of
the vertebral column. A psoas abscess
is present, and swellings occur in the
right groin above and below the right
B
psoas abscess
inguinal ligament.
Injury to the Pelvic Floor
MUSCLES OF THE
Injury to the pelvic floor during a difficult childbirth can re-
sult in the loss of support for the pelvic viscera leading to
uterine and vaginal prolapse, herniation of the bladder
UPPER LIMB
(cystocele), and alteration in the position of the bladder
neck and urethra, leading to stress incontinence. In the lat-
Rotator Cuff Tendinitis
ter condition, the patient dribbles urine whenever the in-
traabdominal pressure is raised, as in coughing. Prolapse of
The rotator cuff, consisting of the tendons of the subscapu-
the rectum may also occur.
laris, supraspinatus, infraspinatus, and teres minor muscles,
Skeletal Muscles
195
2
1
CD Figure 13-4
Stages in rotation
of the baby’s head during the second
stage of labor. The shape of the
pelvic floor plays an important part in
3
this process.
which are fused to the underlying capsule of the shoulder
joint, plays an important role in stabilizing the shoulder
joint. Lesions of the cuff are a common cause of pain in the
shoulder region. Excessive overhead activity of the upper
limb may be the cause of tendinitis, although many cases
appear spontaneously. During abduction of the shoulder
joint, the supraspinatus tendon is exposed to friction against
130˚
the acromion (CD Fig. 13-5). Under normal conditions, the
amount of friction is reduced to a minimum by the large
subacromial bursa, which extends laterally beneath the del-
toid. Degenerative changes in the bursa are followed by de-
generative changes in the underlying supraspinatus tendon,
and these may extend into the other tendons of the rotator
cuff. Clinically, the condition is known as subacromial bur-
50˚
sitis, supraspinatus tendinitis, or pericapsulitis. It is char-
acterized by the presence of a spasm of pain in the middle
range of abduction (CD Fig. 13-5), when the diseased area
impinges on the acromion.
Rupture of the Supraspinatus
Tendon
CD Figure 13-5
Subacromial bursitis, supraspinatus ten-
In advanced cases of rotator cuff tendinitis, the necrotic
dinitis, or pericapsulitis showing the painful arc in the mid-
supraspinatus tendon can become calcified or rupture. Rup-
dle range of abduction, when the diseased area impinges
ture of the tendon seriously interferes with the normal
on the lateral edge of the acromion.
196
Chapter 13
abduction movement of the shoulder joint. It will be re-
(CD Fig. 13-6). Clinically, the syndrome consists of a burn-
membered that the main function of the supraspinatus mus-
ing pain or “pins and needles” along the distribution of the
cle is to hold the head of the humerus in the glenoid fossa at
median nerve to the lateral three and a half fingers and weak-
the commencement of abduction. The patient with a rup-
ness of the thenar muscles. It is produced by compression of
tured supraspinatus tendon is unable to initiate abduction of
the median nerve within the tunnel. The exact cause of the
the arm. However, if the arm is passively assisted for the first
compression is difficult to determine, but thickening of the
15° of abduction, the deltoid can then take over and com-
synovial sheaths of the flexor tendons or arthritic changes in
plete the movement to a right angle.
the carpal bones are thought to be responsible in many cases.
As you would expect, no paresthesia occurs over the thenar
eminence because this area of skin is supplied by the palmar
Axillary Nerve and the
cutaneous branch of the median nerve, which passes super-
ficially to the flexor retinaculum. The condition is dramati-
Quadrangular Space
cally relieved by decompressing the tunnel by making a
A subglenoid dislocation of the head of the humerus into
longitudinal incision through the flexor retinaculum.
the quadrangular space (see text Fig. 13-24) can cause dam-
age to the axillary nerve, as indicated by paralysis of the del-
Tenosynovitis of the Synovial
toid muscle and loss of skin sensation over the lower half of
the deltoid muscle.
Sheaths of the Flexor Tendons
Tenosynovitis is an infection of a synovial sheath. It most
Carpal Tunnel Syndrome
commonly results from the introduction of bacteria into a
The carpal tunnel, formed by the concave anterior surface of
sheath through a small penetrating wound, such as
the carpal bones and closed by the flexor retinaculum, is
that made by the point of a needle or thorn. Rarely, the
tightly packed with the long flexor tendons of the fingers,
sheath may become infected by extension of a pulp-space
their surrounding synovial sheaths, and the median nerve
infection.
palmaris longus
flexor retinaculum
median nerve
palmar cutaneous branch
palmar cutaneous branch of median nerve
of ulnar nerve
muscles of
muscles of thenar eminence
hypothenar eminence
flexor carpi radialis
ulnar artery
ulnar nerve
ridge of trapezium
flexor digitorum
superficialis
flexor pollicis longus
flexor digitorum
profundus
abductor pollicis longus
hamate
trap
hook of hamate
extensor pollicis brevis
trape-
capitate
zoid
superficial branch
flexor synovial sheath
of radial nerve
extensor carpi ulnaris
radial artery
posterior cutaneous branch of
ulnar nerve
cephalic vein
basilic vein
extensor carpi radialis
extensor digiti minimi
longus and brevis
extensor digitorum
extensor pollicis longus
extensor indicis extensor retinaculum
CD Figure 13-6
Cross section of the hand showing the relation of the tendons, nerves,
and arteries to the flexor and extensor retinacula.
Skeletal Muscles
197
extensor digitorum
axis of
interossei and lumbrical
rotation
muscles
dorsal
extensor
vincula
expansion
flexor digitorum
brevia
profundus
vincula
longa
lumbrical
extensor
interosseous
digitorum
3rd metacarpal
flexor digitorum
superficialis
extensor digitorum
3rd metacarpal
interosseous
lumbrical
flexor digitorum
flexor digitorum
profundus
superficialis
CD Figure 13-7
Insertions of long flexor and extensor tendons in the fingers. Insertions
of the lumbrical and interossei muscles are also shown. The uppermost figure illustrates
the action of the lumbrical and interossei muscles in flexing the metacarpophalangeal
joints and extending the interphalangeal joints.
Infection of a digital sheath results in distension of the
and may compress the blood supply to the tendons that travel
sheath with pus; the finger is held semiflexed and is swollen.
in the vincula longa and brevia (CD Fig. 13-7). Rupture or
Any attempt to extend the finger is accompanied by extreme
later severe scarring of the tendons may follow.
pain because the distended sheath is stretched. As the inflam-
A further increase in pressure can cause the sheath to
matory process continues, the pressure within the sheath rises
rupture at its proximal end. Anatomically, the digital sheath
198
Chapter 13
of the index finger is related to the thenar space, whereas
that of the ring finger is related to the midpalmar space. The
sheath for the middle finger is related to both the thenar and
midpalmar spaces. These relationships explain how infec-
tion can extend from the digital synovial sheaths and involve
the palmar fascial spaces.
In the case of infection of the digital sheaths of the little
finger and thumb, the ulnar and radial bursae are quickly in-
volved. Should such an infection be neglected, pus may
burst through the proximal ends of these bursae and enter
the fascial space of the forearm between the flexor digitorum
A
profundus anteriorly and the pronator quadratus and the in-
terosseous membrane posteriorly. This fascial space in the
extensor expansion
forearm is commonly referred to clinically as the space of
Parona.
Trigger Finger
lumbrical
In trigger finger, there is a palpable and even audible snapping
when a patient is asked to flex and extend the fingers. It is
interosseous
caused by the presence of a localized swelling of one of the
extensor digitorum
long flexor tendons that catches on a narrowing of the fibrous
flexor sheath anterior to the metacarpophalangeal joint. It may
take place either in flexion or in extension. A similar condition
occurring in the thumb is called trigger thumb. The situation
can be relieved surgically by incising the fibrous flexor sheath.
B
Mallet Finger
Avulsion of the insertion of one of the extensor tendons into
the distal phalanges can occur if the distal phalanx is
forcibly flexed when the extensor tendon is taut. The last 20°
of active extension is lost, resulting in a condition known as
mallet finger (CD Fig. 13-8).
C
Boutonnière Deformity
Avulsion of the central slip of the extensor tendon proximal
to its insertion into the base of the middle phalanx results in
a characteristic deformity (CD Fig. 13-8C). The deformity
results from flexing of the proximal interphalangeal joint
and hyperextension of the distal interphalangeal joint. This
injury can result from direct end-on trauma to the finger, di-
rect trauma over the back of the proximal interphalangeal
CD Figure 13-8
A. Posterior view of normal dorsal exten-
joint, or laceration of the dorsum of the finger.
sor expansion. The extensor expansion near the proximal
interphalangeal joint splits into three parts: a central part,
which is inserted into the base of the middle phalanx, and
Dupuytren’s Contracture
two lateral parts, which converge to be inserted into the
base of the distal phalanx. B. Mallet or baseball finger. The
Dupuytren’s contracture is a localized thickening and con-
insertion of the extensor expansion into the base of the dis-
tracture of the palmar aponeurosis (CD Fig.13-9). It com-
tal phalanx ruptured; sometimes a flake of bone on the
monly starts near the root of the ring finger and draws that
base of the phalanx is pulled off. C. Boutonnière deformity.
finger into the palm, flexing it at the metacarpophalangeal
The insertion of the extensor expansion into the base of the
middle phalanx is ruptured. The arrows indicate the direc-
joint. Later, the condition involves the little finger in the
tion of the pull of the muscles and the deformity.
same manner. In long-standing cases, the pull on the fibrous
sheaths of these fingers results in flexion of the proximal
Skeletal Muscles
199
palmar digital artery
palmar digital nerve
fibrous flexor sheath
deep transverse
1st dorsal interosseous
palmar ligament
adductor pollicis
palmar aponeurosis
abductor digiti minimi
flexor digiti minimi
abductor pollicis brevis
flexor pollicis brevis
deep branch of ulnar
nerve and artery
flexor retinaculum
palmaris brevis
ridge of trapezium
extensor pollicis brevis
hook of hamate
abductor pollicis longus
pisiform
palmar cutaneous branch
tubercle of scaphoid
of ulnar nerve
radial artery
flexor carpi ulnaris
ulnar nerve
flexor carpi radialis
ulnar artery
palmar cutaneous branch
CD Figure 13-9
Anterior view
flexor digitorum superficialis
of median nerve
of the palm of the hand. The
median nerve
palmar aponeurosis has been
palmaris longus
left in position.
interphalangeal joints. The distal interphalangeal joints are
lar injections. To avoid injury to the underlying sciatic
not involved and are actually extended by the pressure of the
nerve, the injection should be given well forward on the
fingers against the palm.
upper outer quadrant of the buttock.
Bursitis, or inflammation of a bursa, can be caused by
acute or chronic trauma.
MUSCLES OF THE
Gluteus Maximus and Bursitis
LOWER LIMB
An inflamed bursa becomes distended with excessive
amounts of fluid and can be extremely painful. The bursae as-
sociated with the gluteus maximus are prone to inflammation.
Gluteus Maximus and
Gluteus Medius and Minimus and
Intramuscular Injections
Poliomyelitis
The gluteus maximus is a large, thick muscle with coarse
fasciculi that can be easily separated without damage. The
The gluteus medius and minimus muscles may be para-
great thickness of this muscle makes it ideal for intramuscu-
lyzed when poliomyelitis involves the lower lumbar and
200
Chapter 13
sacral segments of the spinal cord. They are supplied by the
The femoral canal, the compartment for the lymphatic
superior gluteal nerve (L4 and 5 and S1). Paralysis of these
vessels, occupies the medial part of the sheath. It is about 0.5
muscles seriously interferes with the ability of the patient to
in. (1.3 cm) long, and its upper opening is referred to as the
tilt the pelvis when walking.
femoral ring. The femoral septum, which is a condensa-
tion of extraperitoneal tissue, plugs the opening of the
femoral ring.
Quadriceps Femoris as a
A femoral hernia is more common in women than in
men (possibly because of their wider pelvis and femoral
Knee-Joint Stabilizer
canal). The hernial sac passes down the femoral canal,
The quadriceps femoris is an important extensor muscle for
pushing the femoral septum before it. On escaping through
the knee joint. Its tone greatly strengthens the joint; there-
the lower end of the femoral canal, it expands to form a
fore, this muscle mass must be carefully examined when
swelling in the upper part of the thigh deep to the deep fas-
disease of the knee joint is suspected. Both thighs should be
cia. With further expansion, the hernial sac may turn up-
examined, and the size, consistency, and strength of the
ward to cross the anterior surface of the inguinal ligament.
quadriceps muscles should be tested. Reduction in size
The neck of the sac always lies below and lateral to the
caused by muscle atrophy can be tested by measuring the
pubic tubercle. This serves to distinguish it from an in-
circumference of each thigh a fixed distance above the su-
guinal hernia, which lies above and medial to the pubic tu-
perior border of the patella.
bercle. The neck of the sac is narrow and lies at the femoral
The vastus medialis muscle extends farther distally than
ring. The ring is related anteriorly to the inguinal ligament,
the vastus lateralis. Remember that the vastus medialis is the
posteriorly to the pectineal ligament and the superior ramus
first part of the quadriceps muscle to atrophy in knee-joint
of the pubis, medially to the sharp free edge of the lacunar
disease and the last to recover.
ligament, and laterally to the femoral vein. Because of these
anatomic structures, the neck of the sac is unable to expand.
Once an abdominal viscus has passed through the neck into
Rupture of the Rectus Femoris
the body of the sac, it may be difficult to push it up and
The rectus femoris muscle can rupture in sudden violent ex-
return it to the abdominal cavity (irreducible hernia).
tension movements of the knee joint. The muscle belly re-
Furthermore, after the patient strains or coughs, a piece of
tracts proximally, leaving a gap that may be palpable on the
bowel may be forced through the neck, and its blood vessels
anterior surface of the thigh. In complete rupture of the
may be compressed by the femoral ring, seriously impairing
muscle, surgical repair is indicated.
its blood supply (strangulated hernia). A femoral hernia
is a dangerous condition and should always be treated
surgically.
Rupture of the Ligamentum
When considering the differential diagnosis of a
femoral hernia, it is important to consider diseases that may
Patellae
involve other anatomic structures close to the inguinal liga-
This can occur when a sudden flexing force is applied to the
ment. For example:
knee joint when the quadriceps femoris muscle is actively
contracting.
■ Inguinal canal: The swelling of an inguinal hernia lies
above the medial end of the inguinal ligament. Should
the hernial sac emerge through the superficial inguinal
Femoral Sheath and Femoral
ring to start its descent into the scrotum, the swelling will
lie above and medial to the pubic tubercle. The sac of a
Hernia
femoral hernia lies below and lateral to the pubic
The hernial sac descends through the femoral canal within
tubercle.
the femoral sheath.
■ Superficial inguinal lymph nodes: Usually, more than
The femoral sheath is a prolongation downward into the
one lymph node is enlarged. In patients with inflam-
thigh of the fascial lining of the abdomen. It surrounds the
mation of the nodes (lymphadenitis), carefully examine
femoral vessels and lymphatic vessels for about 1 in. (2.5 cm)
the entire area of the body that drains its lymph into
below the inguinal ligament (CD Fig. 13-10). The femoral
these nodes. A small, unnoticed skin abrasion may be
artery, as it enters the thigh below the inguinal ligament, oc-
found. Never forget the mucous membrane of the lower
cupies the lateral compartment of the sheath. The femoral
half of the anal canal—it may have an undiscovered
vein, which lies on its medial side and is separated from it by
carcinoma.
a fibrous septum, occupies the intermediate compartment.
■ Great saphenous vein: A localized dilatation of the ter-
The lymphatics, which are separated from the vein by a
minal part of the great saphenous vein, a saphenous
fibrous septum, occupy the most medial compartment.
varix, can cause confusion, especially because a hernia
Skeletal Muscles
201
inguinal ligament
femoral vein
femoral sheath
femoral canal
femoral artery
pubic tubercle
lymphatic vessel
pectineus
femoral nerve
iliopsoas
fascia transversalis
transversus
extraperitoneal fat
external iliac artery and vein
peritoneum
internal oblique
external oblique
femoral sheath
femoral ring
femoral canal
inguinal ligament
membranous layer
femoral artery
fatty layer
fascia
superficial fascia
iliaca
pubis
femoral canal
lymphatic vessel
deep fascia
lymph node
CD Figure 13-10
Right femoral sheath and its contents.
and a varix increase in size when the patient is asked to
■ Femoral artery: An expansile swelling lying along the
cough. (Elevated intraabdominal pressure drives the
course of the femoral artery that fluctuates in time with
blood downward.) The presence of varicose veins else-
the pulse rate should make the diagnosis of aneurysm of
where in the leg should help in the diagnosis.
the femoral artery certain.
■ Psoas sheath: Tuberculous infection of a lumbar verte-
bra can result in the extravasation of pus down the psoas
Adductor Muscles and
sheath into the thigh (CD Fig. 13-3). The presence of a
swelling above and below the inguinal ligament,
Cerebral Palsy
together with clinical signs and symptoms referred
to the vertebral column, should make the diagnosis
In patients with cerebral palsy who have marked spasticity of
obvious.
the adductor group of muscles, it is common practice to
202
Chapter 13
perform a tenotomy of the adductor longus tendon and to
Tenosynovitis and Dislocation of
divide the anterior division of the obturator nerve. In addi-
tion, in some severe cases the posterior division of the obtu-
the Peroneus Longus and Brevis
rator nerve is crushed. This operation overcomes the spasm
of the adductor group of muscles and permits slow recovery
Tendons
of the muscles supplied by the posterior division of the ob-
turator nerve.
Tenosynovitis (inflammation of the synovial sheaths) can af-
fect the tendon sheaths of the peroneus longus and brevis
muscles as they pass posterior to the lateral malleolus. Treat-
The Adductor Magnus and
ment consists of immobilization, heat, and physiotherapy.
Tendon dislocation can occur when the tendons of per-
Popliteal Aneurysms
oneus longus and brevis dislocate forward from behind the
The pulsations of the wall of the femoral artery against the
lateral malleolus. For this condition to occur, the superior
tendon of adductor magnus at the opening of the adductor
peroneal retinaculum must be torn. It usually occurs in
magnus is thought to contribute to the cause of popliteal
older children and is caused by trauma.
aneurysms.
Gastrocnemius and Soleus
Semimembranosus Bursa Swelling
Muscle Tears
Semimembranosus bursa swelling is the most common
swelling found in the popliteal space. It is made tense by
Tearing of the gastrocnemius or soleus muscles will pro-
extending the knee joint and becomes flaccid when the
duce severe localized pain over the damaged muscle.
joint is flexed. It should be distinguished from a Baker’s
Swelling may be present.
cyst, which is centrally located and arises as a pathologic
(osteoarthritis) diverticulum of the synovial membrane
Ruptured Tendo Calcaneus
through a hole in the back of the capsule of the knee
joint.
Rupture of the tendo calcaneus is common in middle-aged
men and frequently occurs in tennis players. The rupture oc-
curs at its narrowest part, about 2 in. (5 cm) above its inser-
Anterior Compartment of the
tion. A sudden, sharp pain is felt, with immediate disability.
The gastrocnemius and soleus muscles retract proximally,
Leg Syndrome
leaving a palpable gap in the tendon. It is impossible for the
patient to actively plantar flex the foot. The tendon should be
The anterior compartment syndrome is produced by an in-
sutured as soon as possible and the leg immobilized with the
crease in the intracompartmental pressure that results from
ankle joint plantar flexed and the knee joint flexed.
an increased production of tissue fluid. Soft tissue injury
associated with bone fractures is a common cause, and
early diagnosis is critical. The deep, aching pain in the an-
Rupture of the Plantaris Tendon
terior compartment of the leg that is characteristic of this
Rupture of the plantaris tendon is rare, although tearing of
syndrome can become severe. Dorsiflexion of the foot at
the fibers of the soleus or partial tearing of the tendo calca-
the ankle joint increases the severity of the pain. Stretching
neus is frequently diagnosed as such a rupture.
of the muscles that pass through the compartment by pas-
sive plantar flexion of the ankle also increases the pain. As
the pressure rises, the venous return is diminished, thus
Plantaris Tendon and Autografts
producing a further rise in pressure. In severe cases, the ar-
terial supply is eventually cut off by compression, and the
The plantaris muscle, which is often missing, can be used
dorsalis pedis arterial pulse disappears. The tibialis ante-
for tendon autografts in repairing severed flexor tendons to
rior, the extensor digitorum longus, and the extensor hal-
the fingers; the tendon of the palmaris longus muscle can
lucis longus muscles are paralyzed. Loss of sensation is
also be used for this purpose.
limited to the area supplied by the deep peroneal nerve—
that is, the skin cleft between the first and second toes. The
Plantar Fasciitis
surgeon can open the anterior compartment of the leg by
making a longitudinal incision through the deep fascia and
Plantar fasciitis, which occurs in individuals who do a great
thus decompress the area and prevent anoxic necrosis of
deal of standing or walking, causes pain and tenderness of
the muscles.
the sole of the foot. It is believed to be caused by repeated
Skeletal Muscles
203
minor trauma. Repeated attacks of this condition induce os-
inflammation: the bursa over the ischial tuberosity; the
sification in the posterior attachment of the aponeurosis,
greater trochanter bursa; the prepatellar and superficial in-
forming a calcaneal spur.
frapatellar bursae; the bursa between the tendons of inser-
tion of the sartorius, gracilis, and semitendinosus muscles
on the medial proximal aspect of the tibia; and the bursa be-
Clinical Problems Associated with
tween the tendo calcaneus and the upper part of the calca-
neum (long-distance runner’s ankle).
the Arches of the Foot
Two important bursae communicate with the knee
See CD Chapter 12.
joint, and they can become distended if excessive amounts
of synovial fluid accumulate within the joint. The supra-
patellar bursa extends proximally about three fingerbreadths
Bursae and Bursitis in the
above the patella beneath the quadriceps femoris muscle.
The bursa, which is associated with the insertion of the
Lower Limb
semimembranosus muscle, may enlarge in patients with os-
A variety of bursae are found in the lower limb where skin,
teoarthritis of the knee joint.
tendons, ligaments, or muscles repeatedly rub against bony
The anatomic bursae described should not be confused
points or ridges.
with adventitious bursae, which develop in response to ab-
Bursitis, or inflammation of a bursa, can be caused by
normal and excessive friction. For example, a subcutaneous
acute or chronic trauma, crystal disease, infection, or dis-
bursa sometimes develops over the tendo calcaneus in re-
ease of a neighboring joint that communicates with
sponse to badly fitting shoes. A bunion is an adventitial
the bursa. An inflamed bursa becomes distended with ex-
bursa located over the medial side of the head of the first
cessive amounts of fluid. The following bursae are prone to
metatarsal bone.
Clinical Problem Solving Questions
Read the following case histories/questions and give
E. The loss of muscle tone is caused by interruption of
the best answer for each.
a nervous reflex arc.
A woman recently took up employment in a factory.
She is a machinist, and for 6 hours a day she has to
General Muscle Information
move a lever repeatedly, which requires that she extend
In a 63-year-old man, a magnetic resonance imaging
and flex her right wrist joint. At the end of the second
scan of the lower thoracic region of the vertebral
week of her employment, she began to experience pain
column reveals the presence of a tumor pressing on the
over the posterior surface of her wrist and noticed a
lumbar segments of the spinal cord. He has a loss of sen-
swelling in the area.
sation in the skin over the anterior surface of the left
2. The following statements concerning this patient are
thigh and is unable to extend his left knee joint. Exam-
correct except which?
ination reveals that the muscles of the front of the left
A. Extension of the wrist joint is brought about by sev-
thigh have atrophied and have no tone and that the left
eral muscles that include the extensor digitorum
knee jerk is absent.
muscle.
1. The following statements concerning this patient are
B. The wrist joint is diseased.
correct except which?
C. Repeated unaccustomed movements of tendons
A. The tumor is interrupting the normal function of
through their synovial sheaths can produce trau-
the efferent motor fibers of the spinal cord on the left
matic inflammation of the sheaths.
side.
D. The diagnosis is traumatic tenosynovitis of the long
B. The quadriceps femoris muscles on the front of the
tendons of the extensor digitorum muscle.
left thigh are atrophied.
C. The loss of skin sensation is confined to the
Head and Neck Muscles
dermatomes L1, 2, 3, and 4.
D. The absence of the left knee jerk is because of
A 43-year-old woman was seen in the emergency de-
involvement of the first lumbar spinal segment.
partment with a large abscess in the middle of the right
204
Chapter 13
posterior triangle of the neck. The abscess was red, hot,
and fell to the floor, catching her right lumbar region
and fluctuant. The abscess showed evidence that it was
on the edge of the chair.
pointing and about to rupture. The physician decided
5. The following statements about this patient are correct
to incise the abscess and insert a drain. The patient
except which?
returned to the department for the dressings to be
A. A lumbar puncture (spinal tap) should always be
changed 5 days later. She stated that she felt much bet-
performed in back injuries to exclude damage to the
ter and that her neck was no longer painful. However,
spinal cord.
there was one thing that she could not understand. She
B. Anteroposterior and lateral radiographs exclude the
could no longer raise her right hand above her head to
presence of a fracture, especially of a transverse
brush her hair.
process.
3.
The following statements explain the signs and symp-
C. A 24-hour specimen of urine should be examined for
toms in this case, suggesting that the spinal part of the
blood to exclude or confirm injury to the right kidney.
accessory nerve had been incised, except which?
D. Careful examination of the erector spinae muscles
A. To raise the hand above the head, it is necessary for
or quadratus lumborum muscle may reveal extreme
the trapezius muscle, assisted by the serratus ante-
tenderness and therefore injury to these muscles.
rior, to contract and rotate the scapula so that the
E. Examination of the back revealed a large bruised
glenoid cavity faces upward.
area in the right lumbar region, which was ex-
B. The trapezius muscle is innervated by the spinal
tremely tender to touch.
part of the accessory nerve.
C. As the spinal part of the accessory nerve crosses the
Muscles of the Thoracic Wall
posterior triangle of the neck, it is deeply placed, be-
ing covered by the skin, the superficial fascia, the in-
A resident obtained a sample of pleural fluid from a pa-
vesting layer of deep cervical fascia, and the levator
tient’s right pleural cavity. He inserted the needle close
scapulae muscle.
to the upper border of the sixth rib in the anterior axil-
D. The surface marking of the spinal part of the acces-
lary line.
sory nerve is as follows: Bisect at right angles a line
6. Name the muscles that the needle pierced in order to
joining the angle of the jaw to the tip of the mastoid
enter the pleural cavity.
process. Continue the second line downward and
A. Trapezius and latissimus dorsi
backward across the posterior triangle.
B. Trapezius and serratus anterior
E. The knife opening the abscess had cut the accessory
C. Serratus anterior, external intercostal, internal inter-
nerve.
costal, and innermost intercostal
A 46-year-old man was seen in the emergency depart-
D. External intercostal and internal intercostal
ment after being knocked down in a street brawl. He
E. Latissimus dorsi, serratus anterior, and external in-
had received a blow on the head with an empty bottle.
tercostal
On examination, the patient was conscious and had a
large gaping wound on the top of the head.
Abdominal Muscles
4.
Why did the wound in this patient gape wide open
A 75-year-old man with chronic bronchitis noticed that
when he was hit with a blunt object and not a knife?
a bulge was developing in his left groin. On examina-
A. The skin on the top of the head was excessively tight.
tion, an elongated swelling was seen above the medial
B. The blow of the bottle had split the epicranial
end of the left inguinal ligament. When the patient
aponeurosis against the underlying skull and the
coughed, the swelling enlarged but did not descend
tone of the occipitofrontalis muscle had pulled the
into the scrotum. The patient had weak abdominal
skin wound open.
muscles.
C. The subcutaneous tissue of the scalp contains
smooth muscle, which pulled the wound open.
7. The symptoms and signs displayed by this patient can
D. A hematoma was formed beneath the scalp and
be explained by the following statements except which?
forced the wound open.
A. The inguinal swelling was a direct inguinal hernia.
E. The underlying parietal bone of the skull was frac-
B. The cause of the hernia was weak abdominal
tured and forced the wound open.
muscles.
C. The hernial sac was wide and in direct communica-
tion with the peritoneal cavity.
Muscles of the Back
D. A rise in intraabdominal pressure on coughing
A 75-year-old woman was dusting the top of a high
caused the hernial swelling to expand.
closet while balanced on a chair. She lost her balance
E. The swelling did not involve the conjoint tendon.
Skeletal Muscles
205
A 40-year-old woman noticed a painful swelling in her
eminence appeared to be functioning normally, al-
right groin after helping her husband move some heavy
though there was some loss of power compared with the
furniture. On examination, a small tender swelling was
activity of the muscles of the left thenar eminence.
noted in the right groin.
12.
The following statements concerning this patient are
8.
The symptoms and signs displayed by this patient can
correct except which?
be explained by the following statements except which?
A. Altered skin sensation was felt in the skin areas sup-
A. The neck of a femoral hernial sac is situated below
plied by the digital branches of the median nerve.
and medial to the pubic tubercle.
B. The muscles of the thenar eminence showed some
B. A hernial sac formed of parietal peritoneum was
evidence of wasting as seen by flattening of the
forced downward.
thenar eminence.
C. The peritoneum was forced through the right
C. The muscles of the thenar eminence are supplied by
femoral canal.
the recurrent muscular branch of the median nerve.
D. The patient had a right-sided femoral hernia.
D. The median nerve enters the palm through the
E. The excessive exertion caused a rise in intraabdom-
carpal tunnel.
inal pressure.
E. The median nerve occupies a large space between
the tendons behind the flexor retinaculum.
9.
Following a sudden severe blow on the anterior ab-
F. This patient has carpal tunnel syndrome.
dominal wall from the hind leg of a horse, a patient
complained of pain and swelling below the umbilicus.
13.
Following a radical mastectomy operation a woman no-
On examination, extensive bruising of the skin was ob-
ticed that her right shoulder blade projected backwards.
served over the lower part of the right rectus muscle. On
Can you explain this deformity?
gentle palpation, a deep swelling confined to the right
14.
A 40-year-old man visited his physician complaining of
rectus sheath was felt. Given that the deep swelling was
pain of 3 weeks’ duration in his right shoulder. On ex-
due to a collection of blood (hematoma), which blood
amination, the patient could actively abduct his right
vessels were likely to have been ruptured?
shoulder to 50°; thereafter, he experienced severe pain
10.
In a patient with a history of tuberculosis, an angular
that prevented further movement. If the arm was then
kyphosis of the lumbar vertebral column suddenly de-
passively raised above a right angle, it could be held ac-
veloped. On examination, a swelling was found in the
tively without pain in that position. If the patient at-
groin, just below the right inguinal ligament. On deep
tempted to lower the arm, he again experienced severe
palpation of the anterior abdominal wall above the right
pain in the middle range of abduction. What is your di-
inguinal ligament, a further swelling could be felt. Dig-
agnosis?
ital pressure on the first swelling caused expansion of
A 64-year-old man consulted his physician because he
the second swelling and vice versa. What is the diagno-
had noticed during the past 6 months a thickening of
sis? Explain the swelling in anatomical terms.
the skin at the base of his left ring finger. As he de-
scribed it: “There appears to be a band of tissue that is
Pelvic Muscles
pulling my ring finger into the palm.” On examination
of the palms of both hands, a localized thickening of
11. A multiparous 57-year-old woman visited her gynecolo-
subcutaneous tissue could be felt at the base of the left
gist complaining of a “bearing-down” feeling in the
ring and little fingers. The metacarpophalangeal joint
pelvis and of low backache, both of which were worse
of the ring finger could not be fully extended, either ac-
when she was tired. On vaginal examination, the exter-
tively or passively.
nal os of the cervix was found to be located just within
the vaginal orifice. A diagnosis of uterine prolapse was
15.
The following statements concerning this patient are
made. What are the main supports of the uterus?
correct except which?
A. The deep fascia beneath the skin of the palm is
thickened to form the palmar aponeurosis.
Muscles of the Upper Limb
B. The distal end of the aponeurosis gives rise to five
A 50-year-old woman complaining of severe “pins and
slips to the five fingers.
needles” in her right hand and lateral fingers visited her
C. Each slip is attached to the base of the proximal
physician. She said that she had experienced difficulty
phalanx and to the fibrous flexor sheath of each
in buttoning up her clothes when dressing. On physical
finger.
examination the patient pointed to her thumb and in-
D. Fibrous contraction of the slip to the ring finger re-
dex, middle, and ring fingers as the areas where she felt
sulted in permanent flexion of the metacarpopha-
discomfort. No objective impairment of sensation was
langeal joint.
found in these areas. The muscles of the thenar
E. The patient had Dupuytren’s contracture.
206
Chapter 13
Muscles of the Lower Limb
C. A large amount of force would be necessary to re-
store the leg to its original length.
D. The hamstrings and quadriceps femoris muscles
A 54-year-old man was told by his physician to reduce
were responsible for the leg shortening.
his weight. He was prescribed a diet and was advised to
E. The right leg was 2 in. (5 cm) shorter than the left
exercise more. One morning while jogging, he heard a
leg.
sharp snap and felt a sudden pain in his right lower calf.
On examination in the emergency department, the
18.
A 42-year-old woman was seen in the emergency de-
physician noted that the upper part of the right calf was
partment after slipping on some ice on the way to work.
swollen and a gap was apparent between the swelling
She complained of pain on movement of her right an-
and the heel. A diagnosis of rupture of the right Achilles
kle joint. The physician asked the patient to evert her
tendon was made.
right foot. Which of the following muscles everts
the foot?
16.
The following statements concerning this patient are
A. The tibialis anterior muscle
correct except which?
B. The flexor hallucis longus muscle
A. With the patient supine, gentle squeezing of the up-
C. The peroneus longus muscle
per part of the right calf did not produce plantar flex-
D. The tibialis anterior muscle
ion of the ankle joint.
E. The flexor digitorum longus muscle
B. The Achilles tendon is the tendon of insertion of the
gastrocnemius and soleus muscles.
19.
A 61-year-old woman was being examined for os-
C. The Achilles tendon is inserted into the posterior
teoarthritis of the left hip joint by an orthopedic sur-
surface of the talus.
geon. He flexed the left hip joint with the knee flexed.
D. Rupture of the Achilles tendon results in the bellies
What structure normally limits the flexion of this joint
of the gastrocnemius and soleus muscles retracting
with the knee flexed?
upward, leaving a gap between the divided ends of
A. The hamstring muscles
the tendon.
B. The iliofemoral ligament
E. Normally, the gastrocnemius and soleus muscles are
C. The adductor magnus muscle
the main muscles responsible for plantar flexion of
D. The anterior abdominal wall
the ankle joint.
E. The ischiofemoral ligament
A 25-year-old man was admitted to the emergency de-
20.
A physician’s assistant asked a patient to walk up and
partment after an automobile accident. Apart from
down the examining room so that she might study his
other superficial injuries, he was found to have a frac-
gait. Which of the following muscles plays an impor-
ture of the middle third of the right femur.
tant role in lifting the left foot off the ground while
walking?
17.
The following statements concerning this patient are
A. The left gluteus medius muscle
possible except which?
B. The left gluteus maximus muscle
A. The soleus muscle was responsible for the backward
C. The right adductor longus muscle
rotation of the distal fragment.
D. The right gluteus medius muscle
B. A lateral radiograph showed overlap of the frag-
E. None of the above
ments, with the distal fragment rotated backward.
Answers and Explanations
1. D is the correct answer. The patellar tendon reflex
scapulae muscle as it crosses the posterior triangle of the
(knee jerk) involves L2, 3, and 4 segments of the spinal
neck (see text Fig. 13-9).
cord.
4. B is the correct answer. A blunt object forcibly striking
2. B is the correct answer. The wrist joint is not diseased.
the head often splits the epicranial aponeurosis against
This patient has traumatic tenosynovitis of the long ten-
the underlying skull, causing the skin wound to gape
dons of the extensor digitorum muscle.
open as if incised by a knife.
3. C is the correct answer. The spinal part of the accessory
5. A is the correct answer. A lumbar puncture (spinal
nerve, which supplies the sternocleidomastoid and
tap) is not required in cases of simple trauma to the
the trapezius muscles, lies superficial to the levator
back.
Skeletal Muscles
207
6.
C is the correct answer. On the anterior axillary line (a
12.
E is the correct answer. The median nerve occupies a
line extending vertically downward from the lower bor-
small restricted space in the carpal (see CD Fig. 13-6).
der of the pectoralis major muscle) at the level of the
13.
This patient has a winged scapula caused by the paraly-
upper border of the sixth rib, the needle would pierce
sis of the serratus anterior muscle. The nerve supply to
the skin, fascia, the serratus anterior muscle, the exter-
the serratus anterior muscle is the thoracodorsal nerve,
nal intercostal muscle, the internal intercostal muscle,
a branch of the posterior cord of the brachial plexus.
the innermost intercostal muscle, and the parietal
Sometimes during a radical mastectomy operation,
pleura (see text Fig. 3-4).
which involves the clearing out of the lymph nodes and
7.
E is the correct answer. The conjoint tendon, formed
fat in the axilla, the nerve is sacrificed since it may be
by the fusion of the tendons of the internal oblique and
involved in malignant disease (see text Fig. 13-23).
transversus abdominis muscles, greatly strengthens the
14.
This patient had supraspinatus tendinitis. During
posterior wall of the inguinal canal. A weakness of the
the middle range of abduction, the tendon of the
conjoint tendon and the lower abdominal musculature
supraspinatus impinges against the outer border of the
was responsible for the bulge, which constitutes a direct
acromion. Normally, the larger subacromial bursa in-
inguinal hernia.
tervenes and ensures that the movement is relatively
8.
A is the correct answer. The neck of the femoral hernial
free of friction and is painless. In this condition, the
sac is situated below and lateral to the pubic tubercle
bursa has degenerated and the supraspinatus tendon ex-
(see CD Fig. 13-10).
hibits a localized area of collagen degeneration (see
CD Fig. 13-5).
9.
A sudden unexpected blow on the anterior abdominal
wall causes excessive stretching of this structure. In this
15.
B is the correct answer. The distal end of the palmar
case the right inferior epigastric artery, which lies
aponeurosis gives rise to four slips, which pass to the
within the rectus sheath, was ruptured and the bleeding
four medial fingers (see CD Fig. 13-9).
occurred into the sheath. If a person is expecting a
16.
C is the correct answer. The Achilles tendon is inserted
blow, he or she automatically contracts his abdominal
into the posterior surface of the calcaneum (see text
muscles and protects the underlying structures.
Fig. 13-55).
10.
The patient had a tuberculous infection of the lumbar
vertebral column with destruction of the bodies of the
17.
A is the correct answer. The gastrocnemius muscle is
vertebrae, hence the kyphosis. The tuberculous pus ex-
responsible for the backward rotation of the distal frag-
tended laterally and to the right and entered the right
ment of the fractured femur.
psoas fascial sheath. From there, it extended downward
18.
C is the correct answer. The peroneus longus everts the
into the thigh, producing a swelling above and below
foot.
the inguinal ligament. Since the pus in each swelling
was continuous, pressure could be transmitted from
19.
D is the correct answer. Flexion of the hip joint (with
one swelling to the other (see CD Fig. 13-3).
the knee flexed) is limited by the thigh coming in con-
tact with the anterior abdominal wall.
11.
The uterus is mainly supported by the tone of the leva-
tores ani muscles. In addition, the ligaments of the
20.
D is the correct answer. The right gluteus medius and
visceral layer of pelvic fascia, namely, the transverse cer-
the right gluteus minimus tilt the pelvis so that the left
vical, sacrocervical, and pubocervical ligaments, play
lower limb is raised, thus permitting the left foot to be
an important role.
advanced forward clear of the ground.
The Skull, the Brain, the
Meninges, and the Blood
Supply of the Brain Relative
to Trauma and Intracranial
14
Hemorrhage
Chapter Outline
The Skull
213
Cerebral Artery Occlusion
219
Anterior Cerebral Artery Occlusion
219
The Thinnest Part of the Lateral Wall of the Skull
213
Middle Cerebral Artery Occlusion
221
Fractures of the Skull
213
Internal Carotid Artery Occlusion
221
Fractures of the Facial Bones
213
Vertebral Artery Occlusion
221
Rises in Supratentorial Pressure
213
Basilar Artery Occlusion
222
Rises in Subtentorial Pressure
213
Central Branch Artery Occlusion
222
Movements of the Brain Relative to the Skull and
Transient Ischemic Attacks
222
Meninges in Head Injuries
214
Hydrocephalus
222
Intracranial Hemorrhage
215
Hydrocephalus Resulting from Excessive Formation
Computed Tomography Scans of Extradural
of Cerebrospinal Fluid
222
Hydrocephalus Resulting from Blockage of
and Subdural Hematomas
215
Cerebrospinal Fluid Circulation
222
Cerebral Arteriography
216
Hydrocephalus Resulting from Diminished
Congenital Aneurysms
217
Absorption of Cerebrospinal Fluid
222
Subarachnoid Hemorrhage
217
Clinical Problem Solving Questions
222
Cerebral Hemorrhage
217
Answers and Explanations
223
Cerebral Ischemia
219
Rises in Supratentorial Pressure
THE SKULL
The common causes of a rise in supratentorial pressure are
intracerebral hemorrhage, subarachnoid hemorrhage, sub-
The Thinnest Part of the Lateral
dural hemorrhage, epidural hemorrhage, and cerebral
edema. Two forms of caudal herniation of the brain through
Wall of the Skull
the tentorial notch of the tentorium cerebelli can occur as a
result of the raised supratentorial pressure:
The thinnest part of the lateral wall of the skull is where
the anteroinferior corner of the parietal bone articulates
■ Central herniation syndrome: In this syndrome the
with the greater wing of the sphenoid; this point is known
thalamus and midbrain are pushed caudally through the
as the pterion. This is a very important area since it over-
tentorial notch.
lies the anterior division of the middle meningeal artery
■ Uncal herniation syndrome: In this syndrome the uncus
and vein.
of the temporal lobe is displaced medially and pushes the
midbrain against the opposite sharp edge of the tentorial
notch. At the same time, the displaced uncus presses on
Fractures of the Skull
the ipsilateral oculomotor nerve at the notch, resulting in
a sluggishly reactive and dilated pupil (CD Fig. 14-1).
See Chapter 11 of the CD-ROM.
Rises in Subtentorial Pressure
Fractures of the Facial Bones
Posterior cranial fossa lesions such as those in cerebellar
See Chapter 11 of the CD-ROM.
hemorrhage cause a rise in pressure that can directly com-
The Skull, the Brain, the Meninges, and the Blood Supply of the Brain
213
left oculomotor nerve
herniated uncus of
falx cerebri
left cerebral hemisphere
superior
sagittal sinus
left cerebral
hemisphere
straight
sinus
midbrain (cut)
tentorium cerebelli
edge of tentorial
right trochlear nerve
notch on right side
temporal lobe
uncus
CD Figure 14-1
A. Lateral view of the interior of the skull showing the falx cerebri, ten-
torium cerebelli, and brainstem. As the result of abnormal supratentorial pressure, the un-
cus of the left cerebral hemisphere has herniated down through the tentorial notch of the
tentorium cerebelli and is pressing on the left oculomotor nerve. B. The position of the
uncus on the temporal lobe of the left cerebral hemisphere in a normal brain.
press the brainstem or its blood supply. Indirect compres-
sion can follow upward herniation of the cerebellum
Movements of the Brain Relative
through the tentorial notch or downward herniation of the
cerebellar tonsils through the foramen magnum. In the
to the Skull and Meninges in
latter instance the medulla will also be displaced and
pressed upon. The problem can be compounded by pres-
Head Injuries
sure on the cerebral aqueduct in the midbrain or the roof
of the fourth ventricle, producing an acute obstructive
Brain injuries are produced by displacement and distortion of
hydrocephalus.
the neuronal tissues at the moment of impact (CD Fig. 14-2).
214
Chapter 14
trauma due to negative pressure
direct cerebral trauma
direct cerebral trauma
trauma due to
negative pressure
distortion of brainstem
direct cerebellar trauma
A
subdural hemorrhage
epidural hemorrhage
intracerebral hemorrhage
direct cerebral
trauma
secondary trauma due to cerebral
B
C momentum
CD Figure 14-2
A. Mechanisms of acute cerebral injury when a blow is applied to the
lateral side of the head. B. Varieties of intracranial hemorrhage. C. Mechanism of cerebral
trauma following a blow on the chin. The movement of the brain within the skull can also
tear the cerebral veins.
The brain, which is incompressible, may be likened to a log
edge of the falx cerebri; the superior surface of the cerebellum
soaked with water floating in water. The brain is floating in
presses against the inferior surface of the tentorium cerebelli.
the cerebrospinal fluid in the subarachnoid space and is ca-
It follows from these anatomic facts that blows on the
pable of a certain amount of anteroposterior and lateral glid-
front or back of the head lead to displacement of the brain,
ing movement. The anteroposterior movement is limited by
which may produce severe cerebral damage, stretching and
the attachment of the superior cerebral veins to the superior
distortion of the brainstem, and stretching and even tearing
sagittal sinus. In lateral movements, the lateral surface of one
of the commissures of the brain. Blows to the side of the
hemisphere hits the side of the skull, and the medial surface
head produce less cerebral displacement, and the injuries to
of the opposite hemisphere hits the side of the falx cerebri (see
the brain consequently tend to be less severe. The falx cere-
CD Fig. 14-2). In superior movements, the superior surfaces
bri, however, is a tough structure and may cause consider-
of the cerebral hemispheres hit the vault of the skull, and the
able damage to the softer brain tissue in cases where there
superior surface of the corpus callosum may hit the sharp free
has been a severe blow to the side of the head (see CD Fig.
The Skull, the Brain, the Meninges, and the Blood Supply of the Brain
215
14-2). Furthermore, glancing blows to the head may result
Subdural hemorrhage results from tearing of the supe-
in considerable rotation of the brain, causing shearing
rior cerebral veins at their point of entrance into the supe-
strains and distortion, particularly in areas where further ro-
rior sagittal sinus. The cause is usually a blow on the front or
tation is prevented by bony prominences in the anterior and
the back of the head, causing excessive anteroposterior dis-
middle cranial fossae. Brain lacerations are likely to occur
placement of the brain within the skull.
when the brain is forcibly thrown against the sharp edges of
This condition, which is much more common than
bone within the skull—the lesser wing of the sphenoid, for
middle meningeal hemorrhage, can be produced by a sud-
example.
den minor blow. Once the vein is torn, blood under low
When the brain is suddenly given momentum within
pressure begins to accumulate in the potential space be-
the skull, the part of the brain that moves away from the
tween the dura and the arachnoid. In about half the cases
skull wall is subjected to diminished pressure, because
the condition is bilateral.
the cerebrospinal fluid has not had time to accommodate
Acute and chronic forms of the clinical condition oc-
the brain movement (see CD Fig. 14-2). This results in a
cur, depending on the speed of accumulation of fluid in the
suction effect on the brain surface, with rupture of surface
subdural space. For example, if the patient starts to vomit,
blood vessels.
the venous pressure will rise as a result of a rise in the in-
A sudden severe blow to the head, as in an automobile
trathoracic pressure. Under these circumstances, the sub-
accident, may result in damage to the brain at the following
dural blood clot will increase rapidly in size and produce
two sites: (1) at the point of impact and (2) at the pole of the
acute symptoms. In the chronic form, over a course of sev-
brain opposite the point of impact, where the brain is
eral months the small blood clot will attract fluid by osmo-
thrown against the skull wall. This is referred to as contre-
sis so that a hemorrhagic cyst is formed, which gradually
coup injury.
expands and produces pressure symptoms. In both forms the
Movements of the brain relative to the skull and dural
blood clot must be removed through burr holes in the skull.
septa may seriously injure the cranial nerves that are teth-
ered as they pass through the various foramina. This partic-
ularly applies to the long, slender nerves, such as the
COMPUTED
trochlear, abducent, and occulomotor nerves. Furthermore,
the fragile cortical veins that tether the brain and drain into
TOMOGRAPHY
the dural sinuses may be torn, resulting in severe subdural
or subarachnoid hemorrhage. The large arteries found at
the base of the brain are tortuous, and this, coupled with
SCANS OF
their strong walls, explains why they are seldom damaged.
EXTRADURAL AND
Intracranial Hemorrhage
SUBDURAL
Intracranial hemorrhage may result from trauma or cerebral
vascular lesions. Four varieties are considered here: ex-
tradural, subdural, subarachnoid, and cerebral.
HEMATOMAS
Extradural hemorrhage results from injuries to the
meningeal arteries or veins. The most common artery to be
The different appearances of blood clots in these two condi-
damaged is the anterior division of the middle meningeal
tions as seen on computed tomography (CT) scans is related
artery. A comparatively minor blow to the side of the head,
to the anatomy of the area (CD Fig. 14-3). In an extradural
resulting in fracture of the skull in the region of the an-
hemorrhage the blood strips the meningeal layer of the dura
teroinferior portion of the parietal bone, may sever the
from the endosteal layer of dura (periosteum of the skull),
artery. The arterial or venous injury is especially liable to oc-
producing a lens-shaped hyperdense collection of blood that
cur if the artery and vein enter a bony canal in this region.
compresses the brain and displaces the midline structures to
Bleeding occurs and strips the meningeal layer of dura from
the opposite side. The shape of the blood clot is determined
the internal surface of the skull. The intracranial pressure
by the adherence of the meningeal layer of dura to the
rises, and the enlarging blood clot exerts local pressure on
periosteal layer of dura.
the underlying motor area in the precentral gyrus. Blood
In patients with subdural hematoma the blood accu-
may also pass outward through the fracture line to form a
mulates in the extensive potential space between the
soft swelling under the temporalis muscle.
meningeal layer of dura and the arachnoid, producing a
To stop the hemorrhage, the torn artery or vein must be
long, crescent-shaped, hyperdense rim of blood that extends
ligated or plugged. The burr hole through the skull wall
from anterior to posterior along the inner surface of the skull.
should be placed about 1 to 1.5 in. (2.5 to 4 cm) above the
With a large hematoma, the brain sulci are obliterated, and
midpoint of the zygomatic arch.
the midline structures are displaced to the opposite side.
216
Chapter 14
periosteum
periosteal
skull bone
(endosteal)
layer of dura
periosteal
layer of
epidural
blood clot
dura
meningeal
layer of
dura
meningeal
arachnoid
layer of
dura
periosteum
distorted
skull bone
arachnoid
right
ventricle
subdural
blood clot
A
periosteal
deflected
layer of
falx cerebri
dura
meningeal
distorted
layer of
lateral
dura
ventricles
arachnoid
B
CD Figure 14-3
Diagrammatic representation of an extradural hemorrhage and a
subdural hemorrhage. A. Extradural hemorrhage from the middle meningeal artery or
vein on the left side. The hematoma is lens-shaped and occupies the space between the
endosteal layer of dura (periosteum of the skull) and the meningeal layer of dura (true
dura, hence the name extradural). B. Subdural hemorrhage from the cerebral veins at the
site of entrance into the venous sinus on the right side. The hematoma is crescent-shaped
and occupies the space between the meningeal layer of dura and the arachnoid, (i.e.,
beneath the dura).
With the patient under general anesthesia and in the supine
CEREBRAL
position, the head is centered on a radiographic apparatus
that will take repeated radiographs at 2-second intervals.
Both anteroposterior and lateral projections are obtained. A
ARTERIOGRAPHY
radiopaque medium is rapidly injected into the lumen of
the common carotid or vertebral arteries. As the radiopaque
The technique of cerebral arteriography is used to detect ab-
material is introduced, a series of films are exposed. By this
normalities of the cerebral arteries and localization of space-
means the cerebral arteries can be demonstrated and their
occupying lesions such as tumors, blood clots, or abscesses.
position and patency determined (CD Figs. 14-4 to 14-7).
The Skull, the Brain, the Meninges, and the Blood Supply of the Brain
217
CD Figure 14-4
Lateral internal carotid arteriogram.
This technique is not without risk because the insertion of a
needle through the wall of an artery or the manipulation of
Subarachnoid Hemorrhage
a catheter within its lumen may dislodge an atheromatous
Subarachnoid hemorrhage results from leakage or rupture
plaque, leading to cerebral embolism.
of a congenital aneurysm on the circle of Willis or, less com-
monly, from an angioma. The symptoms, which are sudden
Congenital Aneurysms
in onset, include severe headache, stiffness of the neck, and
loss of consciousness. The diagnosis is established by with-
Congenital aneurysms occur most commonly at the site
drawing heavily blood-stained cerebrospinal fluid through a
where two arteries join in the formation of the circle of Willis
lumbar puncture (spinal tap).
(CD Fig. 14-8). At this point, there is a deficiency in the tu-
nica media that so weakens the arterial wall that an aneurysm
develops. The enlarging aneurysm may press on neighboring
Cerebral Hemorrhage
structures, such as the optic, oculomotor, trochlear, and ab-
ducent nerves, and produce signs and symptoms or may sud-
Cerebral hemorrhage is generally caused by rupture of the
denly rupture into the subarachnoid space.
thin-walled lenticulostriate artery, a branch of the middle
218
Chapter 14
posterior parietal artery
middle cerebral artery
cortical (parietal) branches
operculofrontal branch
angular artery
posterior temporal artery
callosomarginal trunk
cortical (frontal)
branches
pericallosal artery
anterior cerebral artery
posterior cerebral
frontopolar artery
artery
posterior auricular artery
ophthalmic artery
internal carotid artery
C1
in cavernous sinus
occipital artery
C2
superficial temporal artery
external carotid artery
maxillary artery
C3
internal carotid artery
ascending palatine artery
C4
in neck
facial artery
bifurcation of common carotid
artery
common carotid artery
lingual artery
superior thyroid artery
x-rays
Cassette
CD Figure 14-5
Main features that can be seen in the arteriogram in CD Fig. 14-4.
The Skull, the Brain, the Meninges, and the Blood Supply of the Brain
219
CD Figure 14-6
Anteroposterior internal carotid arteriogram.
cerebral artery. The hemorrhage involves the vital cortico-
lowing blockage of one of the intracranial vessels will depend
bulbar and corticospinal fibers in the internal capsule and
on the location of the blockage and the status of the collat-
produces hemiplegia on the opposite side of the body. The
eral circulation. The blood supply to the functional areas of
patient immediately loses consciousness, and the paralysis is
the cerebral cortex is shown in text Fig. 14-17.
evident when consciousness is regained.
Cerebral Artery Occlusion
Cerebral Ischemia
Anterior Cerebral Artery Occlusion
It has been pointed out that there are two distinct yet inter-
connected vascular systems supplying the brain. The carotid
If the occlusion of the artery is proximal to the anterior com-
arteries are the major suppliers of the cerebral hemispheres,
municating artery, the collateral circulation is usually ade-
and the basilar and vertebral arteries are the major suppliers
quate to preserve the circulation. Occlusion distal to the
of the brainstem and cerebellum. The neurologic deficit fol-
communicating artery may produce the following signs and
220
Chapter 14
posterior cerebral artery
lenticulostriate artery
posterior parietal artery
pericallosal artery
posterior temporal
artery
anterior choroidal artery
middle meningeal
artery
anterior cerebral artery
styloid process
bifurcation of middle
cerebral artery
internal carotid
artery superior to
cavernous sinus
maxillary artery
internal carotid artery
in cavernous sinus
mastoid process
sphenoid sinuses
superficial
temporal artery
bifurcation of
external carotid
artery
styloid process
internal carotid
internal carotid artery
artery in neck
in carotid canal
in petrous part
of temporal bone
external carotid
artery
maxillary artery in pterygopalatine fossa
mandible
common carotid artery
x-rays
15˚
cassette
CD Figure 14-7
Main features that can be seen in the arteriogram in CD Fig. 14-6.
The Skull, the Brain, the Meninges, and the Blood Supply of the Brain
221
anterior communicating artery
anterior cerebral artery
internal carotid artery
middle cerebral artery
posterior communicating artery
posterior cerebral artery
basilar artery
vertebral artery
CD Figure 14-8
A. The formation of the circle of Willis from the two internal carotid and
two vertebral arteries. B. The distribution of blood from the four main arteries.
symptoms:
tion, the following may be seen:
■ Contralateral hemiparesis and hemisensory loss involv-
■ Loss of vision on the same side as the internal carotid
ing mainly the leg and foot
artery occlusion due to blockage of the ophthalmic artery
■ Inability to identify objects correctly, apathy, and person-
■ Decreased level of consciousnes
ality changes
Vertebral Artery Occlusion
Middle Cerebral Artery Occlusion
This produces a variable clinical picture and may include
Occlusion of the artery may produce the following signs and
the following signs and symptoms:
symptoms.
■ Ipsilateral pain and temperature sensory loss of the face and
■ Contralateral hemiparesis and hemisensory loss
contralateral pain and temperature sensory loss of the body
■ Aphasia if the left hemisphere is affected (rarely if the
■ Ipsilateral loss of the gag reflex, dysphagia, and hoarse-
right hemisphere is affected)
ness as the result of lesions of the nuclei of the glos-
■ Homonymous hemianopia
sopharyngeal and vagus nerves
■ Anosognosia if the right hemisphere is affected (rarely if
■ Vertigo, nystagmus, nausea, and vomiting
the left hemisphere is affected)
■ Ipsilateral Horner’s syndrome
■ Ipsilateral ataxia
Internal Carotid Artery Occlusion
If the lesion is more extensive, the corticospinal tracts
This may produce all the symptoms and signs of anterior
may be involved, producing contralateral hemiparesis of the
and middle cerebral artery occlusion, depending on the de-
body. Contralateral loss of position and vibration sense may
gree of collateral circulation at the circle of Willis; in addi-
also be lost due to damage to the medial lemniscus.
222
Chapter 14
the subarachnoid space and cannot be absorbed by the
Basilar Artery Occlusion
arachnoid villi, the hydrocephalus is the communicating
type (i.e., the cerebrospinal fluid inside the brain commu-
Since this artery gives off numerous branches to the pons,
nicates with that on the outside).
cerebellar peduncles, and cerebellum, total blockage of this
artery can produce lesions of the trigeminal, abducent, and
Hydrocephalus Resulting from
facial nerve nuclei, quadriplegia, and coma (reticular for-
Excessive Formation of
mation). If occlusion is restricted to branches of the basilar
Cerebrospinal Fluid
artery, there may be contralateral hemiparesis, contralateral
sensory loss, or evidence of cerebellar dysfunction.
This condition is rare and may occur when there is a tumor
of the choroid plexuses.
Central Branch Artery Occlusion
Hydrocephalus Resulting from Block-
Small artery occlusion will cause discrete areas of brain
age of Cerebrospinal Fluid Circulation
necrosis. The signs and symptoms produced will obviously
depend on the area involved. For example, a lesion of the in-
An obstruction of the interventricular foramen by a tumor
ternal capsule may result in contralateral hemiplegia.
will block the drainage of the lateral ventricle on that side.
The continued production of cerebrospinal fluid by the
choroid plexus of that ventricle will cause distention of that
Transient Ischemic Attacks
ventricle and atrophy of the surrounding neural tissue.
These are brief, self-limited focal neurologic deficits caused
An obstruction in the cerebral aqueduct in the mid-
by embolic or thrombotic occlusion of arteries supplying the
brain may be congenital or result from inflammation or
brain. The signs and symptoms will depend on the area of
pressure from a tumor. This causes a symmetrical disten-
brain involved.
sion of both lateral ventricles and distension of the third
For further information on the clinical neuroanatomy
ventricle.
of this area, please consult Clinical Neuroanatomy, 6th ed.,
Obstruction of the foramina in the roof of the fourth
by R.S. Snell, Lippincott Williams & Wilkins.
ventricle by inflammatory exudate, or by tumor growth, will
produce symmetrical dilatation of both lateral ventricles
and the third and fourth ventricle.
Hydrocephalus
Sometimes inflammatory exudate secondary to menin-
Hydrocephalus is an abnormal increase in the volume of the
gitis will block the subarachnoid space and obstruct the flow
cerebrospinal fluid within the skull. If hydrocephalus is ac-
of cerebrospinal fluid over the outer surface of the cerebral
companied by raised cerebrospinal fluid pressure, it is
hemispheres. Here, again, the entire ventricular system of
caused by either (1) an abnormal increase in fluid formation,
the brain will become distended.
(2) blockage of the fluid circulation, or (3) diminished ab-
sorption of the fluid. Rarely, hydrocephalus occurs with nor-
Hydrocephalus Resulting from
mal cerebrospinal fluid pressure, and in these patients com-
Diminished Absorption of
pensatory hypoplasia or atrophy of the brain substance exists.
Cerebrospinal Fluid
When the block of the movement of cerebrospinal fluid
lies within the brain, the hydrocephalus is the noncommu-
Interference with the absorption of cerebrospinal fluid at the
nicating type (i.e., the cerebrospinal fluid inside the brain
arachnoid granulations can be caused by inflammatory exu-
does not communicate with that on the outside). If the fluid
date, venous thrombosis or pressure on the venous sinuses,
is able to pass through the roof of the fourth ventricle into
or obstruction of the internal jugular vein.
Clinical Problem Solving Questions
Read the following case histories/questions and give
tion, he was found to have a dough-like swelling over the
the best answer for each.
right temporalis muscle. He also had the signs of right-
sided hemiplegia. Later, a right-sided, fixed, dilated pupil
1. A 36-year-old man was admitted to the emergency de-
developed. A lateral radiograph of the skull showed a lin-
partment unconscious. He had been hit on the side of
ear fracture running downward and forward across the
the head by a taxi while crossing the road. On examina-
right pterion. His coma deepened, and he died 6 hours
The Skull, the Brain, the Meninges, and the Blood Supply of the Brain
223
after the accident. Using your knowledge of anatomy,
as a third-floor window, and yet it is known that if an
make the diagnosis. Explain the clinical findings. How
adult falls from a similar height, it would be fatal. Can
would you explain the homolateral hemiplegia?
you give an anatomic explanation, based on age, for this
difference in survival?
2.
Severe injury to the soft structures within the skull may
follow head trauma. What structures exist within the
6.
Using your knowledge of the anatomic pathways along
skull to limit damage to the cerebral hemispheres and
which the cerebrospinal fluid flows, name the sites at
other parts of the brain? Which blood vessels are dam-
which pathologic blockage may occur.
aged more commonly, the cerebral arteries or the
cerebral veins? Which cranial nerves are likely to be
7.
There are no anastomoses of clinical importance be-
damaged in head injuries? What is the reason for their
tween the terminal end arteries within the brain sub-
susceptibility?
stance, but there are many important anastomoses be-
tween the large arteries, both within and outside the
3.
A 51-year-old woman was examined in the emergency
skull, and these may play a major role in determining
department complaining of a severe headache. She said
the extent of brain damage in cerebral vascular disease.
that the headache had started about 1 hour after she
Name the sites at which important arterial anastomoses
had hit her head on the mantle piece of a fireplace af-
take place.
ter bending down to poke the fire. Four hours later it
was noticed that she was becoming mentally confused
8.
A 35-year-old man was seen in the emergency depart-
and was developing a left-sided hemiplegia on the side
ment with a history of sudden excruciating, generalized
opposite the head injury. Her deep reflexes were exag-
headache while gardening. Ten minutes later the pa-
gerated, and she had a positive Babinski response on the
tient collapsed to the ground in a state of unconscious-
left side. A CT scan demonstrated a right subdural
ness. After being carried indoors and placed on a settee,
hematoma. Explain in anatomic terms the develop-
he regained consciousness but appeared confused. He
ment of a subdural hematoma.
complained of a severe headache and a stiff neck. Phys-
ical examination revealed some rigidity of the neck but
4.
Which part of the base of the skull is most prone to frac-
nothing further. A careful neurologic examination 4
ture? Can you give an anatomic reason for this answer?
days later revealed some loss of tone of the muscles of
5.
It is not uncommon to read in newspapers of the sur-
the left leg. Using your knowledge of anatomy, make a
vival of a baby that has fallen from a great height, such
diagnosis. What caused the neck rigidity?
Answers and Explanations
1. The initial loss of consciousness was due to cerebral
2. The meninges and the cerebrospinal fluid afford a re-
trauma. The swelling over the right temporalis muscle
markable degree of protection to the brain tissue. The
and the radiographic finding of a linear fracture over
dural partitions limit the extent of side-to-side, forward
the anterior inferior angle of the right parietal bone
and backward, and rotation movements of the brain
(pterion) would suggest that the right middle
within the skull.
meningeal artery had been damaged and an extradural
The thin-walled cerebral veins are liable to be damaged
hemorrhage had occurred. Blood had extravasated
during excessive movements of the brain relative to the
through the fracture line into the overlying temporalis
skull, especially at the point where the veins join the
muscle and soft tissue. The right homolateral hemi-
dural venous sinuses. The thick-walled cerebral arteries
plegia was due to the compression of the left cerebral
are rarely damaged.
peduncle against the edge of the tentorial notch of the
tentorium cerebelli. This is unusual. A left hemiplegia
The small-diameter cranial nerves of long length are
due to pressure on the right precentral gyrus is more
particularly prone to damage during head injuries. The
common.
trochlear, abducent, and oculomotor nerves are com-
monly injured.
The right-sided, fixed, dilated pupil was due to the
pressure on the right oculomotor nerve by the hip-
3. A subdural hematoma is an accumulation of blood clot
pocampal gyrus, which had herniated through the ten-
in the interval between the meningeal layer of dura and
torial notch.
the arachnoid mater. It results from tearing of the supe-
224
Chapter 14
rior cerebral veins at their point of entrance into the su-
7.
Once the terminal branches of the cerebral arteries
perior sagittal sinus. The cause is usually a blow to the
enter the brain substance, no further anastomoses oc-
front or the back of the head (which may be minor), re-
cur. Blockage of such end arteries by disease is quickly
sulting in excessive anteroposterior displacement of the
followed by neuronal death and necrosis. The follow-
brain within the skull.
ing important anastomoses exist between the cerebral
arteries: (1) the circle of Willis, (2) anastomoses be-
4.
The middle cranial fossa is the part of the skull most
tween the branches of the cerebral arteries on the sur-
prone to fracture, since it possesses numerous foramina
face of the cerebral hemispheres and the cerebellar
and canals and has air spaces, namely, the sphenoid air
hemispheres, and
(3) anastomoses between the
sinus and the tympanic cavity. The foramen magnum
branches of the internal and external carotid arteries at
in the posterior cranial fossa is very large but its bound-
their origin at the common carotid artery, at the anas-
aries are extremely thick.
tomosis between the branches of the ophthalmic
5.
In infants the skull bones are more resilient than in
artery within the orbit and the facial and maxillary ar-
adults, and they are separated by fibrous sutural liga-
teries, and between the meningeal branches of the in-
ments. In adults the inner table of the skull is particu-
ternal carotid artery and the middle meningeal artery.
larly brittle and the sutural ligaments begin to ossify
8.
This patient had a congenital aneurysm of the anterior
during middle age.
communicating artery. The sudden onset of a severe
6.
The common sites for blockage of the flow of cere-
headache, which is often so dramatic that the patient
brospinal fluid are where the passages are narrowest,
feels as though he has been hit on the head, is char-
namely, the interventricular foramina (between the lat-
acteristic of rupture of a congenital aneurysm into the
eral and third ventricles), the cerebral aqueduct of the
subarachnoid space. The stiff or rigid neck is due to
midbrain, the median aperture, and the lateral aper-
meningeal irritation caused by the presence of blood
tures in the roof of the fourth ventricle. It is possible for
in the subarachnoid space. This patient had no
inflammatory exudate secondary to meningitis or a
evidence of previous pressure on the optic nerve lead-
cerebral tumor to narrow down or even obliterate the
ing to unilateral visual defect, which sometimes oc-
opening in the tentorial notch so that the passage of the
curs when the aneurysm is situated on the anterior
cerebrospinal fluid to the outer surface of the cerebral
part of the circle of Willis. The loss of tone in the left
hemisphere is impeded or stopped. Inflammatory exu-
leg muscles is difficult to explain, although it may be
date may also block the drainage of the fluid into the su-
due to penetration of the hemorrhage into the right
perior sagittal sinus at the arachnoid villi.
cerebral hemisphere.
The Skull, the Brain, the Meninges, and the Blood Supply of the Brain
225
The Cranial Nerves and
Trigeminal Nerve Blocks
15
Chapter Outline
Clinical Testing of the Cranial Nerves
227
Infraorbital Nerve Block
232
Area of Anesthesia
232
Testing the Integrity of the Olfactory Nerve
227
Indications
232
Testing the Integrity of the Optic Nerve
227
Procedure
233
Testing the Integrity of the Oculomotor,
Intraoral Method
233
Extraoral Method
233
Trochlear, and Abducent Nerves
227
Pterygopalatine Ganglion Block
233
Testing the Integrity of the Trigeminal Nerve
227
Area of Anesthesia
233
Testing the Integrity of the Facial Nerve
228
Indications
233
Procedure
234
Testing the Integrity of the Vestibulocochlear
Mandibular Nerve Block
234
Nerve
229
Auriculotemporal Nerve Block
234
Testing the Integrity of the Glossopharyngeal
Area of Anesthesia
234
Nerve
229
Indications
234
Procedure
234
Testing the Integrity of the Vagus Nerve
229
Anatomy of Complications
235
Testing the Integrity of the Accessory Nerve
229
Lingual Nerve and Inferior Alveolar Nerve
Testing the Integrity of the Hypoglossal Nerve
229
Blocks
235
Area of Anesthesia
235
Clinical Anatomy of Trigeminal Nerve
Indications
235
Blocks
229
Procedure
235
Ophthalmic Nerve Block
229
Mental Nerve Block
236
Supraorbital Nerve Block
230
Area of Anesthesia
236
Area of Anesthesia
230
Indications
236
Indications
230
Procedure
236
Procedure
230
Intraoral Method
236
Supratrochlear Nerve Block
231
Extraoral Method
237
Area of Anesthesia
231
Special Areas for Nerve Blocks
237
Indications
231
Tooth Nerve Blocks
237
Procedure
231
Supraperiosteal Infiltration
237
Infratrochlear Nerve Block
232
Dental Nerve Blocks
238
Area of Anesthesia
232
Anesthesia of the Nose
238
Indications
232
Nasal Interior
238
Procedure
232
Nasal Exterior
238
External Nasal Nerve Block
232
Anesthesia of the Ear
240
Area of Anesthesia
232
Anesthesia of the Scalp
240
Indications
232
Procedure
232
Clinical Problem Solving Questions
240
Maxillary Nerve Block
232
Answers and Explanations
242
The Cranial Nerves and Trigeminal Nerve Blocks
227
object. It is important not to miss loss or impairment of
vision in the central area of the field (central scotoma).
CLINICAL TESTING
Blindness in one half of each visual field is called hemi-
anopia. Lesions of the optic tract and optic radiation
OF THE CRANIAL
produce the same hemianopia for both eyes, that is,
homonymous hemianopia. Bitemporal hemianopia is a loss
NERVES
of the lateral halves of the fields of vision of both eyes (i.e.,
loss of function of the medial half of both retinas). This con-
Systematic examination of the 12 cranial nerves is an im-
dition is most commonly produced by a tumor of the pitu-
portant part of the examination of every neurologic patient.
itary gland exerting pressure on the optic chiasma.
It may reveal a lesion of a cranial nerve nucleus or its cen-
tral connections, or it may show an interruption of the lower
Testing the Integrity of the
motor neurons.
The letter symbols commonly used to indicate the
Oculomotor, Trochlear, and
functional components of each cranial nerve are shown in
text Table 15-1. The different components of the cranial
Abducent Nerves
nerves, their functions, and the openings in the skull
through which the nerves leave the cranial cavity are sum-
The oculomotor, trochlear, and abducent nerves innervate
marized in text Table 15-2.
the muscles that move the eyeball. The oculomotor nerve
supplies all the orbital muscles except the superior oblique
and the lateral rectus. It also supplies the levator palpebrae
Testing the Integrity of the
superioris and the smooth muscles concerned with accom-
modation—namely, the sphincter pupillae and the ciliary
Olfactory Nerve
muscle. The trochlear nerve supplies the superior oblique
The olfactory nerve can be tested by applying substances
muscle, and the abducent nerve supplies the lateral rectus.
with different odors to each nostril in turn. It should be re-
To examine the ocular muscles, the patient’s head is
membered that food flavors depend on the sense of smell
fixed and he or she is asked to move the eyes in turn to the
and not on the sense of taste. Fractures of the anterior cra-
left, to the right, upward, and downward, as far as possible in
nial fossa or cerebral tumors of the frontal lobes may pro-
each direction.
duce lesions of the olfactory nerves, with consequent loss of
In complete third-nerve paralysis the eye cannot be
the sense of smell (anosmia).
moved upward, downward, or inward. At rest the eye looks
laterally (external strabismus) because of the activity of the
lateral rectus and downward because of the activity of the su-
Testing the Integrity of the
perior oblique. The patient sees double (diplopia). Droop-
ing of the upper eyelid (ptosis) occurs because of paralysis of
Optic Nerve
the levator palpebrae superioris. The pupil is widely dilated
The optic nerve is evaluated by first asking the patient
and nonreactive to light because of the paralysis of the
whether any changes in eyesight have been noted. The acu-
sphincter pupillae and the unopposed action of the dilator
ity of vision is then tested by using charts with lines of print
pupillae (supplied by the sympathetic). Accommodation of
of varying size. The retinas and optic discs should then be
the eye is paralyzed.
examined with an ophthalmoscope. When examining the
In fourth-nerve paralysis the patient complains of dou-
optic disc, it should be remembered that the intracranial
ble vision on looking straight downward. This is because the
subarachnoid space extends forward around the optic nerve
superior oblique is paralyzed and the eye turns medially as
to the back of the eyeball. The retinal artery and vein run in
the inferior rectus pulls the eye downward.
the optic nerve and cross the subarachnoid space of the
In sixth-nerve paralysis the patient cannot turn the eye-
nerve sheath a short distance behind the eyeball. A rise in
ball laterally. When looking straight ahead, the lateral rectus
cerebrospinal fluid pressure in the subarachnoid space will
is paralyzed, and the unopposed medial rectus pulls the
compress the thin walls of the retinal vein as it crosses the
eyeball medially, causing internal strabismus.
space, resulting in congestion of the retinal veins, edema of
the retina, and bulging of the optic disc (papilledema).
Testing the Integrity of the
The visual fields should then be tested. The patient is
asked to gaze straight ahead at a fixed object with the eye be-
Trigeminal Nerve
ing tested, with the opposite eye covered. A small object is
then moved in an arc around the periphery of the field of vi-
The trigeminal nerve has sensory and motor roots. The sen-
sion, and the patient is asked whether he or she can see the
sory root passes to the trigeminal ganglion, from which
228
Chapter 15
emerge the ophthalmic (V1), maxillary (V2), and mandibu-
The anatomic relationship of this nerve to other struc-
lar (V3) divisions. The motor root joins the mandibular
tures enables a physician to localize lesions of the nerve ac-
division.
curately. If the sixth and seventh nerves are not functioning,
The sensory function can be tested by using a cotton
this would suggest a lesion within the pons of the brain. If
wisp over each area of the face supplied by the divisions of
the eighth and seventh nerves are not functioning, this
the trigeminal nerve (CD Fig. 15-1).
would suggest a lesion in the internal acoustic meatus. If the
The motor function can be tested by asking the patient
patient is excessively sensitive to sound in one ear, the lesion
to clench the teeth. The masseter and the temporalis mus-
probably involves the nerve to the stapedius. Loss of taste
cles, which are innervated by the mandibular division of the
over the anterior two thirds of the tongue implies that the
trigeminal nerve, can be palpated and felt to harden as they
seventh nerve is damaged proximal to the point where it
contract.
gives off the chorda tympani.
To test the facial nerve, the patient is asked to show the
teeth by separating the lips with the teeth clenched, and
Testing the Integrity of the
then to close the eyes. Taste on each half of the anterior two
thirds of the tongue can be tested with sugar, salt, vinegar,
Facial Nerve
and quinine for the sweet, salty, sour, and bitter sensations,
The facial nerve supplies the muscles of facial expression;
respectively.
supplies the anterior two thirds of the tongue with taste
It should be remembered that the part of the facial
fibers; and is secretomotor to the lacrimal, submandibular,
nerve nucleus that controls the muscles of the upper part of
and sublingual glands.
the face receives corticobulbar fibers from both cerebral
V1 (ophthalmic
division)
greater
occipital
nerve (C2)
V2 (maxillary
division)
great auricular
nerve (C2 and C3)
V3 (mandibular
C2 and C3
division)
posterior
primary
rami
C3
anterior primary
rami
C4
CD Figure 15-1
The facial cutaneous distribution of the ophthalmic (V1), maxillary (V2),
and mandibular (V3) divisions of the trigeminal nerve. Note that the skin over the angle of
the jaw is supplied by the great auricular nerve (C2 and C3 segments of the spinal cord).
The Cranial Nerves and Trigeminal Nerve Blocks
229
cortices. Therefore, in patients with an upper motor neuron
muscle, which is supplied by the external laryngeal branch
lesion, only the muscles of the lower part of the face will be
of the superior laryngeal branch of the vagus. Hoarseness or
paralyzed. However, in patients with a lower motor neuron
absence of the voice may occur. Laryngoscopic examination
lesion, all the muscles on the affected side of the face will be
may reveal abductor paralysis.
paralyzed. The lower eyelid will droop, and the angle of the
mouth will sag. Tears will flow over the lower eyelid, and
Testing the Integrity of the
saliva will dribble from the corner of the mouth. The patient
will be unable to close the eye and cannot expose the teeth
Accessory Nerve
fully on the affected side.
The accessory nerve supplies the sternocleidomastoid and
the trapezius muscles by means of its spinal part. The pa-
Testing the Integrity of the
tient should be asked to rotate the head to one side against
resistance, causing the sternocleidomastoid of the opposite
Vestibulocochlear Nerve
side to come into action. Then the patient should be asked
The vestibulocochlear nerve innervates the utricle and sac-
to shrug the shoulders, causing the trapezius muscles to
cule, which are sensitive to static changes in equilibrium;
come into action.
the semicircular canals, which are sensitive to changes in
dynamic equilibrium; and the cochlea, which is sensitive to
Testing the Integrity of the
sound.
Disturbances of vestibular function include dizzi-
Hypoglossal Nerve
ness (vertigo) and nystagmus. The latter is an uncontrol-
lable pendular movement of the eyes. Disturbances of
The hypoglossal nerve supplies the muscles of the tongue.
cochlear function reveal themselves as deafness and ringing
The patient is asked to put out the tongue, and if a lesion
in the ears (tinnitus). The patient’s ability to hear a voice or
of the nerve is present, it will be noted that the tongue
a tuning fork should be tested, with each ear tested
deviates toward the paralyzed side (CD Fig. 15-2). This
separately.
can be explained as follows. One of the genioglossus mus-
cles, which pull the tongue forward, is paralyzed on the af-
fected side. The other, normal genioglossus muscle
Testing the Integrity of the
pulls the unaffected side of the tongue forward, leaving the
paralyzed side of the tongue stationary. The result is the
Glossopharyngeal Nerve
tip of the tongue’s deviation toward the paralyzed side.
The glossopharyngeal nerve supplies the stylopharyngeus
In patients with long-standing paralysis, the muscles on the
muscle and sends secretomotor fibers to the parotid gland.
affected side are wasted, and the tongue is wrinkled on
Sensory fibers innervate the posterior one third of the
that side.
tongue.
The integrity of this nerve may be evaluated by testing
the patient’s general sensation and that of taste on the poste-
CLINICAL
rior third of the tongue.
ANATOMY OF
Testing the Integrity of the
Vagus Nerve
TRIGEMINAL
The vagus nerve innervates many important organs, but the
NERVE BLOCKS
examination of this nerve depends on testing the function of
the branches to the pharynx, soft palate, and larynx. The
pharyngeal reflex may be tested by touching the lateral wall
of the pharynx with a spatula. This should immediately
Ophthalmic Nerve Block
cause the patient to gag—that is, the pharyngeal muscles
will contract.
The terminal branches of the ophthalmic division of the
The innervation of the soft palate can be tested by ask-
trigeminal nerve that emerge onto the face and nose include
ing the patient to say “ah.” Normally, the soft palate rises
the supraorbital, supratrochlear, infratrochlear, external
and the uvula moves backward in the midline.
nasal, and lacrimal nerves (CD Fig. 15-3). The latter nerve
All the muscles of the larynx are supplied by the recur-
gives off only a few branches to the skin and is seldom
rent laryngeal branch of the vagus, except the cricothyroid
blocked.
230
Chapter 15
right
hypoglossal nerve
A
B
cut right hypoglossal
intact hypoglossal
nerve
nerve
CD Figure 15-2
Diagrammatic rep-
right half
resentation of the action of the right
of tongue
and left genioglossus muscles of the
atrophied
tongue. A. The right and left muscles
contract equally together and as a re-
C
D
sult (B) the tip of the tongue is pro-
truded in the midline. C. The right
hypoglossal nerve (which innervates
the genioglossus muscle and the in-
trinsic tongue muscles on the same
side) is cut and as a result the right
side of the tongue is atrophied and
wrinkled. D. When the patient is
asked to protrude the tongue, the tip
genioglossus
points to the side of the nerve lesion.
E. The origin and insertion and direc-
muscle
tion of pull of the genioglossus mus-
E
cle.
Supraorbital Nerve Block
This involves the following:
Area of Anesthesia
supraorbital nerve
Skin of the upper eyelid, the forehead, and the scalp as far
supratrochlear nerve
back as the vertex (CD Fig. 15-4)
lacrimal nerve
infratrochlear nerve
Indications
Repair of lacerations of the upper eyelid, forehead, and scalp
external nasal nerve
Procedure
The supraorbital nerve emerges from the orbital cavity in the
same vertical plane as the pupil when the patient is looking
CD Figure 15-3
Anterior view of the skull showing the
straight ahead (see CD Fig. 15-4). If the nerve passes through
branches of the ophthalmic (V1) division of the trigeminal
nerve emerging onto the face.
the supraorbital notch, this can easily be palpated on the
The Cranial Nerves and Trigeminal Nerve Blocks
231
supratrochlear nerve
supraorbital nerve
infratrochlear nerve
external nasal nerve
supratrochlear area
supraorbital
area
site for injection of
supraorbital nerve
site for injection of
infratrochlear
supratrochlear nerv
area
external nasal
site for injection of
area
infratrochlear nerve
site for injection of
external nasal nerve
CD Figure 15-4
Supraorbital, supratrochlear, infratrochlear, and external nasal nerve
blocks. A. The positions of the nerves on the face; the supraorbital nerve emerging from
the orbital cavity in the same vertical plane as the pupil. B. The areas of skin anesthetized
by blocking these nerves. C. Sites where the nerves may be blocked. The supraorbital and
supratrochlear nerves may be blocked by raising a horizontal wheal of anesthetic solution
above the orbital margin.
supraorbital margin, which is the site for injection. If the
Indications
notch is a foramen, however, it is small and difficult to feel,
Repair of lacerations of the medial end of the eyelid and the
and the needle is inserted into the skin over the supraorbital
forehead close to the midline
margin in line with the pupil.
Supratrochlear Nerve Block
Procedure
This involves the following:
The supratrochlear nerve winds around the supraorbital
margin about a fingerbreadth medial to the supraorbital
Area of Anesthesia
nerve. The needle is inserted at the point where the
Skin of the upper eyelid and the lower forehead close to the
bridge of the nose meets the supraorbital margin (see CD
midline (see CD Fig. 15-4)
Fig. 15 -4).
232
Chapter 15
Infratrochlear Nerve Block
Procedure
This involves the following:
The external nasal nerve is blocked at the point where it
emerges between the nasal bone and the upper lateral nasal
Area of Anesthesia
cartilage (see CD Fig. 15-4).
Skin of the medial ends of the eyelids and the side of the root
of the nose (see CD Fig. 15-4)
Maxillary Nerve Block
This block is not used in emergency medicine. The infraor-
Indications
bital nerve, which is a continuation of the maxillary nerve
Repair of lacerations of the medial eyelids and the root of
onto the face, is commonly blocked. Occasionally, the
the nose
pterygopalatine ganglion is blocked.
Procedure
Infraorbital Nerve Block
The infratrochlear nerve emerges from the orbital cavity at
This involves the following:
the junction of the superior and medial walls, which is the
site for injection (see CD Fig. 15-4).
Area of Anesthesia
External Nasal Nerve Block
Skin of the lower eyelid, the lateral nose, the cheek, and
This involves the following:
the skin and mucous membrane of the upper lip and the
upper gingiva. Since the anesthetic agent also blocks the an-
Area of Anesthesia
terior and middle superior alveolar nerves, the upper
Skin of the side of the nose down as far as the tip (see CD
incisor, canine, and premolar teeth are also affected (CD
Fig. 15-4)
Fig. 15-5).
Indications
Indications
Repair of lacerations of the skin of the nose
Lacerations of the cheek, side of the nose, and the upper lip
trigeminal nerve
foramen rotundum
maxillary nerve (V2) in
zygomatic arch
pterygopalatine fossa
(partially removed
for clarity)
lateral
pterygoid
infraorbital nerve
plate
anterior superior alveolar nerve
middle superior alveolar nerve
pterygopalatine ganglion
in pterygopalatine fossa
posterior superior
alveolar nerve
mandibular notch
CD Figure 15-5
Lateral view of the skull showing the maxillary (V2) division of the
trigeminal nerve leaving the trigeminal ganglion and passing forward to become the infra-
orbital nerve, which emerges on the face. Note the location of the pterygopalatine gan-
glion (parasympathetic) in the pterygopalatine fossa. Note also the sensory innervation of
the teeth of the upper jaw.
The Cranial Nerves and Trigeminal Nerve Blocks
233
Procedure
and is directed upward and outward toward the foramen
(see CD Fig. 15-6).
The infraorbital nerve emerges from the infraorbital
foramen as a direct continuation of the maxillary nerve
Pterygopalatine Ganglion Block
(CD Fig. 15-6). The opening of the foramen is situated about
1 cm below the midpoint of the lower border of the orbit and
The pterygopalatine ganglion is a small parasympathetic
faces downward and medially.
ganglion and is suspended from the lower border of the max-
illary nerve in the pterygopalatine fossa (CD Fig. 15-7). Pass-
Intraoral Method
ing through the ganglion without interruption are the sen-
With the index finger of the left hand palpating the infraor-
sory fibers from the orbit, the nose, the hard and soft palate,
bital foramen through the skin of the cheek and serving as a
the gums, and the tonsillar region of the pharynx.
guide, the needle is inserted into the reflection of the mu-
cous membrane from the upper lip onto the gingiva (see
Area of Anesthesia
CD Fig. 15-6). The site for the needle insertion is just pos-
The lower nasal cavity, hard and soft palates, the upper gum,
terior to the canine tooth and is directed upward to the
the teeth of the upper jaw, and the tonsillar region of the
infraorbital foramen.
pharynx
Extraoral Method
Indications
The infraorbital foramen is palpated below the lower mar-
gin of the orbit, and the needle is inserted through the skin
Repair of lacerations involving the palate
infraorbital nerve
CD Figure 15-6
Infraorbital nerve block. A.
Extraoral method shows the infraorbital nerve
emerging from the infraorbital foramen. The
infraorbital foramen lies on the same vertical
line that passes through the supraorbital
notch, the mental foramen, and the first pre-
molar tooth. The blocking needle is inserted in
the direction of the infraorbital foramen just
below the lower margin of the orbit. B. The
area of skin anesthetized by blocking the infra-
infraorbital
orbital nerve. C. Intraoral method. The needle
nerve area
is inserted into the reflection of the mucous
membrane from the upper lip onto the gingiva
just posterior to the canine tooth and is di-
rected toward the infraorbital foramen.
234
Chapter 15
maxillary nerve
nasal nerves
trigeminal ganglion
pterygopalatine
ganglion in
pterygopalatine
nasopalatine
fossa
nerve
greater palatine
nerve emerging
from greater
pharyngeal nerve
palatine foramen
lesser palatine nerve
nasopalatine
nerves
CD Figure
15-7
Blocking the ptery-
gopalatine ganglion. A. Lateral view of the
greater palatine nerve
skull showing the insertion of the needle
into the greater palatine foramen in order
upper 3rd
to block the ganglion. B. The undersurface
molar tooth
of the palate showing the position of the
lesser palatine nerve
greater
greater palatine foramen in relation to the
palatine
upper third molar tooth and the soft
foramen
palate. Note the distribution of the
soft palate
branches of the maxillary nerve through
uvula
the ganglion to the walls of the nose and
the palate.
Procedure
Auriculotemporal Nerve Block
The ganglion and, therefore, the sensory fibers may be
This involves the following:
blocked by inserting a long-angled needle into the
greater palatine foramen with the mouth wide open (see CD
Area of Anesthesia
Fig. 15-7). The foramen is located at the posterior portion of
The external auditory meatus, the tympanic membrane, the
the hard palate just medial to the gumline of the third molar
upper part of the auricle, and the scalp in the temporal re-
tooth. The greater palatine foramen leads superiorly into the
gion (CD Fig. 15-8)
pterygopalatine fossa. Injection of the anesthetic blocks the
greater and lesser palatine nerves, the orbital nerves, the nasal
Indications
nerves, and the pharyngeal nerves.
Repair of lacerations of the auricle and scalp
Mandibular Nerve Block
Procedure
This block is rarely used. However, the auriculotemporal
nerve, the lingual nerve, and the inferior alveolar nerve,
The auriculotemporal nerve is easily blocked as it ascends in
which are branches of the mandibular nerve, are commonly
front of the auricle over the posterior root of the zygoma, be-
blocked.
hind the superficial temporal artery (see CD Fig. 15-8).
The Cranial Nerves and Trigeminal Nerve Blocks
235
auriculotemporal
nerve area
superficial
temporal
auriculotemporal
artery
nerve
tragus
head of
mandible
superficial
temporal
auriculotemporal
artery
nerve
zygomatic
arch
CD Figure 15-8
Blocking the au-
riculotemporal nerve. A. The rela-
tionship of the auriculotemporal
nerve to the superficial temporal
head of
site for injection
artery and the tragus of the ear.
mandible
Note the area of skin supplied by
this sensory nerve. The needle is in-
serted just behind the pulsating su-
perficial temporal artery and in
front of the tragus; the needle is di-
rected horizontally medially. B. The
surface marking of the auriculotem-
poral nerve and its relationship to
the superficial temporal artery and
the temporomandibular joint. X
marks the site for injection.
Anatomy of Complications
and the lower gums. The inferior alveolar nerve supplies the
The superficial temporal artery may be pierced if the needle
lower teeth and gums and the skin of the lower lip and chin.
is inserted too far anteriorly.
Indications
Lingual Nerve and Inferior Alveolar
Repair of lacerations of the tongue, floor of the mouth, and
Nerve Blocks
lower lip and chin
These involve the following:
Procedure
Area of Anesthesia
Both the lingual and inferior alveolar nerves may be blocked
The lingual nerve supplies the mucous membrane of the an-
as they pass downward and forward in the infratemporal
terior two thirds of the tongue and the floor of the mouth (taste
fossa on the lateral surface of the medial pterygoid muscle
is supplied by the chorda tympani branch of the facial nerve),
and on the medial surface of the ramus of the mandible
236
Chapter 15
(CD Fig. 15-9). With the patient’s mouth wide open, the an-
Indications
terior border of the ramus of the mandible is palpated just
Repair of lacerations of the lower lip
above the third molar tooth. The blocking needle is inserted
above the palpating finger and between the mucosa and the
Procedure
inner surface of the ramus of the mandible, and the barrel
of the syringe lies in line with the interval between the
The mental nerve may be blocked as it emerges from the
bicuspids on the opposite side of the mandible (see CD Fig.
mental foramen on the body of the mandible (CD Fig. 15-
15-9). The needle is advanced posteriorly and slightly supe-
10). The foramen lies on the same vertical line that passes
riorly until the tip lies in close proximity to the mandibular
through the supraorbital notch, the infraorbital foramen,
foramen. The anesthetic solution will infiltrate around the
and the first premolar tooth.
nerves.
Intraoral Method
Mental Nerve Block
The left index finger palpates the position of the mental
foramen. The needle is inserted through the reflexion of the
This involves the following:
mucous membrane from the lower lip onto the gum
between the apices of the premolar teeth (see CD Fig. 15-
Area of Anesthesia
10). The point of the needle is directed toward the mental
The lower lip and gums
foramen.
mandibular foramen
buccal nerve
lingual nerve
inferior alveolar
nerve
mandibular nerve
(V3)
nerve to the mylohyoid
and the anterior belly
of the digastric
inferior
alveolar
mental nerve
nerve
emerging from
the mental foramen
CD Figure 15-9
Lingual and inferior alveolar
nerve blocks. A. The location of the buccal, lin-
gual, and inferior alveolar nerves in relation to
the mandible. B. The needle is inserted just
above the lower third molar tooth and directed
between the mucosa and the inner surface of
the ramus of the mandible; the barrel of the sy-
ringe lies in line with the interval between the
bicuspids on the opposite side of the
mandible. The needle is advanced posteriorly
and slightly superiorly until the tip lies in close
proximity to the mandibular foramen.
The Cranial Nerves and Trigeminal Nerve Blocks
237
supraorbital notch for
supraorbital nerve
infraorbital foramen
for infraorbital nerve
mental foramen
for mental nerve
CD Figure 15-10
Mental nerve and
tooth nerve blocks. A. Extraoral mental
nerve block. The surface marking of the
mental nerve as it emerges from the
mental foramen. The mental foramen
lies on the same vertical plane as the
supraorbital notch, the pupil (when the
mental nerve
patient is looking straight ahead), the in-
area
fraorbital foramen, and the first premo-
lar tooth. The mental foramen is pal-
pated, and the needle is inserted through
alveolar bone
the skin and is directed toward the fora-
alveolar nerve
periosteum
men. B. Area of skin anesthesia pro-
apical foramen
duced by blocking the mental nerve. C.
Intraoral mental nerve block. The needle
mucous membrane
pupal sensory
is inserted through the reflection of the
nerve
mucous membrane between the apices
of the premolar teeth and is directed to-
ward the mental foramen. D. Suprape-
riosteal infiltration. Needle is inserted
through the mucous membrane with the
bevel against the periosteum and is ad-
vanced until it reaches the level of the
apex of the tooth.
Extraoral Method
anesthetic diffuses through the periosteum and the alveo-
The mental foramen is palpated, and the needle is inserted
lar bone to reach the dental nerve fibers entering the
through the skin. When the mandible is contacted with the
apices of the dental roots; it also reaches the nerves sup-
needle, the point is directed toward the mental foramen (see
plying the mucoperiosteum of the gums and the periodon-
CD Fig. 15-10).
tal membrane.
The labiogingival or buccogingival folds, where the
mucous membrane lining the lips or cheek are reflected
Special Areas for Nerve Blocks
onto the gums, are identified. This may be accomplished in
the maxilla by pulling the upper lip downward, and in the
Tooth Nerve Blocks
case of the mandible by pulling the lower lip upward. At the
point where the mucous membrane becomes fused with the
Two techniques are commonly used—supraperiosteal
periosteum to form the mucoperiosteum of the gum, the
infiltration and dental nerve blocks.
needle is inserted with the bevel against the periosteum (see
CD Fig. 15-10). The needle is advanced until it reaches the
Supraperiosteal Infiltration
level of the apex of the root of the tooth, and the anesthetic
This technique is commonly used in an emergency for the
solution is injected. If anesthesia is not produced, it may be
relief of toothache. The anesthetic solution is applied di-
necessary to repeat the injection on the palatal surface of the
rectly to the outer surface of the periosteum opposite the
gums. Failure to produce an adequate nerve block may be
apices of the roots of the teeth (see CD Fig. 15-10). The
due to the needle tip being inserted too far away from the
238
Chapter 15
apex of the tooth—that is, too far away from the periosteum
Anesthesia of the Nose
or too far above or below the tooth apex. The technique is
This involves the following:
less successful for mandibular teeth because of the density
of the bone structure of the mandible.
Nasal Interior
The upper teeth are innervated by the anterior, middle,
and superior alveolar branches of the maxillary division of
The lateral wall of the nose is innervated by the anterior eth-
the trigeminal nerve. The buccal nerve, a branch of the
moidal branch of the nasociliary branch of the ophthalmic
mandibular division of the trigeminal nerve, supplies the
division of the trigeminal nerve, from branches of the max-
lateral surface of the gum and the greater palatine and the
illary division of the trigeminal nerve, and from the olfac-
nasopalatine nerves, from the maxillary nerve, supply the
tory nerve. The nasal septum is innervated by branches of
medial surface of the gum.
the anterior ethmoidal nerve, by branches of the maxillary
The lower teeth are innervated by the inferior alveolar
nerve, and from the olfactory nerve.
nerve, a branch of the mandibular division of the trigeminal
Analgesia of the mucous membrane can easily be ob-
nerve. The buccal nerve supplies the lateral surface of the
tained by placing pledgets soaked in local anesthetic in the
gums, and the lingual nerve, a branch of the mandibular
nose between the conchae and the septum for 5 to 10 minutes.
nerve, supplies the medial surface.
Nasal Exterior
Dental Nerve Blocks
The skin of the nose is innervated by the supratrochlear and
For the maxillary teeth, the anterior and middle superior
infratrochlear branches of the ophthalmic division of the
alveolar nerves are blocked along with the infraorbital
trigeminal nerve and the infraorbital nerve, a continuation
nerve as described on page 232 of the CD. For the
of the maxillary division of the trigeminal nerve (CD Fig.
mandibular teeth, the inferior alveolar nerve is blocked as
15-11). Skin analgesia is obtained by infiltrating first the
described on page 235 of the CD.
base of the nose and then the nasofacial groove, thus
supratrochlear
nerve (V1)
infratrochlear
nerve (V1)
infraorbital
x
nerve (V2)
x
x
external nasal
x
x
nerve (V1)
CD Figure 15-11
Anesthesia of the external nose. A. The sensory nerves that supply the skin
of the nose emerging from the skull. B. The extent of the skin supplied by these nerves. C. The
sites (X) where the needle is introduced to produce anesthesia over the area shown in B.
The Cranial Nerves and Trigeminal Nerve Blocks
239
auricular branch
of the vagus (X)
auriculotemporal nerve (V3)
A
lesser occipital
nerve (C2)
greater auricular
nerve (C2, C3)
X
X
X
CD Figure 15-12
Ear nerve blocks. A.
The sensory innervation of the auricle;
note the auricular branch of the vagus
B
X
nerve that supplies part of the external
X
auditory meatus. B. The sites (X) at
which multiple subcutaneous injec-
tions may be made circumferentially
around the auricle to block the sensory
X
nerves. The external auditory meatus
may be anesthetized by using a four-
X
quadrant block (dots).
supratrochlear nerve (V1)
supraorbital nerve (V1)
zygomaticotemporal
nerve (V2)
external occipital
protuberance
greater occipital nerve (C2)
lesser occipital nerve (C2)
auriculotemporal nerve (V3)
CD Figure 15-13
Scalp nerve block. A subcutaneous infiltration with anesthetic solution
is made around the circumference of the head from just above the eyebrows to the region
of the external occipital protuberance.
240
Chapter 15
blocking the terminal branches of the ophthalmic and max-
Anesthesia of the Scalp
illary nerves (see CD Fig. 15-11).
The anterior part of the scalp extending back as far as the
vertex is innervated by the supraorbital and supratrochlear
Anesthesia of the Ear
branches of the ophthalmic division of the trigeminal nerve
The auricle is innervated by the greater auricular nerve (C2
(CD Fig. 15-13). The posterior part of the scalp is inner-
and C3), a branch of the cervical plexus (CD Fig. 15-12).
vated by the greater occipital nerve (C2) and the lesser oc-
This nerve mainly supplies the skin on the medial and lateral
cipital nerve (C2). The lateral part of the scalp is supplied by
surfaces of the inferior part of the auricle. The
the auriculotemporal branch of the mandibular division of
auriculotemporal branch of the mandibular division of the
the trigeminal nerve. A small area over the temple is sup-
trigeminal nerve supplies the lateral and upper part of the au-
plied by the zygomaticotemporal nerve from the maxillary
ricle. The lesser occipital nerve (C2) may also supply a small
division of the trigeminal nerve.
area on the medial surface. The external auditory meatus is
A subcutaneous infiltration with anesthetic solution is
also innervated by the auricular branch of the vagus nerve.
made around the circumference of the head from just
Anesthesia of the skin is obtained by multiple subcuta-
above the nose and eyebrows to the ear and back to the ex-
neous injections along a line that is continued circumferen-
ternal occipital protuberance (see CD Fig. 15-13). A large
tially around the auricle (see CD Fig. 15-12). The external
volume of anesthetic is required to completely anesthetize
auditory meatus may be anesthetized by using a four-quad-
the scalp.
rant block of the canal; in addition, several drops of anes-
thetic solution may be instilled into the canal to anesthetize
the tympanic membrane.
Clinical Problem Solving Questions
Read the following case histories/questions and give
ing the physical examination the patient was asked to pro-
the best answer for each.
trude his tongue, which deviated to the left.
2. The following statements would explain the physical
A 73-year-old woman visited her physician because she had
signs in this patient except which?
noticed that the right side of her face was sagging downward.
A. The genioglossus muscles are responsible for pro-
She first noticed the condition on waking up two mornings
truding the tongue.
ago. Otherwise she felt very well. On examination the pa-
B. The genioglossus muscle is supplied by the glos-
tient had a complete right-sided facial paralysis, the right
sopharyngeal nerve.
lower eyelid was drooping, and the right angle of the mouth
C. Paralysis of the left genioglossus muscle permitted
was sagging. A diagnosis of Bell’s palsy was made.
the right genioglossus to pull the tongue forward and
1. Further examination of this patient demonstrated the
turned the tip to the left side.
following signs and symptoms except which?
D. The hypoglossal nerve descends in the neck be-
A. Tears tended to flow easily over the right lower eyelid.
tween the internal carotid artery and the internal
B. Saliva dribbled from the right corner of her mouth.
jugular vein.
C. The patient was unable to close her right eye com-
E. At about the level of the tip of the greater cornu of
pletely.
the hyoid bone the hypoglossal nerve turns forward
D. The patient was unable to expose the teeth fully on
and crosses the internal and external carotid arteries
the right side of her mouth.
and the lingual artery to enter the tongue.
E. The muscles on the right side of her forehead
F. The point of the knife blade severed the left hy-
worked perfectly normally when she was asked to
poglossal nerve.
raise her right eyebrow.
A 43-year-old woman was seen in the emergency depart-
A 17-year-old boy was seen in the emergency department af-
ment with a large abscess in the middle of the right posterior
ter receiving a stab wound at the front of the neck. The knife
triangle of the neck. The abscess was red, hot, and fluctuant.
entrance wound was located on the left side of the neck just
The abscess showed evidence that it was pointing and about
lateral to the tip of the greater cornu of the hyoid bone. Dur-
to rupture. The physician decided to incise the abscess and
The Cranial Nerves and Trigeminal Nerve Blocks
241
insert a drain. The patient returned to the department for
experienced, the patient mapped out the skin area over the
the dressings to be changed 5 days later. She stated that she
right side of the lower jaw extending backward and upward
felt much better and that her neck was no longer painful.
over the side of the head to the vertex.
However, there was one thing that she could not under-
5. The following signs and symptoms in this patient
stand. She could no longer raise her right hand above her
strongly suggest a diagnosis of trigeminal neuralgia
head to brush her hair.
except which?
3. The following statements explain the signs and symp-
A. The skin area where the patient experienced the
toms in this case, suggesting that the spinal part of the
pain was innervated by the mandibular division of
accessory nerve had been incised, except which?
the trigeminal nerve.
A. To raise the hand above the head, it is necessary for
B. The stabbing nature of the pain is characteristic of
the trapezius muscle, assisted by the serratus ante-
the disease.
rior, to contract and rotate the scapula so that the
C. The trigger mechanism, stimulation of an area
glenoid cavity faces upward.
that received its sensory innervation from the
B. The trapezius muscle is innervated by the spinal
trigeminal nerve, is characteristic of trigeminal
part of the accessory nerve.
neuralgia.
C. As the spinal part of the accessory nerve crosses the
D. Examination of the actions of the masseter and the
posterior triangle of the neck, it is deeply placed, be-
temporalis muscles showed evidence of weakness on
ing covered by the skin, the superficial fascia, the in-
the right side.
vesting layer of deep cervical fascia, and the levator
E. The patient experienced hyperesthesia in the distri-
scapulae muscle.
bution of the right auriculotemporal nerve.
D. The surface marking of the spinal part of the acces-
A 10-year-old boy was playing darts with his friends. He bent
sory nerve is as follows: Bisect at right angles a line
down to pick up a fallen dart when another dart fell from the
joining the angle of the jaw to the tip of the mastoid
dart board and hit him on the side of his face. On examina-
process. Continue the second line downward and
tion in the emergency department a small skin wound was
backward across the posterior triangle.
found over the right parotid salivary gland. Then, 6 months
E. The knife opening the abscess had cut the accessory
later, the boy’s mother noticed that before mealtimes the
nerve.
boy began to sweat profusely on the facial skin close to the
A 35-year-old woman had a partial thyroidectomy for the
healed dart wound.
treatment of thyrotoxicosis. During the operation a ligature
6. The following statements can explain this phenome-
slipped off the right superior thyroid artery. To stop the he-
non except which?
morrhage, the surgeon blindly grabbed for the artery with
A. The point of the dart had entered the parotid salivary
artery forceps. The operation was completed without further
gland and damaged the parasympathetic secretomo-
incident. The following morning the patient spoke with a
tor fibers to the gland.
husky voice.
B. The secretomotor fibers to the parotid gland arise in
4. The following statements about this patient would ex-
the otic ganglion.
plain the husky voice except which?
C. The preganglionic parasympathetic fibers originate
A. Laryngoscopic examination revealed that the right
in the superior salivatory nucleus of the facial nerve.
vocal cord was slack, causing the huskiness of the
D. The skin over the parotid salivary gland is innervated
voice.
by the great auricular nerve, which was also dam-
B. The vocal cord is tensed by the contraction of the
aged by the dart.
cricothyroid muscle.
E. On regeneration of the damaged nerves some of the
C. The cricothyroid muscle tilts back the cricoid carti-
parasympathetic nerves to the parotid salivary gland
lage and pulls forward the thyroid cartilage.
had crossed over and joined the sympathetic secre-
D. The cricothyroid muscle is innervated by the recur-
tomotor nerves to the sweat glands in the distal end
rent laryngeal nerve.
of the great auricular nerve.
E. The superior thyroid artery is closely related to the
F. The patient has Frey’s syndrome.
external laryngeal nerve.
A 31-year-old woman fell off her bicycle and lacerated
A 43-year-old woman visited her physician complaining of
the skin of her forehead just above the left eyebrow.
severe intermittent pain on the right side of her face. The
7. What is the sensory innervation of the skin of the fore-
pain was precipitated by exposing the right side of her face
head? Where may these nerves be blocked?
to a draft of cold air. The pain was stabbing in nature and
lasted about 12 hours before finally disappearing. When
A 27-year-old man was involved in a motorcycle acci-
asked to point out on her face the area where the pain was
dent and was seen in the emergency department with
242
Chapter 15
extensive lacerations of the right ear. It was decided to
10. On examination, a patient is found to have a bitempo-
suture the skin lesions under local anesthesia.
ral hemianopia. An enlargement of which anatomic
structure is likely to cause this condition?
8. How would you anesthetize the ear?
11. A patient is suspected of having a lesion of the glos-
A 63-year-old woman visited her physician with a
sopharyngeal nerve. How would you test the integrity of
swelling over the parotid gland on the right side. She
this cranial nerve?
stated that she had first noticed the swelling
3
months previously, and since that time it had rapidly
12. A 47-year-old woman is seen by a neurologist because of
increased in size. Recently, she had noticed that the
trouble reading the newspaper. She said that the print
right side of her face “felt weak” and she could no
starts to tilt and she begins to see double. She also stated
longer whistle for her dog. On examination, a hard
that she has difficulty walking down steps because she
swelling deeply attached to the parotid gland was
cannot easily look downward with her right eye. On
found. On testing the facial muscles, it was found
physical examination, the patient was found to have
that the muscles on the right side were weaker than
weakness of the movement of the right eye, both down-
those on the left side.
ward and laterally. Using your knowledge of anatomy,
explain the signs and symptoms.
9. What is the connection between the parotid swelling
and the right-sided facial weakness?
Answers and Explanations
1.
E is the correct answer. In this patient all the facial mus-
7.
The skin of the forehead is innervated by the supraor-
cles on the right side were paralyzed. When making the
bital and supratrochlear branches of the frontal nerve, a
diagnosis of Bell’s palsy, it is imperative that one makes
branch of the ophthalmic division of the trigeminal
the distinction between an upper motor neuron palsy
nerve. The nerves may be blocked as they emerge onto
and a lower motor neuron palsy. The part of the facial
the forehead around the superior margin of the orbital
nucleus of the facial nerve that controls the muscles of
cavity.
the upper part of the face receives corticonuclear fibers
8.
The auricle receives its sensory innervation from the
from both cerebral hemispheres. Therefore, it follows
greater auricular nerve (C2 and C3), the auriculotem-
that with a lesion involving the upper motor neurons,
poral nerve (mandibular division of the trigeminal
only the muscles of the lower part of the face will be
nerve), and the auricular branch of the vagus nerve.
paralyzed. In this patient all the facial muscles on the
Analgesia of the skin can be obtained by multiple sub-
affected side were paralyzed, indicating that the lesion
cutaneous injections that are continued circumferen-
was confined to the facial nerve.
tially around the auricle.
2.
B is the correct answer. The genioglossus muscle is sup-
9.
The facial nerve, the retromandibular vein, and the ex-
plied by the hypoglossal nerve.
ternal carotid artery lie within the parotid salivary
3.
C is the correct answer. The spinal part of the accessory
gland. This patient had a highly invasive carcinoma of
nerve lies superficial to the levator scapulae muscle in
the right parotid gland, which quickly involved the
the posterior triangle of the neck.
right facial nerve, with consequent weakness of the
right facial muscles. The method used clinically to test
4.
D is the correct answer. The cricothyroid muscle is in-
the integrity of the facial nerve is fully described on CD
nervated by the external laryngeal nerve, which was
p. 228. A benign tumor of the parotid gland tends not to
damaged in this patient.
damage the facial nerve.
5.
D is the correct answer. The motor portion of the
10.
Bitemporal hemianopia is a loss of both temporal fields
trigeminal nerve is unaffected in patients with trigemi-
of vision and is due to the interruption of the optic
nal neuralgia.
nerve fibers derived from the medial halves of both
6.
C is the correct answer. The secretomotor fibers to the
retinae. Pressure on the optic chiasma by a tumor of
parotid salivary gland originate in the inferior salivatory
the pituitary gland is the most common cause of the
nucleus of the glossopharyngeal nerve.
condition.
The Cranial Nerves and Trigeminal Nerve Blocks
243
11. The glossopharyngeal nerve supplies the mucous mem-
and laterally. This abnormality can be explained as fol-
brane of the posterior third of the tongue with taste
lows: Contraction of the inferior rectus muscle rotates
fibers and those for common sensation. These sensa-
the eyeball so that the cornea is depressed downward.
tions can easily be tested by using appropriate stimuli.
Because of the manner of its insertion, the inferior
rectus muscle also rotates the eyeball medially. This
12. The difficulty with reading and the diplopia can be ex-
tendency to rotate the eyeball medially is normally
plained by paralysis of the right superior oblique mus-
neutralized by simultaneous contraction of the supe-
cle. When a patient with paralysis of the superior
rior oblique muscle, whose action is to rotate the
oblique muscle looks straight downward, the affected
eyeball laterally as well as to depress the cornea
eye turns medially as well as downward. Moreover, the
downward.
patient has great difficulty turning that eye downward
The Vertebral Column,
the Spinal Cord, and the
Meninges
16
Chapter Outline
Vertebral Column
246
Subarachnoid Space
250
Examination of the Back
246
Spinal Tap (Lumbar Puncture)
250
Anatomy of “Not Getting In”
253
Abnormal Curves of the Vertebral Column
246
Anatomy of Complications of Lumbar Puncture
253
Dislocations of the Vertebral Column
246
Block of the Subarachnoid Space
253
Fractures of the Vertebral Column
246
Caudal Anesthesia
253
Spinal Nerve Root Pain
246
Herniated Intervertebral Discs
247
Congenital Anomalies
255
Disease and the Intervertebral Foramina
247
Scoliosis
255
Narrowing of the Spinal Canal
249
Spina Bifida
255
Sacroiliac Joint Disease
249
Relationship of the Vertebral Body to the
Spinal Cord
250
Spinal Nerve
255
Spinal Cord Ischemia
250
Clinical Problem Solving Questions
257
Spinal Cord Injuries
250
Relationship of Spinal Cord Segments to Vertebral
Answers and Explanations
259
Numbers
250
Fractures of the Vertebral Column
VERTEBRAL
See Chapter 12, CD-ROM.
COLUMN
Spinal Nerve Root Pain
Spinal nerve roots exit from the vertebral canal through the
Examination of the Back
intervertebral foramina. Each foramen is bounded superi-
See Chapter 11, CD-ROM.
orly and inferiorly by the pedicles, anteriorly by the inter-
vertebral disc and the vertebral body, and posteriorly by the
articular processes and joints (see text Fig. 16-3). In the lum-
Abnormal Curves of the
bar region, the largest foramen is between the first and sec-
ond lumbar vertebrae and the smallest is between the fifth
Vertebral Column
lumbar and first sacral vertebra.
One of the complications of osteoarthritis of the verte-
See Chapter 11, CD-ROM.
bral column is the growth of osteophytes, which com-
monly encroach on the intervertebral foramina, causing
pain along the distribution of the segmental nerve. The
Dislocations of the
fifth lumbar spinal nerve is the largest of the lumbar spinal
nerves, and it exits from the vertebral column through the
Vertebral Column
smallest intervertebral foramen. For this reason, it is the
See Chapter 12, CD-ROM.
most vulnerable.
The Verterbral Column, the Spinal Cord, and the Meninges
247
Osteoarthritis as a cause of root pain is suggested by the
A lateral herniation may press on one or two roots and often
patient’s age, its insidious onset, and a history of back pain
involves the nerve root going to the intervertebral foramen
of long duration; this diagnosis is made only when all other
just below. However, because C8 nerve roots exist and an
causes have been excluded. For example, a prolapsed disc
eighth cervical vertebral body does not, the thoracic and
usually occurs in a younger age group and often has an
lumbar roots exit below the vertebra of the corresponding
acute onset.
number. Thus, the L5 nerve root exits between the fifth lum-
bar and first sacral vertebrae. Moreover, because the nerve
roots move laterally as they pass toward their exit, the root cor-
Herniated Intervertebral Discs
responding to that disc space (L4 in the case of the L4-5 disc)
The structure and function of the intervertebral disc is
is already too lateral to be pressed on by the herniated disc.
described on text page 581. The resistance of these discs to
Herniation of the L4-5 disc usually gives rise to symptoms
compression forces is substantial, as seen, for example,
referable to the L5 nerve roots, even though the L5 root exits
in circus acrobats who can support four or more of their
between L5 and S1 vertebrae. The nucleus pulposus occa-
colleagues on their shoulders. Nevertheless, the discs are
sionally herniates directly backward, and if it is a large her-
vulnerable to sudden shocks, particularly if the vertebral
niation, the whole cauda equina may be compressed, pro-
column is flexed and the disc is undergoing degene-
ducing paraplegia.
rative changes, that result in herniation of the nucleus
An initial period of back pain is usually caused by the
pulposus.
injury to the disc. The back muscles show spasm, especially
The discs most commonly affected are those in areas
on the side of the herniation, because of pressure on the
where a mobile part of the column joins a relatively immo-
spinal nerve root. As a consequence, the vertebral column
bile part—that is, the cervicothoracic junction and the
shows a scoliosis, with its concavity on the side of the lesion.
lumbosacral junction. In these areas, the posterior part of
Pain is referred down the leg and foot in the distribution of
the anulus fibrosus ruptures, and the nucleus pulposus is
the affected nerve. Since the sensory posterior roots most
forced posteriorly like toothpaste out of a tube. This is
commonly pressed on are the fifth lumbar and the first
referred to as a herniation of the nucleus pulposus. This
sacral, pain is usually felt down the back and lateral side of
herniation can result either in a central protrusion in the
the leg, radiating to the sole of the foot. This condition is
midline under the posterior longitudinal ligament of the
often called sciatica. In severe cases paresthesia or actual
vertebrae or in a lateral protrusion at the side of the posterior
sensory loss may be present.
ligament close to the intervertebral foramen (CD Fig. 16-1).
Pressure on the anterior motor roots causes muscle
The escape of the nucleus pulposus will produce narrowing
weakness. Involvement of the fifth lumbar motor root pro-
of the space between the vertebral bodies, which may be vi-
duces weakness of dorsiflexion of the ankle, whereas pres-
sible on radiographs. Slackening of the anterior and poste-
sure on the first sacral motor root causes weakness of plantar
rior longitudinal ligaments results in abnormal mobility of
flexion, and the ankle jerk may be diminished or absent (see
the vertebral bodies, producing local pain and subsequent
CD Fig. 16-1).
development of osteoarthritis.
A large, centrally placed protrusion may give rise to
Cervical disc herniations are less common than herni-
bilateral pain and muscle weakness in both legs. Acute
ations in the lumbar region (see text Fig. 16-21). The discs
retention of urine may also occur.
most susceptible to this condition are those between the
A correlation between the disc lesion, the nerve
fifth and sixth or sixth and seventh vertebrae. Lateral protru-
roots involved, the pain dermatome, the muscle weakness,
sions cause pressure on a spinal nerve or its roots. Each
and the missing or diminished reflex is shown in CD
spinal nerve emerges above the corresponding vertebra;
Table 16-1.
thus, protrusion of the disc between the fifth and sixth cer-
vical vertebrae can cause compression of the C6 spinal
Disease and the Intervertebral
nerve or its roots (see CD Fig. 16-1). Pain is felt near the
lower part of the back of the neck and shoulder and along
Foramina
the area in the distribution of the spinal nerve involved.
Central protrusions may press on the spinal cord and the an-
The intervertebral foramina (see text Fig. 16-3) transmit
terior spinal artery and involve the various nerve tracts of the
the spinal nerves and the small segmental arteries and
spinal cord.
veins, all of which are embedded in areolar tissue. Each
Lumbar disc herniations are more common than cer-
foramen is bounded above and below by the pedicles of ad-
vical disc herniations (see CD Fig. 16-1). The discs usually
jacent vertebrae, in front by the lower part of the vertebral
affected are those between the fourth and fifth lumbar verte-
body and by the intervertebral disc, and behind by the ar-
brae and between the fifth lumbar vertebra and the sacrum.
ticular processes and the joint between them. In this situa-
In the lumbar region the roots of the cauda equina run pos-
tion, the spinal nerve is vulnerable and may be pressed on
teriorly over several intervertebral discs (see CD Fig. 16-1B).
or irritated by disease of the surrounding structures. Her-
248
Chapter 16
foramen
magnum
occipital bone
C1
atlas
1
C2
2
C3
3
C
L5
C4
4
S1
A
C5
L5—S1
5
disc
C6
6
C7
7
nucleus
C8
pulposus
D
T1
T1
anulus fibrous
3
L3
4
B
L4
5
E
L5
S1
L5
S1
S1
CD Figure 16-1
A and B. Posterior views of vertebral bodies in the cervical and lumbar
regions showing the relationship that might exist between the herniated nucleus pulposus
and the spinal nerve roots. Note that there are eight cervical spinal nerves but only seven
cervical vertebrae. In the lumbar region, for example, the emerging L4 nerve roots pass out
laterally close to the pedicle of the fourth lumbar vertebra and are not related to the inter-
vertebral disc between the fourth and fifth lumbar vertebrae. C. Posterolateral herniation of
the nucleus pulposus of the intervertebral disc between the fifth lumbar vertebra and the
first sacral vertebra showing pressure on the S1 nerve root. D. An intervertebral disc that
has herniated its nucleus pulposus posteriorly. E. Pressure on the L5 motor nerve root pro-
duces weakness of dorsiflexion of the ankle; pressure on the S1 motor nerve root produces
weakness of plantar flexion of the ankle joint.
The Verterbral Column, the Spinal Cord, and the Meninges
249
Summary of Important Features Found in Cervical and Lumbosacral
CD Table 16-1
Root Syndromes
Root Injury
Dermatome Pain
Muscle Supplied
Movement Weakness
Reflex Involved
C5
Lower lateral aspect
Deltoid and biceps
Shoulder abduction,
Biceps
of upper arm
elbow flexion
C6
Lateral aspect of
Extensor carpi radialis
Wrist extensors
Brachioradialis
forearm
longus and brevis
C7
Middle finger
Triceps and flexor carpi
Extension of elbow
Triceps
radialis
and flexion of wrist
C8
Medial aspect of
Flexor digitorum
Finger flexion
None
forearm
superficialis and
profundus
L1
Groin
Iliopsoas
Hip flexion
Cremaster
L2
Anterior aspect of
Iliopsoas, sartorius, hip
Hip flexion, hip
Cremaster
thigh
adductors
adduction
L3
Medial aspect of
Iliopsoas, sartorius,
Hip flexion, knee
Patellar
knee
quadriceps, hip
extension, hip
adductors
adduction
L4
Medial aspect of
Tibialis anterior,
Foot inversion, knee
Patellar
calf
quadriceps
extension
L5
Lateral part of lower
Extensor hallucis
Toe extension, ankle
None
leg and dorsum
longus, extensor
dorsiflexion
of foot
digitorum longus
S1
Lateral edge of
Gastrocnemius, soleus
Ankle plantar flexion
Ankle jerk
foot
S2
Posterior part of
Flexor digitorum longus,
Ankle plantar flexion,
None
thigh
flexor hallucis longus
toe flexion
niation of the intervertebral disc, fractures of the vertebral
stenosis in the cauda equina area can lead to neurologic
bodies, and osteoarthritis involving the joints of the articu-
compression. Symptoms vary from mild discomfort in the
lar processes or the joints between the vertebral bodies
lower back to severe pain radiating down the leg with the
can all result in pressure, stretching, or edema of the
inability to walk.
emerging spinal nerve. Such pressure would give rise to
dermatomal pain, muscle weakness, and diminished or ab-
sent reflexes.
Sacroiliac Joint Disease
The clinical aspects of this joint are referred to again
because disease of this joint can cause low back pain and
Narrowing of the Spinal Canal
may be confused with disease of the lumbosacral joints.
After about the fourth decade of life the spinal canal be-
Essentially, the sacroiliac joint is a synovial joint that has
comes narrowed by aging. Osteoarthritic changes in the
irregular elevations on one articular surface that fit into
joints of the articular processes with the formation of os-
corresponding depressions on the other articular surface.
teophytes, together with degenerative changes in the inter-
It is a strong joint and is responsible for the transfer of
vertebral discs and the formation of large osteophytes be-
weight from the vertebral column to the hip bones. The
tween the vertebral bodies, can lead to narrowing of the
joint is innervated by the lower lumbar and sacral nerves so
spinal canal and intervertebral foramina. In persons in
that disease in the joint may produce low back pain and
whom the spinal canal was originally small, significant
sciatica.
250
Chapter 16
The sacroiliac joint is inaccessible to clinical exami-
below the level of the lesion. The symptoms and signs of
nation. However, a small area located just medial to and
spinal shock and paraplegia in flexion and extension are be-
below the posterosuperior iliac spine is where the joint
yond the scope of this book. For further information, a text-
comes closest to the surface. In disease of the lumbosacral
book of neurology should be consulted.
region, movements of the vertebral column in any
direction cause pain in the lumbosacral part of the
Relationships of Spinal Cord
column. In sacroiliac disease, pain is extreme on rotation
of the vertebral column and is worst at the end of forward
Segments to Vertebral Numbers
flexion. The latter movement causes pain because the
hamstring muscles hold the hip bones in position while
Because the spinal cord is shorter than the vertebral co-
the sacrum is rotating forward as the vertebral column is
lumn, the spinal cord segments do not correspond numeri-
flexed.
cally with the vertebrae that lie at the same level (CD Fig.
16-2). The following list helps determine which spinal seg-
ment is contiguous with a given vertebral body:
SPINAL CORD
Vertebrae
Spinal Segment
Cervical
Add 1
Upper thoracic
Add 2
Spinal Cord Ischemia
Lower thoracic (T7-9)
Add 3
Tenth thoracic
L1 and 2 cord segments
The blood supply to the spinal cord is surprisingly meager,
Eleventh thoracic
L3 and 4 cord segments
considering the importance of this nervous tissue. The
Twelfth thoracic
L5 cord segment
longitudinally running anterior and posterior spinal arteries
First lumbar
Sacral and coccygeal cord
are of small and variable diameter, and the reinforcing seg-
segments
mental arteries vary in number and in size. Ischemia of the
spinal cord can easily follow minor damage to the arterial
supply as a result of regional anesthesia, pain block proce-
dures, or aortic surgery.
SUBARACHNOID
Spinal Cord Injuries
SPACE
The degree of spinal cord injury at different vertebral le-
vels is largely governed by anatomic factors. In the cervical
Spinal Tap (Lumbar Puncture)
region, dislocation or fracture dislocation is common, but
the large size of the vertebral canal often results in the
Lumbar puncture may be performed to withdraw a sample
spinal cord escaping severe injury. However, when consi-
of cerebrospinal fluid for examination. Fortunately, the
derable displacement occurs, the cord is sectioned and
spinal cord terminates below at the level of the lower bor-
death occurs immediately. Respiration ceases if the lesion
der of the first lumbar vertebra in the adult. (In the infant,
occurs above the segmental origin of the phrenic nerves
it may reach as low as the third lumbar vertebra.) The sub-
(C3, 4, and 5).
arachnoid space extends down as far as the lower border of
In fracture dislocations of the thoracic region, dis-
the second sacral vertebra. The lower lumbar part of the
placement is often considerable, and the small size
vertebral canal is thus occupied by the subarachnoid
of the vertebral canal results in severe injury to the spinal
space, which contains the cauda equina—that is, the lum-
cord.
bar and sacral nerve roots and the filum terminale. A nee-
In fracture dislocations of the lumbar region, two
dle introduced into the subarachnoid space in this region
anatomic facts aid the patient. First, the spinal cord in the
usually pushes the nerve roots to one side without causing
adult extends only down as far as the level of the lower bor-
damage.
der of the first lumbar vertebra. Second, the large size of the
With the patient lying on the side with the vertebral col-
vertebral foramen in this region gives the roots of the cauda
umn well flexed, the space between adjoining laminae in
equina ample room. Nerve injury may therefore be mini-
the lumbar region is opened to a maximum (CD Fig. 16-3).
mal in this region.
An imaginary line joining the highest points on the iliac
Injury to the spinal cord can produce partial or complete
crests passes over the fourth lumbar spine (see text Fig. 16-
loss of function at the level of the lesion and partial or com-
22). With a careful aseptic technique and under local anes-
plete loss of function of afferent and efferent nerve tracts
thesia, the lumbar puncture needle, fitted with a stylet, is
The Verterbral Column, the Spinal Cord, and the Meninges
251
C1 spinal nerve
atlas
cervical
axis
C8
segments
seventh cervical
of spinal
vertebra
cord
first thoracic
thoracic
T1
segments
of spinal
cord
twelfth thoracic
lumbar, sacral, and
vertebra
T12
coccygeal segments
of spinal cord
first lumbar
L1
vertebra
lower end of
spinal cord
fifth lumbar
L5
vertebra
S1
sacrum
coccyx
S5
coccygeal spinal nerve one
CD Figure 16-2
Posterior view of the spinal cord showing the origins of the roots of the
spinal nerves and their relationship to the different vertebrae. On the right, the laminae
have been removed to expose the right half of the spinal cord and the nerve roots.
252
Chapter 16
cauda equina
(anterior and posterior nerve roots)
posterior longitudinal
internal vertebral veins
ligament
superficial fascia
spine
anterior longitudinal
ligament
skin
lumbar
L3
puncture
needle
intervertebral
disc
fourth lumbar
L4
spinal nerve
interspinous
articular
ligament
process
L5
transverse
process
ligamentum
flavum
supraspinous
ligament
cauda equina
dura mater
arachnoid mater
CD Figure 16-3
Sagittal section through the lumbar part of the vertebral column in flex-
ion. Note that the spines and laminae are well separated in this position, enabling one to
introduce a lumbar puncture needle into the subarachnoid space.
The Verterbral Column, the Spinal Cord, and the Meninges
253
passed into the vertebral canal above or below the fourth
caudal displacement of the uncus through the tentorial
lumbar spine (see CD Fig. 16-3). The needle will pass
notch or a dangerous displacement of the medulla
through the following anatomic structures before it enters
through the foramen magnum, when the lumbar cere-
the subarachnoid space: skin, superficial fascia, supra-
brospinal fluid pressure is reduced.
spinous ligament, interspinous ligament, ligamentum
flavum, areolar tissue (containing the internal vertebral ve-
Block of the Subarachnoid Space
nous plexus in the epidural space), dura mater, and arach-
A block of the subarachnoid space in the vertebral canal,
noid mater. The depth to which the needle will have to pass
which may be caused by a tumor of the spinal cord or the
varies from 1 in. (2.5 cm) or less in a child to as much as 4
meninges, can be detected by compressing the internal
in. (10 cm) in obese adults.
jugular veins in the neck. This raises the cerebral venous
As the stylet is withdrawn, a few drops of blood com-
pressure and inhibits the absorption of cerebrospinal fluid
monly escape. This usually indicates that the point of the
in the arachnoid granulations, thus producing a rise in the
needle is situated in one of the veins of the internal vertebral
manometric reading of the cerebrospinal fluid pressure. If
plexus and has not yet reached the subarachnoid space. If
this rise fails to occur, the subarachnoid space is blocked
the entering needle should stimulate one of the nerve roots
and the patient is said to exhibit a positive Queckenstedt’s
of the cauda equina, the patient will experience a fleeting
sign.
discomfort in one of the dermatomes, or a muscle will
twitch, depending on whether a sensory or a motor root was
impaled. If the needle is pushed too far anteriorly, it may hit
CAUDAL
the body of the third or fourth lumbar vertebra (see CD Fig.
16-3).
The cerebrospinal fluid pressure can be measured by
ANESTHESIA
attaching a manometer to the needle. In the recumbent
position, the normal pressure is about 60-150 mm H2O. It
Solutions of anesthetics may be injected into the sacral
is interesting to note that the cerebrospinal fluid pressure
canal through the sacral hiatus. The solutions pass upward
normally fluctuates slightly with the heart beat and with
in the loose connective tissue and bathe the spinal nerves
each phase of respiration.
as they emerge from the dural sheath. Caudal anesthesia
is used in operations in the sacral region, including
Anatomy of “Not Getting In”
anorectal surgery and culdoscopy. Obstetricians use this
method of nerve block to relieve the pains during the first
If bone is encountered, the needle should be withdrawn as
and second stages of labor. Its advantage is that, adminis-
far as the subcutaneous tissue, and the angle of insertion
tered by this method, the anesthetic does not affect
should be changed. The most common bone encountered
the infant.
is the spinous process of the vertebra above or below the
The sacral hiatus is palpated as a distinct depression in
path of insertion. If the needle is directed laterally rather
the midline about 1.6 in. (4 cm) above the tip of the coccyx
than in the midline, it may hit the lamina or an articular
in the upper part of the cleft between the buttocks. The hia-
process.
tus is triangular or U shaped and is bounded laterally by the
sacral cornua (CD Fig. 16-4).
Anatomy of Complications of
The size and shape of the hiatus depend on the num-
Lumbar Puncture
ber of laminae that fail to fuse in the midline posteriorly.
■ Postlumbar puncture headache: This headache starts af-
The common arrangement is for the hiatus to be formed
ter the procedure and lasts 24 to 48 hours. The cause is a
by the nonfusion of the fifth and sometimes the fourth
leak of cerebrospinal fluid through the dural puncture,
sacral vertebrae.
and it usually follows the use of a wide-bore needle. The
With a careful aseptic technique and under local anes-
leak reduces the volume of cerebrospinal fluid, which, in
thesia, the needle, fitted with a stylet, is passed into the ver-
turn, causes a downward displacement of the brain and
tebral (sacral) canal through the sacral hiatus.
stretches the nerve-sensitive meninges—a headache fol-
The needle pierces the skin and fascia and the sacro-
lows. The headache is relieved by assuming the recum-
coccygeal membrane that fills in the sacral hiatus (see CD
bent position. Using small-gauge styletted needles and
Fig.
16-4). The membrane is formed of dense fibrous
avoiding multiple dural holes reduce the incidence of
tissue and represents the fused supraspinous and inter-
headache.
spinous ligaments as well as the ligamentum flavum. A
■ Brain herniation: Lumbar puncture is contraindicated in
distinct feeling of
“give” is felt when the ligament is
cases in which intracranial pressure is significantly
penetrated.
raised. A large tumor, for example, above the tentorium
Note that the sacral canal is curved and follows the gen-
cerebelli with a high intracranial pressure may result in a
eral curve of the sacrum (see CD Fig. 16-4). The anterior
254
Chapter 16
fourth sacral
third sacral
spinous process
spinous process
third posterior
lamina of fourth
sacral foramen
sacral vertebra
lateral mass
of sacrum
sacral hiatus
sacral cornu
fourth
fourth posterior
sacro-
posterior
coccyx
sacral foramen
coccygeal
sacral
foramen
ligment
sacrococcygeal
membrane
A
coccyx
B
posterior rami of
spinal nerves
subarachnoid space
sacral hiatus
lower limit of
subarachnoid space
filum terminale
filum terminale
dura and
arachnoid
C
coccyx
sacrococcygeal membrane
sacral hiatus
extradural space
filum terminale
D
CD Figure 16-4
A. The sacral hiatus. Black dots indicate the position of important bony
landmarks. B. Posterior surface of the lower end of the sacrum and the coccyx showing
the sacrococcygeal membrane covering the sacral hiatus. C. The dural sheath (thecal sac)
around the lower end of the spinal cord and spinal nerves in the sacral canal; the laminae
have been removed. D. Longitudinal section through the sacrum showing the anatomy of
caudal anesthesia.
The Verterbral Column, the Spinal Cord, and the Meninges
255
wall, formed by the fusion of the bodies of the sacral verte-
brae, is rough and ridged. The posterior wall, formed by the
fusion of the laminae, is smooth. The average distance be-
tween the sacral hiatus and the lower end of the subarach-
noid space at the second sacral vertebra is about 2 in. (5 cm)
in adults.
Note also that the sacral canal contains the dural sac
(containing the cauda equina), which is tethered to the coc-
cyx by the filum terminale; the sacral and coccygeal nerves
as they emerge from the dural sac surrounded by their dural
sheath; and the thin-walled veins of the internal vertebral
venous plexus.
CONGENITAL
CD Figure 16-5
Posterior view of a woman with scoliosis
ANOMALIES
resulting from a congenital hemivertebra in the lower
thoracic region.
Scoliosis
Scoliosis results from a congenital hemivertebra. A hemiver-
tebra is caused by a failure in development of one of the two
ossification centers that appear in the centrum of the body
RELATIONSHIP OF
of each vertebra (CD Fig. 16-5).
THE VERTEBRAL
Spina Bifida
BODY TO THE
In spina bifida, the spines and arches of one or more adja-
cent vertebrae fail to develop. The condition occurs most
frequently in the lower thoracic, lumbar, and sacral regions.
SPINAL NERVE
Beneath this defect, the meninges and spinal cord may or
may not be involved in varying degrees. This condition is a
Since the fully developed vertebral body is intersegmental in
result of failure of the mesenchyme, which grows in be-
position, each spinal nerve leaves the vertebral canal through
tween the neural tube and the surface ectoderm, to form the
the intervertebral foramen and is closely related to the inter-
vertebral arches in the affected region. The types of spina
vertebral disc. This fact is of great clinical significance in cases
bifida are shown in CD Figs. 16-6 and 16-7.
with prolapse of an intervertebral disc (see CD Fig. 16-1).
256
Chapter 16
spina bifida occulta
meningocele
meningomyelocele
myelocele
syringomyelocele
CD Figure 16-6
Different types of spina bifida.
The Verterbral Column, the Spinal Cord, and the Meninges
257
A
B
CD Figure 16-7
A. Meningocele in the lumbosacral region. (Courtesy of L. Thompson.)
B. Meningomyelocele in the upper thoracic region. (Courtesy of G. Avery.)
Clinical Problem Solving Questions
Read the following case histories/questions and give
physician suspected a displacement of the upper
the best answer for each.
thoracic spines on the sixth thoracic spine.
An 11-year-old boy was showing off in front of friends by div-
2. The following physical signs confirmed a diagnosis of
ing into the shallow end of a swimming pool. After one par-
fracture dislocation between the fifth and sixth thoracic
ticularly daring dive, he surfaced quickly and climbed out of
vertebrae except which?
the pool, holding his head between his hands. He said that
A. A lateral radiograph revealed fractures involving the
he had hit the bottom of the pool with his head and now had
superior articular processes of the sixth thoracic ver-
severe pain in the root of the neck, which was made worse
tebra and the inferior articular processes of the fifth
when he tried to move his neck. A lateral radiograph re-
thoracic vertebra.
vealed that the right inferior articular process of the fifth cer-
B. Considerable forward displacement of the body of
vical vertebra was forced over the anterior margin of the
the fifth thoracic vertebra on the sixth thoracic ver-
right superior articular process of the sixth cervical vertebra,
tebra occurred.
producing a unilateral dislocation with nipping of the right
C. The patient had signs and symptoms of spinal shock.
sixth cervical nerve.
D. The large size of the vertebral canal in the thoracic
1. The following symptoms and signs confirmed the diag-
region leaves plenty of space around the spinal cord
nosis except which?
for bony displacement.
A. The head was rotated to the right.
E. The patient later showed signs and symptoms of
B. There was spasm of the deep neck muscles on the
paraplegia.
right side of the neck, which were tender to touch.
A 66-year-old woman was seen in the emergency depart-
C. The patient complained of severe pain in the region
ment complaining of a burning pain over the upper part of
of the back of the neck and right shoulder.
her right arm. The pain had started 2 days previously and
D. The slightest movement produced severe pain in
had progressively worsened. Physical examination revealed
the right sixth cervical dermatome.
weakness and wasting of the right deltoid and biceps brachii
E. The large size of the vertebral canal in the cervical
muscles. The patient also had hyperesthesia in the skin over
region permitted the spinal cord to escape injury.
the lower part of the right deltoid and down the lateral side
A 50-year-old coal miner was crouching at the mine
of the arm. Radiologic examination showed extensive spur
face when a large rock suddenly became dislodged
formation on the bodies of the fourth, fifth, and sixth cervi-
from the roof of the mine shaft and struck him on the
cal vertebrae. These signs and symptoms suggested severe
upper part of his back. The emergency department
osteoarthritis of the cervical vertebral column.
258
Chapter 16
3. This disease produced the following changes in the ver-
B. An imaginary line joining the anterior superior iliac
tebrae and related structures except which?
spines passes over the fourth lumbar spine.
A. Repeated trauma and aging had resulted in degen-
C. The needle should be inserted above or below the
erative changes at the articulating surfaces of the
fourth lumbar spine.
fourth, fifth, and sixth cervical vertebrae.
D. To enter the subarachnoid space, the needle will pass
B. Extensive spur formation resulted in narrowing of
through the skin, superficial fascia, supraspinous lig-
the intervertebral foramina with pressure on the
ament, interspinous ligament, ligamentum flavum,
nerve roots.
areolar tissue (containing the internal vertebral ve-
C. The burning pain and hyperesthesia were caused by
nous plexus), dura mater, and arachnoid mater.
pressure on the third and fourth cervical posterior
E. The spinal cord ends below in the adult at the level
roots.
of the lower border of the first lumbar vertebra.
D. The weakness and wasting of the deltoid and biceps
F. With the patient in the lateral prone position, the
brachii muscles were caused by pressure on the fifth
normal cerebrospinal fluid pressure is about 60-150
and sixth cervical anterior roots.
mm H2O.
E. Movements of the neck intensified the symptoms by
A 22-year-old student was driving home from a party and
exerting further pressure on the nerve roots.
crashed his car head on into a brick wall. On examination
F. Coughing or sneezing raised the pressure within the
in the emergency department, he was found to have a frac-
vertebral canal and resulted in further pressure on
ture dislocation of the seventh thoracic vertebra, with signs
the roots.
and symptoms of severe damage to the spinal cord.
A medical student offered to move a grand piano for his
6. On recovery from spinal shock he was found to have the
landlady. He had just finished his final examinations in
following signs and symptoms except which?
anatomy and was in poor physical shape. He struggled with
A. Upper motor neuron paralysis of his left leg
the antique monstrosity and suddenly experienced an acute
B. A band of cutaneous hyperesthesia extending
pain in the back, which extended down the back and outer
around the abdominal wall on the left side at the
side of his left leg. On examination in the emergency de-
level of the umbilicus, which was caused by the irri-
partment, he was found to have a slight scoliosis with the
tation of the cord immediately above the site of the
convexity on the right side. The deep muscles of the back in
lesion
the left lumbar region felt firmer than normal. No evidence
C. On the right side, total analgesia, thermoanesthesia,
of muscle weakness was present, but the left ankle jerk was
and partial loss of tactile sense of the skin of the ab-
diminished.
dominal wall below the level of the umbilicus in-
volving the whole of the right leg
4. The symptoms and signs of this patient strongly suggest
D. Fracture dislocation of the seventh thoracic verte-
a diagnosis of prolapsed intervertebral disc except
bra, which would result in severe damage to the sev-
which?
enth thoracic segment of the spinal cord
A. The pain was the worst over the left lumbar region
E. Unequal sensory and motor losses on the two sides,
opposite the fifth lumbar spine.
which indicate a left hemisection of the spinal cord
B. The pain was accentuated by coughing.
C. With the patient supine, flexing the left hip joint
A 45-year-old woman visited her physician because of a low
with the knee extended caused a marked increase in
back pain of 3 months’ duration. She was otherwise very fit.
the pain.
On examination of her back, nothing abnormal was discov-
D. A lateral radiograph of the lumbar vertebral column
ered. The physician then listened to her chest, examined
revealed nothing abnormal.
her thyroid gland, and finally examined both breasts. A
E. A magnetic resonance imaging study revealed the
large, hard mass was found in the left breast.
presence of small fragments of the nucleus pulposus
7. The following facts support the diagnosis of carcinoma
that had herniated outside the anulus in the disc be-
of the left breast with secondaries in the vertebral col-
tween the fifth lumbar vertebra and the sacrum.
umn except which?
F. The pain occurred in the dermatomes of the third
A. The lump in the breast was painless and the patient
and fourth lumbar segments on the left side.
had noticed it while showering 6 months previously.
5. When performing a lumbar puncture (spinal tap) on an
B. Several large, hard, pectoral lymph nodes were
adult, the following anatomic facts have to be taken into
found in the left axilla.
consideration except which?
C. A lateral radiograph of the lumbar vertebral column
A. With the patient in the lateral prone or upright sit-
showed extensive metastases in the bodies of the sec-
ting position, the vertebral column should be well
ond and third lumbar vertebrae.
flexed to separate the spines and laminae of adjacent
D. The lump was situated in the upper outer quadrant
vertebrae.
of the left breast and was fixed to surrounding tissues.
The Verterbral Column, the Spinal Cord, and the Meninges
259
E. Although the cancer had spread by the lymph ves-
B. Anteroposterior and lateral radiographs exclude the
sels, no evidence of spread via the bloodstream was
presence of a fracture, especially of a transverse
present.
process.
A 75-year-old woman was dusting the top of a high closet
C. A 24-hour specimen of urine should be examined
while balanced on a chair. She lost her balance and fell to
for blood to exclude or confirm injury to the right
the floor, catching her right lumbar region on the edge of
kidney.
the chair.
D. Careful examination of the erector spinae muscles
or quadratus lumborum muscle may reveal extreme
8. The following statements about this patient are correct
tenderness and therefore injury to these muscles.
except which?
E. A lumbar puncture (spinal tap) should always be
A. Examination of the back revealed a large bruised
performed in back injuries to exclude damage to the
area in the right lumbar region, which was extremely
spinal cord.
tender to touch.
Answers and Explanations
1. A is the correct answer. The right inferior articular
5. B is the correct answer. An imaginary line joining the
process of the fifth cervical vertebra was forced over the
highest points of the iliac crests passes over the fourth
anterior margin of the right superior articular process of
lumbar spine.
the sixth cervical vertebra, causing the head of the pa-
6. D is the correct answer. Fracture dislocation of the sev-
tient to be rotated to the left.
enth thoracic vertebra would result in severe damage to
2. D is the correct answer. The vertebral canal in the tho-
the tenth thoracic segment of the spinal cord.
racic region is small and round and little space is
7. E is the correct answer. The carcinoma of the left breast
around the spinal cord for bony displacement to occur
was in an advanced stage and had spread by way of the
without causing severe damage to the cord.
lymph vessels to the axillary lymph nodes and by the
3. C is the correct answer. The burning pain and hyperes-
bloodstream to the bodies of the second and third lum-
thesia were caused by pressure on the fifth and sixth cer-
bar vertebrae. Carcinoma of the thyroid, bronchus,
vical posterior roots.
breast, kidney, and prostate tend to metastasize via the
bloodstream to bones.
4. F is the correct answer. The pain occurred in the der-
matomes of the fifth lumbar and first sacral segments on
8. E is the correct answer. A lumbar puncture (spinal tap)
the left side.
is not required in cases of simple trauma to the back.
The Spinal Nerves and
Spinal Nerve Blocks
17
Chapter Outline
Cervical Plexus
263
Arterial Innervation and Raynaud’s Disease
271
Lesions of the Phrenic Nerve and Paralysis of the
Intercostal Nerves
272
Diaphragm
263
Skin Innervation of the Chest Wall and
Brachial Plexus
263
Referred Pain
272
Herpes Zoster
272
Clinical Notes on the Nerves of the Upper
Limb
263
Lumbar Plexus
272
Dermatomes and Cutaneous Nerves
Clinical Notes on the Nerves of the Lower
of the Upper Limb
263
Limb
272
Tendon Reflexes and the Segmental Innervation of
Tendon Reflexes of the Lower Limb
272
Muscles of the Upper Limb
263
Femoral Nerve Injury
272
Brachial Plexus Injuries
263
Sciatic Nerve Injury
272
Upper Lesions of the Brachial Plexus (Erb-Duchenne
Trauma to the Sciatic Nerve
273
Palsy)
264
Sciatica
273
Lower Lesions of the Brachial Plexus (Klumpke
Palsy)
265
Common Peroneal Nerve Injury
273
Compression of the Brachial Plexus, Subclavian Artery,
Tibial Nerve Injury
273
and Subclavian Vein by the Clavicle
265
Obturator Nerve Injury
274
Long Thoracic Nerve Injuries
266
Referred Pain from the Hip Joint
274
Axillary Nerve Injuries
266
Sacral Plexus
274
Radial Nerve Injuries
266
Pressure from the Fetal Head on the Sacral Plexus
274
Injuries to the Radial Nerve in the Axilla
268
Invasion of the Sacral Plexus by Malignant Tumors
274
Motor
268
Sensory
268
Referred Pain from the Obturator Nerve
274
Trophic Changes
268
Clinical Anatomy of Spinal Nerve Blocks
274
Injuries to the Radial Nerve in the Spiral Groove of
the Humerus
268
Brachial Plexus Block
274
Injuries to the Deep Branch of the Radial Nerve
268
Interscalene Block
274
Injuries to the Superficial Radial Nerve
268
Supraclavicular Block
276
Infraclavicular Block
276
Musculocutaneous Nerve Injuries
269
Axillary Block
276
Median Nerve Injuries
269
Musculocutaneous Nerve Block
276
Injuries to the Median Nerve at the Elbow
269
Motor
269
Median Nerve Block
276
Sensory
269
Ulnar Nerve Block
277
Vasomotor Changes
269
Radial Nerve Block
278
Trophic Changes
269
Injuries to the Median Nerve at the Wrist
270
Digital Nerve Blocks
278
Carpal Tunnel Syndrome
270
Thoracic Spinal Nerve Blocks
280
Ulnar Nerve Injuries
270
Intercostal Nerve Block
280
Injuries to the Ulnar Nerve at the Elbow
270
Motor
270
Anterior Abdominal Nerve Blocks
282
Sensory
271
Lumbar Spinal Nerve Blocks
283
Vasomotor Changes
271
Ilioinguinal and Iliohypogastric Nerve Blocks
283
Injuries to the Ulnar Nerve at the Wrist
271
Genitofemoral Nerve Block
283
The Spinal Nerves and Spinal Nerve Blocks
263
Femoral Nerve Block
283
Superficial Peroneal Nerve Block
287
Saphenous Nerve Block
284
Deep Peroneal Nerve Block
288
Lateral Cutaneous Nerve of the Thigh Block
284
Toe Nerve Blocks
289
Sacral Spinal Nerve Blocks
285
Pudendal Nerve Blocks
290
Tibial Nerve Block
285
Clinical Problem Solving Questions
290
Sural Nerve Block
286
Common Peroneal Nerve Block
287
Answers and Explanations
293
they exit from the cord in a spinal nerve of the same seg-
ment, pass to the skin in two or more different cutaneous
CERVICAL PLEXUS
nerves.
The skin over the point of the shoulder and halfway
down the lateral surface of the deltoid muscle is supplied by
Lesions of the Phrenic Nerve and
the supraclavicular nerves (C3 and 4). Pain may be referred
to this region as a result of inflammatory lesions involving
Paralysis of the Diaphragm
the diaphragmatic pleura or peritoneum. The afferent stim-
The diaphragm may be paralyzed because of pressure from
uli reach the spinal cord via the phrenic nerves (C3, 4, and
malignant tumors in the mediastinum on the phrenic nerve.
5). Pleurisy, peritonitis, subphrenic abscess, or gallbladder
Surgical crushing or sectioning of the phrenic nerve in the
disease may therefore be responsible for shoulder pain.
neck, producing paralysis of the diaphragm on one side, was
once used as part of the treatment of lung tuberculosis,
Tendon Reflexes and the Segmental
especially of the lower lobes. The immobile dome of the
diaphragm rests the lung.
Innervation of Muscles of the
Upper Limb
BRACHIAL PLEXUS
The skeletal muscle receives a segmental innervation. Most
muscles are innervated by several spinal nerves and there-
fore by several segments of the spinal cord. A physician
should know the segmental innervation of the following
CLINICAL NOTES
muscles because it is possible to test them by eliciting
simple muscle reflexes in the patient:
ON THE NERVES OF
■ Biceps brachii tendon reflex: C5 and 6 (flexion of the
elbow joint by tapping the biceps tendon)
THE UPPER LIMB
■ Triceps tendon reflex: C6, 7, and 8 (extension of the
elbow joint by tapping the triceps tendon)
■ Brachioradialis tendon reflex: C5, 6, and 7 (supination
Dermatomes and Cutaneous
of the radioulnar joints by tapping the insertion of the
brachioradialis tendon)
Nerves of the Upper Limb
It may be necessary for a physician to test the integrity of the
Brachial Plexus Injuries
spinal cord segments of C3 through T1. The diagrams in
CD Figs. 17-1 and 17-2 show the arrangement of the der-
The roots, trunks, and divisions of the brachial plexus reside
matomes of the upper limb. It is seen that the dermatomes
in the lower part of the posterior triangle of the neck,
for the upper cervical segments C3 to 6 are located along the
whereas the cords and most of the branches of the plexus lie
lateral margin of the upper limb; the C7 dermatome is situ-
in the axilla. Complete lesions involving all the roots of the
ated on the middle finger; and the dermatomes for C8, T1,
plexus are rare. Incomplete injuries are common and are
and T2 are along the medial margin of the limb. The nerve
usually caused by traction or pressure; individual nerves can
fibers from a particular segment of the spinal cord, although
be divided by stab wounds.
264
Chapter 17
transverse cutaneous nerve of neck
C2
supraclavicular nerves
C3
anterior cutaneous branch of second
C4
intercostal nerve
upper lateral cutaneous nerve of arm
C5
T3
medial cutaneous nerve of arm
T2
T4
lower lateral cutaneous nerve of arm
C6
T5
medial cutaneous nerve of forearm
T6
T1
T7
T8
lateral cutaneous nerve of forearm
T9
lateral cutaneous branch of
T10
subcostal nerve
C8
T11
L1
T12
femoral branch of genitofemoral
C7
nerve
median nerve
ulnar nerve
S3
ilioinguinal nerve
S4
lateral cutaneous nerve of thigh
obturator nerve
L2
medial cutaneous nerve of thigh
L3
intermediate cutaneous nerve of thigh
infrapatellar branch of saphenous nerve
L4
lateral sural cutaneous nerve
L5
saphenous nerve
superficial peroneal nerve
S1
deep peroneal nerve
CD
Figure
17-1
Dermatomes
and
distribution of cutaneous nerves on the
anterior aspect of the body.
and infraspinatus (lateral rotator of the shoulder); the sub-
Upper Lesions of the Brachial Plexus
clavius (depresses the clavicle); the biceps brachii (supina-
(Erb-Duchenne Palsy)
tor of the forearm, flexor of the elbow, weak flexor of the
Upper lesions of the brachial plexus are injuries resulting
shoulder), and the greater part of the brachialis (flexor of
from excessive displacement of the head to the opposite
the elbow), and the coracobrachialis (flexor of the shoul-
side and depression of the shoulder on the same side. This
der); and the deltoid (abductor of the shoulder) and the
causes excessive traction or even tearing of C5 and 6 roots
teres minor (lateral rotator of the shoulder). Thus, the limb
of the plexus. It occurs in infants during a difficult delivery
will hang limply by the side, medially rotated by the un-
or in adults after a blow to or fall on the shoulder. The
opposed sternocostal part of the pectoralis major; the fore-
suprascapular nerve, the nerve to the subclavius, and the
arm will be pronated because of loss of the action of the bi-
musculocutaneous and axillary nerves all possess nerve
ceps. The position of the upper limb in this condition has
fibers derived from C5 and 6 roots and will therefore be
been likened to that of a porter or waiter hinting for a tip
functionless. The following muscles will consequently be
(CD Fig.17-3). In addition, there will be a loss of sensation
paralyzed: the supraspinatus (abductor of the shoulder)
down the lateral side of the arm.
The Spinal Nerves and Spinal Nerve Blocks
265
C2
greater occipital nerve
third cervical nerve
C3
great auricular nerve
fourth cervical nerve
C5
lesser occipital nerve
C6
supraclavicular nerve
C4
first thoracic nerve
T2
T3
C5
posterior cutaneous nerve of arm
T4
T5
medial cutaneous nerve of arm
T2
T6
posterior cutaneous nerve of forearm
T7
T8
medial cutaneous nerve of forearm
T9
T1
lateral cutaneous nerve of forearm
T10
T11
lateral cutaneous branch of T12
T12
C7
posterior cutaneous branches of
L1
C6
L1, 2, and 3
S5
radial nerve
ulnar nerve
S4
C8
posterior cutaneous branches of
S3
S1, 2, and 3
L2
branches of posterior cutaneous
S2
nerve of thigh
posterior cutaneous nerve of thigh
L3
obturator nerve
lateral cutaneous nerve
L5
of calf
L4
sural nerve
saphenous nerve
lateral plantar nerve
S1
CD Figure 17-2
Dermatomes and distribu-
L5
medial plantar nerve
tion of cutaneous nerves on the posterior
aspect of the body.
Lower Lesions of the Brachial Plexus
of the arm. If the eighth cervical nerve is also damaged, the
extent of anesthesia will be greater and will involve the medial
(Klumpke Palsy)
side of the forearm, hand, and medial two fingers.
Lower lesions of the brachial plexus are usually traction in-
Lower lesions of the brachial plexus can also be
juries caused by excessive abduction of the arm, as occurs in
produced by the presence of a cervical rib or malignant
the case of a person falling from a height clutching at an ob-
metastases from the lungs in the lower deep cervical lymph
ject to save himself or herself. The first thoracic nerve is usu-
nodes.
ally torn. The nerve fibers from this segment run in the ulnar
and median nerves to supply all the small muscles of the
Compression of the Brachial
hand. The hand has a clawed appearance caused by hyper-
extension of the metacarpophalangeal joints and flexion of
Plexus, Subclavian Artery, and
the interphalangeal joints. The extensor digitorum is unop-
posed by the lumbricals and interossei and extends the
Subclavian Vein by the Clavicle
metacarpophalangeal joints; the flexor digitorum superficialis
and profundus are unopposed by the lumbricals and interos-
The interval between the clavicle and the first rib in some
sei and flex the middle and terminal phalanges, respectively.
patients may become narrowed and thus is responsible for
In addition, loss of sensation will occur along the medial side
compression of nerves and blood vessels.
266
Chapter 17
CD Figure 17-4
Winging of the right scapula.
and the underlying greater tuberosity can be readily pal-
pated. Because the supraspinatus is the only other abductor
of the shoulder, this movement is much impaired. Paralysis
of the teres minor is not recognizable clinically.
CD Figure 17-3
Erb-Duchenne palsy (waiter’s tip).
Radial Nerve Injuries
The radial nerve (see text Fig. 17-21), which arises from the
posterior cord of the brachial plexus, characteristically gives
Long Thoracic Nerve Injuries
off its branches some distance proximal to the part to be
innervated.
The long thoracic nerve, which arises from C5, 6, and 7 and
supplies the serratus anterior muscle, can be injured by
■ In the axilla it gives off three branches: the posterior cu-
blows to or pressure on the posterior triangle of the neck or
taneous nerve of the arm, which supplies the skin on the
during the surgical procedure of radical mastectomy. Paral-
back of the arm down to the elbow; the nerve to the long
ysis of the serratus anterior results in the inability to rotate the
head of the triceps; and the nerve to the medial head of
scapula during the movement of abduction of the arm above
the triceps.
a right angle. The patient therefore experiences difficulty in
■ In the spiral groove of the humerus it gives off four
raising the arm above the head. The vertebral border and
branches: the lower lateral cutaneous nerve of the arm,
inferior angle of the scapula will no longer be kept closely
which supplies the lateral surface of the arm down to the
applied to the chest wall and will protrude posteriorly, a con-
elbow; the posterior cutaneous nerve of the forearm,
dition known as “winged scapula” (CD Fig.17-4).
which supplies the skin down the middle of the back of
the forearm as far as the wrist; the nerve to the lateral
head of the triceps; and the nerve to the medial head of
Axillary Nerve Injuries
the triceps and the anconeus.
The axillary nerve (see text Fig. 17-20B), which arises from
■ In the anterior compartment of the arm above the lat-
the posterior cord of the brachial plexus (C5 and 6), can be
eral epicondyle it gives off three branches: the nerve to a
injured by the pressure of a badly adjusted crutch pressing
small part of the brachialis, the nerve to the brachioradi-
upward into the armpit. The passage of the axillary nerve
alis, and the nerve to the extensor carpi radialis longus.
backward from the axilla through the quadrangular space
■ In the cubital fossa it gives off the deep branch of the
makes it particularly vulnerable here to downward displace-
radial nerve and continues as the superficial radial nerve.
ment of the humeral head in shoulder dislocations or frac-
The deep branch supplies the extensor carpi radialis
tures of the surgical neck of the humerus. Paralysis of the
brevis and the supinator in the cubital fossa and all the
deltoid and teres minor muscles results. The cutaneous
extensor muscles in the posterior compartment of the
branches of the axillary nerve, including the upper lateral
forearm. The superficial radial nerve is sensory and sup-
cutaneous nerve of the arm, are functionless, and conse-
plies the skin over the lateral part of the dorsum of
quently there is a loss of skin sensation over the lower half
the hand and the dorsal surface of the lateral three and a
of the deltoid muscle. The paralyzed deltoid wastes rapidly,
half fingers proximal to the nail beds (CD Fig. 17-5).
The Spinal Nerves and Spinal Nerve Blocks
267
C7
C8
C6
C6
C7
C8
dermatomes
palmar
cutaneous
branch
median nerve
palmar
posterior
cutaneous
cutaneous
branch
ulnar nerve
radial nerve
CD Figure 17-5
Sensory innervation of the skin of the volar (palmar) and dorsal aspects
of the hand; the arrangement of the dermatomes is also shown.
268
Chapter 17
Sensory
(The ulnar nerve supplies the medial part of the dorsum
of the hand and the dorsal surface of the medial one
A small loss of skin sensation occurs down the posterior sur-
and a half fingers; the exact cutaneous areas innervated
face of the lower part of the arm and down a narrow strip on
by the radial and ulnar nerves on the hand are subject to
the back of the forearm. A variable area of sensory loss is pre-
variation.)
sent on the lateral part of the dorsum of the hand and on the
The radial nerve is commonly damaged in the axilla
dorsal surface of the roots of the lateral three and a half fin-
and in the spiral groove.
gers. The area of total anesthesia is relatively small because
of the overlap of sensory innervation by adjacent nerves.
Injuries to the Radial Nerve
in the Axilla
Trophic Changes
In the axilla the nerve can be injured by the pressure of the
Trophic changes are slight.
upper end of a badly fitting crutch pressing up into
the armpit or by a drunkard falling asleep with one arm over
Injuries to the Radial Nerve in the
the back of a chair. It can also be badly damaged in the axilla
Spiral Groove of the Humerus
by fractures and dislocations of the proximal end of the
humerus. When the humerus is displaced downward in dis-
In the spiral groove of the humerus, the radial nerve can be
locations of the shoulder, the radial nerve, which is wrapped
injured at the time of fracture of the shaft of the humerus or
around the back of the shaft of the bone, is pulled down-
subsequently involved during the formation of the callus.
ward, stretching the nerve in the axilla excessively.
The pressure of the back of the arm on the edge of the op-
The clinical findings in injury to the radial nerve in the
erating table in an unconscious patient has also been known
axilla are as follows.
to injure the nerve at this site. The prolonged application of
a tourniquet to the arm in a person with a slender triceps
Motor
muscle is often followed by temporary radial palsy.
The clinical findings in injury to the radial nerve in the
The triceps, the anconeus, and the long extensors of the
spiral groove are as follows:
wrist are paralyzed. The patient is unable to extend the el-
The injury to the radial nerve occurs most commonly
bow joint, the wrist joint, and the fingers. Wristdrop, or flex-
in the distal part of the groove, beyond the origin of the
ion of the wrist (CD Fig. 17-6), occurs as a result of the
nerves to the triceps and the anconeus and beyond the ori-
action of the unopposed flexor muscles of the wrist. Wrist-
gin of the cutaneous nerves.
drop is very disabling because one is unable to flex the fin-
gers strongly for the purpose of firmly gripping an object
■ Motor: The patient is unable to extend the wrist and the
with the wrist fully flexed. (Try it on yourself.) If the wrist
fingers, and wristdrop occurs.
and proximal phalanges are passively extended by holding
■ Sensory: A variable small area of anesthesia is present
them in position with the opposite hand, the middle and
over the dorsal surface of the hand and the dorsal surface
distal phalanges of the fingers can be extended by the action
of the roots of the lateral three and a half fingers.
of the lumbricals and interossei, which are inserted into the
■ Trophic changes: These are very slight or absent.
extensor expansions.
The brachioradialis and supinator muscles are also par-
Injuries to the Deep Branch of the
alyzed, but supination is still performed well by the biceps
Radial Nerve
brachii.
The deep branch of the radial nerve is a motor nerve to the
extensor muscles in the posterior compartment of the fore-
arm. It can be damaged in fractures of the proximal end of the
radius or during dislocation of the radial head. The nerve sup-
ply to the supinator and the extensor carpi radialis longus will
be undamaged, and because the latter muscle is powerful, it
will keep the wrist joint extended, and wristdrop will not oc-
cur. No sensory loss occurs because this is a motor nerve.
Injuries to the Superficial Radial Nerve
Division of the superficial radial nerve, which is sensory, as
in a stab wound, results in a variable small area of anesthe-
sia over the dorsum of the hand and the dorsal surface of the
CD Figure 17-6
Wristdrop.
roots of the lateral three and a half fingers.
The Spinal Nerves and Spinal Nerve Blocks
269
Musculocutaneous Nerve Injuries
The musculocutaneous nerve (see text Fig. 17-9) is rarely in-
jured because of its protected position beneath the biceps
brachii muscle. If it is injured high up in the arm, the biceps
and coracobrachialis are paralyzed and the brachialis mus-
cle is weakened (the latter muscle is also supplied by the ra-
dial nerve). Flexion of the forearm at the elbow joint is then
produced by the remainder of the brachialis muscle and the
flexors of the forearm. When the forearm is in the prone po-
sition, the extensor carpi radialis longus and the brachiora-
dialis muscles assist in flexion of the forearm. There is also
sensory loss along the lateral side of the forearm. Wounds or
cuts of the forearm can sever the lateral cutaneous nerve of
the forearm, a continuation of the musculocutaneous nerve
beyond the cubital fossa, resulting in sensory loss along the
CD Figure 17-7
Median nerve palsy.
lateral side of the forearm.
Median Nerve Injuries
accompanied by adduction. The latter deviation is caused by
The median nerve (see text Fig. 17-9), which arises from the
the paralysis of the flexor carpi radialis and the strength of the
medial and lateral cords of the brachial plexus, gives off no cu-
flexor carpi ulnaris and the medial half of the flexor digito-
taneous or motor branches in the axilla or in the arm. In the
rum profundus. No flexion is possible at the interphalangeal
proximal third of the front of the forearm, by unnamed
joints of the index and middle fingers, although weak flexion
branches or by its anterior interosseous branch, it supplies all
of the metacarpophalangeal joints of these fingers is at-
the muscles of the front of the forearm except the flexor carpi
tempted by the interossei. When the patient tries to make a
ulnaris and the medial half of the flexor digitorum profundus,
fist, the index and to a lesser extent the middle fingers tend
which are supplied by the ulnar nerve. In the distal third of
to remain straight, whereas the ring and little fingers flex (CD
the forearm, it gives rise to a palmar cutaneous branch, which
Fig. 17-7). The latter two fingers are, however, weakened by
crosses in front of the flexor retinaculum and supplies the skin
the loss of the flexor digitorum superficialis.
on the lateral half of the palm (see CD Fig. 17-5). In the palm
Flexion of the terminal phalanx of the thumb is lost be-
the median nerve supplies the muscles of the thenar emi-
cause of paralysis of the flexor pollicis longus. The muscles
nence and the first two lumbricals and gives sensory innerva-
of the thenar eminence are paralyzed and wasted so that the
tion to the skin of the palmar aspect of the lateral three and a
eminence is flattened. The thumb is laterally rotated and
half fingers, including the nail beds on the dorsum.
adducted. The hand looks flattened and “ape-like.”
From a clinical standpoint, the median nerve is injured
occasionally in the elbow region in supracondylar fractures
Sensory
of the humerus. It is most commonly injured by stab
Skin sensation is lost on the lateral half or less of the palm of
wounds or broken glass just proximal to the flexor retinacu-
the hand and the palmar aspect of the lateral three and a half
lum; here it lies in the interval between the tendons of the
fingers. Sensory loss also occurs on the skin of the distal part
flexor carpi radialis and flexor digitorum superficialis, over-
of the dorsal surfaces of the lateral three and a half fingers.
lapped by the palmaris longus.
The area of total anesthesia is considerably less because of
The clinical findings in injury to the median nerve are
the overlap of adjacent nerves.
as follows.
Vasomotor Changes
Injuries to the Median Nerve
at the Elbow
The skin areas involved in sensory loss are warmer and drier
than normal because of the arteriolar dilatation and absence
Motor
of sweating resulting from loss of sympathetic control.
The pronator muscles of the forearm and the long flexor
Trophic Changes
muscles of the wrist and fingers, with the exception of the
flexor carpi ulnaris and the medial half of the flexor digito-
In long-standing cases, changes are found in the hand and
rum profundus, will be paralyzed. As a result, the forearm is
fingers. The skin is dry and scaly, the nails crack easily, and
kept in the supine position; wrist flexion is weak and is
atrophy of the pulp of the fingers is present.
270
Chapter 17
Injuries to the Median Nerve
Having entered the palm by passing in front of the
flexor retinaculum, the superficial branch of the ulnar
at the Wrist
nerve supplies the skin of the palmar surface of the medial
■ Motor: The muscles of the thenar eminence are paralyzed
one and a half fingers (see CD Fig. 17-5), including their
and wasted so that the eminence becomes flattened. The
nail beds; it also supplies the palmaris brevis muscle. The
thumb is laterally rotated and adducted. The hand looks
deep branch supplies all the small muscles of the hand ex-
flattened and “ape-like.” Opposition movement of the
cept the muscles of the thenar eminence and the first two
thumb is impossible. The first two lumbricals are para-
lumbricals, which are supplied by the median nerve.
lyzed, which can be recognized clinically when the
The ulnar nerve is most commonly injured at the
patient is asked to make a fist slowly, and the index and
elbow, where it lies behind the medial epicondyle, and at
middle fingers tend to lag behind the ring and little fingers.
the wrist, where it lies with the ulnar artery in front of the
■ Sensory, vasomotor, and trophic changes: These
flexor retinaculum. The injuries at the elbow are usually
changes are identical to those found in the elbow lesions.
associated with fractures of the medial epicondyle. The su-
perficial position of the nerve at the wrist makes it vulnera-
Perhaps the most serious disability of all in median nerve
ble to damage from cuts and stab wounds.
injuries is the loss of ability to oppose the thumb to the other
The clinical findings in injury to the ulnar nerve are as
fingers and the loss of sensation over the lateral fingers. The
follows.
delicate pincer-like action of the hand is no longer possible.
Carpal Tunnel Syndrome
Injuries to the Ulnar Nerve
at the Elbow
The carpal tunnel, formed by the concave anterior surface
of the carpal bones and closed by the flexor retinaculum, is
Motor
tightly packed with the long flexor tendons of the fingers,
their surrounding synovial sheaths, and the median nerve.
The flexor carpi ulnaris and the medial half of the flexor dig-
Clinically, the syndrome consists of a burning pain or “pins
itorum profundus muscles are paralyzed. The paralysis of
and needles” along the distribution of the median nerve to
the flexor carpi ulnaris can be observed by asking the patient
the lateral three and a half fingers and weakness of the
to make a tightly clenched fist. Normally, the synergistic ac-
thenar muscles. It is produced by compression of the me-
tion of the flexor carpi ulnaris tendon can be observed as it
dian nerve within the tunnel. The exact cause of the com-
passes to the pisiform bone; the tightening of the tendon will
pression is difficult to determine, but thickening of the
be absent if the muscle is paralyzed. The profundus tendons
synovial sheaths of the flexor tendons or arthritic changes in
to the ring and little fingers will be functionless, and the ter-
the carpal bones are thought to be responsible in many
minal phalanges of these fingers are therefore not capable of
cases. As would be expected, no paresthesia occurs over the
being markedly flexed. Flexion of the wrist joint will result
thenar eminence because this area of skin is supplied by the
in abduction, owing to paralysis of the flexor carpi ulnaris.
palmar cutaneous branch of the median nerve, which passes
The medial border of the front of the forearm will show flat-
superficially to the flexor retinaculum. The condition is dra-
tening, owing to the wasting of the underlying ulnaris and
matically relieved by decompressing the tunnel by making a
profundus muscles.
longitudinal incision through the flexor retinaculum.
The small muscles of the hand will be paralyzed, except
the muscles of the thenar eminence and the first two lum-
bricals, which are supplied by the median nerve. The
Ulnar Nerve Injuries
patient is unable to adduct and abduct the fingers and con-
The ulnar nerve (see text Fig. 17-20A), which arises from the
sequently is unable to grip a piece of paper placed between
medial cord of the brachial plexus (C8 and T1), gives off no
the fingers. Remember that the extensor digitorum can
cutaneous or motor branches in the axilla or in the arm. As
abduct the fingers to a small extent, but only when the
it enters the forearm from behind the medial epicondyle, it
metacarpophalangeal joints are hyperextended.
supplies the flexor carpi ulnaris and the medial half of the
It is impossible to adduct the thumb because the
flexor digitorum profundus. In the distal third of the fore-
adductor pollicis muscle is paralyzed. If the patient is
arm, it gives off its palmar and posterior cutaneous branches.
asked to grip a piece of paper between the thumb and the
The palmar cutaneous branch supplies the skin over the hy-
index finger, he or she does so by strongly contracting the
pothenar eminence; the posterior branch supplies the skin
flexor pollicis longus and flexing the terminal phalanx
over the medial third of the dorsum of the hand and the me-
(Froment’s sign).
dial one and a half fingers. Not uncommonly, the posterior
The metacarpophalangeal joints become hyperex-
branch supplies two and a half instead of one and a half
tended because of the paralysis of the lumbrical and
fingers. It does not supply the skin over the distal part of the
interosseous muscles, which normally flex these joints. Be-
dorsum of these fingers.
cause the first and second lumbricals are not paralyzed (they
The Spinal Nerves and Spinal Nerve Blocks
271
CD Figure 17-8
Ulnar nerve palsy.
are supplied by the median nerve), the hyperextension of
muscle is not paralyzed, and marked flexion of the
the metacarpophalangeal joints is most prominent in the
terminal phalanges occurs.
fourth and fifth fingers. The interphalangeal joints are
■ Sensory: The main ulnar nerve and its palmar cuta-
flexed, owing again to the paralysis of the lumbrical and in-
neous branch are usually severed; the posterior cuta-
terosseous muscles, which normally extend these joints
neous branch, which arises from the ulnar nerve trunk
through the extensor expansion. The flexion deformity at
about 2.5 in. (6.25 cm) above the pisiform bone, is usu-
the interphalangeal joints of the fourth and fifth fingers is
ally unaffected. The sensory loss will therefore be
obvious because the first and second lumbrical muscles of
confined to the palmar surface of the medial third of
the index and middle fingers are not paralyzed. In long-
the hand and the medial one and a half fingers and to
standing cases the hand assumes the characteristic “claw”
the dorsal aspects of the middle and distal phalanges of
deformity (main en griffe). Wasting of the paralyzed mus-
the same fingers.
cles results in flattening of the hypothenar eminence and
■ Vasomotor and trophic changes: These are the same as
loss of the convex curve to the medial border of the hand.
those described for injuries at the elbow. It is important
Examination of the dorsum of the hand will show hollow-
to remember that with ulnar nerve injuries, the higher
ing between the metacarpal bones caused by wasting of the
the lesion is, the less obvious is the clawing deformity of
dorsal interosseous muscles (CD Fig. 17-8).
the hand.
Unlike median nerve injuries, lesions of the ulnar nerve
Sensory
leave a relatively efficient hand. The sensation over the lateral
Loss of skin sensation will be observed over the anterior and
part of the hand is intact, and the pincer-like action of the
posterior surfaces of the medial third of the hand and the
thumb and index finger is reasonably good, although there is
medial one and a half fingers.
some weakness, owing to loss of the adductor pollicis.
Vasomotor Changes
Arterial Innervation and
The skin areas involved in sensory loss are warmer and drier
than normal because of the arteriolar dilatation and absence
Raynaud’s Disease
of sweating resulting from loss of sympathetic control.
The arteries of the upper limb are innervated by sympa-
thetic nerves. The preganglionic fibers originate from cell
Injuries to the Ulnar Nerve
bodies in the second to eighth thoracic segments of the
at the Wrist
spinal cord. They ascend in the sympathetic trunk and
■ Motor: The small muscles of the hand will be paralyzed
synapse in the middle cervical, inferior cervical, first tho-
and show wasting, except for the muscles of the thenar
racic, or stellate ganglia. The postganglionic fibers join the
eminence and the first two lumbricals, as described (see
nerves that form the brachial plexus and are distributed to
previous page). The clawhand is much more obvious in
the arteries within the branches of the plexus. For example,
wrist lesions because the flexor digitorum profundus
the digital arteries of the fingers are supplied by postgan-
272
Chapter 17
glionic sympathetic fibers that run in the digital nerves.
Vasospastic diseases involving digital arterioles, such as
Raynaud’s disease, may require a cervicodorsal pregan-
LUMBAR PLEXUS
glionic sympathectomy to prevent necrosis of the fingers.
The operation is followed by arterial vasodilatation, with
consequent increased blood flow to the upper limb.
CLINICAL NOTES
INTERCOSTAL
ON THE NERVES OF
NERVES
THE LOWER LIMB
Skin Innervation of the Chest
Tendon Reflexes of the
Wall and Referred Pain
Lower Limb
Above the level of the sternal angle, the cutaneous innerva-
Skeletal muscles receive a segmental innervation. Most
tion of the anterior chest wall is derived from the supraclav-
muscles are innervated by two, three, or four spinal nerves
icular nerves (C3 and 4). Below this level, the anterior and
and therefore by the same number of segments of the spinal
lateral cutaneous branches of the intercostal nerves supply
cord. The segmental innervation of the following muscles in
oblique bands of skin in regular sequence. The skin on
the lower limb should be known because it is possible to test
the posterior surface of the chest wall is supplied by the pos-
them by eliciting simple muscle reflexes in the patient:
terior rami of the spinal nerves. The arrangement of the
■ Patellar tendon reflex (knee jerk): L2, 3, and 4 (exten-
dermatomes is shown in CD Figs. 17-1 and 17-2.
sion of the knee joint on tapping the patellar tendon)
An intercostal nerve not only supplies areas of skin but
■ Achilles tendon reflex (ankle jerk): S1 and S2 (plantar
also supplies the ribs, costal cartilages, intercostal muscles,
flexion of the ankle joint on tapping the Achilles tendon)
and parietal pleura lining the intercostal space. Further-
more, the seventh to eleventh intercostal nerves leave the
thoracic wall and enter the anterior abdominal wall so that
Femoral Nerve Injury
they, in addition, supply dermatomes on the anterior
The femoral nerve (L2, 3, and 4) enters the thigh from be-
abdominal wall, muscles of the anterior abdominal wall,
hind the inguinal ligament, at a point midway between the
and parietal peritoneum. This latter fact is of great clinical
anterior superior iliac spine and the pubic tubercle; it lies
importance because it means that disease in the thoracic
about a fingerbreadth lateral to the femoral pulse. About 2
wall may be revealed as pain in a dermatome that extends
in. (5 cm) below the inguinal ligament, the nerve splits into
across the costal margin into the anterior abdominal wall.
its terminal branches (see text Fig. 17-29).
For example, a pulmonary thromboembolism or a pneu-
The femoral nerve can be injured in stab or gunshot
monia with pleurisy involving the costal parietal pleura
wounds, but a complete division of the nerve is rare. The
could give rise to abdominal pain and tenderness and rigid-
following clinical features are present when the nerve is
ity of the abdominal musculature. The abdominal pain in
completely divided:
these instances is called referred pain.
■ Motor: The quadriceps femoris muscle is paralyzed, and
the knee cannot be extended. In walking, this is compen-
Herpes Zoster
sated for to some extent by use of the adductor muscles.
Herpes zoster, or shingles, is a relatively common condition
■ Sensory: Skin sensation is lost over the anterior and me-
caused by the reactivation of the latent varicella-zoster virus
dial sides of the thigh, over the medial side of the lower
in a patient who has previously had chickenpox. The lesion
part of the leg, and along the medial border of the foot as
is seen as an inflammation and degeneration of the sensory
far as the ball of the big toe; this area is normally supplied
neuron in a cranial or spinal nerve with the formation of
by the saphenous nerve.
vesicles with inflammation of the skin. In the thorax the first
symptom is a band of dermatomal pain in the distribution
Sciatic Nerve Injury
of the sensory neuron in a thoracic spinal nerve, followed in
a few days by a skin eruption. The condition occurs most
The sciatic nerve (L4 and 5 and S1, 2, and 3) curves later-
frequently in patients older than 50 years.
ally and downward through the gluteal region, situated at
The Spinal Nerves and Spinal Nerve Blocks
273
first midway between the posterosuperior iliac spine and the
The result of operative repair of a sciatic nerve injury is
ischial tuberosity, and lower down, midway between the tip
poor. It is rare for active movement to return to the small
of the greater trochanter and the ischial tuberosity. The
muscles of the foot, and sensory recovery is rarely complete.
nerve then passes downward in the midline on the posterior
Loss of sensation in the sole of the foot makes the develop-
aspect of the thigh and divides into the common peroneal
ment of trophic ulcers inevitable.
and tibial nerves, at a variable site above the popliteal fossa
(see text Figs. 17-42 and 17-46).
Sciatica
Trauma to the Sciatic Nerve
Sciatica describes the condition in which patients have pain
along the sensory distribution of the sciatic nerve. Thus, the
The nerve is sometimes injured by penetrating wounds,
pain is experienced in the posterior aspect of the thigh, the
fractures of the pelvis, or dislocations of the hip joint. It is
posterior and lateral sides of the leg, and the lateral part of
most frequently injured by badly placed intramuscular in-
the foot. Sciatica can be caused by prolapse of an interver-
jections in the gluteal region. To avoid this injury, injec-
tebral disc with pressure on one or more roots of the lower
tions into the gluteus maximus or the gluteus medius should
lumbar and sacral spinal nerves, pressure on the sacral
be made well forward on the upper outer quadrant of the
plexus or sciatic nerve by an intrapelvic tumor, or inflam-
buttock. Most nerve lesions are incomplete, and in 90% of
mation of the sciatic nerve or its terminal branches.
injuries, the common peroneal part of the nerve is the most
affected. This can probably be explained by the fact that the
common peroneal nerve fibers lie most superficial in the
Common Peroneal Nerve Injury
sciatic nerve. The following clinical features are present:
The common peroneal nerve (see text Fig. 17-38) is in an
■ Motor: The hamstring muscles are paralyzed, but weak
exposed position as it leaves the popliteal fossa and winds
flexion of the knee is possible because of the action of the
around the neck of the fibula to enter the peroneus longus
sartorius (femoral nerve) and gracilis (obturator nerve).
muscle.
All the muscles below the knee are paralyzed, and the
It is commonly injured in fractures of the neck of the
weight of the foot causes it to assume the plantar-flexed
fibula and by pressure from casts or splints. The following
position, or foot drop (CD Fig. 17-9).
clinical features are present:
■ Sensory: Sensation is lost below the knee, except for a
■ Motor: The muscles of the anterior and lateral compart-
narrow area down the medial side of the lower part of the
ments of the leg are paralyzed, namely, the tibialis an-
leg and along the medial border of the foot as far as the
terior, the extensor digitorum longus and brevis, the
ball of the big toe, which is supplied by the saphenous
peroneus tertius, the extensor hallucis longus (supplied by
nerve (femoral nerve).
the deep peroneal nerve), and the peroneus longus and
brevis (supplied by the superficial peroneal nerve). As a
result, the opposing muscles, the plantar flexors of the an-
kle joint and the invertors of the subtalar and transverse
tarsal joints, cause the foot to be plantar flexed (foot drop)
and inverted, an attitude referred to as equinovarus.
■ Sensory: Loss of sensation occurs down the anterior and
lateral sides of the leg and dorsum of the foot and toes, in-
cluding the medial side of the big toe. The lateral border
of the foot and the lateral side of the little toe are virtually
unaffected
(sural nerve, mainly formed from tibial
nerve). The medial border of the foot as far as the ball of
the big toe is completely unaffected (saphenous nerve, a
branch of the femoral nerve).
When the injury occurs distal to the site of origin of the
lateral cutaneous nerve of the calf, the loss of sensibility is
confined to the area of the foot and toes.
Tibial Nerve Injury
The tibial nerve (see text Fig. 17-42) leaves the popliteal
CD Figure 17-9
Foot drop. With this condition, the individ-
fossa by passing deep to the gastrocnemius and soleus mus-
ual catches his or her toes on the ground when walking.
cles. Because of its deep and protected position, it is rarely
274
Chapter 17
injured. Complete division results in the following clinical
features:
Invasion of the Sacral Plexus
■ Motor: All the muscles in the back of the leg and the sole
by Malignant Tumors
of the foot are paralyzed. The opposing muscles dorsiflex
the foot at the ankle joint and evert the foot at the subta-
The nerves of the sacral plexus can become invaded by
lar and transverse tarsal joints, an attitude referred to as
malignant tumors extending from neighboring viscera.
calcaneovalgus.
A carcinoma of the rectum, for example, can cause severe
■ Sensory: Sensation is lost on the sole of the foot; later,
intractable pain down the lower limbs.
trophic ulcers develop.
Referred Pain from the
Obturator Nerve Injury
Obturator Nerve
The obturator nerve (L2, 3, and 4) enters the thigh as ante-
rior and posterior divisions through the upper part of the ob-
The obturator nerve lies on the lateral wall of the pelvis and
turator foramen. The anterior division descends in front of
supplies the parietal peritoneum. An inflamed appendix
the obturator externus and the adductor brevis, deep to the
hanging down into the pelvic cavity could cause irritation of
floor of the femoral triangle. The posterior division descends
the obturator nerve endings, leading to referred pain down
behind the adductor brevis and in front of the adductor
the inner side of the right thigh. Inflammation of the ovaries
magnus (see text Fig. 17-33).
can produce similar symptoms.
It is rarely injured in penetrating wounds, in anterior dis-
locations of the hip joint, or in abdominal herniae through
the obturator foramen. It may be pressed on by the fetal head
CLINICAL
during parturition. The following clinical features occur:
■ Motor: All the adductor muscles are paralyzed except
ANATOMY OF
the hamstring part of the adductor magnus, which is
supplied by the sciatic nerve.
SPINAL NERVE
■ Sensory: The cutaneous sensory loss is minimal on the
medial aspect of the thigh.
BLOCKS
Referred Pain from the Hip Joint
Brachial Plexus Block
The femoral nerve not only supplies the hip joint but, via
the intermediate and medial cutaneous nerves of the thigh,
In the neck, the brachial plexus occupies the lower part
also supplies the skin of the front and medial side of the
of the posterior triangle (CD Fig. 17-10). It lies below and
thigh. It is not surprising, therefore, for pain originating in
anterior to a line connecting the cricoid cartilage of
the hip joint to be referred to the front and medial side of the
the larynx to the midpoint of the clavicle. In the axilla, the
thigh. The posterior division of the obturator nerve supplies
brachial plexus and its branches are arranged within
both the hip and knee joints. This would explain why hip
the axillary sheath around the axillary artery, which can be
joint disease sometimes gives rise to pain in the knee joint.
palpated.
Four techniques can be used—interscalene block, supra-
clavicular block, infraclavicular block, and axillary block.
SACRAL PLEXUS
Interscalene Block
Procedure: At the level of the cricoid cartilage (C6) the
Pressure from the Fetal Head on
posterior border of the sternocleidomastoid muscle can
be palpated. With the head turned laterally and upward
the Sacral Plexus
from the side of the block, the palpating finger can feel
During the later stages of pregnancy, when the fetal head
the groove between the scalenus anterior and the
has descended into the pelvis, the mother often complains
scalenus medius muscles just lateral to the sternocleido-
of discomfort or aching pain extending down one of the
mastoid muscle (see CD Fig. 17-10). The blocking
lower limbs. The discomfort, caused by pressure from the
needle is inserted into the interval between the scalene
fetal head, is often relieved by changing position, such as
muscles, and the roots of the upper part of the brachial
lying on the side in bed.
plexus can be blocked.
The Spinal Nerves and Spinal Nerve Blocks
275
scalenus
anterior muscle
sternocleidomastoid
scalenus
muscle
medius muscle
trapezius
muscle
deltoid muscle
lateral pectoral
nerve
musculo-
axillary
cutaneous
artery
nerve
lateral
cord
pectoralis major
muscle
medial cord
axillary
sheath
axillary vein
CD Figure 17-10
A. Brachial plexus block. Supraclavicular block. The needle is inserted
just posterior to the posterior border of the sternocleidomastoid muscle at the level of the
cricoid cartilage at the lower anterior corner of the posterior triangle. The needle is
directed caudally behind the palpable subclavian artery. In an infraclavicular block, the
needle is inserted inferior to the midpoint of the clavicle and is directed laterally in the
direction of the head of the humerus and toward the subclavian artery. B. Sites of
supraclavicular and infraclavicular brachial plexus blocks. C. Axillary nerve block. The
axillary artery is palpated and the needle is inserted into the axillary sheath (see text).
D. Site of the axillary brachial plexus block.
Chapter 17
276
Supraclavicular Block
Musculocutaneous Nerve Block
Procedure: The trunks of the brachial plexus can be
blocked as they cross the first rib and enter the axilla (see
Area of anesthesia: The anterior and posterior surfaces of
CD Fig. 17-10). The third part of the subclavian artery is
the lateral border of the forearm down as far as the thenar
first palpated in the lower anterior corner of the posterior
eminence (see CD Figs. 17-1 and 17-2)
triangle of the neck. The posterior border of the stern-
Indications: Repair of lacerations on the lateral border of
ocleidomastoid muscle is then felt. A blocking needle is
the forearm
inserted at the level of the cricoid cartilage between the
Procedure: These include the following:
scalenus anterior and the scalenus medius muscles and
■ Brachial plexus approach: The musculocutaneous
directed caudally behind the subclavian artery toward
nerve trunk may be blocked with the rest of the brachial
the upper surface of the first rib (see CD Fig. 17-10). It is
plexus (see CD Fig. 17-10). The infraclavicular or axil-
here that the brachial plexus is very compact, consisting
lary approach is used; in the axillary approach great
of the upper middle and lower trunks.
care has to be taken to ensure that the anesthetic agent
Anatomy of complications: The subclavian artery lies
rises sufficiently high in the axillary sheath to block the
between the scalenus anterior and scalenus medius mus-
musculocutaneous nerve.
cles just behind the clavicle and may be pierced by the
■ Lateral cutaneous nerve of the forearm approach: The
needle. The cervical dome of parietal pleura is situated
musculocutaneous nerve may also be blocked as it
close to the brachial plexus, and a pneumothorax can be
emerges between the biceps and the brachialis muscles
caused if the needle enters the pleural cavity.
just above the lateral epicondyle of the humerus, where
it becomes the lateral cutaneous nerve of the forearm
(CD Fig. 17-11). The needle is inserted just lateral to the
Infraclavicular Block
tendon of the biceps muscle on a line between the two
Procedure: The middle of the clavicle is identified. A
epicondyles of the humerus.
blocking needle is inserted 1 in. (2.5 cm) inferior to it
and directed laterally in the direction of the head of the
Median Nerve Block
humerus and toward the subclavian artery. The anes-
thetic solution is infiltrated around the trunks of the
Area of anesthesia: The skin on the lateral half of the
brachial plexus (see CD Fig. 17-10).
palm, the palmar aspect of the lateral three and a half
Anatomy of complications: The close relationship of the
fingers, including the nail beds on the dorsum (see CD
axillary vessels to the brachial plexus within the axillary
Fig. 17-16)
sheath means that vessel puncture and hematoma for-
Indications: Repair of lacerations of the palm and fingers
mation may occur. Frequent aspirations are necessary
Procedures: These include the following:
before the anesthetic agent is injected.
■ Block at the elbow: With the elbow joint extended, the
brachial artery can easily be palpated in the cubital fossa
Axillary Block
on the medial side of the tendon of the biceps muscle.
The needle is inserted on the medial side of the brachial
Procedure: With the arm abducted to an angle greater
artery (CD Fig. 17-12).
than 90°, the axillary artery within the axillary sheath
■ Block at the wrist: Here the median nerve lies on
may be palpated high up in the axilla (see CD Fig. 17-
the medial side of the tendons of the flexor carpi radi-
10). The artery is compressed, and a blocking needle is
alis and to the lateral side of the flexor digitorum su-
inserted just proximal to the point of compression into
perficialis (CD Fig. 17-13); it usually lies posterior
the axillary sheath. The cords and branches of the
to the tendon of the palmaris longus muscle (some-
plexus lie within the sheath along with the artery. The
times absent). The nerve may be infiltrated here with
disadvantage of this approach is the difficulty in block-
local anesthetic just proximal to the flexor retinaculum
ing the musculocutaneous nerve. The object of com-
(i.e., just proximal to the distal transverse crease in front
pressing the artery distal to the point of injection is
of the wrist). The needle is inserted for 3/8 in. between
to close off the axillary sheath distally so that the
the tendons of flexor carpi radialis and the palmaris
anesthetic agent may rise in the sheath to the musculo-
longus.
cutaneous nerve.
Anatomy of complications: The close relationship of the
The palmar cutaneous branch of the median nerve
axillary vessels to the brachial plexus within the axillary
leaves the main trunk just proximal to the distal transverse
sheath means that vessel puncture and hematoma for-
crease of the palm, and, unless this nerve is also blocked,
mation may occur. Frequent aspirations are necessary
the sensation to the skin on the lateral part of the palm will
before the anesthetic agent is injected.
remain intact.
The Spinal Nerves and Spinal Nerve Blocks
277
deltoid muscle
brachialis
muscle
biceps brachii
triceps
muscle
triceps muscle
muscle
brachialis
muscle
lateral
cutaneous
musculocutaneous
nerve of the
nerve becoming
forearm
lateral cutaneous
nerve of
lateral
forearm
biceps
epicondyle
brachii
lateral
muscle
epicondyle
lateral
of humerus
cutaneous
nerve of
forearm
posterior
cutaneous
brachioradialis
nerve of
muscle
forearm
CD Figure 17-11
Lateral cutaneous nerve of the forearm block. A and B show the
musculocutaneous nerve becoming the lateral cutaneous nerve of the forearm. The nerve
is blocked just lateral to the tendon of the biceps brachii muscle on a line between the two
epicondyles of the humerus.
lateral to the tendons of the flexor carpi ulnaris muscle
Ulnar Nerve Block
and the pisiform bone (see CD Fig. 17-13). The ul-
nar artery lies on the lateral side of the ulnar nerve.
Area of anesthesia: The skin of the medial one third of
The needle is inserted just lateral to the flexor carpi ul-
the palmar and dorsal surfaces of the hand and the pal-
naris tendon at the level of the distal transverse crease of
mar and dorsal surfaces of the medial one and a half
the wrist.
fingers (see CD Fig. 17-16)
Indications: Repair of lacerations of the hand and fingers
Note that the dorsal cutaneous branch of the ulnar
Procedures: These involve the following:
nerve (see CD Fig. 17-16) leaves the main trunk about 2 in.
■ Block at the elbow: At the elbow, the ulnar nerve enters
(5 cm) proximal to the wrist; an ulnar nerve block at the
the forearm between the olecranon process of the ulna
wrist will therefore leave the skin sensation on the dorsum of
and the medial epicondyle of the humerus (CD Fig. 17-
the hand and fingers intact.
14). Here the nerve may be palpated and infiltrated with
Also, the superficially placed palmar cutaneous branch
an anesthetic agent.
of the ulnar nerve leaves the nerve trunk a variable distance
■ Block at the wrist: At the wrist, the ulnar nerve en-
proximal to the transverse crease of the wrist; unless this
ters the hand anterior to the flexor retinaculum and
nerve is also infiltrated with anesthetic, the ulnar block at
278
Chapter 17
biceps
brachii
brachialis
muscle
muscle
brachial
artery
cephalic
median
vein
biceps
nerve
brachii
bicipital
brachial
aponeurosis
artery
biceps
biceps
medial
brachii
brachii
epicondyle
tendon
tendon
brachial
basilic
lateral
artery
vein
epicondyle
median
median
nerve
cubital
vein
medial
epicondyle
of humerus
pronator
teres
muscle
CD Figure 17-12
A and B. Median nerve block at the elbow. The brachial artery is
identified in the cubital fossa, and the needle is inserted on the medial side of the artery.
the wrist will leave the sensory nerve supply to the medial
the level of the proximal transverse flexor crease on the
part of the palm intact.
lateral side of the radial artery, the nerve may be infil-
trated with an anesthetic solution. Since other terminal
branches of the radial nerve run in the subcutaneous tis-
Radial Nerve Block
sue on the dorsum of the wrist, a subcutaneous wheal of
Area of anesthesia: The skin of the back of the arm down
local anesthetic is necessary; this should run across the
as far as the elbow, the skin of the lower lateral surface of
lateral half of the dorsum of the wrist.
the arm down to the elbow, the skin down the middle of
the posterior surface of the forearm as far as the wrist, the
Digital Nerve Blocks
skin of the lateral half of the dorsal surface of the hand, and
the dorsal surface of the lateral three and a half fingers
Area of anesthesia: Skin of the fingers. Each finger is
proximal to the nail beds (see CD Figs. 17-1 and 17-2)
supplied by four digital nerves at the 2 o’clock, 5 o’clock,
Indications: Repair of lacerations of the hand:
7 o’clock, and 10 o’clock positions. The palmar digital
Procedures: These involve the following:
nerves are derived from the ulnar and median nerves; the
■
Block at the elbow: At the elbow, the radial nerve de-
dorsal digital nerves are derived from the ulnar and radial
scends anterior to the lateral epicondyle of the humerus
nerves (CD Fig.17-16).
in the interval between the brachialis and the brachiora-
The palmar digital nerves, which arise from the su-
dialis muscles (CD Fig.17-15). With the elbow joint
perficial terminal branch of the ulnar nerve in the hand,
extended, the lateral edge of the biceps tendon is easily
supply the palmar surface of the medial one and a half
palpated. The needle is inserted halfway between the
fingers, including their nail beds. The dorsal digital
tendon and the tip of the lateral epicondyle, and the local
nerves, which arise from the dorsal cutaneous branch of
anesthetic is injected at this point.
the ulnar nerve in the forearm, supply the dorsal surface
■
Block at the wrist: Just proximal to the wrist, the superfi-
of the proximal parts of the medial one and a half fingers
cial branch of the radial nerve lies lateral to the radial
(see CD Fig. 17-16).
artery. The nerve leaves the artery and passes laterally and
The palmar digital nerves, which arise from the me-
backward under the tendon of brachioradialis to reach
dian nerve in the palm, supply the palmar surface of the
the posterior surface of the wrist (see CD Fig. 17-15). At
lateral three and a half fingers, including their nail beds.
flexor
retinaculum
pisiform
bone
flexor carpi
ulnaris tendon
median nerve
ulnar nerve
flexor carpi
radialis tendon
ulnar artery
palmaris longus
tendon
flexor
flexor pollicis
digitorum
longus tendon
superficialis
tendons
CD Figure 17-13
A and B. Me-
dian and ulnar nerve blocks at the
distal transverse
wrist. In a median nerve block, the
pisiform bone
crease (proximal
needle is inserted just proximal to
edge of flexor
the distal transverse crease of the
ulnar nerve
retinaculum)
wrist between the tendons of
median nerve
flexor carpi radialis and the pal-
ulnar artery
maris longus. In an ulnar nerve
block, the needle is inserted just
lateral to the flexor carpi ulnaris
tendon at the level of the distal
transverse crease of the wrist.
olecranon
process
medial epicondyle
of humerus
ulnar
medial
nerve
epicondyle
CD Figure 17-14
A and B. Ulnar
nerve block at the elbow. The
triceps
olecranon
ulnar
ulnar nerve may be palpated
nerve
muscle
process
between the olecranon process of
of ulna
the ulna and the medial epi-
condyle of the humerus, where it
may be infiltrated with anesthetic.
280
Chapter 17
biceps brachii tendon
radial
nerve
lateral
epicondyle
of humerus
superficial branch
CD Figure 17-15
A. Radial nerve
of radial nerve
block at the elbow. The needle is
inserted halfway between the
tendon of the biceps brachii and
the tip of the lateral epicondyle of
the humerus. B. Radial nerve
block at the wrist. The needle is
inserted into the subcutaneous
tissue on the dorsum of the hand,
tendon of
and a wheal of anesthetic is
brachioradialis
placed across the lateral half of
muscle
the dorsum of the wrist.
The dorsal digital nerves, which arise from the superficial
■ Metacarpal head block: The needle is inserted in the
branch of the radial nerve, supply the dorsal surface of
palm at the metacarpal head and directed slightly distally
the proximal parts of the lateral three and a half fingers
and medially and then slightly distally and laterally to
(see CD Fig. 17-16).
block the palmar digital nerves (see CD Fig. 17-17). The
Note that the origins of the dorsal digital nerves from
dorsal digital nerves, if they remain unblocked, are han-
the ulnar and radial nerves are subject to variation.
dled with an injection across the base of the dorsum of
Indications: Repair of lacerations involving individual
the proximal phalanx.
fingers; removal of nails
■ Ring block: Since the digital nerves lie in pairs on ei-
Procedures: These involve the following:
ther side of the proximal phalanges, they are easily
■
Web space method: At the web space, the digital nerves
blocked at the base of the digit (see CD Fig. 17-16).
are about to enter the fingers (CD Fig. 17-17). The nee-
The needle is inserted on both sides of the base of the
dle is inserted about 0.5 cm, and the nerves are infiltrated
proximal phalanx, and the anesthetic agent is infiltrated
with the anesthetic agent. A block on both sides of the fin-
around the nerves between the bone and the skin; this
ger adequately deals with the four digital nerves supplying
produces a half-ring block on either side of the finger
the finger. When blocking the digital nerves of the index
(see CD Fig. 17-17).
and little fingers, a subcutaneous wheal of anesthetic so-
lution must be deposited on the lateral side of the index
Thoracic Spinal Nerve Blocks
finger and the medial side of the little finger.
■ Dorsal metacarpal method: A skin wheal of anesthetic is
raised between the metacarpal bones on the dorsum of
Intercostal Nerve Block
the hand (see CD Fig. 17-17). The needle is inserted
through the wheal and advanced slowly forward between
Area of anesthesia: The skin and the parietal pleura cov-
the metacarpal bones, stopping just short of the palmar
ering the outer and inner surfaces of each intercostal
skin. The anesthetic solution will block the common
space respectively; the seventh to the eleventh intercostal
palmar and dorsal digital nerves.
nerves supply the skin and the parietal peritoneum
The Spinal Nerves and Spinal Nerve Blocks
281
dorsal
dorsal extensor
expansion
dorsal digital nerve
phalanx
long flexor
tendons
palmar digital nerve
palmar
radial
nerve
radial
ulnar
median
nerve
nerve
nerve
ulnar
nerve
median nerve
median nerve
superficial
branch of
dorsal
radial
cutaneous
nerve
branch of
ulnar nerve
radial
ulnar
nerve
nerve
CD Figure 17-16
A. Transverse section of the finger showing the location of the dorsal
and palmar digital nerves. B. Palmar surface of hand and fingers showing the origin of the
palmar digital nerves. C. Palmar surface of the hand and fingers showing the areas of skin
supplied by the ulnar, median, and radial nerves. D. Dorsal surface of the hand and
fingers showing the origin of the dorsal digital nerves. E. Dorsal surface of the hand and
fingers showing the areas of skin supplied by the radial, ulnar, and median nerves.
covering the outer and inner surfaces of the abdominal
Procedure: To produce analgesia of the anterior and lat-
wall, respectively; therefore, these areas will also be anes-
eral thoracic and abdominal walls, the intercostal nerve
thetized. In addition, the periosteum of the adjacent ribs
should be blocked before the lateral cutaneous branch
is anesthetized.
arises at the midaxillary line. The ribs may be identified
Indications: Repair of lacerations of the thoracic and ab-
by counting up from the twelfth or down from the second
dominal walls; relief of pain in rib fractures and to allow
(opposite sternal angle). The needle is directed toward
pain-free respiratory movements
the rib near the lower border (CD Fig. 17-18), and the tip
282
Chapter 17
digital nerve
metacarpal bone
web space method
dorsal metacarpal method
CD Figure 17-17
Digital nerve blocks.
A. Web space method. The needle is
inserted about 0.5 cm into the web space. A
block on both sides of the finger anes-
thetizes the four digital nerves to the finger.
B. Dorsal metacarpal method. The needle is
directed forward between the metacarpal
bones, stopping just short of the palmar
skin. The four digital nerves to each finger
are blocked. C. Metacarpal head block. The
needle is inserted in the palm at the level of
the metacarpal head and directed slightly
distally and medially and then slightly
distally and laterally. D. Ring block. The nee-
dle is inserted on both sides of the base of
the proximal phalanx to produce a half-ring
metacarpal head block
ring block
block on either side of the finger.
comes to rest near the subcostal groove, where the local
always be performed before injecting the anesthetic. A
anesthetic is infiltrated around the nerve. Remember
small hematoma may result.
that the order of structures lying in the neurovascular
bundle from above downward is intercostal vein, artery,
Anterior Abdominal Nerve Blocks
and nerve, and that these structures are situated between
the posterior intercostal membrane of the internal inter-
Area of anesthesia: Skin of the anterior abdominal wall.
costal muscle and the parietal pleura. Furthermore,
The nerves of the anterior and lateral abdominal walls
laterally the nerve lies between the internal intercostal
are the anterior rami of the seventh through the twelfth
muscle and the subcostals and the innermost intercostals
thoracic nerves and the first lumbar nerve.
(i.e., transverse thoracic muscle).
Indications: Repair of lacerations of the anterior
Anatomy of complications: These include the following:
abdominal wall
■
Pneumothorax: This complication can occur if the nee-
Procedure: The anterior ends of the intercostal nerves
dle point misses the subcostal groove and penetrates too
T7 through T11 enter the abdominal wall by leaving the
deeply through the parietal pleura.
intercostal spaces and passing posterior to the costal car-
■ Hemorrhage: Puncture of the intercostal blood vessels.
tilages (CD Fig. 17-19). An abdominal field block is most
This is a common complication so that aspiration should
easily carried out along the lower border of the costal
The Spinal Nerves and Spinal Nerve Blocks
283
posterior ramus
2nd thoracic
internal intercostal
spinal nerve
muscle
artery
anterior ramus
intercostobrachial
vein
nerve
external
intercostal
muscle
intercostal nerve
nerve
anterior
cutaneous
branch
innermost
intercostal
muscle
lateral
cutaneous
branch
CD Figure 17-18
Intercostal nerve block. A. The distribution of two intercostal nerves
relative to the rib cage. B. Section through an intercostal space showing the positions of
the intercostal nerve, artery, and vein relative to the intercostal muscles. The needle is
directed toward the rib near the lower border, and the tip comes to rest near the subcostal
groove.
margin and then infiltrating the nerves as they emerge
The two nerves are easily blocked by inserting the anes-
between the xiphoid process and the tenth or eleventh rib
thetic needle 1 in. (2.5 cm) above the anterior superior iliac
along the costal margin.
spine on the spinoumbilical line (see CD Fig. 17-19).
Lumbar Spinal Nerve Blocks
Genitofemoral Nerve Block
Area of anesthesia: Small area of skin of the thigh below
the inguinal ligament and adjacent part of the scrotum or
Ilioinguinal and Iliohypogastric
labium majus
Indications: Repair of lacerations in the thigh and geni-
Nerve Blocks
tal area
Area of anesthesia: Skin of the lower part of the anterior
Procedure: The genitofemoral nerve (L1 and L2) runs
abdominal wall
downward under the inguinal ligament at a point
Indications: Repair of lacerations on the anterior ab-
halfway between the anterior superior iliac spine and the
dominal wall
symphysis pubis. The terminal branches are most easily
Procedure: The ilioinguinal nerve (L1) passes forward
blocked by infiltrating the subcutaneous tissue through a
around the anterior abdominal wall, through the in-
needle inserted through the skin lateral to the pubic
guinal canal, and emerges through the superficial in-
tubercle (see CD Fig. 17-19).
guinal ring to supply the skin of the groin and part of the
scrotum or labium majus. The iliohypogastric nerve (L1)
Femoral Nerve Block
passes around the abdominal wall and pierces the exter-
nal oblique aponeurosis above the superficial inguinal
Area of anesthesia: Skin of the front and medial side of
ring to supply the skin (see CD Fig. 17-19).
the thigh, extending down the medial side of the knee
284
Chapter 17
iliohypogastric
nerve
ilioinguinal nerve
anterior superior
iliac spine
genitofemoral nerve
pubic turbercle
CD Figure 17-19
Anterior abdominal
wall nerve blocks. A and B. T7
through T11 intercostal nerves are
costal margin
blocked (x) as they emerge from be-
neath the costal margin. The
iliohypogastric and ilioinguinal nerves
are blocked by inserting the needle
about 1 in. above the anterior superior
iliac spine on the spinoumbilical line
(x). The terminal branches of the
anterior superior
pubic tubercle
genitofemoral nerve are blocked by in-
iliac spine
serting the needle through the skin
just lateral to the pubic tubercle and
infiltrating the subcutaneous tissue
with anesthetic solution (x).
and leg, and along the medial border of the foot as far as
medial side of the knee after emerging between
the ball of the big toe
the tendons of sartorius and gracilis muscles (CD Fig.
Indications: Repair of lacerations of the thigh, medial
17-21).
side of the leg, and medial side of the foot
The nerve may be blocked by inserting the anesthetic
Procedure: The femoral nerve (L2 through L 4) enters
needle on the medial side of the knee joint either over the
the thigh beneath the inguinal ligament at a point mid-
medial femoral condyle or lower down over the condyle of
way between the anterior superior iliac spine and the pu-
the tibia (see CD Fig. 17-21). Care should be taken to avoid
bic tubercle (CD Fig. 17-20). Here it lies lateral to the
the great saphenous vein. The nerve may also be blocked at
femoral artery.
the ankle where it passes anterior to the medial malleolus
The nerve may be blocked by introducing the anes-
(see CD Fig. 17-21).
thetic needle just below the midpoint of the inguinal liga-
ment and lateral to the femoral artery (see CD Fig. 17-20).
Lateral Cutaneous Nerve of the
Saphenous Nerve Block
Thigh Block
Area of anesthesia: Skin of the medial side of the leg and
Area of anesthesia: Skin of the anterolateral surface of
the medial border of the foot down as far as the ball of the
the thigh down to the lateral side of the knee
big toe
Indications: Repair of lacerations on the anterolateral
Indications: Repair of lacerations on the medial side of
surface of the thigh
the leg and the medial side of the foot
Procedure: The lateral cutaneous nerve of the thigh
Procedure: The saphenous nerve is a continuation
(L2 and L3) enters the thigh behind (or through)
of the femoral nerve and becomes superficial on the
the lateral end of the inguinal ligament just medial to
The Spinal Nerves and Spinal Nerve Blocks
285
lateral cutaneous nerve
of the thigh
iliacus muscle
anterior superior
psoas muscle
iliac spine
inguinal ligament
femoral nerve
tensor fasciae latae muscle
sartorius muscle (cut)
femoral artery
femoral vein
nerve to sartorious muscle
nerves to rectus femoris
vastus lateralis, and
pubic tubercle
vastus intermedius
medial cutaneous
nerve to vastus
nerve of thigh
medialis muscle
adductor longus
saphenous nerve
muscle
intermediate
cutaneous
nerve of thigh
sartorius muscle (cut)
rectus femoris muscle
anterior
superior
iliac spine
pubic
tubercle
CD Figure 17-20
Femoral nerve block. The needle is directed posteriorly just below the
midpoint of the inguinal ligament and lateral to the femoral artery. In a lateral cutaneous
nerve of the thigh block, the needle is directed posteriorly just inferior to the inguinal liga-
ment about 0.5 in. (1.3 cm) medial to the anterior superior iliac spine.
the anterior superior iliac spine (see CD Fig. 17-20). It
then descends anterior or through the sartorius muscle
Sacral Spinal Nerve Blocks
and divides into terminal anterior and posterior
branches.
Tibial Nerve Block
The nerve may be blocked by inserting the anesthetic
needle just inferior to the inguinal ligament about 0.5 in.
Area of anesthesia: Skin of the sole of the foot (medial
(1.3 cm) medial to the anterior superior iliac spine.
and lateral plantar nerves)
286
Chapter 17
tibialis anterior muscle
common peroneal nerve
saphenous nerve
superficial peroneal nerve
deep peroneal nerve
gastrocnemius muscle
peroneus longus muscle
anterior tibial artery
soleus
peroneus brevis muscle
muscle
extensor hallucis
longus muscle
tibialis
anterior
medial femoral
tendon
interosseous membrane
condyle
extensor hallucis
extensor digitorum
longus tendon
longus muscle
saphenous
medial malleolus
nerve
lateral malleolus
dorsalis
tuberosity
deep peroneal nerve
pedis artery
of tibia
tibialis
anterior tendon
extensor hallucis
longus tendon
saphenous
superficial peroneal nerve
nerve
medial malleolus
lateral malleolus
tibialis anterior tendon
deep peroneal nerve
extensor digitorum
longus tendons
dorsalis pedis artery
extensor hallucis
longus tendon
CD Figure 17-21
Nerve blocks on the front of the lower part of the leg and dorsum of
foot. A. The saphenous nerve, the superficial peroneal nerve, and the deep peroneal nerve
in relation to other important anatomic structures. B. The surface landmarks in the ankle
region and on the dorsum of the foot necessary for performing superficial peroneal nerve
block, saphenous nerve block, and deep peroneal nerve block. C. The surface landmarks
used for performing saphenous nerve block on the medial side of the knee.
Indications: Repair of lacerations on the sole of foot
posterior tibial artery can be felt midway between the medial
Procedure: The tibial nerve (L4 and L5 and S1 through
malleolus and the heel. The nerve lies immediately poste-
S3) is the largest terminal branch of the sciatic nerve. At
rior to the artery, and the anesthetic needle can be inserted
the ankle, the nerve, accompanied by the posterior tibial
at this location (see CD Fig. 17-22).
artery, becomes superficial. It lies behind the medial
malleolus, between the tendons of the flexor digitorum
Sural Nerve Block
longus and the flexor hallucis longus muscles, and is
covered by the flexor retinaculum (CD Fig. 17-22).
Area of anesthesia: Skin of the lateral border of foot and
lateral side of the little toe
The tibial nerve may be blocked as it lies behind the
Indications: Repair of lacerations on the lateral side of
medial malleolus. By careful palpation, the pulsations of the
the foot and little toe
The Spinal Nerves and Spinal Nerve Blocks
287
flexor digitorum
longus muscle
tibial nerve
tibialis posterior muscle
tendo calcaneus
posterior tibial artery
flexor hallucis longus muscle
medial malleolus
flexor retinaculum
medial plantar nerve
lateral plantar nerve
medial malleolus
tibial nerve
posterior tibial artery
CD Figure 17-22
Tibial nerve block.
A. The tibial nerve and its relationships
as it passes behind the medial malleolus
of the tibia. B. The important surface
landmarks used when blocking the tibial
nerve at the ankle.
Procedure: The sural nerve is a branch of the tibial
the fibula, it is subcutaneous and can easily be rolled
nerve in the popliteal space. It descends superficially in
against the bone.
the calf accompanied by the small saphenous vein. It
The common peroneal nerve can be blocked by first pal-
courses behind the lateral malleolus and passes to
pating the nerve below the head of the fibula and infiltrating
its distribution along the lateral border of the foot and
the tissue around the nerve with a local anesthetic solution.
little toe (CD Fig. 17-23).
The sural nerve may be blocked by inserting the anes-
thetic needle midway between the lateral malleolus and the
Superficial Peroneal Nerve Block
tendo calcaneus (Achilles) and infiltrating the subcuta-
Area of anesthesia: Skin on the lower anterior and lateral
neous tissue with anesthetic solution (see CD Fig. 17-23).
sides of the leg and the dorsum of the foot and toes (ex-
cept the cleft between the first and second toes, which is
Common Peroneal Nerve Block
innervated by the deep peroneal nerve and the lateral
side of the little toe, which is supplied by the sural nerve)
Area of anesthesia: Skin on the anterior and lateral sides
Indications: Repair of lacerations in the area of its cuta-
of the leg and the dorsum of the foot and toes, including
neous distribution
the medial side of the big toe
Procedure: The superficial peroneal nerve is a branch of
Indications: Repair of lacerations on the anterior and lat-
the common peroneal nerve. In the lower third of the leg
eral sides of the leg and the dorsum of the foot and toes
it becomes superficial and its terminal branches pass to
Procedure: The common peroneal nerve (L4 and L5
their distribution on the dorsum of the foot and toes (see
and S1 and S2) is the smaller of the terminal branches of
CD Fig. 17-21).
the sciatic nerve. It winds laterally around the neck of the
fibula to pierce the peroneus longus muscle (see CD Fig.
The superficial peroneal nerve is easily blocked in the
17-23). As the nerve lies on the lateral side of the neck of
lower part of the leg by infiltrating the anesthetic in the
288
Chapter 17
tibial nerve
plantaris muscle (cut)
popliteus
biceps femoris
muscle
common peroneal nerve
tendon
lateral head of
soleus
gastrocnemius muscle (cut)
muscle
head of fibula
(cut)
head of fibula
tibialis posterior
flexor hallucis longus
common
muscle
peroneal
peroneus longus muscle
nerve
flexor digitorum longus
muscle
peroneus brevis muscle
medial malleous
lateral malleolus
flexor
sural nerve
retinaculum
tendo calcaneus
sural nerve
lateral malleoulus
CD Figure 17-23
A. The important anatomic relationships of the common peroneal
nerve at the back of the knee joint and the sural nerve behind the lateral malleolus of the
fibula. B. The surface landmarks used for performing a common peroneal nerve block at
the knee. C. The surface landmarks used for performing a sural nerve block at the ankle.
subcutaneous tissue along a transverse line connecting the
on the lateral side of the dorsalis pedis artery and is su-
medial and lateral malleoli (see CD Fig. 17-21).
perficially placed between the tendons of extensor digi-
torum longus and the extensor hallucis longus muscles
(see CD Fig. 17-21).
Deep Peroneal Nerve Block
Area of anesthesia: Skin in the cleft between the big and
First, the dorsalis pedis artery is palpated midway be-
second toes
tween the medial and lateral malleoli. With the foot actively
Indications: Repair of lacerations in the cleft between
dorsiflexed, the tendons of the extensor digitorum longus
the big and second toes
and extensor hallucis longus muscles can be seen. The
Procedure: The deep peroneal nerve is a terminal
nerve lies on the lateral side of the artery between these ten-
branch of the common peroneal nerve. It descends in
dons (see CD Fig. 17-21). The needle is then inserted over
the anterior compartment of the leg and at the ankle it
the nerve, and the surrounding tissues are infiltrated with
passes onto the dorsum of the foot. Here the nerve lies
anesthetic.
The Spinal Nerves and Spinal Nerve Blocks
289
cial peroneal nerve (except the cleft between the big toe
Toe Nerve Blocks
and second toe, which is supplied by the deep peroneal
nerve, and the lateral side of the little toe, which is sup-
Area of anesthesia. Skin of the toes. Each toe is supplied
plied by the sural nerve).
by four digital nerves at the 2 o’clock, 5 o’clock, 7 o’clock,
Indications: Repair of lacerations of the toes, removal of
and 10 o’clock positions. The plantar digital nerves are
foreign bodies, and removal of nails
derived from the medial and lateral plantar nerves (CD
Procedure: The nerves are easily blocked with small vol-
Fig. 17-24); the dorsal digital nerves are from the superfi-
umes of anesthetic solution injected subcutaneously and
saphenous
medial calcaneal
nerve
branch of tibial
medial
nerve
malleolus
medial malleolus
lateral malleolus
lateral plantar
superficial
medial
nerve
peroneal
plantar
nerve
nerve
sural nerve
sural nerve
deep
saphenous
peroneal
lateral
nerve
nerve
malleolus
medial calcaneal
branch of tibial
nerve
deep
peroneal
nerve
superficial
peroneal
nerve
sural
superficial
nerve
peroneal
nerve
CD Figure 17-24
Toe nerve blocks. A, B, C, and D. The sensory nerve supply to the foot
and toes; the heavy lines indicate the boundaries between the different areas of innerva-
tion. The plantar digital nerves are derived from the medial and lateral plantar nerves; the
dorsal digital nerves are from the superficial peroneal nerve (except the cleft between the
big and second toes, which are supplied by the deep peroneal nerve, and the lateral side
of the little toe, which is supplied by the sural nerve). E and F. The sites at the base of
each toe (x) where the anesthetic solution may be injected subcutaneously.
290
Chapter 17
dorsal nerve of clitoris
perineal nerve
CD Figure
17-25
Pudendal nerve blocks.
A. Transvaginal method. The needle is passed
ischial spine
through the vaginal mucous membrane toward
the ischial spine. On passing through the
ischial tuberosity
sacrospinous ligament the anesthetic solution
is infiltrated around the pudendal nerve.
pudendal nerve
B. Perineal method. The ischial tuberosity is
palpated subcutaneously through the buttock.
The needle is inserted on the medial side of the is-
chial tuberosity to a depth of about 1 in. from the
sacrospinous ligament
free surface of the tuberosity. The anesthetic is
infiltrated around the pudendal nerve.
circumferentially around the base of each toe (see CD
inserted through the vagina to palpate the ischial spine.
Fig. 17-24).
The needle of the syringe is then passed through the
vaginal mucous membrane toward the ischial spine. On
passing through the sacrospinous ligament there is a
Pudendal Nerve Block
feeling of “give.” The anesthetic solution is then infil-
Area of anesthesia: Skin of the perineum; it does not, how-
trated into the tissues around the pudendal nerve (see
ever, abolish sensation from the anterior part of the per-
CD Fig. 17-25).
ineum, which is innervated by terminal branches of the il-
■ Perineal method: The bony landmark is the ischial
ioinguinal nerve and genitofemoral nerve. Needless to say,
tuberosity (see CD Fig. 17-25). The tuberosity is palpated
it does not abolish pain from uterine contractions that as-
subcutaneously through the buttock, and the needle is
cend to the spinal cord via the sympathetic afferent nerves.
introduced into the pudendal canal along the medial
Indications: Forceps delivery and episiotomy repair
side of the tuberosity. The canal lies about 1 in. (2.5 cm)
Procedures: These involve the following:
deep to the free surface of the ischial tuberosity. The lo-
■
Transvaginal method: The bony landmark used is the
cal anesthetic is then infiltrated around the pudendal
ischial spine
(CD Fig. 17-25). The index finger is
nerve.
Clinical Problem Solving Questions
Read the following case histories/questions and give
diagnosis of dislocation of the right shoulder joint
the best answer for each.
was made.
1. The following statements concerning this patient are
A 60-year-old woman fell down the stairs and was admitted
consistent with the diagnosis except which?
to the emergency department with severe right shoulder
A. This patient had a subcoracoid dislocation of the
pain. On examination, the patient was sitting up with
right shoulder joint.
her right arm by her side and her right elbow joint
B. The head of the humerus was dislocated down-
supported by her left hand. Inspection of the right
ward through the weakest part of the capsule of the
shoulder showed loss of the normal rounded curvature
joint.
and evidence of a slight swelling below the right clavicle.
C. The pull of the pectoralis major and subscapularis
Any attempt at active or passive movement of the shoulder
muscles had displaced the upper end of the humerus
joint was stopped by severe pain in the shoulder. A
medially.
The Spinal Nerves and Spinal Nerve Blocks
291
D. The greater tuberosity of the humerus no longer
B. The muscles of the thenar eminence showed some
displaced the deltoid muscle laterally, and the curve
evidence of wasting as seen by flattening of the
of the shoulder was lost.
thenar eminence.
E. The integrity of the axillary nerve should always be
C. The muscles of the thenar eminence are supplied by
tested by touching the skin over the upper half of the
the recurrent muscular branch of the median nerve.
deltoid muscle.
D. The median nerve enters the palm through the
carpal tunnel.
A young housewife was on a ladder cleaning a window in her
E. The median nerve occupies a large space between
home, when she lost her balance and started to fall. To pro-
the tendons behind the flexor retinaculum.
tect herself, she held out her right hand, which smashed
F. This patient has carpal tunnel syndrome.
through the glass. On admission to the hospital, she was
bleeding profusely from a superficial laceration in front of her
A 6-year-old boy, running along a concrete path with a
right wrist. She had sensory loss over the palmar aspect of the
glass jam jar in his hand, slipped and fell. The glass from
medial one and a half fingers but normal sensation of the
the broken jar pierced the skin on the front of his left wrist.
back of these fingers over the middle and proximal phalanges.
On examination a small wound was present on the front of
She had difficulty in grasping a piece of paper between her
the left wrist and the palmaris longus tendon had been sev-
right index and middle fingers. All her long flexor tendons
ered. The thumb was laterally rotated and adducted, and
were intact.
the boy was unable to oppose his thumb to the other fin-
gers. There was loss of skin sensation over the lateral half
2. The following statements concerning this patient are
of the palm and the palmar aspect of the lateral three and
correct except which?
a half fingers.
A. The ulnar artery was cut in front of the flexor retinac-
ulum, and this accounted for the profuse bleeding.
4. The following facts concerning this patient are correct
B. The loss of skin sensation on the palmar aspect of
except which?
the medial one and a half fingers was caused by the
A. Sensory loss of the distal part of the dorsal surfaces of
severance of the median nerve as it crossed in front
the lateral three and a half fingers was experienced.
of the flexor retinaculum.
B. The median nerve lies superficial to the palmaris
C. The normal sensation on the back of the medial one
longus proximal to the flexor retinaculum and was
and a half fingers over the proximal phalanges was
severed by the piece of glass.
caused by the fact that the posterior cutaneous branch
C. The median nerve lies in the interval between the
of the ulnar nerve arises about 2.5 in. (6.25 cm) prox-
tendons of the flexor digitorum superficialis and the
imal to the flexor retinaculum and was spared.
flexor carpi radialis muscles just proximal to the
D. The inability to hold the piece of paper was caused
wrist joint.
by the paralysis of the second palmar interosseous
D. Adduction of the thumb was produced by the con-
muscle, which is supplied by the deep branch of the
traction of the adductor pollicis muscle, which is
ulnar nerve.
supplied by the ulnar nerve.
E. There was no sensory loss on the palm of the hand
E. The palmar cutaneous branch of the median nerve
because the palmar cutaneous branch of the ulnar
had been severed.
nerve was not cut.
A 52-year-old woman was admitted to the hospital with a
A 50-year-old woman complaining of severe “pins and nee-
diagnosis of right-sided pleurisy with pneumonia. It was
dles” in her right hand and lateral fingers visited her physi-
decided to remove a sample of pleural fluid from her
cian. She said that she had experienced difficulty in button-
pleural cavity. The resident inserted the needle close to the
ing up her clothes when dressing. On physical examination
lower border of the eighth rib in the anterior axillary line.
the patient pointed to her thumb and index, middle, and
The next morning he was surprised to hear that the patient
ring fingers as the areas where she felt discomfort. No ob-
had complained of altered skin sensation extending from
jective impairment of sensation was found in these areas.
the point where the needle was inserted downward and for-
The muscles of the thenar eminence appeared to be func-
ward to the midline of the abdominal wall above the um-
tioning normally, although there was some loss of power
bilicus.
compared with the activity of the muscles of the left thenar
5. The altered skin sensation in this patient after the nee-
eminence.
dle thoracostomy could be explained by which?
3. The following statements concerning this patient are
A. The needle was inserted too low down in the inter-
correct except which?
costal space.
A. Altered skin sensation was felt in the skin areas
B. The needle was inserted too close to the lower bor-
supplied by the digital branches of the median
der of the eighth rib and damaged the eighth inter-
nerve.
costal nerve.
292
Chapter 17
C. The needle had impaled the eighth rib.
B. The parietal peritoneum in this area is innervated by
D. The needle had penetrated too deeply and pierced
the tenth and eleventh intercostal nerves, which
the lung.
give rise to referred pain in the tenth and eleventh
E. There is a peritoneal abscess beneath the diaphragm
dermatomes on the side and back.
on the left side.
C. The parietal peritoneum on the central part of the
undersurface of the diaphragm is supplied by the
A 43-year-old man was involved in a violent quarrel with his
phrenic nerve.
wife over another woman. In a fit of rage, the wife picked up
D. The spinal segmental nerves within the phrenic
a carving knife and lunged forward at her husband, striking
nerve are C3, C4, and C5.
his anterior neck over the left clavicle. The husband col-
E. The pain was referred to the shoulder along the
lapsed on the kitchen floor, bleeding profusely from the
supraclavicular nerves (C3 and C4).
wound. The distraught wife called an ambulance.
An 8-year-old boy was admitted to the hospital with a tem-
6. On examination in the emergency department of the
perature of 101°F, a furred tongue, and pain in the right
hospital, the following conditions were found except
lower quadrant. On examination, the skin on the right lower
which?
quadrant was tender to the touch, and the abdominal mus-
A. A wound was seen about 1 in. (2.5 cm) wide over the
cles were contracted and rigid. A diagnosis of acute appen-
left clavicle.
dicitis was made.
B. Auscultation revealed diminished breath sounds
over the left hemithorax.
9. The symptoms and signs displayed by this patient can
C. The trachea was deflected to the left.
be explained by the following statements except which?
D. The left upper limb was lying stationary on the table,
A. An acutely inflamed appendix produces an inflam-
and active movement of the small muscles of the left
mation of the peritoneal coat covering it.
hand was absent.
B. Should the inflammatory process spread, for exam-
E. The patient was insensitive to pin prick along the lat-
ple, if the appendix should rupture, the parietal peri-
eral side of the left arm, forearm, and hand.
toneum would become involved.
C. The parietal peritoneum, the abdominal muscles,
A 72-year-old man complaining of burning pain on the
and the overlying skin are supplied by the same seg-
right side of his chest was seen by his physician. On exam-
mental spinal nerves.
ination the patient indicated that the pain passed forward
D. The segmental nerves supplying the right lower
over the right sixth intercostal space from the posterior ax-
quadrant of the abdominal wall are T7, T8, and T9.
illary line forward as far as the midline over the sternum.
E. The pain in the right lower quadrant and the regional
The physician noted that there were several watery blebs
contraction of the abdominal muscles are attempts by
on the skin in the painful area.
the body to keep the inflamed appendix immobile so
7. The following statements are correct except which?
that the inflammatory process remains localized.
A. This patient has herpes zoster.
A 45-year-old woman was shopping in a liquor store when
B. A virus descends along the cutaneous nerves, caus-
an armed robbery took place. A shoot-out occurred and a
ing dermatomal pain and the eruption of vesicles.
bullet ricocheted off the wall and entered her left side. For-
C. The sixth right intercostal nerve was involved.
tunately, the bullet did not enter the peritoneal cavity. One
D. The condition was confined to the anterior cuta-
year later, in addition to diminished skin sensation over the
neous branch of the sixth intercostal nerve.
left lumbar region and umbilicus, she noticed a bulging for-
ward of the left side of her anterior abdominal wall.
An obese 40-year-old woman was seen in the emergency de-
partment complaining of a severe pain over the right shoul-
10. The symptoms and signs displayed by this patient can
der and in her right side and back below the shoulder blade.
be explained by the following statements except which?
She said that she had experienced the pain on several occa-
A. The bullet cut the ninth and tenth intercostal nerves
sions before and that when she ate fatty foods it seemed to
just below the costal margin on the left side.
make the pain worse. Ultrasound demonstrated the pres-
B. The diminished skin sensation was caused by the
ence of gallstones. Her condition was diagnosed as
loss of the sensory nerve supply to the ninth and
cholelithiasis, and the pain was attributed to gallstone colic.
tenth thoracic dermatomes.
8. The symptoms and signs displayed by this patient can
C. Portions of the oblique, transversus, and rectus ab-
be explained by the following statement except which?
dominis muscles on the left side were paralyzed.
A. The fundus of the gallbladder lies against the ante-
D. Atrophy of the pyramidalis muscle resulted in loss of
rior abdominal wall next to the tip of the right ninth
support to the abdominal viscera, which then sagged
costal cartilage.
forward.
The Spinal Nerves and Spinal Nerve Blocks
293
After a major abdominal operation, a patient was given a
B. Skin sensation was lost over the anterior and medial
course of antibiotics by intramuscular injection. The nurse
sides of the thigh.
was instructed to give the injections into the right buttock.
C. Skin sensation was lost along the medial border of
Later, when the patient left the hospital, he developed sev-
the big toe.
eral symptoms and signs that suggested that the injections
D. Skin sensation was lost on the lower part of the leg
into the gluteus maximus muscle had been given over the
and the medial border of the foot as far as the ball of
course of the sciatic nerve and had caused a lesion of the
the big toe.
common peroneal nerve.
E. Weak extension of the knee was possible when walk-
ing because of the use of the adductor muscles.
11. The symptoms and signs displayed by this patient
included the following except which?
13.
A patient was seen in the emergency department with a
A. He experienced numbness and tingling sensations
laceration of the skin over the middle phalanx of the left
down the anterior and lateral sides of the right leg
index finger. What is the sensory nerve supply of that
and the dorsum of the foot.
finger? Where is it possible to perform a nerve block so
B. His right foot tended to catch on steps and on the
that the wound could be sutured?
edges of the carpet.
14.
A 37-year-old woman was involved in an automobile ac-
C. On testing, he had impaired skin sensation on the
cident and sustained a fracture of her sixth right rib. It
lateral side of the right thigh.
was decided to relieve her acute pain caused by the bro-
D. The patient tended to hold the foot plantar flexed
ken rib by performing an intercostal nerve block.
and slightly inverted.
Which intercostal nerve innervates the sixth rib? What
E. Dorsiflexion of the right ankle joint was weaker than
is the course taken by an intercostal nerve in an inter-
the same movement of the left ankle.
costal space? From what part of a spinal nerve is an in-
F. The everter muscles of the right midtarsal joints
tercostal nerve formed? Name the order of structures
were weaker than those of the opposite side.
forming the neurovascular bundle in an intercostal
space from above downward.
A 17-year-old girl was dealing drugs on a street corner
when she became involved in a fight. During the brawl she
15.
A 17-year-old boy received a knife wound on the lateral
received a deep knife wound to the front of her right thigh.
side of his right thigh. What is the sensory nerve supply
After a thorough examination in the emergency depart-
to this region of the thigh? Which important surface
ment of the local hospital, it was determined that the knife
landmarks would you use when blocking the nerves?
point had severed the trunk of the right femoral nerve just
16.
What is the sensory nerve supply to the skin on the dor-
below the inguinal ligament.
sum of the foot? Where would you block these nerves?
12. This patient had the following signs and symptoms
except which?
A. The right quadriceps femoris muscle failed to con-
tract when the patient was asked to extend her right
knee joint.
Answers and Explanations
1. E is the correct answer. The integrity of the axillary nerve
in front of the flexor retinaculum with the ulnar artery,
is tested by touching the skin over the lower half of the
which was also cut (see text Fig. 17-14).
deltoid muscle. The skin of the curve of the shoulder, in-
3. E is the correct answer. The median nerve occupies a
cluding the skin covering the upper half of the deltoid
small restricted space in the carpal tunnel (see text Fig.
muscle, is supplied by the supraclavicular nerves.
17-14).
2. B is the correct answer. The loss of skin sensation of the
4. B is the correct answer. The median nerve lies deep to
palmar aspect of the medial one and a half fingers was
the palmaris longus tendon proximal to the flexor reti-
caused by the severance of the ulnar nerve as it crossed
naculum (see text Fig. 17-12).
294
Chapter 17
5.
B is the correct answer. The needle was inserted too
superficial radial nerve. The nerves are easily blocked
close to the lower border of the eighth rib and damaged
by injecting small volumes of anesthetic solution
the eighth intercostal nerve (see CD Fig. 17-18).
around the base of the finger (see CD Fig. 17-17).
6.
E is the correct answer. The lower trunk of the brachial
14.
The periosteum of the sixth rib is innervated by the
plexus was cut by the knife. This would explain the loss
sixth intercostal nerve. (It is conceivable that in the
of movement of the small muscles of the left hand. It
individual who has a collateral branch of the fifth inter-
would also explain the loss of skin sensation that oc-
costal nerve, the periosteum of the sixth is also inner-
curred in the C8 and T1 dermatomes on the medial not
vated by this nerve.) Intercostal nerves are formed from
on the lateral side of the left forearm and hand. The knife
the anterior rami of T1 through T11 spinal nerves. An
had also pierced the left dome of the cervical pleura,
intercostal nerve passes forward around the chest wall
causing a left pneumothorax with left-sided diminished
first, between the posterior intercostal membrane and
breath sounds and a deflection of the trachea to the left.
the parietal pleura, then between the internal inter-
costal muscle and the innermost intercostal muscle
7.
D is the correct answer. The skin over the sixth inter-
(part of the transversus thoracis). The nerve lies in the
costal space is innervated by the lateral cutaneous
subcostal groove of the rib of its own number. The in-
branch as well as the anterior cutaneous branch of the
tercostal vein, the intercostal artery, and the intercostal
sixth intercostal nerve.
nerve lie within the subcostal groove in that order from
8.
B is the correct answer. The parietal peritoneum in the
above downward.
region of the fundus of the gallbladder is innervated by
15.
The sensory innervation of the skin on the lateral sur-
the eighth and ninth intercostal nerves, which give rise
face of the thigh is the lateral cutaneous nerve of the
to referred pain in the eighth and ninth thoracic der-
thigh, a branch of the lumbar plexus (L2 and L3). The
matomes on the side and back.
nerve may be blocked by inserting an anesthetic needle
9.
D is the correct answer. The segmental nerves supply-
just inferior to the inguinal ligament about 0.5 in. (1.3
ing the right lower quadrant of the abdominal wall are
cm) medial to the anterior superior iliac spine.
T11, T12, and L1 (see CD Fig. 17-1).
16.
The sensory nerve supply to the skin on the dorsum of
10.
D is the correct answer. The pyramidalis muscle (if pre-
the foot is from the superficial peroneal nerve. The cleft
sent) is innervated by the twelfth thoracic nerve.
between the first and second toes is from the deep per-
oneal nerve.
11.
C is the correct answer. The skin on the lateral side of
the thigh is innervated by the lateral cutaneous nerve of
The superficial peroneal nerve can be blocked by infil-
the thigh (L2 and L3), a branch of the lumbar plexus
trating the anesthetic in the subcutaneous tissue along
(see CD Fig. 17-1).
a transverse line connecting the medial and lateral
malleoli (see CD Fig. 17-21). The deep peroneal nerve
12.
C is the correct answer. The skin covering the medial
is blocked by first palpating the dorsalis pedis artery as it
border of the big toe is innervated by the superficial per-
lies between the tendons of the extensor hallucis longus
oneal nerve (see CD Fig. 17-1).
and the extensor digitorum longus. The nerve lies on
13.
The index finger receives the following sensory inner-
the lateral side of the artery between these tendons. The
vation: anterior aspect, two digital branches of the me-
needle is then inserted over the nerve, and the sur-
dian nerve; posterior aspect, two digital branches of the
rounding tissue is infiltrated with anesthetic.
Chapter Outline
The Eye
296
Trauma and the Cornea
299
Corneal Ulcers
299
Eyelids
296
Pupil
300
Clinical Examination of the Eyelids
296
Flashlight Examination of the Pupil
300
Hordeolum (Stye)
296
Pupillary Reflexes
300
Chalazion
297
Retina
300
Edema of the Eyelids
297
Detachment of the Retina
300
Subtarsal Sulcus and Foreign Bodies
297
Central Retinal Artery Occlusion
300
Ptosis (Drooping of the Upper Lid)
297
Papilledema, the Central Vein, and Increased
Lacrimal Apparatus
297
Cerebrospinal Fluid Pressure
300
Inflammation of the Lacrimal Sac
297
Lens
300
Probing the Nasolacrimal Duct
298
Cataract
300
Eye Trauma
298
Examination of the Eye as Seen with the Direct
Blowout Fractures of the Maxilla
298
Ophthalmoscope
300
Movements of the Eye
298
The Ear
303
Clinical Testing for the Actions of the Superior and
External Ear
303
Inferior Recti and the Superior and Inferior
Tympanic Membrane Examination
303
Oblique Muscles
298
Middle Ear
303
Lesions of the Cranial Nerves that Control the Eye
Infections and Otitis Media
303
Movements
298
Complications of Otitis Media
303
Strabismus
298
Eye Structure
298
Clinical Problem Solving Questions
303
Sclera
298
The Lamina Cribrosa, the Cerebrospinal Fluid,
Answers and Explanations
305
and the Aqueous Humor Pressure
298
Cornea
298
Aging Changes in the Cornea
298
Astigmatism
299
and muscular attachments. It is performed for purposes
THE EYE
of inspection of the eye and removing a superficial con-
junctival foreign body. With the patient looking down-
ward, the upper lid is grasped by the central eyelashes
Eyelids
and pulled downward while a cotton-tipped applicator is
applied centrally to the skin on the upper surface of the
Clinical Examination of the Eyelids
upper lid. With the superior tarsal plate serving to stiffen
the upper lid, the upper lid is gently flipped upward over
Retraction of the eyelids: Both the upper and lower lids
the applicator tip so that the conjunctival surface is fully
can be retracted by applying the thumbs to the patient’s
exposed (see CD Fig. 18-1).
forehead and the cheek just above and below the orbital
margins. The lids are then gently retracted away from
Hordeolum (Stye)
the eyeball, and the lower lid may be easily everted (CD
Fig. 18-1).
An external hordeolum is an acute infection of a lash follicle
Eversion of the upper lid: Eversion of the upper lid is
or a sebaceous gland (of Zeis) or a ciliary sweat gland
more difficult than that of the lower lid because of its size
(of Moll); all drain externally to the skin surface of the lid.
The Eye and the Ear
297
eyebrow
orbital part of upper lid
tarsal part of upper lid
superior palpebral furrow
tarsal glands
beneath conjuctiva
lateral
punctum lacrimale
angle of eye
caruncula
lacrimalis
orifices of
tarsal glands
bulbar conjunctiva
palpebral conjunctiva
branches of posterior
conjunctival arteries
upper lid
tarsal glands
CD Figure 18-1
A. Complete eversion of the up-
ducts of
per eyelid of the right eye made possible by stiff-
tarsal glands
lateral
ness of the superior tarsal plate; the lower eyelid is
angle
pulled downward. Note the orifices of the tarsal
of eye
glands and the puncta lacrimalia. B. Posterior view
of the eyelids with the upper and lower lids nearly
closed. Note the tarsal glands with their short ducts
anterior margin of lid
and orifices. In this diagram the conjunctiva has
posterior margin of lid
been removed from the back of the eyelids to re-
lower lid
veal the tarsal glands in situ.
An internal hordeolum is an acute infection of a tarsal gland
described previously. Small particles often migrate and be-
(of Meibom). The tarsal glands drain onto the conjunctival
come lodged in the subtarsal sulcus (see text Fig. 18-1).
surface of the lid.
Corneal abrasions may occur as the result of the foreign
body being carried across the cornea with the movement of
Chalazion
the eyelids.
This is a localized, painless swelling of the lid resulting from
Ptosis (Drooping of the Upper Lid)
chronic inflammation of a tarsal gland. Since the gland lies
on the conjunctival surface of the tarsal plate, the swelling
In Horner’s syndrome, ptosis is caused by loss of sympathetic
should be incised through the conjunctival surface of the lid.
innervation of the smooth muscle component of the levator
palpebrae superioris muscle. In third cranial nerve dysfunc-
Edema of the Eyelids
tion, ptosis is due to paralysis of the striated muscle of the
levator palpebrae superioris.
The looseness of the subcutaneous tissue of the eyelids ex-
plains why edema fluid secondary to renal failure or insect
bites can rapidly accumulate, causing extensive swelling of
Lacrimal Apparatus
the lids.
Inflammation of the Lacrimal Sac
Subtarsal Sulcus and Foreign Bodies
This presents as a tender swelling above the upper margin of
Foreign bodies in the conjunctival sac produce severe pain
the medial palpebral ligament. Gentle pressure on the sac
and reflex tearing. The superior and inferior fornices can be
may result in a yellowish discharge emerging from the
examined for the foreign bodies by everting the eyelids as
puncta lacrimalia.
298
Chapter 18
Probing the Nasolacrimal Duct
oblique and the origin of the inferior oblique muscles lie me-
dial and anterior to their insertions. The ophthalmologist tests
Congenital or acquired blockage of the duct may occur.
the action of these muscles by asking the patient first to look
To relieve the blockage, a probe is passed downward starting
medially, thus placing these muscles in the optimum position
at the punctum lacrimalia of the upper eyelid. The probe is
to lower the cornea (superior oblique) or to raise it (inferior
first directed vertically upward and then medially into the
oblique). In other words, when you ask a patient to look me-
lacrimal sac. It is then turned downward at right angles in the
dially and downward at the tip of his nose, you are testing the
nasolacrimal duct to reach the inferior meatus in the nose.
superior oblique at its best position. Conversely, by asking the
The end of the probe should then be visible within the nose.
patient to look medially and upward, you are testing the infe-
Remember that the nasolacrimal duct inclines downward,
rior oblique at its best position.
backward, and laterally as it descends to the nose.
Because the lateral and medial recti are neutrally placed
relative to the axes of the eyeball, asking the patient to turn his
Eye Trauma
or her cornea directly laterally tests the lateral rectus, and
turning the cornea directly medially tests the medial rectus.
Although the eyeball is well protected by the surrounding
The cardinal positions of the eye and the actions of the
bony orbit, it is protected anteriorly only from large objects,
recti and oblique muscles are shown in CD Fig. 18-2.
such as tennis balls, which tend to strike the orbital margin
but not the globe. The bony orbit provides no protection
Lesions of the Cranial Nerves that
from small objects, such as golf balls, which can cause se-
Control the Eye Movements
vere damage to the eye. Careful examination of the eyeball
relative to the orbital margins shows that it is least protected
Lesions of the oculomotor, trochlear, and abducent nerves
from the lateral side.
are described on CD page 227.
Strabismus
Blowout Fractures of the Maxilla
Many cases of strabismus are nonparalytic and are caused by
Blowout fractures of the orbital floor involving the maxillary
an imbalance in the action of opposing muscles. This type
sinus commonly occur as a result of blunt force to the face.
of strabismus is known as concomitant strabismus and is
If the force is applied to the eye, the orbital fat explodes
common in infancy.
inferiorly into the maxillary sinus, fracturing the orbital
floor. Not only can blowout fractures cause displacement of
Eye Structure
the eyeball, with resulting symptoms of double vision
(diplopia), but also the fracture can injure the infraorbital
Sclera
nerve, producing loss of sensation of the skin of the cheek
and the gum on that side. Entrapment of the inferior rectus
muscle in the fracture may limit upward gaze.
The Lamina Cribrosa, the Cerebrospinal
Fluid, and the Aqueous Humor Pressure
Movements of the Eye
The lamina cribrosa is the area of the sclera that is pierced by
the nerve fibers of the optic nerve. It is a relatively weak area
Clinical Testing for the Actions of the
and can be made to bulge into the eyeball by a rise of cere-
Superior and Inferior Recti and the
brospinal fluid pressure in the tubular extension of the sub-
Superior and Inferior Oblique Muscles
arachnoid space, which surrounds the optic nerve.
If the intraocular pressure rises, due to blockage in the
Since the actions of the superior and inferior recti and the
drainage of aqueous humor, as in glaucoma, the lamina
superior and inferior oblique muscles are complicated
cribrosa will bulge outward, producing a cupped disc, as
when a patient is asked to look vertically upward or vertically
seen through the ophthalmoscope.
downward, the examiner tests the eye movements in which
the single action of each muscle predominates.
Cornea
The origins of the superior and inferior recti are situ-
ated about 23° medial to their insertion and, therefore,
Aging Changes in the Cornea
when the patient is asked to turn the cornea laterally, these
muscle are placed in the optimum position to raise the
With advancing years, the cornea becomes less translucent,
cornea (superior rectus) or lower it (inferior rectus). To test
and dust-like opacities may occur in the deeper parts of the
the superior rectus, have the patient look up and laterally; to
substantia propria. Arcus senilis appears as white arcs near
test the inferior rectus, have the patient look down and out.
the edge of the cornea and is caused by an extracellular
Using the same rationale, the examiner tests the superior
infiltration of lipid; it is present in almost every person over
and the inferior oblique muscles. The pulley of the superior
60 years old.
The Eye and the Ear
299
A
B
C
D
E
F
G
H
I
CD Figure 18-2
The cardinal positions of the right and left eyes and the actions of the
recti and oblique muscles principally responsible for the movements of the eyes. A. Right
eye, superior rectus muscle; left eye, inferior oblique muscle. B. Both eyes, superior recti
and inferior oblique muscles. C. Right eye, inferior oblique muscle; left eye, superior rec-
tus muscle. D. Right eye, lateral rectus muscle; left eye, medial rectus muscle. E. Primary
position, with the eyes fixed on a distant fixation point. F. Right eye, medial rectus muscle;
left eye, lateral rectus muscle. G. Right eye, inferior rectus muscle; left eye, superior
oblique muscle. H. Both eyes, inferior recti and superior oblique muscles. I. Right eye, su-
perior oblique muscle; left eye, inferior rectus muscle.
Astigmatism
Fortunately, the stratified squamous epithelium covering the
anterior surface of the cornea is capable of rapid regeneration
Often the cornea is not the section of a perfect sphere so that
after an abrasion.
the refractive power is not the same in all directions, a
Foreign bodies driven with great force may penetrate
condition known as astigmatism.
the cornea and enter the anterior chamber or even the
deepest parts of the eyeball.
Trauma and the Cornea
Corneal Ulcers
Because a portion of the cornea is exposed between the
eyelids, injuries from foreign bodies or abrasions are very
Corneal ulcers are caused by a bacterial invasion of the
common. Damage to the corneal epithelium causes consid-
cornea with the formation of a stromal abscess. The ability of
erable pain, reflex tearing, and vasodilatation of the conjunc-
the cornea to resist bacterial invasion depends on the cleans-
tival capillaries. Later, edema of the lids will be apparent.
ing action of the tears and their normal circulation and the
300
Chapter 18
integrity of the corneal epithelium. A breakdown of this
hole or tear, allows accumulation of fluid between the
mechanism can occur as the result of mild trauma, such as
pigment epithelium and the neural retina, causing the
that which occurs when soft corneal lenses are worn for an ex-
layers to separate or become detached.
cessive period of time, or in the presence of chronic disease.
Central Retinal Artery Occlusion
Pupil
At the point where the central artery pierces the lamina
cribrosa (CD Fig. 18-3), it is subject to atherosclerosis and
Flashlight Examination of the Pupil
can undergo complete or partial occlusion. Disease changes
in the arteriolar wall can be seen with the ophthalmoscope
Normally, the pupils should be of equal or nearly equal
where the arteries cross the veins as a nicking or narrowing
diameter (within 1 to 2 mm in diameter is normal). They
of the venous blood column.
should be round and react to light and accommodation.
In complete central artery occlusion there is a sudden
onset of unilateral blindness. In branch arteriole occlusion
Pupillary Reflexes
there is a partial loss of sight corresponding to the sector
The pupillary reflexes—that is, the reaction of the pupils to
supplied by the arteriole. Total arterial occlusion lasting
light and accommodation—depend on the integrity of ner-
longer than 11⁄2 hours can produce irreversible retinal
vous pathways. In the direct light reflex, the normal pupil
degeneration.
reflexly contracts when a light is shone into the patient’s eye.
The nervous impulses pass from the retina along the optic
Papilledema, the Central Vein, and
nerve to the optic chiasma and then along the optic tract.
Increased Cerebrospinal Fluid Pressure
Before reaching the lateral geniculate body, the fibers con-
Since the optic nerve is surrounded by the dura and arach-
cerned with this reflex leave the tract and pass to the oculo-
noid sheaths, an increase in the intracranial pressure is
motor nuclei on both sides via the pretectal nuclei. From
transmitted through the cerebrospinal fluid along the exten-
the parasympathetic part of the nucleus, efferent fibers leave
sion of the subarachnoid space to the lamina cribrosa of the
the midbrain in the oculomotor nerve and reach the ciliary
eyeball. Because the central artery and vein of the retina
ganglion via the nerve to the inferior oblique. Postgan-
cross the subarachnoid space to enter or leave the optic
glionic fibers pass to the constrictor pupillae muscles via the
nerve, they will be subject to a rise in cerebrospinal fluid
short ciliary nerves.
pressure. The thick-walled artery is unaffected, but the thin-
The consensual light reflex is tested by shining the
walled vein may be compressed, causing congestion of the
light in one eye and noting the contraction of the pupil in
retinal veins and edema of the retina; bulging of the disc
the opposite eye. This reflex is possible because the afferent
may also occur.
pathway just described travels to the parasympathetic nuclei
of both oculomotor nerves.
Lens
The accommodation reflex is the contraction of the
pupil that occurs when a person suddenly focuses on a near
Cataract
object after having focused on a distant object. The nervous
impulses pass from the retina via the optic nerve, the optic
In this condition the lens becomes opaque. Metabolic prod-
chiasma, the optic tract, the lateral geniculate body, the
ucts accumulate within the lens fibers. Senile cataract is the
optic radiation, and the cerebral cortex of the occipital lobe
most common form; its cause is unknown.
of the brain. The visual cortex is connected to the eye field
of the frontal cortex. From here, efferent pathways pass to
Examination of the Eye as Seen
the parasympathetic nucleus of the oculomotor nerve.
From there, the efferent impulses reach the constrictor
with the Direct Ophthalmoscope
pupillae via the oculomotor nerve, the ciliary ganglion, and
the short ciliary nerves.
Red reflex: On looking through the ophthalmoscope,
holding it about 1 ft away from the patient, the examiner
Retina
notes that the fundus appears red (see CD Fig. 18-3). The
fundus shows red because the light is being reflected
Detachment of the Retina
back from the blood in the choroidal blood vessels, with
The neural retina is firmly attached to the underlying
the intervening retina being transparent. An absent red
pigment epithelium at the optic disc and the ora serrata.
reflex means that either there is an opacity in the refrac-
Pathologic separation of the two layers of the retina may
tive media or the retina is not against the choroid. The
follow trauma to the eyeball or degeneration of the neural
possible opacities include a cataract, a vitreous hemor-
retina. Vitreous traction of the retina, or the presence of a
rhage, and a detached retina.
The Eye and the Ear
301
tributary of central vein of retina
optic disc
pigmentation
of retina
site of
fovea
centralis
branch of central artery of retina
CD Figure 18-3
The left ocular fundus as seen with an ophthalmoscope.
Fundus examination: Without pupillary dilatation, only
optic disc is a weak area, a rise in intraocular pressure can
about 15% of the fundus can be seen. With full pupillary
cause it to bulge outward, producing a cupped disc that
dilatation, about 50% of the fundus can be viewed, but
can be seen with the ophthalmoscope.
the area between the equator of the eyeball and the ora
Retinal arteries and veins: The arteries are bright red;
serrata cannot be seen.
the veins are darker red (see CD Fig. 18-3). The arteries
Optic disc: This structure is circular or oval with a vertical
are smaller than the veins (about a 3:4 ratio). The arter-
orientation (see CD Fig. 18-3). It is pink, with the tempo-
ies have thicker walls, which reflect the light as a shiny
ral side slightly lighter than the nasal side. The disc mea-
central reflex stripe. The walls of the arteries and the
sures about 1.5 mm in diameter and can be used as a unit
veins are transparent, so that the examiner observes a
of measurement. The center of the disc has a pale, almost
moving column of blood. The arteries usually cross the
white, depression called the physiologic cup. The edge of
veins on their superficial or vitreal surface, and normally
the disc is usually flat and sharply defined. In some indi-
the arteries do not compress or nick the veins at the site
viduals in whom the retina does not quite reach the mar-
of crossing. The branching of the vessels is variable.
gin of the disc, an arc of choroid pigment may be visible.
Macula: The macula area lies about two disc diameters
The bright red central artery of the retina becomes
on the lateral side of the optic disc (see CD Fig. 18-3).
visible on the disc surface emerging from the optic cup,
It is darker than the surrounding retina. The superior
where it divides into its superior and inferior branches.
and inferior temporal blood vessels arch above and below
The arteries do not normally pulsate. The darker red
the macular area, and no blood vessels are visible in
main tributaries of the central vein of the retina pass into
the center of the macula. The center of the macula
the cup and unite in the cup or deeper out of site within
shows a small, dark red area called the fovea centralis.
the optic nerve.
A small white-yellow light reflex can be detected at
In glaucoma, the increase in intraocular pressure
the center of the fovea, caused by the reflection of
leads to atrophy of the optic nerve and defects in the vi-
the ophthalmoscope light from the concavity of the
sual field. Since the lamina cribrosa of the sclera at the
fovea.
302
Chapter 18
CD Figure 18-4
A. Different parts of the auricle of the external ear. The arrow indicates
the direction that the auricle should be pulled to straighten the external auditory meatus
before insertion of the otoscope in the adult. B. External and middle portions of the right
ear viewed from in front. C. The right tympanic membrane as seen through the otoscope.
The Eye and the Ear
303
of the pharynx. Acute infection of the middle ear (otitis
THE EAR
media) produces bulging and redness of the tympanic
membrane.
External Ear
Complications of Otitis Media
Inadequate treatment of otitis media can result in the spread
Tympanic Membrane Examination
of the infection into the mastoid antrum and the mastoid air
Otoscopic examination of the tympanic membrane is facili-
cells (acute mastoiditis). Acute mastoiditis may be followed
tated by first straightening the external auditory meatus by
by the further spread of the organisms beyond the confines
gently pulling the auricle upward and backward in the adult
of the middle ear. The meninges and the temporal lobe of
(CD Fig. 18-4), and straight backward or backward and
the brain lie superiorly. A spread of the infection in this
downward in the infant. Normally, the tympanic membrane
direction could produce a meningitis and a cerebral abscess
is pearly gray and concave. Remember that in the adult the
in the temporal lobe. Beyond the medial wall of the middle
external meatus is about 1 in. (2.5 cm) long and is narrow-
ear lie the facial nerve and the internal ear. A spread of
est about 0.2 in. (5 mm) from the tympanic membrane.
the infection in this direction can cause a facial nerve palsy
and labyrinthitis with vertigo. The posterior wall of the
mastoid antrum is related to the sigmoid venous sinus. If
Middle Ear
the infection spreads in this direction, a thrombosis in
the sigmoid sinus may well take place. These various
Infections and Otitis Media
complications emphasize the importance of knowing the
Pathogenic organisms can gain entrance to the middle ear
anatomy of this region.
by ascending through the auditory tube from the nasal part
Clinical Problem Solving Questions
Read the following case histories/questions and give
A 33-year-old woman was riding her bicycle when she
the best answer for each.
swerved to avoid a pothole and lost her balance. She then
crashed and hit her head hard on the sidewalk. When she
A 49-year-old woman was found on ophthalmoscopic exam-
regained consciousness in the hospital, it was immediately
ination to have edema of both optic discs (bilateral pa-
noted that she had medial strabismus (squint) of her left
pilledema) and congestion of both retinal veins. The cause
eye.
of the condition was found to be a rapidly expanding in-
tracranial tumor.
2. Which eye muscle was paralyzed in this injury?
A. The medial rectus muscle
1. The following statements concerning this patient are
B. The inferior rectus muscle
correct except which?
C. The superior rectus muscle
A. An intracranial tumor causes a rise in cerebrospinal
D. The lateral rectus muscle
fluid pressure.
E. The superior obliques muscle
B. The optic nerves are surrounded by sheaths derived
from the pia mater, arachnoid mater, and dura mater.
3. An 18-year-old student went to the clinic complaining
C. The intracranial subarachnoid space extends for-
of an acute tender area on the middle of his right upper
ward around the optic nerve for about half its length.
eyelid. Examination revealed a localized red, indurated
D. The thin walls of the retinal vein will be compressed
area on the eyelid margin. Close inspection showed a
as the vein crosses the extension of the subarachnoid
yellowish spot in the center of the swelling. Gentle
space around the optic nerve.
eversion of the lid showed no evidence of swelling on its
E. Because both subarachnoid extensions are continu-
posterior surface. What is the diagnosis? Which
ous with the intracranial subarachnoid space, both
anatomic structure(s) is (are) involved in the inflamma-
eyes will exhibit papilledema and congestion of the
tory process? On which part of the eyelid does the
retinal veins.
abscess tend to point?
304
Chapter 18
4.
A 13-year-old schoolboy was hit in the left eye by another
C. Saliva tended to accumulate in his right cheek.
boy during recess. During the next hour, both the eyelids
D. The saliva tended to dribble from the corner of his
of the victim swelled up until he could barely see. Ex-
mouth.
amination in the emergency department revealed a
E. All the muscles of the right side of his face were
bluish-red discoloration of both eyelids of his left eye with
paralyzed.
narrowing of the palpebral fissure. The discoloration ex-
7.
A 3-year-old boy was playing with his friend when they
tended to the forehead and the left cheek. Careful sepa-
decided to see how many peas they could stick into
ration of the eyelids showed a localized hemorrhage of
each others ears. Later, the babysitter noticed that one
the inferolateral part of the bulbar conjunctiva (part of
of the boys had become completely deaf in his left ear.
the conjunctiva adherent to the sclera of the eyeball).
On examination in the emergency department of the
When the conjunctiva was gently moved with the tip of
local hospital, the physician’s assistant noticed what
the examiner’s little finger, the hemorrhage moved also.
appeared to be several peas deeply embedded in the left
When the patient was asked to look medially,
external auditory meatus. She decided to attempt the
the physician could clearly see the posterior limit of
removal of the peas through an otoscope. Which direc-
the conjunctival hemorrhage. Does this patient have a
tion should the auricle be pulled in a child to straighten
simple “black eye,” or is this a fracture of the anterior
the meatus and assist in the operation? How does this
cranial fossa of the skull? What role does the orbital
change in the adult?
septum play in enabling one to distinguish between
these lesions? Is the appearance of the conjunctival
8.
Following a severe cold, a 10-year-old girl complained
hemorrhage important in making the diagnosis?
of severe right-sided earache. On examination by her
pediatrician, the tympanic membrane looked reddened
5.
A 6-month-old girl was seen in the emergency depart-
and bulged laterally. A diagnosis of otitis media was
ment because her mother had noticed a yellow, sticky
made. A yellowish area was apparent close to the umbo
discharge from the baby’s left eye. On questioning, the
and it appeared that perforation of the tympanic mem-
mother said that she had first noticed the condition that
brane was about to take place. It was decided to do a
morning when her daughter woke up. She also said that
myringotomy (incise the tympanic membrane). Where
she had noticed that her daughter’s left eye watered
would you do a myringotomy? What structures do you
excessively when she cried ever since birth. The physi-
have to avoid in this operation? What are the features
cian confirmed the epiphora of the left eye and noted
normally seen on the tympanic membrane with an
the emergence of yellow pus into the lacus lacrimalis
otoscope?
from the puncta when gentle pressure was exerted over
the medial palpebral ligament. What is the diagnosis?
9.
A 13-year-old boy was struck on his right ear by another
What is the most likely cause in a child of this age?
boy’s fist during a fight. By the time the boy was exam-
What are the posterior relations of the medial palpebral
ined, the ear was extremely swollen and bluish and very
ligament? Describe the anatomy of the drainage pas-
painful. Explain in anatomic terms where the blood
sages of the conjunctival sac and give the direction of
and edema fluid collect in such a case. Can the ear be
each of the tubes.
treated conservatively or should the hematoma be
drained? What is a cauliflower ear?
A 7-year-old boy with right-sided otitis media was treated with
antibiotics. The organisms did not respond to the treatment,
10.
A 45-year-old woman with a severe cold had to make a
and the infection spread to the mastoid antrum and the mas-
business trip by plane. On takeoff she noticed that her
toid air cells. The surgeon decided to perform a radical mas-
hearing became impaired and she experienced acute
toid operation. After the operation, it was noticed that the
pain in her right ear. She told the stewardess about her
boy’s face was distorted.
problem and asked for an aspirin. The stewardess
6. The following signs and symptoms suggest that the right
advised the patient to relax and swallow hard several
facial nerve had been damaged during the operation
times. On reaching the cruising altitude the right
except which?
ear suddenly popped and the deafness and pain
A. The mouth was drawn upward to the right.
disappeared. In anatomic terms explain this patient’s
B. He was unable to close his right eye.
condition.
The Eye and the Ear
305
Answers and Explanations
1.
C is the correct answer. The intracranial subarachnoid
7.
In a young child, the external auditory meatus may be
space extends forward through the optic canal around
straightened by pulling the auricle directly backward.
the optic nerve as far as the back of the eyeball (see text
In an adult, the meatus is straightened by pulling the
Fig. 18-9).
auricle backward and upward (see CD Fig. 18-4).
2.
D is the correct answer. The left abducent nerve was
8.
A myringotomy is performed through the lower quad-
damaged by the head trauma and resulted in paralysis
rants of the tympanic membrane to avoid damaging the
of the left lateral rectus muscle. As a consequence, the
chorda tympani nerve that crosses the tympanic mem-
medial rectus muscle was unapposed and turned the
brane on the medial side of the upper quadrants (see text
eye medially (medial strabismus).
Fig. 18-15A).The features seen on a normal tympanic
membrane with an otoscope with a good light include
3.
The student had a hordeolum or stye in his right eye.
(1) the long process of the malleus with the umbo; (2) the
The usual cause is a staphylococcal infection of the eye-
anterior and posterior malleolar folds with the pars flac-
lash follicle, the sebaceous gland of Zeis, or the ciliary
cida; (3) the cone of light produced by light reflection on
gland of Moll. The suppurative infection tends to point
the concave tympanic membrane; (4) the tympanic
on the anterior part of the lid margin. Repeated multi-
membrane is pearl colored with no evidence of dilated
ple styes tend to occur as the result of spread of infec-
blood vessels; (5) sometimes when the tympanic mem-
tion along the eyelid margin.
brane is translucent, as in a young child, the long process
4.
This schoolboy has a severe “black eye.” In this patient
of the incus and the promontory on the medial wall of
the contusion involved not only the eyelids but the skin
the middle ear can be seen (see CD Fig. 18-4).
of the cheek and forehead. In anterior cranial fossa frac-
9.
In auricular hematomas the blood tends to accumulate
tures, the hemorrhage occurs into the orbital cavity and
between the perichondrium and the underlying carti-
is limited anteriorly by the attachment of the orbital
lage. The edema fluid has little room to spread since
septum to the orbital margin. In such cases the discol-
the skin is tightly bound down to the perichondrium;
oration tends to be circular. In fractures of the anterior
moreover, the pressure of the fluid causes extreme pain.
cranial fossa, because the bleeding is deeply placed, it
Failure to aspirate the hematoma may lead to necrosis
tends to be purplish from the start, whereas with a black
of the cartilage, since it has been deprived of its blood
eye the color is initially red.
supply due to separation of the perichondrium from the
5.
This girl was suffering from chronic dacryocystitis sec-
cartilage. If cartilaginous necrosis takes place, fibrous
ondary to congenital obstruction of the nasolacrimal
replacement occurs followed by contraction and defor-
duct. The obstruction results from failure of the naso-
mity, the so-called cauliflower ear.
lacrimal duct to open up and drain into the inferior
10.
Inflammation of the mucous membrane of the pharynx
meatus of the nose. The posterior relation of the medial
tends to spread upward to the middle ear via the audi-
palpebral ligament is the lacrimal sac. The drainage
tory tube. The swelling of the mucous membrane lin-
passages start at the puncta on the tip of the lacrimal
ing the stiff wall of the tube results in blockage of the
papilla. The canaliculi first pass vertically in the eyelids
passageway. Very quickly, the trapped air in the middle
for about 2 mm and then turn sharply at right angles
ear becomes absorbed into the bloodstream, creating a
and run medially for about 8 mm to enter the lacrimal
vacuum. As a result, the tympanic membrane is pulled
sac. The lower end of the lacrimal sac is connected to
inward and causes deafness and acute pain. In a plane
the inferior meatus of the nose by the nasolacrimal
that is taking off and climbing quickly, the cabin pres-
duct, which is about 15 mm long. The duct passes
sures are subject to changes and this augments the
downward, backward, and laterally.
pressure differences on the two sides of the tympanic
6.
A is the correct answer. The facial muscles on the left
membrane. Repeated swallowing causes the contrac-
side of the mouth on contraction pull the mouth up-
tion of the salpingopharyngeus muscle and often allows
ward and to the left because the muscles on the right
sufficient air into the tympanic cavity through the audi-
side were paralyzed.
tory tube, thus relieving the problem.
The Abdominal Wall,
the Peritoneal Cavity,
the Retroperitoneal Space,
19
and the Alimentary Tract
Chapter Outline
Abdominal Wall
312
Abdominal Stab Wounds
326
General Appearances of the Abdominal Wall
312
Abdominal Gun Shot Wounds
327
Infection of the Umbilicus
312
Tying the Umbilical Cord
327
Surgical Incisions and Lines of Cleavage
312
Patent Urachus
327
Caval Obstruction
312
Vitellointestinal Duct
327
Portal Vein Obstruction and Caput Medusae
312
Umbilical Vessel Catheterization
327
Indications for Umbilical Artery
Skin and Its Regional Lymph Nodes
312
Catheterization
327
Membranous Layer of the Superficial Fascia
Anatomy of Procedure
327
and a Healing Skin Wound
313
Anatomy of Complications
327
Indications for Umbilical Vein Catheterization
328
Membranous Layer of Superficial Fascia and the
Anatomy of Procedure
328
Extravasation of Urine
313
Anatomy of Complications
329
Hematoma of the Rectus Sheath
313
Peritoneum and Peritoneal Cavity
329
Abdominal Muscles, Abdominothoracic Rhythm,
Movement of Peritoneal Fluid
329
and Visceroptosis
313
Peritoneal Infection
329
Muscle Rigidity and Referred Pain
313
Greater Omentum and the Localization of
Surgery and Tendinous Intersections of the
Infection
329
Rectus Abdominis Muscle
314
Greater Omentum as a Hernial Plug
329
Fate of the Processus Vaginalis
314
Greater Omentum in Surgery
329
Abdominal Herniae
314
Indirect Inguinal Hernia
314
Torsion of the Greater Omentum
329
Direct Inguinal Hernia
315
Ascites
329
Femoral Hernia
316
Peritoneal Pain
330
Umbilical Herniae
319
From the Parietal Peritoneum
330
Epigastric Hernia
320
From the Visceral Peritoneum
331
Separation of the Recti Abdominis
320
Incisional Hernia
320
Peritoneal Dialysis
331
Hernia of the Linea Semilunaris
Internal Abdominal Hernia
331
(Spigelian Hernia)
320
Lumbar Hernia
320
Retroperitoneal Space
331
Internal Hernia
320
Trauma to Organs in the Retroperitoneal Space
331
Abdominal Pain
320
Abscess Formation
332
Somatic Abdominal Pain
320
Leaking Aortic Aneurysm
332
Visceral Abdominal Pain
320
Referred Abdominal Pain
321
The Alimentary Tract
332
Anterior Abdominal Nerve Block
322
Esophagus
332
Surgical Incisions
322
Narrow Areas of the Esophageal Lumen
332
Achalasia of the Cardia (Esophagogastric
Endoscopic Surgery
323
Junction)
332
Paracentesis of the Abdomen
323
Bleeding Esophageal Varices
332
Anatomy of Peritoneal Lavage
324
Anatomy of the Insertion of the
Midline Incision Technique
324
Sengstaken-Blakemore Balloon for
Paraumbilical Incision Technique
325
Esophageal Hemorrhage
332
Anatomy of the Complications of
Anatomy of Complications
332
Peritoneal Lavage
326
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
311
Stomach
332
Cancer of the Rectum
341
Nausea
332
Rectal Injuries
341
Vomiting
332
Anal Canal
341
Trauma to the Stomach
333
Internal Hemorrhoids (Piles)
341
Gastric Ulcer
334
External Hemorrhoids
342
Gastric Pain
334
Perianal Hematoma
343
Cancer of the Stomach
334
Anal Fissure
343
Gastroscopy
334
Perianal Abscesses
345
Nasogastric Intubation
334
Removal of Anorectal Foreign Bodies
345
Anatomic Structures that May Impede
Anal Sphincter Nerve Block and Anesthetizing
the Passage of the Nasogastric Tube
335
the Perianal Skin
345
Anatomy of Complications
335
Incontinence Associated with Rectal
Duodenum
335
Prolapse
345
Trauma to the Duodenum
335
Incontinence after Trauma
345
Duodenal Ulcer
335
Incontinence after Spinal Cord Injury
345
Duodenal Recesses
335
Rectal Examination
346
Important Duodenal Relations
335
Cancer and Lymph Drainage of the
Anal Canal
347
Jejunum and Ileum
335
Trauma to the Jejunum and Ileum
335
Ischiorectal Fossa
347
Recognition of the Jejunum and Ileum
335
The Ischiorectal Fossa and Infection
347
Tumors and Cysts of the Mesentery of the
Small Intestine
335
Congenital Anomalies of the Esophagus
347
Pain Fibers from the Jejunum and Ileum
336
Atresia of the Esophagus
347
Mesenteric Arterial Occlusion
336
Mesenteric Vein Thrombosis
336
Esophageal Stenosis
347
Appendix
336
Congenital Short Esophagus
347
Variability of Position of the Appendix
336
Congenital Anomalies of the Stomach
347
Pelvic Appendix
336
Congenital Hypertrophic Pyloric Stenosis
347
Predisposition of the Appendix to Infection
336
Predisposition of the Appendix to Perforation
336
Congenital Anomalies of the Small
Pain of Appendicitis
336
and Large Intestines
347
Colon and Cecum
336
Diverticula of the Intestine
347
Colonoscopy
336
Atresia and Stenosis of the Small Intestine
348
Trauma of the Cecum and Colon
338
Cancer of the Large Bowel
338
Duplication of the Digestive System
348
Diverticulosis
338
Arrested Rotation or Malrotation of the
Cecostomy and Colostomy
338
Midgut Loop
349
Volvulus
338
Intussusception
338
Complete Absence of Rotation or Incomplete
Rotation
349
Sigmoid Colon
339
Variations in the Length and Location of the
Malrotation of the Midgut Loop
349
Sigmoid Colon
339
Persistence of the Vitellointestinal Duct
349
Cancer of the Sigmoid Colon
339
Meckel’s Diverticulum
349
Volvulus
339
Diverticula
339
Undescended Cecum and Appendix
349
Sigmoidoscopy
339
Anomalies of the Appendix
349
Anatomic Facts Relative to
Sigmoidoscopy
339
Anomalies of the Colon
349
Anatomy of Complications of
Primary Megacolon (Hirschsprung Disease)
349
Sigmoidoscopy
339
Imperforate Anus
349
Colostomy
339
Rectum
340
Clinical Problem Solving Questions
350
Rectal Curves and Mucosal Folds
340
Blood Supply and Internal Hemorrhoids
340
Answers and Explanations
355
Partial and Complete Prolapse of the Rectum
340
312
Chapter 19
line will heal as a narrow scar, whereas one that crosses the
lines will heal as wide or heaped-up scars.
ABDOMINAL WALL
Caval Obstruction
General Appearances of the
If the superior or inferior vena cava is obstructed, the venous
blood causes distension of the veins running from the ante-
Abdominal Wall
rior chest wall to the thigh. The lateral thoracic vein anasto-
The normal abdominal wall is soft and pliable and under-
moses with the superficial epigastric vein, a tributary of the
goes inward and outward excursion with respiration. The
great saphenous vein of the leg. In these circumstances, a
contour is subject to considerable variation and depends on
tortuous varicose vein may extend from the axilla to the
the tone of its muscles and the amount of fat in the subcu-
lower abdomen (CD Fig. 19-1).
taneous tissue. Well-developed muscles or an abundance of
fat can prove to be a severe obstacle to the palpation of the
Portal Vein Obstruction and
abdominal viscera.
Caput Medusae
Infection of the Umbilicus
In cases of portal vein obstruction (CD Fig. 19-2), the super-
In the adult, the umbilicus often receives scant attention in
ficial veins around the umbilicus and the paraumbilical veins
the shower and is consequently a common site of infection.
become grossly distended. The distended subcutaneous veins
radiate out from the umbilicus, producing in severe cases the
clinical picture referred to as caput medusae.
Surgical Incisions and Lines
of Cleavage
Skin and Its Regional Lymph Nodes
If possible, all surgical incisions should be made in the lines
Knowledge of the areas of the skin that drain into a particu-
of cleavage where the bundles of collagen fibers in the
lar group of lymph nodes is clinically important (see text
dermis run in parallel rows. An incision along a cleavage
Fig. 19-3). For example, it is possible to find a swelling in the
lateral thoracic vein
portal vein in porta hepatis
lumbar veins
paraumbilical veins
CD Figure 19-1
Superficial veins of the
anterior abdominal wall. On the left are
anastomoses between systemic veins
and the portal vein via paraumbilical
veins. Arrows indicate the direction taken
varicosed vein
by venous blood when the portal vein is
obstructed. On the right is an enlarged
anastomosis between the lateral thoracic
vein and the superficial epigastric vein.
superficial epigastric vein
This occurs if either the superior or the
interior vena cava is obstructed.
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
313
into the lower part of the anterior abdominal wall deep to
the membranous layer of fascia. The urine is excluded from
the thigh because of the attachment of the fascia to the
fascia lata (see text Fig. 19-4).
Hematoma of the Rectus Sheath
Hematoma of the rectus sheath is uncommon but impor-
tant, since it is often overlooked. It occurs most often on the
right side below the level of the umbilicus. The source of
the bleeding is the inferior epigastric vein or, more rarely,
the inferior epigastric artery. These vessels may be stretched
during a severe bout of coughing or in the later months of
pregnancy, which may predispose to the condition. The
cause is usually blunt trauma to the abdominal wall, such as
a fall or a kick. The symptoms that follow the trauma in-
clude midline abdominal pain. An acutely tender mass
confined to one rectus sheath is diagnostic.
Abdominal Muscles, Abdominotho-
caput Medusae
racic Rhythm, and Visceroptosis
CD Figure 19-2
An example of caput Medusae in a case of
portal obstruction caused by cirrhosis of the liver.
The abdominal muscles contract and relax with respiration,
and the abdominal wall conforms to the volume of the
abdominal viscera. There is an abdominothoracic rhythm.
Normally, during inspiration, when the sternum moves for-
groin (enlarged superficial inguinal node) caused by an in-
ward and the chest expands, the anterior abdominal wall also
fection or malignant tumor of the skin of the lower part of
moves forward. If, when the chest expands, the anterior
the anterior abdominal wall or that of the buttock.
abdominal wall remains stationary or contracts inward, it is
highly probable that the parietal peritoneum is inflamed and
has caused a reflex contraction of the abdominal muscles.
Membranous Layer of the
The shape of the anterior abdominal wall depends on the
tone of its muscles. A middle-aged woman with poor abdom-
Superficial Fascia and a
inal muscles who has had multiple pregnancies is often inca-
pable of supporting her abdominal viscera. The lower part of
Healing Skin Wound
the anterior abdominal wall protrudes forward, a condition
When closing abdominal wounds, it is usual for a surgeon to
known as visceroptosis. This should not be confused with an
put in a continuous suture uniting the divided membranous
abdominal tumor such as an ovarian cyst or with the excessive
layer of superficial fascia. This strengthens the healing
accumulation of fat in the fatty layer of the superficial fascia.
wound, prevents stretching of the skin scar, and makes for a
more cosmetically acceptable result.
Muscle Rigidity and Referred Pain
Sometimes it is difficult for a physician to decide whether
Membranous Layer of Superficial
the muscles of the anterior abdominal wall of a patient are
rigid because of underlying inflammation of the parietal
Fascia and the Extravasation of
peritoneum or whether the patient is voluntarily contracting
the muscles because he or she resents being examined or be-
Urine
cause the physician’s hand is cold. This problem is usually
The membranous layer of the superficial fascia is important
easily solved by asking the patient, who is lying supine on
clinically because beneath it is a potential closed space that
the examination table, to rest the arms by the sides and draw
does not open into the thigh but is continuous with the su-
up the knees to flex the hip joints. It is practically impossible
perficial perineal pouch via the penis and scrotum. Rupture
for a patient to keep the abdominal musculature tensed
of the penile urethra may be followed by extravasation of
when the thighs are flexed. Needless to say, the examiner’s
urine into the scrotum, perineum, and penis and then up
hand should be warm.
314
Chapter 19
A pleurisy involving the lower costal parietal pleura
cannula are inserted through the scrotal skin (see CD
causes pain in the overlying skin that may radiate down into
Fig. 19-4). The following anatomic structures are traversed
the abdomen. Although it is unlikely to cause rigidity of the
by the cannula: skin, dartos muscle and membranous layer
abdominal muscles, it may cause confusion in making a
of fascia (Colles’ fascia), external spermatic fascia, cremas-
diagnosis unless these anatomic facts are remembered.
teric fascia, internal spermatic fascia, and parietal layer of
It is useful to remember the following:
the tunica vaginalis.
Dermatomes over:
■ The xiphoid process-T7
Abdominal Herniae
■ The umbilicus-T10
A hernia is the protrusion of part of the abdominal con-
■ The pubis-L1
tents beyond the normal confines of the abdominal wall
See text Figure 19-1.
(CD Fig. 19-5). It consists of three parts: the sac, the con-
tents of the sac, and the coverings of the sac. The hernial
sac is a pouch (diverticulum) of peritoneum and has a
Surgery and Tendinous
neck and a body. The hernial contents may consist of any
structure found within the abdominal cavity and may vary
Intersections of the Rectus
from a small piece of omentum to a large viscus such as
the kidney. The hernial coverings are formed from the
Abdominis Muscle
layers of the abdominal wall through which the hernial
Transverse tendinous intersections that divide the rectus
sac passes.
abdominis muscle into distinct segments are firmly attached
Abdominal herniae are of the following common types:
to the anterior wall of the rectus sheath, whereas the poste-
■ Inguinal (indirect or direct)
rior wall of the sheath is not attached. This information is of
■ Femoral
great value to the surgeon when entering the abdominal
■ Umbilical (congenital or acquired)
cavity through the anterior abdominal wall.
■ Epigastric
■ Separation of the recti abdominis
Fate of the Processus Vaginalis
■ Incisional hernia
■ Hernia of the linea semilunaris (Spigelian hernia)
The formation of the processus vaginalis and its passage
■ Lumbar hernia (Petit’s triangle hernia)
through the lower part of the anterior abdominal wall with
■ Internal hernia
the formation of the inguinal canal in both sexes were
described in text Chapter 19. Normally, the upper part be-
Indirect Inguinal Hernia
comes obliterated just before birth and the lower part re-
mains as the tunica vaginalis.
The indirect inguinal hernia is the most common form of
The processus is subject to the following common
hernia and is believed to be congenital in origin (CD Fig.
congenital anomalies:
19-6A). The hernial sac is the remains of the processus
vaginalis (an outpouching of peritoneum that in the fetus is
■ It may persist partially or in its entirety as a preformed her-
responsible for the formation of the inguinal canal). It fol-
nial sac for an indirect inguinal hernia (CD Fig. 19-3).
lows that the sac enters the inguinal canal through the deep
■ It may become very much narrowed, but its lumen re-
inguinal ring lateral to the inferior epigastric vessels (CD
mains in communication with the abdominal cavity.
Fig. 19-6). It may extend part of the way along the canal or
Peritoneal fluid accumulates in it, forming a congenital
the full length, as far as the superficial inguinal ring. If the
hydrocele (see CD Fig. 19-3).
processus vaginalis has undergone no obliteration, then the
■ The upper and lower ends of the processus may become
hernia is complete and extends through the superficial
obliterated, leaving a small intermediate cystic area
inguinal ring down into the scrotum or labium majus.
referred to as an encysted hydrocele of the cord (see CD
Under these circumstances the neck of the hernial sac lies
Fig. 19-3).
at the deep inguinal ring lateral to the inferior epigastric
The tunica vaginalis is closely related to the front and
vessels, and the body of the sac resides in the inguinal canal
sides of the testis. It is therefore not surprising to find that
and scrotum (or base of labium majus).
inflammation of the testis can cause an accumulation of
An indirect inguinal hernia is about 20 times more
fluid within the tunica vaginalis. This is referred to simply
common in males than in females, and nearly one third
as a hydrocele
(CD Fig. 19-4). Most hydroceles are
are bilateral. It is more common on the right (normally, the
idiopathic.
right processus vaginalis becomes obliterated after the left;
To remove excess fluid from the tunica vaginalis, a
the right testis descends later than the left). It is most
procedure termed tapping a hydrocele, a fine trocar and
common in children and young adults.
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
315
peritoneal cavity
vas deferens
cyst
persistent
processus
vaginalis
epididymis
testis
peritoneal fluid
A
B
coils of small intestine inside
persistent processus vaginalis, which
forms hernial sac
CD Figure
19-3
Common congenital
anomalies of the processus vaginalis.
A. Congenital hydrocele. B. Encysted hy-
drocele of the cord. C. Preformed hernial
C
sac for indirect inguinal hernia.
The indirect inguinal hernia can be summarized as
Direct Inguinal Hernia
follows:
The direct inguinal hernia makes up about 15% of all
■ It is the remains of the processus vaginalis and therefore
inguinal hernias. The sac of a direct hernia bulges directly
is congenital in origin.
anteriorly through the posterior wall of the inguinal canal
■ It is more common than a direct inguinal hernia.
medial to the inferior epigastric vessels (CD Fig. 19-6B).
■ It is much more common in males than in females.
Because of the presence of the strong conjoint tendon
■ It is more common on the right side.
(combined tendons of insertion of the internal oblique and
■ It is most common in children and young adults.
transversus muscles), this hernia is usually nothing more
■ The hernial sac enters the inguinal canal through the
than a generalized bulge; therefore, the neck of the hernial
deep inguinal ring and lateral to the inferior epigastric
sac is wide.
vessels. The neck of the sac is narrow.
Direct inguinal hernias are rare in women and most are
■ The hernial sac may extend through the superficial in-
bilateral. It is a disease of old men with weak abdominal
guinal ring above and medial to the pubic tubercle.
muscles.
(Femoral hernia is located below and lateral to the pubic
A direct inguinal hernia can be summarized as follows:
tubercle.)
■ The hernial sac may extend down into the scrotum or
■ It is common in old men with weak abdominal muscles
labium majus.
and is rare in women.
316
Chapter 19
acquired hydrocele
hydrocele fluid
scrotal skin
testis
dartos muscle
membranous layer of
superficial fascia
tunica vaginalis
external spermatic fascia
CD Figure 19-4
The tunica vaginalis dis-
tended with fluid (hydrocele). Also shown are
cremasteric fascia
the various anatomic layers traversed by a tro-
internal spermatic fascia
car and cannula when a hydrocele is tapped.
■ The hernial sac bulges forward through the posterior
wall of the inguinal canal medial to the inferior epigas-
neck of hernial sac
tric vessels.
peritoneum
■ The neck of the hernial sac is wide.
An inguinal hernia can be distinguished from a femoral
abdominal wall
hernia by the fact that the sac, as it emerges through the
superficial inguinal ring, lies above and medial to the pubic
tubercle, whereas that of a femoral hernia lies below and
body of hernial sac
lateral to the tubercle (CD Fig. 19-7).
hernial coverings
Femoral Hernia
loop of ileum
The hernial sac descends through the femoral canal within
the femoral sheath, creating a femoral hernia. The femoral
sheath is a protrusion of the fascial envelope lining the
abdominal walls and surrounds the femoral vessels and
lymphatics for about 1 in. (2.5 cm) below the inguinal
ligament (CD Fig. 19-8). The femoral artery, as it enters
the thigh below the inguinal ligament, occupies the lateral
hernial sac
compartment of the sheath. The femoral vein, which lies
CD Figure 19-5
Different parts of a hernia.
on its medial side and is separated from it by a fibrous
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
317
peritoneum
neck of hernia
inferior epigastric artery
extraperitoneal fat
deep inguinal ring
conjoint tendon
A
superficial inguinal ring
pubic tubercle
tunica vaginalis
hernial sac
remains of
processus vaginalis
inferior epigastric artery
neck of hernia
conjoint tendon
deep inguinal ring
B
superficial inguinal ring
CD Figure 19-6
A. Indirect inguinal hernia. B. Direct inguinal hernia. Note that the neck
of the indirect inguinal hernia lies lateral to the inferior epigastric artery, and the neck of
the direct inguinal hernia lies medial to the inferior epigastric artery.
septum, occupies the intermediate compartment. The
end, it expands to form a swelling in the upper part of the
lymph vessels, which are separated from the vein by a
thigh deep to the deep fascia (see CD Fig. 19-8). With
fibrous septum, occupy the most medial compartment.
further expansion, the hernial sac may turn upward to cross
The femoral canal, the compartment for the lymphatics,
the anterior surface of the inguinal ligament.
occupies the medial part of the sheath. It is about 0.5 in.
The neck of the sac always lies below and lateral to the
(1.3 cm) long, and its upper opening is referred to as the
pubic tubercle (see CD Fig. 19-7), which serves to distin-
femoral ring. The femoral septum, which is a condensa-
guish it from an inguinal hernia. The neck of the sac is
tion of extraperitoneal tissue, plugs the opening of the
narrow and lies at the femoral ring. The ring is related
femoral ring.
anteriorly to the inguinal ligament, posteriorly to the
A femoral hernia is more common in women than in
pectineal ligament and the pubis, medially to the sharp
men (possibly because of a wider pelvis and femoral canal).
free edge of the lacunar ligament, and laterally to the
The hernial sac passes down the femoral canal, pushing the
femoral vein. Because of the presence of these anatomic
femoral septum before it. On escaping through the lower
structures, the neck of the sac is unable to expand. Once
318
Chapter 19
inguinal ligament
pubic tubercle
inguinal hernia
femoral hernia
CD Figure 19-7
Relation of inguinal and femoral hernial
sacs to the pubic tubercle.
inguinal ligament
femoral canal
pubic tubercle
lacunar ligament
femoral nerve
pectineus covering
iliopsoas
superior ramus of pubis
femoral vessels
femoral ring
pubic
peritoneum
tubercle
femoral canal
femoral sheath
CD Figure
19-8
The femoral
sheath as seen from below. Arrow
femoral artery
emerging from the femoral canal
femoral vein
indicates the path taken by the
femoral hernial sac. Note relations
femoral hernial sac
of the femoral ring.
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
319
an abdominal viscus has passed through the neck into
Umbilical Herniae
the body of the sac, it may be difficult to push it up and
Congenital umbilical hernia, or exomphalos (omphalo-
return it to the abdominal cavity (irreducible hernia).
cele), is caused by a failure of part of the midgut to return to
Furthermore, after straining or coughing, a piece of
the abdominal cavity from the extraembryonic coelom dur-
bowel may be forced through the neck and its blood
ing fetal life. The hernial sac and its relationship to the um-
vessels may be compressed by the femoral ring, seriously
bilical cord are shown in CD Fig. 19-9.
impairing its blood supply
(strangulated hernia). A
Acquired infantile umbilical hernia is a small hernia
femoral hernia is a dangerous disease and should always be
that sometimes occurs in children and is caused by a weak-
treated surgically.
ness in the scar of the umbilicus in the linea alba (see CD
A femoral hernia can be summarized as follows:
Fig. 19-9). Most become smaller and disappear without
■ A protrusion of abdominal parietal peritoneum down
treatment as the abdominal cavity enlarges.
through the femoral canal forms the hernial sac.
Acquired umbilical hernia of adults is more correctly
■ It is more common in women than in men.
referred to as a paraumbilical hernia. The hernial sac does
■ The neck of the hernial sac lies below and lateral to the
not protrude through the umbilical scar, but through the
pubic tubercle.
linea alba in the region of the umbilicus (see CD Fig. 19-9).
■ The neck of the hernial sac lies at the femoral ring and at
Paraumbilical herniae gradually increase in size and hang
that point is related anteriorly to the inguinal ligament,
downward. The neck of the sac may be narrow, but the body
posteriorly to the pectineal ligament and the pubis, later-
of the sac often contains coils of small and large intestine
ally to the femoral vein, and medially to the sharp free
and omentum. Paraumbilical herniae are much more com-
edge of the lacunar ligament.
mon in women than in men.
linea alba
linea alba
Wharton's jelly
peritoneum
amnion
umbilical cord
hernial sac
D
A
linea alba
weak scar of
B
rectus muscle
linea alba
umbilicus
CD Figure 19-9
A. Congenital
umbilical hernia. B. Infantile
umbilical hernia. C. Paraumbili-
cal hernia. D. Epigastric hernia.
C
E
E. Separation of recti abdominis.
320
Chapter 19
Epigastric Hernia
Internal Hernia
Epigastric hernia occurs through the widest part of the linea
Occasionally, a loop of intestine enters a peritoneal recess
alba, anywhere between the xiphoid process and the um-
(e.g., the lesser sac or the duodenal recesses) and becomes
bilicus. The hernia is usually small and starts off as a small
strangulated at the edges of the recess.
protrusion of extraperitoneal fat between the fibers of the
linea alba. During the following months or years the fat is
Abdominal Pain
forced farther through the linea alba and eventually drags
behind it a small peritoneal sac. The body of the sac often
Abdominal pain is one of the most important problems facing
contains a small piece of greater omentum. It is common in
the physician. This section provides an anatomic basis for the
middle-aged manual workers.
different forms of abdominal pain found in clinical practice.
Three distinct forms of pain exist: somatic, visceral, and
Separation of the Recti Abdominis
referred pain.
Separation of the recti abdominis occurs in elderly multi-
Somatic Abdominal Pain
parous women with weak abdominal muscles (see CD Fig.
19-9). In this condition, the aponeuroses forming the rectus
Somatic abdominal pain in the abdominal wall can arise
sheath become excessively stretched. When the patient
from the skin, fascia, muscles, and parietal peritoneum. It
coughs or strains, the recti separate widely, and a large
can be severe and precisely localized. When the origin is on
hernial sac, containing abdominal viscera, bulges forward
one side of the midline, the pain is also lateralized. The
between the medial margins of the recti. This can be
somatic pain impulses from the abdomen reach the central
corrected by wearing a suitable abdominal belt.
nervous system in the following segmental spinal nerves:
■ Central part of the diaphragm: phrenic nerve (C3, 4,
Incisional Hernia
and 5)
■ Peripheral part of the diaphragm: intercostal nerves
A postoperative incisional hernia is most likely to occur in
(T7-11)
patients in whom it was necessary to cut one of the segmen-
■ Anterior abdominal wall: thoracic nerves (T7-12) and
tal nerves supplying the muscles of the anterior abdominal
the first lumbar nerve
wall; postoperative wound infection with death (necrosis) of
■ Pelvic wall: obturator nerve (L2, 3, and 4)
the abdominal musculature is also a common cause. The
neck of the sac is usually large, and adhesion and strangula-
The inflamed parietal peritoneum is extremely sensitive,
tion of its contents are rare complications. In very obese
and because the full thickness of the abdominal wall is inner-
individuals the extent of the abdominal wall weakness is
vated by the same nerves, it is not surprising to find cutaneous
often difficult to assess.
hypersensitivity (hyperesthesia) and tenderness. Local re-
flexes involving the same nerves bring about a protective phe-
Hernia of the Linea Semilunaris
nomenon in which the abdominal muscles increase in tone.
This increased tone or rigidity, sometimes called guarding, is
(Spigelian Hernia)
an attempt to rest and localize the inflammatory process.
The uncommon hernia of the linea semilunaris occurs
Rebound tenderness occurs when the parietal peri-
through the aponeurosis of the transversus abdominis just
toneum is inflamed. Any movement of that inflamed peri-
lateral to the lateral edge of the rectus sheath. It usually
toneum, even when that movement is elicited by removing
occurs just below the level of the umbilicus. The neck of the
the examining hand from a site distant from the inflamed
sac is narrow, so that adhesion and strangulation of its
peritoneum, brings about tenderness.
contents are common complications.
Examples of acute, severe, localized pain originating in
the parietal peritoneum are seen in the later stages of ap-
Lumbar Hernia
pendicitis. Cutaneous hyperesthesia, tenderness, and mus-
cular spasm or rigidity occur in the lower right quadrant of
The lumbar hernia occurs through the lumbar triangle and
the anterior abdominal wall. A perforated peptic ulcer, in
is rare. The lumbar triangle (Petit’s triangle) is a weak area
which the parietal peritoneum is chemically irritated, pro-
in the posterior part of the abdominal wall. It is bounded
duces the same symptoms and signs but involves the right
anteriorly by the posterior margin of the external oblique
upper and lower quadrants.
muscle, posteriorly by the anterior border of the latissimus
dorsi muscle, and inferiorly by the iliac crest. The floor of
Visceral Abdominal Pain
the triangle is formed by the internal oblique and the
transversus abdominis muscles. The neck of the hernia is
Visceral abdominal pain arises in abdominal organs, visceral
usually large, and the incidence of strangulation is low.
peritoneum, and the mesenteries. The causes of visceral pain
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
321
include stretching of a viscus or mesentery, distension of a
cord. Both somatic and visceral structures can produce re-
hollow viscus, impaired blood supply (ischemia) to a viscus,
ferred pain.
and chemical damage (e.g., acid gastric juice) to a viscus or its
In the case of referred somatic pain, the possible expla-
covering peritoneum. Pain arising from an abdominal viscus
nation is that the nerve fibers from the diseased structure
is dull and poorly localized. Visceral pain is referred to the
and the area where the pain is felt ascend in the central
midline, probably because the viscera develop embryologi-
nervous system along a common pathway, and the cerebral
cally as midline structures and receive a bilateral nerve
cortex is incapable of distinguishing between the sites.
supply; many viscera later move laterally as development pro-
Examples of referred somatic pain follow. Pleurisy involving
ceeds, taking their nerve supply with them.
the lower part of the costal parietal pleura can give rise to
Colic is a form of visceral pain produced by the violent
referred pain in the abdomen because the lower parietal
contraction of smooth muscle; it is commonly caused by
pleura receives its sensory innervation from the lower five
luminal obstruction as in intestinal obstruction, in the
intercostal nerves, which also innervate the skin and mus-
passage of a gallstone in the biliary ducts, or in the passage
cles of the anterior abdominal wall.
of a stone in the ureters.
Visceral pain from the stomach is commonly referred to
Many visceral afferent fibers that enter the spinal cord
the epigastrium (CD Fig. 19-10). The afferent pain fibers
participate in reflex activity. Reflex sweating, salivation,
from the stomach ascend in company with the sympathetic
nausea, vomiting, and increased heart rate may accompany
nerves and pass through the celiac plexus and the greater
visceral pain.
splanchnic nerves. The sensory fibers enter the spinal cord
The sensations that arise in viscera reach the central
at segments T5-9 and give rise to referred pain in der-
nervous system in afferent nerves that accompany the
matomes T5-9 on the lower chest and abdominal walls.
sympathetic nerves and enter the spinal cord through
Visceral pain from the appendix (see CD Fig. 19-10),
the posterior roots. The significance of this pathway is
which is produced by distension of its lumen or spasm of its
better understood in the following discussion on referred
smooth muscle coat, travels in nerve fibers that accompany
visceral pain.
sympathetic nerves through the superior mesenteric plexus
and the lesser splanchnic nerve to the spinal cord (T10
segment). The vague referred pain is felt in the region of the
Referred Abdominal Pain
umbilicus (T10 dermatome). Later, if the inflammatory
Referred abdominal pain is the feeling of pain at a location
process involves the parietal peritoneum, the severe somatic
other than the site of origin of the stimulus but in an area
pain dominates the clinical picture and is localized
supplied by the same or adjacent segments of the spinal
precisely in the right lower quadrant.
gallbladder,
diaphragm
esophagus
heart
gallbladder
gallbladder
stomach
appendix
kidney
ureter
urinary bladder
CD Figure 19-10
Some important skin areas involved in referred pain.
322
Chapter 19
Visceral pain from the gallbladder, as occurs in pa-
extensive operations in which a large exposure is re-
tients with cholecystitis or gallstone colic, travels in nerve
quired, the incision can run the full length of the rectus
fibers that accompany sympathetic nerves. They pass
sheath. The anterior wall of the rectus sheath is exposed
through the celiac plexus and greater splanchnic nerves to
and incised about 1 in. (2.5 cm) from the midline. The
the spinal cord (segments T5-9). The vague referred pain
medial edge of the incision is dissected medially, free-
is felt in the dermatomes (T5-9) on the lower chest and
ing the anterior wall of the sheath from the tendinous
upper abdominal walls (see CD Fig. 19-10). If the inflam-
intersections of the rectus muscle. The rectus abdo-
matory process spreads to involve the parietal peritoneum
minis muscle is retracted laterally with its nerve supply
of the anterior abdominal wall or peripheral diaphragm,
intact, and the posterior wall of the sheath is exposed.
the severe somatic pain is felt in the right upper quadrant
The posterior wall is then incised, together with the
and through to the back below the inferior angle of the
fascia transversalis and the peritoneum. The wound is
scapula. Involvement of the central diaphragmatic parietal
closed in layers.
peritoneum, which is innervated by the phrenic nerve (C3,
■ Pararectus incision: The anterior wall of the rectus
4, and 5), can give rise to referred pain over the shoulder
sheath is incised medially and parallel to the lateral mar-
because the skin in this area is innervated by the supra-
gin of the rectus muscle. The rectus is freed and retracted
clavicular nerves (C3 and 4).
medially, exposing the segmental nerves entering its pos-
terior surface. If the opening into the abdominal cavity is
to be small, these nerves may be retracted upward and
Anterior Abdominal Nerve Block
downward. The posterior wall of the sheath is then in-
See CD Chapter 17.
cised, as in the paramedian incision. The great disadvan-
tage of this incision is that the opening is small, and any
longitudinal extension requires that one or more seg-
Surgical Incisions
mental nerves to the rectus abdominis be divided, with
resultant postoperative rectus muscle weakness.
The length and direction of surgical incisions through the
■ Midline incision: This incision is made through the
anterior abdominal wall to expose the underlying viscera are
linea alba. The fascia transversalis, the extraperitoneal
largely governed by the position and direction of the nerves
connective tissue, and the peritoneum are then incised.
of the abdominal wall, the direction of the muscle fibers,
It is easier to perform above the umbilicus because the
and the arrangement of the aponeuroses forming the rectus
linea alba is wider in that region. It is a rapid method of
sheath. Ideally, the incision should be made in the direction
gaining entrance to the abdomen and has the obvious
of the lines of cleavage in the skin so that a hairline scar is
advantage that it does not damage muscles or their nerve
produced. The surgeon usually has to compromise, placing
and blood supplies. Midline incision has the additional
the safety of the patient first and the cosmetic result second.
advantage that it may be converted into a T-shaped inci-
Incisions that necessitate the division of one of the main
sion for greater exposure. The anterior and posterior
segmental nerves lying within the abdominal wall result in
walls of the rectus sheath are then cut across transversely,
paralysis of part of the anterior abdominal musculature and
and the rectus muscle is retracted laterally.
a segment of the rectus abdominis. The consequent weak-
■ Transrectus incision: The technique of making and
ness of the abdominal musculature causes an unsightly
closing this incision is the same as that used in the para-
bulging forward of the abdominal wall and visceroptosis;
median incision, except that the rectus abdominis mus-
extreme cases may require a surgical belt for support.
cle is incised longitudinally and not retracted laterally
If the incision can be made in the line of the muscle
from the midline. This incision has the great disadvan-
fibers or aponeurotic fibers as each layer is traversed, on
tage of sectioning the nerve supply to that part of the
closing the incision the fibers fall back into position and
muscle that lies medial to the muscle incision.
function normally.
■ Transverse incision: This can be made above or below
Incisions through the rectus sheath are widely used,
the umbilicus and can be small or so large that it ex-
provided that the rectus abdominis muscle and its nerve
tends from flank to flank. It can be made through the
supply are kept intact. On closure of the incisions, the ante-
rectus sheath and the rectus abdominis muscles and
rior and posterior walls of the sheath are sutured separately,
through the oblique and transversus abdominis muscles
and the rectus muscle springs back into position between
laterally. It is rare to damage more than one segmental
the suture lines. The result is a very strong repair, with min-
nerve so that postoperative abdominal weakness is
imum interference with function.
minimal. The incision gives good exposure and is well
The following incisions are commonly used:
tolerated by the patient. Closure of the wound is made
■ Paramedian incision: This may be supraumbilical, for
in layers. It is unnecessary to suture the cut ends of the
exposure of the upper part of the abdominal cavity, or
rectus muscles, provided that the sheaths are carefully
infraumbilical, for the lower abdomen and pelvis. In
repaired.
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
323
■ Muscle splitting, or McBurney’s incision: This is
chiefly used for cecostomy and appendectomy. It gives a
Endoscopic Surgery
limited exposure only, and should any doubt arise about
Endoscopic surgery on the gallbladder, bile ducts, and ap-
the diagnosis, an infraumbilical right paramedian inci-
pendix has become a common procedure. It involves the
sion should be used instead. An oblique skin incision is
passage of the endoscope into the peritoneal cavity through
made in the right iliac region about 2 in. (5 cm) above
small incisions in the anterior abdominal wall. The
and medial to the anterior superior iliac spine. The ex-
anatomic structures traversed by the instruments are similar
ternal and internal oblique and transversus muscles are
to those enumerated for peritoneal lavage. Great care must
incised or split in the line of their fibers and retracted to
be taken to preserve the integrity of the segmental nerves as
expose the fascia transversalis and the peritoneum. The
they course down from the costal margin to supply the
latter are now incised and the abdominal cavity is
abdominal musculature.
opened. The incision is closed in layers, with no postop-
The advantages of this surgical technique are that the
erative weakness.
anatomic and physiologic features of the anterior abdominal
■ Abdominothoracic incision: This is used to expose the
wall are disrupted only minimally and, consequently, con-
lower end of the esophagus, as, for example, in esopha-
valescence is brief. The great disadvantages are that the
gogastric resection for carcinoma of this region. An upper
surgical field is small and the surgeon is limited in the extent
oblique or paramedian abdominal incision is extended
of the operation (CD Fig. 19-11).
upward and laterally into the seventh, eighth, or ninth
intercostal space, the costal arch is transected, and the
diaphragm is incised. Wide exposure of the upper ab-
Paracentesis of the Abdomen
domen and thorax is then obtained by the use of a rib-
Paracentesis of the abdomen may be necessary to withdraw
spreading retractor.
excessive collections of peritoneal fluid, as in ascites
On completion of the operation, the diaphragm is re-
secondary to cirrhosis of the liver or malignant ascites
paired with nonabsorbable sutures, the costal margin is
secondary to advanced ovarian cancer. Under a local anes-
reconstructed, and the abdominal and thoracic wounds
thetic, a needle or catheter is inserted through the anterior
are closed.
abdominal wall. The underlying coils of intestine are not
CD Figure 19-11
Inguinal canal anatomy as viewed during laparoscopic exploration of the
peritoneal cavity. A. The normal anatomy of the inguinal region from within the peritoneal
cavity. Black arrow indicates the closed deep inguinal ring; white arrow, the inferior epigas-
tric vessels. B. An indirect inguinal hernia. Curved black arrow indicates the mouth of the
hernial sac; white arrow, the inferior epigastric vessels. (Courtesy of N.S. Adzick.)
324
Chapter 19
costal margin
superior
epigastric
artery
umbilicus
inferior
anterior
epigastric
superior
artery
iliac spine
CD Figure 19-12
Common sites used in abdom-
deep circumflex
inal paracentesis. Note the position of the supe-
iliac artery
rior and inferior epigastric arteries in the rectus
sheath and the deep circumflex iliac arteries.
damaged because they are mobile and are pushed away by
Fig. 19-14). It is generally employed as a diagnostic tech-
the cannula.
nique in certain cases of blunt abdominal trauma. In non-
If the cannula is inserted in the midline (CD Figs. 19-
trauma situations, peritoneal lavage has been used to
12 and 19-13), it will pass through the following anatomic
confirm the diagnosis of acute pancreatitis and primary
structures: skin, superficial fascia, deep fascia (very thin),
peritonitis, to correct hypothermia, and to conduct dialysis.
linea alba (virtually bloodless), fascia transversalis, extraperi-
The patient is placed in the supine position and the uri-
toneal connective tissue (fatty), and parietal peritoneum.
nary bladder is emptied by catheterization. In small chil-
If the cannula is inserted in the flank (see CD Figs. 19-
dren the bladder is an abdominal organ; in adults, the full
12 and 19-13) lateral to the inferior epigastric artery and above
bladder may rise out of the pelvis and reach as high as the
the deep circumflex artery, it will pass through the following:
umbilicus. The stomach is emptied by a nasogastric tube
skin, superficial fascia, deep fascia (very thin), aponeurosis or
because a distended stomach may extend to the anterior ab-
muscle of external oblique, internal oblique muscle, trans-
dominal wall. The skin is anesthetized and a 2.25 in. (3-cm)
versus abdominis muscle, fascia transversalis, extraperitoneal
vertical incision is made.
connective tissue (fatty), and parietal peritoneum.
Midline Incision Technique
Anatomy of Peritoneal Lavage
The following anatomic structures are penetrated, in order,
Peritoneal lavage is used to sample the intraperitoneal space
to reach the parietal peritoneum (CD Fig. 19-14): skin, fatty
for evidence of damage to viscera and blood vessels (CD
layer of superficial fascia, membranous layer of superficial
1
rectus abdominis
in sheath
skin
supericial fascia
2
linea
external oblique
alba
internal oblique
transversus abdominis
fascia transversalis
coils of
extraperitoneal fat
small intestine
parietal peritoneum
peritoneal cavity
CD Figure 19-13
Paracentesis of the abdominal cavity in midline (1) and laterally (2).
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
325
costal margin
superior epigastric
artery
umbilicus
inferior epigastric
artery
anterior superior
iliac spine
A
fatty layer of
rectus abdominis
superficial fascia
muscle
catheter
skin
membranous layer of
linea alba
superficial fascia
B
fascia transversalis
parietal
extraperitoneal fat
peritoneum
retracted rectus
anterior wall of
abdominis muscle
rectus sheath
umbilicus
inferior epigastric artery
linea alba
fascia transversalis
peritoneum
posterior wall
C
extraperitoneal fat
of rectus sheath
CD Figure 19-14
Peritoneal lavage. A. The two common sites used in this procedure. Note
the positions of the superior and inferior epigastric arteries in the rectus sheath. B. Cross
section of the anterior abdominal wall in the midline. Note the structures pierced by the
catheter. C. Cross section of the anterior abdominal wall just lateral to the umbilicus. Note
the structures pierced by the catheter. The rectus muscle has been retracted laterally.
fascia, thin layer of deep fascia, linea alba, fascia transver-
fatty layer of superficial fascia, membranous layer of superfi-
salis, extraperitoneal fat, and parietal peritoneum.
cial fascia, thin layer of deep fascia, anterior wall of rectus
sheath, the rectus abdominis muscle is retracted, posterior
wall of the rectus sheath, fascia transversalis, extraperitoneal
Paraumbilical Incision Technique
fat, and parietal peritoneum.
The following anatomic structures are penetrated, in order,
It is important that all the small blood vessels in the
to reach the parietal peritoneum (see CD Fig. 19-14): skin,
superficial fascia be secured, because bleeding into the
326
Chapter 19
structures present in the normal umbilicus
umbilicus
patent urachus
umbilical vein
bladder
midgut loop
site of future
umbilicus
umbilical cord
vitelline duct
allantois
urinary bladder
fecal fistula
fibrous band
Meckel's diverticulum
CD Figure 19-15
Umbilicus and
vitelline cyst
fibrous band and a Meckel's diverticulum
some common congenital defects.
peritoneal cavity might produce a false-positive result.
■ Perforation of a full bladder
These vessels are the terminal branches of the superficial
■ Wound infection
and deep epigastric arteries and veins.
Abdominal Stab Wounds
Anatomy of the Complications of
Abdominal stab wounds may or may not penetrate the
Peritoneal Lavage
parietal peritoneum and violate the peritoneal cavity, and
■
In the midline technique, the incision or trochar may
consequently may or may not significantly damage the
miss the linea alba and enter the rectus sheath and
abdominal viscera. The structures in the various layers
traverse the vascular rectus abdominis muscle and en-
through which an abdominal stab wound penetrates will
counter branches of the epigastric vessels. Bleeding from
depend on the anatomic location.
this source could produce a false-positive result.
Lateral to the rectus sheath (see CD Fig. 19-13) are the
■
Perforation of the gut by the scalpel or trocar
following: skin, fatty layer of superficial fascia, membranous
■
Perforation of the mesenteric blood vessels or vessels on
layer of superficial fascia, thin layer of deep fascia, external
the posterior abdominal wall or pelvic walls
oblique muscle or aponeurosis, internal oblique muscle or
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
327
aponeurosis, transversus abdominis muscle or aponeurosis,
lointestinal duct can result in an umbilical fecal fistula (see
fascia transversalis, extraperitoneal connective tissue (often
CD Fig. 19-15). If the duct remains as a fibrous band, a loop
fatty), and parietal peritoneum.
of bowel can become wrapped around it, causing intestinal
Anterior to the rectus sheath (see CD. Fig. 19-13) are
obstruction (see CD Fig. 19-15).
the following: skin; fatty layer of superficial fascia; membra-
Meckel’s diverticulum is a congenital anomaly repre-
nous layer of superficial fascia; thin layer of deep fascia;
senting a persistent portion of the vitellointestinal duct. It
anterior wall of rectus sheath; rectus abdominis muscle,
occurs in 2% of patients (see CD Fig. 19-15), is located
with segmental nerves and epigastric vessels lying behind
about 2 ft (61 cm) from the ileocolic junction, and is about
the muscle; posterior wall of rectus sheath; fascia transver-
2 in. (5 cm) long. It can become ulcerated or cause intesti-
salis; extraperitoneal connective tissue (often fatty); and
nal obstruction.
parietal peritoneum.
In the midline (see CD Fig. 19-13) are the following:
Umbilical Vessel Catheterization
skin, fatty layer of superficial fascia, membranous layer of
superficial fascia, thin layer of deep fascia, linea alba, fascia
The umbilical cord is surrounded by the fetal membrane,
transversalis, extraperitoneal connective tissue (often fatty),
amnion, and contains Wharton’s jelly. Embedded in this
and parietal peritoneum.
jelly are the remains of the vitellointestinal duct and the
In a stab wound, peritoneal lavage may be used to
allantois, and the single umbilical vein and the two
determine whether any damage to viscera or vasculature has
umbilical arteries (CD Fig. 19-16). The vein is a larger thin-
occurred.
walled vessel and is located at the 12 o’clock position when
facing the umbilicus; the two arteries, which lie adjacent to
one another and are located at the 4 and 8 o’clock positions
Abdominal Gunshot Wounds
when facing the umbilicus, are smaller and thick walled.
Gunshot wounds are much more serious than stab wounds;
in most patients, the peritoneal cavity has been entered, and
Indications for Umbilical Artery
significant visceral damage has ensued.
Catheterization
1. Administration of fluids or blood for resuscitation
Tying the Umbilical Cord
purposes
At birth, the cord is tied off close to the umbilicus. About 2
2. Arterial blood gas and blood pressure monitoring. The
in. (5 cm) of cord is left between the umbilicus and the lig-
umbilical arteries may be cannulated most easily dur-
ature, since a piece of intestine may be present as an um-
ing the first few hours after birth, but they may be
bilical hernia in the remains of the extraembryonic coelom.
cannulated up to 6 days after delivery.
After application of the ligature, the umbilical vessels con-
strict and thrombose. Later, the stump of the cord is shed
Anatomy of Procedure
and the umbilical scar tissue becomes retracted and as-
One of the small, thick-walled arteries is identified in the
sumes the shape of the umbilicus, or navel.
Wharton’s jelly in the umbilical stump. Because the umbil-
ical arteries are branches of the internal iliac arteries in the
Patent Urachus
pelvis, the catheter is introduced and advanced slowly in the
direction of the feet. The catheter can be inserted for about
The urachus is the remains of the allantois of the fetus and
2.75 in. (7 cm) in a premature infant and 4.75 in. (12 cm)
normally persists as a fibrous cord that runs from the apex
in a full-term infant. The course of the catheter can be con-
of the bladder to the umbilicus. Occasionally, the cavity of
firmed on a radiograph and is as follows: (1) umbilical artery
the allantois persists, and urine passes from the bladder
(directed downward into the pelvis), (2) internal iliac artery
through the umbilicus. In newborns, it usually reveals
(acute turn into this artery), and (3) common iliac artery and
itself when a congenital urethral obstruction is present.
the aorta.
More often, it remains undiscovered until old age, when
enlargement of the prostate may obstruct the urethra (see
Anatomy of Complications
CD Fig. 19-15).
■ Catheter perforates arterial wall at a point where the
artery turns downward toward the pelvis at the anterior
Vitellointestinal Duct
abdominal wall.
The vitelline duct in the early embryo connects the devel-
■ Catheter enters the thin-walled wider umbilical vein
oping gut to the yolk sac. Normally, as development
instead of the thick-walled smaller artery.
proceeds, the duct is obliterated, severs its connection with
■ Catheter enters the thin-walled persistent urachus (urine
the small intestine, and disappears. Persistence of the vitel-
is returned into catheter).
328
Chapter 19
inferior vena cava
ductus venosus
liver
branch of portal vein
at porta hepatis
umbilical vein
single umbilical vein
note direction of bend
of blood vessels
abdominal
aorta
catheters
common
iliac artery
two umbilical
arteries
stump of
external
umbilical cord
iliac artery
left internal
iliac artery
left umbilical
artery
right umbilical
artery
CD Figure 19-16
Catheterization of the umbilical blood vessels. Arrangement of the single
umbilical vein and the two umbilical arteries in the umbilical cord and the paths taken by the
catheter in the umbilical vein and the umbilical artery.
■ Vasospasm of the umbilical and the iliac arteries causing
2. Exchange transfusions; the umbilical vein may be
blanching of the leg
cannulated up to 7 days after birth.
■ Perforation of arteries distal to the umbilical artery, for
Anatomy of Procedure
example, the iliac arteries or even the aorta
■ Other complications include thrombosis, emboli, and
The umbilical vein is located in the cord stump at the 12 o’-
infection of the umbilical stump.
clock position (see CD Fig. 19-16), as described previously,
and is easily recognized because of its thin wall and large
Indications for Umbilical Vein
lumen. The catheter is advanced gently and is directed
Catheterization
toward the head, because the vein runs in the free margin of
the falciform ligament to join the ductus venosus at the
1. Administration of fluids or blood for resuscitation
porta hepatis. The catheter may be advanced about 2 in.
purposes
(5 cm) in a full-term infant. The course of the catheter may
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
329
be confirmed by radiography and is as follows: (1) the um-
matic peritoneum.) The skin of the shoulder is supplied by
bilical vein, (2) the ductus venosus, and (3) the inferior vena
the supraclavicular nerves (C3 and 4), which have the
cava (4 to 4.75 in.; 10 to 12 cm).
same segmental origin as the phrenic nerve, which sup-
plies the peritoneum in the center of the undersurface of
Anatomy of Complications
the diaphragm.
To avoid the accumulation of infected fluid in the sub-
■ Catheter may perforate the venous wall. This is most
phrenic spaces and to delay the absorption of toxins from in-
likely to occur where the vein turns cranially at the
traperitoneal infections, it is common nursing practice to sit
abdominal wall.
a patient up in bed with the back at an angle of 45°. In this
■ Other complications include liver necrosis, hemorrhage,
position, the infected peritoneal fluid tends to gravitate
and infection.
downward into the pelvic cavity, where the rate of toxin ab-
sorption is slow (see CD Fig. 19-17).
PERITONEUM AND
Greater Omentum and the
PERITONEAL
Localization of Infection
The greater omentum is often referred to by the surgeons as
CAVITY
the abdominal policeman. The lower and the right and left
margins are free, and it moves about the peritoneal cavity in
response to the peristaltic movements of the neighboring
Movement of Peritoneal Fluid
gut. In the first 2 years of life it is poorly developed and thus
The peritoneal cavity is divided into an upper part within
is less protective in a young child. Later, however, in an
the abdomen and a lower part in the pelvis. The abdominal
acutely inflamed appendix, for example, the inflammatory
part is further subdivided by the many peritoneal reflections
exudate causes the omentum to adhere to the appendix and
into important recesses and spaces, which, in turn, are con-
wrap itself around the infected organ (CD Fig. 19-18). By
tinued into the paracolic gutters (CD Fig. 19-17). The at-
this means, the infection is often localized to a small area of
tachment of the transverse mesocolon and the mesentery of
the peritoneal cavity, thus saving the patient from a serious
the small intestine to the posterior abdominal wall provides
diffuse peritonitis.
natural peritoneal barriers that may hinder the movement of
infected peritoneal fluid from the upper part to the lower
Greater Omentum as a Hernial Plug
part of the peritoneal cavity.
It is interesting to note that when the patient is in the
The greater omentum has been found to plug the neck of
supine position the right subphrenic peritoneal space and
a hernial sac and prevent the entrance of coils of small
the pelvic cavity are the lowest areas of the peritoneal cavity
intestine.
and the region of the pelvic brim is the highest area (see CD
Fig. 19-17).
Greater Omentum in Surgery
Surgeons sometimes use the omentum to buttress an
Peritoneal Infection
intestinal anastomosis or in the closure of a perforated
Infection may gain entrance to the peritoneal cavity through
gastric or duodenal ulcer.
several routes: from the interior of the gastrointestinal tract
and gallbladder, through the anterior abdominal wall, via
Torsion of the Greater Omentum
the uterine tubes in females (gonococcal peritonitis in
adults and pneumococcal peritonitis in children occur
The greater omentum may undergo torsion, and if
through this route), and from the blood.
extensive, the blood supply to a part of it may be cut off,
Collection of infected peritoneal fluid in one of the
causing necrosis.
subphrenic spaces is often accompanied by infection of
the pleural cavity. It is common to find a localized
Ascites
empyema in a patient with a subphrenic abscess. It is be-
lieved that the infection spreads from the peritoneum to
Ascites is essentially an excessive accumulation of peritoneal
the pleura via the diaphragmatic lymph vessels. A patient
fluid within the peritoneal cavity. Ascites can occur
with a subphrenic abscess may complain of pain over the
secondary to hepatic cirrhosis (portal venous congestion),
shoulder. (This also holds true for collections of blood
malignant disease (e.g., cancer of the ovary), or congestive
under the diaphragm, which irritate the parietal diaphrag-
heart failure (systemic venous congestion). In a thin patient,
330
Chapter 19
anterior and posterior
anterior left subphrenic space
right subphrenic spaces
phrenicocolic
ligament
right
paracolic
gutter
left
paracolic gutter
2
1
pelvic brim
right posterior subphrenic space
pelvic cavity
pelvic cavity
3
4
CD Figure 19-17
Direction of flow of the peritoneal fluid. 1. Normal flow upward to the
subphrenic spaces. 2. Flow of inflammatory exudate in peritonitis. 3. The two sites where
inflammatory exudate tends to collect when the patient is nursed in the supine position.
4. Accumulation of inflammatory exudate in the pelvis when the patient is nursed in the
inclined position.
as much as 1,500 mL has to accumulate before ascites can
first lumbar nerve. Abdominal pain originating from the
be recognized clinically. In obese individuals, a far greater
parietal peritoneum is therefore of the somatic type, can be
amount has to collect before it can be detected.
precisely localized, and is usually severe (see Abdominal
Pain).
An inflamed parietal peritoneum is extremely sensi-
Peritoneal Pain
tive to stretching. This fact is made use of clinically in
diagnosing peritonitis. Pressure is applied to the ab-
From the Parietal Peritoneum
dominal wall with a single finger over the site of the in-
The parietal peritoneum lining the anterior abdominal
flammation. The pressure is then removed by suddenly
wall is supplied by the lower six thoracic nerves and the
withdrawing the finger. The abdominal wall rebounds,
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
331
CD Figure 19-18
A. The normal greater
omentum. B. The greater omentum
wrapped around an inflamed appendix.
C. Greater omentum adherent to the
base of a gastric ulcer. One important
function of the greater omentum is to
attempt to limit the spread of intraperi-
A
B
C
toneal infections.
resulting in extreme local pain, which is known as re-
the same as peritoneal lavage. The products of metabolism,
bound tenderness.
such as urea, diffuse through the peritoneal lining cells from
It should always be remembered that the parietal peri-
the blood vessels into the dialysate and are removed from
toneum in the pelvis is innervated by the obturator nerve
the patient.
and can be palpated by means of a rectal or vaginal exami-
nation. An inflamed appendix may hang down into the
Internal Abdominal Hernia
pelvis and irritate the parietal peritoneum. A pelvic exami-
nation can detect extreme tenderness of the parietal peri-
Occasionally, a loop of intestine enters a peritoneal pouch
toneum on the right side.
or recess (e.g., the lesser sac or the duodenal recesses) and
becomes strangulated at the edges of the recess. Remember
From the Visceral Peritoneum
that important structures form the boundaries of the
entrance into the lesser sac and that the inferior mesenteric
The visceral peritoneum, including the mesenteries, is in-
vein often lies in the anterior wall of the paraduodenal
nervated by autonomic afferent nerves. Stretch caused by
recess.
overdistension of a viscus or pulling on a mesentery gives
rise to the sensation of pain. The sites of origin of visceral
pain are shown in CD Fig. 19-10.
Because the gastrointestinal tract arises embryologically
RETROPERITONEAL
as a midline structure and receives a bilateral nerve
supply, pain is referred to the midline. Pain arising from an
SPACE
abdominal viscus is dull and poorly localized (see Abdomi-
nal Pain).
Trauma to Organs in the
Peritoneal Dialysis
Retroperitoneal Space
Because the peritoneum is a semipermeable membrane, it
allows rapid bidirectional transfer of substances across itself.
Palpation of the anterior abdominal wall in the lumbar
Because the surface area of the peritoneum is enormous,
and iliac regions may give rise to signs indicative of peri-
this transfer property has been made use of in patients with
toneal irritation (the peritoneum forms the anterior bound-
acute renal insufficiency. The efficiency of this method is
ary of the space; see text Fig.
19-30). In other words,
only a fraction of that achieved by hemodialysis.
tenderness and muscle spasm (rigidity) may be present.
A watery solution, the dialysate, is introduced through a
Palpation of the back in the interval between the twelfth
catheter through a small midline incision through the ante-
rib and the vertebral column may reveal tenderness sug-
rior abdominal wall below the umbilicus. The technique is
gestive of kidney disease.
332
Chapter 19
Abdominal radiographs may reveal air in the extraperi-
portal hypertension develops, resulting in dilatation and
toneal tissues, indicating perforation of a viscus (e.g., as-
varicosity of the portal-systemic anastomoses. Varicosed
cending or descending colon). Computed tomography
esophageal veins may rupture, causing severe vomiting of
scans can often accurately define the extent of the injury to
blood (hematemesis).
the extraperitoneal organs.
Anatomy of the Insertion of the
Sengstaken-Blakemore Balloon
Abscess Formation
for Esophageal Hemorrhage
Infection originating in retroperitoneal organs, such as the
kidneys, lymph nodes, and retrocecal appendix, may extend
The Sengstaken-Blakemore balloon is used for the control
widely into the retroperitoneal space.
of massive esophageal hemorrhage from esophageal varices.
A gastric balloon anchors the tube against the esophageal--
gastric junction. An esophageal balloon occludes the
Leaking Aortic Aneurysm
esophageal varices by counterpressure. The tube is inserted
The blood may first be confined to the retroperitoneal space
through the nose or by using the oral route.
before rupturing into the peritoneal cavity.
The lubricated tube is passed down into the stom-
ach, and the gastric balloon is inflated. In the average
adult the distance between the external orifices of the
nose and the stomach is 17.2 in. (44 cm), and the dis-
THE ALIMENTARY
tance between the incisor teeth and the stomach is 16 in.
(41 cm).
TRACT
Anatomy of the Complications
■ Difficulty in passing the tube through the nose
Esophagus
■ Damage to the esophagus from overinflation of the
esophageal tube
Narrow Areas of the Esophageal
■ Pressure on neighboring mediastinal structures as
Lumen
the esophagus is expanded by the balloon within its
lumen
The esophagus is narrowed at three sites: at the beginning,
■ Persistent hiccups caused by irritation of the diaphragm
behind the cricoid cartilage of the larynx; where the left
by the distended esophagus and irritation of the stomach
bronchus and the arch of the aorta cross the front of
by the blood
the esophagus; and where the esophagus enters the stomach.
These three sites may offer resistance to the passage of a tube
down the esophagus into the stomach (CD Fig. 19-19).
Stomach
Achalasia of the Cardia
Nausea
(Esophagogastric Junction)
Nausea is a very common symptom and may occur as the
The cause of achalasia is unknown, but it is associated with
result of drugs, such as anesthetics and apomorphine,
a degeneration of the parasympathetic plexus (Auerbach’s
pregnancy, motion sickness, and chemotherapy. It often
plexus) in the wall of the esophagus. The primary site of the
precedes vomiting. Nausea is the recognition that the vom-
disorder may be in the innervation of the cardioesophageal
iting center in the medulla oblongata is being stimulated by
sphincter by the vagus nerves. Dysphagia (difficulty in swal-
afferent impulses derived from the stomach and intestines,
lowing) and regurgitation are common symptoms that are
or in the case of motion sickness, impulses derived from the
later accompanied by proximal dilatation and distal narrow-
semicircular canals of the inner ear. It is well known that
ing of the esophagus.
certain offensive odors can initiate nausea and vomiting and
this is presumably due to the direct stimulation of the
Bleeding Esophageal Varices
vomiting center by nerve impulses from the cerebral cortex.
At the lower third of the esophagus is an important
Vomiting
portal-systemic venous anastomosis. Here, the esophageal
tributaries of the left gastric vein (which drains into the por-
Vomiting is the process by which the stomach and upper
tal vein) anastomose with the esophageal tributaries of the
intestinal tract empties itself of its contents. It is caused by
azygos veins (systemic veins). Should the portal vein be-
the presence in the upper gastrointestinal tract of some sub-
come obstructed, as, for example, in cirrhosis of the liver,
stance, chemical, bacterial, or viral, that excessively irritates
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
333
external naris
incisor tooth
cervical constriction
7.2 in. (18 cm)
6 in. (15 cm)
bronchoaortic constriction
11.2 in. (28 cm)
10 in. (25 cm)
tube
diaphragmatic constriction
17.2 in. (44 cm)
16 in. (41 cm)
CD Figure 19-19
The approxi-
mate respective distances from
the incisor teeth (black) and the
nostrils (red) to the normal three
duodenum
constrictions of the esophagus.
23.2-27.2 in. (59-69 cm)
To assist in the passage of a
22-26 in. (56-66 cm)
tube to the duodenum, the dis-
tances to the first part of the
duodenum are also included.
the gut wall and results in overdistension of the upper part
the expulsive phase a deep breath is taken and the larynx is
of the gastrointestinal tract. The act of vomiting is preceded
raised to close the inlet; the nasopharynx is also closed by the
by excessive salivation (presumably an attempt to dilute the
raising of the soft palate. This is quickly followed by the mas-
irritant). This is followed by stimulation of the sympathetic
sive coordinated contraction of the diaphragm and abdomi-
system resulting in dilatation of the pupils, an increase in
nal muscles exerting intense squeezing pressure on the
the heart rate, facial pallor (due to vasoconstriction of the
stomach. Suddenly the gastroesophageal sphincter relaxes
blood vessels), cold sweating, fatigue, and drowsiness. Nerve
and the stomach contents are ejected through the esopha-
impulses travel to the vomiting center from the gastroin-
gus and the mouth. The act of vomiting usually makes the
testinal tract via the vagi and sympathetic afferent fibers.
patient feel better, but it may be repeated if the irritant has
Once the nerve stimulation of the vomiting center reaches
not been expelled or the drug action persists.
a certain level, the vomiting act takes place.
The act of vomiting has two phases. The retching phase
Trauma to the Stomach
is nonproductive and involves one or two rounds of the
coordinated contraction of the diaphragm, the anterior
Apart from its attachment to the esophagus at the cardiac
abdominal wall muscles, and the muscles of inspiration. In
orifice and its continuity with the duodenum at the
334
Chapter 19
Gastric Pain
pylorus, the stomach is relatively mobile. It is protected on
the left by the lower part of the rib cage. These factors
The sensation of pain in the stomach is caused by the stretch-
greatly protect the stomach from blunt trauma to the
ing or spasmodic contraction of the smooth muscle in its walls
abdomen. However, its large size makes it vulnerable to
and is referred to the epigastrium. It is believed that the pain-
gunshot wounds.
transmitting fibers leave the stomach in company with the
sympathetic nerves. They pass through the celiac ganglia and
Gastric Ulcer
reach the spinal cord via the greater splanchnic nerves.
The mucous membrane of the body of the stomach and, to
Cancer of the Stomach
a lesser extent, that of the fundus produce acid and pepsin.
The secretion of the antrum and pyloric canal is mucous
Because the lymphatic vessels of the mucous membrane
and weakly alkaline (CD Fig. 19-20). The secretion of acid
and submucosa of the stomach are in continuity, it is possi-
and pepsin is controlled by two mechanisms: nervous and
ble for cancer cells to travel to different parts of the stomach,
hormonal. The vagus nerves are responsible for the nervous
some distance away from the primary site. Cancer cells also
control, and the hormone gastrin, produced by the antral
often pass through or bypass the local lymph nodes and are
mucosa, is responsible for the hormonal control. In the
held up in the regional nodes. For these reasons, malignant
surgical treatment of chronic gastric and duodenal ulcers,
disease of the stomach is treated by total gastrectomy, which
attempts are made to reduce the amount of acid secretion by
includes the removal of the lower end of the esophagus and
sectioning the vagus nerves (vagotomy) and by removing
the first part of the duodenum; the spleen and the gastros-
the gastrin-bearing area of mucosa, the antrum (partial
plenic and splenicorenal ligaments and their associated
gastrectomy).
lymph nodes; the splenic vessels; the tail and body of the
Gastric ulcers occur in the alkaline-producing mucosa
pancreas and their associated nodes; the nodes along
of the stomach, usually on or close to the lesser curvature.
the lesser curvature of the stomach; and the nodes along the
A chronic ulcer invades the muscular coats and, in time,
greater curvature, along with the greater omentum. This
involves the peritoneum so that the stomach adheres to
radical operation is a desperate attempt to remove the stom-
neighboring structures. An ulcer situated on the posterior
ach en bloc and, with it, its lymphatic field. The continuity
wall of the stomach may perforate into the lesser sac or be-
of the gut is restored by anastomosing the esophagus with
come adherent to the pancreas. Erosion of the pancreas
the jejunum.
produces pain referred to the back. The splenic artery runs
along the upper border of the pancreas, and erosion of this
Gastroscopy
artery may produce fatal hemorrhage. A penetrating ulcer
of the anterior stomach wall may result in the escape of
Gastroscopy is the viewing of the mucous membrane of the
stomach contents into the greater sac, producing diffuse
stomach through an illuminated tube fitted with a lens
peritonitis. The anterior stomach wall may, however, ad-
system. The patient is anesthetized and the gastroscope is
here to the liver, and the chronic ulcer may penetrate the
passed into the stomach, which is then inflated with air.
liver substance.
With a flexible fiberoptic instrument, direct visualization of
different parts of the gastric mucous membrane is possible.
It is also possible to perform a mucosal biopsy through a
gastroscope.
Nasogastric Intubation
Nasogastric intubation is a common procedure and is per-
formed to empty the stomach, to decompress the stomach in
cases of intestinal obstruction, or before operations on the
gastrointestinal tract; it may also be performed to obtain a
sample of gastric juice for biochemical analysis.
1. The patient is placed in the semiupright position or left
lateral position to avoid aspiration.
2. The well-lubricated tube is inserted through the wider
nostril and is directed backward along the nasal floor.
3. Once the tube has passed the soft palate and entered
CD Figure 19-20
Areas of the stomach that produce acid
the oral pharynx, decreased resistance is felt, and the
and pepsin (stippled) and alkali and gastrin (diagonal lines).
conscious patient will feel like gagging.
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
335
4. Some important distances in the adult may be useful.
the escaping fluid into the right lateral paracolic gutter and
From the nostril
(external nares) to the cardiac
thus down to the right iliac fossa. The differential diagnosis
orifice of the stomach is about 17.2 in. (44 cm), and
between a perforated duodenal ulcer and a perforated
from the cardiac orifice to the pylorus of the stomach is
appendix may be difficult.
4.8 to 5.6 in. (12 to 14 cm). The curved course taken by
An ulcer of the posterior wall of the first part of the
the tube from the cardiac orifice to the pylorus is
duodenum may penetrate the wall and erode the relatively
usually longer, 6.0 to 10.0 in. (15 to 25 cm) (see CD
large gastroduodenal artery, causing a severe hemorrhage.
Fig. 19-19).
The gastroduodenal artery is a branch of the hepatic
artery, a branch of the celiac trunk (see text Fig. 19-38).
Anatomic Structures that May Impede the
Passage of the Nasogastric Tube
Duodenal Recesses
■ Deviated nasal septum, making the passage of the tube
The importance of the duodenal recesses and the occur-
difficult on the narrower side
rence of herniae of the intestine were already alluded to in
■ Three sites of esophageal narrowing may offer resistance
this chapter.
to the nasogastric tube—at the beginning of the esopha-
gus behind the cricoid cartilage (7.2 in.; 18 cm), where
Important Duodenal Relations
the left bronchus and the arch of the aorta cross the front
The relation to the duodenum of the gallbladder, the trans-
of the esophagus (11.2 in.; 28 cm), and where the esoph-
verse colon, and the right kidney should be remembered.
agus enters the stomach (17.2 in.; 44 cm). The upper
Cases have been reported in which a large gallstone
esophageal narrowing may be overcome by gently grasp-
ulcerated through the gallbladder wall into the duodenum.
ing the wings of the thyroid cartilage and pulling the
Operations on the colon and right kidney have resulted in
larynx forward. This maneuver opens the normally
damage to the duodenum.
collapsed esophagus and permits the tube to pass down
without further delay.
Jejunum and Ileum
Anatomy of Complications
Trauma to the Jejunum and Ileum
■ The nasogastric tube enters the larynx instead of the
esophagus.
Because of its extent and position, the small intestine is
■ Rough insertion of the tube into the nose will cause nasal
commonly damaged by trauma. The extreme mobility and
bleeding from the mucous membrane.
elasticity permit the coils to move freely over one another in
■ Penetration of the wall of the esophagus or stomach.
instances of blunt trauma. Small, penetrating injuries may
Always aspirate tube for gastric contents to confirm
self-seal as a result of the mucosa plugging up the hole and the
successful entrance into stomach.
contraction of the smooth muscle wall. Material from large
wounds leaks freely into the peritoneal cavity. The presence
of the vertebral column and the prominent anterior margin of
Duodenum
the first sacral vertebra may provide a firm background for
intestinal crushing in cases of midline crush injuries.
Trauma to the Duodenum
Small-bowel contents have nearly a neutral pH and
produce only slight chemical irritation to the peritoneum.
Apart from the first inch, the duodenum is rigidly fixed to
the posterior abdominal wall by peritoneum and therefore
Recognition of the Jejunum and Ileum
cannot move away from crush injuries. In severe crush
injuries to the anterior abdominal wall, the third part of the
A physician should be able to distinguish between the large
duodenum may be severely crushed or torn against the third
and small intestine. He or she may be called on to examine
lumbar vertebra.
a case of postoperative burst abdomen, where coils of gut are
lying free in the bed. The macroscopic differences are de-
Duodenal Ulcer
scribed on text page 738.
As the stomach empties its contents into the duodenum, the
Tumors and Cysts of the Mesentery of
acid chyme is squirted against the anterolateral wall of
the Small Intestine
the first part of the duodenum. This is thought to be an
important factor in the production of a duodenal ulcer at
The line of attachment of the small intestine to the posterior
this site. An ulcer of the anterior wall of the first inch of the
abdominal wall should be remembered. It extends from a
duodenum may perforate into the upper part of the greater
point just to the left of the midline about 2 in. (5 cm) below
sac, above the transverse colon. The transverse colon directs
the transpyloric plane (L1) downward to the right iliac fossa.
336
Chapter 19
Predisposition of the Appendix
A tumor or cyst of the mesentery, when palpated through
the anterior abdominal wall, is more mobile in a direction
to Infection
at right angles to the line of attachment than along the line
of attachment.
The following factors contribute to the appendix’s predilec-
tion to infection:
Pain Fibers from the Jejunum
■ It is a long, narrow, blind-ended tube, which encourages
and Ileum
stasis of large-bowel contents.
■ It has a large amount of lymphoid tissue in its wall.
Pain fibers traverse the superior mesenteric sympathetic
■ The lumen has a tendency to become obstructed by
plexus and pass to the spinal cord via the splanchnic nerves.
hardened intestinal contents (enteroliths), which leads to
Referred pain from this segment of the gastrointestinal tract
further stagnation of its contents.
is felt in the dermatomes supplied by the ninth, tenth, and
eleventh thoracic nerves. Strangulation of a coil of small
Predisposition of the Appendix
intestine in an inguinal hernia first gives rise to pain in the
to Perforation
region of the umbilicus. Only later, when the parietal
peritoneum of the hernial sac becomes inflamed, does the
The appendix is supplied by a long small artery that does not
pain become more intense and localized to the inguinal
anastomose with other arteries. The blind end of the appen-
region (see Abdominal Pain).
dix is supplied by the terminal branches of the appendicular
artery. Inflammatory edema of the appendicular wall com-
Mesenteric Arterial Occlusion
presses the blood supply to the appendix and often leads to
thrombosis of the appendicular artery. These conditions
The superior mesenteric artery, a branch of the abdominal
commonly result in necrosis or gangrene of the appendicu-
aorta, supplies an extensive territory of the gut, from halfway
lar wall, with perforation.
down the second part of the duodenum to the left colic
Perforation of the appendix or transmigration of bacte-
flexure. Occlusion of the artery or one of its branches results
ria through the inflamed appendicular wall results in infec-
in death of all or part of this segment of the gut. The occlu-
tion of the peritoneum of the greater sac. The part that the
sion may occur as the result of an embolus, a thrombus, an
greater omentum may play in arresting the spread of the
aortic dissection, or an abdominal aneurysm.
peritoneal infection is described on CD page 329.
Mesenteric Vein Thrombosis
Pain of Appendicitis
The superior mesenteric vein, which drains the same area of
Visceral pain in the appendix is produced by distention of its
the gut supplied by the superior mesenteric artery, may
lumen or spasm of its muscle. The afferent pain fibers enter
undergo thrombosis after stasis of the venous bed. Cirrhosis
the spinal cord at the level of the tenth thoracic segment,
of the liver with portal hypertension may predispose to this
and a vague referred pain is felt in the region of the
condition.
umbilicus. Later, the pain shifts to where the inflamed
appendix irritates the parietal peritoneum. Here the pain is
Appendix
precise, severe, and localized.
Variability of Position of the Appendix
Colon and Cecum
The inconstancy of the position of the appendix should be
Colonoscopy
borne in mind when attempting to diagnose appendicitis.
A retrocecal appendix, for example, may lie behind a
Since colorectal cancer is a leading cause of death in the
cecum distended with gas, and thus it may be difficult to
Western world, colonoscopy is now being extensively used
elicit tenderness on palpation in the right iliac region.
for early detection of malignant tumors. In this procedure,
Irritation of the psoas muscle, conversely, may cause the
the mucous membrane of the colon can be directly visual-
patient to keep the right hip joint flexed.
ized through an elongated flexible tube, or endoscope.
Following a thorough washing out of the large bowel, the
Pelvic Appendix
patient is sedated, and the tube is gently inserted into the
An appendix hanging down in the pelvis may result in
anal canal. The interior of the large bowel can be observed
absent abdominal tenderness in the right lower quadrant,
from the anus to the cecum (CD Fig. 19-21). Photographs
but deep tenderness may be experienced just above the
of suspicious areas, such as polyps, can be taken and biopsy
symphysis pubis. Rectal or vaginal examination may reveal
specimens can be removed for pathologic examination.
tenderness of the peritoneum in the pelvis on the right side.
Although a relatively expensive procedure, it provides a
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
337
CD Figure 19-21
Series of the interior of the large bowel taken during a colonoscopy
procedure. A. The rectal mucosa shows a small benign polyp (arrowhead). B. The sigmoid
mucous membrane shows evidence of a mild diverticulosis. Arrowheads indicate the en-
trances into the mucosal pouches. C. The splenic flexure is normal. Note the light reflections
from the drops of mucus on the mucous membrane. D. The transverse colon shows the
characteristic normal folds or ridges (arrowheads) between the sacculations of the wall of
the colon. E. The ileocecal valve shows the upper lip (arrowheads) of the valve, which has
a normal appearance. F. Finally, the mucous membrane lining the inferior wall or floor of
the cecum looks normal. (Courtesy of M.H. Brand.)
338
Chapter 19
Cecostomy and Colostomy
more complete screening examination for colorectal cancer
than combined fecal occult blood testing and the examina-
Because of the anatomic mobility of the cecum, transverse
tion of the distal colon with sigmoidoscopy.
colon, and sigmoid colon, they may be brought to the
surface through a small opening in the anterior abdominal
Trauma of the Cecum and Colon
wall. If the cecum or transverse colon is then opened,
Blunt or penetrating injuries to the colon occur. Blunt
the bowel contents may be allowed to drain by this
injuries most commonly occur where mobile parts of the
route. These procedures are referred to as cecostomy or
colon (transverse and sigmoid) join the fixed parts (ascend-
colostomy, respectively, and are used to relieve large-bowel
ing and descending).
obstructions.
Penetrating injuries following stab wounds are common.
Volvulus
The multiple anatomic relationships of the different parts of
the colon explain why isolated colonic trauma is unusual.
Because of its extreme mobility, the sigmoid colon some-
times rotates around its mesentery. This may correct itself
Cancer of the Large Bowel
spontaneously or the rotation may continue until the blood
Cancer of the large bowel is relatively common in persons
supply of the gut is cut off completely.
older than 50 years. The growth is restricted to the bowel
Intussusception
wall for a considerable time before it spreads via the
lymphatics. Bloodstream spread via the portal circulation to
Intussusception is the telescoping of a proximal segment of
the liver occurs late. If a diagnosis is made early and a partial
the bowel into the lumen of an adjoining distal segment.
colectomy is performed, accompanied by removal of the
Needless to say, there is a grave risk of cutting off the blood
lymph vessels and lymph nodes draining the area, then a
supply to the gut and developing gangrene. It is common in
cure can be anticipated.
children. Ileocolic, colocolic, and ileoileal forms do occur,
but ileocolic is the most common.
Diverticulosis
The high incidence in children may be caused by the
Diverticulosis of the colon is a common clinical condition.
relatively large size of the large bowel compared with
It consists of a herniation of the lining mucosa through the
the small intestine at this time of life. Another factor may be
circular muscle between the teniae coli and occurs at points
the possible swelling of Peyer’s patches secondary to infec-
where the circular muscle is weakest—that is, where the
tion. In the latter case, the swollen patch protrudes into the
blood vessels pierce the muscle (CD Fig. 19-22). The com-
lumen and violent peristalsis of the ileal wall tries to pass it
mon site for herniation is shown in CD Fig. 19-22.
distally along the gut lumen.
teniae coli
appendices epiploicae
colic artery
diverticulum
CD Figure 19-22
Blood supply to the
colon (A) and formation of the diverticu-
marginal
lum (B). Note the passage of the mucosal
artery
diverticulum through the muscle coat
A
B
along the course of the artery.
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
339
■ The sigmoidoscope is gently inserted into the anus and
Sigmoid Colon
anal canal in the direction of the umbilicus to ensure that
the instrument passes along the long axis of the canal.
Variation in the Length and Location
Gentle but firm pressure is applied to overcome the re-
of the Sigmoid Colon
sistance of the anal sphincters (see text Fig. 19-68).
■ After a distance of about 1.5 in. (4 cm), the instrument
The sigmoid colon shows great variation in length and may
enters the ampulla of the rectum. At this point, the tip of
measure as much as 36 in. (91 cm). In the young child,
the sigmoidoscope should be directed posteriorly in the
because the pelvis is small, this segment of the colon may lie
midline to follow the sacral curve of the rectum (see CD
mainly in the abdomen.
Fig. 19-23).
■ Slow advancement is made under direct vision. Some
Cancer of the Sigmoid Colon
slight side-to-side movement may be necessary to bypass
The sigmoid colon is a common site for cancer of the large
the transverse rectal folds.
bowel. Because the lymphatic vessels of this segment of the
■ At approximately 6.5 in. (16.25 cm) from the anal mar-
colon drain ultimately into the inferior mesenteric nodes, it
gin, the rectosigmoid junction will be reached. The sig-
follows that an extensive resection of the gut and its associated
moid colon here bends forward and to the left, and the
lymphatic field is necessary to extirpate the growth and its lo-
lumen appears to end in a blind cul-de-sac. To negotiate
cal lymphatic metastases. The colon is removed from the left
this angulation, the tip of the sigmoidoscope must be
colic flexure to the distal end of the sigmoid colon, and the
directed anteriorly and to the patient’s left side. This
transverse colon is anastomosed to the rectum.
maneuver can cause some discomfort in the anal canal
from distortion of the anal sphincters by the shaft of the
Volvulus
sigmoidoscope. Another possibility is that the point of
the instrument may stretch the wall of the colon, giving
Because of its extreme mobility, the sigmoid colon some-
rise to colicky pain in the lower abdomen.
times rotates around its mesentery. This may correct itself
■ Once the instrument has entered the sigmoid colon, it
spontaneously, or the rotation may continue until the blood
should be possible to pass it smoothly along its full extent
supply of the gut is cut off completely. The rotation com-
and, using the full length of the sigmoidoscope, enter the
monly occurs in a counterclockwise direction and is
descending colon.
referred to as volvulus.
■ The sigmoidoscope may now be slowly withdrawn, care-
fully inspecting the mucous membrane. The normal
Diverticula
rectal and colonic mucous membrane is smooth and
Diverticula of the mucous membrane along the course of
glistening and pale pink with an orange tinge, and blood
the arteries supplying the sigmoid colon is a common clini-
vessels in the submucosa can be clearly seen. The mu-
cal condition and is described on page 338. In patients with
cous membrane is supple and moves easily over the end
diverticulitis or ulcerative colitis, the sigmoid colon may
of the sigmoidoscope.
become adherent to the bladder, rectum, ileum, or ureter
Anatomy of Complications
and produce an internal fistula.
of Sigmoidoscopy
Sigmoidoscopy
Perforation of the bowel at the rectosigmoid junction can
Because the sigmoid colon lies only a short distance from
occur. This is almost invariably caused by the operator fail-
the anus (6.5 in. [17 cm]) it is possible to examine the
ing to negotiate carefully the curve between the rectum and
mucous membrane under direct vision for pathologic
the sigmoid colon. In some patients, the curve is in the form
conditions. A flexible tube fitted with lenses and illuminated
of an acute angulation, which may frustrate the overzealous
internally is introduced through the anus and carefully
advancement of the sigmoidoscope. Perforation of the sig-
passed up through the anal canal, rectum, sigmoid colon,
moid colon results in the escape of colonic contents into the
and descending colon. This examination, called sigmoi-
peritoneal cavity.
doscopy, can be carried out without an anesthetic in an out-
patient clinic. Biopsy specimens of the mucous membrane
Colostomy
can be obtained through this instrument.
The sigmoid colon is often selected as a site for performing
a colostomy in patients with carcinoma of the rectum. Its
Anatomic Facts Relative to Sigmoidoscopy
mobility allows the surgeon to bring out a loop of colon,
■ The patient is placed in the left lateral position with
with its blood supply intact, through a small incision in the
the left knee flexed and the right knee extended (CD
left iliac region of the anterior abdominal wall. Its mobility
Fig. 19-23). Alternatively, the patient is placed kneeling
also makes it suitable for implantation of the ureters after
in the knee-chest position.
surgical removal of the bladder.
340
Chapter 19
umbilicus
sigmoid
colon
A
S1
S2
S3
area of
referred
discomfort or
pain as instrument
enters sigmoid
6.5 in.
colon
1 1/2
inches
1
3
2
B
CD Figure 19-23
Sigmoidoscopy. A. Patient in the left lateral position with the left knee
flexed and the right knee extended. B. Sagittal section of the male pelvis showing the
positions (1, 2, and 3) of the tube of the sigmoidoscope relative to the patient as it ascends
the anal canal and rectum. The area of discomfort or pain experienced by the patient as the
tube is negotiated around the bend into the sigmoid colon is referred to the skin of the
anterior abdominal wall below the umbilicus.
branch divides into an anterior and a posterior branch. The
Rectum
tributaries of the superior rectal vein are arranged in a simi-
lar manner, so that it is not surprising to find that internal he-
Rectal Curves and Mucosal Folds
morrhoids are arranged in three groups (see CD p. 341): two
on the right side of the lower rectum and anal canal and one
The anteroposterior flexure of the rectum, as it follows the
on the left.
curvature of the sacrum and coccyx, and the lateral flexures
must be remembered when one is passing a sigmoidoscope
Partial and Complete Prolapse of
to avoid causing the patient unnecessary discomfort.
the Rectum
The crescentic transverse mucosal folds of the rectum
must also be borne in mind when passing an instrument
Partial and complete prolapses of the rectum through the
into the rectum. It is thought that these folds serve to support
anus are relatively common clinical conditions. In partial
the weight of the feces and to prevent excessive distension of
prolapse, the rectal mucous membrane and submucous
the rectal ampulla.
coat protrude for a short distance outside the anus (CD Fig.
19-24). In complete prolapse, the whole thickness of the
Blood Supply and Internal
rectal wall protrudes through the anus. In both conditions,
Hemorrhoids
many causative factors may be involved. However, damage
The chief arterial supply to the rectum is from the superior
to the levatores ani muscles as the result of childbirth and
rectal artery, a continuation of the inferior mesenteric artery.
poor muscle tone in the aged are important contributing
In front of the third sacral vertebra, the artery divides into
factors. A complete rectal prolapse may be regarded as a
right and left branches. Halfway down the rectum, the right
sliding hernia through the pelvic diaphragm.
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
341
involve the ureter. An anterior penetration in the male may
mucous membrane
peritoneum
involve the prostate, seminal vesicles, or bladder; in the
female, the vagina and uterus may be invaded.
levator ani
It is clear from the anatomic features of the rectum and
rectum
its lymph drainage that a wide resection of the rectum with
its lymphatic field offers the best chance of cure. When the
tumor has spread to contiguous organs and is of a low
internal anal
sphincter
grade of malignancy, some form of pelvic evisceration may
be justifiable.
external anal
It is most important for a medical student to remember
sphincter
that the interior of the lower part of the rectum can be exam-
ined by a gloved index finger introduced through the anal
canal. The anal canal is about 1.5 in. (4 cm) long so that the
anus
pulp of the index finger can easily feel the mucous membrane
prolapse
lining the lower end of the rectum. Most cancers of the rec-
of mucous
tum can be diagnosed by this means. This examination can
A
membrane
be extended in both sexes by placing the other hand on the
lower part of the anterior abdominal wall. With the bladder
empty, the anterior rectal wall can be examined bimanually.
rectum
In the female, the placing of one finger in the vagina and an-
other in the rectum may enable the physician to make a thor-
ough examination of the lower part of the anterior rectal wall.
external anal
sphincter
Rectal Injuries
The management of penetrating rectal injuries will be de-
termined by the site of penetration relative to the peritoneal
covering. The upper third of the rectum is covered on the
peritoneum
anterior and lateral surfaces by peritoneum, the middle
internal anal
sphincter
third is covered only on its anterior surface, and the lower
third is devoid of a peritoneal covering (CD Fig. 19-25). The
complete
prolapse
treatment of penetration of the intraperitoneal portion of the
B
of rectal wall
rectum is identical to that of the colon, because the peri-
toneal cavity has been violated. In the case of penetration of
CD Figure 19-24
Coronal section of the rectum and anal
canal. A. Incomplete rectal (mucosal) prolapse. B. Complete
the extraperitoneal portion, the rectum is treated by divert-
rectal prolapse.
ing the feces through a temporary abdominal colostomy,
administering antibiotics, and repairing and draining the
tissue in front of the sacrum.
Cancer of the Rectum
Cancer (carcinoma) of the rectum is a common clinical
Anal Canal
finding that remains localized to the rectal wall for a
considerable time. At first, it tends to spread locally in the
Internal Hemorrhoids (Piles)
lymphatics around the circumference of the bowel. Later, it
spreads upward and laterally along the lymph vessels,
Internal hemorrhoids are varicosities of the tributaries of the
following the superior rectal and middle rectal arteries.
superior rectal (hemorrhoidal) vein and are covered by
Venous spread occurs late, and because the superior rectal
mucous membranes (CD Fig. 19-26). The tributaries of the
vein is a tributary of the portal vein, the liver is a common
vein, which lie in the anal columns at the 3, 7, and 11 o’-
site for secondary deposits.
clock positions when the patient is viewed in the lithotomy
Once the malignant tumor has extended beyond the
position,* are particularly liable to become varicosed.
confines of the rectal wall, knowledge of the anatomic rela-
Anatomically, a hemorrhoid is therefore a fold of mucous
tions of the rectum will enable a physician to assess the
structures and organs likely to be involved. In both sexes,
a posterior penetration involves the sacral plexus and
*The patient is in the supine position with both hip joints flexed
can cause severe intractable pain down the leg in the distri-
and abducted; the feet are held in position by stirrups. The position
bution of the sciatic nerve. A lateral penetration may
is commonly used for pelvic examinations of the female.
342
Chapter 19
sigmoid colon
coil of ileum
S3
peritoneum
rectouterine pouch
cavity of uterus
uterovesical pouch
rectum
bladder
anococcygeal body
cervix
anal canal
anus
urogenital diaphragm
urethra
vagina
perineal body
CD Figure 19-25
Sagittal section of the female pelvis.
membrane and submucosa containing a varicosed tributary
muscular coat of the rectal wall during defecation. Chronic
of the superior rectal vein and a terminal branch of the su-
constipation, associated with prolonged straining at stool, is
perior rectal artery. Internal hemorrhoids are initially con-
a common predisposing factor. Pregnancy hemorrhoids are
tained within the anal canal (first degree). As they enlarge,
common owing to pressure on the superior rectal veins by
they extrude from the canal on defecation but return at the
the gravid uterus. Portal hypertension as a result of cirrhosis
end of the act (second degree). With further elongation,
of the liver can also cause hemorrhoids. The possibility that
they prolapse on defecation and remain outside the anus
cancerous tumors of the rectum are blocking the superior
(third degree).
rectal vein must never be overlooked.
Because internal hemorrhoids occur in the upper half
of the anal canal, where the mucous membrane is inner-
External Hemorrhoids
vated by autonomic afferent nerves, they are painless and
are sensitive only to stretch. This may explain why large in-
External hemorrhoids are varicosities of the tributaries of
ternal hemorrhoids give rise to an aching sensation rather
the inferior rectal (hemorrhoidal) vein as they run laterally
than acute pain.
from the anal margin. They are covered by skin (see
The causes of internal hemorrhoids are many. They fre-
CD Fig. 19-26) and are commonly associated with well-
quently occur in members of the same family, which sug-
established internal hemorrhoids.
gests a congenital weakness of the vein walls. Varicose veins
External hemorrhoids are covered by the mucous
of the legs and hemorrhoids often go together. The superior
membrane of the lower half of the anal canal or the skin,
rectal vein is the most dependent part of the portal circula-
and they are innervated by the inferior rectal nerves. They
tion and is valveless. The weight of the column of venous
are sensitive to pain, temperature, touch, and pressure,
blood is thus greatest in the veins in the upper half of the
which explains why external hemorrhoids tend to be
anal canal. Here, the loose connective tissue of the submu-
painful. Thrombosis of an external hemorrhoid is common.
cosa gives little support to the walls of the veins. Moreover,
Its cause is unknown, although coughing or straining may
the venous return is interrupted by the contraction of the
produce distension of the hemorrhoid followed by stasis.
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
343
tributary of superior rectal vein
internal anal sphincter
external anal sphincter
anal columns
inferior
rectal vein
internal hemorrhoid
mucous membrane
skin
external hemorrhoid
perianal hematoma
A
anal valves
B
11 o'clock
3 o'clock
7 o'clock
C
CD Figure 19-26
A. Normal tributary of the superior rectal vein within the anal column.
B. Varicosed tributary of the superior rectal vein forming the internal hemorrhoid. Dotted
lines indicate degrees of severity of condition. C. Positions of three internal hemorrhoids as
seen through a proctoscope with the patient in the lithotomy position.
The presence of a small, acutely tender swelling at the anal
Anal Fissure
margin is immediately recognized by the patient.
The lower ends of the anal columns are connected by
small folds called anal valves (CD Fig. 19-26A). In people
Perianal Hematoma
suffering from chronic constipation, the anal valves may be
A perianal hematoma is a small collection of blood beneath
torn down to the anus as the result of the edge of the fecal
the perianal skin (see CD Fig. 19-26). It is caused by a
mass catching on the fold of mucous membrane. The
rupture of a small subcutaneous vein, possibly an external
elongated ulcer so formed, known as an anal fissure (CD
hemorrhoid, and is extremely painful.
Fig. 19-27), is extremely painful. The fissure occurs most
344
Chapter 19
rectum
levator ani
anal columns
external anal sphincter
anal fissure
anal valves
A
pelvirectal abscess
submucous abscess
ischiorectal abscess
subcutaneous abscess
B
pelvirectal abscess
fistulae
CD Figure 19-27
A. Tearing down-
ward of the anal valve to form an anal
fissure. B. Common locations of peri-
anal abscesses. C. Common positions
C
of perianal fistulae.
commonly in the midline posteriorly or, less commonly,
The site of the anal fissure in the sensitive lower half of
anteriorly, and this may be caused by the lack of support
the anal canal, which is innervated by the inferior
provided by the superficial part of the external sphincter
rectal nerve, results in reflex spasm of the external anal
in these areas. (The superficial part of the external sphinc-
sphincter, aggravating the condition. Because of the intense
ter does not encircle the anal canal, but sweeps past its
pain, anal fissures may have to be examined under local
lateral sides.)
anesthesia.
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
345
Perianal Abscesses
Anal Sphincter Nerve Block and
Anesthetizing the Perianal Skin
Perianal abscesses are produced by fecal trauma to the anal
mucosa (see CD Fig. 19-27). Infection may gain entrance to
By blocking the branches of the inferior rectal nerve and
the submucosa through a small mucosal lesion, or the ab-
the perineal branch of the fourth sacral nerve, the anal
scess may complicate an anal fissure or the infection of an
sphincters will be relaxed and the perianal skin anes-
anal mucosal gland. The abscess may be localized to the
thetized.
submucosa (submucous abscess), may occur beneath the
The procedure is as follows:
perianal skin (subcutaneous abscess), or may occupy the is-
1. An intradermal wheal is produced by injecting a small
chiorectal fossa (ischiorectal abscess). Large ischiorectal ab-
amount of anesthetic solution behind the anus in the
scesses sometimes extend posteriorly around the side of the
midline.
anal canal to invade the ischiorectal fossa of the opposite
2. A gloved index finger is inserted into the anal canal to
side (horseshoe abscess). An abscess may be found in the
serve as a guide.
space between the ampulla of the rectum and the upper sur-
3. A long needle attached to a syringe filled with
face of the levator ani (pelvirectal abscess). Anatomically,
anesthetic solution is inserted through the cuta-
these abscesses are closely related to the different parts of the
neous wheal into the sphincter muscles along the
external sphincter and levator ani muscles, as seen in CD
posterior and lateral surfaces of the anal canal. The
Fig. 19-27.
procedure is repeated on the opposite side. The pur-
Anal fistulae develop as the result of spread or inade-
pose of the finger in the anal canal is to guide the
quate treatment of anal abscesses. The fistula opens at one
needle and to prevent penetration of the anal mucous
end at the lumen of the anal canal or lower rectum and at
membrane.
the other end on the skin surface close to the anus (see CD
Fig. 19-27). If the abscess opens onto only one surface, it is
known as a sinus, not a fistula. The high-level fistulae are
Incontinence Associated with
rare and run from the rectum to the perianal skin. They are
Rectal Prolapse
located above the anorectal ring; as a result, fecal material
constantly soils the clothes. The low-level fistulae occur
Fecal incontinence can accompany severe rectal prolapse
below the level of the anorectal ring, as shown in CD
of long duration. It is thought that the prolonged and
Fig. 19-27.
excessive stretching of the anal sphincters is the cause of
The most important part of the sphincteric mechanism
the condition. The condition can be treated by restoring
of the anal canal is the anorectal ring. It consists of the deep
the anorectal angle by tightening the puborectalis part of the
part of the external sphincter, the internal sphincter, and the
levator ani muscles and the external anal sphincters behind
puborectalis part of the levator ani. Surgical operations on
the anorectal junction.
the anal canal that result in damage to the anorectal ring
will produce fecal incontinence.
Incontinence after Trauma
Removal of Anorectal Foreign Bodies
Trauma, such as childbirth, or damage to the sphincters
during surgery or perianal abscesses or fistulae can be
Normally, the anal canal is kept closed by the tone of the
responsible for incontinence after trauma.
internal and external anal sphincters and the tone of the
puborectalis part of the levator ani muscles. The rectal
contents are supported by the levator ani muscles, possibly
Incontinence after Spinal Cord Injury
assisted by the transverse rectal mucosal folds. For these
After severe spinal cord injuries, the patient is not aware
reasons, the removal of a large foreign body, such as a vase
of rectal distension. Moreover, the parasympathetic
or electric light bulb, from the rectum may be a formida-
influence on the peristaltic activity of the descending
ble problem.
colon, sigmoid colon, and rectum is lost. In addition,
The following procedure is usually successful:
control over the abdominal musculature and sphincters
1. The foreign body must first be fixed so that the sphinc-
of the anal canal may be severely impaired. The rectum,
teric tone, together with external attempts to grab the
now an isolated structure, responds by contracting
object, do not displace the object farther up the
when the pressure within its lumen rises. This local re-
rectum.
flex response is much more efficient if the sacral segments
2. Large, irregular, or fragile foreign bodies may not be re-
of the spinal cord are spared. At best, however, the force
moved so easily, and it may be necessary to paralyze the
of the contractions of the rectal wall is small, and
anal sphincter by giving the patient a general anesthetic
constipation and impaction of feces are the usual
or by performing an anal sphincter nerve block.
outcome.
346
Chapter 19
Rectal Examination
■ Opposite the proximal phalanx are the perineal body,
the urogenital diaphragm, and the bulb of the penis.
The following structures can be palpated by the gloved in-
dex finger inserted into the anal canal and rectum in the
In the female:
normal patient.
■ Opposite the terminal phalanx are the rectouterine
Anteriorly
pouch, the vagina, and the cervix (CD Fig. 19-25).
In the male:
■ Opposite the middle phalanx are the urogenital di-
aphragm and the vagina.
■ Opposite the terminal phalanx are the contents of the
■ Opposite the proximal phalanx are the perineal body
rectovesical pouch, the posterior surface of the bladder,
and the lower part of the vagina.
the seminal vesicles, and the vasa deferentia (CD Fig.
19-28).
Posteriorly
■ Opposite the middle phalanx are the rectoprostatic
The sacrum, coccyx, and anococcygeal body can be felt.
fascia and the prostate.
Laterally
seminal vesicle
bladder
prostate
external os of uterus
A
B
head of baby
anterior lip of cervix
CD Figure 19-28
A. Rectal ex-
amination in a pregnant woman
showing how it is possible to
palpate the cervix through the
anterior rectal wall. B. Rectal ex-
amination in the male showing
how it is possible to palpate the
prostate and the seminal vesicles
through the anterior rectal wall.
site for episiotomy
C. Position of the episiotomy inci-
sion in a woman during the sec-
ond stage of labor. The baby’s
head is presenting at the vaginal
C
orifice.
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
347
The ischiorectal fossae and ischial spines can be
palpated.
Congenital Short Esophagus
Abnormal shortness of the esophagus is caused by an
Cancer and the Lymph Drainage of the
esophageal hiatus hernia in the diaphragm. Stomach con-
Anal Canal
tents flow into the esophagus, resulting in esophagitis.
The upper half of the mucous membrane of the anal canal
is drained upward to lymph nodes along the course of the
superior rectal artery. The lower half of the mucous
CONGENITAL
membrane is drained downward to the medial group of
superficial inguinal nodes. Many patients have thought they
ANOMALIES OF
had an inguinal hernia, and the physician has found a
cancer of the lower half of the anal canal, with secondary
deposits in the inguinal lymph nodes.
THE STOMACH
Congenital Hypertrophic
ISCHIORECTAL
Pyloric Stenosis
FOSSA
Hypertrophic pyloric stenosis is a relatively common emer-
gency in infants between the ages of 3 and 6 weeks. The
child ejects the stomach contents with considerable force.
The Ischiorectal Fossa
The exact cause of the stenosis is unknown, although
evidence suggests that the number of autonomic ganglion
and Infection
cells in the stomach wall is fewer than normal. This
The ischiorectal fossae (ischioanal fossae) are filled with fat
possibility leads to prenatal neuromuscular incoordination
that is poorly vascularized. The close proximity to the anal
and localized muscular hypertrophy and hyperplasia of
canal makes them particularly vulnerable to infection.
the pyloric sphincter. It is much more common in male
Infection commonly tracks laterally from the anal mucosa
children.
through the external anal sphincter. Infection of the peri-
anal hair follicles or sweat glands may also be the cause of
infection in the fossae. Rarely, a perirectal abscess bursts
CONGENITAL
downward through the levator ani muscle. An ischiorectal
abscess may involve the opposite fossa by the spread of in-
fection across the midline behind the anal canal.
ANOMALIES OF
THE SMALL AND
CONGENITAL
LARGE INTESTINES
ANOMALIES OF
THE ESOPHAGUS
Diverticula of the Intestine
All coats of the intestinal wall are found in the wall of a con-
genital diverticulum. In the duodenum, diverticula are
Atresia of the Esophagus
found on the medial wall of the second and third parts (CD
Atresia of the esophagus, with and without fistula, with the
Fig. 19-29). Usually, these are symptomless. Jejunal diver-
trachea is considered in detail on CD Chapter 3.
ticula occasionally occur and usually give rise to no symp-
toms. For Meckel’s diverticulum of the ileum, see CD page
327. A diverticulum of the cecum is commonly situated on
Esophageal Stenosis
the medial side of the cecum close to the ileocecal valve. It
Esophageal stenosis is a narrowing of the lumen of the
may be subject to acute inflammation and then is confused
esophagus, which commonly occurs in the lower part. It is
with appendicitis. Diverticula of the colon are acquired, not
treated by dilatation.
congenital (see CD p. 338).
348
Chapter 19
1
2
3
4
5
6
CD Figure 19-29
Some common congen-
ital anomalies of the intestinal tract.
1-3. Congenital atresias of the small intes-
tine. 4. Diverticulum of the duodenum or
jejunum. 5. Mesenteric cyst of the small in-
testine. 6. Absence of the appendix. 7. Dou-
ble appendix. 8. Malrotation of the gut, with
the appendix lying in the left iliac fossa. For
7
8
Meckel’s diverticulum, see CD Fig. 19-15.
obstruction occurs at multiple sites. The cause is possibly
Atresia and Stenosis of the
the failure of the lumen to become recanalized after it has
been blocked by epithelial proliferation of the cells of the
Small Intestine
mucous membrane. Other causes have been suggested,
such as vascular damage associated with twisting or volvulus
The most common site of an atretic or stenotic obstruction
of the intestine. Persistent bile-stained vomiting occurs from
is in the duodenum. During the development of the
birth. Surgical relief of the obstruction should be carried out
duodenum, the lining cells proliferate at such a rate that the
as soon as possible.
lumen becomes completely obliterated. Later, as a result of
degeneration of these cells, the gut becomes recanalized.
Failure of recanalization could produce atresia or stenosis.
Duplication of the Digestive System
Different forms of duodenal atresia and stenosis are shown
in CD Fig. 19-29. Vomiting is the most common presenting
In duplication of the digestive system, the normal degener-
symptom, and the vomitus usually is bile stained. Surgical
ation of the mucous membrane cells, which have prolifer-
treatment during the first few days of life is essential.
ated to temporarily block the lumen, occurs at two sites
The next most common sites are the ileum and je-
simultaneously instead of at one. In this way, two lumina are
junum, respectively (see CD Fig. 19-29). Frequently, the
formed side by side. The additional segment of bowel
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
349
should be removed as soon as possible, since it may cause
2% of individuals. The diverticulum is important clinically,
obstruction or be the site of hemorrhage or perforation.
since it may possess a small area of gastric mucosa, and
bleeding may occur from a “gastric” ulcer in its mucous
membrane. Moreover, the pain from this ulcer may be con-
Arrested Rotation or Malrotation
fused with the pain from appendicitis. Should a fibrous
band connect the diverticulum to the umbilicus, a loop of
of the Midgut Loop
small bowel may become wrapped around it, causing in-
testinal obstruction.
Complete Absence of Rotation or
Undescended Cecum and Appendix
Incomplete Rotation
In cases of undescended cecum and appendix, an inflam-
Complete absence of rotation is rare. In cases of incomplete
mation of the appendix would give rise to tenderness in the
rotation, no further rotation occurs after the initial counter-
right hypochondrium, which may lead to a mistaken diag-
clockwise rotation of 90° in the umbilical cord. Thus, the
nosis of inflammation of the gallbladder.
duodenum, jejunum, and ileum remain on the right side of
the abdomen, and the cecum and colon are on the left side
of the abdomen (see CD Fig. 19-29). In other cases, a coun-
Anomalies of the Appendix
terclockwise rotation of 180° occurs, and although the duo-
Agenesis of the appendix (failure to develop) is extremely
denum may take up its correct position posterior to the
rare; however, a few examples of double appendix have
superior mesenteric artery, the cecum comes to lie anterior
been reported (see CD Fig. 19-29). The possibility of left-
and to the left of the duodenum. Abnormal adhesions form,
sided appendix in individuals with transposition of thoracic
which run across the anterior surface of the duodenum and
and abdominal viscera or in cases of arrested rotation of
cause obstruction to its second part.
the midgut should always be remembered (see CD Fig.
19-29).
Malrotation of the Midgut Loop
Anomalies of the Colon
Counterclockwise rotation of 90° followed by clockwise ro-
tation of 90° or 180° may occur. In these cases, the duode-
The congenital anomaly of undescended cecum or failure
num comes to lie anterior to the superior mesenteric artery,
of rotation of the gut so that the cecum lies in the left iliac
and the colon may come to lie anterior to the mesentery of
fossa may give rise to confusion in diagnosis. The pain of ap-
the small intestine. Repeated vomiting is usually the pre-
pendicitis, for example, although initially starting in the um-
senting symptom and is caused by duodenal obstruction.
bilical region, may shift not to the right iliac fossa but to the
Surgical correction of the incomplete rotation or malrota-
right upper quadrant or to the left lower quadrant.
tion of the gut is performed, and all adhesions are divided.
Primary Megacolon
Persistence of the
(Hirschsprung Disease)
Vitellointestinal Duct
Hirschsprung disease shows a familial tendency and is more
The vitelline duct in the early embryo connects the devel-
common in males than in females. Symptoms usually appear
oping gut to the yolk sac (see text Fig. 19-78). Normally, as
during the first few days after birth. The child fails to pass
development proceeds, the duct is obliterated, severs its con-
meconium, and the abdomen becomes enormously dis-
nection with the intestine, and disappears. Persistence of the
tended. The sigmoid colon is greatly distended and hyper-
vitellointestinal duct can result in an umbilical fistula (see
trophied, while the rectum and anal canal are constricted
CD Fig. 19-15). If the duct remains as a fibrous band, a loop
(CD Fig. 19-30). It is the constricted segment of the bowel
of small intestine can become wrapped around it, causing
that causes the obstruction, and histologic examination re-
intestinal obstruction (see CD Fig. 19-15).
veals a complete failure of development of the parasympa-
thetic ganglion cells in this region. The treatment is opera-
tive excision of the aganglionic segment of the bowel.
Meckel’s Diverticulum
Meckel’s diverticulum, a congenital anomaly, represents a
Imperforate Anus
persistent portion of the vitellointestinal duct (see CD Fig.
19-15). The diverticulum is located on the antimesenteric
About 1 child in 4,000 is born with imperforate anus caused
border of the ileum about 2 ft (61 cm) from the ileocecal
by an imperfect fusion of the entodermal cloaca with the
junction. It is about 2 in. (5 cm) long and occurs in about
proctodeum (see text Fig. 19-77).
350
Chapter 19
distended and hypertrophied
sigmoid colon
constricted rectum
and anal canal
commonest area to find absence
of parasympathetic
ganglion cells
CD Figure 19-30
Main characteristics of primary megacolon (Hirschsprung disease).
Clinical Problem Solving Questions
Read the following case histories/questions and give
his perineum, scrotum, and penis. He was unable to
the best answer for each.
urinate normally, passing only a few drops of blood-
stained urine. The lower part of the anterior abdominal
An 8-year-old boy was admitted to the hospital with a tem-
wall was also swollen, but his thighs were normal.
perature of 101°F, a furred tongue, and pain in the right
2. The symptoms and signs displayed by this patient can
lower quadrant. On examination, the skin on the right
be explained by the following statements except which?
lower quadrant was tender to the touch, and the abdominal
A. The patient’s fall ruptured the urethra in the per-
muscles were contracted and rigid. A diagnosis of acute ap-
ineum.
pendicitis was made.
B. When the patient attempted to micturate, the urine
1. The symptoms and signs displayed by this patient can
extravasated beneath Colles’ fascia.
be explained by the following statements except which?
C. The urine passed over the scrotum and penis under
A. An acutely inflamed appendix produces an inflam-
the membranous layer of superficial fascia.
mation of the peritoneal coat covering it.
D. The urine passed upward beneath the membranous
B. Should the inflammatory process spread, for exam-
layer of superficial fascia on the anterior abdominal
ple, if the appendix should rupture, the parietal peri-
wall.
toneum would become involved.
E. The urine could not extend posteriorly because of the
C. The parietal peritoneum, the abdominal muscles,
attachment of Colles’ fascia to the tip of the coccyx.
and the overlying skin are supplied by the same seg-
F. The urine did not extend into the thigh because of
mental spinal nerves.
the attachment of the membranous layer of superfi-
D. The segmental nerves supplying the right lower
cial fascia to the fascia lata, just below the inguinal
quadrant of the abdominal wall are T7, T8, and T9.
ligament.
E. The pain in the right lower quadrant and the re-
A 45-year-old woman was shopping in a liquor store when
gional contraction of the abdominal muscles is an
an armed robbery took place. A shootout occurred and a
attempt by the body to keep the inflamed appendix
bullet ricocheted off the wall and entered her left side. For-
immobile so that the inflammatory process remains
tunately, the bullet did not enter the peritoneal cavity.
localized.
One year later, in addition to diminished skin sensation
A workman engaged in demolishing a building lost his
over the left lumbar region and umbilicus, she noticed a
balance and fell astride a girder on the floor below. On
bulging forward of the left side of her anterior abdominal
examination, he was found to have extensive swelling of
wall.
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
351
3. The symptoms and signs displayed by this patient can
6. The symptoms and signs displayed by this patient can
be explained by the following statements except which?
be explained by the following statements except which?
A. The bullet cut the ninth and tenth intercostal nerves
A. The excessive exertion caused a rise in intraabdom-
just below the costal margin on the left side.
inal pressure.
B. The diminished skin sensation was caused by the
B. A hernial sac formed of parietal peritoneum was
loss of the sensory nerve supply to the ninth and
forced downward.
tenth thoracic dermatomes.
C. The peritoneum was forced through the right
C. Portions of the oblique, transversus, and rectus
femoral canal.
abdominis muscles on the left side were paralyzed.
D. The patient had a right-sided femoral hernia.
D. Atrophy of the pyramidalis muscle resulted in loss of
E. The neck of a femoral hernial sac is situated below
support to the abdominal viscera, which then sagged
and medial to the pubic tubercle.
forward.
A 55-year-old man was admitted to the hospital with a large
A 9-week-old boy was admitted to the hospital with a
hard, fixed, intraabdominal mass. On examination of the ab-
swelling in the right groin that extended down into the up-
domen, the mass was situated on the transpyloric plane. The
per part of the scrotum. When he cried, the swelling en-
inguinal lymph nodes were normal.
larged. On careful palpation it was possible to reduce the
7. The symptoms and signs displayed by this patient can
size of the swelling, and this procedure was accompanied by
be explained by the following statements except which?
a gurgling noise.
A. Radiologic examination of the stomach showed
4. The symptoms and signs displayed by this patient can
nothing abnormal.
be explained by the following statements except which?
B. The right testicle was enlarged and was much
A. The swelling was situated above and medial to the
harder than normal.
pubic tubercle on the right side.
C. A diagnosis of malignant disease of the right testis
B. The child had a right indirect inguinal hernia.
was made.
C. The processus vaginalis in its upper part had failed
D. The malignant tumor had metastasized to the lum-
to become obliterated before birth.
bar lymph nodes lying on the transpyloric plane on
D. The hernial sac in an indirect inguinal hernia
the posterior abdominal wall, which is the normal
emerges from the superficial inguinal ring.
lymphatic drainage of the testis.
E. The superficial inguinal ring lies above and medial
E. In malignant disease of the testis the superficial
to the pubic tubercle.
inguinal lymph nodes only become involved if the
F. The contents of the hernial sac consisted only of the
tumor spreads to involve the scrotal skin.
greater omentum.
F. The normal testis is tethered to the skin of the
scrotum.
A 75-year-old man with chronic bronchitis noticed that a
bulge was developing in his left groin. On examination, an
A 25-year-old man involved in purchasing drugs was knifed
elongated swelling was seen above the medial end of the left
in the abdomen in the left upper quadrant. On examination
inguinal ligament. When the patient coughed, the swelling
in the emergency department, it was difficult to determine
enlarged but did not descend into the scrotum. The patient
whether the knife had penetrated the peritoneal cavity. It
had weak abdominal muscles.
was decided to do a midline peritoneal lavage below the
umbilicus to see if there was any free blood in the peritoneal
5. The symptoms and signs displayed by this patient can
cavity.
be explained by the following statements except which?
A. The inguinal swelling was a direct inguinal hernia.
8. The following layers of tissue were penetrated by the
B. The cause of the hernia was weak abdominal
trocar and cannula to enter the peritoneal cavity except
muscles.
which?
C. The hernial sac was wide and in direct communica-
A. Skin
tion with the peritoneal cavity.
B. Fatty and membranous layers of superficial fascia
D. A rise in intraabdominal pressure on coughing
C. Rectus sheath and rectus abdominis muscle
caused the hernial swelling to expand.
D. Deep fascia
E. The swelling occured lateral to the inferior epigas-
E. Fascia transversalis
tric artery.
F. Extraperitoneal tissue and parietal peritoneum
A 40-year-old woman noticed a painful swelling in her right
A 45-year-old man was admitted to the emergency
groin after helping her husband move some heavy furniture.
department complaining of severe pain in the right lower
On examination, a small tender swelling was noted in the
quadrant of the anterior abdominal wall. He had repeatedly
right groin.
vomited, and his temperature and pulse rate were elevated.
352
Chapter 19
His history indicated that he had acute appendicitis and that
E. The lesser sac of peritoneum
the pain had suddenly increased. On examination, the mus-
F. The splenic artery
cles of the lower part of the anterior abdominal wall in the
A 58-year-old man was in a restaurant when he suddenly
right lower quadrant showed rigidity. The diagnosis of peri-
started to vomit blood. He was taken unconscious to the
tonitis after perforation of the appendix was made.
emergency department of a local hospital. On examination,
9. The symptoms and signs displayed by this patient can
he had all the signs of severe hypovolemic shock. On palpa-
be explained by the following statements except which?
tion of the anterior abdominal wall, the right lobe of the
A. The perforation of the appendix had resulted in the
liver was felt three fingerbreadths below the costal margin.
spread of the infection from the appendix to involve
Several enlarged superficial veins could be seen around the
the parietal peritoneum.
umbilicus. His wife said that he had vomited blood 3
B. The parietal peritoneum in the right iliac region,
months previously and had nearly died. She admitted that
the muscles of the anterior abdominal wall, and the
he was a chronic alcoholic. The diagnosis was cirrhosis of
overlying skin are all supplied by the segmental
the liver secondary to chronic alcoholism.
nerves T12 and L1.
12. The symptoms and signs displayed by this patient can
C. Irritation of the parietal peritoneum reflexly increases
be explained by the following statements except which?
the tone of the abdominal muscles, causing rigidity.
A. The normal flow of portal blood through the liver is
D. The greater omentum tends to become stuck down
impaired by cirrhosis of the liver.
to the appendix and restricts the spread of infection.
B. The portal-systemic anastomoses become enlarged
E. The pain was intensified after perforation of the ap-
in this condition.
pendix because of stimulation of the autonomic
C. At the lower end of the esophagus, a branch from the
pain endings in the parietal peritoneum.
right gastric vein anastomoses with an esophageal
tributary of the azygos vein.
A 63-year-old man with a long history of a duodenal ulcer
D. Rupture of a varicosed esophageal vein could pro-
was seen in the emergency department after vomiting
duce a severe hemorrhage so that the patient would
blood-stained fluid and exhibiting all the signs and symp-
vomit up blood.
toms of severe hypovolemic shock.
E. With portal hypertension the paraumbilical veins
10. The following statements concerning duodenal ulcers
linking the superficial veins of the skin (systemic
could apply to the patient’s condition except which?
veins) to the portal vein become congested and
A. Hemorrhage from a duodenal ulcer often reveals it-
visible.
self by the passage of black stools on defecation.
A 48-year-old woman with a history of repeated vomiting
B. The pyloric sphincter prevents most of the blood
was admitted to the hospital with a diagnosis of large bowel
from the duodenal lumen from passing up into the
obstruction. To decompress the stomach a nasogastric tube
stomach.
was passed.
C. The gastroduodenal artery lies behind the first part of
the duodenum and was probably eroded by the ulcer.
13. When passing a nasogastric tube some important
D. The gastroduodenal artery is a small branch of the
anatomic facts should be considered except which?
hepatic artery.
A. The well-lubricated tube is inserted through the
E. The duodenal ulcer was most likely to be situated on
wider nostril.
the posterior wall of the first part of the duodenum.
B. The tube is directed backward along the nasal floor
and not upward because it may become caught on
A 47-year-old woman was operated on for the treatment of a
the nasal choanae.
chronic gastric ulcer that had not responded to medical treat-
C. The distance between the nostril and the cardiac
ment. At operation for partial gastrectomy, it was found that
orifice of the stomach is about 23 in. (57.5 cm).
the posterior wall of the stomach was stuck down to the pos-
D. The distance between the cardiac orifice and the py-
terior abdominal wall. The surgeon had to proceed with great
lorus is 4.8 to 5.6 in. (12 to 14 cm).
care to avoid damaging important structures lying on the pos-
E. Esophageal narrowing may offer resistance to the
terior abdominal wall.
tube behind the cricoid cartilage, 7.2 in. (18 cm)
11. The following structures located on the posterior ab-
from the nostril.
dominal wall were possibly involved in the disease
F. The left bronchus and the arch of the aorta cross in
process except which?
front of the esophagus and may impede the descent
A. The right kidney
of the tube, 11.2 in. (28 cm) from the nostril.
B. The pancreas
G. Where the esophagus enters the stomach there is a
C. The left suprarenal gland
slight resistance to the descent of the tube.
D. The left kidney
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
353
14. The following statements concerning an indirect
in the sitting position on the leg of an upturned bar stool.
inguinal hernia are correct except which?
While under observation he developed the signs and symp-
A. It is the most common form of abdominal hernia.
toms of peritonitis.
B. The neck of the hernial sac lies medial to the infe-
17. The signs and symptoms displayed by this patient could
rior epigastric artery.
be explained by the following anatomic statements ex-
C. The sac is the remains of the processus vaginalis.
cept which?
D. The hernial sac can extend into the scrotum.
A. The patient had impaled his rectum on the leg of
E. At the superficial inguinal ring, the hernial sac lies
the upturned bar stool.
above and medial to the pubic tubercle.
B. At operation, a laceration of the anterior wall of the
A mother took her 20-day-old baby boy to a pediatrician be-
middle of the rectum was found.
cause he had started to vomit after his feeds. The baby was
C. The leg of the bar stool had entered the rectovesical
breast-fed. For the first 15 days after birth, the baby had
pouch.
taken his feeds very well and had slept contentedly in his
D. The rectal contents had contaminated the peri-
crib following the normal after-feed burp. However, in the
toneal cavity and were responsible for the develop-
previous 5 days, the baby had begun to vomit toward the end
ment of peritonitis.
of each feed, shooting the milk out of his mouth for a dis-
E. The anterior surface of the middle third of the rec-
tance of 1 to 2 ft. After carefully questioning the mother and
tum has no peritoneal covering.
after a physical examination of the boy, the pediatrician
A 46-year-old man had been treating himself for hemor-
made the diagnosis of congenital hypertrophic pyloric
rhoids for the past 3 years. He had noticed that his feces were
stenosis.
often slightly blood stained. For the past 12 months, he had
15. He was able to ascertain the following additional signs
noticed that when he had his bowels open, he always felt that
and symptoms except which?
more was to come. Sometimes he went to the toilet several
A. Once the milk had been vomited, the child imme-
times a day but was only able to pass flatus and blood-stained
diately would feed again, only to repeat the same
mucus. Recently, pain had developed down the outside of
performance.
his right leg. Digital examination of the rectum revealed a
B. On gentle palpation of the anterior abdominal wall,
large, hard-based ulcer on the posterior wall of the rectum
a small firm swelling was felt just below and medial
with extensive induration of the pararectal tissues. A diagno-
to the tip of the left eighth costal cartilage.
sis of advanced carcinoma of the rectum was made.
C. On observing the anterior abdominal wall, an occa-
18. The following statements about this patient are proba-
sional wave of gastric peristalsis was seen traveling
bly correct except which?
across the epigastrium from left to right.
A. Some of the bleeding was from the carcinomatous
D. The stools were small in quantity and infrequent.
ulcer of the rectum as well as from the hemorrhoids.
E. The child showed signs of dehydration as evidenced
B. The lymphatic drainage of the rectum takes place
by a depressed anterior fontanelle of the skull.
first into the pararectal lymph nodes.
A 6-year-old girl was examined by a pediatrician because she
C. Carcinoma of the rectum never metastasizes to the
had a history of recurrent pain in the region of the umbili-
liver.
cus. The pain was dull and aching in nature and lasted for
D. Examination of the right leg revealed some weak-
about 1 week. It had recurred on four occasions in the pre-
ness of the muscles supplied by the sciatic nerve.
vious 2 years. Then 2 days before the examination, the child
E. The carcinoma had extended posteriorly to involve
had severe rectal bleeding and had fainted.
the sacral plexus.
F. The patient indicated that the leg pain was felt in
16. On examination of the child, the pediatrician found the
skin areas supplied by branches of the sciatic nerve.
following signs and symptoms consistent with the diag-
nosis of Meckel’s diverticulum except which?
A 72-year-old woman was suspected of having a tumor of the
A. Tenderness of the anterior abdominal wall in the
sigmoid colon. The physician decided to confirm the diag-
right iliac region
nosis by performing a sigmoidoscopy.
B. Anemia
19. The following anatomic statements are correct con-
C. Stools streaked with dark red blood
cerning the procedure of sigmoidoscopy except which?
D. Pyrexia of 102°F
A. After inserting the instrument into the anus, the
A 30-year-old man involved in a barroom brawl was seen in
lighted end enters the ampulla of the rectum after a
the emergency department. He was found to have a blood-
distance of about 1.5 in. (4 cm).
stained tear on the seat of his trousers and lacerations of the
B. Some side-to-side movement may be necessary to
anal margin. During the fight he was knocked down and fell
avoid the transverse rectal folds.
354
Chapter 19
C. The rectosigmoid junction will be reached approxi-
D. The swellings bulged downward when the patient
mately 6.5 in. (16.25 cm) from the anal margin.
was asked to strain.
D. To negotiate the rectosigmoid junction, the tip of
E. Large, congested veins were seen in the swellings.
the sigmoidoscope should be directed anteriorly and
F. The swellings remained outside the anus after defe-
to the patient’s left.
cation.
E. Stretching of the colonic wall may give rise to col-
G. Abrasion of the mucous membrane was responsible
icky pain in the upper part of the abdomen in the re-
for the bleeding.
gion of the xiphoid process.
A 42-year-old woman visited her physician because she ex-
A 3-week-old boy was taken to a pediatrician because of re-
perienced an agonizing pain in the rectum, which occurred
peated vomiting and reluctance to feed. On questioning,
on defecation. She had first noticed the pain a week before
the mother said the child had started to vomit on the first
when she tried to defecate. The pain lasted for about an
day of life and has vomited at least once a day since then.
hour, then passed off, only to return with the next bowel
Early on, the mother had been reassured and told that the
movement. She said that she suffered from constipation and
baby was taking his feedings too quickly and that the vom-
admitted that sometimes her stools were streaked with
iting eventually would cease. While initially accepting this
blood. After a careful examination, a diagnosis of anal fissure
reassurance, the mother now noticed that the child did not
was made.
seem hungry at feeding time; moreover, she could see that
22. The following statements concerning this case are cor-
the abdomen was becoming distended. She added that the
rect except which?
child definitely was constipated; very occasionally, hard
A. Examination of the anal canal was difficult because
meconium was passed. After a thorough physical examina-
any attempt to insert a gloved finger into the canal
tion of the child, the pediatrician made the diagnosis of
caused severe pain.
primary megacolon (Hirschsprung disease).
B. The anus was kept tightly closed by the spasm of the
20. The examination of the child revealed the following
external anal sphincter.
possible signs except which?
C. Gentle eversion of the anal margin under local anes-
A. The abdomen was found to be distended.
thesia revealed the lower edge of a linear tear in the
B. A rectal examination with the gloved little finger re-
posterior wall of the anal canal; a small tag of skin
sulted in the passage of a large amount of flatus and
projected from the lower end of the tear.
the abdominal distension became visibly less.
D. The forward edge of a hard fecal mass may have
C. A low barium enema followed by an X-ray examina-
caught one of the anal valves and torn it downward
tion showed a normal rectum.
as it descended.
D. On the radiograph, above the rectum, a narrowed
E. Anal fissures tend to occur on the anterior and pos-
part of the colon led to a funnel-shaped expansion,
terior walls of the anal canal because the mucous
which in turn led to a greatly dilated descending
membrane is poorly supported in this region by the
colon and transverse colon.
superficial external sphincter muscle.
E. On placing a stethoscope on the abdominal
F. The mucous membrane of the lower half of the anal
wall, the physician could not hear sounds of peri-
canal is innervated by autonomic afferent nerves
stalsis.
and is sensitive only to stretch.
A 53-year-old man complained that for the past 4 years he
A 41-year-old woman was seen in the emergency depart-
had frequently passed blood-stained stools. Recently, he had
ment complaining of a painful swelling in the region of the
noticed that his “bowel” protruded from his anus after defe-
anus. On examination, a hot, red, tender swelling was found
cation, and this caused him considerable discomfort.
on the right side of the anal margin. A diagnosis of
ischiorectal abscess was made.
21. The following symptoms and signs in this patient were
consistent with a diagnosis of third-degree internal he-
23. The following statements concerning this case are prob-
morrhoids except which?
ably correct except which?
A. The patient suffered from intense perianal irritation
A. An ischiorectal abscess is a common complication
caused by the mucous secretions from the prolapsed
of anal fissure.
mucous membrane.
B. The fat in the ischiorectal fossa is prone to infection
B. Proctoscopic examination revealed three pink
that might extend laterally through the base of the
swellings of mucous membrane at the level of the
anal fissure.
anal valves.
C. The fat in the ischiorectal fossa has a profuse blood
C. The swellings were situated at the 1, 4, and 9 o’-
supply.
clock positions with the patient in the lithotomy
D. A surgical incision of the abscess should provide
position.
adequate drainage of the pus.
The Abdominal Wall, the Peritoneal Cavity, the Retroperitoneal Space, and the Alimentary Tract
355
E. The surgeon should avoid the inferior rectal nerve
26. Following a terrorist bomb attack, a young child was
and vessels that cross the ischiorectal fossa from the
seen in the emergency department with a gaping hole
lateral to the medial side.
in the anterior abdominal wall, and coils of gut were
exposed on the surface. How would you determine by
24. The differential diagnosis between a perforated duode-
inspection whether the gut was small or large intes-
nal ulcer and a perforated appendix may prove difficult.
tine?
Can you explain this in anatomic terms?
25. The pain of acute appendicitis is commonly first felt in
the umbilical region and later in the right iliac region.
Can you explain this in anatomic terms?
Answers and Explanations
1.
D is the correct answer. The segmental nerves supply-
12.
C is the correct answer. At the lower end of the esoph-
ing the right lower quadrant of the abdominal wall are
agus, a branch from the left gastric vein anastomoses
T11, T12, and L1.
with an esophageal tributary of the azygos vein.
2.
E is the correct answer. The urine could not ex-
13.
C is the correct answer. The distance between the nos-
tend posteriorly because of the attachment of the
tril and the cardiac orifice of the stomach is about 17.2
Colles’ fascia to the posterior edge of the perineal
in. (44 cm).
membrane.
14.
B is the correct answer. The neck of the hernial sac in
3.
D is the correct answer. The pyramidalis muscle (if pre-
an indirect inguinal hernia lies lateral to the inferior
sent) is innervated by the twelfth thoracic nerve.
epigastric artery (see CD Fig. 19-6).
4.
F is the correct answer. The contents of this hernial sac
15.
B is the correct answer. In congenital hypertrophic py-
included coils of small intestine, which were responsi-
loric stenosis, there is a localized muscular hypertrophy
ble for the gurgling noises that occurred as the hernia
and hyperplasia of the pyloric sphincter, which is larger
was reduced.
than normal and can usually be palpated just below and
medial to the tip of the right ninth costal cartilage.
5.
E is the correct answer. The swelling occurs medial to
the inferior epigastric artery (see CD Fig. 19-6).
16.
D is the correct answer. In many cases of Meckel’s di-
6.
E is the correct answer. The neck of a femoral hernial
verticulum, a small area of ectopic gastric mucosa is
sac is situated below and lateral to the pubic tubercle
present, which is capable of producing hydrochloric
(see CD Fig. 19-7).
acid and pepsin. In the adjoining mucous membrane,
this child had a chronic ulcer that was responsible for
7.
F is the correct answer. The normal testis is freely
the umbilical pain. Sudden severe hemorrhage from
mobile within the scrotum and is not tethered to the
an artery in the floor of the ulcer was the cause of the
subcutaneous tissue or skin.
rectal bleeding and fainting attack. The condition is
8.
C is the correct answer. The linea alba lies in the mid-
not associated with pyrexia. After restoration of the
line; the rectus sheath lies lateral to the linea alba.
blood volume and hemoglobin to a normal level, a
child with this condition should be operated on and
9.
E is the correct answer. In the parietal peritoneum
the diverticulum should be widely excised. The cut
lining the anterior abdominal wall in the right
ends of the ileum then are joined by an end-to-end
iliac fossa, the sensation of pain originates in the nerve
anastomosis.
endings of somatic spinal nerves (T12 and L1).
17.
E is the correct answer. The upper third of the rectum
10.
D is the correct answer. The gastroduodenal artery is a
has peritoneum on its anterior and lateral surfaces; the
large branch of the hepatic artery.
middle third has peritoneum on its anterior surface;
11.
A is the correct answer. The right kidney does not lie
and the lower third has no peritoneal covering (see text
behind the stomach (see text Fig. 19-38)
Fig. 19-64).
356
Chapter 19
18. C is the correct answer. Advanced carcinoma of the rec-
23.
C is the correct answer. The fat in the ischiorectal fossa
tum not only extends to the pararectal and inferior
has a poor blood supply.
mesenteric nodes but may also spread via the superior
24.
A small perforation of the first part of the duodenum
rectal, inferior mesenteric, splenic, and portal veins to
may result in the contents of the duodenum running
the liver.
down the right paracolic gutter to the right iliac fossa.
19. E is the correct answer. Colicky pain from the colon is
The signs then closely resemble those of a perforated
referred to the lower part of the anterior abdominal wall
appendix.
above the symphysis pubis (see CD Fig. 19-23).
25.
The initial pain of acute appendicitis is a vague dis-
20. E is the correct answer. In patients with primary mega-
comfort and is referred to the umbilical region. The af-
colon, the muscle of the colon immediately proximal to
ferent nerve fibers from the appendix accompany the
the obstruction is hypertrophied as the result of at-
sympathetic nerves to the superior mesenteric plexus.
tempting to force the meconium and feces onward.
They enter the thorax via the splanchnic nerves and en-
Usually very active peristalsis is heard on listening to the
ter the spinal cord at the level of the tenth thoracic seg-
abdomen with a stethoscope.
ment. The tenth thoracic intercostal nerve supplies the
skin of the umbilicus, and for this reason pain is com-
21. C is the correct answer. The swellings of internal he-
monly referred to the umbilicus. Once the inflamma-
morrhoids are situated at the 3, 7, and 11 o’clock po-
tory process has extended beyond the confines of the
sitions with the patient in the lithotomy position.
appendix and has involved the parietal peritoneum, a
These swellings are caused by a dilatation of the three
severe localized pain is felt in the right iliac region. The
main tributaries of the superior rectal vein (see CD
parietal peritoneum, the overlying muscles of the ante-
Fig. 19-26).
rior abdominal wall, and the covering skin are all sup-
22. F is the correct answer. The mucous membrane of the
plied by the first lumbar nerve.
lower half of the anal canal is innervated by the inferior
26.
A list of naked-eye differences between the small and
rectal nerve and is very sensitive to pain, temperature,
large intestine are given on text page 751.
touch, and pressure.
The Viscera Associated
with the Alimentary
Tract: The Liver, the
20
Pancreas, and the Spleen
Chapter Outline
The Liver
358
Accessory Bile Duct
361
Liver Supports and Surgery
358
Congenital Choledochal Cyst
361
Liver Trauma
358
The Pancreas
362
Liver Biopsy
358
Diagnosis of Pancreatic Disease
362
Subphrenic Spaces
359
Trauma of the Pancreas
362
Portal-Systemic Anastomoses
359
Cancer of the Head of the Pancreas
and the Bile Duct
362
Portal Hypertension
359
The Pancreatic Tail and Splenectomy
362
Blood Flow in the Portal Vein and
Malignant Disease
359
Congenital Anomalies of the Pancreas
362
Gallstones
359
Anular Pancreas
362
Biliary Colic
359
Ectopic Pancreas
363
Acute Cholecystitis
359
Congenital Fibrocystic Disease
363
Cholecystectomy and the Arterial Supply to the
The Spleen
363
Gallbladder
359
Splenic Enlargement
363
Gangrene of the Gallbladder
359
Trauma to the Spleen
363
Congenital Anomalies of the Gallbladder
359
Congenital Anomalies of the Spleen
363
Biliary Atresia
359
Supernumerary Spleens
363
Absence of the Gallbladder
361
Clinical Problem Solving Questions
363
Double Gallbladder
361
Absence of the Cystic Duct
361
Answers and Explanations
364
the thorax or upper abdomen are common causes of liver
THE LIVER
injury. Blunt traumatic injuries from automobile accidents
are also common, and severe hemorrhage accompanies
tears of this organ.
Liver Supports and Surgery
Because anatomic research has shown that the bile
ducts, hepatic arteries, and portal vein are distributed in a
The liver is held in position in the upper part of the abdom-
segmental manner, appropriate ligation of these structures
inal cavity by the attachment of the hepatic veins to the in-
allows the surgeon to remove large portions of the liver in
ferior vena cava. The peritoneal ligaments and the tone of
patients with severe traumatic lacerations of the liver or with
the abdominal muscles play a minor role in its support. This
a liver tumor. (Even large, localized carcinomatous metasta-
fact is important surgically because even if the peritoneal
tic tumors have been successfully removed.)
ligaments are cut, the liver can be only slightly rotated.
Liver Biopsy
Liver Trauma
Liver biopsy is a common diagnostic procedure. With the
The liver is a soft, friable structure enclosed in a fibrous cap-
patient holding his or her breath in full expiration—to re-
sule. Its close relationship to the lower ribs must be empha-
duce the size of the costodiaphragmatic recess and the like-
sized. Fractures of the lower ribs or penetrating wounds of
lihood of damage to the lung—a needle is inserted through
The Viscera Associated with the Alimentary Tract: The Liver, the Pancreas, and the Spleen
359
the right eighth or ninth intercostal space in the midaxillary
determines whether infected bile is likely to enter the pan-
line. The needle passes through the diaphragm into the
creatic duct.
liver, and a small specimen of liver tissue is removed for
Gallstones have been known to ulcerate through the
microscopic examination.
gallbladder wall into the transverse colon or the duodenum.
In the former case, they are passed naturally per the rectum,
but in the latter case, they may be held up at the ileocecal
Subphrenic Spaces
junction, producing intestinal obstruction.
The important subphrenic spaces and their relationship to
the liver are described on text page 713. Under normal
Acute Cholecystitis
conditions these are potential spaces only, and the peri-
toneal surfaces are in contact. An abnormal accumulation
Acute cholecystitis produces discomfort in the right upper
of gas or fluid is necessary for separation of the peritoneal
quadrant or epigastrium. Inflammation of the gallbladder
surfaces. The anterior surface of the liver is normally dull
may cause irritation of the subdiaphragmatic parietal peri-
on percussion. Perforation of a gastric ulcer is often ac-
toneum, which is supplied in part by the phrenic nerve (C3,
companied by a loss of liver dullness caused by the accu-
4, and 5). This may give rise to referred pain over the shoul-
mulation of gas over the anterior surface of the liver and in
der, because the skin in this area is supplied by the supra-
the subphrenic spaces.
clavicular nerves (C3 and 4).
Portal-Systemic Anastomoses
Cholecystectomy and the Arterial
See CD Chapter 8.
Supply to the Gallbladder
Before attempting a cholecystectomy operation, the surgeon
Portal Hypertension
must be aware of the many variations in the arterial supply
to the gallbladder and the relationship of the vessels to the
See CD Chapter 8.
bile ducts (CD Fig. 20-1). Unfortunately, there have been
several reported cases in which the common hepatic duct or
Blood Flow in the Portal Vein and
the main bile duct has been included in the arterial ligature
with disastrous consequences.
Malignant Disease
See CD Chapter 8.
Gangrene of the Gallbladder
Unlike the appendix, which has a single arterial supply, the
Gallstones
gallbladder rarely becomes gangrenous. In addition to the
cystic artery, the gallbladder also receives small vessels from
Gallstones are usually asymptomatic; however, they can
the visceral surface of the liver.
give rise to gallstone colic or produce acute cholecystitis.
Biliary Colic
CONGENITAL
Biliary colic is usually caused by spasm of the smooth
muscle of the wall of the gallbladder in an attempt to ex-
ANOMALIES OF
pel a gallstone. Afferent nerve fibers ascend through the
celiac plexus and the greater splanchnic nerves to the tho-
THE GALLBLADDER
racic segments of the spinal cord. Referred pain is felt in
the right upper quadrant or the epigastrium (T7, 8, and 9
dermatomes).
Biliary Atresia
Obstruction of the biliary ducts with a gallstone or by
compression by a tumor of the pancreas results in backup of
Failure of the bile ducts to canalize during development
bile in the ducts and development of jaundice. The im-
causes atresia. The various forms of atresia are shown in CD
paction of a stone in the ampulla of Vater may result in the
Fig. 20-2. Jaundice appears soon after birth; clay-colored
passage of infected bile into the pancreatic duct, producing
stools and very dark colored urine are also present. Surgical
pancreatitis. The anatomic arrangement of the terminal part
correction of the atresia should be attempted when possible.
of the bile duct and the main pancreatic duct is subject to
If the atresia cannot be corrected, the child will die of liver
considerable variation. The type of duct system present
failure.
360
Chapter 20
right hepatic artery
left hepatic artery
cystic artery
hepatic artery
bile duct
CD Figure 20-1
Some common
variations of blood supply to the
gallbladder.
atresia of bile duct
atresia of hepatic duct
CD Figure 20-2
Some common congeni-
atresia of entire extrahepatic apparatus
atresia of hepatic ducts
tal anomalies of the biliary ducts.
The Viscera Associated with the Alimentary Tract: The Liver, the Pancreas, and the Spleen
361
duct. The gallbladder drains directly into the bile duct. The
Absence of the Gallbladder
condition may not be recognized when performing a chole-
cystectomy, and the bile duct may be seriously damaged by
Occasionally, the outgrowth of cells from the hepatic bud
the surgeon (see CD Fig. 20-3).
fails to develop. In these cases, there is no gallbladder and
no cystic duct (CD Fig. 20-3).
Accessory Bile Duct
Double Gallbladder
A small accessory bile duct may open directly from the liver
into the gallbladder, which may cause leakage of bile into
Rarely, the outgrowth of cells from the hepatic bud bifur-
the peritoneal cavity after cholecystectomy if it is not recog-
cates so that two gallbladders are formed (see CD Fig. 20-3).
nized at the time of surgery (see CD Fig. 20-3).
Absence of the Cystic Duct
Congenital Choledochal Cyst
In absence of the cystic duct, the entire outgrowth of cells
Rarely, a choledochal cyst develops because of an area of
from the hepatic bud develops into the gallbladder and fails
weakness in the wall of the bile duct. A cyst can contain 1 to
to leave the narrow stem that would normally form the cystic
2 L of bile. The anomaly is important in that it may press
congenital absence of gallbladder
double gallbladder
absence of cystic duct
abnormally long cystic duct
CD Figure 20-3
Some common congeni-
accessory bile duct
choledochal cyst
tal anomalies of the gallbladder.
362
Chapter 20
on the bile duct and cause obstructive jaundice (see CD
Fig. 20-3).
Cancer of the Head of the Pancreas
and the Bile Duct
Because of the close relation of the head of the pancreas to
THE PANCREAS
the bile duct, cancer of the head of the pancreas often
causes obstructive jaundice.
Diagnosis of Pancreatic Disease
The Pancreatic Tail and Splenectomy
The deep location of the pancreas sometimes gives rise to
The presence of the tail of the pancreas in the splenicorenal
problems of diagnosis for the following reasons:
ligament sometimes results in its damage during splenec-
■
Pain from the pancreas is commonly referred to the back.
tomy. The damaged pancreas releases enzymes that start to
■
Because the pancreas lies behind the stomach and trans-
digest surrounding tissues, with serious consequences.
verse colon, disease of the gland can be confused with
that of the stomach or transverse colon.
■ Inflammation of the pancreas can spread to the peri-
CONGENITAL
toneum, forming the posterior wall of the lesser sac. This
in turn can lead to adhesions and the closing off of the
ANOMALIES OF
lesser sac to form a pseudocyst.
THE PANCREAS
Trauma of the Pancreas
The pancreas is deeply placed within the abdomen and is
Anular Pancreas
well protected by the costal margin and the anterior ab-
dominal wall. However, blunt trauma, such as in a sports in-
In anular pancreas, the ventral pancreatic bud becomes
jury when a sudden blow to the abdomen occurs, can com-
fixed so that, when the stomach and duodenum rotate, the
press and tear the pancreas against the vertebral column.
ventral bud is pulled around the right side of the duode-
The pancreas is most commonly damaged by gunshot or
num to fuse with the dorsal bud of the pancreas, thus en-
stab wounds.
circling the duodenum (CD Fig. 20-4). This may cause
Damaged pancreatic tissue releases activated pancre-
obstruction of the duodenum, and vomiting may start a
atic enzymes that produce the signs and symptoms of acute
few hours after birth. Early surgical relief of the obstruction
peritonitis.
is necessary.
dorsal pancreatic bud
duodenum
ventral pancreatic bud
dorsal bud
narrowed lumen of duodenum
CD Figure 20-4
Formation of the anular
fixed ventral pancreatic bud
pancreas, producing duodenal obstruction.
Note the narrowing of the duodenum.
The Viscera Associated with the Alimentary Tract: The Liver, the Pancreas, and the Spleen
363
The spleen is situated at the beginning of the splenic
Ectopic Pancreas
vein, and in cases of portal hypertension it often enlarges
from venous congestion.
Ectopic pancreatic tissue may be found in the submucosa of
the stomach, duodenum, small intestine
(including
Meckel’s diverticulum), and gallbladder and in the spleen.
Trauma to the Spleen
It is important in that it may protrude into the lumen of the
Although anatomically the spleen gives the appearance of
gut and be responsible for causing intussusception.
being well protected, automobile accidents of the crushing
or run-over type commonly produce laceration of the
Congenital Fibrocystic Disease
spleen. Penetrating wounds of the lower left thorax can also
damage the spleen.
Basically, congenital fibrocystic disease in the pancreas is
caused by an abnormality in the secretion of mucus. The mu-
cus produced is excessively viscid and obstructs the pancre-
atic duct, which leads to pancreatitis with subsequent fibrosis.
CONGENITAL
The condition also involves the lungs, kidneys, and liver.
ANOMALIES OF
THE SPLEEN
THE SPLEEN
Splenic Enlargement
Supernumerary Spleens
A pathologically enlarged spleen extends downward and
In 10% of people, one or more supernumerary spleens may
medially. The left colic flexure and the phrenicocolic liga-
be present, either in the gastrosplenic omentum or in the
ment prevent a direct downward enlargement of the organ.
splenicorenal ligament. Their clinical importance is that
As the enlarged spleen projects below the left costal margin,
they may hypertrophy after removal of the major spleen and
its notched anterior border can be recognized by palpation
be responsible for a recurrence of symptoms of the disease
through the anterior abdominal wall.
for which splenectomy was initially performed.
Clinical Problem Solving Questions
Read the following case histories/questions and give
C. Referred pain is felt in the right upper quadrant or
the best answer for each.
the epigastrium.
D. T7 through T9 dermatomes are involved.
A 55-year-old woman with a history of flatulent dyspepsia
E. The violent contractions of the gallbladder wall are
suddenly experienced an excruciating colicky pain across
attempts to expel the gallstones.
the upper part of the abdomen. On examination in the
emergency department, she was found to have some rigidity
On examination of the abdomen of a 31-year-old woman, a
and tenderness in the right upper quadrant. A diagnosis of
large swelling was found to extend downward and medially
biliary colic was made.
below the left costal margin. On percussion, a continuous
band of dullness was noted to extend upward from the left of
1. The following statements would explain this patient’s
the umbilicus to the left axillary region. On palpation, a
symptoms except which?
notch was felt along the anterior border of the swelling. A di-
A. The pain of gallstone colic is caused by spasm of the
agnosis of splenic enlargement was made.
smooth muscle in the wall of the gallbladder and
distension of the bile ducts by the stones.
2. The signs displayed by this patient can be explained by
B. The pain fibers from the gallbladder and bile ducts
the following statements except which?
ascend through the superior mesenteric plexus and
A. The spleen has a notched anterior border caused by
the greater splanchnic nerves to enter the thoracic
incomplete fusion of its parts during development.
segments of the spinal cord.
364
Chapter 20
B. Because of the presence of the left colic flexure and
across the upper part of the abdomen. On examination
the phrenicocolic ligament, the spleen is unable to
after the attack, some rigidity and tenderness was noted
expand vertically downward.
in the right hypochondrium. Two days later the patient
C. A pathologically enlarged spleen extends downward
became jaundiced, and it was noticed that the degree of
and forward, toward the umbilicus.
jaundice varied from day to day. The diagnosis of biliary
D. The spleen is situated in the upper left quadrant of
colic was made. Why should a person passing a gall-
the abdomen beneath the diaphragm.
stone experience pain? Why is the pain experienced in
E. The long axis of the spleen lies along the twelfth rib.
the area described above? Why does the jaundice vary
in intensity?
3. A 19-year-old football player was accidently kicked on
the left side of his chest. On returning to the locker
6.
A 65-year-old woman was admitted to the hospital with
room he said he felt faint and collapsed to the floor. On
progressive jaundice of three months’ duration and
examination in the emergency department, he was
weight loss. She had not experienced any colicky pain.
found to be in hypovolemic shock. He had tenderness
On examination, a soft swelling could be felt in the ab-
and guarding in the left upper quadrant of his ab-
domen in the region of the tip of the right ninth costal
domen. He also had extreme local tenderness over his
cartilage. A diagnosis of cancer of the head of the pan-
left tenth rib in the midaxillary line. A diagnosis of a
creas was made. What anatomic structure is responsible
ruptured spleen and the possibility of a fractured tenth
for the swelling?
rib was made. Explain the tenderness and guarding in
7.
A patient with thrombocytopenic purpura was advised
the abdomen in this patient.
to have a splenectomy to stop the episodes of bleeding
A 40 year-old obese woman complaining of indigestion was
from the gums and gastrointestinal tract. The operation
admitted to the hospital for investigation. She had a past
was successful. Eighteen months later the clinical fea-
history of gallstones and transient attacks of jaundice.
tures returned. Can you explain in anatomic terms the
Large gallstones have been known to erode through the
recurrence of the bleeding after the condition had ap-
posterior wall of the gallbladder and enter the intestinal
parently been cured by splenectomy?
tract.
8.
Following a splenectomy, it was noticed that pancreatic
4. Which part of the intestinal tract is likely to initially
juice was exuding through the patient’s abdominal
contain the stone?
wound. Is the pancreas likely to be damaged during
A. The sigmoid colon
splenectomy? Which part of the pancreas?
B. The descending colon
9.
The anatomic arrangement of the terminal part of the
C. The transverse colon
bile duct and the main pancreatic duct is subject to
D. The ascending colon
considerable variation. Which variations are likely to be
E. The jejunum
associated with a pancreatitis should a gallstone be-
5. A 50-year-old woman with a history of flatulent dyspep-
come impacted at the lower end of the bile duct?
sia suddenly experienced an excruciating colicky pain
Answers and Explanations
1. B is the correct answer. The pain fibers from the gall-
quadrant and reflex guarding of the muscles in the
bladder and bile ducts ascend through the celiac plexus.
same area.
2. E is the correct answer. The long axis of the spleen lies
4. C is the correct answer. The transverse colon is in close
along the tenth rib (see text Fig. 20-27).
posterior relation to the gallbladder.
3. Initially in this patient, the spleen underwent a
5. The pain is due to the spastic contraction of the muscle
subcapsular hemorrhage, and later, in the locker
of the gallbladder attempting to flush the stone down
room, the capsule gave way, allowing the blood to
the bile ducts and to the distension of the ducts by the
escape into the peritoneal cavity. The presence of
stone. The afferent pain fibers from the gallbladder and
blood in the peritoneal cavity irritated the parietal
bile ducts enter the spinal cord between segments T5
peritoneum, causing tenderness in the left upper
and T9. Pain is referred to the epigastrium via the sev-
The Viscera Associated with the Alimentary Tract: The Liver, the Pancreas, and the Spleen
365
enth to the ninth intercostal nerves. A variable amount
8. The tail of the pancreas lies within the splenicorenal
of bile gets past the stone.
ligament, and its tip is related to the hilus of the spleen.
The surgeon has to take extreme care not to damage the
6. A small carcinoma of the head of the pancreas was
tail of the pancreas during a splenectomy.
found at operation to be compressing the bile duct.
Back pressure along the bile ducts produced dilatation
9. Any variation in which the bile duct and the pancreatic
of the gallbladder, which could be felt in the region of
duct open by a common orifice into the duodenum is
the tip of the right ninth costal cartilage.
likely to cause this problem (see text Fig. 20-26). Gall-
7. About 10% of persons have accessory spleens. These
stones are usually associated with infected bile. A stone
should always be looked for when performing a
impacted at the orifice into the duodenum will allow
splenectomy for such conditions as thrombocytopenic
reflux of infected bile along the main pancreatic duct,
purpura. If an accessory spleen is missed, it will enlarge
and pancreatitis will occur.
and take over the functions of the main spleen.
The Kidneys, the Ureters,
the Bladder, and the
Urethra
21
Chapter Outline
The Kidneys
370
Bladder Distension
375
Renal Mobility
370
Urinary Retention
375
Kidney Trauma
370
Suprapubic Aspiration
375
Kidney Tumors
371
Cystoscopy
375
Renal Pain
371
Bladder Injuries
375
Transplanted Kidneys
371
Difficulty with Micturition after Spinal Cord Injury
375
The Male Urethra
377
The Ureters
371
Urethral Infections
377
Traumatic Ureteral Injuries
371
Injuries to the Penis
377
Ureteric Stones
372
Rupture of the Urethra
377
Renal Colic
372
Catheterization
377
Congenital Anomalies of the Kidneys
372
Anatomy of the Procedure of Catheterization
377
Polycystic Kidney
372
The Female Urethra
378
Pelvic Kidney
372
Urethral Infections
378
Horseshoe Kidney
372
Urethral Injuries
378
Unilateral Double Kidney
373
Catheterization
378
Rosette Kidney
373
Congenital Anomalies of the Bladder
378
Supernumerary Renal Arteries
373
Exstrophy of the Bladder (Ectopia Vesicae)
378
Congenital Anomalies of the Ureters
374
Congenital Anomalies of the Urethra
378
Double Pelvis
374
Meatal Stenosis
378
Bifid Ureter
374
Hypospadias
378
Megaloureter
374
Epispadias
378
Postcaval Ureter
375
Clinical Problem Solving Questions
380
The Urinary Bladder
375
Palpation of the Urinary Bladder
375
Answers and Explanations
382
poorly developed abdominal musculature. Should the
THE KIDNEYS
amount of perirenal fat be reduced, the mobility of the kidney
may become excessive and produce symptoms of renal colic
caused by kinking of the ureter. Excessive mobility of the kid-
Renal Mobility
ney leaves the suprarenal gland undisturbed because the latter
occupies a separate compartment in the renal fascia.
The kidneys are maintained in their normal position by in-
traabdominal pressure and by their connections with the
perirenal fat and renal fascia. Each kidney moves slightly with
Kidney Trauma
respiration. The right kidney lies at a slightly lower level than
the left kidney, and the lower pole may be palpated in the right
The kidneys are well protected by the lower ribs, the lumbar
lumbar region at the end of deep inspiration in a person with
muscles, and the vertebral column. However, a severe blunt
The Kidneys, the Ureters, the Bladder, and the Urethra
371
injury applied to the abdomen may crush the kidney against
subcostal nerve (T12) to the flank and the anterior abdom-
the last rib and the vertebral column. Depending on the
inal wall.
severity of the blow, the injury varies from a mild bruising to
a complete laceration of the organ. Penetrating injuries are
Transplanted Kidneys
usually caused by stab wounds or gunshot wounds and often
involve other viscera. Because 25% of the cardiac outflow
The iliac fossa on the posterior abdominal wall is the usual site
passes through the kidneys, renal injury can result in rapid
chosen for transplantation of the kidney. The fossa is exposed
blood loss. A summary of the injuries to the kidneys is shown
through an incision in the anterior abdominal wall just above
in CD Fig. 21-1.
the inguinal ligament. The iliac fossa in front of the iliacus
muscle is approached retroperitoneally. The kidney is posi-
tioned and the vascular anastomosis constructed. The renal
Kidney Tumors
artery is anastomosed end to end to the internal iliac artery and
Malignant tumors of the kidney have a strong tendency to
the renal vein is anastomosed end to side to the external iliac
spread along the renal vein. The left renal vein receives the
vein (CD Fig. 21-2). Anastomosis of the branches of the inter-
left testicular vein in the male, and this may rarely become
nal iliac arteries on the two sides is sufficient so that the pelvic
blocked, producing left-sided varicocele.
viscera on the side of the renal arterial anastomosis are not at
risk. Ureterocystostomy is then performed by opening the
bladder and providing a wide entrance of the ureter through
Renal Pain
the bladder wall.
Renal pain varies from a dull ache to a severe pain in the
flank that may radiate downward into the lower abdomen.
Renal pain can result from stretching of the kidney capsule
THE URETERS
or spasm of the smooth muscle in the renal pelvis. The
afferent nerve fibers pass through the renal plexus around
the renal artery and ascend to the spinal cord through
Traumatic Ureteral Injuries
the lowest splanchnic nerve in the thorax and the sympa-
thetic trunk. They enter the spinal cord at the level of T12.
Because of its protected position and small size, injuries to
Pain is commonly referred along the distribution of the
the ureter are rare. Most injuries are caused by gunshot
A
B
C
CD Figure 21-1
Injuries to the kidney. A. Contu-
sion, with hemorrhage confined to the cortex be-
neath the intact fibrous capsule. B. Tearing of the
capsule and cortex with bleeding occurring into
the perirenal fat. C. Tearing of the capsule, the
cortex, and the medulla. Note the escape of blood
into the calyces and therefore the urine. Urine as
well as blood may extravasate into the perirenal
and pararenal fat and into the peritoneal cavity.
D. Shattered kidney with extensive hemorrhage
and extravasation of blood and urine into the
perirenal and pararenal fat; blood also enters the
calyces and appears in the urine. E. Injury to the
renal pedicle involving the renal vessels and pos-
D
E
sibly the renal pelvis.
372
Chapter 21
inferior vena cava
abdominal aorta
transplanted
kidney
common iliac
artery
internal iliac artery
external iliac artery
external iliac vein
CD Figure 21-2
The transplanted kidney.
wounds and, in a few individuals, penetrating stab wounds.
Because the ureters are retroperitoneal in position, urine
CONGENITAL
may escape into the retroperitoneal tissues on the posterior
abdominal wall.
ANOMALIES OF
Ureteric Stones
THE KIDNEYS
There are three sites of anatomic narrowing of the ureter
where stones may be arrested, namely, the pelviureteral
Polycystic Kidney
junction, the pelvic brim, and where the ureter enters the
bladder. Most stones, although radiopaque, are small
A hereditary disease, polycystic kidney can be transmitted by
enough to be impossible to see definitely along the course of
either parent. It may by associated with congenital cysts of
the ureter on plain radiographic examination. An intra-
the liver, pancreas, and lung. Both kidneys are enormously
venous pyelogram is usually necessary. The ureter runs down
enlarged and riddled with cysts. Polycystic kidney is thought
in front of the tips of the transverse processes of the lumbar
to be caused by a failure of union between the developing
vertebrae, crosses the region of the sacroiliac joint, swings out
convoluted tubules and collecting tubules. The accumula-
to the ischial spine, and then turns medially to the bladder.
tion of urine in the proximal tubules results in the formation
of retention cysts.
Renal Colic
Pelvic Kidney
The renal pelvis and the ureter send their afferent nerves into
the spinal cord at segments T11 and 12 and L1 and 2. In renal
In pelvic kidney, the kidney is arrested in some part of its
colic, strong peristaltic waves of contraction pass down the
normal ascent; it usually is found at the brim of the pelvis
ureter in an attempt to pass the stone onward. The spasm of the
(CD Fig. 21-3). Such a kidney may present with no signs
smooth muscle causes an agonizing colicky pain, which is re-
or symptoms and may function normally. However,
ferred to the skin areas that are supplied by these segments of
should an ectopic kidney become inflamed, it may—be-
the spinal cord, namely, the flank, loin, and groin.
cause of its unusual position—give rise to a mistaken
When a stone enters the low part of the ureter, the pain
diagnosis.
is felt at a lower level and is often referred to the testis or the
tip of the penis in the male and the labium majus in the fe-
Horseshoe Kidney
male. Sometimes ureteral pain is referred along the femoral
branch of the genitofemoral nerve (L1 and 2) so that pain is
When the caudal ends of both kidneys fuse as they de-
experienced in the front of the thigh. The pain is often so se-
velop, the result is horseshoe kidney (see CD Fig. 21-3).
vere that afferent pain impulses spread within the central
Both kidneys commence to ascend from the pelvis, but
nervous system, giving rise to nausea.
the interconnecting bridge becomes trapped behind the
The Kidneys, the Ureters, the Bladder, and the Urethra
373
aorta
inferior
mesenteric
horseshoe kidney
pelvic kidney
unilateral double kidney
aberrant renal arteries
rosette kidney (cake kidney)
aberrant renal artery causing
CD Figure 21-3
Some common congenital
urinary obstruction
anomalies of the kidney.
inferior mesenteric artery so that the kidneys come to rest
the ureter may result in stasis of the urine and may require
in the low lumbar region. Both ureters are kinked as they
surgical treatment.
pass inferiorly over the bridge of renal tissue, producing
urinary stasis, which may result in infection and stone
Rosette Kidney
formation. Surgical division of the bridge corrects the
condition.
Both kidneys may fuse together at their hila, and they usu-
ally remain in the pelvis. The two kidneys together form a
rosette (see CD Fig. 21-3). This is the result of the early
Unilateral Double Kidney
fusion of the two ureteric buds in the pelvis.
The kidney on one side may be double, with separate
ureters and blood vessels. In unilateral double kidney, the
Supernumerary Renal Arteries
ureteric bud on one side crosses the midline as it ascends,
and its upper pole fuses with the lower pole of the normally
Supernumerary renal arteries are relatively common. They
placed kidney (see CD Fig. 21-3). Here again, angulation of
represent persistent fetal renal arteries, which grow in
374
Chapter 21
sequence from the aorta to supply the kidney as it ascends
lower groups of calyces. The cause is a premature division of
from the pelvis. Their occurrence is clinically important be-
the ureteric bud near its termination.
cause a supernumerary artery may cross the pelviureteral
junction and obstruct the outflow of urine, producing dila-
Bifid Ureter
tion of the calyces and pelvis, a condition known as
hydronephrosis (see CD Fig. 21-3).
In bifid ureter, the ureters may join in the lower third of
their course, may open through a common orifice into the
bladder, or may open independently into the bladder (see
CD Fig. 21-4). In the latter case, one ureter crosses its fellow
CONGENITAL
and may produce urinary obstruction. The cause of bifid
ureter is a premature division of the ureteric bud.
ANOMALIES OF
Cases of double pelvis and double ureters may be found
by chance on radiologic investigation of the urinary tract.
They are more liable to become infected or to be the seat of
THE URETERS
calculus formation than is a normal ureter.
Double Pelvis
Megaloureter
Double pelvis of the ureter is usually unilateral (CD Fig.
Megaloureter may be unilateral or bilateral and shows com-
21-4). The upper pelvis is small and drains the upper group
plete absence of motility (see CD Fig. 21-4). The cause is
of calyces; the larger lower pelvis drains the middle and
unknown. Because of the urinary stasis, the ureter is prone
double pelvis
bifid ureter
bifid ureter
megaloureter
CD Figure 21-4
Some common conge-
ectopic ureteric orifice
postcaval ureter
nital anomalies of the ureter.
The Kidneys, the Ureters, the Bladder, and the Urethra
375
to infection. Plastic surgery is required to improve the rate of
anterior abdominal wall. In cases of acute retention of
drainage.
urine, when catheterization has failed, it is possible to pass
a needle into the bladder through the anterior abdominal
wall above the symphysis pubis, without entering the peri-
Postcaval Ureter
toneal cavity. This is a simple method of draining off the
The right ureter may ascend posterior to the inferior vena
urine in an emergency.
cava and may be obstructed by it (see CD Fig. 21-4). Surgi-
cal rerouting of the ureter with reimplantation of the distal
Cystoscopy
end into the bladder is the treatment of choice.
The mucous membrane of the bladder, the two ureteric ori-
fices, and the urethral meatus can easily be observed by
THE URINARY
means of a cystoscope. With the bladder distended with
fluid, an illuminated tube fitted with lenses is introduced
into the bladder through the urethra. Over the trigone, the
BLADDER
mucous membrane is pink and smooth. If the bladder is par-
tially emptied, the mucous membrane over the trigone re-
mains smooth, but it is thrown into folds elsewhere. The
Palpation of the Urinary Bladder
ureteric orifices are slit-like and eject a drop of urine at in-
The full bladder in the adult projects up into the abdomen
tervals of about 1 minute. The interureteric ridge and the
and may be palpated through the anterior abdominal wall
uvula vesicae can easily be recognized.
above the symphysis pubis.
Bimanual palpation of the empty bladder with or with-
Bladder Injuries
out a general anesthetic is an important method of examin-
ing the bladder. In the male, one hand is placed on the
The bladder may rupture intraperitoneally or extraperi-
anterior abdominal wall above the symphysis pubis, and the
toneally. Intraperitoneal rupture usually involves the supe-
gloved index finger of the other hand is inserted into the rec-
rior wall of the bladder and occurs most commonly when
tum. From their knowledge of anatomy, students can see
the bladder is full and has extended up into the abdomen.
that the bladder wall can be palpated between the examin-
Urine and blood escape freely into the peritoneal cavity.
ing fingers. In the female, an abdominovaginal examination
Extraperitoneal rupture involves the anterior part of the
can be similarly made. In the child, the bladder is in a
bladder wall below the level of the peritoneal reflection; it
higher position than in the adult because of the relatively
most commonly occurs in fractures of the pelvis when
smaller size of the pelvis.
bony fragments pierce the bladder wall. Lower abdominal
pain and blood in the urine (hematuria) are found in most
patients.
Bladder Distension
In young children, the bladder is an abdominal organ,
The normal adult bladder has a capacity of about 500 mL.
so abdominal trauma can injure the empty bladder.
In the presence of urinary obstruction in males, the bladder
may become greatly distended without permanent damage
to the bladder wall; in such cases, it is routinely possible to
Difficulty with Micturition after
drain 1,000 to 1,200 mL of urine through a catheter.
Spinal Cord Injury
Urinary Retention
After injuries to the spinal cord, the nervous control of mic-
turition is disrupted.
In adult males, urinary retention is commonly caused by
The normal bladder is innervated as follows:
obstruction to the urethra by a benign or malignant
enlargement of the prostate. An acute urethritis or prostati-
■ Sympathetic outflow is from the first and second lumbar
tis can also be responsible. Acute retention occurs much less
segments of the spinal cord. The sympathetic nerves (see
frequently in females. The only anatomic cause of urinary
the footnote on text p. 819) inhibit contraction of the de-
retention in females is acute inflammation around the
trusor muscle of the bladder wall and stimulate closure of
urethra (e.g., from herpes).
the sphincter vesicae.
■ Parasympathetic outflow is from the second, third, and
fourth sacral segments of the spinal cord. The parasym-
Suprapubic Aspiration
pathetic nerves stimulate the contraction of the detrusor
As the bladder fills, the superior wall rises out of the pelvis
muscle of the bladder wall and inhibit the action of the
and peels the peritoneum off the posterior surface of the
sphincter vesicae.
376
Chapter 21
■ Sensory nerve fibers enter the spinal cord at the above
■ The automatic reflex bladder (CD Fig. 21-5) occurs af-
segments. The normal process of micturition is described
ter the patient has recovered from spinal shock, provided
on text page 819.
that the cord lesion lies above the level of the parasympa-
thetic outflow (S2, 3, and 4). It is the type of bladder nor-
Disruption of the process of micturition by spinal cord
mally found in infancy. The bladder fills and empties
injuries may produce the following types of bladder:
reflexly. Stretch receptors in the bladder wall are stimu-
■
The atonic bladder occurs during the phase of spinal
lated as the bladder fills, and the afferent impulses pass to
shock, immediately after the injury, and may last for a
the spinal cord (segments S2, 3, and 4). Efferent impulses
few days to several weeks. The bladder wall muscle is re-
pass down to the bladder muscle, which contracts; the
laxed, the sphincter vesicae tightly contracted, and the
sphincter vesicae and the urethral sphincter both relax.
sphincter urethrae relaxed. The bladder becomes greatly
This simple reflex occurs every 1 to 4 hours.
distended and finally overflows. Depending on the level
■ The autonomous bladder (see CD Fig. 21-5) is the con-
of the cord injury, the patient either is or is not aware that
dition that occurs if the sacral segments of the spinal cord
the bladder is full.
are destroyed. The sacral segments of the spinal cord are
bladder wall
spinal cord
sphincter vesicae
prostate
sphincter urethrae
A
CD Figure 21-5
A. Nervous control
of the bladder after section of the
spinal cord in the upper thoracic
region. Destruction of the sacral
segments of the spinal cord. B. The
afferent sensory fibers from the blad-
der entering the central nervous sys-
tem and the parasympathetic efferent
fibers passing to the bladder are
shown; the sympathetic fibers have
B
been omitted for clarity.
The Kidneys, the Ureters, the Bladder, and the Urethra
377
situated in the upper part of the lumbar region of the ver-
passes forward over the scrotum beneath the membranous
tebral column. The bladder is without any external reflex
layer of the superficial fascia, as described on CD page 313.
control. The bladder wall is flaccid, and the capacity of
If the membranous part of the urethra is ruptured, urine
the bladder is greatly increased. It merely fills to capacity
escapes into the deep perineal pouch and can extravasate
and overflows; continual dribbling is the result. The blad-
upward around the prostate and bladder or downward into
der may be partially emptied by manual compression of
the superficial perineal pouch.
the lower part of the anterior abdominal wall, but infec-
tion of the urine and backpressure effects on the ureters
Catheterization
and kidneys are inevitable.
The following anatomic facts should be remembered before
passing a catheter or other instrument along the male
urethra:
THE MALE
■ The external orifice at the glans penis is the narrowest
part of the entire urethra.
URETHRA
■ Within the glans, the urethra dilates to form the fossa ter-
minalis (navicular fossa).
■ Near the posterior end of the fossa, a fold of mucous
Urethral Infections
membrane projects into the lumen from the roof (CD
The most dependent part of the male urethra is that which
Fig. 21-6).
lies within the bulb. Here, it is subject to chronic inflam-
■ The membranous part of the urethra is narrow and fixed.
mation and stricture formation.
■ The prostatic part of the urethra is the widest and most di-
The many glands that open into the urethra—includ-
latable part of the urethra.
ing those of the prostate, the bulbourethral glands, and
■ By holding the penis upward, the S-shaped curve to the
many small penile urethral glands—are commonly the site
urethra is converted into a J-shaped curve.
of chronic gonococcal infection.
If the point of the catheter passes through the external
orifice and is then directed toward the urethral floor until it
Injuries to the Penis
has passed the mucosal fold, it should easily pass along a
normal urethra into the bladder.
Injuries to the penis may occur as the result of blunt trauma,
penetrating trauma, or strangulation. Amputation of the en-
Anatomy of the Procedure
tire penis should be repaired by anastomosis using micro-
of Catheterization
surgical techniques to restore continuity of the main blood
vessels.
The procedure is as follows:
1. The patient lies in a supine position.
Rupture of the Urethra
2. With gentle traction, the penis is held erect at right
Rupture of the urethra may complicate a severe blow on the
angles to the anterior abdominal wall. The lubricated
perineum. The common site of rupture is within the bulb of
catheter is passed through the narrow external urethral
the penis, just below the perineal membrane. The urine
meatus. The catheter should pass easily along the pe-
extravasates into the superficial perineal pouch and then
nile urethra. On reaching the membranous part of the
external urethral
orifice
fossa terminalis
fold of mucous membrane
corona
corpus spongiosum
lacunae
skin
openings of
CD Figure 21-6
The penile urethra slit open to
urethral
show the folds of mucous membrane and glandular
glands
orifices in the roof of the urethra.
378
Chapter 21
urethra, a slight resistance is felt because of the tone of
Because of the urinary incontinence and almost certain
the urethral sphincter and the surrounding rigid per-
occurrence of ascending urinary infection, surgical recon-
ineal membrane.
struction of the bladder is attempted.
3. The penis is then lowered toward the thighs, and the
catheter is gently pushed through the sphincter.
CONGENITAL
4. Passage of the catheter through the prostatic urethra
and bladder neck should not present any difficulty.
ANOMALIES OF
THE URETHRA
THE FEMALE
URETHRA
Meatal Stenosis
The external urinary meatus normally is the narrowest part
Urethral Infections
of the male urethra, but occasionally the opening is exces-
sively small and may cause back pressure effect on the entire
The short length of the female urethra predisposes to as-
urinary system. In severe cases, dilatation of the orifice by in-
cending infection; consequently, cystitis is more common
cision is necessary.
in females than in males.
Hypospadias
Urethral Injuries
Hypospadias is the most common congenital anomaly affect-
Because of the short length of the urethra, injuries are rare. In
ing the male urethra. The external meatus is situated on the
fractures of the pelvis, the urethra may be damaged by shear-
ventral or undersurface of the penis anywhere between the
ing forces as it emerges from the fixed urogenital diaphragm.
glans and the perineum. Five degrees of severity may occur,
the first of which is the most common: (1) glandular, (2) coro-
Catheterization
nal, (3) penile, (4) penoscrotal, and (5) perineal (CD Fig. 21-
8). In all except the first type, the penis is curved in a down-
Because the female urethra is shorter, wider, and more
ward or ventral direction, a condition referred to as chordee.
dilatable, catheterization is much easier than in males.
Types 1 and 2 are caused by a failure of the bud of
Moreover, the urethra is straight, and only minor resistance
ectodermal cells from the tip of the glans to grow into the
is felt as the catheter passes through the urethral sphincter.
substance of the glans and join the entodermal cells lining
the penile urethra. Types 3, 4, and 5 are caused by a failure
of the genital folds to unite on the undersurface of the de-
CONGENITAL
veloping penis and convert the urethral groove into the
penile urethra. In the penoscrotal variety, the genital
swellings fail to fuse completely, so that the meatal orifice
ANOMALIES OF
occurs in the midline of the scrotum. Type 1 requires no
treatment; for the remainder, plastic surgery is necessary.
THE BLADDER
Epispadias
Exstrophy of the Bladder
Epispadias is a relatively rare condition and is more com-
monly found in the male. In the male, the external meatus
(Ectopia Vesicae)
is situated on the dorsal or upper surface of the penis
Exstrophy of the bladder occurs three times more com-
between the glans and the anterior abdominal wall (CD Fig.
monly in males than in females. The posterior bladder wall
21-9). The most severe type is associated with exstrophy of
protrudes through a defect in the anterior abdominal wall
the bladder. In the female, the urethra is split dorsally and is
below the umbilicus (CD Fig. 21-7). The condition is
associated with a double clitoris. It is thought that epispadias
caused by a failure of the embryonic mesenchyme to invade
is caused by failure of the embryonic mesenchyme to
the embryonic disc caudal to the cloacal membrane (CD
develop in the lower part of the anterior abdominal wall, so
Fig.
21-7). The absence of intervening mesenchyme
that when the cloacal membrane breaks down, the urogen-
between the ectoderm and entoderm produces an unstable
ital sinus opens onto the surface of the cranial aspect of the
state, which is followed by breakdown of this area.
penis. Plastic surgery is the required treatment.
The Kidneys, the Ureters, the Bladder, and the Urethra
379
ureteric orifices
trigone of bladder
epispadias
A
embryonic disc
cloacal membrane
primitive streak
tail fold
cloacal membrane
absence of mesenchyme here
B
C
is responsible for exstrophy
normal path taken by
of the bladder
embryonic mesenchyme
umbilical cord
body stalk
CD Figure 21-7
A. Exstrophy of the bladder. B. Dorsal view of the embryonic disc. The
normal path taken by the growing embryonic mesenchyme in the region of the cloaca is
shown. C. Fetus as seen from the side. The head and tail folds have developed, but the
mesenchyme has failed to enter the ventral body wall between the cloaca and the umbili-
cal cord.
380
Chapter 21
1
exstrophy of bladder
2
3
penile
urethra
4
glans
glans
5
scrotum
CD Figure 21-9
Types of epispadias.
anus
CD Figure 21-8
Types of hypospadias: (1) glandular,
(2) coronal, (3) penile, (4) penoscrotal, and (5) perineal.
Ventral flexion (chordee) of the penis also is present.
Clinical Problem Solving Questions
Read the following case histories/questions and give
F. Both kidneys lie on the posterior abdominal wall
the best answer for each.
and are at the same vertebral level.
A 16-year-old boy received a severe kick in the right
A 19-year-old boy was involved in a gang fight. It started
flank while playing football at school. On examination
as an argument but quickly worsened into a street brawl
in the emergency department, his right flank was se-
with the use of knives. He was examined in the emer-
verely bruised, and his right costovertebral angle was ex-
gency department and found to have a bleeding stab
tremely tender on palpation. A specimen of urine
wound in his left flank. A urine specimen revealed
showed microscopic hematuria. A diagnosis of damage
frank blood.
to the right kidney was made.
2. Stab wounds of the kidneys involve other abdominal or-
1. The following statements concerning blunt trauma to
gans in a high percentage of cases. Of the organs listed,
the kidney are correct except which?
which one is least likely to be damaged in this patient?
A. The kidney tends to be crushed between the twelfth
A. Stomach
rib and the vertebral column.
B. Spleen
B. The kidney can be injured by fractures of the twelfth
C. Inferior vena cava
rib (right kidney) or eleventh and twelfth ribs (left
D. Left colic flexure
kidney).
E. Left suprarenal gland
C. In most patients the kidney damage is mild and re-
F. Coils of jejunum
sults in nothing more than microscopic hematuria,
G. Body of the pancreas
as in this patient.
D. In severe kidney lacerations, extensive hemorrhage
An inebriated 40-year-old man was involved in a fight
and extravasation of blood and urine into the
over a woman. The woman’s husband gave the man a se-
pararenal fat occurs.
vere blow to the lower part of the anterior abdominal
E. In severe kidney lacerations, a mass caused by ex-
wall, whereupon he doubled up with pain and collapsed
travasated blood and urine behind the peritoneum
on the floor. On admission to the emergency department
may be palpated, especially on the right side.
of the local hospital, the man was in a state of shock and
The Kidneys, the Ureters, the Bladder, and the Urethra
381
complaining of severe pain in the lower abdominal
5.
The following statements concerning this case are cor-
region. He was unable to pass urine since the fight. A di-
rect except which?
agnosis of ruptured urinary bladder was made.
A. Rupture of the bulbous part of the urethra had taken
place.
3.
The following statements concerning this patient are
B. The urine had escaped from the urethra and ex-
correct except which?
travasated into the superficial perineal pouch.
A. Rectal examination revealed a bulging backward of
C. The urine had passed forward over the scrotum and
the rectovesical fossa.
penis to enter the anterior abdominal wall.
B. Although the patient had consumed a considerable
D. The urine had extended posteriorly into the is-
volume of liquor, dullness was not present on per-
chiorectal fossae.
cussion of the anterior abdominal wall above the
E. The urine was located beneath the membranous
symphysis pubis.
layer of superficial fascia.
C. The urine accumulated in the rectovesical pouch.
D. A full bladder is more likely to be ruptured by a blow
A 34-year-old man was suffering from postoperative re-
to the anterior abdominal wall than an empty
tention of urine after an appendectomy. The patient’s
bladder.
urinary tract was otherwise normal. Because the patient
E. In the adult, as the normal bladder fills, its superior
was in considerable discomfort, the resident decided to
wall extends upward into the abdomen, leaving the
pass a catheter.
covering of parietal peritoneum behind.
6.
The following statements concerning the catheteriza-
A 39-year-old woman was admitted to the local hospital
tion of a male patient are correct except which?
after experiencing a gunshot wound to the lower part of
A. Because the external urethral orifice is the narrow-
her back. Radiographic examination revealed that the
est part of the urethra, once the tip of the catheter
bullet was lodged in the vertebral canal at the level of
has passed this point, further passage should be
the third lumbar vertebra. A comprehensive neurologic
easy.
examination indicated that a complete lesion of the
B. Near the posterior end of the fossa terminalis, a fold
cauda equina had occurred.
of mucous membrane projects from the roof and
may catch the end of the catheter.
4.
The following statements concerning this patient are
C. The membranous part of the urethra is narrow and
likely to be true except which?
fixed and may produce some resistance to the pas-
A. The cauda equina, which consists of anterior and
sage of the catheter.
posterior nerve roots below the level of the first lum-
D. The prostatic part of the urethra is the widest and
bar segment, was sectioned at the level of the third
most easily dilated part of the urethra and should
lumbar vertebra.
cause no difficulty to the passage of the catheter.
B. The preganglionic sympathetic nerve fibers to the
E. The bladder neck is surrounded by the sphincter
vesical sphincter that descend in the anterior roots of
vesicae and always strongly resists the passage of the
the fourth and fifth lumbar nerves were sectioned.
tip of the catheter.
C. The preganglionic parasympathetic fibers to the
detrusor muscle that descend in the anterior roots
7.
An explorer in the Amazon jungle was found alive af-
of the second, third, and fourth sacral nerves were
ter having lost contact with the outside world for 6
sectioned.
months. On physical examination, he was found to be
D. The patient would have an autonomous bladder.
in an emaciated condition. On palpation of the ab-
E. The bladder would fill to capacity and then overflow.
domen, a rounded, smooth swelling appeared in the
F. Micturition could be activated by powerful contrac-
right loin at the end of inspiration. On expiration, the
tion of the abdominal muscles and manual pressure
swelling moved upward and could no longer be felt.
on the anterior abdominal wall in the suprapubic
What anatomic structure could produce such a
region.
swelling?
A 15-year-old boy was taking part in a bicycle race
8.
An intravenous pyelogram revealed that a patient’s left
when, on approaching a steep hill, he stood up on the
kidney was in its normal position, but the right kidney
pedals to increase the speed. His right foot slipped off
was situated in front of the right sacroiliac joint. Can
the pedal and he fell violently, his perineum hitting
you explain this on embryologic grounds?
the bar of the bicycle. Several hours later he was ad-
mitted to the hospital unable to micturate. On exami-
9.
An examination of a patient revealed that she had a
nation, he was found to have extensive swelling of the
horseshoe kidney. What anatomic structure prevents a
penis and scrotum. A diagnosis of ruptured urethra
horseshoe kidney from ascending to a level above the
was made.
umbilicus?
382
Chapter 21
10. An intravenous pyelogram revealed that the calyces
13. Renal pain is a common symptom faced by medical
and pelvis of a patient’s right kidney were grossly dilated
professionals. Describe the course taken by pain nerve
(a condition known as hydronephrosis). What embry-
fibers from the kidneys. In which regions of the body is
ologic anomaly may be responsible for this condition?
pain commonly referred to?
11. A 55-year-old woman was found rolling on her kitchen
14. In relation to abdominal trauma, can you explain the
floor, crying out from agonizing pain in her abdomen.
differences between the bladder position in a child
The pain came in waves and extended from the right
compared with that of an adult? Does the degree of fill-
loin to the groin and to the front of the right thigh. An
ing of the adult bladder affect the signs and symptoms
anteroposterior radiograph of the abdomen revealed a
presented by the patient with a ruptured bladder? Can
calculus in the right ureter. What causes the pain when
you explain how it is possible to pass an aspirating
a ureteral calculus is present? Why is the pain felt in
needle through the anterior abdominal wall into the
such an extensive area? Where does one look for the
full bladder in an adult without entering the peritoneal
course of the ureter in a radiograph? Where along the
cavity?
ureter is a calculus likely to be held up?
15. Why is acute cystitis more common in females than in
12. Which congenital anomaly of the ureter is likely to
males? In anatomic terms explain stress incontinence.
present as a case of urinary incontinence?
Answers and Explanations
1.
F is the correct answer. Because of the large size of the
contracted diaphragm has pushed it down to its lowest
right lobe of the liver, the right kidney lies at a lower
level. When the diaphragm relaxes on expiration, the
level than the left kidney.
kidney returns to its original position.
2.
C is the correct answer. The inferior vena cava lies at
8.
Both kidneys originate in the pelvis and with develop-
some distance from the left flank.
ment rise up on the posterior abdominal wall until the
hili lie opposite the second lumbar vertebra. Occasion-
3.
E is the correct answer. In the adult, as the normal blad-
ally, one of the kidneys fails to reach its normal position.
der fills, its superior wall bulges upward into the
abdomen, peeling off the peritoneum from the poste-
9.
The bridge of renal tissue, which unites the lower poles
rior surface of the anterior abdominal wall (see text
of the two kidneys to form the horseshoe, becomes
Fig. 21-17).
trapped behind the inferior mesenteric artery (see CD
Fig. 21-3). The artery arrests the ascent of the kidneys.
4.
B is the correct answer. The preganglionic sympathetic
nerve fibers to the vesical sphincter descend in the an-
10.
An aberrant renal artery may cross the pelviureteric junc-
terior roots of the first and second lumbar nerves and
tion and obstruct the flow of urine (see CD Fig. 21-3).
were left intact.
11.
Spasm of the smooth muscle in the wall of the pelvis
5.
D is the correct answer. The superficial perineal pouch
and ureter occurs as it attempts to move the calculus
is closed off posteriorly by the attachment of the mem-
down the urinary tract. Afferent pain nerve fibers enter
branous layer of superficial fascia to the posterior mar-
the spinal cord in the first and second lumbar segments.
gin of the urogenital diaphragm (see text Fig. 21-15).
The anterior rami of the first lumbar nerves are distrib-
Because of this attachment, the extravasated urine can-
uted in the skin in the lumbar region and groin as the
not enter the ischiorectal fossae.
iliohypogastric and ilioinguinal nerves. The pain expe-
rienced in the front of the thigh was referred along the
6.
E is the correct answer. The bladder neck does not
femoral branch of the genitofemoral nerve (L1and 2).
cause obstruction to the passage of the catheter. In this
One could look for the course of the ureter in front of
patient, the sphincter may provide some minor resis-
the tips of the transverse processes of the lumbar verte-
tance that is easily overcome.
brae, in front of the sacroiliac joint, and in the region of
7.
The right kidney was felt. It is the only normal kidney
the spine of the ischium. A calculus is likely to be held
that can be palpated. The lower pole may be felt in a
up at the pelviureteric junction, where the ureter
thin person at the end of inspiration, when the
crosses the pelvic brim and where it enters the bladder.
The Kidneys, the Ureters, the Bladder, and the Urethra
383
12.
The congenital anomaly is a case of bifid ureters in
When the bladder is empty, the anterior wall of the
which one ureter opens into the urinary tract below the
bladder lies behind the symphysis pubis. Trauma to the
bladder sphincter in the male, or into the vagina in the
lower abdomen in these circumstances may not dam-
female (see CD Fig. 21-4).
age the bladder. However, if the pubic bones are frac-
tured, the anterior wall of the bladder may be damaged
13.
Renal pain may result from stretching the renal capsule
by bone fragments, and urine escapes below the reflec-
or spasm of the smooth muscle in the pelvis or the
tion of the peritoneum and does not enter the peri-
ureter. The afferent nerve fibers pass through the renal
toneal cavity. Lower abdominal pain and hematuria are
plexus around the renal artery and ascend to the spinal
present in the majority of such patients.
cord through the lowest thoracic splanchnic nerve and
It is possible to pass an aspirating needle through
the sympathetic trunk. They enter the twelfth thoracic
the lower part of the anterior abdominal wall into the
spinal nerve through the white rami communicantes
full bladder in an adult without entering the peritoneal
and the twelfth thoracic segment of the spinal cord
cavity. This can be explained because as the bladder
through the posterior root of the spinal nerve. The pain
fills, the superior wall rises and strips the peritoneum
fibers are then believed to ascend to the brain in the lat-
off the lower part of the anterior abdominal wall.
eral spinal thalamic tracts. The pain is referred along
Thus, the aspirating needle will enter the bladder be-
the distribution of the subcostal nerve (T12) to the flank
low the peritoneal reflection and avoid the peritoneal
and the anterior abdominal wall.
cavity.
14.
In young children, the empty bladder lies in the ab-
domen; later, as the pelvis enlarges, the bladder sinks to
15.
Acute cystitis is much more common in females than
become a pelvic organ.
males because the urethra is much shorter. In females
In adults, the full bladder lies behind the lower part
the urethra measures 1.5 in. long, whereas in males the
of the anterior abdominal wall. Severe trauma to the
urethra measures about 8 in. long, and thus bacteria
lower abdomen in patients with a full bladder may
have a shorter distance to travel in the female.
cause the superior wall of the bladder to rupture into
Stress incontinence usually follows a difficult
the peritoneal cavity. The blood and urine irritates the
childbirth, where there has been injury to the pelvic
peritoneum, causing lower abdominal tenderness and
floor. This results in an alteration in the position of the
later muscle rigidity.
bladder neck relative to the urethra.
The Male Genital
Organs, the Penis, and
the Scrotum
22
Chapter Outline
The Scrotum
388
The Bulbourethral Glands
391
Lymph Drainage of the Scrotum
388
Infection of the Bulbourethral Glands
391
Hydrocele
388
The Penis
391
The Testis and the Epididymis
388
Circumcision
391
Varicocele
388
Urethral Infection
391
Malignant Tumor of the Testis
389
Catheterization
391
Torsion of the Testis
389
Blunt Trauma to the Penis
391
Congenital Anomalies of the Testis
389
Penetrating Trauma to the Penis
391
Appendix of the Testis and Appendix of the
Strangulation of the Penis
391
Epididymis
389
Phimosis
392
The Vas Deferens
390
Erection and Ejaculation after Spinal Cord Injuries
392
Vasectomy
390
Congenital Anomalies of the Penis
392
The Prostate
390
Meatal Stenosis
392
Prostate Examination
390
Hypospadias
392
Prostate Activity and Disease
390
Epispadias
392
Benign Enlargement of the Prostate
390
Clinical Problem Solving Questions
392
Prostate Cancer and the Prostatic Venous Plexus
390
Answers and Explanations
393
THE TESTIS AND
THE SCROTUM
THE EPIDIDYMIS
Lymph Drainage of the Scrotum
It is important to remember that the lymph drainage of the
Varicocele
scrotal wall, including the fascia and tunica vaginalis, is into
the superficial inguinal nodes. The lymph drainage of the
A varicocele is a condition in which the veins of the
testis and epididymis (which develop on the posterior ab-
pampiniform plexus are elongated and dilated. It is a com-
dominal wall) is into the lumbar or paraaortic nodes at the
mon disorder in adolescents and young adults, with most oc-
level of the first lumbar vertebra.
curring on the left side. This is thought to be because the
right testicular vein joins the low-pressure inferior vena
cava, whereas the left vein joins the left renal vein, in which
Hydrocele
the venous pressure is higher. Rarely, malignant disease of
This is an accumulation of fluid within the tunica
the left kidney extends along the renal vein and blocks the
vaginalis. Most hydroceles are idiopathic, but some may be
exit of the testicular vein. A rapidly developing left-sided
caused by spread of infection from the testis or epididymis.
varicocele should therefore always lead one to examine the
Tapping a hydrocele is described on CD page 314.
left kidney.
The Male Genital Organs, the Penis, and the Scrotum
389
■ Imperfect descent (cryptorchidism):
Malignant Tumor of the Testis
Incomplete descent (CD Fig. 22-1), in which the
testis, although traveling down its normal path, fails to
A malignant tumor of the testis spreads upward via the lymph
reach the floor of the scrotum. It may be found within the
vessels to the lumbar (paraaortic) lymph nodes at the level of
abdomen, within the inguinal canal, at the superficial
the first lumbar vertebra. It is only later, when the tumor
inguinal ring, or high up in the scrotum.
spreads locally to involve the tissues and skin of the scrotum,
Maldescent (CD Fig. 22-2), in which the testis
that the superficial inguinal lymph nodes are involved.
travels down an abnormal path and fails to reach the
scrotum. It may be found in the superficial fascia of the
Torsion of the Testis
anterior abdominal wall above the inguinal ligament, in
front of the pubis, in the perineum, or in the thigh.
Torsion of the testes is a rotation of the testis around the sper-
matic cord within the scrotum. It is often associated with an
It is necessary for the testes to leave the abdominal cav-
excessively large tunica vaginalis. Torsion commonly occurs
ity because the temperature there retards the normal process
in active young men and children and is accompanied by
of spermatogenesis. If an incompletely descended testis is
severe pain. If not treated quickly, the testicular artery may
brought down into the scrotum by surgery before puberty, it
be occluded, followed by necrosis of the testis.
will develop and function normally. A maldescended testis,
although often developing normally, is susceptible to trau-
matic injury and, for this reason, should be placed in the
scrotum. Many authorities believe that the incidence of tu-
CONGENITAL
mor formation is greater in testes that have not descended
into the scrotum.
ANOMALIES OF
THE TESTIS
Appendix of the Testis and
The testis may be subject to the following congenital
Appendix of the Epididymis
anomalies:
These are embryologic remnants found at the upper poles of
■ Anterior inversion, in which the epididymis lies anteri-
these organs that may become cystic. The appendix of the
orly and the testis and the tunica vaginalis lie posteriorly
testis is derived from the paramesonephric ducts, and the ap-
■ Polar inversion, in which the testis and epididymis are
pendix of the epididymis is a remnant of the mesonephric
completely inverted
tubules.
1
2
3
4
CD Figure 22-1
Four degrees of incomplete descent
of the testis. 1. In the abdominal cavity close to the
deep inguinal ring. 2. In the inguinal canal. 3. At
the superficial inguinal ring. 4. In the upper part of
scrotum.
390
Chapter 22
estrogens circulating in the bloodstream. The secretions of
1
the prostate are poured into the urethra during ejaculation
and are added to the seminal fluid. Acid phosphatase is an
2
important enzyme present in the secretion in large
4
amounts. When the glandular cells producing this enzyme
cannot discharge their secretion into the ducts, as in carci-
noma of the prostate, the serum acid phosphatase level of
the blood rises.
It has been shown that trace amounts of proteins
produced specifically by prostatic epithelial cells are found
in peripheral blood. In certain prostatic diseases, notably
1
cancer of the prostate, this protein appears in the blood in
increased amounts. The specific protein level can be mea-
2
sured by a simple laboratory test called the PSA (prostatic-
3
specific antigen) test.
Benign Enlargement of the Prostate
Benign enlargement of the prostate is common in men
older than 50 years. The cause is possibly an imbalance in
CD Figure 22-2
Four types of maldescent of the testis. 1. In
the hormonal control of the gland. The median lobe of the
the superficial fascia of the anterior abdominal wall, above
gland enlarges upward and encroaches within the sphinc-
the superficial inguinal ring. 2. At the root of the penis. 3. In
ter vesicae, located at the neck of the bladder. The leakage
the perineum. 4. In the thigh.
of urine into the prostatic urethra causes an intense reflex
desire to micturate. The enlargement of the median and
lateral lobes of the gland produces elongation and lateral
compression and distortion of the urethra so that the pa-
THE VAS DEFERENS
tient experiences difficulty in passing urine and the stream
is weak. Backpressure effects on the ureters and both
kidneys are a common complication. The enlargement
Vasectomy
of the uvula vesicae (owing to the enlarged median lobe)
Bilateral vasectomy is a simple operation performed to pro-
results in the formation of a pouch of stagnant urine
duce infertility. Under local anesthesia, a small incision is
behind the urethral orifice within the bladder (CD Fig.
made in the upper part of the scrotal wall, and the vas def-
22-3). The stagnant urine frequently becomes infected,
erens is divided between ligatures. Spermatozoa may be pre-
and the inflamed bladder (cystitis) adds to the patient’s
sent in the first few postoperative ejaculations, but that is
symptoms.
simply an emptying process. Now only the secretions of the
In all operations on the prostate, the surgeon regards
seminal vesicles and prostate constitute the seminal fluid,
the prostatic venous plexus with respect. The veins have thin
which can be ejaculated as before.
walls, are valveless, and are drained by several large trunks
directly into the internal iliac veins. Damage to these veins
can result in a severe hemorrhage.
THE PROSTATE
Prostate Cancer and the Prostatic
Prostate Examination
Venous Plexus
The prostate can be examined clinically by palpation by per-
Many connections between the prostatic venous plexus and
forming a rectal examination (see CD Chapter 19). The ex-
the vertebral veins exist. During coughing and sneezing or
aminer’s gloved finger can feel the posterior surface of the
abdominal straining, it is possible for prostatic venous blood
prostate through the anterior rectal wall.
to flow in a reverse direction and enter the vertebral veins.
This explains the frequent occurrence of skeletal metastases
in the lower vertebral column and pelvic bones of patients
Prostate Activity and Disease
with carcinoma of the prostate. Cancer cells enter the skull
It is now generally believed that the normal glandular
via this route by floating up the valveless prostatic and verte-
activity of the prostate is controlled by the androgens and
bral veins.
The Male Genital Organs, the Penis, and the Scrotum
391
enlarged median lobe of prostate
bladder wall
pouch of stagnant urine
sphincter vesicae
ejaculatory duct
posterior lobe
CD Figure 22-3
Sagittal section of a prostate that
had undergone benign enlargement of the median
lobe. Note the bladder pouch filled with stagnant
urethra
urine behind the prostate.
these reasons, prophylactic circumcision is commonly prac-
THE
ticed. For Jews, it is a religious rite.
BULBOURETHRAL
Urethral Infection
See CD Chapter 21.
GLANDS
Catheterization
Infection of the Bulbourethral
See CD Chapter 21.
Glands
Blunt Trauma to the Penis
The bulbourethral glands are the common sites for chronic
This may cause penile fracture when it is in the erect state.
venereal infection (e.g., gonorrhoea). The organisms reach
A transverse laceration of the fibrous envelopes of the erec-
the gland by ascending from the bulbous part of the urethra
tile tissue of the penis occurs followed by the formation of a
along the duct of the gland.
large hematoma; the base of the penis is the common site of
injury. Rupture of the penile urethra may also occur and is
accompanied by a bloody urethral discharge.
THE PENIS
Penetrating Trauma to the Penis
This may injure the skin, fascia, erectile tissue, and urethra.
Circumcision
Amputation of the entire penis should be repaired by anas-
Circumcision is the operation of removing the greater part
tomosis using microsurgical techniques to restore continu-
of the prepuce, or foreskin. In many newborn males, the
ity of the main blood vessels.
prepuce cannot be retracted over the glans. This can result
in infection of the secretions beneath the prepuce, leading
Strangulation of the Penis
to inflammation, swelling, and fibrosis of the prepuce. Re-
peated inflammation leads to constriction of the orifice of
Strangulation of the penis by means of a ring or ligature may
the prepuce (phimosis) with obstruction to urination. It is
cause ischemia of the entire penis. It is imperative that the
now generally believed that chronic inflammation of the
constriction be removed without delay to avoid compromis-
prepuce predisposes to carcinoma of the glans penis. For
ing the blood supply.
392
Chapter 22
damage to the spinal cord results in loss of ejaculation.
Phimosis
Later, reflex ejaculation may be possible in patients with
spinal cord transections in the thoracic or cervical regions.
In this condition the opening in the prepuce is narrowed so
that it is impossible to retract the prepuce over the glans pe-
nis. Occasionally the narrowing is so extreme that the uri-
nary flow is obstructed. The usual cause of the condition is
CONGENITAL
infection under the prepuce, causing fibrosis and subse-
quent contraction of the prepuce.
ANOMALIES OF
Erection and Ejaculation after
THE PENIS
Spinal Cord Injuries
Meatal Stenosis
Erection of the penis is controlled by the parasympathetic
nerves that originate from the second, third, and fourth
See CD Chapter 21.
sacral segments of the spinal cord. Bilateral damage to the
reticulospinal nerve tracts in the spinal cord will result in
Hypospadias
loss of erection. Later, when the effects of spinal shock have
disappeared, spontaneous or reflex erection may occur if the
See CD Chapter 21.
sacral segments of the spinal cord are intact.
Ejaculation is controlled by sympathetic nerves
Epispadias
that originate in the first and second lumbar segments of
the spinal cord. As in the case of erection, severe bilateral
See CD Chapter 21.
Clinical Problem Solving Questions
Read the following case histories/questions and give
While bathing her 5-month-old boy, a mother no-
the best answer for each.
ticed that his penis tended to curve downward. She
decided to seek advice from a pediatrician.
A 55-year-old man was admitted to the hospital with a large
hard, fixed, intraabdominal mass. On examination of the ab-
2. The pediatrician examined the child and made the
domen, the mass was situated on the transpyloric plane and
following possible correct observations and statements
appeared to be attached to the posterior abdominal wall.
except which?
The inguinal lymph nodes were normal.
A. The penis had a definite downward curvature
1. The symptoms and signs displayed by this patient can
(chordee).
be explained by the following statements except which?
B. Both testes were in the scrotum.
A. Radiologic examination of the stomach showed
C. The external urethral meatus opened halfway along
nothing abnormal.
the undersurface of the penis.
B. The right testicle was enlarged and was much
D. The fusion of the genital folds on the ventral or un-
harder than normal.
dersurface of the shaft of the penis was incomplete
C. A diagnosis of malignant disease of the right testis
so that the urethra opened on the ventral surface.
was made.
E. The condition is a rare congenital anomaly.
D. The malignant tumor had metastasized to the lum-
bar lymph nodes lying on the transpyloric plane on
3. The pediatrician made the following possible correct
the posterior abdominal wall, which is the normal
statements to the mother regarding the diagnosis and
lymphatic drainage of the testis.
treatment except which?
E. In malignant disease of the testis the superficial
A. The child had hypospadias associated with chordee.
inguinal lymph nodes only become involved if the
B. The proximal portion of the penile urethra had
tumor spreads to involve the scrotal skin.
developed normally but was incomplete.
F. The normal testis is tethered to the skin of the
C. The bud of cells (ectodermal) on the tip of the glans
scrotum.
penis had failed to grow into the substance of the
The Male Genital Organs, the Penis, and the Scrotum
393
glans and join with the cells (entodermal cells) of
left thigh. What is the diagnosis? Is surgical treatment
the penile urethra.
required?
D. The treatment is the surgical correction of the
8.
A 25-year-old man developed a swelling above the me-
chordee, which is followed by the plastic recon-
dial end of the right inguinal ligament. It was associated
struction of the penile urethra.
with a dull, aching pain, bit it did not expand on cough-
E. In view of the delicate tissues involved, the treat-
ing. On palpation, the swelling appeared to fluctuate,
ment should be delayed until the child is at least 10
and on grasping the right testis through the scrotal wall
years old.
and gently pulling it inferiorly, the swelling moved me-
4.
A 65-year-old man with a history of prostatic disease was
dially along the inguinal canal. What was the swelling?
found on radiographic examination of his skeleton to
Why did it move with the testis?
have extensive carcinomatous metastases in his skull
9.
A patient suffering from tuberculosis of the left epi-
and lumbar vertebrae. His PAS levels in his blood were
didymis was found to have an ulcer on the posterior sur-
very much higher than normal. Using your knowledge
face of the scrotum. Which group of lymph nodes
of anatomy, can you suggest a possible route taken by
would you examine for local spread of the disease?
the cancer cells as they migrated from the prostate to (1)
the lumbar vertebrae and (2) the skull?
10.
A resident was asked to examine the vas deferens of a pa-
tient. Where would you examine the vas deferens and
5.
An 88-year-old man had a history of prostatic disease.
what does a normal vas feel like?
His latest symptoms included difficulty in starting to
micturate, a poor urinary stream, and difficulty in stop-
11.
In a patient with a history of venereal disease, a large,
ping the flow of urine. Which lobe or lobes of the
fluctuant swelling developed in front of the left testis.
prostate are related to the sphincter vesicae? The en-
From your knowledge of anatomy, and given that there
largement of which lobe is likely to interfere with the
is fluid present in the scrotum, where in the scrotum is
sphincter’s function?
the fluid likely to collect?
6.
A 6-year-old boy was examined by a pediatrician and
12.
A 50-year-old man was found on examination to have a
found to have no testicle present in the right side of his
small cystic swelling above his right testis. What
scrotum. On careful palpation, a deep, firm ovoid struc-
anatomic structure is likely to be involved? Can you ex-
ture could be felt above the medial part of the inguinal
plain the presence of this structure embryologically?
ligament. What is the diagnosis? Is surgical treatment
13.
A 25-year-old man was found, during a physical exami-
necessary?
nation, to have an abnormal scrotum. On feeling the
7.
An 18-year-old boy, at a medical examination for ad-
scrotum with the palm of the hand, it felt like a bag of
mission to the army, was found to have no testis in the
worms. This situation was caused by an enlargement of
left side of the scrotum. Nothing abnormal could be
the pampiniform plexus on the left side. The physician
palpated in the inguinal canal, but a small, firm ovoid
examined the scrotum and then the left kidney. Can
structure could be felt in front of the upper part of the
you explain why he should examine the left kidney?
Answers and Explanations
1. F is the correct answer. The normal testis is freely mo-
4. The prostatic venous plexus is drained into the internal
bile within the scrotum and is not tethered to the sub-
iliac veins. Large valveless veins also connect the plexus
cutaneous tissue or skin.
to the valveless vertebral veins. On coughing or sneez-
ing, the blood may be forced from the prostatic plexus
2. E is the correct answer. The condition is one of the
in the pelvis into the vertebral veins. Dislodged prosta-
most common congenital anomalies affecting the male
tic cancer cells may be carried along this route to the
urethra.
vertebral column. They may also pass up the vertebral
3. E is the correct answer. The surgical treatment should
plexus to enter the veins of the skull.
start at about the age of 2 years and be complete before
the child goes to school. Little boys like to look the same
5. The median (middle) lobe of the prostate is located be-
as other little boys.
tween the prostatic urethra and the ejaculatory ducts,
394
Chapter 22
just inferior to the sphincter vesicae. Benign hypertro-
tunica vaginalis, the cyst was pulled medially by the
phy of the median lobe results in its upward expansion
fibrous strand.
within the sphincter vesicae. The sphincter can no
9.
The skin of the scrotum, the fascia, and the tunica vagi-
longer function effectively, and urine continues to drib-
nalis drain their lymph into the superficial inguinal
ble into the urethra, giving the patient an intense desire
lymph nodes.
to continue to micturate.
10.
Palpate the upper part of the scrotum between finger
6.
The boy had an incompletely descended testis on the
and thumb, and you can roll the vas deferens as a cord-
right side. The right testis was situated in the inguinal
like structure. It has a smooth external wall and is firm
canal. Spontaneous descent of the testis usually occurs
in consistency. Remember there are two sides and to
without treatment. The injection of gonadotropic hor-
always compare the two.
mone can be used to speed up the descent. However, if
the descent has not occurred by the age of 10 years, sur-
11.
The tunica vaginalis covers the front and sides of the
gical treatment is necessary to place the testis in the
testis, and the visceral layer is in direct contact with the
scrotum. The high temperature of the abdominal cavity
tunica albuginea of the testis. Infection causes an ex-
and inguinal canal inhibits normal spermatogenesis.
cessive production and accumulation of fluid within
the tunica, a condition known as hydrocele.
7.
The boy had a maldescended testis on the left side.
Instead of following the gubernaculum down into the
12.
The patient has a cyst of the appendix of the testis, a
scrotum, it passed laterally and came to rest in the su-
structure that is derived embryologically from the para-
perficial fascia in the upper part of the left thigh. A
mesonephric duct.
maldescended testis is very prone to injury and should
13.
The left pampiniform plexus is drained by the left
be placed in the scrotum by surgical means.
testicular vein, which is drained into the left renal vein.
8.
The patient had a right encysted hydrocele of the sper-
A malignant tumor of the left kidney could spread along
matic cord. This is a cyst in the remnant of the upper
the left renal vein, blocking the exit of the left testicular
part of the processus vaginalis and is connected to the
vein and causing congestion and varicosity of the left
tunica vaginalis by a fibrous strand (a further remnant
pampiniform plexus. This is a rare cause. The majority
of the processus). On pulling down the testis and the
of varicoceles are idiopathic.
The Perineum, the
Female Genital Organs,
and Childbirth
23
Chapter Outline
The Vulva
397
The Anatomy of Emergency Cesarean
Section
403
Vulval Infection
397
The Anatomy of the Technique
403
The Vulva and Pregnancy
397
Prolapse of the Uterus
403
The Urethra
397
Urethral Infection
397
Hysterectomy and Damage to the Ureter
404
Urethral Injuries
397
Congenital Anomalies of the Uterus
404
Catheterization
397
Agenesis of the Uterus
404
The Ovary
397
Infantile Uterus
404
Position of the Ovary
397
Failure of Fusion of the Paramesonephric Ducts
404
Cysts of the Ovary
397
The Placenta
404
Congenital Anomalies of the Ovary
397
The Placenta and Bleeding in Late Pregnancy
404
Ovarian Dysgenesis
397
Placenta Previa
404
Imperfect Descent of the Ovary
397
Placental Abruption
405
The Uterine Tube
397
The Vagina
405
The Uterine Tube as a Conduit for Infection
397
Vaginal Examination
405
Pelvic Inflammatory Disease
397
Prolapse of the Vagina
406
Ectopic Pregnancy
398
Culdocentesis
406
Anatomic Structures through which the
Tubal Ligation
398
Needle Passes
406
The Uterus
398
Anatomic Features of the Complications of
Rectal Examination
398
Culdocentesis
406
Bimanual Pelvic Examination of the Uterus
398
Vaginal Trauma
406
Congenital Anomalies of the Vagina
406
Basic Anatomy of a Normal Pregnancy
399
Vaginal Agenesis
406
Ultrasound Anatomy of the Developing Fetus
400
Double Vagina
406
Anatomy of Childbirth
400
Imperforate Vagina and Imperforate Hymen
406
Labor Pains
400
Visceral Pelvic Fascia
406
Labor
400
Visceral Pelvic Fascia and Infection
406
The Uterus in Pregnancy
401
The Pelvic Peritoneum
406
The Role of the Uterus in the Onset of Labor
401
The Rectouterine Pouch and Disease
406
Injury to the Perineum during Childbirth
402
Varicosed Veins and Hemorrhoids in Pregnancy
403
Clinical Problem Solving Questions
407
Answers and Explanations
408
The Perineum, the Female Genital Organs, and Childbirth
397
broad ligament is lax, and the ovaries may prolapse into the
rectouterine pouch (pouch of Douglas). In these circum-
THE VULVA
stances, the ovary may be tender and cause discomfort on
sexual intercourse (dyspareunia). An ovary situated in the
rectouterine pouch may be palpated through the posterior
Vulval Infection
fornix of the vagina.
In the region of the vulva, the presence of numerous glands
and ducts opening onto the surface makes this area prone to
Cysts of the Ovary
infection (see text Fig. 23-7). The sebaceous glands of the
Follicular cysts are common and originate in unruptured
labia majora, the ducts of the greater vestibular glands, the
graafian follicles; they rarely exceed 0.6 in. (1.5 cm) in di-
vagina (with its indirect communication with the peritoneal
ameter. Luteal cysts are formed in the corpus luteum.
cavity), the urethra, and the paraurethral glands can all be-
Fluid is retained, and the corpus luteum cannot become
come infected. The vagina itself has no glands and is lined
fibrosed. Luteal cysts rarely exceed 1.2 in. (3 cm) in
with stratified squamous epithelium. Provided that the pH
diameter.
of its interior is kept low, it is capable of resisting infection to
a remarkable degree.
Congenital Anomalies of the Ovary
The Vulva and Pregnancy
Ovarian Dysgenesis
An important sign in the diagnosis of pregnancy is the ap-
Complete failure of both ovaries to develop is found in
pearance of a bluish discoloration of the vulva and vagina as
Turner’s syndrome. The classic features of this syndrome
a result of venous congestion. It appears at the eighth to
are webbed neck, short stocky build, increased carrying an-
twelfth week and increases as the pregnancy progresses.
gle of the elbows, lack of secondary sex characteristics, and
amenorrhea.
THE URETHRA
Imperfect Descent of the Ovary
The ovary may fail to descend into the pelvis or very rarely
Urethral Infection
may be drawn downward with the round ligament of the
uterus into the inguinal canal or even into the labium
The short length of the female urethra predisposes to as-
majus.
cending infection; consequently, cystitis is more common
in females than in males.
THE UTERINE
Urethral Injuries
Because of the short length of the urethra, injuries are rare. In
TUBE
fractures of the pelvis, the urethra may be damaged by shear-
ing forces as it emerges from the fixed urogenital diaphragm.
The Uterine Tube as a Conduit
for Infection
Catheterization
The uterine tube lies in the upper free border of the broad
Because the female urethra is shorter, wider, and more di-
ligament (see text Fig. 23-10) and is a direct route of com-
latable, catheterization is much easier than in males. More-
munication from the vulva through the vagina and uterine
over, the urethra is straight, and only minor resistance is felt
cavity to the peritoneal cavity.
as the catheter passes through the urethral sphincter.
Pelvic Inflammatory Disease
THE OVARY
The pathogenic organism(s) enter the body through sexual
contact and ascend through the uterus and enter the uter-
ine tubes. Salpingitis may follow, with leakage of pus into
Position of the Ovary
the peritoneal cavity, causing pelvic peritonitis. A pelvic
The ovary is kept in position by the broad ligament and the
abscess usually follows, or the infection spreads farther,
mesovarium (see text Fig. 23-10). After pregnancy, the
causing general peritonitis.
398
Chapter 23
thin-walled uterine tube
fundus of uterus
thick decidua lining
CD Figure 23-1
An ectopic pregnancy
mucous plug
body of uterus
located where the ampulla of the uterine
tube narrows down to join the isthmus.
Note the thin tubal wall compared to the
thick decidua that lines the body of the
uterus.
Anteriorly: The anterior structures include the
Ectopic Pregnancy
following:
Implantation and growth of a fertilized ovum may occur out-
1. Opposite the terminal phalanx are the rectouterine
side the uterine cavity in the wall of the uterine tube (CD Fig.
pouch of Douglas, the vagina, and the cervix.
23-1). This is a variety of ectopic pregnancy. There being no
2. Opposite the middle phalanx are the urogenital di-
decidua formation in the tube, the eroding action of the tro-
aphragm and the vagina.
phoblast quickly destroys the wall of the tube. Tubal abortion
or rupture of the tube, with the effusion of a large quantity of
3. Opposite the proximal phalanx are the perineal body
blood into the peritoneal cavity, is the common result.
and the lower part of the vagina.
The blood pours down into the rectouterine pouch
Posteriorly: The posterior structures include the
(pouch of Douglas) or into the uterovesical pouch. The blood
following:
may quickly ascend into the general peritoneal cavity, giving
rise to severe abdominal pain, tenderness, and guarding. Irri-
1. The sacrum, coccyx, and anococcygeal body
tation of the subdiaphragmatic peritoneum (supplied by
Laterally: The lateral structures include the following:
phrenic nerves C3, C4, and C5) may give rise to referred pain
to the shoulder skin (supraclavicular nerves C3 and C4).
1. The ischiorectal fossae and ischial spines
Tubal Ligation
Bimanual Pelvic Examination of
Ligation and division of the uterine tubes is a method of ob-
the Uterus
taining permanent birth control and is usually restricted to
women who already have children. The ova that are dis-
A great deal of useful clinical information can be obtained
charged from the ovarian follicles degenerate in the tube
about the state of the uterus, uterine tubes, and ovaries from
proximal to the obstruction. If, later, the woman wishes to
a bimanual examination. The examination is easiest in
have an additional child, restoration of the continuity of the
parous women who are able to relax while the examination is
uterine tubes can be attempted, and, in about 20% of
in progress. In patients in whom it causes distress, the exami-
women, fertilization occurs.
nation may be performed under an anesthetic. With the blad-
der empty, the vaginal portion of the cervix is first palpated
with the index finger of the right hand. The external os is cir-
THE UTERUS
cular in the nulliparous woman but has anterior and posterior
lips in the multiparous woman. The cervix normally has the
consistency of the end of the nose, but in the pregnant uterus
Rectal Examination
it is soft and vascular and has the consistency of the lips. The
The following structures can be palpated by the gloved in-
left hand is then placed gently on the anterior abdominal wall
dex finger inserted into the anal canal and rectum in the
above the symphysis pubis, and the fundus and body of the
healthy patient (CD Fig. 23-2 and see CD Fig. 23-8).
uterus may be palpated between the abdominal and vaginal
The Perineum, the Female Genital Organs, and Childbirth
399
external os of uterus
A
head of baby
anterior lip of cervix
CD Figure 23-2
A. Rectal exami-
nation in a pregnant woman
showing how it is possible to
palpate the cervix through the
site for episiotomy
anterior rectal wall. B. Position of
the episiotomy incision in a
woman during the second stage
of labor. The baby’s head is pre-
B
senting at the vaginal orifice.
fingers situated in the anterior fornix. The size, shape, and
23-3). The ascent of the fundus is fairly uniform. At 12
mobility of the uterus can then be ascertained.
weeks, it lies just above the symphysis pubis; at 20 weeks, it
In most women, the uterus is anteverted and anteflexed.
lies about halfway between the symphysis pubis and the um-
A retroverted, retroflexed uterus can be palpated through
bilicus; at 24 weeks, it is level with the umbilicus; at 32
the posterior vaginal fornix.
weeks, it lies halfway between the umbilicus and the
xiphoid process; at 36 weeks, it has reached the xiphoid
process; and at 40 weeks; in the first pregnancy, the fetus
sinks downward as the presenting part enters the pelvic cav-
BASIC ANATOMY OF
ity and the fundus again takes up the position halfway be-
tween the xiphoid and the umbilicus. In multipara, the pre-
A NORMAL
senting part of the fetus descends at a later date.
Further evidence of fetal growth can be determined by
PREGNANCY
the mother first recognizing movements of the fetus (quick-
ening), which usually occurs between the sixteenth and twen-
As the fetus enlarges, the uterus increases in size, and
tieth weeks of pregnancy. Fetal heart sounds may be heard as
the fundus gradually rises out of the pelvic cavity (CD Fig.
early as the twelfth week, when a Doppler stethoscope is used.
400
Chapter 23
part of the anterior abdominal wall and the lower part of the
32 weeks
back (dermatomes T10 through T12).
24 weeks
Labor
Labor, or parturition, is the series of processes by which the
baby, the fetal membranes, and the placenta are expelled
from the genital tract of the mother. Forceful uterine con-
tractions occurring at regular intervals indicate the onset of
symphysis pubis
labor. The first stage is dilatation of the cervix. The second
stage is expulsion of the fetus. The third stage begins im-
mediately following the delivery of the baby and ends with
expulsion of the placenta and fetal membranes.
Duration of labor: This depends on (1) the strength and
36 weeks
frequency of the uterine contractions and (2) the resis-
40 weeks
tance offered to the passage of the baby by the bony pelvis
32 weeks
28 weeks
and the soft tissues of the lower part of the genital tract,
24 weeks
namely, the cervix, the vagina, the pelvic floor, and the
20 weeks
perineum. The approximate length of each stage is as fol-
lows: first stage, 9 1/2 hours; second stage, 50 minutes;
12 weeks
and third stage, 10 minutes. In multigravida the duration
of the first and second stages is shorter because of the re-
CD Figure 23-3
The height of the fundus of the uterus at
duced resistance offered by the maternal soft tissues.
various weeks of pregnancy. A. As seen in sagittal section.
Processes of Labor: During the first stage of labor, the
B. As felt through the anterior abdominal wall.
liquor amnii and the fetal membranes are forced down
into the cervical canal as a hydrostatic wedge, and the
cervix slowly dilates (CD Fig. 23-4). The pulling away of
the membranes from the uterine wall in the region of the
Ultrasound Anatomy of the
internal os of the cervix causes a little bleeding, and this,
together with the cervical plug of mucus that fills the
Developing Fetus
canal of the cervix, forms the so-called bloody show. The
rupture of the membranes and the escape of the liquor
With sequential longitudinal and transverse scans of the
amnii usually occur when the first stage of labor is well
uterus, the developing fetus, amniotic fluid, and placenta
advanced. The escape of the liquor amnii allow the
can be studied. The gestational sac can be recognized at
uterus to exert pressure directly on the baby and force it
about 5 weeks after the first day of the last menstrual period.
down.
By 6 to 7 weeks the fetal pole (extreme end or ends of fetus)
can be visualized, and the beating heart can be seen. Later,
During the second stage of labor, the combined actions
the fetal head, trunk, and limbs can be identified (see text
of the very strong uterine contractions and the reflex and
Fig. 23-30).
voluntary contractions of the abdominal muscles force the
baby through the maternal passages (CD Fig. 23-5).
The pelvic floor, formed by the levatores ani and coc-
Anatomy of Childbirth
cygeus muscles, serves an important function during the
second stage of labor. From their origin on the two sides of
Labor Pains
the pelvis, the muscle fibers slope downward and backward
The underlying cause of labor pains is believed to be the
in the midline, producing a gutter that slopes downward
anoxia of the uterine muscle brought about by the uterine
and forward. To begin with, the long axis of the baby’s
contractions. Afferent pain fibers from the fundus and body
head is transversely positioned at the pelvic inlet. When
of the uterus ascend to the spinal cord through the hypogas-
the head reaches the pelvic floor, the gutter shape of the
tric plexuses, entering the cord through the posterior roots of
floor tends to cause the baby’s head to rotate, so that its
the tenth, eleventh, and twelfth thoracic spinal nerves. Sen-
long axis comes to lie in the anteroposterior position, with
sory fibers from the cervix run in the pelvic splanchnic
the occiput anteriorly in the majority. The occipital part of
nerves and enter the spinal cord through the posterior roots
the head now moves downward and forward along the gut-
of the second, third, and fourth sacral nerves. Contraction
ter until it lies under the pubic arch. As the baby’s head
pains from the fundus and body are referred to the lower
passes through the lower part of the birth canal, the small
The Perineum, the Female Genital Organs, and Childbirth
401
uterus
placenta
umbilical cord
amnion and chorion
cervix
vagina
CD Figure 23-4
A. The relation of the
amniotic fluid
fetus to the uterus, placenta, and the
fetal membranes at the fortieth week of
pregnancy. B and C. The cervix dilat-
ing during the first stage of labor as the
result of the fetal membranes being
forced down into the cervical canal as a
hydrostatic
hydrostatic wedge. The bloody show
wedge (bag
consists of the mucous plug from the
of water)
cervical canal mixed with the small
cervical canal
bloody showamount of bleeding that occurs follow-
ing separation of the fetal membrane
mucous plug
from the uterine wall in the region of
vagina
the internal os.
gap that exists in the anterior part of the pelvic floor be-
the afterbirth. The uterine muscle becomes firmly con-
comes enormously enlarged, so that the head may slip
tracted and little bleeding occurs.
through into the perineum. Once the baby has passed
through the perineum, the levatores ani muscles recoil and
The Uterus in Pregnancy
take up their previous position.
The third stage of labor then commences, and the
During pregnancy, the uterus becomes greatly enlarged as
uterus contracts downward so that the fundus lies at the
a result of the increasing production of estrogens and prog-
level of the umbilicus. Rhythmic uterine contractions con-
esterone, first by the corpus luteum of the ovary and later
tinue, as in the second stage, but they are painless. Separa-
by the placenta. At first it remains as a pelvic organ, but by
tion of the placenta from the uterine wall takes place. As the
the third month the fundus rises out of the pelvis, and by
uterus diminishes in size, there is a decrease in the surface
the ninth month it has reached the xiphoid process (see
area at the site of placental attachment. The placenta, being
CD Fig. 23-3). The increase in size is largely a result of
unable to accommodate itself to the decreased area, begins
hypertrophy of the smooth muscle fibers of the my-
to fold up and is squeezed off the uterine wall (CD Fig. 23-
ometrium, although some hyperplasia takes place.
6). Separation takes place at the spongy layer of the decidua,
and some bleeding occurs. In a similar manner, the fetal
Role of the Uterus in the Onset
membranes and the remains of the decidua are squeezed
from the remainder of the uterine wall. As the placenta is fi-
of Labor
nally expelled from the uterus by the uterine contractions,
the membranes that are attached to it are dragged after it
Normally labor takes place at the end of the tenth lunar
and peeled off from the inner surface of the uterus. The ex-
month, at which time the pregnancy is said to be at term.
pelled placenta and fetal membranes are often referred to as
The cause of the onset of labor is not definitely known. By
402
Chapter 23
2
1
CD Figure 23-5
Stages in rotation of
the baby’s head during the second
stage of labor. The shape of the pelvic
floor plays an important part in this
3
process.
the end of pregnancy, the contractility of the uterus has
The uterine muscular activity is largely independent
been fully developed in response to estrogen, and it is par-
of the extrinsic innervation. In women in labor, spinal
ticularly sensitive to the actions of oxytocin at this time. It is
anesthesia does not interfere with the normal uterine con-
possible that the onset of labor is triggered by the sudden
tractions. Severe emotional disturbance, however, can
withdrawal of progesterone. Once the presenting part (usu-
cause premature parturition.
ally the fetal head) starts to stretch the cervix, it is thought
that a nervous reflex mechanism is initiated and increases
Injury to the Perineum during
the force of the contractions of the uterine body.
Childbirth
fetal
The perineal body is a wedge of fibromuscular tissue that
membranes
lies between the lower part of the vagina and the anal canal.
placenta
bladder
It is held in position by the insertion of the perineal muscles
uterus
and by the attachment of the levatores ani muscles. In the
female, it is a much larger structure than in the male, and it
serves to support the posterior wall of the vagina. Damage by
vagina
laceration during childbirth can be followed by permanent
weakness of the pelvic floor.
Few women escape some injury to the birth canal dur-
ing delivery. In most, this is little more than an abrasion of
the posterior vaginal wall. Spontaneous delivery of the child
with the patient unattended can result in a severe tear of the
umbilical cord
lower third of the posterior wall of the vagina, the perineal
body, and overlying skin. In severe tears, the lacerations may
CD Figure 23-6
The third stage of labor showing the sep-
arated placenta with the attached fetal membranes about to
extend backward into the anal canal and damage the exter-
be expelled through the vagina.
nal sphincter. In these cases, it is imperative that an accurate
The Perineum, the Female Genital Organs, and Childbirth
403
repair of the walls of the anal canal, vagina, and perineal
two hemostats; an incision is then made between the
body be undertaken as soon as possible.
hemostats.
In the management of childbirth, when it is obvious to
3. The bladder is identified, and a cut is made in the floor
the obstetrician that the perineum will tear before the
of the uterovesical pouch. The bladder is then sepa-
baby’s head emerges through the vaginal orifice, a planned
rated from the lower part of the body of the uterus and
surgical incision is made through the perineal skin in a
depressed downward into the pelvis.
posterolateral direction to avoid the anal sphincters. This
procedure is known as an episiotomy (see CD Fig. 23-2).
4. The uterus is palpated to identify the presenting part of
Breech deliveries and forceps deliveries are usually pre-
the fetus.
ceded by an episiotomy.
5. A transverse incision about 1 in. (2.5 cm) long is made
into the exposed lower segment of the body of the
Varicosed Veins and Hemorrhoids
uterus. Care is taken that the uterine wall is not imme-
diately penetrated and the fetus injured.
in Pregnancy
6. When the uterine cavity is entered, the amniotic cavity
Varicosed veins and hemorrhoids are common conditions
is opened, and amniotic fluid spurts. The uterine inci-
in pregnancy. The following factors probably contribute to
sion is then enlarged sufficiently to deliver the head and
their cause: pressure of the gravid uterus on the inferior vena
trunk of the fetus. When possible, the large tributaries
cava and the inferior mesenteric vein, impairing venous re-
and branches of the uterine vessels in the myometrial
turn, and increased progesterone levels in the blood, leading
wall are avoided. Great care has to be taken to avoid the
to relaxation of the smooth muscle in the walls of the veins
large uterine arteries that course along the lateral mar-
and venous dilatation.
gin of the uterus.
7. Once the fetus is delivered, the umbilical cord is
clamped and divided.
THE ANATOMY OF
8. The contracting uterus will cause the placenta to bulge
through the uterine incision. The placenta and fetal
EMERGENCY
membranes are then delivered.
9. The uterine incision is closed with a full-thickness con-
CESAREAN SECTION
tinuous suture. The peritoneum over the bladder and
lower part of the uterine body is then repaired to restore
An emergency cesarean section is rarely performed. How-
the integrity of the uterovesical pouch. Finally, the ab-
ever, a physician may need to perform this surgery in cases
dominal wall incision is closed in layers.
in which the mother may die after suffering a severe trau-
matic incident. Following maternal death, placental circu-
lation ceases, and the child must be delivered within 10
minutes; after a delay of more than 20 minutes, neonatal
PROLAPSE OF
survival is rare.
THE UTERUS
The Anatomy of the Technique
The great importance of the tone of the levatores ani muscles
in supporting the uterus has already been emphasized. The
1. The bladder is emptied, and an indwelling catheter is
importance of the transverse cervical, pubocervical, and
left in position. This allows the empty bladder to sink
sacrocervical ligaments in positioning the cervix within the
down away from the operating field.
pelvic cavity has been considered. Damage to these structures
2. A midline skin incision is made that extends from just
during childbirth or general poor body muscular tone may re-
below the umbilicus to just above the symphysis pubis.
sult in downward displacement of the uterus called uterine
The following structures are then incised: superficial
prolapse. It most commonly reveals itself after menopause,
fascia, fatty layer, and membranous layer; deep fascia
when the visceral pelvic fascia tends to atrophy along with the
(thin layer); linear alba; fascia transversalis; extraperi-
pelvic organs. In advanced cases, the cervix descends the
toneal fatty layer; and parietal peritoneum. To avoid
length of the vagina and may protrude through the orifice.
damaging loops of the small intestine or the greater
Because of the attachment of the cervix to the vaginal
omentum, which might be lying beneath the parietal
vault, it follows that prolapse of the uterus is always accom-
peritoneum, a fold of peritoneum is raised between
panied by some prolapse of the vagina.
404
Chapter 23
HYSTERECTOMY
THE PLACENTA
AND DAMAGE TO
The Placenta and Bleeding in
THE URETER
Late Pregnancy
During the surgical procedure of hysterectomy, great care
The common causes of substantial vaginal bleeding in the
must be exercised to not damage the ureters. When the sur-
third trimester are placenta previa and placental abruption.
geon is looking for the uterine artery on each side at the base
of the broad ligament (see text Fig. 23-10), it is essential that
Placenta Previa
he or she first identifies the ureter before clamping and ty-
ing off the artery. The uterine artery passes forward from the
Placenta previa occurs in about 1 of every 200 pregnancies.
internal iliac artery and crosses the ureter at right angles to
It is more common in multiparous women and in those who
reach the cervix at the level of the internal os.
have had surgery on the lower part of the uterus. Normally,
the placenta is situated in the upper half of the uterus.
Should implantation occur in the lower half of the body of
the uterus, the condition is called placenta previa.
CONGENITAL
Three types of placenta previa may be recognized
(CD Fig. 23-7): central placenta
previa, in which the
ANOMALIES OF
Type 1
THE UTERUS
Agenesis of the Uterus
Rarely the uterus will be absent as the result of a failure of
the paramesonephric ducts to develop.
Infantile Uterus
Some adults may have an infantile uterus, a condition in
which the uterus is much smaller than normal and resem-
bles that present before puberty. Amenorrhea is present, but
lateral placenta previa
lateral placenta previa
the vagina and ovaries may be normal.
Failure of Fusion of the
Type 2
Type 3
Paramesonephric Ducts
Failure of the paramesonephric ducts to fuse may cause a
variety of uterine defects: (1) The uterus may be dupli-
cated with two bodies and two cervices; (2) there may be a
complete septum through the uterus, making two uterine
cavities and two cervices; (3) there may be two separate
uterine bodies with one cervix; (4) one paramesonephric
duct may fail to develop, leaving one uterine tube and half
of the body of the uterus. Clinically, the main problems
with a double uterus may be seen when pregnancy occurs.
marginal placenta previa
central placenta previa
Abortion is frequent, and the nonpregnant half of the
uterus may cause obstruction at labor.
CD Figure 23-7
The different types of placenta previa.
The Perineum, the Female Genital Organs, and Childbirth
405
entire internal os is covered by placental tissue; marginal
compromised by the placental separation and the
placenta previa, when the edge of the placenta is en-
increased pressure on the placenta by the increased uterine
croaching on the internal os; and a low-lying lateral pla-
tone.
centa previa, when the placenta lies low down in the
uterus, lateral to the internal os. Severe, painless hemor-
rhage occurring from the twenty-eighth week onward is the
clinical sign of placenta previa and is caused by expansion
THE VAGINA
of the lower half of the uterine wall at this time and by its
tearing away from the placenta.
Vaginal Examination
Placental Abruption
The anatomic relations of the vagina are of great clinical
importance. Many pathologic conditions occurring in the
Placental abruption is the premature separation of the pla-
female pelvis may be diagnosed using a simple vaginal
centa in which normal implantation has occurred. It occurs
examination.
in about 1% of pregnancies. It is more common in multi-
The following structures can be palpated through the
parous women and in women with hypertension in preg-
vaginal walls from above downward:
nancy. As the placenta separates, hemorrhage occurs; the
blood clot dissects the fetal membranes away from the uter-
■ Anteriorly: The bladder and the urethra (CD Fig. 23-8)
ine wall. The blood usually escapes through the cervix or
■ Posteriorly: Loops of ileum and the sigmoid colon in
ruptures into the amniotic cavity. The blood irritates the
the rectouterine peritoneal pouch (pouch of Douglas),
myometrium, and uterine muscle tone is increased, which
the rectal ampulla, and the perineal body (see CD Fig.
results in contractions. The placental circulation is
23-8)
sigmoid colon
coil of ileum
S3
peritoneum
rectouterine pouch
cavity of uterus
uterovesical pouch
rectum
bladder
anococcygeal body
cervix
anal canal
anus
urogenital diaphragm
urethra
vagina
perineal body
CD Figure 23-8
Sagittal section of the female pelvis.
406
Chapter 23
■ Laterally: The ureters, the pelvic fascia and the ante-
Congenital Anomalies of the
rior fibers of the levatores ani muscles, and the uro-
genital diaphragm
Vagina
Prolapse of the Vagina
Vaginal Agenesis
The vaginal vault is supported by the same structures that
If the paramesonephric ducts fail to develop, the wall of the
support the uterine cervix. Prolapse of the uterus is
urogenital sinus will fail to form the vaginal plate. In these
necessarily associated with some degree of sagging of the
patients, there is an absence of the vagina, uterus, and uter-
vaginal walls. However, if the supports of the bladder, ure-
ine tubes. Plastic surgical construction of a vagina should be
thra, or anterior rectal wall are damaged in childbirth,
attempted.
prolapse of the vaginal walls occurs, with the uterus re-
maining in its correct position.
Double Vagina
Sagging of the bladder results in the bulging of the an-
terior wall of the vagina, a condition known as a cystocele.
A double vagina is caused by incomplete canalization of the
When the ampulla of the rectum sags against the posterior
vaginal plate.
vaginal wall, the bulge is called a rectocele.
Imperforate Vagina and Imperforate
Culdocentesis
Hymen
The closeness of the peritoneal cavity to the posterior vagi-
Imperforate vagina is caused by a failure of the cells to de-
nal fornix enables the physician to drain a pelvic abscess
generate in the center of the vaginal plate. Imperforate hy-
through the vagina without performing a major operation.
men is caused by a failure of the cells of the lower part of
It is also possible to identify blood or pus in the peritoneal
the vaginal plate and wall of the urogenital sinus to degen-
cavity by the passage of a needle through the posterior
erate. These conditions lead to retention of the menstrual
fornix.
flow, a clinical condition called hematocolpos. Surgical
incision of the obstruction, followed by dilatation, relieves
the condition.
Anatomic Structures through which
the Needle Passes
The needle passes through the mucous membrane of the
THE VISCERAL
vagina, muscular coat of the vagina, connective tissue coat
of the vagina, visceral layer of pelvic fascia, and visceral layer
PELVIC FASCIA
of peritoneum.
Anatomic Features of the
Visceral Pelvic Fascia and Infection
Complications of Culdocentesis
Clinically, the pelvic fascia in the region of the uterine
Complications are as follows: (1) The loops of ileum and
cervix is often referred to as the parametrium. It is a com-
the sigmoid colon, structures that are normally present
mon site for the spread of acute infections from the uterus
within the pouch of Douglas, could be impaled by the
and vagina, and here the infection often becomes chronic
needle. However, the presence of blood or pus within the
(pelvic inflammatory disease).
pouch tends to deflect the viscera superiorly. (2) Occa-
sionally, when the uterus is somewhat retroflexed, the
needle may enter the posterior wall of the body of the
THE PELVIC
uterus.
PERITONEUM
Vaginal Trauma
Coital injury, picket fence-type of impalement injury, and
The Rectouterine Pouch and Disease
vaginal perforation caused by water under pressure, as oc-
curs in water skiing, are common injuries. Lacerations of
Since the rectouterine pouch (pouch of Douglas) is the
the vaginal wall involving the posterior fornix may violate
most dependent part of the entire peritoneal cavity (see CD
the pouch of Douglas of the peritoneal cavity and cause pro-
Fig. 23-8) (when the patient is in the standing position), it
lapse of the small intestine into the vagina.
frequently becomes the site for the accumulation of blood
The Perineum, the Female Genital Organs, and Childbirth
407
(from a ruptured ectopic pregnancy) or pus (from a rup-
A needle may be passed into the pouch through the
tured pelvic appendicitis or in gonococcal peritonitis).
posterior fornix in the procedure known as culdocentesis
Because the pouch lies directly behind the posterior
(see CD p. 406). Surgically, the pouch may be entered in
fornix of the vagina, it is commonly violated by misguided
posterior colpotomy.
nonsterile instruments, which pierce the wall of the poste-
The interior of the female pelvic peritoneal cavity may
rior fornix in a failed attempt at an illegal abortion. Pelvic
be viewed for evidence of disease through an endoscope;
peritonitis, often with fatal consequences, is the almost
the instrument is introduced through a small colpotomy
certain result.
incision.
Clinical Problem Solving Questions
Read the following case histories/questions and give
E. Tubal rupture occurs as a result of the eroding
the best answer for each.
action of the trophoblast.
F. Once a tubal pregnancy dies the decidual lining of
1.
The following anatomic statements concerning uterine
the uterus begins to be shed because of lack of
prolapse are correct except which?
hormonal support, and this causes vaginal bleed-
A. The most important support to the uterus is the tone
ing.
of the levatores ani muscles.
G. The dough-like mass is produced by the accumula-
B. The transverse cervical, pubocervical, and sacrocer-
tion of blood in the pouch of Douglas.
vical ligaments play an important role in supporting
A 35-year-old woman was seen by her gynecologist
the uterus.
complaining of a swelling in the genital region. On
C. Damage to the levatores ani and the cervical liga-
examination, a tense cystic swelling was found be-
ments during childbirth can be responsible for pro-
neath the posterior two thirds of the right labium ma-
lapse of the uterus.
jus and minus. A diagnosis of a cyst of the right greater
D. Prolapse most commonly reveals itself before
vestibular gland (Bartholin’s cyst) was made.
menopause.
E. Prolapse of the uterus is always accompanied by
3.
The following statements concerning this case are
some prolapse of the vagina.
probably correct except which?
A. The cyst of the greater vestibular gland is produced
A 25-year-old woman was seen in the emergency de-
by the retention of secretion caused by the blockage
partment complaining of severe pain in the right iliac
of the duct.
region. Just before admission she had fainted. On phys-
B. Infection of the duct by the gonococcus is a com-
ical examination, her abdominal wall was extremely
mon cause of the blockage.
tender on palpation in the lower right quadrant, and
C. Infection of the cyst may occur, forming a painful
some rigidity and guarding of the lower abdominal
abscess.
muscles were noticed. A vaginal examination revealed
D. The lymphatic drainage of this area is into the lateral
a rather soft cervix with a circular external os. A tender
group of superficial inguinal nodes.
“dough-like” mass could be felt through the posterior
E. A small tender swelling was detected below and me-
fornix. The patient had missed her last period.
dial to the inguinal ligament.
2.
The following statements concerning this patient are
4.
In anatomic terms explain the procedure of
correct except which?
culdocentesis.
A. A diagnosis of ruptured ectopic pregnancy was
made.
5.
A 23-year-old woman was seen in the emergency de-
B. Tubal pregnancies commonly occur where the am-
partment with severe vaginal bleeding. She was 35
pulla narrows to join the isthmus.
weeks pregnant. On questioning she stated that she
C. Each uterine tube is situated in the base of the broad
had slight bleeding a week previously but this had
ligament.
stopped spontaneously. There was absolutely no pain
D. An ectopic tubal pregnancy almost invariably results
associated with the bleeding. On examining the ab-
in rupture of the tube with severe intraperitoneal
domen, it was found that the fetal head was high, and
hemorrhage.
it was not possible to make it enter the pelvis. The
408
Chapter 23
uterus had a normal consistency and was not tender.
was found on the medial aspect of the right labium
On examination of the genital organs, no cause for the
majus. A diagnosis of squamous cell carcinoma of the
bleeding could be determined. A diagnosis of placenta
skin was made. What is the lymphatic drainage of this
previa was made. What is placenta previa? What is the
region, and which group of lymph nodes would you
cause of the bleeding? Why is the bleeding painless?
therefore examine for evidence of metastases?
6.
What is believed to be the cause of pain in labor? De-
11.
A mother took her 15-year-old daughter to a physician
scribe the pathways taken by the afferent pain fibers in
because she had failed to start to menstruate. On exam-
labor and explain the distribution of the areas of re-
ination the child was noted to be short and stocky with
ferred pain.
a webbed neck. She had an abnormally large carrying
angle of the elbow (cubitus valgus), a broad chest with
7.
The postnatal vaginal examination of a young woman
lack of breast development, and an absence of pubic
revealed that the fundus and body of the uterus could
and axillary hair. No further abnormalities were found
be palpated in the rectouterine pouch (pouch of Dou-
on physical examination. What is your diagnosis? What
glas). What is the normal position of the uterus?
investigations would you undertake to confirm your di-
8.
A multiparous 57-year-old woman visited her physi-
agnosis? How would you treat this patient?
cian complaining of a “bearing-down” feeling in the
12.
During the third stage of labor, the placenta and fetal
pelvis and of low backache, both of which were worse
membranes are expelled from the uterus. The obstetri-
when she was tired. On vaginal examination, the
cian or midwife must carefully examine the placenta
external os of the cervix was found to be located just
and the membranes to make sure that no part of them
within the vaginal orifice. A diagnosis of uterine
has been retained in the uterus. What is the approxi-
prolapse was made. What are the main supports of
mate diameter and thickness of a normal placenta?
the uterus?
Describe the appearance of the maternal and fetal sur-
9.
During the vaginal examination of a multiparous
faces of a full-term placenta. Is it possible to separate the
woman, she was asked to strain downward. The anterior
amnion from the chorion?
wall of the vagina was found to sag downward. A diag-
13.
A 12-year-old girl was taken to a pediatrician because
nosis of prolapsed anterior vaginal wall was made. What
she experienced cyclic monthly pain, but there was no
structures lie anterior to the vagina and will sag down-
actual menstrual flow. On physical examination of the
ward with the vaginal wall?
vulva, the hymen was seen as a bulging septum. No
10.
A 65-year-old woman went to her physician complain-
vaginal orifice could be detected. What is your diagno-
ing of irritation, discharge, and bleeding of the genital
sis? How would you explain this condition embryologi-
region. On physical examination, a hard-based ulcer
cally? How would you treat this patient?
Answers and Explanations
1. D is the correct answer. Prolapse of the uterus most of-
5. Normally the placenta is situated in the upper half of
ten reveals itself after menopause, when the pelvic fas-
the uterus. Should implantation occur in the lower half
cia tends to atrophy.
of the body of the uterus, the condition is called pla-
centa previa. As the lower half of the body of the uterus
2. C is the correct answer. Each uterine tube is situated in
dilates toward the end of pregnancy, the placenta is sep-
the upper free margin of the broad ligament (see text
arated from the uterine wall and hemorrhage occurs.
Fig. 23-10).
The bleeding is painless since the blood escapes
3. D is the correct answer. The lymphatic drainage of
through the cervix, and the uterus does not contract and
this area is into the medial group of superficial in-
is not distended.
guinal nodes situated below the inguinal ligament.
6. The cause of labor pains has been fully discussed in this
The spread of infection can result in an enlargement
chapter, as have the path taken by the afferent pain
of one of the nodes, as in this case, which becomes
fibers from the uterus and the areas of the body to which
tender to palpation.
labor pains are referred.
4. See discussion of culdocentesis in this chapter.
The Perineum, the Female Genital Organs, and Childbirth
409
7.
The long axis of a normal uterus usually lies at right an-
trogen and progesterone in this case will bring about
gles to the long axis of the vagina (anteverted); the body
the development of normal female secondary sexual
of the uterus is also bent forward on the cervix at the in-
characteristics and cyclic menstrual function.
ternal os (anteflexion).
12.
The normal placenta is flattened and circular in
8.
The uterus is mainly supported by the tone of the leva-
shape, with a diameter of about 8 in. (20 cm) and a
tores ani muscles and the ligaments of the visceral layer
thickness of about 1 in. (2.5 cm). The maternal sur-
of pelvic fascia, namely, the transverse cervical, sacro-
face is dark red in color and oozes blood from the torn
cervical, and pubocervical ligaments.
maternal vessels. It has a sponge-like consistency. The
outer surface is rough, and the margins of the lobules
9.
The urethra lies directly in contact with the lower half
or cotyledons may be recognized. The fetal surface is
of the anterior vaginal wall, and the bladder lies in con-
smooth and shining and is covered by amnion, which
tact with the upper half of the vaginal wall. The bulging
is fused with the underlying chorion. The umbilical
downward of the bladder with the anterior vaginal wall
cord is attached near its center, and the umbilical ves-
is referred to as a cystocele.
sels radiate out under the amnion from the point of at-
10.
The vulva is drained into the medial group of horizon-
tachment. The amnion may be peeled from the
tal superficial inguinal nodes.
chorion up to the umbilical cord. This procedure
should always be carried out following delivery to de-
11.
This case is a typical example of Turner’s syndrome, in
termine if the chorion is complete and to make sure
which there is complete failure of both ovaries to de-
that some part has not been retained in the uterus ad-
velop. In Turner’s syndrome the cells have only 45
herent to the decidua.
chromosomes because one X chromosome is missing
(XO). In this case the clinical signs and symptoms make
13.
This girl has an imperforate hymen. The pelvic dis-
the diagnosis obvious. A simple buccal smear and the
comfort and the absence of menstrual flow are due to
finding of absent nuclear sex chromatin make the diag-
the accumulation of blood and old menstrual secre-
nosis absolute. In difficult cases, where the diagnosis is
tions (hematocolpos) above the intact hymen. This
in doubt, culdoscopy shows the absence of ovaries in
condition is caused by a failure of the cells of the lower
the pelvis. Since these individuals are females in ap-
part of the vaginal plate and the wall of the urogenital
pearance and psychological outlook, they should be
sinus to degenerate. Surgical incision of the hymen,
brought up as females. The cyclic administration of es-
followed by dilatation, cures the condition.
Chapter Outline
Endocrine Glands in the Head and Neck
414
Hypoparathyroidism
418
Congenital Anomalies of the Parathyroid
Pituitary Gland (Hypophysis Cerebri)
414
Glands
418
Pituitary Enlargement and the Optic Chiasma
414
Absence and Hypoplasia of the Parathyroid
Gigantism and Acromegaly
414
Glands
418
Dwarfism
415
Ectopic Parathyroid Glands
418
Diabetes Insipidus
415
Endocrine Glands in the Abdomen
Pineal Gland
415
and Pelvis
419
Pineal Calcification
415
Pineal Tumors and Reproductive Function
415
Suprarenal Glands
419
Cushing’s Syndrome
419
Thyroid Gland
415
Addison’s Disease
419
Swellings of the Thyroid Gland and Movement
Pheochromocytoma
419
on Swallowing
415
Surgical Significance of the Renal Fascia
419
The Thyroid Gland and the Airway
415
Suprarenal Susceptibility to Trauma at Birth
419
Retrosternal Goiter
415
Thyroid Arteries and Important Nerves
415
Islets of Langerhans of the Pancreas
419
Thyroidectomy and the Parathyroid Glands
415
Islets of Langerhans and Diabetes Mellitus
419
Hyperthyroidism
416
Interstitial Cells of the Testis
419
Hypothyroidism
416
Testosterone Deficiency
419
Thyroid Tumors
417
Congenital Anomalies of the Thyroid Gland
417
Ovaries
420
Agenesis of the Thyroid
417
Menopause
420
Incomplete Descent of the Thyroid
417
Hypogonadism
420
Ectopic Thyroid Tissue
418
Placenta
420
Persistent Thyroglossal Duct
418
Hydatidiform Mole
420
Thyroglossal Cyst
418
Thyroglossal Sinus (Fistula)
418
Clinical Problem Solving Questions
420
Parathyroid Glands
418
Thyroidectomy and the Parathyroid Glands
418
Answers and Explanations
422
Hyperparathyroidism
418
A pituitary tumor classically pushes the diaphragma sellae
ENDOCRINE
upward and causes pressure on the optic chiasma. This re-
sults in interference with the function of the nerve fibers
crossing in the chiasma (from the inner quadrants of the
GLANDS IN THE
retina), and the patient presents with bitemporal hemi-
anopia (see text Fig. 15-1B). Further expansion of the pitu-
HEAD AND NECK
itary tumor causes erosion of the body of the sphenoid bone.
Gigantism and Acromegaly
Pituitary Gland (Hypophysis Cerebri)
Excessive production of the growth hormone by the soma-
totrope cells of the pars anterior or by tumors of these cells
Pituitary Enlargement and the
can produce abnormal growth of the skeleton. Gigantism
Optic Chiasma
occurs in the young before the epiphyses in long bones fuse
Since the pituitary is located in the bony sella turcica, en-
with the diaphysis. The growth hormone stimulates the car-
largement causes it to expand superiorly (see text Fig. 24-2).
tilage cells of the epiphyseal cartilage to continue laying
The Endocrine Glands
415
down new matrix, so that fusion of the epiphyses with the
the midbrain, producing hydrocephalus. Occasionally, the
shaft of long bones is delayed and the bones lengthen enor-
tumor destroys the pineal gland and causes precocious
mously. In this way, giants 9 ft tall have been produced be-
puberty.
fore the epiphyseal cartilage finally stops growing.
Acromegaly is a form of abnormal skeletal and soft tis-
sue growth that occurs after adolescence, following the fu-
Thyroid Gland
sion of the epiphyses in long bones with the diaphysis. In
this disease, the individual cannot grow taller, but over-
Swellings of the Thyroid Gland and
growth occurs in the bones and soft tissues of the forehead,
Movement on Swallowing
nose, lower jaw, hands, and feet. In the fully developed syn-
The thyroid gland is invested in a sheath derived from the
drome, the prominent supraorbital ridges and mandible, the
pretracheal fascia
(see text Fig.
24-10). This tethers
very large nose, and the very large, thick hands and feet
the gland to the larynx and the trachea and explains
make the diagnosis relatively easy.
why the thyroid gland follows the movements of the lar-
ynx in swallowing. This information is important be-
Dwarfism
cause any pathologic neck swelling that is part of the
A deficiency in the growth hormone secreted by the soma-
thyroid gland will move upward when the patient is asked
totrope cells of the pars anterior during childhood leads to
to swallow.
pituitary dwarfism. Growth does not stop entirely, and the
different parts of the body are in relatively normal propor-
The Thyroid Gland and the Airway
tions. The person is of normal intelligence, but the facial
The close relationship between the trachea and the lobes
skin is often wrinkled and sexual maturation is delayed.
of the thyroid gland commonly results in pressure on the
Diabetes Insipidus
trachea in patients with pathologic enlargement of the
thyroid.
This syndrome results from a lesion of the supraoptic and
paraventricular nuclei of the hypothalamus and a failure of
Retrosternal Goiter
these cells to synthesize the antidiuretic hormone, or from
destruction of the hypothalamohypophysial tract. There are
The attachment of the sternothyroid muscles to the thyroid
many causes of this syndrome, including cerebral tumors,
cartilage effectively binds down the thyroid gland to the lar-
cerebral abscesses, surgical or radiation damage, and head
ynx and limits upward expansion of the gland. There being
injuries.
no limitation to downward expansion, it is not uncommon
Characteristically, the patient passes large volumes of
for a pathologically enlarged thyroid gland to extend down-
urine (polyuria) of low specific gravity. The absence of an-
ward behind the sternum. A retrosternal goiter (any abnor-
tidiuretic hormone results in a failure to conserve water,
mal enlargement of the thyroid gland) can compress the
which is not reabsorbed in the collecting tubules of the kid-
trachea and cause dangerous dyspnea; it can also cause se-
neys. As a result, the patient is extremely thirsty (polydipsia)
vere venous compression.
and drinks large quantities of fluids. The condition must be
distinguished from diabetes mellitus, in which there is
Thyroid Arteries and Important Nerves
glucosuria.
It should be remembered that the two main arteries supply-
ing the thyroid gland are closely related to important nerves
Pineal Gland
that can be damaged during thyroidectomy operations (CD
Fig. 24-1). The superior thyroid artery on each side is re-
Pineal Calcification
lated to the external laryngeal nerve, which supplies the
cricothyroid muscle. The terminal branches of the inferior
With age, the pineal gland accumulates magnesium phos-
thyroid artery on each side are related to the recurrent la-
phate and carbonate within the glial cells and connective
ryngeal nerve. Damage to the external laryngeal nerve
tissue. These deposits are useful to radiologists, because
results in an inability to tense the vocal folds and in hoarse-
they serve as a landmark and assist in determining whether
ness. For the results of damage to the recurrent laryngeal
the pineal gland has been displaced laterally by a space-
nerve, see CD page 24.
occupying lesion within the skull.
Pineal Tumors and Reproductive
Thyroidectomy and The Parathyroid
Function
Glands
Pineal tumors may have an antigonadotropic effect. As they
The parathyroid glands are usually four in number and are
increase in size, they may obstruct the cerebral aqueduct of
closely related to the posterior surface of the thyroid gland
416
Chapter 24
internal carotid artery
right vagus nerve
external carotid artery
inferior contrictor
of pharynx
internal laryngeal nerve
left vagus nerve
external laryngeal
nerve
superior thyroid
left common
artery and vein
carotid artery
right lobe of
thyroid gland
esophagus
superior right
parathyroid gland
inferior
thyroid artery
inferior right
left recurrent
parathyroid gland
laryngeal nerve
right recurrent
laryngeal nerve
left subclavian
artery and vein
right subclavian
artery and vein
CD Figure 24-1
The pharynx, esoph-
agus, and trachea as seen from the
right
vagus nerve
posterior aspect. Note the positions of
aorta
the thyroid and parathyroid glands
superior
and the relationships of the large
vena cava
blood vessels and nerves. The dotted
lines indicate the level of the cricothy-
left vargus nerve
roid membrane.
(see CD Fig. 24-1). In partial thyroidectomy, the posterior
The hair thins, and the eyes may protrude (exophthalmos).
part of the thyroid gland is left undisturbed so that the
The heart rate is increased and frequent bowel movements
parathyroid glands are not damaged. The development of
may occur; the menstrual periods may be missed or scanty.
the inferior parathyroid glands is closely associated with the
Three forms of therapy are available for the treatment of
thymus. For this reason it is not uncommon for the surgeon
hyperthyroidism: (1) surgical excision of thyroid tissue, (2)
to find the inferior parathyroid glands in the superior medi-
antithyroid drugs, and (3) radioactive iodine.
astinum because they have been pulled down into the tho-
rax by the thymus.
Hypothyroidism
Hypothyroidism occurs in two forms: cretinism in infants
Hyperthyroidism
and myxedema in adults.
In hyperthyroidism
(thyrotoxicosis, Grave’s disease),
Cretinism can occur as a result of a failure in the de-
which is common in middle-aged women, the thyroid
velopment of the thyroid gland. The child is born with a
gland is diffusely enlarged. The walls of the thyroid folli-
normal appearance, caused by the mother’s thyroid hor-
cles are much infolded, and the epithelial cells lining the
mones having crossed the placenta. Soon after birth, the
follicular walls are taller than normal. Production of the
child shows signs of retarded mental and physical growth. If
thyroid hormones is greatly increased, and the colloid
cretinism is diagnosed early and the child is given adequate,
present is usually reduced in volume. The serum thyroid-
lifelong thyroid hormone therapy, he or she will develop
stimulating hormone level is normal or below normal. In
normally and live a normal life.
most patients, there is a thyroid-stimulating immunoglob-
Myxedema may be caused in adults by many condi-
ulin in the blood that is capable of stimulating increased
tions ranging from spontaneous degeneration of the thyroid
thyroid activity.
gland to hypopituitarism or hypothalamic failure. Excessive
The symptoms of hyperthyroidism are caused by
treatment of hyperthyroidism with drugs or surgery is an-
the excessive stimulation of the tissues by the thyroid hor-
other possible cause. The majority of the patients are fe-
mones. There is excessive sweating and loss of weight;
male. The symptoms include the slowing of mental and
increased nervousness, with fine tremor of the extended
physical processes of the individual. There is an increase in
fingers; intolerance to heat; and muscular weakness.
body weight and a preference for a warm environment.
The Endocrine Glands
417
tongue
anterior
thyroglossal cyst
path taken by thyroid gland
as it descends in the neck
thyroglossal fistula
CD Figure 24-2
A thyroglossal
cyst in the midline in the neck and
a thyroglossal fistula.
Constipation is present, and the heart rate is slowed. The
Incomplete Descent of the Thyroid
skin is dry and cold, and the hair is dry and brittle and tends
The descent of the thyroid may be arrested at any point
to fall out. Libido is diminished in both sexes, and menor-
between the base of the tongue and the trachea (CD Fig.
rhagia is common in the female. The condition can be
24-2). Lingual thyroid is the most common form of in-
successfully treated by the daily oral administration of the
complete descent (CD Fig. 24-3). The mass of tissue
thyroid hormones.
Thyroid Tumors
Benign thyroid tumors occur in the form of adenomas.
Carcinoma of the thyroid gland is relatively rare.
Congenital Anomalies of the
Thyroid Gland
Agenesis of the Thyroid
Failure of development of the thyroid gland may occur and
is the commonest cause of cretinism.
CD Figure 24-3
Lingual thyroid. (Courtesy of J. Randolph.)
418
Chapter 24
found just beneath the foramen cecum may be sufficiently
of an infection of a cyst. All remnants of the thyroglossal
large to obstruct swallowing in the infant.
duct should be removed surgically.
Ectopic Thyroid Tissue
Parathyroid Glands
Ectopic thyroid tissue is occasionally found in the thorax in
relation to the trachea or bronchi or even the esophagus. It
Thyroidectomy and the Parathyroid
is assumed that this thyroid tissue arises from entodermal
Glands
cells displaced during the formation of the laryngotracheal
tube or from entodermal cells of the developing esophagus.
See previous section of this CD chapter.
Persistent Thyroglossal Duct
Hyperparathyroidism
Conditions related to a persistence of the thyroglossal duct
This condition is caused by a benign adenoma or hyperpla-
usually appear in childhood, in adolescence, or in young
sia of the parathyroid glands. As a result, there is an excessive
adulthood.
secretion of the parathyroid hormone, and the blood cal-
cium level rises to as much as 15 mg/100 mL from the
Thyroglossal Cyst
normal level of 10 mg/100 mL. The raised levels of blood
calcium in this disease may cause the repeated occurrence
Cysts may occur at any point along the thyroglossal tract (see
of renal stones as the result of the spilling over of the cal-
CD Fig. 24-2 and CD Fig. 24-4). They occur most com-
cium salts into the urine. The high blood calcium levels also
monly in the region below the hyoid bone. Such a cyst oc-
affect the central and peripheral nervous systems. Neuro-
cupies the midline and develops as a result of persistence of
logic abnormalities include emotional instability, memory
a small amount of epithelium that continues to secrete mu-
loss, and muscular weakness. The treatment is surgical
cus. As the cyst enlarges, it is prone to infection and so it
removal of the diseased gland.
should be removed surgically. Since remnants of the duct
often traverse the body of the hyoid bone, this may have to
Hypoparathyroidism
be excised also to prevent recurrence.
This condition is most commonly caused by injury to or re-
Thyroglossal Sinus (Fistula)
moval of the glands during surgical procedures on the
thyroid gland.
Occasionally, a thyroglossal cyst ruptures spontaneously,
The main symptoms and signs of low blood calcium are
producing a sinus (see CD Fig. 24-2). Usually, this is a result
numbness and tingling in the fingers and toes and cramps of
the muscles in the hands and feet. These cramps are called
carpopedal spasms. The spasm, or tetany, of muscles may
also involve the facial or laryngeal muscles. The central ner-
vous system may also be involved, as evidenced by signs of
mental confusion and loss of memory.
The condition is treated by giving the patient calcium
gluconate and large quantities of vitamin D by mouth.
Congenital Anomalies of the
Parathyroid Glands
Absence and Hypoplasia of the
Parathyroid Glands
Agenesis or incomplete development of the parathyroid
glands has been demonstrated in individuals with idiopathic
hypoparathyroidism.
Ectopic Parathyroid Glands
The close relationship between the parathyroids III and the
developing thymus explains the frequent finding of parathy-
CD Figure 24-4
A thyroglossal cyst. (Courtesy of
roid tissue in the superior mediastinum of the thorax (see
L. Thompson.)
text Fig. 24-14). If the parathyroid glands remain attached to
The Endocrine Glands
419
the thymus, they may be pulled inferiorly into the lower part
Suprarenal Susceptibility to Trauma
of the neck or thoracic cavity. Moreover, this also explains
at Birth
the variable position of the inferior parathyroid glands in re-
lation to the lower poles of the lateral lobes of the thyroid
At birth, the suprarenal glands are relatively large because of
gland.
the presence of the fetal cortex; later, when this part of the
cortex involutes, the gland becomes reduced in size. During
the process of involution, the cortex is friable and suscepti-
ble to damage and severe hemorrhage.
ENDOCRINE
Islets of Langerhans of the
GLANDS IN THE
Pancreas
ABDOMEN AND
Islets of Langerhans and Diabetes
Mellitus
PELVIS
In diabetes mellitus, the beta cells of the islets of Langerhans
lose their ability to secrete insulin or the target cells of the tis-
Suprarenal Glands
sues become insensitive to circulating insulin. In juvenile di-
abetes, there is total absence of insulin, but when the onset
Cushing’s Syndrome
of diabetes occurs in adulthood, the plasma levels of insulin
Suprarenal cortical hyperplasia is the most common cause
may be normal or only slightly below normal. The exact
of Cushing’s syndrome, the clinical manifestations of which
cause of diabetes mellitus is not known. Genetic, metabolic,
include moon-shaped face, truncal obesity, abnormal hairi-
and autoimmune factors, as well as viral infections, are
ness (hirsutism), and hypertension; if the syndrome occurs
thought to play an important causative role in many patients.
later in life, it may result from an adenoma or carcinoma of
In all patients with diabetes mellitus, the blood glucose
the cortex.
level is above normal (hyperglycemia). Once the blood glu-
cose level reaches a certain threshold value, approximately
Addison’s Disease
180 mg/100 mL, the glucose spills over into the urine (glu-
cosuria). The osmotic pressure exerted by the high concen-
Adrenocortical insufficiency (Addison’s disease), which is
tration of glucose in the urine inhibits the reabsorption of
characterized clinically by increased pigmentation, muscu-
water in the kidney tubules, causing excessive urination
lar weakness, weight loss, and hypotension, may be caused
(polyuria). The patient becomes thirsty and dehydration
by tuberculous destruction or bilateral atrophy of both
may occur. There is an upset in the carbohydrate, fat, and
cortices.
protein metabolism in these patients that leads to loss of
weight and lack of energy.
Pheochromocytoma
The treatment of patients with diabetes mellitus in-
cludes giving sufficient insulin and a special diet so that the
Pheochromocytoma, a tumor of the medulla, produces a
carbohydrate metabolism returns to normal. In those pa-
paroxysmal or sustained hypertension. The symptoms and
tients with the less severe type of diabetes, the hyperglycemia
signs result from the production of a large amount of cate-
often can be treated with a low-calorie, low-carbohydrate diet
cholamines, which are then poured into the bloodstream.
without the administration of insulin.
Because of their position on the posterior abdominal
wall, few tumors of the suprarenal glands can be palpated.
Computed tomography (CT) scans can be used to visualize
Interstitial Cells of the Testis
the glandular enlargement; however, when interpreting CT
scans, remember the close relationship of the suprarenal
Testosterone Deficiency
glands to the crura of the diaphragm.
The function of the testes is the production of spermatozoa
and the secretion of the male sex hormones, particularly
Surgical Significance of the
testosterone, by the interstitial cells. The two functions may
Renal Fascia
be interfered with simultaneously by a severe acute infec-
The suprarenal glands, together with the kidneys, are en-
tion or by the occlusion of the blood supply during a repair
closed within the renal fascia; the suprarenal glands, how-
operation for inguinal hernia. Total absence of testosterone
ever, lie in a separate compartment, which allows the two
follows surgical castration, which may be necessary follow-
organs to be separated easily at operation.
ing severe trauma to the perineum. Testosterone deficiency
420
Chapter 24
is not present in patients with incompletely descended or
fat, or shrink, because of atrophy of the glandular ducts. The
maldescended testes. If testosterone deficiency occurs be-
patient usually gains weight from a diffuse deposition of fat.
fore puberty, the accessory organs of reproduction do not
The patient often complains of pains in the joints, fatigue,
develop; the penis, scrotum, seminal vesicles, and prostate
and insomnia. Anxiety, depression, and emotional instabil-
remain small. The secondary sexual characteristics do not
ity may also be present.
appear. There is no growth of the hair on the face or trunk
The lack of estrogen also increases protein catabolism.
or in the axillae. The pubic hair is of the female distribution
This change reveals itself by an alteration in the texture of
and develops in response to the suprarenal androgens. The
the hair and nails, wrinkling of the skin, and osteoporosis.
larynx fails to enlarge, and the voice remains high pitched
In the great majority of women, the symptoms of the
and infantile. The muscles are poorly developed. There is
menopause are slight, but for some, the body changes and
delay in the fusion of the epiphyses in the long bones with
emotional disturbances are very severe, requiring consider-
the diaphysis. Excessive fat deposits may occur in the pec-
able patience and understanding from the husband and
toral region, abdomen, and buttocks, and on the hips.
relatives.
Testosterone deficiency after puberty causes the acces-
sory sex organs to atrophy and the secondary sexual charac-
Hypogonadism
teristics to regress. Those organs and structures that do not
require testosterone for their maintenance are unaffected,
Ovarian hypofunction may be associated with lesions of the
however. Thus, the penis remains of normal size, the voice
hypothalamus that impair the release of the gonadotropic-
remains unchanged, and facial hair growth may be affected
releasing hormone. Via a similar mechanism, emotional
only slightly. Sexual desire and erection may be absent.
strain, such as leaving home and attending college, may
change the afferent nervous input of the hypothalamus,
causing amenorrhea. Hypopituitarism with a failure of folli-
Ovaries
cle-stimulating hormone and luteinizing hormone secre-
tion caused by a pituitary tumor may also cause ovarian
Menopause
hypofunction. Removal of the ovaries in the adult results in
a premature, artificial menopause.
Menopause is the period of life when the ovaries normally
cease to respond to the gonadotropic hormones of the ante-
rior lobe of the pituitary. Menopause occurs on average be-
tween ages 45 and 50. The ovaries become smaller, and the
Placenta
graafian follicles atrophy and are replaced by fibrous tissue.
Hydatidiform Mole
The tunica albuginea thickens. The corpora lutea and the
ovarian hormones are no longer produced.
Excessive proliferation of the trophoblast during the early
As a result of the cessation of the production of ovarian
stages of placenta formation may lead to the condition of hy-
estrogens and progesterone, menstruation ceases and the
datidiform mole. The uterus may become filled with vesic-
genital organs atrophy to some extent. Vasomotor changes,
ular structures, which may be the size of grapes, and the
in the form of hot flashes, occur in the skin of the face, neck,
fetus dies. Very large quantities of chorionic gonadotropin
and chest. The vaginal mucous membrane thins and atro-
are produced by the trophoblast, and the hormone appears
phies. The breasts may enlarge, because of the deposition of
in the urine.
Clinical Problem Solving Questions
Read the following case histories/questions and give
symptoms. Six months later, the patient started to com-
the best answer for each.
plain of frequency of micturition and was passing very
large quantities of pale urine. She also said that she al-
1. On examination, a patient is found to have a bitempo-
ways seemed thirsty and would often drink 10 glasses of
ral hemianopia. An enlargement of which anatomic
water in one morning. Using your knowledge of
structure is likely to cause this condition?
anatomy and physiology, do you think there is any con-
nection between the urinary symptoms and her auto-
2. A 40-year-old woman was involved in an automobile
mobile accident?
accident in which she sustained severe head injuries.
Following a slow but uneventful recovery, she was re-
3. A 17-year-old boy is taken by his parents to a pediatri-
leased from the hospital without any residual signs or
cian because the parents are concerned about his
The Endocrine Glands
421
excessive height and his complaints of fatigue and gen-
B. Each lobe of the thyroid gland is closely related to
eral lassitude. His standing height is 84 in. Questioning
the sides of the trachea.
reveals that the boy has grown very rapidly since his thir-
C. The isthmus of the thyroid gland was found to cross in
teenth birthday. As a young child, he excelled in com-
front of the third, fourth, and fifth rings of the trachea.
petitive sports, but for the past 3 years, he has experi-
D. The sudden increase in the size of the swelling can
enced weakness and fatigue and has ceased to compete.
be explained by a hemorrhage into the adenoma.
His nose is broad, and his mandible and facial features
E. The swelling was located superficial to the left ster-
appear larger than normal. He has large hands and feet
nothyroid muscle.
and takes a size 18 shoe. There is no family history of
F. The breathlessness was caused by the adenoma press-
unusual tallness. The patient is of normal intelligence,
ing on the trachea, partially occluding the lumen.
and the size of his external genitalia is normal for his
A 35-year-old woman had a partial thyroidectomy for
age. His secondary sexual characteristics are normal.
the treatment of thyrotoxicosis. During the operation a
Using your knowledge of anatomy and physiology,
ligature slipped off the right superior thyroid artery. To
make a diagnosis. Which cell groups are likely to have
stop the hemorrhage, the surgeon blindly grabbed for
undergone pathologic changes? How do you account
the artery with artery forceps. The operation was com-
for the excessive tallness and the presence of a large
pleted without further incident. The following morning
mandible, hands, and feet in the same individual?
the patient spoke with a husky voice.
4.
A 25-year-old woman has been in labor for several
7.
The following statements about this patient would ex-
hours. Her uterine contractions are weak, and her labor
plain the husky voice except which?
is not progressing. The obstetrician decides to give her
A. Laryngoscopic examination revealed that the right vo-
some Pitocin, a synthetic oxytocin hormone. What is
cal cord was slack, causing the huskiness of the voice.
the effect of oxytocin on the uterus? In which part of the
B. The vocal cord is tensed by the contraction of the
pituitary is this hormone normally released into the
cricothyroid muscle.
bloodstream?
C. The cricothyroid muscle tilts back the cricoid carti-
5.
A 45-year-old woman visits her physician for a medical
lage and pulls forward the thyroid cartilage.
checkup. The woman has no complaints, but her hus-
D. The cricothyroid muscle is innervated by the recur-
band has noted the following changes in her appear-
rent laryngeal nerve.
ance during the previous year: She has gained a con-
E. The superior thyroid artery is closely related to the
siderable amount of weight and is becoming mentally
external laryngeal nerve.
and physically slow, often falling asleep while talking to
8.
Following a total thyroidectomy for carcinoma of the
friends. Her face is puffy, and her hair is dry and has de-
thyroid gland, a 55-year-old man noticed tingling and
veloped a tendency to fall out. The lateral third of her
numbness of the fingers, toes, and lips. Painful cramps
eyebrows is missing. Her skin is pale and dry, and her
of the hands and feet were also experienced. Strong
voice is becoming deep and her articulation slow. She
muscle spasms producing adduction of the thumb, flex-
frequently complains of the cold when others feel
ion of the wrist and metacarpophalangeal joints, and
warm. Using your knowledge anatomy and physiology,
plantar flexion of the feet also occurred. Laboratory ex-
what do you think is wrong with this patient? What do
amination of the blood revealed a blood calcium level
you think would be the appropriate treatment?
of 4 mg/100 mL. Which organ was damaged during the
A 25-year-old woman complaining of a swelling on the
total thyroidectomy?
front of the neck and breathlessness visited her physi-
cian. On examination, a small, solitary swelling of firm
An 18-year-old woman went to her physician because
consistency was found to the left of the midline of the
she had noticed a swelling in the midline of her neck.
neck below the thyroid cartilage of the larynx. The
She said she had first noticed this swelling 3 years pre-
swelling was not attached to the skin but moved upward
viously, and it had gradually increased in size. On phys-
on swallowing. About 2 weeks previously the swelling
ical examination, a small swelling was found in the
had suddenly increased in size and had become tender
midline of the neck; it measured about 0.5 in. (1.25 cm)
to touch; following this increase in size the patient be-
in diameter. It was situated just below the body of the
came breathless.
hyoid bone, was soft and fluctuant, and moved upward
on swallowing. Nothing else abnormal was discovered.
6.
The following statements concerning this case would
suggest a diagnosis of adenoma of the thyroid gland ex-
9.
The physician made the diagnosis of thyroglossal cyst
cept which?
based on the following symptoms and signs except
A. The pretracheal layer of deep cervical fascia binds
which?
the thyroid gland to the larynx, which moves upward
A. The swelling was not hard.
on swallowing.
B. The swelling was fluctuant.
422
Chapter 24
C. The swelling was located in the midline of the
nary content of catecholamines. What hormones are
neck.
secreted by the cells of the suprarenal medulla, and
D. It moved upward on swallowing, which indicated
what is their action?
that it was tethered to tissue associated with the
12.
A 51-year-old man is concerned because he has noticed
thyroid gland.
during the past few weeks that he has started to urinate
E. A thyroglossal cyst is always found below the hyoid
more frequently and is always hungry and thirsty. He is
bone.
also worried because he has been treated for skin infec-
10.
A 38-year-old man is admitted to the hospital for labo-
tions on six occasions during the past year. The fasting
ratory tests. When seen by his physician, he complains
blood glucose level is measured, and a glucose toler-
of increasing tiredness and muscular weakness over the
ance test is performed. The results show that the patient
previous year. He has experienced five attacks of nausea
has diabetes mellitus. What is the normal fasting blood
and vomiting, and diarrhea during this period. His rea-
glucose level? Why does glucose appear in the urine in
son for visiting his physician is that his friends have no-
diabetes mellitus? What is the underlying cause of dia-
ticed that his skin is becoming darker. After a complete
betes mellitus?
physical examination, a diagnosis of Addison’s disease is
made, and it is confirmed by laboratory tests. What is
13.
A 21-year-old man sustains a severe injury to the per-
the cause of Addison’s disease? The secretions of which
ineum following an explosion of a road-side bomb
hormones are defective in this disease? What is respon-
by a terrorist. The surgeon is forced to amputate the
sible for the weakness and increased pigmentation of
scrotum and remove both testes. Using your knowl-
the skin in this condition?
edge of physiology, describe the changes that will take
place because of the absence of testosterone. Is testos-
11.
A 29-year-old man recently experienced what he de-
terone produced in patients with bilateral undescended
scribes as severe pounding palpitations. The attacks
testicles?
had lasted about 20 minutes each and had been ac-
companied by severe sweating, headache, and pale-
14.
What are the clinical signs and symptoms of meno-
ness and coldness of the skin. While in the hospital
pause? What is responsible for menopause? Is it caused
clinic he has another attack. His pulse rate is 120 beats
by a cessation of the activity of the hypothalamus, a ces-
per minute, and his blood pressure is 240/140 mm Hg.
sation of the activity of the pars anterior, or a failure of
A preliminary diagnosis of pheochromocytoma is
the ovary to respond to hormonal stimulation from the
made, which is later confirmed by analysis of the uri-
pituitary?
Answers and Explanations
1. Bitemporal hemianopia is a loss of both temporal fields
the absorption of water in the distal convoluted tubules
of vision and is due to the interruption of the optic nerve
and collecting tubules of the kidney.
fibers derived from the medial halves of both retinae.
3. This patient has the signs and symptoms of gigantism
Pressure on the optic chiasma by a tumor of the pituitary
and acromegaly caused by the excessive secretion of
gland is the most common cause of the condition.
growth hormone by the acidophil cells of the anterior
lobe of the pituitary gland. The condition started before
2. Yes, there is a connection between the accident and the
the epiphyses of the long bones fused with the diaph-
urinary symptoms. This patient is suffering from dia-
ysis, hence the gigantism, and continued growth after
betes insipidus caused by traumatic damage either to
the fusion had taken place, hence the acromegalic
the posterior lobe of the pituitary gland or to the
changes.
supraoptic or paraventricular nuclei of the hypothala-
mus. In any event, production of vasopressin was inhib-
4. Oxytocin stimulates the smooth muscle of the uterus to
ited. It should be pointed out that a lesion of the poste-
contract. Normally, it plays an important role in labor
rior lobe of the pituitary is usually not followed by
and delivery. During the third stage of labor, when the
diabetes insipidus, since the vasopressin (antidiuretic
placenta and the fetal membranes have been delivered,
hormone) produced by the neurons of the supraoptic
it stimulates the uterine muscle to contract and pre-
and paraventricular nuclei escapes directly into the
vents excessive bleeding. In this patient the obstetrician
bloodstream. The action of vasopressin is to increase
was supplementing the patient’s own oxytocin with
The Endocrine Glands
423
synthetic hormone to increase the force of the uterine
the pars anterior of the pituitary, which results in atro-
contractions.
phy of the suprarenal cortex. Cortisol and aldosterone
are the two hormones that are lacking in this disease.
Oxytocin is produced by the nerve cells in the hypothal-
The weakness is caused by the absence of cortisol se-
amus. The hormone reaches the posterior lobe of the pi-
cretion, which causes a fall in the level of blood glu-
tuitary via the hypothalamohypophysial tract, where it is
cose. The increased melanin pigmentation in the skin
stored and later released from the nerve endings.
and buccal mucous membrane is caused by the in-
5.
This patient has the signs and symptoms of hypothy-
creased secretion of ACTH from the pars anterior of the
roidism and myxedema. After confirming the diagnosis
pituitary. (The increased pigmentation does not occur
by estimating the PBI (protein-bound iodine concen-
in patients in whom the disease is caused by hypopitu-
tration) and serum T4 levels, which are low in this dis-
itarism.) ACTH stimulates the melanocytes in the skin
ease, the doctor should prescribe daily doses of thyroid
to increase their production of melanin.
hormone, and this treatment should be continued
11.
The epithelial cells of the suprarenal medulla synthe-
indefinitely.
size and secrete norepinephrine and epinephrine.
6.
E is the correct answer. The thyroid gland lies deep to
12.
The normal fasting blood glucose level is about 110
the sternothyroid muscle (see text Fig. 24-10).
mg/100 mL. Once the blood glucose level in diabetes
mellitus reaches a certain threshold value, approxi-
7.
D is the correct answer. The cricothyroid muscle of the
mately 180 mg/100 mL, the glucose spills out into the
larynx is innervated by the external laryngeal nerve,
urine. The exact cause of diabetes mellitus is not
which was damaged in this patient.
known. Genetic, metabolic, and autoimmune factors,
8.
The patient is suffering from parathyroid tetany due to
as well as viral infections, are thought to play an impor-
accidental removal of one or more of the parathyroid
tant causative role in many patients. Excessive glucagon
glands during the operation of total thyroidectomy.
secretion combined with insulin deficiency has been
Sometimes the condition occurs following interference
suggested as a contributing cause of the high levels of
with the blood supply to these glands. The function of
blood glucose. It should be remembered that insulin
the parathyroid gland is to secrete a hormone that
stimulates the uptake and storage of glucose in the liver
regulates calcium metabolism and plasma calcium
and muscle, whereas glucagon inhibits this process.
concentration. A low level of plasma calcium results in
13.
Because the testes were removed after puberty, many of
increased neuromuscular excitability and the clinical
the accessory sex organs of this patient will atrophy and
syndrome known as tetany.
the secondary sexual characteristics will regress. Testos-
9.
E is the correct answer. A thyroglossal cyst occurs most
terone is produced in individuals with undescended
commonly in the midline of the neck below the hyoid
testes because the interstitial cells are not as sensitive to
bone and above the isthmus of the thyroid gland. It
heat as are the germinal epithelium of the seminiferous
should be emphasized that it can occur anywhere along
tubules.
the path of the thyroglossal tract, even as far superiorly
14.
A summary of the clinical signs and symptoms of
as the foramen cecum of the tongue. As the cyst en-
menopause are given on CD page 420. At menopause,
larges it is prone to infection, so it should be removed
the few remaining graafian follicles of the ovary cease to
surgically.
be sensitive to stimulation by the gonadotropic hor-
10.
Addison’s disease occurs as a result of the destruction of
mones of the pars anterior of the pituitary, even though
the suprarenal cortex by tuberculosis or idiopathic
the blood levels of these hormones rise after menopause.
atrophy; it may also occur secondary to a failure of elab-
The hypothalamus-pituitary- ovary hormonal mecha-
oration of adrenocorticotropic hormone (ACTH) from
nism thus ceases to operate.
Useful Anatomical Data of
Appendix
Clinical Significance
Appendix Outline
Respiratory System
426
Table VII. Summary of the Movements of the
Knee Joint and the Muscles Producing
Table I. Important Airway Distances (Adult)
426
Those Movements
434
Table II. Important Data Concerning the Trachea
426
Table VIII. Summary of the Movements of the Ankle
Musculoskeletal System
427
Joint and the Muscles Producing Those
Table III. Summary of the Movements of the
Movements
435
Shoulder Joint and the Muscles Producing
Digestive System
436
Those Movements
427
Table IX. Lengths and Capacities
436
Table IV. Summary of the Movements of the
Urinary System
436
Elbow Joint and the Muscles Producing
Those Movements
429
Table X. Lengths and Capacities
436
Table V. Summary of the Movements of the
Reproductive System
436
Wrist Joint and the Muscles Producing
Table XI. Dimensions
436
Those Movements
430
Embryology
437
Table VI. Summary of the Movements of the
Hip Joint and the Muscles Producing
Table XII. The Size and Weight of the Developing
Those Movements
432
Human Embryo and Fetus
437
Respiratory System
Important Airway Distances
Important Data Concerning
Table I
Table II
(Adult)a
the Tracheaa
Distances
Length (approx.)
Diameter (approx.)
Airway
(approx.)
Adults
4.5 in. (11.4 cm)
1 in. (2.5 cm)
Incisor teeth to the vocal cords
5.9 in. (15 cm)
Infants
1.6-2 in. (4-5 cm)
As small as 3 mmb
Incisor teeth to the carina
7.9 in. (20 cm)
External nares to the carina
11.8 in. (30 cm)
a Extension of the head and neck, as when maintaining
an airway in an anesthetized patient, may stretch the
trachea and increase its length by 25%. In the adult,
a Average figures given
1-2 cm.
the carina may descend by as much as 3 cm on deep
inspiration. At the carina, the right bronchus leaves the
trachea at an angle of 25° from the vertical and the left
bronchus leaves the trachea at an angle of 45° from
the vertical. In children younger than 3 years, both
bronchi arise from the trachea at equal angles.
b As children grow, the diameter in millimeters
corresponds approximately to their age in years.
Appendix
427
Musculoskeletal System
Summary of the Movements of the Shoulder Joint and the Muscles Producing
Table III
Those Movementsa
Segmental
Movements
Muscles
Origin
Insertion
Nerve Supply
Nerveb
Flexion
Deltoid (anterior
Clavicle
Middle of lateral
Axillary nerve
C5, 6
fibers)
surface of shaft
of humerus
Pectoralis major
Clavicle
Lateral lip bicipital
Medial and lateral
C5, 6
(clavicular
groove of humerus
pectoral nerves
part)
from brachial
plexus
Biceps brachii
Long head
Supraglenoid
Tuberosity of
Musculocutaneous
C5, 6
tubercle of scapula
radius, deep fascia
nerve
of forearm
Short head
Coracoid process
of scapula
Coraco-
Coracoid process
Medial aspect of
Musculocutaneous
C5, 6, 7
brachialis
of scapula
shaft of humerus
nerve
Extension
Deltoid
Spine of scapula
Middle of lateral
Axillary nerve
C5, 6
(posterior
surface of shaft
fibers)
of humerus
Latissimus dorsi
Iliac crest, lumbar
Floor of bicipital
Thoracodorsal
C6, 7, 8
fascia, spines of
groove of
nerve
lower six thoracic
humerus
vertebrae, lower
three or four ribs,
and inferior angle
of scapula
Teres major
Lower third lateral
Medial lip of
Lower subscapular
C6, 7
border of scapula
bicipital groove
nerve
of humerus
Abduction
Middle fibers
Acromion process
Middle of lateral
Axillary nerve
C5, 6
of deltoid
of scapula
surface of shaft
of humerus
Supraspinatus
Supraspinous fossa
Greater tuberosity
Suprascapular
C4, 5, 6
of scapula
of humerus
nerve
Adduction
Pectoralis major
Sternum and upper
Lateral lip of
Medial and lateral
C7, 8; T1
(sternal part)
six costal
bicipital groove
pectoral nerves
cartilages
of humerus
Latissimus dorsi
Iliac crest, lumbar
Floor of bicipital
Thoracodorsal
C6, 7, 8
fascia, spines of
groove of humerus
nerve
lower six thoracic
vertebrae, lower
three or four ribs,
inferior angle of
scapula
428
Appendix
Table III
(continued)
Segmental
Movements
Muscles
Origin
Insertion
Nerve Supply
Nerveb
Teres major
Lower third lateral
Medial lip of
Lower subscapular
C6, 7
border of scapula
bicipital groove
nerve
of humerus
Teres minor
Upper two thirds
Greater tuberosity
Axillary nerve
C5, 6
lateral border of
of humerus
scapula
Lateral
Infraspinatus
Infraspinous fossa
Greater tuberosity
Suprascapular
C5, 6
rotation
of scapula
of humerus
nerve
Teres minor
Upper two thirds
Greater tuberosity
Axillary nerve
C5, 6
lateral border of
of humerus
scapula
Deltoid
Spine of scapula
Middle of lateral
Axillary nerve
C5, 6
(posterior
surface of shaft
fibers)
of humerus
Medial
Subscapularis
Subscapular fossa
Lesser tuberosity
Upper and lower
C5, 6
rotation
of humerus
subscapular
nerves
Latissimus
Iliac crest, lumbar
Floor of bicipital
Thoracodorsal
C6, 7, 8
dorsi
fascia, spines of
groove of
nerve
lower three or
humerus
four ribs, inferior
angle of scapula
Teres major
Lower third lateral
Medial lip bicipital
Lower subscapular
C6, 7
border of
groove of
nerve
scapula
humerus
Deltoid (anterior
Clavicle
Middle of lateral
Axillary nerve
C5, 6
fibers)
surface of shaft
of humerus
a Circumduction is a combination of all the movements described.
b The predominant segmental nerve supply is indicated by boldface type.
Appendix
429
Musculoskeletal System
Summary of the Movements of the Elbow Joint and the Muscles Producing
Table IV
Those Movements
Segmental
Movements
Muscles
Origin
Insertion
Nerve Supply
Nervea
Flexion
Brachialis
Front of lower
Coronoid process
Musculocutaneous
C5, 6
half of humerus
of ulna
nerve
Biceps brachii
Long head
Supraglenoid
Tuberosity of
Musculocutaneous
C5, 6
tubercle of
radius, deep
nerve
scapula
fascia of forearm
Short head
Coracoid process
of scapula
Brachioradialis
Lateral
Styloid process
Radial nerve
C5, 6, 7
supracondylar
of radius
ridge of humerus
Pronator teres
Humeral head
Medial epicondyle
Lateral aspect of
Median nerve
C6, 7
of humerus
shaft of radius
Ulnar head
Coronoid process
of ulna
Extension
Triceps
Long head
Infraglenoid tubercle
Olecranon
Radial nerve
C6, 7, 8
of scapula
process of ulna
Lateral head
Posterior surface of
shaft of humerus
Medial head
Lower half of
posterior surface
of shaft of humerus
Anconeus
Lateral epicondyle
Olecranon
Radial nerve
C7, 8; T1
of humerus
process of ulna
aThe predominant segmental nerve supply is indicated by boldface type.
430
Appendix
Musculoskeletal System
Summary of the Movements of the Wrist Joint and the Muscles Producing Those
Table V
Movements
Segmental
Movements
Muscles
Origin
Insertion
Nerve Supply
Nervea
Flexion
Flexor carpi
Medial epicondyle
Bases of second
Median nerve
C6, 7
radialis
of humerus
and third
metacarpal bones
Flexor carpi
ulnaris
Humeral head
Medial epicondyle
Pisiform bone,
Ulnar nerve
C7, 8
of humerus
hook of hamate,
base of fifth
metacarpal bone
Ulnar head
Olecranon process,
posterior border
of ulna
Palmaris longus
Medial epicondyle
Flexor
Median nerve
C7, 8
of humerus
retinaculum,
palmar
aponeurosis
Flexor digitorum
superficialis
Humeroulnar
Medial epicondyle
Middle phalanx
Median nerve
C7, 8; T1
head
of humerus,
of medial four
coronoid process
fingers
of ulna
Radial head
Oblique line anterior
surface shaft of
radius
Flexor digitorum
Anterior surface
Distal phalanx
Ulnar half—
C8; T1
profundus
shaft of ulna,
of medial four
ulnar nerve,
interosseous
fingers
radial half—
membrane
median nerve
Flexor pollicis
Anterior surface
Distal phalanx
Anterior
C8; T1
longus
shaft of radius
of thumb
interosseous
branch of
median nerve
Extension
Extensor carpi
Lateral supracondylar
Base of second
Radial nerve
C6, 7
radialis longus
ridge of humerus
metacarpal bone
Extensor carpi
Lateral epicondyle of
Base of third
Deep branch
C7, 8
radialis brevis
humerus
metacarpal bone
of radial nerve
Extensor carpi
Lateral epicondyle
Base of fifth
Deep branch
C7, 8
ulnaris
of humerus
metacarpal bone
of radial nerve
Extensor
Lateral epicondyle
Middle and distal
Deep branch of
C7, 8
digitorum
of humerus
phalanges of
radial nerve
medial four
fingers
Appendix
431
Table V
(continued)
Segmental
Movements
Muscles
Origin
Insertion
Nerve Supply
Nervea
Extensor indicis
Shaft of ulna and
Extensor
Deep branch of
C7, 8
interosseous
expansion of
radial nerve
membrane
index finger
Extensor digiti
Lateral epicondyle
Extensor
Deep branch of
C7, 8
minimi
of humerus
expansion of
radial nerve
little finger
Extensor pollicis
Shaft of ulna and
Base of distal
Deep branch of
C7, 8
longus
interosseous
phalanx of thumb
radial nerve
membrane
Abduction
Flexor carpi
Medial epicondyle
Bases of second
Median nerve
C6, 7
radialis
of humerus
and third
metacarpal bones
Extensor carpi
Lateral
Base of second
Radial nerve
C6, 7
radialis longus
supracondylar
metacarpal bone
ridge of humerus
Extensor carpi
Lateral epicondyle
Bases of third
Deep branch of
C7, 8
radialis brevis
of humerus
metacarpal bone
radial nerve
Abductor pollicis
Shafts of radius
Base of first
Deep branch of
C7, 8
longus
and ulna
metacarpal bone
radial nerve
Extensor pollicis
Shaft of ulna and
Base of distal
Deep branch of
C7, 8
longus
interosseous
phalanx of thumb
radial nerve
membrane
Extensor pollicis
Shaft of radius and
Base of proximal
Deep branch of
C7, 8
brevis
interosseous
phalanx of thumb
radial nerve
membrane
Adduction
Flexor carpi
ulnaris
Humeral head
Medial
Pisiform bone,
Ulnar nerve
C7, 8
epicondyle of
hook of
humerus
hamate, base
of fifth
metacarpal bone
Ulnar head
Olecranon process
of ulna
Extensor carpi
Lateral epicondyle
Base of fifth
Deep branch of
C7, 8
ulnaris
of humerus
metacarpal
radial nerve
bone
a The predominant segmental nerve supply is indicated by boldface type.
432
Appendix
Musculoskeletal System
Summary of the Movements of the Hip Joint and the Muscles Producing
Table VI
Those Movementsa
Segmental
Movements
Muscles
Origin
Insertion
Nerve Supply
Nerveb
Flexion
Iliacus
Iliac fossa
Lesser trochanter
Femoral nerve
L2, 3
of femur
Psoas
Body of twelfth
Lesser trochanter
Lumbar plexus
L1, 2, 3
thoracic vertebra,
of femur
transverse
processes, bodies
and intervertebral
discs of the five
lumbar vertebrae
Rectus femoris
Straight head
Anterior inferior
Patella
Femoral nerve
L2, 3, 4
iliac spine
Reflected head
Ilium above
acetabulum
Sartorius
Anterior superior
Upper medial
Femoral nerve
L2, 3
iliac spine
surface of shaft
of tibia
Extension
Gluteus
Outer surface of
Iliotibial tract,
Inferior gluteal
L5; S1, 2
(a posterior
maximus
ilium, sacrum,
gluteal
nerve
movement
coccyx, sacrotuber-
tuberosity of
of the flexed
ous ligament
femur
thigh)
Biceps femoris
Long head: ischial
Head of fibula
Tibial nerve
L5; S1, 2
tuberosity
(sciatic nerve)
Semitendinosus
Ischial tuberosity
Upper part of
Tibial nerve
L5; S1, 2
medial surface of
(sciatic nerve)
shaft of tibia
Semimembra-
Ischial tuberosity
Medial condyle of
Tibial nerve
L5; S1, 2
nosus
tibia
(sciatic nerve)
Adductor magnus
Ischial tuberosity
Adductor tubercle
Tibial nerve
L2, 3, 4
of femur
(sciatic nerve)
Abduction
Gluteus medius
Outer surface of
Greater
Superior gluteal
L5; S1
ilium
trochanter of
nerve
femur
Gluteus minimus
Outer surface of
Greater
Superior
L5; S1
ilium
trochanter of
gluteal nerve
femur
Sartorius
Anterior superior
Upper medial
Femoral nerve
L2, 3
iliac spine
surface of shaft
of tibia
Tensor fasciae
Iliac crest
Iliotibial tract
Superior gluteal
L4, 5
latae
nerve
Piriformis
Anterior surface of
Greater
Sacral plexus
L5; S1, 2
sacrum
trochanter of
femur
Appendix
433
Table VI
(continued)
Segmental
Movements
Muscles
Origin
Insertion
Nerve Supply
Nervea
Adduction
Adductor longus
Body of pubis
Posterior surface
Obturator nerve
L2, 3, 4
of shaft of femur
Adductor brevis
Inferior ramus of
Posterior surface
Obturator nerve
L2, 3, 4
pubis
of shaft of femur
Adductor magnus
Inferior ramus of
Posterior surface
Obturator nerve
L2, 3, 4
(adductor fibers)
pubis, ramus of
of shaft of femur,
ischium, ischial
adductor tubercle
tuberosity
of femur
Pectineus
Superior ramus of
Upper end of
Femoral nerve
L2, 3
pubis
shaft of femur
Gracilis
Inferior ramus of
Upper part of
Obturator nerve
L2, 3
pubis, ramus of
shaft of tibia on
ischium
medial surface
Lateral
Piriformis
Anterior surface of
Greater trochanter
Sacral plexus
L5; S1, 2
rotation
sacrum
of femur
Obturator
Inner surface of
Greater trochanter
Sacral plexus
L5; S1
internus
obturator membrane
of femur
Obturator
Outer surface of
Greater trochanter
Obturator nerve
L3, 4
externus
obturator membrane
of femur
Superior
Spine of ischium
Greater trochanter
Sacral plexus
L5; S1
gemellus
of femur
Inferior gemellus
Ischial tuberosity
Greater trochanter
Sacral plexus
L5; S1
of femur
Quadratus
Ischial tuberosity
Quadrate tubercle
Sacral plexus
L5; S1
femoris
on upper end of
posterior
surface of femur
Gluteus maximus
Outer surface of
Iliotibial tract,
Inferior gluteal
L5; S1, 2
ilium, sacrum,
gluteal tuberosity
nerve
coccyx,
of femur
sacrotuberous
ligament
Medial
Gluteus medius
Outer surface of
Greater trochanter
Superior gluteal
L5; S1
rotation
ilium
of femur
nerve
Gluteus
Outer surface of ilium
Greater trochanter
Superior gluteal
L5; S1
minimus
of femur
nerve
Tensor fasciae
Iliac crest
Iliotibial tract
Superior
L4, 5
latae
gluteal nerve
a Circumduction is a combination of all the movements described.
b The predominant segmental nerve supply is indicated by boldface type.
434
Appendix
Musculoskeletal System
Summary of the Movements of the Knee Joint and the Muscles
Table VII
Producing Those Movements
Segmental
Movements
Muscles
Origin
Insertion
Nerve Supply
Nervea
Flexion
Biceps femoris
Long head
Ischial tuberosity
Head of fibula
Tibial nerve
L5; S1, 2
Short head
Shaft of femur
Common
peroneal
nerve
Semitendinosus
Ischial tuberosity
Upper part of
Tibial nerve
L5; S1, 2
medial surface
of shaft of tibia
Semimem-
Ischial tuberosity
Medial condyle of
Tibial nerve
L5; S1, 2
branosus
tibia
Gastrocnemius
Medial, lateral
Via Achilles tendon
Tibial nerve
S1, 2
condyles of
into calcaneum
femur
Extension
Quadriceps
femoris: rectus
femoris
Straight head
Anterior inferior
Patella
Femoral nerve
L2, 3, 4
iliac spine
Reflected head
Ilium above
acetabulum
Vastus lateralis
Upper end and
Patella
Femoral nerve
L2, 3, 4
shaft of femur
Vastus medialis
Upper end and
Patella
Femoral nerve
L2, 3, 4
shaft of femur
Vastus inter-
Shaft of femur
Patella
Femoral nerve
L2, 3, 4
medius
Medial
Sartorius
Anterior superior
Upper medial
Femoral nerve
L2, 3
rotation
iliac spine
surface of shaft
of tibia
Gracilis
Interior ramus of
Upper part of shaft
Obturator nerve
L2, 3
pubis, ramus
of tibia on medial
of ischium
surface
Lateral
Biceps femoris
rotation
Long head
Ischial tuberosity
Head of fibula
Tibial nerve
L5; S1, 2
Short head
Shaft of femur
—
Common
L5; S1, 2
peroneal
nerve
a The predominant segmental nerve supply is indicated by boldface type.
Appendix
435
Musculoskeletal System
Summary of the Movements of the Ankle Joint and the Muscles Producing
Table VIII
Those Movements
Nerve
Segmental
Movements
Muscles
Origin
Insertion
Supply
Nervea
Dorsiflexion
Tibialis anterior
Shaft of tibia,
Medial cuneiform,
Deep peroneal
L4,5
interosseous
base of first
nerve
membrane
metatarsal bone
Extensor hallucis
Shaft of fibula,
Base of distal
Deep peroneal
L5, S1
longus
interosseous
phalanx of great
nerve
membrane
toe
Extensor digitorum
Shaft of fibula,
Dorsal extensor
Deep peroneal
L5, S1
longus
interosseous
expansion of
nerve
membrane
lateral four toes
Peroneus tertius
Shaft of fibula,
Base of fifth
Deep peroneal
L5, S1
interosseous
metatarsal bone
nerve
membrane
Plantar-
Gastrocnemius
Medial, lateral
Via Achilles tendon
Tibial nerve
S1,2
flexion
condyles of
into calcaneum
femur
Soleus
Shaft of tibia
Via Achilles tendon
Tibial nerve
S1,2
and fibula
into calcaneum
Plantaria
Lateral supra-
Calcaneum
Tibial nerve
S1,2
condylar ridge
of femur
Peroneus longus
Shaft of fibula
Base of first
Superficial
L5; S1,2
metatarsal and
peroneal nerve
medial cuneiform
Peroneus brevis
Shaft of fibula
Base of fifth
Superficial
L5; S1,2
metatarsal bone
peroneal nerve
Tibialis posterior
Shaft of tibia,
Tuberosity of
Tibial nerve
L4,5
fibula, in-
navicular
terosseous
membrane
Flexor digitorum
Shaft of tibia
Distal phalanges
Tibial nerve
S2,3
longus
of lateral four toes
Flexor hallucis
Shaft of fibula
Base of distal
Tibial nerve
S2,3
longus
phalanx of big toe
a The predominant segmental nerve supply is indicated by boldface type.
436
Appendix
Digestive System
Table IX
Lengths and Capacities
Region (approx.)
Lengths (approx.)
Capacities (Approx.)
Esophagus
10 in. (25 cm)
—
Stomacha
Lesser curvature 4.8-5.6 in. (12-14 cm)
1,500 mL
Duodenum
10 in. (25 cm)
—
Jejunum
8 ft (2.4 M)
—
Ileum
12 ft (3.7 M)
—
Appendix
3-5 in. (8-13 cm)
—
Ascending colon
5 in. (13 cm)
—
Transverse colon
15 in. (38 cm)
—
Descending colon
10 in. (25 cm)
—
Sigmoid colon
10-15 in. (25-38 cm)
—
Rectum
5 in. (13 cm)
—
Anal canal
1.5 in. (4 cm)
—
Gallbladder
2.8-3.9 in. (7-10 cm)
30-50 mL
Cystic duct
1.5 in. (3.8 cm)
—
Bile duct
3 in. (8 cm)
—
a The curved course taken by a nasogastric tube from the cardiac orifice to the pylorus is usually
longer, 6-10 in. (15-25 cm).
Urinary System
Reproductive System
Table X
Lengths and Capacities
Table XI
Dimensions
Capacity
Organ
Dimensions (approx.)
Organ
Lengths (approx.)
(approx.)
Male
Ureter
10 in. (25 cm)
—
Testis
2
1 in. (5
2.5 cm)
Bladder
—
500 mL
Vas deferens
18 in. (45 cm)
Male urethra
8 in. (20 cm)
—
Penis (erect)
6 in. (15 cm)
Penile
6 in. (15.7 cm)
—
Female
Membranous
0.5 in. (1.25 cm)
—
Ovary
1.5
0.75 in. (4
2 cm)
Prostatic
1.25 in. (3 cm)
—
Uterine tube
4 in. (10 cm)
Female urethra
1.5 in. (3.8 cm)
—
Uterus
3
2
1 in. (8
5
2.5 cm)
Vagina
3 in. (8 cm)
Appendix
437
Embryology
The Size and Weight of the
Table XII
Developing Human Embryo
and Fetus
Age of
Conception
Crown-Rump
(weeks)
Length (mm)
Weight (g)
4
5
0.02
5
8
—
8
23
1
12
56
14
16
112
105
20
160
310
24
203
640
28
242
1,080
32
277
1,670
36
313
2,400
Full term
350
3,300
Reprinted with permission, Arey 1966.
CD Figure APP-1
Critical times in the maturation of the human fetus during which
mutant genes, drugs, or environmental factors may alter normal development of specific
structures.