1488
PART VIII
GENITOURINARY DISORDERS
resolve, or the degree of ureteral dilation may improve
Complications of cutaneous vesicostomy include stomal
enough that ureteral tapering is not required at the time of
stenosis, prolapse, peristomal dermatitis, and bladder calculi.
reimplantation.3-4
Although bacterial colonization of the
Stomal stenosis is more common with a stiff or thick bladder
open system is common, symptomatic infections and urosepsis
wall as in posterior urethral valves. Failure to fashion the vesi-
are reduced. One concern about prolonged vesicostomy
costomy from the dome of the bladder may allow the posterior
drainage in the non-neuropathic population is failure of
bladder wall to prolapse through the vesicostomy. This is one
the bladder to develop normally in the absence of cyclic
advantage of the Blocksom technique over the Lapides vesi-
filling and emptying.10-11 Several studies have refuted this
costomy. Prolapse is managed by manual reduction with tem-
concern.4,12-13
porary catheter drainage and revision of the low vesicostomy.
Once the urinary tract is stabilized and the long-term po-
Dermatitis is particularly bothersome in some patients and is
tential of the bladder becomes clearer, the vesicostomy is eas-
managed with application of a zinc oxide barrier cream or top-
ily closed. It may be closed primarily or in combination with
ical treatment for obvious candidiasis. Bladder calculi are un-
continent diversion. Some patients and families are not appro-
usual provided that the vesicostomy is functioning well and
priate candidates for vesicostomy closure or find that vesicos-
the upper tracts are drained.
tomy and diaper drainage is an acceptable low-maintenance
permanent option. Vesicostomy, with or without the use of
CUTANEOUS URETEROSTOMY
an ostomy appliance, can also be performed in adult patients
who are not candidates for continent diversion.9
Ureterostomy for temporary supravesical urinary diversion is
Two techniques for cutaneous vesicostomy have been used
rarely performed today. It has been used historically for drain-
for many years. Lapides described elevation of an anterior blad-
age of a profoundly dilated upper urinary tract in the face of
der wall flap with deep insertion of an abdominal skin flap to
urosepsis17 or to maximize drainage of the renal units in cases
fashion the cutaneous vesicostomy.14 The more common tech-
of severe obstruction. Percutaneous or endourologic drainage
nique was described by Blocksom in 195715 and modified by
of these systems is possible now in children, but tube size
Duckett (Fig. 118-1).16 The Blocksom vesicostomy is fashioned
limits the utility of this in very small infants.18 Low diversion
through a small transverse incision halfway between the umbi-
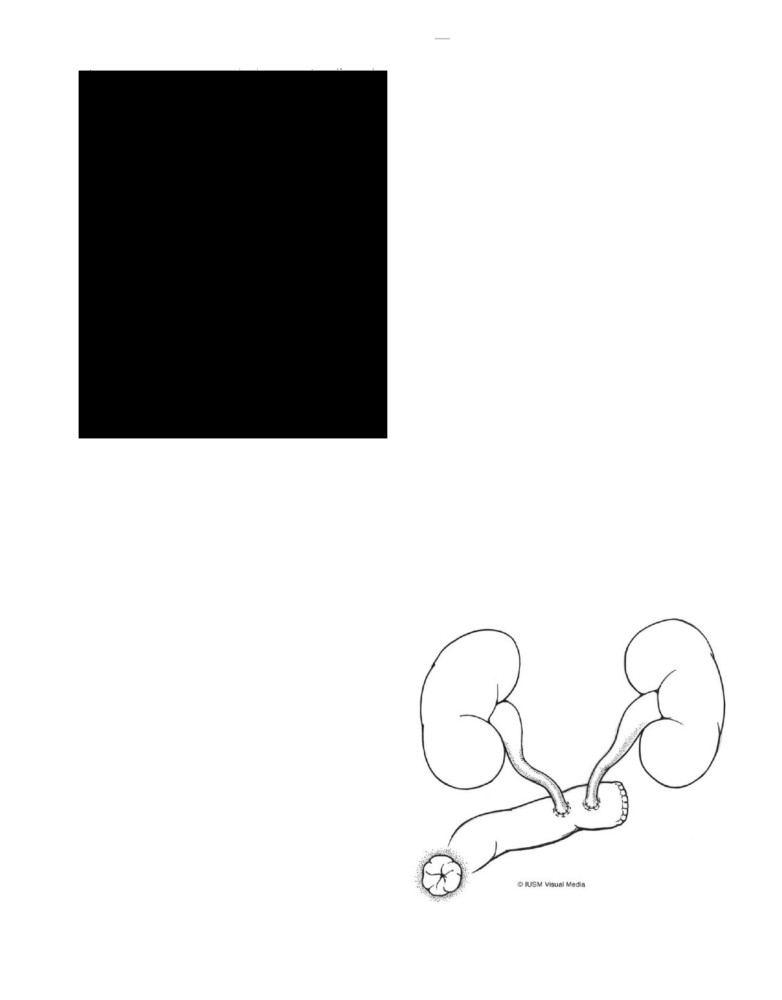
can be performed as a loop or end cutaneous ureterostomy
licus and the pubis. The fascia is incised, and the peritoneum is
(Figs. 118-2 and 118-3), and subsequent takedown involves
pushed superiorly off the dome of the bladder. The urachal
ureteroneocystostomy. The diversion allows the caliber of
remnant is divided, and the dome of the bladder is pulled
the ureter to decrease, thereby reducing the complexity of
up to the skin. The fascia is secured to the bladder wall to form
the reimplantation. Diversion at the level of the kidney is per-
a 24-Fr defect, and the bladder is matured as a flush stoma.
formed through a flank incision and can be performed as a
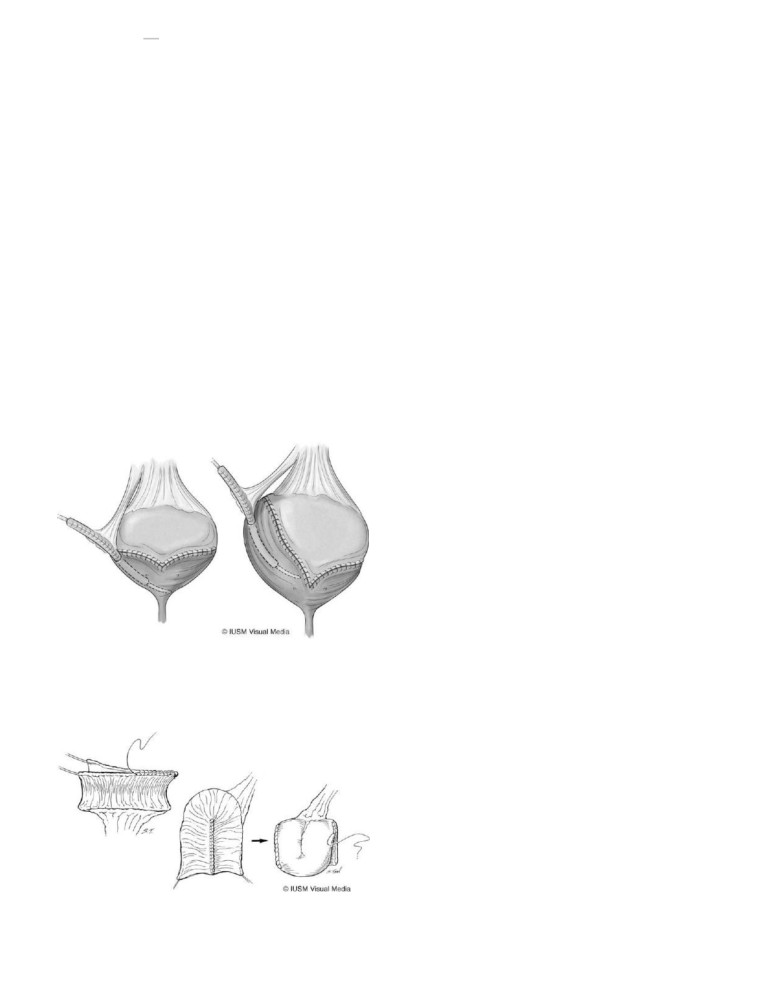
FIGURE 118-1
The Blocksom vesicostomy, showing the incision in the
FIGURE 118-2
The loop ureterostomy is easily taken down and there-
dome of the bladder, the fixation to the overlying fascia, and the everted
fore allows for an excellent temporary diversion.
stoma.
CHAPTER 118
INCONTINENT AND CONTINENT URINARY DIVERSION
1489
Another method to treat distal ureteral obstruction is cre-
ation of a freely refluxing end-to-side or side-to-side ureteral
reimplant.23 This alternative approach, while obviating the
continual drainage of urine via a cutaneous stoma, remains
controversial.
CUTANEOUS PYELOSTOMY
As with cutaneous ureterostomy, proximal diversion by pye-
lostomy has limited indications in current practice. The con-
troversies surrounding this type of diversion are similar. With
direct drainage of the renal pelvis, pyelostomy may be used for
temporary diversion in select cases of obstruction at the ure-
teropelvic junction but could also be used as discussed earlier
for posterior urethral valves. Pyelostomy requires a dilated
extrarenal pelvis to create a tension-free anastomosis to the
skin. Takedown of the pyelostomy at the time of a definitive
procedure is relatively simple due to reliable blood supply
to the renal pelvis.
ILEAL CONDUIT/COLON CONDUIT
Permanent supravesical urinary diversion was popular many
decades ago as reliable means to manage neuropathic bladder,
bladder outlet obstruction, and severe urinary incontinence.
Conduit diversions have been created with most intestinal
segments, although the ileum (Fig. 118-4) and colon are used
FIGURE 118-3
The end ureterostomy requires formal reimplantation to
most commonly. Both simple refluxing and tunneled nonre-
reverse.
fluxing ureterointestinal anastomoses have been used. The
primary advantage of the colon conduit over an ileal conduit
loop ureterostomy, Sober ureterostomy, or end ureterostomy.
is the reliable antireflux reimplantation achievable with colon.
A loop ureterostomy can easily be taken down and is the more
The risk of upper tract deterioration after ileal conduit di-
appropriate choice for temporary diversion. End ureterostomy
version has exceeded 50% in some series.24-26 Although this
just below the ureteropelvic junction makes reconstitution of
is not a tremendous concern in the older patient after cystec-
the ureter more difficult and should be reserved as a rare per-
tomy for bladder carcinoma, the long-term impact on the kid-
manent form of diversion in cases of severe bladder dysfunc-
neys is extremely relevant in the pediatric population. The
tion.18 Sober ureterostomy, with its proximal diverting limb
ability to create a nonrefluxing anastomosis between the ureter
and reanastomosis of the distal limb to the renal pelvis, is rarely
used today and is technically much more involved and may
therefore be less appropriate for diversion during acute illness.
On the other hand, it offers the advantage of diversion and
continued antegrade drainage to cycle the bladder.19 In all
cases, care should be taken to preserve the medial blood sup-
ply and adventitial vessels and to create a tension-free anasto-
mosis to the skin. Given the profoundly dilated nature of the
ureter in most of these cases, stomal stenosis is rarely an issue.
Supravesical diversion may be warranted in select posterior
urethral valve patients when renal function fails to improve af-
ter bladder drainage.19 Persistent ureterovesical junction ob-
struction is the concern. Ureterostomy and pyelostomy
would maximize upper tract drainage, but percutaneous
nephrostomy is a less invasive temporary means to assess the
potential of the affected kidney.20 Patients who demonstrate
improvement in renal function after supravesical diversion
may do so because of better drainage or just due to normal renal
maturation.21 As with cutaneous vesicostomy, there is concern
that the valve bladder will fail to develop normally if the urine is
diverted. In patients with a solitary functioning kidney, a loop
ureterostomy or an end ureterostomy would defunctionalize
the bladder. Several studies suggest that bladder dysfunction
is due to bladder wall abnormalities from infravesical obstruc-
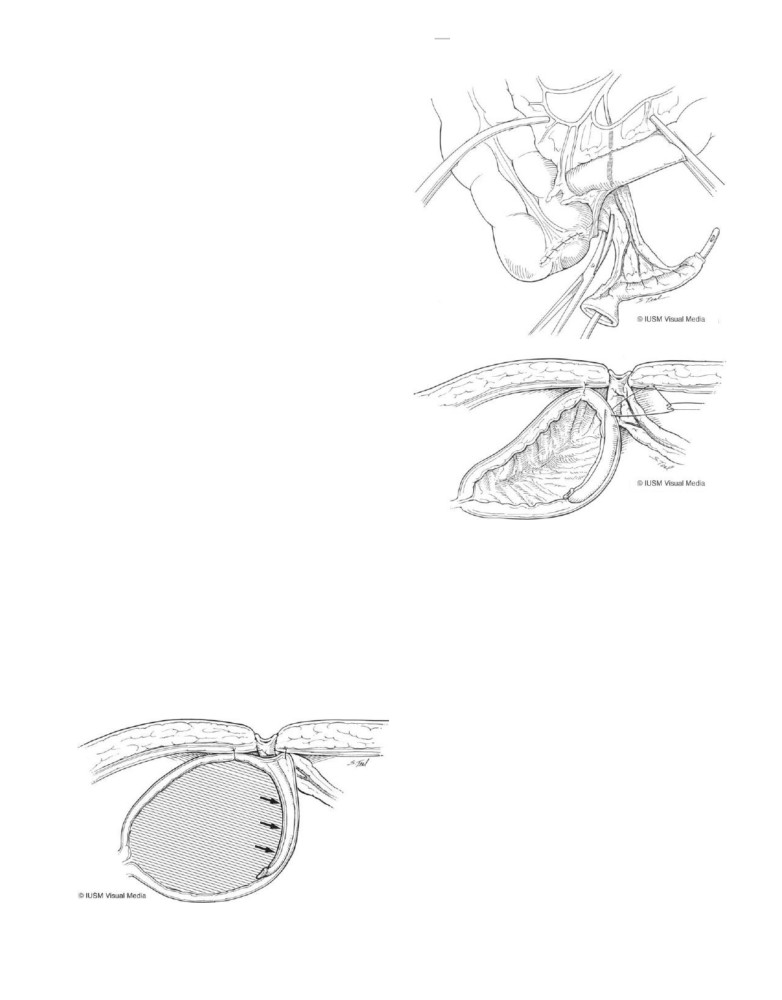
FIGURE 118-4
The ileal conduit is the standard permanent supravesical
tion rather than supravesical diversion of urine.13,22
diversion for patients whose bladder is absent.
1490
PART VIII
GENITOURINARY DISORDERS
and colon gives colon conduits a theoretical advantage over
other efforts to manage the bladder pressures and urinary in-
ileal conduits. Unfortunately, deterioration of the upper tracts
continence and refused or were not candidates for continent
occurs in 26% to 48% of cases and ureteral reflux persists in
diversion. Many suffered severe complications from use of a
8% to 58% of colon conduits.27
Anastomotic stricture
chronic indwelling urethral catheter. Several series report ex-
occurs with similar frequency with ileum and colon (9%
cellent results with regard to preservation of renal function,
to 22%).24,27
incidence of urinary tract infection and urolithiasis, and sto-
Koch and colleagues24 compared a cohort of myelomenin-
mal complications.32-35 The ileovesicostomy functions as a
gocele patients with ileal conduit diversion to another group
pop-off valve to maintain safe bladder storage pressures. Sto-
managed with CIC. The ileal conduit group suffered renal de-
mal leak-point pressures are low, and a moderate residual
terioration, nephrolithiasis, and pyelonephritis significantly
urine remains.35
more than the catheterization group. Bone density was de-
Incontinent ileovesicostomy is an option to consider in
creased in both groups and the incidence of fractures was
select pediatric patients with limited dexterity and social
equal, but the diversion group had impaired linear growth,
support. Although it does require a permanent stoma, pres-
more spinal curvature, and more complications from orthope-
ervation of renal function appears superior when compared
dic procedures. The metabolic alterations associated with in-
with standard conduit diversion. In addition, the disruption
corporation of intestinal segments into the urinary tract do
of the ureterovesical junction is not required. Parents may
occur with incontinent diversions.24
have difficulty accepting permanent diversion even if the
Other complications of conduit diversion included stomal
child has limited potential to perform self-catheterization
stenosis, stomal prolapse, peristomal hernia, and peristomal
in the future. Some families are not ready to assume the care
dermatitis. Stomal stenosis occurred in 8% to 61% of cases.
required for bladder augmentation or continent urinary
Stoma complications are best prevented with careful surgical
reservoir, despite the fact that the child needs reconstruction
technique including preservation of intestinal perfusion, cre-
to preserve the upper urinary tracts. In these instances,
ation of a straight and adequate caliber fascial window, and fix-
incontinent ileovesicostomy with both an efferent inconti-
ation of the conduit to the fascia. A protuberant rosebud stoma
nent limb and a large open patch of ileum to augment the
enhances the fit of the stoma appliance and prevents stenosis.
bladder can be considered. Consideration could be given
Bacteriuria is nearly universal but does not cause upper
to creation of a Mitrofanoff catheterizable channel at the time
tract damage if the ureterointestinal anastomosis and the con-
of the initial procedure. Should the family later embrace
duit itself function appropriately.27-28
Stasis of colonized
continence and the long-term care of bladder augmentation,
urine, however, may contribute to upper tract stone formation
the ileal chimney can be amputated to leave a continent
and may have other implications as well. Nitrosamines pro-
diversion.36
duced by the mixture of urine and bacteria appear to have
Thorough preoperative bowel preparation and sterilization
some role in induction of malignancy in the isolated intestinal
of the urine are required. A stoma site is carefully preplanned
segment.27,29
for the right lower quadrant to ensure optimal fit of the stoma
Austen recently reviewed the world literature and identi-
appliance. The bladder is bivalved in the coronal plane in
fied 81 tumors collectively in a variety of continent and incon-
preparation for anastomosis to the isolated ileal segment.
tinent diversions with incorporated bowel segments. This
The proximal end of the ileum is opened widely on its antime-
total is exclusive of the large number of malignancies reported
senteric border and anastomosed to the bladder in a running
after ureterosigmoidostomy. Neoplasia was reported in 12 ileal
fashion. The length of the ileal segment can be tailored to ac-
conduits and 5 colon conduits with a mean latency of 22 and
count for body habitus and for the need to augment the native
10 years, respectively. Colon conduit tumors were exclusively
bladder capacity.32 A rosebud stoma is fashioned in the right
adenocarcinoma, but transitional cell carcinoma, squamous
lower quadrant, and a 22-Fr catheter is left in place for 3
cell carcinoma, and carcinoid and anaplastic tumors were also
weeks to maintain the caliber of the ileovesical anastomosis.
found in ileal conduits. Chronic inflammation of the intestinal
If significant augmentation is performed, a suprapubic
segment may play a role in the malignant changes. Early yearly
catheter should be left as well to maximize perioperative
surveillance for tumor is recommended.30
drainage. In select patients with perineal excoriation from
Preoperative preparation for conduit diversion involves a
urinary incontinence, a bladder neck or urethral procedure
full mechanical and antibiotic bowel preparation and paren-
in conjunction with an ileovesicostomy may be used to create
teral antibiotic to sterilize the urine on the day before surgery.
outlet resistance.
Patients with severe neuropathic bowel may actually require
more than one day of preparation for adequate cleanout. It
is critical that an enterostomal therapist mark potential stoma
sites bilaterally after examining the patient in multiple posi-
Continent Urinary Diversion
------------------------------------------------------------------------------------------------------------------------------------------------
tions. The abdominal contour can change significantly in mye-
lomeningocele patients when seated, and an ill-fitting ostomy
Many different types of continent urinary diversions have
appliance will be a lasting source of dissatisfaction.
been developed to improve or replace the native lower urinary
tract. The chosen technique depends largely on the surgeon’s
experience and preference, but the primary pathology plays a
INCONTINENT ILEOVESICOSTOMY
large role in any given patient. Reconstruction is tailored to the
Incontinent ileovesicostomy, initially described by McGuire
specific anatomy and related functional deficits. A fundamen-
and colleagues in 1994,31 has primarily been used in the adult
tal difference exists in pediatric lower urinary tract reconstruc-
population with bladder and sphincter dysfunction secondary
tion versus that of adults. In adult reconstruction, a particular
to spinal cord injury and multiple sclerosis. Patients had failed
type of reconstruction (i.e., Kock pouch, Indiana pouch) may
CHAPTER 118
INCONTINENT AND CONTINENT URINARY DIVERSION
1491
be chosen preoperatively. In children, the principles of a low-
The vast majority of augmentations are performed with
pressure reservoir with a means of catheterization without
gastrointestinal segments because bowel segments are readily
leakage or reflux must be achieved from the tissues available
available and easily configured. Ileum is currently the most
at this time of reconstruction. Whenever possible, enhance-
popular segment,41-43 but sigmoid is often used. Stomach
ment of the native bladder and outlet is preferred to avoid
and ileocecal segments have been used but have only a small
the potential complication associated with ureteral anastomo-
role in contemporary management.44-47 Their abundance en-
sis to a CUR. CUR would be performed if the native bladder is
sures that adequate capacity is obtained while detubulariza-
absent or not salvageable. Patients with bladder agenesis syn-
tion and the natural viscoelastic properties allow for the
dromes, the most severe bladder exstrophy, and pelvic organ
low-pressure reservoir.48-49 However, the secretive50-51 and
destruction secondary to trauma or malignancy would be
absorptive52 nature of this tissue is also responsible for most
candidates for CUR.
of the common complications associated with this procedure.
Continent urinary diversion is now common, but one must
Requirements for a successful augmentation include proper
remember that it requires a broad spectrum of surgical skills
patient selection,53
the ability and willingness to perform
and must address the varied underlying diagnoses. By defini-
CIC,50,54
proper selection of augmentation material, and
tion, a reservoir that must be emptied by intermittent catheter-
recognition and treatment of complications.
ization is created. This may include the augmentation of an
intact but severely diseased bladder or the creation of a reser-
voir completely from heterologous tissue. The surgical goals
PATIENT EVALUATION AND SELECTION
and principles are similar: to create the ideal storage reservoir
for urine that can be easily emptied with the minimum of com-
The patient, family, and entire health care team must be in-
plications. Because the gastrointestinal (GI) tract is plentiful
volved in the decision to pursue major surgery. The common
and accessible, it is the most common source of tissue. The
risks of incorporating GI segments into the urinary tract in-
physiologic variability along the GI tract allows the surgeon
clude mucus production, urinary tract infection, bladder
to tailor the reconstruction to the patient. However,
and renal calculi, and metabolic changes. Life-threatening
these complex surgeries are not without complications, and
risks such as malignant degeneration and spontaneous perfo-
these have to be understood and anticipated.
ration must be explained to the family and child, and they
must be understood.50,51,54 Everyone involved in caring for
the child must be committed to the appropriate postoperative
care including mandatory use of CIC and regular bladder
BLADDER AUGMENTATION
irrigation.50,54,55
Bladder augmentation is an essential component of the pedi-
Clinical evaluation requires a thorough history and physi-
atric urologist’s surgical armamentarium. It has a prominent
cal examination. Particular attention should be paid to latex
role in the management of many lower urinary tract (LUT) dis-
allergy because this can be a fatal complication. Preoperative
orders including neurogenic bladder, posterior urethral
evaluation should include a renal-bladder ultrasound (RBUS)
valves, and bladder exstrophy. The modern application often
and a voiding cystourethrogram (VCUG). Serum chemistries
includes the use of a continent catheterizable abdominal wall
are required because impaired renal function may change
stoma based on the Mitrofanoff principle. This is generally
the gastrointestinal segment used.54 Initially, it was suggested
performed using either the appendix (appendicovesicostomy)
that a creatinine clearance of less than 60 mL/minute might be
or reconfigured ileum (Monti) and may require an additional
a contraindication for the use of ileum as a continent urinary
procedure to improve the continence mechanism at the blad-
reservoir,56-57 but augmentation often stabilizes renal func-
der neck. Intermittent emptying via the native urethra remains
tion and reconstruction has been done before renal transplan-
an option.
tation. Urodynamic studies are necessary to determine outlet
As previously discussed, children with severe LUT dys-
resistance, bladder capacity, and storage pressures. Cystos-
function were historically treated with urinary diversion.
copy will confirm anatomy and ensure that no untoward
Lapides’ introduction of clean intermittent catheterization en-
findings that may hinder reconstruction are present.50
sured that any child could safely empty his or her bladder.1,37
The net result of these investigations is a comprehensive
This brought the dawning of lower urinary tract reconstruc-
surgical plan. The exact procedure will depend on which seg-
tion and allowed the urinary tract to remain intact and avoid
ment is to be used and whether the patient requires concom-
the use of external collecting devices. Advances in urodynamic
itant ureteric reimplantation, bladder neck procedure, and a
monitoring improved our ability to predict who would best
catheterizable channel. Patients with a neurogenic bladder
benefit from bladder reconstruction and therefore prevent re-
may also undergo an antegrade continence procedure to assist
nal deterioration.2 Parallel medical advances ensured the sur-
evacuation of their neurogenic bowel.58
vival of these complex patients and allowed for the shift of
Preoperative preparation usually involves bowel prepara-
focus toward continence as an important aspect of their
tion, as described previously for conduit diversion. Perioper-
quality of life.38-39 Recent advances with cutaneous catheter-
ative antibiotics and a sterile urine are required and are
izable channels continue to simplify care and increase its
particularly important if the patient has a ventriculoperitoneal
popularity.40
shunt.59
The primary goal of lower urinary tract reconstruction is to
Long-term follow-up is required with all patients. After the
store urine safely without leakage. Adequate storage requires a
postoperative visit, and assuming the absence of complica-
low-pressure, highly compliant reservoir of adequate volume,
tions, the patient should be seen annually with a history, phys-
whereas continence results from limited contractility and an
ical examination, creatinine and electrolytes, an ultrasound,
effective sphincter mechanism.
and an annual cystoscopy 5 to 10 years out from surgery.50,54
1492
PART VIII
GENITOURINARY DISORDERS
GASTROINTESTINAL CYSTOPLASTY
ILEOCYSTOPLASTY
Most children undergoing lower urinary tract reconstruction
Ileum has become the segment of choice due to its inherently
for hostile bladder dynamics can have their native bladder
low contractility, abundance, and ease of manipulation.41-43
preserved but need to have it augmented to lower intravesical
In children 20 to 30 cm are harvested, with the distal margin
pressures, limit contractility, and improve compliance. Gas-
located 15 to 20 cm from the ileocecal valve to prevent vitamin
trointestinal segments are generally used, but this requires
B12
and bile salt malabsorption.49,64
Ileum is known to
reconfiguration and detubularization to prevent their own
produce less mucus than colon, and we noted a lower rate
inherent contractile properties.44,48,49,60
Maximum storage
of perforation when compared with sigmoid.35 It has the dis-
capacity requires approximation of the spherical shape.48
tinct disadvantage of being difficult to create submucosal
A widely bivalved bladder enables this and helps to prevent
tunnels for ureteral reimplantation or catheterizable channel
the augment behaving as a diverticulum (Fig. 118-5). The
placement.
volume of the sphere is maximized by folding the ileum into
a U or an S shape, which increases the potential radius and
SIGMOID CYSTOPLASTY
volume (Fig. 118-6).54 This reconfiguration, as well as detu-
bularization along the antimesenteric border, is critical to dis-
Advantages of the sigmoid include its proximity to the bladder
rupting intestinal contractions because the intact intestine
and its marked dilation in the neuropathic population. Ap-
can create pressures of 40 to 100 cm H2O.61-63 The recon-
proximately 15 to 20 cm are isolated and irrigated with an an-
structive surgeon should err on the side of a larger rather
tibiotic solution. Due to the extreme contractile nature of the
than smaller augmentation.50 Regardless of the bowel seg-
sigmoid, complete detubularization is essential.46 Spontane-
ment selected, a water-tight anastomosis using absorbable su-
ous perforation rates have been shown to be higher with sig-
ture is done. A suprapubic tube is placed into the native
moid as opposed to ileal augmentations,65 presumably due to
bladder and secured to the abdominal wall, and a perivesical
their increased contractile pressure.66
drain is placed.
ILEOCECAL CYSTOPLASTY
The main advantage of the ileocecal segment is the consistent
blood supply. Two main techniques exist, each with multiple
variations. Either both the ileal and cecal segment are
tabularized and reconfigured together, or solely the cecum
is tubularized and the ileum used to create a continent stoma47
or for ureteric replacement.54 This segment is infrequently
used in the neuropathic population because loss of the ileo-
cecal valve can result in intractable diarrhea.67
GASTROCYSTOPLASTY
The stomach is much less absorptive than other intestinal seg-
ments, and its secretion of hydrogen ions may be beneficial in
patients with chronic renal failure and metabolic acidosis.44,68
A 10- to 15-cm wedge from the greater curvature is mobilized
FIGURE 118-5
The offset cystoplasty allows for more mobility of the
along the right gastroepiploic vessel and passed through the
detrusor muscle and provides better access to the muscular backing that
mesentery of the transverse colon to the bladder. Originally
is essential for implantation of the catheterizable channel.
felt to be an option for all augmentation candidates, its role
is now limited primarily due to the hematuria dysuria
syndrome, which occurs in up to 70% of patients.
Autoaugmentation
------------------------------------------------------------------------------------------------------------------------------------------------
Described by Cartwright and Snow,69 in order to decrease
intravesical pressures and increase bladder capacity, a large
diverticulum is created at the dome of the bladder by a detrusor-
ectomy while leaving the bladder mucosa intact. Unfortunately,
although the initial reports of urodynamic improvements
seemed promising, the results were not as durable as those
patients treated with an enterocystoplasty and seem to do better
in adults than in children.70-72 In general, autoaugmentation
will decrease intravesical pressures. It will not reliably increase
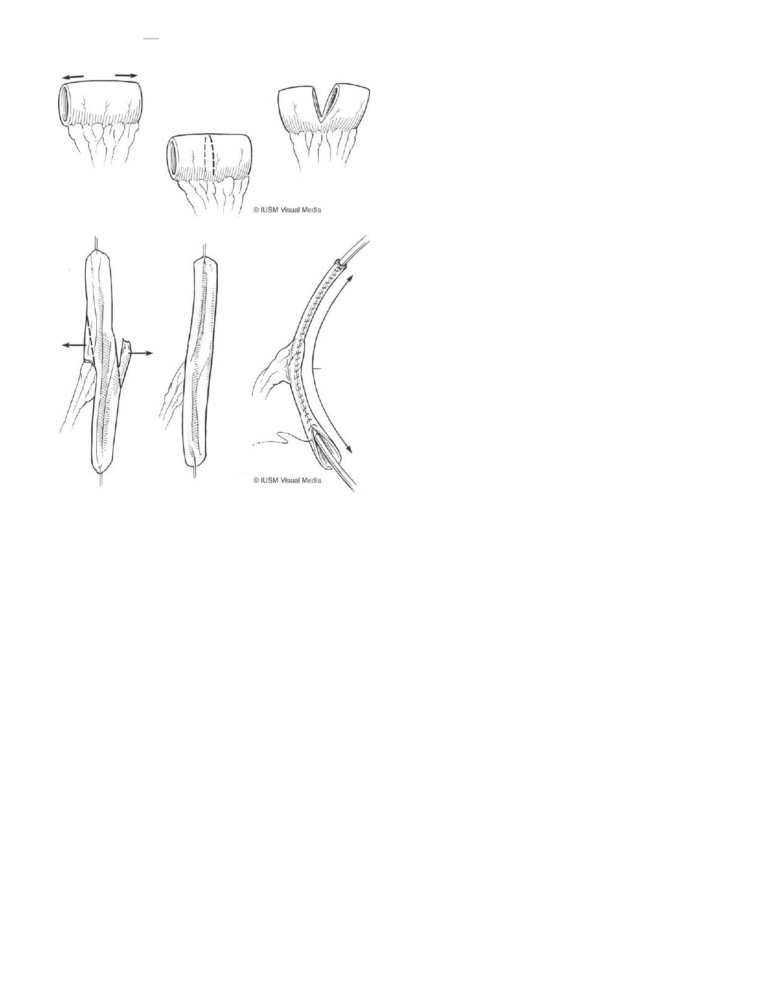
FIGURE 118-6
The ideal bladder augmentation will increase both capac-
ity and compliance, which are required for continence and renal
capacity that is often necessary in children. It does remain an
protection.
option for a select group of patients.
CHAPTER 118
INCONTINENT AND CONTINENT URINARY DIVERSION
1493
SEROMUSCULAR SEGMENTS (WITH
UROTHELIAL LINING)
To avoid the incorporation of intestinal mucosa with the uri-
nary tract, Shoemaker and Marcucci described using seromus-
cular segments of bowel overlying an autoaugmented
bladder.73 Most experiences have demonstrated that whether
the segment is facing the bladder lumen or is reversed, signif-
icant contracture develops.74-75
Most recently, some have
demonstrated success with demucosalized colon over urothe-
lium with findings of increased bladder capacity and low fill-
ing pressures.76 Long-term results and more experience are
necessary to help determine the efficacy of this approach.
CONTINENT CATHETERIZABLE CHANNELS
Bladder augmentation and bladder neck surgery markedly de-
crease the patient’s ability to empty spontaneously while in-
creasing the consequences of incomplete emptying. Not
A
adhering to a strict CIC schedule can result in an increased
risk of urinary tract infection, bladder stones,77 and spontane-
ous bladder perforation.78-79 In 1980 Mitrofanoff introduced
the principle of a continent channel by using the vermiform
appendix and implanting it submucosally into the bladder.80
What is now known as the “Mitrofanoff Principle” states
that any supple tube implanted submucosally with sufficient
muscle backing acts as a flap valve and results in a reliable
continence mechanism (Fig. 118-7).
The Mitrofanoff principle has been widely embraced and ap-
plied to a variety of tissues because the appendix (Fig. 118-8) is
not always appropriate or available, especially if a simultaneous
Malone antegrade continence enema (MACE) procedure is be-
B
ing performed. The use of stomach, colon, bladder, ureters,
and fallopian tubes have all been reported with good suc-
FIGURE 118-8
A, The appendix is readily accessible and mobilized with
maintenance of its vasculature. B, It is implanted easily beneath the blad-
cess.81-92 However, the utility of the tubularized ileal channel
der mucosa to provide a reliable catheterizable channel.
was introduced by Yang87 and Monti82 and has assumed a lead-
ing role in genitourinary reconstruction (Fig. 118-9).84,93
The continent catheterizable channel requires a supple
Monti-Yang technique requires the isolation of 2 cm of ileum,
tube, straight path, and short intra-abdominal segment. The
opening it along its antimesenteric border and retubularizing
appendicovesicostomy requires full mobilization of the right
it over a 12-Fr catheter. The channel is then preferentially
colon to ensure adequate mobility. Amputation should in-
implanted into the submucosa of the bladder because its thick
clude some cecum because this allows for a larger-caliber cu-
muscle is ideal for a continent valve; however, stomach and
taneous stoma or can be tubularized to increase stomal
the tenia coli have been successfully used. Reimplantation into
length.81,94 The appendix is then carefully mobilized with
ileum is the most challenging and requires the creation of a
the mesoappendix to ensure adequate blood supply. The
seromuscular trough. The stoma site can be hidden within
the umbilicus or placed in the right lower quadrant, the latter
being favored as a shorter and more direct route. Great care is
taken to ensure a catheter, usually 12-Fr, passes easily and that
the channel is as straight and tension free as possible. When
satisfied, the surgeon fixes the channel to the abdominal wall
with a permanent suture. Many ingenious skin flap techniques
are used to minimize the chance of stomal stenosis, all insert-
ing into the spatulated channel. An indwelling catheter is
left for 2 to 3 weeks, and the first catheterization is usually
performed in the clinic setting.
Stomal continence is excellent, and rates of 90% to 99% are
reported in the two largest published series.84,95 Complica-
tions pertain primarily to difficulties with catheterization,
most commonly at the skin level, but may also occur deeper
within the channel itself. Stomal stenosis is reported to occur
FIGURE 118-7
The Mitrofanoff principle states that a supple tube will
in 5% to 25%,95-96 with a lower rate potentially seen with
compress with increasing intravesical pressure and provide continence.
tubularized ileum.84
1494
PART VIII
GENITOURINARY DISORDERS
replacement. When required, however, it allows the complex
3.5 cm
patient to achieve continence and enjoy the benefits of such.
Patient selection for the procedure is as important as with
bladder augmentation because noncompliance will result in
the same myriad of complications, despite a technically per-
fect operation. Preoperative evaluation is similar to the blad-
der augmentation patient, with the acquisition of sufficient
clinical, metabolic, anatomic, and functional data to develop
a detailed surgical plan.
The goals of the continent urinary diversion include the
creation of a reservoir of adequate capacity and compliance,
nonrefluxing ureteric implantations, a continent cutaneous
stoma, and a minimum of complications.
Although the gastrointestinal tract again provides for the
reservoir, several key differences exist with an augmentation.
Colon and stomach have assumed a larger role because the
musculature of the tenia coli and stomach allow for more re-
liable nonrefluxing ureteric and catheterizable channel anas-
tomoses. The three most common types of continent
reservoir in children are (1) a reservoir fashioned solely from
ileum (Kock pouch), (2) a gastroileal composite, and (3) an
ileal reservoir (Indiana pouch).95 Each has a myriad of varia-
12-14 cm
tions described, all attempting to decrease complications and
assist construction. However, because published reports in
children are usually limited to small numbers, each reservoir
having subtle variations and no published direct comparisons,
it is impossible to determine an ideal reservoir.55,95,99 There-
fore the reconstructive surgeon must be familiar with several
techniques because each has advantages that may require ex-
ploitation with any clinical situation.
FIGURE 118-9
Normally, a 2-cm segment of ileum can be opened along
its antimesenteric border and tubularized for an effective channel. A
KOCK POUCH
slightly longer piece (3.5 cm) can be partially divided, both ends tubular-
ized, and reanastomosed for a spiral Monti, for situations demanding more
Kock first described a continent ileostomy in 1971100-101 and
channel length.
from this developed the Kock pouch in 1982.102 This continent
ileal reservoir was among the original nonorthotopic
Several authors have described continent catheterizable
bladder substitutions used and remains popular today.103-105
tubes fashioned from native bladder. Casale’s original descrip-
It requires the construction of an efferent nipple for continence
tion of the “intravesical channel”97 was modified by Rink.98
and an afferent limb for the prevention of reflux. This tech-
Although continence rates of
100% were reported, the
nically demanding aspect usually requires the use of stapling
technique is hampered by a 45% incidence of stomal stenosis.
devices, and these can be the source of its most significant
Although still a useful technique if an intraperitoneal pro-
complications (stone formation) and long-term failure rate.106
cedure can be avoided, it has been largely replaced by the
Approximately 80 cm of ileum is harvested in adults, with
appendicovesicostomy and reconfigured ileovesicostomies.
the proximal 15 to 20 cm used in an isoperistaltic fashion to
These channels provide a more convenient and more so-
create the antireflux mechanism. The distal 12 to 15 cm are
cially acceptable means of catheterization. It is especially ben-
used for the continent cutaneous stoma. These lengths are de-
eficial for those with a sensate urethra and in the obese or
creased appropriately depending on the size of the child. The
wheelchair-bound female. It also assists caregiver comfort
bowel is intussuscepted through its full thickness, and this is
and, most importantly, patient independence.
secured by three rows of gastrointestinal staples, although
absorbable mesh has also been described.107 Significant mod-
ifications include removing the distal
6 staples from the
CONTINENT URINARY RESERVOIRS
device,106 stripping the distal mesentery,108 and the use of
If the entire bladder has been replaced by nonurothelial tissue
absorbable staples.109
(usually gastrointestinal) and requires emptying by means
other than the urethra, it is referred to as continent urinary di-
GASTROILEAL POUCH
version. Although popular and with many refinements over the
past several decades, it is not commonly used in pediatrics
The advantages of both gastric and ileal segments can be max-
today because generally the bladder can be incorporated into
imized while offsetting their complications by incorporating
the reconstruction.50
them both into a composite reservoir. The metabolic derange-
A few diagnoses such as bladder agenesis or malignancy
ments complement each other, as the acidic gastric secretion
resulting in cystectomy will require complete bladder
will neutralize the absorptive properties of the colon or
CHAPTER 118
INCONTINENT AND CONTINENT URINARY DIVERSION
1495
ileum.110-112 Furthermore, in patients at high risk for short
STRUCTURAL COMPLICATIONS
gut syndrome, as in cloacal exstrophy, it allows a minimum
of valuable absorptive tissue to be lost.50 However, it is a more
Structural complications include the requirement of a second
complex reconstruction, requiring two anastomoses and lon-
augmentation, spontaneous perforation, and long-term malig-
ger operating time, but is a valuable alternative for select
nancy potential. A secondary augmentation may be required
patients.
in up to 6% of patients,66 and most are due to high intravesical
pressures from persistent bowel contractility.117-118 The hall-
mark clinical signs are incontinence or hydronephrosis with
INDIANA POUCH
screening ultrasound, and this is confirmed with urodynamic
The ileocecal segment has been popularized due to the poten-
studies.
tial continence or antireflux mechanism inherent to the ileo-
A spontaneous perforation can be a fatal complication and
cecal valve. Many surgical techniques have been described,
must not be underestimated. Early urine leaks are likely due to
in the attempt to maximize cutaneous continence, simplify
technical error, but late complications usually originate in the
the surgical procedure, and minimize complications. The In-
bowel, approximately 1 cm from the anastomotic line.50 Pa-
diana group modified the pouch described by Gilchrist and
tients often present later in the course, as their neurologic def-
Merricks with a unique plication method that has retained
icit impedes symptoms. Therefore sepsis and death are
its popularity. An Indiana pouch uses the detubularized ce-
realistic possibilities, and a high index of suspicion must pre-
cum as its reservoir, with ureters implanted in a nonrefluxing
vail. Diagnosis is with a CT cystogram and treatment is usually
manner into the tenia. The ileum is then plicated to the ileo-
by laparotomy and primary closure,78 but conservative treat-
cecal valve, which is reinforced by Lembert sutures (Fig. 118-10).
ment with catheter drainage has been successful in select
Continence has been reported in 95% to 99%,113-114 in part due
patients.119
to its large capacity.115 Complication rates have been acceptable,
The development of an adenocarcinoma is concerning due
as low as 0.6%,113 but not all surgeons have reported such
to the well-documented occurrence following ureterosigmoi-
success.116
dostomy.120-124 It arises from the ureterointestinal junction
and occurs in these patients with a 7000-fold risk over the
general population.123 Although a tumor has been reported
as soon as 3 years after augmentation,125-126 the mean latency
COMPLICATIONS FROM THE
is 21.5 to 26 years.30,123 At our institution, 3 malignancies
INCORPORATION OF INTESTINE
have occurred in our series of more than 500 augmentations.
IN THE URINARY TRACT
All patients died of metastatic disease, with a mean time from
Despite the popularity of using the gastrointestinal tract as a
augmentation to diagnosis of 19 years.127 Husmann and col-
urinary reservoir, the potential complications are numerous
leagues128 have suggested that patients with neurogenic blad-
and can be significant. A broad categorization would include
ders, exstrophy, and other congenital anomalies requiring CIC
(1) complications due to structural defects, (2) complications
are at higher risk for malignancy regardless of whether enter-
secondary to the loss of the intestinal segment, (3) complica-
ocystoplasty is performed. The risk of carcinoma (both adeno-
tions due to secretions, and
(4) complications from
carcinoma and transitional cell) in this patient population is
absorption.
increased with exposure to other carcinogens (e.g., tobacco)
and immunosuppression.129 Although most surgeons appre-
ciate the risk, definitive guidelines for surveillance have not
been established. Annual cystoscopy has been recommended
to begin 3 to 10 years after augmentation.30,50
LOSS OF INTESTINAL SEGMENT
Removal of an intestinal segment places the patient at risk for a
bowel obstruction, and this occurs in approximately 3% of
cases.50,60,65,130 Because many of these are due to internal her-
niation through the pedicle of the augment, Leonard and col-
leagues131 have recommended early exploration to minimize
the risk of augmentation ischemia.
The removal of a gastrointestinal segment for CUR or aug-
mentation is usually well tolerated; however, bowel dysfunc-
tion has been reported in 10% to 54% of patients.132-133
Removal of the ileocecal valve can result in problematic diar-
rhea and rectal incontinence, especially in the neurogenic
population.134-135 Loss of the distal ileum can also result in
diarrhea, in these cases due to an interruption in the entero-
hepatic circulation,136 but can usually be prevented by leaving
the distal 15 to 20 cm intact. Treatment of mild cases is usually
successful with anion-exchange resins.54
FIGURE 118-10
The Indiana pouch uses the ileocecal valve as a conti-
Vitamin B12 deficiency can develop in up to 35% of patients
nence mechanism and the cecum for urinary storage.
following an
80-cm small bowel resection for a Kock