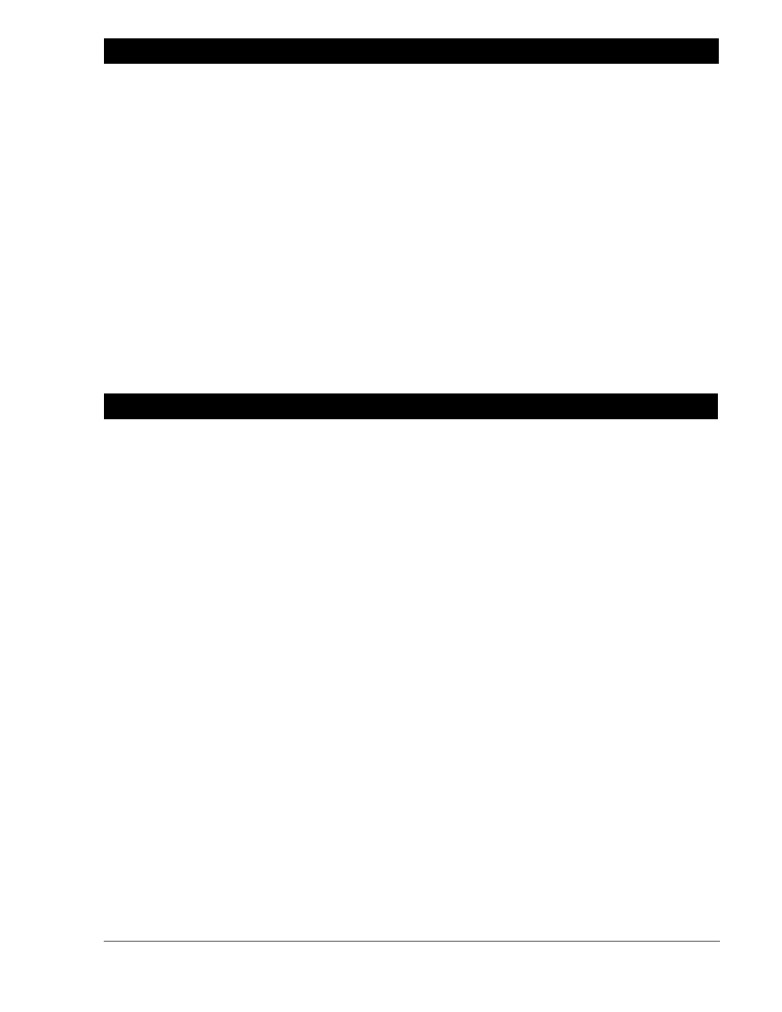OPHTHALMOLOGY
Dr. J.H. Fowler
Philip Dopp and Asif Salyani, chapter editors
Anna Kulidjian, associate editor
COMMON COMPLAINTS
3
CONJUNCTIVA
14
Common Ocular Problems in the Elderly
Pinguecula
Common Ocular Problems in Contact Lens Wearer
Pterygium
Subconjuctival Hemorrhage
THE OCULAR EXAMINATION
5
Conjunctivitis
Vision Assessment
Bacterial Conjunctivitis
Visual Fields
Viral Conjunctivitis
Pupils
Chlamydia Conjunctivitis
Anterior Chamber Depth
Allergic Conjuctivitis
Extraocular Muscles
Giant Papillary Conjunctivitis (GPC)
External Examination
Vernal Conjunctivitis
Slit-Lamp Examination
Tonometry
SCLERA
16
Ophthalmoscopy/Fundoscopy
Episcleritis
Scleritis
OPTICS
7
Scleromalacia Perforans
Emmetropia
Blue Sclerae
Refractive Errors
Staphyloma
Myopia
Hyperopia
CORNEA
17
Astigmatism
Foreign Bodies
Presbyopia
Corneal Abrasion
Anisometropia
Recurrent Erosions
Refraction
Corneal Ulcers
Refractive Eye Surgery
Herpes Simplex Keratitis
Herpes Zoster
THE ORBIT
9
Keratoconus
Exophthalmos (Proptosis)
Arcus Senilis
Enophthalmos
Kayser-Fleischer Rings
Preseptal Cellulitis
Orbital Cellulitis
THE UVEAL TRACT
19
Uveitis
LACRIMAL APPARATUS & LYMPH NODES
. .10
Anterior Uveitis
Lymph Nodes
Posterior Uveitis
Lacrimal Apparatus
Keratoconjunctivitis Sicca (Dry Eyes)
GLOBE
20
Epiphora (Tearing)
Endophthalmitis
Dacryocystitis
Dacryoadenitis
LENS
21
Cataracts
LIDS AND LASHES
12
Dislocated Lens
Lid Swelling
Ptosis
Trichiasis
Entropion
Ectropion
Hordeolum
Chalazion
Blepharitis
Xanthelasma
Lid Carcinoma
MCCQE 2006 Review Notes
Ophthalmology - OP1
. . . CONT.
OPHTHALMOLOGY
RETINA AND VITREOUS
22
OCULAR MANIFESTATIONS OF
32
Vitreous
SYSTEMIC DISEASE
Vitreous Hemorrhage
HIV
Retina
Other Systemic Infections
Central Retinal Artery Occlusion (CRAO)
Diabetes Mellitus (DM)
Branch Retinal Artery Occlusion
Multiple Sclerosis (MS)
Central Retinal Vein Occlusion (CRVO)
Hypertension
Retinal Detachment (RD)
Amaurosis Fugax
Retinitis Pigmentosa
Hyperthyroidism/Graves' Disease
Roth Spots
Connective Tissue Disorder
Age-Related Macular Degeneration (ARMD)
Giant Cell Arteritis
Sarcoidosis
BLURRED OPTIC DISC MARGINS
25
Drusen
STRABISMUS
34
Myelinated Nerve Fibres
Tropia
Phoria
GLAUCOMA
26
Paralytic Strabismus
Primary Open Angle Glaucoma
Non-Paralytic Strabismus
Primary Angle Closure Glaucoma
Secondary Open Angle Glaucoma
PEDIATRIC OPHTHALMOLOGY
36
Secondary Angle Closure Glaucoma
Amblyopia
Normal Pressure Glaucoma
Leukocoria
Congenital Glaucoma
Nasolacrimal System Defects
Ophthalmia Neonatorum
PUPILS
28
Rubella
Pupillary Light Reflex
Dilated Pupil: Differential Diagnosis
OCULAR TRAUMA
37
Constricted Pupil: Differential Diagnosis
Blunt Trauma
Relative Afferent Pupillary Defect (RAPD)
Penetrating Trauma
Chemical Burns
NEURO-OPHTHALMOLOGY
30
Hyphema
Visual Field Defects
Blow Out Fractures
Bitemporal Hemianopsia
Sympathetic Ophthalmia
Homonymous Hemianopsia
Internuclear Ophthalmoplegia (INO)
OCULAR EMERGENCIES
38
Nystagmus
DRUGS WITH OCULAR TOXICITY
39
INTRAOCULAR MALIGNANCIES
31
Topical Ocular Diagnostic Drugs
Malignant Melanoma
Glaucoma Medications
Retinoblastoma
Topcial Ocular Therapeutic Drugs
Metastases
OCULAR DRUG TOXICITY
40
REFERENCES
40
OP2 - Ophthalmology
MCCQE 2006 Review Notes
COMMON COMPLAINTS
Persistent Loss of Vision
gradual (weeks to months)
• refractive error
• cataracts
• diabetes
• macular degeneration
• glaucoma (chronic)
• intracranial compressive lesion
• tumour infiltration
• toxic degeneration
acute (minutes to days)
• vascular/ischemia
• cortical blindness
• central retinal vein/artery occlusion (CRVO/CRAO)
• vitreous hemorrhage
• optic neuropathy
• giant cell (temporal) arteritis
• anterior ischemic optic neuropathy (AION)
• optic neuritis
• multiple sclerosis (MS)
• papillitis or retrobulbar neuritis
• retinal detachment
• acute glaucoma
• acute iritis
Transient Loss of Vision (Amaurosis Fugax)
transient ischemic attack (TIA), microemboli
migrainous spasm of artery
hypertension
Floaters
physiologic; vitreous syneresis
vitreous hemorrhage
retinal detachment
Flashing Lights
vitreous traction
retinal tear/detachment
migraine
Ocular Pain
corneal abrasion, corneal ulcer, foreign body
acute angle closure glaucoma
acute uveitis
scleritis, episcleritis
optic neuritis
differentiate from ocular ache: eye fatigue/asthenopia
Photophobia (Light Sensitivity)
iritis
meningitis, encephalitis
light dispersion by mucus, lens, corneal opacities
retinal degeneration
acute glaucoma
Diplopia (Double Vision)
binocular diplopia: strabismus, CN paresis (III,IV,VI), muscle entrapment
monocular diplopia: dislocated lens, cataract, corneal scar
MCCQE 2006 Review Notes
Ophthalmology - OP3
COMMON COMPLAINTS
. . CONT.
Red Eye
Table 1. Differential Diagnosis of Red Eye
Conjunctivitis
Acute Iritis
Acute Glaucoma
Angle Closure Keratitis
Discharge
Bacteria: pus
No
No
Profuse tearing
Virus: serous
Allergy: mucous
Pain
No
++
++++
+++
(tender globe)
With nausea
With blinking
Photophobia
No
++++
+
++
Vision
Normal
Reduced
Reduced
Varies with
(cloudy
(corneal edema)
site of lesion
aqueous)
Pupil
Normal
Smaller
Fixed
Same or smaller
in mid dilation
Clinical Pearl
All red eyes are not necessarily conjunctivitis.
Table 2. Additional Features of Red Eye
Conjunctivitis
Acute Iritis
Acute Angle Closure Glaucoma
Injection
Palpebral+bulbar
Ciliary flush
Diffuse
(limbal palor)
Intraocular Pressure (IOP)
Normal
Lower
Increased
Ant.chamber
Normal
Cells/flare
Shallow
Cornea
Normal
Keratic
Steamy
precipitates
Other
Preauricular node
Synechiae
Nausea/vomiting
(if viral)
other causes of red eye
• adnexal and lacrimal system
• hordeolum/stye
• chalazion
• blepharitis
• dacryocystitis
• canaliculitis
• dacryoadenitis
• preseptal cellulitis
• orbital cellulitis
• conjunctiva
• subconjunctival hemorrhage
• pterygium, pinguecula
• sclera
• episcleritis
• scleritis
• cornea
• abrasion
• ulcer
• foreign body
• endophthalmitis
OP4 - Ophthalmology
MCCQE 2006 Review Notes
COMMON COMPLAINTS
. . CONT.
COMMON OCULAR PROBLEMS
IN THE ELDERLY
cataracts
age-related macular degeneration (ARMD)
epiphora
• overflow of tears
• due to dry eyes, entropion, ectropion, trichiasis
neoplasia
vascular disease: CRVO, CRAO, giant cell arteritis
dry eyes
ptosis
COMMON OCULAR PROBLEMS
IN CONTACT LENS WEARER
corneal abrasion
superficial punctate keratitis
giant papillary conjunctivitis
sterile infiltrates (immunologic)
infected ulcers ( Pseudomonas, S. aureu)
THE OCULAR EXAMINATION
suprachoroidal space
sinus venosus sclerae
choroid
(canal of schlemm)
sclera
vitreous body
visual part of retina
lens
fovea centralis
aqueous outflow
hyaloid canal
sheath of optic nerve
anterior chamber
cornea
posterior chamber
central artery and vein of retina
iris
suspensory ligament
optic nerve
anterior chamber angle
of lens
lamina cribrosa of sclera
ciliary part of retina
ciliary body and
conjunctiva
ciliary muscle
intervaginal space
ora serrata
bulbar fascia (tendon’s capsule)
tendon of medial rectus muscle
Figure 1. Diagram of the Eye
Drawing by Luke Itani
VISION ASSESSMENT
always note best corrected vision first (e.g. with glasses if possible), especially in emergency room
test both near and distance vision
pinhole test will improve vision with most refractive errors
Visual Acuity (VA) Far
Snellen Fraction = testing distance (usually 6 metres or 20 feet)
smallest line patient can read on the chart
e.g. 20/40 -2 (missed two letters of 20/40 line)
OD = RIGHT EYE, OS = LEFT EYE, OU = BOTH EYES
Heirarchy for low vision - Snellen acuity - count fingers - hand motion - light perception - no light perception
Legal blindness is 20/200 or < 10 degress of visual field in better eye
Minimum visual acuity to operate an automobile is 20/40 in the better eye
Visual Acuity (VA) Near
use pocket vision chart (e.g. Rosenbaum)
record number and testing distance (usually 30 cm)
e.g. J2 @ 30cm
MCCQE 2006 Review Notes
Ophthalmology - OP5
THE OCULAR EXAMINATION . . . CONT.
Visual Acuity for Children,Illiterate Adults or Dysphasics with CVA
Sheridan-Gardiner matching test (most 4 year olds able to do it)
illiterate "E" chart (patient states direction of “E”)
Infant Visual Acuity
6-12 months - 20/120
1-2 years - 20/80
2-4 years - 20/20
VISUAL FIELDS
test visual field quadrants grossly by confrontation
automated field testing (e.g. Humphrey, Goldmann), or Tangent Screen
PUPILS
examine pupils with respect to
• equality, size, shape
• reactivity to light (both direct and consensual)
test for relative afferent pupillary defect (RAPD)
• use "swinging flashlight test" (use ophthalmoscope with “+4” setting especially with dark brown iris)
test pupillary constriction portion of near reflex
• bringing object from far to near results in
• lens accommodation
• eye convergence
• pupil constriction
• must use reduced illumination or pupillary constriction will be produced
ANTERIOR CHAMBER DEPTH
shine light tangentially from temporal side
shallow = > 2/3 of nasal iris in shadow
EXTRAOCULAR MUSCLES
Alignment
examine in primary position of gaze (e.g. straight ahead)
Hirschberg test (shine light into patient's eyes from 30 cm away)
• corneal light reflex should be symmetric and near centre of each cornea
strabismus testing as indicated - see Strabismus section
Movement
examine movement of eyeball through the nine diagnostic positions of gaze
(with six muscles responsible for extra-ocular movement (EOM))
determine if diplopia is present in any position of gaze
observe for nystagmus (horizontal and vertical)
EXTERNAL EXAMINATION
the four L’s
• lymph nodes
• lacrimal apparatus
• lids
• lashes
SLIT-LAMP EXAMINATION
systematically examine all structures of the anterior segment
• lids and lashes, including upper lid eversion if necessary
• conjunctiva and sclera
• cornea
• anterior chamber
• iris
• lens
also examine with
• fluorescein staining: (water-soluble dye stains de-epithelialized cornea green),
with cobalt blue filter
• Rose Bengal dye (stains devitalized corneal epithelium)
can examine structures in the posterior segment with special lenses (78D, 90D)
OP6 - Ophthalmology
MCCQE 2006 Review Notes
THE OCULAR EXAMINATION . . . CONT.
TONOMETRY
measurement of intraocular pressure
normal range is 8-21 mm Hg
commonly measured by
• indentation (Schiotz or Tonopen)
• applanation (Goldmann) - gold standard
• non-contact (air puff)
use topical anesthetic for Schiotz, Goldmann, Tonopen
OPHTHALMOSCOPY/FUNDOSCOPY
examination of the anterior segment
• fluorescein and colbat blue filter and +20 lens
• corneal opacity
• cataract
• the red reflex
examination of the posterior segment of the eye
• vitreous
• optic disc (colour, cup, margins, cup/disc ratio)
• nasal retinal vessels
• retina, macula (temporal)
best with pupillary dilatation (e.g. tropicamide) (see Table 6)
contraindications to dilatation
• narrow anterior chamber angles
• neurologic abnormality requiring pupillary evaluation
• iris supported anterior chamber lens implant (square pupil)
OPTICS
main refractive mechanisms are: cornea (2/3), lens (1/3)
EMMETROPIA
no refractive error
image of distant objects focused on the retina without accommodation
REFRACTIVE ERRORS(see Figure 2 and Figure 3)
distant light is not focused on retina, without accommodation
three types: myopia, hyperopia, and astigmatism
MYOPIA
"nearsightedness"
to remember: LMN (Long eyeball is Myopic, requiring negative/concave lens, and is Nearsighted)
Pathophysiology
globe too long relative to refractive mechanisms or refractive mechanisms too strong
image of distant object falls in front of retina without accommodation --> blurring of distant vision
Presentation
usually presents in 1st or 2nd decade, stabilizes in 2nd and 3rd decade;
rarely begins after 25 years except in diabetes or cataracts
blurring of distance vision
near vision usually unaffected
Complications
retinal degeneration and detachment
chronic open angle glaucoma
complications not prevented with refractive correction
Management
correct with concave negative (-) spectacles or contact lenses, which diverge light rays
refractive eye surgery - see below
HYPEROPIA
"farsightedness"
hyperopia may be developmental, or may be due to any cause which shortens the eyeball
to quantitate hyperopia, cycloplegic drops are used to prevent accommodation
Pathophysiology
globe too short or refractive mechanisms too weak
image of distant object falls behind retina without accommodation
person will accommodate to try to bring image onto retina
MCCQE 2006 Review Notes
Ophthalmology - OP7
OPTICS . . . CONT.
Presentation
youth: usually do not require glasses (still have sufficient accommodative ability to focus image on retina),
+/- accommodative esotropia (see Strabismus section)
30s: blurring of near vision due to decreased accommodation, may need reading glasses
> 50s: blurring of distance vision due to severely decreased accommodation
Complications
angle closure glaucoma, particularly in later life as lens enlarges
Management
when symptomatic, correct with convex positive (+) lenses, which converge light rays
refractive eye surgery - see below
ASTIGMATISM
light rays not refracted uniformly in all meridians
due to non-spherical surface of cornea or non-spherical lens (e.g. football shaped)
regular astigmatism: curvature is uniformly different in meridians at right angles to each other
irregular astigmatism: distorted cornea, due to injury or keratoconus (cone-shaped cornea)
Management
correct with cylindrical lens, toric contact lens, arcuate keratotomy or refractive eye surgery (see below)
PRESBYOPIA
decreased ability of eye to accommodate with aging (decrease in lens elasticity, NOT a refractive error)
experienced by emmetropes as well as patients with refractive errors
normal decline in near vision with age (> 40 years) with distance spectacles in place
Presentation
if initially emmetropic, starts holding things further away to read, but distance vision unaffected
if initially myopic, remove distance glasses to read
if initially hyperopic, symptoms of presbyopia occurs earlier;
the hyperope needs distance glasses in later decades
Management
correct vision with convex positive (+) lens for reading
reading lens will blur distance vision; options are half-glasses or bifocals
ANISOMETROPIA
difference in refractive error between eyes
• second most common cause of amblyopia in children
Emmetropia
Converges
Hyperopia corrected with positive lens
Myopia
Hyperopia
Diverges
Figure 2. Refractive Errors and Emmetropia
Myopia corrected with negative lens
Figure 3. Correction of
Refractory Errors
OP8 - Ophthalmology
MCCQE 2006 Review Notes
OPTICS . . . CONT.
REFRACTION
technique of determining the lenses needed to correct the optical defects of the eye (ametropia)
two techniques used
1) Flash/Streak Retinoscopy
• refractive error determined objectively by use of retinoscope and lenses
2) Manifest (Acceptance)
• subjective trial of lenses used to refine retinoscopy findings
• a typical lens prescription would contain
• sphere power in D (diopters)
• cylinder power in D to correct astigmatism
• axis of cylinder (in degrees)
• add (reading lens) for presbyopes
• e.g. -1.50 + 1.00 x 120 degrees, add +2.00
REFRACTIVE EYE SURGERY
permanently altering the refractive properties of the cornea
used for correction of myopia, hyperopia, and astigmatism
most commonly using excimer laser system
ablation of the corneal surface - photorefractive keratectomy (PRK)
ablation of the stroma below a flap of corneal tissue (LASIK)
THE ORBIT
EXOPHTHALMOS (PROPTOSIS)
eyeball protrusion
Etiology
hyperthyroidism: Graves' disease (unilateral or bilateral, the most common cause in adults)
orbital cellulitis (unilateral, most common cause in children)
primary or secondary orbital tumours
orbital/retrobulbar hemorrhage
cavernous sinus thrombosis or fistula
sinus mucoceles
Diagnosis
exophthalmometer (Hertel): measure at lateral canthi
CT head
ENOPHTHALMOS
retracted globe
often due to "blow-out" fracture (see Ocular Trauma section)
PRESEPTAL CELLULITIS
infection of soft tissue anterior to orbital septum
Etiology
stye, chalazion, acute meibomitis
insect bite
secondary to lid laceration or lacrimal system inflammation
Symptoms and Signs
tender and erythematous lids
may have adenopathy and fever
normal VA, pupil, EOMs
no exophthalmos or RAPD
Management
topical and systemic antibiotics
warm compress
ORBITAL CELLULITIS
inflammation of orbital contents posterior to orbital septum
common in children, but also in the aged and immunocomprimised
Etiology
secondary to sinusitis, facial and/or tooth infections and trauma
MCCQE 2006 Review Notes
Ophthalmology - OP9
THE ORBIT . . . CONT.
Symptoms and Signs
RED FLAG - opthalmoplegia (because of pain on ocular movement)
lids swollen shut, chemosis (conjunctival swelling)
exophthalmos
decreased VA
RAPD due to optic disc edema may occur
adenopathy and fever
Management
admit, IV antibiotics, blood cultures and orbital CT
serious complications exist e.g. cavernous sinus thrombosis, meningitis and blindness
surgical evacuation of abscess if it develops
Table 3. Differences Between Preseptal and Orbital Cellulitis
Finding
Preseptal Cellulitis
Orbital Cellulitis
Fever
Present
Present
Lid edema
Moderate to severe
Severe
Chemosis
Absent or mild
Moderate or marked
Proptosis
Unusual
Present
Pain on eye movement
Absent
Present
Ocular mobility
Normal
Decreased
Vision
Normal
Diminished vision +/- diplopia
RAPD
Absent
May be seen
Leukocytosis
Minimal or moderate
Marked
Adenopathy
Absent
May be seen
ESR
Normal or elevated
Very elevated
Additional findings
Skin infection
Sinusitis; dental abscess
LACRIMAL APPARATUS AND LYMPH NODES
LYMPH NODES
temporal conjunctival lymphatics drain to preauricular and parotid nodes
nasal conjunctival lymphatics drain to submandibular nodes
enlarged nodes significant for infectious etiology, especially viral or chlamydial conjunctivitis
LACRIMAL APPARATUS
tear film made up of three layers
• an outer oily layer, secreted by the meibomian glands
• a middle watery layer, constant secretion from conjunctival glands and
reflex secretion by lacrimal gland with ocular irritation or emotion
• an inner mucous layer, secreted by conjunctival goblet cells
KERATOCONJUNCTIVITIS SICCA (DRY EYES)
Etiology
with aging, tear production normally decreases
lid abnormality (ectropion), decreased blinking e.g. CN VII palsy
systemic diseases: rheumatoid arthritis, Sjögren's syndrome, sarcoidosis, amyloidosis, leukemia, lymphoma
vitamin A deficiency, especially in malnourished areas
post-cataract surgery
medications: anticholinergics, diuretics, antihistamines
Symptoms and Signs
dry eyes, red eyes, blurred vision, overflow tearing
Diagnosis
slit-lamp exam: decreased tear meniscus, decreased tear break up time (BUT),
superficial punctate keratitis (SPK)
revealed by fluorescein staining, rose bengal staining
Schirmer test: measures tear quantity on surface of eye in 5 minute time period
(< 10 mm of strip wetting in 5 minutes is considered a dry eye)
Complications
erosions and scarring of cornea
OP10 - Ophthalmology
MCCQE 2006 Review Notes
LACRIMAL APPARATUS AND LYMPH NODES.. . CONT.
Management
artificial tears and ointments
punctal occlusion
tarsorrhaphy (sew lids together)
treat underlying cause
EPIPHORA (TEARING)
Etiology
emotions
ocular irritation/inflammation (including entropion, trichiasis)
blocked tear outflow (ectropion; punctal, canalicular or nasolacrimal duct (NLD) obstruction)
• aging
• infection (dacryocystitis)
• rhinitis
• in infants: failure of NLD opening
paradoxical lacrimation (crocodile tears)
• excessive tearing while eating
• sequelae to Bell's palsy, due to aberrant regeneration of CN VII
• nerve fibres that formerly went to the salivary glands regrow to the lacrimal gland
Diagnosis
history and observation of lids
fluorescein dye put in eye, examine for punctal reflux by pressing on canaliculi
irrigate through punctum into nose, noting resistance/reflux
Management
lid repair for ectropion/entropion
punctal irrigation
NLD probe (infants)
tube placement: temporary (Crawford) or permanent (Jones)
surgical: dacryocystorhinostomy (DCR) = joining the lacrimal sac to the nasal mucosa,
thus restoring lacrimal drainage
DACRYOCYSTITIS
infection of the lacrimal sac
usually due to obstruction of the nasolacrimal duct
usually very young children (due to failure of NLD opening) or in persons > 40 years old
commonly associated with S. aureus or rarely ß-hemolytic streptococcus infection in acute setting;
S. pneumoniaein chronic infections
Symptoms and Signs (see Colour Atlas OP1)
tearing and discharge
inflammation, pain, swelling over lacrimal sac at inner canthus
pressure on the lacrimal sac may extrude pus through the punctum
in the chronic form, tearing may be the only symptom
Management
warm compresses, nasal decongestants
in newborns - gentle massage over sac, +/- probing
in adults - local or systemic antibiotics +/- irrigation (refer to ophthalmologist)
if chronic, treatment is surgical: dacryocystorhinostomy (DCR)
DACRYOADENITIS
very rare, usually children
inflammation of the lacrimal gland (outer third of upper eyelid)
acute causes: (infectious etiology) mumps, measles, influenza in children, gonorrhea in adults
chronic causes: lymphoma, leukemia, sarcoidosis, tuberculosis
Symptoms and Signs (see Colour Atlas OP9)
pain, swelling, redness of the outer region of the upper eyelid
Management
+/- systemic antibiotics
incision and drainage if required
MCCQE 2006 Review Notes
Ophthalmology - OP11
LIDS AND LASHES
LID SWELLING
Etiology
commonly due to allergy, with shrivelling of skin between episodes
dependent edema on awakening (e.g. CHF, renal or hepatic failure)
orbital venous congestion due to mass or cavernous sinus fistula
dermatochalasis: loose skin due to aging
lid cellulitis, hypothyroidism (e.g. myxedema), trauma (e.g. bruising), chemosis
adenoviral conjunctivitis
PTOSIS
drooping of upper lid > 2 mm below the superior corneal margin
Etiology
congenital: very rare
CN III palsy
• complete: eye is down and out, mydriasis (pupil dilation) (e.g. external compression)
• incomplete: pupil-sparing (e.g. diabetes mellitus)
Horner's syndrome
• ptosis, miosis, anhidrosis
• loss of sympathetic innervation causing Muller muscle paralysis
• see Pupils section for causes
myasthenia gravis (see Neurology Chapter)
• easy fatiguability, with ptosis and diplopia
• diagnose with Tensilon test
myogenic: disinsertion or dehiscence of levator aponeurosis
• most common cause of acquired ptosis in geriatrics
pseudoptosis (e.g. dermatochalasia, enophthalmos, contralateral endocrine exophthalmos)
trauma, infection (e.g. cellulitis)
mechanical
• eyelid prevented from opening completely by mass or scarring
Management
treat underlying cause
diabetic CN III palsy may resolve spontaneously
surgical correction if interferes with vision or for cosmesis
TRICHIASIS
eyelashes turn inward causing corneal irritation +/- ulceration
patient complains of irritation, tearing, mucous discharge
Management
pluck eyelash, electrolysis, surgery to remove eyelash +/- destroy hair follicles
ENTROPION
lid margin turns in towards globe
most commonly affects lower lid
symptoms: tearing, dry eye, cosmetic
may cause abrasions with secondary corneal scarring
Etiology
involutional (aging)
scar contraction (burns, surgery)
orbicularis oculi muscle spasm
congenital
Management
lubricants, evert lid with tape, surgery
ECTROPION
eversion of lower lid
often bilateral
symptoms: dry eye, tearing, cosmetic
may cause exposure keratitis
Etiology
weak orbicularis oculi (aging)
CN VII palsy
scarring (burns, surgery)
mechanical (tumour, herniated fat)
Management
upward massage with ointment or surgery
lubricants
OP12 - Ophthalmology
MCCQE 2006 Review Notes
LIDS AND LASHES . . . CONT.
HORDEOLUM ‘STYE’
infection of the glands of the eyelid, usually with S. aureus
painful, red swelling of lid
internal
• acute infection of meibomian gland (Meibomitis)
• chalazion in chronic stage
external
• stye, pimple
• acute infection of hair follicle or of glands of Zeis or Moll
Management
warm compresses, lid care
topical antibiotics
cellulitis may develop (necessitates systemic antibiotics)
usually resolves in 2-5 days
CHALAZION(see Colour Atlas OP10)
due to chronic sterile granuloma of a meibomian gland (following acute meibomitis),
usually pointing towards the conjunctiva
painless, often subsides
differential diagnosis: basal cell carcinoma, sebaceous cell adenoma, meibomian gland carcinoma
differentiate from hordeolum by absence of acute inflammatory signs
Management
warm compresses
surgical incision and curettage if needed
BLEPHARITIS (see Colour Atlas OP11)
chronic inflammation of lid margins
symptoms: redness of lid margins, scaling and discharge with misdirection or loss of lashes,
burning and/or itching of lids
most common types
• S. aureus
• ulcerative, with dry scales
• seborrheic
• no ulcers, with greasy scales
association with allergy, acne rosacea, seborrheic dermatitis
Complications
recurrent chalazia
conjunctivitis
keratitis
corneal ulceration and neovascularization (late sequelae from trichiasis)
Management (S. aureus )
warm compresses and lid hygiene
cleansing with dilute baby shampoo
topical or systemic antibiotics as needed
XANTHELASMA
lipid deposits in histiocytes in dermis of lids
frequently near inner canthus, may be bilateral
appears as pale, slightly raised yellowish patches or streaks
sometimes associated with increased serum cholesterol
of more concern in young; common in elderly
Management
surgical removal for cosmesis only, recurrences common
LID CARCINOMA
Etiology
basal cell carcinoma (95%)
• spread via local invasion
• rodent ulcer, indurated base with pearly rolled edges
squamous cell carcinoma (5%)
• spread via local invasion, may also spread to nodes and metastasize
• ulceration, keratosis of lesion
sebaceous cell carcinoma (rare)
• can present as non-resolving blepharitis (unilateral)
• highly invasive, metastasize
Management
(see Dermatology/Plastic Surgery Chapter)
surgical excision
irradiation optional for basal cell, sebaceous cell
biopsy to confirm diagnosis
MCCQE 2006 Review Notes
Ophthalmology - OP13
CONJUNCTIVA
a mucous membrane/epithelium
bulbar conjunctiva: covers sclera to the corneal limbus
palpebral conjunctiva: covers inside of lids
PINGUECULA
yellow nodule of hyaline and elastic tissue
commonly deep to conjunctiva adjacent to the limbus
associated with sun and wind exposure
common, benign, usually nasal
Management
does not require treatment, surgical excision rarely indicated
if ulcerated, topical antibiotics may be required
PTERYGIUM(see Colour Atlas OP8)
fleshy triangular encroachment of epithelial tissue onto the cornea (extension of pinguecula)
usually nasal and bilateral
associated with wind, ultraviolet light exposure
Management
surgery if threatens visual axis, causes irritation, or for cosmesis
may recur (10% with conjunctival grafts) and require repeated surgery
may decrease recurrence with conjunctival autograft or mitomycin C (anti-neoplastic) drops
SUBCONJUNCTIVAL HEMORRHAGE
blood beneath the conjunctiva
painless, normal vision
causes: idiopathic, valsalva, trauma, bleeding disorders
if bilateral and recurrent, rule out blood dyscrasias, hypertension, HIV, Kaposi sarcoma
Management
reassurance as it resorbs in 2-3 weeks, discourage rubbing
CONJUNCTIVITIS
Etiology
(see Table 4)
tired or dry eyes
allergy: pollutants, wind dust
infection: bacterial, viral, chlamydial, fungal, rickettsial, parasitic
chemical
irradiation associated with systemic disease
immune reaction e.g. giant papillary conjunctivitis especially in contact lens wearer
secondary to dacryocystitis or canaliculitis
Symptoms and Signs
gritty sensation, purulent discharge, crusts on lids upon awakening
inflamed and injected conjunctiva usually with limbal pallor
follicles (common)
• pale lymphoid elevations of the conjunctiva
• found in viral and chlamydial conjunctivitis
papillae
• vascularized elevations of the palpebral conjunctiva (contain PMNs)
• found in giant papillary conjunctivitis (GPC) and vernal conjunctivitis
(see Colour Atlas OP13)
often has a purulent white-yellow discharge, and less commonly papillae
causes: S. aureus , S. pneumoniae, and H. influenzae
may also be due to N. gonorrhea (in neonates and sexually active people),
Chlamydia is the most common cause in neonates
classification
1.Hyperacute: N. gonorrhea, N. meningitis
2.Acute: H.egyptius, S. pneumoniae
3.Subacute: H. influenzae
Management
topical antibiotics
systemic antibiotics if indicated
course - self-limited - 10-14 days if no treatment, 1-3 days with treatment
OP14 - Ophthalmology
MCCQE 2006 Review Notes
CONJUNCTIVA.. . CONT.
(see Colour Atlas OP14)
watery discharge (mucopurulent common), follicles, subepithelial corneal infiltrates may occur at 10-14 days
associated with cold symptoms, (recent upper respiratory tract infection (URTI) history)
preauricular node often palpable and tender
initially unilateral, often progresses to the other eye
cause: adenovirus
Management
self-limiting - (7 - 10 days or longer)
adenovirus is highly contagious therefore proper hygiene is very important
CHLAMYDIAL CONJUNCTIVITIS
caused by Chlamydia trachomatis
(various serotypes)
affects neonates on day 3-5, sexually active people
causes trachoma, inclusion conjunctivitis, lymphogranuloma venereum (L1, L2, L3)
Trachoma
severe keratoconjunctivitis
leading cause of blindness in the world
papillae and follicles on superior palpebral conjunctiva
conjunctival scarring leads to entropion, causing trichiasis, corneal abrasions +/- ulceration and scarring
keratitis leads to superior vascularization (pannus) and corneal scarring
treatment: systemic tetracycline
Inclusion Conjunctivitis
follicles with occasional keratitis
most common cause of conjunctivitis in newborns
prevention: topical erythromycin at birth
treatment: topical tetracycline and systemic erythromycin
(see Colour Atlas OP15)
intermittent
chemosis/injection with itching and burning
mucous discharge, lid edema, palpebral conjunctival papillae
Management
avoid irritants
cold compresses
topical medications: decongestant/antihistamines (e.g. Albalon-A), mast cell stabilizer (e.g. Opticrom)
combinations (e.g. Patanol), NSAIDs (e.g. Acular), steroids (not used in primary care)
GIANT PAPILLARY CONJUNCTIVITIS (GPC)
immune reaction to mucous debris on lenses in contact lens wearers
large papillae form on superior palpebral conjunctiva
Management
decrease wearing time, clean lenses thoroughly
switch to disposable lenses or hard lenses
topical mast cell stabilizer
if refractory to treatment stop using contacts
VERNAL CONJUNCTIVITIS
allergic condition, seasonal (warm weather)
large papillae on superior palpebral conjunctiva may cause corneal abrasions
occurs in first decade, may last for many years
Management
topical and/or systemic antihistamines
topical NSAIDs, mast cell stabilizer, steroids (not in primary care)
MCCQE 2006 Review Notes
Ophthalmology - OP15
SCLERA
sclera is the white fibrous outer protective coat of the eye
continuous with the cornea anteriorly and the dura of the optic nerve posteriorly
made of avascular collagen, biochemically similar to joint cartilage,
thus rheumatoid conditions may affect sclera and episclera
episclera is a thin layer of vascularized tissue covering the sclera anteriorly
EPISCLERITIS
usually unilateral; simple or nodular
non-specific immune response to irritants
Etiology
mostly idiopathic
associated with rheumatoid arthritis (RA), gout, Sjögren's syndrome, SLE,
herpes zoster, tuberculosis, syphilis or coccidioidomycosis in one third of cases
more frequent in women than men (3:1)
Symptoms and Signs (see Colour Atlas OP16)
localized, elevated, segmental hyperemia, pink/purple-coloured globe
pain, swelling, tenderness, photophobia, lacrimation
topical vasoconstrictor reduces redness
lasts for weeks, typically recurs
Management
generally self limited
chilled artificial tears
topical corticosteroids for 3-5 days if painful (prescribed and monitored by ophthalmologist)
SCLERITIS
uni- or bilateral; sectoral, diffuse, nodular or necrotizing
anterior scleritis: engorgement of vessels deep to conjunctiva
may cause scleral melt, corneal ulceration, secondary glaucoma
posterior scleritis: may cause exudative retinal detachment
usually with episcleral involvement
Etiology
over half are a manifestation of systemic disease
• autoimmune e.g. SLE, RA
• granulomatous e.g. TB, sarcoidosis, syphilis
• metabolic e.g. gout, thyrotoxicosis
• infectious e.g. S. aureus, S. pneumoniae, P. aeurginosa
, HSV, herpes zoster
chemical or physical agents e.g. thermal, alkali or acid burns
idiopathic
Symptoms and Signs (see Colour Atlas OP17)
severe pain and tenderness, more severe than in episcleritis
pain is best indicator of disease progression
conjunctival injection/scleral engorgement
bluish-red hue (in contrast to brighter red of episcleritis)
• topical vasoconstrictors will decrease redness of episcleritis, facilitating examination of scleritis
+/- decrease in visual acuity
Management
topical steroids, not used in primary care (may thin sclera)
systemic NSAIDs or steroids
SCLEROMALACIA PERFORANS
associated with severe rheumatoid arthritis (rare)
thinning of the sclera may lead to uveal dehiscence and globe rupture with minor trauma
prognosis poor, avoid steroids
very gentle examination of eye (Schiotz tonometry contraindicated)
BLUE SCLERAE
rare, uveal pigment seen through thin sclera
associated with: collagen vascular diseases (CVD) (e.g. osteogenesis imperfecta,
Ehlers-Danlos syndrome, Marfan's syndrome), prolonged use of corticosteroids
may occur in normal newborns
STAPHYLOMA
localized ballooning of thinned sclera - anteriorly, equatorially or posteriorly
seen in rheumatoid arthritis, high myopia, glaucoma, trauma
OP16 - Ophthalmology
MCCQE 2006 Review Notes
CORNEA
function
• transmission of light
• refraction of light (2/3 of total refractive power)
• barrier against infection, foreign bodies
transparency due to avascularity, uniform structure and deturgescence
5 layers: epithelium, Bowman's membrane, stroma, Descemet's membrane, endothelium
extensive sensory fibre network (V1 distribution); therefore abrasions and inflammation
(keratitis) are very painful
two most common corneal lesions: abrasions and foreign bodies
FOREIGN BODIES (see Colour Atlas I5)
RED FLAG -foreign body behind lid may cause multiple vertical epithelial abrasion due to blinking
tearing, photophobia, foreign body sensation
detected with fluorescein staining viewed under cobalt blue light of ophthalmoscope or slitlamp
Complications
scarring, infection, rust ring, secondary iritis
Management
remove under magnification using local anesthetic and sterile needle
or refer to ophthalmologist (depending on depth and location)
topical antibiotics
cycloplegia (paralysis of ciliary body = loss of accommodation) if iritis already present
no pressure patch if from contact lens wear
must see the next day and check for secondary iritis and infection
CORNEAL ABRASION
Etiology
trauma (e.g. fingernails, paper, twigs), contact lens
Symptoms and Signs (see Colour Atlas OP2)
pain on blinking, conjunctival injection, tearing, photophobia (after 24-48 hours)
de-epithelialized area stains green with fluorescein dye
pain relieved with topical anesthetic
Complications
infection, ulceration, recurrent erosion, secondary iritis
Management
topical antibiotics
+/- short acting topical cycloplegics (rest iris for comfort - prevents secondary iritis and posterior synechiae)
patch affected eye for comfort only if abrasion is large
NEVER patch abrasion secondary to contact lens wear (prone to Pseudomonas infection)
NEVER give topical analgesics (except to facilitate examination) - impedes epithelial healing
(unless needed to facilitate examination)
systemic analgesics as needed
most abrasions clear within 24-48 hours
bilateral occlusion gives fastest healing
RECURRENT EROSIONS
localized area of superficial corneal edema +/- de-epithelialization where the epithelium fails to
properly adhere to the underlying Bowman's membrane, therefore epithelial cells detach easily
Etiology
previous injury with incomplete healing
corneal dystrophy
spontaneous, idiopathic
Symptoms and Signs
patient usually awakes with pain in morning when poorly adherent epithelium
is dislodged during first eye opening of the day
examination reveals localized epithelial irregularity
Management
as for corneal abrasion
bandage contact lens (to protect corneal epithelium), bed rest
topical hypertonic 2% or 5% sodium chloride solution to dehydrate epithelial edema
anterior stromal needle puncture or YAG laser for chronic recurrence
excimer laser superficial keratectomy
MCCQE 2006 Review Notes
Ophthalmology - OP17
CORNEA . . . CONT.
Table 4. Corneal Abrasion vs. Corneal Ulcer
Abrasion
Ulcer
Time course
Acute (hours)
Subacute (days)
History of trauma
Yes
Yes
Cornea
Clear
White, necrotic
Iris detail
Clear
Obscured
Corneal thickness
Normal
May have crater effect
Extent of lesion
Limited to epithelium
Extension into stroma
CORNEAL ULCERS
Etiology
secondary to corneal abrasions, conjunctivitis, blepharitis, usually bacterial, rarely viral or fungal
contact lens use (50% of ulcers)
marginal ulcers are mostly due to staphylococcal toxins from associated blepharitis
and various autoimmune disorders
central ulcers are most serious because they can perforate or scar
Symptoms and Signs
RED FLAG - pain NOT relieved with topical anesthetic
pain, photophobia, tearing, decreased visual acuity (if central ulcer)
area of thinning with infiltrative base
surrounding corneal edema, conjunctivitis
+/- hypopyon (pus in anterior chamber)
Complications
corneal perforation
infection of globe - endopthalmitis
Management
OCULAR EMERGENCY - refer to Ophthalmology service
culture first
topical antibiotics every hour
must treat vigorously to avoid complications
HERPES SIMPLEX KERATITIS
usually HSV type I
may be triggered by stress, fever, UV light, immunosuppression
Symptoms and Signs (see Colour Atlas OP3)
pain, tearing, foreign body sensation, redness,
may have visual acuity loss
corneal hypoesthesia
occasional cold sore on lip, vesicles on skin
dendritic lesion seen in corneal epithelium with fluorescein staining + cobalt blue illumination
Complications
geographic ulcer (delicate denritic lesions) may often arise
corneal scarring (can lead to loss of vision)
chronic interstitial keratitis due to penetration of virus into stroma
secondary iritis
Management
epithelial debridement
NO STEROIDS initially - may exacerbate condition
antivirals such as topical trifluridine (Viroptic), or oral acyclovir (Zovirax)
ophthalmologist must exercise caution if adding topical steroids for chronic keratitis or iritis
OP18 - Ophthalmology
MCCQE 2006 Review Notes
CORNEA . . . CONT.
HERPES ZOSTER KERATITIS
CN V1 territory
Symptoms and Signs (see Colour Atlas OP18)
neuralgia-type pain (vesicular skin eruption ~ 2 weeks)
ocular tearing, pain and photophobia
corneal hypoesthesia
Hutchinson's sign: if tip of nose involved (nasociliary branch of V1), eye involvement likely (75% chance)
Complications
corneal keratitis, ulceration, perforation and scarring
uveititis
glaucoma secondary to trabeculitis
muscle palsies (rare) due to CNS involvement
occasionally severe post-herpetic neuralgia
Management
oral acyclovir, valcyclovir or famcyclovir +/- cycloplegic agent
topical steroids as indicated for keratitis, iritis (prescribed by an Ophthalmologist)
KERATOCONUS
bilateral central thinning and bulging (ectasia) of the cornea to form a conical shape
associated with Descemet's and Bowman's membrane folds
onset between 1st and 3rd decade
results in irregular astigmatism, corrects poorly with glasses
apical scarring
blurring of visual acuity is the only symptom
Management
contact lens initially if spectacle correction unsatisfactory
penetrating keratoplasty (corneal transplant) 90% successful
post-operative complications: endophthalmitis, graft rejection, graft dehiscence
ARCUS SENILIS
hazy white ring in peripheral cornea, < 2 mm wide, clearly separated from limbus
common, bilateral, benign corneal degeneration due to lipid deposition, part of the aging process
may be associated with hypercholesterolemia if age < 50 years
no associated visual symptoms, no complications
no treatment necessary
KAYSER-FLEISCHER RINGS
rare
pigmented ring 1-3 mm wide, located in the peripheral cornea
due to copper pigment deposition in Descemet's membrane
associated with Wilson's disease (hepatolenticular degeneration)
Management
penicillamine to chelate copper
THE UVEAL TRACT
uveal tract = iris, ciliary body, and choroid
vascularized, pigmented middle layer of the eye
UVEITIS
may involve one or all three parts of the tract
idiopathic or associated with autoimmune, infectious, granulomatous, malignant causes
should be managed by an Ophthalmologist
IRITIS
inflammation of iris
usually unilateral
Etiology
usually idiopathic
connective tissue diseases: juvenile rheumatoid arthritis (JRA), ankylosing spondylitis (AS), Reiter's syndrome,
inflammatory bowel disease (IBD)
infectious: syphilis, Lyme disease, toxoplasmosis, TB, HSV, herpes zoster
other: sarcoidosis, trauma
MCCQE 2006 Review Notes
Ophthalmology - OP19
THE UVEAL TRACT. . . CONT.
Symptoms and Signs (see Colour Atlas OP4)
ocular pain,tenderness of the globe, PHOTOPHOBIA, decreased visual acuity,
brow ache (ciliary muscle spasm)
ciliary flush (perilimbal conjunctival injection), miosis
anterior chamber cells (WBC in anterior chamber due to anterior segment inflammation)
and flare (protein precipitates in anterior chamber secondary to inflammation)
occasionally keratitic precipitates (clumps of cells on corneal endothelium)
iritis typically reduces intraocular pressure though severe iritis may cause an inflammatory glaucoma
Complications
inflammatory glaucoma
posterior synechiae
• iritis leading to iris bombe (posterior iris adheres to anterior lens capsule entrapping aqueous
in posterior chamber) - angle closure glaucoma
• indicated by an irregularly shaped pupil
anterior synechiae (rare): adhesions of iris to cornea --> glaucoma
cataracts
band keratopathy (with chronic iritis)
• superficial corneal calcification keratopathy
macular edema with chronic iritis
Management
dilate pupil to prevent formation of posterior synechiae and to decrease pain from ciliary spasm
topical, subconjunctival, or systemic steroids
systemic analgesia
medical workup may be indicated to determine etiology
POSTERIOR UVEITIS
inflammation of the choroid
Etiology
bacterial: syphilis, tuberculosis
viral: herpes simplex virus, cytomegalovirus in AIDS
fungal: histoplasmosis, candidiasis
parasitic: toxoplasma, toxocara
immunosuppression may predispose to any of the above infections
autoimmune: Behcet's disease
malignancies: metastatic lesions, malignant melanoma
Symptoms and Signs
decreased visual acuity
floaters
frequently there is no conjunctival or scleral injection
vitreous cells and opacities
hypopion formation
Management
retrobulbar, or systemic steroids if indicated (e.g. threat of vision loss)
GLOBE
ENDOPHTHALMITIS
most commonly a postoperative complication of cataract surgery, or due to post-penetrating injury to eye,
but also bloodstream dissemination from elsewhere
Symptoms and Signs (see Colour Atlas OP6)
very painful, red eye with circumlimbal flush
anterior chamber cells, hypopyon
reduced vision, extreme photophobia
Management
OCULAR EMERGENCY: immediate admission to prevent loss of eye
vitreous tap and/or vitrectomy
intravitreal, topical, IV antibiotics
OP20 - Ophthalmology
MCCQE 2006 Review Notes
LENS
consists of an outer capsule surrounding a soft cortex and a firm inner nucleus
CATARACTS
lens opacity
most common cause of reversible blindness
Etiology
increased age is the most common cause
• includes nuclear sclerosis, cuneiform (spoke-like), cortical and posterior subcapsular cataracts
congenital
• presents with leukocoria
• treat promptly to prevent amblyopia
juvenile onset: diabetes mellitus, metabolic abnormalities
(e.g. Wilson's disease, galactosemia, homocystinuria)
medication toxicity
• steroids: posterior subcapsular cataracts
• phenothiazines: anterior subcapsular cataracts
• hypocalcemia: zonular cataracts (rare)
inflammatory: uveitis
radiation, UV light
traumatic: typically leaf-shaped or rosette cataracts, may see subcapsular cataracts
Symptoms and Signs (see Colour Atlas OP7)
gradual, progressive, painless decrease in visual acuity
• “second sight” phenomenon: only in cataracts due to nuclear sclerosis
• cataract increases power of lens causing artificial myopia - patient may read without reading glasses
halos around lights at night, double and triple images
diagnose by slit-lamp exam and by eliciting red reflex with direct ophthalmoscope
if severe enough may not be able to see fundus on ophthalmic exam
Management
surgical extraction of the cataract
phacoemulsification
• more common
• remove cataract nucleus and cortex, leaving the posterior capsule and a
peripheral rim of anterior capsule
• less commonly by extracapsular nuclear expression and leaving the
posterior capsule behind
• leaving an intact posterior capsule confines the vitreous to the posterior
segment, thereby reducing the incidence of retinal detachments and macular edema
• allows for posterior chamber intraocular lens, lowering risk of hyphema,
glaucoma and corneal endothelial damage
• approximately 5-30% get an "after-cataract" (opacification of posterior capsule)
which is treated with YAG laser capsulotomy
intracapsular: (now rarely used)
• remove whole lens with the cataract still in the capsule
• use with anterior chamber intraocular lens, glasses, or contact lenses
post-operative complications: retinal detachment, endophthalmitis, opacified
posterior capsule, corneal edema secondary to endothelial damage, macular edema
Indication for Surgery
absolute indications: trauma, congenital cataracts
relative indications: age related (elective surgery when cataract interferes with daily living)
DISLOCATED LENS ‘ECTOPIA LENTIS’
Etiology
associated with Marfan's Syndrome, Ehlers-Danlos type VI, homocystinuria, syphilis,
lens coloboma (congenital cleft due to failure of ocular adnexa to complete growth)
traumatic
Symptoms and Signs
decreased visual acuity
may get unilateral diplopia
iridodenesis (quivering of iris with movement)
direct ophthalmoscopy may elicit abnormal red reflex
Complications
cataract, glaucoma, uveitis
Management
surgical correction +/- lens replacement
MCCQE 2006 Review Notes
Ophthalmology - OP21
RETINA AND VITREOUS
VITREOUS
clear collagen-containing gel that fills the posterior segment of eye
normally firmly attached to optic disc and pars plana and apposed to the retina
commonly liquefies with age (syneresis)
when syneresis occurs, remaining vitreous gel can collapse on itself and lift
away from retinal surface (posterior vitreous detachment)
posterior vitreous detachment can cause vitreous hemorrhage, retinal tears and retinal detachment
if abnormal vitreoretinal adhesions are present (see Retinal Detachment and Vitreous Hemorrhage sections)
vitreous floaters
• shadow of a mobile vitreous opacity cast upon the retina
• must rule out retinal tears or hemorrhagic diseases
• harmless if no serious pathology
VITREOUS HEMORRHAGE
Etiology
diabetic retinopathy (most common cause)
retinal detachment/tear
retinal vein occlusion
posterior vitreous detachment
trauma
Symptoms and Signs
sudden loss of visual acuity
may be preceded by many floaters and/or flashes of light
ophthalmoscopy: retina not visible due to blood in vitreous
Management
ultrasound to rule out retinal detachment
expectant: in non-urgent cases (e.g. no retinal detachment) blood resorbs in 3-6 months
surgical: vitrectomy, retinal detachment repair
retinal endolaser to possible bleeding sites/vessels
RETINA
sensory component of eye
made up of photoreceptor, nerve cells and pigment epithelial layer
macula: area rich in cones, most sensitive area of retina and is darker
due to lack of retinal vessels and thinning of retina in this region
fovea: centre of macula, responsible for the most acute, fine vision
optic disc: normally reddish-orange, with central yellow cup (normal cup/disc (C:D) ratio is < 0.5),
retinal artery and vein pass through cup
CENTRAL RETINAL ARTERY OCCLUSION (CRAO)
Etiology
emboli from carotid arteries or heart (e.g. arrhythmia, endocarditis, valvular disease)
thrombus
temporal arteritis
Symptoms and Signs (see Colour Atlas OP19)
sudden, painless (except in temporal arteritis), unilateral loss of vision
relative afferent pupillary defect (RAPD)
fundoscopy
• cherry red spot (macula), retinal pallor
• boxcars (segmentation of blood in arteries), narrowed arteries
• non-pulsatile empty veins
• Hollenhorst plaques (small glistening cholesterol emboli, located commonly
at bifurcation of retinal arteries, originating from the carotid arteries or the aortic arch)
Management
OCULAR EMERGENCY: attempt to restore blood flow within 2 hours
if < 2 hours
• massage the globe
• decrease intraocular pressure
• topical ß-blockers
• inhaled oxygen - carbon dioxide mixture
• IV Diamox (carbonic anhydrase inhibitor)
• IV Mannitol (draws fluid from eye)
• anterior chamber paracentesis (carries risk of endophthalmitis)
BRANCH RETINAL ARTERY OCCLUSION (BRAO)
only part of the retina becomes ischemic resulting in loss of a visual field
more likely than a CRAO to be embolic; search for source
management: if < 2 hrs since onset of symptoms, ocular massage to dislodge embolus if VA is affected
OP22 - Ophthalmology
MCCQE 2006 Review Notes
RETINA AND VITREOUS . . . CONT.
CENTRAL RETINAL VEIN OCCLUSION (CRVO)
an uncommon cause of blindness in the elderly
choriocapillaris protects retina from ischemia
Predisposing Factors
hypertension
arteriosclerotic vascular disease
diabetes mellitus
glaucoma
hyperviscosity e.g. polycythemia rubra vera, sickle-cell disease, lymphoma, leukemia, macroglobulinemia
any condition that slows venous blood flow
Symptoms and Signs (see Colour Atlas OP20)
painless, unilateral, gradual or sudden visual loss
relative afferent pupillary defect (RAPD)
retina engorged with blood, "ketchup retina", "blood and thunder"
swollen disc, dilated veins, marked flamed-shaped hemorrhages
cotton wool spots in resolving phase
two fairly distinct groups
• venous stasis/non-ischemic retinopathy
• VA approximately 20/80, no RAPD
• mild hemorrhage, few cotton wool spots
• resolves spontaneously over weeks to months
• may regain normal vision if macula intact
• hemorrhagic/ischemic retinopathy
• usually older patient with deficient arterial supply
• VA approximately 20/200, reduced peripheral vision, RAPD
• more hemorrhages, cotton wool spots, congestion
• poor visual prognosis
Complications
occurs in 33% of cases
degeneration of retinal pigment epithelium
liquefaction of vitreous
neovascularization of retina and especially iris (secondary rubeosis),
which can lead to secondary glaucoma
iritis
Management
retinal laser photocoagulation to reduce neovascularization
RETINAL DETACHMENT (RD)
fluid collects between the neurosensory retina and the underlying retinal pigment epithelium
three types
rhegmatogenous
• most common type of RD
• indicates that the detachment originally started with a hole or tear in the retina
• tears may be caused by posterior vitreous detachment, trauma or iatrogenically
• fluid goes through the hole and lifts the neuroretina off the pigment layer and choroid
• more likely to occur spontaneously in high myopes, or after ocular surgery/trauma
tractional
• found in proliferative retinopathies such as diabetes, CRVO, sickle cell disease,
retinopathy of prematurity (ROP) and ocular trauma
• results from vitreal preretinal traction (due to vitreal, epiretinal or subretinal membrane)
pulling the sensory retina away from the underlying pigment epithelium
exudative
• may be due to choroidal tumour, metastatic tumour, uveitis
• caused by local or systemic conditions that damage the retinal pigment epithelium
which allows passage of the choroidal fluid into the subretinal space
Symptoms and Signs (see Colour Atlas OP24)
sudden onset
flashes of light
• due to mechanical stimulation of the retinal photoreceptors
floaters
• hazy spots in the line of vision which move with eye position, due to drops
of blood in the vitreous (blood vessels torn as the retina tears)
curtain of blackness (late)
• darkness in one field of vision when the retina detaches in that area and function is reduced
decreased vision
• visual acuity dramatically drops if the macula becomes detached
relative afferent pupillary defect (RAPD) may be seen
MCCQE 2006 Review Notes
Ophthalmology - OP23
RETINA AND VITREOUS . . . CONT.
Management
prophylactic: if a symptomatic tear (flashes or floaters) is detected, it can be sealed
off with laser therapy or cryotherapy, thereby preventing progression to detachment
therapeutic
• rhegmatogenous retinal detachment:
• scleral buckling (retinal break is mounted on sclera indented by an explant)
• pneumatic retinopexy (intraocular injection of air or an expandable gas
in order to tamponade the retinal break while the chorioretinal adhesion forms)
• both treatments used in combination with localization of the retinal break and treatment
with diathermy, cryotherapy or laser to create adhesion between the pigment epithelium
and the sensory retina
• intraocular injection of silicone oil in cases of recurrent retinal detachments
• tractional retinal detachment:
• vitreoretinal surgery (may involve vitrectomy, membrane removal,
scleral buckling and injection of intraocular gas)
• exudative
• treatment of underlying cause
complications: loss of vision, vitreous hemorrhage, recurrent retinal detachment
a retinal detachment should be considered an emergency, especially if the macula is still attached
prognosis for visual recovery varies inversely with the amount of time the retina
is detached and whether the macula is attached or not
RETINITIS PIGMENTOSA
hereditary degenerative disease of the retina
degeneration of rod cells and retinal atrophy
areas of peppery/"bone-spicule" pigmentary degeneration scattered through mid- and peripheral retina
symptoms: night blindness, often beginning in adolescence, with expanding ring scotoma
(abnormal blind spot) leading to blindness
no satisfactory treatment
ROTH SPOTS
flame-shaped hemorrhages with central white fibrin thrombosis
seen in
• subacute bacterial endocarditis (SBE)
• leukemia (hemorrhage and extravasation of leukocytes)
• severe anemia
AGE-RELATED MACULAR DEGENERATION (ARMD)
leading cause of blindness in people > 65 years old
10% of people > 65 years old have some degree of ARMD
female > male
Non-Neovascular (Non-Exudative/"Dry") ARMD
most common type of ARMD - 90% of cases
drusen: pale, yellow-white deposits of membranous vesicles and collagen deposited between the
retinal pigment epithelium (RPE) and Bruch’s membrane (area separating inner choroidal vessels from RPE)
• no visual loss unless atrophy of overlying RPE and photoreceptors
RPE atrophy: coalescence of depigmented RPE, clumps of focal hyperpigmentation
Neovascular (Exudative/"Wet") ARMD
10% of ARMD, yet 80% results in severe visual loss
choroidal neovascularization: drusen predispose to breaks in Bruch’s membrane,
subsequent growth and proliferation of choroidal capillaries
• may get serous detachment of overlying RPE and retina, hemorrhage
and lipid precipitates into subretinal space
disciform scarring
• an elevated subretinal mass due to fibrous metaplasia of hemorrhagic retinal detachment
• causes severe central visual loss
Risk Factors
female
increased age
family history
smoking
Symptoms and Signs
variable amount of progressive visual loss
metamorphopsia (distorted vision characterized by straight parallel lines appearing convergent or wavy)
OP24 - Ophthalmology
MCCQE 2006 Review Notes
RETINA AND VITREOUS . . . CONT.
Investigations
Amsler Grid: commonly held at normal reading distance with glasses on, assesses macular function
fluorescein angiography: see neovascularization, leaks
Management
non-neovascular ARMD
• monitor
• low vision aids e.g. magnifiers, closed-circuit television
• query - anti-oxidants
neovascular ARMD
• laser photocoagulation for neovascularization
• 50% of choroidal neovascularization cannot be treated initially
• no definitive treatment for disciform scarring
• focal laser for macular edema
• photodynamic therapy with verteporfin: IV injection of verteporfin followed
by low intensity laser to area of choroidal neovascularization;
Treatment of Age-Related Macular Degeneration with Photodynamic Therapy (TAP)
Study Group indicate that for selected patients with subfoveal lesions in
ARMD with predominantly classic choroidal neovascularization, verteporfin
treatment can reduce the risk of moderate vision loss for at least 1 year;
this therapy cannot stop or reverse vision loss in all patients with ARMD;
investigations are ongoing
BLURRED OPTIC DISC MARGINS
DRUSEN
German, plural for "granules"
"giant drusen": hyaline deposits at disc margin and in disc itself, commonly producing field defects
more common form is deposited in Bruch's membrane
(area separating inner choroidal vessels from retinal pigment epithelium)
seen with increasing age, retinal and choroidal degeneration and as a primary dystrophy
with drusen alone, vision is normal or near normal
MYELINATED NERVE FIBRES
a variant of normal in which the retinal nerve fibres are myelinated anterior to the cribriform plate
appear as white streaks extending from the cup and occasionally in retina remote from disc
Table 5. Differential Diagnosis of Blurred Optic Disc Margins
Papilledema
Optic
Ischemic
Central Retinal
(see Colour Atlas OP11)
Neuritis
Neuropathy
Vein Occlusion (CRVO)
Age
Any
< 50
> 50
> 50
Etiology
Increased intracranial
Idiopathic,
Idiopathic, vascular,
Idiopathic
pressure (ICP)
associated with MS
Giant Cell Arteritis (GCA)
VA
Normal
Reduced
Reduced
Reduced
Other
Bilateral, enlarged
Unilateral, pain on
Altitudinal field loss,
Unilateral, hypertension,
sign or
blind spot,
eye movement,
+/- GCA findings
diabetes, increased
symptom
neurologic findings
RAPD, reduced
(e.g.jaw claudication,
viscosity, arteriosclerotic
(e.g. headache)
color vision,
headache, tender
vascular disease
+/- MS findings
scalp)
Fundoscopic
Swollen disc,
Hyperemic
Pale, swollen
“Blood and thunder”,
findings
hemorrhage,
swollen disc,
disc, flame
swollen disc,
dilated
normal if
hemorrhage
venous engorgement,
retinal veins
retrobulbar
retinal hemmorhage
neuritis
Investigation
CT head
Visual field (VF),
ESR
Fluorescein angiography,
CT (if atypical VF
medial evaluation
or if no improvement
in 6 weeks)
Treatment
Neurosurgy consult,
Steroids
High dose steroids
Panretinal laser
treat underlying
(for GCA)
photocoagulation
cause
steroids
MCCQE 2006 Review Notes
Ophthalmology - OP25
GLAUCOMA
Definition
progressive optic neuropathy involving characteristic structural changes to
optic nerve head with associated visual field changes
commonly associated with high intraocular pressure (IOP)
Background
aqueous is produced by the ciliary body and flows from the posterior chamber to the anterior chamber
through the pupil, and drains into the episcleral veins via the trabecular meshwork and the
canal of Schlemm (see Figure 1)
an isolated increase in IOP is termed ocular hypertension (or glaucoma suspect) and these patients
should be followed because ~10% if 20-30 mmHg; 40% if 30-40 mmHg; most if > 40 mm Hg (or more)
will develop glaucoma
normal, average IOP is 16 +/- 2 mm Hg (diurnal variation, higher in a.m.)
pressures > 21 more likely to be associated with glaucoma
normal C/D (cup/disc) ratio < 0.4
suspect if glaucoma if C/D ratio > 0.6, difference between eyes > 0.2 or cup approaches disc margin
loss of peripheral vision most commonly precedes central loss
sequence of events: gradual pressure rise, followed by increased in C/D ratio, followed by visual field loss
as cup approaches disc margin (usually asymptomatic)
screening tests should include
• medical and family history
• visual acuity testing
• slit lamp exam: to assess anterior chamber depth
• ophthalmoscopy: to assess the disc features
• tonometry by applanation or indentation: to measure the IOP
• Humphrey visual field testing
PRIMARY OPEN ANGLE GLAUCOMA
most common form, > 55% of all glaucoma cases
due to obstruction to aqueous drainage within the trabecular meshwork and its drainage
into the canal of Schlemm
screening is critical for early detection
Risk Factors
elevated intraocular pressure (> 21 mm Hg)
age > 40
higher incidence in blacks
myopes
familial, polygenic (10x increased risk)
diabetes
chronic topical steroid use on eyes in steroid responders
previous ocular trauma
anemia/hemodynamic crisis (ask about blood transfusions in past)
hypertension
Symptoms and Signs (see Colour Atlas OP26)
asymptomatic initially
insidious, painless, gradual rise in IOP due to restriction of aqueous outflow
bilateral, but usually asymmetric
visual field loss
• slow, progressive, irreversible loss of peripheral vision
• arcuate scotoma and nasal step are characteristic
late loss of central vision if untreated
earliest signs are optic disc changes
• increased cupping of disc with a cup/disc ratio > 0.4 (the cup is usually enlarged asymmetrically
(i.e. eye more affected initially) and cup approaches disc margin)
• large vessels become nasally displaced
may have hemorrhage at disc margin
safe to dilate pupil
Management
principles: increase the drainage of aqueous and/or decrease the production of aqueous
medical treatment: see Ocular Medications section
• increases aqueous outflow
• topical cholinergics
• topical adrenergics
• topical prostaglandin agonist
• decreases aqueous outflow
• topical beta-blockers
• topical and oral carbonic anhydrase inhibitor
• topical adrenergics
surgical treatment
• laser: trabeculoplasty, selective destruction of ciliary body
• microsurgery: trabeculectomy, tube shunt placement
visual field testing to monitor course of disease
OP26 - Ophthalmology
MCCQE 2006 Review Notes
GLAUCOMA. . . CONT.
PRIMARY ANGLE CLOSURE GLAUCOMA
12% of all glaucoma cases
peripheral iris bows forward in an already susceptible eye with a shallow
anterior chamber obstructing aqueous access to the trabecular meshwork
Risk Factors
hyperopia: small eye, big lens - large lens crowds the angle
age > 70, female
family history, more common in Asians and Inuit
mature cataracts
shallow anterior chamber
pupil dilation (topical and systemic anticholinergics, stress, darkness)
Symptoms
unilateral, but other eye predisposed
RED FLAG: red, painful eye
decreased visual acuity, vision acutely blurred from corneal edema
halo around lights
nausea and vomiting
abdominal pain
Signs
fixed mid-dilated pupil
corneal edema with conjunctival injection
marked increase in IOP even to palpation (> 40 mm Hg)
shallow anterior chamber, +/- cells in anterior chamber
Complications
irreversible loss of vision if untreated, within hours to days
permanent peripheral anterior synechiae
Management
immediate treatment important to
• preserve vision
• prevent adhesions of peripheral iris to trabecular meshwork (peripheral anterior synechiae)
resulting in permanent closure of angle
medical treatment: see Ocular Medications section
• miotic drops (pilocarpine)
• topical beta-blockers
• systemic carbonic anhydrase inhibitors
• systemic hyperosmotic agents (oral glycerine; IV hypertonic mannitol)
• topical steroids (not in primary care)
surgical treatment (for acute angle closure glaucoma)
• laser iridotomy or surgical iridectomy
SECONDARY OPEN ANGLE GLAUCOMA
increased IOP secondary to ocular/systemic disorders which clog the trabecular meshwork
steroid-induced glaucoma
• due to topical/systemic corticosteroid use
• develop in 25% (higher in extended use) of general population (responders) after 4 weeks (or less)
of QID topical steroid use
• 5% of population are super-responders
traumatic glaucoma
• hyphema-induced increase in IOP
• angle recession glaucoma occurs with blunt, non-penetrating trauma to globe and orbit,
causing tears in trabecular meshwork and ciliary body with secondary scarring
pigmentary dispersion syndrome
• iris pigment clogs trabecular meshwork
• typically seen in younger myopes
pseudoexfoliation syndrome
• abnormal basement membrane-like material clogs trabecular meshwork
• seen mostly in the elderly
neovascular glaucoma
• abnormal blood vessels develop on surface of iris (rubeosis iridis)
• due to retinal ischemia associated with proliferative diabetic retinopathy and CRVO
• treatment with laser therapy to retina, to reduce neovascular stimulus to iris vessels
MCCQE 2006 Review Notes
Ophthalmology - OP27
GLAUCOMA. . . CONT.
SECONDARY ANGLE CLOSURE GLAUCOMA
uveitis
• inflamed iris adheres to lens (posterior synechiae)
NORMAL PRESSURE GLAUCOMA
IOP in normal range but cupping and field loss typical of glaucoma are present
often found in women > 60 but may occur earlier
may see splinter hemorrhages of disc margin
damage to optic nerve may be due to vascular insufficiency
Management
treat any underlying medical condition and lower the IOP still further
CONGENITAL GLAUCOMA
due to inadequate development of the filtering mechanism of the anterior chamber angle
Symptoms and Signs
cloudy cornea, increased IOP
photophobia, tearing
buphthalmos (large eye), blepharospasm
Management
filtration surgery is required soon after birth to prevent blindness
PUPILS
PUPILLARY LIGHT REFLEX(see Figure 4)
light shone directly into eye travels along optic nerve (1) to optic tracts (2) to both sides of midbrain
impulses enter both sides of midbrain via pretectal area (3) and Edinger-Westphal nuclei (4)
nerve impulses then travel down both CNs III (5) to reach the ciliary ganglia (6),
and finally to the iris sphincter muscle, which results in direct and consensual light reflex
1. optic nerve
2. optic tracts
3. pretectal area
4. Edinger-Wesphal nuclei
5. cranial nerve III
6. ciliary ganglia
LGB = lateral geniculate body
1
6
6
5
2
2
4
4
3
3
LGB
LGB
Figure 4. Pathway of direct light reflex from left eye and
consensual light reflex from right eye
Illustration by Aimée Worrell
OP28 - Ophthalmology
MCCQE 2006 Review Notes
PUPILS . . . CONT.
DILATED PUPIL (MYDRIASIS) DIFFERENTIAL DIAGNOSIS
Physiologic Anisocoria (unequal pupil size)
occurs in 20% of population
difference < 1-2 mm, most pronounced in dark
normal light reactivity, may vary from day to day
Sympathetic Stimulation
fight or flight response
drugs: epinephrine, dipivefrin (Propine), phenylephrine
Parasympathetic Understimulation
cycloplegics/mydriatics: atropine, tropicamide, cyclopentolate (parasympatholytic)
CN III palsy
• eye deviated down and out with ptosis present
• etiology includes cerebrovascular accident (CVA), neoplasm, aneurysm, diabetes mellitus (DM)
(may spare pupil)
dilated pupil from medication does not respond to constricting drugs (e.g. pilocarpine), unlike a CN III palsy
Acute Angle Closure Glaucoma
fixed, mid-dilated pupil
Adie's Tonic Pupil
80% unilateral, females > males
pupil reacts poorly to light (both direct and consensual) constricts with accomodation
hyporeflexic (Adie's syndrome)
defect at ciliary ganglion: results in denervation hypersensitivity of constrictor muscle
• 0.125% solution of pilocarpine will constrict tonic pupil
• no effect on normal pupil
pupil eventually gets smaller than the unaffected eye
Trauma
damage to iris sphincter from blunt or penetrating trauma
iris transillumination defects may be apparent using ophthalmoscope or slit lamp
pupil may be dilated (traumatic mydriasis) or irregularly shaped
CONSTRICTED PUPIL (MIOSIS) DIFFERENTIAL DIAGNOSIS
Physiologic Anisocoria (unequal pupil size)
as for Dilated Pupil section above
Senile Miosis
decreased sympathetic stimulation with age
Parasympathetic Stimulation
local or systemic medications
cholinergic agents: pilocarpine, carbachol
cholinesterase inhibitor: phospholine iodide
opiates, barbiturates
Horner's Syndrome
lesion in sympathetic pathway
difference in pupil size greater in dim light, due to decreased innervation of adrenergics to iris dilator muscle
associated with anhidrosis, ptosis of ipsilateral face/neck
application of cocaine to eye does not result in pupil dilation (vs. normal pupil)
causes: brainstem infarct, demyelinating disease, cervical or mediastinal tumour,
aneurysm of carotid or subclavians, goiter, cervical lymphadenopathy, surgical sympathectomy
Iritis
miotic initially
later, may be irregularly shaped pupil due to posterior synechiae
does not react to light in later stages
Argyll Robertson Pupil
pupils irregular and < 3 mm diameter, may have ptosis
does not respond to light stimulation
does respond to accommodation
suggestive of CNS syphilis or other conditions (DM, encephalitis, MS)
MCCQE 2006 Review Notes
Ophthalmology - OP29
PUPILS . . . CONT.
RELATIVE AFFERENT PUPILLARY DEFECT (RAPD)(see Neurology Chapter)
defect in visual afferent pathway anterior to optic chiasm
differential diagnosis: optic nerve compression, optic neuritis, large retinal detachment,
CRAO, CRVO, advanced glaucoma
does not occur with media opacity e.g. corneal edema, cataracts
test: swinging flashlight
• if light is shone in the affected eye, direct and consensual response to light is decreased
• if light is shone in the unaffected eye, direct and consensual response to light is normal
• if the light is moved quickly from the unaffected eye to the affected eye,
"paradoxical" dilation of both pupils occurs
• use ophtalmoscope with “+4” setting, using red reflex especially in patients with dark irides
Clinical Pearl
Even dense cataracts do not produce a relative afferent pupillary defect.
NEURO-OPHTHALMOLOGY
VISUAL FIELD DEFECTS(see Neurology Chapter)
lesions in the visual system have characteristic pattern losses
several tests used: confrontation (screening), tangent screen, Humphrey fields, Goldman perimetry
BITEMPORAL HEMIANOPSIA
a chiasmal lesion
Etiology
In children: craniopharyngioma
In middle aged: pituitary mass
In elderly: meningioma
HOMONYMOUS HEMIANOPSIA
a retrochiasmal lesion
the more congruent, the more posterior the lesion
check all hemiplegic patients for ipsilateral homonymous hemianopsia
e.g. left hemisphere --> right visual field (VF) defect in both eyes
INTERNUCLEAR OPHTHALMOPLEGIA
commonly seen in multiple sclerosis (MS)
lesion of medial longitudinal fasciculus (MLF) (see Figure 5)
delayed movement in ipsilateral adducting eye
monocular nystagmus in contralateral abducting eye
The MLF connects the Pontine Paramedian
Reticular Formation (PPRF) to the nucleus of
CN III contralaterally. When looking left, nerve
impulses originate in the right frontal cortex
Lateral Rectus
Medial Rectus
“Look left”
(not shown) and travel to the left PPRF. The
Muscle
Muscle
impulses then travel to the ipsilateral CN VI
nucleus and to the contralateral CN III nucleus
CN III
via the MLF. In INO, an MLF lesion inhibits
CN VI
transmission from the PPRF to the
PPRF
contralateral medial rectus muscle.
MLF
Figure 5. Pathway for left lateral gaze, in patient with
right internuclear ophthalmoplegia (INO)
NYSTAGMUS(see Otolaryngology Chapter)
definition: rapid, involuntary, small amplitude movements of the eyes that are rhythmic in nature
direction of nystagmus is defined by the rapid eye component of motion
can be categorized by movement type (pendular, jerking, rotatory, coarse) or as normal vs. pathological
Pendular Nystagmus
due to poor macular function or cerebellar lesion
eye oscillates equally about a fixation point
may be present in people who become blind early in life
OP30 - Ophthalmology
MCCQE 2006 Review Notes
NEURO-OPHTHALMOLOGY. . . CONT.
Jerking Nystagmus
due to brainstem, labyrinthine, cerebellar disease
rapid movement in one direction, slow movement in opposite direction
Coarse Nystagmus
due to weakness of ocular muscles or lower motor neuron disease
coarse jerking in the direction of the weakened muscle
Normal Nystagmus
endpoint
• at extremes of gaze, subsides after a few beats
• also seen in patients on anticonvulsant therapy
evoked
• optokinetic: occurs when patient viewing a moving object
• vestibular: labyrinthine stimulation from thermal or rotatory movement
• unlike central lesions, vestibular nystagmus is suppressed by fixation
Abnormal Nystagmus
any nystagmus which occurs in the field of binocular vision persistently
vertical nystagmus
• always abnormal if persistent
• up-beating: usually due to acquired disease or lesion in medulla
• down-beating: usually due to lesion in lower brainstem or upper cervical cord
congenital nystagmus
• pendular, may cause amblyopia from poor fixation
gaze-evoked nystagmus
• in certain fields of gaze
• with a brainstem/cerebellar lesion, acoustic neuroma phenytoin, ethanol, barbiturates,
demyelinating diseases
spasmus nutans
• asymmetrical fine nystagmus of unknown pathogenesis
• in children 4-12 months of age, usually recover by 2 years
• head nodding to offset pathological eye movements
ataxic nystagmus
• one eye has more marked nystagmus than the other
• associated with internuclear ophthalmoplegias
INTRAOCULAR MALIGNANCIES
uncommon site for primary malignancies
eye usually affected secondarily by cancer or cancer treatments
MALIGNANT MELANOMA
most common primary intraocular malignancy
more prevalent in Caucasians
arise from uveal tract
hepatic metastases predominate
Management
choice is dependent on the size of the tumour
radiotherapy, enucleation, limited surgery
RETINOBLASTOMA
incidence: 1/1000; sporadic or genetic transmission
unilateral or bilateral (in 1/3 of cases)
malignant - direct or hematogenous spread
diagnosis
• may be detected by leukocoria (white pupil) in infant
• CT scan: dense radiopaque appearance (contains calcium)
Management
radiotherapy, enucleation(removal of globe from eye socket), or both
METASTASES
most common intraocular malignancy in adults
most common from breast and lung
usually infiltrate the choroid, but may also affect the optic nerve or extraocular muscles
may present with decreased or distorted vision, irregularly shaped pupil, iritis, hyphema
Management
local radiation, chemotherapy
enucleation if blind painful eye
MCCQE 2006 Review Notes
Ophthalmology - OP31
OCULAR MANIFESTATIONS OF SYSTEMIC DISEASE
HIV
up to 75% of patients with AIDS have ocular manifestations
ocular findings include: opportunistic infections, ocular vascular manifestations, neoplasms,
Lids/Conjunctiva
Kaposi's sarcoma
• affects conjunctiva of lid or globe
• numerous vascular skin malignancies
• DDx: subconjunctival hemmorhage (non-clearing), hemangioma
molluscum contagiosum
herpes zoster
Cornea
herpes simplex keratitis
herpes zoster
Retina
HIV retinopathy
• most common ocular manifestation of HIV
• cotton wool spots
• capillary abnormalities
• intraretinal hemorrhage
cytomegalovirus (CMV) retinitis(see Colour Atlas OP25)
• most common ocular opportunistic infection in HIV patients
• most common cause of visual loss in HIV patients, occurring in > 25% of patients
• develops in late stages of HIV when severely immunocompromised (CD4 count <= 50)
• a necrotizing retinitis, with retinal hemorrhage and vasculitis, brushfire or pizza pie appearance
• untreated infection will progress to other eye in 4-6 weeks
• symptoms and signs: scotomas related to macular involvement and retinal detachment,
blurred vision, and floaters
• treat with virostatic agents: gancyclovir IV or intravitreal injection, foscarnet IV
necrotizing retinitis
• from herpes simplex virus, herpes zoster, Pneumocystis carinii , toxoplasmosis
disseminated choroiditis
• Pneumocystis carinii, Mycobacterium avium intracellulare
, Candida
OTHER SYSTEMIC INFECTIONS
most common are herpes zoster and candidiasis
herpes zoster (see Cornea section)
Candida
• fluffy, white-yellow, superficial retinal infiltrate that may eventually result in vitritis
• may see inflammation of the anterior chamber
• treatment: amphotericin B
DIABETES MELLITUS (DM)
most common cause of blindness in young people in North America
blurring of distance vision with rise of blood sugar
consider DM if unexplained retinopathy, cataract, EOM palsy, optic neuropathy,
sudden change in refractive error
loss of vision due to
• progressive microangiopathy, leading to macular edema
• progressive diabetic retinopathy --> neovascularization --> vitreous hemorrhage --> traction
--> retinal detachment
• Rubeosis Iridis (neovascularization of the iris) leading to neovascular glaucoma (poor prognosis)
Retina
background
• altered vascular permeability
• retinal vessel closure
non-proliferative: increased vascular permeability and retinal ischemia
• dot and blot hemorrhages
• microaneurysms
• retinal edema
• hard exudates (lipid deposits)
advanced non-proliferative (or pre-proliferative):
• non-proliferative findings plus
• venous sausaging (in 2 of 4 retinal quadrants)
• intraretinal microvascular anomalies-IRMA (in 1 of 4 retinal quadrants)
• IRMA: dilated, leaky vessels within the retina
• macular edema
• cotton wool spots (nerve fibre layer infarcts)
OP32 - Ophthalmology
MCCQE 2006 Review Notes
OCULAR MANIFESTATIONS OF SYSTEMIC DISEASE
. . CONT.
proliferative (see Colour Atlas OP23)
• 5% of patients with diabetes will reach this stage)
• neovascularization: iris, disc, retina to vitreous
• neovascular glaucoma (secondary to rubeosis iridis)
• vitreous hemorrhage, fibrous scarring, retinal detachment
• increased risk of severe visual loss
Screening Guidelines for Diabetic Retinopathy
Type I DM
• screen for retinopathy beginning annually 5 years after disease onset
• screening not indicated before the onset of puberty
TYPE II DM
• initial examination shortly after diagnosis, then repeat annually
• if initial exam negative, repeat in 4 years, then annual exams
pregnancy
• ocular exam in 1st trimester, close follow-up throughout
• gestational diabetics not at risk for retinopathy
Management
Diabetic Control and Complications Trial (DCCT) (see Endocrinology Chapter)
- tight control of blood sugar decreases frequency and severity of microvascular complications
blood pressure control
focal laser for macular edema
panretinal laser photocoagulation, reduces neovascularization by decreasing retinal metabolic demand
- reduces risk of blindness
vitrectomy for vitreous hemorrhage and retinal detachment
Lens
earlier onset of senile nuclear sclerosis and cortical cataract
may get hyperglycemic cataract, due to sorbitol accumulation (rare)
sudden changes in refraction of lens: changes in blood glucose levels (poor control)
may cause refractive changes by 3-4 diopters
Exrtra Ocular Movement (EOM) Palsy
usually secondary to CN III infarct
pupil usually spared in diabetic CN III palsy, but get ptosis
may involve CN IV and VI
usually recover within one year
Optic Neuropathy
visual acuity loss due to infarction of optic disc/nerve
MULTIPLE SCLEROSIS (see Neurology Chapter)
relapsing or progressive CNS disease characterized by disseminated patches of
demyelination in the brain and spinal cord resulting in varied symptoms and signs
many ocular manifestations
Symptoms
blurred vision secondary to optic neuritis
decreased colour vision secondary to optic neuritis
central scotoma, since papillomacular bundle of retinal nerve fibres tends to be affected
diplopia secondary to internuclear ophthalmoplegia (see Figure 5)
Signs
RAPD, ptosis, nystagmus, uveitis
optic atrophy (see Colour Atlas OP22)
, optic neuritis
internuclear ophthalmoplegia (INO)
Management
with optic neuritis, treatment with oral steroids leads to greater likelihood of getting MS
later on than treatment with IV steroids
HYPERTENSION
Keith-Wagener Grading
I: arteriosclerosis (slight narrowing of arterioles)
II: AV nicking, copper wire arterioles, cotton wool spots, hard exudates
III: flame hemorrhages (superficial), retinal edema, macular star
IV: papilledema (choked disc) (see Colour Atlas OP21)
AMAUROSIS FUGAX
sudden, transient blindness from intermittent vascular compromise
typically monocular, lasting < 5-10 minutes
may be associated with paresthesia/weakness in contralateral limbs
Hollenhorst plaques (glistening microemboli seen at branch points of retinal arterioles)
MCCQE 2006 Review Notes
Ophthalmology - OP33
OCULAR MANIFESTATIONS OF SYSTEMIC DISEASE
. . CONT.
HYPERTHYROIDISM/GRAVES' DISEASE
mnemonic - NO SPECS
Grade 0: No signs or symptoms
Grade 1: Only signs are proptosis < 22 mm (measure by Hertel
exolphthalmometer) +/- lid lag; +/- lid retraction
Grade 2: Soft tissue involvement - conjunctival + lid miosis
Grade 3: P roptosis > 22 mm
Grade 4: Extraocular muscle involvement
Grade 5: Corneal involvement - exposure keratitis
Grade 6: Sight loss due to optic neuropathy from compression
ocular changes are often permanent
Management
treat the hyperthyroidism
proptosis can cause exposure of the cornea
• mild stage: use artificial tears
• more severe: steroids, surgery (lateral tarsorrhaphy, orbital decompression), radiation
CONNECTIVE TISSUE DISORDERS
most common ocular manifestation: dry eyes (keratoconjunctivitis sicca)
RA, JRA, SLE, Sjogren's syndrome
ankylosing spondylitis, polyarteritis nodosa (PAN), giant cell arteritis
GIANT CELL (TEMPORAL) ARTERITIS
abrupt monocular loss of vision
ischemic optic atrophy
- 50% lose vision in other eye if untreated
see Blurred Disc Margin section
SARCOIDOSIS
granulomatous uveitis with large "mutton fat" keratitic precipitates and posterior synechiae
neurosarcoidosis: optic neuropathy, oculomotor abnormalities, visual field loss
Management
steroids and mydriatics
STRABISMUS
non-alignment of eyes, found in 3% of children
object not visualized simultaneously by fovea of each eye
complications: amblyopia, cosmetic
TROPIA
a manifest (apparent) deviation
deviation not corrected by the fusion mechanism
Types
exo- (lateral deviation), eso- (medial deviation)
hyper- (upward deviation), hypo- (downward deviation)
esotropia = "crossed-eyes"; exotropia = "wall-eyed"
pseudoesotropia: epicanthal folds give appearance of esotropia but Hirschberg test is normal,
more common in Asians
Tests
Hirschberg: positive if the light reflex in the cornea of the two eyes is asymmetrical
• light reflex lateral to central cornea indicates esodeviation; medial to central cornea
indicates exodeviation
cover test (see Figure 6)
• ask patient to fixate on target
• cover the non-deviated eye, the deviated eye will then move to fixate on the target
• the covered eye will move in the same direction under the cover
• if deviated eye moves inward on covering the fixating other eye = exotropia
• if deviated eye moves outward on covering the fixating other eye = esotropia
the deviation can be quantified using prisms
PHORIA
a latent deviation
a deviation corrected in the binocular state by the fusion mechanism
(therefore deviation not seen when patient is using both eyes)
the Hirschberg test will be normal (light reflexes symmetrical)
very common - majority are asymptomatic
may be associated with asthenopia (eye strain)
OP34 - Ophthalmology
MCCQE 2006 Review Notes
STRABISMUS . . . CONT.
Tests
cover-uncover test (see Figure 6)
• placing a cover over an eye with a phoria causes a breakdown of fixation of that eye,
which allows it to move to a misaligned position
• then, uncovering the covered eye will allow it to return to a normal central position
• covered eye moves inward on removing cover = exophoria
• covered eye moves outward on removing cover = esophoria
alternating cover test
• alternating the cover back and forth from eye to eye detects both tropia and phoria
• maintain cover over one eye for 2-3 seconds before rapidly shifting to other eye
ET
COVER TEST
XT
TROPIA
COVER TEST
E
COVER-UNCOVER
TEST
X
PHORIA
COVER-UNCOVER
TEST
ET = ESOTROPIA
XT = EXOTROPIA
E = ESOPHORIA
X = EXOPHORIA
Figure 6. Cover and Cover-Uncover Tests for Detection of Tropias and Phorias
PARALYTIC STRABISMUS
non-comitant strabismus
deviation varies in different positions of gaze
Etiology
neural: arteriosclerotic (CVA), DM, MS, brain tumour
muscular: myasthenia gravis, Grave's disease
structural: orbital fracture due to trauma
Features
mostly in adults, acquired
diplopia (since adults do not get amblyopia)
greatest deviation in field of action of the weakened muscle
vision is usually unaffected in either eye, unless CN II is involved
NON-PARALYTIC STRABISMUS
comitant strabismus
deviation equal in all directions of gaze
Features
usually begins in infancy
no diplopia (child suppresses the image from the misaligned eye)
deviated eyes may become amblyopic (see Amblyopia section) if not treated when the child is young
i.e. 3-4 years old
amblyopia treatment rarely successful after age 8
amblyopia will not develop if child has alternating strabismus or intermittency -
allow neural pathways for both eyes to develop
Clinical Pearl
All children with strabismus should be promptly referred to Ophthalmology.
All children with defective vision should be promptly referred to detect and
treat non-strabismic amblyopia (e.g. from anisometropia: difference in
refraction between two eyes).
Accommodative Esotropia
normal response to approaching object is near reflex: convergence, accommodation, and miosis
hyperopes must constantly accommodate - excessive accommodation can lead to esotropia
usually reversible with correction of refractive error
Nonaccommodative Esotropia
accounts for 50% of childhood strabismus
most are idiopathic
may be due to ocular pathology (e.g. anisoemetropia, cataract, retinoblastoma)
MCCQE 2006 Review Notes
Ophthalmology - OP35
PEDIATRIC OPHTHALMOLOGY
AMBLYOPIA
Definition
decrease in visual acuity due to inappropriate visual stimulation during development
not due to ocular pathology and not correctable by refraction
note: pathology in visual cortex and lateral geniculate body
Detection
"Holler Test": younger child upset if good eye covered
quantitative visual acuity by age 3-4 years using picture charts and/or matching game (Sheridan-Gardiner),
testing each eye separately
not commonly treatable after age 8-9 years since the neural pathways for vision are now formed
prognosis: 90% will have good vision restored and maintained if treated < 4 years old
Etiology and Management
strabismus
• correct with glasses for accommodative esotropia (50% of children experience relief
of their esotropia with glasses and will not require surgery)
• surgery: recession (weakening) = moving muscle insertion further back on the globe;
or resection (strengthening) = shortening the muscle
• botulinum toxin for single muscle weakening
• cycloplegics or miotics (not commonly used)
• even after ocular alignment is restored (glasses, surgery, botulinum toxin),
patching is frequently necessary until approximately age 8
refractive errors
• anisometropia (amblyopia usually in the more hyperopic eye)
• causes the less hyperopic eye to receive a clear image while the more hyperopic eye receives
a blurred image so that its optic pathway does not develop normally
• astigmatism
• treat with glasses to correct refractive errors
• patching is required if amblyopia persists > 4-8 weeks
other
• occlusion due to ptosis, cataract, retinoblastoma, corneal opacity
• occlusion amblyopia: prolonged patching of good eye may cause it to become amblyopic
General Treatment
correct the cause
patching of good eye (duration is individually determined)
monitor vision until age 8-9 years
LEUKOCORIA
white pupil (red reflex is absent)
Differential Diagnosis
retinoblastoma, retinal coloboma
retinopathy of prematurity (ROP) (retrolental fibroplasia):
associated with supplemental oxygen use in premature infants
persistent hyperplastic primary vitreous (PHPV)
total retinal detachment
congenital cataract
corneal scar
NASOLACRIMAL SYSTEM DEFECTS
delay in duct formation for a few weeks after birth may be normal
increased tearing, crusting and discharge (sometimes mucopurulent)
treatment: massage over lacrimal sac
usually resolve within 8 months
consider referral for lacrimal probing if persistent at 9-12 months
OPHTHALMIA NEONATORUM
newborn conjunctivitis
Chlamydia is most common cause
other causes include: chemical (i.e. silver nitrate), bacterial (N. gonorrhea, S. aureus, Pseudomonas
), HSV
gonococcal infection is the most serious threat to sight
topical prophylaxis most commonly with erythromycin is required by law, less commonly with
silver nitrate or providone-iodine
RUBELLA
infection in the mother in first trimester
the infant may suffer from any or all of the following:
congenital cataract, heart disease, deafness, microcephaly, microphthalmos, mental deficiency
OP36 - Ophthalmology
MCCQE 2006 Review Notes
OCULAR TRAUMA
Clinical Pearl
Always test visual acuity (VA) first! - medicolegal protection.
BLUNT TRAUMA
e.g. fist, squash ball
history: injury, ocular history, drug allergy, tetanus status
exam: VA first, pupil size and reaction, EOM (diplopia), external and slit lamp exam, ophthalmoscopy
if VA normal or slightly reduced, globe less likely to be perforated
if VA reduced, may be perforated globe, corneal abrasion, lens dislocation, retinal tear
bone fractures
• blow out fracture: restricted upgaze, diplopia
• ethmoid fracture: subcutaneous emphysema of lid
lids (swelling, laceration, emphysema)
conjunctiva (subconjunctival hemorrhage)
cornea (abrasions - detect with fluorescein and cobalt blue)
anterior chamber (assess depth, hyphema, hypopyon)
iris (prolapse, iritis)
lens (cataract, dislocation)
refer if you observe any of these signs of ocular trauma: decreased VA, shallow anterior chamber, hyphema,
abnormal pupil, ocular misalignment or retinal damage
PENETRATING TRAUMA
include ruptured globe +/- prolapsed iris, intraocular foreign body
be suspicious if history of "metal striking metal"
initial management: refer immediately
• ABCs
• don't press on eyeball!
• check vision, diplopia
• apply rigid eye shield to minimize further trauma
• keep head elevated 30-45 degrees to keep IOP down
CHEMICAL BURNS
alkali burns have a worse prognosis vs. acid burns because acids coagulate tissue
and inhibit further corneal penetration
poor prognosis if cornea opaque, likely irreversible stromal damage
even with a clear cornea initially, alkali burns can progress for weeks (thus, very guarded prognosis)
Management
IRRIGATE at site of accident immediately, with water or buffered solution
• IV drip for at least 20-30 minutes with eyelids retracted in emergency department
do not attempt to neutralize because the heat produced by the reaction will damage the cornea
cycloplegic drops to decrease iris spasm (pain) and prevent secondary glaucoma
(due to posterior synechiae formation)
topical antibiotics and patching
topical steroids (not in primary care) to decrease inflammation, use for less than two weeks
(in the case of a persistent epithelial defect)
HYPHEMA
bleed into anterior chamber, often due to damage to root of the iris
may occur with blunt trauma
Management
refer to Ophthalmology
• patch, shield and bedrest x 5 days
may need surgical drainage if hyphema persists or if re-bleed occurs
Complications
risk of rebleed highest on days 2-5, resulting in secondary glaucoma, corneal staining, and iris necrosis
never prescribe aspirin as it will increase the risk of a rebleed
MCCQE 2006 Review Notes
Ophthalmology - OP37
OCULAR TRAUMA. . . CONT.
BLOW OUT FRACTURES(see Plastic Surgery Chapter)
blunt trauma causing fracture of orbital floor and orbital contents to herniate into maxillary sinus
orbital rim remains intact
inferior rectus and/or inferior oblique muscles may be incarcerated at fracture site
infraorbital nerve may be damaged
Symptoms and Signs
pain and nausea at time of injury
diplopia, restriction of upgaze
infraorbital and upper lip paresthesia (CN V2)
enophthalmos, periorbital ecchymoses
Diagnosis
plain films: Waters view and lateral
CT: anteroposterior and coronal view of orbits
Management
refrain from coughing, blowing nose
systemic antibiotics may be indicated
surgery if fracture > 50% orbital floor, diplopia not improving, or enophthalmos > 2 mm
may delay surgery if the diplopia improves
SYMPATHETIC OPHTHALMIA
severe bilateral granulomatous uveitis
occurs after ocular trauma (usually penetrating and involving uveal tissue) or eye surgery,
10 days to years later
possibly due to a hypersensitivity reaction to uveal pigment
the injured eye becomes inflamed first and the other eye (sympathizing) second
Symptoms and Signs
photophobia
blurred vision
red eye
Management
if vision not salvageable in affected eye, enucleate to prevent sympathizing reaction
if inflammation in sympathizing eye is advanced, treat with local steroids and atropine --> cyclosporin
OCULAR EMERGENCIES
these require urgent consultation to an ophthalmologist for management
trauma, especially intraocular foreign bodies, lacerations
corneal ulcer
gonococcal conjunctivitis
orbital cellulitis
chemical burns
acute iritis
acute angle closure glaucoma
central retinal artery occlusion (CRAO)
retinal detachment
endophthalmitis
giant cell arteritis
OP38 - Ophthalmology
MCCQE 2006 Review Notes
OCULAR MEDICATIONS
TOPICAL OCULAR DIAGNOSTIC DRUGS
Fluorescein Dye
water soluble orange-yellow dye
green under cobalt blue light - ophthalmoscope or slit lamp
stains damaged corneal and conjunctival and mucus epithelium and contact lenses
Anesthetics
e.g. proparacaine HCl 0.5%, tetracaine 0.5%
indications: removal of foreign body and sutures, tonometry, examination of painful cornea
toxic to corneal epithelium and can lead to corneal ulceration and scarring with prolonged use,
therefore NEVER prescribe
Mydriatics
dilate pupils
cycloplegic
indications: refraction, ophthalmoscopy, therapy for iritis
cholinergic blocking
• paralyze iris sphincter i.e. dilation and cycloplegia
Table 6. Mydriatic Drugs and Duration of Action
Drugs
Duration of action
Tropicamide 0.5%, 1%
4-5 hours
Cyclopentolate HCL 0.5%, 1%
3-6 hours
Homatropine HBr 1%, 2%
3-7 days
Atropine sulfate 0.5%, 1%
1-2 weeks
Scopolamine HBr 0.25%, 5%
1-2 weeks
adrenergic stimulating
• stimulate pupillary dilator muscles, no effect on accommodation
• e.g. phenylephrine HCl 2.5% (duration: 30-40 minutes)
• usually used with tropicamide for additive effects
• side effects: hypertension, tachycardia, arrhythmias
GLAUCOMA MEDICATIONS
Beta-Adrenergic Blockers
decrease aqueous humour formation
nonselective beta-blockers (e.g. Timolol, Levobunolol, Metapranolol)
systemic side effects: bronchospasm, bradycardia, heart block, hypotension,
impotence, depression, exacerbation of congestive heart failure
Cholinergic Stimulating
increases aqueous outflow
e.g. pilocarpine, carbachol
side effects: miosis, decreased night vision, headache, increased GI motility, decreased heart rate
Adrenergic Stimulating
decrease aqueous production and increase flow
e.g. epinephrine HCl, dipivifrin (Propine), brimonidine (Alphagan)
side effects: contact allergy, hypotension in children
Carbonic Anhydrase Inhibitor
decrease aqueous production
e.g. oral acetazolamide (Diamox), topical dorzolamide
side effects: renal calculi, nausea, vomiting, diarrhea, weight loss, aplastic anemia,
bone marrow suppression, systemic acidosis
side effects generally absent with topical preparations
Prostaglandin Agonists
improves uveoscleral outflow
e.g. latanoprost (Xalatan)
side effects: iris colour change, lash growth, trichiasis
TOPICAL OCULAR THERAPEUTIC DRUGS
Decongestants
weak adrenergic stimulating drugs (vasoconstrictor)
e.g. naphazoline HCl 0.012%, phenylephrine HCl 0.12%, tetrahydrazaline 0.05%
rebound vasodilation with over use can exacerbate angle closure glaucoma
MCCQE 2006 Review Notes
Ophthalmology - OP39
OCULAR MEDICATIONS. . . CONT.
Corticosteroids
never prescribed by primary care physician unless emergency indications
complications
• potentiates herpes simplex keratitis and fungal keratitis as well as masking symptoms (within days)
• posterior subcapsular cataract (within months)
• increased IOP, more rapidly in steroid responders (within weeks)
Antibiotics
indications: bacterial conjuntivitis, keratitis, or blepharitis
commonly as topical drops or ointments, may give systemically
e.g. sulfonamide (sodium sulfacetamide, sulfisoxazole), gentamicin, erythromycin, tetracycline,
bacitracin, polymyxin
OCULAR DRUG TOXICITY
Table 7. Drugs with Ocular Toxicity
Amiodarone
Corneal microdeposits and superficial keratopathy
Chloroquine
Bull’s eye lesion at macula
Secondary keratopathy
Chlorpromazine
Anterior subcapsular cataract
Contraceptive Pills
Decreased tolerance to contact lenses
Migraine
Optic neuritis
Central vein occlusion
Digitalis
Yellow vision
Blurred vision
Ethambutol
Optic neuropathy
Haloperidol (Haldol)
Oculogyric crises
Blurred vision
Indomethacin
Superficial keratopathy
Isoniazid
Optic neuropathy
Nalidixic Acid
Papilloedema
Steroids
Posterior subcapsular cataracts
Glaucoma
Papilloedema (systemic steroids)
Increased severity of HSV infections (geographic ulcers)
Predisposition to fungal infections
Tetracycline
Papilloedema
Thioridazine
Pigmentary degeneration of retina
Vitamin A Intoxication
Papilloedema
Vitamin D Intoxication
Band keratopathy
REFERENCES
Coakes R, and Holmes Sellors P. Outline of Ophthalmology . 2nd Edition . 1995. Butterworth-Heinemann Ltd.: Oxford.
Stein R, Stein H, and Slat B. M anagement of Ocular Emergencies . 2nd Edition. 1994. An Allergen Handbook.
Vaugha D, Asbury T, and Piordan-Eva P. General Ophthalmology . 15th Edition . 1999. Prentice Hall Canada: Toronto.
OP40 - Ophthalmology
MCCQE 2006 Review Notes