1516
PART VIII
GENITOURINARY DISORDERS
Mesonephric
duct
Allantois
Primitive
Bladder
urogenital
Phallus
sinus
Mesonephric
Perineal
Cloacal
duct
body
membrane
Ureteric bud
Urorectal
Hindgut
Anorectal
Urorectal
septum
Ureter
A
septum
B
canal
C
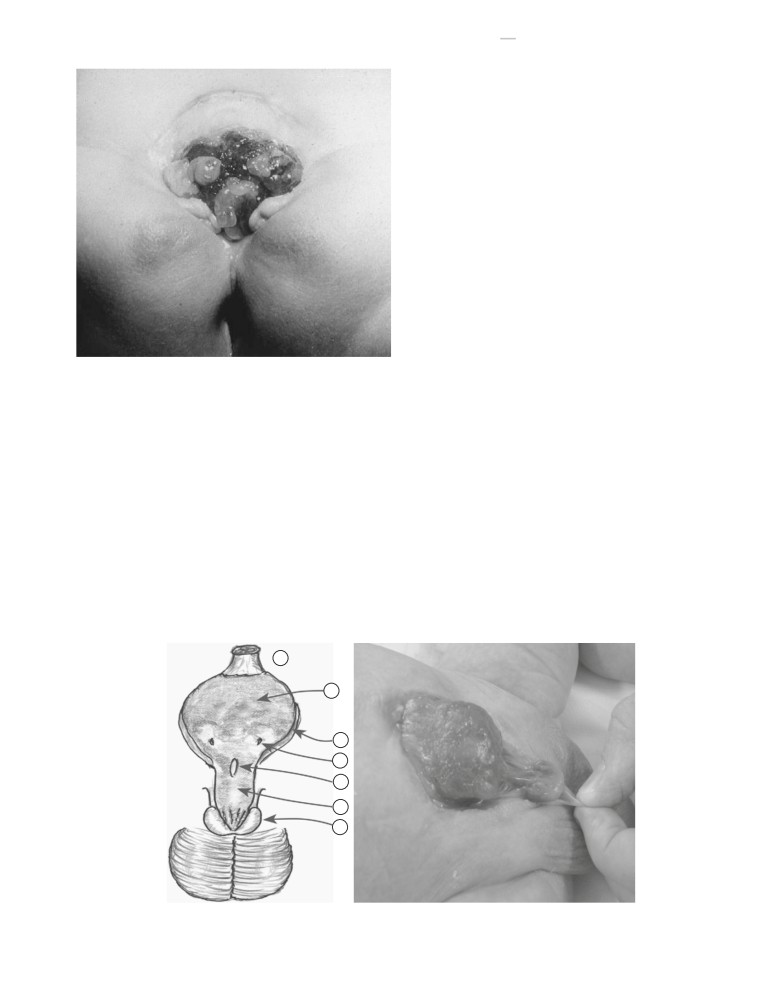
FIGURE 120-1
Division of the cloaca in the urogenital sinus and rectum. A, At the end of the fifth week. B, At 7 weeks. C, At 8 weeks. (Modified from Sadler
TW: Langman’s Medical Embryology, 8th ed. Philadelphia, Lippincott Williams and Wilkins, 2000, p 316.)
development, lateral ingrowth of mesoderm occurs between
submucosal tunnel in the bladder wall.22 With continued ex-
the two layers of the cloacal membrane during the fourth
posure and chronic inflammation, the exstrophied bladder
and fifth weeks of gestation. This results in formation of the
becomes thickened and polypoid (Fig. 120-3). Long-term
lower abdominal wall and pelvis. Subsequent caudal growth
exposure may eventually result in a fibrotic, rigid bladder
of the urorectal septum results in its fusion with the cloacal
plate that is ultimately unsuitable for closure.
membrane, thus fully separating the cloaca into the bladder
anteriorly and the rectum posteriorly (Fig. 120-1). The paired
GENITAL DEFECTS—MALE
genital tubercles, which will give rise to the phallus, migrate
medially to fuse in the midline. Normal perforation of the clo-
In the male infant, the open and everted urethral plate can be
acal membrane occurs after fusion with the urorectal septum,
seen joining the exposed bladder. The penis is characteristi-
at approximately the sixth week, resulting in formation of
cally short with a flattened, everted glans. The prepuce is lo-
separate urogenital and anal openings.17
cated on the penile ventrum (Fig. 120-4). The ejaculatory
Migratory failure of the lateral mesodermal folds and ab-
ducts are typically normal and exit at the exposed verumon-
normal overdevelopment of the cloacal membrane have both
tanum in the posterior urethra. The base of the penis and scro-
been proposed as potential causes of the prevention of normal
tum are widely separated, with lateral displacement of the
mesodermal ingrowth to the cloacal membrane.16,18 The lack
corporal bodies and neurovascular bundles. Historically it
of adequate mesodermal reinforcement is thought to result in
was believed that the individual corpora were of normal cal-
premature rupture of the cloacal membrane, the timing of
iber and appeared shortened because of their attachment to
which determines the extent of the abdominal wall defect
the widened pubic diastasis and associated dorsal chordee.
and degree/severity of urogenital tract involvement.19 Rupture
of the cloacal membrane after fusion with the urorectal sep-
tum results in bladder exstrophy, whereas rupture before fu-
sion gives rise to the more severe presentation of cloacal
exstrophy (see later discussion).
CLINICAL PRESENTATION
In general infants with bladder exstrophy are born full term,
without coexisting anatomic anomalies. At birth, an everted
posterior bladder plate of varying size is seen in the midline
of the lower abdomen. The mucosa of the exposed bladder
in the newborn is typically smooth and pink. The umbilical
cord exits from the superior-most border of the bladder plate,
and a small umbilical hernia may be present (Fig. 120-2). In
addition, there is significant widening of the pubic symphysis
and the anus is anteriorly displaced. The levator ani complex
is also divergent, leading to an inherent weakness in the pelvic
floor and a tendency toward rectal prolapse and varying de-
grees of fecal incontinence. Associated inguinal hernias are
common and have been reported in 82% of boys and 10%
of girls.20 The upper urinary tract is usually normal, though
renal anomalies including ectopic, horseshoe, hypoplastic,
FIGURE 120-2
Typical findings of classic bladder exstrophy in a new-
dysplastic kidneys, and megaureters may be observed.21 Vesi-
born male. The bladder plate is small, and a small hernia is evident at its
coureteral reflux occurs in the vast majority of children after
superior border. The penis is foreshortened, with widely splayed corporal
bladder closure, secondary to an exaggerated lateral course
bodies and glanular separation. The urethral plate is short and located on
of the ureters within the pelvis and lack of adequate
the anterior surface of the split phallus.
CHAPTER 120
BLADDER AND CLOACAL EXSTROPHY
1517
GENITAL DEFECTS—FEMALE
The clitoris is bifid, with divergence of the mons pubis, labia,
and clitoral halves (Fig. 120-6). The urethra and vagina are
shortened, and the introitus is anteriorly displaced. The vag-
inal orifice is often stenotic. The uterus and adnexa are typi-
cally normal, though vaginal and uterine duplication have
been reported.24,25
Uterine prolapse occurs commonly in
female patients, secondary to the inherent weakness in pelvic
floor support.
PELVIC DEFECTS
Some degree of widening of the pubic symphysis is present in
all cases of bladder exstrophy and contributes to outward ro-
tation and eversion of the pubic rami at their junctions with
the ischial and iliac bones (Fig. 120-7). Using computed to-
mography (CT), Sponseller and colleagues further character-
ized the pelvic anatomy of a large group of exstrophy
patients, noting a significantly increased distance between
the triradiate cartilages (31%), external rotation of the anterior
pelvis (18%), and 30% shortening of the pubic rami.26 On the
FIGURE 120-3
When the bladder has been exposed for at least 1 week
basis of three-dimensional models generated by CT, Stec and
after birth and the mucosa is subjected to continued exposure and inflam-
colleagues observed that among children with exstrophy, the
mation, polypoid excrescences typically appear, as in this female infant.
levator ani muscles were more posteriorly positioned and out-
wardly rotated. Furthermore, the puborectal sling had a more
More recently, an MRI-based study by Silver and colleagues of
flattened configuration and supported twice the body cavity
adult men with exstrophy and age-matched controls found
area in exstrophy patients.27 As mentioned previously, these
that although the length of the posterior corporal bodies
pelvic floor defects predispose to pelvic organ and rectal
was the same between groups, anterior corporal length in
prolapse in this patient population.
men with exstrophy was nearly 50% shorter than that of con-
trols.23 Therefore the penis appears shortened not only second-
PRENATAL DIAGNOSIS
ary to corporal divergence, dorsal chordee, and abnormal
crural attachments to the corpora cavernosa but also because
The use of prenatal ultrasound (US) and MRI has improved
of an inherent deficiency of corporal tissue (Fig. 120-5). The
the antenatal diagnosis of bladder exstrophy, allowing for ap-
testes may appear to be undescended, but in most cases they
propriate parental counseling and planning of postnatal man-
are actually retractile and will eventually reside in the scrotum
agement. The prenatal diagnosis of bladder exstrophy may be
without the need for formal orchiopexy. Should it be required,
suggested on US by failure to visualize the bladder in the pres-
orchiopexy is performed in conjunction with inguinal hernia
ence of normal kidneys and amniotic fluid.28-30 In a review of
repair.
prenatal US studies from 25 women who delivered infants
1
2
3
4
5
6
7
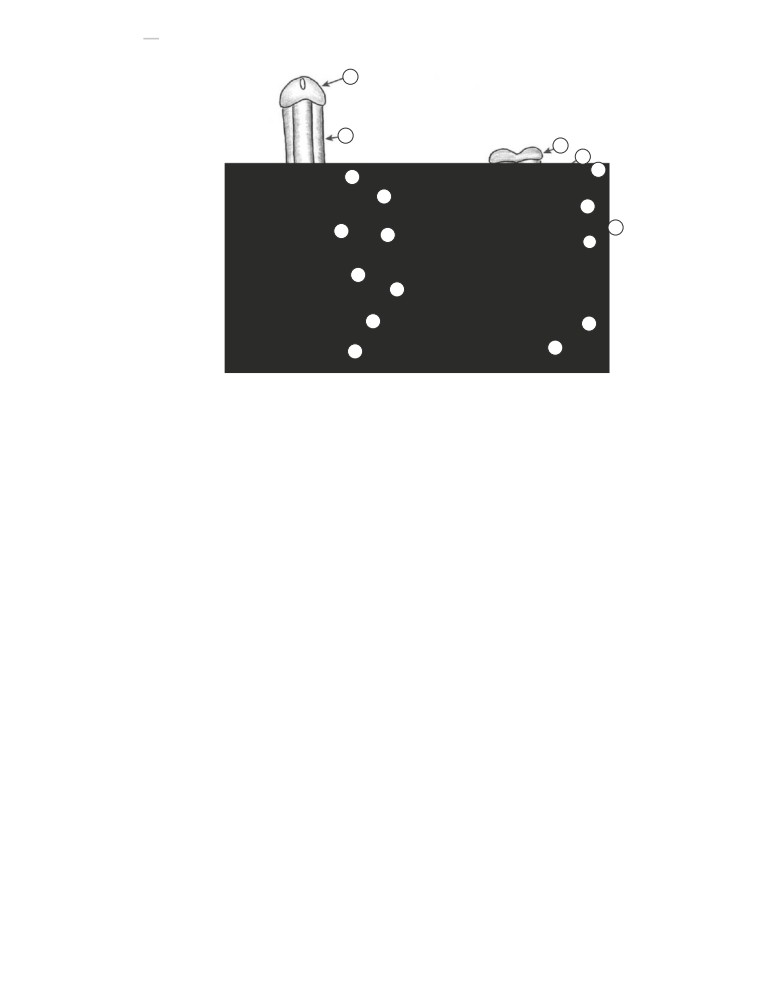
FIGURE 120-4
Classic exstrophy in the male. The penis is pulled downward to expose the dorsal aspect, revealing the urethral plate leading to the
exposed bladder. 1, umbilical cord; 2, bladder mucosa; 3, paraexstrophy tissues; 4, left ureteric orifice; 5, verumontanum; 6, urethral plate; 7, glans penis.
1518
PART VIII
GENITOURINARY DISORDERS
2
1
2
11
9
3
FIGURE 120-5
Penile configura-
tion in classic bladder exstrophy.
4
Normal male perineum (A) and with
7
bladder exstrophy (B). Note the loss
8
of the normal triangular shape of
7
8
the perineum and widening of the
6
pubic symphysis. In the setting of
exstrophy, the corpora cavernosa
are widely separated and are intrin-
6
sically shorter.
1, corpus caverno-
9
sum of the penis; 2, glans penis;
3, corpus spongiosum;
4, bul-
bospongiosus muscle;
5, ischium;
5
5
6, ischiopubic ramus;
7, pubis;
8,
ischio-cavernosus muscle and crus
10
10
of penis; 9, urogenital diaphragm;
10, anus and external anal sphincter.
A
B
with exstrophy, Gearhart and colleagues observed the follow-
be accomplished in a multi- or single-stage (complete) repair.
ing features: absent bladder (71%), lower abdominal bulge
Multiple contemporary approaches including the modern
(47%) and anteriorly displaced scrotum with small phallus
staged reconstruction of exstrophy
(MSRE) and complete
in male fetuses (57%), low-set umbilical cord (29%), and
primary reconstruction of exstrophy (CPRE) along with War-
abnormal widening of the iliac crest (18%).31
saw,32 Erlangen,24 Mainz,33 and Kelly34 techniques have been
published; however, for the purposes of this review, only the
major principles of MRSE and CPRE are discussed.
SURGICAL RECONSTRUCTION
Surgical management of classic bladder exstrophy consists of
functional closure of the native bladder, closure of the epispa-
dic urethra and genitalia, and creation of a continence mech-
anism to allow for proper urine storage. Reconstruction may
FIGURE 120-6
Typical appearance of classic bladder exstrophy in a fe-
FIGURE 120-7
Plain radiograph of a neonate with bladder exstrophy
male. Note the widely divergent labia and anterior displacement of the
demonstrates the soft tissue mass effect of the exposed bladder, the wide
vaginal introitus and anus.
diastasis of the symphysis pubis, and the posterior rotation of the
acetabula.
1520
PART VIII
GENITOURINARY DISORDERS
A
B
C
D
E
F
G
H
I
J
K
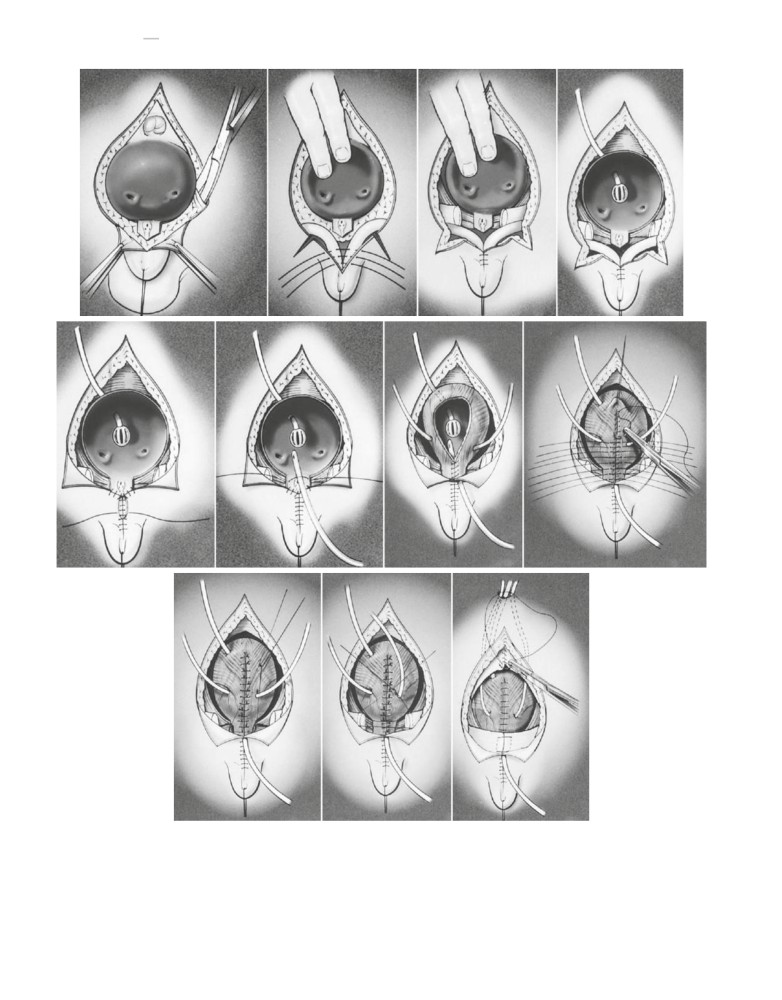
FIGURE 120-9
Sequence of repair of bladder exstrophy in a male. A, Completion of the dissection around the periphery of the bladder and the urethral
plate. B, Inversion of the bladder plate and approximation of the corpora as a first stage in epispadias repair. Also note the inferior paraexstrophy incisions.
C, Further closure of the skin over the corpora and their partial freeing from the pubis. D, Placement of a suprapubic drainage tube. E, Further closure of the
skin inferiorly, with approximation to the urethral plate. Creation of the paraexstrophy flaps is now evident. F, The urethral plate is prepared for tubular-
ization over a catheter. G, The urethral plate is now tubularized, and ureteral catheters are placed bilaterally and brought out on each side of the bladder.
The bladder is also in the process of being tubularized. H, Completion of tubularization of the bladder and urethra, and location of the various drainage
tubes. I, After two-layer closure of the bladder and urethral plate, the bladder is reduced into the pelvis and fixed with sutures. J, Sutures are placed to
encourage approximation of the pubic halves. K, Drainage tubes are brought out superiorly, and fascia, subcutaneous tissue, and skin are approximated.
Approximation of the pubis helps protect the bladder closure and the abdominal wall closure.