ABC of heart failure
History and epidemiology
R C Davis, F D R Hobbs, G Y H Lip
Heart failure is the end stage of all diseases of the heart and is a
“The very essence of cardiovascular
major cause of morbidity and mortality. It is estimated to
practice is the early detection of heart
account for about 5% of admissions to hospital medical wards,
failure”
with over 100 000 annual admissions in the United Kingdom.
Sir Thomas Lewis, 1933
The overall prevalence of heart failure is 320 per 1000
population, although this exceeds 100 per 1000 in those aged
65 years and over. The annual incidence of heart failure is 15
per 1000, and the relative incidence doubles for each decade of
life after the age of 45 years. The overall incidence is likely to
Some definitions of heart failure
increase in the future, because of both an ageing population
“A condition in which the heart fails to discharge its contents
and therapeutic advances in the management of acute
adequately” (Thomas Lewis, 1933)
“A state in which the heart fails to maintain an adequate circulation
myocardial infarction leading to improved survival in patients
for the needs of the body despite a satisfactory filling pressure”
with impaired cardiac function.
(Paul Wood, 1950)
Unfortunately, heart failure can be difficult to diagnose
“A pathophysiological state in which an abnormality of cardiac
clinically, as many features of the condition are not organ
function is responsible for the failure of the heart to pump blood
specific, and there may be few clinical features in the early
at a rate commensurate with the requirements of the metabolising
stages of the disease. Recent advances have made the early
tissues” (E Braunwald, 1980)
recognition of heart failure increasingly important as modern
“Heart failure is the state of any heart disease in which, despite
adequate ventricular filling, the heart’s output is decreased or in
drug treatment has the potential to improve symptoms and
which the heart is unable to pump blood at a rate adequate for
quality of life, reduce hospital admission rates, slow the rate of
satisfying the requirements of the tissues with function parameters
disease progression, and improve survival. In addition, coronary
remaining within normal limits” (H Denolin, H Kuhn, H P
revascularisation and heart valve surgery are now regularly
Krayenbuehl, F Loogen, A Reale, 1983)
performed, even in elderly patients.
“A clinical syndrome caused by an abnormality of the heart and
recognised by a characteristic pattern of haemodynamic, renal,
neural and hormonal responses” (Philip PooleWilson, 1985)
A brief history
“[A] syndrome . . . which arises when the heart is chronically unable to
maintain an appropriate blood pressure without support” (Peter
Descriptions of heart failure exist from ancient Egypt, Greece,
Harris, 1987)
and India, and the Romans were known to use the foxglove as
“A syndrome in which cardiac dysfunction is associated with reduced
exercise tolerance, a high incidence of ventricular arrhythmias and
medicine. Little understanding of the nature of the condition
shortened life expectancy” (Jay Cohn, 1988)
can have existed until William Harvey described the circulation
“Abnormal function of the heart causing a limitation of exercise
in 1628. Röntgen’s discovery of x rays and Einthoven’s
capacity” or “ventricular dysfunction with symptoms” (anonymous
development of electrocardiography in the 1890s led to
and pragmatic)
improvements in the investigation of heart failure. The advent
“Symptoms of heart failure, objective evidence of cardiac dysfunction
of echocardiography, cardiac catheterisation, and nuclear
and response to treatment directed towards heart failure” (Task
Force of the European Society of Cardiology, 1995)
medicine have since improved the diagnosis and investigation
of patients with heart failure.
Blood letting and leeches were used for centuries, and
William Withering published his account of the benefits of
digitalis in 1785. In the 19th and early 20th centuries, heart
failure associated with fluid retention was treated with Southey’s
tubes, which were inserted into oedematous peripheries,
allowing some drainage of fluid.
Southey’s tubes were at one time used for removing fluid from oedematous
peripheries in patients with heart failure
The foxglove was used as a medicine in heart
disease as long ago as Roman times
1
A brief history of heart failure
1628
William Harvey describes the circulation
1785
William Withering publishes an account of medical
use of digitalis
1819
René Laennec invents the stethoscope
1895
Wilhelm Röntgen discovers x rays
1920
Organomercurial diuretics are first used
1954
Inge Edler and Hellmuth Hertz use ultrasound to
image cardiac structures
1958
Thiazide diuretics are introduced
1967
Christiaan Barnard performs first human heart
transplant
1987
CONSENSUSI study shows unequivocal survival
benefit of angiotensin converting enzyme inhibitors in
severe heart failure
1995
European Society of Cardiology publishes guidelines
for diagnosing heart failure
In 1785 William Withering of Birmingham published
an account of medicinal use of digitalis
0.8
It was not until the 20th century that diuretics were
Placebo
Enalapril
developed. The early, mercurial agents, however, were
0.7
associated with substantial toxicity, unlike the thiazide diuretics,
0.6
which were introduced in the 1950s. Vasodilators were not
widely used until the development of angiotensin converting
0.5
enzyme inhibitors in the 1970s. The landmark CONSENSUSI
0.4
study (first cooperative north Scandinavian enalapril survival
0.3
study), published in 1987, showed the unequivocal survival
benefits of enalapril in patients with severe heart failure.
0.2
0.1
Epidemiology
0
0
1
2
3
4
5
6
7
8
9
10
11
12
Months
Studies of the epidemiology of heart failure have been
complicated by the lack of universal agreement on a definition
Mortality curves from the CONSENSUSI study
of heart failure, which is primarily a clinical diagnosis. National
and international comparisons have therefore been difficult,
and mortality data, postmortem studies, and hospital admission
rates are not easily translated into incidence and prevalence.
Several different systems have been used in large population
studies, with the use of scores for clinical features determined
from history and examination, and in most cases chest
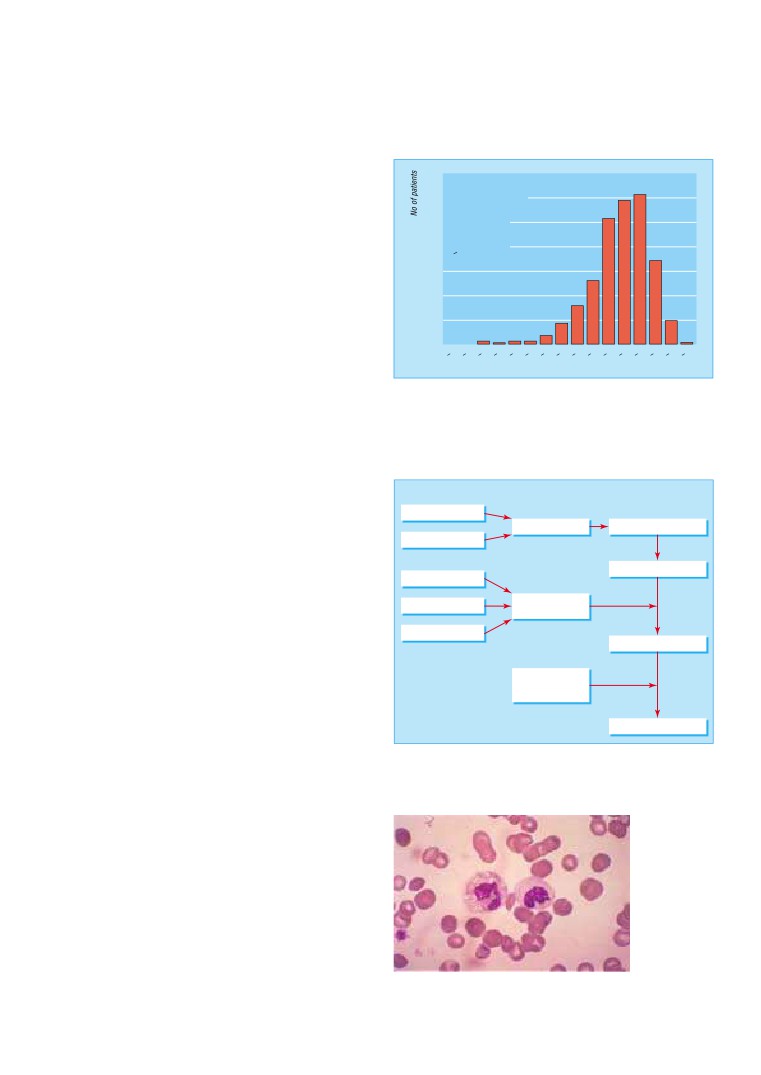
The Framingham heart study has been
radiography, to define heart failure.
the most important longitudinal source of
The Task Force on Heart Failure of the European Society of
data on the epidemiology of heart failure
Cardiology has recently published guidelines on the diagnosis
of heart failure, which require the presence of symptoms and
objective evidence of cardiac dysfunction. Reversibility of
symptoms on appropriate treatment is also desirable.
Echocardiography is recommended as the most practicable way
of assessing cardiac function, and this investigation has been
used in more recent studies.
In the Framingham heart study a cohort of 5209 subjects
Contemporary studies of the epidemiology of heart failure
in United Kingdom
has been assessed biennially since 1948, with a further cohort
(their offspring) added in 1971. This uniquely large dataset has
Study
Diagnostic criteria
been used to determine the incidence and prevalence of heart
failure, defined with consistent clinical and radiographic criteria.
Hillingdon heart failure study
Clinical (for example, shortness of
(west London)
breath, effort intolerance, fluid
Several recent British studies of the epidemiology of heart
retention), radiographic, and
failure and left ventricular dysfunction have been conducted,
echocardiographic
including a study of the incidence of heart failure in one west
ECHOES study (West Midlands) Clinical and echocardiographic
London district (Hillingdon heart failure study) and large
(ejection fraction < 40%)
prevalence studies in Glasgow (north Glasgow MONICA study)
MONICA population
Clinical and echocardiographic
and the West Midlands ECHOES (echocardiographic heart of
(north Glasgow)
(ejection fraction <30%)
England screening) study. It is important to note that
2
epidemiological studies of heart failure have used different
Prevalence of heart failure (per 1000 population),
levels of ejection fraction to define systolic dysfunction. The
Framingham heart study
Glasgow study, for example, used an ejection fraction of 30% as
their criteria, whereas most other epidemiological surveys have
Age (years)
Men
Women
used levels of 4045%. Indeed, prevalence of heart failure seems
5059
8
8
similar in many different surveys, despite variation in the levels
8089
66
79
of ejection fraction, and this observation is not entirely
All ages
7.4
7.7
explained.
Prevalence of heart failure
During the 1980s the Framingham study reported the age
adjusted overall prevalence of heart failure, with similar rates
for men and women. Prevalence increased dramatically with
increasing age, with an approximate doubling in the prevalence
of heart failure with each decade of ageing.
In Nottinghamshire, the prevalence of heart failure in 1994
Methods of assessing prevalence of heart failure in
was estimated from prescription data for loop diuretics and
published studies
examination of the general practice notes of a sample of these
x Clinical and radiographic assessment
patients, to determine the number who fulfilled predetermined
x Echocardiography
criteria for heart failure. The overall prevalence of heart failure
x General practice monitoring
was estimated as 1.0% to 1.6%, rising from 0.1% in the 3039
x Drug prescription data
age range to 4.2% at 7079 years. This method, however, may
exclude individuals with mild heart failure and include patients
treated with diuretics who do not have heart failure.
Incidence of heart failure
The Framingham data show an age adjusted annual incidence
of heart failure of 0.14% in women and 0.23% in men. Survival
in the women is generally better than in the men, leading to the
same point prevalence. There is an approximate doubling in the
Annual incidence of heart failure (per 1000 population),
Framingham heart study
incidence of heart failure with each decade of ageing, reaching
3% in those aged 8594 years.
Age (years)
Men
Women
The recent Hillingdon study examined the incidence of
heart failure, defined on the basis of clinical and radiographic
5059
3
2
findings, with echocardiography, in a population in west
8089
27
22
London. The overall annual incidence was 0.08%, rising from
All ages
2.3
1.4
0.02% at age 4555 years to 1.2% at age 86 years or over. About
80% of these cases were first diagnosed after acute hospital
admission, with only 20% being identified in general practice
and referred to a dedicated clinic.
The Glasgow group of the MONICA study and the
ECHOES Group have found that coronary artery disease is the
most powerful risk factor for impaired left ventricular function,
either alone or in combination with hypertension. In these
studies hypertension alone did not appear to contribute
The MONICA study is an international
substantially to impairment of left ventricular systolic
study conducted under the auspices of
contraction, although the Framingham study did report a more
the World Health Organisation to
substantial contribution from hypertension. This apparent
monitor trends in and determinants of
difference between the studies may reflect improvements in the
mortality from cardiovascular disease
treatment of hypertension and the fact that some patients with
hypertension, but without coronary artery disease, may develop
heart failure as a result of diastolic dysfunction.
Prevalence of left ventricular dysfunction
Large surveys have been carried out in Britain in the 1990s, in
Glasgow and the West Midlands, using echocardiography.
Prevalence (%) of left ventricular dysfunction, north Glasgow
In Glasgow the prevalence of significantly impaired left
(MONICA survey)
ventricular contraction in subjects aged 2574 years was 2.9%;
in the West Midlands, the prevalence was 1.8% in subjects aged
Asymptomatic
Symptomatic
45 and older.
Age group
(years)
Men
Women
Men
Women
The higher rates in the Scottish study may reflect the high
prevalence of ischaemic heart disease, the main precursor of
4554
4.4
1.2
1.4
1.2
impaired left ventricular function in both studies. The numbers
5564
3.2
0.0
2.5
2.0
of symptomatic and asymptomatic cases, in both studies, were
6574
3.2
1.3
3.2
3.6
about the same.
3
Ethnic differences
Ethnic differences in the incidence of and mortality from heart
In the United States mortality from heart
failure have also been reported. In the United States,
failure at age <65 years has been reported
AfricanAmerican men have been reported as having a 33%
as being up to 2.5fold higher in black
greater risk of being admitted to hospital for heart failure than
patients than in white patients
white men; the risk for black women was 50%.
A similar picture emerged in a survey of heart failure
among acute medical admissions to a city centre teaching
hospital in Birmingham. The commonest underlying
aetiological factors were coronary heart disease in white
Cost of heart failure
patients, hypertension in black AfroCaribbean patients, and
coronary heart disease and diabetes in IndoAsians. Some of
% Healthcare
% Of costs due
these racial differences may be related to the higher prevalence
Country
Cost
costs
to admissions
of hypertension and diabetes in black people and coronary
UK, 19901
£360m
1.2
60
artery disease and diabetes mellitus in IndoAsians.
US, 1989
$9bn
1.5
71
France, 1990
FF11.4bn
1.9
64
Impact on health services
New Zealand, 1990
$NZ73m
1.5
68
Sweden, 1996
Kr2.6m
2.0
75
Heart failure accounts for at least 5% of admissions to general
medical and geriatric wards in British hospitals, and admission
rates for heart failure in various European countries (Sweden,
Netherlands, and Scotland) and in the United States have
doubled in the past 1015 years. Furthermore, heart failure
Key references
accounts for over 1% of the total healthcare expenditure in the
United Kingdom, and most of these costs are related to hospital
x Clarke KW, Gray D, Hampton JR. Evidence of inadequate
admissions. The cost of heart failure is increasing, with an
investigation and treatment of patients with heart failure. Br Heart J
1994;71:5847.
estimated UK expenditure in 1996 of £465m (£556m when the
x Cowie MR, Mosterd A, Wood DA, Deckers JW, PooleWilson PA,
costs of community health services and nursing homes are
Sutton GC, et al. The epidemiology of heart failure. Eur Heart J
included).
1997;18:20825.
Hospital readmissions and general practice consultations
x Cowie MR, Wood DA, Coats AJS, Thompson SG, PooleWilson PA,
often occur soon after the diagnosis of heart failure. In elderly
Suresh V, et al. Incidence and aetiology of heart failure: a
patients with heart failure, readmission rates range from
populationbased study. Eur Heart J 1999;20:4218.
x Dries DL, Exner DV, Gersh BJ, Cooper HA, Carson PE, Domanski
2947% within 3 to 6 months of the initial hospital discharge.
MJ. Racial differences in the outcome of left ventricular dysfunction.
Treating patients with heart failure with angiotensin converting
N Engl J Med 1999;340:60916.
enzyme inhibitors can reduce the overall cost of treatment
x Ho KK, Pinsky JL, Kannel WB, Levy D. The epidemiology of heart
(because of reduced hospital admissions) despite increased drug
failure: the Framingham study. J Am Coll Cardiol 1993;22:613A.
expenditure and improved long term survival.
x Lip GYH, Zarifis J, Beevers DG. Acute admissions with heart failure
to a district general hospital serving a multiracial population. Int J
The pictures of William Withering and of the foxglove are reproduced
Clin Pract 1997;51:2237.
with permission from the Fine Art Photographic Library. The box of
x McDonagh TA, Morrison CE, Lawrence A, Ford I, TunstallPedoe H,
definitions of heart failure is adapted from PooleWilson PA et al, eds
McMurray JJV, et al. Symptomatic and asymptomatic leftventricular
(Heart failure. New York: Churchill Livingstone, 1997:270). The table show
ing the prevalence of left ventricular dysfunction in north Glasgow is
systolic dysfunction in an urban population. Lancet 1997;350:82933.
reproduced with permission from McDonagh TA et al (see key references
x The Task Force on Heart Failure of the European Society of
box). The table showing costs of heart failure is adapted from McMurray J
Cardiology. Guidelines for the diagnosis of heart failure. Eur Heart J
et al (Br J Med Econ 1993;6:99110).
1995;16:74151.
The ABC of heart failure is edited by C R Gibbs, M K Davies, and
G Y H Lip. CRG is research fellow and GYHL is consultant
cardiologist and reader in medicine in the university department of
R C Davis is clinical research fellow and F D R Hobbs is professor in
medicine and the department of cardiology, City Hospital,
the department of primary care and general practice, University of
Birmingham; MKD is consultant cardiologist in the department of
Birmingham.
cardiology, Selly Oak Hospital, Birmingham. The series will be
published as a book in the spring.
BMJ 2000;320:3942
One hundred years ago
The Bogey of Medical Etiquette.
There is a widespread opinion amongst the public that a rule of
their property, and we believe that the petty tyranny sometimes
conduct obtains in the medical profession the object of which is
exercised is responsible for the opinions upon medical etiquette
to protect the profession and individual members thereof against
which are undoubtedly entertained by the laity. But these extreme
the consequences of their ignorance or mistakes. Probably
views are not endorsed by any representative body in the medical
opinions differ as to the extent to which we are prepared to go in
profession, and we are quite certain that we are expressing the
this direction, and perhaps few believe that we would go so far as
general view when we say that the profession recognises no other
to commit perjury or sacrifice human life, but we certainly are
rules of medical etiquette than are consistent with the best
supposed to be capable of suppressing the truth in order to avoid
interests of our patients and with courtesy and consideration for
exposing the mistakes of a colleague. We admit that there are
our colleagues. (BMJ 1900;i:156)
members of the medical profession who regard their patients as
4
ABC of heart failure
Aetiology
G Y H Lip, C R Gibbs, D G Beevers
The relative importance of aetiological factors in heart failure is
Causes of heart failure
dependent on the nature of the population being studied, as
Coronary artery disease
coronary artery disease and hypertension are common causes
x Myocardial infarction
of heart failure in Western countries, whereas valvar heart
x Ischaemia
disease and nutritional cardiac disease are more common in the
Hypertension
developing world. Epidemiological studies are also dependent
Cardiomyopathy
on the clinical criteria and relevant investigations used for
x Dilated (congestive)
diagnosis, as it remains difficult, for example, to distinguish
x Hypertrophic/obstructive
whether hypertension is the primary cause of heart failure or
x Restrictive—for example, amyloidosis, sarcoidosis,
whether there is also underlying coronary artery disease.
haemochromatosis
x Obliterative
Valvar and congenital heart disease
Coronary artery disease and its risk
x Mitral valve disease
x Aortic valve disease
factors
x Atrial septal defect, ventricular septal defect
Coronary heart disease is the commonest cause of heart failure
Arrhythmias
in Western countries. In the studies of left ventricular
x Tachycardia
x Bradycardia (complete heart block, the sick sinus
dysfunction (SOLVD) coronary artery disease accounted for
syndrome)
almost 75% of the cases of chronic heart failure in male white
x Loss of atrial transport—for example, atrial
patients, although in the Framingham heart study, coronary
fibrillation
heart disease accounted for only 46% of cases of heart failure in
Alcohol and drugs
men and 27% of chronic heart failure cases in women.
x Alcohol
Coronary artery disease and hypertension (either alone or in
x Cardiac depressant drugs (â blockers, calcium
combination) were implicated as the cause in over 90% of cases
antagonists)
of heart failure in the Framingham study.
“High output” failure
Recent studies that have allocated aetiology on the basis of
x Anaemia, thyrotoxicosis, arteriovenous fistulae,
noninvasive investigations—such as the Hillingdon heart failure
Paget’s disease
study—have identified coronary artery disease as the primary
Pericardial disease
aetiology in 36% of cases of heart failure. In the Hillingdon
x Constrictive pericarditis
x Pericardial effusion
study, however, researchers were not able to identify the
primary aetiology in 34% of cases; this methodological failing
Primary right heart failure
x Pulmonary hypertension—for example,
has been addressed in the current Bromley heart failure study,
pulmonary embolism, cor pulmonale
which uses coronary angiography as well as historical and
x Tricuspid incompetence
noninvasive findings.
Coronary risk factors, such as smoking and diabetes
mellitus, are also risk markers of the development of heart
failure. Smoking is an independent and strong risk factor for
the development of heart failure in men, although the findings
in women are less consistent.
In the prevention arm of SOLVD diabetes was an
independent risk factor (about twofold) for mortality, the
Epidemiological studies of aetiology of heart failure. Values
Relative risks for development of heart failure: 36 year
are percentages
follow up in Framingham heart study
Teerlink
Framingham
Age (years)
et al
heart study*
(31 studies
Hillingdon
Men
Women
Aetiology
198990)
Men W
omen
study
Variable
3564
6594
3564
6594
Ischaemic
50
59
48
36
Nonischaemic:
50
41
52
64
Serum cholesterol
1.2
0.9
0.7
0.8
( > 6.3 mmol/l)
Hypertension
4
70
78
14
Hypertension
4.0
1.9
3.0
1.9
Idiopathic
18
0
0
0
( > 160/95 mm Hg or
Valvar
4
22
31
7
receiving treatment)
Other
10
7
7
10
Glucose intolerance
4.4
2.0
7.7
3.6
“Unknown”
13
0
0
34
Electrocardiographic left
ventricular hypertrophy
15.0
4.9
12.8
5.4
Because of rounding, totals may not equal 100%.
*Total exceeds 100% as coronary artery disease and hypertension were not
considered as mutually exclusive causes.
5
development of heart failure, and admission to hospital for
heart failure, whereas in the Framingham study diabetes and
left ventricular hypertrophy were the most significant risk
markers of the development of heart failure. Body weight and a
high ratio of total cholesterol concentration to high density
lipoprotein cholesterol concentration are also independent risk
factors for heart failure. Clearly, these risk factors may increase
the risks of heart failure through their effects on coronary
artery disease, although diabetes alone may induce important
structural and functional changes in the myocardium, which
further increase the risk of heart failure.
Hypertension
Hypertension has been associated with an increased risk of
heart failure in several epidemiological studies. In the
Framingham heart study, hypertension was reported as the
cause of heart failure—either alone or in association with other
factors—in over 70% of cases, on the basis of noninvasive
assessment. Other community and hospital based studies,
however, have reported hypertension to be a less common
cause of heart failure, and, indeed, the importance of
hypertension as a cause of heart failure has been declining in
the Framingham cohort since the 1950s. Recent community
based studies that have assessed aetiology using clinical criteria
and relevant noninvasive investigations have reported
hypertension to be the cause of heart failure in 1020%.
Two dimensional echocardiogram (top) and M mode echocardiogram
However, hypertension is probably a more common cause of
(bottom) showing left ventricular hypertrophy. A=interventricular
septum; B=posterior left ventricular wall
heart failure in selected patient groups, including females and
black populations (up to a third of cases).
Hypertension predisposes to the development of heart
failure via a number of pathological mechanisms, including left
ventricular hypertrophy. Left ventricular hypertrophy is
associated with left ventricular systolic and diastolic dysfunction
Effective blood pressure lowering in
and an increased risk of myocardial infarction, and it
patients with hypertension reduces the
risk of heart failure; an overview of trials
predisposes to both atrial and ventricular arrhythmias.
has estimated that effective
Electrocardiographic left ventricular hypertrophy is strongly
antihypertensive treatment reduces the
correlated with the development of heart failure, as it is
age standardised incidence of heart
associated with a 14fold increase in the risk of heart failure in
failure by up to 50%
those aged 65 years or under.
Cardiomyopathies
Cardiomyopathies are defined as the diseases of heart muscle
Causes of dilated cardiomyopathy
that are not secondary to coronary disease, hypertension, or
Familial
congenital, valvar, or pericardial disease. As primary diseases of
Infectious
heart muscle, cardiomyopathies are less common causes of
x Viral (coxsackie B, cytomegalovirus, HIV)
heart failure, but awareness of their existence is necessary to
x Rickettsia
make a diagnosis. Cardiomyopathies are separated into four
x Bacteria (diphtheria)
functional categories: dilated (congestive), hypertrophic,
x Mycobacteria
x Fungus
restrictive, and obliterative. These groups can include rare,
x Parasites (Chagas’ disease, toxoplasmosis)
specific heart muscle diseases (such as haemochromatosis (iron
x Alcohol
overload) and metabolic and endocrine disease), in which
x Cardiotoxic drugs (adriamycin, doxorubicin, zidovudine)
cardiac involvement occurs as part of a systemic disorder.
x Cocaine
Dilated cardiomyopathy is a more common cause of heart
x Metals (cobalt, mercury, lead)
failure than hypertrophic and restrictive cardiomyopathies;
x Nutritional disease (beriberi, kwashiorkor, pellagra)
x Endocrine disease (myxoedema, thyrotoxicosis, acromegaly,
obliterative cardiomyopathy is essentially limited to developing
phaeochromocytoma)
countries.
Pregnancy
Collagen disease
Dilated cardiomyopathy
x Connective tissue diseases (systemic lupus erythematosus,
Dilated cardiomyopathy describes heart muscle disease in
scleroderma, polyarteritis nodosa)
which the predominant abnormality is dilatation of the left
Neuromuscular
ventricle, with or without right ventricular dilatation. Myocardial
x Duchenne muscular dystrophy, myotonic dystrophy
cells are also hypertrophied, with increased variation in size and
Idiopathic
increased extracellular fibrosis. Family studies have reported
6
that up to a quarter of cases of dilated cardiomyopathy have a
familial basis. Viral myocarditis is a recognised cause; connective
tissue diseases such as systemic lupus erythematosus, the
ChurgStrauss syndrome, and polyarteritis nodosa are rarer
causes. Idiopathic dilated cardiomyopathy is a diagnosis of
exclusion. Coronary angiography will exclude coronary disease,
and an endomyocardial biopsy is required to exclude
underlying myocarditis or an infiltrative disease.
Dilatation can be associated with the development of atrial
and ventricular arrhythmias, and dilatation of the ventricles
leads to “functional” mitral and tricuspid valve regurgitation.
Hypertrophic cardiomyopathy
Hypertrophic cardiomyopathy has a familial inheritance
(autosomal dominant), although sporadic cases may occur. It is
characterised by abnormalities of the myocardial fibres, and in
its classic form involves asymmetrical septal hypertrophy, which
may be associated with aortic outflow obstruction (hypertrophic
obstructive cardiomyopathy).
Nevertheless, other forms of hypertrophic cardiomyopathy
exist—apical hypertrophy (especially in Japan) and symmetrical
left ventricular hypertrophy (where the echocardiographic
distinction between this and hypertensive heart disease may be
unclear). These abnormalities lead to poor left ventricular
compliance, with high end diastolic pressures, and there is a
common association with atrial and ventricular arrhythmias, the
latter leading to sudden cardiac death. Mitral regurgitation may
Two dimensional (long axis parasternal view) echocardiogram (top) and
contribute to the heart failure in these patients.
M mode echocardiogram (bottom) showing severely impaired left ventricular
function in dilated cardiomyopathy
Restrictive and obliterative cardiomyopathies
Restrictive cardiomyopathy is characterised by a stiff and poorly
compliant ventricle, which is not substantially enlarged, and this
is associated with abnormalities of diastolic function (relaxation)
that limit ventricular filling. Amyloidosis and other infiltrative
diseases, including sarcoidosis and haemochromatosis, can
cause a restrictive syndrome. Endomyocardial fibrosis is also a
cause of restrictive cardiomyopathy, although it is a rare cause
of heart failure in Western countries. Endocardial fibrosis of the
inflow tract of one or both ventricles, including the subvalvar
regions, results in restriction of diastolic filling and cavity
obliteration.
Valvar disease
Two dimensional, apical, four chamber echocardiogram
Rheumatic heart disease may have declined in certain parts of
showing dilated cardiomyopathy. A=left ventricle; B=left
the world, but it still represents an important cause of heart
atrium; C=right atrium; D=right ventricle
failure in India and other developing nations. In the
Framingham study rheumatic heart disease accounted for heart
failure in 2% of men and 3% of women, although the overall
incidence of valvar disease has been steadily decreasing in the
Framingham cohort over the past 30 years.
Mitral regurgitation and aortic stenosis are the most
common causes of heart failure, secondary to valvar disease.
Mitral regurgitation (and aortic regurgitation) leads to volume
overload (increased preload), in contrast with aortic stenosis,
which leads to pressure overload (increased afterload). The
progression of heart failure in patients with valvar disease is
dependent on the nature and extent of the valvar disease. In
aortic stenosis heart failure develops at a relatively late stage
and, without valve replacement, it is associated with a poor
prognosis. In contrast, patients with chronic mitral (or aortic)
regurgitation generally decline in a slower and more
Colour Doppler echocardiograms showing mitral regurgitation (left) and
progressive manner.
aortic regurgitation (right)
7
Arrhythmias
Arrhythmias and heart failure: mechanisms
Cardiac arrhythmias are more common in patients with heart
Tachycardias
failure and associated structural heart disease, including
x Reduce diastolic ventricular filling time
hypertensive patients with left ventricular hypertrophy. Atrial
x Increase myocardial workload and myocardial oxygen demand,
fibrillation and heart failure often coexist, and this has been
precipitating ischaemia
x If they are chronic, with poor rate control, they may lead to
confirmed in large scale trials and smaller hospital based
ventricular dilatation and impaired ventricular function
studies. In the Hillingdon heart failure study 30% of patients
(“tachycardia induced cardiomyopathy”)
presenting for the first time with heart failure had atrial
Bradycardias
fibrillation, and over 60% of patients admitted urgently with
x Compensatory increase in stroke volume is limited in the presence
atrial fibrillation to a Glasgow hospital had echocardiographic
of structural heart disease, and cardiac output is reduced
evidence of impaired left ventricular function.
Abnormal atrial and ventricular contraction
Atrial fibrillation in patients with heart failure has been
x Loss of atrial systole leads to the absence of active ventricular filling,
associated with increased mortality in some studies, although
which in turn lowers cardiac output and raises atrial pressure—for
example, atrial fibrillation
the vasodilator heart failure trial (VHeFT) failed to show an
x Dissociation of atrial and ventricular activity impairs diastolic
increase in major morbidity or mortality for patients with atrial
ventricular filling, particularly in the presence of a tachycardia—for
fibrillation. In the stroke prevention in atrial fibrillation (SPAF)
example, ventricular tachycardia
study, the presence of concomitant heart failure or left
ventricular dysfunction increased the risk of stroke and
thromboembolism in patients with atrial fibrillation. Ventricular
arrhythmias are also more common in heart failure, leading to
Prevalence (%) of atrial fibrillation in major heart failure
a sudden deterioration in some patients; such arrhythmias are a
trials
major cause of sudden death in patients with heart failure.
Prevalence of
Trial
NYHA class*
atrial fibrillation
Alcohol and drugs
SOLVD
I-III
6
Alcohol has a direct toxic effect on the heart, which may lead to
VHeFT I
II-III
15
acute heart failure or heart failure as a result of arrhythmias,
VHeFT II
II-III
15
commonly atrial fibrillation. Excessive chronic alcohol
CONSENSUS
III-IV
50
consumption also leads to dilated cardiomyopathy (alcoholic
CONSENSUS = cooperative north Scandinavian enalapril survival study.
heart muscle disease). Alcohol is the identifiable cause of
*Classification of the New York Heart Association.
chronic heart failure in 23% of cases. Rarely, alcohol misuse
may be associated with general nutritional deficiency and
thiamine deficiency (beriberi).
Chemotherapeutic agents (for example, doxorubicin) and
I
aVR
V1
V4
antiviral drugs (for example, zidovudine) have been implicated
in heart failure, through direct toxic effects on the myocardium.
II
aVL
V2
V5
Other causes
III
aVF
V3
V6
Infections may precipitate heart failure as a result of the toxic
metabolic effects (relative hypoxia, acid base disturbance) in
combination with peripheral vasodilation and tachycardia,
II
leading to increased myocardial oxygen demand. Patients with
chronic heart failure, like patients with most chronic illnesses,
are particularly susceptible to viral and bacterial respiratory
infections. “High output” heart failure is most often seen in
Electrocardiogram showing atrial fibrillation with a rapid ventricular response
patients with severe anaemia, although thyrotoxicosis may also
be a precipitating cause in these patients. Myxoedema may
present with heart failure as a result of myocardial involvement
Key references
or secondary to a pericardial effusion.
x Cowie MR, Wood DA, Coats AJS, Thompson SG, PooleWilson PA,
The table of epidemiological studies of the aetiology of heart failure is
Suresh V, et al. Incidence and aetiology of heart failure: a
adapted and reproduced with permission from Cowie MR et al (Eur Heart J
populationbased study. Eur Heart J 1999;20:4218.
1997;18:20825). The table showing relative risks for development of heart
x Eriksson H, Svardsudd K, Larsson B, Ohlson LO, Tibblin G, Welin
failure (36 year follow up) is adapted and reproduced with permission from
Kannel WB et al (Br Heart J 1994;72:S39).
L, et al. Risk factors for heart failure in the general population: the
study of men born in 1913. Eur Heart J 1989;10:64756.
D G Beevers is professor of medicine in the university department of
x Levy D, Larson MG, Vasan RS, Kannel WB, Ho KKL. The
medicine and the department of cardiology, City Hospital,
progression from hypertension to congestive heart failure. JAMA
Birmingham.
1996;275:155762.
The ABC of heart failure is edited by C R Gibbs, M K Davies, and
x Oakley C. Aetiology, diagnosis, investigation, and management of
cardiomyopathies. BMJ 1997;315:15204.
G Y H Lip. CRG is research fellow and GYHL is consultant
x Teerlink JR, Goldhaber SZ, Pfeffer MA. An overview of
cardiologist and reader in medicine in the university department of
contemporary etiologies of congestive heart failure. Am Heart J
medicine and the department of cardiology, City Hospital,
1991;121:18523.
Birmingham; MKD is consultant cardiologist in the department of
x Wheeldon NM, MacDonald TM, Flucker CJ, McKendrick AD,
cardiology, Selly Oak Hospital, Birmingham. The series will be
McDevitt DG, Struthers AD. Echocardiography in chronic heart
published as a book in the spring.
failure in the community. Q J Med 1993;86:1723.
BMJ 2000;320:1047
8
ABC of heart failure
Pathophysiology
G Jackson, C R Gibbs, M K Davies, G Y H Lip
Heart failure is a multisystem disorder which is characterised by
Developments in our understanding of
abnormalities of cardiac, skeletal muscle, and renal function;
the pathophysiology of heart failure have
stimulation of the sympathetic nervous system; and a complex
been essential for recent therapeutic
pattern of neurohormonal changes.
advances in this area
Myocardial systolic dysfunction
The primary abnormality in nonvalvar heart failure is an
impairment in left ventricular function, leading to a fall in
cardiac output. The fall in cardiac output leads to activation of
Poor ventricular function/myocardial damage
several neurohormonal compensatory mechanisms aimed at
(eg post myocardial infarction, dilated cardiomyopathy)
improving the mechanical environment of the heart. Activation
of the sympathetic system, for example, tries to maintain cardiac
Heart failure
output with an increase in heart rate, increased myocardial
contractility, and peripheral vasoconstriction (increased
catecholamines). Activation of the reninangiotensin
Decreased stroke volume and cardiac output
aldosterone system (RAAS) also results in vasoconstriction
(angiotensin) and an increase in blood volume, with retention
of salt and water (aldosterone). Concentrations of vasopressin
Neurohormonal response
and natriuretic peptides increase. Furthermore, there may be
progressive cardiac dilatation or alterations in cardiac structure
Activation of sympathetic system
Renin angiotensin aldosterone system
(remodelling), or both.
• Vasoconstriction: increased sympathetic tone, angiotensin II, endothelins,
Neurohormonal activation
impaired nitric oxide release
• Sodium and fluid retention: increased vasopressin and aldosterone
Chronic heart failure is associated with neurohormonal
activation and alterations in autonomic control. Although these
Further stress on ventricular wall and dilatation (remodelling)
compensatory neurohormonal mechanisms provide valuable
leading to worsening of ventricular function
support for the heart in normal physiological circumstances,
they also have a fundamental role in the development and
Further heart failure
subsequent progression of chronic heart failure.
Reninangiotensinaldosterone system
Neurohormonal mechanisms and compensatory mechanisms in heart
failure
Stimulation of the reninangiotensinaldosterone system leads
to increased concentrations of renin, plasma angiotensin II, and
aldosterone. Angiotensin II is a potent vasoconstrictor of the
renal (efferent arterioles) and systemic circulation, where it
stimulates release of noradrenaline from sympathetic nerve
terminals, inhibits vagal tone, and promotes the release of
Liver
Vessels
Brain
aldosterone. This leads to the retention of sodium and water
and the increased excretion of potassium. In addition,
angiotensin II has important effects on cardiac myocytes and
Renin substrate (angiotensinogen)
may contribute to the endothelial dysfunction that is observed
in chronic heart failure.
Renin
(kidney)
Sympathetic nervous system
Angiotensin I
The sympathetic nervous system is activated in heart failure, via
Angiotensin converting enzyme
low and high pressure baroreceptors, as an early compensatory
(lungs and vasculature)
mechanism which provides inotropic support and maintains
Angiotensin II
cardiac output. Chronic sympathetic activation, however, has
deleterious effects, causing a further deterioration in cardiac
function.
Vasoconstriction
Aldosterone release
Enhanced sympathetic activity
The earliest increase in sympathetic activity is detected in
the heart, and this seems to precede the increase in sympathetic
outflow to skeletal muscle and the kidneys that is present in
advanced heart failure. Sustained sympathetic stimulation
Salt and water retention
activates the reninangiotensinaldosterone system and other
neurohormones, leading to increased venous and arterial tone
Reninangiotensinaldosterone axis in heart failure
9
(and greater preload and afterload respectively), increased
Myocardial damage
plasma noradrenaline concentrations, progressive retention of
salt and water, and oedema. Excessive sympathetic activity is
also associated with cardiac myocyte apoptosis, hypertrophy,
Activation of sympathetic nervous system
and focal myocardial necrosis.
In the long term, the ability of the myocardium to respond
to chronic high concentrations of catecholamines is attenuated
Renin-angiotensin
Vasoconstriction
Increased heart rate
Direct
by a down regulation in â receptors, although this may be
system
and contractility
cardiotoxicity
associated with baroreceptor dysfunction and a further increase
in sympathetic activity. Indeed, abnormalities of baroreceptor
Fluid retention
Increased wall stress
function are well documented in chronic heart failure, along
with reduced parasympathetic tone, leading to abnormal
autonomic modulation of the sinus node. Moreover, a reduction
Increased myocardial oxygen demand
in heart rate variability has consistently been observed in
chronic heart failure, as a result of predominantly sympathetic
Myocardial hypertrophy
Decreased contractility
Myocyte damage
and reduced vagal modulation of the sinus node, which may be
a prognostic marker in patients with chronic heart failure.
Sympathetic activation in chronic heart failure
Natriuretic peptides
Concentrations of plasma norepinephrine
There are three natriuretic peptides, of similar structure, and
100
these exert a wide range of effects on the heart, kidneys, and
>5.32 nmol/l
90
>3.55 nmol/l and <5.32 nmol/l
central nervous system.
80
<3.55 nmol/l
Atrial natriuretic peptide (ANP) is released from the atria in
70
response to stretch, leading to natriuresis and vasodilatation. In
60
humans, brain natriuretic peptide (BNP) is also released from
the heart, predominantly from the ventricles, and its actions are
50
similar to those of atrial natriuretic peptide. Ctype natriuretic
40
peptide is limited to the vascular endothelium and central
30
nervous system and has only limited effects on natriuresis and
2 year P<0.0001
20
Overall P<0.0001
vasodilatation.
10
The atrial and brain natriuretic peptides increase in
response to volume expansion and pressure overload of the
00
6
12
18
24
30
36
42
48
54
60
heart and act as physiological antagonists to the effects of
Months
angiotensin II on vascular tone, aldosterone secretion, and
renaltubule sodium reabsorption. As the natriuretic peptides
Norepinephrine concentrations and prognosis in chronic heart failure
are important mediators, with increased circulating
concentrations in patients with heart failure, interest has
Stretch or increase in cardiac
developed in both the diagnostic and prognostic potential of
chamber volume leads to release
these peptides. Substantial interest has been expressed about
of natriuretic peptides
the therapeutic potential of natriuretic peptides, particularly
Atrium
Atrium
with the development of agents that inhibit the enzyme that
metabolises atrial natriuretic peptide (neutral endopeptidase),
Ventricles
and nonpeptide agonists for the A and B receptors.
Atrial
N-terminal
natriuretic
atrial
peptide
natriuretic
Antidiuretic hormone (vasopressin)
Brain natriuretic
peptide
Antidiuretic hormone concentrations are also increased in
peptide
severe chronic heart failure. High concentrations of the
hormone are particularly common in patients receiving diuretic
treatment, and this may contribute to the development of
Vasodilatation
hyponatraemia.
Increased urinary sodium excretion
Effects of natriuretic peptides
Endothelins
Endothelin is secreted by vascular endothelial cells and is a
potent vasoconstrictor peptide that has pronounced
Other hormonal mechanisms in chronic heart failure
vasoconstrictor effects on the renal vasculature, promoting the
x The arachidonic acid cascade leads to increased concentrations of
retention of sodium. Importantly, the plasma concentration of
prostaglandins (prostaglandin E
2 and prostaglandin I2), which
protect the glomerular microcirculation during renal
endothelin1 is of prognostic significance and is increased in
vasoconstriction and maintain glomerular filtration by dilating
proportion to the symptomatic and haemodynamic severity of
afferent glomerular arterioles
heart failure. Endothelin concentration is also correlated with
x The kallikrein kinin system forms bradykinin, resulting in both
indices of severity such as the pulmonary artery capillary wedge
natriuresis and vasodilatation, and stimulates the production of
pressure, need for admission to hospital, and death.
prostaglandins
In view of the vasoconstrictor properties of endothelin,
x Circulating concentrations of the cytokine tumour necrosis factor
(áTNF) are increased in cachectic patients with chronic heart
interest has developed in endothelin receptor antagonists as
failure. áTNF has also been implicated in the development of
cardioprotective agents which inhibit endothelin mediated
endothelial abnormalities in patients with chronic heart failure
vascular and myocardial remodelling.
10
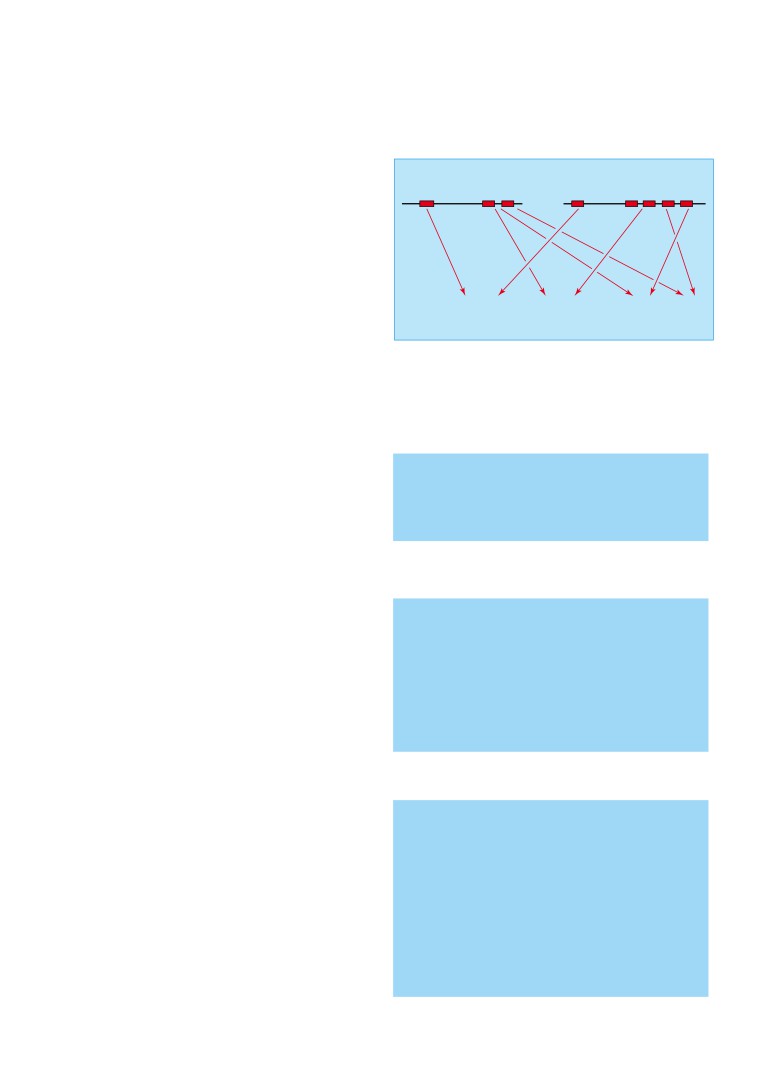
Patterns of neurohormonal activation
After myocardial infarction
and prognosis
x Plasma noradrenaline is of prognostic value in patients early after
myocardial infarction, predicting subsequent changes in left
Asymptomatic left ventricular dysfunction
ventricular volume
Plasma norepinephrine concentrations increase early in the
x Natriuretic peptides have also been shown to predict outcome after
development of left ventricular dysfunction, and plasma renin
myocardial infarction, although it is not clear whether the predictive
activity usually increases in patients receiving diuretic treatment.
value is additive to measurements of ventricular function
Norepinephrine concentration in asymptomatic left ventricular
dysfunction is a strong and independent predictor of the
development of symptomatic chronic heart failure and long
term mortality. Plasma concentrations of Nterminal proatrial
natriuretic peptide and brain natriuretic peptide also seem to be
Myocardial or
good indicators of asymptomatic left ventricular dysfunction
valvar damage
and may be useful in the future as an objective blood test in
Arrhythmias
these patients.
+
Ventricular
performance
Congestive heart failure
In severe untreated chronic heart failure, concentrations of
Cardiac
renin, angiotensin II, aldosterone, noradrenaline, and atrial
output
Left ventricular
natriuretic peptide are all increased. Plasma concentrations of
afterload
various neuroendocrine markers correlate with both the
severity of heart failure and the long term prognosis. For
Activation of
example, raised plasma concentrations of Nterminal and
neurohormonal
systems
Cterminal atrial natriuretic peptide and of brain natriuretic
Vascular
peptide are independent predictors of mortality in patients with
resistance plus
chronic heart failure. Patients with congestive heart failure and
sodium retention
-
Angiotensin converting
enzyme inhibitors
raised plasma noradrenaline concentrations also have a worse
prognosis.
Effect of angiotensin converting enzyme inhibitors in heart failure
Other noncardiac abnormalities in
chronic heart failure
Vasculature
The vascular endothelium has an important role in the
regulation of vascular tone, releasing relaxing and contracting
factors under basal conditions or during exercise. The increased
peripheral resistance in patients with chronic heart failure is
related to the alterations in autonomic control, including
heightened sympathetic tone, activation of the
reninangiotensinaldosterone system, increased endothelin
concentrations, and impaired release of endothelium derived
relaxing factor (or nitric oxide). There is emerging evidence that
impaired endothelial function in chronic heart failure may be
Contrast left ventriculogram in patient with poor systolic function (diastolic
(left) and systolic (right) views)
improved with exercise training and drug treatment, such as
angiotensin converting enzyme inhibitors.
Skeletal muscle changes
Considerable peripheral changes occur in the skeletal muscle of
patients with chronic heart failure. These include a reduction in
muscle mass and abnormalities in muscle structure,
metabolism, and function. There is also reduced blood flow to
active skeletal muscle, which is related to vasoconstriction and
the loss in muscle mass. All these abnormalities in skeletal
muscles, including respiratory muscles, contribute to the
symptoms of fatigue, lethargy, and exercise intolerance that
occur in chronic heart failure.
Diastolic dysfunction
Diastolic dysfunction results from impaired myocardial
relaxation, with increased stiffness in the ventricular wall and
reduced left ventricular compliance, leading to impairment of
diastolic ventricular filling. Infiltrations, such as amyloid heart
Two dimensional echocardiogram in patient with hypertrophic
disease, are the best examples, although coronary artery
cardiomyopathy showing asymmetrical septal hypertrophy
11
disease, hypertension (with left ventricular hypertrophy), and
hypertrophic cardiomyopathy are more common causes.
The incidence and contribution of diastolic dysfunction
remains controversial, although it has been estimated that
3040% of patients with heart failure have normal ventricular
systolic contraction. Indices of diastolic dysfunction can be
obtained noninvasively with Doppler echocardiography or
invasively with cardiac catheterisation and measurement of left
ventricular pressure changes. There is no agreement as to the
most accurate index of left ventricular diastolic dysfunction, but
the Doppler mitral inflow velocity profile is probably the most
Contrast left ventriculogram in patient with hypertrophic cardiomyopathy
widely used.
(diastolic (left) and systolic (right) views)
Although pure forms exist, in most patients with heart
failure both systolic and diastolic dysfunction can be present.
Knowing about diastolic dysfunction, however, has little effect
on management of most patients with chronic heart failure, as
there are still many uncertainties over its measurement and
optimal management strategies.
Acute myocardial
Myocardial remodelling, hibernation,
infarction
and stunning
After extensive myocardial infarction, cardiac contractility is
frequently impaired and neurohormonal activation leads to
regional eccentric and concentric hypertrophy of the
noninfarcted segment, with expansion (regional thinning and
Age
dilatation) of the infarct zone. This is known as remodelling.
Risk of heart failure and relation with age and history of myocardial
Particular risk factors for this development of progressive
infarction
ventricular dilatation after a myocardial infarction include a
large infarct, anterior infarctions, occlusion (or nonreperfusion)
of the artery related to the infarct, and hypertension.
Myocardial dysfunction may also occur in response to
“stunning” (postischaemic dysfunction), which describes delayed
Myocardial infarction
recovery of myocardial function despite restoration of coronary
blood flow, in the absence of irreversible damage. This is in
Reduced systolic function
contrast to “hibernating” myocardium, which describes
persistent myocardial dysfunction at rest, secondary to reduced
myocardial perfusion, although cardiac myocytes remain viable
Increased left ventricular end
Neurohormonal
and myocardial contraction may improve with revascularisation.
diastolic volume and pressure
activation
When stunning or hibernation occurs, viable myocardium
retains responsiveness to inotropic stimulation, which can then
be identified by resting and stress echocardiography, thallium
Increased wall stress
scintigraphy and positron emission tomography.
Revascularisation may improve the overall left ventricular
Non-infarcted segment:
Infarcted segment:
Increased cardiac
function with potential beneficial effects on symptoms and
regional hypertrophy
infarct expansion
output
prognosis.
Heart failure
Key references
x Grossman W. Diastolic dysfunction in congestive heart failure.
N Engl J Med 1991;325:155764.
Death
x Love MP, McMurray JJV. Endothelin in heart failure: a promising
therapeutic target. Heart 1997;77:934.
Process of ventricular remodelling
x McDonagh TA, Robb SD, Murdoch DR, Morton JJ, Ford I, Morrison
CE, et al. Biochemical detection of left ventricular systolic
dysfunction. Lancet 1998;351:913.
x Rahimtoola SH. The hibernating myocardium. Am Heart J
1989;117:21121.
G Jackson is consultant cardiologist in the department of cardiology,
x Wilkins MR, Redondo J, Brown LA. The natriureticpeptide family.
Guy’s and St Thomas’s Hospital, London.
Lancet 1997;349:130710.
The ABC of heart failure is edited by C R Gibbs, M K Davies, and
x Packer M. The neurohormonal hypothesis: a theory to explain the
G Y H Lip. CRG is research fellow and GYHL is consultant
mechanisms of disease progression in heart failure. J Am Coll
cardiologist and reader in medicine in the university department of
Cardiol 1992;20:24854.
medicine and the department of cardiology, City Hospital,
Birmingham; MKD is consultant cardiologist in the department of
cardiology, Selly Oak Hospital, Birmingham. The series will be
The graph showing mortality curves is adapted from Cohn et al (N Engl J
published as a book in the spring.
Med 1984;311:81923); the diagram of the process of ventricular
remodelling is adapted from McKay et al (Circulation 1986;74:693702).
BMJ 2000;320:16770
12
ABC of heart failure
Clinical features and complications
R D S Watson, C R Gibbs, G Y H Lip
Clinical features
Patients with heart failure present with a variety of symptoms,
Symptoms and signs in heart failure
most of which are nonspecific. The common symptoms of
congestive heart failure include fatigue, dyspnoea, swollen
Symptoms
ankles, and exercise intolerance, or symptoms that relate to the
Dyspnoea
Orthopnoea
underlying cause. The accuracy of diagnosis by presenting
Paroxysmal nocturnal dyspnoea
clinical features alone, however, is often inadequate, particularly
Reduced exercise tolerance, lethargy, fatigue
in women and elderly or obese patients.
Nocturnal cough
Wheeze
Symptoms
Ankle swelling
Dyspnoea
Anorexia
Exertional breathlessness is a frequent presenting symptom in
Signs
heart failure, although it is a common symptom in the general
Cachexia and muscle wasting
Tachycardia
population, particularly in patients with pulmonary disease.
Pulsus alternans
Dyspnoea is therefore moderately sensitive, but poorly specific,
Elevated jugular venous pressure
for the presence of heart failure. Orthopnoea is a more specific
Displaced apex beat
symptom, although it has a low sensitivity and therefore has
Right ventricular heave
little predictive value. Paroxysmal nocturnal dyspnoea results
Crepitations or wheeze
from increased left ventricular filling pressures (due to
Third heart sound
Oedema
nocturnal fluid redistribution and enhanced renal reabsorption)
Hepatomegaly (tender)
and therefore has a greater sensitivity and predictive value.
Ascites
Nocturnal ischaemic chest pain may also be a manifestation of
heart failure, so left ventricular systolic dysfunction should be
excluded in patients with recurrent nocturnal angina.
Fatigue and lethargy
Common causes of lower limb oedema
Fatigue and lethargy in chronic heart failure are, in part, related
x Gravitational disorder—for example, immobility
to abnormalities in skeletal muscle, with premature muscle
x Congestive heart failure
lactate release, impaired muscle blood flow, deficient endothelial
x Venous thrombosis or obstruction, varicose veins
x Hypoproteinaemia—for example, nephrotic syndrome, liver disease
function, and abnormalities in skeletal muscle structure and
x Lymphatic obstruction
function. Reduced cerebral blood flow, when accompanied by
abnormal sleep patterns, may occasionally lead to somnolence
and confusion in severe chronic heart failure.
Oedema
Sensitivity, specificity, and predictive value of symptoms,
Swelling of ankles and feet is another common presenting
signs, and chest x ray findings for presence of heart failure
feature, although there are numerous noncardiac causes of this
(ejection fraction <40%) in 1306 patients with coronary
symptom. Right heart failure may manifest as oedema, right
artery disease undergoing cardiac catheterisation
hypochondrial pain (liver distension), abdominal swelling
Positive
(ascites), loss of appetite, and, rarely, malabsorption (bowel
Sensitivity
Specificity
predictive
oedema). An increase in weight may be associated with fluid
Clinical features
(%)
(%)
value (%)
retention, although cardiac cachexia and weight loss are
History:
important markers of disease severity in some patients.
Shortness of breath
66
52
23
Orthopnoea
21
81
2
Physical signs
Physical examination has serious limitations as many patients,
Paroxysmal nocturnal
dyspnoea
33
76
26
particularly those with less severe heart failure, have few
History of oedema
23
80
22
abnormal signs. In addition, some physical signs are difficult to
Examination:
interpret and, if present, may occasionally be related to causes
Tachycardia ( > 100
other than heart failure.
beats/min)
7
99
6
Oedema and a tachycardia, for example, are too insensitive
Crepitations
13
91
27
to have any useful predictive value, and although pulmonary
Oedema (on
crepitations may have a high diagnostic specificity they have a
examination)
10
93
3
low sensitivity and predictive value. Indeed, the commonest
Gallop (S3)
31
95
61
cause of lower limb oedema in elderly people is immobility, and
Neck vein distension
10
97
2
pulmonary crepitations may reflect poor ventilation with
Chest x ray examination:
infection, or pulmonary fibrosis, rather than heart failure.
Cardiomegaly
62
67
32
Jugular venous distension has a high specificity in diagnosing
13
heart failure in patients who are known to have cardiac disease,
although some patients, even with documented heart failure, do
not have an elevated venous pressure. The presence of a
displaced apex beat in a patient with a history of myocardial
infarction has a high positive predictive value. A third heart
sound has a relatively high specificity, although its universal
value is limited by a high interobserver variability, with
interobserver agreement of less than 50% in nonspecialists.
In patients with preexisting chronic heart failure, other
clinical features may be evident that point towards precipitating
causes of acute heart failure or deteriorating heart failure.
Common factors that may be obvious on clinical assessment
and are associated with relapses in congestive heart failure
include infections, arrhythmias, continued or recurrent
myocardial ischaemia, and anaemia.
Clinical diagnosis and clinical scoring systems
Gross oedema of ankles,
Several epidemiological studies, including the Framingham
including bullae with serous
heart study, have used clinical scoring systems to define heart
exudate
failure, although the use of these systems is not recommended
for routine clinical practice.
In a patient with appropriate symptoms and a number of
physical signs, including a displaced apex beat, elevated venous
Precipitating causes of heart failure
pressure, oedema, and a third heart sound, the clinical diagnosis
of heart failure may be made with some confidence. However,
x Arrhythmias, especially atrial fibrillation
x Infections (especially pneumonia)
the clinical suspicion of heart failure should also be confirmed
x Acute myocardial infarction
with objective investigations and the demonstration of cardiac
x Angina pectoris or recurrent myocardial ischaemia
dysfunction at rest. It is important to note that, in some patients,
x Anaemia
exerciseinduced myocardial ischaemia may lead to a rise in
x Alcohol excess
ventricular filling pressures and a fall in cardiac output, leading
x Iatrogenic cause—for example, postoperative fluid replacement or
to symptoms of heart failure during exertion.
administration of steroids or nonsteroidal antiinflammatory drugs
x Poor drug compliance, especially in antihypertensive treatment
x Thyroid disorders—for example, thyrotoxicosis
Classification
x Pulmonary embolism
x Pregnancy
Symptoms and exercise capacity are used to classify the severity
of heart failure and monitor the response to treatment. The
classification of the New York Heart Association (NYHA) is
used widely, although outcome in heart failure is best
European Society of Cardiology’s guidelines for diagnosis of
determined not only by symptoms (NYHA class) but also by
heart failure
echocardiographic criteria. As the disease is progressive, the
Essential features
importance of early treatment, in an attempt to prevent
Symptoms of heart failure (for example, breathlessness, fatigue, ankle
progression to more severe disease, cannot be overemphasised.
swelling)
and
Objective evidence of cardiac dysfunction (at rest)
Complications
Nonessential features
Response to treatment directed towards heart failure (in cases where
Arrhythmias
the diagnosis is in doubt)
Atrial fibrillation
Atrial fibrillation is present in about a third (range 1050%) of
patients with chronic heart failure and may represent either a
cause or a consequence of heart failure. The onset of atrial
fibrillation with a rapid ventricular response may precipitate
NYHA classification of heart failure
overt heart failure, particularly in patients with preexisting
Class I: asymptomatic
ventricular dysfunction. Predisposing causes should be
No limitation in physical activity despite presence of heart disease.
considered, including mitral valve disease, thyrotoxicosis, and
This can be suspected only if there is a history of heart disease which
sinus node disease. Importantly, sinus node disease may be
is confirmed by investigations—for example, echocardiography
associated with bradycardias, which might be exacerbated by
Class II: mild
antiarrhythmic treatment.
Slight limitation in physical activity. More strenuous activity causes
shortness of breath—for example, walking on steep inclines and
Atrial fibrillation that occurs with severe left ventricular
several flights of steps. Patients in this group can continue to have an
dysfunction following myocardial infarction is associated with a
almost normal lifestyle and employment
poor prognosis. In addition, patients with heart failure and
Class III: moderate
atrial fibrillation are at particularly high risk of stroke and other
More marked limitation of activity which interferes with work. Walking
thromboembolic complications.
on the flat produces symptoms
Class IV: severe
Ventricular arrhythmias
Unable to carry out any physical activity without symptoms. Patients
Malignant ventricular arrhythmias are common in end stage
are breathless at rest and mostly housebound
heart failure. For example, sustained monomorphic ventricular
14
tachycardia occurs in up to 10% of patients with advanced heart
Predisposing factors for ventricular arrhythmias
failure who are referred for cardiac transplantation. In patients
x Recurrent or continued coronary ischaemia
with ischaemic heart disease these arrhythmias often have
x Recurrent myocardial infarction
reentrant mechanisms in scarred myocardial tissue. An episode
x Hypokalaemia and hyperkalaemia
of sustained ventricular tachycardia indicates a high risk for
x Hypomagnesaemia
recurrent ventricular arrhythmias and sudden cardiac death.
x Psychotropic drugs—for example, tricyclic antidepressants
Sustained polymorphic ventricular tachycardia and torsades
x Digoxin (leading to toxicity)
de pointes are more likely to occur in the presence of
x Antiarrhythmic drugs that may be cardiodepressant (negative
inotropism) and proarrhythmic
precipitating or aggravating factors, including electrolyte
disturbance (for example, hypokalaemia or hyperkalaemia,
hypomagnesaemia), prolonged QT interval, digoxin toxicity,
drugs causing electrical instability (for example, antiarrhythmic
drugs, antidepressants), and continued or recurrent myocardial
ischaemia. â Blockers are useful for treating arrhythmias, and
these agents (for example, bisoprolol, metoprolol, carvedilol)
are likely to be increasingly used as a treatment option in
patients with heart failure.
Stroke and thromboembolism
Congestive heart failure predisposes to stroke and
thromboembolism, with an overall estimated annual incidence
of approximately 2%. Factors contributing to the increased
thromboembolic risk in patients with heart failure include low
cardiac output (with relative stasis of blood in dilated cardiac
chambers), regional wall motion abnormalities (including
formation of a left ventricular aneurysm), and associated atrial
fibrillation. Although the prevalence of atrial fibrillation in some
of the earlier observational studies was between 12% and
36%—which may have accounted for some of the
thromboembolic events—patients with chronic heart failure
who remain in sinus rhythm are also at an increased risk of
stroke and venous thromboembolism. Patients with heart failure
and chronic venous insufficiency may also be immobile, and this
contributes to their increased risk of thrombosis, including deep
venous thrombosis and pulmonary embolism.
24 Hour Holter tracing showing frequent ventricular extrasystoles
Recent observational data from the studies of left ventricular
dysfunction (SOLVD) and vasodilator heart failure trials
(VHeFT) indicate that mild to moderate heart failure is
associated with an annual risk of stroke of about 1.5%
(compared with a risk of less than 0.5% in those without heart
failure), rising to 4% in patients with severe heart failure. In
addition, the survival and ventricular enlargement (SAVE) study
Complications of heart failure
recently reported an inverse relation between risk of stroke and
Arrhythmias—Atrial fibrillation; ventricular arrhythmias (ventricular
left ventricular ejection fraction, with an 18% increase in risk for
tachycardia, ventricular fibrillation); bradyarrhythmias
every 5% reduction in left ventricular ejection fraction; this
Thromboembolism—Stroke; peripheral embolism; deep venous
thrombosis; pulmonary embolism
clearly relates thromboembolism to severe cardiac impairment
Gastrointestinal—Hepatic congestion and hepatic dysfunction;
and the severity of heart failure. As thromboembolic risk seems
malabsorption
to be related to left atrial and left ventricular dilatation,
Musculoskeletal—Muscle wasting
echocardiography may have some role in the risk stratification
Respiratory—Pulmonary congestion; respiratory muscle weakness;
of thromboembolism in patients with chronic heart failure.
pulmonary hypertension (rare)
Prognosis
Most long term (more than 10 years of follow up) longitudinal
studies of heart failure, including the Framingham heart study
(1971), were performed before the widespread use of
angiotensin converting enzyme inhibitors. In the Framingham
Morbidity and mortality for all grades of
study the overall survival at eight years for all NYHA classes was
symptomatic chronic heart failure are
high, with a 2030% one year mortality in
30%, compared with a one year mortality in classes III and IV of
mild to moderate heart failure and a
34% and a one year mortality in class IV of over 60%. The
greater than 50% one year mortality in
prognosis in patients whose left ventricular dysfunction is
severe heart failure. These prognostic
asymptomatic is better than that in those whose left ventricular
data refer to patients with systolic heart
dysfunction is symptomatic. The prognosis in patients with
failure, as the natural course of diastolic
congestive heart failure is dependent on severity, age, and sex,
dysfunction is less well defined
with a poorer prognosis in male patients. In addition, numerous
prognostic indices are associated with an adverse prognosis,
15
including NYHA class, left ventricular ejection fraction, and
neurohormonal status.
Some predictors of poor outcome in chronic heart failure
Survival can be prolonged in chronic heart failure that
x High NYHA functional class
results from systolic dysfunction if angiotensin converting
x Reduced left ventricular ejection fraction
enzyme inhibitors are given. Longitudinal data from the
x Low peak oxygen consumption with maximal exercise (% predicted
Framingham study and the Mayo Clinic suggest, however, that
value)
x Third heart sound
there is still only a limited improvement in the one year survival
x Increased pulmonary artery capillary wedge pressure
rate of patients with newly diagnosed symptomatic chronic
x Reduced cardiac index
heart failure, which remains at 6070%. In these studies only a
x Diabetes mellitus
minority of patients with congestive heart failure were
x Reduced sodium concentration
appropriately treated, with less than 25% of them receiving
x Raised plasma catecholamine and natriuretic peptide
angiotensin converting enzyme inhibitors, and even among
concentrations
treated patients the dose used was much lower than doses used
in the clinical trials.
Cardiac mortality in placebo controlled heart failure trials
Cardiovascular mortality
Ischaemic
Patients’
heart
Treatment
Placebo
Follow up
Trial
characteristics
disease (%)
Treatment
(%)
(%)
(years)
CONSENSUS
NYHA IV (cardiomegaly)
73
Enalapril
38
54
1
SOLVDP
Asymptomatic (EF < 35%)
83
Enalapril
13
14
4
SOLVDT
Symptomatic (EF < 35%)
71
Enalapril
31
36
4
SAVE
Postmyocardial infarction (EF < 40%)
100
Captopril
17
21
4
VHeFT I
NYHA IIIII (EF < 45%)
44
HISDN
37
41
5
VHeFT II
NYHA IIIII (EF < 45%)
52
Enalapril
28
34*
5
PRAISE
NYHA IIIIV (EF < 30%)
63
Amlodipine
28
33
1.2
EF ejection fraction. SOLVDP, SOLVDT = studies of left ventricular dysfunction prevention arm (P) and treatment arm (T).
HISDN = hydralazine and isosorbide dinitrate.
*Treatment with HISDN.
Treatment with angiotensin converting enzyme inhibitors
Key references
prevents or delays the onset of symptomatic heart failure in
patients with asymptomatic, or minimally symptomatic, left
x Doval HC, Nul DR, Grancelli HO, Perrone SV, Bortman GR,
Curiel R, et al. Randomised trial of lowdose amiodarone in severe
ventricular systolic dysfunction. The increase in mortality with
congestive heart failure. Lancet 1994;334:4938.
the development of symptoms suggests that the optimal time
x Gradman A, Deedwania P, Cody R, Massie B, Packer M, Pitt B, et al.
for intervention with these agents is well before the onset of
Predictors of total mortality and sudden death in mild to moderate
substantial left ventricular dysfunction, even in the absence of
heart failure. J Am Coll Cardiol 1989;14:56470.
overt clinical symptoms of heart failure. This benefit has been
x Guidelines for the diagnosis of heart failure. The Task Force on
confirmed in several large, well conducted, postmyocardial
Heart Failure of the European Society of Cardiology. Eur Heart J
infarction studies.
1995;16:74151.
x Rodeheffer RJ, Jacobsen SJ, Gersh BJ, Kottke TE, McCann HA,
Sudden death
Bailey KR, et al. The incidence and prevalence of congestive heart
The mode of death in heart failure has been extensively
failure in Rochester, Minnesota. Mayo Clin Proc 1993;68:114350.
x The SOLVD Investigators. Effect of enalapril on mortality and the
investigated, and progressive heart failure and sudden death
development of heart failure in asymptomatic patients with reduced
seem to occur with equal frequency. Some outstanding
left ventricular ejection fractions. N Engl J Med 1992;327:68591.
questions still remain, however. Although arrhythmias are
x The CONSENSUS Trial Study Group. Effects of enalapril on
common in patients with heart failure and are indicators of
mortality in severe congestive heart failure: results of the
disease severity, they are not powerful independent predictors
cooperative north Scandinavian enalapril survival study
of prognosis. Sudden death may be related to ventricular
(CONSENSUS). N Engl J Med 1987;316:142935.
arrhythmias, although asystole is a common terminal event in
severe heart failure. It has not been firmly established whether
these arrhythmias are primary arrhythmias or whether some
are secondary to acute coronary ischaemia or indicate in situ
coronary thrombosis. The cause of death is often uncertain,
The table on the sensitivity, specificity, and predictive value of symptoms,
especially as the patient may die of a cardiac arrest outside
signs, and chest x ray findings is adapted with permission from Harlan et al
(Ann Intern Med 1977;86:1338).
hospital or while asleep.
The ABC of heart failure is edited by C R Gibbs, M K Davies, and
G Y H Lip. CRG is research fellow and GYHL is consultant
R D S Watson is consultant cardiologist in the university department
cardiologist and reader in medicine in the university department of
of medicine and the department of cardiology, City Hospital,
medicine and the department of cardiology, City Hospital,
Birmingham.
Birmingham; MKD is consultant cardiologist in the department of
cardiology, Selly Oak Hospital, Birmingham. The series will be
BMJ 2000;320:2369
published as a book in the spring.
16
ABC of heart failure
Investigation
M K Davies, C R Gibbs, G Y H Lip
Clinical assessment is mandatory before detailed investigations
Investigations if heart failure is suspected
are conducted in patients with suspected heart failure, although
Initial investigations
specific clinical features are often absent and the condition can
x Chest radiography
be diagnosed accurately only in conjunction with more
x Electrocardiography
objective investigation, particularly echocardiography. Although
x Echocardiography, including Doppler studies
open access echocardiography is now increasingly available,
x Haematology tests
appropriate prereferral investigations include chest
x Serum biochemistry, including renal function and glucose
radiography, 12 lead electrocardiography, and renal chemistry.
concentrations, liver function tests, and thyroid function tests
x Cardiac enzymes (if recent infarction is suspected)
Other investigations
Chest x ray examination
x Radionuclide imaging
x Cardiopulmonary exercise testing
The chest x ray examination has an important role in the
x Cardiac catheterisation
routine investigation of patients with suspected heart failure,
x Myocardial biopsy—for example, in suspected myocarditis
and it may also be useful in monitoring the response to
treatment. Cardiac enlargement (cardiothoracic ratio > 50%)
may be present, but there is a poor correlation between the
cardiothoracic ratio and left ventricular function. The presence
of cardiomegaly is dependent on both the severity of
haemodynamic disturbance and its duration: cardiomegaly is
frequently absent, for example, in acute left ventricular failure
secondary to acute myocardial infarction, acute valvar
regurgitation, or an acquired ventricular septal defect. An
increased cardiothoracic ratio may be related to left or right
ventricular dilatation, left ventricular hypertrophy, and
occasionally a pericardial effusion, particularly if the cardiac
silhouette has a globular appearance. Echocardiography is
required to distinguish reliably between these different causes,
although in decompensated heart failure other radiographic
features may be present, such as pulmonary congestion or
pulmonary oedema.
In left sided failure, pulmonary venous congestion occurs,
initially in the upper zones (referred to as upper lobe diversion
or congestion). When the pulmonary venous pressure increases
further, usually above 20 mm Hg, fluid may be present in the
horizontal fissure and Kerley B lines in the costophrenic angles.
In the presence of pulmonary venous pressures above 25 mm
Hg, frank pulmonary oedema occurs, with a “bats wing”
appearance in the lungs, although this is also dependent on the
rate at which the pulmonary oedema has developed. In
addition, pleural effusions occur, normally bilaterally, but if they
are unilateral the right side is more commonly affected.
Nevertheless, it is not possible to distinguish, when viewed in
isolation, whether pulmonary congestion is related to cardiac or
noncardiac causes (for example, renal disease, drugs, the
respiratory distress syndrome).
Rarely, chest radiography may also show valvar calcification,
a left ventricular aneurysm, and the typical pericardial
calcification of constrictive pericarditis. Chest radiography may
also provide valuable information about noncardiac causes of
dyspnoea.
12 lead electrocardiography
The 12 lead electrocardiographic tracing is abnormal in most
patients with heart failure, although it can be normal in up to
Chest radiographs showing gross cardiomegaly in patient
10% of cases. Common abnormalities include Q waves,
with dilated cardiomyopathy (top); cardiomegaly and
abnormalities in the T wave and ST segment, left ventricular
pulmonary congestion with fluid in horizontal fissure
hypertrophy, bundle branch block, and atrial fibrillation. It is a
(bottom)
17
useful screening test as a normal electrocardiographic tracing
Value of electrocardiography* in identifying heart failure
makes it unlikely that the patient has heart failure secondary to
resulting from left ventricular systolic dysfunction
left ventricular systolic dysfunction, since this test has high
sensitivity and a negative predictive value. The combination of a
Sensitivity
94%
normal chest x ray finding and a normal electrocardiographic
Specificity
61%
tracing makes a cardiac cause of dyspnoea very unlikely.
Positive predictive value
35%
In patients with symptoms (palpitations or dizziness), 24 hour
Negative predictive value
98%
electrocardiographic (Holter) monitoring or a Cardiomemo
*Electrocardiographic abnormalities are defined as atrial fibrillation, evidence of
device will detect paroxysmal arrhythmias or other abnormalities,
previous myocardial infarction, left ventricular hypertrophy, bundle branch
block, and left axis deviation.
such as ventricular extrasystoles, sustained or nonsustained
ventricular tachycardia, and abnormal atrial rhythms
(extrasystoles, supraventricular tachycardia, and paroxysmal atrial
fibrillation). Many patients with heart failure, however, show
complex ventricular extrasystoles on 24 hour monitoring.
I
aVR
V1
V4
Echocardiography
Echocardiography is the single most useful noninvasive test in
II
aVL
V2
V5
the assessment of left ventricular function; ideally it should be
conducted in all patients with suspected heart failure. Although
III
aVF
V3
V6
clinical assessment, when combined with a chest x ray
examination and electrocardiography, allows a preliminary
diagnosis of heart failure, echocardiography provides an
II
objective assessment of cardiac structure and function. Left
ventricular dilatation and impairment of contraction is
observed in patients with systolic dysfunction related to
ischaemic heart disease (where a regional wall motion
abnormality may be detected) or in dilated cardiomyopathy
(with global impairment of systolic contraction).
I
aVR
V1
V4
A quantitative measurement can be obtained from
calculation of the left ventricular ejection fraction. This is the
stroke volume (the difference between the end diastolic and end
II
aVL
V2
V5
systolic volumes) expressed as a percentage of the left
ventricular end diastolic volume. Measurements, and the
assessment of left ventricular function, are less reliable in the
III
aVF
V3
V6
presence of atrial fibrillation. The left ventricular ejection
fraction has been correlated with outcome and survival in
patients with heart failure, although the assessment may be
II
unreliable in patients with regional abnormalities in wall
motion. Regional abnormalities can also be quantified into a
wall motion index, although in practice the assessment of
systolic function is often based on visual assessment and the
observer’s experience of normal and abnormal contractile
Electrocardiograms showing previous anterior myocardial infarction with Q
waves in anteroseptal leads (top) and left bundle branch block (bottom)
function. These abnormalities are described as hypokinetic
(reduced systolic contraction), akinetic (no systolic contraction)
and dyskinetic (abnormalities of direction or timing of
contraction, or both), and refer to universally recognised
Who should have an echocardiogram?
segments of the left ventricle. Echocardiography may also show
x Almost all patients with symptoms or signs of heart failure
other abnormalities, including valvar disease, left ventricular
x Symptoms of breathlessness in association with signs of a murmur
aneurysm, intracardiac thrombus, and pericardial disease.
x Dyspnoea associated with atrial fibrillation
Mitral incompetence is commonly identified on
x Patients at “high risk” for left ventricular dysfunction—for example,
echocardiography in patients with heart failure, as a result of
those with anterior myocardial infarction, poorly controlled
ventricular and annular dilatation (“functional” mitral
hypertension, or arrhythmias
incompetence), and this must be distinguished from mitral
incompetence related to primary valve disease. Two
dimensional echocardiography allows the assessment of valve
structure and identifies thickening of cusps, leaflet prolapse,
cusp fusion, and calcification. Doppler echocardiography allows
Echocardiography as a guide to management
the quantitative assessment of flow across valves and the
x Identification of impaired systolic function for decision on
identification of valve stenosis, in addition to the assessment of
treatment with angiotensin converting enzyme inhibitors
right ventricular systolic pressures and allowing the indirect
x Identification of diastolic dysfunction or predominantly right
diagnosis of pulmonary hypertension. Doppler studies have
ventricular dysfunction
x Identification and assessment of valvar disease
been used in the assessment of diastolic function, although
x Assessment of embolic risk (severe left ventricular impairment with
there is no single reliable echocardiographic measure of
mural thrombus)
diastolic dysfunction. Colour flow Doppler techniques are
18
particularly sensitive in detecting the direction of blood flow
and the presence of valve incompetence.
Advances in echocardiography include the use of contrast
agents for visualisation of the walls of the left ventricle in more
detail, especially as in about 10% of patients satisfactory images
cannot be obtained with standard transthoracic
echocardiography. Transoesophageal echocardiography allows
the detailed assessment of the atria, valves, pulmonary veins,
and any cardiac masses, including thrombi.
The logistic and health economic aspects of large scale
screening with echocardiography have been debated, but the
development of open access echocardiography heart failure
services for general practitioners and the availability of proved
treatments for heart failure that improve prognosis, such as
angiotensin converting enzyme inhibitors, highlight the
importance of an agreed strategy for the echocardiographic
assessment of these patients.
Haematology and biochemistry
Routine haematology and biochemistry investigations are
recommended to exclude anaemia as a cause of breathlessness
and high output heart failure and to exclude important
preexisting metabolic abnormalities. In mild and moderate
heart failure, renal function and electrolytes are usually normal.
In severe (New York Heart Association, class IV) heart failure,
however, as a result of reduced renal perfusion, high dose
Transthoracic echocardiograms: two dimensional apical view (top) and
diuretics, sodium restriction, and activation of the
Doppler studies (bottom) showing severe calcific stenosis, with an estimated
neurohormonal mechanisms (including vasopressin), there is an
aortic gradient of over 70 mm Hg (A=left ventricle, B=aortic valve, and
inability to excrete water, and dilutional hyponatraemia may be
C=left atrium)
present. Hyponatraemia is, therefore, a marker of the severity of
chronic heart failure.
Natriuretic peptides
A baseline assessment of renal function is important before
x Biochemical markers are being sought for the diagnosis of
starting treatment, as the renal blood flow and the glomerular
congestive heart failure
filtration rate fall in severe congestive heart failure. Baseline
x Brain natriuretic peptide concentrations correlate with the severity
serum creatinine concentrations are important: increasing
of heart failure and prognosis
creatinine concentrations may occur after the start of treatment,
x These could, in the future, be used to distinguish between patients
particularly in patients who are receiving angiotensin
in whom heart failure is extremely unlikely and those in whom the
converting enzyme inhibitors and high doses of diuretics and in
probability of heart failure is high
x At present, however, the evidence that blood natriuretic peptide
patients with renal artery stenosis. Proteinuria is a common
concentrations are valuable in identifying important left ventricular
finding in severe congestive heart failure.
systolic dysfunction is conflicting, and their use in routine practice is
Hypokalaemia occurs when high dose diuretics are used
still limited
without potassium supplementation or potassium sparing
x Further studies are necessary to determine the most convenient
agents. Hyperkalaemia can also occur in severe congestive heart
and cost effective methods of identifying patients with heart failure
failure with a low glomerular filtration rate, particularly with the
and asymptomatic left ventricular dysfunction
concurrent use of angiotensin converting enzyme inhibitors
and potassium sparing diuretics. Both hypokalaemia and
hyperkalaemia increase the risk of cardiac arrhythmias;
hypomagnesaemia, which is associated with long term diuretic
treatment, increases the risk of ventricular arrhythmias. Liver
function tests (serum bilirubin, aspartate aminotransferase, and
lactate dehydrogenase) are often abnormal in advanced
congestive heart failure, as a result of hepatic congestion.
Thyroid function tests are also recommended in all patients, in
view of the association between thyroid disease and the heart.
Radionuclide methods
Radionuclide imaging—or multigated ventriculography—allows
the assessment of the global left and right ventricular function.
Images may be obtained in patients where echocardiography is
not possible. The most common method labels red cells with
technetium99m and acquires 16 or 32 frames per heart beat by
Multigated ventriculography scan in patient with
synchronising (“gating”) imaging with electrocardiography. This
history of extensive myocardial infarction and
allows the assessment of ejection fraction, systolic filling rate,
coronary bypass grafting (left ventricular ejection
fraction of 30%)
diastolic emptying rate, and wall motion abnormalities. These
19
variables can be assessed, if necessary, during rest and exercise;
Stress studies use graded physical
this method is ideal for the serial reassessment of ejection
exercise or pharmacological stress with
fraction, but these methods do expose the patient to radiation.
agents such as adenosine, dipyridamole,
Radionuclide studies are also valuable for assessing
and dobutamine. Stress echocardiography
myocardial perfusion and the presence or extent of coronary
is emerging as a useful technique for
ischaemia, including myocardial stunning and hibernating
assessing myocardial reversibility in
myocardium.
patients with coronary artery disease
Angiography, cardiac catheterisation,
Coronary angiography is essential for
and myocardial biopsy
accurate assessment of the coronary
arteries
Angiography should be considered in patients with recurrent
ischaemic chest pain associated with heart failure and in those
with evidence of severe reversible ischaemia or hibernating
myocardium. Cardiac catheterisation with myocardial biopsy
Cardiopulmonary exercise testing
can be valuable in more difficult cases where there is diagnostic
x Exercise tolerance is reduced in patients with heart failure,
doubt—for example, in restrictive and infiltrating
regardless of method of assessment
cardiomyopathies (amyloid heart disease, sarcoidosis),
x Assessment methods include a treadmill test, cycle ergometry, a 6
myocarditis, and pericardial disease. Left ventricular
minute walking test, or pedometry measurements
angiography can show global or segmental impairment of
x Exercise testing is not routinely performed for all patients with
function and assess end diastolic pressures, and right heart
congestive heart failure, but it may be valuable in identifying
catheterisation allows an assessment of the right sided pressures
substantial residual ischaemia, thus leading to more detailed
(right atrium, right ventricle, and pulmonary arteries) and
investigation
x Respiratory physiological measurements may be made during
pulmonary artery capillary wedge pressure, in addition to
exercise, and most cardiac transplant centres use data obtained at
oxygen saturations.
cardiopulmonary exercise testing to aid the selection of patients for
transplantation
x The maximum oxygen consumption is the value at which
Pulmonary function tests
consumption remains stable despite increasing exercise, and it
represents the upper limit of aerobic exercise tolerance
Objective measurement of lung function is useful in excluding
x The maximum oxygen consumption and the carbon dioxide
respiratory causes of breathlessness, although respiratory and
production correlate well with the severity of heart failure
cardiac disease commonly coexist. Peak expiratory flow rate and
x The maximum oxygen consumption has also been independently
forced expiratory volume in one second are reduced in heart
related to long term prognosis, especially in patients with severe left
failure, although not as much as in severe chronic obstructive
ventricular dysfunction
pulmonary disease. In patients with severe breathlessness and
wheeze, a peak expiratory flow rate of < 200 l/min suggests
reversible airways disease, not acute left ventricular failure.
Further reading
x Cheeseman MG, Leech G, Chambers J,
Monaghan MJ, Nihoyannopoulos P. Central
role of echocardiography in the diagnosis
Assessments for the investigation and diagnosis of heart failure
and assessment of heart failure. Heart
1998;80(suppl 1):S15.
Diagnosis of heart failure
Suggests
x Dargie HJ, McMurray JVV. Diagnosis and
alternative or
management of heart failure. BMJ
Assessments
Necessary
Supports
Opposes additional disease
1994;308:3218.
Symptoms of heart
+ +
+ +
x Schiller NB, Foster E. Analysis of left
failure
(if absent)
ventricular systolic function. Heart
1996;75(suppl 2):1726.
Signs of heart failure
+ +
+
(if absent)
Response to treatment
+ +
+ +
(if absent)
Electrocardiography
+ +
The table showing the value of electrocardiography is
(if normal)
adapted from Davie et al (BMJ 1996;312:222). The
Chest radiography
+ +
+
Pulmonary
table of assessments for the investigation and
(cardiomegaly or
(if normal)
diagnosis of heart failure is adapted with permission
congestion)
from the Task Force on Heart Failure of the European
Society of Cardiology (Eur Heart J 1995;16:74151).
Echocardiography
++
+ +
(cardiac dysfunction)
(if absent)
The ABC of heart failure is edited by C R Gibbs,
Haematology
Anaemia
M K Davies, and G Y H Lip. CRG is research
fellow and GYHL is consultant cardiologist and
Biochemistry (renal,
Renal, liver,
reader in medicine in the university department of
liver function, and
thyroid
medicine and the department of cardiology, City
thyroid function tests)
Hospital, Birmingham; MKD is consultant
Urine analysis
Renal
cardiologist in the department of cardiology, Selly
Pulmonary function
Pulmonary
Oak Hospital, Birmingham. The series will be
tests
published as a book in the spring.
+ + = Great importance; + = some importance.
BMJ 2000;320:297300
20
ABC of heart failure
Nondrug management
C R Gibbs, G Jackson, G Y H Lip
Approaches to the management of heart failure can be both
Nonpharmacological measures for the management of heart
nonpharmacological and pharmacological; each approach
failure
complements the other. This article will discuss
x Compliance—give careful advice about disease, treatment, and self
nonpharmacological management.
help strategies
x Diet—ensure adequate general nutrition and, in obese patients,
weight reduction
Counselling and education of patients
advise patients to avoid high salt content foods and not to add
x Salt—
salt (particularly in severe cases of congestive heart failure)
Effective counselling and education of patients, and of the
x Fluid—urge overloaded patients and those with severe congestive
relatives or carers, is important and may enhance long term
heart failure to restrict their fluid intake
adherence to management strategies. Simple explanations
x Alcohol—advise moderate alcohol consumption (abstinence in
about the symptoms and signs of heart failure, including details
alcohol related cardiomyopathy)
on drug and other treatment strategies, are valuable. Emphasis
x Smoking—avoid smoking (adverse effects on coronary disease,
should be placed on self help strategies for each patient; these
adverse haemodynamic effects)
x Exercise—regular exercise should be encouraged
should include information on the need to adhere to drug
x Vaccination—patients should consider influenza and pneumococcal
treatment. Some patients can be instructed how to monitor
vaccinations
their weight at home on a daily basis and how to adjust the dose
of diuretics as advised; sudden weight increases ( > 2 kg in 13
days), for example, should alert a patient to alter his or her
treatment or seek advice.
Lifestyle measures
Urging patients to alter their lifestyle is important in the
management of chronic heart failure. Social activities should be
Self management
Daily weighing
of diuretics
encouraged, however, and care should be taken to ensure that
patients avoid social isolation. If possible, patients should
continue their regular work, with adaptations to accommodate a
Self help strategies
reduced physical capacity where appropriate.
Compliance with
Regular
Contraceptive advice
medication
exercise
Advice on contraception should be offered to women of
childbearing potential, particularly those patients with advanced
heart failure (class IIIIV in the New York Heart Association’s
Self help strategies for patients with heart failure
classification), in whom the risk of maternal morbidity and
mortality is high with pregnancy and childbirth. Current
hormonal contraceptive methods are much safer than in the
past: low dose oestrogen and third generation progestogen
derivatives are associated with a relatively low thromboembolic
risk.
Intrauterine devices are a suitable form of
contraception, although these may be a
Smoking
problem in patients with primary valvar
Cigarette smoking should be strongly discouraged in patients
disease, in view of the risks of infection
with heart failure. In addition to the well established adverse
and risks associated with oral
effects on coronary disease, which is the underlying cause in a
anticoagulation
substantial proportion of patients, smoking has adverse
haemodynamic effects in patients with congestive heart failure.
For example, smoking tends to reduce cardiac output, especially
in patients with a history of myocardial infarction.
Other adverse haemodynamic effects include an increase in
heart rate and systemic blood pressure (double product) and
mild increases in pulmonary artery pressure, ventricular filling
Menopausal women with heart failure
pressures, and total systemic and pulmonary vascular resistance.
x Observational data indicate that hormone replacement therapy
The peripheral vasoconstriction may contribute to the
reduces the risk of coronary events in postmenopausal women
observed mild reduction in stroke volume, and thus smoking
x However, there is limited prospective evidence to advise the use of
increases oxygen demand and also decreases myocardial
such therapy in postmenopausal women with heart failure
x Nevertheless, there may be an increased risk of venous thrombosis
oxygen supply owing to reduced diastolic filling time (with
in postmenopausal women taking hormone replacement therapy,
faster heart rates) and increased carboxyhaemoglobin
which may exacerbate the risk associated with heart failure
concentrations.
21
Alcohol
In general, alcohol consumption should be restricted to
moderate levels, given the myocardial depressant properties of
Community and social support
alcohol. In addition to the direct toxic effects of alcohol on the
x Community support is particularly important for elderly or
myocardium, a high alcohol intake predisposes to arrhythmias
functionally restricted patients with chronic heart failure
x Support may help to improve the quality of life and reduce
(especially atrial fibrillation) and hypertension and may lead to
admission rates
important alterations in fluid balance. The prognosis in alcohol
x Social services support and community based interventions, with
induced cardiomyopathy is poor if consumption continues, and
advice and assistance for close relatives, are also important
abstinence should be advised. Abstinence can result in marked
improvements, with echocardiographic studies showing
substantial clinical benefit and improvements in left ventricular
function. Resumed alcohol consumption may subsequently lead
to acute or worsening heart failure.
Managing cachexia in chronic heart failure
Combined management by physician and dietician is recommended
x Alter size and frequency of meals
Immunisation and antiobiotic prophylaxis
x Ensure a higher energy diet
Chronic heart failure predisposes to and can be exacerbated by
x Supplement diet with (a) water soluble vitamins (loss associated
pulmonary infection, and influenza and pneumococcal
with diuresis), (b) fat soluble vitamins (levels reduced as a result of
vaccinations should therefore be considered in all patients with
poor absorption), and (c) fish oils
heart failure. Antibiotic prophylaxis, for dental and other
surgical procedures, is mandatory in patients with primary valve
disease and prosthetic heart valves.
Diet and nutrition
Date
Although controlled trials offer only limited information on diet
Pulse
and nutritional measures, such measures are as important in
BP (lying)
heart failure, as in any other chronic illness, to ensure adequate
BP (standing)
and appropriate nutritional balance. Poor nutrition may
Urine
contribute to cardiac cachexia, although malnutrition is not
Weight
limited to patients with obvious weight loss and muscle wasting.
Drug 1
Patients with chronic heart failure are at an increased risk
Drug 2
from malnutrition owing to (a) a decreased intake resulting
from a poor appetite, which may be related to drug treatment
Drug 3
(for example, aspirin, digoxin), metabolic disturbance (for
Drug 4
example, hyponatraemia or renal failure), or hepatic
Drug 5
congestion; (b) malabsorption, particularly in patients with
Drug 6
severe heart failure; and (c) increased nutritional requirements,
Serum urea/creatinine
with patients who have congestive heart failure having an
Serum potassium
increase of up to 20% in basal metabolic rate. These factors may
Other investigations
contribute to a net catabolic state where lean muscle mass is
Next visit
reduced, leading to an increase in symptoms and reduced
Doctor's signature
exercise capacity. Indeed, cardiac cachexia is an independent
risk factor for mortality in patients with chronic heart failure. A
formal nutritional assessment should thus be considered in
Heart failure cooperation card: patients and doctors are able to monitor
those patients who appear to have a poor nutritional state.
changes in clinical signs (including weight), drug treatment, and baseline
investigations. Patients should be encouraged to monitor their weight
Weight loss in obese patients should be encouraged as
between clinic visits
excess body mass increases cardiac workload during exercise.
Weight reduction in obese patients to within 10% of the optimal
body weight should be encouraged.
Commonly consumed processed foods that have a high
Salt restriction
sodium content
No randomised studies have addressed the role of salt
x Cheese
restriction in congestive heart failure. Nevertheless restriction to
x Sausages
about 2 g of sodium a day may be useful as an adjunct to
x Crisps, salted peanuts
treatment with high dose diuretics, particularly if the condition
x Milk and white chocolate
x Tinned soup and tinned vegetables
is advanced.
x Ham, bacon, tinned meat (eg corned beef)
In general, patients should be advised that they should avoid
x Tinned fish (eg sardines, salmon, tuna)
foods that are rich in salt and not to add salt to their food at the
x Smoked fish
table.
Fluid intake
Fluid restriction (1.52 litres daily) should be considered in
Fresh produce, such as fruit, vegetables,
patients with severe symptoms, those requiring high dose
eggs, and fish, has a relatively low salt
diuretics, and those with a tendency towards excessive fluid
content
intake. High fluid intake negates the positive effects of diuretics
and induces hyponatraemia.
22
Exercise training and rehabilitation
Exercise training has been shown to benefit patients with heart
Effects of deconditioning in heart failure
failure: patients show an improvement in symptoms, a greater
sense of wellbeing, and better functional capacity. Exercise does
Peripheral alterations
Increased peripheral vascular resistance;
impaired oxygen utilisation during
not, however, result in obvious improvement in cardiac function.
exercise
All stable patients with heart failure should be encouraged
to participate in a supervised, simple exercise programme.
Abnormalities of
Enhanced sympathetic activation; vagal
Although bed rest (“armchair treatment”) may be appropriate
autonomic control
withdrawal; reduced baroreflex sensitivity
in patients with acute heart failure, regular exercise should be
Skeletal muscle
Reduced mass and composition
encouraged in patients with chronic heart failure. Indeed,
abnormalities
chronic immobility may result in loss of muscle mass in the
Reduced functional
Reduced exercise tolerance; reduced
lower limb and generalised physical deconditioning, leading to
capacity
peak oxygen consumption
a further reduction in exercise capacity and a predisposition to
thromboembolism. Deconditioning itself may be detrimental,
Psychological effects
Reduced activity; reduced overall sense of
with peripheral alterations and central abnormalities leading to
wellbeing
vasoconstriction, further deterioration in left ventricular
function, and greater reduction in functional capacity.
Importantly, regular exercise has the potential to slow or
stop this process and exert beneficial effects on the autonomic
profile, with reduced sympathetic activity and enhanced vagal
tone, thus reversing some of the adverse consequences of heart
failure. Large prospective clinical trials will establish whether
these beneficial effects improve prognosis and reduce the
incidence of sudden death in patients with chronic heart failure.
Regular exercise should therefore be advocated in stable
patients as there is the potential for improvements in exercise
tolerance and quality of life, without deleterious effects on left
ventricular function. Cardiac rehabilitation services offer benefit
to this group, and patients should be encouraged to develop
their own regular exercise routine, including walking, cycling,
and swimming. Nevertheless, patients should know their limits,
and excessive fatigue or breathlessness should be avoided. In
the first instance, a structured walking programme would be the
easiest to adopt.
Beneficial effects of exercise in chronic heart failure
Has positive effects on:
x Skeletal muscle
Exercise class for group of patients with heart failure (published with
x Autonomic function
permission of participants)
x Endothelial function
x Neurohormonal function
x Insulin sensitivity
No positive effects on survival have been shown
Treatment of underlying disease
Treatment should also be aimed at slowing or reversing any
underlying disease process.
Hypertension
Good blood pressure control is essential, and angiotensin
converting enzyme inhibitors are the drugs of choice in patients
with impaired systolic function, in view of their beneficial effects
on slowing disease progression and improving prognosis. In
cases of isolated diastolic dysfunction, either â blockers or
calcium channel blockers with rate limiting properties—for
example, verapamil, diltiazem—have theoretical advantages. If
severe left ventricular hypertrophy is the cause of diastolic
dysfunction, however, an angiotensin converting enzyme
inhibitor may be more effective at inducing regression of left
ventricular hypertrophy. Angiotensin II receptor antagonists
M mode echocardiogram showing left ventricular hypertrophy in
should be considered as an alternative if cough that is induced
hypertensive patient (A=interventricular septum; B=posterior wall of left
by angiotensin converting enzyme inhibitors is problematic.
ventricle)
23
I
aVR
V1
V4
II
aVL
V2
V5
III
aVF
V3
V6
II
Electrocardiogram showing left ventricular hypertrophy on voltage criteria, with associated T wave and ST changes in the
lateral leads (“strain pattern”)
Surgery
If coronary heart disease is the underlying cause of chronic
heart failure and if cardiac ischaemia is present, the patient may
benefit from coronary revascularisation, including coronary
angioplasty or coronary artery bypass grafting.
Role of surgery in heart failure
Revascularisation may also improve the function of previously
hibernating myocardium. Valve replacement or valve repair
Type of surgery
Reason
should be considered in patients with haemodynamically
Coronary revascularisation
Angina, reversible ischaemia,
important primary valve disease.
(PTCA, CABG)
hibernating myocardium
Cardiac transplantation is now established as the treatment
Valve replacement (or repair)
Significant valve disease (aortic
of choice for some patients with severe heart failure who
stenosis, mitral regurgitation)
remain symptomatic despite intensive medical treatment. It is
Permanent pacemakers and
Bradycardias; resistant ventricular
associated with a one year survival of about 90% and a 10 year
implantable cardiodefibrillators
arrhythmias
survival of 5060%, although it is limited by the availability of
Cardiac transplantation
End stage heart failure
donor organs. Transplantation should be considered in younger
Ventricular assist devices
Short term ventricular
patients (aged < 60 years) who are without severe concomitant
support—eg awaiting
disease (for example, renal failure or malignancy).
transplantation
Bradycardias are managed with conventional permanent
Novel surgical techniques
Limited role (high mortality,
cardiac pacing, although a role is emerging for biventricular
limited evidence of substantial
cardiac pacing in some patients with resistant severe congestive
benefit)
heart failure. Implantable cardiodefibrillators are well
established in the treatment of some patients with resistant life
PTCA = percutaneous transluminal coronary angioplasty; CABG = coronary
artery bypass graft.
threatening ventricular arrhythmias. New surgical approaches
such as cardiomyoplasty and ventricular reduction surgery
(Batista procedure) are rarely used owing to the high associated
morbidity and mortality and the lack of conclusive trial
evidence of substantial benefit.
The box about managing cachexia is based on recommendations from the
Scottish Intercollegiate Guidelines Network (SIGN) (publication No 35,
1999).
Key references
x Demakis JG, Proskey A, Rahimtoola SH, Jamil M, Sutton GC, Rosen
G Jackson is consultant cardiologist in the department of cardiology,
KM, et al. The natural course of alcoholic cardiomyopathy. Ann
Guy’s and St Thomas’s Hospital, London.
Intern Med 1974;80:2937.
x The Task Force of the Working Group on Heart Failure of the
The ABC of heart failure is edited by C R Gibbs, M K Davies, and
European Society of Cardiology. Guidelines on the treatment of
G Y H Lip. CRG is research fellow and GYHL is consultant
heart failure. Eur Heart J 1997;18:73653.
cardiologist and reader in medicine in the university department of
x Kostis JB, Rosen RC, Cosgrove NM, Shindler DM, Wilson AC.
medicine and the department of cardiology, City Hospital,
Nonpharmacologic therapy improves functional and emotional
Birmingham; MKD is consultant cardiologist in the department of
status in congestive heart failure. Chest 1994;106:9961001.
cardiology, Selly Oak Hospital, Birmingham. The series will be
x McKelvie RS, Teo KK, McCartney N, Humen D, Montague T, Yusuf
published as a book in the spring.
S. Effects of exercise training in patients with congestive heart
failure: a critical review. J Am Coll Cardiol 1995;25:78996.
BMJ 2000;320:3669
24
ABC of heart failure
Management: diuretics, ACE inhibitors, and nitrates
M K Davies, C R Gibbs, G Y H Lip
In the past 15 years several large scale, randomised controlled
Aims of heart failure management
trials have revolutionised the management of patients with
To achieve improvement in symptoms
chronic heart failure. Although it is clear that some drugs
x Diuretics
improve symptoms, others offer both symptomatic and
x Digoxin
prognostic benefits, and the management of heart failure
x ACE inhibitors
should be aimed at improving both quality of life and survival.
To achieve improvement in survival
Diuretics and angiotensin converting enzyme (ACE)
x ACE inhibitors
inhibitors, when combined with nonpharmacological
x â blockers (for example, carvedilol and bisoprolol)
measures, remain the basis of treatment in patients with
x Oral nitrates plus hydralazine
congestive heart failure. Digoxin has a possible role in some of
x Spironolactone
these patients, however, and the potential benefits of â blockers
and spironolactone (an aldosterone antagonist) in chronic heart
failure are now increasingly recognised.
Diuretics
Diuretics are effective in providing symptomatic relief and
In general, diuretics should be introduced
remain the first line treatment, particularly in the presence of
at a low dose and the dose increased
oedema. Nevertheless, there is no direct evidence that loop and
according to the clinical response. There
are dangers, however, in either
thiazide diuretics confer prognostic benefit in patients with
undertreating or overtreating patients
congestive heart failure.
with diuretics, and regular review is
necessary
Loop diuretics
Loop diuretics—frusemide (furosemide) and bumetanide—have
a powerful diuretic action, increasing the excretion of sodium
and water via their action on the ascending limb of the loop of
Henle. They have a rapid onset of action (intravenously 5
minutes, orally 12 hours; duration of action 46 hours). Oral
absorption of frusemide may be reduced in congestive heart
How to use diuretics in advanced heart failure
failure, although the pharmacokinetics of bumetanide may
x Optimise diuretic dose
allow improved bioavailability.
x Consider combination diuretic treatment with a loop and thiazide
Patients receiving high dose diuretics (frusemide >80 mg or
(or thiazidelike) diuretic
x Consider combining a low dose of spironolactone with an ACE
equivalent) should be monitored for renal and electrolyte
inhibitor, provided that there is no evidence of hyperkalaemia
abnormalities. Hypokalaemia, which may precipitate
x Administer loop diuretics (either as a bolus or a continuous
arrhythmias, should be avoided, and potassium
infusion) intravenously
supplementation, or concomitant treatment with a potassium
sparing agent, should generally be used unless
contraindicated—for example, in renal dysfunction with
potassium retention. Acute gout is a relatively common adverse
effect of treatment with high dose intravenous diuretics.
Thiazide diuretics
2
Distal tubule
3
Thiazides—such as bendrofluazide (bendroflumethiazide)—act
Early Late
on the cortical diluting segment of the nephron. They are often
Proximal
ineffective in elderly people, owing to the age related and heart
tubule
failure mediated reduction in glomerular filtration rate.
Cortical collecting
Hyponatraemia and hypokalaemia are commonly associated
duct
1
with higher doses of thiazide diuretics, and potassium
supplementation, or concomitant treatment with a potassium
sparing agent, is usually needed with high dose thiazide therapy.
Thick
ascending
In some patients with chronic severe congestive heart
limb
failure, particularly in the presence of chronic renal
Medullary collecting
impairment, oedema may persist despite conventional oral
duct
Loop of
doses (frusemide 40160 mg daily) of loop diuretics. In these
Henle
patients, a thiazide diuretic (for example, bendrofluazide) or a
thiazidelike diuretic (for example, metolazone) may be
Diagram of nephron showing sites of action of different diuretic classes:
combined with a loop diuretic. This combination blocks
1=loop (eg frusemide); 2=thiazide (eg bendrofluazide); and 3=potassium
reabsorption of sodium at different sites in the nephron
sparing (eg amiloride)
25
(“double nephron blockade”), and this synergistic action leads
The two main potassium sparing
to a greater diuretic effect. The incidence of associated
diuretics, amiloride and spironolactone,
metabolic abnormalities is, however, increased, and such
have a weak diuretic action when used
treatment should be started only under close supervision. In
alone; amiloride is most commonly used
some patients, a large diuretic effect may occur soon after a
in fixed dose combinations with a loop
combination regimen (loop diuretic plus either thiazide or
diuretic—for example, coamilofruse
metalozone) has been started. It is advisable, therefore, to
consider such a combination treatment on a twice weekly basis,
at least initially.
1.0
Potassium sparing diuretics
Amiloride acts on the distal nephron, while spironolactone is a
Spironolactone
0.9
competitive aldosterone inhibitor. Potassium sparing diuretics
Placebo
have generally been avoided in patients receiving ACE
0.8
inhibitors, owing to the potential risk of hyperkalaemia.
Nevertheless, a recent randomised placebo controlled study, the
0.7
randomised aldactone evaluation study (RALES), reported that
0.6
hyperkalaemia is uncommon when low dose spironolactone
(<25 mg daily) is combined with an ACE inhibitor. Risk factors
0.5
for developing hyperkalaemia include spironolactone dose
> 50 mg/day, high doses of ACE inhibitor, or evidence of renal
impairment. It is recommended that measurement of the serum
0
0
3
6
9
12
15
18
21
24
27
30
33
36
creatinine and potassium concentrations is performed within
Months
57 days of the addition of a potassium sparing diuretic to an
ACE inhibitor until the levels are stable, and then every one to
Survival curve for randomised aldactone evaluation study (RALES) showing
30% reduction in all cause mortality when spironolactone (up to 25 mg) was
three months.
added to conventional treatment in patients with severe (New York Heart
Association class IV) chronic heart failure
ACE inhibitors
ACE inhibitors have consistently shown beneficial effects on
mortality, morbidity, and quality of life in large scale, prospective
Guidelines for using ACE inhibitors
clinical trials and are indicated in all stages of symptomatic
x Stop potassium supplements and potassium sparing diuretics
heart failure resulting from impaired left ventricular systolic
x Omit (or reduce) diuretics for 24 hours before first dose
function.
x Advise patient to sit or lie down for 24 hours after first dose
x Start low doses (for example, captopril 6.25 mg twice daily,
enalapril 2.5 mg once daily, lisinopril 2.5 mg once daily)
Mechanisms of action
x Review after 12 weeks to reassess symptoms, blood pressure, and
ACE inhibitors inhibit the production of angiotensin II, a
renal chemistry and electrolytes
potent vasoconstrictor and growth promoter, and increase
x Increase dose unless there has been a rise in serum creatinine
concentrations of the vasodilator bradykinin by inhibiting its
concentration (to > 200 ìmol/l) or potassium concentration (to
degradation. Bradykinin has been shown to have beneficial
> 5.0 mmol/l)
effects associated with the release of nitric oxide and
x Titrate to maximum tolerated dose, reassessing blood pressure and
renal chemistry and electrolytes after each dose titration
prostacyclin, which may contribute to the positive
haemodynamic effects of the ACE inhibitors. Bradykinin may
If patient is “high risk” consider hospital admission to start treatment
also be responsible, however, for some of the adverse effects,
such as dry cough, hypotension, and angiooedema.
ACE inhibitors also reduce the activity of the sympathetic
nervous system as angiotensin II promotes the release of
noradrenaline and inhibits its reuptake. In addition, they also
improve â receptor density (causing their up regulation),
variation in heart rate, baroreceptor function, and autonomic
function (including vagal tone).
Clinical effects
Symptomatic left ventricular dysfunction
ACE inhibitors, when added to diuretics, improve symptoms,
exercise tolerance, and survival and reduce hospital admission
rates in chronic heart failure.
These beneficial effects are apparent in all grades of systolic
heart failure—that is, mild to moderate chronic heart failure (as
evident, for example, in the Munich mild heart failure study, the
vasodilator heart failure trials (VHeFT), and the studies of left
ventricular dysfunction treatment trial (SOLVDT)) and severe
chronic heart failure (as, for example, in the first cooperative
Front view and side view of woman with angiooedema related to treatment
north Scandinavian enalapril survival study (CONSENSUS I).
with ACE inhibitors (published with permission of patient)
26
Asymptomatic left ventricular dysfunction
No of patients to be
treated per year to
330
66
76
22
2
ACE inhibitors have also been shown to be effective in
prevent one death
asymptomatic patients with left ventricular systolic dysfunction.
1.2
The studies of left ventricular dysfunction prevention trial
1.0
(SOLVDP) confirmed the benefit of ACE inhibitors in
asymptomatic left ventricular systolic dysfunction, where
0.8
enalapril reduced the development of heart failure and related
0.6
hospital admissions.
0.4
Left ventricular dysfunction after myocardial infarction
0.2
SOLVD
SAVE
SOLVD
AIRE
CONSENSUS
Large scale, randomised controlled trials—for example, the
(prevention)
(treatment)
acute infarction ramipril efficacy (AIRE) study, the survival and
Mortality in control
group (per 100
5.1
8.1
11.5
19.1
123.3
ventricular enlargement (SAVE) study, and the trial of
patients/year)
trandolapril cardiac evaluation (TRACE)—have shown lower
ACE inhibitors in left ventricular dysfunction: best benefit for ACE
mortality in patients with impaired systolic function after
inhibitors in higher risk group
myocardial infarction, irrespective of symptoms.
Slowing disease progression
ACE inhibitors also seem to influence the natural course of
Metaanalysis of effects of ACE inhibitors on mortality and
chronic heart failure. The Munich mild heart failure study
admissions in chronic heart failure
showed that ACE inhibitors combined with standard treatment
No
Total No
Active
Risk
slowed the progression of heart failure in patients with mild
of
of
Placebo
treatment
reduction
symptoms, with significantly fewer patients in the active
trials
patients
(%)
(%)
(%)
P value
treatment group developing severe heart failure.
32
7105
32.6
22.4
35
< 0.001
Doses and tolerability
ACE inhibitors should be started at a low dose and gradually
titrated to the highest tolerated maintenance level. The recent
prospective assessment trial of lisinopril and survival (ATLAS)
randomised patients with symptomatic heart failure to low dose
ACE inhibitors: high risk patients warranting hospital
(2.55 mg daily) or high dose (32.535 mg daily) lisinopril, and,
admission for start of treatment
although there was no significant mortality difference, high
x Severe heart failure (NYHA class IV) or decompensated heart
dose treatment was associated with a significant reduction in the
failure
x Low systolic blood pressure ( < 100 mm Hg)
combined end point of all cause mortality and all cause
x Resting tachycardia > 100 beats/minute
admissions to hospital. Adverse effects of the ACE inhibitors
x Low serum sodium concentration ( < 130 mmol/l)
include cough, dizziness, and a deterioration in renal function,
x Other vasodilator treatment
although the overall incidence of hypotension and renal
x Severe chronic obstructive airways disease and pulmonary heart
impairment in the CONSENSUS and SOLVD studies was only
disease (cor pulmonale)
5%. Angiooedema related to ACE inhibitors is rare, although
more common in patients of AfroCaribbean origin than in
other ethnic groups.
ACE inhibitors can therefore be regarded as the
cornerstone of treatment in patients with all grades of
Doses of ACE inhibitors used in large controlled trials
symptomatic heart failure and in patients with asymptomatic
Target
Mean daily
left ventricular dysfunction. Every attempt should be made to
Trial
ACE inhibitor
dose (mg)
dose (mg)
provide this treatment for patients, unless it is contraindicated,
and to use adequate doses.
CONSENSUS
Enalapril
20*
18.4
VHeFT II
Enalapril
10*
15.0
SOLVD
Enalapril
10*
16.6
Angiotensin receptor antagonists
SAVE
Captopril
50†
NA
Orally active angiotensin II type 1 receptor antagonists, such as
*Twice daily; †three times daily. NA = information not available.
losartan, represent a new class of agents that offer an alternative
method of blocking the reninangiotensin system. The effects of
angiotensin II receptor antagonists on haemodynamics,
neuroendocrine activity, and exercise tolerance resemble those
Recommended maintenance doses of ACE inhibitors
of ACE inhibitors, although it still remains to be established
fully whether these receptor antagonists are an effective
Drug
Starting dose (mg)
Maintenance dose (mg)
substitute for ACE inhibitors in patients with chronic heart
Captopril
6.25†
2550†
failure.
Enalapril
2.5‡
10*
The evaluation of losartan in the elderly (ELITE) study
Lisinopril
2.5‡
520‡
compared losartan with captopril in patients aged 65 or over
Quinapril
2.55‡
510*
with mild to severe congestive heart failure. Although the
Perindopril
2‡
4‡
ELITE study was designed as a tolerability study, and survival
Ramipril
1.252.5‡
2.55*
was not the primary end point, it did report a reduction in all
Trandolapril
0.5‡
24‡
cause mortality (4.8% v 8.7%) in patients treated with losartan.
Important limitations of the ELITE study included the limited
*Twice daily; †three times daily; ‡once daily.
27
size and the relatively short follow up. However, the recently
ELITE II study: the losartan heart failure survival study
reported ELITE II mortality study failed to show that treatment
x Multicentre, randomised, parallel group trial of captopril v losartan
with losartan was superior to captopril, although it confirmed
in chronic stable heart failure
improved tolerability with losartan.
x 3152 patients; age > 60 years (mean age 71.5 years); NYHA class
ACE inhibitors, therefore, remain the treatment of choice in
IIIV heart failure; mean follow up of 2 years
patients with left ventricular systolic dysfunction, although
x No significant difference in all cause mortality between the
angiotensin II receptor antagonists are an appropriate
captopril group (15.9%) and losartan group (17.7%)
alternative in patients who develop intolerable side effects from
x Better tolerability with losartan (withdrawal rate 9.4%) than with
captopril (14.5%)
ACE inhibitors.
Oral nitrates and hydralazine
The VHeFT trials showed a survival benefit from combined
treatment with nitrates and hydralazine in patients with
Vasodilator heart failure (VHeFT) studies
symptomatic heart failure (New York Heart Association class
NYHA
IIIII). The VHeFT II trial also showed a modest improvement
Study
Comparison
class*
Outcome
in exercise capacity, although the nitrate and hydralazine
combination was less well tolerated than enalapril, owing to the
VHeFT I
Hydralazine plus
II, III
Improved mortality
isosorbide
with active treatment
dose related adverse effects (dizziness and headaches). There is
dinitrate v placebo
no reproducible evidence of symptomatic improvement from
VHeFT II
Hydralazine plus
II, III
Enalapril superior to
other randomised placebo controlled trials, however, and
isosorbide
hydralazine plus
survival rates were higher with ACE inhibitors than with the
dinitrate v
isosorbide dinitrate
nitrate and hydralazine combination (VHeFT II trial).
enalapril
for survival
In general, oral nitrates should be considered in patients
*I = asymptomatic, II = mild, III = moderate, IV = severe.
with angina and impaired left ventricular systolic function. The
combination of nitrates and hydralazine is an alternative
regimen in patients with severe renal impairment, in whom
ACE inhibitors and angiotensin II receptor antagonists are
contraindicated. Although it is rational to consider the addition
0.75
of a combination of nitrates and hydralazine in patients who
Enalapril
continue to have severe symptoms despite optimal doses of
Hydralazine plus isosorbide dinitrate
ACE inhibitors, no large scale trials have shown an additive
0.50
effect of these combinations.
Other vasodilators
0.25
Long acting dihydropyridine calcium channel blockers
generally have neutral effects in heart failure, although others,
0
such as diltiazem and verapamil, have negatively inotropic and
0
6
12
18
24
30
36
42
48
54
60
chronotropic properties, with the potential to exacerbate heart
Months
failure. Two recent trials of the newer calcium channel blockers
Cumulative mortality in VHeFT II trial: enalapril v hydralazine plus
amlodipine (the prospective randomised amlodipine survival
isosorbide dinitrate in patients with congestive heart failure (mild to
evaluation (PRAISE) trial) and felodipine (VHeFT III) in
moderate)
patients with heart failure suggest that long acting calcium
antagonists may have beneficial effects in nonischaemic dilated
cardiomyopathy, although further studies are in progress—for
example, PRAISE II. Importantly, these studies indicate that
Key references
amlodipine and felodipine seem to be safe in patients with
x Cohn JN, Johnson G, Ziesche S, Cobb F, Francis G, Tristani F, et al.
congestive heart failure and could therefore be used to treat
A comparison of enalapril with hydralazineisosorbide dinitrate in
angina and hypertension in this group of patients.
the treatment of chronic congestive heart failure. N Engl J Med
1991;325:30310.
The two tables on recommended doses of ACE inhibitors are adapted and
x Cohn JN, Ziesche S, Smith R, Anand I, Dunkman WB, Loeb H, et al.
reproduced with permission from Remme WJ (Eur Heart J 1997;18:
Effect of the calcium antagonist felodipine as supplementary
73653). The metaanalysis table is adapted and used with permission from
vasodilator therapy in patients with chronic heart failure treated
Garg R et al (JAMA 1995;273:14506). The graph showing the benefit of
with enalapril. VHeFT III. Circulation 1997;96:85663.
ACE inhibitors in left ventricular dysfunction is adapted from Davey Smith
x Packer M, O’Connor CM, Ghali JK, Pressler ML, Carson PE, Belkin
et al (BMJ 1994;308:734).
RN, et al. Effect of amlodipine on morbidity and mortality in severe
chronic heart failure. N Engl J Med 1996;335:110714.
x Pitt B, Segal R, Martinez FA, Meurers G, Cowley AJ, Thomas I, et al.
The ABC of heart failure is edited by C R Gibbs, M K Davies, and
Randomised trial of losartan versus captopril in patients over 65
G Y H Lip. CRG is research fellow and GYHL is consultant
with heart failure. Lancet 1997;349:74752.
cardiologist and reader in medicine in the university department of
x Remme WJ. The treatment of heart failure. The Task Force of the
medicine and the department of cardiology, City Hospital,
Working Group on Heart Failure of the European Society of
Birmingham; MKD is consultant cardiologist in the department of
Cardiology. Eur Heart J 1997;18:73653.
cardiology, Selly Oak Hospital, Birmingham. The series will be
x Pitt B, Zannad F, Remme WJ, Cody R, Castaigne A, Perez A, et al.
published as a book in the spring.
The effect of spironolactone on morbidity and mortality in patients
with severe heart failure. N Engl J Med 1999;341:70917.
BMJ 2000;320:42831
28
ABC of heart failure
Management: digoxin and other inotropes, â blockers, and
antiarrhythmic and antithrombotic treatment
C R Gibbs, M K Davies, G Y H Lip
Digoxin
Use of digoxin for heart failure varies between countries across
Digoxin should be considered in patients
Europe, with high rates in Germany and low rates in the United
with sinus rhythm plus (a) continued
Kingdom. It is potentially invaluable in patients with atrial
symptoms of heart failure despite optimal
fibrillation and coexistent heart failure, improving control of the
doses of diuretics and angiotensin
ventricular rate and allowing more effective filling of the
converting enzyme inhibitors; (b) severe
ventricle. Digoxin is also used in patients with chronic heart
left ventricular systolic dysfunction with
cardiac dilatation; or (c) recurrent hospital
failure secondary to left ventricular systolic impairment, in sinus
admissions for heart failure
rhythm, who remain symptomatic despite optimal doses of
diuretics and angiotensin converting enzyme inhibitors, where
it acts as an inotrope.
Evidence of symptomatic benefit from digoxin in patients
with chronic heart failure in sinus rhythm has been reported in
several randomised placebo controlled trials and several smaller
trials. The RADIANCE and PROVED trials, for example,
reported that the withdrawal of digoxin from patients with
congestive heart failure who had already been treated with the
50
Placebo
drug was associated with worsening heart failure and increased
Digoxin
hospital readmission rates. The Digitalis Investigation Group’s
40
large study found that digoxin was associated with a
symptomatic improvement in patients with congestive heart
30
failure, when added to treatment with diuretics and angiotensin
converting enzyme inhibitors. Importantly, there were greater
20
absolute and relative benefits in the patients who had resistant
symptoms and more severe impairment of left ventricular
10
P< 0.001
systolic function. However, although there was a reduction in
the combined end points of admission and mortality resulting
00
4
8
12
16
20
24
28
32
36
40
44
48
52
from heart failure, there was no significant improvement in
Months
overall survival. â Blockers were used rarely in the Digitalis
Incidence of death or admission to hospital due to worsening heart failure
Investigation Group’s study, and as a result it is not clear
in two groups of patients: those receiving digoxin and those receiving
whether digoxin is additive to both the â blockers and
placebo (Digitalis Investigation Group’s study—see key references box at end
angiotensin converting enzyme inhibitors in congestive heart
of article)
failure.
Digoxin: practical aspects
x Ensure a maintenance dose of 125375 ìg (0.1250.375 mg) daily
x Give a reduced maintenance dose in elderly people, when renal
impairment is present, and when used with drugs that increase
digoxin concentrations (amiodarone, verapamil)
x Concentrations should be monitored especially in cases of
Study of effect of digoxin on mortality and morbidity in
uncertainty about whether therapeutic levels have been achieved
(range 6 hours after dose: 1.21.9 ng/ml)
patients with heart failure*
x Monitor potassium concentrations (avoid hypokalaemia) and renal
Number of participants: 6800
function
Design: prospective, randomised, double blind, placebo controlled
x Digoxin toxicity may be associated with: (a) adverse symptoms (for
Participants: left ventricular ejection fraction < 45%
example, nausea, vomiting, headache, confusion, visual symptoms);
Intervention: randomised to digoxin (0.1250.500 mg) or placebo;
and (b) arrhythmias (for example, atrioventricular junctional
follow up at 37 months
rhythms, atrial tachycardia, atrioventricular block, ventricular
tachycardia)
Results:
x Serious toxicity should be treated by correcting potassium
x Reduced admissions to hospital owing to heart failure (greater
concentrations and with drugs such as â blockers and glycoside
absolute and relative benefits in the patients with resistant
binding agents (cholestyramine), and in severe cases specific
symptoms and more severe impairment of left ventricular systolic
digoxin antibodies (Digibind)
function)
x No effect on overall survival
Source of information: Uretsky et al (J Am Coll Cardiol 1993;22:955) and Packer
et al (N Engl J Med 1993;329:1)
*The Digitalis Investigation Group’s study (see key references box)
29
Other inotropes
The potential role of inotropic agents other than digoxin in
Inotropic drugs associated with increased mortality in
chronic heart failure has been addressed in several studies.
chronic heart failure
Although these drugs seem to improve symptoms in some
patients, most have been associated with an increase in
Inotropic
mortality.
Drug
Class
activity
For example, the PRIME II trial (a prospective randomised
Xamoterol
â Receptor antagonist
Mild
study) examined ibopamine, a weak inotrope, in patients with
Dobutamine
Dopamine, á, and â receptor
Strong
chronic heart failure who were already receiving standard
antagonist
treatment. An excess mortality was shown, however,
Ibopamine
Dopamine, á, and â receptor
Weak
particularly in those with severe symptoms; this was possibly
antagonist
related to an excess of arrhythmias. In addition, a previous trial
Amrinone
Phosphodiesterase inhibitor
Strong
evaluating intermittent dobutamine infusions in patients with
Enoximone
Phosphodiesterase inhibitor
Strong
chronic heart failure was stopped prematurely because of
Flosequinan
Attenuates inositol triphosphate
Weak
excess mortality in the group taking dobutamine. Xamoterol, a
Milrinone
Phosphodiesterase inhibitor
Strong
â receptor antagonist with mild agonist inotropic effects, also
Vesnarinone
Phosphodiesterase inhibitor
Mild
failed to show any positive benefits in patients with heart
failure.
In overall terms, no evidence exists at present to support the
use of oral catecholamine receptor (or postreceptor pathway)
stimulants in the treatment of chronic heart failure. Digoxin
remains the only (albeit weak) positive inotrope that is valuable
in the management of chronic heart failure.
Potential mechanisms and benefits of
â blockers: improved left ventricular
function; reduced sympathetic tone;
â Blockers
improved autonomic nervous system
balance; up regulation of â adrenergic
â Adrenoceptor blockers have traditionally been avoided in
receptors; reduction in arrhythmias,
patients with heart failure due to their negative inotropic effects.
ischaemia, further infarction, myocardial
However, there is now considerable clinical evidence to support
fibrosis, and apoptosis
the use of â blockers in patients with chronic stable heart failure
resulting from left ventricular systolic dysfunction. Recent
randomised controlled trials in patients with chronic heart
failure have reported that combining â blockers with
conventional treatment with diuretics and angiotensin
converting enzyme inhibitors results in improvements in left
ventricular function, symptoms, and survival, as well as a
Randomised, placebo controlled â blocker trials in
reduction in admissions to hospital.
congestive heart failure
Recently, two randomised controlled trials have studied the
effects of carvedilol, a â blocker with á blocking and vasodilator
NYHA
Study
Treatment
class*
Outcome
properties, in patients with symptomatic heart failure. The US
multicentre carvedilol study programme was stopped early
MDC
Metoprolol
II, III
Improved clinical state
because of a highly significant (65%) mortality benefit in
without effect on
survival. Reduction in
patients receiving carvedilol, when compared to placebo, and
need for transplantation
the Australia/New Zealand heart failure study reported a 41%
in patients with dilated
reduction in the combined primary end point of all cause
cardiomyopathy
hospital admission and mortality. Bisoprolol has also been
CIBIS I
Bisoprolol
II, III
Trend (nonsignificant)
studied, and, although the first cardiac insufficiency bisoprolol
towards improved
study (CIBIS I) reported a trend towards a reduction in
survival
mortality and need for cardiac transplantation, there was no
ANZ trial
Carvedilol
I, II
Carvedilol superior to
conclusive survival benefit. The recent CIBIS II study, however,
placebo for morbidity
was stopped prematurely because of the beneficial effects of
and mortality
active treatment on both morbidity and mortality. Metoprolol
Carvedilol
Carvedilol
II, III
Carvedilol superior to
(US)
placebo for morbidity
has also shown similar prognostic advantages in the metoprolol
and mortality
randomised intervention trial in heart failure (MERITHF),
CIBIS II
Bisoprolol
III, IV
Bisoprolol superior to
which was also stopped early. In summary, evidence is now
placebo for morbidity
and mortality
MERITHF Metoprolol
II, III
Metoprolol superior to
Metaanalysis of effects of â blockers on mortality and
placebo for morbidity
admissions to hospital in chronic heart failure
and mortality
No of trials
% receiving
Risk
Placebo groups in all trials received appropriate conventional treatment
(total No of
% receiving
active
reduction
P
(diuretics alone; diuretics plus either digoxin or angiotensin converting enzyme
inhibitors; or diuretics plus digoxin and angiotensin converting enzyme
patients)
placebo
treatment
(%)
value
inhibitors). Trials still in progress: COMET (carvedilol v metoprolol) and
COPERNICUS (carvedilol in severe chronic heart failure).
18
(3023)
24.6
15.8
38
< 0.001
*Classification of the New York Heart Association (I = no symptoms, II = mild,
III = moderate, IV = severe).
30
available to support the use of â blockers in chronic heart
Summary of the cardiac insufficiency bisoprolol study II
failure, as the benefits supplement those already obtained from
(CIBIS II)*
angiotensin converting enzyme inhibitors.
x Randomised, double blind, parallel group study
Carvedilol is now licensed in the United Kingdom for use in
x 2647 participants (class IIIIV (moderate to severe) according to
mild to moderate chronic stable heart failure, although at
classification of the New York Heart Association)
present its use is still not recommended in patients with severe
x Bisoprolol, increased in dose to a maximum of 10 mg a day
symptoms (New York Heart Association class IV). This latter
x Trial stopped because of significant mortality benefit in patients
group has been underrepresented in the trials to date.
treated with bisoprolol:
In general, â blockers should be started at very low doses,
(a) 32% reduction in all cause mortality
with the dose being slowly increased, under expert supervision,
(b) 32% reduction in admissions to hospital for worsening heart
to the target dose if tolerated. In the short term there may be a
failure
deterioration in symptoms, which may improve with alterations
(c) 42% reduction in sudden death
in other treatment, particularly diuretics.
*CIBIS II Investigators and Committee (Lancet 1999;353:913)
Dose and titration of â blockers in large, placebo controlled heart failure trials
Weekly titration schedule: total daily dose (mg)
Target
Initial dose
total daily
â Blocker
(mg)
1
2
3
4
5
6
7
8-11
12-15
dose (mg)
Metoprolol (MDC trial)
5
10
15
20
50
75
100
150
NI
NI
100-150
Carvedilol (US trials)
3.125
6.25
NI
12.5
NI
25
NI
50
NI
NI
50
Bisoprolol (CIBIS II)
1.25
1.25
2.5
3.75
5
5
5
5
7.5
10
10
References: Waagstein F et al (Lancet 1993;342:14426), Packer M et al (N Engl J Med 1996;334:134955), and CIBIS II Investigators and Committee (Lancet
1999;353:913).
NI = no increase in dose.
Antithrombotic treatment
In patients with chronic heart failure the incidence of stroke
and thromboembolism is significantly higher in the presence of
atrial and left ventricular dilatation, particularly in severe left
ventricular dysfunction. Nevertheless, there is conflicting
evidence of benefit from routine treatment of patients with
heart failure who are in sinus rhythm with antithrombotic
treatment, although anticoagulation should be considered in
the presence of mobile ventricular thrombus, atrial fibrillation,
and severe cardiac impairment. Large scale, prospective
randomised controlled trials of antithrombotic treatment in
heart failure are in progress, such as the WATCH study (a trial
of warfarin and antiplatelet therapy); the full results are awaited
with interest.
The combination of atrial fibrillation and heart failure (or
evidence of left ventricular systolic dysfunction on
echocardiography) is associated with a particularly high risk of
thromboembolism, which is reduced by long term treatment
with warfarin. Aspirin seems to have little effect on the risk of
thromboembolism and overall mortality in such patients.
Echocardiogram showing thrombus at left ventricular apex in patient with
Antiarrhythmic treatment
dilated cardiomyopathy (A=thrombus, B=left ventricle, C=left atrium)
Chronic heart failure and atrial fibrillation
Restoration and long term maintenance of sinus rhythm is less
successful in the presence of severe structural heart disease,
particularly when the atrial fibrillation is longstanding. In
The use of class I antiarrhythmic agents
patients with a deterioration in symptoms that is associated with
in patients with atrial fibrillation and
recent onset atrial fibrillation, treatment with amiodarone
chronic heart failure substantially
increases the long term success rate of cardioversion. Digoxin is
increases the risk of mortality
otherwise appropriate for controlling ventricular rate in most
patients with heart failure and chronic atrial fibrillation, with the
addition of amiodarone in resistant cases.
31
Chronic heart failure and ventricular arrhythmias
Ventricular arrhythmias are a common cause of death in severe
1.00
heart failure. Precipitating or aggravating factors should thus be
Amiodarone
addressed, including electrolyte disturbance (for example,
0.9
Control
hypokalaemia, hypomagnesaemia), digoxin toxicity, drugs
causing electrical instability (for example, antiarrhythmic drugs,
0.8
antidepressants), and continued or recurrent myocardial
0.7
ischaemia.
Amiodarone is effective for the symptomatic control of
0.6
ventricular arrhythmias in chronic heart failure, although most
studies have reported that long term antiarrhythmic treatment
0.5
with amiodarone has a neutral effect on survival. An
0.4
Argentinian trial (the GESICA study) of empirical amiodarone
0
90
180
270
360
450
540
630
720
in patients with chronic heart failure reported, however, that
Days from randomisation
active treatment was associated with a 28% reduction in total
Survival curves from GESICA trial (see key references box), showing
mortality, although this trial included a high incidence of
difference between patients taking amiodarone and controls
patients with nonischaemic heart failure. In contrast, in the
survival trial of antiarrhythmic therapy in congestive heart
failure (CHFSTAT), amiodarone did not improve overall
Summary of drug management in chronic heart failure
survival, although there was a significant (46%) reduction in
cardiac death and admission to hospital in the patients with
Drug class
Potential therapeutic role
nonischaemic chronic heart failure.
Diuretics
Symptomatic improvement of congestion.
In general, amiodarone should probably be reserved for
Spironolactone improves survival in severe
patients with chronic heart failure who also have symptomatic
(NYHA class IV) heart failure
ventricular arrhythmias. Interest has also developed in
Angiotensin
Improved symptoms, exercise capacity, and
implantable cardioverter defibrillators, which reduce the risk of
converting enzyme
survival in patients with asymptomatic and
sudden death in high risk patients with ventricular arrhythmias
(ACE) inhibitors
symptomatic systolic dysfunction
(MADIT and AVID studies), although the role of these devices
Digoxin
Improved symptoms, exercise capacity, and
in patients with chronic heart failure still remains to be
fewer admissions to hospital
established.
Angiotensin II
Treatment of symptomatic heart failure in
receptor antagonists
patients intolerant to ACE inhibitors*
Nitrates and
Improved survival in symptomatic patients
hydralazine
intolerant to ACE inhibitors or angiotensin II
receptor antagonists*
â Blockers
Improved symptoms and survival in stable
patients who are already receiving ACE
Key references
inhibitors
x Australia/New Zealand Heart Failure Research Collaborative
Amiodarone
Prevention of arrhythmias in patients with
Group. Randomized, placebocontrolled trial of carvedilol in
symptomatic ventricular arrhythmias
patients with congestive heart failure due to ischaemic heart
disease. Lancet 1997;349:37580.
*Recommendations of when these agents might be considered (the use of these
x Lip GYH. Intracardiac thrombus formation in cardiac impairment:
agents has not been addressed in randomised trials of patients intolerant to
ACE inhibitors).
investigation and the role of anticoagulant therapy. Postgrad Med J
1996;72:7318.
x Massie BM, Fisher SG, Radford M, Deedwania PC, Singh BN,
The survival graph is adapted with permission from Doval et al (Lancet
Fletcher RD, et al for the CHFSTAT Investigators. Effect of
1994;344:4938). The table of inotropic drugs is adapted with permission
amiodarone on clinical status and left ventricular function in
from Niebauer et al (Lancet 1997;349:966). The table of results of a
patients with congestive heart failure. Circulation 1996;93:212834.
metaanalysis of effects of â blockers is adapted with permission from
x MERITHF Study Group. Effect of metoprolol CR/XL in chronic
Lechat P et al (Circulation 1998;98:118491). The table on doses and titra
heart failure: metoprolol CR/XL randomised intervention trial in
tion of â blockers is adapted with permission from Remme WJ (Eur Heart J
congestive heart failure (MERITHF). Lancet 1999;353:20017.
1997;18:73653).
x Doval HC, Nul DR, Grancelli HO, Perrone SV, Bortman GR, Curiel
R, et al. Randomised trial of lowdose amiodarone in severe
The ABC of heart failure is edited by C R Gibbs, M K Davies, and
congestive heart failure [GESICA trial]. Lancet 1994;344:4938.
G Y H Lip. CRG is research fellow and GYHL is consultant
x Packer M, Bristow MR, Cohn JN, Colucci WS, Fowler MB, Gilbert
cardiologist and reader in medicine in the university department of
EM, et al. Effect of carvedilol on morbidity and mortality in patients
medicine and the department of cardiology, City Hospital,
with chronic heart failure. N Engl J Med 1996;334:134955.
Birmingham; MKD is consultant cardiologist in the department of
x Digitalis Investigation Group. The effect of digoxin on mortality and
cardiology, Selly Oak Hospital, Birmingham. The series will be
morbidity in patients with heart failure. N Engl J Med 1997;
published as a book in the spring.
336:52533.
BMJ 2000;320:4958
32
ABC of heart failure
Acute and chronic management strategies
T Millane, G Jackson, C R Gibbs, G Y H Lip
Acute and chronic management strategies in heart failure are
aimed at improving both symptoms and prognosis, although
Survival rates (%) compared with chronic heart failure
management in individual patients will depend on the
At 1 year
At 2 years
At 3 years
underlying aetiology and the severity of the condition. It is
imperative that the diagnosis of heart failure is accompanied by
Breast cancer
88
80
72
an urgent attempt to establish its cause, as timely intervention
Prostate cancer
75
64
55
may greatly improve the prognosis in selected cases—for
Colon cancer
56
48
42
example, in patients with severe aortic stenosis.
Heart failure
67
41
24
Management of acute heart failure
Assessment
Killip classification
Common presenting features include anxiety, tachycardia, and
Hospital
dyspnoea. Pallor and hypotension are present in more severe
mortality
cases: the triad of hypotension (systolic blood pressure < 90
Class
Clinical features
(%)
mm Hg), oliguria, and low cardiac output constitutes a
diagnosis of cardiogenic shock. Severe acute heart failure and
Class I
No signs of left ventricular dysfunction
6
cardiogenic shock may be related to an extensive myocardial
Class II
S3 gallop with or without mild to
30
moderate pulmonary congestion
infarction, sustained cardiac arrhythmias (for example, atrial
Class III
Acute severe pulmonary oedema
40
fibrillation or ventricular tachycardia), or mechanical problems
(for example, acute papillary muscle rupture or postinfarction
Class IV
Shock syndrome
8090
ventricular septal defect).
Severe acute heart failure is a medical emergency, and
effective management requires an assessment of the underlying
cause, improvement of the haemodynamic status, relief of
pulmonary congestion, and improved tissue oxygenation.
Clinical and radiographic assessment of these patients provides
a guide to severity and prognosis: the Killip classification has
been developed to grade the severity of acute and chronic heart
failure.
Treatment
Basic measures should include sitting the patient in an upright
position with high concentration oxygen delivered via a face
mask. Close observation and frequent reassessment are
required in the early hours of treatment, and patients with acute
severe heart failure, or refractory symptoms, should be
monitored in a high dependency unit. Urinary catheterisation
facilitates accurate assessment of fluid balance, while arterial
blood gases provide valuable information about oxygenation
and acidbase balance. The “base excess” is a guide to actual
Chest x ray film in patient with acute pulmonary oedema
tissue perfusion in patients with acute heart failure: a worsening
(more negative) base excess generally indicates lactic acidosis,
which is related to anaerobic metabolism, and is a poor
Basic measures
prognostic feature. Correction of hypoperfusion will correct the
metabolic acidosis; bicarbonate infusions should be reserved for
Sit patient upright
only the most refractory cases.
High dose oxygen
Corrects hypoxia
Intravenous loop diuretics, such as frusemide (furosemide),
induce transient venodilatation, when administered to patients
Initial drug treatment
with pulmonary oedema, and this may lead to symptomatic
improvement even before the onset of diuresis. Loop diuretics
Intravenous loop diuretics
Cause venodilatation and diuresis
also increase the renal production of vasodilator prostaglandins.
Intravenous opiates/opioids
Reduce anxiety and preload
This additional benefit is antagonised by the administration of
(morphine/diamorphine)
(venodilatation)
prostaglandin inhibitors, such as nonsteroidal
antiinflammatory drugs, and these agents should be avoided
Intravenous, buccal, or
Reduce preload and afterload, ischaemia
where possible. Parenteral opiates or opioids (morphine or
sublingual nitrates
and pulmonary artery pressures
diamorphine) are an important adjunct in the management of
severe acute heart failure, by relieving anxiety, pain, and distress
Acute heart failure: basic measures and initial drug treatment
33
and reducing myocardial oxygen demand. Intravenous opiates
Second line drug treatment
and opioids also produce transient venodilatation, thus
reducing preload, cardiac filling pressures, and pulmonary
Inotropes: β agonists
Increase myocardial contractility
(dobutamine)
congestion.
Nitrates (sublingual, buccal, and intravenous) may also
Increases renal perfusion, sodium
Dopamine (low dose)
excretion, and urine flow
reduce preload and cardiac filling pressures and are particularly
valuable in patients with both angina and heart failure. Sodium
Inotropes: phosphodiesterase
Increase myocardial contractility and
nitroprusside is a potent, directly acting vasodilator, which is
inhibitors (enoximone)
venodilatation
normally reserved for refractory cases of acute heart failure.
Weak inotropic effect, diuretic effect,
Intravenous aminophylline
bronchodilating effect
Short term inotropic support
In cases of severe refractory heart failure in which the cardiac
Advanced management
output remains critically low, the circulation can be supported
Reduces myocardial oxygen demand;
Assisted ventilation
improves alveolar ventilation
for a critical period of time with inotropic agents. For example,
dobutamine and dopamine have positive inotropic actions,
Circulatory assist devices
Give mechanical support
acting on the â1 receptors in cardiac muscle. Phosphodiesterase
inhibitors (for example, enoximone) are less commonly used,
Acute heart failure: second line drug treatment and advanced management
and long term use of these agents is associated with increased
mortality. Intravenous aminophylline is now rarely used for
treating acute heart failure. Inotropic agents in general increase
the potential for cardiac arrhythmias.
Intravenous inotropes and circulatory assist devices
x Short term support with intravenous inotropes or circulatory assist
devices, or with both, may temporarily improve haemodynamic
Chronic heart failure
status and peripheral perfusion
Chronic heart failure can be “compensated” or
x Such support can act as a bridge to corrective valve surgery or
cardiac transplantation in acute and chronic heart failure
“decompensated.” In compensated heart failure, symptoms are
stable, and many overt features of fluid retention and
pulmonary oedema are absent. Decompensated heart failure
refers to a deterioration, which may present either as an acute
episode of pulmonary oedema or as lethargy and malaise, a
Management of chronic heart failure
reduction in exercise tolerance, and increasing breathlessness
on exertion. The cause or causes of decompensation should be
General advice
x Counselling—about symptoms and compliance
considered and identified; they may include recurrent
x Social activity and employment
ischaemia, arrhythmias, infections, and electrolyte disturbance.
x Vaccination (influenza, pneumococcal)
Atrial fibrillation is common, and poor control of ventricular
x Contraception
rate during exercise despite adequate control at rest should be
General measures
addressed.
x Diet (for example, reduce salt and fluid intake)
Common features of chronic heart failure include
x Stop smoking
breathlessness and reduced exercise tolerance, and
x Reduce alcohol intake
management is directed at relieving these symptoms and
x Take exercise
improving quality of life. Secondary but important objectives
Treatment options—pharmacological
are to improve prognosis and reduce hospital admissions.
x Diuretics (loop and thiazide)
x Angiotensin converting enzyme inhibitors
x â Blockers
Initial management
x Digoxin
Nonpharmacological and lifestyle measures should be
x Spironolactone
addressed. Loop diuretics are valuable if there is evidence of
x Vasodilators (hydralazine/nitrates)
fluid overload, although these may be reduced once salt and
x Anticoagulation
x Antiarrhythmic agents
water retention has been treated. Angiotensin converting
x Positive inotropic agents
enzyme inhibitors should be introduced at an early stage, in the
Treatment options—devices and surgery
absence of clear contraindications. Angiotensin II receptor
x Revascularisation (percutaneous transluminal coronary angioplasty
antagonists are an appropriate alternative in patients who are
and coronary artery bypass graft)
intolerant to angiotensin converting enzyme inhibitors. â
x Valve replacement (or repair)
Blockers (carvedilol, bisoprolol, metoprolol) are increasingly
x Pacemaker or implantable cardiodefibrillator
used in stable patients, although these agents require low dose
x Ventricular assist devices
initiation and cautious titration under specialist supervision.
x Heart transplantation
Oral digoxin has a role in patients with left ventricular systolic
impairment, in sinus rhythm, who remain symptomatic despite
optimal doses of diuretics and angiotensin converting enzyme
inhibitors. Warfarin should be considered in patients with atrial
fibrillation.
Supervised exercise programmes are of
proved benefit, and regular exercise
should be encouraged in patients with
Severe congestive heart failure
chronic stable heart failure
Despite conventional treatment with diuretics and angiotensin
converting enzyme inhibitors, hospital admission may be
necessary in severe congestive heart failure. Fluid restriction is
34
important—fluid intake should be reduced to 11.5 litres/24 h,
and dietary salt restriction may be helpful.
Short term bed rest is valuable until signs and symptoms
improve: rest reduces the metabolic demand and increases
Weighing the patient daily is valuable in
renal perfusion, thus improving diuresis. Although bed rest
monitoring the response to treatment
potentiates the action of diuretics, it increases the risk of venous
thromboembolism, and prophylactic subcutaneous heparin
should be considered in immobile inpatients. Full
anticoagulation is not advocated routinely unless concurrent
atrial fibrillation is present, although it may be considered in
patients with very severe impairment of left ventricular systolic
Education, counselling, and support
function, associated with significant ventricular dilatation.
x A role is emerging for heart failure liaison nurses in educating and
Intravenous loop diuretics may be administered to overcome
supporting patients and their families, promoting long term
the short term problem of gut oedema and reduced absorption
compliance, and supervising treatment changes in the community
of tablets, and these may be used in conjunction with an oral
x Depression is common, underdiagnosed, and often undertreated;
counselling is therefore important for patients and families, and the
thiazide or thiazidelike diuretic (metolazone). Low dose
newer antidepressants (particularly the selective serotonin reuptake
spironolactone (25 mg) improves morbidity and mortality in
inhibitors) seem to be well tolerated and are useful in selected
severe (New York Heart Association class IV) heart failure,
patients
when combined with conventional treatment (loop diuretics
and angiotensin converting enzyme inhibitors). Potassium
concentrations should be closely monitored after the addition
of spironolactone.
Treatment of left ventricular systolic dysfunction
• Confirm diagnosis by echocardiography
• If possible, discontinue aggravating drugs (eg non-steroidal anti-inflammatory drugs)
• Address non-pharmacological and lifestyle measures
Symptomatic
Asymptomatic
Add loop diuretic (eg frusemide)
Angiotensin converting
Angiotensin converting enzyme inhibitor
enzyme inhibitor
Consider β blocker* in patients with chronic, stable condition
Persisting clinical features of heart failure
Atrial fibrillation
Angina
Options
• Optimise dose of loop diuretic
Options
• Digoxin
Options
• β blocker (if not already given)
• Low dose spironolactone (25mg once a day)
• β blocker (if not already given)
• Oral nitrates
• Digoxin
• Warfarin
• Calcium antagonist
• Combine loop and thiazide diuretics
(eg amlodipine)
• Oral nitrates/ hydralazine
Consider specialist referral in patients with atrial fibrillation (electrical cardioversion or
In the United Kingdom carvedilol is licensed
other antiarrhythmic agents - eg amiodarone - may be indicated), angina (coronary
for mild to moderate symptoms and bisoprolol
angiography and revascularisation may be indicated), or persistent or severe symptoms
for moderate to severe congestive heart failure
* Initial low dose (eg carvedilol, bisoprolol, metoprolol) with cautious titration under expert supervision
Example of management algorithm for left ventricular dysfunction
Special procedures
Intraaortic balloon pumping and mechanical devices
Intraaortic balloon counterpulsation and left ventricular assist
devices are used as bridges to corrective valve surgery, cardiac
transplantation, or coronary artery bypass surgery in the
presence of poor cardiac function. Mechanical devices are
indicated if (a) there is a possibility of spontaneous recovery (for
example, peripartum cardiomyopathy, myocarditis) or (b) as a
bridge to cardiac surgery (for example, ruptured mitral
papillary muscle, postinfarction ventricular septal defect) or
transplantation. Intraaortic balloon counterpulsation is the
Left ventricular
most commonly used form of mechanical support.
assist device
35
Revascularisation and other operative strategies
Indications and contraindications to cardiac transplantation
Impaired ventricular function in itself is not an absolute
in adults
contraindication to cardiac surgery, although the operative risks
Indications
are increased. Ischaemic heart disease is the most common
x End stage heart failure—for example, ischaemic heart disease and
precursor of chronic heart failure in Britain: coronary
dilated cardiomyopathy
ischaemia should be identified and revascularisation considered
x Rarely, restrictive cardiomyopathy and peripartum cardiomyopathy
with coronary artery bypass surgery or occasionally
x Congenital heart disease (often combined heartlung
percutaneous coronary angioplasty. The concept of
transplantation required)
“hibernating” myocardium is increasingly recognised, although
Absolute contraindications
the most optimal and practical methods of identifying
x Recent malignancy (other than basal cell and squamous cell
hibernation remain open to debate. Revascularisation of
carcinoma of the skin)
hibernating myocardium may lead to an improvement in the
x Active infection (including HIV, Hepatitis B, Hepatitis C with liver
disease)
overall left ventricular function.
x Systemic disease which is likely to affect life expectancy
Correction of valve disease, most commonly in severe aortic
x Significant pulmonary vascular resistance
stenosis or mitral incompetence (not secondary to left
Relative contraindications
ventricular dilatation), relieves a mechanical cause of heart
x Recent pulmonary embolism
failure; closure of an acute ventricular septal defect or mitral
x Symptomatic peripheral vascular disease
valve surgery for acute mitral regurgitation, complicating a
x Obesity
myocardial infarction, may be lifesaving. Surgical excision of a
x Severe renal impairment
left ventricular aneurysm (aneurysectomy) is appropriate in
x Psychosocial problems—for example, lack of social support, poor
compliance, psychiatric illness
selected cases. Novel surgical procedures such as extensive
x Age (over 6065 years)
ventricular reduction (Batista operation) and cardiomyoplasty
have been associated with successful outcome in a small
number of patients, although the high mortality, and the limited
evidence of substantial benefit, has restricted the widespread use
of these procedures.
4500
31
Transplantations
4000
30
Cardiac transplantation
Age of donors
3500
29
The outcome in cardiac transplantation is now good, with long
3000
28
term improvements in survival and quality of life in patients
2500
27
with severe heart failure. However, although the demand for
cardiac transplantation has increased over recent years, the
2000
26
number of transplant operations has remained stable, owing
1500
25
primarily to limited availability of donor organs.
1000
24
The procedure now carries a perioperative mortality of less
500
23
than 10%, with approximate one, five, and 10 year survival rates
0
22
of 92%, 75%, and 60% respectively (much better outcomes than
with optimal drug treatment, which is associated with a one year
Year
mortality of 3050% in advanced heart failure). Cardiac
transplantation should be considered in patients with an
Number of heart transplantations worldwide and mean age of donors
estimated one year survival of < 50%. Well selected patients
over 5560 years have a survival rate comparable to those of
younger patients. Patients need strong social and psychological
Key references
support; transplant liaison nurses are valuable in this role.
The long term survival of the transplanted human heart is
x Dargie HJ, McMurray JJ. Diagnosis and management of heart
compromised by accelerated graft atherosclerosis which results
failure. BMJ 1994;308:3218.
x ACC/AHA Task Force Report. Guidelines for the evaluation and
in small vessel coronary artery disease and an associated
management of heart failure. J Am Coll Cardiol 1995;26:137698.
deterioration in left ventricular performance. This can occur as
x Hunt SA. Current status of cardiac transplantation. JAMA
early as three months and is the major cause of graft loss after
1998;280:16928.
the first year. The antirejection regimens currently used may
x Remme WJ. The treatment of heart failure. The Task Force of the
result in an acceleration of preexisting atherosclerotic vascular
Working Group on Heart Failure of the European Society of
disease—hence the exclusion of patients who already have
Cardiology. Eur Heart J 1997;18:73653.
significant peripheral vascular disease. Rejection is now a less
serious problem, with the use of cyclosporin and other
immunosuppressant agents.
T Millane is consultant cardiologist in the department of cardiology,
Nevertheless, the supply of donors limits the procedure. The
City Hospital, Birmingham; G Jackson is consultant cardiologist in the
Eurotransplant database (19905) indicates that 25% of patients
department of cardiology at Guy’s and St Thomas’s Hospital, London.
listed for transplantation die on the waiting list, with 60%
receiving transplants at two years (most within 12 months).
The ABC of heart failure is edited by C R Gibbs, M K Davies, and
Although ventricular assist devices may be valuable during the
G Y H Lip. CRG is research fellow and GYHL is consultant
wait for transplantation, the routine use of xenotransplants is
cardiologist and reader in medicine in the university department of
unlikely in the short or medium term.
medicine and the department of cardiology, City Hospital,
Birmingham; MKD is consultant cardiologist in the department of
The graph showing cardiac transplantations worldwide is adapted with
cardiology, Selly Oak Hospital, Birmingham. The series will be
permission from Hosenpud et al (J Heart Lung Transplant 1998;17:6568).
published as a book in the spring.
The table showing survival rates is adapted from Hobbs (Heart 1999;
82(suppl IV):IV810).
BMJ 2000;320:55962
36
ABC of heart failure
Heart failure in general practice
F D R Hobbs, R C Davis, G Y H Lip
Management of heart failure in general practice has been
Heart failure affects at least 20 patients
hampered by difficulties in diagnosing the condition and by
on the average general practitioner’s list
perceived difficulties in starting and monitoring treatment in
the community. Nevertheless, improved access to diagnostic
testing and increased confidence in the safety of treatment
should help to improve the primary care management of heart
failure. With improved survival and reduced admission rates
(achieved by effective treatment) and a reduction in numbers of
hospital beds, the community management of heart failure is
likely to become increasingly important and the role of general
practitioners even more crucial.
Clinical assessment of patient,
history, and hospital records
together suggest heart failure
Diagnostic accuracy
Heart failure is a difficult condition to diagnose clinically, and
No
Echocardiography shows
Yes
Heart failure: start
hence many patients thought to have heart failure by their
moderate or severe left
angiotensin converting
general practitioners may not have any demonstrable
ventricular dysfunction?
enzyme inhibitor
abnormality of cardiac function on objective testing.
A study from Finland reported that only 32% of patients
Not available
suspected of having heart failure by primary care doctors had
Yes
definite heart failure (as determined by a clinical and
Yes
Documented previous
Probability of heart
radiographic scoring system). A recent study in the United
myocardial infarction?
failure high: are you
Kingdom showed that only 29% of 122 patients referred to a
confident of diagnosis?
“rapid access” clinic with a new diagnosis of heart failure fully
No, inconclusive,
met the definition of heart failure approved by the European
or not known
Society of Cardiology—that is, appropriate symptoms, objective
Electrocardiogram abnormal?
Yes
evidence of cardiac dysfunction, and response to treatment if
(Q waves, left bundle
doubt remained.
branch block)
Similar findings have been reported in the
No
echocardiographic heart of England screening (ECHOES)
No, inconclusive,
or not known
study, in which only about 22% of the patients with a diagnosis
of heart failure in their general practice records had definite
Chest x ray film shows
Yes
impairment of left ventricular systolic function on
pulmonary congestion
echocardiography, with a further 16% having borderline
or cardiomegaly?
impairment. In addition, 23% had atrial fibrillation, with over
half of these patients having normal left ventricular systolic
No, inconclusive,
or not known
contraction. Finally, a minority of patients may have clinical
heart failure with normal systolic contraction and abnormal
No
Yes
Heart failure
Remaining unexplained
Refer for further
diastolic function; management of such patients with diastolic
unlikely
indication of heart failure?
investigation
dysfunction is very different from those with impaired systolic
function.
Diagnostic algorithm for suspected heart failure in primary care. Based on
guidance from the north of England evidence based guideline development
project (see key references box)
Open access echocardiography and
diagnosis
Owing to the noninvasive nature of echocardiography, its high
acceptability to patients, and its usefulness in assessing
ventricular size and function, as well as valvar heart disease,
many general practitioners now want direct access to
echocardiography services for their patients. Although open
Recent studies have shown that with
access echocardiography services are available in some districts
appropriate education of general
in Britain, many specialists still have reservations about
practitioners the workload of an open
introducing such services because of financial and staffing issues
access echocardiography service can be
manageable
and concern that general practitioners would have difficulty
interpreting technical reports. The cost of echocardiography
(£50 to £70 per patient) is relatively small, however, compared
with the cost of expensive treatment for heart failure that may
not be needed. The cost is also small compared with the costs of
37
hospital admission, which may be avoided by appropriate, early
treatment of heart failure.
One approach may be to refer only patients with abnormal
Open access services have proved
baseline investigations as heart failure is unlikely if the
popular and are likely to become even
electrocardiogram and chest x ray examination are normal and
more common; indeed,
there are no predisposing factors for heart failure—for example,
echocardiographic screening of patients
previous myocardial infarction, angina, hypertension, and
in the high risk categories may well be
diabetes mellitus. Requiring general practitioners to perform
justified and cost effective
electrocardiography and arrange chest radiography, as a
complement to careful assessment of the risk factors for heart
failure, is likely to reduce substantially the number of
inappropriate referrals to an open access echocardiography
service.
Role of natriuretic peptides
Given the difficulties in diagnosing heart failure on clinical
grounds alone, and current limited access to echocardiography
and specialist assessment, the possibility of using a blood test in
Sensitivity and specificity of brain natriuretic peptides in
general practice to diagnose heart failure is appealing.
diagnosis of heart failure
Determining plasma concentrations of brain natriuretic
peptide, a hormone found at an increased level in patients with
New diagnosis of
left ventricular systolic dysfunction, may be one option. Such a
heart failure
Left ventricular
blood test has the potential to screen out patients in whom
(primary care)
systolic dysfunction
heart failure is extremely unlikely and identify those in whom
Sensitivity
97%
77%
the probability of heart failure is high—for example, in patients
Specificity
84%
87%
with suspected heart failure who have low plasma
Positive predictive
concentrations of brain natriuretic peptide, the heart is unlikely
value
70%
16%
to be the cause of the symptoms, whereas those who have
higher concentrations warrant further assessment.
Primary prevention and early detection
General practitioners have a vital role in the early detection and
treatment of the main risk factors for heart failure—namely,
Other cardiovascular disease
Detect and treat hypertension
prevention strategies
hypertension and ischaemic heart disease—and other
(eg avoid smoking, lipid lowering)
cardiovascular risk factors, such as smoking and
hyperlipidaemia. The Framingham study has shown a decline in
hypertension as a risk factor for heart failure over the years,
Prevent progression to
which probably reflects improvements in treatment. Ischaemic
symptomatic heart failure
heart disease, however, remains very common. Aspirin, â
blockers, and lipid lowering treatment, as well as smoking
Angiotensin converting enzyme
cessation, can reduce progression to myocardial infarction in
inhibitors in asymptomatic left
patients with angina, and â blockers may also reduce ischaemic
ventricular dysfunction
left ventricular dysfunction. Early detection of left ventricular
dysfunction in “high risk” asymptomatic patients—for example,
Strategies for preventing progression to symptomatic heart failure in high
those who have already had a myocardial infarction or who
risk asymptomatic patients
have hypertension or atrial fibrillation—and treatment with
angiotensin converting enzyme inhibitors can minimise the
progression to symptomatic heart failure.
Starting angiotensin converting enzyme inhibitors in chronic
heart failure in general practice
Starting and monitoring drug treatment
x Measure blood pressure and determine electrolytes and creatinine
Both hospital doctors and general practitioners used to be
concentrations before treatment
concerned about the initiation of angiotensin converting
x Consider referring “high risk” patients to hospital for assessment
enzyme inhibitors outside hospital. It is now accepted, however,
and supervised start of treatment
x Angiotensin converting enzyme inhibitors should be used with
that most patients with heart failure can safely be established on
some caution in patients with severe peripheral vascular disease
such treatment without needing hospital admission. The
because of the possible association with atherosclerotic renal artery
previous concern—over first dose hypotension—was heightened
stenosis
by the initial experience of large doses of captopril, especially in
x Doses should be gradually increased over two to three weeks,
those with severe heart failure, who are at greater risk of
aiming to reach the doses used in large clinical trials
problems. Patients with mild or moderate heart failure, who
x Blood pressure and electrolytes or renal chemistry should be
monitored after start of treatment, initially at one week then less
have normal renal function and a systolic blood pressure over
frequently depending on the patient and any abnormalities
100 mm Hg and who have stopped taking diuretics for at least
detected
24 hours rarely have problems, especially if the first dose of an
38
angiotensin converting enzyme inhibitor is taken at night,
before going to bed.
Conditions indicating that referral to a specialist is necessary
x Diagnosis in doubt or when specialist investigation and
management may help
Heart failure clinics
x Significant murmurs and valvar heart disease
x Arrhythmias—for example, atrial fibrillation
Dedicated heart failure clinics within general practices, run by a
x Secondary causes—for example, thyroid disease
doctor or nurse with an interest in the subject, have the
x Severe left ventricular impairment—for example, ejection fraction
< 20%
potential to improve the care of patients with the condition, as
x Preexisting (or developing) metabolic abnormalities—for example,
they have for other chronic conditions, such as diabetes.
hyponatraemia (sodium < 130 mmol/l) and renal impairment
Blood should be taken for electrolytes and renal chemistry
x Severe associated vascular disease—for example, caution with
at least every 12 months, but more frequently in new cases and
angiotensin converting enzyme inhibitors in case of coexisting
when drug treatment has been changed or results have been
renovascular disease
abnormal. The clinics should be used to educate patients about
x Relative hypotension (systolic blood pressure < 100 mm Hg before
their condition, particularly in relation to their treatment, with
starting angiotensin converting enzyme inhibitors)
x Poor response to treatment
messages being reinforced and drug treatment simplified and
rationalised where appropriate. Patients whose condition is
deteriorating may be referred for specialist opinion.
Variables that should be monitored in patients with
established heart failure comprise changes in symptoms and
severity (New York Heart Association classification); weight;
Examples of topics for audit of heart failure management in
blood pressure; and signs of fluid retention or excessive diuresis.
general practice
Means of diagnosis
Has left ventricular function been assessed, by echocardiography or
Impact of heart failure on the
other means?
Appropriateness of treatment
community
Are all appropriate patients taking angiotensin converting enzyme
After a patient is diagnosed as having heart failure, substantial
inhibitors (unless there is a documented contraindication)? Have
doses been increased where possible to those used in the large clinical
monitoring by the general practitioner is required. In our
trials?
survey of heart failure in three general practices from the west
Monitoring treatment
of Birmingham, 44% of general practice consultations (average
Were blood pressure and renal function recorded before and after
2.6 visits per patient) took place within three months of the first
start of angiotensin converting enzyme inhibitors, and at intervals
diagnosis of heart failure, 23% were at three to six months (1.4
subsequently?
visits per patient), and 33% were at six to 12 months (2.0 visits
per patient). Such management requires regular supervision
and audit.
Relevance to hospital practice
Causes of readmission in patients with heart failure
In our survey of acute hospital admissions of patients with heart
x Angina
failure to a city centre hospital, the median duration of stay was
x Infections
8
(range 196) days, with 20% inpatient mortality. Clinical
x Arrhythmias
variables associated with an adverse prognosis include the
x Poor compliance
presence of atrial fibrillation, poor exercise tolerance, electrolyte
x Inadequate drug treatment
abnormalities, and the presence of coronary artery disease.
x Iatrogenic factors
Angiotensin converting enzyme inhibitors were prescribed in
x Inadequate discharge planning or follow up
x Poor social support
only 51% of heart failure patients on discharge; after the first
diagnosis of heart failure, the average number of hospital
attendances (inpatient and outpatient) in the first 12 months
was 3.2 visits per patient, with an average of 6.0 general practice
consultations per patient. However, 44% of hospital attendances
(1.4 visits per patient) took place within three months of
diagnosis, 33% were at three to six months (1.0 visits per
Admissions with heart failure over six months to a district
patient), and 23% were at 612 months (0.74 visits per patient).
general hospital serving a multiracial population
These figures represent the collective burden of heart failure
on hospital practice. Indeed, about 200 000 people in the
Presentation (%)
Associated medical history (%)
United Kingdom require admission to hospital for heart failure
Pulmonary oedema (52) Ischaemic heart disease (54)
each year.
Congestive heart failure,
Hypertension (34)
with fluid overload (32)
Myocardial infarction
Valve disease (12); previous stroke (10)
Specialist nurse support
and heart failure (9)
The important role of nurses in the management of heart
Associated atrial
Diabetes mellitus (19); peripheral vascular
failure has been relatively neglected in Britain. In the United
fibrillation (29)
disease (13); cardiomyopathy (1)
States the establishment of a nurse managed heart failure clinic
Population of 300 000 (7451 admissions; 348 (5%) had heart failure (mean age
in South Carolina resulted in a reduction in readmissions of 4%
73 years)).
39
and in length of hospital stay of almost two days. In another
North American study a comprehensive, multidisciplinary
100
Home based intervention (n=49)
approach to heart failure management, including supervision
Usual care (n=48)
by nurses, resulted in a significant (56%) reduction in
90
readmissions and hospital stay, with a trend towards reduced
mortality. Quality of life scores also improved in the
80
intervention group. A more dramatic result was obtained in a
study from Adelaide, Australia, where multidisciplinary
intervention resulted in a 20% reduction in mortality.
70
Nurse management of heart failure has implications for the
provision of care in patients with chronic heart failure, sharing
60
the increasing burden of heart failure. Specialist nurses would
P= 0.049
provide advice, information, and support to patients with heart
failure and to their families and would ensure that the best
500
4
8
12 16 20 24 28 32 36 40 44 48 52 56 60 64 68 72 76 80
treatment is given. The potential benefits are substantial, with
Week of study follow up
reduced hospital admission rates, improved quality of life, and
lower costs.
Cumulative survival curves from the Adelaide nurse intervention study: 18
month follow up (see Stewart et al, key references box at end of article)
Economic considerations
With an increasingly elderly population, the prevalence of heart
Economic cost of heart failure to NHS in UK, 19901
failure could have increased by as much as 70% by the year
Total cost (£m)
% of total cost
2010. Heart failure currently accounts for 12% of total
spending on health care in Europe and in the United States. In
General practice visits
8.3
2.5
1993 in the United Kingdom, heart failure cost the NHS
Referrals to hospital from
8.2
2.4
£360m a year; the figure now is probably closer to £600m,
general practice
equivalent to 12% of the total NHS budget, and hospital
Other outpatient attendances
31.8
9.4
admissions account for 6070% of this expenditure. Admissions
Inpatient stay
213.8
63.5
for heart failure have been increasing and are expected to
Diagnostic tests
45.6
13.5
increase further. Preventing disease progression, hence
Drugs
22.1
6.6
reducing the frequency and duration of admissions, is therefore
Surgery
7.2
2.1
an important objective in the treatment of heart failure in the
future.
Total
337.0
100
Heart failure is likely to continue to
Educating patient and family
Promoting long term compliance
become a major public health problem in
the coming decades; new and better
management strategies are necessary,
including risk factor interventions, for
Nurse specialising
patients at risk of developing heart
in heart failure
failure
Monitoring weight and blood tests
Implementing treatment algorithms
(renal chemistry and electrolytes)
Key references
Role of specialist nurse in management of patients with heart failure
x Eccles M, Freemantle N, Mason J, for the North of England
Guideline Development Group. North of England evidence based
development project: guideline for angiotensin converting enzyme
The table on sensitivity and specificity is based on information in Cowie et
inhibitors in primary care management of adults with symptomatic
al (Lancet 1997;350:134953) and McDonagh et al (Lancet 1998;351:913).
heart failure. BMJ 1998;316:136975.
The table showing admissions with heart failure to a district general
x Francis CM, Caruana L, Kearney P, Love M, Sutherland GR, Starkey
hospital is adapted with permission from Lip et al (Int J Clin Prac 1997;51:
IR, et al. Open access echocardiography in the management of
2237). The table showing the economic costs of heart failure is published
heart failure in the community. BMJ 1995;310:6346.
with permission from McMurray et al (Eur Heart J 1993;14(suppl):133).
x Lip GYH, Sarwar S, Ahmed I, Lee S, Kapoor V, Child D, et al. A
survey of heart failure in general practice. The west Birmingham
R C Davis is clinical research fellow and F D R Hobbs is professor in
heart failure project. Eur J Gen Pract 1997;3:859.
the department of primary care and general practice, University of
x Remes J, Miettinen H, Reunanen A, Pyorala K. Validity of clinical
Birmingham.
diagnosis of heart failure in primary health care. Eur Heart J
1991;12:31521.
The ABC of heart failure is edited by C R Gibbs, M K Davies, and
x Rich MW, Beckham V, Wittenberg C, Leven CL, Freedland KE,
G Y H Lip. CRG is research fellow and GYHL is consultant
Carney RM, et al. A multidisciplinary intervention to prevent the
cardiologist and reader in medicine in the university department of
readmission of elderly patients with congestive heart failure. N Engl
medicine and the department of cardiology, City Hospital,
J Med 1995:333:11905.
Birmingham; MKD is consultant cardiologist in the department of
x Stewart S, Vandenbroek AJ, Pearson S, Horowitz JD. Prolonged
cardiology, Selly Oak Hospital, Birmingham. The series will be
beneficial effects of homebased intervention on unplanned
published as a book in the spring.
readmissions and mortality among patients with congestive heart
failure. Arch Intern Med 1999;159:25761.
BMJ 2000;320:6269
40