Chapter4 The Anterior Compartmen49
Urethra
On translabial imaging, te urethra is evident as a vertical hypoechoic area
(see Figures 1…4.4). This ea is thoughtto include mucosa, vascular
plexus, and the urethral smooth musculature. Its hypoechoic appearance
is largely attributable to the fact that mucosal layers and smooth muscula-
ture run parallel to the incident beam (seeChapter 2). This is evident
wheneverthere is signi“cant urethral rotation, bcausea more perpendicu-
lar orientation of the urethra relative to the incident beam makes the struc-
ture more isoechoic and therefore less evident. The urethral rhabdosphincter
surrounds this hypoechoic structure and appears as a double hyperechoic
stripe on translabial ultrasound at rest, ventral and dorsal of the urethra
proper. Its appearance seems to vary markedly depending on the approach
used, i.
44 transrectal45 or translabial/perineal.
Recent improvements in tissue discrimination have made ide
cation
much easier (seFigure 4.9).
In general, the rhab
sphincter seems more obvious in the axial com-
pared with the midsagittal plane, as evident from Figures 6.2 and 6.5…6.9
in Chapter 6. Thisis at least partly attributable to the relative ease with
which the human eye recognizes ring structures, a legacy of hundreds of
millions of years of predator…prey relationships. Clearly, a number of
authors, incuding this one, havm isinterpreted “ndings in the past.35 On
principle, intraurethral ultrasound with transducers de
loped for intra-
vascular imaging should help in id
tifying urethral morphology and h
lp
us determine what exa
y we are imaging. Several authors used such
44,46,47
48 con“ rming that the
rhabdosphincter often shows sonograp
evidence of impaiment in stress
incontinent women, both in the sen
of reduced contra
ility as well as
changes in
hogenicity and integrity.48 However, the very limited avail-
ability of such transduers means that these techniques are unlikely to
enter clinical practice in the near future.
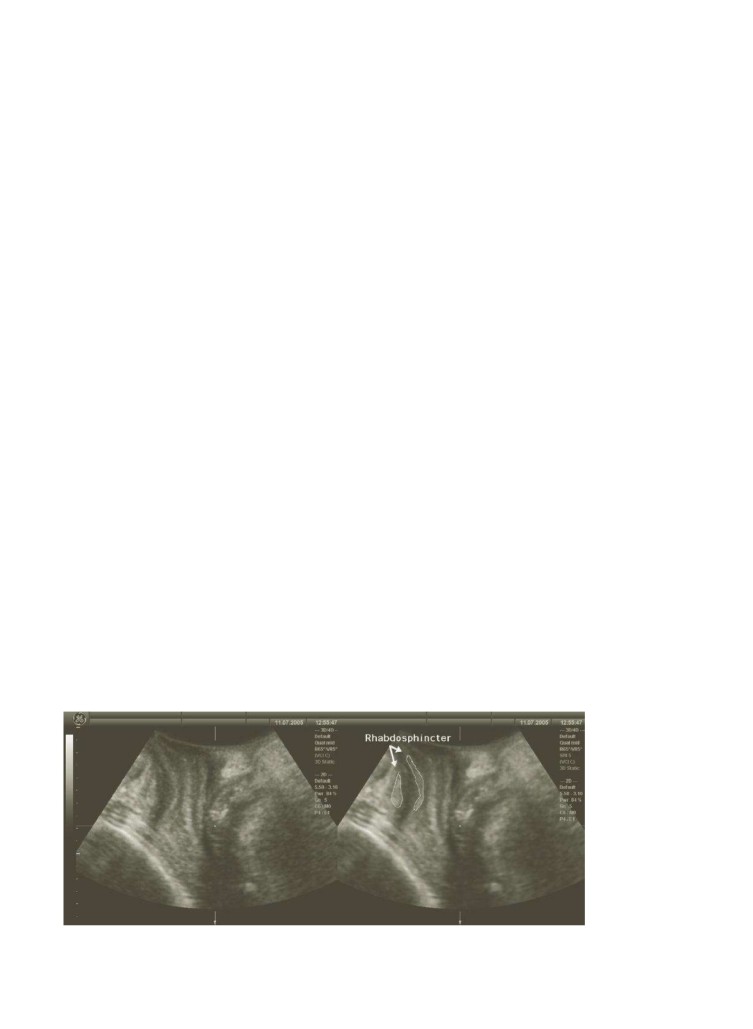
Figure 4.9The urethral rhabh
ncter as imaged in the midsagittal plane (native imaging, left image) and on speckle reduction
imaging (right image). Improved tissue discrimination allows recognition of a structure that is oth
50 H.P. Dietz
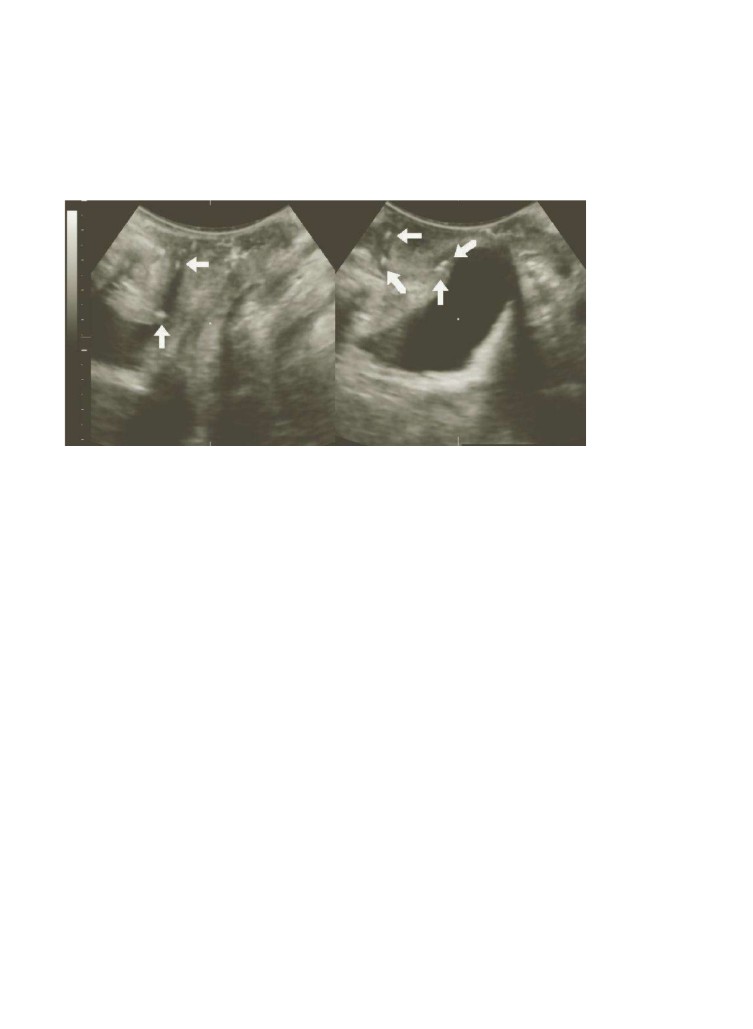
Figure 4.10Hyperechoic urethral foci (ar
a patient with mixed urinary incontinence, a second-degree cystocele, and USI.
Office cyst
throscopy was n
. The foci are more evident on Valsalva (right image).
On translabial sanning at rest,the rhabdosphinctr appears hypere-
choic as the incidnt beamis perpendicular to those “bers. On tansvaginal
ultrasound, p
rts of this circular or near-circular structure are vertical to
the incident beam, others ae parallel, and this has resulted in spurious
“ ndings, lea
ing some authors toconclude that the rhabdosphincter is
48
The resolution of curretly used transduers for translabial imaging is
insuf“ cient to allow more than a global ass
ment of the dimensions of
the urethra,but occasionally abnor
alities such as st
osis or diverticula
may beseen.49 Although there have been attempts at quantitative assess-
50,51
the above-mentined artifacts
make the data ob
ined by this methodologysomewhat susp
t. To date,
no quantitative assessment of the urethr
rhabdosphincter as seen on
translabial ultrasound seems to ha
been undertaken, probably because
of resolution issues.
Hyperechoic foci withinthe urethra (see Figur4.10) are cmmon, may
be isolatedor multiple, and probably are attributable to cal
ed urethral
glands. Thee seems to be no association between symptoms or lower
urinary tract conditions andthe presence ofsuch foci.52
Bladder Wall Thickness
There has recentlb een renewedinterest in the quanti“cation of bladder
wall or detrusor wall thickness (BWT orDWT) by transvaginal and/or
translabial ultrasound.53,54 Measurements are obtained after bladder emp-
tying and perpendicular to the mucosa, leading edge to leading edge (see
Figure 4.11), close to the midline as ide
ed by the urehra and bladder
neck. Originally, three sites were assessed by transvaginal ultrasound: ante-
rior wall, trigone, and dome of the bladder, and the mean of all three was
calculated. The author b
eves thatthe trigone (because it io f different
Chapter4 The Anterior Compartmen51
embryologic origin) is dif“cult to justify as a measurement location
compared withthe dome. In addition, there often is marked variation in
trigonal thicknessbetween the bladder neck and the interureteric ridge.
Another approach, currently used by the author, is to measure three sites
on the dome, wich can be performed either by translabial/introital or
by transvaginal ultrasound. Above a bladd
lling of 50 mL, DWT starts
53 which is why in urogynecol
y measurements are usually
undertaken after bladder emptying. DWT measurement by translabial
ultrasound seems tobe highly reproducible, withan intraclass correlation
of 0.82 (CI0.63…0.91) fou
in a series o6 7 patients.55
A DWT of more than 5 mm seems to be associated with detrusor overactiv-
57 In our own data, DWT
is clearly higherin women with symptoms of urge incontinence and urody-
namically proven detrusoo veractivity, but the strength of the association
seems insufcient to beof much use in clinical practice.58 IncreasedDWT is
likely the result of hypertrophy of the detrusor muscle, which is most evident
at the dome;this may be the cause of symptomor simply the effect of an
underlying abnormality.Although DWT onits own seems only moderately
predictive of d
trusor overactivity, the methom ay be clinicallyuseful when
combined with symptoms ofthe overactive badder.59 In young women, DWT
55
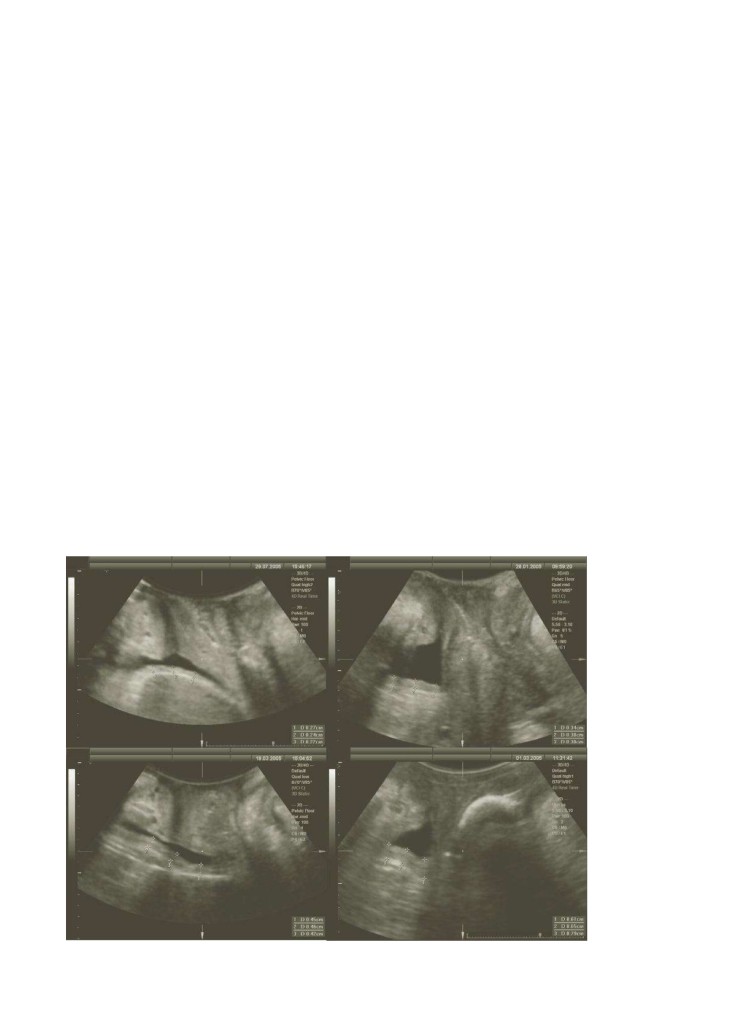
Figure 4.11DWT as
sured at the d
after bladder emptying: mean DWT is 2.5 (top left), 3.7 (top right), 4.4 (bottom left),
and 6.8 (bottom right). Measurements of 5 mm and above are associated with symptoms and signs of detrusor overactivity.
52
H.P. Dietz
60 which supports
the hypothesis that increased DWT is indicative of acquired detrusor
hypertrophy, and probably the result of yars or deades of isometric con-
tractions against a cl
ed outlet. This is
so supported by the “nding that
a history of nocturnal enuesis in childhood is
sociated with increased
61 which implies
that, at least in sme women, increa
d DWT is attributable to an underly-
ing disorder that is either congenial or acquired in early chidhood.
Recently, DWT was shown to be a predictor of de novo detrusor overactivity
62 It is likely but remains to be proven that
determination of this parameter can contribute to the workup of a patient
with pelvic ”oor and bladder dysfunction, e.g., as a predictor of postopera-
tive voiding function or de novo/
orsened symptoms of the irritable
bladder. See also Appendix Case 3 for increased DWT in a young patient
with symptoms ofurgency, frequency, and urge incontinence.
LevatorAc
ivity
Perineal ultrasound has
en used for the quantication of pelvic ”oor
muscle function, both inwomen with stress in
ntinence and continent
controls,63 as well as before and after childbir646,5 A cranioventral shift
of pelvic organs image
in the midsagittal plane is taken as evidence of a
levator contraction. The resulting displacement of the internal urethral
Figure 4.12A pelvic floor muscle contraction as documented by translabial ultrasound in the midsagittal plane. The left image
shows findings at rest; the right demonstrates cranioventral displacement of the bladder neck at man-mal pelvic floor muscle co
traction. (From ziHP, Ultrasound Imaging of the pelvic floor: 2D aspects. Ultrasound Obstet Gynaecol 2004; 23: 80…92, with
permission.)
Chapte4 The Anterior Compartmen53
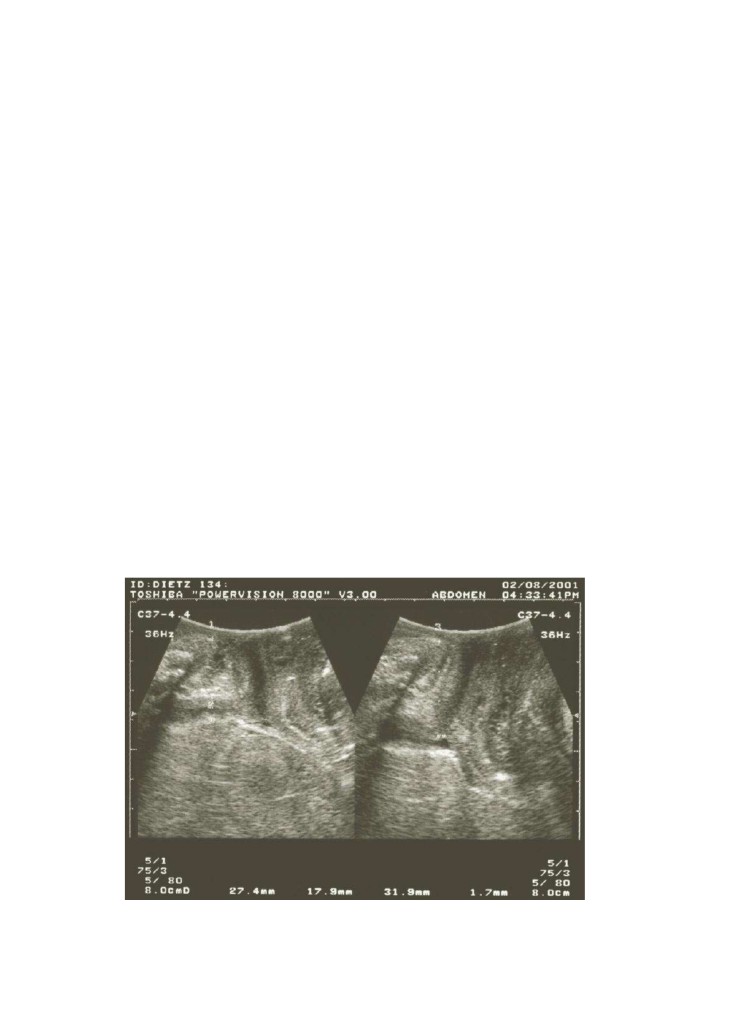
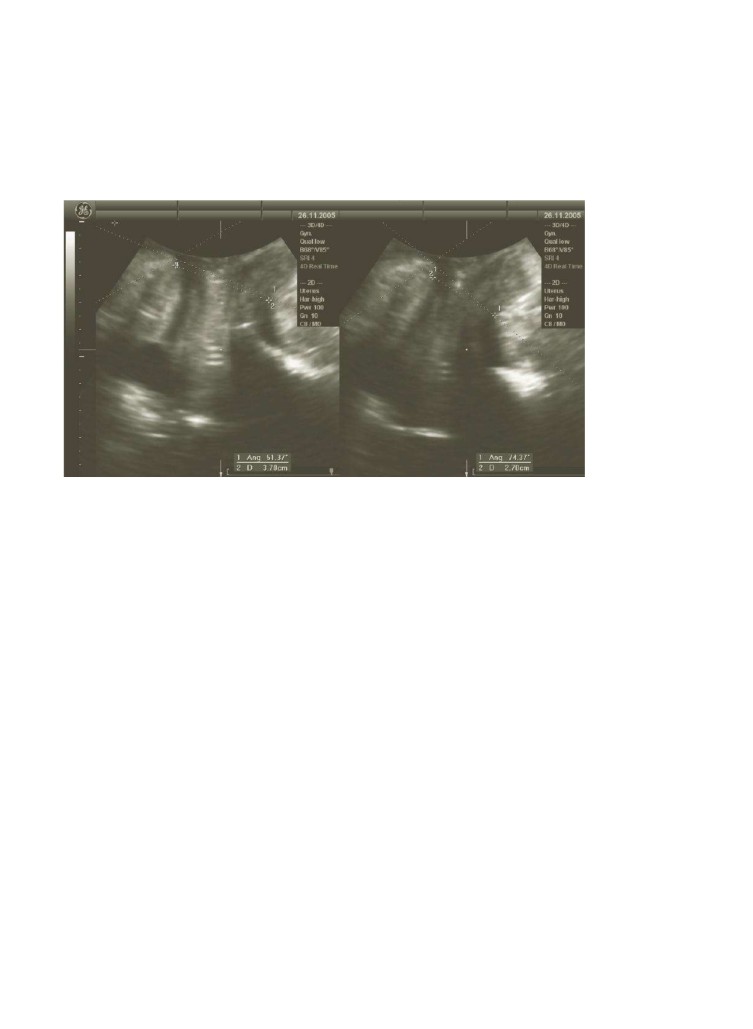
Figure 4.13Quantification of pelvic floor
ontraction by measuring the reduction in hiatal dimensions (from 37 to 27 mm,
i.e., by 10 mm) or the increase in levator plate angle (from 51.37 to 74.37°, i.e., by 23°) on max
raction.
meatus is measured rel
ve to the inferoposterior symphyseal margin (see
Figure 4.12).
se 2b o
the Appendix demo
trates apelvic ”oor contrac-
tion in a healthy nulliparous volunteer.
Another means of quantifying levator activity is to measure reduction of
the levator hiatus in the midsagittal plane, or to determine the changing
angle of the hiatal plane (the •levator plate angleŽ) relative to the central
symphyseal axis (s
Figure 4.13). Narrowing
the hiatus without cranio-
ventral displacement of the bladder neck implies that the patient has
increased intraabdominal pressure weilcontracting the levator ani. This
is a common poblem and should be corrected by teaching proper tech-
7
Translabial ultrasound oservation of pelvic ”oor activity has hlped
validate the concept of hte knack,Ž e.., of a re”ex levator contraction
immediately before increases in intraabdominal pressure such as those
resulting from coughing.68 Correlations between cr
ioventral shift of the
bladder neck on the one hand and palpation/perineometry on the other
hand have been
own to begood.69 More recently, physiotherapists have
begun to ue transabdominal and translabial ultrasound to document
pelvic ”oor muscle activit, with one author concluding that the translabial
technique70 is probably more accurate for this indication.
Prolapse
antification
1,72
The inferior marginof the symphyss pubis serves as a convenient (if imper-
fect) line of reference against which the maximal descent of bladder, uterus,
cul-de-sac, and rectal
pulla on Valsalva ma
uver can be measured
54 H.P. Dietz
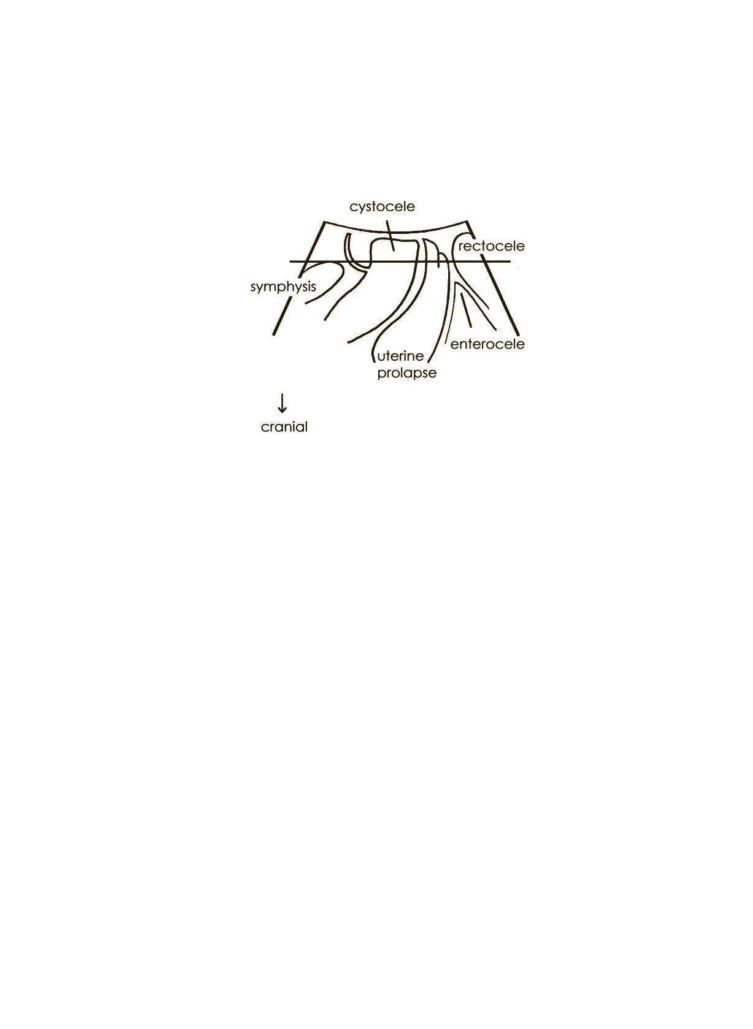
Figure 4.14Prolapse quacaition as demonst
in a schematic drawing of ultrasound find-
ings in the midsagittal plane. The inferior margin of the symphysis pubis is used as reference line.
(From DzeHP, Ultrasound Imaging of the pelvic floor: 2D aspects. Ultrasound Obstet Gynaecol 2004;
23: 80…92, with permission.)
(Figure 4.1) (see also Chapter 5 for uterine and posterior compartment
prolapse). Because the hu
s on Valsalva is gen
lly too large … especially
in women with proapse … to allow for simultaneous imaging of the entire
symphysis pubis and the posterior compartment, it is often not possible to
3 as refer-
ence for descent of a rectocele or enterocele. Needless to say, procidentia or
complete vaginal eversion generally preclude translabial imaging.
The main ue of imaging for prolapse quantc“ation may prove to be in
outcome assessmentter pelvic reconstuctive surgery, bth clinically and
for research. The elevation (and frequently distortion) of the bladder neck
74,75
(see Figure 4.15 and
Cases 7,
and 14 of the Appendix). Fascial and synthetic slings are visible
posterior to the trigone or the urethra (see Chapter 7 and Cases 11 and 14 of the
Appendix). Bulking agentsuch as Mcroplastique show up anterior, lateral,
and posterior to the proximal urethra (see Chapter 7). It has been demon-
strated that overel
ation of the bladder neck on colposuspension is unneces-
sary for cure ofUSI, and elev
ion may also have a bearing on postoperative
symptoms of voiding dsfunction and de novo detrusor overactivi74.,75
Other Findings
Residual urine can conveniently be determined at the time of a routine
translabial pelvic ”oor assessmeņtalthough the formula used for this
purpose was developed for transvaginal ultrasound and has not yet been
formally validated for translabial use. It my be necessary to let the patient
perform a mild Valsalva maneuver to allow the most ventral part of the
dome to rotate downward. The two largest diameters are measured perpen-
dicular to each othr (see Figure 4.16), and the result in centimeters is
6,77
multiplied by 5.9. Deducting 14.9
according
to the formula X * Y * 5.
Š 14.9= residual volumein milliliters.
Chapter4 The Anterior Compartmen55
Figure 4.15Immobilization of the bladder neck after successful Burch colposuspension, resulting in less than 6 mm of BND on
Valsalva.eTarrows indicate the point of reference, i.e., the inferoposterior margin of the symphysiU
ltra-
sound Imaginof the pelvic floor: 2D
s. Ultrasound O
Gynaecol 2004; 23: 80…92, with permission.)
Figure 4.16Determination of resid
ne volume on translabial ultrasound. The two largest
bladder diameta
e measured perpendicular to each other and multiplied by 5.9. Deducting 14.9
gives residual urine volu
illimeters, in this case resulting in 4.31 Š 1
4.9= 28 mL.
56
H.P. Dietz
A range of other abnormalities, incidental or expected, may at times be
imaged on translabial ultrasound, alth
gh a full pelvic ultrasound assess-
ment does ofcourse requirea transvaginal approach.Urethral divertic-
ula78,79 (see Figure
4.17) er unlikely to be missed, especially if the
examination is perormed after the patient voids, and if care is taken to
inspect the paraurethral areas. Most are located dorsal to the urethra as in
Figure 4.17, but occasionally one may be found ventral or anterior to the
urethra, i.e., developing into the s
e of Retzius,as in Case 15 of the
Appendix. The main differential diagnosis is Gartner cysts, i.e., a cystic
remnant of the Wolf“an duct located in the vaginal wall (seeFigure 4.18
and Case9 of the Appendix), but it is generally possible to differentiate the
two becaue of their location relative to the urethra. In addition, urethral
diverticula are more likely to be symptomatic and tender on examination,
and often appear rather complex showing a convoluted or multicystic struc-
ture, often with internal echogenicity. Both urethral diverticula and Gartner
cysts may occasionally be confused with a nabothian follicle, but correct
identi“ cation of the cervixwill make such a mi
ake highly unlikely. A
Valsalva maneuvew ill lead to differential movement of the tissues and
help in correctly attributing cystic structures to the vginal walļ cervix,
bladder, or urethra.
Finally, labial cysts may be detected close to the transducer surface in
parasagittal planes, and the odd vagin
broma may cause circumscribed
isoechoic “ ndings within the vaginal wall. Occasionally, a bladder tumor
may be found (Figure 4.19), and intravesical stents and bladder diverticula
Figure 4.17Urethral diverticulum mimicking a cystourethrocele as seen on the right image taken on maximal Valsalva. The neck
of the diverticulum was situated close to the bladder neck, and this was confirmed on surgical exp
ra-
sound Imaginof the pelvic floor: 2D
s. Ultrasound O
Gynaecol 2004; 23: 80…92, with permission.)
Chapte4 The Anterior Compartmen57
Figure 4.18Gartner d
cyst (arrowose to the bladder neck and cervix. (From Dietz HP, Ultra-
sound Iaging of the pelvic flo
aspects. Ultrasound Obna
ecol 2004; 23: 80…92, with
permission.)
Figure 4.19Transitional carlccinoma (arrow) of the bladder, an incidental finding on translabial
ultrasound performesyfmrptoms of stres
ntinence. (From Dietz HP, Ultrasound Imaging of
the pelvic floor: 2D aspects. UltrasetG
ynaecol
; 23: 80…92, with permission.)
58 H.P. Dietz
Figure 4.20Hematoma surrounding mesh after l
ic sacropolpexy (large arrow). There
is a second, smaller hematoma under a posterior colporrhaphy (small arrow). The patient was exam-
ined because of persistent postoperative voiding difficulty and pain. (From Dietz HP, Ultrasound
Imaging of the pelvic floor: 2D aspaso
und Obstet
aecol 2004; 23: 80…92, with
permission.)
can also bevisualized.38 Postoperative hmatomata may be visible after
vaginal surgey or suburethral slings and at times explain clinical symp-
toms such as voiding dysfunction
persistent pain (ee Figure 4.20).
References
1. Schaer GN, Koe
i OR, Schuessler B, Haller U. Perineal ultrasound: determi-
nation of reliable examination procedures. Ultrasound Obstet Gynecol 1996;
7(5):347…352.
2. Dietz HP, Wilson PD. Anatomical assessment of the bladder outlet and proxi-
mal urethra using ultrasoundand videocystourethrogrphy. Int Urogynecol J
1998;9(6):365…369.
3. Dietz HP, Wilson PD. The i
uence of blad
r volume on the position and
mobility of the urethrovesical junction. Int Urogynecol J 1999;10(1):3…6.
4. Dietz HP, Clarke B. The inuence of posture on perineal ultrasound imaging
parameters. Int UrogynecolJ 2001;12(2):104…106.
5. Alper T, Cetinkaya M, Okutgen S, Kokcu A, Lu E. Evaluation of urethrovesical
angle by ultrasound in women with and without urinary stress incontinence.
Int UrogynecolJ 2001;12(5):308…311.
6. Martan A, Masata J, Halaska M, Voigt U. ltrasound imaging of the lower
urinary system in womenafter Burch colposuspension. Ultrasound Obstet
Gynecol 2001;17(1):58…64.
7. Dietz HP, Clarke B, Herbison P. Bladder neck mobility and urethral closure
pressure as predictors of genuine stress incontinence. Int Urogynecol J 2002;
13(5):289…293.
Chapte4 The Anterior Compartmen59
8. Dietz HP, Eldridge A, Grace M, Clarke B. Test-retest reliability of the ultrasound
assessment of bladder ck mobility. Int UrogynecolJ 2003;14(S1):S57…S58.
9. Reed H, Watereld A, Freema
RM, Adekanmi OA. Bladder neck mobility in
continent nulliparous women: normal references. Int Urogynecol J 2002;13(suppl
1):S4.
10. Brandt FŢ Albuquerque CD, Lorenzato FR, Amaral FJ. Perineal assessment of
urethrovesical junction mbility in young continent females. Int Urogynecol J
2000;11(1):18…22.
11. PescherU M, Fanger G,
haer GN, Vod
sek DB, DeLancey JO, Schuessler B.
Bladder neck mobilityin continent nulliparous womn. Br J Ob
et Gynaecol
2001;108
):320
324.
12. Dietz HP, Eldridge A, Grace M, Clarke B. Pelvic organ descent in young nulli-
gravid women. AmJ Obstet Gynecol 2004;191:95…99.
13. Oerno A, Di
z HP. Levator co-activation is an important confounder of pelvic
organ descent on Valsalva. ICS Annual SciectM“ eeting 2006, Christchurch,
New ZealandA bstract.
14. van der Velde J, Laan E, Everaerd W. Vaginismus, a component of a general
defensive reaction. An investigation of pelvio or muscle activity during expo-
sure to emotion-inducing “ lm excerpts in women
th and without vaginis-
mus. Int UrogynecolJ 2001;12(5):328…331.
15. King JK, Fr
man RM. Is ante
tal bladder neck mobility a risk factor for
postpartum stress incontinence? Br J Obstet Gynaecol 1998;105(12):1300…
1307.
16. Martan A, Msata J, HalaskM , KasikovaE, Otcenasek M,
igt R. The effect
of increasing of intraabdominal pressuron the position ofthe bladder neck
in ultrasound imaging. Annual Meeting, International Continence Society
2001, Seoul,South Korea.Abstract.
17. Fritel X, Zbak K, Pigne A, Demaria F, Bena” JL. Predictive value of urethral
mobility before suburethral tape proc
ure for urinary stress incontinence in
women. J Urol 2002;168(6):2472…2475.
18. Liapis A, Ba
s P, Lazris D, CreatsaG. Tension-free vaginal tape in the man-
agement of recurrent stress incontinence. Arch Gynecol Obstet 2004;269(3):205…
207.
19. Baks P, Liapis A, Creatsas G. Q-tip test and tension-free vaginal tape in the
management of female
tients with genuine stress incontinence. Gynecol
Obstet Invest 2002;53(3):170…173.
20. Masata J, Martan
Svabik K, Drahoradova P, Pavlikova M, Hlasenska J.
Changes in ur
hra mobility after TVT operation [article in Czech]. Ceska
Gynekol 2005;70(3):220…225.
21. Diez HP, Wilson PD. The •iris effect•: how two-dimensional and three-
dimensional ultrasound can help us understand anti-incontinence procedures.
Ultrasound Obstet Gy
col 2004;23(3):267…271.
22. Diez HP, Hansell NK, Grace ME, Eldridge AM, Clarke B, Martin NG. Bladder
neck mobility is a heritable trait. Br J Obstet Gynaecol 2005;112(3):334…339.
23. Diez HP, Bennett MJ. The effect of childbirth on pelvic organ mobility. Obstet
Gynecol 2003;102(2):223…228.
24. Peschers U, S
er G, Anthuber C, DeLancey JO, Schuessler B. Changes in
vesical neck mobility following vaginal delivery. Obstet Gynecol 1996;88(6):
1001…1006.
25. Meyer S, De Grandi P, Hohlfeld P, Megalo A. The birth trauma: short and long
term effects of foreps delivery compared to spontaneous delivery on different
pelvic ”oor parameter. Int Urogynecol J 1999;10(S1):S1.
26. Diez HP, Clarke B, Vancaillie TG. Vaginal childbirth and bladder neck mobil-
ity. Aust N Z J Obstet Gynaecol 2002;42(5):522…525.
60
H.P. Dietz
27. Dietz HP, Eldridge AM, Grace ME, Clarke B. Does pregnancy affect pelvic organ
mobility? Aust NZ J Obstet Gynaecol 2004;44:517…520.
28. Meyer S, De GranPi, Schreyer A,
ccia G. The assess
t of bladder neck
position andmobility in continent nullipara, multipara, forceps-delivered and
incontinent women using perineal ultraound: a future of“ce procedure? Int
Urogynecol J 1996;7(3):138…146.
29. Dietz HP, Lanzarone V. Levator trauma after vaginal delivery. Obstet Gynecol
2005;106
07…712.
30. Digesu G,Toosz-Hobson P, Bidmead J, Cardozo LD, Robinson D. Pregnancy,
childbirth and urinary incontinence: Caesarean for all? Neurourol Urodyn
2000;19(4):508…509.
31. Balmforh J, Toosz-Hobson P, Cardozo L. Ask not what childbirth can do to
your pelvic ”oor but what your pelvic ”oor can do in childbirth. Neurourol
Urodyn 2003;22(5):540…542.
32. Dietz H
, Moore KH, Steensma AB. Antenatal pelvic organ mobility is associ-
ated with delivery mode. Aust N Z J Obstet Gynaecol 2003;43:70…74.
33. Diez HP, Lanzarone V, Simpson JM. Predicting operative delivery. Ultrasound
Obstet Gynecol
06;27(4):409…415.
34. Schaer
, Perucchini D, Munz E, Peschers U, Koechli OR, DeLancey JO. Sono-
graphic evaluation of the bladder ne
in continent and sress-incontinent
women. Obstet Gynecol 1999;93(3):412…416.
35. Dietz H
, Clarke B. The ur
hral pressure pro“le and ultrasound imaging of
the lower urinary tract. Int Urogynecol J 2001;12(1):38…41.
36. Huang W
, Yang JM. Bladder neck funneling on ultrasound cystourethrogra-
phy in primary stressurinary incontinence: a sign associated with urethral
hypermobility and intrinsic sphincter deciency. Urology 203;61(5):936…941.
37. Gren TH. Urinary stress incontinence: differential diagnosis, pathophysiol-
ogy, and managment. Am J Obstet Gynecol 1975;122(3):378…400.
38. Tunn R,
tri E. Introital and transvaginal ultrasound as the main tool in the
assessment of urog
ital and pelvic ”oor dysfunction: animaging panel and
practical approach. Ultrasound Obst
Gynecol 20
;22:205…213.
39. Diez HP. What•s •normalŽ pelvic organ descent, and what•s prolapse? ICS
Annual Scienti“c Meeting 2006, Christchurch, New Zealand. Abstract.
40. Diez HP, McKnoulty L, Clarke B. Translabial color Doppler for imaging in
urogynecology: a prelimiary report. Ultrasound Obstet Gynecol 1999;14:144…
147.
41. Dietz H
, Clarke B. Translabial color Doppler urodynamics. Int Urogynecol J
2001;12(5):304…307.
42. Masata J, Mart
A, Halaska M, Kasikova E,
enasek M, VoitR. Detection
of Valsalva leak point pressure with colour Doppler: new method for routine
use. Neurourol Urodyn2001;20(4):494…496.
43. Kremkau FW. Diagnostic Ultrasound: Principles and Instruments. St. Louis:
WB Saunders; 2005.
44. Schaer
, Schmid T, Peschers U, DeLancey JO. Intraurethral ultrasound cor-
related with urethral histology. Obstet Gynecol 1998;91(1):60…64.
45. Kuo HC. Transrectal sonographic investigation of urethral and paraurethral
structures in women with stress urinary incontinence. J Ultrasound Med
1998;17(5):311…320.
46. Klein HM, Kirschner Hermanns R, Lagunilla J, Gunther RW. Assessment of
incontinence with intraurethral US: preliminary results. Radiology 1993;187(1):
141…143.
47. Kirschner Hermanns R, Klein HM, Mueller U, Schaefer W, Jakse G. Intra-
urethral ultrasoundin women with stress incontience. BrJ Urol 1994;74(3):
315…318.
Chapter4 The Anterior Compartmen61
48. Mitterberger M, Pinggera GM,
eller T, et al. Dynamic transurethral sonog-
raphy and 3D reconstruction of the rhabdosphincter and urethra. J Ultrasound
Med 2006;25:315…320.
49. Huang WC, Yang JM. Transvaginal sonography in the treatment of a rare case
of total urethral stenosis with a vesicovagin
stula. J Ultraound Med 2002;
21(4):4
63…467.
50. Toozs-Hobson P, Khu
r V, Cardozo L. Three-dimensional ultrasound: a novel
technique for investigating the urethral sphincter in the third trimester of
pregnancy. Ultrasound Obstet Gynecol 2001;17(5):421…424.
51. Robinon D, Toozs Hobson P, Cardozo L, Digesu GA. Correlating structure and
function: three-dimensional ultrasound of the urehral sphincter. Ultrasound
Obstet Gynecol2004;23272…276.
52. Yang JM, Hu
g WC. The signicance of urethral hperechogenicity in
female lower urinary tract symptoms. Ultrasound Obstet Gynecol 2004;24(1):
67…71.
53. Khullar V, Salvatore M, Cardozo L, Bourne T, Abbott D, Kelleher C. A novel
technique for measuring bladder wall thickness in women using transvaginal
ultrasound. Utrasound Obstet Gy
col 1994;:220…223.
54. Khullar V, Cardozo LD, Salvatore S, Hill S. Ultrasound: a noninvasive screening
test for detrusor instability. Br J Obstet Gynaecol 1996;103(9):904…908.
55. LekskulchiO, Dietz HP. Normal values for detrusor wall thickness in young
Caucasian women. Inteantional Continence Society Annual Scie
c Meeting
2005, Montreal. Abstract.
56. Robinon D, Anders K, Cardozo L, Bidmead J, Toozs-Hobson P, Khullar V. Can
ultrasound replace ambulatory urod
amics when invest
ating women with
irritative urinary symptoms? BrJ Obstet Gynaec
2002;109
):145
148.
57. Yang JM, Huang WC. Bladder wall thickness on ultrasound cystourethrogra-
phy. J Ultrasound Med 2003;22:777…782.
58. Lekskulchai O,
etz HP. Detrusor wall thickness as a test for detrusor over-
activity in women. ICS Annual Scientic Meeting 2006, Christchurch, New
Zealand.
59. Soligo M, Khullar V, Salvatore S, Luppino G, Arcari V, Milani R. Overactive
bladder de“ nition and ultrasound measurement of bladder wall thickness: the
right way without urodynamics. Neurourol Urodyn 2002;21(4):284…285.
60. Vela M, Parsons M, Cardozo L. Does bladder wall thickness increase with age?
Int Urogynecol J 2005
6(S2)S100.
61. LekskulchiO, Dietz HP. Detrusor wall thickness in women with a history of
childhood nocturnal enuresis. ICS Annual General Meeting 2006, Christ-
church, New Zealnd. Abstract.
62. Robinson D, Khullar V, Cardozo L. Can bladder wall thickness predict post-
operative detrusor overactivity? Int Urogynecol J 2005;16(S2):S106.
63. Wijma J, Tinga DJ, Visser GH. Perineal ultrasonography in women with stress
incontinence and controls: the role of the pelvio or muscles.
necol Obstet
Invest 1991;32(3):176…179.
64. PescherU M, Schaer GŅDeLancey JO, Schuessler B. Levator ani function
before and aftr childbirth. Br J Obstet Gynaecol 1997;104(9):1004…1008.
65. Dietz HP. Levator function before and after childbirth. Aust N Z J Obstet
Gynaecol 2004;44(1):19…23.
66. Bo K, LarsoS , Oseid S, Kvarste
B, Hagen R, Jorge
n J. Knowledge about
and ability to do correct pelvic oor muscle exercises iw omen with urinary
stress inco
inence. Neurourol Urodyn 1988;7:261…262.
67. Dietz HP, Wilson PD, Clarke B. The use of perineal ultrasound to quantify
levator activity and teach pelvico”or muscle exercises.
t Urogynecol J Pelvic
Floor Dysfunct 201;12(3):166…168.
62
H.P. Dietz
68. Miller JM, Perucchini D,
rchidi LT, DeLancey JO, Ashton-Miller J. Pelvic
” oor muscle contraction dring a cough and decreased vesical neck mobility.
Obstet Gynecol
01;97(2):255…260.
69. Dietz HP, Jarvis SK, Vancaillie TG. The assessment of levator muscle strength:
a validation of three ultrasound techniques. Int Urogynecol J 2002;13(3):
156…159.
70. Thompson J, O•S
van PB, Briffa K,
umann P, Court S.
sessment of pelvic
” oor movement using transabdominal and transperineal ultrasound. Int
Urogynecol J PelviF loor Dysfunct 20 5;16(4):285…292.
71. CreightonSM, Pearce JM, Stanton SL. Perineal video-ultrasonography in the
assessment of vaginal
olapse: early observations. Br J Obstet Gynaecol
1992;99(4):310…313.
72. Diez HP, Haylen BT, Broome J. Ultrasound in the quacaition of female
pelvic organ prolaps
Ultrasound Obstet Gy
col 2001;1
5):511…514.
73. Schaer GN, Koelbl H, Voigt R, et al. Recommendations of the German Associa-
tion of Urogynecology on functional sonography of the lower female urinary
tract. Int UrogynecolJ 1996;7
):105
108.
74. Bombieri L,Freeman RM. Do bladder neck position and amount of elevation
in” uence the outcome of colposuspension? Br J Obstet Gynaecol 2003;110(2):
197…200.
75. Viereck V, Pauer HU, Bader W, et al. Introital ultrasound of the lower genital
tract before ad after colposuspension: a 4-year objective follow-up. Ultra-
sound ObstetGynecol 2004;23(3):277…283.
76. Haylen BŢFrazer MI, Sutherst JR, West CR. Transvaginal ultrasound in the
assessment of bladder v
mes in women. Preliminary report. Br J Urol 1989;
63(2):149…151.
77. HaylenBT. Veri“cation of the accurcy and range of transvaginal ultrasound
in measuring bladder volumes in wo
n. Br J Uol 1989;6
4):350…352.
78. Mouritsen L, Bernstein I. Vaginal ultrasonography: a diagnostic tool for
urethral diverticulum. Acta ObsteG ynecol Scand 1996;75(2):188…190.
79. Tunn R, Bergmann-Hensel U, Beyers
f D, Heinrich G, Fischer W, Hamm B.
Diagnosis of urethral dive
icula and periurethral masses [article in German].
Rofo 2001;1
(2):109…114.
5
The Central and Posterior Compartments
Anneke B. Steensma
ProlapsA ssessment
Translabial ultrasoundhas been utilizedfor prolapse quanti“cation, not just
for the anterior compartment, but in the assessment of central and posterior
compartmentas well.1,2 The uterus itslf may be dif“cult to identify because
it is iso- to hypoechoic, similar to vaginal tissues. A specular (line-like) echo
often indicates the leading edge of the cervix. At times, nabothian follicles
help with identi“ cation of the cerix, but in postmenopausal women the
uterus may be so small as to be virtually invisible on translabial imaging,
even if thee is signi“cant descent. Thsame holds trueor a retroverted
uterus, especially if sign
cant rectal contets or a recocele shadowthe area
of interest, and a well-supported uterus may be outside theld of view,
in particular if higher-frequency transducers ae used. Needless to say, a
full sonographic asessment of the etrus requires trasvaginal scanning.
Despite all those limitations, however, the cervix can often be located trans-
labially (see Figure5.1 for a second-degree uterine prolapse), and the same
holds true for the apex of the vault after hysterectomy (see Figure 5.2).
The bladder neck or the leading edge of a cystocele is used for the quan-
ti“ cation of anteriorvaginal wall descent, the cervix or Pouch of Douglas
for the central compartment, and the most caudal aspect of the rectal
ampulla … or the leading edge of rectocele contents … for qca
ion of
posterior compartment descent. The inferior margin of the symphysis
pubis anchos a horizontal line of reference against which descent can be
measured (see Figures 5.1 and 5.5). Ultrasound qu
cation ofcentral and
anterior compartments seems to agrewell with clinical prolapseassess-
ment by the prolapse quantc“ation system of the
ternational continence
3, with correlations of r= 0.77 for uterine prolapse, =
0.72 for anteriorvaginal wall, and r = 0.53 for poserior vaginal wall pro-
lapse descri
d in a comparative stud2.The vault after hysterectomy may
also be visualized in
e midsagittal plane (see Figure 5.2), but can be dif-
“ cult to identify, especiallyif there isa rectocele or if the ampulla is unusu-
ally full.
Descent of the posterior compartment is associated with symptoms of
prolapse, althoughthe correlation is not as strong as for the anterior com-
63
64 A.B. Steensma
Figure 5.1Prolapse quantification by transperineal ultrasound. Measurements are against a hori-
zontal line through the inferior margin of the symphysis pubis. Clinically there is a second-degree
cystoceledasecond-degree uterine prolapse.
partment. In women with isolated posterior compartment prolapse, descent
of the rectal ampual or of rectocele contents to 15 mm below the symphysis
or below see
s to be associated with symptoms of prolapse and has been
proposed as a
toff for •signi“ cant descentŽ on the
is of receiver opera-
4
Figure 5.2The midsagltp
lane at rest in a patient after abdominal hyst=
vagina,
b = bladder). ehpouch of Douglas is outlined by intraperitoneal fluid.
Chapter5 The Central and Posterior Compartm
65
ROC Curve
symptomatic
1.0
Cutoffs:
0.8
…2mm
…1mm
0.6
…10m
0.4
asymptomatic
0.2
c = 0.821
0.0
…50
…40
…30
…20
…10
0
10
20
30
40
50
0.0
0.2
0.4
0.6
0.8
1.0
1-specificity
Figure 5.3Historams for maximurectal descent relative to the inferoposterior margin of the symphysis pubis, in millimeters
(left) in ymptomatic (gray) and sy
tic wo
n (black) and receiver operator curve (ROC) for rectal descent as a test for
symptom
c prolapse (right). Lines define proposed cutoffs.
AnteriorRectoele
Correlations between cl
ical prolapse grading and ultrasound may not be
quite as good for the posterior compartment as they are for cystocele or
uterine descent, but it is possible to distinguish between •trueŽ and •falseŽ
rectocele, i.e., a defect of the rectovaginal septum (see Figure 5.4) and
increased distensibility of the septum and/or perineal hypermobility
without fascial defects5 (see Figure 5.5). This distinction matters, because
both entities may produe symptoms of prolapse, but only •trueŽ rectoceles
are associated with sympmos of straining at stool, incomplete bowel emp-
tying, and vagnal digitation, i.e, symptoms of ob
ructed defecation.6
The traditional distinction among low, midlevel, and high rectoc7le
is not supported by ultrasound data. From experience to date, •true
Figure 5.4•TrueŽ rectocele with an obvious rectovaginal
apparent on Valsalva,
ing about 25 mm in depth.
The presumptive ms
of the defect are indicated by arrows.
66 A.B. Steensma
Figure5.5. Descent ofethrectal ampulla without actual herniation of rectal contents into the vagina, termed •perineal hyper-
mobility.Ž (Fromz
HP, Steensma AB. Posterior compartment prolapse on two-dimensional and three-dimensional pelvic floor
ultrasound:ethdistinction between true rectocele, perineal hypermobility and enterocele. Ultrasound Obstet Gynaecol 2005; 26:
73…77, with permission.)
rectocelesŽ or fascial defects seem to almost always be found in the same
area, i.e., very close to the anorectal junction, and they are usually trans-
verse. Quanti“cation involves me
urement of rectocele depth, using a line
extending the cranioventral aspect ofethinternal anal sphincter as a base-
5 as shown
in Figures 56 and 5.10. Rendered volumes at the level of the hiatus in the
Figure 5.6Small but typical defect of the rectovaginal septum at the level of the anorectal junction, imaged in the midsagittal
plane (le
and as seen on a rendered volume in the axial p=adep
th,
= width.
Chapter5 The Central and Posterior Compartm
67
axial plane, orC plane imaging in general, can show the total extent of the
defect and demonstrate asymmetries (see Figure 5.6).
8 but they
are more common in the parous.5 In some women, they clearly arise in
childbirth, and if they are present before the delivery, defects tend to
enlarge.9 Many are asym
omatic, but thee is a signicant association
between bo
l symptoms such as incomplete bowel emptying and manual
evacuation on the one
nd, and the presence and depth of defects on the
other hand.6 Routine posteior repair often results in reduction or distor-
tion of suchdefects, without achieving actual closure. Defect-spc
repair
tends to be more effective in closing defects but may not affect concomitant
perineal hypermobility. Major levatorplasty, as frequently performed in the
past, often creates a hyperechogenic scar plate in front of the defect.
PosterioR ectocele
Posterior rectocele is
id to be a cmmon “ nding in children with consti-
pation and evacuatory dysfunction but is rarely seen in adults. As in ante-
rior rectocele, thearea of defct is veryclose tothe anorectal junction, but
seems to de
lop posteriorly or dorsally (see Figure 5.7). At times, appear-
ances ae suggestive of an intussusception of the anal canal into the
rectum.
Enterocele
One of the main advantages of translabial ultrasound is the ease with which
rectocele ca
5 The latter isdiagnos
d if
there isa herniation of ”uid-containing peritoneum, small bowel, sigmoid,
Figure 5.7Posteri
rectocelethe le
l of the anorectal junction.
68 A.B. Steensma
Figure 5.8Enterocele as demonstrated in the midsagittal plane on maximal Valsalva. The hernia-
tion is filled by a l
f small bowel, giving a bull•s eye…like appearance. Peristalsis often puts the
diagnosis beyond doubt. In
ent, there alsa ismall rectocele.
or omentum anterior to the anorect
junction, separating the vagina from
the rectal ampula (see Figure 5.8). Hysterectomy is considered to be the
main risk factorfor enterocele, and the majority of patients will have other
concomitant pelvic ”oor abnormalities.
Enterocele is freq
ntly overlooked on clinical examination, and its rela-
tion to pelvic ”oor symptoms remais unclear. At defecogram, multiorgan
opaci“ cation is necess
y for the diagnosis of enterocele, and this exposes
the patient to a relatively high dose oradiation. Magnetic resonance
imaging (MRI) has the advantage of demonstrating all compartments as
well as the capability to perform a limited dynamic investigation, but MRI
is expensiveand not widely available.
With transperineal imaging it is relatively easy to detect enterocele. In
the midsagital plane, a maximal Valsalva will demonstrate downward
movement of io- to hyperechoic abdominal contents anterior to the
anorectal junction, withor without vault prolapse. Sm
l bowel peristalsis
may help with the identi“ cation of structures
lling the hernia
(see
Figure 5.8).
Functional Imaging
Most recently, colrectal surgeons have started to use translabial ultra-
sound to complement or replace defecography, although it seems t
rst
10,11
It is very likely that
ultrasound will become useful in eh clinical assessment of women with
symptoms of obstrcted defecation.
t just rectocele (anterior or poste-
Chapter5 The Central and Posterior Compartm
69
A
B
Figure 5.9Comparison3Df translalualtrasou
(A)and defecogr
B)at maximum levator contraction in a 57-year-old
patient.
rior) and enterocelecan be demonstrated using dynamic 2D or 3D ultra-
sound, anismusmay be evient as a spastic levator that does not allow
descent of pelvic structures during Valsalva. As in conventional proctogra-
phy, it is possible to measure the anorectal angle to assess the levator ani
complex during contraction and relaxation of the pelvi
oor and at strain-
ing. Figures
9 and 5.10 show comparisons of translabial ultrasound and
defecation proctography, on levator contraction (Figure 5.9) and on maximal
Valsalva (Figure 5.
), in a patient with symptoms of ostructed defecation
and a large rectocele.
Figure 5.10Large rect
e as seen on maximal Valsalva, in the same patient as in Figure 5.9. Both methods demonstrate a
rectocele of more than 3 cm in depth.
70 A.B. Steensma
Figure 5.11Incipient rectal prolapse in a patient after vaginal vault suspension and enterocele
repair.
Rectal Intussusception and Rectal Prolapse
On functional pelvic ”oor ultrasound imaging, rctal intussusception or
occult rectal proapse is occasionally demonstrated in women without any
symptoms of evac
tory dysfunction.However, themethod is also capable
of demonstrating sympto
tic rectal prolapse. Normally, the anal canal is
tubular, with little difference betw
n luminal diameters along most of its
length (see, e.g., Figures 5.9 and 5.10). In less marked cases of rectal intus-
susception or •occultŽ prolapse, rectal wall and small bowel enter the proxi-
mal anal canal,
rcing it openand producing an arrow-shaped distension
on Valsalva (ee Figures 5.1and 5.12). Tis appearance is pathognomonic
Figure 5.12Developmentaor ectal intussusception on Valsalva: There is an enterocele which initially compresses the rectal
ampulla (central image) and then invaginates the rectal mucosa and muscularis (right image) into the anal canal which opens up
in a typical conical configuration.
Chapte5 The Central and Posterior Compartm
71
Figure 5.13First-degree uterine descent, with the cervix •pluggingŽ the anal canal in a patient with obstructed defecation.
and very similar to images obtained odefecation proctograph1.2 If there
is overt rectal proapse, the enterocele will be seen toow”Ž through the
anal canal, inverting rectal mucosu,ntil the prolapse exits through the
external anal sphincter. The mximal depth of an intussusceptin may be
measured by conn
ting the most proximal aspects of te internal anal
sphincter and measuring to the apex of the intussusception (see Figure
5.11).
Apart from rectocele and rectal intussusc
ion or prolapse, pelvic
” oor ultrasound may identify other, less cmmon causes of obstructed
defecation. It appears aht an abnormally mobileanteverted uterus may
impinge on the rectal ampulla and virtually •plugŽ it on Valsalva, a situa-
tion that is termeda •colpoceleŽ by colorectal surgeons (see Figure 5.13).
This may cuse the sensation of incomplete emptying and prompt the
patient to strain at stool … which only makes matters worse, similar to the
situation in rectal intussusception. There may be no oth
nding that
more graphically illustrates how much we still have to learn about pelvic
” oor function … and how much pelvi
oor ultrasound can teah us as well
as our patient. Once the situation is demonstrated to the patient on
imaging, attemptsat behavior modi“cation may well be much more likely
to succeed.
Clearly, muchwork will have to be done in d
ning the roleof the new
method in the evaluation of wo
n with obstructed defecation, in particu-
lar in comparisonwith defecationproctography.
Anal Sphi
ter Imaging
The anal sphinct
is generally imaged by ena
nal ultrasound, using high-
resolution probes with a eld of visionof 360°. Thismethod is “rmly estab-
lished as one
the cornerstones ofa colorectal diagnostic workup for anal
incontinence and coveree xtensively in the colorectal and radiologic lit-
Because
the limited availability of suchprobes ingynecology,
72
A.B. Steensma
obstetricians and gynecologists have taken to using high-frequency curved
array probes placeexoanally, i.e
in the coronal rather
than the midsagittal plane as described for all other applications in this
text.
There ae advantages to this approach … not just from the point of view
of the patient. Eoanal imaging reduces distortion of the anal canal and
allows dynamic evaluation of the anslphincter and mucosa at rest and on
sphincter contraction, which seems to enhance thenition of muscular
2 and good comparative
studies ae still lacking.
Figure 5.14 demonstrates normal
earances on tranabial imaging of
the anal sphinter complex in the coronal plane. The mucosa is visualized
as a hypere
oic area, often star-shaped, representing the folds of the empty
anal canal.20 The internal anal sphincter (IAS) is seen as a hypoechoic ring,
the external anal sphi
ter (EAS) as an echogenic structure surrounding
the internal sphincter.19…21There may be some variation of appearances
depending on age
d hormonal status.13 On contraction, the anal canal
narrows slightly, the mucosal star may be less pronounced, and defects of
the sphincter will become more obvious.
Anal sphincter injuriesseem to occur mch more frequntly than pre-
viously reported, although this may well be attributable to ineffective
intrapartum detecion rather than covered, truly •occultŽ defec23.On
ultrasound, sphincter defects appear as a discontinuity of the ring struc-
tures of theEAS and/or IAS. In te coronal plane, defects are conveniently
described using a clock face notation. In the longitudinal plane, sphincter
defects can be described by measuring the length of the defect relative to
total sphincter length.
After repair of third- and fourth-degree tears, ultr
ound frequently
demonstrates residual defects (see Figures 5.15…5.17), and the extent of
Figure 5.14Tranalbial imaging of a normal anal sphincter at rest.
Chapter5 The Central and Posterior Compartm
73
Figure 5.15Full-thickness
ect in the external anal
ter (EAS) complex from 11 to 12
o•clock, as visuawi
ith translabial ultrasound
transverse or coronal pla=
internal
anal sphincter.
such incompletely or inadequately repaired defects seems associated
with decreased sphincre pressures and an increased risk of anal
incontinence.24
Childbirth and obstetric trauma is by far the dominant cause of anal
sphincter defects. The main risk f
or is considered to beinstrumental
vaginal delivery.25 Anal incontinence is common after third- and fourth-
degree tears, evn if they are reco
ized and repaired atthe time ofinjury,
and can have a devastating effect on a woman•s quality of life. The condition
may have been underrep
ed because of the social stigma involved. Early
Figure 5.16Varying appances 6…8 weeks after repair of third-degree tears.
74 A.B. Steensma
Figure 5.17Defect of the internal
ternal sphincter complex as visualized in the transverse (coronal) (left) from 11 to 1
o•clock and in 50% of the IAS visualized in the longitudinal plane (midsagittal) (right) in a 60-year
severe
fecal incontinence.
recognition and repair of sphincter injuries are likely to be of be
.26
Pelvic ”oor ultrasound may well have a major role in the evaluation of
patients after traumatic delivery, but further studies are needed ton
e
the role of eoanal in comparison toendoanal ultrasound.
References
1. CreightonSM, Pearce JM, Stanton SL. Perineal video-ultrasonography in the
assessment of vaginal paopse: early observations. Br J Obstet Gynaecol 1992;
99(4):3
10…313.
2. Dietz H
, Haylen BT, Broome J. Ultrasound in the qua
cation of female
pelvic organ prolaps
Ultrasound Obstet Gy
col 2001;1
5):511…514.
3. Bump RC, Mattiasson A, Bo K, et al. The standardization of terminology of
female pelvic organ prolapse and pelvico”or dysfunction. AmJ Obstet Gynecol
1996;175(1):10…17.
4. Dietz HP. What•s •normalŽ pelvic organ descent, and what•s prolapse? ICS
Annual Scienti“c Meeting 2006, Christchurch, New Zealand.
5. Dietz HP, Steensma AB. Posterior compartment prolapse on two-dimensional
and three-dimenional pelvic ”oor ultrasound: the distinction between true
rectocele, perineal hypermobility and enterocele. Ultrasound Obstet Gynecol
2005;26:73…77.
6. Dietz HP,Korda A. Which bowel symptoms are most strongly associated with
a true rectocele? Aust N Z J Obstet Gynaecol 2005;45:505…508.
7. Davis K, Kmar D. Post
ior pelvic ” oor compartment disorders. Best Pract
Res Clin Obstet Gyna
l
2006;1
6):941…958.
8. Dietz HP, Clarke B. Prevalence of rectocele in young nulliparous women. Aust
N Z J Obstet Gynaecol 2005;45(5):391…394.
9. Dietz HP, Steensma AB. The role of childbirth in the actiology of rectocele. Br
J Obstet Gynaecol 2006;13:264…267.
10. Beer-
abel MMD. Dynamic transperineal ultrasound in the diagnosis of pelvic
” oor disorders: pilot study. Dis Colon Rectum 2002;45(2):239…248.
11. Beer-
abel M, Tesh
r M, Schechtman E, Zbar AP. Dynamic transperineal
ultrasound vs. defe
graphy in patients with evacuatory dic“ulty: a pilot
study. Int J Colorectal Dis 2004;19(1):60…67.
Chapter5 The Central and Posterior Compartm
75
12. Mellgren A, Bremmer S, Johansson C, et al. Defecography. Results of investiga-
tions in 2816 pati
ts. Dis Colon Rectum 1994;37(11):1133…1141.
13. Starck M, BohM, Fortling B, Valentin L. Endosonography of the anal sphinc-
ter in women of different ages and parity. Ultrasound Obstet Gynecol 2005;
25(2):169…176.
14. Damon H, Henry L, Bretones S, Mellier G, Minaire Y, Mion F. Postdelivery anal
function in primiparous females: ultrasound and ma
metric study. Dis Colon
Rectum 2000;43(4):472…477.
15. Williams AB, Bartram CI, Halligan S, et al. Alteration of anal sphincter mor-
phology following vaginal delivery revealed by multiplanar anal endosonogra-
phy. BJOG 20
;109(8):942…946.
16. Gold DM, Bartram CI, Halligan S, Humphries KN, Kamm MA, Kmiot WA.
Three-dimensional endoan
sonography in asessing anal ca
l injury. Br J
Surg 1999;86(3):365…370.
17. Frudinger A, Bartram CI, Halligan S, Kamm M. Examination techniques for
endosonography of the anal can
Abdom Imaging 19
;23(3):301…303.
18. Schaefer A,
ck P, Fuerst GĶ ahn T, FrielingT, Luebke HJA natomy of the
anal sphincters. Comparison of anen dosonography tomagnetic resonance
imaging. Dis Colon Reutm 1994;3(8):777…781.
19. Peschers U,DeLancey JO, Schaer GN, Schuessler B. Exoanal ultrasound of the
anal sphincter: normal anatomy and s
ncter defects. Br J Obstet Gynaecol
1997;104
):999…1003.
20. Timor-Tritsch IE, Monteagudo A, Porges RF,n
tos R. Simple ultrasound eval-
uation of the a
al sphincter in femalepatients usinga transvaginal transducer.
Ultrasound Obstet Gy
col 2005;2
2):177…183.
21. YaglS, Valsky DV. Three-dimensional transperineal sonography for evalua-
tion of the anal sphinctrcomplex: another dimension in understanding peri-
partum sphincter trauma. Ultrasound Obstet Gynecol 2006;27(2):119…123.
22. Cornelia L, Stephan B, Michel B,t
ine W, Felix K. Trans-perineal versus
endo-anal ultrasound in te detection of anal sphincter tears. Eur J Obstet
Gynecol Reprod Biol 2002;103(1):79…82.
23. Andrews A, SultanA, Thakar R,Jones P. Occult ansp hincter injuries…myth
or reality? BJOG 2006;113:195…200.
24. Starck M,
he M, Vale
in L. The extent of endosonograhic anal sphincter
defects aftr primary repair of obstetric sphincter tears increases over time
and is related to anal incontinence. Ultrasound Obstet Gynecol 2006;27(2):
188…197.
25. Sultan AH, Kamm MA, Hudson CN, Thomas JM, Bartram CI. Anal sphincter
disruption during vaginal delivery. N Engl J Med 1993;329(26):1905…1911.
26. Faltin DL, Boulvain M, Floris LA, Irion O. Diagnosis of anal sphincter tears to
prevent fecal incontinence: a randomized controlled trial. Obstet Gynecol
2005;106:6…13.
6
Axial Plane Imaging
Hans Peter Dietz
Levator Ani Complex
It is only very recently that imaging of eh levator ani has become feasible
using translabial ultrasound. The inferior aspects of the levator ani were
identi“ ed in early stu
1 and translabial
2 as well as on tranabial ultrasound using a
Voluson system3 but the focus of these reports was on the urethra and
paraurethral tissues. With translabial acquisition, the whole levator hiatus
and surrounding muscle (pubococcygeus and puborectalis) can be visual-
ized, provided acquisition angle
are at or aboe 70°. As
th magnetic
resonance imaging (MRI), it is currently impossible to distinguish the dif-
ferent components of te pubovisceralor puborectalis/pubococcygeus
complex. Several studies in nulliparous women have found no major asym-
4 and on utrasound,5,6
supporting the hypothesis that signi“cant morphologic abnormalities of
the levator are likely to be evidence of delivery-related trauma. Contrary to
MRI data,7 no signi“ cant side differeces were foud on ultrasound biom-
etry, neither for thickness nor for area.
Regarding biometric parameters of the puborectalis/pubococcygeus
complex and the levator hiatus, there has been good agreement between
three-dimensional ultrasond and MRI, bothfor dimensions of the levator
hiatus5,7 and levator thickness.5,8 In general, it is to be expected that ultra-
sound measure
ents shouldbe morereproducible because of the ease with
which measure
ents in the axial plane can be obtained in the plane of
minimal dimensions, whether at rest, on Valsalva, or on pelvoco”r muscle
contraction. Fgure 6.1 demonstrat
the process of ob
ining the plane of
minimal dimensions.
On MRI, the pane of minmal dimensions is virually impossble to
image reproduciblybecause of slow quisition speeds, even of single pre-
de“ ned planes. The latest software developments available for 3D/4D ultra-
sound such as
lume contrast imaging and speckle reduction imaging
should resultin a further improvement in resolution and therefore repro-
ducibility of ultrasound measurements. Diameter and area measurements
of the pubococcygeus…puborectalis complex may not bec
iently repro-
76
Figure 6.1Determination
iatal dimensions. The left-hand image shows the location of the plane of minimal dimensions as
seen on the mids
l view. This plane is tilted in a ventrocaudal to dorsocranial direction as eviden
ting
the im
e running from the posterior surface of the symphysis to the anterior margin of the most centa
lis
loop (white arr
). The rithimage represents the plane of minimal dimensions in the axial or C plane, with the vertical line
showing the location of the midsagittal plane. Arrows identify the minimal sagittal diameter of the hiatus.
Figure 6.2Area and diameter measuremenleva
tr hiatus [plane of minimal dim
at rest (left) and on Valsalva
(right)] in a
iparous volunteer. (From Dietz HP, Shek C, Clarke B. Biometry of the pubovisceral
y 3D
pelvic floor ultrasound. Ultrasound
aecol 2005;25(6):
85 , with permission.)
78 H.P. Dietz
and descet(because downward isplacement of organs may displace the
levatorlaterally), it is much more interesting that hiatal area at rest is asso-
ciated with pelvicorgan descent on Valsalva. These data constitute
rst
real evidence for the hypothesis that the state of the levator ani is important
9 even in the abse
e of levator trauma.
As a rule of thumba hiatal area of less than 25 2on Valsalva is unlikely
to be associ
ed with signi“cant prolapse. We classiayn area of 30…34.92cm
2 as moderate, and 4+ cm2 as severe ballooning, with
2 and above. Interestin
y, there ae nullipa-
rous women who show moderate to marked ballooning on Valsalva. Whereas
the highe
2 the
author has recently document
ballooning to m
2 in a nul-
liparous professional athlete with an asymptomatic three-compartment
prolapse and enterocel
without there being any evidence of an abnormal
connectivetissue phenotypeTo put this in perspective, the area required
2.
Apart from static dimenions, relative enlargement of the hiatus on Val-
salva m
y be a measure of compliance or elasticity which mayu
ence the
progress of lbor, pelvic ”oor trauma, and future prolapse. However, child-
birth obviously has an effecton width and distensibility of the hiatus
(see Figure6.3). And “ nally, hiatal dimensions
e likely to affect treat-
ment outcome if (or when) treatment for pelvico”or dysfunction becomes
Figure 6.3Increase in hiatal dimensions on Valsalva after vaginal delivery (rendered volumes, axial plane).
Chapter6 Axial Plane Imaging79
Figure 6.4Avulsionjunry of the right pubovisceral muscle, on MRI (left) and 3D ultrasound (right). Although the images were
obtained in different patients, they illustrate the m
pattern of delivery-rel
vator trauma. The arrows indicate
vaginal detachment (top
) and detachment of the levator ani (bottom arrows). (MRI courtesy of Dr. Ben Adekanmi,
York, UK.)
necessary. The author believes that marked enlargement of the levator hiatus
on Valsalva redu
s the likelihood of successful pessary management and
probably makes
10 In
women that show a hiatal area
2 one would
expect a high likelihood of posterior compartment prolapseafter a colpo-
suspension procedure … or a large cystocele after sacrospinous colpopexy,
because neit
r procedure would be expected to address the issue of exces-
sive distensibility of the levator hiat
. Clearly, much workwill have to be
done in this “ eld over the next decade, and pelvi
oor imaging is likely to
havea signi“cant impacton the development of prolapse surgery.
The most commonmorphologic abnormality of the levator ani, an
avulsion of the puboviscer
muscle off the pelvic sidewall, is clearly related
to childbirth (see Figures 6.4…6.6 and Cases 5, 10, 12, and 13 of the Appen-
dix) and is often palpable as an asymmetricsls of substancin the infero-
medial or ventrocaudal portion of the muscle. The digital detection of
morphologic abnormality seems to require sig
cant training however,
11
In a recently completed blinded study, the author found poor agreement
2
Technical issues also heepxplain the poor agreement found in this study.
In women with poorresting tone and minimal or absent voluntary func-
tion, defecs may be impossible to detect by digital examination. However,
a recent study using MR detection of levator defects demonstrated much
better agreement between imagingdanvaginal palpation, provided the
operators were trained speci“cally for this task.13
80 H.P. Dietz
Figure 6.5Axial pl
e rendered volumes. The right image shows a left-sided minor defect of the pubovisceral muscle 4 months
after vaginal delivery.
Figure6.6. Bilateral avulsion injury. The left image was o
weeks• gestation in a nulliparous patient. The right image
shows a bilateral major defect of the pubovisceral muscle 4 months after vaginal delivery in the same patient.
Chapter6 Axial Plane Imaging81
Thinning of muscle, which may be obvious on imaging, is harder to
palpate than gaps inthe continuity of the muscle or complete absence as in
avulsion injury. Having said that, biteral defects (see Figure 6.6, also
Figures 3.4 and 3.7, and Cases 10 and 13 of the Appendix) may be more
dif“ cult to palpate than unilateral avusion because of the lack of asym-
metry, and they are so much less common.
The detection of avulsion defects by translabial 3D/4D ultrasound seems
highly reproducible.14 Both rendered volumes
urface/transparency mode,
rendered from caudally tocranially) and single slices in the C or axial
plane may be used to help with the ide
cation of defecs. Therecent
development of tomographic ultrasound imaging (TUI) (see Figures 3.6,
3.7, 6.8, and
) is particula
ly useful in this regard beca
e it allows the
screening of oe 3D volume at a glance, especially once speckle reduction
algorithms have ben used to enhance resolutions in the axial plane.
Generally, defects seem boe most cleayl evident on levator contraction.
On Valsalva, de
cts may open up fu
her, but oncefull distension of the
hiatus is reachedthe defect is oftn obscured by attening of the area of
interest against te pelvic sidewall, particularly in women with sig
cant
prolapse.
Dif“ culties may arise in elderly women with marked urogenital
atrophy and/or scarrng, especially if voluntary
nction is absnt or with
very thin or atrophic muscle. Whenin doubt, the author has found
that measure
15 i.e., the distance
between the urethral lumen and the most medial aspect of the pubovisceral
muscle insertion, is helpful, with a gap of<2.6 mm likelyto indicate normal
anatomy (unpublished da
). Once oneis more famliar with the identi“ ca-
tion of defectsby vaginal palpation, an internal examination will further
help with the interpretation of ultrasound “ndings, especiallyif they are
equivocal.
Such defects of the pubovisceral muscle are surprisingly common for a
form of childbirth-related trauma that has receivevirtually no attention
to date. In a recently completed study, the author found that more than one
third of women delivering vaginally at an average age of 31.6 years had such
injuries,6 an incidence that is unexpectedly high compared with observa-
tions in older symptomatic wome
4 and previously published rates in
women who had their rst child at a younger age, both on clinical examina-
tion11 and MRI.4 This discrepancy
y be explained by an association
between materal ageat “ rst delivery and the incidence of major levator
trauma14,16 which is worrying gven the marked trend toward delayed child-
bearing in developed countriesIt seems likely tat women today run a
higher risk of sustaining signicant trauma to the lvator ani muscle, com-
pared with their mothers or grandmothers. This implies that urogynecol-
ogy„and urogynecologic imaging„is likely to be a growth area for the
foreseeable future.
Regarding causation, there seems to be an association with operative
delivery,6 but analogous to the situation with anal sphincter trauma, it
seems that precipatte delivery my also cause major levator trauma. This
impl ies that any association with length of second stage and other para-
meters indicating a dif“ cult delivery maynot be linear, making prediction
more dif“ cult.
82
H.P. Dietz
The clinical signi“cance of such def
s is becoming clearer. The author•s
own data sugg
t that levator avulsion is
sociated with anterior and
central compartment prolapse,14 but not with urodynamic “ndings or
symptoms of bladder dysfunction in a series of more than 300 primary
urogynecoogic assessments. Cross-sectional studies of levator anatomy in
asymptomatic and symptmatic older women are needed to determine
whether such abnor
alities are associated with clinical symptoms or con-
ditions in the general population. Another interesting question is whether
major morphologic abnormalities of the levator ani affect surgical out-
17 it appears that major
levator trauma, i.e., avulsion of the puborectalis/pubococcygeus from the
pelvic sidewall, sems to be associated with early presentation and recur-
rent prolapse after surgical repair.
Clearly, thereare different degrees of levator trauma. In the future we
should be able to distinguish not ju
unilateral and bilateral trauma, but
also isolated de
cts of the pubococcygeus or muscle, partial (Figure 6.5)
and/or complete avulsions puborectalis (Figure 6.6), and globalciencies
of the whoe levator (Figure 6.7) which are probably more likely to be
caused by neuropathy rather than direct trauma. In the meantime,
we may be able toquantify the extent oftrauma by using TUI which
allows both scoringaccording to the number of slices showing defects (see
Figure 6.8), and quantication of cranioventraland ventrodorsal defect
dimensions. Both defe
score and maxi
l width seem associated with
18
Figure 6.7Virtually complete absence of the pubovisceral muscle on the right side after Forceps
delivery.
Chapter6 Axial Plane Imaging83
Figure 6.8TUI of limdtebilateral levator trauma, affecting the lowermost aspects of the right pubovisceral muscle and more
cranial asps
on the left. The defect score is 6 (2 on right, 4 on left).
On a “ nal note, it appears thatthe literature to date contains no reports
of attempts at surgical correction.
is is nothing shot of amazing when
one consides that such defects may in fact be visible in the delivery suite.
Most avulsion injuries are occult,
t some become visible due to vaginal
tears, resulting in a typical appearance with the vagina detached from the
pelvic sidewall, te inferior public ramus and obturator fascia denuded of
muscle, ad the muscle retracted pararectally. We may have to learn how
to reattach the levator, a task that may require us to acquire some of the
skills of orthopedic surgens. Imaging will of course be instrumental in
documenting the success of failure of such attempts.
Paravaginal Supports
It has long been spec
ted that anterior va
nal wall prolapse and
stress uinary incontinence are at least
tly attributable to disruption
of paravaginal andør paraurethral support strctures, ie., the endopelvic
fascia and pubourethraligaments, atthe time of vaginal delivery.19 In
a pilot study using the now obsolete technology of freehand acquisition
of 3D volumes,alterations in paravaginal supports were observed in 5
of
21 women see
both ante- and postpartum, and the interobserver
84
H.P. Dietz
variability of the qualitative assessment of paravaginal supports was
shown to be good.2 In light of current knowledge, however, the loss of
tenting documented in this study was probably at least partly attributable
to levator avulsion.
Structures supporting urethra and bladder can also be assessed by tran-
srectal or transvaginal 3D ultrasound using probes designed for pelvic or
prostatic imaging.1,20 In a recent s
all series, researchers from Austria have
claimed that the endopelvic fascia may be evaluated directly by transrectal
3D ultrasound, describingdefects in an echog
c structure underlying
the bladder neck and proximal urethra. Such defects almost exclusively
21
occurred in vaginally parous wo
It remains to be shown whet
r loss of paravaginal tenting or defects
in suburethral/paraurethral echogenic structures are in fact equivalent
to what is clinically described as a •paravaginal defect,Ž a concept that is
22…24
In a recent sudy on 62 women
presenting
th pelvic ”oor disorders, only weakcorrelations were found
between a blinded clinical assessment for paravaginal defects and the
presence or abseec of tenting in single planes or rendered volumes
obtained by 3D translabial ultrasound, and even this weak correlation was
only seen on Valsalv2.5 This may be attributable to inadequate clinical
assessment techniqueor possibly an insuf“ciently sensitive imaging
method. Recent evidence suggests that the clinical assessment for para-
vaginal defecs has poor repeatabilit2.6,27 However, another (if less likely)
explanation may be that true paravaginal defects are either not common
and/or irrelevant for anterior vaginal wall support.
Urethra ad Urethral Supports
The “rst use of 3D pelvic ”oor ultrasound, albeit with a transvaginal probe,
28,29
Although there seems to be
disagreement ato what has actuallybeen measured in some of the studies
20,28,30
it seems thathe volume of the hypechoic
structures surrounding the urethra (smooth muscle, vascular plexus, and
mucosa) is associat
with closure pressure.28 On 3D ultrasound in the axial
plane, one is generally able to detect a circular hyperechogenic structure
surrounding the mid urethra (see Figure 6.9) which, judging from intraure-
thral ultrasound and axial plane MRI, corresponds to the striated urethral
sphincter.
It is less clear, however, whether obser
ion of static urethral
anatomy isof any clinical relevance. We ,after all, have inexpensive and
practical diagnostic toos to assess urethral function. In the author•s
opinion, resolutions atpresent ae not suf“cient for translabial ultrasound
to contribute to the as
ssment of urethral function. This may change with
the advent of sm
l parts 4D and matrix probes which will likely allow
much more detailedinsights into urethral anatomy, without distortion
and in a noninvasive manner. This probably also applies to urethral sup-
ports which are starting to be studied in more detail on MRI and
ultrasound.21
Chapter6 Axial Plane Imaging85
Figure 6.9TUI ia parous patient without bladder symptoms and normal pelvic floor anatomy. There is a hyperechogenic ring
structure (arrows) s
ding the midportion of the urethra in slices 1…4, i.e., extending over at least
ts
the urethral rhabdosphincter.
Other Findings
At times, imaging in the axial plane can help clarify anatomic relationships
in more complex prolapsecases, especialif there is signi“cant asymme-
try. The extentof a cystoc
e may become more obvious (see Figure 6.10),
and side differences, e,gcaused by major levator trauma or neuropathy,
can be detecte
n the coronal plane (see Figure 6.11). Rectoceles are usually
clearly apparent because of their hyperechoic nature (see Figure 6.12 and
Case 6 of te Appendix).
Cystic structures in the vagina are more e
ly assessedon 3D ultra-
sound, especially regardgntheir relationship with the urethra (see Figure
6.13 and Cas9 of the Appendix for Gartner cysts, Case 15 for a urethral
diverticulum). The exact location oa pessary can also be determined
more easily on 3Dimaging, although Figure 6.14 is mainly given to
acquaint readers with the very dis
ct appearances of a ring pessary.
Theseappear virtually completely anechoic because of totale
ction of
incoming acoustic waves.Implants and suburethral slings will be dis-
cussed inChapter 7.
Figure 6.10Large cyst
e with intact retrovesical angle as seen on 3D ultrasound in the midsagittal plane (top left), coronal
plane (top ri
, axial plane (bottom left), and in a rendered volume (axial plane) (bottom right). Inureteric
orifices are c
y visible and well outside the pelvis. The axial plane and rendered volume do not sh
se
they are situated well beeoh
atus. (Dietz HP. Pelvic Floor Ultrasound. Current Medical Imaging Reviews 2006; 2: in print,
Bentham Publishers.)
Figure 6.11Marked asymmetry of prolapse as seen in the axial plane. The left pubovisceral muscle
is globally impaired, likely because ofh
, with asymmetriclopmeent of recto- and
enterocele on Valsalva.
Chapter6 Axial Plane Imaging87
Figure 6.12A rendered volume of a patient with a second-degree rectocele. The hyperechoic
structure of th
ctocele is s
to fill a large part of the hiatus. There also is a suburethral tape.
(Dietz HP. P
Floor Ultrasound. Current Medical Imaging Reviews 2006; 2: in print, Bentham
Publishers, with permission.)
Figure 6.13The com
x appearance of a Gartner cyst on 3D ultrasound, mimicking a cystocele on clinical examination.
88 H.P. Dietz
Figure 6.14Prolapse pessaries may cause unusual and distinct sonographic patterns. In this case, a silicone ring pessary results
in complete reflection (and refraction) of incoming soundwaves, resulting in anechoic areas encompassing the pessary and an
acoustic shadow which is evident in the midsagittal and the coronal plane.
References
1. Wisser J, Scear G, Kurmanavicius J, Huch R, Huch A. Use of 3D ultrasound as
a new approach to assess obstetrical trauma to the pe
oor. Ultraschall Med
1999;20(1):15…18.
2. Dietz HP, Steensma AB, Hastings R. Three-dimensional ultrasound imaging of
the pelvic ”oor: the effectof parturition on paravaginal support structures.
Ultrasound Obstet Gy
col 2003;2
6):589…595.
3. Khullar V, Cardozo L. Three-dimensional ultrasound in urogynecology. In:
Merz E, ed. 3-D Ultrasound in Obstetrics and Gynecology. Philadelphia: Lip-
pincott Williams & Wilkins Healthcare; 1998:65…71.
4. DeLancey JO, K
ney R, Chou Q, Speights S, Binno S. The appearance of
levator ani muscle abnormalities in magnetic resonance images after vaginal
delivery. Obstet Gy
col 2003;101(1):46…53.
5. Dietz HP, Shek C, Clarke B. Biometry of the pubovisceral muscle and levator
hiatus by three-dmensional pelvic
o
or ultrasound. Ultrasound Obstet
Gynecol 2005;25(6):580…585.
6. Dietz HP, Lanzar
e V. Levator trauma after vaginal delivery. Obstet Gynecol
2005;106(4):707…712.
Chapter6 Axial Plane Imaging89
7. Fielding JR, Dumanli HŞchreyer AG,
al. MR-based thre-dimensional mod-
eling of the n
rmal pelvic ”oor in women: quanti“ cation of muscle mass. AJR
Am J Roentgenol 2000;174(3):657…660.
8. Tunn R, DeLa
ey JO, Ho
rd D, Thorp JM, Ashton-Miller JA, Quint LE. MR
imaging of levatorani musclerecovery following vaginal delivery. Int Urogy-
necol J 1999;10(5):300…307.
9. DeLanceyJO. Anatomy.In: Cardozo L, Staskin D, eds. Textbook of Female
Urology and Urogynaecology. London: Isis Medical Media; 2001:112…124.
10. Bary C, Dietz HP, Rane A. An independent audit of mesh repair for the treat-
ment of rectocele. 34th An ual Scienti“c Meeting of the International Conti-
nence Society 2004, Paris, France. Abstract 435.
11. Gainey HL. Postaprtum observation of pelvic tissue damage. Am J Obstet
Gynecol 1943;46:457…466.
12. Dietz HP, Hay-Smith J, Hyland G. Vaginal palpation and 3D pe
oor ultra-
sound in the diagnosi of avulsion defects of the levator ani. Neurourol Urodyn
2006;25(5):424…427.
13. Kearny R, Miller JM, Delancey JO. Interrater reliability and physical examina-
tion of the pubovisceral portion of the levator ani muscle, validity comparisons
using MR imaging. Neurourol Urodyn2006;25(1):50…54.
14. Diez HP, Steensma AB. The prevalence of major abnormalities of the levator
ani in urogynaecological patients.
J Obstet Gynaecol 2005;113:1…5.
15. Hoye L, Schierlitz L, Zou K, Flesh G, Fielding JR. Two- and 3-dimensional
MRI comparison of levatr ani structure, volume, and integrity in women
with stress inco
inence and prolap
. Am J Obstet Gynecol 2001;185(1):
11…19.
16. Kearny R, Miller J, Ashton-Miller J, Delancey J. Obstetric factors associated
with levator ani musle injury after vaginal birth. Obstet Gynecol 2006;107(1):
144…149.
17. AdekanmiOA, Freeman R,
ckett M, Jackson S. C
ocele: does anterior
repair fail because we fail to correct the fascial defects? A clinical and radiologi-
cal study.Int Urogynecol J 2005;16(S2):S73.
18. Diez HP. The classc“ation of major m
rphological abnormalities of the pubo-
visceral muscle. ICS 2006, Christchurch. Abstract.
19. DeLancey
. The anatomy of the pelvico”or. Curr Opin Obstet Gynecol 1994;
6(4):313…316.
20. Kuo H. The relationships of urethral and pelvi
oor muscles and the urethral
pressure meas
ements in women with stre
urinary incontinence. Eur Urol
2000;37(2):149…155.
21. Reisin
r E, Stummvoll W. Visualization of the endopelvic fascia by transrectal
three-dimensional ultasound. Int Urogynecol J 2006;17:165…169.
22. Ostrzenski A, Osborne NG. Ultraso
raphy asa screening tool for paravagi-
nal defects in wmen with stress incontinence: a pilot study. Int Urogynecol J
1998;9(4):195…199.
23. Martan A, MasataJ, Halaska M, Otcenasek M, Svabik K. Ultrasound imaging
of paravaginal defects in women with stress incontinence before and after
paravaginal defect repair. Ultrasou
Obstet Gyncol 2002;1
5):496…500.
24. Nguyen JĶHall CD, Taber E, Bhatia NN. Sonographic diagnosis of paravaginal
defects: a stan
rdization of technique. Int Urogynecol J 2000;11(6):341…345.
25. Diez HP, Pang S, Korda A, Benness C. Paravaginal defects: a comparison
of clinical examination and 2D/3D ultrasound imaging. Aust N Z J Obstet
Gynaecol 2005;45:187…190.
26. Se
l JL, Vassallo BJ, Kleeman SD, Silva WA, Karram MM. Paravaginal defects:
prevalence and accuracy of preoperative detection. Int Urogynecol J 2004;15(6):
378…383.
90 H.P. Dietz
27. Whiteside JL, Barber MD, Paraiso MF, Hugney CM, Walters MD. Clinical evalu-
ation of anterior vaginal wall support defects: interexaminer and intraexam-
iner reliability. Am J ObsteG ynecol 2004;191(1):100…104.
28. Khullar V, Salatore S, Cardozo LD. Three dimensional ultrasound of the
urethra and urethral pressure proles. Int Urogynecol J 1994;5(S1):319.
29. Athanasiou S, Khullar V, Boos K, Salvatore S, Cardozo L. Imaging the urethral
sphincter with three-dimensional
trasound. Obstet
necol
1999;94(2):
295…301.
30. Schaer
, Schmid T, Peschers U, Delancey JO. Intraurethral ultrasound cor-
related with urethral histology. Obstet Gynecol 1998;91(1):60…64.
7
Imaging of Implant Materials
Hans Peter Dietz
Suburethral Slings
The imaging of synthetic implants may yet prove to be a major factor in the
uptake ofpelvic ”oor ultrasound in cinical practice, in particular because
currently used mesh implants seemto be much more difcult (if not
1…3Syn-
thetic suburethral slings such as the tensionless vaginal tape (TVT), supra-
pubic arc tape
(Sparc), intravaginal slingplasty
(IVS), Monarc, and
transobturator TVT (TOT) have becomevery popular during the last 10
years4…7and are now the primary anti-incontinence procedures in many
developed countries. These slings are not without their problems, even if
biocompatibility is markedly betterthan for previously used synthetic
slings, a
d they differ from each other in someimportant aspects.
Imaging may be indicated in research, in order to determine location and
function of suchslings, and possibly even for assessing in vivo biomechani-
cal characteristics. Clinically, compli
ions such as re
rrence of stress
incontinence, voiding dysfunction,
osion, and postoperative symptoms
of the irritablebladder may bene“t from imaging assessment. Often, patients
will not remember the exact naturof previous incontinence or prolapse
surgery, and implants may be iden
ed in women whoare not aware of
their presenc, let alone their type.
Allografts such asPelvicol are impossible tvisualize after as short a
time as 2 monhs, and the echogenicity of fascial grafts seems to vary
widely. In contrast, most of the modern synthetic implant materials are
highly echogenic,with TVT, Spac, TOT, and Monar
usually being more
clearly visble thanthe IVS. Three-dimnsional (3D) ultrasound canlocate
the implant over its entire intrapelvic cours8,from the pubic rami to
behind the uethra, and bac
up on the contralateral side (ee Figure 7.1
and Case 14
the Appendix).
Variations in placement such as asymmetry, varying width, the effect of
tape division, ad tape twisting can be visualized (see Figure 7.2). The dif-
ference betw
n transobturator tapes and TVT-type implants, d
cult to
distinguish on 2D imaging (see Figu7e.3), is reaily apparenton rendered
volumes (see Figure 7.4 and Cases 11 and 14 of the Appendix). Another way
91
92 H.P. Dietz
Figure
7.1Rendered volume, axial
plane, sho
g the levator hiatus and a
TVT sur
nding te urethra. There is
a localized abnormality of the right
levatr ani that is of uncertain signifi-
cance. (From DieUz
trasound Imaging
of the Pelvic Floor: 3D aspects. Ultrasound
Obstet Gynecol 23
(6):615
5, with
permission.)
Figure 7.2Pelvic floor
ultrasound can document
vaiations in tape
placement, especially in
the axlaplane: usual
appearan
(A), very
tight placem
(B), tape
twisting(C, and findings
after tape division (arrow)
(D). (Modified from: Dietz
HP, Wilson PD. The Iris
effect: How 2D and 3D
volume uatsound can
help us understand anti-
incontinence procedures.
Ultrasound Obstet Gynecol
2004;23:2
271, with
permission.)
Chapter7 Imaging of Implant Materials93
Figure 7.3Transretzius tapes (TVT, IVS, Sparc, etc.) and transobturator tapes (Monarc, TOT) are impossible to distinguish in the
midsagittal plane. The left-hand images are taken at rest, the right ones on maximal Valsalva. (FrRaneietz HP, Barry C, Lim Y,
A (2006) TVT vs Monarc: a comparative study. Int Urogynecol J Pelvic Dysfunct DOI 10.1007/s00192-006-0065-2.)
Figure 7.4The distin
n between transobturator tapes and transretzius tapes is obvious in the axial plane. (From Dietz HP, Barry
C, Lim Y, Rane A (2006M
onar
a comparative study. Int Urogynecol J Pelvic Dysfunct DOI 10.1007/s00192-006-0065-2.)